Professional Documents
Culture Documents
I-123 Datscan Spect Brain Imaging in Parkinsonian Syndromes: Utility of The Putamen-To-Caudate Ratio
Uploaded by
nurul auliaOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
I-123 Datscan Spect Brain Imaging in Parkinsonian Syndromes: Utility of The Putamen-To-Caudate Ratio
Uploaded by
nurul auliaCopyright:
Available Formats
I-123 DaTscan SPECT Brain Imaging in Parkinsonian Syndromes:
Utility of the Putamen-to-Caudate Ratio
Manuela Matesan , Santhosh Gaddikeri, Katelan Longfellow, Robert Miyaoka, Saeed Elojeimy, Shana Elman,
Shu-Ching Hu, Satoshi Minoshima, David Lewis
From the Department of Radiology, University of Washington, Seattle, WA (MM, RM, SE, DL); Department of Diagnostic Radiology and Nuclear Medicine at Rush University
Medical Center, Chicago, IL (SG); CHI Franciscan Health, Tacoma, WA (KL); University of New Mexico, Albuquerque, NM (SE); Department of Neurology, University of
Washington, Seattle, WA (S-CH); and Department of Radiology, University of Utah, Salt Lake City, UT (SM).
ABSTRACT
BACKGROUND AND PURPOSE: Computer-based analysis of Dopamine transporter imaging (DaTscan) can aid in image
interpretation. In this study, we examined the distribution of putamen-to-caudate ratios (PCRs) obtained by using a clinically
available semiquantification method.
METHODS: Medical records of 32 patients (M:16) with a diagnosis of Parkinson’s disease (PD) (n = 22) or Parkinson’s
plus syndromes (PPS) (n = 10) based on clinical follow-up, were retrospectively reviewed. Single photon emission tomography
(SPECT) imaging was performed 4 hours after intravenous injection of 3–5 mCi [I-123]-ioflupane. Semiquantitative evaluation
using DaTQUANT software was performed. Utility of PCR with a cutoff of .7 and .8 in the diagnosis of nigrostriatal degeneration
was assessed. PD and PPS groups based on clinical assessment and caudate-to-background ratio (CBR) were assessed separately.
RESULTS: Minimum PCR for both hemispheres was .74 ± .09 (Mean ± SD, range: .58-.89), with 65.63% patients (21/32)
having PCR > .7. Mean PCR in mild nigrostriatal degeneration was .77 ± .08 (range: .62-.89) and in advanced nigrostriatal
degeneration was .73 ± .09 (range: .58-.89). Mean PCR in PD group was .73 ± .09 (range: .58-.89) and in PPS group was .75 ±
.10 (range: .61-.88).
CONCLUSIONS: Although PCR can intrinsically be a useful indication of disease, this ratio obtained in our analysis by using
one of the clinically available automatic semiquantitative methods has large variability and might not be a reliable numeric
marker in interpretation of [I-123]ioflupane studies. This may be due to difficulty in separating caudate from putamen on SPECT
images, as well as the nonuniform decreased Ioflupane uptake in both putamen and caudate.
Keywords: I-123-Ioflupane, DaTscan, quantification.
Acceptance: Received March 19, 2018, and in revised form May 14, 2018. Accepted for publication May 21, 2018.
Correspondence: Address correspondence to Manuela Matesan MD, PhD, Department of Radiology, University of Washington, 1959 NE Pacific Street,
Box 357115, Seattle 98195-0001. E-mail: mmatesan@u.washington.edu.
Acknowledgment and disclosures: There are no known conflicts of interest associated with this publication and there has been no financial support
for this work.
J Neuroimaging 2018;00:1-6.
DOI: 10.1111/jon.12530
Introduction (VOI), and more advanced automated systems using VOI or
123
I- Ioflupane single photon emission tomography (SPECT) voxel-based mathematic systems.6–9
imaging is used to evaluate the integrity of the nigrostriatal Semiquantitative methods can generate several numeric
pathway primarily through binding to the presynaptic plasma parameters such as striatum-to-background ratio, caudate-
membrane dopamine transporter, though the radiotracer can to-background ratio (CBR) or putamen-to-background ratio,
also bind to the serotonergic raphe nuclei.1 By binding to the putamen-to-caudate ratio (PCR), asymmetry between left and
dopamine transporter, 123 I- Ioflupane imaging can provide a right putamen and caudate, and caudate-putamen index.9,10
visual display of the density of the dopamine neurons in the The ratio between caudate and putamen has been suggested
substantia nigra, and can help differentiate neurodegenerative to be particularly valuable since it is background-, age- and
causes of parkinsonism in which dopamine neurons are de- camera-independent (cross-camera calibration not needed).10
creased such as Parkinson’s disease (PD) and Parkinson’s plus In this study, we assessed the distribution of PCR in a group
syndromes (PPS) from disorders that have intact dopamine of patients with Parkinson’s or Parkinson plus disease and the
neurons such as essential tremor, vascular parkinsonism, drug- capacity to predict the presence of nigrostriatal degeneration
induced parkinsonism, and psychogenic Parkinsonism.2–4 based on these ratio values.
Commonly 123 I-Ioflupane SPECT study interpretation is
made qualitatively by visual assessment, which is sufficient for
Materials and Methods
diagnosis of nigrostriatal system degeneration in most of the
Subjects
cases.5 As an aid to visual interpretation, various semiquantita-
tive methods have been proposed. These methods can be clas- This is a retrospective study that included 32 patients with an
sified into four categories: classic manual delineation of regions average age of 67 ± 10.2 years, 16 male and 16 female. Based
of interest (ROI), manual delineation of volumes of interest on the evaluation by a movement disorder specialist, there
Copyright ◦ 2018 by the American Society of Neuroimaging
C 1
were 22 patients with a diagnosis of Parkinsons’s disease and group with mild nigrostriatal degeneration (CBR more than 2;
10 patients with PPS. The PPS group included 5 patients with n = 8 patients), there were 7 patients (87.5%) with PCR > .7 and
multisystem atrophy, 3 patients with progressive supranuclear in the group with advanced nigrostriatal degeneration (CBR
palsy, 1 patient with corticobasal degeneration, and 1 patient less than 2; n = 24), there were 14 patients (58.33%) with PCR
with nonspecified PPS. Only 1 patient had autopsy performed, > .7. In PD group (mean CBR 1.62 ± .88; n = 22), there were
which confirmed the clinical diagnosis of progressive supranu- 15 patients (68.18%) with PCR more than >.7. In Parkinson’s
clear palsy. The study was approved by the Institutional Review plus disease (mean CBR: 1.5 ± .75; n = 10), there were 6
Board. patients (60%) with PCR more than .7. A separate analysis
with a cutoff value for PCR higher than .8 is also included in
Scanning Table 1.
Patients received between 111 and 185 MBq (3-5 mCi) [I-123]- Two illustrative examples, one for a patient with PD and
ioflupane and SPECT/CT images were acquired at approxi- one with PPS, are presented in Figures 3 and 4, respectively.
mately 4 hours postinjection using a dual-head gamma camera
(BrightView XCT Philips) with a low-energy high-resolution
collimator. Two to three drops of Lugol’s solution were given Discussion
orally 1 hour before the tracer injection. The patient’s head was Several parameters that analyze striatal uptake can be obtained
positioned in a head holder. A total of 128 views of 30 seconds by applying quantification software to [I-123]-ioflupane images.
each over 360 degrees were acquired on a 128 × 128 matrix. Among these, caudate-to-putamen ratio (CPR) was shown to
The field of view included the entire brain, and the rotational be particularly useful in the interpretation since it is not only
radius used was approximately 13 cm. Data reconstruction was age-independent but also camera-independent10,12,13 and is less
performed using filtered backprojection with Butterworth filter affected by the reconstruction methods. CPR was shown to
.55, power of 8, and no attenuation correction was applied. be a relevant measure to discriminate early PD from control
subjects.14,15
Data Analysis CPR values obtained on non-attenuation correction (AC)
All subjects included in this study had a positive DaTscan by images from healthy controls in the European Normal Control
visual interpretation. Database of DaTscan (ENC-DaT) showed a normal range of
Semiquantitative analysis was performed using 1.13 ± .13 (mean ± SD) for the right and 1.09 ± .13 for the
DaTQUANT software (GE Healthcare, Little Chalfont, left.10 This corresponds to a PCR cutoff for normal of >.72
England). DaTQUANT uses a fully automated registration and .74, respectively (when the mean CPR plus 2SD is used
of the patient SPECT scan to a template followed by inter- for the normal range).11 Alternatively, Brass Datscan (Hermes
rogation of uptake in the striatal regions using a volume of Medical Solutions, Stockholm, Sweden) analysis uses a refer-
interest (VOI). The template is based on the large European ence number for mean CPR of less than 1.29 (corresponding
multicenter database of healthy controls for the [123 I]-FP-CIT to a PCR mean of .78).10 A normal value of PCR higher than
SPECT (ENC-DAT trial).11 .7 has been previously suggested as a normal reference value;16
In this study, we examined the distribution of PCRs ob- however, more recently data from the PPMI trial (Parkinson
tained by using a clinically available semiquantification method Progression Marker Initiative) suggest a slightly higher normal
(DaTQUANT software). We also assessed the utility of PCR ra- value of more than .9 ± .06 (for 2 SD, normal reference of .78)
tio when .7 and respective .8 are used as cutoff values in the on the right and more than .9 ± .07 (for 2 SD, normal reference
diagnosis of nigrostriatal degeneration. The normal PCR range of .76) on the left.
for health control group was based upon the latest update of Our study assessed the utility of PCR values in a group
DaTQUANT normal database (ie, .91 ± .06, right; .90 ± .07, of 32 patients with [I-123]-ioflupane study read as positive for
left) that is also used in daily clinical interpretation. Analysis nigrostriatal system degeneration by visual interpretation and
was separately made by using two different ways to classify the validated by diagnosis of a movement disorder specialist. There
patients: one based on the clinical diagnosis (PD and PPS) and were 21 out of 32 patients (65.63%) with PCR higher than .7;
another one based on the CBR values (mild nigrostriatal degen- when .8 was used as cutoff for normal PCR, there were 10 out
eration [CBR > 2] and severe nigrostriatal system degeneration of 32 (31%) with PCR higher than .8.
[CBR ࣘ 2]). There are a couple of possible explanations for these results.
Prior studies showed that the preferential decrease of posterior
putamen uptake might not be found in patients with progressive
Results supranuclear palsy or corticobasal degeneration and decrease
For the 32 patients included in the study, the values obtained uptake in the caudate might also lead to PCR values previously
from [I-123]-ioflupane scans quantification using DaTQUANT defined as “normal range.”17 Indeed, as seen in Table 1, the
are presented in Table 1, Figures 1(A) and (B), and Figures 2(A) results did show that a smaller percentage of the patients in
and (B). PD group has PCRs higher than .8 (22.7%) compared to PPS
PCR for both hemispheres ranged from .58 to .95. However, group of patients (50%). In addition, our study included a high
because even only one site of abnormal (low) putamen uptake number of patients with CBR lower than 2 (24 patients) who
(left or right) satisfies the criteria for a positive study for nigros- have probably more advanced nigrostriatal system degenera-
triatal degeneration, only the lowest value for each patient was tion and loss of preferential decreased in putamen compared
included in the analysis. The range of PCR for the lowest value to caudate. Other contributing factor is the limited spatial reso-
was .58-.89 with a mean of .74 ± .09. A total of 21 patients out lution on SPECT images, which makes the separation between
of 32 (65.63%) had lowest PCR (left or right) above .7. In the the caudate and putamen difficult. However, Soderlund et al
2 Journal of Neuroimaging Vol 00 No 0 xxxx 2018
Table 1. Putamen-to-Caudate Ratio (PCR) Values Obtained for the 32 Patients Included in the Study. Only the Lowest PCR Value for 1 Patient
(Either Left or Right Side) Was Included in the Analysis. The Values Were Obtained Using the Semiquantification Method Provided by
DaTQUANT Software
PCR Range; Percentage of Patients Percentage of Patients with
Patients No. of Patients Average ± SD with PCR more than .7 PCR more than .8
Entire population 32 .58-.89; .74 ± .09 65.63% (21 patients) 31% (10 patients)
Parkinson’s disease 22 .58-.89; .73 ± .09 68.185% (15 patients) 22.7% (5 out of 22 patients)
Parkinson’s plus syndromes 10 .61-.88; .75 ± .1 60% (6 patients) 50% (5 out of 10 patients)
Patients with mild nigrostriatal 8 .62-.89; .77 ± .08 87.5% (7 patients) 37.5% (3 out of 8 patients)
degeneration CBR>2
Patients with severe nigrostriatal 24 .58-.89, .73 ± .09 58.33% (14 patients) 29.1% (7 out of 24 patients)
degeneration CBR ࣘ2
CBR = caudate-to-background ratio; SD = standard deviation.
Fig 1. (A) Scattergram of putamen-to-caudate ratios for the group of patients with high caudate uptake (caudate-to-background ratio more
than 2) versus low caudate uptake (caudate-to-background value less than 2) and (B) for the Parkinson’s patients versus Parkinson’s plus
patients.
have shown that ratio methods using SPECT data may be less We hypothesized that PCR values would have decreased
affected by issues related to limited spatial resolution and corre- utility in patients with CBR lower than 2, who probably have
spond to improved interobserver variability.10 Nevertheless, it more advanced nigrostriatal system degeneration and loss of
is clear that full width half maximum (FWHM) spatial measures preferential decrease in putamen compared to caudate. Sub-
of low or no activity zones in SPECT using filtered backprojec- group analysis comparing patients with CBR more or less than
tion may not be optimal for separation of caudate and putamen 2 (high and low caudate uptake groups) showed that a majority
regions, particularly if there are variances in between-subject of patients (58.3%) with CBR < 2 did demonstrate a PCR > .7,
anatomy and size. supporting our expectation that PCR would perform poorly in
Matesan et al: DaTscan: Putamen-to-Caudate Ratio 3
Fig 2. (A) Distribution of PCR values obtained for patients with caudate to background values more (8 patients) and less than 2 (14 patients)
and (B) distribution of PCR values for patients with Parkinson’s disease (22 patients) and Parkinson’s plus syndromes (10 patients).
Fig 3. A 64-year-old patient with Parkinson’s plus syndrome (multisystem atrophy-cerebellar type with ataxia and autonomic dysfunction
diagnosed by a movement disorder specialist) with significantly abnormal DaTscan by visual interpretation but high values of putamen-
to-caudate ratio. Oblique transverse [I-123]-ioflupane images without (A) and with (B) quantification display of the region of interest show
decrease uptake worse in the bilateral putamen (worse in the posterior putamen) and also right caudate. (C) Axial noncontrast CT image
showed generalized volume loss within the posterior fossa (pons, middle cerebellar peduncles, and cerebellar hemispheres), in a distribution
suggestive of multisystem atrophy-cerebellar subtype. Chronic posterior circulation ischemia was excluded by brain MRI/MR angiography.
Putamen-to-caudate ratio values are high (.94 right and .88 on the left)—bottom row.
4 Journal of Neuroimaging Vol 00 No 0 xxxx 2018
Fig 4. A 72-year-old male with Parkinson disease, abnormal [I-123]-ioflupane scan by visual interpretation and high putamen-to-caudate ratio.
Oblique transverse [I-123]-ioflupane images without (A) and with (B) quantification show severely decreased uptake in the bilateral putamen
and mild decreased uptake in bilateral caudate (worse on the right). Quantification showed decreased overall caudate-to-background ratio;
however, the putamen-to-caudate ratio values are higher than .8 (.81 both left and right).
the group of patients with advanced nigrostriatal degeneration. Thus, although PCR can intrinsically be a useful indication
However, an even higher percentage of patients with CBR > 2 of disease, this ratio obtained by using the automatic semiquan-
(87.5%) had a PCR > .7, suggesting that PCR has poor perfor- titative assessment methods (in particular investigated here—
mance irrespective of disease severity. DaTQUANT) has large variability and might not be a reliable
numeric marker in interpretation of [I-123]ioflupane studies.
Limitations of the Study This is likely due to small ROI size, associated difficulty in ac-
curately separating caudate from putamen using SPECT scans,
Our study is limited by the small sample size. In addition, while as well as the nonuniform decreased [I-123]-ioflupane uptake in
all patients had a clinical diagnosis of PD or PPS based on the putamen. In addition, in the advanced nigrostriatal degener-
clinical assessment by a movement disorder specialist, only 1 ation, there might be a nonuniform decreased [I-123]-ioflupane
patient had pathologic confirmation.18 uptake in both putamen and caudate that can further contribute
Although our analysis split the patients with CBR more or to the large variability of the results.
less than 2 (high and low caudate uptake groups), there were
mixed results in previously published studies regarding correla-
tion between disease severity and the values of [I-123]-ioflupane
uptake, probably depending on the quantification methods.14,19 References
1. Qamhawi Z, Towey D, Shah B, et al. Clinical correlates of
Only one semiquantification software (DaTQUANT) was
raphe serotonergic dysfunction in early Parkinson’s disease. Brain
used in our study, and further analysis using other methods 2015;138:2964-73.
(like BRASS or SBRquant) might bring more information re- 2. Meyer PT, Hellwig S. Update on SPECT and PET in parkinson-
garding this parameter. Even if there is a gradient of decreased ism - part 1: imaging for differential diagnosis. Curr Opin Neurol
uptake between the putamen and caudate, SPECT resolution 2014;27:390-7.
is limited, making it difficult to accurately delineate the border 3. Zijlmans JC, Daniel SE, Hughes AJ, et al. Clinicopathological in-
between the caudate and putamen, which would also affect the vestigation of vascular parkinsonism, including clinical criteria for
diagnosis. Mov Disord 2004;19:630-40.
quantification.
4. Brooks DJ. Molecular imaging of dopamine transporters. Ageing
It is known that the reconstruction methods have an im- Res Rev 2016;30:114-21.
pact in quantification;12,13 however, since PCR is a ratio, it is 5. Djang DS, Janssen MJ, Bohnen N, et al. SNM practice guideline
less influenced by the reconstruction methods (our processing for dopamine transporter imaging with 123I-ioflupane SPECT 1.0.
methods used filter backprojection and ENC-DAT data for in- J Nucl Med 2012;53:154-63.
stance used OSEM method of processing). On the other hand, 6. Linke R, Gostomzyk J, Hahn K, et al. [123I]IPT binding to the
presynaptic dopamine transporter: variation of intra- and interob-
our images were reconstructed without attenuation or scatter
server data evaluation in parkinsonian patients and controls. Eur J
correction. This can lead to a spatially variant bias in the im- Nucl Med 2000;27:1809-12.
ages that can impact the PCR ratio. Thus, while using a ratio 7. Matesan MC, Cross DJ, Lewis DH, et al. Differential alterations of
helps to mitigate differences between imaging systems and re- dopamine transporter in the striatum and midbrain in patients with
construction methods, it is not a complete solution. parkinsonian syndrome. Clin Nucl Med 2015;40:191-4.
Matesan et al: DaTscan: Putamen-to-Caudate Ratio 5
8. Badiavas K, Molyvda E, Iakovou I, et al. SPECT imaging evalu- cross-systems correction factor? Q J Nucl Med Mol Imaging
ation in movement disorders: far beyond visual assessment. Eur J 2007;51:194-203.
Nucl Med Mol Imaging 2011;38:764-73. 14. Tissingh G, Booij J, Bergmans P, et al. Iodine-123-N-omega-
9. Yokoyama K, Imabayashi E, Sumida K, et al. Computed- fluoropropyl-2beta-carbomethoxy-3beta-(4-iod ophenyl)tropane
tomography-guided anatomic standardization for quantitative as- SPECT in healthy controls and early-stage, drug-naive Parkinson’s
sessment of dopamine transporter SPECT. Eur J Nucl Med Mol disease. J Nucl Med 1998;39:1143-8.
Imaging 2017;44:366-72. 15. Seibyl JP, Marek KL, Quinlan D, et al. Decreased single-photon
emission computed tomographic [123I]beta-CIT striatal uptake
10. Soderlund TA, Dickson JC, Prvulovich E, et al. Value of semiquan-
correlates with symptom severity in Parkinson’s disease. Ann Neu-
titative analysis for clinical reporting of 123I-2-beta-carbomethoxy-
rol 1995;38:589-98.
3beta-(4-iodophenyl)-N-(3-fluoropropyl)nortropane SPECT stud-
16. Moncayo V, Barron B, Halkar R. Spectrum of findings on 123I
ies. J Nucl Med 2013;54:714-22.
Ioflupane (DatScan) Imaging: normal, abnormal, artifacts and in-
11. Varrone A, Dickson JC, Tossici-Bolt L, et al. European multicen- terpretative Pitfalls. Presented at RSNA, 2014, Chicago.
tre database of healthy controls for [123I]FP-CIT SPECT (ENC- 17. Brooks DJ. Diagnosis and management of atypical parkinsonian
DAT): age-related effects, gender differences and evaluation of dif- syndromes. J Neurol Neurosurg Psychiatry 2002;72(Suppl 1):I10-
ferent methods of analysis. Eur J Nucl Med Mol Imaging 2013;40: 6.
213-27. 18. Matesan MC, Elojeimy S, Minoshima S. 123I-FP-CIT and 99mTc-
12. Dickson JC, Tossici-Bolt L, Sera T, et al. The impact of reconstruc- HMPAO in pathologically confirmed progressive supranuclear
tion method on the quantification of DaTSCAN images. Eur J Nucl palsy. Clin Nucl Med 2016;41:e514-6.
Med Mol Imaging 2010;37:23-35. 19. Tinaz S, Chow C, Kuo PH, et al. Semiquantitative analysis of
13. Zaknun JJ, Schucktanz H, Aichner F. Impact of instrumen- dopamine transporter scans in patients with Parkinson disease. Clin
tation on DaTSCAN imaging: how feasible is the concept of Nucl Med 2018;43:e1-7.
6 Journal of Neuroimaging Vol 00 No 0 xxxx 2018
You might also like
- Articulo para Sensibilidad y EspecificidadDocument5 pagesArticulo para Sensibilidad y Especificidadkiara lopez bustosNo ratings yet
- Parámetros Cinemáticos en La Prueba de Tapping en Pacientes Con Enfermedad de ParkinsonDocument7 pagesParámetros Cinemáticos en La Prueba de Tapping en Pacientes Con Enfermedad de ParkinsonFernando Rodríguez BogasNo ratings yet
- Pro BNP MetanalisisDocument30 pagesPro BNP MetanalisisOrkito Alvarez MontenegroNo ratings yet
- Extrapyramid SynDocument7 pagesExtrapyramid SynZahra Namika AiharaNo ratings yet
- Identifikasi QRS Kompleks Pada EKG Non-StasionariDocument6 pagesIdentifikasi QRS Kompleks Pada EKG Non-StasionariMuhammad SyaifullahNo ratings yet
- Pilot Study of An Intracranial ElectroencephalographyDocument6 pagesPilot Study of An Intracranial Electroencephalographymisacho82No ratings yet
- Clinical Neurology and NeurosurgeryDocument5 pagesClinical Neurology and NeurosurgeryAffan AdibNo ratings yet
- Art:10.1007/s00330 015 3805 1Document8 pagesArt:10.1007/s00330 015 3805 1Mihaela ToaderNo ratings yet
- 10 1002@sam 11480Document16 pages10 1002@sam 11480daytdeenNo ratings yet
- Journal Neuro 6Document8 pagesJournal Neuro 6mercy taniaNo ratings yet
- Minimal Hepatic EncephalopathyDocument8 pagesMinimal Hepatic EncephalopathyGuillermoNo ratings yet
- A Neurophysiological Grading Scale For Carpal Tunnel SyndromeDocument4 pagesA Neurophysiological Grading Scale For Carpal Tunnel SyndromemikhaelyosiaNo ratings yet
- Franca 2020 AtaxiaDocument6 pagesFranca 2020 AtaxiainervavsNo ratings yet
- Color Density Spectral Array For Early EvaluationDocument7 pagesColor Density Spectral Array For Early EvaluationMunna KendreNo ratings yet
- EJMCM - Volume 9 - Issue 3 - Pages 5157-5169Document13 pagesEJMCM - Volume 9 - Issue 3 - Pages 5157-5169AjeetalbertNo ratings yet
- 123I-MIBG Cutoff Points for PDDocument8 pages123I-MIBG Cutoff Points for PDPUIGCOZARNo ratings yet
- Pluripotent Anti-Inflammatory Immunomodulatory Effects of Papaverine Against Cerebral Ischemic-Reperfusion InjuryDocument23 pagesPluripotent Anti-Inflammatory Immunomodulatory Effects of Papaverine Against Cerebral Ischemic-Reperfusion InjuryDragomir MirunaNo ratings yet
- A Study of Urinary Tract Abnormalities: Role of Low Dose MDCT UrographyDocument9 pagesA Study of Urinary Tract Abnormalities: Role of Low Dose MDCT UrographyIJAR JOURNALNo ratings yet
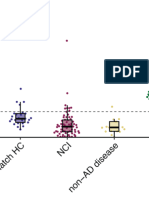
- Comparing Progression Biomarkers in Clinical Trials of Early Alzheimer’ S DiseaseDocument13 pagesComparing Progression Biomarkers in Clinical Trials of Early Alzheimer’ S DiseaseeastareaNo ratings yet
- Spal LazziDocument13 pagesSpal LazziPriscila SelingardiNo ratings yet
- Salzburg Criteria, A Useful Tool in Non-Convulsive Status Epilepticus Diagnosis: A Retrospective StudyDocument5 pagesSalzburg Criteria, A Useful Tool in Non-Convulsive Status Epilepticus Diagnosis: A Retrospective StudyGerardo Lerma BurciagaNo ratings yet
- Clinical Characteristics and PDocument10 pagesClinical Characteristics and Pmiss betawiNo ratings yet
- 2Document18 pages2Research Assistant of Dr. Rizal HamidNo ratings yet
- Prevention of Contrast Induced Renal Failure NAC ReviewDocument9 pagesPrevention of Contrast Induced Renal Failure NAC Reviewnaxo128No ratings yet
- Thesis TopicsDocument14 pagesThesis TopicskiranNo ratings yet
- Clinical EEG and Neuroscience: Improving Alzheimer's Disease Diagnosis With Machine Learning TechniquesDocument7 pagesClinical EEG and Neuroscience: Improving Alzheimer's Disease Diagnosis With Machine Learning Techniqueskubranur karaNo ratings yet
- Diagnostic Performance of Radiologic Methods in Genital Prolapse: A Systematic Review/meta-AnalysisDocument21 pagesDiagnostic Performance of Radiologic Methods in Genital Prolapse: A Systematic Review/meta-AnalysisJose CaldeiraNo ratings yet
- PF Pathfath EquipoDocument6 pagesPF Pathfath EquipoWilliams Alejandro Choroco VillegasNo ratings yet
- E016028 FullDocument8 pagesE016028 FullM Ali AdrianNo ratings yet
- Of March 15, 2024. This Information Is Current As K.M. Schmainda, M.A. Prah, Z. Zhang, B.S. Snyder, S.DDocument9 pagesOf March 15, 2024. This Information Is Current As K.M. Schmainda, M.A. Prah, Z. Zhang, B.S. Snyder, S.DAhana MukherjeeNo ratings yet
- Clinical Outcomes of Neonatal Hypoxic Ischemic Encephalopathy Evaluated With Diffusion-Weighted Magnetic Resonance ImagingDocument6 pagesClinical Outcomes of Neonatal Hypoxic Ischemic Encephalopathy Evaluated With Diffusion-Weighted Magnetic Resonance ImagingDrsandy SandyNo ratings yet
- Prospective Evaluation of Panc 3 Score in Predicting Severity of Acute PancreatitisDocument6 pagesProspective Evaluation of Panc 3 Score in Predicting Severity of Acute PancreatitisIJAR JOURNALNo ratings yet
- Update On Neuroimaging For Categorization of Parkinson's Disease and Atypical ParkinsonismDocument11 pagesUpdate On Neuroimaging For Categorization of Parkinson's Disease and Atypical ParkinsonismYo MismoNo ratings yet
- Assessment of Prognostic Value and Interreader AgrDocument7 pagesAssessment of Prognostic Value and Interreader AgreugeniaNo ratings yet
- 408.fullDocument8 pages408.fullAmany KhansaNo ratings yet
- Original Article Same-Patient Processing'' For Multiple Cardiac SPECT Studies. 1. Improving LV Segmentation AccuracyDocument7 pagesOriginal Article Same-Patient Processing'' For Multiple Cardiac SPECT Studies. 1. Improving LV Segmentation Accuracymanuel pilco riosNo ratings yet
- 2022 CTAD Poster - Cassava SciencesDocument1 page2022 CTAD Poster - Cassava Sciencesj15martiNo ratings yet
- Pet Vs Mbgi NeuroblastomaDocument12 pagesPet Vs Mbgi NeuroblastomaItzia VerduzcoNo ratings yet
- Differentiating Ischemic From Hemorrhagic Stroke Using Plasma Biomarkers: The S100B/RAGE PathwayDocument8 pagesDifferentiating Ischemic From Hemorrhagic Stroke Using Plasma Biomarkers: The S100B/RAGE PathwayMade SudarjanaNo ratings yet
- NPH RadscaleDocument8 pagesNPH RadscaleLeChuckNo ratings yet
- Questionnaire tools diagnose carpal tunnel syndromeDocument6 pagesQuestionnaire tools diagnose carpal tunnel syndromeMiguelNo ratings yet
- Neuroimage: Clinical: SciencedirectDocument8 pagesNeuroimage: Clinical: SciencedirectHOA DAONo ratings yet
- ASL Perfusion Differentiating Neoplastic From Neoplastic Intraaxial Brain LesionsDocument10 pagesASL Perfusion Differentiating Neoplastic From Neoplastic Intraaxial Brain LesionspoppyNo ratings yet
- Radiation Dose AnalysisDocument24 pagesRadiation Dose Analysisbrian mgabiNo ratings yet
- MriCS EnglishDocument8 pagesMriCS Englishstefania caselleNo ratings yet
- A Deep Learning Model To Predict RNA-Seq Expression of Tumours From Whole Slide ImagesDocument15 pagesA Deep Learning Model To Predict RNA-Seq Expression of Tumours From Whole Slide ImagesquodicNo ratings yet
- TSWJ2012 731089Document9 pagesTSWJ2012 731089samamansorNo ratings yet
- Shimizu 2017Document1 pageShimizu 2017María VélezNo ratings yet
- Albumin in Acute PancreatitisDocument1 pageAlbumin in Acute PancreatitisYuniati ValentinaNo ratings yet
- SdarticleDocument6 pagesSdarticleClaudia Alejandra Molina SepulvedaNo ratings yet
- 1726-Article Text-23983-2-10-20220330Document6 pages1726-Article Text-23983-2-10-20220330CL X-RAY IMAGESNo ratings yet
- Accuracy of Abbreviated Protocol ofDocument5 pagesAccuracy of Abbreviated Protocol ofBella YulandaNo ratings yet
- A Trial of Imaging Selection and Endovascular Treatment For Ischemic StrokeDocument10 pagesA Trial of Imaging Selection and Endovascular Treatment For Ischemic StrokelorenaNo ratings yet
- Poh 2018Document8 pagesPoh 201823Riya Khot VcetNo ratings yet
- Dalrymplealford2010 PDFDocument11 pagesDalrymplealford2010 PDFAleja ToPaNo ratings yet
- ContentServer AspDocument8 pagesContentServer AspYuda FhunkshyangNo ratings yet
- 68Ga-DOTATOC PET/CT Detects Recurrent Renal Cell CarcinomaDocument7 pages68Ga-DOTATOC PET/CT Detects Recurrent Renal Cell CarcinomaCamilleNo ratings yet
- Brain SPECT in Neurology and PsychiatryDocument13 pagesBrain SPECT in Neurology and PsychiatryCarol ArtigasNo ratings yet
- Serum Caffeine and Metabolites Are Reliable Biomarkers of Early Parkinson DiseaseDocument9 pagesSerum Caffeine and Metabolites Are Reliable Biomarkers of Early Parkinson DiseaseFirah Triple'sNo ratings yet
- JBI Critical Appraisal-Checklist For Case Reports2017Document5 pagesJBI Critical Appraisal-Checklist For Case Reports2017AriaDanurdoroNo ratings yet
- Pavel It Es 2011Document6 pagesPavel It Es 2011nurul auliaNo ratings yet
- Alves Cardoso2018Document20 pagesAlves Cardoso2018nurul auliaNo ratings yet
- Dinisoliveira2015 PDFDocument22 pagesDinisoliveira2015 PDFnaufal12345No ratings yet
- Forensic Science International: Effrosyni Michopoulou, Pierrick Negre, Efthymia Nikita, Elena F. KraniotiDocument7 pagesForensic Science International: Effrosyni Michopoulou, Pierrick Negre, Efthymia Nikita, Elena F. Kraniotinurul auliaNo ratings yet
- A Roadmap To The Safe Practice of Forensic Medicine in The COVID-19 Pandemic PDFDocument8 pagesA Roadmap To The Safe Practice of Forensic Medicine in The COVID-19 Pandemic PDFjlbermudezcNo ratings yet
- Dinisoliveira2015 PDFDocument22 pagesDinisoliveira2015 PDFnaufal12345No ratings yet
- Calce 2011Document10 pagesCalce 2011nurul auliaNo ratings yet
- Navega 2017Document7 pagesNavega 2017nurul auliaNo ratings yet
- Galeazzi Fracture: Acute and Chronic Distal Radioulnar Joint InstabilityDocument11 pagesGaleazzi Fracture: Acute and Chronic Distal Radioulnar Joint Instabilitynurul auliaNo ratings yet
- Current and Emerging Topical Scar Mitigation Therapies For Craniofacial Burn Wound HealingDocument14 pagesCurrent and Emerging Topical Scar Mitigation Therapies For Craniofacial Burn Wound Healingnurul auliaNo ratings yet
- 2019 Article 3223Document15 pages2019 Article 3223nurul auliaNo ratings yet
- Afifah 2019 IOP Conf. Ser. Earth Environ. Sci. 335 012031Document10 pagesAfifah 2019 IOP Conf. Ser. Earth Environ. Sci. 335 012031nurul auliaNo ratings yet
- Galeazzi Fracture-Dislocations: David E. Ruchelsman, MD, Keith B. Raskin, MD, and Michael E. Rettig, MDDocument9 pagesGaleazzi Fracture-Dislocations: David E. Ruchelsman, MD, Keith B. Raskin, MD, and Michael E. Rettig, MDnurul auliaNo ratings yet
- Wheeless' Textbook of OrthopaedicsDocument6 pagesWheeless' Textbook of Orthopaedicsnurul auliaNo ratings yet
- Oroaj MS Id 555832Document3 pagesOroaj MS Id 555832nurul auliaNo ratings yet
- Galeazzi Fracture - LITFL Medical Blog - Medical Eponym LibraryDocument9 pagesGaleazzi Fracture - LITFL Medical Blog - Medical Eponym Librarynurul auliaNo ratings yet
- Forensic Science International: Elmarije K. Van Straalen, Christianne J. de Poot, Marijke Malsch, Henk ElffersDocument11 pagesForensic Science International: Elmarije K. Van Straalen, Christianne J. de Poot, Marijke Malsch, Henk Elffersnurul auliaNo ratings yet
- Galeazzi Fracture Diagnosis and Surgical TreatmentDocument3 pagesGaleazzi Fracture Diagnosis and Surgical Treatmentnurul auliaNo ratings yet
- Sexual Assault and General Body Injuries: A Detailed Cross-Sectional Australian Study of 1163 WomenDocument9 pagesSexual Assault and General Body Injuries: A Detailed Cross-Sectional Australian Study of 1163 WomenYogiHadityaNo ratings yet
- Forensic Science InternationalDocument12 pagesForensic Science Internationalnurul auliaNo ratings yet
- Galeazzi Fracture Treatment & Management - Approach Considerations, Surgical Therapy, Postoperative CareDocument1 pageGaleazzi Fracture Treatment & Management - Approach Considerations, Surgical Therapy, Postoperative Carenurul auliaNo ratings yet
- Sexual Assault and General Body Injuries: A Detailed Cross-Sectional Australian Study of 1163 WomenDocument9 pagesSexual Assault and General Body Injuries: A Detailed Cross-Sectional Australian Study of 1163 WomenYogiHadityaNo ratings yet
- Determination of Sex by Osteometry of Third MetatarsalDocument6 pagesDetermination of Sex by Osteometry of Third Metatarsalnurul auliaNo ratings yet
- Sexual Assault and General Body Injuries: A Detailed Cross-Sectional Australian Study of 1163 WomenDocument9 pagesSexual Assault and General Body Injuries: A Detailed Cross-Sectional Australian Study of 1163 WomenYogiHadityaNo ratings yet
- Forensic Science International: Elmarije K. Van Straalen, Christianne J. de Poot, Marijke Malsch, Henk ElffersDocument11 pagesForensic Science International: Elmarije K. Van Straalen, Christianne J. de Poot, Marijke Malsch, Henk Elffersnurul auliaNo ratings yet
- Forensic Science International: Eoghan Casey, Thomas R. SouvignetDocument9 pagesForensic Science International: Eoghan Casey, Thomas R. Souvignetnurul aulia100% (1)
- Forensic Science International: Elmarije K. Van Straalen, Christianne J. de Poot, Marijke Malsch, Henk ElffersDocument11 pagesForensic Science International: Elmarije K. Van Straalen, Christianne J. de Poot, Marijke Malsch, Henk Elffersnurul auliaNo ratings yet
- Uncorrected Author Proof: How I Do It: Clinical ApplicationDocument7 pagesUncorrected Author Proof: How I Do It: Clinical Applicationnurul auliaNo ratings yet
- Imaging Biomarkers in Parkinson 'S Disease and Parkinsonian Syndromes: Current and Emerging ConceptsDocument25 pagesImaging Biomarkers in Parkinson 'S Disease and Parkinsonian Syndromes: Current and Emerging Conceptsnurul auliaNo ratings yet
- Fall Health & Wellness (October 2022)Document20 pagesFall Health & Wellness (October 2022)Watertown Daily TimesNo ratings yet
- OET SpeakingDocument13 pagesOET SpeakingWarangkana96% (23)
- Gastrointestinal Disorders GuideDocument14 pagesGastrointestinal Disorders GuideAnna Sofia Reyes100% (1)
- Cost Accounting Horngren 15th Edition Test BankDocument38 pagesCost Accounting Horngren 15th Edition Test Bankmitchellunderwooda4p4d100% (16)
- Uttaranchal PG College of Biomedical Sciences and HospitalDocument14 pagesUttaranchal PG College of Biomedical Sciences and HospitalpawanNo ratings yet
- Drug Reactions Med Clin North Am. 2020Document20 pagesDrug Reactions Med Clin North Am. 2020Ana Maria MoralesNo ratings yet
- Head Circumference For Age ChartDocument1 pageHead Circumference For Age ChartKaran TripathiNo ratings yet
- The Importance of Proper Body Mechanics - Keeping Your Spine HealthyDocument25 pagesThe Importance of Proper Body Mechanics - Keeping Your Spine HealthyCristine PraycoNo ratings yet
- 19 04 2020 Mumbai PDFDocument33 pages19 04 2020 Mumbai PDFShaji VkNo ratings yet
- Aproach To Patient With FeverDocument61 pagesAproach To Patient With Feverfatima fatima92% (12)
- © 2017 Lanternfish ESL @Document5 pages© 2017 Lanternfish ESL @DanniNo ratings yet
- Tuberculosis Nursing Care Plan - Ineffective Airway ClearanceDocument2 pagesTuberculosis Nursing Care Plan - Ineffective Airway ClearanceCyrus De Asis86% (36)
- Student Application FormDocument13 pagesStudent Application FormWag NasabiNo ratings yet
- A Guide To Clinical Differential Diagnosis of Oral Mucosal LesionDocument46 pagesA Guide To Clinical Differential Diagnosis of Oral Mucosal LesionFasmiya ShariffNo ratings yet
- PI Kidmin 200 MLDocument2 pagesPI Kidmin 200 MLFayza AdelNo ratings yet
- African Traditional Medicine's Contributions to Nigeria's HealthcareDocument12 pagesAfrican Traditional Medicine's Contributions to Nigeria's HealthcareAliNo ratings yet
- The Effect of Smoking OnDocument42 pagesThe Effect of Smoking OnAndreina AcevedoNo ratings yet
- Hysterosalpingography A Re - Emerging Study With CDocument7 pagesHysterosalpingography A Re - Emerging Study With CTuyul Yelsi 1No ratings yet
- Obesity-Associated Cognitive Decline: Excess Weight Affects More Than The WaistlineDocument2 pagesObesity-Associated Cognitive Decline: Excess Weight Affects More Than The WaistlineHarry HuangNo ratings yet
- Zinobacilly Final TrainingDocument12 pagesZinobacilly Final TrainingShima ElshewyNo ratings yet
- A Case Study In:: Hirschsprung DiseaseDocument18 pagesA Case Study In:: Hirschsprung DiseaseJaimie La PenaNo ratings yet
- OsteopetrosisDocument13 pagesOsteopetrosisDeep SavaliaNo ratings yet
- BREAST MCQSDocument8 pagesBREAST MCQSNehal IbrahimNo ratings yet
- Pedia Prof - OamilDocument147 pagesPedia Prof - OamilOne Click Online ShopNo ratings yet
- Perioperative nursing considerationsDocument9 pagesPerioperative nursing considerationsKoleen Kirsten100% (1)
- When and Where Did The First Quarantines Take Place?Document1 pageWhen and Where Did The First Quarantines Take Place?Raghavendra SharmaNo ratings yet
- Neurologic ExaminationDocument67 pagesNeurologic Examinationሀይደር ዶ.ር100% (1)
- Unit 3 BK Academic Connections 1 2Document22 pagesUnit 3 BK Academic Connections 1 2api-515535366No ratings yet
- Review of The Medicinal Potential of The Flora of Embu-Verde Environmental Preservation AreaDocument16 pagesReview of The Medicinal Potential of The Flora of Embu-Verde Environmental Preservation AreaJamesNo ratings yet
- MICROORGANISMS Class 8Document2 pagesMICROORGANISMS Class 8AyushNo ratings yet