Professional Documents
Culture Documents
Aortic Regurgitation Physical Signs
Uploaded by
Malueth Angui0 ratings0% found this document useful (0 votes)
9 views2 pages1) Aortic regurgitation occurs when the aortic valve leaflets do not close properly, allowing blood to flow back into the left ventricle.
2) Over time, the left ventricle enlarges and the walls thicken to compensate for the increased volume load, maintaining normal wall stress.
3) Eventually, the left ventricle transitions to a decompensated state with spherical shape and reduced function, leading to heart failure symptoms.
Original Description:
Original Title
AORTIC REGURGITATION.doc
Copyright
© © All Rights Reserved
Available Formats
DOC, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Document1) Aortic regurgitation occurs when the aortic valve leaflets do not close properly, allowing blood to flow back into the left ventricle.
2) Over time, the left ventricle enlarges and the walls thicken to compensate for the increased volume load, maintaining normal wall stress.
3) Eventually, the left ventricle transitions to a decompensated state with spherical shape and reduced function, leading to heart failure symptoms.
Copyright:
© All Rights Reserved
Available Formats
Download as DOC, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
9 views2 pagesAortic Regurgitation Physical Signs
Uploaded by
Malueth Angui1) Aortic regurgitation occurs when the aortic valve leaflets do not close properly, allowing blood to flow back into the left ventricle.
2) Over time, the left ventricle enlarges and the walls thicken to compensate for the increased volume load, maintaining normal wall stress.
3) Eventually, the left ventricle transitions to a decompensated state with spherical shape and reduced function, leading to heart failure symptoms.
Copyright:
© All Rights Reserved
Available Formats
Download as DOC, PDF, TXT or read online from Scribd
You are on page 1of 2
AORTIC REGURGITATION Physical signs
Background: Hemodynamically severe AR causes a widened
Primary disease of the aortic valve leaflets, the wall of the pulse pressure, often greater than 100 mm Hg,
aortic root, or both may cause aortic regurgitation (AR). associated with a low diastolic pressure, often less
Pathophysiology: than 60 mm Hg.
-Chronic AR produces left ventricular (LV) volume
overload that leads to a series of compensatory changes,
including LV enlargement and eccentric hypertrophy. The de Musset sign is when patients' heads
-The enlarged ventricle is more compliant and is well suited frequently bob with each heartbeat.
to deliver a large stroke volume.
-The dilated left ventricle can accommodate increased end- The Corrigan pulse is when patients' pulses are
diastolic volume and deliver a larger stroke volume to of the water-hammer or collapsing type, with
compensate for the regurgitant aortic flow. abrupt distention and quick collapse.
-Wall thickness must increase to compensate for the
increased ventricular dimensions. These compensatory The Quincke sign is when light transmitted
changes are necessary to minimize or normalize wall stress
through the patient's fingertip shows capillary
according to the Laplace law (ie, wall tension/stress is
pulsations.
related to the product of intraventricular pressure and radius
divided by wall thickness).
- Increased wall thickness hypertrophy observed in a The Hill sign is when popliteal cuff systolic
volume-overload state usually is eccentric, as opposed to pressure exceeds brachial cuff pressure by more
concentric hypertrophy observed in a pressure-overload than 60 mm Hg.
state (ie, aortic stenosis).
-The increased myocardial mass in a hypertrophic heart The Duroziez sign is when a systolic murmur is
enables individual sarcomeres to shorten to a normal heard over the femoral artery when compressed
degree. proximally and when a diastolic murmur is heard
-As long as LV wall stress is maintained in the normal when the femoral artery is compressed distally.
range, the LV preload reserve, contractility, and ejection
fraction (EF) remain within the normal range. This is the The Müller sign is systolic pulsations of the
chronic compensated stage. During this phase of the uvula.
disease, most patients remain asymptomatic for decades
because chronic AR generally is a slow and insidious
disease with very low morbidity during a long The Traube sign (also called pistol-shot sounds)
asymptomatic phase. refers to booming systolic and diastolic sounds
-With time, transition from a compensated to a heard over the femoral artery.
decompensated state marks the progression of the disease.
Progressive LV enlargement beyond that required by the The apical impulse in chronic AR is diffuse,
valvular regurgitation occurs and is associated with a hyperdynamic, and displaced inferiorly and
change of the left ventricle from an elliptical shape to a leftward.
spherical shape.
-The cause of this pathologic dilatation is not well
understood, but loss of the collagen support system that acts S3 gallop correlates with development of LV
as a skeleton for the heart may play a substantial role. These dysfunction.
maladaptive changes in the interstitial of the heart are an
intricate part of the LV hypertrophy process. In addition, The typical diastolic murmur of AR has a
diminished coronary flow reserve in this hypertrophied decrescendo shape. A high-frequency early
ventricle is thought to result in chronic subendocardial diastolic murmur often occurs in mild AR,
ischemia, even in the absence of epicardial coronary artery whereas a rough holodiastolic or decrescendo
disease (CAD). Eventually, subendocardial necrosis and diastolic murmur occurs more commonly in
fibrosis occur, along with disruption of the collagen support severe AR. The volume and velocity of blood
system, with loss of LV systolic function. The across the incompetent aortic valve tapers off in
neurohormonal response complicates the disease state mid-to-last diastole as the aortic and LV pressures
further by its excessive growth stimuli, which are thought to equilibrate. The diastolic murmur of AR is
be partially responsible for apoptosis (programmed cell usually best heard adjacent to the sternum in the
death) of the remaining functional myocytes. second to fourth left intercostal space. A
concomitant systolic ejection murmur is common
The vicious cycle continues until the decompensated stage in moderate-to-severe AR
develops over many years. Progressive LV enlargement,
spherical LV shape, increased wall stress, decline in the The murmur associated with acute AR may not be
contractility and EF, increased afterload, and decreased impressive. If cardiac decompensation is present,
the diastolic murmur of acute AR may be very
diastolic compliance with a rise in end-diastolic pressure soft and surprisingly short.
characterize this stage. Frequently, development of
congestive symptoms heralds this stage, but an insidious Antegrade flow across the mitral valve is thought
deterioration of ventricular function may occur without to cause an Austin Flint murmur, which is a
overt clinical signs. mid- and late-diastolic apical low-frequency
murmur or rumble. The rumble occurs during
In acute AR, the normal-sized left ventricle poorly tolerates rapid closure of the mitral valve as flow velocity
the sudden large volume imposed on it. The left ventricle is increasing across the valve and LV diastolic
poorly accommodates the abrupt increase in end-diastolic pressure is rising rapidly because of severe aortic
volume, and diastolic filling pressure increases rapidly and reflux. Its presence indicates severe AR.
dramatically. This leads to an acute decrease in forward
stroke volume, and, although tachycardia develops as a
compensatory mechanism to maintain cardiac output, this
often is insufficient. The rise in LV filling pressure is
transmitted to the left atrium, pulmonary veins, and
pulmonary capillaries, leading to pulmonary edema and
congestion. Acute AR usually is severe and rapidly leads to
LV decompensation and/or failure and cardiogenic shock
You might also like
- Step 1 ShartzDocument333 pagesStep 1 ShartzDaniella Vazquez100% (1)
- CardiologyDocument62 pagesCardiologysee yinNo ratings yet
- 4.3.aortic StenosisDocument61 pages4.3.aortic StenosisMuh BluNo ratings yet
- Heart Murmurs Topic Review - From Description To AuscultationDocument15 pagesHeart Murmurs Topic Review - From Description To AuscultationRapmle PrasadNo ratings yet
- Medicine in Brief: Name the Disease in Haiku, Tanka and ArtFrom EverandMedicine in Brief: Name the Disease in Haiku, Tanka and ArtRating: 5 out of 5 stars5/5 (1)
- Aortic RegurgitationDocument19 pagesAortic RegurgitationsunilgenextNo ratings yet
- Wk7 PLP Cardiovascular Disorder Part 1,2,3,4Document210 pagesWk7 PLP Cardiovascular Disorder Part 1,2,3,4claire yowsNo ratings yet
- Aortic StenosisDocument20 pagesAortic Stenosisvasarhely imolaNo ratings yet
- Pharmacology SamplexDocument12 pagesPharmacology SamplexLiezel Dejumo BartolataNo ratings yet
- DimensionsDocument103 pagesDimensionslaurariton100% (1)
- Chemotherapy: Chemotherapy, in Its Most General Sense, Refers To Treatment of Disease byDocument42 pagesChemotherapy: Chemotherapy, in Its Most General Sense, Refers To Treatment of Disease byMalueth AnguiNo ratings yet
- Rheumatic Heart DiseaseDocument39 pagesRheumatic Heart DiseaseRezwanul Hoque Bulbul100% (1)
- Valvular Heart DiseaseDocument27 pagesValvular Heart DiseaseOwen J. WieseNo ratings yet
- Mitral Valve Prolapse, Flailed Mitral Valve Mitral Annular CalcificationDocument33 pagesMitral Valve Prolapse, Flailed Mitral Valve Mitral Annular CalcificationcafemedNo ratings yet
- Valvular Heart DiseaseDocument73 pagesValvular Heart Diseaseindia2puppy100% (4)
- Just Walk Across The RoomDocument8 pagesJust Walk Across The Roomstuutterrs100% (1)
- Antimalarial DrugsDocument49 pagesAntimalarial DrugsMalueth Angui0% (1)
- Pathophysiology Congenital Heart Disease-1Document54 pagesPathophysiology Congenital Heart Disease-1single_ladyNo ratings yet
- PedsnotesDocument18 pagesPedsnoteskp13oyNo ratings yet
- Methodology and Specifications Guide: Crude OilDocument34 pagesMethodology and Specifications Guide: Crude Oil066709No ratings yet
- Cardiac Tamponade and ManagementDocument42 pagesCardiac Tamponade and Managementأم حمدNo ratings yet
- Multiple MyelomaDocument17 pagesMultiple MyelomaAhmed AbouelwafaNo ratings yet
- Lisa-Operation Manual: Installation and Operation Instructions (Part B)Document41 pagesLisa-Operation Manual: Installation and Operation Instructions (Part B)majdNo ratings yet
- Presentation RAB Jalan Dan Jembatan PT. GUNUNG TANGINDocument9 pagesPresentation RAB Jalan Dan Jembatan PT. GUNUNG TANGINMuhammad Rabbil AlbadriNo ratings yet
- Bright: Insidecrochet - Co.ukDocument100 pagesBright: Insidecrochet - Co.ukЕкатерина Матушинец100% (2)
- Technology and The Transformation of Performance - Chris Salter PDFDocument49 pagesTechnology and The Transformation of Performance - Chris Salter PDFFelipe Merker Castellani100% (1)
- Aortic RegurgitationDocument134 pagesAortic RegurgitationAbnet WondimuNo ratings yet
- Angelina A Joho MSC in Critical Care and TraumaDocument50 pagesAngelina A Joho MSC in Critical Care and TraumaZabron LuhendeNo ratings yet
- Valvular Heart Disease1Document80 pagesValvular Heart Disease1Abnet WondimuNo ratings yet
- IVMS Heart and Lung Auscultation Sounds NotesDocument7 pagesIVMS Heart and Lung Auscultation Sounds NotesMarc Imhotep Cray, M.D.No ratings yet
- Differential Diagnosis of The Diseases With Systolic MurmursDocument2 pagesDifferential Diagnosis of The Diseases With Systolic MurmursXiang Yun TanNo ratings yet
- Valvular Heart Disease: Etiology PathophysiologyDocument34 pagesValvular Heart Disease: Etiology PathophysiologyensiNo ratings yet
- Pericardial Disease: Adel Hasanin Ahmed 1Document5 pagesPericardial Disease: Adel Hasanin Ahmed 1Shaz ChindhyNo ratings yet
- Acyanotic Heart DiseaseDocument18 pagesAcyanotic Heart DiseaseShishir ShresthaNo ratings yet
- Kuliah MITRAL STENOSISDocument19 pagesKuliah MITRAL STENOSISekaseptiani312No ratings yet
- Mid-Systolic Ejection: Time Condition DescriptionDocument3 pagesMid-Systolic Ejection: Time Condition DescriptionZahrosofi AhmadahNo ratings yet
- Bahan Refrat Anes!!!!Document6 pagesBahan Refrat Anes!!!!Ajeng Oktri DewantiNo ratings yet
- Aortic RegurgitationDocument2 pagesAortic RegurgitationJustine CastilloNo ratings yet
- Valvular Heart DiseaseDocument5 pagesValvular Heart DiseaseElyas MehdarNo ratings yet
- 28 Valvular Heart Disease DR - YusraDocument46 pages28 Valvular Heart Disease DR - YusraSurya ArhNo ratings yet
- Mitral Stenosis Etiology and TreatmentDocument19 pagesMitral Stenosis Etiology and TreatmentAdi TrisnoNo ratings yet
- Department of Internal Medicine III Aortic Stenosis: - Rajkumar Subasaravanan Subgroup "12"Document51 pagesDepartment of Internal Medicine III Aortic Stenosis: - Rajkumar Subasaravanan Subgroup "12"Suba Saravanan 12No ratings yet
- Cardiac TamponadeDocument6 pagesCardiac TamponadeVicky XieNo ratings yet
- Aortic StenosisDocument8 pagesAortic Stenosisdr.moni.co.ukNo ratings yet
- Aortic Stenosis Causes, Symptoms, and TreatmentDocument4 pagesAortic Stenosis Causes, Symptoms, and TreatmentSukuria UsmanNo ratings yet
- 4 Valvular Heart Disease#36f7Document40 pages4 Valvular Heart Disease#36f7Natasha LiberisNo ratings yet
- Cardiovascular Exam: Examination Includes The FollowingDocument37 pagesCardiovascular Exam: Examination Includes The FollowingyayayanizaNo ratings yet
- Aortic RegurgitationDocument14 pagesAortic RegurgitationKamalAbdurrosidRosidNo ratings yet
- Aortic Stenosis - LecturioDocument13 pagesAortic Stenosis - Lecturiokujtimepira2No ratings yet
- Right Ventricular Failure Causes and PathophysiologyDocument4 pagesRight Ventricular Failure Causes and PathophysiologyZakwan AhmadNo ratings yet
- Congenital Heart Disease ExplainedDocument74 pagesCongenital Heart Disease ExplainedKeith LajotNo ratings yet
- Heart Failure (Muir)Document5 pagesHeart Failure (Muir)Ganashiam NadarasaNo ratings yet
- Collapsing PulseDocument3 pagesCollapsing Pulsemartiqo50% (2)
- Aortic Regurgitation by DR DilmoDocument37 pagesAortic Regurgitation by DR Dilmosinan kNo ratings yet
- The Third Heart Sound, Murmurs from Valvular Lesions, and Associated Heart ConditionsDocument2 pagesThe Third Heart Sound, Murmurs from Valvular Lesions, and Associated Heart ConditionsAIKA BAYANo ratings yet
- Cardiovascular System Step 1Document6 pagesCardiovascular System Step 1tomisin99gordonNo ratings yet
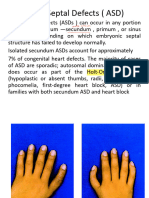
- Atrial Septal Defects ( ASD)Document30 pagesAtrial Septal Defects ( ASD)wissam salimNo ratings yet
- Pathophys VHD-Final (Budi S. Pikir)Document155 pagesPathophys VHD-Final (Budi S. Pikir)Muhammad DaviqNo ratings yet
- 2 Valvular Heart Disease1Document87 pages2 Valvular Heart Disease1Danny DesuNo ratings yet
- Aortic Regurgitation: Vitrag24-Www - Medic ComDocument68 pagesAortic Regurgitation: Vitrag24-Www - Medic ComAlshare NisreenNo ratings yet
- Mitral Regurgitation Etiology and Pathophysiology: Physical ExaminationsDocument11 pagesMitral Regurgitation Etiology and Pathophysiology: Physical ExaminationsDelmy SanjayaNo ratings yet
- Aortic RegurgitationDocument16 pagesAortic Regurgitationrobby zayendraNo ratings yet
- RHEUMATIC HEART DISEASE GUIDEDocument30 pagesRHEUMATIC HEART DISEASE GUIDEDhiraj PantNo ratings yet
- Mitral StenosisDocument95 pagesMitral StenosisAbnet WondimuNo ratings yet
- Aortic Regurgitation: Group IvDocument28 pagesAortic Regurgitation: Group IvKim Michael PabatangNo ratings yet
- 3 - Valvular Heart DiseasesDocument43 pages3 - Valvular Heart DiseasesHamzehNo ratings yet
- Approach To Cardiac MurmursDocument11 pagesApproach To Cardiac Murmurstouthang0074085No ratings yet
- Case Scenerio: DR Sourath Munir Malkani Fcps-Ii TraineDocument31 pagesCase Scenerio: DR Sourath Munir Malkani Fcps-Ii TraineSoonh ChannaNo ratings yet
- Valvular Heart Disease 2Document46 pagesValvular Heart Disease 2Topea BogdanNo ratings yet
- Diagnosis Depend On: 1-Clinical Features: - Palpation - Auscultation 2 - CXR: - Chamber Enlargement - Plethoric LungDocument11 pagesDiagnosis Depend On: 1-Clinical Features: - Palpation - Auscultation 2 - CXR: - Chamber Enlargement - Plethoric LungYasir Al-KhateebNo ratings yet
- Other Anti-HivDocument24 pagesOther Anti-HivMalueth AnguiNo ratings yet
- ART Classification and UsesDocument22 pagesART Classification and UsesMalueth AnguiNo ratings yet
- Antifungal Drugs: A Guide to Classes, Mechanisms & PrecautionsDocument66 pagesAntifungal Drugs: A Guide to Classes, Mechanisms & PrecautionsMalueth AnguiNo ratings yet
- TUBERCULOSIS TREATMENT DRUGSDocument29 pagesTUBERCULOSIS TREATMENT DRUGSMalueth AnguiNo ratings yet
- Hiv HaartDocument12 pagesHiv HaartMalueth AnguiNo ratings yet
- Anti-infective drugs overviewDocument31 pagesAnti-infective drugs overviewMalueth AnguiNo ratings yet
- Protease Inhibitors (Pi) : Anyika CelpherDocument22 pagesProtease Inhibitors (Pi) : Anyika CelpherMalueth AnguiNo ratings yet
- Nnrtis: Nonnucleoside Reverse Trancriptase InhibitorsDocument12 pagesNnrtis: Nonnucleoside Reverse Trancriptase InhibitorsMalueth AnguiNo ratings yet
- Antiviral DrugsDocument13 pagesAntiviral DrugsMalueth AnguiNo ratings yet
- Antiretroviral Therapy: Pharmacology: Cristina Gruta, PharmdDocument47 pagesAntiretroviral Therapy: Pharmacology: Cristina Gruta, PharmdMalueth AnguiNo ratings yet
- Head & Neck TumoursDocument15 pagesHead & Neck TumoursMalueth AnguiNo ratings yet
- Human Immunodeficiency VirusDocument24 pagesHuman Immunodeficiency VirusMalueth AnguiNo ratings yet
- Antiviral TherapyDocument19 pagesAntiviral TherapyMalueth AnguiNo ratings yet
- K 17 Colorectal CarcinomaDocument63 pagesK 17 Colorectal CarcinomaMalueth AnguiNo ratings yet
- Antiviral AgentsDocument54 pagesAntiviral AgentsMalueth AnguiNo ratings yet
- Malignant Lymphoma 2Document54 pagesMalignant Lymphoma 2Malueth AnguiNo ratings yet
- Cancer ChemotherapyDocument97 pagesCancer ChemotherapyMalueth AnguiNo ratings yet
- Prostate CancerDocument67 pagesProstate CancerMalueth AnguiNo ratings yet
- Head & Neck TumoursDocument15 pagesHead & Neck TumoursMalueth AnguiNo ratings yet
- Hepatocellular CarcinomaDocument10 pagesHepatocellular CarcinomaMalueth AnguiNo ratings yet
- Local Anaesthetic AgentsDocument16 pagesLocal Anaesthetic AgentsMalueth AnguiNo ratings yet
- Local Anaesthetics ExplainedDocument24 pagesLocal Anaesthetics ExplainedMalueth AnguiNo ratings yet
- Understanding General AnestheticsDocument21 pagesUnderstanding General AnestheticsMalueth AnguiNo ratings yet
- Targeted Therapy: Specific Targeted Molecules Needed For Carcinogenesis and Tumor GrowthDocument9 pagesTargeted Therapy: Specific Targeted Molecules Needed For Carcinogenesis and Tumor GrowthMalueth AnguiNo ratings yet
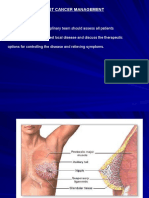
- Breast Cancer PresentationDocument71 pagesBreast Cancer PresentationMalueth AnguiNo ratings yet
- 2 INTRAVENOUS ANESTHESIA EgertonDocument21 pages2 INTRAVENOUS ANESTHESIA EgertonMalueth AnguiNo ratings yet
- 3 GENERAL ANAESTHETICS EgertonDocument59 pages3 GENERAL ANAESTHETICS EgertonMalueth AnguiNo ratings yet
- Spare Parts Quotation For Scba & Eebd - 2021.03.19Document14 pagesSpare Parts Quotation For Scba & Eebd - 2021.03.19byhf2jgqprNo ratings yet
- Daftar PustakaDocument2 pagesDaftar PustakaJohny Iskandar Arsyad NstNo ratings yet
- SC3 User Manual - V1.06 PDFDocument196 pagesSC3 User Manual - V1.06 PDFJoeNo ratings yet
- Thermal Engineering IDocument30 pagesThermal Engineering IRamphani NunnaNo ratings yet
- Amended Consent Decree and Draft Interim Action Work Plan For The Hansville General R Men Store Site - Available Fo Public Review and Com TDocument4 pagesAmended Consent Decree and Draft Interim Action Work Plan For The Hansville General R Men Store Site - Available Fo Public Review and Com TCommunityNewsNo ratings yet
- Critical Planning Issues in MTODocument2 pagesCritical Planning Issues in MTOAzhar QadriNo ratings yet
- Asus Prime b250m Plus RGDocument13 pagesAsus Prime b250m Plus RGRenattech SilvaNo ratings yet
- Effects of Flooding on Dagupan City TourismDocument4 pagesEffects of Flooding on Dagupan City TourismTaehyung KimNo ratings yet
- Orallichenplanus 170929075918Document40 pagesOrallichenplanus 170929075918Aymen MouradNo ratings yet
- 2004 Timbre To DissonanceDocument4 pages2004 Timbre To DissonancetgraubaenaNo ratings yet
- Zeroing Neural Networks, An Introduction To, A Survey Of, and Predictive Computations For Time-Varying Matrix ProblemsDocument24 pagesZeroing Neural Networks, An Introduction To, A Survey Of, and Predictive Computations For Time-Varying Matrix ProblemsgoatcockNo ratings yet
- Manual Sony HCD-SH2000 (88 Páginas)Document2 pagesManual Sony HCD-SH2000 (88 Páginas)Alberto CaseroNo ratings yet
- PDFDocument110 pagesPDFBikash NayakNo ratings yet
- Carte Tehnica Panou Fotovoltaic Cu Celule Policristaline Eging 250 WDocument1 pageCarte Tehnica Panou Fotovoltaic Cu Celule Policristaline Eging 250 WConstantin CilibiuNo ratings yet
- Thermal Physics SLDocument4 pagesThermal Physics SLIBstudent10No ratings yet
- Computer Graphics Chapter-1Document61 pagesComputer Graphics Chapter-1abdi geremewNo ratings yet
- 1822 B.E Cse Batchno 154Document53 pages1822 B.E Cse Batchno 154maniuyyala65No ratings yet
- Ahmedabad BRTS strategiesDocument3 pagesAhmedabad BRTS strategiesVishal JainNo ratings yet
- Report NovelDocument12 pagesReport NovelHasan Moh'd Al AtrashNo ratings yet
- CivilFEM GeotechnicaDocument107 pagesCivilFEM GeotechnicaRR886No ratings yet
- 2.2 - NDEP-C1574-5-6-7-8 - Rev.0 NDE Procedures Book PDFDocument59 pages2.2 - NDEP-C1574-5-6-7-8 - Rev.0 NDE Procedures Book PDFGeorge JhonsonNo ratings yet