Professional Documents
Culture Documents
Pancreas: Module 11: Endocrine System
Uploaded by
LANCE GILL TolentinoOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Pancreas: Module 11: Endocrine System
Uploaded by
LANCE GILL TolentinoCopyright:
Available Formats
MODULE 11: ENDOCRINE SYSTEM
Pancreas
JULIE ANNE L. GABAT MD, FPCP, DPSEDM
03/31/2020 (08:00-17:00)
PHYSIOLOGY
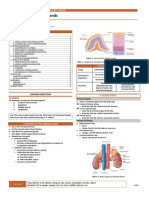
TABLE OF CONTENTS The pancreas is an elongated, accessory digestive gland that lies
retroperitoneally, transversely crossing L1 and L2 vertebra (Moore, 265).
I. OVERVIEW OF THE PANCREAS ................................................................................... 1 It is divided into four parts: head, neck, body and tail (Moore, 266).
A. STRUCTURES ....................................................................................................... 1 It is located in the curvature of the duodenum (12.09, 2023).
B. CELL TO CELL COMMUNICATION........................................................................ 1 • Made up of two types of tissues:
II. INSULIN STRUCTURE & SYNTHESIS ........................................................................... 2
o Exocrine: Pancreatic Acini
A. PROPERTIES OF INSULIN ..................................................................................... 2
B. SYNTHESIS OF INSULIN ....................................................................................... 2 Greater bulk of the pancreas
C. METABOLISM OF INSULIN AND C-PEPTIDE ........................................................ 2 Comprised of Acini, which produce the alkaline fluid and digestive
D. OTHER BETA CELL SECRETIONS .......................................................................... 3 juices that is secreted into the ductal system (pancreatic duct) to
III. PHYSIOLOGY OF INSULIN SECRETION ...................................................................... 3 facilitate digestion of food
A. GLUCOSE STIMULATED INSULIN SECRETION...................................................... 3 RECALL: Pancreatic duct is joined by the common bile duct, and
B. FACTORS THAT AFFECT INSULIN SECRETION...................................................... 3 eventually drains into the duodenal papilla.
C. INCRETINS ........................................................................................................... 3
Location of acini: Surrounds the ducts
D. INSULIN SECRETION............................................................................................ 4
IV. PHYSIOLOGY OF INSULIN ACTION ........................................................................... 5 o Endocrine: Islets of Langerhans
A. INSULIN RECEPTOR ............................................................................................. 5 Localized in Islets of Langerhans that are most commonly found in
B. STEPS OF INSULIN ACTION.................................................................................. 5 the tail of pancreas.
C. REGULATION OF INSULIN RECEPTION ................................................................ 5 Secretes hormones directly into the bloodstream
D. INSULIN SIGNALING ............................................................................................ 5 Location of Islets: Near the capillaries
E. INSULIN AND ITS METABOLIC EFFECT................................................................. 5
• Islets of Langerhans
V. ACTIONS OF INSULIN ................................................................................................ 5
A. EFFECT OF CARBOHYDRATE METABOLISM ........................................................ 5 o Approximately 1-2 million islets with 2,500 cells per islet
B. EFFECT ON FAT METABOLISM ............................................................................ 6 o Ovoid and organized around small capillaries into which its cells secrete
C. EFFECT ON PROTEIN METABOLISM .................................................................... 6 their hormones
D. OTHER ACTIONS ................................................................................................. 6 o Richly vascularized, and receives 10% of pancreatic blood flow
VI. ACTIONS OF INSULIN ON TISSUES ........................................................................... 6 o Accounts for ONLY 1% of the pancreatic mass
A. LIVER CELLS ......................................................................................................... 6 o Contain 4 cell types: Beta, Alpha, Delta and F/PP Cells
B. MUSCLE CELLS..................................................................................................... 7
C. ADIPOSE CELLS .................................................................................................... 7
D. TISSUES UNAFFECTED BY INSULIN ..................................................................... 7
Table 1. Cell Types in the Islets
E. METABOLISM AND EXCRETION OF INSULIN ....................................................... 7 HORMONE LOCATION
CELL TYPE % OF TOTAL
VII. GLUCAGON ............................................................................................................. 7 SECRETED
A. GLUCAGON SECRETION ...................................................................................... 7 Beta (β) Cells ≈ 60% Insulin Central
B. MECHANISM OF ACTION .................................................................................... 7 Alpha (α) Cells ≈ 25% Glucagon Periphery
VIII. DELTA CELLS: SOMATOSTATIN .............................................................................. 7 Delta (δ) Cells ≈ 10% Somatostatin Periphery
IX. F CELLS: PANCREATIC POLYPEPTIDE ........................................................................ 8
X. IMPORTANCE OF CONTROLLING BLOOD SUGAR LEVELS ......................................... 8 Pancreatic
F-cells/PP Cell < 2%
QUICK REVIEW .............................................................................................................. 8 Polypeptide
SUMMARY OF TERMS ............................................................................................. 8
SUMMARY OF PROCESSES ...................................................................................... 8
REVIEW QUESTIONS................................................................................................ 9
REFERENCES .................................................................................................................. 9
REQUIRED ............................................................................................................... 9
FREEDOM SPACE ........................................................................................................... 9
I. OVERVIEW OF THE PANCREAS
A. STRUCTURES
Figure 2. Distribution of Cells Across the Islets
B. CELL TO CELL COMMUNICATION
• Intimate relationship of cells within the islets suggests their paracrine and
counter-regulatory function
o Insulin inhibits glucagon
o Amylin inhibits insulin
o Somatostatin inhibits both glucagon & insulin
• Communication is done through:
o Gap Junctions
o Unique blood supply of the Islets
o Innervation
Figure 1. Anatomy of the Pancreas
Transcribed by TG 16: Antonio, Bantilan, Cases, Cruz, Hermoso, Lintag, Singson, Sy
YL5: 11.03
Checked by TG 4: Caraang, Dy, Gonzales, Liberato, Montaus, Ologenio, Sumang 1 of 9
Gap Junctions 2) Preproinsulin MRNA Preproinsulin synthesis
o Preproinsulin mRNA directs ribosomal synthesis (translation) of
• Connect alpha cells to each other, beta cells to each other, and alpha cells
preproinsulin, which contains 4 peptides:
to beta cells
Signal Peptide
• Allows rapid cell to cell communication via ionic current flow or transfer of
Alpha Chain
molecules (up to 1,000 MW)
Beta Chain
Connecting Peptide (C-Peptide)
Unique Blood Supply 3) Preproinsulin Proinsulin
• Islets receive 10% of total pancreatic blood flow o Preproinsulin (11,500 MW) is cleaved by microsomal enzymes in the
• Scheme: Arterioles enter the core of the islet and its fenestrated endoplasmic reticulum to form proinsulin
capillaries, and then converge into venules that carry blood to the rim of Amino-terminal signal peptide was removed almost immediately
the islet. after synthesis
• Important so venous blood carries insulin from beta cells to alpha and delta Proinsulin consists of: alpha and beta chains, C-peptide
cells found in the periphery of the islets (hormone-rich blood bathes 4) Proinsulin Transport to Golgi
structures surrounding the cell source for regulatory purposes) o Proinsulin (9,000 MW) is transported to the Golgi apparatus and is
cleaved by proteases to form the active insulin and C-peptide
Innervation 5) Active insulin + C-peptide Packaging
o Active insulin (5,805 MW) and C-peptide (3,000 MW) are packaged into
• Islets are innervated by adrenergic, cholinergic & peptidergic neurons
secretory granules
• Delta cells send dendrite-like processes to beta cells (suggestive of intra- o Mature secretory granules contain insulin and C-peptide in equimolar
islet neural communication) amounts (1 C-peptide : 1 insulin molecule)
o 5-10% of the secretory products are uncleaved proinsulin
II. INSULIN STRUCTURE & SYNTHESIS 6) Insulin Release
A. PROPERTIES OF INSULIN o Both insulin and C-peptide are released into circulation in equimolar
amounts when stimulus is present
Proinsulin
• Single chain made up of 86 amino acids
• Consists of the alpha and beta chains of the insulin molecule, and a
connecting segment of 35 amino acids
Figure 4. Proinsulin Cleaved Into Active Insulin and C-peptide within a
Secretory Granule
Figure 3. Structure of Human Proinsulin C peptides and Insulin Molecules
Connected at Two Sites by Dipeptide Links
Insulin
• A small protein composed of 51 amino acids with two peptide chains joined
by a disulfide bond
o A chain: 21 amino acids
Contains an intrachain disulfide bridge that links peptides 6 and 11
o B chain: 30 amino acids
• The functional activity of insulin is lost when the two peptide chains are
split apart
• Goal: Increases blood glucose concentration
• Storage:
o Fat synthesis and storage
o Protein synthesis
o Glycogen synthesis
• Insulin is the first hormone to:
o Be isolated from animal sources that could be therapeutically
Figure 5. Synthesis of Insulin
administered to humans
o Have its mechanism of action elucidated C. METABOLISM OF INSULIN AND C-PEPTIDE
o Be measured by radioimmunoassay
o Be synthesized from a larger precursor/prohormone • Insulin circulates in free form
o Be synthesized via recombinant DNA o t1/2 (half-life) = 6 mins
o Clearance = 10-15 mins
• A gene in the short arm of chromosome 11 (part of a superfamily of genes
that encode related growth factors) directs insulin synthesis • Inactivated by insulinase in the liver (mainly), kidneys, and muscles (lesser
amount)
• C-peptide is cleared more slowly
B. SYNTHESIS OF INSULIN o Useful marker for endogenous insulin secretion
1) Transcription factors activate preproinsulin transcription o Allows discrimination between endogenous and exogenous sources of
o Unique set of transcription factors found in β cell nucleus activates the insulin
transcription of preproinsulin mRNA from the insulin gene Evaluation of hypoglycemia and Type 1 Diabetes Mellitus
YL5: 11.03 ENDOCRINE SYSTEM: Pancreas 2 of 9
B. FACTORS THAT AFFECT INSULIN SECRETION
D. OTHER BETA CELL SECRETIONS
• Islet Amyloid Polypeptide (IAPP) or amylin is a 37 amino acid peptide that Table 3. Factors and conditions that Increase or decrease insulin secretion
is secreted along with insulin (12.09, 2023).
o Released from beta cells as a satiation signal following food intake INCREASE INSULIN SECRETION DECREASE INSULIN SECRETION
o Slows down gastric emptying to prevent hypoglycemia a few hours after Increased blood glucose Decreased blood glucose
a meal; hence, it takes about 4 hours to fully digest a meal Increased blood free fatty acids Fasting
o Major component of amyloid fibrils found in islets of patients with Type Increased blood amino acids Somatostatin
2 Diabetes Mellitus Gastrointestinal hormones
(gastrin, cholecystokinin, secretin, -Adrenergic activity
Table 2. Stimulants, Amplifiers, and Inhibitors of Insulin Release gastric inhibitory peptide)
AMPLIFIERS OF Glucagon, growth hormone,
STIMULANTS OF INHIBITORS OF INSULIN Leptin
GLUCOSE-INDUCED cortisol
INSULIN RELEASE RELEASE
INSULIN RELEASE Parasympathetic stimulation
Neural: Alpha (Acetylcholine)
Enteric Hormones:
adrenergic effect of
Glucose GLP, GIP, CCK, -Adrenergic stimulation
catecholamines
Secretin, Gastrin Insulin Resistance (obesity)
Sulfonylurea drugs (glyburide and
Neural Amplifiers:
Humoral: tolbutamide)
Mannose Beta adrenergic
Somatostatin
stimulation
• Note that the following were emphasized by Doc last year:
Leucine Drugs: Diazoxide,
o Increased blood amino acids
Vagal Stimulation Phenytoin,
Amino Acids: Arginine Specifically arginine and lysine
Vinblastine,
Sulfonylureas , of glucose-stimulated insulin secretion
Colchicine
However, these do not stimulate insulin release in the absence of
glucose
III. PHYSIOLOGY OF INSULIN SECRETION o Gastrointestinal hormones
• Glucose is the key regulator of insulin secretion by the pancreatic beta-cell Specifically the incretins glucose-dependent Insulinotropic Peptide
o Glucose levels >70mg/dL (3.0 mmol/L) stimulate insulin synthesis by (GIP) and glucagon-like Peptide-1 (GLP-1)
enhancing protein translation and processing Enhance the rate of insulin release in response to oral glucose
Normal Fasting Blood Glucose: 80-90mg/dL (12.09, 2023). load
• Insulin down-regulates its own receptor by decreasing the rate of synthesis Inhibit glucagon secretion
and increasing the rate of degradation o Glucagon, growth hormone, and cortisol
These hormones have stimulatory effects on insulin secretion
A. GLUCOSE STIMULATED INSULIN SECRETION If the secretion of these hormones are prolonged and are in large
quantities, these can cause exhaustion of beta cells leading to an
• Glucose is transported into the beta cell by a facilitative glucose transporter
increased risk of diabetes mellitus
GLUT-2 (facilitated diffusion)
Glucose concentrations can also be detected by:
Glucokinase catalyzes the phosphorylation of glucose to prevent it from
Specialized neurons of the hypothalamus and brainstem
leaving the cell (12.09, 2023).
o Rate-limiting step of glucose-stimulated insulin secretion Glucose-sensing cells in peripheral locations (e.g. liver)
o Major mechanism for glucose sensing and control of amount of insulin o Parasympathetic stimulation through acetylcholine
secreted into the blood o Progesterone and Estrogen also have stimulatory effects on insulin
secretion but to a lesser extent
• Glucose is phosphorylated to glucose-6-phosphate, then oxidized with ATP
as one of the products
• ATP closes ATP SENSITIVE POTASSIUM CHANNELS C. INCRETINS
• Potassium conductance decreases and the membrane is depolarized • Released from the neuroendocrine cells of the gastrointestinal tract
Sulfonylurea drugs also inhibit potassium channels (12.09, 2023). following food ingestion
• Depolarization opens VOLTAGE-SENSITIVE CALCIUM CHANNELS • Amplifies glucose-stimulated insulin secretion and suppress glucagon
• Increased intracellular calcium causes exocytosis of vesicles and release of secretion
insulin into the pancreatic venous blood and systemic circulation • GLUCAGON-LIKE PEPTIDE-1
o The most potent incretin
o Released from the L cells in the small intestine
o Stimulates insulin secretion only when the blood glucose is above the
fasting level
Incretin analogues/pharmacologic agents that prolong activity of
endogenous GLP-1 enhance insulin secretion (12.09, 2023).
• Oral vs. Intravenous Glucose (12.09, 2023)
o Oral glucose leads to higher secretions of insulin due to the presence
of incretins
o Consequently, higher blood glucose fluctuations are observed when
intravenous glucose is administered
Figure 6. Mechanism of Glucose-Stimulated Secretion of Insulin in Beta Cells
YL5: 11.03 ENDOCRINE SYSTEM: Pancreas 3 of 9
Figure 8. Approximate Insulin Secretion at Different Plasma Glucose Levels
Prandial Insulin Secretion
• First phase
o Rapid insulin peak
o Lasts 10 minutes
o Suppresses hepatic glucose production
o Not maintained
o Decreases in 5-10 minutes but does not reach the basal level
o Facilitates phase 2 release
• Second phase
o Directly related to the level of glucose elevation
o Lasts for two hours
o Covers mealtime carbohydrates
Figure 7. The Incretin Concept o More prolonged and more pronounced
o Amount of insulin secreted in this phase is greater than first phase
Table 4. GLP-1 (Glucagon-like Peptide-1) vs GIP (Glucose-Dependent
o Comes from additional release of preformed insulin and from newly
Insulinotropic Polypeptide)
synthesized insulin from beta cells
GLP-1 GIP
• Third phase
Secreted by L-cells in the distal gut Secreted by K-cells in the proximal
o 1.5 to 3 hours after exposure to glucose
(ileum and colon) gut (duodenum)
o With a spontaneous decline in secretion to 15%-25% of the amount
Stimulates glucose-dependent Stimulates glucose-dependent
released during peak secretion
insulin release insulin release
NOTE: Insulin Secretion Before and After a Meal (12.09, 2023)
Inhibits glucagon secretion in a
o 0-60 minutes: Basal secretion (insulin release before a meal)
glucose-dependent manner
o 60 minutes onward: Postprandial secretion (insulin release after a meal)
(suppresses hepatic glucose
Enhances beta-cell proliferation
output)
and survival in islet cell lines
Enhances beta-cell proliferation
and survival in animal models and
isolated human islets
Experimentally, administration of GLP-1 above physiologic levels has
shown dose-dependent inhibition of gastric emptying (12.09, 2023).
o Furthermore, it promotes beta-cell mass through proliferative and anti-
apoptotic pathways
However, while GIP stimulates a glucose-dependent insulin response, it
does not affect gastric emptying (12.09, 2023).
o Insulinotropic activity of GIP was less in type 2 diabetic patients
o Does not appear to affect satiety or body weight
D. INSULIN SECRETION
Figure 9. Portal Insulin Secretion Before and After Meal Ingestion (arrow) in a
Basal Insulin Secretion
Representative Dog
• 50% of the total insulin secreted
• Independent of glucose intake: you produce insulin whether you eat or not Total Insulin Secretion
• Released in pulsatile manner 50% of total insulin secreted under basal conditions (12.09, 2023)
o Rapid Oscillations: occur every 8-15 minutes o 18-32 units per 24 hours (0.7 – 1.3 mg)
o Slower Oscillations: occur at periods of 80-150 minutes from insulin- Remainder is secreted in response to meals (12.09, 2023)
glucose feedback mechanism o Insulin secretory response is rapid
• Circadian variation of secretion in normal individuals: o Increases approximately 5x over baseline to reach a peak within 60
o Maximal postprandial responses are observed after breakfast minutes
o If insulin is not maximally stimulated, the secretion will be dampened • Clinical Correlation:
and may not reach maximum during lunch or dinner o For type 1 diabetics, you provide the entire insulin dose for both basal
o Not the case for people with diabetes mellitus, obesity and insulin & after-meals (because no insulin is synthesized at all)
resistance. o For type 2 diabetics, your beta cells can still respond to acute increases
in blood glucose
Control of Insulin Secretion You may provide the basal dose first and then add increments of the
• The “x” in the Fig. 8 shows the fasting level (80-90mg/100mL) after-meal dose according to the patient’s need
• As blood glucose rises above 100mg/100mL, secretion of insulin rises
rapidly (up to 10-25x at concentrations between 400-600 mg/ 100mL)
• Turnover of insulin is almost just as rapid, occurring within 3-5 minutes
after a reduction in blood glucose concentration back to fasting levels
YL5: 11.03 ENDOCRINE SYSTEM: Pancreas 4 of 9
IV. PHYSIOLOGY OF INSULIN ACTION • IRS will then activate two distinct pathways via phosphorylation
o Phosphatidyl-inositol 3-kinase (PI3K) pathway
A. INSULIN RECEPTOR mediates the rapid effects of insulin signaling
Primarily, this leads to the increased uptake of glucose
Increased uptake of other materials like amino acids and ions
o Mitogen-activated protein kinase (MAPK) pathway
mediates insulin’s long-term effects
Gene expression
E. INSULIN AND ITS METABOLIC EFFECT
• Insulin’s main effect: increased glucose uptake
o Marked increase in uptake is seen in 80% of cells in the body,
particularly muscle cells and adipose cells, but not in most neurons in
the brain
• Increases glycogen production and fat accumulation
• Cell membrane becomes more permeable to amino acids, potassium ions,
and phosphate ions, causing increased transport of said materials into the
cell
• Slower changes occur in the next 10 to 15 minutes
o It changes the activity level of intracellular enzymes because of
phosphorylation
• Much slower effects occur within the next hours and even days
o It affects the rate of translation from mRNA and later, the rate of
transcription from DNA—therefore, affecting the rate of protein
synthesis
Figure 10. Insulin Receptor
V. ACTIONS OF INSULIN
• Composed of four subunits held together by disulfide linkages
o Two α-subunits: lie entirely outside and to which insulin binds to A. EFFECT OF CARBOHYDRATE METABOLISM
o Two β-subunits: traverse the cell membrane and protrude into the Peripheral Uptake of Glucose
cytoplasm
Glucose is the primary stimulus of insulin secretion (12.09, 2023).
• It is an enzyme-linked receptor
o Glucose can’t diffuse across cell membranes
o Insulin binding to the α-subunits causes conformational changes that
Glucose is hydrophilic, not lipophilic (12.09, 2023).
result in the autophosphorylation of the β-subunits
• Tissue uptake of glucose is by facilitated transport
o β-subunits are closely linked to tyrosine kinases that cause
In some tissues, insulin regulates the number of membrane transporters
phosphorylation of multiple other intracellular enzymes, including a
(12.09, 2023).
group called insulin-receptor substrates (IRS).
GLUT 1 and GLUT 3
B. STEPS OF INSULIN ACTION
• Mediate basal glucose uptake in most tissues, including brain, neurons, and
1) Insulin binds to the α-subunits, causing dimerization and conformational RBC
changes
• Its high affinities for glucose ensure glucose entry even during periods of
2) Conformational changes are transmitted to the β-subunits, which
relative hypoglycemia
autophosphorylate in the presence of ATP The brain has GLUT receptors, but it doesn’t need insulin to increase the
o The subunits will then activate tyrosine kinase permeability of glucose (12.09, 2023).
3) Activation of tyrosine kinase leads to either the activation or inhibition of
more enzymes involved in the physiologic action of insulin via
GLUT 2
phosphorylation
4) Insulin-Receptor complex (IRC) is taken in via endocytosis • A low affinity transporter in the hepatocytes and 𝝱 islets
5) Insulin Receptor can be degraded by proteases, stored, or recycled Signals must be present for it to be activated (12.09, 2023).
After a meal, portal blood from the intestine is rich in glucose (12.09,
2023).
C. REGULATION OF INSULIN RECEPTION
GLUT 2 captures the excess glucose primarily for storage (12.09, 2023).
• Insulin binds to elements in the nucleus, the Golgi apparatus, and the When glucose concentration drops below the Km for the transporter,
endoplasmic reticulum much of the remainder leaves the liver and enters the peripheral
o Insulin mediates gene transcription, similar to both IGF-1 and IGF-2 circulation (12.09, 2023).
• Insulin downregulates its own receptor by GLUT 4
o Decreasing rate of synthesis
o Increasing rate of degradation • In adipose tissue and muscles
o Responds to glucose concentration in peripheral blood
• Insulin’s ability to downregulate its own receptor becomes a problem in
o The rate of glucose transport in adipose tissue and muscle is increased
Diabetes Mellitus Type 2
by insulin
o Main pathophysiology: increased insulin resistance rather than lack of
Insulin-dependent (12.09, 2023).
insulin
o Body responds by increasing plasma insulin levels to overcome
resistance Blood Glucose Concentration
o This, in turn, further downregulates insulin receptors, adding to the • Insulin decreases blood glucose concentration
inability of target cells to respond • Increases glucose transport into target cells such as muscle and adipose
o Promotes a vicious cycle tissue by causing the insertion of glucose transporters (GLUT 4) into the cell
membranes
D. INSULIN SIGNALING Excess glucose in the muscle that are not utilized are stored as glycogen
• Activated insulin receptor (IR) phosphorylates tyrosine kinases, which in (12.09, 2023).
turn phosphorylate insulin-receptor substrates (IRS) and other enzymes • Increases glycogen formation from glucose (glycogenesis) in the liver and
involved in the physiologic action of insulin inhibits glycogenolysis
o Signaling leads to regulation of both lipid and glucose metabolism Insulin secretion decreases between meals when blood glucose
concentrations decrease (12.09, 2023).
o Glycogen is split back into glucose and released into the blood
Inhibits gluconeogenesis (12.09, 2023).
YL5: 11.03 ENDOCRINE SYSTEM: Pancreas 5 of 9
o By increasing the production of fructose-2,6-bisphosphate, which
increases phosphofructokinase activity C. EFFECT ON PROTEIN METABOLISM
Directs substrates away from the formation of glucose
Promotes conversion of excess glucose into fatty acids Promotes Protein Synthesis and Storage
• Insulin decreases blood amino acid concentration
B. EFFECT ON FAT METABOLISM • Increases amino acid and protein uptake into cells
o most commonly transported amino acids: valine, leucine, isoleucine,
Blood Fatty Acids and Keto Acid Concentration tyrosine, and phenylalanine
• Insulin decreases blood fatty acids and keto acid concentration • Increases protein synthesis
• Inhibits mobilization and oxidation of fatty acids • Inhibits protein degradation
• Increases storage of fatty acids • Suppresses gluconeogenesis
Net Effect: Fat deposition and inhibition of lipolysis (12.09, 2023).
• Inhibits ketoacid formation (𝝱-hydroxybutyric and acetoacetic acid) in the Synergistic Interaction of Insulin and Growth Hormone
liver
o Decreased fatty acid degradation means less acetyl CoA will be
available for ketoacid formation NOTE: This section was not part of the Pancreas Handout posted in the
Google Classroom but was part of the 2023 Trans.
Promotion of Fat Synthesis and Storage
• Insulin increases the transport of glucose into the liver cells
• More glucose becomes available to form fat (acetyl CoA from pyruvate to
make fatty acids)
After the liver glycogen reaches 5-6%, glucose becomes available to form
fat (12.09, 2023).
Increased citrate and isocitrate from acetyl CoA activates acetyl CoA
carboxylase
The conversion of acetyl CoA malonyl CoA is the first stage of fatty acid
synthesis
• Most of the fatty acids are synthesized within the liver to form triglycerides
Triglycerides are carried by VLDL and LDL into adipose tissue (12.09,
2023).
Lipoprotein lipase (LPL) is activated by insulin and facilitates triglyceride
uptake and storage into fat cells (12.09, 2023).
• Insulin inhibits the action of hormone-sensitive lipase (HSL)
Lipase causes hydrolysis of already stored triglycerides (12.09, 2023).
Inactivation inhibits release of FA from adipose (12.09, 2023).
Promotes glucose transport through the membrane into the fat cells
(12.09, 2023).
o Allows glucose to be converted into fatty acids Figure 11. The Effect of GH alone, Insulin alone, and GH+Insulin on Growth in
o Forms -glycerol phosphate a Depancreatized and Hypophysectomized Rat
Supplies glycerol backbone of triglycerides
D. OTHER ACTIONS
Effects of Insulin Deficiency on Fat Metabolism • Promotes K+ uptake into cells by increasing the activity of Na-K-ATPase
This K+-lowering action of insulin is used to treat acute, life-threatening
hyperkalemia (12.09, 2023).
NOTE: This section was not part of the Pancreas Handout posted in the
• Has a direct effect on the hypothalamic satiety center independent of the
Google Classroom but was part of the 2023 Trans.
changes it produces in blood glucose concentrations
• Lipolysis of storage fat and the release of FA Table 5. Summary: Actions of Insulin
o Loss of inhibition of HSL ACTIONS OF INSULIN EFFECT ON BLOOD LEVEL
o Activation of HSL causes release of FA and glycerol into blood Increased glucose uptake into cells Decreases blood glucose
o Subsequent increase in plasma FA (within minutes), which becomes Increased glycogen formation
available as energy substitute Decreased glycogenolysis
o FAs become the main energy substrate in tissues except the brain Decreased gluconeogenesis
• Insulin deficiency increases plasma cholesterol and phospholipid Increased protein synthesis Decreases blood amino acids
concentrations (from increased fatty acid level) Increased fat deposition Decreases blood fatty acids
o Promotes conversion (by the liver) of FA into phospholipids and Decreased lipolysis Decreases blood ketoacids
cholesterol, which is released into the blood Increased K+ uptake into cells Hypokalemia
o Leads to atherosclerosis
High lipid concentration, especially cholesterol, promotes
VI. ACTIONS OF INSULIN ON TISSUES
development of atherosclerosis in people with severe diabetes
• Excess usage of fats causes ketosis and acidosis A. LIVER CELLS
o Causes excessive acetoacetic acid formation in liver cells • Glycogen storage after a meal (5-6% of liver mass, 100 grams of glycogen
o Increased 𝝱-oxidation of fats produces Acetyl CoA which then in the liver)
condenses to form Acetoacetic Acid o 60% of glucose in the meal is stored as glycogen in the liver
FAs → Increase carnitine transport → Increase 𝝱-oxidation → o Inactivates liver phosphorylase
Increase Acetyl CoA → Excess Acetyl CoA condense to form o Activates glycogen synthase
acetoacetic acid o Enhances glucose uptake by increasing glucokinase
o Absence of insulin depresses acetoacetic acid utilization in peripheral • Reduces blood glucose concentrations
tissues → Increase in Acetoacetic Acid concentration → Acidosis o Stimulates glycogenesis
o Some Acetoacetic Acid is converted to Hydroxybutyric Acid and Acetone o Increase glucose transport into cells
(Ketone Bodies) • Increase protein synthesis
o Accumulation of Ketone Bodies leads to severe Acidosis, Coma, and o Increase amino acid transport into cells
Death o Positive nitrogen balance
• Insulin Deficiency is seen in patients with Type 1 DM and can lead to death
YL5: 11.03 ENDOCRINE SYSTEM: Pancreas 6 of 9
B. MUSCLE CELLS Table 6. Factors Affecting Glucagon Secretion
STIMULATORY FACTORS INHIBITORY FACTORS
• Increase glucose and amino acid uptake
Fasting Insulin
• Increase protein synthesis (enzymes & structural)
Decreased blood glucose
• Decrease protein degradation Somatostatin
concentration
• Increase muscle glycogen synthesis
Increased amino acid
o 2-3% of muscle Increased fatty acid and ketoacid
concentration (esp. Alanina and
o Glycogen is stored when muscle is not exercised after a meal concentration
Arginine)
o Glycogen during short periods of extreme energy →
Cholecystokinin (CCK) Increased blood glucose level
anaerobic energy → glycolysis and lactic acid
Beta adrenergic agonists
• During basal/resting state, muscle cell depends on fatty acids for energy
because the cell is only slightly permeable to glucose Acetylcholine
• 2 conditions when muscle uses up glucose Exercise
o Moderate to heavy exercise: muscle contraction increases GLUT4
independent of insulin B. MECHANISM OF ACTION
o Few hours after a meal: Insulin-mediated process
C. ADIPOSE CELLS
• Increase glucose uptake into cells
• Increase lipid formation (lipogenesis)
• Decrease lipid degradation (lipolysis)
D. TISSUES UNAFFECTED BY INSULIN
• Nervous tissue
• Kidney tubules
• Intestinal mucosa
• RBCs and β-cells of pancreas
• Insulin accelerates, but is not required for glucose uptake by the
liver
E. METABOLISM AND EXCRETION OF INSULIN
• Insulin is cleared from circulation within 10-15 minutes Figure 13. Major Biological Actions of Insulin and Glucagon
• Insulin is metabolized in the liver and kidneys by enzymes that
CELLULAR MECHANISM OF GLUCAGON ACTION:
break disulfide bonds
1) Glucagon binds with its receptor in the cell membrane (GPCR), which is
o Insulinase can degrade half the amount of insulin released
coupled to adenylyl cyclase via a Gs protein.
before it leaves the liver
2) Causes the formation of the second messenger, cAMP
• A and B chains are released (now inactive) and are excreted in the
3) cAMP activates protein kinase regulator protein
urine
4) Protein kinase regulator protein activates protein kinase
• Same metabolism and excretion for endogenous and exogenous 5) Protein kinase activates phosphorylase b kinase (inactive) by
insulin phosphorylating it into phosphorylase a kinase (active)
6) Phosphorylase a kinase converts glycogen phosphorylase b (inactive) into
VII. GLUCAGON glycogen phosphorylase a (active) by phosphorylation.
• Hormone of starvation 7) Promotes the degradation of glycogen into glucose-1-phosphate (G1P)
• Promotes the mobilization & utilization of metabolic fuels 8) G1P glucose-6-phosphate (G6P) via phosphoglucomutase.
• Acts opposite to insulin 9) G6P glucose via glucose-6-phosphatase. Then, it is released from the
• Secreted from the alpha cells of the Islets of Langerhans liver cells.
• Structure:
o Single straight polypeptide with 29 amino acids Actions of Glucagon on the Liver
o Formed by proteolytic cleavage of a larger precursor • Increases blood glucose concentration
o Preproglucagon → proglucagon → glucagon o Stimulates glycogenolysis
• Same family of hormones as gastric inhibitory peptide (GIP) o Inhibits glycogen synthesis from glucose
o Increases gluconeogenesis by decreasing the production of
A. GLUCAGON SECRETION fructose 2,6-bisphosphate
• Main action: to maintain the blood glucose concentration This decreases phosphofructokinase activity
• Factors that stimulate glucagon secretion are those that inform the • Increases blood fatty acid & ketoacid concentration
alpha cells that a decrease in blood glucose has occurred o Glucagon increases lipolysis and inhibits FA synthesis, which also shunts
o Low blood glucose levels stimulate glucagon secretion towards gluconeogenesis
o The ketoacids β-hydroxybutyric acid & acetoacetic acid are produced
from fatty acids
• Glucagon in high concentrations also:
o Increases heart strength
o Increases blood flow to tissues especially the kidneys
o Increases bile secretion
o Inhibits gastric secretion
VIII. DELTA CELLS: SOMATOSTATIN
• Pancreatic somatostatin: polypeptide with 14 amino acids
• As opposed to GI somatostatin which has 28 amino acids
• Secreted by delta cells
• Secretion:
o Stimulated by glucagon, beta-agonists, and ingestion of all forms of
nutrients
Almost all factors related to ingestion of food stimulate
Figure 12. Structural Features of Glucagon somatostatin secretion such as:
YL5: 11.03 ENDOCRINE SYSTEM: Pancreas 7 of 9
Increased blood glucose Weight loss,
Increased amino acids thiazolidinediones,
Therapy Insulin
Increased fatty acids metformin,
Increased concentrations of several GI hormones released from sulfonylureas, insulin
the upper GI tract in response to food intake
o Inhibited by insulin through paracrine actions QUICK REVIEW
• Action:
o Inhibits secretion of insulin and glucagon via paracrine actions
SUMMARY OF TERMS
on the alpha & beta cells OVERVIEW OF THE PANCREAS
Secreted by delta cells in response to a meal and • EXOCRINE: Greater bulk of pancreas, comprised of acini
diffuses to nearby alpha and beta cells • ENDOCRINE: Islets of Langerhans most commonly found at tail of pancreas
Modulates or limits the response of insulin and glucagon • CELL TO CELL COMMUNICATION: Gap Junctions, Unique Blood Supply,
to ingestion of food Innervation
o Decreases motility of the stomach, small intestines, and
gallbladder INSULIN STRUCTURE AND SYNTHESIS
o Decreases secretion and absorption in the GI tract • PROINSULIN: Single chain of 86 amino acids composed of the alpha and
• The function of somatostatin is to increase the time in which food nutrients beta chain of insulin and a conneting segment of 35 amino acids
are assimilated into the blood and allow it to last longer • INSULIN: 51 amino acids with two peptide chains connected by a disulfide
bond
IX. F CELLS: PANCREATIC POLYPEPTIDE
PHYSIOLOGY OF INSULIN SECRETION
• Important feedback inhibitor of pancreatic secretion after a meal
• GLUCOSE: Key regulator of insulin secretion by pancreatic beta cells
• It arises from both islet and acinar cells of the pancreas
• NORMAL FASTING BLOOD GLUCOSE: 80-90mg/dL
• Release of pancreatic polypeptide (PP) by a meal, primarily
• INCRETINS: Released from the neuroendocrine cells of the GI tract
protein, occurs in a biphasic manner
following ingestion of food (functions to amplify glucose-stimulated insulin
o First rapid release: vagal stimulation
secretion and suppress glucagon secretion)
o Second, more prolonged rise (intestinal phase): in response
• GLP-1 (GLUCAGON-LIKE PEPTIDE-1): Secreted by L-cells in distal gut (ileum
to hormonal stimulation (cholecystokinin)
and colon)
• GIP (GLUCOSE-DEPENDENT INSULINOTROPIC POLYPEPTIDE): Secreted by
K-cells in proximal gut (duodenum)
PHYSIOLOGY OF INSULIN ACTION
• INSULIN RECEPTOR: An enzyme-linked receptor made up of four subunits
held together by disulfide linkages
o Two α-subunits: lie entirely outside and to which insulin binds
o Two β-subunits: traverse the cell membrane and protrude into the
cytoplasm
PERIPHERAL UPTAKE OF GLUCOSE
• GLUT 1 AND GLUT 3: Mediates basal glucose uptake in most tissues
including brain, neurons, and RBC
• GLUT 2: a low affinity transporter in the hepatocytes and 𝝱 islets
• GLUT 4: Responds to glucose concentration in peripheral blood (found in
adipose tissue and muscles)
ACTIONS OF INSULIN ON TISSUES
• LIVER CELLS: Glycogen storage after a meal (5-6% of liver mass, 100 grams
of glycogen in the liver)
• MUSCLE CELLS: Increase glucose and amino acid uptake
• ADIPOSE CELLS: Increase glucose uptake into cells
• TISSUES UNAFFECTED BY INSULIN: Nervous tissue, Kidney tubules,
Intestinal mucosa, RBCs, and β-cells of pancreas
Figure 13. Summary of the Control of Blood Glucose • GLUCAGON: Promotes the mobilization & utilization of metabolic fuels and
is secreted by alpha cells of the Islets of Langerhans
X. IMPORTANCE OF CONTROLLING BLOOD SUGAR LEVELS
• SOMATOSTATIN: Secreted by delta cells; it inhibits the secretion of insulin
• High glucose levels cause increased osmotic pressure in the ECF and glucagon via paracrine action on alpha and beta cells of the pancreas.
o Cellular dehydration • PANCREATIC POLYPEPTIDE: Important feedback inhibitor of pancreatic
• Osmotic diuresis → dehydration and depletion of electrolytes secretion after a meal that is secreted by F cells
• Vascular injury associated with uncontrolled diabetes mellitus leads to
increased risk for heart attack, stroke, end-stage renal disease, and
blindness
SUMMARY OF PROCESSES
• Presence of tissues which rely mainly on glucose for energy SYNTHESIS OF INSULIN
o Brain, retina, germinal epithelium of the gonads 1) Unique set of transcription factors found in β cell nucleus activates the
transcription of preproinsulin mRNA from the insulin gene
Table 6. Clinical Characteristics of Patients with Type 1 and Type 2 DM 2) Preproinsulin mRNA directs ribosomal synthesis (translation) of
FEATURE TYPE 1 TYPE 2 preproinsulin, which contains 4 peptides:
Age of onset Usually <20 years Usually >30 years o Signal Peptide
Low (wasted) to o Alpha and Beta Chains
Body Mass Visceral obesity o Connecting Peptide (C-Peptide)
normal
3) Preproinsulin (11,500 MW) is cleaved by microsomal enzymes in the
Normal to High
Plasma Insulin Low or Absent endoplasmic reticulum to form proinsulin
initially
o Amino-terminal signal peptide was removed almost immediately after
High, can be High, resistant to
Plasma Glucagon synthesis
suppressed suppression
o Proinsulin consists of: alpha and beta chains, C-peptide
Plasma Glucose Increased Increased
4) Proinsulin (9,000 MW) is transported to the Golgi apparatus and is cleaved
Insulin Sensitivity Normal Reduced by proteases to form the active insulin and C-peptide
YL5: 11.03 ENDOCRINE SYSTEM: Pancreas 8 of 9
5) Active insulin (5,805 MW) and C-peptide (3,000 MW) are packaged into IMPORTANT LINKS
secretory granules
o Mature secretory granules contain insulin and C-peptide in equimolar Errata Tracker: https://tinyurl.com/2024YL5ErrataTracker11
amounts (1 C-peptide : 1 insulin molecule) Trans Feedback Form: https://tinyurl.com/2024YL5TransFeedbackForm
o 5-10% of the secretory products are uncleaved proinsulin
6) Both insulin and C-peptide are released into circulation in equimolar
amount when stimulus is present
STEPS OF INSULIN ACTION
1) Insulin binds to the α-subunits, causing dimerization and conformational
changes
2) Conformational changes are transmitted to the β-subunits, which
autophosphorylate in the presence of ATP
o The subunits will then activate tyrosine kinase
3) Activation of tyrosine kinase leads to either the activation or inhibition of
more enzymes involved in the physiologic action of insulin via
phosphorylation
4) Insulin-Receptor complex (IRC) is taken in via endocytosis
5) Insulin Receptor can be degraded by proteases, stored, or recycled
CELLULAR MECHANISM OF GLUCAGON ACTION:
1) Glucagon binds with its receptor in the cell membrane (GPCR), which is
coupled to adenylyl cyclase via a Gs protein.
2) Causes the formation of the second messenger, cAMP.
3) cAMP activates protein kinase regulator protein
4) Protein kinase regulator protein activates protein kinase
5) Protein kinase activates phosphorylase b kinase phosphorylase a
kinase by phosphorylation
6) Phosphorylase a kinase converts glycogen phosphorylase b glycogen
phosphorylase a by phosphorylation.
7) Glycogen phosphorylase a promotes the degradation of
glycogen glucose-1-phosphate (G1P)
8) G1P glucose-6-phosphate (G6P) via phosphoglucomutase.
9) G6P glucose via glucose-6-phosphatase. Then, it is released from the
liver cells.
REVIEW QUESTIONS
1. Which of the following stimulates somatostatin secretion?
a) Increased fatty acids
b) Increased blood glucose
c) Increased amino acids
d) All of the above
2. Islets of Langerhans receive 1% of the pancreatic blood flow. It accounts
for only 10% of the pancreatic mass.
a) Statement 1 is True. Statement 2 is False
b) Statement 1 is False. Statement 2 is True
c) Both statements are True
d) Both statements are False
3. Which among the following is true:
a) GLUT 1 and GLUT 2 mediate basal glucose uptake in most tissues,
including brain, neurons, and RBC
b) Insulin increases glycogenesis in the liver and inhibits glycogenolysis
c) Insulin suppresses K+ uptake into cells by decreasing the activity of Na-
K-ATPase
d) None of the above
4. The third phase of prandial insulin secretion happens
a) 1.5 hours to 3 hours after exposure to glucose
b) 2.5 hours to 4 hours after exposure to glucose
c) 1.5 hours to 3 hours before exposure to glucose
d) 2.5 hours to 4 hours before exposure to glucose
ANSWERS:
1D, 2D, 3B, 4A
REFERENCES
REQUIRED
Moore, Keith L., Dalley, Arthur F., Agur, Anne M. R. Clinically Oriented
Anatomy 7th ed. Philadelphia, Wolters Kluwer, 2014.
ASMPH Batch 2023. 05/14/2019. 12.09: Pancreas lectured by Julie Anne
L. Gabat, MD, FPCP, DPSEDM.
(1) Julie Anne L. Gabat. 03/31/2020. Pancreas Handout.
YL5: 11.03 ENDOCRINE SYSTEM: Pancreas 9 of 9
You might also like
- Artemia:: Basic and Applied BiologyDocument297 pagesArtemia:: Basic and Applied BiologyNiqh Rafiqah100% (1)
- All About Albumin: Biochemistry, Genetics, and Medical ApplicationsFrom EverandAll About Albumin: Biochemistry, Genetics, and Medical ApplicationsNo ratings yet
- Checklist Code ReviewDocument2 pagesChecklist Code ReviewTrang Đỗ Thu100% (1)
- Polakof 2011Document27 pagesPolakof 2011Guilherme VarellaNo ratings yet
- Penyerapan & Asimilasi (DLP)Document2 pagesPenyerapan & Asimilasi (DLP)KomathiNo ratings yet
- Aneuploidy and TumorigenesisDocument7 pagesAneuploidy and TumorigenesisAlejandraOsegueraNo ratings yet
- Lipids QPDocument14 pagesLipids QPJainam Mehta100% (1)
- ZoogeographyDocument11 pagesZoogeographyAther FarooqNo ratings yet
- Human Nutrition - 90 QPDocument16 pagesHuman Nutrition - 90 QPStephen AreriNo ratings yet
- Holiday Package Year 10 BiologyDocument7 pagesHoliday Package Year 10 Biologyemmanuelkasumba50No ratings yet
- In Cretin AsDocument43 pagesIn Cretin AsGaby Isela Sifuentes LucioNo ratings yet
- UntitledDocument9 pagesUntitled박준수No ratings yet
- Monomers and Polymers QPDocument10 pagesMonomers and Polymers QPJainam MehtaNo ratings yet
- The International Journal of Biochemistry & Cell BiologyDocument15 pagesThe International Journal of Biochemistry & Cell BiologyNathalia PietraniNo ratings yet
- Summery 2Document45 pagesSummery 2BiologistAhmedNo ratings yet
- Translational Research in Anatomy: James P. Nott, Elizabeth A. Bonney, James D. Pickering, Nigel A.B. SimpsonDocument7 pagesTranslational Research in Anatomy: James P. Nott, Elizabeth A. Bonney, James D. Pickering, Nigel A.B. Simpsonangela_karenina_1No ratings yet
- Brain, Behavior, and Immunity: Aravinthan Varatharaj, Ian GaleaDocument12 pagesBrain, Behavior, and Immunity: Aravinthan Varatharaj, Ian GaleaDavid James PNo ratings yet
- The Role of Edible Mushrooms in Health Evaluation of The EvidenceDocument23 pagesThe Role of Edible Mushrooms in Health Evaluation of The EvidencekierkegardNo ratings yet
- Cisplatin Resistance and Opportunities For Precision MedicineDocument10 pagesCisplatin Resistance and Opportunities For Precision MedicineRoxanna BallesterosNo ratings yet
- Brochure Gastrointestinal Diseases - October 2015Document48 pagesBrochure Gastrointestinal Diseases - October 2015CARLOSNo ratings yet
- The Biology Of: Trifolium Repens L. (White Clover)Document41 pagesThe Biology Of: Trifolium Repens L. (White Clover)ROBERTO MIRANDA CALDASNo ratings yet
- 5 1 1 Cellular ControlDocument40 pages5 1 1 Cellular ControlPramudith LiyanageNo ratings yet
- Work Sheet Class 9 Bio For Google ClassroomDocument2 pagesWork Sheet Class 9 Bio For Google Classroomvaibhavrajsingh56No ratings yet
- Monomers and Polymers QP PDFDocument17 pagesMonomers and Polymers QP PDFRaihanNo ratings yet
- Ecology Ex 1 2014Document8 pagesEcology Ex 1 2014jokelNo ratings yet
- Set 1 ExamDocument6 pagesSet 1 Examecadet232No ratings yet
- Science Checkpoint WorkbookDocument130 pagesScience Checkpoint WorkbookAgung PambudionoNo ratings yet
- Endogenous Cardiotonic SteroidsDocument30 pagesEndogenous Cardiotonic SteroidsSebastian NemethNo ratings yet
- Organoid Culture HandbookDocument40 pagesOrganoid Culture HandbookGabriella Panuccio100% (1)
- 2001 Jan Module 1Document9 pages2001 Jan Module 1paolo maldiniNo ratings yet
- Exciting Times Beyond The Brain: Metabotropic Glutamate Receptors in Peripheral and Non-Neural TissuesDocument24 pagesExciting Times Beyond The Brain: Metabotropic Glutamate Receptors in Peripheral and Non-Neural TissuesAndi WijayaNo ratings yet
- 1 s2.0 S0169409X22000722 MainDocument11 pages1 s2.0 S0169409X22000722 MainIrfan HussainNo ratings yet
- 2018 SAM Protocol EnglishDocument166 pages2018 SAM Protocol EnglishMurtaza HamdardNo ratings yet
- Lesliegunatilaka 1999Document101 pagesLesliegunatilaka 1999Chiến NguyễnNo ratings yet
- Astrocytes Multitaskers in Chronic PainDocument9 pagesAstrocytes Multitaskers in Chronic PainPedro FonsecaNo ratings yet
- Extra Enzymes Qs and MSDocument6 pagesExtra Enzymes Qs and MSKhushi ShahNo ratings yet
- Properties of Cordyceps Sinensis A Review - 2013 - Journal of Functional FoodsDocument20 pagesProperties of Cordyceps Sinensis A Review - 2013 - Journal of Functional FoodsSara SanabriaNo ratings yet
- Caffeineornlreport PDFDocument392 pagesCaffeineornlreport PDFmahesh babu100% (1)
- Cell Owners ManualDocument104 pagesCell Owners ManualpeterNo ratings yet
- Edexcel International GCSE Biology Hard PPQ MSDocument14 pagesEdexcel International GCSE Biology Hard PPQ MSTravel UnlimitedNo ratings yet
- Year 10 Revision Paper QPDocument15 pagesYear 10 Revision Paper QPketamineNo ratings yet
- Endomorfin 2 PDFDocument36 pagesEndomorfin 2 PDFMuhammad Ichsan MustariNo ratings yet
- Mock Cells TestDocument5 pagesMock Cells TestDavid LeechNo ratings yet
- Cells-Microscopes-Cell-Cycle-and-Immunity-Questions GRADE 12 HOLIDAY ASSIGNMENTDocument36 pagesCells-Microscopes-Cell-Cycle-and-Immunity-Questions GRADE 12 HOLIDAY ASSIGNMENTAsha justin joseph100% (1)
- Molecular and Cellular EndocrinologyDocument12 pagesMolecular and Cellular Endocrinologyزياد سلمانNo ratings yet
- Section 2 - Lower Limb AnatomyDocument58 pagesSection 2 - Lower Limb AnatomyAliyah LuharNo ratings yet
- 先天免疫学糖生物学Document673 pages先天免疫学糖生物学Wenbo Yan100% (1)
- Penetration of Anti Infective Agents Into.3Document28 pagesPenetration of Anti Infective Agents Into.3Thawatchai NakkaratniyomNo ratings yet
- G Protein - Coupled Receptors in Asthma Therapy: Pharmacology and Drug ActionDocument49 pagesG Protein - Coupled Receptors in Asthma Therapy: Pharmacology and Drug ActionFachri AliefNo ratings yet
- Gr-10 Practice Questions Biology Ch-4Document9 pagesGr-10 Practice Questions Biology Ch-4Sultan ZaibNo ratings yet
- MP90 4Document77 pagesMP90 4vadimbagetNo ratings yet
- PhDThesis Scheuring ScreenDocument115 pagesPhDThesis Scheuring Screenodiaz01100% (1)
- Biology Unit 2.1Document190 pagesBiology Unit 2.1KimNo ratings yet
- Barreras en El Crebro en DesarrolloDocument19 pagesBarreras en El Crebro en DesarrolloAlvarez Flores GilmerNo ratings yet
- The Inositol Pyrophosphate Pathway in Health and Diseases: Anutosh ChakrabortyDocument25 pagesThe Inositol Pyrophosphate Pathway in Health and Diseases: Anutosh ChakrabortyLarisjoursNo ratings yet
- Fatty Acid Metabolism and Its Regulation 1984Document223 pagesFatty Acid Metabolism and Its Regulation 1984عمار مصعب عادلNo ratings yet
- PR 117 015305Document72 pagesPR 117 015305Md. Ahsan-Ul BariNo ratings yet
- The Biomass Distribution On EarthDocument113 pagesThe Biomass Distribution On EarthSarita QuinteroNo ratings yet
- Biochemical and Biophysical Research CommunicationsDocument10 pagesBiochemical and Biophysical Research CommunicationsYuanda KhanNo ratings yet
- Caffeine and The CNSDocument31 pagesCaffeine and The CNSSantiagoGuardoMayaNo ratings yet
- Università Degli Studi Di Trieste: Biomarkers To Define Optimal Protein RequirementDocument119 pagesUniversità Degli Studi Di Trieste: Biomarkers To Define Optimal Protein RequirementDadi SindhuNo ratings yet
- Adrenal Glands: Module 11: Endocrine SystemDocument9 pagesAdrenal Glands: Module 11: Endocrine SystemLANCE GILL Tolentino100% (2)
- Molecular Biology of HormonesDocument11 pagesMolecular Biology of HormonesLANCE GILL TolentinoNo ratings yet
- (11.10) Imaging of The Endocrine System (TG1-CG14) Final VersionDocument12 pages(11.10) Imaging of The Endocrine System (TG1-CG14) Final VersionLANCE GILL TolentinoNo ratings yet
- Hypothalamus and Pituitary GlandDocument9 pagesHypothalamus and Pituitary GlandLANCE GILL Tolentino100% (3)
- (11.05) Adrenal Glands (TG18-CG6) FinalDocument9 pages(11.05) Adrenal Glands (TG18-CG6) FinalLANCE GILL TolentinoNo ratings yet
- (11.10) Imaging of The Endocrine System (TG1-CG14) Final VersionDocument12 pages(11.10) Imaging of The Endocrine System (TG1-CG14) Final VersionLANCE GILL TolentinoNo ratings yet
- Meta Model of Planned ChangeDocument8 pagesMeta Model of Planned ChangeLANCE GILL TolentinoNo ratings yet
- Chin and Benne - General Strategies of ChangeDocument5 pagesChin and Benne - General Strategies of ChangeLANCE GILL TolentinoNo ratings yet
- Basic Life Support - Hands-Only CPRDocument1 pageBasic Life Support - Hands-Only CPRLANCE GILL TolentinoNo ratings yet
- Chapter 2 - Structure and Functions For The Cells of The Nervous SystemDocument14 pagesChapter 2 - Structure and Functions For The Cells of The Nervous SystemLANCE GILL Tolentino100% (1)
- A Series of Articles From William BridgesDocument7 pagesA Series of Articles From William BridgesLANCE GILL TolentinoNo ratings yet
- Homework 2 (Cell Module) PDFDocument3 pagesHomework 2 (Cell Module) PDFLANCE GILL TolentinoNo ratings yet
- Cell Homework 1Document1 pageCell Homework 1LANCE GILL TolentinoNo ratings yet
- Cell Homework 1Document1 pageCell Homework 1LANCE GILL TolentinoNo ratings yet
- Neurological History TakingDocument3 pagesNeurological History TakingLANCE GILL TolentinoNo ratings yet
- Neurological History TakingDocument3 pagesNeurological History TakingLANCE GILL TolentinoNo ratings yet
- Erectus Ever Found Within The Boundaries of China. The Two Fossil Teeth Unearthed WereDocument6 pagesErectus Ever Found Within The Boundaries of China. The Two Fossil Teeth Unearthed WereenerankenNo ratings yet
- Caracterisation D'une Entreprise anglosaxonne-ETLV - STMG1.Document2 pagesCaracterisation D'une Entreprise anglosaxonne-ETLV - STMG1.meredith.licagaNo ratings yet
- Ingredients EnsaymadaDocument3 pagesIngredients Ensaymadajessie OcsNo ratings yet
- SAP IAG Admin GuideDocument182 pagesSAP IAG Admin GuidegadesigerNo ratings yet
- OD - SAP Connector UtilityDocument22 pagesOD - SAP Connector UtilityShivani SharmaNo ratings yet
- Student's T DistributionDocument6 pagesStudent's T DistributionNur AliaNo ratings yet
- Study of Bond Properties of Concrete Utilizing Fly Ash, Marble and Granite PowderDocument3 pagesStudy of Bond Properties of Concrete Utilizing Fly Ash, Marble and Granite PowderLegaldevil LlabsNo ratings yet
- GP 43-45-DRAFT - Site RestorationDocument48 pagesGP 43-45-DRAFT - Site Restorationmengelito almonte100% (1)
- Catalyst 4500 SeriesDocument1,230 pagesCatalyst 4500 SeriesnvleninkumarNo ratings yet
- Consumer Price SummaryDocument5 pagesConsumer Price SummaryKJ HiramotoNo ratings yet
- Anzsco SearchDocument6 pagesAnzsco SearchytytNo ratings yet
- Lab 08: SR Flip Flop FundamentalsDocument6 pagesLab 08: SR Flip Flop Fundamentalsjitu123456789No ratings yet
- PCI Secure Software Standard v1 - 0Document67 pagesPCI Secure Software Standard v1 - 0Antonio ClimaNo ratings yet
- The Community Reinvestment Act in The Age of Fintech and Bank CompetitionDocument28 pagesThe Community Reinvestment Act in The Age of Fintech and Bank CompetitionHyder AliNo ratings yet
- How To Measure Light Levels and Lux LevelsDocument4 pagesHow To Measure Light Levels and Lux LevelsAngelo PalamingNo ratings yet
- Biology Concepts and Applications 9th Edition Starr Solutions ManualDocument9 pagesBiology Concepts and Applications 9th Edition Starr Solutions Manualscarletwilliamnfz100% (31)
- Article On Role of Cyberspace in Geopolitics-PegasusDocument5 pagesArticle On Role of Cyberspace in Geopolitics-PegasusIJRASETPublicationsNo ratings yet
- Updated PDPDocument540 pagesUpdated PDPnikulaaaasNo ratings yet
- Spermatogenesis: An Overview: Rakesh Sharma and Ashok AgarwalDocument25 pagesSpermatogenesis: An Overview: Rakesh Sharma and Ashok Agarwalumar umarNo ratings yet
- Queen - Hammer To Fall ChordsDocument3 pagesQueen - Hammer To Fall ChordsDavideContiNo ratings yet
- Business Maths Chapter 5Document9 pagesBusiness Maths Chapter 5鄭仲抗No ratings yet
- Statement 1680409132566Document11 pagesStatement 1680409132566úméshNo ratings yet
- Shsa1105 - Unit-III Course MaterialsDocument58 pagesShsa1105 - Unit-III Course Materialssivanikesh bonagiriNo ratings yet
- Annexure I Project Details DateDocument4 pagesAnnexure I Project Details DateAshish SinghaniaNo ratings yet
- Cover Sheet: Online Learning and Teaching (OLT) Conference 2006, Pages Pp. 21-30Document12 pagesCover Sheet: Online Learning and Teaching (OLT) Conference 2006, Pages Pp. 21-30Shri Avinash NarendhranNo ratings yet
- LLB IV Sem GST Unit I Levy and Collection Tax by DR Nisha SharmaDocument7 pagesLLB IV Sem GST Unit I Levy and Collection Tax by DR Nisha Sharmad. CNo ratings yet
- Travel OrderDocument2 pagesTravel OrderStephen EstalNo ratings yet
- Belimo ARB24-SR Datasheet En-UsDocument2 pagesBelimo ARB24-SR Datasheet En-Usian_gushepiNo ratings yet