Professional Documents
Culture Documents
Modeling and Prediction of Outcome For The Superovulation Stage in in Vitro Fertilization Jfiv.1000122
Uploaded by
Reni ReniOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Modeling and Prediction of Outcome For The Superovulation Stage in in Vitro Fertilization Jfiv.1000122
Uploaded by
Reni ReniCopyright:
Available Formats
n: In Vit
atio
Journal of Fertilization: In vitro - IVF-Worldwide, Yenkie et al., JFIV Reprod Med Genet 2014, 2:2
ro
liz
rti
-IV
DOI: 10.4172/jfiv.1000122
al of Fe
F-Worldwide
Reproductive Medicine, Genetics & Stem Cell Biology
urn
Jo
ISSN: 2375-4508
Research Article
Modeling and Prediction of Outcome for the Superovulation Stage in In-
Vitro Fertilization (IVF)
Yenkie KM1,2, Diwekar UM1,2* and Bhalerao V3
1
Department of Bioengineering, University of Illinois, Chicago, IL 60607, USA
2
Center for Uncertain Systems: Tools for Optimization & Management (CUSTOM), Vishwamitra Research Institute, Clarendon Hills, IL 60514, USA
3
Jijamata Hospital, Nanded, Maharashtra, India
Abstract
Background: IVF is divided into four stages: superovulation, egg-retrieval, fertilization and embryo transfer.
The superovulation stage has specific protocols which include daily injections of hormones, decided by regular
monitoring and testing involving cost intensive methods like ultrasound, to enable multiple ovulations per menstrual
cycle. However, there is a lack of systematic planning and hormonal dosage prediction for successful superovulation
using apriori information.
Methods: This work aims at developing a systematic outcome projection method for superovulation based on
initial observations in an IVF cycle. The information about the size range and number of follicles was transformed to
moment based information using the mathematical approach from crystallization literature. The follicle growth was
modeled as a function of injected hormones and the properties of the follicles were represented in terms of moments.
The model parameters were estimated using the data obtained from initial two days of observation. This information
was used to project the follicle size distribution for the remaining cycle days.
Results and Conclusion: The model assumptions and its correlation to batch crystallization prove promising
on comparison of the simulated follicle size and number to the observed data for the patients. The model prediction
accuracy is determined by the statistical analysis of clinical data available for 50 superovulation cycles. Thus, it can
act as an indicator for the success or failure of the ongoing superovulation stage in the IVF cycle and the decision
whether to continue with the procedure or abandon it and start from donor eggs can be made, thus saving treatment
cost and time on unsuccessful attempts.
Keywords: Predictive model; Infertility; Moment; Follicle release periodic gametes (eggs/oocytes), produce steroid hormones;
estrogen and progesterone. The process of follicle maturation,
Introduction ovulation, corpus luteum formation and regression occurs repeatedly
Infertility is the inability of a couple to achieve conception or to and its cyclic nature is measured in weeks. Usually only one egg
bring a pregnancy to term after a year or more of regular, unprotected ovulates per menstrual cycle. This selection of the follicle which enters
intercourse. The World Health Organization (WHO) has estimated into the ovulatory stage is affected by several factors, discussed by Baird
that about 8-10% couples experience some form of infertility problems. [4]. The rise in Follicle Stimulating Hormone (FSH) level beyond a
The occurrence of infertility in male and female population is almost certain limit activates a single small follicle (2-4 mm diameter); this
identical. In most countries cost is a major hurdle in the access of follicle dominates over all the other follicles for growth and ultimately
infertility services. Most centers offering treatment for infertility operate enters the ovulatory phase. Multiple ovulations can be achieved by
outside the government financed health facilities. The treatment is only extending the period during which the level of FSH remains above the
accessible to elites who can afford to pay for such high tech therapies. threshold. This is known as widening the gate for multiple ovulations.
Even in a country like United States, the cost for an IVF cycle amounts Thus, regulation of FSH secretion plays the most important role in
to almost 20% the total annual income of a median American family. In determining ovulation and growth of the follicles. In our work, the
developing nations, this cost is about 50% of the total annual income model uses FSH dose in determining the kinetics for follicle growth.
[1,2]. The other hormones like Gonadotropin Releasing Hormone (GnRH),
Luteinizing Hormone (LH), estrogen, progesterone and human
In-vitro fertilization is a process by which oocytes or egg cells chorionic gonadotropin (hCG) also affect the phenomena, but their
are fertilized by a sperm outside the body in a laboratory simulating effect is negligible in comparison to FSH levels [5].
the similar conditions in the body and then the fertilized eggs or
embryos are implanted back in the uterus for full term pregnancy. Superovulation has specific protocols [5] to be followed and
Superovulation [3] is the first stage of IVF in which multiple eggs are
retrieved using drug induced stimulation of the ovaries. Major risks
involved in IVF treatment are failure to conceive, multiple pregnancies, *Corresponding author: Urmila M Diwekar, Center for Uncertain Systems: Tools
ectopic pregnancy, ovarian hyper stimulation syndrome. IVF is an for Optimization & Management (CUSTOM), Vishwamitra Research Institute,
expensive treatment. There are a lot of complications associated with Clarendon Hills, IL 60514, USA, Tel: (630)-886-3047; E-mail: urmila@vri-custom.org
each stage and hence the success rate is highly unpredictable. Also, Received January 29, 2014; Accepted April 27, 2014; Published April 27, 2014
the treatment strategies used are not modified according to the patient Citation: Yenkie KM, Diwekar UM, Bhalerao V (2014) Modeling and Prediction of
history. The success of IVF is primarily dependent on the quality and Outcome for the Superovulation Stage in In-Vitro Fertilization (IVF). JFIV Reprod
quantity of eggs or oocytes retrieved from the superovulation stage. Med Genet 2: 122. doi:10.4172/jfiv.1000122
Thus, superovulation is an important stage in the overall success of IVF. Copyright: © 2014 Yenkie KM, et al. This is an open-access article distributed
under the terms of the Creative Commons Attribution License, which permits
It is important to understand the actual functioning of the ovaries unrestricted use, distribution, and reproduction in any medium, provided the
in order to better understand the process of superovulation. The ovaries original author and source are credited.
JFIV Reprod Med Genet Volume 2 • Issue 2 • 1000122
ISSN: JFIV, an open access journal
Citation: Yenkie KM, Diwekar UM, Bhalerao V (2014) Modeling and Prediction of Outcome for the Superovulation Stage in In-Vitro Fertilization (IVF).
JFIV Reprod Med Genet 2: 122. doi:10.4172/jfiv.1000122
Page 2 of 8
includes daily injections of multiple agents from time durations The crystals can be separated into two classes based on the kinetics
varying in weeks to months. The protocols were developed to prevent [10,11] which cause their changes; (i) seed crystals - initially some
premature ovulation and control the hormonal levels. The ‘long crystals of the desired product are added to the solution. These crystals
protocol’ is the most widely used and it involves injection of GnRH are known as ‘seed’ and they follow the growth kinetics, (ii) due to
agonist that suppresses the endogenous functions of the ovary and the excessive supersaturation, new crystals are formed from the solution
release of FSH and LH [5-7]. GnRH agonists are injected daily from the which is due to the nucleation kinetics. Thus, moments can be separated
mid-luteal phase (usually the 21st day in a 28 day cycle) of the previous into seeded moments and nucleated moments. The generalized moment
menstrual cycle, until follicle maturation is triggered. The exogenous equations for the nucleated and seeded crystals as defined in literature
FSH is injected from the 1st day of the next cycle and is continued by Hu et al., [10] are;
for about 9 to 12 days depending upon the follicle growth until the
Moment equations for the nucleated crystals:
maturation is triggered on the final day using the hCG.
d µ0n
The expense of IVF increases due to high cost of medication and = B(t )
dt
frequent monitoring. The idea is to project the treatment response of G = k ∆C fshα (3)
the patient for the complete superovulation cycle by using initial two
Moment equations for seeded crystals:
day response which shall act as an indicator for the success or failure
of the cycle. In superovulation the multiple follicles with different µ0s = constant
sizes result into a Follicle Size Distribution (FSD). Since distributions
are more common in processes where the system properties can d µis (4)
= iG
= (t ) µis−1 (t ), i 1, 2,3
dt
be estimated by analyzing the representative distribution, we try to
correlate mathematical modeling of the superovulation process to one Thus, using the moment Eqs. (3) and (4), the complex Eq. (1) can
of the most extensively studied particulate process of crystallization [8]. be simplified and the mathematics of process modelling and control
Preliminary results of this model appeared recently in Yenkie et al. [9]. become easier.
Materials and Methods Model development
In batch crystallization, the aim is to get maximum number and
Batch crystallization
uniformity in crystal size and shape for all particles [11]. This correlates
Batch crystallization [8,10,11] is an industrial separation and well with the objective of superovulation [6,7], ‘to obtain multiple eggs of
purification process. The process objective is to enhance the product similar size and quality’. To emphasize the point an analogy is presented
quality defined in terms of its shape and size by maintaining certain in Table 1.
operating conditions. Maintenance of supersaturation condition is
an essential aspect in crystallization. Supersaturation is a condition The superovulation follicle growth model in general resembles
in which the solute concentration in the solution is higher than the greatly to the growth of seeded batch crystals. The aim of seeded batch
solubility at a particular temperature. Thus, controlling the process crystallization is to allow the seeds added to the solution to grow to
temperature can maintain the desired supersaturation levels and hence desired shape and size and truncate the process of nucleation by
enable the crystallization. maintaining certain process conditions. The number of seeds added to
the solution are constant and hence the zeroth moment of seeded batch
The crystalline particles are observed as a size distribution and the crystals which corresponds to its number is constant [10]. Similarly,
product purity is decided in terms of the size range of the crystals. Thus,
when we look at superovulation, the number of follicles activated
the particle size is modelled as population balance. The general form of
during an IVF cycle is constant. Thus, the moment models for both
the population balance [10] can be written as Eq. (1).
the processes remain the same. The growth term which is a function of
∂n( r, t ) ∂ (G ( r, t )n( r, t ) (1) process variables like temperature and supersaturation in seeded batch
+ B
=
∂t ∂r crystallization will become a function of medicinal dosage in case of
where, n is the number density distribution, t is time, r represents superovulation process.
characteristic dimension for size measurements, G is the crystal growth
The first four moments have a special significance [12] in terms
rate, B is the nucleation rate.
of the properties related to shape and size of the particles. The zeroth
Both growth and nucleation processes describe crystallization moment is a representative of the number of particles, first moment
kinetics and their expression may vary depending upon the system of the shape, etc. The information provided by these moments will
under consideration. This complex equation involving partial help in formulating a predictive model for superovulation. The desired
derivatives can be simplified into a set of ordinary differential equations outcomes for this stage can be specified mathematically in terms of the
by using the method of moments [12]. The nth moment of the particle moment values.
size distribution is defined as in Eq. (2).
Let us assume the activated number of follicles to be constant and
µi = ∫ r i n( r, t )dr
∞
(2) hence the zeroth moment corresponding to it shall also have a constant
0
Batch Crystallization Superovulation (IVF stage I)
Production of multiple crystals Production of multiple oocytes or eggs
Crystal quality is determined in terms of size distribution and purity Oocyte quality is determined in terms of no abnormalities, similar size.
The rate of crystallization or crystal growth varies with time and process conditions The rate of ovulation or oocyte growth varies with time and drug interactions
Process is affected by external variables like agitation, and process operating Process is affected by externally administered drugs and body conditions of the
variables like temperature, pressure, etc. patient undergoing the process
Table 1: Analogy between batch crystallization and IVF superovulation stage.
JFIV Reprod Med Genet Volume 2 • Issue 2 • 1000122
ISSN: JFIV, an open access journal
Citation: Yenkie KM, Diwekar UM, Bhalerao V (2014) Modeling and Prediction of Outcome for the Superovulation Stage in In-Vitro Fertilization (IVF).
JFIV Reprod Med Genet 2: 122. doi:10.4172/jfiv.1000122
Page 3 of 8
value. The data from a successful superovulation cycle in Table 2 shows d µ1 (8)
G ( t ) µ0 ( t )
that during FSH dosage regime, as time progresses the size of the dt
follicles increase. (9)
d µ2
= 2G (t ) µ1 (t )
Moment evaluation dt
Conversion of the data available on follicle number and size to d µ3 (10)
= 3G (t ) µ2 (t )
moments [12] using the Eq. (5). dt
=µi ∑ n ( r, t ) r
i i
i
∆ri (5) d µ4
= 4G (t ) µ3 (t ) (11)
where µi - ith moment, ni(r,t) - number of follicles in bin of mean dt
radius ‘r’ at time ‘t’, ri - mean radius of ith bin, Δr - range of radii variation
d µ5
in each bin. The moments evaluated are shown in Table 3. = 5G (t ) µ4 (t ) (12)
dt
Model equations
d µ6
= 6G (t ) µ5 (t )
The rate expression for follicle growth is dependent on FSH dt (13)
administered. Thus, we can write the growth term as in Eq. (6)
Solution method
G = k ∆C fshα (6)
We integrate the Eqs. (8) to (13) for predicting the kinetic constants
where G - growth term, ΔCfsh - amount of FSH injected, k, α - kinetic
in the follicle growth expression. Integrated equations for the moments
constants.
are shown in Eqs. (14) to (19):
Assuming moment model, we consider only the first seven
μ1 = Gμ0t + c1 (14)
moments; zeroth moment corresponding to follicle number, the first
moment corresponding to follicle size and the other 5 moments. The 1st μ2= G μ0t + 2Gc1t + c2
2 2
(15)
to 6th order moments are being used since they help in recovering the
μ3= G3μ0t3 + 3G2c1t2 +3Gc2t + c3 (16)
size distributions more precisely as against lower number of moments
[13]. It is essential to use 6 moments for recovering FSD since we μ4= G4μ0t4 + 4G3c1t3+ 6G2c2t2 +4Gc3t + c4 (17)
have divided the data into six size bins depending upon the size of the
follicles. μ5= G5μ0t5 + 5G4c1t4+ 10G3c2t3 + 10G2c3t2 +5Gc4t + c5 (18)
μ6 = G μ0t + 6G c1t + 15G c2t + 20G c3t +15G c4t + 6 Gc5t + c6 (19)
6 6 5 6 4 4 3 3 2 2
µ0 = constant (7)
Model validation
Number of Follicles The current moment model will predict the moment values, however
Size Bins(mm)
/Time Day 1 Day 5 Day 7 Day 9 our desired output is in the form of follicle size distribution, thus in
0-4 4 0 0 0 model validation the approach to obtain FSD from moment values is
4-8 12 0 0 0 shown. The method is adapted from the literature by Flood [13], where
8 - 12 8 17 1 0 he demonstrated a method to recover particle size distribution from
12 - 16 2 6 15 3 moments in crystallization. In this method the particle size distribution
16 - 20 0 3 10 15 is approximated using the inversion matrix, A shown in Table 4 along
20 - 24 0 0 0 8 with a non-linear constrained optimization technique. Moment
FSH dose (IU/ml) 150 75 75 75 (µ)=A.n, thus we can write
IU – International units used for hormonal dosage measurement n=A-1μ (20)
Table 2: Variation of follicle size (diameter) with time and FSH dose in Patient A.
Using the model predicted moment values we evaluate n(r,t) using
Time FSH the ‘follicle number prediction algorithm’ and compare with the actual
Sr. No μ1 μ1 μ2 μ3 μ1 μ5 μ6
(day) (IU/ml) data to check the model accuracy. The number of follicles in a particular
1. 1 52 188 820 4028 21556 123068 738100 150 size bin on a cycle day of FSH dosage regime can be evaluated by using
2. 5 52 308 1924 12740 89428 662228 5131684 75 an algorithm based on constrained optimization [9,14]. The decision
3. 7 52 400 3140 25120 204500 1691440 14189540 75 variables are the number of follicles in each bin per day in the cycle.
4. 9 52 488 4660 45224 445492 4449128 44994100 75 Thus, by using this follicle number prediction algorithm, the moment
Table 3: Experimental moments evaluated using Eq. (1). model for follicle growth can be validated for a given patient.
2 6 10 14 18 22
Predictive value of the model
2 18 50 98 162 242 If the changes in the follicle size associated with the administration
A = 2 54 250 686 1458 2662 of hormones are monitored for two days, we can evaluate all the
unknown parameters of the model. After evaluating them, the model
2 162 1250 4802 13122 29282
can then be used to project the outcome according to the hormonal
2 486 6250 33614 118098 322102
dosage on the successive days. The flowchart in Figure 1 shows the
2 1458 31250 235298 1062882 3543122 methodology for decision making regarding the continuation of the
Table 4: The inversion matrix A (6x6) to recover size distribution from moments. cycle or discontinuing it.
JFIV Reprod Med Genet Volume 2 • Issue 2 • 1000122
ISSN: JFIV, an open access journal
Citation: Yenkie KM, Diwekar UM, Bhalerao V (2014) Modeling and Prediction of Outcome for the Superovulation Stage in In-Vitro Fertilization (IVF).
JFIV Reprod Med Genet 2: 122. doi:10.4172/jfiv.1000122
Page 4 of 8
parameter estimation methods is quite close to the actual observations.
Thus, the assumption of the zeroth moment being the representative of
the number of follicles entering the growth stage proves reasonable as
suggested by Baird [4].
Using the parameter values in Table 5, the results for the next days
of the cycle were projected using the moment model. The moment
values for the successive cycle days were evaluated by using Eqs. (14)
to (19) and the parameter values estimated from the initial two day
data. The FSD was back predicted using the correlation given by Flood
[13] and the algorithm on follicle number prediction [9]. The results
for FSDs predicted from the parameters estimated using the initial two
day data as well as the complete data available for the patient A are
also shown in Figure 2. The smooth curve shows the predicted values,
while the discrete markers denote the actual follicle count. It is intuitive
that the fit will be better for the all-day data (complete data) fit for a
particular patient. It provides a check on the model accuracy as well as a
good comparative estimate against the two day data projections. In this
paper, all day data fitting and FSD predictions have always been used
as an additional standard along with the clinical observations available
from our collaborators for testing the claim, “two days of observation are
sufficient to project the outcome of the superovulation cycle”.
Along with the results reported for Patient - A, 49 more such
superovulation cycles was studied and their data for initial two days and
on all days was used to project the superovulation outcome based on
Parameter Values
µ0 53.2
k 10
α -0.66
c1 158.45
c2 590.39
Figure 1: Flowchart for prediction of successful superovulation. c3 2186.86
c4 21151.86
c5 11104.30
The follicle size measurements along with the FSH dosage for first
c6 100201.10
two days will provide us with the 1st to 6th moment values for initial
two days of observation. For projection of the FSD in the later days, we Table 5: Parameter values from the initial two day observation data:
need the enlisted parameter values to be evaluated from the available
data; k, α, µ0, c1, c2, c3, c4, c5, c6. Thus, we shall have 9 unknowns and 12
equations (two sets since we are using two day data). The 9 unknowns
are evaluated using the Eqs. (14) to (19) for the first two days. From
the parameter values and the moment model for the FSD the results
are projected for the remaining cycle days. The projected results
provide us with the idea about the success of the current cycle. If we
observe desired number of follicles within a particular size range so
as to retrieve them on the final day; the cycle can be continued with
the projected FSH dosage, otherwise it is advisable to discontinue the
ongoing cycle and start again. The patient and doctor can also decide to
start directly with donor eggs.
Results
Since we used the data for the initial two days observed, in this case
the data for day 1 and day 5 has been used for patient A (see columns
for day 1 and 5 in Table 2). Using this data the moments were evaluated
from Eq. 5 (see row (1) and (2) of Table 3). Substituting the moment
values along with the FSH doses in Eqs., (14) to (19), we had 12 equations
to be solved for estimating 9 model parameters. These equations were Figure 2: Predicted follicle size distribution using 2 day (S-2) and all day (S-all)
data for model fitting for Patient A (discrete markers ■ and are data points
solved in Matlab, and the parameter values obtained are listed in Table
and continuous curves are model predictions).
5. It can be seen that the value of the evaluated zeroth moment from
JFIV Reprod Med Genet Volume 2 • Issue 2 • 1000122
ISSN: JFIV, an open access journal
Citation: Yenkie KM, Diwekar UM, Bhalerao V (2014) Modeling and Prediction of Outcome for the Superovulation Stage in In-Vitro Fertilization (IVF).
JFIV Reprod Med Genet 2: 122. doi:10.4172/jfiv.1000122
Page 5 of 8
the same methodology. Table 6 summarizes the follicle number and size
predictions from the clinical data available for 50 patients. The results
from model projections for four more patients are reported in Figure
3-6. It can be observed that the predicted results are in well agreement
with the actual observations.
Statistical analysis
Statistical analysis was performed on the model predictions
No. of Follicles observed No. of Follicles predicted Mean size predicted
(2 day) (final day) (final day)
Number No. of Number No. of Size No. of
Range Patients Range Patients Range Patients
4-10 36 4-10 34 6-7 7
11-15 5 11-15 6 7-8 5
16-20 3 16-20 4 8-9 17
21-25 4 21-25 4 9-10 17
26-30 2 26-30 2 10-11 4
Table 6: Follicle number and size predictions based on the available clinical data. Figure 5: Predicted follicle size distribution using 2 day (S-2) and all day (S-all)
data for model fitting for Patient D.
Figure 3: Predicted follicle size distribution using 2 day (S-2) and all day (S-all) Figure 6: Predicted follicle size distribution using 2 day (S-2) and all day (S-all)
data for model fitting for Patient B. data for model fitting for Patient E.
obtained for the fifty patients clinical data used in this study. The
predictions of the ‘mean follicle size’ and the ‘Follicle Size Distribution
(FSD)’ on the final day of FSH administration were compared with the
actual observations. The percentage error was used as the measure of
the accuracy of prediction for the mean follicle size on the final day of
FSH administration and the sum of squares of error for the accuracy in
FSD projection, which is referred as the ‘Mean Square Error (MSE) in
model prediction’ in this paper. The error evaluations were performed
by two methods (i) using the available data on all days and (ii) using the
data for initial two days of observations. In MSE evaluation the follicles
in the size bins corresponding to the desired size range of 9-12 mm
were used.
In Figure 7, it can be observed that the mean follicle size prediction
is better when all day data is used, which is a more likely result from the
model predictions. In case of mean follicle size predictions using initial
two day data, we observed more than 85% patients lie within the error
range of 0% to 30%. Thus, even the two day data predicts the mean size
Figure 4: Predicted follicle size distribution using 2 day (S-2) and all day (S-all) for most of the patients with reasonable accuracy and hence regular
data for model fitting for Patient C.
monitoring and testing can be eliminated in most of the patients.
JFIV Reprod Med Genet Volume 2 • Issue 2 • 1000122
ISSN: JFIV, an open access journal
Citation: Yenkie KM, Diwekar UM, Bhalerao V (2014) Modeling and Prediction of Outcome for the Superovulation Stage in In-Vitro Fertilization (IVF).
JFIV Reprod Med Genet 2: 122. doi:10.4172/jfiv.1000122
Page 6 of 8
the model projections will provide better results and hence reduce the
requirement for further testing.
Model prediction using additional data
As stated earlier, patients whose ‘G’ values are not in the range
0.3-0.6 show poor prediction with two day data. For these patients, we
included three day data to see if the predictions improve. The Figure 9
shows the results using three day observation data for two patients F
and G which had a MSE value greater than two. In Table 7 a summary
of the results for patients F and G in terms of the comparison of mean
follicle size and mean square error value for all day, two day and three
day data predictions is shown. It can be seen that if we include an
additional day data for these patients, the predictability of the model
is enhanced.
Discussion
Figure 7: Frequency distribution of percentage error in mean follicle size on
final FSH day. Previous work
Earlier work on follicular growth was mostly theoretical and
involved the study of ovarian dynamics as a function of gonadotropins.
Peters et al. [15] mentioned the emerging of a single follicle from a
pool of small follicles. This selection phenomena was later mentioned
by Baird [4] as the specific gonadotropin environment which facilitates
the growth of dominant follicle while suppressing the others causing
follicular atresia. The concept of ‘gate widening’ denoting the time for
which the gonadotropin environment is favorable for follicle selection
for maturation, enabled the selection of multiple follicles for ovulation.
Chang et al. [16] also mentioned about the antral follicle count affecting
the early follicle growth. Gougeon et al. [17] studied age-related
changes to growing and non-growing follicles. Selgrade et al. [18] and
Reinecke and Deuflhard [19], report about the hormonal control of
the normal menstrual cycle in terms of mathematical equations. The
Figure 8: Frequency distribution of mean square error in model prediction on
final FSH day.
In Figure 8, the formula used for Mean Square Error (MSE) in
model prediction is shown in Eq. (21).
2
ni ,obs − ni ,sim (21)
MSE = ∑
max( ni ,obs , ni ,sim )
where ni,obs – number of follicles observed in the patient and ni,sim –
number of follicles predicted by the model in the ith bin on last day of
FSH administration.
The model accuracy is lower when initial two day data is used as
compared to all day data. However, the model predictions for more
than 50% of the patients lie within two MSE, which is a low error value.
Figure 9: Comparison of follicle size distribution for patient F and G on final
Insight into parameter range FSH day. (O - observed, 2 - 2day data and 3 - 3day data).
In addition to the measures of model accuracy we also checked
the most probable parameter values and their range of variation to Patient Measure of Accuracy Data used
get more insight into the predictive value. We found out that for most All day 2 day 3 day
patients the follicle growth term ‘G’ had values in the range of 0.3-0.6
Mean follicle size 9.25 5.878 8.14
and these cases the initial two day data was sufficient for FSD projection F
on successive days of the cycle. Also, for most patients the number of Mean square error 0.07652 2.644 0.417
follicles entering the growth phase varied from 7–12 follicles, which Mean follicle size 8.051 6.459 7.822
means they had ‘μ0’ ranging from 14-24. These observations prove that G
Mean square error 0.00899 2.432057 0.06473
if we have a patient whose parameter values for ‘G’ and ‘μ0’ from two
day data model fitting are in the above mentioned ranges in those cases Table 7: Improvement in model predictions using three day data.
JFIV Reprod Med Genet Volume 2 • Issue 2 • 1000122
ISSN: JFIV, an open access journal
Citation: Yenkie KM, Diwekar UM, Bhalerao V (2014) Modeling and Prediction of Outcome for the Superovulation Stage in In-Vitro Fertilization (IVF).
JFIV Reprod Med Genet 2: 122. doi:10.4172/jfiv.1000122
Page 7 of 8
model by Reinecke and Deuflhard [19] was highly complex involving predicts an unsuccessful outcome the patients still have to undergo
the dynamic studies in the pituitary and ovaries. The single follicle some initial days of treatment which are cost intensive and puts an
dynamics was studied and the hormones LH and FSH were the ones emotional burden since they start the treatment with a lot of hope.
affecting significantly. However, the model did not refer to external
stimulation and multiple ovulations which is a novel aspect of the Summary
simplified moment model. On the whole, the current work provides a novel methodology
for predicting the probable outcome of the superovulation cycle and
Study findings
saving overall IVF treatment costs. The moment model developed for
The model tries to capture the actual number of follicles observed IVF superovulation on the lines of the well-known process of batch
on the later days in the superovulation cycle by utilizing the initial crystallization provides a new approach in modeling biomedical
observations as projection guideline. The results are not exact, but they processes. The FSD predictions by the model are in good agreement
provide a general idea about the successful growth of the follicles. It can with the actual size distributions. The advantage lies in the treatment
help in deciding whether to continue with the cycle or discontinue it. variation depending upon each patient’s initial response. Thus, drug
It can save costs on futile superovulation cycles and help in deciding dosage can be customized and optimized. The proposed approach will
whether to start the IVF cycle from donor eggs. The method provides help the medical practitioners to modify the treatment protocols and
information about the number of follicles entering into the growth stage ensure a higher success rate with lesser chances of health risks.
which provides an idea about the probable number of oocytes (matured
The current model can be used to formulate a mathematical
follicles) to be retrieved. This will help in better decision making for the
function relating to the follicle size, their growth and number. The aim
next stages in the IVF cycle.
of superovulation is to maximize the number of follicles retrieved in
From the statistical analysis of 50 patient cycles, we can conclude the desired size range. The mathematical model would prove beneficial
that in the cases where model error exceeds two, the initial two day in predicting the optimal dosage regime for desired outcome by
observations are insufficient and hence in some cases more monitoring application of optimal control (Diwekar [14]) theory to the system.
and testing will be required. The analysis of desirable parameter range The current model does not consider variability depending upon the
and predictions using additional data provide the necessary distinction patient’s medical history, age and treatment response. This model
between cases where two the proposed method can work and when the can be extended to involve such variability and solve the problem for
patient may need additional observation and care. optimal dose. Thus, the current model has several advantages in terms
of predictive value and will aid the medical community and society in
Novelty of the work an area which was previously based on trial and error and required
In existing protocols the dosage prediction is done by trial and continuous medical supervision. Most importantly, it will aid in
error and involves daily monitoring using cost intensive techniques enhancing the IVF success rate.
like ultrasound. The work performed in this research is the first attempt Acknowledgements
to model follicular growth in the form of differential equations, which
We thank the Jijamata Hospital in Nanded, India for help with the data for
are able to predict the follicle size and number changes with time. It is superovulation. We also thank the Institutional Review Board at UIC for approving
also the first study where the customized model has been developed the current research to meet with the requirements of Protection of Human Subjects
from the initial response of the patient in the same cycle to project the research under the Protocol # 2012-0317 titled ‘Understanding the Superovulation
Stage of IVF Process for Optimal Drug Delivery’.
outcome on the successive days.
References
Overall benefit in terms of some key factors
1. Nachtigall RD (2006) International disparities in access to infertility services.
Financial benefit: The customized model for each patient cycle and Fertil Steril 85: 871-875.
the outcome projections will ensure a better success rate thus saving 2. Ombelet W, Cooke I, Dyer S, Serour G, Devroey P (2008) Infertility and the
the costs on unsuccessful attempts. It will reduce the requirement of provision of infertility medical services in developing countries. Hum Reprod
pathological tests and expensive monitoring methods. Update 14: 605-621.
3. Speroff L, Fritz MA (2005) Clinical Gynecology Endocrinology and Infertility.
Time saving: If the initial two day observations can project the (7th edn), Lippincott Wilkins & Williams, Philadelphia, USA.
success or failure of the superovulation cycle, time can be saved on
futile attempts. The decision to start the IVF cycle from donor eggs can 4. Baird DT (1987) A model for follicular selection and ovulation: lessons from
superovulation. J Steroid Biochem 27: 15-23.
be made within a few days of the start of the cycle.
5. Janát-Amsbury MM, Gupta KM, Kablitz CD, Peterson CM (2009) Drug delivery
Emotional factor: The emotional state of the patient is affected for in vitro fertilization: rationale, current strategies and challenges. Adv Drug
significantly since the treatment involves interference in the hormonal Deliv Rev 61: 871-882.
balance of the body. The model prediction can alleviate this problem. 6. Meniru GI, Craft IL (1997) Utilization of retrieved oocytes as an index of the
efficiency of superovulation strategies for in-vitro fertilization treatment. Hum
Health risks: The superovulation failures can be very hazardous. Reprod 12: 2129-2132.
Higher dose of medicines may result in ovarian hyperstimulation
7. Loutradis D, Drakakis P, Vomvolaki E, Antsaklis A (2007) Different ovarian
syndrome [3,20], which at times can be life-threatening. Also the stimulation protocols for women with diminished ovarian reserve. J Assist
external intake of hormones may increase the chances of ovarian cancer. Reprod Genet 24: 597-611.
8. Hill PJ, Korovessi EL, Linninger AA (2006) Batch Processes: Batch
Limitations Crystallization. Taylor & Francis CRC Press.
Biological systems are inherently uncertain; in this work we have 9. Yenkie KM, Diwekar UM, Bhalerao V (2013) Modeling the superovulation stage
not considered the associated uncertainties [11,14]. In the current in in vitro fertilization. IEEE Trans Biomed Eng 60: 3003-3008.
study, the decision of continuing or discontinuing the cycle can be 10. Hu Q, Rohani S, Jutan A (2005) Modeling and optimization of seeded batch
made only after the cycle has been started. Therefore, when the model crystallizers. Comput Chem Eng 29: 911-918.
JFIV Reprod Med Genet Volume 2 • Issue 2 • 1000122
ISSN: JFIV, an open access journal
Citation: Yenkie KM, Diwekar UM, Bhalerao V (2014) Modeling and Prediction of Outcome for the Superovulation Stage in In-Vitro Fertilization (IVF).
JFIV Reprod Med Genet 2: 122. doi:10.4172/jfiv.1000122
Page 8 of 8
11. Yenkie KM, Diwekar UM (2013) Stochastic optimal control of seeded batch reproduction: The antral follicle count predicts the outcome of pregnancy in a
crystallizer applying Ito process. Ind Engg Chem Res 52: 108-122. controlled ovarian hyperstimulation/ intrauterine insemination program. J Assist
Reprod Genet 15: 12-17.
12. Randolph AD, Larson MA (1988) Theory of particulate processes: Analysis and
Techniques of Continuous Crystallization. (2nd edn), Academic Press, San 17. Gougeon A, Ecochard R, Thalabard JC (1994) Age-related changes of the
Diego. population of human ovarian follicles: increase in the disappearance rate of
non-growing and early-growing follicles in aging women. Biol Reprod 50: 653-
13. Flood AE (2002) Thoughts on recovering particle size distributions from the 663.
moment form of the population balance. Dev Chem Eng Mineral Process 10:
501-519. 18. Selgrade JF, Harris LA, Pasteur RD (2009) A model for hormonal control of
the menstrual cycle: structural consistency but sensitivity with regard to data. J
14. Diwekar UM (2008) Introduction to Applied Optimization. (2nd edn), Springer, Theor Biol 260: 572-580.
New York.
19. Reinecke I, Deuflhard P (2007) A complex mathematical model of the human
15. Peters H, Byskov AG, Himelstein-Braw R, Faber M (1975) Follicular growth: menstrual cycle. J Theor Biol 247: 303-330.
the basic event in the mouse and human ovary. J Reprod Fertil 45: 559-566.
20. Fishel S, Jackson P (1989) Follicular stimulation for high tech pregnancies: are
16. Chang MY, Chiang CH, Chiu TH, Hseih TT, Soong YK (1998) Clinical assisted we playing it safe? BMJ 299: 309-311.
JFIV Reprod Med Genet Volume 2 • Issue 2 • 1000122
ISSN: JFIV, an open access journal
You might also like
- IVF-recent Research and Clinical Guideline-2007Document9 pagesIVF-recent Research and Clinical Guideline-2007QuackeryNo ratings yet
- Immature Oocyte Incidence Contributing Factors and Effects OnDocument7 pagesImmature Oocyte Incidence Contributing Factors and Effects OnTrang Nguyễn NhưNo ratings yet
- Selecting Male Or Female Child Here's How It Works - Based On The Teachings Of Dr. Andrew Huberman: A Guide To Gender SelectionFrom EverandSelecting Male Or Female Child Here's How It Works - Based On The Teachings Of Dr. Andrew Huberman: A Guide To Gender SelectionNo ratings yet
- A History of Developments To Improve in Vitro Ferti Lizati OnDocument4 pagesA History of Developments To Improve in Vitro Ferti Lizati OnichaNo ratings yet
- 02 - IRAOvulation Induction For TheDocument11 pages02 - IRAOvulation Induction For TheHartanto LieNo ratings yet
- The Impact of Ovarian Stimulation For IVF On The DDocument13 pagesThe Impact of Ovarian Stimulation For IVF On The DDrHeteaNo ratings yet
- 1 s2.0 S0301211523003202 main (科研通 ablesci.com)Document28 pages1 s2.0 S0301211523003202 main (科研通 ablesci.com)Carlos ParraNo ratings yet
- IN-vitro FertilisationDocument17 pagesIN-vitro FertilisationAbhishek MNo ratings yet
- Prevailing Knowledge About Male and Female Lifestyle Habits and in Vitro Fertilization in The 21st CenturyDocument18 pagesPrevailing Knowledge About Male and Female Lifestyle Habits and in Vitro Fertilization in The 21st CenturyAnonymous FyiOqjZ0nHNo ratings yet
- Original Articles: Assisted ReproductionDocument7 pagesOriginal Articles: Assisted ReproductionNirmal KumawatNo ratings yet
- Treatment Strategy for Unexplained Infertility and Recurrent MiscarriageFrom EverandTreatment Strategy for Unexplained Infertility and Recurrent MiscarriageKeiji KurodaNo ratings yet
- Early Follicular Phase LH Concentration PDFDocument7 pagesEarly Follicular Phase LH Concentration PDFgeorgianaNo ratings yet
- BiologyDocument21 pagesBiologyMeghana SNo ratings yet
- Effects of Anti M Llerian Hormone and Follicle Sti - 2014 - Taiwanese Journal ofDocument4 pagesEffects of Anti M Llerian Hormone and Follicle Sti - 2014 - Taiwanese Journal ofSami KahtaniNo ratings yet
- Pi Is 1472648310611716Document4 pagesPi Is 1472648310611716GayathriMaranNo ratings yet
- Modul Pelatihan Inseminasi Intra UterinDocument47 pagesModul Pelatihan Inseminasi Intra UterindrnyolNo ratings yet
- 5 PGS提高高龄人群的植入率和活产率Document11 pages5 PGS提高高龄人群的植入率和活产率zjuwindNo ratings yet
- Mild Ovarian Stimulation For IVFDocument17 pagesMild Ovarian Stimulation For IVFanyka2No ratings yet
- IVF Unveiled: A Comprehensive Guide to Fertility TreatmentsFrom EverandIVF Unveiled: A Comprehensive Guide to Fertility TreatmentsNo ratings yet
- Diminished Ovarian Reserve and Assisted Reproductive Technologies: Current Research and Clinical ManagementFrom EverandDiminished Ovarian Reserve and Assisted Reproductive Technologies: Current Research and Clinical ManagementOrhan BukulmezNo ratings yet
- Double Stimulations During The Follicular and Luteal Phases of Poor Responders in IVF/ICSI Programmes (Shanghai Protocol)Document8 pagesDouble Stimulations During The Follicular and Luteal Phases of Poor Responders in IVF/ICSI Programmes (Shanghai Protocol)Nirmal KumawatNo ratings yet
- The Positive and Negative Effects of in Vitro FertilizationDocument6 pagesThe Positive and Negative Effects of in Vitro Fertilizationapi-670497077No ratings yet
- Pi Is 0015028209011005Document6 pagesPi Is 0015028209011005Meli AnaNo ratings yet
- Hadawale N. M, Thorat R. M., Gaikwad D. D., Jadhav S. LDocument4 pagesHadawale N. M, Thorat R. M., Gaikwad D. D., Jadhav S. LAditya VirayudhaNo ratings yet
- Assisted Reproductive Technology - WikipediaDocument8 pagesAssisted Reproductive Technology - WikipediaBikash ChinharaNo ratings yet
- Cerm 44 96Document9 pagesCerm 44 96madeNo ratings yet
- Prof Budi Wiweko - Protokol Dan Pemantauan Stimulasi Ovarium SederhanaDocument36 pagesProf Budi Wiweko - Protokol Dan Pemantauan Stimulasi Ovarium SederhanaAnisanang BanjarNo ratings yet
- What Is in Vitro Fertilization (IVF) and Its ProcessDocument4 pagesWhat Is in Vitro Fertilization (IVF) and Its ProcessPlanet womenNo ratings yet
- Modified Natural Cycle IvfDocument5 pagesModified Natural Cycle Ivfdr zahra MahioutNo ratings yet
- BIOLOGY PROJECT FinalDocument21 pagesBIOLOGY PROJECT Finalanees hameedNo ratings yet
- Unit 2 Summary NotesDocument14 pagesUnit 2 Summary NotesQuesyNo ratings yet
- An Ethical Comparison - Vitro Fertilization: Rev. Juan R. VélezDocument11 pagesAn Ethical Comparison - Vitro Fertilization: Rev. Juan R. VélezMica BongalaNo ratings yet
- In-Vitro Fertilisation (Ivf) in Singapore: Charges and Success RatesDocument4 pagesIn-Vitro Fertilisation (Ivf) in Singapore: Charges and Success RatesLászló ÉvaNo ratings yet
- Treatment With Piroxicam Before Embryo Transfer Increases The Pregnancy Rate After in Vitro Fertilization and Embryo TransferDocument5 pagesTreatment With Piroxicam Before Embryo Transfer Increases The Pregnancy Rate After in Vitro Fertilization and Embryo TransferVasantham HospitalNo ratings yet
- Obstetrical, Neonatal, and Long-Term Outcomes of Children Conceived From in Vitro Matured OocytesDocument9 pagesObstetrical, Neonatal, and Long-Term Outcomes of Children Conceived From in Vitro Matured OocytesGeos KarNo ratings yet
- Nursing Research Paper IvfDocument14 pagesNursing Research Paper Ivfapi-739571998No ratings yet
- Assisted Reproductive Technology: Shanty Olivia F.JDocument41 pagesAssisted Reproductive Technology: Shanty Olivia F.Jshanty Olivia jasirwanNo ratings yet
- Cycle Characteristics and Pregnancy Outcomes of EaDocument13 pagesCycle Characteristics and Pregnancy Outcomes of EaterraNo ratings yet
- The Use of Acupuncture With in Vitro Fertilization: Is There A Point?Document10 pagesThe Use of Acupuncture With in Vitro Fertilization: Is There A Point?lu salviaNo ratings yet
- The Science Behind 25 Years of Ovarian Stimulation For IVFDocument38 pagesThe Science Behind 25 Years of Ovarian Stimulation For IVFPatrick BayuNo ratings yet
- Understanding IVF Success Rates and Legal Recourses For MisrepresentationDocument4 pagesUnderstanding IVF Success Rates and Legal Recourses For MisrepresentationAinur 'iin' RahmahNo ratings yet
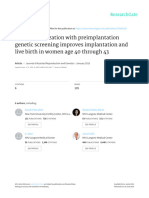
- Recurrent Implantation Failure-Update Overview OnDocument19 pagesRecurrent Implantation Failure-Update Overview Onn2763288100% (1)
- In Vitro Treatment Strategies: Over The Years Charts Have Demonstrated That There HasDocument4 pagesIn Vitro Treatment Strategies: Over The Years Charts Have Demonstrated That There HasBảo Duy Nguyễn HuỳnhNo ratings yet
- The Use of Hormonal Contraceptives in Fertility Treatments - A Committee OpinionDocument7 pagesThe Use of Hormonal Contraceptives in Fertility Treatments - A Committee Opinionjorge nnNo ratings yet
- Scaramuzzi 2011 PDFDocument24 pagesScaramuzzi 2011 PDFKarol Mariam VelázquezNo ratings yet
- Sperma Analisis PaperDocument6 pagesSperma Analisis PaperFedrik Monte Kristo LimbongNo ratings yet
- Best Practice & Research Clinical Obstetrics and GynaecologyDocument12 pagesBest Practice & Research Clinical Obstetrics and GynaecologyGrit WingsNo ratings yet
- In Vitro Fertilization: The A.R.T. of Making Babies (Assisted Reproductive Technology)From EverandIn Vitro Fertilization: The A.R.T. of Making Babies (Assisted Reproductive Technology)Rating: 4 out of 5 stars4/5 (1)
- Biology Investigatory Project Class 12 - EditedDocument17 pagesBiology Investigatory Project Class 12 - Editedharveylenseena2006No ratings yet
- PT-1-IN-SCIENCE (1) .OdtDocument14 pagesPT-1-IN-SCIENCE (1) .OdtJhersy CentenoNo ratings yet
- ART Handbook: A Step by Step GuideDocument25 pagesART Handbook: A Step by Step GuideNilesh SuvagiyaNo ratings yet
- Mehta 2012 Intrauterine Insemination With Special Reference To Density Gradient CentrifugationDocument13 pagesMehta 2012 Intrauterine Insemination With Special Reference To Density Gradient Centrifugationvominhnguyetpy01No ratings yet
- BiologyDocument17 pagesBiologyharveylenseena2006No ratings yet
- Ellenbogen 2020Document17 pagesEllenbogen 2020MD LarasatiNo ratings yet
- 2018 Article 414Document18 pages2018 Article 414Haribabu ArumugamNo ratings yet
- Ovulation Induction and Controlled Ovarian Stimulation: A Practical GuideFrom EverandOvulation Induction and Controlled Ovarian Stimulation: A Practical GuideNo ratings yet
- Bio IvfDocument40 pagesBio IvfkowsikakaruppasamyNo ratings yet
- Ivf and Icsi Consent FormDocument10 pagesIvf and Icsi Consent FormSantosoNo ratings yet
- In-Vitro Fertilisation: Shruti Samal ROLL NUMBER - 1120096 B.Sc. Life Science Second SemesterDocument20 pagesIn-Vitro Fertilisation: Shruti Samal ROLL NUMBER - 1120096 B.Sc. Life Science Second SemesterSHRUTI SAMALNo ratings yet
- HAving A Baby After MenopauseDocument3 pagesHAving A Baby After MenopauseReni ReniNo ratings yet
- Live Birth After IVF in A 46-Year-Old Woman: Case ReportDocument3 pagesLive Birth After IVF in A 46-Year-Old Woman: Case ReportReni ReniNo ratings yet
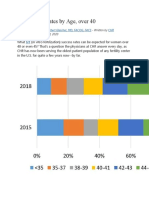
- IVF Success Rates by AgeDocument5 pagesIVF Success Rates by AgeReni ReniNo ratings yet
- INF After 43Document5 pagesINF After 43Reni ReniNo ratings yet
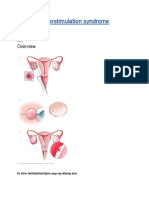
- Ovarian Hyperstimulation SyndromeDocument5 pagesOvarian Hyperstimulation SyndromeReni ReniNo ratings yet
- Outcome of in Vitro Fertilization in Women 45 Years and OlderDocument16 pagesOutcome of in Vitro Fertilization in Women 45 Years and OlderReni ReniNo ratings yet
- The History of The Mediterranean Sea Is The HistoryDocument6 pagesThe History of The Mediterranean Sea Is The HistoryReni ReniNo ratings yet
- Anti-Mullerian Hormone As A Predictor of Ovarian Reserve and Ovarian Response in IVF Women From Gaza StripDocument9 pagesAnti-Mullerian Hormone As A Predictor of Ovarian Reserve and Ovarian Response in IVF Women From Gaza StripReni ReniNo ratings yet
- Follicle Size On Day of Trigger Most Likely To Yield A Mature OocyteDocument28 pagesFollicle Size On Day of Trigger Most Likely To Yield A Mature OocyteReni ReniNo ratings yet
- Biomarkers of Ovarian ReserveDocument15 pagesBiomarkers of Ovarian ReserveReni ReniNo ratings yet
- Folicle Size ResearchDocument3 pagesFolicle Size ResearchReni ReniNo ratings yet
- Equino PiroplasmoseDocument13 pagesEquino PiroplasmoseRogério Oliva CarvalhoNo ratings yet
- Biological Basis of Sexual OrientationDocument18 pagesBiological Basis of Sexual OrientationIndira EspitiaNo ratings yet
- Perception of A Teenage MotherDocument30 pagesPerception of A Teenage MotherLourainne Faith AloceljaNo ratings yet
- SynopsisDocument10 pagesSynopsisAhmedMalikNo ratings yet
- Hernandez, Et Al.Document11 pagesHernandez, Et Al.Yet Barreda BasbasNo ratings yet
- Compilation of Sex TipsDocument5 pagesCompilation of Sex TipsChris Hansen100% (1)
- 3 Placenta Previa Nursing Care PlansDocument7 pages3 Placenta Previa Nursing Care PlansAjay RajpootNo ratings yet
- Beyond Magenta Press ReleaseDocument3 pagesBeyond Magenta Press ReleaseCandlewick PressNo ratings yet
- The Significance of MeiosisDocument5 pagesThe Significance of MeiosisKaren CasternoboNo ratings yet
- Kasus Ujian PhantomDocument4 pagesKasus Ujian PhantomMishael Octaviany JirehNo ratings yet
- Chapter 15 - TeratogenesisDocument29 pagesChapter 15 - TeratogenesisMaula AhmadNo ratings yet
- Clowes Brian - Case Against Condoms Death by LatexDocument36 pagesClowes Brian - Case Against Condoms Death by LatexGHP1967No ratings yet
- The 9th Annual NY Men Having Babies Surrogacy Seminar & Gay Parenting Expo - at The JCC in ManhattanDocument24 pagesThe 9th Annual NY Men Having Babies Surrogacy Seminar & Gay Parenting Expo - at The JCC in ManhattanMenHavingBabiesNo ratings yet
- SJK (T) Dato' Sithambaram Pillay March Monthly Test Sceince Year 5Document10 pagesSJK (T) Dato' Sithambaram Pillay March Monthly Test Sceince Year 5Thilai Nathan JeyaramanNo ratings yet
- Lecture Maternal and Child Health NursingDocument6 pagesLecture Maternal and Child Health NursingAmpie EmNo ratings yet
- Final PaperDocument75 pagesFinal PaperJohanna CesarNo ratings yet
- 2.parts of A PlantDocument20 pages2.parts of A PlantcriselNo ratings yet
- Cytoplasmic InheritanceDocument13 pagesCytoplasmic InheritanceIzza NafisaNo ratings yet
- Recurrent Pregnancy LossDocument40 pagesRecurrent Pregnancy LossJagannath MaaleNo ratings yet
- National Standards and Guidelines For Adolescent Friendly Health ServicesDocument40 pagesNational Standards and Guidelines For Adolescent Friendly Health ServicesRyzen John Blando100% (1)
- Premature Rupture of MembranesDocument29 pagesPremature Rupture of MembranesIda YosopaNo ratings yet
- CDGP Versus HypogonadismDocument25 pagesCDGP Versus HypogonadismmpintobNo ratings yet
- Multiple Pregnancy NOR PosterDocument1 pageMultiple Pregnancy NOR PosterbigbossNo ratings yet
- CBLM Tle-Afa LG Gr. 10 Animal ProductionDocument281 pagesCBLM Tle-Afa LG Gr. 10 Animal ProductionPj TvNo ratings yet
- Kapling Jayan, Borobudur, Magelang, IndonesiaDocument16 pagesKapling Jayan, Borobudur, Magelang, IndonesiaAnggi purtikaNo ratings yet
- BDSM Negotiation Checklist PDFDocument2 pagesBDSM Negotiation Checklist PDFJulia Marie Flautt80% (5)
- Senate Bill No 2635Document5 pagesSenate Bill No 2635CBCP for LifeNo ratings yet
- Sabrina and Corina Final DraftDocument7 pagesSabrina and Corina Final DraftMichael CandlerNo ratings yet
- Young Talk, August 2008Document4 pagesYoung Talk, August 2008Straight Talk FoundationNo ratings yet
- Lesson 3 Male and Female Rep. SystemDocument21 pagesLesson 3 Male and Female Rep. SystemHye JinNo ratings yet