Professional Documents
Culture Documents
Module 3
Uploaded by
arrian arraCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Module 3
Uploaded by
arrian arraCopyright:
Available Formats
NCM 107 – Care of the Mother, Child and Adolescent
S.Y. 2021-2022 | 1st Semester | Preliminary Term
Module 3 – Reproductive Life Planning
Description
Reproductive life planning includes all the decisions an individual or couple make about
whether and when to have children, how many children to have and how they are spaced. This
module will provide the student an understanding of the different methods of reproductive life
planning and the advantages and disadvantages, and the risk factors associated with each. It
will also tackle how the couple can utilize the chosen method considering their religious,
personal and cultural beliefs.
Learning Outcomes
LO1 Integrate concepts of different methods of reproductive life planning and the
advantages and disadvantages, and the risk factors associated with each in the formulation and
application of appropriate nursing care during childbearing and childrearing years.
LO3 Assess clients for reproductive life planning needs
LO4 Formulate nursing diagnosis/es related to reproductive planning
LO5 Implement safe and quality nursing interventions related to reproductive planning.
LO6 Conduct individual/group health education activities such as educating adolescents
about the use of condoms as a safer practice as well as to prevent unintended pregnancy.
LO7 Evaluate with the client the health outcomes of nurse-client relationship.
Module Outline
I. Reproductive life planning
II. Commonly used birth control methods
III. Assessment for reproductive life planning needs
IV. Nursing Diagnoses Related to Reproductive Life Planning
V. Interventions Related to Reproductive Life Planning
VI. Evaluating Outcomes Related to Reproductive Life Planning
Module 3 – Reproductive Life Planning 1
Module
I. Reproductive life planning Includes all decisions an individual or a couple make about
having children, including
1. If and when to have children
2. How many children to have?
3. The length of time between having children
Counseling may include the topics of avoiding conception, increasing fertility, and/or
what to do if contraception has failed.
An ideal contraceptive should be
a. Safe
o Effective
o Compatible with religious and cultural beliefs and personal preferences of user
and partner
o Free of bothersome side effects
o Convenient to use and easy to obtain
o Affordable and needing few instructions for use
o Free of effects on future pregnancies after discontinuation
II. Commonly Used Birth Control Methods
A. Natural Family Planning
Natural family planning methods, also called periodic abstinence methods, involve no
introduction of chemical or foreign material into the body. The effectiveness of these
Module 3 – Reproductive Life Planning 2
methods varies greatly from a 2% ideal failure rate to about 25% failure rate, depending
mainly on the couple’s ability to refrain from having sexual relations on fertile days.
1. Abstinence
Abstinence has a theoretical 0% failure rate and is also the most effective way to prevent STIs.
Because it is difficult for many couples to adhere to abstinence, the method has a high failure
rate.
2. Lactation Amenorrhea Method (LAM)
When a woman is breastfeeding, there is a natural suppression of bothovulation and menses.
Lactation amenorrhea method is a safe birth control method with failure rate of about 1% to
5% if:
a. An infant
1. under 6 months of age
2. Exclusive breastfeeding
3. No supplementary feedings
b. Menses has not returned
3. Coitus interruptus
Coitus interruptus or withdrawal method is one of the oldest methods of contraception. The
couple proceeds with coitus until the moment of ejaculation. Then, the man withdraws and
spermatozoa are emitted outside the vagina. Unfortunately, ejaculation may occur before
withdrawal is completed and, despite the caution used, some spermatozoa may be deposited in
the vagina. Furthermore, spermatozoa may be present in pre-ejaculation fluid, fertilization may
occur even if withdrawal seems controlled. For these reasons, coitus interruptus is only about
82% effective and can also lead to STIs.
4. Fertility Awareness Method
Module 3 – Reproductive Life Planning 3
Fertility awareness methods rely on detecting when a woman will be fertile so she can use
periods of abstinence during that time. There are a variety of ways to determine a fertile
period:
• Calendar
• Body temperature
• Consistency of cervical mucus
A fertile period exists from about 5 days before ovulation to 3 days after.
• Calendar (Rhythm) Method
The calendar method requires the couple to abstain from coitus on the days of a menstrual
cycle when the woman is fertile. To plan for this, the woman keeps a diary of about six
menstrual cycles. To calculate for “safe” days, she subtracts 11 from her longest cycle and 18
from shortest cycle. To avoid pregnancy, the couple should avoid coitus during these days
Example: menstrual cycle ranging from 25 to 29 days
Shortest cycle = 25 days – 18 days = 7
Longest cycle = 29 days – 11 days = 18
FERTILE PERIOD = 7th to 18th day of the menstrual cycle.
• Basal Body Temperature
Just before the day of ovulation, a woman’s basal body temperature (BBT) falls about 0.5oF. At
the time of ovulation, her BBT rises 1oF (0.2oC) because of the rise in progesterone
(thermogenic hormone) with ovulation. To use this method, the woman takes her temperature
each morning immediately after waking before she rises form bed or undertakes any activity;
this is her BBT. As soon as a woman notices a slight dip in temperature followed by an increase
she knows she has ovulated. She refrains from having coitus for the next three days.
A problem with assessing BBT for fertility awareness is that many factors can affect BBT. For
example, a temperature rise caused by illness, activity or warm environment could be mistaken
as the signal for ovulation.
• Cervical Mucus Method (Billing’s Method)
Module 3 – Reproductive Life Planning 4
Each month before ovulation, the cervical mucus is thick and does not stretch when pulled
between the thumb and finger. Just before ovulation, mucus secretion increases. On the day
of ovulation (the peak day), it becomes copious, thin, watery, and transparent. It feels slippery
(like egg white) and stretches at least 1 inch before the strand breaks (spinnbarkeit). All the
days on which cervical mucus is copious, and for at least 3 to 4 days afterward, are considered
to be fertile days, or days on which the woman should abstain from coitus to avoid conception.
This method has a potentially high failure because of difficulty in interpreting mucus status,
therefore this method should be combined with a calendar method for best results.
• Symptothermal Method
The symptothermal method combines the cervical mucus and BBT method. The woman takes
her temperature daily, watching for the rise in temperature that marks ovulation such as
mittleschemerz or cervix feels softer than usual. The couple then abstain coitus until 3 days
after the rise in temperature or the fourth day after the peak of mucus change. The
symptothermal method, because it assesses more clues to ovulation, is more effective that
either the BBT or cervical mucus alone.
Natural family planning methods do not have side effects. If there is contraindication to their
use, it would be for couples who must prevent conception because their failure rate of all forms
is about 25%.
B. Barrier Methods of Contraception
Barrier methods are forms of birth control that place a chemical or latex barrieron the cervix
and advancing sperm so sperm cannot reach and fertilize an ovum.
1. Spermicides
A spermicide is an agent that causes the death of spermatozoa before they can enter the cervix.
It is a chemical barrier method and is often used in combination with other physical barrier
methods. Spermicides not only actively kill sperm but also change the vagina pH to a strong
acid level, a condition not conducive to sperm survival. They do not protect against STIs.
Spermicidal foam, cream, jelly, and suppository capsules are over-the-counter (OTC)
Module 3 – Reproductive Life Planning 5
contraceptives. They have a failure rate of 21%. The use of other methods of family planning
with spermicide increases the contraceptive effectiveness
Spermicides can cause local irritation in the vagina or on the penis. The irritation can cause tiny
cracks that provide portals of entry for infection.
2. Condoms
Male condoms are sheaths of thin latex, polyurethane, or natural membrane worn on the penis
during intercourse. Condoms collect semen before, during, and after ejaculation. They come in
various styles, such as ribbed, lubricated, and colored, and with or without spermicide. They
are single-use, low cost items that are available OTC. Latex condoms provide some protection
from STIs. Natural membrane condoms do not prevent the passage of viruses. To prevent
condom breakage, water-soluble lubricants should be used of the condom or vagina is dry.
Female condoms are essentially used for the same purpose as malt condoms. Two flexible rings,
one that fits into the vagina and one that remains outside, connected by a polyurethane
sheath. They are prelubricated, single-use items that are available OTC.
Side effects of and contraindications to condom use are rare. Either or the partners maybe
allergic to latex, in which case a polyurethane or natural membrane condom can be used
successfully. The failure rate is 18%.
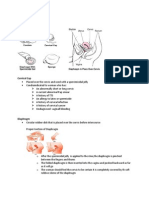
3. Diaphragm and cervical cap
Diaphragms and cervical caps are rubber domes that fit over the cervix and are used with
spermicides to kill sperm that pass the mechanical barrier. A health care provider fits the
diaphragm and cervical cap. The woman must learn how to insert and remove the diaphragm
or cervical cap and to verify proper placement.
Before insertion, the woman should check either device for weak spots or pinholes by holding it
up to the light. Diaphragm or cervical cap is inserted before coitus and should be removed six
hours after sexual intercourse but not longer than 24 hours (Diaphragm) or 48 hours (Cervical
cap). The diaphragm must be refitted after each birth or after a weight change of 10 pounds or
more. The cap must be refitted yearly and after birth, abortion, or surgery.
Module 3 – Reproductive Life Planning 6
User misplacement, especially of the small cervical cap, is acommon reason for unintended
pregnancy. The typical failure rate is 12%.
Contraindications for Diaphragm include:
o history of toxic shock syndrome (TSS; a staphylococcal infection introduced
through the vagina
o allergy to rubber or spermicide
o history of recurrent UTI
o during menstrual period
Contraindications for Cervical cap
o abnormally short or long cervix
o abnormal Pap smear
o history of TSS
o history of latex or spermicide allergy
o history of cevicitis or cervical cancer
o undiagnosed vaginal bleeding
C. Hormonal Contraceptives
Hormonal contraceptives include one or more of these contraceptive effects:
• Prevent ovulation.
• Make the cervical mucus thick and resistant to sperm penetration.
• Make the uterine endometrium less hospitable if a fertilized ovum does
arrive.
1. Oral contraceptives
Oral contraceptives, commonly known as pill, OCs (for oral contraceptive), or COCs (for
combination oral contraceptives), are composed of varying amounts of natural estrogen or
synthetic estrogen combined with small amounts of synthetic progesterone (progestin). The
estrogen acts to suppress follicle-stimulating hormone (FSH) and Leutinizing hormone (LH) to
Module 3 – Reproductive Life Planning 7
suppress ovulation. The progesterone action causes a decrease in the permeability of cervical
mucus and so limits sperm motility and access to ova. Progesterone also interferes with tubal
transport and endometrial proliferation to such an extent the possibility of implantation is
decreased.
Combination oral contraceptives are available in 21-or 28- pill packs. If the woman has a 21-pill
pack, she takes one pill each day at the same time for 21 days and then stops for 7 days. The
woman who has a 28-day pack takes a pill each day; the last seven pills of the pack are inactive
(usually iron supplement) but help her maintain the habit of taking the pill each day.
Menstruation occurs during the 7-day period when either no pills or inactive pill are ingested.
Because COCs are not effective for the first 7 days, advise women to use a second form of
contraception during the initial 7 days that they take pills.
Common side effects of OCs include nausea, headache, breast tenderness, weight gain, and
spotting between periods or amenorrhea. These effects generally decrease within a few
months and are seen less frequently with low dose of OCs.
Women with the following disorders should not take OCs or should take them with caution:
o Thromboembolic disorders (blood clots)
o Cerebrovascular accident or heart disease
o Breast cancer
o Smoking of more than 15 cigarettes a day for women older than 35 years
o Impaired liver function
o Confirmed or possible pregnancy
o Undiagnosed vaginal bleeding
o Diabetes mellitus
o Breastfeeding and less than 6 weeks postpartum
Some medications reduce the effectiveness of OCs include:
o Some antibiotics (ampicillin, tetracycline)
o Anticonvulsants
o Rifampin, barbiturates
Module 3 – Reproductive Life Planning 8
The acronym ACHES can help a woman recall the warning signs to report when taking
OCs:
o Abdominal pain (severe)
o Chest pain, dyspnea, bloody sputum
o Headache (severe), weakness, or numbness of the extremities
o Eye problems (blurring, double vision, vision loss)
o Severe leg pain or swelling, speech disrubance
o
2. Hormone implants
A progestin-filled miniature rod no bigger than a matchstick, etonogestrel implant (Nexplanon)
can be embedded just under the skin on the inside of the upper arm where it will slowly release
progestin over a period of 3 years. The implant suppresses ovulation, thickens cervical mucus,
and changes the endometrium lining, making the implantation difficult.
3. Intramascular injection
A single intramuscular injection of depot medroxyprogesterone acetate or DMPA (Depo-
Provera), a progesterone given every 12 weeks (3 months). The effectiveness rate of this
method is almost 100%. The injection is made deep into major muscle before the fifth day after
the beginning of a menstrual flow. The woman should not massage the injection site after the
administration so the drug can be absorbed slowly form the muscle.
D. Intrauterine Device
An intrauterine device (IUD) is a small plastic device that is inserted into the uterus through the
vagina by a healthcare provider. IUDs can be either hormonal or non-hormonal. It prevents
fertilization and it creates a local sterile inflammatory reaction that prevents implantation. The
method has a failure rate of 0.1% and reversible, and no specific actions are required related to
intercourse. The hormonal IUD is usually replaced every 3 to 6 years.
Module 3 – Reproductive Life Planning 9
Cramping and bleeding are likely to occur with insertion. Increased menstruation and
dysmenorrheal may occur, and these are common reasons that a woman decides to have the
IUD removed. The IUD does not protect against STIs.
The acronym PAINS can help a woman with IUD recall the warning signs to report:
o Period which late, heavy or prolonged
o Abdominal pain
o Increased body temperature (or any signs of infection)
o Noticeable vaginal discharge (foul-smelling)
E. Surgical method of reproductive planning
Surgical methods of reproductive planning, often called sterilization, include tubal ligation for
women and vasectomy for men. Both have 99.5% effectiveness.
1. Vasectomy
In a vasectomy, a small puncture wound (referred to as “no-scalpel technique”) is made on the
scrotum. The vas deferens on each side are then pulled forward, cut and tied, cauterized, or
plugged, blocking the passage of spermatozoa. A vasectomy can be done under local anesthesia
in an ambulatory setting, such as in primary healthcare provider’s office or a reproductive life
planning clinic. Although the procedure is about 99.5% effective, spermatozoa, which were
present in the vas deferens at the time of surgery, can be viable for as long as 6 months.
Therefore, although the man can resume sexual intercourse 1 week, an additional birth control
method should be used until two negative sperm reports at about 6 and 10 weeks have been
obtained (proof all sperm in the vas deferens have been eliminated, usually requiring 10 to 20
ejaculations).
2. Tubal ligation
Sterilization of women could include removal of uterus or ovaries (hysterectomy), but it
usually refers to a minor surgical procedure, such as tubal ligation, where the fallopian
tubes are occluded by cautery, crushed, clamped, or blocked, and thereby preventing
passage of both sperm and ova. A fimbriectomy, or removal of the fibria at the distal
Module 3 – Reproductive Life Planning 10
end of the tubes is another possible but little used technique. Three methods may be
used:
a. A minilaparatomy uses an incision near the umbilicus in the immediate postpartum
period or just above the symphisis pubis at other times. The surgeon makes a tiny
incision, brings each tube through it, and ligates, and cuts the tube.
b. Laparoscopic surgery is similar, but the tubes are identified and ligated tube called
laparoscope
c. The traditional approach is performed during other abdominal surgery, usually a
cesarean birth.
III. Assessment for reproductive life planning needs
As a result of changing social values and lifestyles, many women are interested in
reproductive life planning and so are able to talk easily about types and methods
today. Other people are uncomfortable or not interested in using a planning
method so may not voice their interest in the subject independently. For this
reason, at health assessments, ask clients if they want more information or need
any help with reproductive life planning as part of obtaining a basic health history.
Before people are begun on a new contraceptive, other information that needs to
be obtained is:
• A Pap smear, pregnancy test, gonococcal and chlamydial screening, perhaps
hemoglobin for detection of anemia or a mammogram to rule out breast
disease
• Obstetric history, including sexually transmitted infections (STIs), past
pregnancies, previous elective abortions, failure of previously used methods,
and compliance record
• Subjective assessment of the client’s desires, needs, feelings, and
understanding of conception (teens, for example, may believe that they are too
young to get pregnant; many women in the immediate postpartum period may
Module 3 – Reproductive Life Planning 11
believe that they cannot conceive immediately, especially if they are
breastfeeding)
• Sexual practices, such as frequency, number of partners, feelings about sex and
body image, or latex allergy
IV. Nursing Diagnoses Related to Reproductive Life Planning
Because reproductive life planning touches so many facets of life, nursing diagnoses
can differ greatly depending on the circumstances.
Examples might include:
• Health-seeking behaviors regarding contraception options related to desire to
prevent pregnancy
• Deficient knowledge related to use of diaphragm
• Spiritual distress related to partner’s preferences for contraception
• Decisional conflict regarding choice of birth control because of health concerns
• Decisional conflict related to unwanted pregnancy
• Powerlessness related to failure of chosen contraceptive
• Ineffective sexuality pattern related to fear of pregnancy
• Risk for ineffective health maintenance related to lack of knowledge about
natural family planning method
V. Interventions Related to Reproductive Life Planning
When establishing expected outcomes for care in this area, be certain that they
are realistic for the individual. Women’s decisions are influenced by many factors; a
nurse’s role is to educate about contraceptives and support a woman about her
contraceptive decision. If a woman has a history of poor compliance with medication,
for instance, it might not be realistic for her to plan to take an oral contraceptive every
day. Be certain to be sensitive to a couple’s religious, cultural, and moral beliefs before
suggesting possible methods. It is equally important to explore your own beliefs and
values. This not only helps develop self-awareness of how these beliefs affect nursing
Module 3 – Reproductive Life Planning 12
care, but it allows you to become more sensitive to the beliefs of others. Some couples
cannot make realistic plans about contraception because they are uninformed or
misinformed about the options. When counselling, be certain to emphasize safer sex
practices as well as contraceptive ones.
VI. Evaluating Outcomes Related to Reproductive Life Planning
Evaluation is important in reproductive life planning, because anything that
causes clients to discontinue or misuse a particular method will leave them at risk of
pregnancy. Reassess early (within 1 to 3 weeks) after a couple begins a new method of
contraception, to prevent such an occurrence. Evaluate not only whether a chosen
method is effective but whether the woman and her partner are satisfied with the
method.
Examples of expected outcomes include:
• Client voices correct technique for using chosen method
• Client voices confidence in chosen method by next visit
• Client expresses satisfaction with chosen method at follow-up visit
• Client consistently uses chosen method without pregnancy for 1 year’s
time
References
Flagg, J. (2018). Maternal and child health nursing: Care of the childbearing and childbearing
family (8thed.). Philadelphia, PA: WoltersKluwer.
Credits and Quality Assurance
Prepared by:
Noriel P. Calaguas, MSHSA, RN
Assistant Professor & Chairperson, Nursing
MELANIE C. TAPNIO, MAN, RN Program
Academic Rank
Recommending Approval:
Module 3 – Reproductive Life Planning 13
Reviewed by:
Louie Roy E. Catu, PhD, RN
Assistant Professor & OBE Facilitator
Approved by:
Al D. Biag, EdD, RN, RM
Professor & Dean
Module 3 – Reproductive Life Planning 14
You might also like
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (589)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (842)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5806)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (345)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1091)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Sexual SAAQ Manual PDFDocument44 pagesSexual SAAQ Manual PDFLacatus AlinaNo ratings yet
- Family Planning PPT For MSCDocument183 pagesFamily Planning PPT For MSCSeid wodajo100% (1)
- Contraceptive TechnologyDocument68 pagesContraceptive TechnologySravanthi Karingula100% (1)
- Case Analysis: Thinking Critically To Analyze Data: QuestionsDocument2 pagesCase Analysis: Thinking Critically To Analyze Data: Questionsarrian arraNo ratings yet
- FAMILY PLANNING MCN 101Document31 pagesFAMILY PLANNING MCN 101kaycelyn jimenezNo ratings yet
- Maternal and Child Health Pracice Test 1-2-3Document84 pagesMaternal and Child Health Pracice Test 1-2-3chuppepay100% (1)
- Set 3 PNLE IDocument52 pagesSet 3 PNLE IDarnell Adrian EstobioNo ratings yet
- Health Talk On ContraceptionDocument32 pagesHealth Talk On Contraceptionvaishali TMU studentNo ratings yet
- Case Analysis: Thinking Critically To Analyze Data: QuestionsDocument2 pagesCase Analysis: Thinking Critically To Analyze Data: Questionsarrian arraNo ratings yet
- Chapter 11Document26 pagesChapter 11arrian arraNo ratings yet
- Critical Care Nursing of Infants and Children: ScholarlycommonsDocument26 pagesCritical Care Nursing of Infants and Children: Scholarlycommonsarrian arraNo ratings yet
- Module 1Document10 pagesModule 1arrian arraNo ratings yet
- The Role of The Youth in Nation BuildingDocument1 pageThe Role of The Youth in Nation Buildingarrian arraNo ratings yet
- Activity - Analyzing Family Structure, Dynamics, and FunctionalityDocument15 pagesActivity - Analyzing Family Structure, Dynamics, and Functionalityarrian arraNo ratings yet
- Bayan" "Oo, Lagi Naman May Binibigay Na Libreng Gamot Sa Clinic"Document2 pagesBayan" "Oo, Lagi Naman May Binibigay Na Libreng Gamot Sa Clinic"arrian arraNo ratings yet
- HSC 430 Lesson PlanDocument17 pagesHSC 430 Lesson Planapi-381179599No ratings yet
- Chapter 10. Prevention of Pregnancy and Sexually Transmitted InfectionsDocument24 pagesChapter 10. Prevention of Pregnancy and Sexually Transmitted InfectionsMonica CiorneiNo ratings yet
- Family PlanningDocument10 pagesFamily Planningdalvin20207967No ratings yet
- Contraceptive MethodsDocument73 pagesContraceptive MethodsDIPENDRA KUMAR KUSHAWAHANo ratings yet
- Family PlanningDocument34 pagesFamily PlanningArenz Rubi Tolentino IglesiasNo ratings yet
- Lesson 11 - Appled Ethics and Reproductive IssuesDocument8 pagesLesson 11 - Appled Ethics and Reproductive IssuesTheodosia KNo ratings yet
- Family PlanningDocument6 pagesFamily PlanningDhanica Yvonne ReymonteNo ratings yet
- Oral Contraceptive PillDocument21 pagesOral Contraceptive Pilljuly3ciaNo ratings yet
- ThesisDocument5 pagesThesisJulia ConceNo ratings yet
- Family Planning: Sunita Sapkota Suraj Thapa Sushma Neupane Yamjee MahatoDocument50 pagesFamily Planning: Sunita Sapkota Suraj Thapa Sushma Neupane Yamjee Mahatosuraj supremeNo ratings yet
- An Overview of Properties of Amphora (Acidform) Contraceptive Vaginal GelDocument10 pagesAn Overview of Properties of Amphora (Acidform) Contraceptive Vaginal GelardirshajiNo ratings yet
- Key Points in Obstetrics and Gynecologic Nursing A: Ssessment Formulas !Document6 pagesKey Points in Obstetrics and Gynecologic Nursing A: Ssessment Formulas !June DumdumayaNo ratings yet
- Chapter 6 - Nursing Care For The Family in Need of Reproductive Life PlanningDocument7 pagesChapter 6 - Nursing Care For The Family in Need of Reproductive Life PlanningBern NerquitNo ratings yet
- Postpartum Car1Document11 pagesPostpartum Car1Claire Alvarez OngchuaNo ratings yet
- Contraception ReviewerDocument7 pagesContraception ReviewerGerlie Anne ChicanoNo ratings yet
- Lesson Plan Contraception Part I and IIDocument12 pagesLesson Plan Contraception Part I and IIMary Pyie KinkaewNo ratings yet
- Barrier MethodDocument3 pagesBarrier MethodJaninaPatriciaBNo ratings yet
- Family Planning and Contrceptives For Midwifery StudentsDocument190 pagesFamily Planning and Contrceptives For Midwifery StudentsAbdusamed100% (1)
- 2.3.1 Family PlanningDocument36 pages2.3.1 Family PlanningLive with CjNo ratings yet
- Contraception: Objective at The End of This Lecture The 5 Year Student Should Be Able ToDocument22 pagesContraception: Objective at The End of This Lecture The 5 Year Student Should Be Able ToAmmarNo ratings yet
- Bell Hooks - Ain't I A Woman. Black Women and FeminismDocument24 pagesBell Hooks - Ain't I A Woman. Black Women and FeminismFausto Gómez GarcíaNo ratings yet
- Downloadable Solution Manual For An Invitation To Health Brief Edition 6th Edition HalesDocument23 pagesDownloadable Solution Manual For An Invitation To Health Brief Edition 6th Edition HalesAntonioCohensirt100% (38)
- Maternal and Child Nursing Answers and RationaleDocument94 pagesMaternal and Child Nursing Answers and RationaleAnn Michelle Tarrobago100% (1)