Professional Documents
Culture Documents
Led Astray: Clinical Problem-Solving
Uploaded by
meganOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Led Astray: Clinical Problem-Solving
Uploaded by
meganCopyright:
Available Formats
The n e w e ng l a n d j o u r na l of m e dic i n e
Clinical Problem-Solving
Caren G. Solomon, M.D., M.P.H., Editor
Led Astray
Samantha Young, M.D., Luke Chen, M.D., Wesley Palatnick, M.D.,
Patrick Wong, M.D., and Justin Wong, M.D.
In this Journal feature, information about a real patient is presented in stages (boldface type) to an expert
clinician, who responds to the information by sharing relevant background and reasoning with the reader
(regular type). The authors’ commentary follows.
From the British Columbia Centre on A 34-year-old man presented to a community hospital in Vancouver, Canada, with a
Substance Use (S.Y.), and the Depart- 1-month history of constant diffuse abdominal pain, fatigue, and anorexia associ-
ment of Medicine (S.Y.), the Division of
Hematology (L.C.), the Centre for Health ated with a weight loss of 2.7 kg but no fevers or night sweats. He reported constipa-
Education Scholarship (L.C.), and the Di- tion but no diarrhea, melena, or hematochezia. His medical history and travel his-
vision of Critical Care (J.W.), University of tory were unremarkable.
British Columbia, Vancouver, the Depart-
ment of Emergency Medicine (W.P.) and
the Department of Internal Medicine The differential diagnosis of subacute, diffuse abdominal pain in a young man is
Section of Critical Care (J.W.), University broad. It includes inflammatory conditions (e.g., Crohn’s disease), cancer, an ob-
of Manitoba, Winnipeg, and the Depart-
ment of Pathology and Laboratory Medi- struction, a hepatic or biliary pathologic condition, pancreatitis, celiac disease,
cine, Richmond General Hospital, Rich- adrenal insufficiency, acute intermittent porphyria, infection (e.g., helminthic or
mond, BC (P.W.) — all in Canada. human immunodeficiency virus [HIV]–related), metabolic causes (e.g., hypercal-
Address reprint requests to Dr. Young at
the British Columbia Centre on Substance cemia or ingestion of toxic substances), and as a diagnosis of exclusion, func-
Use, 400-1045 Howe St., Vancouver, BC tional causes.
V6Z 2A9, Canada, or at samantha.young@
alumni.ubc.ca.
The patient was from India but had lived in Canada since he was 13 years of age. He
N Engl J Med 2020;383:578-83. worked at a family-run business and lived with his wife and his parents. His medica-
DOI: 10.1056/NEJMcps1900799
Copyright © 2020 Massachusetts Medical Society. tions included gabapentin, ibuprofen, and acetaminophen with codeine, all of which
had been prescribed for his recent pain. He reported that he did not use nicotine-
containing products, drink alcohol, or use illicit drugs.
On examination, the patient’s temperature was 36.7°C, the blood pressure
117/73 mm Hg, the pulse 99 beats per minute, the oxygen saturation 99% while he
was breathing ambient air, and the respiratory rate 16 breaths per minute. He ap-
peared thin with conjunctival pallor. The jugular venous pressure was 1 cm above the
sternal angle. The cardiac, respiratory, and neurologic examinations were normal.
There was no palpable lymphadenopathy. The abdominal examination revealed
mild tenderness in the left lower quadrant, with no rebound tenderness, guarding,
ascites, masses, or organomegaly. Bowel sounds were normal.
The patient is afebrile, with no obvious focus of infection. The jugular venous
pressure suggests volume depletion, which could be a manifestation of the condi-
tion that is causing his abdominal pain (e.g., adrenal insufficiency) or a conse-
quence of the pain (e.g., decreased oral intake).
The hemoglobin level was 7.7 g per deciliter, and the hematocrit 25%, with a mean
corpuscular volume of 73 fl. The platelet count was 344,000 per cubic millimeter, and
578 n engl j med 383;6 nejm.org August 6, 2020
The New England Journal of Medicine
Downloaded from nejm.org by JONATHAN MAISEL on August 20, 2020. For personal use only. No other uses without permission.
Copyright © 2020 Massachusetts Medical Society. All rights reserved.
Clinical Problem-Solving
The abnormalities noted on CT warrant endo-
scopic investigation. The patient’s microcytic
anemia with nucleated red cells is of interest. A
ferritin level of greater than 200 ng per deciliter,
along with elevated levels of serum iron and
transferrin saturation, are inconsistent with iron
deficiency. The normal C-reactive protein level
makes an inflammatory cause of anemia (i.e.,
anemia of chronic disease) unlikely, although it
does not rule it out. In a patient of South Asian
ancestry, thalassemia should be considered; how-
ever, it would not explain his abdominal pain.
10 µm
Serum and urine protein electrophoresis, a direct
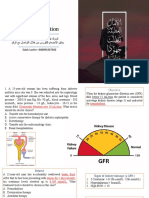
Figure 1. Peripheral-Blood Smear. antiglobulin test, measurement of the haptoglo-
A peripheral-blood smear shows microcytosis of red bin level, and measurement of the hemoglobin
cells with basophilic stippling (Wright–Giemsa stain). level with the use of high-performance liquid
chromatography should be performed. Serologic
tests for HIV and hepatitis A, B, and C viruses
should also be performed, particularly given the
the white-cell count 11,300 per cubic millimeter, patient’s elevated liver-enzyme levels. It would also
with 90% polymorphonuclear leukocytes and a be worthwhile to measure the blood lead level,
normal eosinophil count. The ferritin level was since lead poisoning can cause microcytic anemia
316 ng per milliliter (normal range, 15 to 300), the with basophilic stippling and abdominal pain.
iron level 184 μg per deciliter (33 μmol per liter)
(normal range, 60 to 150 μg per deciliter [11 to The patient was admitted to the hospital for fur-
27 μmol per liter]), the total iron-binding capacity ther investigation. Upper and lower endoscopy
290 μg per deciliter (52 μmol per liter) (normal revealed normal-appearing mucosa, with no bleed-
range, 250 to 425 μg per deciliter [45 to 76 μmol ing or inflammation; random biopsy specimens
per liter]), and the transferrin saturation 63% of the rectum, terminal ileum, duodenum, and
(normal range, 20 to 55). A peripheral-blood stomach were obtained. Ultrasonography of the
smear showed occasional nucleated red cells, liver revealed diffuse fatty infiltration. The patient
polychromasia, basophilic stippling, Pappen- received morphine, which reduced his pain. He
heimer bodies, teardrop cells, and microcytosis was discharged home with pantoprazole at a dose
(Fig. 1). The aspartate aminotransferase level was of 40 mg per day; given the presence of microcytic
100 U per liter (normal range, 10 to 38), the anemia, the presumptive diagnosis was thalas-
alanine aminotransferase level 162 U per liter semia, although the results of the hemoglobin
(normal range, 10 to 80), the γ-glutamyltransfer electrophoresis were pending. After discharge,
ase level 195 U per liter (normal range, 15 to 80), the gastric-biopsy specimens showed evidence of
and the alkaline phosphatase level 132 U per liter Helicobacter pylori infection; despite treatment with
(normal range, 30 to 135); the bilirubin and lac- lansoprazole, amoxicillin, and clarithromycin,
tate dehydrogenase levels were normal. No recent the symptoms did not abate. Examinations of the
blood test results were available for comparison. other biopsy specimens were negative, as was the
The results of renal-function tests were normal, test for hemoglobinopathy.
as were the levels of electrolytes, thyrotropin, se- During the next 6 weeks, the patient had three
rum vitamin B12, and C-reactive protein; the inter- subsequent visits to the emergency department
national normalized ratio; and the activated par- for ongoing abdominal pain. He was referred to
tial-thromboplastin time. Computed tomography a gastroenterologist for a capsule endoscopy; the
(CT) of the abdomen revealed thickening of the results were normal. He was then readmitted to
rectum and sigmoid colon near the hepatic flex- the hospital; he had lost an additional 11 kg of
ure, with a normal-appearing terminal ileum and weight and had a new headache on the right side
no lymphadenopathy. that had lasted 2 to 3 hours, with associated nau-
n engl j med 383;6 nejm.org August 6, 2020 579
The New England Journal of Medicine
Downloaded from nejm.org by JONATHAN MAISEL on August 20, 2020. For personal use only. No other uses without permission.
Copyright © 2020 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
sea but no photophobia or neck stiffness. He re- hood. Acquired sideroblastic anemia can be
mained afebrile. An additional workup included caused by alcohol use, medications such as iso-
serologic testing for hepatitis A, B, and C viruses, niazid and linezolid (which the patient has not
testing for syphilis and HIV infection, serum pro- received), or copper deficiency, which can be
tein electrophoresis, lumbar puncture, blood cul- caused by excess ingestion of zinc or by mal-
tures, urine cultures, chest radiography, and absorptive disorders. Given an ongoing unex-
magnetic resonance imaging (MRI) of the head plained microcytic anemia with nucleated red
and spine, all of which were unremarkable. The cells, the blood levels of lead and copper should
patient was seen by a neurologist, a rheumatolo- be assessed; if the levels are normal, I would
gist, and an infectious-disease specialist. He was recommend a bone marrow biopsy.
ultimately discharged home with an unclear diag-
nosis (with his presentation postulated to be re- One week later, the patient returned to the hospi-
lated to a viral illness), and outpatient follow-up tal after having a witnessed generalized seizure.
with a hematologist was planned. He received a Despite treatment with diazepam and phenytoin,
prescription for hydromorphone to be used as he had subsequent recurrent seizures with inter-
needed for ongoing abdominal pain. ictal somnolence that resulted in intubation and
transfer to the intensive care unit. He was afebrile
The patient continues to have abdominal pain on presentation. A neurologic examination did
and progressive weight loss, with no unifying not suggest any focal lesions. CT of the head was
diagnosis. Quadruple therapy for H. pylori infec- unremarkable. Urine drug screening was positive
tion — rather than the triple therapy he received only for opioids, a finding that was consistent
— is preferable, and eradication should be con- with his prescribed medications, and ethanol was
firmed, although the possible presence of such not detected in the serum. His blood tests contin-
an infection still does not explain the clinical ued to indicate microcytic anemia, and he had a
picture of anemia that is not due to iron defi- normal C-reactive protein level. His liver-enzyme
ciency. Although α-thalassemia is not yet ruled levels were now normal.
out by testing, this disorder would not account The trachea was extubated on hospital day 2.
for his abdominal pain or headache. The hepatic Examination of a bone marrow–biopsy specimen
steatosis noted on ultrasonography may explain and bone marrow aspirate showed normal triline-
his elevated liver-enzyme levels; his history of age hematopoiesis with occasional ringed sidero-
alcohol use should be reassessed, and other blasts (Fig. 2) and no evidence of myelodysplasia
metabolic risk factors should be considered. The or a lymphoproliferative disorder. On hospital
absence of fever combined with a normal C-reac-
tive protein level, negative cultures, and normal
findings on cerebrospinal fluid analysis do not
support infectious or inflammatory causes. When
one is faced with a constellation of unexplained
symptoms, it can be helpful to focus on an ob-
jective finding with a limited differential diag-
nosis. Microcytic anemia is one such finding.
Iron deficiency, the most common cause, has
been ruled out, as has thalassemia; the other
conditions that can cause a microcytic anemia
are inflammation, sideroblastic anemia (congeni-
tal or acquired), and lead poisoning. The sidero-
blastic anemias are rare bone marrow disorders 10 µm
characterized by abnormal iron accumulation in Figure 2. Bone Marrow Aspirate Smear.
the mitochondria of erythroid precursors, which A bone marrow aspirate smear shows ringed sidero-
manifest as ring sideroblasts in the bone mar- blasts with iron granules accumulating around the
row aspirate. Congenital forms such as X-linked nuclei of erythroid precursors (Prussian blue stain).
sideroblastic anemia typically manifest in child-
580 n engl j med 383;6 nejm.org August 6, 2020
The New England Journal of Medicine
Downloaded from nejm.org by JONATHAN MAISEL on August 20, 2020. For personal use only. No other uses without permission.
Copyright © 2020 Massachusetts Medical Society. All rights reserved.
Clinical Problem-Solving
day 6, a critically elevated serum level of free pro- substance use. He had begun using opium, which
toporphyrin was reported (612.4 μg per deciliter he had obtained from a customer at his business,
[10.84 μmol per liter]) (normal range, 15 to 50 μg 2 years earlier. Before the patient was hospital-
per deciliter [0.27 to 0.88 μmol per liter]); this ized, he had been using opium on a daily basis
blood test had been ordered to investigate for por- and had spent approximately $2,000 in Canadian
phyria. dollars (approximately $1,500 in U.S. dollars) per
month on opium. He had ingested it orally, with
Acute hepatic porphyrias — the most common no intravenous use. His withdrawal symptoms
of which is acute intermittent porphyria — can had included nausea, sweating, and tremors. He
produce neurovisceral symptoms, such as ab- was motivated to stop using opium and to begin
dominal pain and seizures, but would not cause opioid-agonist therapy with buprenorphine–
anemia. Acute intermittent porphyria also does naloxone.
not cause elevated protoporphyrin levels, which
are associated with protoporphyria, a cutaneous Stigma often prevents patients from being forth-
form of porphyria that is not compatible with coming when asked about their substance use in
this patient’s presentation. Rather, an elevated a clinical setting. At a minimum, this patient
free protoporphyrin level can be caused by lead meets the criteria for a moderate opioid use dis-
poisoning, and this now seems to be the likely order; opioid-agonist therapy with buprenorphine
diagnosis. Occasional ringed sideroblasts can or methadone is recommended, along with psy-
also be seen in patients with toxic effects from chosocial treatment, if desired. It is notable that
exposure to lead. A blood lead level should be he had received prescriptions for several opioids,
measured, although the patient had had suffi- including codeine and hydromorphone, to treat
cient evidence to warrant this having been per- his abdominal pain without medical personnel
formed much earlier in the clinical course. having knowledge of his opioid use disorder.
Unbeknownst to his treating physicians, these
The elevated serum level of free protoporphyrin, opioids would have also treated any opioid with-
combined with the patient’s abdominal pain, sei- drawal he was having, although he risked having
zures, and laboratory evidence of microcytic ane- toxic effects and an overdose if he continued to
mia, was considered to be indicative of lead poi- use opium. Opium is the likely source of his lead
soning. The blood lead level was markedly poisoning, on the basis of several case reports
elevated, at 94.4 μg per deciliter (4.6 μmol per li- of this phenomenon, particularly from the Mid
ter) (normal value, <5 μg per deciliter [0.2 μmol dle East.
per liter]).
A sample of the opium was obtained for analysis;
Now that the diagnosis of lead poisoning has inductively coupled plasma–mass spectrometry
been confirmed, it is important to identify the confirmed the presence of lead, at 23 ppm. In
source in order to prevent ongoing exposure. A consultation with the local poison control center,
thorough occupational history should be taken, and with no residual changes in mental status,
as well as an assessment of any potential envi- the patient received chelation therapy with oral
ronmental or home exposures. Specific sources meso 2,3-dimercaptosuccinic acid (succimer) for
to ask about are Ayurvedic therapies, herbal sup- 18 days. He was discharged home with instruc-
plements, and glazed ceramic cookware. tions to take buprenorphine–naloxone (at a dose
of 4 mg and 1 mg, respectively) and was referred
No potential occupational or environmental ex- to community addiction support services.
posures were identified, and the patient reported The patient’s symptoms of abdominal and
no use of herbal supplements or Ayurvedic medi- musculoskeletal pain, lethargy, and anorexia
cations and no use of glazed ceramic cookware. abated rapidly, and at a follow-up visit 6 months
Although the patient had previously reported that later, his blood lead level had dropped to 35.0 μg
he did not use any illicit drugs, his father dis- per deciliter (1.7 μmol per liter). On follow-
closed that the patient had been using opium. The up more than 1 year later, he remained absti-
patient subsequently divulged the details of his nent from opium with continued treatment with
n engl j med 383;6 nejm.org August 6, 2020 581
The New England Journal of Medicine
Downloaded from nejm.org by JONATHAN MAISEL on August 20, 2020. For personal use only. No other uses without permission.
Copyright © 2020 Massachusetts Medical Society. All rights reserved.
The n e w e ng l a n d j o u r na l of m e dic i n e
buprenorphine–naloxone, and he reported that hypertension, seen in patients with long-term
he had not had any recurrent seizures since his exposure; and peripheral neuropathy, seen in pa-
previous hospitalization for a witnessed general- tients who have had either short-term or long-
ized seizure. term exposure — although none of these signs
are particularly sensitive for lead poisoning.5,7,8
Anemia typically manifests at a blood lead level
C om men ta r y
of greater than 50 μg per deciliter (2.4 μmol per
Lead poisoning is a diagnosis that is often over- liter).7 Severe encephalopathy, which can include
looked. Although the typical clinical features of the occurrence of seizures, characteristically
abdominal pain and weight loss are nonspecific, occurs at a very high blood lead level (>100 μg
a focus on the limited number of causes of micro- per deciliter [4.8 μmol per liter] in adults); in
cytic anemia ultimately led to the diagnosis. In this patient, seizure occurred at a slightly lower
this case, iron-deficiency anemia was initially blood lead level (94.4 μg per deciliter), but it is
considered to be a likely diagnosis, despite the presumed to be attributable to lead, in the ab-
patient having a serum ferritin level above 200 ng sence of an alternative explanation.9 With long-
per milliliter, which made iron deficiency ex- term low-level exposure, neurologic manifesta-
tremely unlikely.1 The diagnostic errors in this tions may be more insidious and can include
case stemmed predominantly from faulty knowl- memory impairment and irritability.7 Mild long-
edge synthesis,2 whereby the clinicians failed to term elevations of the blood lead level (>10 μg
consider lead poisoning earlier in the clinical per deciliter [0.5 μmol per liter]) are associated
course despite highly suggestive clinical signs with an increased risk of cardiovascular disease,
and symptoms, including abdominal pain, micro- renal dysfunction, and neurocognitive effects,
cytic anemia, and basophilic stippling. As a re- highlighting the need to avoid even low-level
sult, the patient underwent repeated endoscopic exposure.8-11 Basophilic stippling of erythrocytes
studies and had added complications. Given the is a characteristic finding in cases of lead poi-
availability, accuracy, and relatively low cost of soning, but it can also be associated with arsenic
serum lead testing, this test should be performed poisoning, sideroblastic anemia, myelodysplastic
promptly in patients whose presentation is com- syndrome, thalassemia, and other conditions.12
patible with lead poisoning. Once a high lead Chelation therapy with succimer or calcium
level is documented, the source must be identi- disodium EDTA is indicated for patients with a
fied to prevent continued exposure. Lead-con- blood lead level above 80 μg per deciliter
taminated opium has led to thousands of cases (3.9 μmol per liter), as in this case. Depending
of lead poisoning in the Middle East3 and sev- on the duration of lead exposure and symptoms,
eral cases in Europe4,5 and Australia.6 This case such therapy may also be indicated for patients
highlights the effect of globalized illicit drug with lower blood lead levels; involvement of a
trade, whereby lead poisoning from opium oc- toxicologist or an occupational and environmen-
curred in North America. tal medicine physician is useful in decision mak-
Lead poisoning can result from short-term or ing. Once chelation therapy is initiated, patients
long-term exposure, the latter being more com- are monitored closely for potential side effects,
mon among adults. This patient’s symptoms are including hepatic and renal impairment, as well
probably a result of steady exposure over an ex- as transiently worsening symptoms due to the
tended period of time, although they may have mobilization of lead from tissue and bone into
been exacerbated by larger, short-term ingestions. the blood. The magnitude of reduction in symp-
Lead affects numerous organ systems; common toms is variable; such changes may occur over
symptoms and signs include gastrointestinal dis- the course of several weeks or substantially lon-
comfort, constipation, and altered mental status, ger (more than a year). Given that the removal of
although the presentation is variable and depends lead from the central nervous system is a slow
on the duration of exposure. Features common process, neurocognitive effects may resolve slow
ly seen on physical examination that are consis- ly and incompletely, and there is concern that
tent with lead poisoning include bluish pigmen- cumulative lead exposure may accelerate age-
tation at the gum line (termed “lead lines”); related cognitive decline.10
582 n engl j med 383;6 nejm.org August 6, 2020
The New England Journal of Medicine
Downloaded from nejm.org by JONATHAN MAISEL on August 20, 2020. For personal use only. No other uses without permission.
Copyright © 2020 Massachusetts Medical Society. All rights reserved.
Clinical Problem-Solving
In Iran and other Middle Eastern countries, creasing. Further research is needed to identify
numerous cases of lead poisoning from lead- the prevalence of lead-contaminated opium in the
contaminated opium have been reported.3 Dur- illicit drug supply in North America.
ing an 18-month period from 2016 to 2017, more Once the diagnosis of lead poisoning is es-
than 4000 persons across two large hospitals in tablished, the source of lead is often revealed
Tehran were treated for lead poisoning resulting from an occupational history, review of medica-
from ingestion of opium.3 The concentration of tion, or examination of cookware for leaded
lead found in the opium sample tested in this glazes.12 In the case of lead-containing opium,
case, 23 ppm, is within the range of concentra- patients may not disclose their substance use or
tions reported in other cases of opium ingestion, may not be aware of the possibility of opium as
in which concentrations ranged from 1.8 to a potential source. A heightened awareness
3200 ppm.13,14 The reason for lead contamination among practitioners and physicians is needed to
in opium is not known, but two leading hypoth- make the diagnosis and to connect the patient
eses are that lead is added to increase the with addiction services.
weight, thereby increasing profit, or that it re- No potential conflict of interest relevant to this article was
sults from the manufacturing process. reported.
Disclosure forms provided by the authors are available with
The majority of the world’s 10,500 tons of illicit the full text of this article at NEJM.org.
opium supply comes from Afghanistan.15 The We thank Dr. Morris Pudek and Dr. Benjamin Jung for their
percentage of illicit opium that is contaminated analysis of the opium sample, Dr. Karen Ung for her input re-
garding the bone marrow biopsy and peripheral-blood smears,
with lead is unclear, but the number of cases of and Dr. Robert Mitchell for his advice on an earlier version of
lead poisoning from opium appears to be in- the manuscript.
References
1. Guyatt GH, Oxman AD, Ali M, Willan 6. Law S, Ackerly I, Scott-Rimmington B, 11. Shih RA, Hu H, Weisskopf MG,
A, McIlroy W, Patterson C. Laboratory Nallaratnam K. Two cases of lead poison- Schwartz BS. Cumulative lead dose and
diagnosis of iron-deficiency anemia: an ing from inhaled opium in Victoria. Emerg cognitive function in adults: a review of
overview. J Gen Intern Med 1992;7:145-53. Med Australas 2019;31:144-5. studies that measured both blood lead
2. Graber ML, Franklin N, Gordon R. 7. Abadin H, Ashizawa A, Stevens Y-W, and bone lead. Environ Health Perspect
Diagnostic error in internal medicine. et al. Toxicological profile for lead. Atlan- 2007;115:483-92.
Arch Intern Med 2005;165:1493-9. ta:Agency for Toxic Substances and Dis- 12. Fralick M, Thomspson A, Mourad O.
3. Ghane T, Zamani N, Hassanian- ease Registry, 2007 (https://www.ncbi.nlm Lead toxicity from glazed ceramic cook-
Moghaddam H, Beyrami A, Noroozi A. Lead .nih.gov/pubmed/24049859). ware. CMAJ 2016;188:E521-E524.
poisoning outbreak among opium users in 8. Navas-Acien A, Guallar E, Silbergeld 13. Aghaee-Afshar M, Khazaeli P, Behnam
the Islamic Republic of Iran, 2016-2017. EK, Rothenberg SJ. Lead exposure and B, Rezazadehkermani M, Ashraf-Ganjooei
Bull World Health Organ 2018;96:165-72. cardiovascular disease — a systematic re- N. Presence of lead in opium. Arch Iran
4. Azizi A, Ferguson K, Dluzewski S, view. Environ Health Perspect 2007;115: Med 2008;11:553-4.
Hussain T, Klein M. Chronic lead poison- 472-82. 14. Zamani N, Hassanian-Moghaddam H.
ing in an Iranian opium smoker resident 9. Gidlow DA. Lead toxicity. Occup Med Ingestion of lead-contaminated packs of
in London. BMJ Case Rep 2016; 2016: (Lond) 2015;65:348-56. opium. N Engl J Med 2018;379:1861.
bcr2016215965. 10. Kosnett MJ, Wedeen RP, Rothenberg 15. United Nations Office on Drugs and
5. Helmich F, Lock G. Burton’s line from SJ, et al. Recommendations for medical Crime. World drug report 2018. Vienna:
chronic lead intoxication. N Engl J Med management of adult lead exposure. Envi- United Nations, June 2018.
2018;379(19):e35. ron Health Perspect 2007;115:463-71. Copyright © 2020 Massachusetts Medical Society.
n engl j med 383;6 nejm.org August 6, 2020 583
The New England Journal of Medicine
Downloaded from nejm.org by JONATHAN MAISEL on August 20, 2020. For personal use only. No other uses without permission.
Copyright © 2020 Massachusetts Medical Society. All rights reserved.
You might also like
- DiagnosisDocument6 pagesDiagnosisZackNo ratings yet
- Hiding in The Water: Clinical Problem-SolvingDocument6 pagesHiding in The Water: Clinical Problem-SolvingtabareeNo ratings yet
- Nejmcps 2307875Document7 pagesNejmcps 2307875Srinivas PingaliNo ratings yet
- Copycat: Clinical Problem-SolvingDocument6 pagesCopycat: Clinical Problem-SolvingjohnNo ratings yet
- Nejmcps 2108909Document7 pagesNejmcps 2108909GÜLHANE DAHİLİYENo ratings yet
- Cryptic Cachexia: Clinical Problem-SolvingDocument7 pagesCryptic Cachexia: Clinical Problem-SolvingrestiNo ratings yet
- Hepatology - 1983 - Viola - Exudative Ascites in The Course of Acute Type B HepatitisDocument3 pagesHepatology - 1983 - Viola - Exudative Ascites in The Course of Acute Type B HepatitisAudryaNo ratings yet
- 74 Year Old Woman With Fatigue, Anorexia, and AbdoDocument6 pages74 Year Old Woman With Fatigue, Anorexia, and AbdoRamiro Arraya MierNo ratings yet
- HEMATURIADocument9 pagesHEMATURIAAndreina AcevedoNo ratings yet
- Nejmcps 1808494Document6 pagesNejmcps 1808494dias100% (1)
- Clinical Presentation: by Dr. Raffiq AbbasDocument36 pagesClinical Presentation: by Dr. Raffiq AbbasKarthick UnleashNo ratings yet
- Rounds: GrandDocument7 pagesRounds: GrandHưng Nguyễn KiềuNo ratings yet
- A Treacherous Course: Clinical Problem-SolvingDocument6 pagesA Treacherous Course: Clinical Problem-SolvingMorocco CandycatyNo ratings yet
- Pi Is 0272638698001097Document6 pagesPi Is 0272638698001097Mita AdrianiNo ratings yet
- Spiraling Out of Control: Clinical Problem-SolvingDocument6 pagesSpiraling Out of Control: Clinical Problem-SolvingjjjkkNo ratings yet
- Nejmcpc 1904048Document10 pagesNejmcpc 1904048luca.win92No ratings yet
- Nejmcpc 1102202Document10 pagesNejmcpc 1102202FrinkooFrinkoBNo ratings yet
- Crim Em2013-948071Document2 pagesCrim Em2013-948071m.fahimsharifiNo ratings yet
- 2019 Explanation k2Document261 pages2019 Explanation k2berdaderagaNo ratings yet
- 44 Year Old Man With Fatigue, Weight Loss, and LeuDocument5 pages44 Year Old Man With Fatigue, Weight Loss, and LeuRamiro Arraya MierNo ratings yet
- 72_Progressive multifocal leukoencephalopathy in an immunocompetent patientDocument7 pages72_Progressive multifocal leukoencephalopathy in an immunocompetent patientFaras ArinalNo ratings yet
- Intestinal Tuberculosis: A Diagnostic Challenge: Open Access Case DOI: 10.7759/cureus.13058Document4 pagesIntestinal Tuberculosis: A Diagnostic Challenge: Open Access Case DOI: 10.7759/cureus.13058ATIKA INDAH SARINo ratings yet
- Gastroent 09 06665Document3 pagesGastroent 09 06665HandayaniNo ratings yet
- Case HT 5Document4 pagesCase HT 5farhah ayunizar ramadhaniNo ratings yet
- Abdominal Tuberculosis Presenting As Ascites in An Older Indigenous Woman: A Case ReportDocument5 pagesAbdominal Tuberculosis Presenting As Ascites in An Older Indigenous Woman: A Case ReportauliaNo ratings yet
- Step by Step: Clinical Problem-SolvingDocument5 pagesStep by Step: Clinical Problem-SolvingMirin ApuniusNo ratings yet
- Angioedema HereditarioDocument13 pagesAngioedema HereditarioLUCIAMELENDEZSNo ratings yet
- Hepatocellular Carcinoma Causing Severe.1057Document1 pageHepatocellular Carcinoma Causing Severe.1057Vardan KocharNo ratings yet
- Acute Kidney Injury and Proteinuria in A Man With HemoptysisDocument3 pagesAcute Kidney Injury and Proteinuria in A Man With HemoptysisChe GuevaraNo ratings yet
- AML Case Study AnalysisDocument14 pagesAML Case Study AnalysisIssaiah Nicolle CeciliaNo ratings yet
- Hypokalemic NephropathyDocument7 pagesHypokalemic NephropathyGoris HariyadiNo ratings yet
- Primary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportDocument6 pagesPrimary Congenital Choledochal Cyst With Squamous Cell Carcinoma: A Case ReportRais KhairuddinNo ratings yet
- Megaloblastic Anemia Case Report Focuses on Hypotension and DeliriumDocument5 pagesMegaloblastic Anemia Case Report Focuses on Hypotension and DeliriumNindy PutriNo ratings yet
- Case Report and Literature Review On Good's Syndrome, A Form of Acquired Immunodeficiency Associated With ThymomasDocument7 pagesCase Report and Literature Review On Good's Syndrome, A Form of Acquired Immunodeficiency Associated With ThymomasMudassar SattarNo ratings yet
- Autoimmune Hemolytic Anemia Warm-Antibody Type (Warm AIHA) in An 8-Year-Old Balinese GirlDocument5 pagesAutoimmune Hemolytic Anemia Warm-Antibody Type (Warm AIHA) in An 8-Year-Old Balinese GirlFatimatuzzahra ShahabNo ratings yet
- Primary Peritonitis Due To Streptococcus Pyogenes: Eview RticleDocument5 pagesPrimary Peritonitis Due To Streptococcus Pyogenes: Eview RticleGabriNo ratings yet
- Case 15-2018: An 83-Year-Old Woman With Nausea, Vomiting, and ConfusionDocument8 pagesCase 15-2018: An 83-Year-Old Woman With Nausea, Vomiting, and ConfusionivanNo ratings yet
- BCR 2012 006927Document5 pagesBCR 2012 006927Aarathi raoNo ratings yet
- Monitoring Day 6 (19 December 2017) : Costa and 1 CM Below The Left Lobe Proccesusxyphoideus, ChewyDocument8 pagesMonitoring Day 6 (19 December 2017) : Costa and 1 CM Below The Left Lobe Proccesusxyphoideus, ChewyIvana YunitaNo ratings yet
- Case 14-2020: A 37-Year-Old Man With Joint Pain and Eye RednessDocument9 pagesCase 14-2020: A 37-Year-Old Man With Joint Pain and Eye RednessWho's Alewii?No ratings yet
- Letters To The Editor: Membranous Glomerulonephritis in A Patient With SyphilisDocument2 pagesLetters To The Editor: Membranous Glomerulonephritis in A Patient With SyphilisBetty Romero BarriosNo ratings yet
- Case StudiesDocument6 pagesCase StudiesPatricia CruzNo ratings yet
- NEJM Case of AMS and SeizureDocument9 pagesNEJM Case of AMS and SeizureBÁCH NGUYỄN ĐẮCNo ratings yet
- FAST 5 MCQS 10.3.24slidesDocument7 pagesFAST 5 MCQS 10.3.24slidesDr Nikita NNo ratings yet
- Case 34-2021: A 38-Year-Old Man With Altered Mental Status and New Onset of SeizuresDocument9 pagesCase 34-2021: A 38-Year-Old Man With Altered Mental Status and New Onset of Seizuresskrv99No ratings yet
- 28-Year-Old Man With Crohn Disease and Hematuria: Residents ' ClinicDocument5 pages28-Year-Old Man With Crohn Disease and Hematuria: Residents ' ClinicDesi HutapeaNo ratings yet
- Visceral Leishmaniasis Turning into Chronic Liver DiseaseDocument4 pagesVisceral Leishmaniasis Turning into Chronic Liver DiseasePratyay HasanNo ratings yet
- Chagas Therapy NEJM 2011Document8 pagesChagas Therapy NEJM 2011Ever LuizagaNo ratings yet
- NBME 1 RatioDocument87 pagesNBME 1 RatioBugs Caslib100% (1)
- PIIS0016508515000359Document2 pagesPIIS0016508515000359Christofel JomanNo ratings yet
- Prolonged Fever, Hepatosplenomegaly, and Pancytopenia in A 46-Year-Old WomanDocument6 pagesProlonged Fever, Hepatosplenomegaly, and Pancytopenia in A 46-Year-Old WomanFerdy AlviandoNo ratings yet
- In-Depth Review: Nonocclusive Mesenteric Ischemia: A Lethal Complication in Peritoneal Dialysis PatientsDocument6 pagesIn-Depth Review: Nonocclusive Mesenteric Ischemia: A Lethal Complication in Peritoneal Dialysis PatientsFernandoNo ratings yet
- Diagnosing Cerebral Toxoplasmosis in an Immunocompromised PatientDocument3 pagesDiagnosing Cerebral Toxoplasmosis in an Immunocompromised PatientYukii Triby-a AnniimesztNo ratings yet
- Art2 Eq6 PDFDocument6 pagesArt2 Eq6 PDFmaky yrigoyenNo ratings yet
- Case 22-2017: A 21-Year-Old Woman With Fever, Headache, and MyalgiasDocument11 pagesCase 22-2017: A 21-Year-Old Woman With Fever, Headache, and MyalgiasMaria Dolores Herrero MendozaNo ratings yet
- Pi Is 0272638621007721Document12 pagesPi Is 0272638621007721Carlos QuirogaNo ratings yet
- Tuberculous Lymphadenitis Coexists With Non-Hodgkin LymphomaDocument5 pagesTuberculous Lymphadenitis Coexists With Non-Hodgkin LymphomaThania WazintaNo ratings yet
- Caso 1Document14 pagesCaso 1Luanna DávilaNo ratings yet
- Fast Facts: Blastic Plasmacytoid Dendritic Cell Neoplasm: Shedding light on a rare diseaseFrom EverandFast Facts: Blastic Plasmacytoid Dendritic Cell Neoplasm: Shedding light on a rare diseaseNo ratings yet
- Acute Ischemic StrokeDocument9 pagesAcute Ischemic Strokepuskesmas tarikNo ratings yet
- Opioid Back PainDocument11 pagesOpioid Back PainmeganNo ratings yet
- Lower Back PainDocument18 pagesLower Back PainmeganNo ratings yet
- Press Ganey and PainDocument13 pagesPress Ganey and PainmeganNo ratings yet
- Jamainternal Thiruganasambandamoorthy 2020 Oi 200011Document8 pagesJamainternal Thiruganasambandamoorthy 2020 Oi 200011meganNo ratings yet
- Primary Paper - Say No To TPA (3 - 4.5h)Document8 pagesPrimary Paper - Say No To TPA (3 - 4.5h)meganNo ratings yet
- Primary Paper - Say No To TPA (3 - 4.5h)Document8 pagesPrimary Paper - Say No To TPA (3 - 4.5h)meganNo ratings yet
- Mapp AEM Double Sequential Defibrillation Case ControDocument9 pagesMapp AEM Double Sequential Defibrillation Case ContromeganNo ratings yet
- Jamainternal Thiruganasambandamoorthy 2020 Oi 200011Document8 pagesJamainternal Thiruganasambandamoorthy 2020 Oi 200011meganNo ratings yet
- IE - Antibiotic TableDocument5 pagesIE - Antibiotic TablemeganNo ratings yet
- Thrombolysis With Alteplase 3 To 4.5 Hours After Acute Ischemic StrokeDocument13 pagesThrombolysis With Alteplase 3 To 4.5 Hours After Acute Ischemic Strokeandreina100% (1)
- Race Conscious Medicine - Tsai Et AlDocument4 pagesRace Conscious Medicine - Tsai Et AlmeganNo ratings yet
- 10 1056@NEJMcpc2002420 PDFDocument13 pages10 1056@NEJMcpc2002420 PDFMартин ДончевNo ratings yet
- Fischer-Corbin Trauma Informed CareDocument10 pagesFischer-Corbin Trauma Informed CaremeganNo ratings yet
- INSERVICE Study GuideDocument2 pagesINSERVICE Study GuidemeganNo ratings yet
- NEJM mRNA VaccineDocument12 pagesNEJM mRNA VaccinemeganNo ratings yet
- Review QuestionsDocument1 pageReview QuestionsmeganNo ratings yet
- IE - Antibiotic TableDocument5 pagesIE - Antibiotic TablemeganNo ratings yet
- Peer IX QuestionsDocument176 pagesPeer IX Questionsmegan100% (2)
- ALiEM in Training Exam Review Quiz Sets 1 5 2nd EdDocument388 pagesALiEM in Training Exam Review Quiz Sets 1 5 2nd EdAbidi Hichem100% (2)
- Stock. Questions.Document18 pagesStock. Questions.Laura CavalcantiNo ratings yet
- Year CompassDocument10 pagesYear CompassmeganNo ratings yet
- Week 1 Fluids and Access - 100553 - 284 - 11749 - v1 1cvvlu2 PDFDocument36 pagesWeek 1 Fluids and Access - 100553 - 284 - 11749 - v1 1cvvlu2 PDFmeganNo ratings yet
- OBGYN Study GuideDocument6 pagesOBGYN Study GuidemeganNo ratings yet
- Study Guide Exam 3Document10 pagesStudy Guide Exam 3meganNo ratings yet
- EM Basic - Pocket Guide PDFDocument97 pagesEM Basic - Pocket Guide PDFHansK.Boggs100% (1)
- WKF Para-Karate Kata Competition RulesDocument14 pagesWKF Para-Karate Kata Competition RulesMohamad IbrahimNo ratings yet
- Guide To Dating For Autistic AdultsDocument3 pagesGuide To Dating For Autistic AdultsManasi PhanseNo ratings yet
- Hypnosis ScriptsDocument94 pagesHypnosis ScriptsOgist DipenNo ratings yet
- UntitledDocument21 pagesUntitledYakoub AbdelliNo ratings yet
- Best Body FitnessDocument3 pagesBest Body FitnessLavinia Chirila-StefanutNo ratings yet
- Columbia-Suicide Severity Rating Scale (C-SSRS) : Past 3 Months LifetimeDocument1 pageColumbia-Suicide Severity Rating Scale (C-SSRS) : Past 3 Months LifetimeIzabel EstevamNo ratings yet
- Mom 202108003Document2 pagesMom 202108003Ckucku AranetaNo ratings yet
- IELTS READING TEST 33: Bilingualism Advantages and Changing Health RulesDocument12 pagesIELTS READING TEST 33: Bilingualism Advantages and Changing Health RulesDollar KhokharNo ratings yet
- Passion Project Action PlanDocument3 pagesPassion Project Action PlanMeresa W. MartinNo ratings yet
- NGYouthSDGs PlaybookDocument50 pagesNGYouthSDGs PlaybookLaura noguesNo ratings yet
- Trainee's Record Book SWBLDocument12 pagesTrainee's Record Book SWBLaaronjules100% (2)
- CONCRETING TITLEDocument5 pagesCONCRETING TITLEChristian Bulaong100% (1)
- Timeless Beauty - Over 100 Tips, Secrets, and Shortcuts To Looking Great (PDFDrive)Document488 pagesTimeless Beauty - Over 100 Tips, Secrets, and Shortcuts To Looking Great (PDFDrive)Isabel Matta100% (1)
- Operational Management Assignment PDFDocument7 pagesOperational Management Assignment PDFYonas D. EbrenNo ratings yet
- Programmatic Safety Plan (PSP) : Required For High Risk Routine & Repetitive WorkDocument4 pagesProgrammatic Safety Plan (PSP) : Required For High Risk Routine & Repetitive WorkSteve ParkerNo ratings yet
- Personal Values, Beliefs and AttitudesDocument10 pagesPersonal Values, Beliefs and Attitudesapi-282066793No ratings yet
- Muscle and Bone Activities for a Strong BodyDocument13 pagesMuscle and Bone Activities for a Strong BodyAlex ValdecañasNo ratings yet
- Journal - Pone.0227695 EndometriosisDocument13 pagesJournal - Pone.0227695 EndometriosisRominaNo ratings yet
- SINP International Skilled Workers: Expression of Interest (EOI) Selection ResultsDocument14 pagesSINP International Skilled Workers: Expression of Interest (EOI) Selection ResultsSaquib.MahmoodNo ratings yet
- How To Sleep BetterDocument9 pagesHow To Sleep BetterMariaNo ratings yet
- Lab1 MEM14089A Cluster AT3A Student 191106Document12 pagesLab1 MEM14089A Cluster AT3A Student 191106Shan YasirNo ratings yet
- Hemodynamic Effects of Dexmedetomidine vs ClonidineDocument12 pagesHemodynamic Effects of Dexmedetomidine vs ClonidinezzzzNo ratings yet
- Contemporary World Exemplar T L ModuleDocument111 pagesContemporary World Exemplar T L ModuleChrizelle Mae Rodriguez100% (1)
- Workplace Hazards and Safety PoliciesDocument4 pagesWorkplace Hazards and Safety Policiesmaya_muthNo ratings yet
- Lecture 3.2.3: Erection III: Steel Construction: Fabrication and ErectionDocument4 pagesLecture 3.2.3: Erection III: Steel Construction: Fabrication and ErectionMihajloDjurdjevicNo ratings yet
- Full Download Test Bank For The Sociology of Health Illness and Health Care A Critical Approach 7th Edition PDF Full ChapterDocument35 pagesFull Download Test Bank For The Sociology of Health Illness and Health Care A Critical Approach 7th Edition PDF Full Chapterforceepipubica61uxl95% (21)
- Conduct Disorder and Somatic Health in ChildrenDocument3 pagesConduct Disorder and Somatic Health in ChildrenJeric C. ManaliliNo ratings yet
- Unit 6 Progress Test - Key Vocabulary and Grammar ConceptsDocument2 pagesUnit 6 Progress Test - Key Vocabulary and Grammar ConceptsKatren OrobchukNo ratings yet
- Optometry SeniorDocument8 pagesOptometry Seniorapi-504989033No ratings yet
- Directory 18-08-21Document34 pagesDirectory 18-08-21api-309412486100% (1)