Professional Documents
Culture Documents
0.7 Surgery Trans PDF
Uploaded by
Joy ManzanoOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
0.7 Surgery Trans PDF
Uploaded by
Joy ManzanoCopyright:
Available Formats
Surgery Rotation CLERKSHIP
crucial role in capacitance by undergoing receptive relaxation
ILOILO DOCTORS’ COLLEGE OF MEDICINE site of the autonomic pacemaker responsible for initiating
Molo, Iloilo City S.Y. 2020-2021 gastric motor activity inferior extent of the fundus is
considered to be the horizontal plane of the GE junction
BATCH 2021
DISCIMUS SAPIENCIA UT VIRTUS Body/ Corpus: from the cardiac orifice to the incisura
angularis (angular notch) this contains most of the
SURGERY CLERKSHIP oxyntic or parietal cells that are also present in cardia
and fundus which secrete HCl and intrinsic factors.
LECTURER: DR. BITO-ONON
MAIN TOPIC: STOMACH Antrum: from the incisura angularis to the pylorus
forms the distal 25-30% of stomach
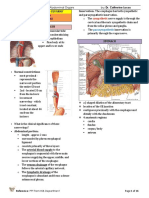
ANATOMY:
ARTERIAL AND VENOUS SUPPLY
ARTERIAL SUPPLY
Lesser Curvature:
-Right gastic artery
-Left Gastric artery
Greater Curvature:
-Right Gastroepiplioc Artery
-Left Gastroepiploic Artery
Fundus:
-Short Gastric Artery
VENOUS DRAINAGE
-Tributaries of Portal Vein
-Tributaries of Splenic Vein
-Tributaries of Superior Mesenteric Vein
NOTES: The arteries are derived from the branches of the
celiac artery.
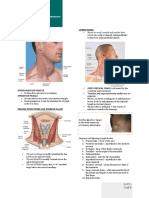
MAIN PARTS:
The left gastric artery arises from the celiac artery. It supplies
• CARDIA
the lower third of the esophagus and the upper right part of
• FUNDUS
the stomach.
• BODY (CORPUS)
The right gastric artery arises from the hepatic artery. It
• ANTRUM
supplies the lower right part of the stomach.
• PYLORUS
The left gastroepiploic artery arises from the splenic
NOTES: The stomach is the most proximal abdominal organ of
artery at the hilum of the spleen and passes forward in the
the digestive tract and function in storing and facilitates the
gastrosplenic omentum (ligament) to supply the stomach
digestion and absorption of ingested food and helps regulate
along the upper part of the greater curvature.
appetite. Important secretory functions include the
production of acid, pepsin, intrinsic factor, mucus, and a
The right gastroepiploic artery arises from the
variety of GI hormones. Important motor functions include
gastroduodenal branch of the hepatic artery, supplies the
food storage (receptive relaxation and accommodation),
stomach along the lower part of the greater curvature.
grinding and mixing, controlled emptying of ingested food,
and periodic interprandial “housekeeping.”
The short gastric arteries arise from the splenic artery
at the hilum of the spleen and pass forward in the
Cardia: connects to the esophagus first region of the
gastrosplenic omentum (ligament)
stomach into which material (food) passes important for HCl
secretion
The veins drain into the portal circulation. The left and right
gastric veins drain directly into the portal
Fundus: superior most part and distensible bounded
vein.
superiorly by the diaphragm and laterally by the spleen. has
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 1|8
Surgery Rotation CLERKSHIP
The short gastric veins and the left gastroepiploic veins join Food ingestion is the physiologic stimulus for acid
the splenic vein. secretion. There are 3 phases in which gastric
secretion occurs namelu, the cephalic phase, gastric
The right gastroepiploic vein joins the superior mesenteric phase and intestinal phase. Cephalic phase which
vein. begins in the thought, sight, smell and or taste of
food. These stimulate the brain in the cortical and
LYMPHATIC DRAINAGE: hypothalamic sites and the signals are transmitted to
the stomach by the vagal nerves. Acetylcholine is
• All of the following eventually drain to the celiac released which in turn stimulates the ECL cells and
nodes: parietal cells. Cephalic phase accounts for the 30% of
• Left and right gastric nodes total acid secretion in response to a meal.
• Left and right gastroepiploic nodes
• Short gastric nodes
INNERVATION:
• Sympathetic: Celiac plexus from T5-TlO
• Parasympathetic:
– Right vagus (Posterior surface)
– Left vagus (Anterior surface)
• Functions of the vagus nerve:
– Gastric motility
– Relaxation of the pyloric sphincter
– Stimulation of parietal cells for acid
production
NOTES: The nerve supply includes sympathetic fibers derived
from the celiac plexus and parasympathetic fibers from the
right and left vagus nerves
The sympathetic innervation of the stomach carries a
proportion of pain-transmitting nerve fibers, whereas
the parasympathetic vagal fibers are secretomotor to the
gastric glands and motor to the muscular wall of the
stomach.
HISTOLOGY:
Four layers of the gastric wall:
• Mucosa
• Submucosa
• Muscularis propia
• Serosa
NOTES:
Meissner’s autonomic plexus: regulates the
configuration of the luminal surface, controls
glandular secretions, alters electrolyte and water
transport, and regulates local blood flow.
Auerbach myenteric plexus: provides motor
innervation to both layers of the muscular layer of
the gut having both para and sympa input
PHYSIOLOGY:
NOTES:
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 2|8
Surgery Rotation CLERKSHIP
The intestinal phase is poorly understood. This phase starts addition to that stomach distention stimulates acid secretion
when gastric emptying of ingested food begins and continues via vasovagal reflex arch which is abolished by truncal or
as long as nutrients remain in the proximal small intestine. Highly Selective Vagotomy. Finally, ongoing cephalic vagal
10% of meal induced acid secretion. input stimulates gastrin release, which in turn stimulates
histamine release from ECL cells and acid secretion.
MECHANISM OF GASTRIC SECRETION:
STIMULATION OF GASTRIC H+ SECRETION
Parietal cells secrete HCl into the lumen of the stomach and, • Vagal stimulation
concurrently, absorb HCO3 into the bloodstream as follows: • direct pathway and an indirect
a. In the parietal cells, CO2 and H2O are converted pathway
to H+ and HCO3 –catalyzed by carbonic anhydrase. • Gastrin
• released in response to eating a
b. H+ is secreted into the lumen of the stomach by meal
the H+K+ pump (H+,K+-ATPase). Cl– is
secreted along with H+; thus, the secretion product
of the parietal cells is HCl. • Histamine
• stimulates H+ secretion by
■ A “proton pump inhibitor” inhibits the H+,K+- activating
ATPase and blocks H+ secretion. • H2 receptors on the parietal cell membrane
c. HCO3 – produced in the cells is absorbed into the
• Potentiating effects of ACh, histamine,
bloodstream in exchange for Cl (Cl––HCO3 –
and gastrin on H+ secretion
exchange). As HCO3– is added to the
venous blood, the pH of the blood increases
(“alkaline tide”).
INHIBITION OF GASTRIC H+ SECRETION:
• Negative feedback mechanisms.
a. Low pH (< 3.0) in the stomach
b. Somatostatin
c. Prostaglandins
NOTES: When food reaches the stomach the gastric phase of NOTES: Negative feedback mechanisms inhibit the secretion
secretion begins. This phase lasts until the stomach is empty of H+ by the parietal cells.
and accounts for about 60% of the total acid secretion in
response to a meal. This phase has several components, A. LOW PH (< 3.0) IN THE STOMACH
Amino acids and small peptides from ingested food stimulate
Antral G-cells to secrete gastrin which is then carried in the ■ After a meal is ingested, H+ secretion is
blood stream to ECL cells and parietal cells and stimulates stimulated. After the meal is digested and the
acid secretion in an endocrine fashion (discuss next slide). In stomach emptied, further H+ secretion decreases
the pH of the stomach contents. When the pH of the
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 3|8
Surgery Rotation CLERKSHIP
stomach contents is <3.0, gastrin secretion is GASTRIC HORMONES
inhibited and, by negative feedback, inhibits further
H+ secretion.
B. SOMATOSTATIN
■ inhibits gastric H+ secretion by a direct pathway
and an indirect pathway.
In the direct pathway, somatostatin binds to
receptors on the parietal cell that are coupled to
adenylyl cyclase, inhibiting adenylyl cyclase and
decreasing cAMP levels. In this pathway,
somatostatin antagonizes the stimulatory action of
histamine on H+ secretion.
■ In the indirect pathway somatostatin inhibits
release of histamine and gastrin, thus decreasing H+
secretion indirectly.
C. PROSTAGLANDINS
GASTRIC MOTILITY AND EMPTYING
• inhibit gastric H+ secretion by activating a Gi , • Stomach Relaxes to accommodate meal at the
inhibiting adenylyl cyclase and decreasing cAMP beginning of a meal
levels. • Food breakdown by regulated motor activity and
controls output to duodenum
GASTRIC MUCOSAL BARRIER • Coordinated muscle relaxation and contraction of
• Provides resistance to autodigestion by HCl the various gastric segments
and active pepsin
• Maintains intact gastric mucosal layer SOLID VS LIQUID EMPTYING
• When these defences breakdown—ULCERATION LIQUID EMPTYING
• follows first-order kinetics, with a half
emptying time around 12 minutes.
• Caloric density, osmolarity and nutrient
composition of the liquid changes
• 1M osmolarity= 200kcal/hour
• Duodenal osmoreceptors and hormones–
modulators
• Delayed in supine position
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 4|8
Surgery Rotation CLERKSHIP
BARIUM UPPER GI STUDY:
SOLID EMPTYING • Plain Abdominal X-rays
• Half emptying time: <2 hours • Gastric Perforation
• Initial lag phase (Pneumoperitoneum)
• Meal particle size, caloric content and • Delayed gastric emptying (Large air
composition fluid level)
• Stored in fundus and delivered to distal
stomach at constant rates Double Contrast upper GI-series
• Better than EGD at elucidating
DIAGNOSIS OF GASTRIC DISEASES Gastric diverticula, fistula,
• Signs and symptoms: tortuosity, stricture location and
• Pain size of hiatal hernia.
• Nausea
• Weight loss *Gatric ulcers require biopsy.
• Vomiting
• Early satiety COMPUTED TOMOGRAPHY SCANNING
• Bloating AND MAGNETIC RESONANCE IMAGING
• Anorexia
• Anemia • should be part of routine staging work-up for
patients with malignant gastric tumor
*Dyspepsia – pain, bloating, nausea, and early MRI:
satiety – common causes are GERD, • quantitative test for gastric
helicobacter gastritis, and other disorders • in patients with gastroparesis
of the stomach. emptying.
• analysis of myoelectric
derangements.
Arteriography:
• Occasional poor risk patient with
gastric hemorrhage or in patients with
occult gastic bleeding.
ENDOSCOPIC ULTRASOUND:
DIAGNOSTIC TESTS: • Accurate for local staging of gastric adenocarcinoma
Esophagogastroduodenoscopy and therapy plan
• Indication: Patients with 1 or more of the alarm • Used to assess tumor response to chemotherapy
symptoms • Can provide reassurance but no guarantee that small
• Advantage: lesions are benign.
• Safe and accurate • Assess submucosal varices
• Smaller flexible scopes with
excellent optics SCINTIGRAPHY
• Procedure: • Standard evaluation of gastric emptying which
Following an 8 hour fast, the flexible scope involves the ingestion of a test meal with one or two
is advanced under direct vision in the isotopes and scanning the patient under a gamma
esophagus, stomach and duodenum , the camera.
fundus and GE junction are inspected by • Allows the semiquantitative assessment of how
retroflexing the scope. much isotopes refluxes to the stomach.
• Complications: TEST FOR HELICOBACTER PYLORI
• Perforation (rare), aspiration and • Positive serologic test
respiratory depression from • Histologic examination of gastric mucosal biopsy
excessive sedation. (Gold Standard).
• Commercially available rapid urease tests for the
presence of urease in mucosal biopsy specimens
(strong presumptive evidence of infection).
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 5|8
Surgery Rotation CLERKSHIP
• Urease is an omnipresent enzyme in H pylori strains OTHER CAUSES:
that colonize the gastric mucosa. ZES (Gastrinoma), antral G-cell
• Urea Breath Test: standard test for eradication of H. hyperfunction and/or hyperplasia,
pylori after treatment systemic mastocytosis, trauma, burns
and major physiologic stress,
ANTRODUODENAL MOTILITY TESTING AND drugs,smoking and psychologic stress
ELECTROGASTROGRAPHY
• Performed in specialized centers and may be useful
in the evaluation of the occasional patient with
dyspeptic symptoms.
• EGG consists of the transcutaneous recording of
gastric myoelectric activity.
• Antroduodenal motility testing is done with a tube
placed transnasally or transorally into the distal
duodenum.
DISEASES OF THE STOMACH
Helicobacter pylori Infection
• H. pylori- uniquely equipped for survival in hostile
environment of the stomach.
CLASSIFICATION BASED ON ANATOMIC LOCATION &
• Urease– converts urea to ammonia and bicarbonate,
PATHOPHYSIOLOGY (PUD)
buffers acid secreted by stomach
• Types I and IV: associated with normal or low acid
output
• Causes disturbance in gastric acid secretion leading
• Types II and Ill: associated with gastric acid
to gastric injury.
hypersecretion (similar to duodenal ulcers)
NOTES: Modified johnson classification.
Human beings are the only reservoir for H pylori. • The most common, Johnson type I gastric ulcer, is
H. pylori– specialized flagella and a rich supply of typically located near the angularis incisura on the
urease lesser curvature, close to the border between antral
• Infection can occur by oral ingestion of the and corpus mucosa. Patients with type I gastric ulcer
bacterium usually have normal or decreased acid secretion.
• Pathogenesis: survival in the acidic gastric lumen, Type II gastric ulcer is associated with active or
flagellated movement from the lumen across the quiescent duodenal ulcer disease, and type III gastric
mucus layer to the surface epithelial cell, adhesion ulcer is prepyloric ulcer disease. Both type II and
to the surface epithelial cell, and toxin production. type III
• Major cause of peptic ulceration. • Gastric ulcers are associated with normal or
• Noninvasive methods for diagnosis: include the urea increased gastric acid secretion and surgically are
breath test, serology, and detection of stool antigen. treated similar to duodenal ulcer. Type IV gastric
• Antimicrobial drugs must be combined with gastric
acid secretion inhibitors or bismuth salts.
PEPTIC ULCER DISEASE
• Focal defects in the gastric or duodenal mucosa
which extends into the submucosa or deeper
• caused by an imbalance between the action of acid
and mucosal defense
• PATHOPHYSIOLOGY AND ETIOLOGY:
• Caused by H. pylori infection
and/or NSAID use
• Final common pathway: Acid-
peptic injury of the gastroduodenal
mucosal barrier.
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 6|8
Surgery Rotation CLERKSHIP
ulcers occur near the GE junction, and acid secretion
is normal or below normal. Type V gastric ulcers are
medication induced and may occur anywhere in the
stomach.
SURGICAL OPTIONS.
NOTES: Choice of operation depend on the physiologic status
of the patient (most important). The location of the ulcer
(gastric vs. duodenal), and the type of ulcer complication
Majority of peptic ulcers were treated by a variant of one of
the three basic operations: parietal cell vagotomy, also called
highly selective vagotomy (HSV) or proximal gastric
vagotomy, vagotomy and drainage (V+D), and vagotomy and
distal gastrectomy. Recurrence rates are lowest but morbidity
highest with the distal gastrectomy, while in highly selective
vagotomy high recurrence rate. HSV has not performed
particularly well for type II (gastric and duodenal) and type III
(prepyloric) gastric ulcer, perhaps because of
NOTES: hypergastrinemia caused by gastric outlet obstruction and
Medications persistent antral stasis.
• Proton pump inhibitors are the mainstay of medical
therapy for PUD, but highdose H2RAs and sucralfate V + D is widely accepted as a successful definitive operation
can also be effective. Patients hospitalized for ulcer for complicated PUD. Although vagotomy and antrectomy (V
complications should receive high-dose intravenous + A) is associated with a very low ulcer recurrence rate and is
PPI and, when discharged, should be considered for applicable to many patients with complicated PUD, V + A has
lifelong PPIs unless the definitive cause is eliminated a higher operative mortality risk (compared with HSV or V +
or a definitive operation performed D), and is irreversible. V + A should be avoided in
• Antibiotics: Amoxicillin, Tetracycline, Clarithromycin. hemodynamically unstable patients, and in patients with
Diagnostics extensive inflammation and/or scarring of the proximal
• Upper GI endoscopy duodenum, because secure anastomosis (Billroth I) or
• Sclerosing agents duodenal closure (Billroth II) may be difficult.
• Upper GI series or barium swallow
NOTES:
Indication for Surgery: Pyloroplasty: dilation of the pylorus (done to compensate for
1. Intractability decreased gastric emptying after vagotomy)
2. Bleeding Heineke-Mikulicz pyloroplasty consists of a longitudinal
3. Perforation→ peritonitis→ air under the incision through the pylorus from the distal antrum to the
diaphragm proximal duodenum. This incision is closed transversely to
TERMS USED IN SURGICAL MANAGEMENT increase the diameter of the pyloric channel.
Following antrectomy, GI continuity may be reestablished
with a Billroth I gastroduodenostomy or a Billroth II loop
gastrojejunostomy
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 7|8
Surgery Rotation CLERKSHIP
NOTES:
• Bleeding is the most common cause of ulcer related
death.
• It is likely that patients currently coming to
operation for bleeding PUD are at higher risk for a
poor outcome than ever before.
• The surgical options for treating bleeding PUD
include:
▪ Suture ligation of the bleeder
▪ Suture ligation and definitive non-resective
ulcer operation
▪ Gastric resection
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 8|8
Surgery Rotation CLERKSHIP
A. Airway Management with Cervical Spine
ILOILO DOCTORS’ COLLEGE OF MEDICINE Protection
Molo, Iloilo City S.Y. 2020-2021 ➢ Level of Consciousness
➢ Establish Definitive Airway
BATCH 2021
DISCIMUS SAPIENCIA UT VIRTUS ➢ Assess Need for:
◆ Intubation
SURGERY CLERKSHIP ◆ Cricothyroidotomy
◆ Emergent Tracheostomy
LECTURER: DR. LAGOS
MAIN TOPIC: TRAUMA ➢ Ensuring a patent airway is the priority in
the primary survey.
TRAUMA ➢ Ssimultaneously, all patients with blunt
✓ Cellular disruption caused by environmental trauma require cervical spine
energy that is beyond the body’s resilience, immobilization until injury is excluded.
which is compounded by cell death due to ➢ All patients with blunt injury should be
ischemia/ reperfusion. assumed to have unstable cervical spine
✓ Most common cause of death in ages 1-44 injuries until proven otherwise.
years
✓ 3rd most common cause of death regardless ➢ Options for Endotracheal Intubation
of age 1. Orotracheal Intubation
2. Nasotracheal Intubation
INITIAL EVALUATION AND RESUSCITATION 3. Operative Routes
Phases: (Cricothyroidotomy,
1. Primary Survey Tracheostomy)
2. Secondary Survey ➢ Indication for emergency endotracheal
3. Definitive Care intubation:
4. Tertiary Care ✓ acute airway obstruction
✓ hypoventilation
Primary Survey ✓ severe hypoxemia despite
Goal: To identify and treat conditions that constitute an supplemental oxygen
immediate threat to life ✓ altered mental status (eg GCS
“ABCDE”: <8)
Airway ✓ Cardiac arrest
Breathing ✓ Severe hemorrhagic shock
Circulation
Disability
Exposure
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 1|13
Surgery Rotation CLERKSHIP
B. Breathing and Ventilation 2. Open Pneumothorax
➢ Adequate oxygenation and ventilation
must be ensured. ➢ “sucking chest wound”
➢ Assess for: ➢ Permits free communication between the
1. Tension pneumothorax pleural space and the atmosphere.
2. Open pneumothorax ➢ Complete occlusion of the chest wall defect
3. Flail chest with underlying without a tube thoracostomy may convert
pulmonary contusion an open pneumothorax to a tension
4. Massive hemothorax, and pneumothorax.
5. Major air leak due to a ➢ Open Pneumothorax Management
tracheobronchial injury. Temporary management: cover the
wound with an occlusive dressing
1. Tension Pneumothorax that is taped on three sides
➢ Respiratory distress and hypotension with any of
the following: Definitive treatment: closure of the
1. Tracheal deviation away from the affected side chest wall defect and tube
2. Lack/decreased breath sounds on the affected thoracostomy remote from the
side wound
3. Subcutaneous emphysema on the affected
side
➢ Patients may have distended neck veins due to
impedance of venous return, but the neck veins
may be flat due to concurrent systemic
hypovolemia.
A. Full-thickness loss of the chest wall results in an
open pneumothorax. B. The defect is temporarily
managed with an occlusive dressing that is taped on
three sides, which allows accumulated air to escape
from the pleural space and thus prevents a tension
pneumothorax. Repair of the chest wall defect and
tube thoracostomy remote from the wound is definitive
treatment.
3. Flail Chest
➢ Occurs when three or more contiguous ribs are
fractured in at least two locations.
➢ Paradoxical movement of this free-floating
segment of chest wall is usually evident in
patients with spontaneous ventilation, due to the
negative intrapleural pressure of inspiration.
➢ Pulmonary contusions often progress during the
first 12 hours.
➢ Resultant hypoventilation and hypoxemia may
require intubation and mechanical ventilation.
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 2|13
Surgery Rotation CLERKSHIP
interfere with the performance of other
diagnostic and therapeutic thoracic
procedures.
➢ A rule of thumb to consider for
secondary access is placement of
femoral access for thoracic trauma and
jugular or subclavian access for
abdominal trauma.
➢ On this section of the primary survey,
A. Admission chest film may not show the full extent of four life-threatening injuries must be
the patient’s pulmonary parenchymal injury. This identified promptly:
patient’s left pulmonary contusion blossomed 12 hours 1. massive hemothorax
later, and its associated opacity is noted on repeat chest 2. cardiac tamponade
radiograph. The patient’s initial chest radiograph often 3. massive hemoperitoneum and
underestimates the extent of the pulmonary 4. mechanically unstable pelvic
parenchymal damage close monitoring and frequent fractures with bleeding
clinical re-evaluation are warranted.
1. Massive Hemothorax
➢ >1500 mL of blood
4. Major Air Leak ➢ >25% of the patient’s blood volume
➢ Occurs from tracheobronchial injuries in the pleural space (pediatrics)
➢ Type I: ➢ Tube thoracostomy is the only
◆ occurring within 2 cm of the carina. reliable means to quantify the
◆ these may not be associated with a amount of hemothorax
pneumothorax due to the envelopment
in the mediastinal pleura.
➢ Type II:
◆ more distal injuries within the
tracheobronchial tree and hence
manifest with a pneumothorax.
➢ Bronchoscopy confirms the extent of the
injury and its location, and directs
management.
C. Circulation with Hemorrhage Control
➢ In general, any episode of hypotension
(defined as a SBP <90 mmHg) is
assumed to be caused by hemorrhage A massive hemothorax is an indication for operative
until proven otherwise. intervention. Tube thoracostomy is critical to facilitate
➢ Blood pressure and pulse should be lung reexpansion, which may improve
measured at least every 5 minutes in oxygenation and cardiac performance as well as
patients with significant blood loss until tamponade venous bleeding.
normal vital sign values are restored.
➢ Intravenous (IV) access for fluid Picture: More than 1500 mL of blood in the pleural
resuscitation and medication space is considered a massive hemothorax. Chest film
administration is obtained with two findings reflect the positioning
peripheral catheters of the patient. A. In the supine position, blood tracks
➢ Intraosseous infusions are indicated for along the entire posterior section of the chest and is
patients in whom one or two attempts at most notable pushing the lung away
IV access have failed. from the chest wall. B. In the upright position, blood is
➢ In general, initial access in trauma visible dependently in the right pleural space.
patients is best secured in the groin so
that placement of the catheter will not
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 3|13
Surgery Rotation CLERKSHIP
2. Cardiac Tamponade because the one-handed massage technique
➢ Occurs after penetrating thoracic wounds poses the risk of myocardial perforation with the
➢ <100mL of pericardial blood may cause thumb.
pericardial tamponade
➢ Beck’s Triad:
dilated neck veins
muffled heart sounds
decline in arterial pressure
➢ Pericardiocentesis is successful in decompressing
tamponade in approximately 80% of cases;
the majority of failures are due to the
presence of clotted blood within the
pericardium.
➢ Patients with a persistent SBP <60 mmHg warrant
resuscitative thoracotomy (RT) with opening
of the pericardium for rapid decompression
and control of bleeding.
D. Disability and Exposure
➢ The Glasgow Coma Scale (GCS) score
should be determined for all injured
patients.
➢ The GCS is a quantifiable determination
of neurologic function that is useful for
triage, treatment, and prognosis.
➢ An abnormal mental status should
prompt an immediate reevaluation of the
patient’s ABCs and consideration of
central nervous system injury.
1. Pericardiocentesis is indicated for patients with
evidence of pericardial tamponade. A. Access to GCS 15 - normal
the pericardium is obtained through a subxiphoid GCS 3 - lowest
approach, with the needle angled 45° up from the Mild injury - GCS 13-15
chest wall and toward the left shoulder. B. Moderate injury - GCS 9 to 12
Seldinger technique is used to place a pigtail Severe injury - GCS ≤8
catheter. Blood can be repeatedly aspirated with a
syringe, or the tubing may be attached to a gravity
drain. Evacuation of unclotted pericardial blood
prevents subendocardial ischemia and stabilizes
the patient for transport to the operating room for
sternotomy.
2. A. Resuscitative thoracotomy (RT) is performed
through the fifth intercostal space using the
anterolateral approach. B and C. The pericardium
is opened anterior to the phrenic nerve, and the
heart is rotated out for evaluation. D. Open
cardiac massage should be performed with a
hinged, clapping motion of the hands, with
sequential closing from palms to fingers. The two-
handed technique is strongly recommended
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 4|13
Surgery Rotation CLERKSHIP
Shock Classification and Initial Fluid Resuscitation 3. NONRESPONDERS
➢ Classic signs and symptoms: ✓ persistent hypotension despite
tachycardia aggressive resuscitation
hypotension
tachypnea Persistent Hypotension
altered mental status ➢ Underlying causes:
diaphoresis ✓ hemorrhagic
pallor ✓ cardiogenic
➢ Tachycardia (HR >110 bpm) is often the ✓ neurogenic
earliest sign of ongoing blood loss, but the ➢ Persistent hypotension- high mortality
critical issue is change in HR over time. ➢ Rapid search for the source of hemorrhage -
➢ Bradycardia can occur with rapid severe visual inspection, eFAST, and chest and pelvic
blood loss; this is an ominous sign, often radiographs.
heralding impending cardiovascular ➢ In patients with persistent hypotension and no
collapse. clear operative indications, evaluate the scalp,
chest, abdomen, pelvis, and extremities.
➢ Fracture-related blood loss, when additive,
may be a potential source of the patient’s
hemodynamic instability.
rib fracture-100-200mL of blood loss
tibial fractures- 300-500 mL of blood loss
femur fractures- 800-1000 mL of blood
loss
pelvic fractures- >2000 mL of blood loss
SSECONDARY SURVEY
➢ In general, the quantity of acute blood loss ✓ Thorough History
correlates with physiologic abnormalities. ✓ AMPLE history (Allergies, Medications, Past
➢ The goal of fluid resuscitation is to re- illnesses or Pregnancy, Last meal, and Events
establish tissue perfusion. related to the injury).
➢ Fluid resuscitation usually begins with isotonic ✓ Complete Physical Examination (special
crystalloid, typically Ringer’s lactate attention to the patient’s back, axillae, and
➢ Urine output is a reliable indicator of organ perineum)
perfusion but requires time to quantitate. ✓ Digital Rectal Examination
➢ Adequate urine output: ✓ Vaginal examination
✓ 0.5 mL/kg/hr- adult
✓ 1 mL/kg/hr- child DIAGNOSTIC EVALUATION
✓ 2 mL/kg/hr- infant <1 year of age ➢ Selective radiography and lab tests
➢ For patients with severe blunt trauma: lateral
Hypovolemic Patients cervical spine, chest and pelvic radiographs
1. RESPONDERS (Big three)
✓ Stable ➢ For patients with truncal gunshot wounds: AP
✓ Have a good response to initial fluid and lateral radiographs of the chest and
therapy abdomen
✓ Normal vital signs, mental status and ➢ In critically injured patients: blood samples
urine output for a routine trauma panel (type and cross-
✓ No hemorrhage match, CBC, blood chemistries, coagulation
✓ Diagnostic evaluation for occult injuries studies, lactate level, and ABG)
can proceed in an orderly fashion ➢ For less severely injured patients: CBC and
urinalysis
2. TRANSIENT RESPONDERS
✓ Respond initially to volume loading
with improvement in vital signs but
subsequently deteriorate
hemodynamically
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 5|13
Surgery Rotation CLERKSHIP
Mechanisms and Patterns of Injury
1. Blunt trauma
➢ In blunt trauma, organs that cannot yield to
impact by elastic deformation are most likely
to be injured, namely, the solid organs (liver,
spleen, and kidneys).
➢ It is associated with multiple widely
distributed injuries.
2. Penetrating trauma
➢ Organs with the largest surface area are most
prone to injury (small bowel, liver, and colon).
Additionally, because bullets and knives Epidural hematomas
usually follow straight lines, adjacent A. have a distinctive convex shape on computed
structures are commonly injured. tomographic scan, whereas subdural
➢ Can be stab, gunshot or shotgun wound. hematomas
B. are concave along the surface of the brain.
Regional Assessment and Special Diagnostic Tests
➢ Based on mechanism, location of injuries
identified on physical examination, screening 2. NECK assessment
radiographs, and the patient’s overall condition, ➢ All blunt trauma patients should be
additional diagnostic studies often are indicated. assumed to have cervical spine injuries,
until proven otherwise
1. HEAD assessment ➢ PE: maintain cervical spine precautions
➢ includes examination for injuries to the and in-line stabilization.
scalp, eyes, ears, nose, mouth, facial ➢ Patients with high spinal cord disruption:
bones, and intracranial structures risk for shock
➢ Head palpation: identify scalp lacerations ➢ Indications for immediate operative
(depth and associated depressed/open intervention for penetrating cervical
skull fractures) injury: hemodynamic instability,
➢ Eye examination: pupillary size and significant external hemorrhage,
reactivity, visual acuity and presence of evidence of aerodigestive injury.
hemorrhage within the globe ➢ For the purpose of evaluating
◆ Ocular entrapment: penetrating injuries, the neck is divided
impingement of the ocular into three zones.
muscles, patient cannot move Zone I is to the level of the clavicular
eyes through an entire range of heads and is also known as the thoracic
motion outlet.
➢ Tympanic membrane examination: Zone II is located between the
identify hemotympanum, otorrhea, or clavicles and the angle of the mandible.
rupture Zone III is above the angle of the
◆ Basilar skull fracture: otorrhea, mandible
rhinorrhea, raccoon eyes, and ➢ For the purpose of evaluating
Battle’s sign (ecchymosis penetrating injuries, the neck is divided
behind the ear) into three zones. Zone I is to the level of
➢ All patients with a significant closed head the clavicular heads and is also known as
injury (GCS score <14) should undergo the thoracic outlet. Zone II is located
CT scanning of the head. between the clavicles and the angle of
➢ Intracranial lesions following trauma the mandible. Zone III is above the angle
include hematomas, contusions, of the mandible
hemorrhage into ventricular and
subarachnoid spaces, and diffuse axonal
injury (DAI).
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 6|13
Surgery Rotation CLERKSHIP
➢ TREATMENT: Head Injuries
Intracranial Injuries 1. Le Fort type I
✓ CT scanning in patients with a a) horizontal maxillary fracture,
significant closed head injury (GCS separating the teeth from the upper
score <14). face
✓ Indications for operative intervention b) fracture line passes through the
to remove space occupying alveolar ridge, lateral nose and
hematomas: clot volume, amount of inferior wall of the maxillary sinus
midline shift, location of the clot, 2. Le Fort type II
GCS score, and ICP. a) pyramidal fracture, with the teeth at
✓ CT scanning, performed on all the pyramid base, and nasofrontal
patients with a significant closed suture at its apex
head injury (GCS score <14), b) fracture arch passes through the
identifies and quantitates posterior alveolar ridge, lateral walls
intracranial lesions as well as of maxillary sinuses, inferior orbital
intracranial hypertension. Patients rim and nasal bones
with intracranial hemorrhage, c) uppermost fracture line can pass
including epidural hematoma, through the nasofrontal junction or
subdural hematoma, subarachnoid the frontal process of the maxilla 3
hemorrhage 3. Le Fort type III
✓ Intracerebral hematoma or a) craniofacial disjunction
contusion, and diffuse axonal injury, b) transverse fracture line passes
are admitted to the SICU. through nasofrontal suture, maxillo-
✓ A burr hole is made for frontal suture, orbital wall,
decompression of an epidural and zygomatic
hematoma as a life-saving arch / zygomaticofrontal suture
maneuver. One or more branches of c) because of the involvement of the
the external carotid artery usually zygomatic arch, there is a risk of
must be ligated to gain access to the the temporalis muscle impingement
skull. No attempt should be made to
control intracranial hemorrhage ✓ maxillofacial complex 3 regions: the
through the burr hole. Rather, the upper face (frontal sinus and brain), the
patient’s head should be wrapped midface (orbits, nose, and zygomatico-
with a bulky absorbent dressing and maxillary complex), and the lower face
the patient transferred to a (mandible)
neurosurgeon for definitive care. ✓ most common scenario (life-threatening):
bleeding from facial fractures
Maxillofacial Injuries ✓ After initial stabilization systematic head
✓ common with multisystem trauma & neck PE
✓ coordinated management: trauma &
specialists (otolaryngology, plastic
surgery, ophthalmology, and oral
and maxillofacial surgery)
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 7|13
Surgery Rotation CLERKSHIP
➢ TREATMENT: Neck Injuries ➢ INJURY TO THE GREAT VESSELS
Cervical Injuries
A. Spine: level of injury, the stability of the
spine, the presence of subluxation, the
extent of angulation, the level of
neurologic deficit, and the overall
condition of the patient
B. Vascular: repair techniques apply to
carotid injuries; end-to-end primary
repair, graft interposition, and
transposition procedures
C. Aerodigestive: Fractures of the larynx
and trachea may manifest as cervical
emphysema. Fractures documented by LEFT SIDED HEMATOMAS-Descending blunt aortic
CT scan are usually repaired. injuries
3. CHEST assessment RIGHT SIDED HEMATOMAS-
➢ Most common injuries from both blunt
and penetrating thoracic trauma are A. Widening of the mediastinum on initial
hemothorax and pneumothorax. anteroposterior chest radiograph, caused by a
➢ Blunt trauma to the chest: hematoma around an injured vessel that is
1. The chest wall contained by the mediastinal pleura.
2. Thoracic spine and thoracic B. Location of the hematoma within the mediastinal
aorta silhouette suggests the type of great vessel
3. Heart, and Great vessels injury
4. Lungs C. Left-sided hematomas are associated with
5. Esophagus (Rarely) descending blunt aortic injuries
➢ EVALUATION: PE, *CHEST D. Right-sided hematomas are seen with innominate
RADIOGRAPHY, CT SCANNING injuries
Persistent pneumothorax - Fiber optic bronchoscopy to
exclude tracheobronchial injury or foreign bodies
Persistent hemothorax/Caked Hemothorax -
Immediate thoracotomy
Apical capping
FINDINGS ON CHEST RADIOGRAPH SUGGESTIVE OF
DESCENDING
THORACIC AORTIC TEAR:
1. WIDENED MEDIASTINUM
2. ABNORMAL AORTIC CONTOUR
3. TRACHEAL SHIFT
4. NASOGASTRIC TUBE SHIFT
5. LEFT APICAL CAP
6. LEFT OR RIGHT PARASPINAL STRIPE
Persistent pneumothorax- large air leaks after tube THICKENING
thoracostomy 7. DEPRESSION OF THE LEFT MAIN
BRONCHUS
Caked hemothorax- is not drained by two chest tubes. 8. OBLITERATION OF AORTIC PULMONARY
WINDOW
9. LEFT PULMONARY HILAR HEMATOMA
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 8|13
Surgery Rotation CLERKSHIP
➢ Penetrating thoracic trauma -Over 90% of thoracic In the picture, “clamshell” thoracotomy provides
great vessel injuries are due to penetrating exposure to bilateral thoracic cavities
trauma
1. Physical examination ➢ Median sternotomy with cervical
2. Plain posteroanterior and lateral chest extension
radiographs with metallic markings of wounds 1. Proximal subclavian,
3. Pericardial ultrasound innominate, or proximal carotid
➢ More than 85% of patients can be definitively artery injuries.
treated with a chest tube. 2. Care must be taken- avoid
➢ Indications for thoracotomy injury to the phrenic and vagus
nerves
Care must be taken- avoid injury to
the phrenic and vagus nerves that pass
over the subclavian artery and to the
recurrent laryngeal nerve passing
posteriorly
➢ Posterolateral thoracotomies
A. Right posterolateral
thoracotomy- injuries to the
trachea or main stem bronchi
near the carina or the upper
esophagus
B. Left posterolateral
thoracotomy-descending
thoracic aorta or lower
esophagus
➢ GREAT VESSELS -
✓ Bypass exclusion technique-
Innominate artery injuries
➢ THORACIC INCISIONS
ANTEROLATERAL THORACOTOMY
1. Supine
2. Most versatile incision for
emergent thoracic exploration
3. 5th interspace inframammary
line
➢ Clamshell thoracotomy
1. For access to both pleural
cavities,
2. Original incision can be .
extended across the sternum In the first stage of the bypass exclusion technique, a
with a Lebsche knife 12-mm polytetrafluoroethylene graft is anastomosed
end to side from the proximal undamaged aorta,
tunneled under the vein, and anastomosed end to end
to the innominate artery. C. The origin of the
innominate is then oversewn at its base to exclude the
pseudoaneurysm.
✓ Descending BAI may require urgent intervention.
✓ To prevent aortic rupture:
✓ pharmacologic therapy with a selective
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 9|13
Surgery Rotation CLERKSHIP
✓ B1-antagonist, esmolol, should be instituted in the ➢ CHEST- Other injuries
trauma bay, Trachea, Bronchi and Lung
✓ with a target SBP of <100 mmHg and heart rate of Parenchyma
<100/min.41,98 1. < 1% of all injured patients
✓ Endovascular stenting is now the mainstay of sustain intrathoracic
treatment tracheobronchial injuries,
2. Small number require operative
intervention. T
Open Repair of Descending 3. Empyema- most common
aorta complication. Management is
based on CT diagnostic criteria.
When repairing a tear of the Esophagus
descending thoracic aorta, 1. Injuries often occur with
perfusion of the spinal cord tracheobronchial injuries
while the aorta is clamped is achieved by using partial 2. With sufficient mobilization, a
left heart bypass. The venous cannula is inserted into primary single-layer end-to-end
the left superior pulmonary vein because it is less anastomosis may be performed
prone to tearing than the left atrium. after appropriate debridement
Chest Wall and Diaphragm:
✓ Lateral aortorrhaphy- Simple lacerations of the Virtually all chest wall injuries are
ascending or transverse aortic arch treated non-operatively with:
✓ Full cardiopulmonary bypass- Posterior aortic 1. Pain control
injuries, complex ascending or transverse 2. Pulmonary toilet or ventilatory
injuries, interposition grafting of the arch management
✓ PTFE graft interposition- Subclavian artery 3. Drainage of the pleural space as
injuries indicated.
Blunt diaphragmatic injuries usually
➢ CHEST- HEART result in a linear tear and most are large
Definitive repair of cardiac injuries is Penetrating diaphragmatic injuries are
performed with either running 3-0 variable in size and location depending on
polypropylene suture or interrupted, the agent of injury.
pledgeted 2-0 polypropylene suture * Regardless of the etiology, acute
diaphragmatic injuries are usually repaired
through an abdominal approach to manage
potential associated visceral injury.
4. Abdomen assessment
➢ Evaluation of the head includes
examination for injuries to the scalp,
eyes, ears, nose, mouth, facial bones,
and intracranial structures
Liver and Extrahepatic Biliary Tract:
✓ The liver’s large size makes it the organ
most susceptible to blunt trauma, and it
is frequently involved in upper torso
A variety of techniques may be necessary penetrating wounds.
to repair cardiac wounds. Generally, pledget ✓ Initial control of hemorrhage is best
support is used for the relatively thinwalled accomplished using perihepatic packing
right ventricle and manual compression.
✓ With extensive injuries and major
hemorrhage, a Pringle maneuver should
be done immediately.
✓ If bleeding continues despite repeated
attempts at packing, then direct repair,
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 10|13
Surgery Rotation CLERKSHIP
with or without hepatic vascular isolation, ✓ Extensive injuries of the first portion of
should be attempted. the duodenum (proximal to the duct of
✓ Pringle Maneuver - technique to Santorini) can be repaired by
minimize blood loss during hepatic debridement and end-to-end
surgery by clamping the vascular pedicle anastomosis.
✓ Three Techniques used in hepatic ✓ The second portion is tethered to the
vascular isolation: head of the pancreas by its blood supply
a) direct repair with suprahepatic and and the ducts of Wirsung and Santorini,
infrahepatic clamping of the vena should be “patched” with a Roux-en-Y
cava and stapled assisted duodenojejunostomy.
parenchymal resection ✓ Injuries in the distal third and fourth
b) temporary shunting of the portions of the duodenum (behind the
retrohepatic vena cava mesenteric vessels) should be resected,
c) venovenous bypass and a duodenojejunostomy should be
performed on the D3 side of the superior
Spleen: mesenteric vessels
✓ Splenic injuries are managed operatively ✓ Optimal management of pancreatic
by splenectomy, partial splenectomy, or trauma is determined by
splenic repair (splenorrhaphy), based on 1. Where the parenchymal damage is
the extent of the injury and the located and
physiologic condition of the patient. 2. Whether the intrapancreatic
✓ Subphrenic abscess common bile duct and main
1. Common complication after pancreatic duct remain intact.
splenectomy ✓ Pancreatic contusions- non-operatively or
2. Percutaneous drainage with closed suction drainage.
✓ Postsplenectomy sepsis ✓ Proximal pancreatic injuries- closed
◼ caused by Streptococcus suction drainage
pneumoniae, Haemophilus ✓ Distal ductal disruption- distal
influenzae, and Neisseria pancreatectomy, preferably with splenic
meningitidis, preservation.
◼ Resistant to antimicrobial treatment. ✓ Pancreatic head injuries- Distal
◼ Prophylaxis: vaccine administered pancreatectomy or Central
optimally at >14 days postinjury. pacreatectomy
✓ Complications:
Stomach and Small Intestine: Delayed hemorrhage-
✓ Gastric wounds can be oversewn with a angioembolization
running single-layer suture line or closed Pancreatic and duodenal fistulas-
with a stapler. adequate drainage
✓ Small intestine injuries can be repaired Pancreatic pseudocysts- ERCP
using a transverse running 3-0 PDS Intra-abdominal abscesses-
suture if the injury is less than one-third percutaneous drainage
the circumference of the bowel.
Colon and Rectum
Duodenum and Pancreas: There are 3 methods used for treating
✓ The spectrum of injuries to the colonic injuries:
duodenum includes hematomas, 1. Primary repair
perforation and combined pancreatico 2. End colostomy
duodenal injuries. 3. Primary repair with diverting loop
✓ The majority of duodenal hematomas are ileostomy
managed non-operatively with ✓ All suturing and anastomoses are
nasogastric suction and parenteral performed using a running single-layer
nutrition. technique.
✓ Patients with suspected associated ✓ Current options for treating rectal injuries
perforation should undergo operative are loop ileostomy and sigmoid loop
exploration. colostomy.
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 11|13
Surgery Rotation CLERKSHIP
✓ If the rectal injury is extensive, another 5. Extremity Vascular Injuries, Fractures, and
option is to divide the rectum at the level Compartment Syndromes
of the injury, oversew or staple the distal ➢ Patients with injured extremities,
rectal pouch if possible, and create an immediate stabilization of fractures or
end colostomy (Hartmann’s procedure). unstable joints is done in the ED using
Hare traction, knee immobilizers, or
plaster splints.
➢ Patients with open fractures, the wound
should be covered with povidone-iodine
(Betadine)-soaked gauze and antibiotics
administered.
➢ Options for fracture fixation include
external fixation or open reduction and
internal fixation with plates or
intramedullary nails.
➢ Vascular injuries, either isolated or in
combination with fractures, require
emergent repair
➢ Common combined injuries:
1. clavicle/first rib fractures and
subclavian artery injuries
Abdominal and Pelvic Vasculature 2. dislocated shoulder/proximal
✓ Penetrating trauma indiscriminately humeral fractures and axillary artery
affects all blood vessels, blunt trauma injuries
most commonly involves renal 3. supracondylar fractures/elbow
vasculature and occasionally the dislocations and brachial artery
abdominal aorta. injuries
4. femur fracture and superficial
Genitourinary Tract femoral artery injuries
✓ Parenchymal renal injuries are treated 5. knee dislocation and popliteal
with hemostatic and reconstructive vessel injuries
techniques.
✓ Bladder injuries are subdivided into: Compartment Syndromes
1. Intraperitoneal extravasation- ➢ acute increase in pressure inside a closed
operatively closed with a running, space, which impairs blood flow to the
single-layer, 3-0 absorbable structures within.
monofilament suture ➢ Causes:
2. Extraperitoneal extravasation- ◼ arterial hemorrhage
treated non-operatively with bladder ◼ venous ligation or thrombosis
decompression for 2 weeks. ◼ crush injuries
✓ Urethral injuries are managed by ◼ reperfusion injury
bridging the defect with a Foley catheter, ➢ In conscious patients, pain is the
with or without direct suture repair. prominent symptom, and active or
passive motion of muscles in the involved
compartment increases the pain.
Paresthesias may also be described. In
the lower extremity, numbness between
the first and second toes is the hallmark
of early compartment syndrome.
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 12|13
Surgery Rotation CLERKSHIP
Abdominal Compartment Syndrome
➢ Classified as pathologic intra-abdominal Generally, no specific bladder pressure prompts
hypertension due to intra-abdominal therapeutic intervention, except when the pressure is
injury (primary) or splanchnic reperfusion >35 mmHg. Emergent decompression is carried out
after massive resuscitation (secondary). when intra-abdominal hypertension reaches a level at
➢ The most common technique for the which end-organ dysfunction occurs.
diagnosis is to measure the patient’s
bladder pressure. Abdominal compartment syndrome is defined by the
➢ Fifty milliliters of saline is instilled into the end organ sequelae of intra-abdominal hypertension.
bladder via the aspiration port of the CO = cardiac output;
Foley catheter with the drainage tube CVP = central venous pressure; ICP = intracranial
clamped, and a three-way stopcock and pressure; PA = pulmonary artery; SV = stroke volume;
water manometer is placed at the level of SVR = systemic vascular resistance; UOP = urine
the pubic symphysis output; VEDV = ventricular end diastolic volume.
➢ Secondary abdominal compartment
syndrome may result from any condition
requiring extensive crystalloid
resuscitation, including extremity trauma,
chest trauma, or even postinjury sepsis.
➢ The sources of increased intra-abdominal
pressure include bowel edema, ascites,
bleeding, and packs. A diagnosis of intra-
abdominal hypertension cannot reliably
be made by physical examination;
therefore, it is obtained by measuring the
intraperitoneal pressure. The most
common technique is to measure the
patient’s bladder pressure
First picture - Bladder pressure is measured on the
manometer in centimeters of water and correlated with
the physiologic sequelae. Conditions in which the
bladder pressure is unreliable include bladder rupture,
external compression from pelvic packing, neurogenic
bladder, and adhesive disease.
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 13|13
Surgery Rotation CLERKSHIP
ILOILO DOCTORS’ COLLEGE OF MEDICINE ANATOMY
Molo, Iloilo City S.Y. 2020-2021 • A true diverticulum of the cecum as it contains all
the histological layers of the colon
• Average appendix measures 6-9 cm
BATCH 2021
DISCIMUS SAPIENCIA UT VIRTUS • Base – follows the longitudinally oriented taeniae
coli to their confluence on the cecum; constant in
SURGERY CLERKSHIP location
• Tip – is not constant of its location
LECTURER: DR. FERNANDEZ ET AL • Outer diameter: 3-8 mm
MAIN TOPIC: APPENDIX • Luminal Diameter: 1-3 mm
FUNCTION
HISTORY • Previously believed to be a vestigial organ
❑ Claudius Amyand (early 18th century) - first surgeon • Currently linked to the development and
to describe a successful appendectomy preservation of gut-associated lymphoid tissue
❑ Chester McBurney (1889) - advocated for early (GALT)
appendectomy • Maintenance of intestinal flora
❑ 1940’s - introduction and widespread use of • An immunologic organ that actively participates in
antibiotics the secretion of immunoglobulins, particularly
❑ Kurst Semm (1982) - a gynecologist, reported on immunoglobulin A
first laparoscopic appendectomy • A reservoir to recolonize the colon with healthy
bacteria
EMBRYOLOGY
POSITION
• In the 6th week of human embryonic
development, the appendix and cecum appear
as outpouchings from the caudal limb of the
midgut.
• Appendicial outpouching, initially noted in the
8th week, begins to elongate at about the 5th
month to achieve a vermiform appearance.
• As the gut rotates medially, the cecum becomes
fixed in the right lower quadrant, thus
determining the final position of the appendix
HISTOLOGY
MCBURNEY’S POINT
• 3 LAYERS: • It is found 1/3 of the distance between the right
o OUTER SEROSA – extension of the peritoneum anterior superior iliac spine and the umbilicus
o MUSCULARIS LAYER – not well defined and • Often the point of maximal tenderness in a patient
may be absent in certain locations with anatomically normal appendix
o SUBMUCOSA AND MUCOSA
– lymphoid aggregates occur in the BLOOD SUPPLY
submucosal layer and may extend into the
• Arterial supply: APPENDICULAR BRANCH OF THE
muscularis mucosa
ILEOCOLIC ARTERY
– the mucosa is like that of the large
• Originates posterior to the terminal ileum, entering
intestine, except for the density of the lymphoid
the mesoappendix close to the base of the appendix
follicles
AUTONOMIC INNERVATION
• CRYPTS (Crypts of Lieberkuhn)
• Derived from sympathetic elements contributed by
o APPENDIX: irregularly sized and shaped
the superior mesenteric plexus (T10-L1)
o COLON: more uniform in appearance
• Afferents from the parasympathetic elements via the
o Neuroendocrine complexes (ganglion cells,
vagus nerves.
Schwann cells, neural fibers, and neurosecretory
cells) are positioned just below the crypts.
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 1|8
Surgery Rotation CLERKSHIP
ACUTE APPENDICITIS diapedesis, appendiceal distention due to
accumulated fluid, and increasing
• Inflammation of the appendix caused by obstruction intraluminal pressure.
of the appendiceal lumen - Visceral afferent nerve fibers are
• More common in males (8.6%), while in females stimulated, and the patient perceives mild
(6.7%) visceral periumbilical or epigastric pain,
• Highest incidence in the 2nd and 3rd decades of life which usually lasts 4-6 hours.
• SUPPURATIVE
ETIOLOGY - Obstruction of lymphatic and venous
• Luminal obstruction due to lymphoid hyperplasia drainage leading to bacterial multiplication
(pediatrics) or due to fecaliths, fibrosis, foreign - Inflammation progresses to the parietal
bodies (parasite and food), or neoplasia (adults) peritoneum, classic shift of pain from the
MICROBIOLOGY periumbilicus to the right lower abdominal
• 60% of aspirates of inflamed appendices have quadrant (RLQ) will occur.
anaerobes (25% in normal appendices) • GANGRENOUS
• Tissue specimens from the inflamed appendix wall - Intramural venous and arterial thromboses
virtually all grow Escherichia coli and • RUPTURED/PERFORATED
Bacteroides species - Persistent tissue ischemia results in
• Fusobacterium nucleatum/necrophorum (not appendiceal infarction and perforation.
present in normal cecal flora) has been - Perforation can cause localized or
identified in 62% of inflamed appendices. generalized peritonitis.
• Peptostreptococcus, Pseudomonas, Bacteroides
splanchnicus, Bacteroides intermedius,
Lactobacillus
• Fastidious gram-negative anaerobic bacili
• Bacteroides – more common in patients with
gangrene or perforated appendicitis
PATHOPHYSIOLOGY
SYMPTOMS
• Vague, dull, diffuse mid-abdominal pain
• Crampy abdominal pain
• Anorexia
• Nausea
• Vomiting
• Localization to the right lower quadrant
• Generalized abdominal pain
SIGNS
• Early in presentation: Vital signs are minimally
altered
• Changes of greater magnitude in vital signs:
complication
• Patients move slowly
PERIUMBILICAL PAIN: Due to visceral nerve fibers and • Prefer to lie supine due to the peritoneal irritation
stimulation & dermatome affected
LOCALIZATION TO THE RLQ: Serosa of the appendix is already PHYSICAL EXAM
involved
• INSPECTION:
o Patients move slowly, and prefer to lie supine
STAGES
• PALPATION:
• CONGESTIVE
o Warm to touch (low-grade fever, ~38.0oC)
- Obstruction of the appendiceal lumen leads
o Tenderness with maximum at or near
to mucosal edema, ulceration, bacterial
McBurney’s point
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 2|8
Surgery Rotation CLERKSHIP
o Deep palpation: muscular resistance (guarding) DIAGNOSTIC AND ANCILLARY PROCEDURE
in the right iliac fossa • COMPLETE BLOOD COUNT
o Mild leukocytosis (10,000 cells/mm3) - is
• SIGNS TO BE ELICITED often present in patients with acute,
o Rovsing’s sign – pain in the right lower quadrant uncomplicated appendicitis and is usually
after release of gentle pressure on the left lower accompanied by a polymorphonuclear
quadrant (normal position) prominence.
o Dunphy’s sign – pain with coughing (retrocecal o Higher leukocytosis (>18,000 cells/mm3)-
appendix) counts above this level raise the possibility
o Obturator sign – pain with internal rotation of of a perforated appendix with or without an
the hip (pelvic appendix) abscess
o Iliopsoas sign – pain with flexion of the hip • C REACTIVE PROTEIN
(pelvic appendix) o strong indicator of appendicitisespecially
for complicated appendicitis
• PAIN WITH RECTAL/CERVICAL EXAM – pelvic • URINALYSIS
appendicitis o Useful to rule out the urinary tract as the
source of infection
CLINICAL SCORING SYSTEMS o Several white or red blood cells can be
• The method relies on a combination of factors present from irritation of the ureter or
derived from physical signs, symptoms, and bladder
laboratory tests and produces a numerical score o Bacteriuria is generally not seen
used to rule in or rule out acute appendicitis.
NORMAL APPENDIX VS INFLAMED APPENDIX
ALVARADO SCORE • Normal appendix
o Ultrasonography and computed
• Most widespread scoring system. tomography (CT) scan - seen as a blind-
• Useful for ruling out appendicitis and selecting ending nonperistaltic tubular structure
patients for further workup arising from the base of the cecum. The
location of the base of the appendix is
relatively constant, located roughly
between the ileocecal valve and the apex of
the caecum.
• Inflamed appendix
o Outer-to-outer diameter - is the most
important imaging criterium.
o Threshold value of 6-7 mm is generally
used.
o An inflamed appendix has a diameter larger
than 6 mm and is usually surrounded by
inflamed fat. The presence of a fecolith or
hypervascularity on power Doppler strongly
supports inflammation.
APPENDICITIS INFLAMMATORY RESPONSE o graded compression ultrasonography
o Inexpensive, can be performed rapidly,
• Resembles the Alvarado score but uses more graded does not require a contrast medium, and
variables and includes C reactive protein. can be used in pregnant patients
• Studies have shown that it performs better than the
Alvarado score in accurately predicting appendicitis Findings supportive of the diagnosis of appendicitis include:
• Aperistaltic, noncompressible, dilated appendix
• >6 mm outer diameter
• Appendicolith
• Distinct appendiceal wall layers
• Echogenic prominent pericecal fat
• Periappendiceal hyperechoic structure (PHS)
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 3|8
Surgery Rotation CLERKSHIP
• an ultrasound finding described as an amorphous TIMING
hyperechoic structure (usually greater than 10mm) ➢ Urgent (12-24 hrs) appendectomy
• Periappendiceal fluid collection ➢ Emergent (<12 hours) appendectomy
• Target appearance (axial section) o Study shows that there is no significant
o Alternating echogenicity of the appendix difference in terms of complicated
that represents the presence of appendicitis, surgical site infection and
periappendiceal fluid and intact echogenic abscess formation.
submucosal layer
• COMPLICATED APPENDICITIS
CONTRAST-ENHANCED CT SCAN o Refers to perforated appendicitis commonly
• Highly sensitive (94-98%) and specific (up to 97%) associated with an abscess
• Allows for alternative causes of abdominal pain also o IV Antibiotics (at least 30-60 minutes prior
to be diagnosed to skin incision)
• Findings supportive of the diagnosis of appendicitis o Monotherapywith piperacillin/ tazobactam
include: or combination of cephalosporin with
• Double wall thickness metronidazole.
• dilated appendix with distended lumen o The duration of postoperative antibiotics is
• >6 mm generally less than 4 days once complete
• Thickened and enhancing wall source control has been achieved
o Conservative management - is considered
• >2 mm
for confined abscess and in patients with
• Periappendiceal fat stranding
limited peritonitis.
• periappendiceal inflammation, including stranding of
o Broad spectrum antibiotics
the adjacent fat and thickening of the lateroconal
o Bowel rest (NPO)
fascia or mesoappendix.
o Fluids (crystalloid)
• Appendicolith
o Possible percutaneous drainage - drain if
• Appendiceal wall thickening abscess is >3cm in diameter
• Arrowhead sign
o Seen as secondary sign. OPERATIVE MANAGEMENT
o Refers to the Focal cecal thickening • Failed conservative management
centered on the appendiceal orifice
• Patients with free intra-peritoneal perforation
o Applicable only when enteric contrast
• Interval Appendectomy
distends the cecum.
• Successful conservative management
o Contrast material in the cecal lumen
• 6-12 weeks later when inflammation diminished
assumes arrowhead configuration
• Prevents the recurrence
MANAGEMENT • May identify the presence of malignancy
• Uncomplicated appendicitis
o Refers to non-perforated and non- OPERATIVE INTERVENTION
gangrenous appendicitis.
o IV Antibiotics (at least 30-60 minutes prior OPEN APPENDECTOMY
to skin incision)
o Cefoxitin,ampicillin/sulbactam, and
cefazolin plus metronidazole.
o Post-op antibiotics - not necessary
o Operative: surgical treatment has been the
standard of treatment
o Non operative: is possible for patients in an
environment where surgical treatment is
not available. Study shows that treatment
with antibiotics alone was noted to be
effective. Also, many patients with signs • INDICATIONS
and symptoms consistent with appendicitis o Acute appendicitis
who did not pursue operative treatment o Interval appendectomy following
would occasionally have spontaneous conservative treatment of appendiceal
resolution of their illness. abscess
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 4|8
Surgery Rotation CLERKSHIP
o Mucocele of appendix
o Adenocarcinoma and carcinoid of appendix
• INDICATIONS
• PITFALLS o Acute appendicitis
o Inadvertent laceration of inflamed cecum o Right lower quadrant pain of unknown
dissection etiology
o Inadequate control of blood vessels in o Interval appendectomy
edematous mesoappendix
o Performed with a patient under general • PITFALLS
anesthesia. o Injury to bladder from trocars
o The patient is placed in supine position. o Injury to cecum from traction or dissection
o The bed is positioned in Trendelenburg’s o Incomplete appendectomy, resulting in a
with the left side down. retained stump
o Early nonperforated appendicitis, o Performed with a patient under general
➢ McBurney’s incision - oblique anesthesia.
fashion o The patient is placed in supine position.
➢ Rocky- Davis incision - transverse o The bed is positioned in Trendelenburg’s
incision with the left side down
o Perforated appendicitis o Location of port sites for laparoscopic
➢ Lower midline laparotomy incision appendectomy.
o Division of the mesoappendix from ➢ 5-mm ports are placed at the
appendiceal artery suprapubic and left lower quadrant
➢ Fowler extension - In the event of areas
retraction of the appendiceal ➢ 10-12-mm port is placed at the
artery or unexpected bleeding, right upper quadrant
extension or the incision can be
extended medially.
• Division of the mesoappendix using the harmonic
• Figure B - Ligation of the base and division of the scalpel.
appendix. • Figure B - Placement of an absorbable endoloop
• Figure C - Placement of purse-string suture or Z encircling the base of the appendix
stitch • Figure C - Division of the appendix between
• Figure D - Inversion of the appendiceal stump endoloops. The base of the appendix is divided
• Skin closure is performed in a layered fashion either with an endoscopic stapler or after placing an
o secondary intention or delayed primary endoloop.
closure is done if there is abscess or • Figure D - Placement of the appendix into a
contamination specimen bag before removal of the appendix with
the umbilical port.
LAPAROSCOPIC APPENDECTOMY
ADVANTAGES
• OPEN APPENDECTOMY
o Shorter operating time
o Lower operating room costs
o Fewer intraabdominal abscess
o Lower hospital costs
• LAPAROSCOPIC APPENDECTOMY
o Diagnosis of other conditions
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 5|8
Surgery Rotation CLERKSHIP
o Decreased pain and lower narcotic C. Stump Appendicitis
requirement • Stump appendicitis is defined by the recurrent
o Reduced length of stay inflammation of the residual appendix after
o Fewer wound infections the appendix has been only partially removed during
o Quicker return to usual activities an appendectomy for appendicitis
• Patients typically present with recurrent symptoms
INCIDENTAL APPENDECTOMY of appendicitis approximately 9 years after their
• Neither clinically nor economically appropriate initial surgery.
• Special patient groups in whom this can be done: • Prevention is done by using the “appendiceal critical
- Children about to undergo chemotherapy view of safety”
- Disabled who cannot describe symptoms or react • The remaining stump should be no longer than 0.5
normally to abdominal pain cm
- Patients with Chron’s disease
- Individuals who are about to travel to remote Additional notes:
places where there is no access to medical or • The key to avoiding Stump appendicitis is
surgical care “Prevention.So the appendix placed at 10 o’clock,
Additional notes: taenia coli/libera at 3 o’clock, and terminal ileum at
• In patients ten to 30 years of age--the age group 6 o’clock and identification of where the taeniae coli
associated with a higher incidence of acute merge and disappear is paramount to identifying
appendicitis--who are otherwise healthy, incidental and ligating the base of the appendix during the
appendectomy is effective in preventing morbidity initial operation.
and death associated with acute appendicitis • The remaining stump should be no longer than 0.5
• In patients 30 to 50 years of age, incidental cm, as stump appendicitis has only been noted in
appendectomy should be left to the discretion of the stumps ≥0.5 cm in the literature.
surgeon
• In mentally handicapped patients less than 50 years SPECIAL CIRCUMSTANCES
of age and who are physically healthy, incidental A. APPENDICITIS IN CHILDREN
appendectomy should be performed • Infants and young children - most likely to
present perforated disease
POST-OP CARE AND COMPLICATIONS • PE findings with highest sensitivity rate in
A. Surgical Site Infection: children with appendicitis:
• Most common site of surgical site infection - Maximal tenderness in the right lower
following Lap Appendectomy :Extraction Port quadrant
Site - The inability to walk or walking with a limp
• In patients with incisional surgical site infection: - Pain with percussion, coughing, and
treatment should be opening of the incision and hopping
obtaining a culture. • Management: Laparoscopic Appendectomy
B. Intra-abdominal abscesses Additional notes:
• Small abscesses can be simply treated with • The inability of young children to give an
antibiotics accurate history, diagnostic delays by both
• Larger abscesses require drainage. parents and physicians, and the frequency of
gastrointestinal distress in children are all
Additional notes: contributing factors to the misdiagnosis and
• Patients with postoperative intra-abdominal delay in diagnosis.
abscesses can present in a variety of ways. Although • The more rapid progression to rupture and the
fever, leukocytosis, and abdominal pain are common inability of the underdeveloped greater
presentations, patients with ileus, bowel omentum to contain a rupture lead to
obstruction, diarrhea, and tenesmus may also harbor significant morbidity rates in children.
intra-abdominal abscesses
• Most commonly, percutaneous drainage with CT or
ultrasound guidance is effective. For abscesses not
amenable to percutaneous drainage, laparoscopic
abscess drainage is a viable option.
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 6|8
Surgery Rotation CLERKSHIP
B. APPENDICITIS IN THE ELDERLY Additional notes:
• The perforation rate appears to increase with • The majority of carcinoids are located in the tip of
age greater than 80 years. the appendix. Malignant potential is related to size,
• Higher risk for complications because of their with tumors <1 cm rarely resulting in extension
premorbid conditions outside of the appendix or adjacent to the mass
• Laparoscopic appendectomy is safe and might • Symptoms attributable directly to the carcinoid are
allow patients to reduce pain and their hospital rare, although the tumor can occasionally obstruct
stay the appendiceal lumen much like a fecalith and
result in acute appendicitis
Additional notes:
• The perforation rate appears to increase with B. ADENOCARCINOMA
age greater than 80 years. • Three major histologic subtypes:
• Higher risk for complications because of their -mucinous adenocarcinoma
premorbid conditions -colonic adenocarcinoma
• Laparoscopic appendectomy is safe and might -adenocarcinoid
allow patients to reduce pain and their hospital • Most common mode of presentation: that of acute
stay appendicitis
• Recommended treatment: right hemicolectomy
C. APPENDICITIS IN PREGNANT WOMEN Additional notes:
• Can occur at any time during pregnancy but is • Primary adenocarcinoma of the appendix is a rare
rare in the third trimester. neoplasm with three major histologic subtypes:
• The most consistent sign encountered in acute mucinous adenocarcinoma, colonic adenocarcinoma,
appendicitis during pregnancy is pain in the right and adenocarcinoid
side of the abdomen. • The most common mode of presentation for
• When the diagnosis is in doubt, abdominal appendiceal carcinoma is that of acute appendicitis.
ultrasound may be beneficial. Patients also may present with ascites or a palpable
• Management: Laparoscopic appendectomy mass, or the neoplasm may be discovered during an
operative procedure for an unrelated cause
Additional notes: • Overall 5-year survival is 55% and varies with stage
• Appendectomy for presumed appendicitis is the and grade.
most common surgical emergency during
pregnancy. C. MUCOCELE
• Another option is magnetic resonance imaging, • May be caused by one of four processes: Surgery
which has no known deleterious effects on the -Retention cysts
fetus. The American College of Radiology -Mucosal hyperplasia
recommends the use of nonionizing radiation -Cystadenomas
techniques for front-line imaging in -Cystadenocarcinomas.
• Laparoscopic appendectomies can be safely • Surgery:
performed in pregnant patients but with -Resection of the appendix, wide resection of the
increase pregnancy-related complications. mesoappendix
- Right hemicolectomy is reserved for patients with a
NEOPLASMS OF THE APPENDIX positive margin at the base of the appendix or
A. Carcinoid positive periappendiceal lymph nodes.
• Characteristics:firm, yellow, bulbar mass
• Appendix: Most common site of GI carcinoid Additional notes:
• Location of the majority of carcinoids:in the tip • A mucocele of the appendix is an obstructive
of the appendix dilatation by intraluminal accumulation of mucoid
• The mean tumor size for carcinoids is 2.5 cm. material. The clinical presentation of a mucocele is
nonspecific, is often an incidental finding at
operation for acute appendicitis.
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 7|8
Surgery Rotation CLERKSHIP
• An intact mucocele presents no future risk for the
patient; however, the opposite is true if the
mucocele has ruptured and epithelial cells have
escaped into the peritoneal cavity. As a result, when
a mucocele is visualized at the time of laparoscopic
examination, conversion to open laparotomy is
recommended.
• Resection of the appendix, wide resection of the
mesoappendix to include all the appendiceal lymph
nodes, collection and cytologic examination of all
intraperitoneal mucus, and careful inspection of the
base of the appendix.
CONGRATULATIONS ON FINISHING SURGERY CLERKSHIP!
HELLO PCM!
-ijdg-
BATCH 2021-DSV | ILOILO DOCTORS’ COLLEGE OF MEDICINE Page 8|8
You might also like
- CPM7th TB in Infancy and ChildhoodDocument41 pagesCPM7th TB in Infancy and ChildhoodJackyNo ratings yet
- Pre-Op Case Protocol #4Document2 pagesPre-Op Case Protocol #4IC BNo ratings yet
- Senses Lab Activities For Online LabDocument5 pagesSenses Lab Activities For Online Labhzlatan100% (1)
- Laura Otis Mullers Lab 2007Document337 pagesLaura Otis Mullers Lab 2007guilhermefsantosNo ratings yet
- Major Basic Set (Operating Room Instruments)Document5 pagesMajor Basic Set (Operating Room Instruments)Ralph Jetzon MorillaNo ratings yet
- Abdominal TraumaDocument47 pagesAbdominal TraumaWidya Rahayu100% (1)
- Clerks REVALIDA Review 2017Document51 pagesClerks REVALIDA Review 2017Mara Medina - BorleoNo ratings yet
- Osce Cranial Nerves PDFDocument42 pagesOsce Cranial Nerves PDFriczen vilaNo ratings yet
- Head and Neck SchwartzDocument10 pagesHead and Neck Schwartz2013SecBNo ratings yet
- Digging Up The Bones - MicrobiologyDocument31 pagesDigging Up The Bones - MicrobiologyMossa Di Base100% (1)
- HumanEye PDFDocument16 pagesHumanEye PDFsneha Mary AntonyNo ratings yet
- Practice Midterm ReviewDocument14 pagesPractice Midterm Reviewasjiodjw100% (2)
- 0.6 Surgery Trans PDFDocument17 pages0.6 Surgery Trans PDFJoy ManzanoNo ratings yet
- Case 1 History & PEDocument3 pagesCase 1 History & PEcbac1990No ratings yet
- OB TransDocument10 pagesOB TransJoan Caacbay De GuzmanNo ratings yet
- Upper Gastrointestinal Bleeding (Ugib) : First Shift: August 13, 2018Document10 pagesUpper Gastrointestinal Bleeding (Ugib) : First Shift: August 13, 2018Angelo Dela Cruz VillaromanNo ratings yet
- OB - TransesDocument112 pagesOB - TransesAldwin BagtasNo ratings yet
- TOPNOTCH Diagnostic Exam ANSWER KEY September 2018Document20 pagesTOPNOTCH Diagnostic Exam ANSWER KEY September 2018CDNo ratings yet
- TRP Surgery Study GuideDocument27 pagesTRP Surgery Study GuidekatNo ratings yet
- Emed - OB Part 1Document6 pagesEmed - OB Part 1Princess Cate MercadoNo ratings yet
- Thalassemia TableDocument2 pagesThalassemia TableMeevie ToledoNo ratings yet
- Pharmacology Table - GonzalesDocument14 pagesPharmacology Table - GonzalesMark Angelo PonferradoNo ratings yet
- Management of Acute Appendicitis in Adults - UpToDateDocument28 pagesManagement of Acute Appendicitis in Adults - UpToDateaulia rachman100% (1)
- Anesth BarashDocument6 pagesAnesth BarashIAN GABRIELLE MERCADO CUYNONo ratings yet
- Pedia SummaryDocument10 pagesPedia SummaryBea GozaNo ratings yet
- Intussusception TransDocument4 pagesIntussusception TransJames Maravillas100% (1)
- Clinpath - : Red Blood CellsDocument14 pagesClinpath - : Red Blood CellsYolanda Primrosa NurhanNo ratings yet
- Surgery Trans 2a - Fluid and Electrolyte Management of The Surgical PatientDocument14 pagesSurgery Trans 2a - Fluid and Electrolyte Management of The Surgical PatientJoan Caacbay De GuzmanNo ratings yet
- January 11 January 25 February 6 February 22: Date SubjectsDocument3 pagesJanuary 11 January 25 February 6 February 22: Date SubjectsShams JailaniNo ratings yet
- Esophageal Achalasia DysphagiaDocument14 pagesEsophageal Achalasia DysphagiaTirtha Taposh100% (1)
- TRIVIA: Dr. Tan Is The Father/Pioneer of Laparoscopic Surgery in The PhilippinesDocument48 pagesTRIVIA: Dr. Tan Is The Father/Pioneer of Laparoscopic Surgery in The PhilippinesJüdith Marie Reyes BauntoNo ratings yet
- Pediatric ProblemsDocument4 pagesPediatric ProblemsRencel Hope Bañez100% (1)
- A Disease Study On: AppendectomyDocument8 pagesA Disease Study On: Appendectomybryan leguiabNo ratings yet
- Git PathologyDocument113 pagesGit PathologyanggitaNo ratings yet
- Physio Ob ReviewDocument368 pagesPhysio Ob ReviewMark LopezNo ratings yet
- Maternal PhysiologyDocument73 pagesMaternal PhysiologyAbegail IbañezNo ratings yet
- High Yield OSCE - SurgeryDocument2 pagesHigh Yield OSCE - SurgerymashupNo ratings yet
- Nasal Cavity and Paranasal Sinuses AnatomyDocument19 pagesNasal Cavity and Paranasal Sinuses AnatomyLicensed to HealNo ratings yet
- History Cs Admitting Notes: + 10 "U" Oxytocin X 8 HDocument7 pagesHistory Cs Admitting Notes: + 10 "U" Oxytocin X 8 HKarl Martin PinedaNo ratings yet
- Republic of The Philippines Professional Regulation Commission ManilaDocument3 pagesRepublic of The Philippines Professional Regulation Commission ManilaTheSummitExpressNo ratings yet
- 07.02 Topnotch Pharmacology TableDocument64 pages07.02 Topnotch Pharmacology TableskzskzNo ratings yet
- Biochemistry: OBSTETRICS 1: The Menstrual Cycle: DNA Replication and RepairDocument3 pagesBiochemistry: OBSTETRICS 1: The Menstrual Cycle: DNA Replication and RepairPatricia Anne ReyesNo ratings yet
- Surgery Revalida Review PDFDocument11 pagesSurgery Revalida Review PDFMara Medina - BorleoNo ratings yet
- University of Perpetual Help Rizal Jonelta Foundation School of Medicine Department of Surgery - ConsortiumDocument17 pagesUniversity of Perpetual Help Rizal Jonelta Foundation School of Medicine Department of Surgery - Consortiummefav7778520No ratings yet
- Anatomy Supertable PDFDocument14 pagesAnatomy Supertable PDFAlex Ondevilla100% (1)
- Abdominal Trauma Signs, Symptoms and Nursing CareDocument24 pagesAbdominal Trauma Signs, Symptoms and Nursing CareSurgeryClassesNo ratings yet
- Legal Medicine and Medical Jurisprudence Comprehensive Exam ReviewerDocument17 pagesLegal Medicine and Medical Jurisprudence Comprehensive Exam ReviewerYeshua Tura100% (1)
- The "Most Common" . According To NelsonDocument31 pagesThe "Most Common" . According To NelsonKenneth NuñezNo ratings yet
- Gynecology: Recurrent Pregnancy LossDocument6 pagesGynecology: Recurrent Pregnancy LossDawn Marco100% (1)
- Approach To Breast..maha - PPTX 2Document38 pagesApproach To Breast..maha - PPTX 2Meno Ali50% (2)
- Urinary Tract InfectionDocument9 pagesUrinary Tract InfectionTom Mallinson100% (1)
- Oral Revalida Review2019: Concise Guide to Ophthalmology ExamDocument10 pagesOral Revalida Review2019: Concise Guide to Ophthalmology ExamanonymousNo ratings yet
- New Intern Guide Quick NotesDocument8 pagesNew Intern Guide Quick NotesTrisNo ratings yet
- Multifetal Gestation: Department of Obstetrics and Gynecology FEU - NRMF Institute of MedicineDocument40 pagesMultifetal Gestation: Department of Obstetrics and Gynecology FEU - NRMF Institute of Medicinereamer27100% (1)
- Esphagus Stomach Duodenum Gross AnatomyDocument9 pagesEsphagus Stomach Duodenum Gross AnatomyWinchester LoapedNo ratings yet
- Approach To Acute Lower Gastrointestinal Bleeding in Adults - UpToDateDocument21 pagesApproach To Acute Lower Gastrointestinal Bleeding in Adults - UpToDateChrista OvalleNo ratings yet
- Surgery Trans CheckedDocument5 pagesSurgery Trans CheckedHaloula MINo ratings yet
- Abdominal Wall SurgeryDocument8 pagesAbdominal Wall SurgeryRae Marie AquinoNo ratings yet
- Junior Intern Review - Oral Revalida 2016Document170 pagesJunior Intern Review - Oral Revalida 2016Cyrus ZalameaNo ratings yet
- Scaffold Assessment of The AbdomenDocument13 pagesScaffold Assessment of The AbdomenDaniella Tupas100% (1)
- CD PD 2.1 NECK 2017 Bates Outline PDFDocument3 pagesCD PD 2.1 NECK 2017 Bates Outline PDFGiaFelicianoNo ratings yet
- Benign Gynecologic LesionsDocument103 pagesBenign Gynecologic Lesions201286% (7)
- Problem-based Approach to Gastroenterology and HepatologyFrom EverandProblem-based Approach to Gastroenterology and HepatologyJohn N. PlevrisNo ratings yet
- BCA-Human Structural Biology- Abdominal Organs OverviewDocument16 pagesBCA-Human Structural Biology- Abdominal Organs OverviewPatricia Ann ClariñoNo ratings yet
- AUF SOM - Disease of Stomach & Duodenum PDFDocument203 pagesAUF SOM - Disease of Stomach & Duodenum PDFYestin Reece Corpus ArcegaNo ratings yet
- Lecture StomachDocument31 pagesLecture StomachAmaetenNo ratings yet
- Anatomi & Histologi GasterDocument24 pagesAnatomi & Histologi Gastersalvaryn neNo ratings yet
- List of APMCI Affiliated Hospitals by RegionDocument6 pagesList of APMCI Affiliated Hospitals by RegionJoy ManzanoNo ratings yet
- TRAUMA Trans PDFDocument14 pagesTRAUMA Trans PDFJoy ManzanoNo ratings yet
- Pedia 2 CHD Acyanotic PDFDocument9 pagesPedia 2 CHD Acyanotic PDFJoy ManzanoNo ratings yet
- The BreastDocument10 pagesThe BreastJoy ManzanoNo ratings yet
- Breast Cancer Didactics - ManzanoDocument49 pagesBreast Cancer Didactics - ManzanoJoy ManzanoNo ratings yet
- BATCH 2021: Healing by Primary IntentionDocument20 pagesBATCH 2021: Healing by Primary IntentionJoy ManzanoNo ratings yet
- Breast Cancer Risk Factors, Diagnosis and ManagementDocument49 pagesBreast Cancer Risk Factors, Diagnosis and ManagementJoy ManzanoNo ratings yet
- Surgery Notes2 W BreastDocument6 pagesSurgery Notes2 W BreastJoy ManzanoNo ratings yet
- National Tuberculosis Control Program Manual of Procedures 5th EditionDocument192 pagesNational Tuberculosis Control Program Manual of Procedures 5th EditionBlue Pielago100% (9)
- Pocket Book of Hospital Care For ChildrenDocument438 pagesPocket Book of Hospital Care For ChildrenTawangNo ratings yet
- Complications: Virus Produces Antigen That Destroys PancreasDocument1 pageComplications: Virus Produces Antigen That Destroys PancreasJoy ManzanoNo ratings yet
- Pedia Didactics Dengue - 2Document75 pagesPedia Didactics Dengue - 2Joy ManzanoNo ratings yet
- Module 5 ExamDocument3 pagesModule 5 ExamGlenn ClementeNo ratings yet
- Bioenergetics and Lipid MetabolismDocument34 pagesBioenergetics and Lipid MetabolismM Daffa Abhista ReviansyahNo ratings yet
- Results of Analysis - Kae Kru ArtDocument3 pagesResults of Analysis - Kae Kru ArtDr. Siraphop OneSongchai RatanasubanNo ratings yet
- Mutationbreedingppt 161203184149Document41 pagesMutationbreedingppt 161203184149MuneebNo ratings yet
- WBCs Chap 2Document119 pagesWBCs Chap 2Hoor ul Ain RamzanNo ratings yet
- Fisiologi Sistem Pencernaan: Kristanti, DRDocument64 pagesFisiologi Sistem Pencernaan: Kristanti, DRFeny Maharani100% (1)
- Biology: Concepts and Connections, 6e (Campbell) : Test Bank (1) PartDocument21 pagesBiology: Concepts and Connections, 6e (Campbell) : Test Bank (1) Partluchi_babezNo ratings yet
- Effect of Different Physical and Chemical Treatments On Detoxification of Ricin in Castor CakeDocument10 pagesEffect of Different Physical and Chemical Treatments On Detoxification of Ricin in Castor CakeL D Mendoza UrbinaNo ratings yet
- Medicina Mitocondrial Vol 1Document485 pagesMedicina Mitocondrial Vol 1ArianPedrozaNo ratings yet
- Chapter 2.2. The Cell Cycle Meiosis and MitosisDocument23 pagesChapter 2.2. The Cell Cycle Meiosis and MitosisB. ThuậnNo ratings yet
- 2 Murthy Et Al 2014 Secondary Metabolites Review Murthy2014 PDFDocument16 pages2 Murthy Et Al 2014 Secondary Metabolites Review Murthy2014 PDFmartha glezNo ratings yet
- 12.1 Pediatri - Sirkulasi FetalDocument22 pages12.1 Pediatri - Sirkulasi Fetalwa ode nur salsabilahNo ratings yet
- Colon Large Intestine: ColorectalDocument3 pagesColon Large Intestine: ColorectalAlina AldeaNo ratings yet
- Rationale PDFDocument3 pagesRationale PDFAriNo ratings yet
- Overview of Nerve Conduction Studies - UpToDateDocument41 pagesOverview of Nerve Conduction Studies - UpToDate邱磊中No ratings yet
- SaudiJHealthSci4142-1740933 045009Document9 pagesSaudiJHealthSci4142-1740933 045009Ramona BordeaNo ratings yet
- Neurotrauma Rural Guidelines 2edDocument27 pagesNeurotrauma Rural Guidelines 2edAldion ZericoNo ratings yet
- Voluntary Muscle: Muscle We Can Control It: The Muscular SystemDocument4 pagesVoluntary Muscle: Muscle We Can Control It: The Muscular SystemAbrar HussamNo ratings yet
- Pathfast PresepsinDocument6 pagesPathfast PresepsinWulan Ervinna SimanjuntakNo ratings yet
- What Makes It Beautiful VitaDocument8 pagesWhat Makes It Beautiful VitaVladimir DrăgoiNo ratings yet
- Silkworm moth: from egg to emergenceDocument78 pagesSilkworm moth: from egg to emergenceSoubhik MondalNo ratings yet
- Efeito Anti-Hipertensivo Do Exercicio The Anti-HypDocument9 pagesEfeito Anti-Hipertensivo Do Exercicio The Anti-HypRicardo Tavares ArrudaNo ratings yet
- Super Coils and Linking NumberDocument5 pagesSuper Coils and Linking NumberShaher Bano MirzaNo ratings yet
- Bio Topic 1.4 WorksheetDocument4 pagesBio Topic 1.4 WorksheetMahina WongNo ratings yet