Professional Documents
Culture Documents
The Beneficial Effect of ST-36 (Zusanli) Acupressure On Postoperative Gastrointestinal Function in Patients With Colorectal Cancer
Uploaded by
Alwan Dhafi UmarOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
The Beneficial Effect of ST-36 (Zusanli) Acupressure On Postoperative Gastrointestinal Function in Patients With Colorectal Cancer
Uploaded by
Alwan Dhafi UmarCopyright:
Available Formats
See discussions, stats, and author profiles for this publication at: https://www.researchgate.
net/publication/235755598
The Beneficial Effect of ST-36 (Zusanli) Acupressure on Postoperative
Gastrointestinal Function in Patients With Colorectal Cancer
Article in Oncology Nursing Forum · March 2013
DOI: 10.1188/13.ONF.E61-E68 · Source: PubMed
CITATIONS READS
28 1,939
7 authors, including:
Henry Hsin-chung Lee
Cathay General Hospital, Hsinchu, Taiwan
57 PUBLICATIONS 367 CITATIONS
SEE PROFILE
All content following this page was uploaded by Henry Hsin-chung Lee on 17 September 2014.
The user has requested enhancement of the downloaded file.
© 2013 by the Oncology Nursing Society. Unauthorized reproduction is prohibited.
For permission to post online, reprint, adapt, or reuse, e-mail pubpermissions@ons.org. Online Exclusive Article
The Beneficial Effect of ST-36 (Zusanli) Acupressure
on Postoperative Gastrointestinal Function in Patients
With Colorectal Cancer
Hui-Lin Chao, RN, MSN, Shang-Jun Miao, RN, Pei-Fen Liu, MS, Henry Hsin-Chung Lee, MD,
Ying-Miao Chen, RN, Chung-Tay Yao, MD, and Hsiu-Ling Chou, RN, PhD
A
loss of bowel peristalsis is common
after abdominal surgery and can lead to Purpose/Objectives: To evaluate the effectiveness of
ST-36 (Zusanli) acupressure on recovery of postoperative
abdominal distention, pain, reduced bowel gastrointestinal function in patients with colorectal cancer.
sounds, emesis, or other discomforts. If
Design: A longitudinal, randomized, controlled trial design.
patients do not have bowel sounds or
Setting: An urban medical center in Taiwan.
bowel movement by the fourth day postsurgery, they
Sample: 60 patients with colorectal cancer who had un-
are considered to be at risk for postoperative ileus
dergone abdominal surgery.
(POI). POI is a significant clinical consequence and can
Methods: Patients were randomly assigned to two groups,
prolong hospitalization, which is a financial burden on the ST-36 acupressure group (n = 30) and a sham acupres-
patients and the healthcare system (Behm & Stollman, sure group (n = 30). Patients in the ST-36 group received an
2003; Chen et al., 2003; Delaney, Senagore, et al., 2006; acupressure procedure in a three-minute cycle performed
Meng et al., 2010). three times per day during the five days after surgery. Pa-
tients in the control group received routine postoperative
After surgical stress, which is the hormonal and
care and sham acupressure. Generalized estimating equa-
metabolic changes following an injury or operation, tions (GEEs) were used to gauge longitudinal effects of the
large amounts of catecholamines release because of two groups of patients.
overactive sympathetic tone and result in suppressed Main Research Variables: Frequency of bowel sounds, the
bowel function (Behm & Stollman, 2003). Inflammatory time to first flatus passage, first liquid intake, solid intake,
response following abdominal surgery also can stimu- and defecation.
late the release of prostaglandins and cytokines, which Findings: Patients who received acupressure had sig-
inhibit bowel activity (Delaney, Kehlet, et al., 2006). The nificantly earlier flatus passage and time to liquid intake
as compared to patients in the control group. Other main
intestine is more sensitive to anesthetic drugs because
variables, including the first time to solid intake and defeca-
of a lack of gaps between neuronal cells in the bowel. tion, did not show significant difference between the two
Anesthetics such as atropine, enflurane, and halo- groups. The GEE method revealed that all patients had
thane can inhibit gastrointestinal (GI) function (Baig increasing bowel sounds over time, and the experimental
& Wexner, 2004). Analgesics, particularly opioids such group had greater improvement of bowel motility than the
control group within the period of 2–3 days postoperatively.
as morphine, also can inhibit bowel sound (Baig &
Wexner, 2004). Nasogastric intubation is a supportive Conclusions: ST-36 acupressure was able to shorten the
time to first flatus passage, oral liquid intake, and improve
therapy to prevent abdominal distension, vomiting, gastrointestinal function in patients after abdominal surgery.
and POI, which may complicate the postoperative
Implications for Nursing: ST-36 acupressure can be
course after abdominal surgery; however, studies have integrated into postoperative adjunct nursing care to assist
shown that the use of nasogastric intubation does not patients’ postoperative gastrointestinal function.
shorten the bowel function recovery time. Instead, Knowledge Translation: Few studies have explored the
intubation further slows the passage of flatus and can effectiveness of acupressure techniques on promoting
interfere with food intake (Lee, Hyung, & Noh, 2002; bowel sounds. Evidence from this study suggests stimulation
Vermeulen, Storm-Versloot, Busch, & Ubbink, 2006). of the ST-36 acupressure point can increase bowel sound
frequency for patients with colorectal cancer in the first
Voluntary flatus passage is an important indicator of
three days after surgery. Application of this technique may
postoperative bowel function recovery. According to improve a patient’s comfort after surgery.
the literature, the recovery of small intestine motility is
Oncology Nursing Forum • Vol. 40, No. 2, March 2013 E61
the earliest activity in the postoperative period; stomach Acupuncture and electro-acupuncture, however, are
motility returns within 24–48 hours and colonic motility not suitable for clinical nursing care because they are
recovers within 3–5 days (Carroll & Alavi, 2009; Nachlas, invasive techniques that require specialized training.
Younis, Roda, & Wityk, 1972; Wilson, 1975). No consen- Acupressure is a form of Chinese traditional medi-
sus exists on a guideline for treatment of postoperative cine therapy and is based on the same principles as
GI function recovery; however, and current clinical acupuncture. However, acupressure is a noninvasive
interventions of GI function recovery include restrict- technique that uses fingers to rub, knead, nail pinch,
ing oral intake of food and liquid, increasing physical and press instead of using needle insertion at the dif-
activity, and prescribing prokinetics, laxatives, or enemas ferent acupressure points on the body. Acupressure
(Behm & Stollman, 2003; Delaney, Kehlet, et al., 2006). involves stimulating surface acupoints to stimulate the
The effectiveness of these approaches on restoring GI energy, or Qi, of the body to achieve comfort and relief
function is still in question. Therefore, knowing what (Chang, Liu, Li, Chen, & Chou, 2006; Takahashi, 2006).
care the nursing staff can apply to promote postoperative A study by Chen et al. (2003) demonstrated that acu-
GI recovery is crucial. pressure at ST-36, PC-6, and SP-6 (Sanyinjiao) applied
Studies have shown that stimulations from acu- after surgery increased GI motility in patients who
puncture and electro-acupuncture can increase bowel underwent hysterectomy. Acupressure was continued
sounds. In an animal study by Iwa et al. (2006), electro- for three days twice a day on the three acupoints for
acupuncture of ST-36, or Zusanli, stimulated terminal three minutes each, and the increase in GI motility in
rectal activity through parasympathetic transmission. A the experimental group was found to be significant
study by Chen, Song, Yin, Koothan, and Chen (2008) on (p < 0.05). However, researchers from that study were
canines suggested that, by stimulating ST-36, impaired unable to tell which acupoint is predominant in im-
gastric motility from rectal distension could be restored proving bowel sounds.
by exerting a modulating effect on gastric dysrhythmia. To fill the gaps in knowledge, the current study was
One approach in human studies is to measure the pe- conducted to test whether ST-36—being one of the most
riod dominant power, which is defined as the power important “hubs” in the various acupressure points—
at the dominant frequency in the power spectrum of can be used alone to improve bowel sounds. ST-36
electrogastrogram (EGG). The dominant frequency of is used primarily for treating ailments related to the
EGG has been shown to be equal to the frequency of digestive, neurologic, and respiratory systems (Chang
the gastric slow wave measured from implanted sero- et al., 2006). ST-36 is located lateral to the tibia and is
sal electrodes (Chen, Schirmer, & McCallum, 1994). A four finger breadths down from the patella (see Figure
study by Shiotani, Tatewaki, Hoshino, and Takahashi 1). The acupressure practitioner can apply pressure on
(2004) used a single-group, pre-/post-test design to as- ST-36 using his or her thumb, which makes it a more
sess the level of change in gastric musculature before suitable nursing care skill because of the less-invasive
and after stimulation of ST-36 and PC-6 (Neiguan). The nature and being a simpler technique to perform than
EGG assessment demonstrated that stimulating ST-36 acupuncture.
alone could increase the gastric period dominant power The purpose of the current study was to compare the
by 154% (SD = 28%). However, simultaneous stimula- effectiveness of ST-36 acupressure with that of sham acu-
tion of both ST-36 and PC-6 did not change the percent- pressure on the frequency of bowel sounds, time to first
age of normal slow waves or the percentage of tachy- passage of flatus, time to first oral liquid intake, time to
gastria (Shiotani et al., 2004). The findings suggested first solid intake, and time to first defecation in patients
that stimulation of ST-36 alone could increase gastric with colorectal cancer after abdominal surgery. Based
motility. Chang, Ko, Wu, and Chen (2001) indicated that on the effects of ST-36 acupressure on increasing bowel
electrical acupuncture stimulation at the ST-36 points sound (Chang et al., 2006), the authors hypothesized
could significantly increase the percentages of normal that stimulation of ST-36 can promote bowel sounds
EGG frequency, suggesting that stimulation of ST-36 and reduce the time required for solid food intake and
alone could increase gastric motility. Therefore, electri- bowel movement.
cal acupuncture stimulation at ST-36 could significantly
increase the percentages of normal EGG frequency Methods
(Chang et al., 2001). Another study using healthy
human participants found that electrical stimulation Sample and Setting
of acupuncture points may enhance the regularity of The study used a randomized, controlled trial,
gastric myoelectrical activity, which increases bowel repeated-measures, random-sequencing design to com-
movement (Chou, Chang, Chang, & Chen, 2003). pare the frequency of bowel sounds, the time to first
All of the studies involved either acupuncture or passage of flatus, and the time to oral liquid and solid
electro-acupuncture at ST-36 to increase GI motility. intake and defecation in patients with colorectal cancer
E62 Vol. 40, No. 2, March 2013 • Oncology Nursing Forum
after abdominal surgery between the ST-36 experimen- the study in detail and obtained informed consent from
tal and control groups. Participants were recruited by participants who met the study criteria.
convenience sampling from an urban medical center
in Taipei, Taiwan, and were limited to patients with
ST-36 Acupressure Method
colorectal cancer who had undergone either colectomy Patients in the experimental group received routine
or rectal resection. All participants met the following postoperative care and ST-36 acupressure. Before ap-
inclusion criteria: (a) aged 18 years or older, (b) under- plying acupressure, a licensed physician of traditional
went colorectal surgery for the first time, (c) had only Chinese medicine would locate and mark the ST-36
one surgery while hospitalized, (d) and had no lower acupressure point, and the trained research nurse ap-
limb defects or infections that would hinder the ac- plied acupressure on the ST-36 point. The acupressure
curacy of ST-36 identification and pressure or worsen procedure involved one press per second, and, after
local infections. Patients with chronic pain requiring five continuous one-second presses and a two-second
long-term use of analgesics or sleeping pills, those with rest, the cycle was repeated for three minutes. The
mental disabilities, or those with communication and depth of each press had a reach of 1–1.5 cm and the
compliance difficulty also were excluded. force was about 3–5 kg. The procedure was repeated on
Eighty patients with colorectal cancer who were the contralateral leg (Chen et al., 2003; Chen, Wang, &
about to undergo abdominal surgery were recruited. Tsai, 1998; Ma, Chang, & Lin, 2007). During each two-
A total of 66 participants fit the inclusion criteria. In second rest period, the patient was asked whether he
the follow-up period, three patients underwent a sec- or she felt soreness, fullness, or heat sensation, which
ond surgery, and three patients refused participation, are indicative of the correct ST-36 site. If the patient an-
and were therefore excluded from the study. The total swered “yes,” the acupressure session continued; if the
number of participants included for final analysis was patient answered “no,” the location of acupressure was
60, with 30 in the ST-36 experimental group and 30 readjusted until the patient responded with positive
in the control group. The study was approved by the soreness, fullness, or heat sensation before applying the
institutional review board and research committee at same cycles once more. Patients in the control group
Cathay General Hospital. The first author explained received routine postoperative care and sham acupres-
sure, which applied pressure on a location along the
nonacupressure point of the tibia and in the same way
as the experimental group, but participants were only
asked whether the pressure was causing any discomfort.
Measurements
The data categories of the current study are patient’s
basic information, medical history, clinical information,
and measurement of the effectiveness of acupressure.
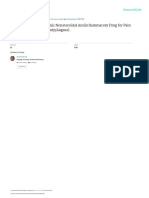
Patella
The basic information and medical history included
gender, age, highest level of education achieved,
whether or not the patient had regularly exercised in
the past six months, a history of diseases related to
the gastrointestinal tract, and whether the patient had
taken any drugs in the past weeks that could affect def-
ST-36
(Zusanli) ecation. The clinical information included cancer TNM
(tumor size, lymph node involvement, and distant
metastases) staging, primary cancer location, surgery
method, whether a nasogastric tube was in place, and
whether opioid analgesics and sedatives had been
used. Measurements of acupressure effectiveness made
by a research nurse included (a) a daily record of the
frequency of bowel sounds during the three-minute ob-
servation period, (b) the time to the first flatus passage
Note. ST-36 (Zusanli) is bilaterally located about four finger and defecation, and (c) the time to oral liquid and solid
breadths from the lower border of the patella, lateral to the tibia. intake. Bowel sounds were auscultated and measured
at each of the four quadrants of the abdomen using a
Figure 1. Acupressure at ST-36 (Zusanli)
stethoscope. A timer was set for three minutes for each
Note. Photo courtesy of Pei-Fen Liu. Used with permission.
assessment. The frequency of bowel sounds per minute
Oncology Nursing Forum • Vol. 40, No. 2, March 2013 E63
was counted and recorded. To prevent assessment error, Results
a physician concomitantly confirmed the accuracy of
measurement by performing the assessments simulta-
Demographic and Clinical Data
neously. The interobserver correlation was 0.95. Sixty participants were included for analysis; 30 in
the experimental group and 30 in the control group.
Procedures The mean age was 61.9 years (SD = 13.3 years) in the
Two trained research nurses were involved in this experimental group and 62.8 years (SD = 15.7 years)
study. One research nurse performed acupressure on in the control group. Fourteen patients (47%) in the
all of the patients; the other research nurse, who was experimental group were men, as were 17 (57%) in the
blinded to patients’ assigned groups, did not perform control group. The highest education level for both the
acupressure but was, instead, responsible for bowel experimental and control groups was primary or junior
sounds measurement and general data collection. After high school (47% and 53%, respectively). Twenty-eight
abdominal surgery, patients in both the ST-36 experi- patients (93%) in both groups had no history of disease
mental and control groups had their first baseline (T0) related to the gastrointestinal tract. In the experimental
bowel sounds assessment after returning to the general group, 16 (53%) exercised regularly, compared to 12
surgical ward from the postoperative recovery room. (40%) in the control group. Most patients in the experi-
Taking into consideration that the patients were not fully mental and control groups had not taken any medication
recovered from the effect of anesthesia, and to ensure that affects defecation one week prior to hospitalization
that the patients were not disturbed on their first night (90% and 87%, respectively). When all of the variables
after surgery, the intervention was begun at 6:30 am on were analyzed with the independent t test and the
the first day after surgery. Acupressure was performed Chi-square test, no differences were found between the
every eight hours at three different times, 6:30 am, 3:30 demographic characteristics of the two groups.
pm, and 11:30 pm, for five consecutive days, yielding 15 Colon cancer was indicated in 21 (70%) of the patients
measurements (T1–T15). After each session of ST-36 or in the experimental group, compared to 23 (77%) in the
sham acupressure was completed, the blinded research control group. Patients in this study all underwent open
nurse then measured the frequency of bowel sounds, abdominal colectomy or rectal resection. Fifteen patients
the time to first flatus passage, defecation, and when (50%) in the experimental group had right or left hemico-
oral liquid and solid intake started after surgery. The lectomy, compared to 13 (43%) in the control group. Low
research nurse then recorded the data on an electronic anterior resection accounted for 11 patients (37%) in the
spreadsheet. experimental group compared to 10 (33%) in the control
group. As for cancer stage distribution, seven participants
Data Analysis (23%) in the experimental group and 11 (37%) in the con-
Demographic and clinical data were summarized trol group had clinical TNM stages 0 and I. TNM stage II
with descriptive statistics such as frequency, percent- was noted in 12 participants (40%) from the experimental
ages, and means. The chi-square test or Fisher’s exact group and 13 (43%) of the control group. TNM stage III
test was used to compare the categorical data between was noted in six participants (20%) of the experimental
experimental and control groups. For continuous data, group and four (13%) of the control group. TNM stage
the independent t test was used to compare the time IV occurred in five participants (16%) of the experimental
to first passage of flatus, defecation, and oral liquid group and three (7%) of the control group.
and solid intake between the two groups. The authors Twenty-nine patients in the experimental and twenty-
also used the independent t test to compare the bowel seven patients in the control groups received PCA (97%
sounds between the two groups at each observation and 90%, respectively), and 29 patients in the experimen-
time point. GEE method’s generalized linear models tal and 28 in the control groups were given analgesics
were used to estimate longitudinal effects of ST-36 point (meperidine 1 mg/kg every three hours) as needed (97%
acupressure on bowel sounds. Independent variables and 93%, respectively). As for sedatives, two patients
were two groups each with 15 observation points; the (6%) in the experimental group and three patients (7%)
interaction variable was 15 observation points by two in the control group had sedative drugs prescribed. A
groups. Potential control variables were age, location nasogastric tube had been placed in 14 patients (47%) in
of the tumor, cancer stage, surgical procedure, use of the experimental group compared to 17 (57%) in the con-
a nasogastric tube, patient-controlled analgesia (PCA), trol group. After chi-square test analysis, no differences
and opioid analgesics or sedative medicine. SPSS®, were found between the clinical data in the two groups.
version 17.0, statistical analysis program was used
for data management and analysis. The p values were Effects of Acupressure
two-tailed, and p < 0.05 was considered statistically The frequency of bowel sounds increased in all
significant. patients after surgery (see Table 1). The independent
E64 Vol. 40, No. 2, March 2013 • Oncology Nursing Forum
t test was used to evaluate the
Table 1. Difference in the Frequencies of Bowel Sounds Between
differences in frequency of bowel
Experimental and Control Groups Every Eight Hours Postsurgery (N = 60)
sounds in both groups. The fre-
quency of bowel sounds in the Experimental (n = 30) Control (n = 30)
Observation
experimental group was signifi- Time Point —
X SD Range
—
X SD Range p
cantly higher than in the control
group for the first two days (T1– T0: Baseline a 0.93 1.08 0–3 0.9 1.75 0–6 0.522
T1: 6:30 am 4.1 4.12 0–16 1.23 2.49 0–10 0.002
T7) after surgery, but not after. T2: 8 hours after T1 4.53 3.7 0–14 1.57 2.37 0–8 0.001
GEE was used to estimate T3: 16 hours after T1 5.6 4.21 0–15 2.27 3.18 0–10 0.001
group longitudinal effects of ST- T4: 24 hours after T1 5.4 3.1 0–11 2.87 3.67 0–13 0.006
T5: 32 hours after T1 8.3 4.68 2–18 4.77 4.09 0–12 0.003
36 acupressure on bowel sounds, T6: 40 hours after T1 9.33 5.27 0–23 5.9 5.25 0–23 0.014
and the model indicated no sta- T7: 48 hours after T1 10.07 6.21 1–32 6.73 6.31 0–32 0.044
tistically significant differences T8: 56 hours after T1 10.47 3.85 4–2 8.33 7.5 0–30 0.106
between the two groups in fre- T9: 64 hours after T1 10.27 3.95 2–18 9.27 7.47 0–28 0.52
T10: 72 hours after T1 10.9 4.53 2–27 9.17 5.65 0–27 0.195
quency of bowel sounds. For time T11: 80 hours after T1 10.73 4.13 4–21 9.47 5.8 2–20 0.334
effects, both groups showed an T12: 88 hours after T1 10.73 3.81 5–22 10.03 5.77 2–22 0.581
increasing trend of bowel sounds T13: 96 hours after T1 11.23 4.43 2–26 10.63 5.6 4–26 0.647
with time since surgery. From T1 T14: 104 hours after T1 11 3.79 3–19 11.43 5.04 3–20 0.708
T15: 112 hours after T1 12.33 3.37 3–20 11.57 4.22 5–22 0.44
to T7, the changes in bowel sound
frequency of the experimental a The morning after surgery
group were significantly better
than in the control group (p <
0.001, p < 0.001, p < 0.001; p = 0.002, p = 0.001, p = 0.01, symptoms in Taiwan (Chen et al., 2003; Ming, Kuo,
and p = 0.041). The changing pattern at the remaining Lin, & Lin, 2003). The study demonstrated that apply-
time points (T8–T15) did not show any difference be- ing acupressure on ST-36 after colorectal surgery can
tween the control and experimental groups. Based on increase the frequency of bowel sounds, shorten the
these findings, the authors concluded that the ST-36 flatus passage time, and accelerate recovery of bowel
acupressure can stimulate increased and earlier bowel function. The findings are consistent with those previ-
sounds, extending to two to three days after abdominal ously reported in the literature. Another advantage
surgery. In the GEE method, after controlling for clini- of acupressure of the ST-36 is that this technique can
cal variables, patients using a PCA device had more be easily taught and can be used to relieve abdominal
bowel sounds compared to those not using it (p = bloating, increase the frequency of bowel sounds, and
0.032); patients who received meperidine analgesic had shorten time required for flatus passage after surgery.
fewer bowel sounds than those who did not (p < 0.001); The findings support the authors’ study hypothesis
patients with nasogastric intubation had fewer bowel and demonstrate that changes of bowel sounds at T1
sounds than those without (p = 0.022) (see Table 2). (6:30 am the first day after surgery) to T7 (48 hours after
The times to first passage of flatus, oral liquid food, T1) were greater among patients in the experimental
solid food intake, and defecation in the patients were group than among patients in the control group, in-
evaluated. As seen in Table 3, the mean time to first dicating that pressing on ST-36 has a significant effect
flatus passage after surgery was 2.78 days (SD = 0.92 on bowel sounds within 48 hours after T1. Previous
days) in the experimental group and 3.61 days (SD = studies (Chang et al., 2001; Shiotani et al., 2004) have
1.15 days) in the control group (p = 0.003). Mean time indicated that applied acupressure or acupuncture can
to first liquid intake was 3.43 days (SD = 0.97 days) stimulate several GI hormones (e.g., motility, gastrin,
in the experimental group, which is earlier than the pancreatic polypeptide) that regulate the contraction of
—
control group (X = 4.26 days, SD = 1.42 days, p = 0.01). gastric smooth muscle or small intestinal mucosa and
However, no difference was noted between the two increase gastric emptying in the human body.
—
groups in the mean time to first solid food intake (X = In addition, the current study demonstrated that
4.54 versus 5.11 days, p = 0.177) and the time to first the time to first flatus passage after surgery in the ex-
—
defecation (X = 4.75 versus 5.25 days, p = 0.236). perimental group was 2.78 days, which is sooner than
3.6–4 days reported in patients who underwent open
colectomy (Liu, Lin, Ye, & Teng, 2010; Salimath, Jones,
Discussion Hunt, & Lane, 2007). In Taiwan, patient solid food
Acupressure therapy, as part of Chinese traditional intake depends on the individual patient’s subjective
medicine therapy, is accepted by the local population comfort level with a clear liquid diet after first flatus
(Yu et al., 2006) and is commonly sought to relieve GI passage, and no difference was seen between the two
Oncology Nursing Forum • Vol. 40, No. 2, March 2013 E65
groups in terms of the first time to solid food intake and perception of pain by the cerebral cortex (Kharkevich
defecation. Two previous studies indicated that first & Churukanov, 1999). Since opioid analgesics act on
defecation took 4.4 days for open colectomy and that the central nervous system, aside from complications
acupuncture did not benefit earlier solid food intake such as respiratory inhibition, sedation, or addic-
and defecation for postoperative patients (Meng et al., tion, opioid analgesics also can reduce the secretion
2010; Salimath et al., 2007). In Taiwan, patient solid food of intestinal fluids, decrease propulsive motility, and
intake depends on the individual patient’s subjective increase absorption of water and salts from feces, caus-
comfort level with a clear liquid diet after first flatus ing constipation (Murphy, Sutton, Prescott, & Murphy,
passage. On the other hand, patients who have a naso- 1997). The current study’s findings demonstrated that
gastric tube in place for several days are given IV fluid intramuscular injection of meperidine does reduce GI
or nasogastric feeding, thus leading to prolonged time motility, but IV infusion of PCA was associated with
before solid food intake and defecation. increased bowel sounds. The authors postulate that
Opioid analgesics, such as morphine and meperidine, the reason for this was that patients who received PCA
are commonly prescribed postoperatively for pain re- in this study were prescribed a regimen that included
lief. Their pharmacologic mechanism involves blocking ketorolac, a nonsteroidal anti-inflammatory drug that
the transmission of pain sensation and reducing the mainly acts on the peripheral nervous system and can
inhibit the production of prostaglandins, which in
turn reduce the inhibitory effects on bowel sound
Table 2. Changes in Bowel Sounds by Generalized (Lee et al., 2002; Vermeulen et al., 2006). Another
Estimating Equation Model clinical study investigated 79 patients who under-
Variable Estimate SE 95% CI p
went a colectomy and found that adding ketorolac
to PCA not only reduced consumption of morphine
Intercept 3.56 2.29 [–1, 8.03] 0.118 by 29%, but shortened the time for flatus passage as
Groupa
Experimental –0.45 0.62 [–1.6, 0.764] 0.654
well (Chen et al., 2005). A combination, therefore, of
Time b analgesics can decrease the direct damage of opioid
T1 0.33 0.18 [–0.03, 0.7] 0.071 analgesics on intestinal tract function. In contrast to
T2 0.67 0.2 [0.26, 1.07] 0.001 intramuscular injection of meperidine-type drugs,
T3 1.37 0.37 [0.64, 2.1] < 0.001
T4 1.97 0.56 [0.87, 3.07] < 0.001
PCA can relieve not only pain but also inflammation,
T5 3.87 0.65 [2.59, 5.15] < 0.001 and has a degree of protection on the GI tract. Such
T6 5 0.91 [3.22, 6.78] < 0.001 a combination of medicine can help patients return
T7 5.83 1.09 [3.68, 7.99] < 0.001 to physical function (Chen et al., 2005).
T8 7.43 1.34 [4.82, 10.05] < 0.001
T9 8.37 1.19 [6.03, 10.71] < 0.001 Clinically, nasogastric tube placement, usually
T10 7.93 0.99 [6.36, 10.17] < 0.001 after abdominal surgery, is used to decompress the
T11 8.57 0.98 [6.46, 10.49] < 0.001 stomach and to avoid postoperative complications
T12 9.13 1.01 [7.15, 11.12] < 0.001 such as abdominal bloating, nausea, vomiting, bowel
T13 9.73 0.97 [7.84, 11.63] < 0.001
T14 10.53 0.87 [8.82, 12.25] < 0.001 obstruction, and leakage at the site of the anastomo-
T15 10.67 0.75 [9.19, 12.15] < 0.001 sis (Nelson, Tse, & Edwards, 2005; Wolff et al., 1989).
Interactionc Results from this study suggest that the prolonged
T0–T1 2.83 0.67 [1.52, 4.15] < 0.001
placement of a nasogastric tube has a negative
T0–T2 2.93 0.64 [1.68, 4.19] < 0.001
T0–T3 3.3 0.83 [1.67, 4.93] < 0.001 relationship with the frequency of bowel sounds.
T0–T4 2.5 0.8 [0.93, 4.07] 0.002 That result is consistent with the findings of a meta-
T0–T5 3.5 1.03 [1.48, 5.52] 0.001 analysis study by Yang, Zheng, and Wang (2008)
T0–T6 3.4 1.33 [0.81, 5.99] 0.01
that showed time to flatus was shorter in the group
T0–T7 3.07 1.5 [0.13, 6] 0.041
Control without nastrogastric decompression and that de-
Use PCAd 1.93 0.9 [0.16, 3.7] 0.032 compression may not prevent but actually facilitate
Inject meperidinee –4.35 0.92 [–6.15, –2.54] < 0.001 postoperative ileus. Vermeulen et al. (2006) indicated
Nasogastric tubef –1.37 0.6 [–2.55, –0.2] 0.022
that, after abdominal surgery, patients without naso-
CI—confidence interval; PCA—patient-controlled analgesia; SE—standard gastric tubes did not experience more postoperative
error complications such as pneumonia, wound infection,
a
Compared to control group and leakage at the site of anastomosis compared to
b
Compared to baseline (T0) those with nasogastric intubation. The studies sug-
c
Experimental compared to control group time
gest that no clinical evidence exists showing that a
d
Compared to non-use of PCA
nasogastric tube can be beneficial to postoperative
e
Compared to non-use of meperidine
recovery. To the contrary, it might cause some unex-
f
Compared to those without a nasogastric tube
pected side effects, such as discomfort, damage to
E66 Vol. 40, No. 2, March 2013 • Oncology Nursing Forum
should target a more diversified sample. Researchers
Table 3. Days After Surgery to First Passage of
should study the physiological mechanisms of ST-36
Flatus, Liquid Intake, Solid Intake, and Defecation
by Group (N = 60) acupressure on GI function. Also, ST-36 acupressure
for facilitating bowel motility after surgery should be
Experimental Control examined with a larger and more diverse sample.
(n = 30) (n = 30)
— —
Variable X SD X SD p
Conclusion
Passage of flatus 2.78 0.92 3.61 1.15 0.003
Liquid intake 3.43 0.97 4.26 1.42 0.01 This study demonstrated that ST-36 acupressure
Solid intake 4.54 1.17 5.11 1.99 0.177 alone can improve postoperative GI function in patients
Defecation 4.75 1.17 5.25 1.96 0.236 with colorectal cancer by increasing the frequency of
bowel sounds and shortening the time to first flatus
passage and first liquid food intake. Acupressure is a
the nasal cavity and throat, esophageal or gastric ulcers, noninvasive, safe, and an easy-to-perform technique.
electrolyte imbalance, restrictions in food intake, pneu- Under guidance, the caretaker or even the patient can
monia, and psychological problems such as impaired be taught to perform the technique to achieve earlier
consciousness (Manning, Winter, McGreal, Kirwan, & return of bowel function. It also is a simple adjunct
Redmond, 2001; Vermeulen et al., 2006). Prolonged na- technique that nurses can apply. By integrating ST-36
sogastric tube use may interfere with normal physical acupressure into nursing care practice, patients’ post-
function (Rao et al., 2011; Sagar, Kruegener, & MacFie, operative bowel dysfunction can be reduced.
1992). The effects of early tube removal on the recovery
of GI function for patients who remain on gastric intu- The authors gratefully acknowledge the study participants for their
cooperation. The authors also thank John Ting, BA, and Elizabeth
bation after surgery should be assessed in the future. Earl Phillips, BA, for revising the English version of this article.
Strengths and Limitations Hui-Lin Chao, RN, MSN, is the deputy director, Shang-Jun
Miao, RN, is a head nurse, and Pei-Fen Liu, MS, is a staff man-
The current study was strengthened by (a) the aid of ager, all in the Department of Nursing, Henry Hsin-Chung Lee,
a physician licensed in traditional Chinese medicine to MD, is chair of the Department of Surgery, Ying-Miao Chen,
locate the ST-36 acupoint, (b) the use of a single inter- RN, is a head nurse in the Department of Nursing, and Chung-
vener to apply the acupressure technique, (c) a separate Tay Yao, MD, is an attending physician in the Department of
Surgery, all at Cathay General Hospital in Taipei, Taiwan; and
outcome assessor and intervener to prevent measure- Hsiu-Ling Chou, RN, PhD, is deputy director and associate
ment bias, and (d) five days of continued intervention professor in the Department of Nursing at Far Eastern Me-
to discover the full scope of the technique. morial Hospital and Oriental Institute of Technology in New
Taipei City, Taiwan. This article was supported by a research
One limitation is that only a small and specialized grant from Cathay General Hospital (CMR19618). Chou can
sample was used. This sample included only patients be reached at chl@mail.femh.org.tw, with copy to editor at
with colorectal cancer; therefore, the authors cannot ONFEditor@ons.org. (Submitted June 2012. Accepted for
determine what effect this technique will have on other publication June 26, 2012.)
patients undergoing abdominal surgery. Future studies Digital Object Identifier: 10.1188/13.ONF.E61-E68
References
Baig, M.K., & Wexner, S.D. (2004). Postoperative ileus: A review. waves induced by rectal distension in dogs. American Journal of
Diseases of the Colon and Rectum, 47, 516–526. doi:10.1007/s10350 Physiology Gastrointestinal Liver Physiology, 295(3), G614–G620.
-003-0067-9 doi:10.1152/ajpgi.90322
Behm, B., & Stollman, N. (2003). Postoperative ileus: Etiologies and Chen, J.D., Schirmer, B.D., & McCallum, R.W. (1994). Serosal and
interventions. Clinical Gastroenterology and Hepatology, 1, 71–80. cutaneous recordings of gastric myoelectrical activity in patients
doi:10.1053/cgh.2003.50012 with gastroparesis. American Journal of Physiology, 266(1), G90–G98.
Carroll, J., & Alavi, K. (2009). Pathogenesis and management of Chen, J.Y., Wu, G.J., Mok, M.S., Chou, Y.H., Sun, W.Z., Chen, P.L., . . .
postoperative ileus. Clinics in Colon and Rectal Surgery, 22, 47–50. Wen, Y.R. (2005). Effect of adding ketorolac to intravenous mor-
doi:10.1055/s-0029-1202886. phine patient-controlled analgesia on bowel function in colorectal
Chang, C.S., Ko, C.W., Wu, C.Y., & Chen, G.H. (2001). Effect of surgery patients: A prospective, randomized, double-blind study.
electrical stimulation on acupuncture points in diabetic patients Acta Anaesthesiologica Scandinavica, 49, 546–551.
with gastric dysrhythmia: A pilot study. Digestion, 64, 184–190. Chen, L.L., Hsu, S.F., Wang, M.H., Chen, C.L., Lin, Y.D., & Lai, J.S.
doi:10.1159/000048860 (2003). Use of acupressure to improve gastrointestinal motility in
Chang, H.C., Liu, H.M., Li, Y.T., Chen, H.F., & Chou, P.H. (2006). The women after trans-abdominal hysterectomy. American Journal of
review of application of acupressure massage in clinical nursing Chinese Medicine, 31, 781–790.
care. Journal of Long Term Care, 10, 91–101. Chen, L.L., Wang, C.C., & Tsai, H.C. (1998). Exploration of the effect
Chen, J., Song, G.Q., Yin, J., Koothan, T., & Chen, J.D.Z. (2008). in improving bowel sound of using acupoint massage on post-
Electroacupuncture improves impaired gastric motility and slow cesarean section women. Nursing Research, 6, 526–534.
Oncology Nursing Forum • Vol. 40, No. 2, March 2013 E67
Chou, J.W., Chang, Y.H., Chang, C.S., & Chen, G.H. (2003). The ef- Murphy, D.B., Sutton, J.A., Prescott, L.F., & Murphy, M.B. (1997).
fect of different frequency electrical acu-stimulation on gastric Opioid-induced delay in gastric emptying: A peripheral mecha-
myoelectrical activity in healthy subjects. Hepatogastroenterology, nism in humans. Anesthesiology, 87, 765–770.
50, 582–586. Nachlas, M.M., Younis, M.T., Roda, C.P., & Wityk, J.J. (1972). Gastro-
Delaney, C.P., Kehlet, H., Senagore, A.J., Bauer, A.J., Beart, R., Billing- intestinal motility studies as a guide to postoperative management.
ham, R., . . . Steinbrook, R.A. (2006). Postoperative ileus: Profiles, risk Annals of Surgery, 175, 510–522.
factors, and definitions: A framework for optimizing surgical outcomes in Nelson, R., Tse, B., & Edwards, S. (2005). Systematic review of
patients undergoing major abdominal and colorectal surgery. Retrieved prophylactic nasogastric decompression after abdominal surgeries.
from http://www.clinicalwebcasts.com/pdfs/GenSurg_WEB.pdf British Journal of Surgery, 92, 673–680. doi:10.1002/bjd.5090
Delaney, C.P., Senagore, A.J., Viscusi, E.R., Wolff, B.G., Fort, J., Du, W., Rao, W., Zhang, X., Zhang, J., Yan, R., Hu, Z., & Wang, Q. (2011). The
. . . Wallin, B. (2006). Postoperative upper and lower gastrointesti- role of nasogastric tube in decompression after elective colon and
nal recovery and gastrointestinal morbidity in patients undergoing rectum surgery: A meta-analysis. International Journal of Colorectal
bowel resection: Pooled analysis of placebo data from 3 random- Disease, 26, 423–429.
ized controlled trials. American Journal of Surgery, 191, 315–319. Sagar, P.M., Kruegener, G., & MacFie, J. (1992). Nasogastric intuba-
doi:10.1016/j.amjsurg.2005.10.026 tion and elective abdominal surgery. British Journal of Surgery, 79,
Iwa, M., Matsushima, M., Nakade, Y., Pappas, T.N., Fujimiya, M., 1127–1131. doi:10.1002/bjs.1800791105
& Takahashi, T. (2006). Electroacupuncture at ST-36 accelerates Salimath, J., Jones, M.W., Hunt, D.L., & Lane, M.K. (2007). Com-
colonic motility and transit in freely moving conscious rats. Ameri- parison of return of bowel function and length of stay in patients
can Journal of Physiology Gastrointestinal and Liver Physiology, 290, undergoing laparoscopic versus open colectomy. Journal of the
285–292. doi:10.1152/ajpgi.00068.2005 Society of Laparoendoscopic Surgeons, 11, 72–75.
Kharkevich, D.A., & Churukanov, V.V. (1999). Pharmacological regu- Shiotani, A., Tatewaki, M., Hoshino, E., & Takahashi, T. (2004). Ef-
lation of descending cortical control of the nociceptive processing. fects of electroacupuncture on gastric myoelectrical activity in
European Journal of Pharmacology, 375(1–3), 121–131. healthy humans. Neurogastroenterology and Motility, 16, 293–298.
Lee, J.H., Hyung, W.J., & Noh, S.H. (2002). Comparison of gastric doi:10.1111/j.1365-2982.2004.00504.x
cancer surgery with versus without nasogastric decompression. Takahashi, T. (2006). Acupuncture for functional gastrointestinal
Yonsei Medical Journal, 43, 451–456. disorders. Journal of Gastroenterology, 41, 408–417.
Liu, F.L., Lin, J.J., Ye, F., & Teng, L.S. (2010). Hand-assisted laparo- Vermeulen, H., Storm-Versloot, M.N., Busch, O.R.C., & Ubbink, D.T.
scopic surgery versus the open approach in curative resection of (2006). Nasogastric intubation after abdominal surgery: A meta-
rectal cancer. Journal of International Medical Research, 38, 916–922. analysis of recent literature. Archives of Surgery, 141, 307–314.
Ma, H.W., Chang, M.L., & Lin, C.J. (2007). A systematic review of Wilson, J.P. (1975). Postoperative motility of the large intestine in
acupressure for the application on nursing practice. Journal of man. Gut, 16, 689–692.
Nursing, 54(4), 35–44. Wolff, B.G., Pembeton, J.H., van Heerden, J.A., Beart, R.W., Jr., Nivat-
Manning, B.J., Winter, D.C., McGreal, G., Kirwan, W.O., & Redmond, vongs, S., Devine, R.M., . . . Ilstrup, D.M. (1989). Elective colon and
H.P. (2001). Nasogastric intubation causes gastroesophageal reflux rectal surgery without nasogastric decompression. A prospective,
in patients undergoing elective laparotomy. Surgery, 130, 788–791. randomized trial. Annals of Surgery, 209, 673–675.
doi:10.1067/msy.2001.116029 Yang, Z., Zheng, Q., & Wang, Z. (2008). Meta-analysis of the need for
Meng, Z.Q., Garcia, M.K., Chiang, J.S., Peng, H.T., Shi, Y.Q., Fu, J., nasogastric or nasojejunal decompression after gastrectomy for
. . . Cohen, L. (2010). Electro-acupuncture to prevent prolonged gastric cancer. British Journal of Surgery, 95, 809–816. doi:10.1002/
postoperative ileus: A randomized clinical trial. World Journal of bjs.6198
Gastroenterology, 16(1), 104–111. doi:10.3748/wjg.v16.i1.104 Yu, F., Takahashi, T., Moriya, J., Kawaura, K., Yamakawa, J., Kusaka,
Ming, J.L., Kuo, B.I., Lin, J.G, & Lin, L.C. (2003). The efficacy of K., . . . Kanda, T. (2006). Traditional Chinese medicine and Kampo:
acupressure to prevent nausea and vomiting in post-operative A review from the distant past for the future. Journal of International
patients. Journal of Advanced Nursing, 39, 343–351. Medical Research, 34, 231–239.
E68 Vol. 40, No. 2, March 2013 • Oncology Nursing Forum
View publication stats
You might also like
- EVALUATION OF THE INFLUENCE OF TWO DIFFERENT SYSTEMS OF ANALGESIA AND THE NASOGASTRIC TUBE ON THE INCIDENCE OF POSTOPERATIVE NAUSEA AND VOMITING IN CARDIAC SURGERYFrom EverandEVALUATION OF THE INFLUENCE OF TWO DIFFERENT SYSTEMS OF ANALGESIA AND THE NASOGASTRIC TUBE ON THE INCIDENCE OF POSTOPERATIVE NAUSEA AND VOMITING IN CARDIAC SURGERYNo ratings yet
- Effect of Early Physical Therapy Interventions On Post-Operative Ileus Following Abdominal HysterectomyDocument4 pagesEffect of Early Physical Therapy Interventions On Post-Operative Ileus Following Abdominal HysterectomyririnNo ratings yet
- 1 s2.0 S0965229915000552 MainDocument8 pages1 s2.0 S0965229915000552 MainUtami DewiNo ratings yet
- Gum Chewing SurgeryDocument3 pagesGum Chewing SurgeryTony YuliantoNo ratings yet
- Jurnal Pemulihan Fungsi Kandung Kemih Pasca PembedahanDocument20 pagesJurnal Pemulihan Fungsi Kandung Kemih Pasca Pembedahananra setiasariNo ratings yet
- hmg0tcDocument10 pageshmg0tcBruno GonçalvesNo ratings yet
- Periop UrologyKoubaartikelDocument4 pagesPeriop UrologyKoubaartikeljustin_saneNo ratings yet
- Manual Therapy: Hsiu-Chuan Hung, Sheng-Mou Hsiao, Shu-Yun Chih, Ho-Hsiung Lin, Jau-Yih TsauoDocument7 pagesManual Therapy: Hsiu-Chuan Hung, Sheng-Mou Hsiao, Shu-Yun Chih, Ho-Hsiung Lin, Jau-Yih TsauoSara AguiarNo ratings yet
- Pre-Op NPO and Traditional Post-Op Diet Advancement: Time To Move OnDocument7 pagesPre-Op NPO and Traditional Post-Op Diet Advancement: Time To Move OnDaru KristiyonoNo ratings yet
- Postoperative Paralytic IleusDocument9 pagesPostoperative Paralytic IleusazisaaiNo ratings yet
- TAP BlockDocument5 pagesTAP BlockclaucardemilNo ratings yet
- WJS GastrografinDocument12 pagesWJS Gastrografinkelly_ann23No ratings yet
- Perioperative Fasting: A Time To Relook: Guest EditorialDocument2 pagesPerioperative Fasting: A Time To Relook: Guest EditorialIbraim CervantesNo ratings yet
- El Bandrawy342013BJMMR4005Document9 pagesEl Bandrawy342013BJMMR4005Mochamad ZulfanNo ratings yet
- Efficay TAP Block PDFDocument5 pagesEfficay TAP Block PDFMarius PapuricaNo ratings yet
- Gastro Graf inDocument12 pagesGastro Graf inquileuteNo ratings yet
- Effect of I Love You (ILU) Massage On Rehabilitation of Children Digestive Function Postoperative StomachDocument7 pagesEffect of I Love You (ILU) Massage On Rehabilitation of Children Digestive Function Postoperative StomachYustian PaleriNo ratings yet
- Effect of I Love You (ILU) Massage On Rehabilitation of Children Digestive Function Postoperative StomachDocument7 pagesEffect of I Love You (ILU) Massage On Rehabilitation of Children Digestive Function Postoperative StomachSufi NurkhairunnisaNo ratings yet
- Pi Is 1743919114008735Document3 pagesPi Is 1743919114008735Firman FajriNo ratings yet
- A Myth About Anastomotic LeakDocument3 pagesA Myth About Anastomotic LeakAvinash RoyNo ratings yet
- A Comparison of Two PFMT Programs in Females With Stress Urinary IncontineneceDocument11 pagesA Comparison of Two PFMT Programs in Females With Stress Urinary Incontinenecemenna lNo ratings yet
- A Study of Intragastric and Intravesicular Pressure Changes During Rest, Coughing, Weight Lifting, Retching, and VomitingDocument5 pagesA Study of Intragastric and Intravesicular Pressure Changes During Rest, Coughing, Weight Lifting, Retching, and VomitingBelen GuzmanNo ratings yet
- Effects of Pelvic Floor Muscle Training Combined With Estriol On Pelvic Floor Dysfunction After Total Hysterectomy Applied in PerimenopauseDocument6 pagesEffects of Pelvic Floor Muscle Training Combined With Estriol On Pelvic Floor Dysfunction After Total Hysterectomy Applied in PerimenopauseChoirul AkbarNo ratings yet
- Anterior Vaginal Wall Reconstruction: Anterior Colporrhaphy Reinforced With Tension Free Vaginal Tape Underneath Bladder BaseDocument5 pagesAnterior Vaginal Wall Reconstruction: Anterior Colporrhaphy Reinforced With Tension Free Vaginal Tape Underneath Bladder BaseMarkoNo ratings yet
- Postoperative Oral Feeding After Cesarean Section-Early Versus Late Initiation: A Prospective Randomized TrialDocument5 pagesPostoperative Oral Feeding After Cesarean Section-Early Versus Late Initiation: A Prospective Randomized Trialjustin_saneNo ratings yet
- Effect of Pelvic-Floor Re-Education On Duration and Degree of Incontinence After Radical Prostatectomy: A Randomised Controlled TrialDocument5 pagesEffect of Pelvic-Floor Re-Education On Duration and Degree of Incontinence After Radical Prostatectomy: A Randomised Controlled Trialpalomachagas1986No ratings yet
- International Journal of Surgery: Emma J. Noble, Ros Harris, Ken B. Hosie, Steve Thomas, Stephen J. LewisDocument6 pagesInternational Journal of Surgery: Emma J. Noble, Ros Harris, Ken B. Hosie, Steve Thomas, Stephen J. LewisChristopher AdhisasmitaNo ratings yet
- Fast-Track Recovery Programme After Pancreatico-Duodenectomy Reduces Delayed Gastric EmptyingDocument7 pagesFast-Track Recovery Programme After Pancreatico-Duodenectomy Reduces Delayed Gastric EmptyinghoangducnamNo ratings yet
- Committee Opinion: Onabotulinumtoxina and The BladderDocument4 pagesCommittee Opinion: Onabotulinumtoxina and The Bladderw yNo ratings yet
- Chewing Gum PDFDocument5 pagesChewing Gum PDFIndriHariMurtiNo ratings yet
- JCDR 10 QCmmju11Document4 pagesJCDR 10 QCmmju11Walaa AbuzaidNo ratings yet
- PIIS2405456922002619Document7 pagesPIIS2405456922002619Oriol Colet GuitertNo ratings yet
- Usefulness of Gum Chewing To Decrease Postoperative Ileus in Colorectal Surgery With Primary Anastomosis: A Randomized Controlled TrialDocument5 pagesUsefulness of Gum Chewing To Decrease Postoperative Ileus in Colorectal Surgery With Primary Anastomosis: A Randomized Controlled TrialTay LiMinNo ratings yet
- Early Feeding After Digestive Surgery Is 43f243f3Document4 pagesEarly Feeding After Digestive Surgery Is 43f243f3sarahsamaliaNo ratings yet
- Postoperative Ileus: UCSF Postgraduate Course in General Surgery Maui, HI March 20, 2011Document10 pagesPostoperative Ileus: UCSF Postgraduate Course in General Surgery Maui, HI March 20, 2011Dhenbagoes Dama DewantoroNo ratings yet
- Riginal Research: LucasDocument11 pagesRiginal Research: Lucas'fanny Quenhita'No ratings yet
- 6 Incontinencia PDFDocument6 pages6 Incontinencia PDFAngelica CoronaNo ratings yet
- Li 2018Document7 pagesLi 2018Thu TranNo ratings yet
- Acup Utk TonsiltektomiDocument7 pagesAcup Utk Tonsiltektominewanda1112No ratings yet
- Complementary Therapies in Clinical PracticeDocument7 pagesComplementary Therapies in Clinical PracticeAsriyani HamidNo ratings yet
- Preventing Paralytic Ileus: Can The Anesthesiologist Help e A.M. FDocument8 pagesPreventing Paralytic Ileus: Can The Anesthesiologist Help e A.M. FVina TandiariNo ratings yet
- Chapter No# 1: Definition of Cesarean SectionDocument27 pagesChapter No# 1: Definition of Cesarean SectionRabiaNo ratings yet
- 468 2715 1 PBDocument8 pages468 2715 1 PBPutri NabilahNo ratings yet
- NZJP Volume 47 Number 2 02Document10 pagesNZJP Volume 47 Number 2 02Suman DeyNo ratings yet
- When To Feed Animals Post Surgery ArticleDocument6 pagesWhen To Feed Animals Post Surgery Articleariadne.georgiou.91No ratings yet
- Effectiveness of Standard Nursing Care With Gum Chewing To Reduce Bowel Ileus in Post-Operative Gynecologic Patients Randomized Controlled TrialsDocument8 pagesEffectiveness of Standard Nursing Care With Gum Chewing To Reduce Bowel Ileus in Post-Operative Gynecologic Patients Randomized Controlled TrialsdetrikaNo ratings yet
- Postoperative Ileus Strategies For ReductionDocument6 pagesPostoperative Ileus Strategies For Reductionon miniNo ratings yet
- Pengaruh Mobilisasi Dini Terhadap Waktu Pemulihan Peristaltik Usus Pada Pasien Pasca Operasi Abdomen Di Ruang Icu Bprsud Labuang Baji Makassar Stefanus Mendes KiikDocument8 pagesPengaruh Mobilisasi Dini Terhadap Waktu Pemulihan Peristaltik Usus Pada Pasien Pasca Operasi Abdomen Di Ruang Icu Bprsud Labuang Baji Makassar Stefanus Mendes KiikWahyu WijayaNo ratings yet
- Ebn CADocument7 pagesEbn CASarah Mae SinceroNo ratings yet
- Articulo de HombroDocument8 pagesArticulo de HombroYesenia OchoaNo ratings yet
- 2013 - Y R Silva - Doestheadditionofdeepbreathingexercisestophysiothe (Retrieved-2016-12-10)Document7 pages2013 - Y R Silva - Doestheadditionofdeepbreathingexercisestophysiothe (Retrieved-2016-12-10)wgNo ratings yet
- Improvement and Effect of Stress Responses and Ovarian Reserve Function in Patients With Ovarian Cysts After Laparoscopic SurgeryDocument11 pagesImprovement and Effect of Stress Responses and Ovarian Reserve Function in Patients With Ovarian Cysts After Laparoscopic SurgerymadilaNo ratings yet
- 01 HepatogastroDocument3 pages01 Hepatogastroyacine26No ratings yet
- 1 s2.0 S0004951405700210 MainDocument9 pages1 s2.0 S0004951405700210 Mainjavier garzonNo ratings yet
- Parrish April 2016Document9 pagesParrish April 2016neiris lopezNo ratings yet
- Implementation of A Urogynecology-Specific EnhancedDocument10 pagesImplementation of A Urogynecology-Specific EnhancedangelinputriNo ratings yet
- Jurnal Iqlima Alvein N (1401460042)Document10 pagesJurnal Iqlima Alvein N (1401460042)iqlima nafiisahNo ratings yet
- Complementary Therapies in Clinical PracticeDocument7 pagesComplementary Therapies in Clinical PracticeChetan AmberkarNo ratings yet
- The Effects of Bladder Training On Bladder Functions After Transurethral Resection of ProstateDocument21 pagesThe Effects of Bladder Training On Bladder Functions After Transurethral Resection of Prostatetrisna workNo ratings yet
- Pengaruh Mobilisasi Dini Terhadap Waktu Pemulihan Peristaltik Usus Pada Pasien Pasca Operasi Abdomen Di Ruang Icu BPRSUD Labuang Baji MakassarDocument9 pagesPengaruh Mobilisasi Dini Terhadap Waktu Pemulihan Peristaltik Usus Pada Pasien Pasca Operasi Abdomen Di Ruang Icu BPRSUD Labuang Baji MakassarSukma RahmayantiNo ratings yet
- HRZE (Kid's Kit), Toradol, CiprobayDocument4 pagesHRZE (Kid's Kit), Toradol, CiprobayiloveanneNo ratings yet
- NCP For CholecystitisDocument9 pagesNCP For Cholecystitisjmravago220% (1)
- Introduction To PharmacologyDocument119 pagesIntroduction To PharmacologyYzel Vasquez AdavanNo ratings yet
- Perioperative Care For CABG PatientsDocument32 pagesPerioperative Care For CABG PatientsAya EyadNo ratings yet
- Ama Painmgmt m6Document12 pagesAma Painmgmt m6Palakshi GoudaNo ratings yet
- Post Operative Pain Management in Paediatric Patients: Dr. R. P. GehdooDocument9 pagesPost Operative Pain Management in Paediatric Patients: Dr. R. P. GehdooT RonaskyNo ratings yet
- Unit V NSAIDsDocument7 pagesUnit V NSAIDsMriganka KarmakarNo ratings yet
- Stages of General AnesthesiaDocument8 pagesStages of General Anesthesiaamier90No ratings yet
- Drug Card ToradolDocument2 pagesDrug Card ToradolAdrianne Bazo100% (1)
- Final NcarDocument47 pagesFinal NcarLeixter Win BalingaoNo ratings yet
- Obat ObgynDocument8 pagesObat ObgynMuhammad Naqiuddin JalaluddinNo ratings yet
- Jurnal AnalgesikDocument7 pagesJurnal AnalgesikAnung IndrasNo ratings yet
- Analgesic in Oral SurgeryDocument24 pagesAnalgesic in Oral SurgeryPushpa KumariNo ratings yet
- Nepafenac An Ophthalmic Nonsteroidal Antiinflammatory DrugDocument6 pagesNepafenac An Ophthalmic Nonsteroidal Antiinflammatory DrugLalo ZaraloNo ratings yet
- N A - D (Nsaid) : Onsteroidal NTI Inflammatory Rugs SDocument43 pagesN A - D (Nsaid) : Onsteroidal NTI Inflammatory Rugs STes B FourieNo ratings yet
- Acute Gatritis With Dehydration: Wesleyan University - Philippines College of Nursing and Allied Medical SciencesDocument15 pagesAcute Gatritis With Dehydration: Wesleyan University - Philippines College of Nursing and Allied Medical SciencesKate QuibanNo ratings yet
- Drug Study (Romel) Feb 1&2 - Ventura PDFDocument4 pagesDrug Study (Romel) Feb 1&2 - Ventura PDFJian VenturaNo ratings yet
- NPLEX Combination Review Neurology - C: Paul S. Anderson, ND Medical Board Review ServicesDocument46 pagesNPLEX Combination Review Neurology - C: Paul S. Anderson, ND Medical Board Review ServicesValeria AcevedoNo ratings yet
- Pharmacy Guide Vancuver ParalympicDocument146 pagesPharmacy Guide Vancuver ParalympicVsevolod BentsianovNo ratings yet
- NCP Background, Demographic Data, Dordon's Functional Health, Drug Study SAint Louis UniversityDocument21 pagesNCP Background, Demographic Data, Dordon's Functional Health, Drug Study SAint Louis Universitypa3kmedinaNo ratings yet
- Drug StudyDocument4 pagesDrug StudyJeboy SadioaNo ratings yet
- Diagnosis and Acute Management of Suspected Nephrolithiasis in Adults - UpToDateDocument44 pagesDiagnosis and Acute Management of Suspected Nephrolithiasis in Adults - UpToDateManu Luciano100% (1)
- Drug StudyDocument10 pagesDrug StudyCieLouie Cauilan-DomingoNo ratings yet
- Drug StudyDocument16 pagesDrug StudygabbyNo ratings yet
- Name of DrugDocument6 pagesName of DrugKathleen ColinioNo ratings yet
- JIMENEZKaycelyn-Drus StudyDocument11 pagesJIMENEZKaycelyn-Drus Studykaycelyn jimenezNo ratings yet
- Midyr Case Study NewDocument18 pagesMidyr Case Study NewAndres Ham Samson BernabeNo ratings yet
- Acute Pain Questions - LathaDocument5 pagesAcute Pain Questions - LathaNishanth yedavalliNo ratings yet
- Ketorolac (Systemic) - Drug Information - UpToDateDocument42 pagesKetorolac (Systemic) - Drug Information - UpToDateJosué Pablo Chicaiza AbadNo ratings yet
- Post Op Pain ManagementDocument42 pagesPost Op Pain ManagementMuhammad Iqbal A GhaniNo ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (403)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (80)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (23)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (5)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- 12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosFrom Everand12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosRating: 4.5 out of 5 stars4.5/5 (207)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- Algorithms to Live By: The Computer Science of Human DecisionsFrom EverandAlgorithms to Live By: The Computer Science of Human DecisionsRating: 4.5 out of 5 stars4.5/5 (722)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningFrom EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningRating: 4 out of 5 stars4/5 (3)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (1)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)