Professional Documents
Culture Documents
(IM2) 6.6 Sepsis & Septic Shock - DR - Chungunco
Uploaded by
Maria Gracia YamsonOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
(IM2) 6.6 Sepsis & Septic Shock - DR - Chungunco
Uploaded by
Maria Gracia YamsonCopyright:
Available Formats
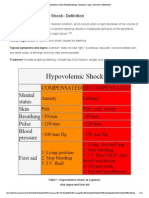
SEPSIS AND SEPTIC SHOCK INTERNAL MEDICINE
Carmen Chungunco, MD, FPCP, FPCC
May 4, 2021
6.6
OUTLINE lactate of 2 despite adequate serum resuscitation. Sa ating
I. Case patient (Case), di pa niya nafufulfill ang criteria na ito so we
II. Definition of Sepsis
would consider her as SEPSIS. We have a possible infectious
III. Sepsis
IV. Organ Dysfunction and Shock etiology which is your UTI
V. Clinical Manifestations
VI. Diagnosis
DEFINITION OF TERMS
VII. Complications
VIII. Treatment SYSTEMIC INFLAMMATORY RESPONSE (SIRS)
IX. Surviving Sepsis Guidelines Two or more of the following conditions:
X. Summary o Fever (oral temperature >38°C) or hypothermia
XI. Appendix
(<36°C)
LEGEND o Tachypnea (>24 breaths/min)
Book Recording Previous Trans Must know o Tachycardia (heart rate >90 beats/min) at rest
Important Concept o Leukocytosis (>12,000/L), leukopenia (<4,000/L),
or >10% bands
References: May have a non-infectious etiology and infectious
1. Dr. Chungunco’s Powerpoint etiology
2. 2019, 2020 & 2021 Trans
3. 20 edition HPIM
SEPSIS
CASE SIRS that has a proven or suspected microbial etiology
84 y/o female admitted for decreased sensorium o SIRS with PROVEN INFECTION – for our case,
Hypertensive on Ramipril, Amlodipine she has SIRS plus UTI
Diabetic on Sitagliptin (DPP-4 inhibitor), Metformin it is a life-threatening organ dysfunction caused by a
3-day history of dry cough and fever, anorexia and body dysregulated host response to infection
malaise
Common clinical features:
Noted to be drowsy on day of consult
o Signs of infection
o (+) organ dysfunction
AT THE ER
o Altered mentation
Drowsy, disoriented
o Tachypnea
BP=80/40 mmHg, HR=125/min, RR=24/min, T=38.7C
o Hypotension
Pink palpebral conjunctivae, anicteric sclerae, (-) cervical o Hepatic, renal, or hematologic dysfunction
lymphadenopathies (CLAD), (-) neck vein engorgement OLD CRITERIA: suspected (or documented) infection
No retractions, Clear breath sounds plus ≥ 2 SIRS criteria
(-) Heaves/thrills, AB at 5th LICS MCL, good S1, (-) NEW CRITERIA (2016): suspected (or documented)
murmurs infection and an acute increase in ≥ 2 sepsis-related
Soft abdomen, NABS, nontender, liver and spleen not organ failure assessment (SOFA) points)
palpable
(-) Edema, warm extremities, pulses +1 SEPTIC SHOCK
Warm extremities due to vasodilation A subset of sepsis in which underlying circulatory and
cellular/metabolic abnormalities lead to substantially
LAB RESULTS increased mortality risk
CBC – Hgb 11 g/dl, WBC 33,000, 85% neutrophils Common clinical features:
Chem: RBS 220, creatinine 1.8 mg/dl, Na 160, K 4 o Signs of infection
CXR – no infiltrates o Altered mentation
Urinalysis – (+) nitrites, WBC 70/hpf o Oliguria
o Cool peripheries
Question: What is the most appropriate diagnosis for this o hyperlactemia
patient’s condition? 2003 criteria: suspected (or documented) infection plus
A. Systemic Inflammatory Response Syndrome persistent arterial hypotension (systolic arterial pressure
(SIRS) <90 mmHg; mean arterial pressure <60mmHg; or change
B. Sepsis in SBP by >40 mmHg less from baseline) This was very
C. Severe Sepsis tedious and very confusing for a lot of people.
D. Septic Shock 2016 CRITERIA (currently used): Suspected (or
(Refer to the 2003 and2016 definition of septic shock) If we use the old definition, documented) infection plus vasopressor therapy
then the patient in the case is in septic shock. However, in the needed to maintain mean arterial pressure at ≥65 mmHg
new definition, it is septic shock only when you are in and serum lactate >2.0 mmol/L despite adequate fluid
vasopressor therapy to maintain this MAP at 65 and serum resuscitation I want you to remember the latest definition
RAMIREZ & SUELO EDITOR: NICDAO Page 1 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
of septic shock importance of that is seen in the clinical setting
now.
Gram-negative negative bacteria most likely to cause
sepsis
o E. coli, Klebsiella, Pseudomonas
o Pseudomonas — nosocomial-acquired
pneumonia; cyano-green/blue green specimen
(sputum, urine, etc.)
Pulmonary/respiratory (most common) and
intraabdominal infections – eightfold more likely to cause
sepsis or severe sepsis
I.PATHOPHYSIOLOGY
Figure 1. Sequence
The term severe sepsis is not used anymore
Table 1. Sequential (or sepsis-related) organ failure assessment
(SOFA) score Figure 2. Select mechanisms implicated in the pathogenesis of sepsis-
Again, to delineate between sepsis and septic shock, it really is the use induced organ and cellular dysfunction
of fluid resuscitation tsaka vasopressor therapy to maintain the blood Basically, it is brought about by extreme inflammatory
pressure and serum lactate levels (SEPTIC SHOCK) response. There is an inflammatory response that happens
and the only difference is now we have a pathogen that’s
SEPSIS
causing the inflammatory response.
Increasing incidence
Here’s the pathogen on the left corner, when it comes
o Due to increasing age and pre-existing
in, there are immune cells that recognize the pathogen and
comorbidities
start a chain reaction of inflammatory mediators, the cytokines,
o Use of immunosuppressive drugs, indwelling
which will now cause the inflammation to occur. That includes
catheters and other mechanical devices
in the microcirculation, a lot of thrombosis, so there is thrombus
(implants), antibiotic resistance This is why in the
production, there is leakage of the endothelial cells or the
first lecture that we had we talked about antibiotic
endothelial leak or dysfunction, and there’s a lot of adhesions
stewardship kasi if we give antibiotics left and
and transmigrations of the leukocytes. In the microcirculation,
right, we do run the risk of causing resistance.
because of all of these processes, you now cause some tissue
Many things can bring in sepsis in that record. So what is
edema which goes into the interstitium. So the tissue edema
sepsis? It is usually triggered most often by microbial
now increases the 02 diffusion distance between the
pathogens which do NOT usually cause systemic
microcirculation going to the cell. Because there’s a lot of
disease in immunocompetent hosts. Usually happens in
edema in the interstitium, the oxygen diffusion from the
people who are immunocompromised. Either because of
microcirculation to the cell becomes harder. And because of
illness or immunocompromised because of a certain state.
that, tissue oxygenation goes down, lactate is produced, and
Sometimes it can be a “perfect storm”. Somebody who is
now we have a lot of lactate that is produced and causing a lot
usually immunocompetent but it happens that they were
of damage as well. So now with all of these, we will get
immunocompromised relatively because they were under
hypotension, hypovolemia and vasodilation.
a lot of stress, working long hours, not eating, and not
The inflammatory response is the same for SIRS and
really taking good care of themselves. And this exposure
sepsis. Give me an example of SIRS without an infection? For
to a pathogen in high concentration, remember we said
instance in burns, patient who have burns, there is
that for you to get any infection, it has to be a “perfect
inflammatory response. They are edematous but not really due
storm” between the host, the pathogen and the
to pathogen. Allergies is also an inflammatory response but
environment that you’re in. This is what also increases
again, there is no pathogen in that situation. If there is
your risk for sepsis. It is usually trigger by a pathogen,
pathogen that is triggering the inflammatory response, it is
o Not recognized by host receptors
sepsis.
o Elaborate toxins or other virulence factors Some
of these you encountered in microbiology last The host response to sepsis involves multiple mechanisms that
year. Marami pinamemorize sa inyo anong lead to decreased oxygen delivery (DO2) at the tissue level.
toxins, anong virulence factors, what number, the
RAMIREZ & SUELO EDITOR: NICDAO Page 2 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
The duration, extent, and direction of these interactions are Figure 3. Pathogenesis
modified by the organ under threat, host factors (e.g., age, Here very clearly we see the difference. For gram
genetic characteristics, medications), and pathogen factors negative bacteria, the lipopolysaccharide is the one in the cell
(e.g., microbial load and virulence). wall of the bacteria and the one that really triggers the
The inflammatory response is typically initiated by an response. Whereas in the gram positive bacteria, the teichoic
interaction between pathogen-associated molecular patterns acid and the lipoteichoic acid come in and once they are
(PAMPs) expressed by pathogens and pattern recognition recognized by the cell surface, they go down the pathway (see
receptors expressed by innate immune cells on the cell
illustration) Proinflammatory cytokines are produced, platelet
surface (Toll-like receptors [TLRs] and C-type lectin receptors
activating factor, Nitric oxide, coagulation, and now cause an
[CLRs]), in the endosome (TLRs), or in the cytoplasm (retinoic
acid inducible gene 1–like receptors and nucleotide-binding inflammatory cascade. Now you have diffused endothelial
oligomerization domain–like receptors [NLRs]). disruption and microcirculation defects causing global tissue
The resulting tissue damage and necrotic cell death lead to hypoxia and organ dysfunction. Eventually, if the organ
release of damage associated molecular patterns (DAMPs) dysfunction and the vasodilation is severe, you now get a
such as uric acid, high-mobility group protein B1, S100 proteins, septic shock.
and extracellular RNA, DNA, and histones.
These molecules promote the activation of leukocytes, II. ORGAN DYSFUNCTION AND SHOCK
leading to greater endothelial dysfunction, expression of Widespread vascular endothelial injury due to
intercellular adhesion molecule (ICAM) and vascular cell cytokines: major mechanism for multiorgan dysfunction
adhesion molecule 1 (VCAM-1) on the activated endothelium,
Tumor Necrosis Factor (TNF) – induce vascular
coagulation activation, and complement activation.
endothelial cells to produce and release:
This cascade is compounded by macrovascular changes
o Cytokines (IL-1 and 6)
such as vasodilation and hypotension, which are exacerbated
by greater endothelial leak tissue edema, and relative Increase blood flow to the target tissues
intravascular hypovolemia. (rubor)
Subsequent alterations in cellular bioenergetics lead to greater Enhance permeability of local blood vessels
glycolysis (e.g., lactate production), mitochondrial injury, (tumor)
release of reactive oxygen species, and greater organ Recruit neutrophils and other cells (calor)
dysfunction Elicit pain (dolor)
Etiology Sepsis is a pro-inflammatory state.
o Procoagulant molecules
Microbial invasion of the bloodstream is not essential
Promote coagulation. It may also put the
because local inflammation can also elicit distant organ
patient at risk for DIC
dysfunction and hypotension
o Platelet activating factor
Blood cultures yield bacteria or fungi in only ~20–40% of
o Nitric oxide and other mediators – induce
severe sepsis and 40–70% of septic shock.
vasodilation and may contribute to shock
Microbiologic results were positive in 70% of individuals
Endothelial cell activation can promote increased vascular
considered infected;
permeability, microvascular thrombosis, DIC, hypotension
o 62% were gram-negative bacteria: E. coli &
Tissue oxygenation decreases
pseudomonas were most common
Poorly functioning "septic" organs usually appear normal
o 47% were gram positive bacteria: Staph aureus
at autopsy → Little necrosis → Organ dysfunction during
was most common
severe sepsis has a basis that is principally biochemical,
o 19% were fungi (Candida species)
not structural. It’s the exchange of oxygen from the
microcirculation going to the cell that is diminished so the
organs die because there’s not enough tissue
oxygenation.
HALLMARK OF SEPTIC SHOCK:
o Decrease in peripheral vascular resistance
despite increased levels of vasopressor
catecholamines So remember, septic shock
happens because of the inflammation, the
vasodilation has occurred, some of the fluids has
gone into the interstitium, and because it is
vasodilated, blood pressure drops. There is no
vascular resistance to hold it up. Catecholamines
will come out as a “fight-or-flight” response kaya
lang, what will catecholamine supposed to do?
Catecholamines are supposed to cause
vasoconstriction. However in overwhelming sepsis
leading to septic shock, even the catecholamines
are not enough to generate good vasoconstriction
causing blood pressure to drop.
RAMIREZ & SUELO EDITOR: NICDAO Page 3 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
In patients with severe sepsis, persistence of leukocyte IV. DIAGNOSIS
hyporesponsiveness has been associated with an NO SPECIFIC DIAGNOSTIC TEST FOR SEPSIS!
increased risk of dying; at this time, the most predictive Definitive etiologic diagnosis requires identification of the
biomarker is a decrease in the expression of HLA-DR organism from blood or local site of infection
(class II) molecules on the surfaces of circulating o Blood cultures from 2 different sites (from two
monocytes (Trans 2019) different venipuncture sites) and we also get from
the site of infection. In this patient, if we’re
PHASES OF SEPTIC SHOCK thinking UTI, we do need to send some urine
From Trans 2020: specimen as well.
Hypodynamic vasodilatory phase – compromised o Negative (blood) cultures in many cases (prior
oxygen delivery to tissues ↑ blood lactate, ↓ central antibiotic use, slow-growing organism like TB,
venous oxygen saturation absence of microbial invasion of bloodstream i.e
Hyperdynamic vasodilatory phase – after fluid UTI/cystitis) Kung negative ang blood culture, this
administration does not mean that the patient doesn’t have
o Normal or high cardiac output, oxygen sepsis. You really have to go to the clinical
consumption declines despite adequate oxygen picture.
delivery; normal or increased blood lactate Possible markers of sepsis:
o Normalization of central venous oxygen o Procalcitonin (if value is >2)
saturation may reflect improved oxygen delivery, A new marker that is being used to
decreased oxygen uptake by tissues, or left-to- check if the patient have a bacterial
right shunting infection vs a viral infection.
Prognosticating factor
III. CLINICAL MANIFESTATION Tells you “likelihood” of sepsis
Clinical manifestations are due to the local and systemic May produce false positives
host response to invading microbes not because of the o Lactate
direct response of the toxins or the bacteria The longer that tissues are not well
Fever (may be absent in elderly, immunocompromised, perfused, there is formation of lactic acid
uremia, alcoholism) Serum lactate of >1.5x elevated =
Hyperventilation – an early sign of the septic response likelihood of sepsis
Why would the patient go into tachypnea? Where else do
you see tachypnea happening? Pneumonia, metabolic CRITERIA
acidosis (Kussmaul’s phenomenon). What do you think o SOFA (Sequential Organ Failure Assessment)
is causing the metabolic acidosis in sepsis? Lactic o qSOFA (quick SOFA) - shorter version of the
acidosis. sofa
MUDPILES
Encephalopathy (decreased sensorium/cognition)
because not enough perfusion going to the brain
Hypotension and poor perfusion – most commonly on
the digits
DIC
Skin lesions
o Cellulitis, pustules, bullae, or hemorrhagic lesions
o N. meningitidis should be suspected if cutaneous
petechiae or purpura is seen
o Presence of Ecthyma gangrenosum suggests P.
aeruginosa infection.
Why do you think skin lesion manifests? So remember
when you have low blood pressure, they will all go to the
central organs first, leading the skin and the other
peripheral organs last. So syempre because of that, you
will get poor perfusion and they are very prone to skin
breakage and stress ulceration
Stress ulceration – for the GI tract
Cholestatic jaundice, acute liver injury, ischemic
Figure 4. Algorithm of SOFA
bowel necrosis – As we said, everything will be given to
Basically the patient comes in with a suspected
the skin organs first.
infection, we use our quick SOFA to see if they are at high risk
for sepsis. Quick SOFA includes these 3 parameters:
Respiratory rate, mental status and systolic blood
RAMIREZ & SUELO EDITOR: NICDAO Page 4 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
pressure. If more than 2 of these is affected, then we assess 6. Renal: Creatinine and Urine Output
for evidence of organ dysfunction and organ dysfunction is
seen more with the SOFA variables (Refer to the diagram). If V. LABORATORY FINDINGS
patient has more than 2 of these variables, then the patient is Leukocytosis with a left shift or leukopenia
in sepsis. And if you include vasodepressor and serum lactate Thrombocytopenia (sign of hematologic organ dysfunction)
that we mentioned earlier, then it is septic shock. The SOFA Hyperbilirubinemia
scores allow us to know whether the patient is at high risk for Proteinuria
mortality while in the hospital. Prolongation of the thrombin time, decreased fibrinogen,
and the presence of D-dimers
Quick (q) SOFA Points o suggests the presence of DIC
1 point for each criteria (Remember: “HAT”) Azotemia
1. Hypotension: Systolic BP ≤ 100 mmHg Elevated aminotransferases – SGOT and SGPT are very
2. Altered mental status: GCS < 15 high lalo na if it’s ischemic it will go up to the thousands.
3. Tachypnea: RR≥ 22/min Respiratory alkalosis (early) progressing to metabolic
acidosis
qSOFA ≥2 suggests high in-hospital mortality Hypoxemia
ICU admission Hyperglycemia because of the adrenaline response
OTHER LABORATORY FINDINGS:
o CXR: Could be normal or could show underlying
pneumonia, vol. overload, ARDS
o ECG: tachycardia or nonspecific ST-T wave
abnormalities
o Most diabetic pxs w/ sepsis develop hyperglycemia
(severe infection can precipitate DKA which could
exacerbate hypotension)
o Hypoglycemia occurs rarely and may indicate
adrenal insufficiency
o Serum albumin level declines as sepsis continues
VI. COMPLICATIONS
CARDIOPULMONARY COMPLICATIONS
o ALI/ARDS
Progressive diffuse pulmonary infiltrates and
Figure 5. Factore of qSOFA & SOFA arterial hypoxemia occurring within 1 week of
a known insult
Sequential Organ Failure Assessment (SOFA) Points
Acute Lung Injury (ALI) develops in 50% of
patients with septic shock / severe sepsis
o Normal or increased cardiac output
o Decreased systemic vascular resistance
o Normal or increased cardiac output and decreased
systemic vascular resistance distinguish septic shock
from cardiogenic, extracardiac obstructive, and
hypovolemic shock
ADRENAL INSUFFICIENCY – critical illness–related
corticosteroid insufficiency (CIRCI) from secondary cause
Table 2: Sequential Organ Failure Assessment (SOFA) Points
o Common for those who stay longer in the ICU
o Normal cortisol levels but there is increased body
**check for larger picture, demand, making it insufficient
Scoring system if the patient is in sepsis and what are the o Maybe due to abnormalities in glucocorticoid
chances of in-hospital mortality. receptors or increased conversion of cortisol to
Parameters: cortisone due to HIGH DEMAND caused by stress
1. Respiration: PaO2/FiO2 – ARDS parameter – you need o Major clinical manifestation of CIRCI: hypotension
to get an ABG for the arterial oxygenation and that is refractory to fluid replacement and requires
PaO2/FiO2 ratio pressor therapy
2. Coagulation: Platelet ct RENAL COMPLICATIONS – most renal failure is due to
3. Liver: Bilirubin Acute Tubular Necrosis
4. CV: MAP = SBP+DBP/DBP – in response to o induced by hypotension or capillary injury
vasopressors o Oliguria, azotemia, proteinuria, and nonspecific
5. CNS: GCS urinary casts are frequently found
RAMIREZ & SUELO EDITOR: NICDAO Page 5 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
COAGULOPATHY – thrombocytopenia/DIC Fecalysis
NEUROLOGIC COMPLICATIONS UTZ (solid organs), CT scan (intestines)
o Hypotension causing decrease perfusion in the brain o For intraabdominal infections
causing septic encephalopathy Peritoneal aspiration if there is ascites
o "Critical illness" polyneuropathy – may prevent
weaning from ventilator support and produce distal ANTIBIOTICS
motor weakness We recommend that administration of IV antimicrobials be
o Delirium (Acute encephalopathy) – often an early initiated as soon as possible after recognition and within
manifestation of sepsis (10-70%) 1h for both sepsis and septic shock. (Strong
IMMUNOSUPPRESSION recommendation, moderate quality of evidence)
o Loss of delayed type hypersensitivity reactions to We recommend empiric broad-spectrum therapy or
common antigens, failure to control the primary combination therapy with one or more antimicrobials to
infection, and increased risk for secondary infection cover all likely pathogens. (Strong recommendation,
moderate quality of evidence)
VII. TREATMENT
We suggest empiric combination therapy (using at least
GOALS two antibiotics of different antimicrobial classes) for
1. URGENT MEASURES TO TREAT INFECTIONS
instance somebody who has pneumonia, you will give
Empiric antibiotics started within 1 hour of diagnosis (refer piperacillin-tazobactam and maybe a macrolide. For UTI,
to Table 325-3 in the appendix) you can also give piperacillin-tazobactam while waiting for
o Should be given IV, with adjustment for those with the cultures aimed at the most likely bacterial pathogen(s)
impaired renal function for the initial management of septic shock. (Weak
o Empiric ANTIFUNGAL therapy strongly considered if recommendation; low quality of evidence)
patient receiving broad spectrum antibiotics or o Must cover gram-negative bacteria.
parenteral nutrition has been neutropenic for ≥5 days o If with abscess, must also cover anaerobes.
or has been in ICU for a prolonged period.
2. PROVIDE HEMODYNAMIC AND RESPIRATORY SUPPORT INITIAL RESUSCITATION
Measured by BP, mentation, urine output, skin perfusion We recommend that in the resuscitation from sepsis-
induced hypoperfusion, at least 30ml/kg of intravenous
3. REMOVE SOURCE OF INFECTION crystalloid fluid be given within the first 3 hours.
Seek the site of infection carefully lalo na sa lungs, (Strong recommendation; low quality of evidence) Kahit na
abdomen, and urinary tract. sabihin na “why do we need to resuscitate wala naman
Catheters should be removed, and the tip cultured. siya fluid losses hindi naman siya nagbleed hindi naman
For those with NGT, consider paranasal sinusitis din as a siya nag diarrhea, why do we have to give fluid
source of infection resuscitation? Precisely because of the main problem of
In a neutropenic patient, check for cutaneous sites of sepsis which is vasodilation. All of the inflammatory
tenderness and erythema particularly sa perianal region mediators have caused vasodilation so we need to give a
(consider AIDS) lot of fluids so that the microcirculation is well perfused.
Example: Patient is 60 kg, how much fluid are we going to
SURVIVING SEPSIS CAMPAIGN: INTERNATIONAL
GUIDELINES FOR SEPSIS AND SEPTIC SHOCK give in the first 3hrs? 1.8L in 3 hrs. Pero hindi lahat yan
ibibigay niyo as fast drip. Ang gagawin niyo is you divide
“Sepsis and septic shock are medical emergencies and we that into the 3 hours which is about 600mL per hour. This
recommend that treatment and resuscitation begin maybe a problem for example in patients with cardiac
immediately.” dysfunction let’s say may heart failure si patient, then
– Best Practice Statement, SSC 2016 maybe we can adjust. But for the most part if there is no
problem with the cardiac status of the patient, you have to
SOURCE CONTROL push that 600cc per hour for the first 3 hours. You have to
We recommend that a specific anatomic diagnosis of do this with close monitoring to the patient.
infection requiring emergent source control be o Crystalloids (NSS, LR) are recommended!
identified or excluded as rapidly as possible in (usually NSS)
patients with sepsis or septic shock, and that any required Albumin may be added to crystalloid if the
source control intervention be implemented as soon as patient requires substantial amounts of
medically and logistically practical after the diagnosis is crystalloid
made. Hydroxyethyl starches (HES) are NOT
o Cultures recommended
Blood We recommend that following initial fluid resuscitation,
Urine additional fluids be guided by frequent reassessment of
Lungs (Sputum, Endotracheal Aspirate) hemodynamic status. (Best Practice Statement)
Gastrointestinal
Goals of Initial Resuscitation:
RAMIREZ & SUELO EDITOR: NICDAO Page 6 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
o CVP maintained at 8-12 cmH2O to prevent However, do not delay the antibiotic therapy. Start therapy
pulmonary edema within an hour.
o Maintain Mean Arterial Pressure at >65 mmHg
(systolic pressure >90 mmHg)
o Urine output should be kept at >0.5 mL/kg per hour
We suggest guiding resuscitation to normalize lactate in
patients with elevated lactate levels as a marker of
tissue hypoperfusion (weak recommendation, low quality
of evidence)
VASOACTIVE AGENTS
What if after the first hour of giving 600cc of fluid hydration
sometimes you even go beyond that, the BP is still very low.
You know that if the BP is low for a very long time will already
cause hypoperfusion for the organ. After you give fluid boluses,
you can already start vasopressors if your blood pressure does
not go up. Normally, if it’s 80/40 and you give around 600cc in
the first hour or kahit 300 in the first half hour, the blood
pressure will start to pick up a little bit. If it doesn’t, you really
have to start vasopressors.
We recommend Norepinephrine as the first-choice
vasopressor for all patients with sepsis. It is the first
choice because it will cause vasoconstriction and hopefully
bring up the BP. (strong recommendation, moderate Table 4. Initial Antimicrobial Therapy for Severe Sepsis with No
quality of evidence). Obvious Source in Adults with Normal Renal Function. For empirical
If the patient is at maximum NE, We suggest adding either antibiotic therapy the appropriate choice depends on the suspected
site of infection, the location of infection onset (i.e., the community, a
vasopressin (up to 0.03 U/min) or epinephrine to
nursing home, or a hospital), the patient’s medical history, and local
norepinephrine with the intent of raising MAP to target, or microbial susceptibility patterns
adding vasopressin (up to 0.03 U/min) to decrease
norepinephrine dosage. (weak recommendation; low 1. SEPTIC SHOCK for immunocompetent adult – piperacillin-
tazobactam, cefepime or meropenem.
quality of evidence) If they have a device in their body (e.g. catheter) –
TARGET MAP = 65mmHg or higher give vancomycin loading dose
o MAP Formula: 2. NEUTROPENIA –cefepime, meropenem or piperacillin
tazobactam
MAP = (SP + 2 DP) / 3
3. SPLENECTOMY - Ceftriaxone
So for our patient, BP is 80/40.
MAP = [80 + 2 (40) ] / 3 o Remarks: Appropriate routine microbiologic
MAP = 53.33 (low because cultures always include at least TWO sets of
target is 65) blood cultures (aerobic and anaerobic)
Dopamine is suggested as an alternative vasopressor
to norepinephrine ONLY in HIGHLY SELECTED ANTIMICROBIAL THERAPY AND ANTIBIOTIC
PATIENTS: STEWARDSHIP
o Low risk of tachyarrhythmia and absolute or We recommend that empiric antimicrobial therapy be
relative bradycardia narrowed once pathogen identification and sensitivities
are established and/or adequate clinical improvement is
noted
We suggest that an antimicrobial treatment duration of 7-
10 days is adequate for most serious infections
associated with sepsis and septic shock sometimes up to
14 days depending on the patient’s situation.
We recommend daily assessment for de-escalation of
Table 3. Clinical guidelines for the management of patients with sepsis
antimicrobial therapy in patients with sepsis and
and septic shock – RESUSCITATION bigger picture in the appendix septic shock
o Criteria for de-escalation
DIAGNOSIS Afebrile for 24 hours
Improved mental status (conscious)
We recommend that appropriate routine microbiologic
Able to tolerate oral meds
cultures (including blood) be obtained BEFORE starting
Clinically better (good BP, urine output, etc)
antimicrobial therapy in patients with suspected sepsis
We suggest that measurement of procalcitonin levels
and septic shock if doing so results in no substantial delay
in the start of antimicrobials. (Best Practice Statement) be used to support shortening the duration of antimicrobial
RAMIREZ & SUELO EDITOR: NICDAO Page 7 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
therapy in sepsis patients. Procalcitonin levels is the signal
to go to the oral antibiotics therapy.
CORTICOSTEROIDS
What role do corticosteroids play in sepsis? Generally, sepsis
causes adrenal insufficiency because of the overwhelming
inflammatory response. The body is in a fight-or-flight mode
and one of them is to bring up cortisol. If that happens, we
have a patient who is hypotensive and kahit magbigay tayo ng
vasopressors and fluids, hindi tumataas ang kanilang BP. In
those cases, that’s the only time that we can assume that there
might be some adrenal insufficiency and give some IV Table 5. Clinical guidelines for the management of patients
hydrocortisone. with sepsis and septic shock bigger picture in the appendix
We suggest AGAINST using intravenous 1. INFECTION CONTROL
hydrocortisone to treat septic shock patients IF adequate 2. RESPIRATORY SUPPORT –
fluid resuscitation and vasopressor therapy are able to Target tidal volume of 6mL/kg body weight.
restore hemodynamic stability. If this is not achievable, we Prone Positioning – we do this a lot in our
suggest intravenous hydrocortisone at a dose of 200 covid patients trying to see if we can avoid
mg per day. (Weak recommendation; low quality of them being intubated or if they’re intubated,
evidence) we do prone positioning so they can be
For CIRCI: Hydrocortisone (50 mg IV every 6 hours) extubated as quickly as possible.
should be given Conservative fluid strategy
Read the table above
VENTILATOR THERAPY (HARRISON’S) 3. GENERAL SUPPORTIVE CARE
Indicated for progressive hypoxemia, hypercapnia, Vasopressor
neurologic deterioration, or respiratory muscle failure Hydrocortisone
Sustained tachypnea (RR of >30 breaths/min) is a Sedation – sometimes being in the ICU for
harbinger of impending respiratory collapse; therefore, patients who have sepsis is very difficult.
mechanical ventilation is necessary Sometimes they fight the ventilators and try
Stress ulcer prophylaxis to take out all of the tubes so they do need a
o Histamine H2 receptor antagonist may decrease little bit of sedation
the risk of GI hemorrhage in ventilated patient Prophylaxis for DVT – because they are
quite sedentary and they can be
hypercoagulable as you have seen in the
OTHER RECOMMENDATIONS
inflammatory cascade, procoagulants are
Glucose control: 180mg/dL
produced. So those who have sepsis have a
Nutrition: Enteral feeding as soon as possible
really high risk for DVT
oral or NGT
Stress ulcer prophylaxis (PPIs) – to prevent
Use of prokinetics –allow the gut to move forward to
gastritis and GI bleeding.
avoid ileus from happening
PROGNOSIS (HARRISON’S)
SETTING GOALS OF CARE 20-35% of patients with severe sepsis and 40-60% with
We recommend that goals of care and prognosis be septic shock die within 30 days
discussed with patients and families. (Best Practice Age and prior health status are the most important risk
Statement) factors
o Guarded prognosis for the first 72 hours
Septic shock is also a strong predictor of both short and
We recommend that the goals of care be incorporated into long-term mortality
treatment and end-of-life care planning, utilizing palliative
care principles where appropriate. (Strong
recommendation; moderate quality of evidence) PREVENTION (HARRISON’S)
Reduce number of invasive procedures undertaken
We suggest that goals of care be addressed as early as
Limit use of indwelling vascular and bladder catheters
feasible, but no later than within 72 hours of ICU
Reduce incidence and duration of profound neutropenia
admission. (Weak recommendation; low quality of
evidence) Aggressively treat nosocomial and community acquired
infections
Indiscriminate use of antimicrobial agents and glucocorticoids
should be avoided, and optimal infection-control measures
should be used.
RAMIREZ & SUELO EDITOR: NICDAO Page 8 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
o Get blood culture
VIII. BACK TO THE PATIENT o HCO3 infusion
What is the most appropriate diagnosis for this patient’s o Start epinephrine drip
condition? o Start norepinephrine drip
Not sure if A or E, kasi septic shock na and by
A. Urinary Tract Infection
definition, nabigyan na po sya ng fluids over 3 hours
B. Systemic Inflammatory Response Syndrome (SIRS) and still not responsive. Also, empiric antibiotics should
C. Sepsis be given within 1 hour of diagnosis.
D. Septic Shock I-aassume na ba na nabigyan sya ng antibiotics? Wala
po sila sagot
SEPSIS – considering that the patient was not given any
intervention yet like vasopressors, fluids, etc. A 48 year old diabetic patient is brought to the ER for decreased
SEPTIC SHOCK – consider this if after an hour in the ER with sensorium. Upon examination, she is drowsy, with BP=80/60,
HR=120/min, RR=24/min and temp=39C, lung and cardiac exams are
intervention if the patient is still hypotensive unremarkable, a gangrenous non-healing wound with foul-smelling
purulent discharge is noted on her left leg. Her relatives claim that the
Sepsis and SIRS – warm extremities due to vasodilation patient had been self-medicating the wound for the past month with no
Cardiogenic shock and hypovolemia - cold and clammy improvement.
Which is the most appropriate diagnosis for this patient’s
extremities
condition?
o Systemic inflammatory response syndrome (SIRS)
What other diagnostic tests will we do? o Sepsis
o Urine and blood culture o Septic shock
Why do you need blood cultures? If your o Refractory septic shock
urine CS is positive for bacteria and o Multiple-organ dysfunction syndrome (MODS)
sensitivities are there, is that enough to
Which is NOT included in the criteria for systemic inflammatory
diagnose sepsis? Not really because Urine
response syndrome (SIRS)?
CS will tell us a localized source of infection o Temperature < 36C
but not really a systemic one. Sepsis tends o WBC >12,000 u/L
to be a systemic response. Usually it should o Heart rate >100/min
be in the blood as well like bacteremia and o Bacteremia
septicemia can confirm the diagnosis (if o May be due to non-infectious etiology
we’re just talking about labs. But in our
Which of the following statements about sepsis is TRUE?
patient we have a clinical picture, urine CS
o Tissue factor activates both the intrinsic and
is enough to diagnose sepsis. extrinsic clotting pathways.
o Intravascular coagulation enables the spread of
What is the best management for this patient? microorganisms through the bloodstream.
o Hydration: 30mL/kg for the first 3 hrs o Protein C levels are markedly elevated in patients with
If no improvement, give inotrope – sepsis.
Norepinephrine o Serum cortisol acts as a pro-inflammatory stimulus.
o Empiric Antibiotics: within an hour (i.e. 3rd-gen o All of the above
RATIONALE:
cephalosporins) and broad spectrum (PipTazo)
B: Intravascular thrombosis, a hallmark of the local
o Consider giving CORTICOSTEROIDS if necessary
(indications are discussed above) inflammatory response, may help wall off invading
microbes and prevent infection and inflammation from
o Admit to ICU until stable
spreading to other tissues.
o check for fluid status: Urine Output - insert a C: Clotting is also favored by impaired function of the protein
catheter; JVP C-protein S inhibitory pathway and depletion of antithrombin
Sunken eyeballs are only used as a parameter and proteins C and S
D: Glucocorticoids inhibit cytokine synthesis by monocytes in
for PEDIA px vitro; the increase in blood cortisol levels that occurs early in
o If hypoxemic: Intubate the systemic response presumably plays a similarly inhibitory
o Feeding: NGT since pt. is drowsy; preferred over role
TPN total parenteral nutrition (may cause further
Which is the first-line treatment for this patient’s hypotension?
infection and more expensive) o Crystalloids and colloids
o Ventilatory support with positive end-expiratory
IX. QUIZZES FROM PREVIOUS BATCH pressure
Patient with infection, drowsy, BP = 80/60, tachycardic, did not o Nitric oxide analogues
respond to administration of IV fluid. What category? o Oxygen supplementation
o Severe sepsis o Intravenous inotropic support such as dopamine
o Sepsis
o Septic Shock END OF TRANS
o Refractory Septic Shock
o Multiorgan dysfunction
Initial management for septic shock?
o Start antibiotic therapy
RAMIREZ & SUELO EDITOR: NICDAO Page 9 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
X. TISSUE A. Start prophylactic proton-pump inhibitors
CASE QUESTIONS B. Do tracheostomy instead
CASE 1: 65-year old female is seen at the ER for 3-day C. Suction secretions frequently
history of fever, chills, cough, and dyspnea. D. Start prophylactic antibiotic
E. Maintain the head of bed at an angle >30
PE: Looks weak , BP 100/60 , HR 125, RR 26, TEMP 39C,
degrees
Warm ext, (+) Dullness on percussion, right lower lung field QUIZ
LABS: CBC: Hgb 10g/dL, WBC 18,000, Neutrophils 80%,
Creatinine 1.8mg/dL 1. Which of the following is TRUE regarding the
CXR: consolidation, Shows right lower lobe pathophysiology of sepsis and septic shock?
A. Organ dysfunction in severe sepsis mainly occurs due to
1. DIAGNOSIS? SEPSIS widespread vascular endothelial injury caused by release of
2. Which of the following is the most appropriate pro-inflammatory cytokines
additional initial treatment for this patient? B. The hallmark of septic shock is increased peripheral
A. Normal saline vascular resistance with low levels of vasopressor
B. Hydrocortisone catecholamines
C. Blood transfusion with PRBC C. Bacterial pathogens directly attack the different organs in
D. Norepinephrine severe sepsis causing widespread dysfunction.
D. Gram positive pathogens are more likely to cause sepsis.
CASE 2: ST, an 80-yeard old diabetic male, is admitted for
an acute infarct in the right cerebral hemisphere. He is
intubated upon admission due to respiratory distress. On his SUMMARY
4th hospital day, he develops ventilator-associated SIRS Two or more of the following
pneumonia and is started on IV antibiotics. However, he is
conditions:
then noted to have BP 70/50, HR 110/min, RR 30/min, and
T 38.6C. He is given IL of intravenous normal saline as fast o Fever (oral temperature
drip but the blood pressure does not improve. A urine >38°C) or hypothermia
catheter is placed to monitor his output. (<36°C)
o Tachypnea (>24
1. Which of the following is most effective in breaths/min)
preventing catheter-associated UTI? o Tachycardia (heart rate
A. Administration of a prophylactic antibiotic
>90 beats/min) at rest
B. Changing the catheter every 72 hours
C.Checking for and treating asymptomatic o Leukocytosis
bacteriuria (>12,000/L), leukopenia
D.Removing the urinary catheter as soon as (<4,000/L), or >10%
possible bands
E. Using silver-impregnated urinary catheters Infectious or non-infectious
2. What is the single most important strategy in
preventing this patient from getting a hospital-
SEPSIS SIRS that has a proven or
acquired infection? suspected microbial etiology
A. Foregoing the weaning process and immediately life-threatening organ dysfunction
extubating the patient caused by a dysregulated host
B. Administration of a prophylactic antibiotic response to infection
C. Advising this patient to wear a mask at all time
NEW CRITERIA (2016):
D. Placing this patient in reverse isolation
E. Following strict staff hand hygiene practices suspected (or documented)
3. Which is the most appropriate diagnosis of this infection and an acute
patient’s present condition? increase in ≥ 2 sepsis-related
A. Severe sepsis organ failure assessment
B. Septic shock (SOFA) points)
C. SIRS SEPTIC A subset of sepsis in which
D. Sepsis SHOCK
E. Refractory septic shock underlying circulatory and
4. Goals of initial resuscitation cellular/metabolic
A. CVP maintained at 10-12 cmH2O abnormalities lead to
B. MAP at <65mmHg substantially increased
C. Urine Output of 0.5ml/kg per hour mortality risk
D. LDH < 40
2016 CRITERIA (currently
5. What should be your next step in management?
A. Start norepinephrine drip used): Suspected (or
B. Change IV antibiotics for broader spectrum documented) infection plus
coverage vasopressor therapy needed to
C. Start dopamine drip maintain mean arterial pressure
D. Administer sodium bicarbonate at ≥65 mmHg and serum lactate
E. Administer hydrocortisone IV >2.0 mmol/L despite adequate
6. Which of the following is the most appropriate
fluid resuscitation
measure to prevent another ventilator-associated
pneumonia in this patient? PHASES
RAMIREZ & SUELO EDITOR: NICDAO Page 10 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
o Hypodynamic hospital mortality
vasodilatory phase – ICU admission
compromised oxygen COMPLICATIONS
delivery to tissues ↑ Cardiopulmonary
blood lactate, ↓ central Adrenal insufficiency
venous oxygen Renal complications
saturation
Coagulopathy
o Hyperdynamic
Neurological complications
vasodilatory phase –
Immunosuppression
after fluid administration
TREATMENT
CLINICAL MANIFESTATIONS
GOAL
Clinical manifestations are due to the local and 1. Urgent measures to treat infections
systemic host response to invading microbes not 2. Provide Hemodynamic and respiratory support
because of the direct response of the toxins or the 3. Remove source of infection
bacteria Source control specific anatomic diagnosis of
o Fever (may be absent in elderly, infection requiring emergent source
immunocompromised, uremia, alcoholism) control be identified or excluded as
o Hyperventilation – an early sign of the rapidly as possible in patients
septic response
Antibiotics Administration of IV
o Encephalopathy (decreased
antimicrobials be initiated as
sensorium/cognition)
soon as possible after
o Hypotension and poor perfusion – most
recognition and within 1h for
commonly on the digits
both sepsis and septic
o DIC
shock.
o Skin lesions- Cellulitis, pustules, bullae, or
Empiric broad-spectrum
hemorrhagic lesions
therapy or combination
o Stress ulceration – for the GI tract
therapy with one or more
o Cholestatic jaundice, acute liver injury,
antimicrobials to cover all
ischemic bowel necrosis – As we said,
likely pathogens.
everything will be given to the skin organs
Empiric combination
first.
therapy (using at least two
DIAGNOSIS
NO SPECIFIC DIAGNOSTIC TEST FOR SEPSIS! antibiotics of different
antimicrobial classes)
Definitive Identification of the organism from
etiologic blood or local site of infection Initial Resuscitation from sepsis-induced
diagnosis o Blood cultures from 2 resuscitation hypoperfusion, at least 30ml/kg of
different sites (from two intravenous crystalloid fluid be
different venipuncture sites) given within the first 3 hours.
o Negative (blood) cultures in Vasoactive Norepinephrine as the first-
many cases (prior antibiotic agent choice vasopressor for all
use, slow-growing organism patients with sepsis.
like TB, absence of microbial Dopamine is suggested as
invasion of bloodstream i.e an alternative vasopressor
UTI/cystitis) to norepinephrine ONLY in
Possible Procalcitonin (if value is >2) HIGHLY SELECTED
markers Lactate PATIENTS
SOFA (Sequential Organ Failure Corticosteroid AGAINST using intravenous
Assessment) hydrocortisone to treat septic shock
qSOFA (quick SOFA) - shorter version of the patients IF adequate fluid
sofa resuscitation and vasopressor
therapy are able to restore
1 point for each criteria (Remember: hemodynamic stability. If this is not
“HAT”) achievable, we suggest intravenous
4. Hypotension: Systolic BP ≤ 100 hydrocortisone at a dose of 200 mg
mmHg per day. (Weak recommendation; low
5. Altered mental status: GCS < quality of evidence)
15 Ventilator Indicated for progressive hypoxemia,
6. Tachypnea: RR ≥ 22/min Therapy hypercapnia, neurologic deterioration,
or respiratory muscle failure
qSOFA ≥2 suggests high in-
RAMIREZ & SUELO EDITOR: NICDAO Page 11 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
APPENDIX
Table 2: Sequential Organ Failure Assessment (SOFA) Points
Table 3&5. Clinical guidelines for the management of patients with sepsis and septic shock (Lifted from HPIM).
RAMIREZ & SUELO EDITOR: NICDAO Page 12 of 13
INTERNAL MEDICINE SEPSIS AND SEPTIC SHOCK LECTURE 6.6
Table 4. Initial Antimicrobial Therapy for Severe Sepsis with No Obvious Source in Adults with Normal Renal Function. For empirical
antibiotic therapy the appropriate choice depends on the suspected site of infection, the location of infection onset (i.e., the community,
a nursing home, or a hospital), the patient’s medical history, and local microbial susceptibility patterns
RAMIREZ & SUELO EDITOR: NICDAO Page 13 of 13
You might also like
- Management of Tuberculosis: A guide for clinicians (eBook edition)From EverandManagement of Tuberculosis: A guide for clinicians (eBook edition)No ratings yet
- SepsisDocument3 pagesSepsisPhilip Poerworahjono100% (3)
- Sepsis and Septic ShockDocument4 pagesSepsis and Septic ShockFebyan AbotNo ratings yet
- Evaluation and Management of Suspected Sepsis and Septic Shock in AdultsDocument62 pagesEvaluation and Management of Suspected Sepsis and Septic Shock in AdultsGiussepe Chirinos CalderonNo ratings yet
- Liver Cirrhosis: Causes, Complications and ManagementDocument55 pagesLiver Cirrhosis: Causes, Complications and ManagementAnonymous vUEDx8100% (1)
- Diarrhea in ChildrenDocument42 pagesDiarrhea in ChildrenIPNATC NEPALNo ratings yet
- Stemi Vs NstemiDocument31 pagesStemi Vs NstemiFadhilAfifNo ratings yet
- TYPES OF SHOCK: HYPOVOLEMIC, CARDIOGENIC, DISTRIBUTIVE & OBSTRUCTIVEDocument2 pagesTYPES OF SHOCK: HYPOVOLEMIC, CARDIOGENIC, DISTRIBUTIVE & OBSTRUCTIVEhanh247No ratings yet
- SepsisDocument14 pagesSepsislengkong100% (9)
- Comprehensive Adult Health History ReviewDocument8 pagesComprehensive Adult Health History ReviewJoseph HernandezNo ratings yet
- Pathophysiology Septic ShockDocument26 pagesPathophysiology Septic ShockTinea Sycillia100% (1)
- Arterial Blood Gas Analysis-Gaya3'sDocument29 pagesArterial Blood Gas Analysis-Gaya3'spolarbear121212100% (2)
- History Case: "Red Currant Jelly" StoolDocument60 pagesHistory Case: "Red Currant Jelly" Stoolaella gracieNo ratings yet
- Disseminated Intravascular CoagulationDocument2 pagesDisseminated Intravascular CoagulationGerardLum100% (1)
- Sepsis and Septic ShockDocument4 pagesSepsis and Septic Shocksarguss14100% (4)
- Hypovolemic Shock Pathophysiology, Symptoms, Signs, Treatment - EHealthStarDocument15 pagesHypovolemic Shock Pathophysiology, Symptoms, Signs, Treatment - EHealthStarKaloy KamaoNo ratings yet
- Acute Respiratory Distress Syndrome - ReviewDocument13 pagesAcute Respiratory Distress Syndrome - ReviewMr. L0% (1)
- Critical Care NursingDocument159 pagesCritical Care Nursinggretchen marie80% (5)
- Novilyn C. Pataray BSN - Ii Hemophilia: St. Paul College of Ilocos SurDocument1 pageNovilyn C. Pataray BSN - Ii Hemophilia: St. Paul College of Ilocos SurCharina AubreyNo ratings yet
- Nursing Care of Cardiovascular DisordersDocument38 pagesNursing Care of Cardiovascular Disordersprototypeallhell100% (1)
- Kawasaki DiseaseDocument14 pagesKawasaki DiseaseFransiskus Beat Batmomolin100% (1)
- Cardiogenic ShockDocument2 pagesCardiogenic ShockChristine QuironaNo ratings yet
- Diverticular DiseaseDocument15 pagesDiverticular DiseaseRogie SaludoNo ratings yet
- Heart Failure COncept MapDocument2 pagesHeart Failure COncept MapJrBong SemaneroNo ratings yet
- Severe Sepsis and Septic ShockDocument39 pagesSevere Sepsis and Septic ShockYogi Agil MurdjitoNo ratings yet
- Sepsis, Septic Shock, MODSDocument19 pagesSepsis, Septic Shock, MODSPaul Zantua80% (5)
- SyncopeDocument28 pagesSyncopeDurgesh PushkarNo ratings yet
- Urinary Tract InfectionDocument4 pagesUrinary Tract InfectionGerardLum100% (2)
- Upper Respiratory Tract InfectionDocument9 pagesUpper Respiratory Tract InfectionCHRISTIE MONTANO100% (1)
- Status Asthmaticus in ChildrenDocument76 pagesStatus Asthmaticus in ChildrenJesterCruzNo ratings yet
- Paediatric Septic Shock ManagementDocument37 pagesPaediatric Septic Shock ManagementJauhari DesloNo ratings yet
- Hypovolemic ShockDocument2 pagesHypovolemic Shockatilano_patrickNo ratings yet
- Stroke and Cerebrovascular DiseaseDocument14 pagesStroke and Cerebrovascular DiseaseMarwan M.No ratings yet
- Viral HepatitisDocument40 pagesViral Hepatitisinvisibleyetinvincible100% (4)
- Cardiovascular DrugsDocument12 pagesCardiovascular DrugshannahcoNo ratings yet
- 0413 Massive Upper GI Bleeding PDFDocument12 pages0413 Massive Upper GI Bleeding PDFhectulNo ratings yet
- Peripheral Vascular Disease PDFDocument28 pagesPeripheral Vascular Disease PDFمبدر حامد100% (1)
- Prepared and Presented by Marc Imhotep Cray, M.DDocument30 pagesPrepared and Presented by Marc Imhotep Cray, M.DMarc Imhotep Cray, M.D.100% (1)
- Pathophysiology PneumoniaDocument2 pagesPathophysiology PneumoniaChiro Rouy Malaluan100% (2)
- Hirschsprung's Disease and The Allied Disorders PDFDocument278 pagesHirschsprung's Disease and The Allied Disorders PDFriri siahaanNo ratings yet
- Acute Myocardial InfarctionDocument14 pagesAcute Myocardial InfarctionJardee DatsimaNo ratings yet
- Preoperative and Post Liver Transplant Nursing Care Plan, Nursing ProcessDocument2 pagesPreoperative and Post Liver Transplant Nursing Care Plan, Nursing ProcessOctoober100% (3)
- Acute Lymphocytic LeukemiaDocument7 pagesAcute Lymphocytic Leukemiamildred alidon100% (1)
- Sickle Cell DiseaseDocument15 pagesSickle Cell DiseaseNatukunda DianahNo ratings yet
- CellulitisDocument8 pagesCellulitisgrool29rNo ratings yet
- Pulmonary HypertensionDocument36 pagesPulmonary HypertensionDiana_anca6100% (2)
- Idiopathic Thrombocytopenic Purpura Case StudyDocument38 pagesIdiopathic Thrombocytopenic Purpura Case Studygiadda100% (9)
- Clavicle FractureDocument6 pagesClavicle FractureYbis LizarzaburuNo ratings yet
- Name: Muhyee S. Idjad Year&Sec: BSNIII-B: What Is in A Emergency Cart?Document3 pagesName: Muhyee S. Idjad Year&Sec: BSNIII-B: What Is in A Emergency Cart?Yeng Cries50% (2)
- 2 Acute Myocardial InfarctionDocument15 pages2 Acute Myocardial InfarctionpauchanmnlNo ratings yet
- Initial PE and Labs History Initial Impression: Location &Document1 pageInitial PE and Labs History Initial Impression: Location &kaydee.arNo ratings yet
- CvaDocument42 pagesCvad_94No ratings yet
- Hyponatremia Algorhythm Concept MapDocument2 pagesHyponatremia Algorhythm Concept Mapnursing concept mapsNo ratings yet
- Acute Rheumatic FeverDocument37 pagesAcute Rheumatic FeverQadriyah Ramadhani100% (1)
- Anatomy and Types of Respiratory Tract InfectionsDocument50 pagesAnatomy and Types of Respiratory Tract InfectionsAvi Verma100% (2)
- Clinical Concept Map-7Document1 pageClinical Concept Map-7Brandi Offield100% (1)
- Community Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandCommunity Acquired Pneumonia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- A Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Hypovolemia, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Respiratory Alkalosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandRespiratory Alkalosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- (OPHTHA) - 10.1 CaseDiscussion-Dr. AtienzaDocument32 pages(OPHTHA) - 10.1 CaseDiscussion-Dr. AtienzaMaria Gracia YamsonNo ratings yet
- The Strife For Meaning: PhilsophyDocument22 pagesThe Strife For Meaning: PhilsophyMaria Gracia YamsonNo ratings yet
- Catechism For Filipino Catholics (CFC)Document368 pagesCatechism For Filipino Catholics (CFC)Xylee Gonzales86% (57)
- The Strife For Meaning: PhilsophyDocument22 pagesThe Strife For Meaning: PhilsophyMaria Gracia YamsonNo ratings yet
- Earth and Life - 2ND SemDocument3 pagesEarth and Life - 2ND SemMaria Gracia YamsonNo ratings yet
- (OPHTHA) 7.1-Pediatric Ophthalmology-Strabismus and Amblyopia - Dr. AtienzaDocument14 pages(OPHTHA) 7.1-Pediatric Ophthalmology-Strabismus and Amblyopia - Dr. AtienzaMaria Gracia YamsonNo ratings yet
- UCSP - Challenges individuals to evaluate and criticize their own cultureDocument4 pagesUCSP - Challenges individuals to evaluate and criticize their own cultureMaria Gracia YamsonNo ratings yet
- 2-Analyzing The Meaning of The Data and Drawing ConclusionsDocument37 pages2-Analyzing The Meaning of The Data and Drawing ConclusionsMaria Gracia YamsonNo ratings yet
- OPHTHA 8.0 Neuro Ophthalmology Fundamentals Dr. AtienzaDocument14 pagesOPHTHA 8.0 Neuro Ophthalmology Fundamentals Dr. AtienzaMaria Gracia YamsonNo ratings yet
- (OPHTHA) 9.1 - Ocular Manifestations of Systemic Disease - Dr. AtienzaDocument12 pages(OPHTHA) 9.1 - Ocular Manifestations of Systemic Disease - Dr. AtienzaMaria Gracia YamsonNo ratings yet
- (OPHTHA) 9.1 - Ocular Manifestations of Systemic Disease - Dr. AtienzaDocument12 pages(OPHTHA) 9.1 - Ocular Manifestations of Systemic Disease - Dr. AtienzaMaria Gracia YamsonNo ratings yet
- M8L3LEC - Benign Prostatic Hyperplasia (Special Lecture-Online)Document5 pagesM8L3LEC - Benign Prostatic Hyperplasia (Special Lecture-Online)Maria Gracia YamsonNo ratings yet
- M8L3LEC - Benign Prostatic Hyperplasia (Special Lecture-Online)Document5 pagesM8L3LEC - Benign Prostatic Hyperplasia (Special Lecture-Online)Maria Gracia YamsonNo ratings yet
- (OPHTHA) - 10.1 CaseDiscussion-Dr. AtienzaDocument32 pages(OPHTHA) - 10.1 CaseDiscussion-Dr. AtienzaMaria Gracia YamsonNo ratings yet
- OPHTHA 8.0 Neuro Ophthalmology Fundamentals Dr. AtienzaDocument14 pagesOPHTHA 8.0 Neuro Ophthalmology Fundamentals Dr. AtienzaMaria Gracia YamsonNo ratings yet
- (IM2) 6.6 Sepsis & Septic Shock - DR - ChunguncoDocument13 pages(IM2) 6.6 Sepsis & Septic Shock - DR - ChunguncoMaria Gracia Yamson100% (1)
- (OPHTHA) 7.1-Pediatric Ophthalmology-Strabismus and Amblyopia - Dr. AtienzaDocument14 pages(OPHTHA) 7.1-Pediatric Ophthalmology-Strabismus and Amblyopia - Dr. AtienzaMaria Gracia YamsonNo ratings yet
- Sensitivity of LUS Compared To Chest CT For The Screening of COVID-19Document18 pagesSensitivity of LUS Compared To Chest CT For The Screening of COVID-19Maria Gracia YamsonNo ratings yet
- OPHTHA 8.0 Neuro Ophthalmology Fundamentals Dr. AtienzaDocument14 pagesOPHTHA 8.0 Neuro Ophthalmology Fundamentals Dr. AtienzaMaria Gracia YamsonNo ratings yet
- Prueba de Tamizaje - Demencia (Ad8) PDFDocument3 pagesPrueba de Tamizaje - Demencia (Ad8) PDFOscar J AlmedaNo ratings yet
- Alzheimers Screening MSEDocument7 pagesAlzheimers Screening MSEMaria Gracia YamsonNo ratings yet
- TX article-HPV Vaccine Against Cervical Infection Trial-2015Document13 pagesTX article-HPV Vaccine Against Cervical Infection Trial-2015Maria Gracia YamsonNo ratings yet
- The Role of LUS As A Frontline Diagnostic Tool in The Era of COVID-19 OutbreakDocument8 pagesThe Role of LUS As A Frontline Diagnostic Tool in The Era of COVID-19 OutbreakMaria Gracia YamsonNo ratings yet
- RAI and Pregnancy OutcomesDocument8 pagesRAI and Pregnancy OutcomesMaria Gracia YamsonNo ratings yet
- Lung Injury in Patients With or Suspected COVID-19Document22 pagesLung Injury in Patients With or Suspected COVID-19Maria Gracia YamsonNo ratings yet
- Mod 1.3 INTRO TO EVIDENCE-BASED MED MEDRES1A2021Document7 pagesMod 1.3 INTRO TO EVIDENCE-BASED MED MEDRES1A2021Maria Gracia YamsonNo ratings yet
- Point of Care LUS Is Useful When Screeing For CoVid-19Document22 pagesPoint of Care LUS Is Useful When Screeing For CoVid-19Maria Gracia YamsonNo ratings yet
- Diagnosing Covid-19 Pneumonia in A Pandemic SettingDocument43 pagesDiagnosing Covid-19 Pneumonia in A Pandemic SettingMaria Gracia YamsonNo ratings yet
- Forgotten But Not Gone? A Probable Case of Wet BeriberiDocument6 pagesForgotten But Not Gone? A Probable Case of Wet BeriberiMaria Gracia YamsonNo ratings yet
- Medical Management of Postpartum HemorrhageDocument17 pagesMedical Management of Postpartum HemorrhageCatherine PingNo ratings yet
- Amniotic Fluid EmbolismDocument13 pagesAmniotic Fluid EmbolismDrNorNo ratings yet
- Obstetric Nursing DrillsDocument14 pagesObstetric Nursing DrillsClarence AnescoNo ratings yet
- Risk For Diseases Cheat SheetDocument1 pageRisk For Diseases Cheat SheetRick Frea100% (5)
- Acquired Coagulation DisordersDocument11 pagesAcquired Coagulation DisordersAli AhmedNo ratings yet
- Robbins Pathology Chapter 14 - RBCsDocument7 pagesRobbins Pathology Chapter 14 - RBCsscorpiosphinx79100% (10)
- Farmakoterapi Coagulation DisorderDocument55 pagesFarmakoterapi Coagulation DisorderNur Astuty PurnamasariNo ratings yet
- Hematologic DisorderDocument16 pagesHematologic Disorderjulesubayubay5428No ratings yet
- A - Covid 19Document3 pagesA - Covid 19JESUS YOBALNo ratings yet
- DIC Blood Component TherapyDocument30 pagesDIC Blood Component TherapySameer KumarNo ratings yet
- Blood Transfusion Protocols in NeonatesDocument12 pagesBlood Transfusion Protocols in NeonatesSupriya M A SuppiNo ratings yet
- Nycocard Brochure 01 PDFDocument2 pagesNycocard Brochure 01 PDFelfarik sulistonNo ratings yet
- Pathphysiology CurriculumDocument14 pagesPathphysiology Curriculumapi-3728690No ratings yet
- Hypothermia Alcohol Related IllnessDocument42 pagesHypothermia Alcohol Related IllnessSritharan GaneshamoorthyNo ratings yet
- Unit 4 Study Guide PathoDocument10 pagesUnit 4 Study Guide Pathoangieswenson100% (1)
- Disseminated Intravascular Coagulopathy Dic 1 1Document25 pagesDisseminated Intravascular Coagulopathy Dic 1 1api-394684626No ratings yet
- Blood Components Dosage and Their Administration (Compatibility Mode)Document7 pagesBlood Components Dosage and Their Administration (Compatibility Mode)Chandra SekarNo ratings yet
- Disseminated Intravascular CoagulationDocument37 pagesDisseminated Intravascular CoagulationhipoclaudioNo ratings yet
- Care of The Clients With Cancer: Prof. Hashim N. Alawi Jr. RN, MANDocument78 pagesCare of The Clients With Cancer: Prof. Hashim N. Alawi Jr. RN, MANjisooNo ratings yet
- Abnormal ObstetricsDocument286 pagesAbnormal ObstetricsJen Ilagan100% (3)
- 62 Coagulation Failure in ObstetricsDocument28 pages62 Coagulation Failure in ObstetricscollinsmagNo ratings yet
- HIPERLEUKOSITOSIS & LEUKOSTASISDocument16 pagesHIPERLEUKOSITOSIS & LEUKOSTASISShapira alNo ratings yet
- Hematologic Disorders Test Drill For Ikonek 2Document4 pagesHematologic Disorders Test Drill For Ikonek 2Jan Cyrel ColomaNo ratings yet
- Circulatory Shock in Children:: An OverviewDocument10 pagesCirculatory Shock in Children:: An Overviewsugarp_3No ratings yet
- Multiple Organ Dysfunction SyndromeDocument4 pagesMultiple Organ Dysfunction SyndromeJenny SisonNo ratings yet
- Pre Gestational ConditionsDocument68 pagesPre Gestational ConditionsQuinonez Anna MarieNo ratings yet
- Immuno-Serology & Blood Banking Case Study: Systemic Lupus ErythematosusDocument6 pagesImmuno-Serology & Blood Banking Case Study: Systemic Lupus ErythematosusRomie SolacitoNo ratings yet
- Acute Lymphocytic LeukemiaDocument8 pagesAcute Lymphocytic LeukemiaWendy EscalanteNo ratings yet
- Hematologic Test TherapyDocument71 pagesHematologic Test Therapyyasin shifaNo ratings yet
- Cardiac Biomarkers: Cardiac Enzymes and BiomarkerDocument21 pagesCardiac Biomarkers: Cardiac Enzymes and Biomarkeranamika sharmaNo ratings yet