Professional Documents
Culture Documents
Adequate Thromboprophylaxis Un Critically Ill Patients
Adequate Thromboprophylaxis Un Critically Ill Patients
Uploaded by
Carolina RamirezOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Adequate Thromboprophylaxis Un Critically Ill Patients
Adequate Thromboprophylaxis Un Critically Ill Patients
Uploaded by
Carolina RamirezCopyright:
Available Formats
Levi Critical Care 2010, 14:142
http://ccforum.com/content/14/2/142
CO M M E N TA R Y
Adequate thromboprophylaxis in critically ill patients
Marcel Levi*
See related research by Robinson et al., http://ccforum.com/content/14/2/R41
limited bioavailability (that is, lower plasma anti-factor
Abstract
Xa activity) of subcutaneously administered heparin in
Venous thromboembolism is a relatively frequently those patients with impaired peripheral circulation, due
occurring complication in critically ill patients admitted to vasopressor medication to maintain central blood
to the ICU despite prophylactic treatment with pressure, might be important. Indeed, in a first
subcutaneous low molecular weight heparin. Several comparative trial it was shown that critically ill patients
studies show that critically ill patients have significantly on high dose vasopressor medication had much lower
lower plasma anti-factor-Xa activity levels compared to anti-factor Xa concentrations after the subcutaneous
control patients after administration of subcutaneous administration of LMW heparin in comparison with
heparin. Robinson and colleagues show in this issue of intensive care patients that had lower doses of vaso-
Critical Care dose-dependent but relatively low levels of pressor or in comparison with patients in the surgical
anti-factor Xa activity at increasing doses of enoxaparin. ward [3]. A subsequent study also found consistently
Anti-factor Xa levels thought to be required for lower anti-factor Xa levels after subcutaneous heparin in
adequate thromboprophylaxis are observed only at critically ill patients [4]. In another similar study, critically
doses of enoxaparin that are one and a half times ill patients with excessive subcutaneous oedema had
higher than the conventional dose (40 mg). lower anti-factor Xa concentrations compared to a
control group without oedema [5]. This observation was
confirmed in a group of critically ill multiple trauma
In this issue of Critical Care, Robinson and colleagues [1] patients, who showed variable and low heparin concen-
investigate the effect of increasing doses of the low mole- trations after subcutaneous injections [6].
cular weight (LMW) heparin enoxaparin (commonly Robinson and colleagues [1] compared plasma anti-
used as prophylaxis against venous thromboembolism factor Xa levels after the subcutaneous administration of
(VTE)) on systemic heparin concentrations, expressed as the LMW heparin enoxaparin at the conventional dose
anti-factor Xa levels. VTE is a common complication in (40 mg) and at increasingly higher doses (up to 70 mg) in
critically ill patients. Reported rates for deep venous intensive care patients. They found a dose-dependent
thrombosis in patients admitted to the ICU range from increase in peak anti-factor Xa levels (4 hours after the
22 to 80% depending on patient characteristics. injection) ranging from 0.13 IU/ml at the conventional
Thromboprophylaxis with unfractionated or LMW 40 mg dose to 0.29 IU/ml at the 70 mg dose. Considering
heparin lowers the risk for deep venous thrombosis by that optimal efficacy and safety of LMW heparin for
more than 50% [2]. Nevertheless, the risk of VTE in thromboprophylaxis in orthopaedic and abdominal
critically ill patients receiving LMW heparin prophylaxis surgery was achieved with dosages of heparin resulting in
is still much higher than in other patient groups. peak plasma anti-factor Xa activities ranging between
Amongst several factors that may explain the higher 0.25 and 0.30 IU/ml [7], it may be concluded that
incidence of VTE in critically ill patients, such as full critically ill patients need much higher doses of LMW
immobilisation or withholding anticoagulant prophylaxis heparin than other patients. Based on the findings of
because of a high bleeding risk, it was hypothesized that Robinson and colleagues, the subcutaneous dose of
LMW heparin should be increased to 60 mg daily.
Alternatively, direct intravenous administration of
*Correspondence: m.m.levi@amc.uva.nl
Department of Vascular Medicine and Internal Medicine, Academic Medical
(LMW) heparin may be considered; however, experience
Center, University of Amsterdam, Meibergdreef 9, 1105 AZ Amsterdam, with this type of thromboprophylaxis is limited.
The Netherlands The mechanism by which critically ill patients have
lower anti-factor Xa levels after subcutaneous adminis-
© 2010 BioMed Central Ltd © 2010 BioMed Central Ltd tration of heparin is not completely understood. The
Levi Critical Care 2010, 14:142 Page 2 of 2
http://ccforum.com/content/14/2/142
initial hypothesis was that patients on high dose Competing interests
vasopressor medication had impaired subcutaneous The author declares that he has no competing interests.
blood flow and thereby limited ability to adsorb the Published: 21 April 2010
subcutaneous heparin [3]. An alternative explanation is
that the presence of oedema hinders the absorption of References
1. Robinson S, Zincuk A, Strøm T, Larsen TB, Rasmussen B, Toft P: Enoxaparin,
heparin, although that hypothesis was not proven [5]. In effective dosage for intensive care patients: double-blinded, randomised
addition, it has been suggested that systemic inflamma- clinical trial. Crit Care 2010, 14:R41.
tion and associated multiple organ dysfunction may have 2. Cook DJ, Crowther MA: Thromboprophylaxis in the intensive care unit:
focus on medical-surgical patients. Crit Care Med 2010, 38:S76-S82.
an impact on heparin binding to plasma proteins and 3. Dörffler-Melly J, de Jonge E, Pont AC, Meijers J, Vroom MB, Büller HR, Levi M:
drug metabolism [8]. Bioavailability of subcutaneous low-molecular-weight heparin to patients
The clinical relevance of lower anti-factor Xa levels on vasopressors. Lancet 2002, 359:849-850.
4. Priglinger U, Delle Karth G, Geppert A, Joukhadar C, Graf S, Berger R,
after conventional doses of (LMW) heparin in critically Hülsmann M, Spitzauer S, Pabinger I, Heinz G: Prophylactic anticoagulation
ill patients is also not totally clear. Theoretically, the low with enoxaparin: Is the subcutaneous route appropriate in the critically ill?
anti-factor Xa levels may lead to suboptimal prophylaxis Crit Care Med 2003, 31:1405-1409.
5. Rommers MK, Van der Laan N, Egberts TC, van den Bemt PM: Anti-Xa activity
and could indeed be a contributory factor to the higher after subcutaneous administration of dalteparin in ICU patients with and
incidence of thromboembolic complications in critically without subcutaneous oedema: a pilot study. Crit Care 2006, 10:R93.
ill patients despite routine thromboprophylaxis. How- 6. Haas CE, Nelsen JL, Raghavendran K, Mihalko W, Beres J, Ma Q, Forrest A:
Pharmacokinetics and pharmacodynamics of enoxaparin in multiple
ever, this has never been demonstrated in a clinical study. trauma patients. J Trauma 2005, 59:1336-1343; discussion 1343-1344.
Based on the observations of Robinson and colleagues 7. Leyvraz PF, Bachmann F, Hoek J, Büller HR, Postel M, Samama M, Vandenbroek
and others, a randomized controlled trial with conven- MD: Prevention of deep vein thrombosis after hip replacement:
randomised comparison between unfractionated heparin and low
tional versus higher doses of thrombosis prophylaxis in molecular weight heparin. BMJ 1991, 303:543-548.
critically ill patients aiming at the reduction of the 8. Mayr AJ, Dünser M, Jochberger S, Fries D, Klingler A, Joannidis M, Hasibeder
incidence of VTE and other clinically relevant outcomes W, Schobersberger W: Antifactor Xa activity in intensive care patients
receiving thromboembolic prophylaxis with standard doses of
is justified. Such a study would also enable the evaluation
enoxaparin. Thromb Res 2002, 105:201-204.
of bleeding complications related to the administration of 9. Levi MM, Eerenberg E, Lowenberg E, Kamphuisen PW: Bleeding in patients
prophylactic heparin, as intensive care patients are at using new anticoagulants or antiplatelet agents: risk factors and
higher risk for hemorrhage as well [9,10]. management. Neth J Med 2010, 68:68-76.
10. Cook D, Douketis J, Meade M, Guyatt G, Zytaruk N, Granton J, Skrobik Y, Albert
In summary, there is ample evidence that conventional M, Fowler R, Hebert P, Pagliarello G, Friedrich J, Freitag A, Karachi T, Rabbat C,
thromboprophylaxis leads to lower systemic heparin Heels-Ansdell D, Geerts W, Crowther M; Canadian Critical Care Trials Group:
levels in critically ill patients. It is not clear whether this Venous thromboembolism and bleeding in critically ill patients with
severe renal insufficiency receiving dalteparin thromboprophylaxis:
contributes to the relatively high incidence of VTE in prevalence, incidence and risk factors. Crit Care 2008, 12:R32.
intensive care patients. A clinical trial evaluating higher
doses of heparin for prevention of VTE and assessing the
bleeding risk of such an approach is justified. doi:10.1186/cc8949
Cite this article as: Levi M: Adequate thromboprophylaxis in critically ill
Abbreviations patients. Critical Care 2010, 14:142.
LMW = low molecular weight; VTE = venous thromboembolism.
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (842)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5807)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1091)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (346)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Project Risk Management Guide: Part I: Guidance For WSDOT Projects Part II: Guidelines For CRA-CEVP WorkshopsDocument132 pagesProject Risk Management Guide: Part I: Guidance For WSDOT Projects Part II: Guidelines For CRA-CEVP WorkshopsGnamaSayaNo ratings yet
- Kings Applied Neuroscience Course BrochureDocument9 pagesKings Applied Neuroscience Course BrochureImg UsmleNo ratings yet
- Syll4stud CPE104 FacilitatingDocument2 pagesSyll4stud CPE104 FacilitatingMark neil a. Galut100% (1)
- Above 80 Age Not Vaccinated DetailsDocument9 pagesAbove 80 Age Not Vaccinated DetailsSimbakutty VenkataramananNo ratings yet
- Javma-Javma 21 04 0213Document5 pagesJavma-Javma 21 04 0213Black manNo ratings yet
- SAI AFI Online Coaching Course Microcycle PlanningDocument27 pagesSAI AFI Online Coaching Course Microcycle PlanningMazid MubaraqNo ratings yet
- Rapid Damage Assestments Report 2021Document2 pagesRapid Damage Assestments Report 2021Vin XhyneNo ratings yet
- Boiser, Klein Xavier: Giving Validation Boost Self-Confidence and Reciprocates Self-CareDocument1 pageBoiser, Klein Xavier: Giving Validation Boost Self-Confidence and Reciprocates Self-CareKlein Xavier BoiserNo ratings yet
- Space Travel Thesis StatementDocument8 pagesSpace Travel Thesis Statementohbmogxff100% (1)
- Psychophysiologic Effects of Hatha Yoga On Musculoskeletal and Cardiopulmonary Function: A Literature ReviewDocument17 pagesPsychophysiologic Effects of Hatha Yoga On Musculoskeletal and Cardiopulmonary Function: A Literature ReviewNi Made Wirastuti ShantiNo ratings yet
- Preterm LaborDocument29 pagesPreterm LaborBer AnneNo ratings yet
- Community Health Information Tracking System: Submitted By: Gerna Maie Anne CabilingDocument5 pagesCommunity Health Information Tracking System: Submitted By: Gerna Maie Anne CabilingRammiel Saylo CarlosNo ratings yet
- Personal Finance Canadian 2nd Edition Madura Test BankDocument48 pagesPersonal Finance Canadian 2nd Edition Madura Test Bankannabellaauroravb5cf100% (22)
- SDS - 80214 - Sto Flexible Crack Filler - ENDocument6 pagesSDS - 80214 - Sto Flexible Crack Filler - ENMichael A FarinNo ratings yet
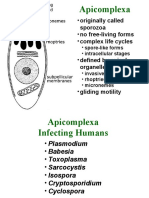
- Apicomplexa: - Originally Called - No Free-Living Forms - Complex Life Cycles - Defined by ApicalDocument19 pagesApicomplexa: - Originally Called - No Free-Living Forms - Complex Life Cycles - Defined by ApicalYota MahmoudNo ratings yet
- Gonorrhea Case StudyDocument2 pagesGonorrhea Case StudyDonna LLerandi100% (1)
- Culturally Competent Practice: A Framework For Understanding Diverse GroupsDocument75 pagesCulturally Competent Practice: A Framework For Understanding Diverse GroupsSiti BadriahNo ratings yet
- President Uhuru Kenyatta Makes New AppointmentsDocument40 pagesPresident Uhuru Kenyatta Makes New AppointmentsGerald GekaraNo ratings yet
- Data AnalysisDocument9 pagesData AnalysisSayid hasan joarderNo ratings yet
- Phillips Hmo Enrollee Subscription FormDocument2 pagesPhillips Hmo Enrollee Subscription FormJack EzehNo ratings yet
- Star Health Premium Chart Jan-23Document45 pagesStar Health Premium Chart Jan-23Star HealthNo ratings yet
- NCP Chronic Renal FailureDocument15 pagesNCP Chronic Renal FailureNurul BariyyahNo ratings yet
- Lab Report 5 EtDocument18 pagesLab Report 5 EtPeach BabyNo ratings yet
- Pharma 4th YearDocument10 pagesPharma 4th YearSchooch NibblleNo ratings yet
- Camouflage Therapy: Victoria L. RaynerDocument4 pagesCamouflage Therapy: Victoria L. RaynerTushar SoniNo ratings yet
- Pharmacology A Patient Centered Nursing Process Approach 8th Edition Kee Test BankDocument6 pagesPharmacology A Patient Centered Nursing Process Approach 8th Edition Kee Test Bankselinadu4in1100% (23)
- BWwinter2023-6 Economy and EAEUDocument35 pagesBWwinter2023-6 Economy and EAEULiliaNo ratings yet
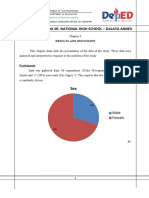
- Licerio Antiporda Sr. National High School - Dalaya Annex: Results and DiscussionDocument6 pagesLicerio Antiporda Sr. National High School - Dalaya Annex: Results and Discussionadrianpaul villenaNo ratings yet
- Butner LawsuitDocument71 pagesButner LawsuitLeigh TaussNo ratings yet
- Research Paper On Emotional StabilityDocument8 pagesResearch Paper On Emotional Stabilityegw48xp5100% (1)