Professional Documents
Culture Documents
A Second-Degree Burn After MRI: The Clinical Picture
Uploaded by
SLMC-QC IROriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
A Second-Degree Burn After MRI: The Clinical Picture
Uploaded by
SLMC-QC IRCopyright:
Available Formats
THE CLINICAL PICTURE
NICOLE S. MANDEL, MD JEREMY L. RAMDIAL, MD ERIN N. MARCUS, MD
Department of Obstetrics and Gynecology, Department of Hematology/Oncology, Department of Internal Medicine,
Mount Sinai Beth Israel Hospital, New York, NY Jackson Memorial Hospital, Miami, FL Jackson Memorial Hospital, Miami, FL
A second-degree burn after MRI
uncomplicated cellulitis despite intravenous
antibiotic therapy. The MRI showed multiple
enlarged inguinal lymph nodes and cellulitis of
the superficial soft tissues of the thigh without
discrete drainable collections.
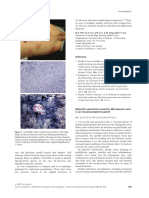
After the procedure, the patient was noted
to have a bullous lesion on each thigh, each
lesion roughly 1 cm in diameter and filled with
clear serous fluid (Figure 1). He reported that
his legs had been pressed together before en-
tering the MRI machine and that he had felt
a burning sensation in both thighs during
the test. Examination confirmed that the le-
sions indeed aligned with each other when he
pressed his thighs together.
Study of a biopsy of one of the lesions re-
vealed subepidermal cell blisters with focal
epidermal necrosis and coagulative changes in
the superficial dermis, consistent with a ther-
mal injury (Figure 2).
■ HOW BURNS CAN OCCUR DURING MRI
Thermal burns are a potential cause of injury
during MRI. Most have been observed in pa-
tients connected to external metal-containing
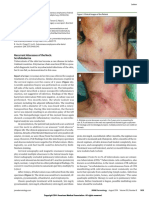
FIGURE 1. (A) Articulating 1-cm lesions developed
monitoring devices, such as electrocardiogram
after magnetic resonance imaging. The black and leads and pulse oximeters.1,2 Thermal burns in
red tracings on the right inner thigh indicate the patients unconnected to external devices have
original area of cellulitis. (B) A bullous lesion with occurred when the patient’s body was touch-
clear serous fluid on the right medial thigh. ing radiofrequency coils3 or, as with our pa-
tient, when skin touches skin.2,4,5 Skin-to-skin
48-year-old Nicaraguan man under-
A went magnetic resonance imaging (MRI) 3
days after admission to a South Florida hospital
contact during MRI can cause the scanner to
emit high-power electromagnetic radiofre-
quency pulses that are conducted through the
for treatment of cellulitis of the right thigh with body, creating heat. Tissue loops are created
vancomycin. MRI had been ordered to evaluate at points of skin-to-skin contact, thus forming
for a possible drainable source of infection, as a closed conducting circuit. The current flow-
the clinical picture and duration of illness was ing through this circuit can produce second-
worsening and longer than expected for typical degree burns.4
We believe that during placement in the
doi:10.3949/ccjm.84a.15164 scanner, our patient inadvertently moved his
348 C LEV ELA N D C L INIC J OURNAL OF MEDICINE VOL UME 84 • NUM BE R 5 M AY 2017
MANDEL AND COLLEAGUES
thighs together, forming a closed loop conduc- A
tion circuit and resulting in a thermal burn.
This case illustrates the importance of
correct positioning during MRI. The MRI
technicians had taken standard precau-
tions, placing a sheet over the patient and
ensuring no direct contact with the radio-
frequency transmitter receiver (MR unit).
However, precautions against skin-to-skin
contact were not taken, and the patient’s
legs were not separated.
■ LESSONS LEARNED
Appropriate positioning prevents closed skin- B
to-skin loops, but this may be more challeng-
ing in a larger patient.6 While the patient is in
the scanner, a “squeeze ball” alert system allows
the patient to signal the technologist should
unexpected distress or heating occur.6,7 A pa-
tient’s inability to utilize the squeeze ball con-
tributes to the risk of a severe injury. Further,
in this instance, there may have been a lan-
guage barrier. Also, proximity of the anatomic
skin-to-skin loop to the imaged body part (and
therefore the center of the MRI coil) may have
conferred risk related to field strength in this FIGURE 2. Focal epidermal necrosis
patient. (arrows) and coagulative changes in the
The MRI technologist, under supervision superficial dermis were consistent with
Afterward,
of a radiologist, is primarily responsible for po- thermal injury (hematoxylin and eosin; the patient
sitioning the patient to decrease the risk of this panel A magnification × 2.5; panel B
magnification × 10).
said his legs
complication and for following institutional
MRI safety protocols and professional guide- had been
lines.6–8 MRI technologist certification training pressed
highlights all aspects of safety, including skin-
to-skin conducting loop prevention.7,8 ■ together before
he entered the
■ REFERENCES 5. Landman A, Goldfarb S. Magnetic resonance-induced
1. Dempsey MF, Condon B. Thermal injuries associated with thermal burn. Ann Emerg Med 2008; 52:308–309. MRI machine
MRI. Clin Radiol 2001; 56:457–465. 6. Expert Panel on MR Safety; Kanal E, Barkovich AJ, Bell
2. Haik J, Daniel S, Tessone A, Orenstein A, Winkler E. MRI C, et al. ACR guidance document on MR safe practices:
induced fourth-degree burn in an extremity, leading to 2013. J Magn Reson Imaging 2013; 37:501–530.
amputation. Burns 2009; 35:294–296. 7. Magnetic resonance safety. Radiol Technol 2010; 81:615–616.
3. Friedstat J, Moore ME, Goverman J, Fagan SP. An un- 8. Shellock FG, Crues JV. MR procedures: biologic effects,
usual burn during routine magnetic resonance imaging. safety, and patient care. Radiology 2004; 232:635–652.
J Burn Care Res 2013; 34: e110–e111.
4. Eising EG, Hughes J, Nolte F, Jentzen W, Bockisch A. ADDRESS: Jeremy L. Ramdial, MD, Department of Hematol-
Burn injury by nuclear magnetic resonance imaging. Clin ogy/Oncology, Jackson Memorial Hospital, 1611 NW, 12th
Imaging 2010; 34:293–297. Avenue, Miami, FL 33136; jramdial@med.miami.edu
CL E V E L AND CL I NI C J O URNAL O F M E DI CI NE V O L UM E 84 • NUM BE R 5 M AY 2 0 1 7 349
You might also like
- Artigo Microcurrent As An Adjunct TherapyDocument10 pagesArtigo Microcurrent As An Adjunct TherapyDaniella MattosNo ratings yet
- Cars4u Project: Proprietary Content. © Great Learning. All Rights Reserved. Unauthorized Use or Distribution ProhibitedDocument30 pagesCars4u Project: Proprietary Content. © Great Learning. All Rights Reserved. Unauthorized Use or Distribution ProhibitedAbhay Poddar100% (2)
- Robin Alston Library History SourcesDocument52 pagesRobin Alston Library History SourcesAndrew PrescottNo ratings yet
- Standard Kessel Cat - Gral.Document40 pagesStandard Kessel Cat - Gral.Marcelo ResckNo ratings yet
- TRB Study Materials Operating System: WWW - Governmentexams.co - in 1Document9 pagesTRB Study Materials Operating System: WWW - Governmentexams.co - in 1Jeyaraman DhanarajNo ratings yet
- Marjolin Ulcer POSTER (RSCM)Document1 pageMarjolin Ulcer POSTER (RSCM)Juli Jamnasi100% (1)
- Löfgren's SyndromeDocument1 pageLöfgren's SyndromeLakshya J BasumataryNo ratings yet
- Interdisciplinary Neurosurgery: Technical Notes & Surgical TechniquesDocument5 pagesInterdisciplinary Neurosurgery: Technical Notes & Surgical TechniquesYovanka Naryai ManuhutuNo ratings yet
- Evento AdversoDocument3 pagesEvento AdversoSofia Bohorquez DazaNo ratings yet
- Subjective: Independent:: Nursing Care PlanDocument2 pagesSubjective: Independent:: Nursing Care PlanJade HemmingsNo ratings yet
- Case Report 1Document7 pagesCase Report 1Ussy FmsNo ratings yet
- 2014 - Intramuscular Cysticercosis - The Solitary ReaperDocument3 pages2014 - Intramuscular Cysticercosis - The Solitary Reaperizza mNo ratings yet
- A S C C F e V H W H C: A C RDocument5 pagesA S C C F e V H W H C: A C RMasithaNo ratings yet
- Adventitious Bursitis in The Plantar Fat Pad of Forefoot Presenting As A Tumoral MassDocument9 pagesAdventitious Bursitis in The Plantar Fat Pad of Forefoot Presenting As A Tumoral MassAaron SmithNo ratings yet
- Magnetic Resonance Imaging - 2010 - Jordanov - Minute Amounts of Intraarticular Gas Mimicking Torn Discoid Lateral MenisciDocument5 pagesMagnetic Resonance Imaging - 2010 - Jordanov - Minute Amounts of Intraarticular Gas Mimicking Torn Discoid Lateral Meniscinessim zouariNo ratings yet
- The History of Clinical Musculoskeletal RadiologyDocument8 pagesThe History of Clinical Musculoskeletal RadiologyVALENTINA LOPEZ MARINNo ratings yet
- Paper No 7Document4 pagesPaper No 7sahil jadhavNo ratings yet
- 2009 The Author(s) Journal Compilation 2009 British Association of Dermatologists - Clinical and Experimental Dermatology, 35, 440-450Document3 pages2009 The Author(s) Journal Compilation 2009 British Association of Dermatologists - Clinical and Experimental Dermatology, 35, 440-450nadyasantikaNo ratings yet
- DR MisbahDocument2 pagesDR MisbahAqee FarooqNo ratings yet
- JMT 23 162Document7 pagesJMT 23 162dark_PinchoNo ratings yet
- High-Resolution MRI of A Peroneal Intraneural Ganglion Cyst Arising From The Knee Joint: Illustrative CaseDocument4 pagesHigh-Resolution MRI of A Peroneal Intraneural Ganglion Cyst Arising From The Knee Joint: Illustrative CaseKrishna VamshiNo ratings yet
- Giant Cell Tumor of Tendon Sheath YjfasDocument6 pagesGiant Cell Tumor of Tendon Sheath YjfasPaulo Victor Dias AlmeidaNo ratings yet
- 71 Full PDFDocument3 pages71 Full PDFshiningdreamNo ratings yet
- RJZ 269Document3 pagesRJZ 269Saffa AzharaaniNo ratings yet
- Kim 2008Document3 pagesKim 2008HendrawanDianAgungWicaksanaNo ratings yet
- Jcis 8 6Document4 pagesJcis 8 6boy bionardoNo ratings yet
- Cardiac Assesement, CausalgiaDocument7 pagesCardiac Assesement, CausalgiaShubham SinghNo ratings yet
- Cheesborough2014 PDFDocument5 pagesCheesborough2014 PDFGregorius Thomas PrasetiyoNo ratings yet
- Post-Traumatic Neuroma After Hair Transplantation: LettersandcommunicationsDocument2 pagesPost-Traumatic Neuroma After Hair Transplantation: LettersandcommunicationsNishanthini AnnamalaiNo ratings yet
- Traumatic Aneurysm of Perforating Peroneal ArteryDocument4 pagesTraumatic Aneurysm of Perforating Peroneal ArteryDiana PredenciucNo ratings yet
- Cuti Bacterium 2019 Aid2019Document10 pagesCuti Bacterium 2019 Aid2019Vita BūdvytėNo ratings yet
- Travell 1952Document11 pagesTravell 1952Marita PalacoNo ratings yet
- UV-Induced Cutaneous Photobiology: Stefan Beissertll and Richard D. Gransfein2Document24 pagesUV-Induced Cutaneous Photobiology: Stefan Beissertll and Richard D. Gransfein2Darlyn HernandezNo ratings yet
- Painful Intramuscular Lipoma of The Infraspinatus Unusual Location and PresentationDocument4 pagesPainful Intramuscular Lipoma of The Infraspinatus Unusual Location and PresentationWewik PenaNo ratings yet
- 2005 Article 0117Document3 pages2005 Article 0117Gustavo BECERRA PERDOMONo ratings yet
- Review: The Diagnosis and Management of Morton's NeuromaDocument11 pagesReview: The Diagnosis and Management of Morton's NeuromaNishanthini AnnamalaiNo ratings yet
- Congenital Indifference To Pain: An Illustrated Case Report and Literature ReviewDocument8 pagesCongenital Indifference To Pain: An Illustrated Case Report and Literature ReviewNICOLÁS ANDRÉS AYELEF PARRAGUEZNo ratings yet
- A Case of Malignant Transformation of Solitary RecDocument4 pagesA Case of Malignant Transformation of Solitary RecDiana CantúNo ratings yet
- Muchemwa 2007Document4 pagesMuchemwa 2007prajwal guptaNo ratings yet
- Skeletal GB Mimant SarcomeDocument7 pagesSkeletal GB Mimant Sarcomeal qurtubi al andalusiNo ratings yet
- Compression of The Posterior Interosseous Nerve Sec 2024 International JournDocument4 pagesCompression of The Posterior Interosseous Nerve Sec 2024 International JournRonald QuezadaNo ratings yet
- JWMR 2021 01753Document5 pagesJWMR 2021 01753CSSNo ratings yet
- 10 1902@jop 1973 44 1 43Document6 pages10 1902@jop 1973 44 1 43ZEHRA ESENNo ratings yet
- Spinal Epidural Cavernous Hemangiomas in The 2024 International Journal of SDocument3 pagesSpinal Epidural Cavernous Hemangiomas in The 2024 International Journal of SRonald QuezadaNo ratings yet
- Diffuse LipomaDocument4 pagesDiffuse LipomaSASNo ratings yet
- Ncp-Case Pre Impaired Tissue Integrity-1Document2 pagesNcp-Case Pre Impaired Tissue Integrity-1Jade HemmingsNo ratings yet
- 3 Essay OrthoDocument11 pages3 Essay Orthogamal attamNo ratings yet
- Hemangioma SurgeryDocument5 pagesHemangioma Surgeryparsam618No ratings yet
- Atraumatic Muscle DisordersDocument23 pagesAtraumatic Muscle DisordersIgor MoraisNo ratings yet
- Neurocutaneous Vascular Hamartomas Mimicking Cobb Syndrome: Case ReportDocument4 pagesNeurocutaneous Vascular Hamartomas Mimicking Cobb Syndrome: Case ReportPam MoyolemaNo ratings yet
- Predicting Neurologic Outcome With MR Imaging in A Patient in Spinal ShockDocument1 pagePredicting Neurologic Outcome With MR Imaging in A Patient in Spinal ShockNabil FahliansyahNo ratings yet
- Pseudotumor Deltoideus Touch Me Not Lesion of TheDocument5 pagesPseudotumor Deltoideus Touch Me Not Lesion of TheneelimagooglyNo ratings yet
- Shubh Mpasicon Hydatid PosterDocument1 pageShubh Mpasicon Hydatid PosterShubh GhanghoriaNo ratings yet
- Atypical Presentation of Superficial Peroneal Nerve Schwannoma 2329 910X 2 151Document2 pagesAtypical Presentation of Superficial Peroneal Nerve Schwannoma 2329 910X 2 151amineNo ratings yet
- MSK UltrasoundDocument11 pagesMSK UltrasoundsafaNo ratings yet
- Recurrent Abscesses of The Neck: Scrofuloderma: Bacterium Tuberculosis PCR Were Negative. A Culture Was NotDocument2 pagesRecurrent Abscesses of The Neck: Scrofuloderma: Bacterium Tuberculosis PCR Were Negative. A Culture Was NothadriantiNo ratings yet
- TMP EADFDocument5 pagesTMP EADFFrontiersNo ratings yet
- Management of Right Pelvic Non Metastatic Grade 2 Chondrosarcoma Using Surgical Resection, ECRT and Reimplantation and Fixation Using Custom Made 3D Printed Plates A Case ReportDocument7 pagesManagement of Right Pelvic Non Metastatic Grade 2 Chondrosarcoma Using Surgical Resection, ECRT and Reimplantation and Fixation Using Custom Made 3D Printed Plates A Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- 2021 Article 572Document9 pages2021 Article 572Ous TNo ratings yet
- Rapid Recurrence of A Malignant Meningioma Case ReDocument4 pagesRapid Recurrence of A Malignant Meningioma Case Revivi talawoNo ratings yet
- RAL SURGERY - Chapter 31 - Management of Temporomandibular DisordersDocument4 pagesRAL SURGERY - Chapter 31 - Management of Temporomandibular DisordersIsabelle TanNo ratings yet
- Single Stage Release of Bilateral Amniotic Band Syndrome: Education-Family Physician CornerDocument4 pagesSingle Stage Release of Bilateral Amniotic Band Syndrome: Education-Family Physician CornerWara Samsarga GedeNo ratings yet
- Lesson Plan Electromagnetic SpectrumDocument5 pagesLesson Plan Electromagnetic SpectrumDanna Liza NilloNo ratings yet
- Relative Radiation Sensitivities of Human Organ SystemsFrom EverandRelative Radiation Sensitivities of Human Organ SystemsKurt I. AltmanNo ratings yet
- Learning The Nodal Stations in The AbdomenDocument9 pagesLearning The Nodal Stations in The Abdomentufis02No ratings yet
- Imaging Findings of Vascular Lesions in The Head and NeckDocument7 pagesImaging Findings of Vascular Lesions in The Head and NeckSLMC-QC IRNo ratings yet
- Hypopharynx and Larynx Anatomy: Poster No.: Congress: Type: AuthorsDocument21 pagesHypopharynx and Larynx Anatomy: Poster No.: Congress: Type: AuthorsSLMC-QC IRNo ratings yet
- NIH Public Access: Author ManuscriptDocument4 pagesNIH Public Access: Author ManuscriptSLMC-QC IRNo ratings yet
- Zeelandia Article X-FreshDocument2 pagesZeelandia Article X-Freshafb4No ratings yet
- Computer Graphics and AnimationDocument3 pagesComputer Graphics and AnimationRajeev GairolaNo ratings yet
- Commercial Non-Commercial: Customs InvoiceDocument2 pagesCommercial Non-Commercial: Customs InvoiceJavierNo ratings yet
- Allama Iqbal Open University, Islamabad (Assignment#2)Document12 pagesAllama Iqbal Open University, Islamabad (Assignment#2)ahsanNo ratings yet
- Datesheet Final Master Sept 2021 - 0Document1 pageDatesheet Final Master Sept 2021 - 0Tanushree JhaNo ratings yet
- Almaz BaruDocument9 pagesAlmaz BaruHarry WSNo ratings yet
- Current & Saving Account Statement: Ajju Cotton Mill 321 2 Vettuvapalayam Mangalam Tiruppur TiruppurDocument2 pagesCurrent & Saving Account Statement: Ajju Cotton Mill 321 2 Vettuvapalayam Mangalam Tiruppur Tiruppurajju computersNo ratings yet
- The Verb To Be ExplanationsDocument5 pagesThe Verb To Be ExplanationsLuz Maria Batista MendozaNo ratings yet
- After Hours - AR ThomasDocument338 pagesAfter Hours - AR ThomasThinaya JayarathneNo ratings yet
- Adobe AnalyticsDocument17 pagesAdobe AnalyticsGourav ChakrabortyNo ratings yet
- Lesson 1 M2Document6 pagesLesson 1 M2Ede ShingNo ratings yet
- Chapter 4: Redemption of Pref Share & Debentures Topic: Redemption of Debentures. Practice QuestionsDocument53 pagesChapter 4: Redemption of Pref Share & Debentures Topic: Redemption of Debentures. Practice QuestionsMercy GamingNo ratings yet
- CEC OrganisationDocument3 pagesCEC OrganisationAndreas ErnstNo ratings yet
- Design Build AgreementDocument21 pagesDesign Build AgreementMICHAELNo ratings yet
- Fashion - February 2014 CADocument144 pagesFashion - February 2014 CAAlmaMujanovićNo ratings yet
- Honeywell CT45XP CT45 Configuration Guide GLOBAL V2Document47 pagesHoneywell CT45XP CT45 Configuration Guide GLOBAL V2Roy SalasNo ratings yet
- Token Bus (IEEE 802)Document9 pagesToken Bus (IEEE 802)anon_185146696No ratings yet
- Group 2 - Mini Project Slide (Currypuff Maker)Document24 pagesGroup 2 - Mini Project Slide (Currypuff Maker)Muhd Khairul AmriNo ratings yet
- Science: Fourth Quarter - Module 1A Coordinate SystemDocument24 pagesScience: Fourth Quarter - Module 1A Coordinate Systemrollen grace fabulaNo ratings yet
- The Evidence Base For The Efficacy of Antibiotic Prophylaxis in Dental PracticeDocument17 pagesThe Evidence Base For The Efficacy of Antibiotic Prophylaxis in Dental PracticebmNo ratings yet
- Initial Nutrition Assessment FormDocument3 pagesInitial Nutrition Assessment FormAmina HaiderNo ratings yet
- Stone Washing Process of Denim FabricDocument11 pagesStone Washing Process of Denim FabricNguyễn Huy CườngNo ratings yet
- Yarn RequisitionDocument8 pagesYarn RequisitionAzim UddinNo ratings yet
- Republic of The Philippines Batangas State UniversityDocument13 pagesRepublic of The Philippines Batangas State UniversityGio LlanosNo ratings yet
- Enterprise Resources Planning (ERP) 2610002Document2 pagesEnterprise Resources Planning (ERP) 2610002Virendra Arekar100% (1)
- Academic CV Working DraftDocument3 pagesAcademic CV Working Draftapi-548597996No ratings yet