Professional Documents
Culture Documents
Enlargement of The Thyroid Gland: Embryology & Anatomy Surgical Anatomy
Uploaded by
Kiara GovenderOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Enlargement of The Thyroid Gland: Embryology & Anatomy Surgical Anatomy
Uploaded by
Kiara GovenderCopyright:
Available Formats
Enlargement of the Thyroid Gland
Physiological - puberty / pregnancy
Pathological
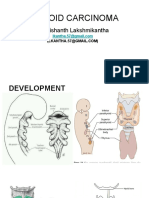
Embryology & Anatomy
Thyroid gland develops from 1st & 2nd pharyngeal pouches Surgical Anatomy
● Derived from epithelial proliferation in the floor of the pharynx
● Migrates downwards in front of forgegut to lie anterior to trachea - during movement – remains Gland → invested by thick fibrous sheath (pretracheal fascia)
attached to floor of mouth by thyroglossal duct – which ultimately disappears Sends septa into gland and binds it to larynx therefore → normal gland =
If the thyroglossal duct persists – results in: Thyroglossal sinus or Thyroglossal cyst moves on swallowing
Hormone synthesis begins @ 10-12 wks gestation ● Rich blood supply → superior & inferior thyroid arteries
Maternal hormones thus NB in 1st half of pregnancy ↑’d BF in hyperthyroidism therefore → surgery = difficult
● When thyroid gland reaches position it occupies in adult, just below the cricoid cartilage → divides ● Lymphatic drainage → via mid & lower deep jugular, pretracheal & mediastinal
into 2 lobes LN’s
● Isthmus → thin midline band of tissue – lies horizontally below the cricoid cartilage ● Gland → laterally traversed by recurrent laryngeal nerve (RLN)
● Normal thyroid weighs 15-25g & is attached to trachea by loose CT Injury → paralysis of vocal cords
● Close relationship to Parathyroid glands – thus during surgery may remove them
accidentally = hypoparathyroidism
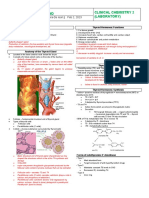
Histo Physiology
Follicles (acini) Thyroid Gland produces 2 hormones
→ roughly spherical – diameter = 3mm THYROXINE – regulates metabolic rate
IODINE TRAPPING → Iodine reduced to iodide in GIT→ absorbed from small bowel → actively trapped by follicular cells
Lined with epithelial cells → ORGANIFICATION → Iodide → oxidized and bound to tyrosine in thyroglobulin → forms mono-iodotyrosine (MIT) & di-iodotyrosine (DIT) via
secrete thyroid hormones → action of Thryoid Peroxidase
stored in colloid of follicle COUPLING → MIT & DIT - cleaved then coupled to form tri-iodotyrosine (T3) & thyroxine (T4) via action of Thryoid Peroxidase → stored in
Epithelial cells → cuboidal follicles
cells – but become columnar TRH released from hypothalamus – causes release of TSH from anterior pituitary → TSH binds to receptors on thyroid gland → ↑ adenylyl
in response to TSH cyclase (AC) activity - ↑ cAMP (phosphoinositide pathway also stimulated – may stimulate thyroid growth)
In response to TSH → thyroglobulin hydrolysed → T3 & T4 secreted into plasma - bind to thyroxine-binding globulin (TBG) and albumin
C-cells = btwn follicles (also T4 de-iodinated peripherally – form T3 (common site of conversion = liver)
Parafollicular cells) – make and Negative feedback – TSH & TRH ↓
secrete Calcitonin CALCITONIN – calcium homeostasis
↓ calcium concentration in serum – via inhibition of osteoclast – therefore ↓ calcium absorption by bone & ↑ renal excretion of calcium
Approach to the Thyroid
Embryology & Anatomy
A. Dysfunction Hyperthyroidism
Hypothyroidism
B. Organic Mass growing in the neck
No dysfunction
- multinodular goiter
- solitary nodule
C. Combination Growth + dysfunction
- Hashimoto’s
- Toxic multinodular goiter
- Solitary nodule
- Grave’s
1st Important Question for any growth: Is it malignant or benign?
tissue.
similarly to normal thyroid
tumours - behave very
Well-differentiated
Behaviour:
Then: Take a History Most commonly slow growth - Rapid growth seen only in Anaplastic & Medullary carcinoma
Behaviour of the growth Usually no weight loss
Risk factors Spread: Tracheal invasion
- Personal (the patient) Radiation exposure to the head/neck Bone pain
Extremes of ages (very young/old) Headaches
Female sex (3:1) Odynophagia
Poorer prognosis (males) Dysphonia (hoarseness)
Hx of previous thyroid cancer
- Family (history) MEN II Examination of the growth (thyroid):
+ Family Hx for Ca other than MEN Lesion fixed to surrounding tissues (hardly ever to the skin)
Lymphadenopathy - unilateral
- isolated cervical
Then: Clinical Examination
- immobile
Signs of malignancy in any growth - firm
Hoarseness (dysphonia)
Diagnosis of a thyroid growth in the neck:
1. Hx & Clinical Diffuse / Multinodular / Solitary
2. TSH blood test
3. Ultrasound
4. CT scan
5. Ionised iodine
Investigating the Thyroid
Patient presents with suspicious Clinical & Blood = Hyperthyroidism Ultrasound NORMAL On U/S:
clinical history of thyroid a thyroid Diffuse goitre OR Non-palpable - no toxic adenoma - Solidary nodule
problem. … - Multinodular nodule
Grave’s Disease Distinguishing between Grave’s and - Diffuse goitre
(overstimulated cells) Hashimoto’s
Step 1 Hashimoto’s Thyroididits Must check cellular architecture
(gland destroyed, thyroid
hormone release)
Benign vs.
Toxic Adenoma
Malignant
TSH Ultrasound Auto-Antibodies FNA
TSH Hyperthyroidism Must do ultrasounds Graves: Done under guidance
High T3 T4 Confirm clinical findings TSH antibodies 80% sensitive for malignancy
Radioisotope Scan
TSH Hypothyroidism Rule out small nodules (Toxic Hashimoto’s: Repeated 2x if negative
Low T3 T4 Adenoma) Anti-microsomal antibodies
Anti-thyroglobulin antibodies Can’t report X Follicular
TSH Sub-Clin hyperthyroidism Can report Papillary Serves to map out dysfunction
U/S is the most sensitive test for
Normal T3 T4 98% Sensitivity Medullary through the entire gland - visual
nodules!
TSH Sub-Clin hypothyroidism Anaplastic pattern of functionality.
Normal T3 T4
Info Gathered from U/S: Other distinguishing test: Hot - active
TSH:T4 ratio >20 = Graves Usually normal gland
- cystic vs. solitary nodule
Done in pts not on hormone - features of malignancy ESR = Hashimoto’s Cold - decreased uptake
replacement therapy, with no other - find non-palpable nodules Hypoactive (e.g. Hashi)
influencing drugs. - confirm solitary nodule Patchy
98% Sensitivity - solitary vs. multi-nodular Toxic multinodular goitre
- size of lesion (of either type) Hashimoto’s
- find scary lymphadenopathy Isolated uptake (Focal Hot)
Toxic adenoma
Diffuse dysfunction
Grave’s
Treating Thyroid Problems
Grave’s Disease Hashimoto’s Thyroiditis Toxic Adenoma Cancer
Or PLUMMER’S DISEASE Follicular Ca
- toxic multinodular goitre Self-limiting disease U/S showed solitary nodule Won’t see on FNA report
Usually reaches euthyroid state Toxic patient Can’t distinguish Follicular Ca /
Make the patient euthyroid
Protect target organs
B-Blockers Do Isotope scan (see focal hot
Adenoma
Do complete lobectomy
Best
Anti-thyroid drugs
Protect target organs
Rx hypothyroid state
Altroxin
spots)
Areas of good uptake - do
Follicular adenoma = leave
alone
Success
B-Blockers lobectomy & isthmectomy
Radioactive Ablation Beta-Blockers Totally suppressed gland - do Medullary
Once patient is euthyroid - Prevent’s T4 - T3 conversion radical thyroidectomy Total neck dissection
Follow up - After 4 months - - Protects the heart Investigate for MEN
should indicate success of
ablation (past peak, enter Papillary Ca
euthyroid or hypothyroid Total thyroidectomy
phase)
Anaplastic
Ablation:
Can Dx on FNA
95% cure rate with 1st dose
Very often presents in
should reach euthyroid state 12 advanced stage
weeks post-ablation
For METS: surgery for primary
first
CI X for Ablation:
- pregnancy Ablation can follow surgery
- iodine allergy (better uptake by metastatic
- failed medical Rx cells)
- pressure symptoms
(need surgery) NB: Follicular / Papillry - TSH
dependent. Needs post-op ablation
& TSH suppression for 2 yrs .
You might also like
- Thyroid ExamDocument4 pagesThyroid Examquojo041No ratings yet
- Thyroid Examination FiryaLDocument3 pagesThyroid Examination FiryaLFiryal Balushi100% (1)
- Thyroid DisordersDocument14 pagesThyroid DisordershaleyNo ratings yet
- Endocrinology Lectures 1 3 DR - LigonDocument14 pagesEndocrinology Lectures 1 3 DR - LigonJealine Marie BernabeNo ratings yet
- Midline Neck SwellingDocument62 pagesMidline Neck Swellingranjit.mohapatra1968No ratings yet
- Differential Diagnosis of Neck Swellings PDFDocument3 pagesDifferential Diagnosis of Neck Swellings PDFSiddharth KatyalNo ratings yet
- Week 1.3Document23 pagesWeek 1.3ginny.mycookiecanNo ratings yet
- Thyroid PathologyDocument9 pagesThyroid PathologyNada MuchNo ratings yet
- LEC 1-3Document21 pagesLEC 1-3Kramm AnulNo ratings yet
- ENT Approach To Thyroid MassesDocument2 pagesENT Approach To Thyroid MassesVanessa HermioneNo ratings yet
- Thyroid DiseaseDocument65 pagesThyroid DiseaseIan FordeNo ratings yet
- Thyroid Carcinoma - DR - NishanthDocument88 pagesThyroid Carcinoma - DR - Nishanth57- Kalanidhi mNo ratings yet
- Endocrine NursingDocument5 pagesEndocrine NursingMiss GNo ratings yet
- ONCOLOGYDocument29 pagesONCOLOGYmendozaayajulienneNo ratings yet
- Thyroid DisordersDocument61 pagesThyroid DisordersdrmamodoNo ratings yet
- Genus Clostridium-C.tetaniDocument11 pagesGenus Clostridium-C.tetaniStefy BarranoNo ratings yet
- Hypothyroidism: By: Judhaimah Mardhiah BT Mat Tari 0810544Document23 pagesHypothyroidism: By: Judhaimah Mardhiah BT Mat Tari 0810544Jujue MardhiahNo ratings yet
- Physical Examination Thyroid & Neck 2023-2024Document1 pagePhysical Examination Thyroid & Neck 2023-202482cxp4n46wNo ratings yet
- Thyroid Disorders (Final Draft)Document17 pagesThyroid Disorders (Final Draft)mogesie1995No ratings yet
- Endocrine - BoardsDocument9 pagesEndocrine - BoardsSoojung Nam100% (4)
- Thyroid Disorders 1Document29 pagesThyroid Disorders 1zxcvbzaki123No ratings yet
- ThyroidDocument20 pagesThyroidheartaoneNo ratings yet
- HypothyroidismDocument49 pagesHypothyroidismBahaa ShaabanNo ratings yet
- Thyroid/Parathyroid Glands: Dec 2013 DR Dechen NidupDocument16 pagesThyroid/Parathyroid Glands: Dec 2013 DR Dechen NidupPhuntsho OngmoNo ratings yet
- h1 Reproductive Physiology Course Summary NotesDocument11 pagesh1 Reproductive Physiology Course Summary NotesHoney BaseriNo ratings yet
- Neck Masses: Thyroid DiseaseDocument49 pagesNeck Masses: Thyroid DiseaseRashed ShatnawiNo ratings yet
- 9.the Thyroid Gland-1Document18 pages9.the Thyroid Gland-1abdullahi bashiirNo ratings yet
- Thyroid GlandDocument22 pagesThyroid Glandrazan asadNo ratings yet
- Anatomy, Physiology and Pathology of The Thyroid Gland: DR Suchitra Iyrpg Department of Prosthodontics SRMCDocument46 pagesAnatomy, Physiology and Pathology of The Thyroid Gland: DR Suchitra Iyrpg Department of Prosthodontics SRMCdrsuchitramohanNo ratings yet
- 008 164 Anatomy of Thyroid Gland PDFDocument10 pages008 164 Anatomy of Thyroid Gland PDFWILLIAMNo ratings yet
- Neck MassDocument40 pagesNeck Massdryojanasharma57100% (1)
- NNYGDocument13 pagesNNYGrose ONo ratings yet
- Thyroid ReportDocument105 pagesThyroid ReportAARVNo ratings yet
- Report Thyroid Doc Chan SurgDocument70 pagesReport Thyroid Doc Chan SurgShari TernolaNo ratings yet
- MS 1Document5 pagesMS 1kingpinNo ratings yet
- An Approach To Thyroid EnlargementDocument3 pagesAn Approach To Thyroid EnlargementHardik JeenaNo ratings yet
- AIRP NotesDocument5 pagesAIRP NotesSamuel AzezeNo ratings yet
- Approach To STNDocument56 pagesApproach To STNAbhishek VaidyaNo ratings yet
- Thanatophoric Dysplasia: A Case Report: Uruj Jahan, Astha Sharma, Neena Gupta, Shruti Gupta, Fatima UsmaniDocument4 pagesThanatophoric Dysplasia: A Case Report: Uruj Jahan, Astha Sharma, Neena Gupta, Shruti Gupta, Fatima UsmaniPrima Hari PratamaNo ratings yet
- Guidelines For NHS Shortlist and InterviewDocument22 pagesGuidelines For NHS Shortlist and InterviewabduljajiNo ratings yet
- Tutorial On Goiter GadedDocument117 pagesTutorial On Goiter GadedhindabdalgadirNo ratings yet
- Developmental Dysplasia of The HipDocument33 pagesDevelopmental Dysplasia of The HipQasem Rababah100% (1)
- Patologia Chir GL TiroidaDocument72 pagesPatologia Chir GL TiroidaIoachim Friedmann100% (1)
- Thyroid Gland Clinical Chemistry 2 (Laboratory) : LessonDocument4 pagesThyroid Gland Clinical Chemistry 2 (Laboratory) : LessonCherry Ann ColechaNo ratings yet
- Thyroid Status ExaminationDocument10 pagesThyroid Status ExaminationamilaNo ratings yet
- 2 Endocrine ThyroidDocument4 pages2 Endocrine ThyroidJillKellyNo ratings yet
- Development of Thyroid GlandDocument37 pagesDevelopment of Thyroid GlandnrahmaNo ratings yet
- Surgery Revalida Review PDFDocument11 pagesSurgery Revalida Review PDFMara Medina - BorleoNo ratings yet
- Thyroid PathophysiologyDocument7 pagesThyroid PathophysiologyS RiarNo ratings yet
- First Aid For The Surgery Thyroid AnatomyDocument4 pagesFirst Aid For The Surgery Thyroid Anatomyeiuj497No ratings yet
- TIRMODDocument66 pagesTIRMODYaniNo ratings yet
- Cancer of The ThyroidDocument1 pageCancer of The ThyroidCamille Joy BaliliNo ratings yet
- Pathology of Thyroid GlandDocument13 pagesPathology of Thyroid GlandChokri MAKTOUFNo ratings yet
- Breast ExamDocument4 pagesBreast ExamLuke MatupiNo ratings yet
- Thyroid and Parathyroid GlandsDocument5 pagesThyroid and Parathyroid GlandsChristopher PhilipsNo ratings yet
- The Thyroid HyperthyroidismDocument6 pagesThe Thyroid HyperthyroidismhamidseidnaNo ratings yet
- 382 Thyroid Gland Physiology and TestingDocument7 pages382 Thyroid Gland Physiology and TestingJetmoon BlackNo ratings yet
- Obstetrics - Neoplastic Disease of The Ovary (Epithelial) 2014 FinalDocument3 pagesObstetrics - Neoplastic Disease of The Ovary (Epithelial) 2014 FinalJonathanNo ratings yet
- PEDIA Thyroid Gland DisordersDocument6 pagesPEDIA Thyroid Gland DisordersEmerson QuimbaNo ratings yet
- CholangiocaDocument21 pagesCholangiocaKiara GovenderNo ratings yet
- Gastric Carcinoma: Morphologic Classifications and Molecular ChangesDocument48 pagesGastric Carcinoma: Morphologic Classifications and Molecular ChangesKiara GovenderNo ratings yet
- TG13 Updated Tokyo Guidelines For The Management of AcuteDocument7 pagesTG13 Updated Tokyo Guidelines For The Management of AcutechizonaNo ratings yet
- Abdominal SymptomsDocument21 pagesAbdominal SymptomsKiara GovenderNo ratings yet
- 2013 09 30 Tokyo Guideline 2013Document72 pages2013 09 30 Tokyo Guideline 2013Zieky YoansyahNo ratings yet
- Adenocarcinoma of The Esophagogastric JunctionDocument9 pagesAdenocarcinoma of The Esophagogastric JunctionKiara GovenderNo ratings yet
- 2013 09 30 Tokyo Guideline 2013Document72 pages2013 09 30 Tokyo Guideline 2013Zieky YoansyahNo ratings yet
- Adenocarcinoma of The Gastroesophageal JunctionDocument8 pagesAdenocarcinoma of The Gastroesophageal JunctionKiara GovenderNo ratings yet
- Acute Limb Ischemia Vs Critical Limb Ischemia: Clinical PracticeDocument54 pagesAcute Limb Ischemia Vs Critical Limb Ischemia: Clinical PracticeKiara GovenderNo ratings yet
- Bowel ObstructionDocument1 pageBowel ObstructionKiara GovenderNo ratings yet
- Colon, Rectum and AnusDocument30 pagesColon, Rectum and AnusKiara GovenderNo ratings yet
- MSK Exam and Blue BoxesDocument5 pagesMSK Exam and Blue BoxesKiara GovenderNo ratings yet
- SurgeryDocument160 pagesSurgerymudasir61100% (2)
- Internal Medicine NotesDocument54 pagesInternal Medicine NotesKiara Govender100% (1)
- The Nervous SystemDocument24 pagesThe Nervous SystemKiara GovenderNo ratings yet
- Respiratory Examination 2Document4 pagesRespiratory Examination 2Kiara GovenderNo ratings yet
- Rheumatology: HistoryDocument6 pagesRheumatology: HistoryKiara GovenderNo ratings yet
- How To Examine A Vascular PatientDocument33 pagesHow To Examine A Vascular PatientKiara GovenderNo ratings yet
- MSK Exam and Blue BoxesDocument5 pagesMSK Exam and Blue BoxesKiara GovenderNo ratings yet
- Respiratory System SummaryDocument6 pagesRespiratory System SummaryKiara GovenderNo ratings yet
- Wound Care: Wound Assessment: Management of Wounds: AimDocument1 pageWound Care: Wound Assessment: Management of Wounds: AimKiara GovenderNo ratings yet
- Distal To Ligament of Treitz: CausesDocument8 pagesDistal To Ligament of Treitz: CausesKiara GovenderNo ratings yet
- Neck Anatomy: Lymph NodesDocument5 pagesNeck Anatomy: Lymph NodesKiara GovenderNo ratings yet
- Vascular Dise Ase: Arterial AnatomyDocument6 pagesVascular Dise Ase: Arterial AnatomyKiara GovenderNo ratings yet
- Y Malignant MelanomaDocument3 pagesY Malignant MelanomaKiara GovenderNo ratings yet
- Upper GITDocument13 pagesUpper GITKiara Govender100% (1)
- Skin InfectionsDocument5 pagesSkin InfectionsKiara GovenderNo ratings yet
- Y LipomaDocument1 pageY LipomaKiara GovenderNo ratings yet
- Thyroid DisordersDocument16 pagesThyroid DisordersKiara GovenderNo ratings yet
- Cox TechniqueDocument9 pagesCox TechniquemyokamaltaNo ratings yet
- OsteomyelitisDocument29 pagesOsteomyelitisAishath Samha HussainNo ratings yet
- Listening Book 3Document89 pagesListening Book 3Samia FarooqNo ratings yet
- Kevin Clark NCTMB: Back Pain and MassageDocument4 pagesKevin Clark NCTMB: Back Pain and MassageKevin ClarkNo ratings yet
- The Adornment of The Muslim Doctor (With Good Character)Document49 pagesThe Adornment of The Muslim Doctor (With Good Character)abu salmanNo ratings yet
- Model Poster MedicinaDocument1 pageModel Poster MedicinaGabriela BichirNo ratings yet
- Community MedicineDocument24 pagesCommunity MedicineSrinidhi Nandhini PandianNo ratings yet
- Interview MBBS UIADocument7 pagesInterview MBBS UIANur Diyana Asyiqin MansorNo ratings yet
- Liebes Kind 2014Document11 pagesLiebes Kind 2014marcosNo ratings yet
- Introduction PeDocument25 pagesIntroduction PeRodelJohnMarmolNo ratings yet
- Client InformationDocument2 pagesClient InformationJonathanAllenLMTNo ratings yet
- Academy of Life Underwriting - ALU 101 - Basic Life Insurance Underwriting - Textbook For 2022 Exam Cycle (2021)Document359 pagesAcademy of Life Underwriting - ALU 101 - Basic Life Insurance Underwriting - Textbook For 2022 Exam Cycle (2021)KALPESH SHAHNo ratings yet
- Euthanasia ThesisDocument11 pagesEuthanasia ThesisAyush MathurNo ratings yet
- Our Survival of SoulDocument463 pagesOur Survival of SoulAnonymous Mq8EkiAyhM100% (2)
- Drug StudyDocument6 pagesDrug StudyIrveen Joy RamirezNo ratings yet
- What Is A Hypochondriac?: ENG - B2.0902RDocument25 pagesWhat Is A Hypochondriac?: ENG - B2.0902RAnelNo ratings yet
- Olivia Herliani, DR., M.Si: DarahDocument82 pagesOlivia Herliani, DR., M.Si: DarahDaniel VictorNo ratings yet
- 1 Ext. Office Building - NightDocument23 pages1 Ext. Office Building - NightDarrell RoathNo ratings yet
- Toacs FCPS - IiDocument2 pagesToacs FCPS - IineptorNo ratings yet
- Final TouchDocument49 pagesFinal TouchmalathiNo ratings yet
- Truth & Lies About Saturated FatDocument33 pagesTruth & Lies About Saturated Fatalekad65No ratings yet
- Action Research BMIDocument7 pagesAction Research BMIKosaki SmithNo ratings yet
- Gestational Diabetes PDFDocument13 pagesGestational Diabetes PDFahaqullahNo ratings yet
- PR 10 Point Plan TemplateDocument15 pagesPR 10 Point Plan TemplateMegaEcoGuy100% (1)
- The Only Way To Achieve Harmony Is Through Practicing MindfulnessDocument8 pagesThe Only Way To Achieve Harmony Is Through Practicing MindfulnessAnn ZhyhalkinaNo ratings yet
- Scenario 3 Strange IllnessDocument2 pagesScenario 3 Strange IllnessYassin KhanNo ratings yet
- Srotas - Channels of The BodyDocument13 pagesSrotas - Channels of The BodySreedhar RaoNo ratings yet
- 2 - Carbohydrate MetabolismDocument30 pages2 - Carbohydrate MetabolismcayyoanisNo ratings yet
- TERMINOLOGI 2 ST - PencernaanDocument61 pagesTERMINOLOGI 2 ST - PencernaanSarah Suzanna Sitepu0% (1)
- Chronic Fatigue Syndrome/myalgic Encephalomyelitis (Or Encephalopathy)Document56 pagesChronic Fatigue Syndrome/myalgic Encephalomyelitis (Or Encephalopathy)Wilder Zuñiga AlcantaraNo ratings yet