Professional Documents
Culture Documents
Cvs 1,2
Uploaded by
atefmoussa0 ratings0% found this document useful (0 votes)
21 views36 pagesOriginal Title
cvs 1,2
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
21 views36 pagesCvs 1,2
Uploaded by
atefmoussaCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 36
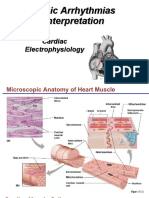
The Heart
Functional structure of cardiac
muscle
• The basic structural unit is the sarcomere.
• Tight and gab junctions.
– the gab junctions act as a low resistance bridges that
allow spread of excitation wave between cardiac cells
– The tight juctions exert mechanical connection between
cardiac muscle fibers.
• It contains actin and myosin with striations
of dark A-bands and light I- bands.
• each transverse tubule is surrounded by
cisternae of sarcoplasmic reticulum.
• Most of the energy of the heart is derived
from aerobic oxidation
The cardiac muscle differs from
skeletal muscle in:
being not dependent on central nervous
system.
having no neuromuscular junctions.
acting as a single unit or functional
syncitium.
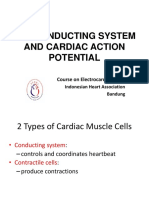
Functional division:
• Nodal or pacemaker tissue
– It is the tissue that is able to initiate nerve impulse
in an automatic and regular manner, examples :
SAN (sinoatrial node) and AVN (atrio-ventricular
node).
• Junctional (Conductive tissue) : this
system conducts nerve impulse from site of
initiation to all parts of the heart as fast as
possible.
• Contractile (muscular) tissue : It is the
issue that is able to contract and act as a
pump.
Properties of cardiac muscle
Autorhythmicity
Conductivity
Excitability
Contractility
Autorhythmicity
It is the ability of autorhythmic cells
present in the heart to generate nerve
impulses in regular and independent
manner.
Autorhythmic cells
◦ SAN Its rhythm is 100 impulse / minute
◦ AVN.: Its rhythm is 50 imulse/ minute
◦ Purkinje fibers: Its rhythm is 25 impulse /
minute
Autorhythmic cells
have unstable resting membrane potential
at – 60 mv resting level, there is
spontaneous depolarization due to
decrease in K+ and increase in Na+ and
Ca+ permeability
SAN is the pacemaker of the heart
because it discharge nerve impulses at
the highest rhythm about 100 impulse /
minute.
Factors affecting Autorhythmicity
Sympathetic stimulation increases
autorhythmicity by decreasing membrane
permeability to K+
Parasympathetic stimulation decreases
automaticity due to increase in K+
permeability
Increase in body temperature by 1o C
increases heart rate by 20 bpm
Mechanical stretch of right atrium stimulates
SAN
Catecholamines also stimulate SAN.
• Chrotropic effect:
– It is the increase of rate of discharge of SAN
and hence increase heart rate.
• Positive chronotropic effect : Increase of
HR
– Examples
• Sympathetic stimulation
• Catecholamines (adrenaline and noradrenaline)
• Negative chronotropic effect: Decrease of
HR
– Examples
• Parasympathetic (vagal) stimulation
• Acetylcholine.
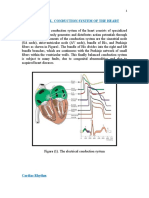
Conductivity:
It is the ability of the heart to conduct
nerve impulses from the site of initiation
to all parts of the ventricles through a
specialized conductive system as fast as
possible.
Importance of AVN
• It acts as one way conduction of nerve
impulse from atrium to ventricle
• It delays the nerve impulse for about 0.1
second to allow atrial excitation to be
completed before the start of ventricular
excitation
• AVN also has a long absolute refractory
period to protect the ventricle from high
atrial rhythms
• AVN act as a latent pacemakerin case of
damage of SAN
The highest conductive velocity
occurs in Purkinje fibers while the
highest rate of discharge occurs in
SAN
Excitability
It is the ability of cardiac muscle to
respond to stimulation by producing action
potential.
Two types of electrical responses.
◦ Fast response is recorded from fast response
fibers or contractile fibers
◦ slow response recorded from slow response
fibers or autorhythmic cells.
Slow Response
• It is the action potential recorded from SAN
or AVN. It is formed from the following
phases:
– Prepotential : it is the unstable resting membrane
potential of the slow fibers.
• The membrane potential changes from -60 mv to the
firing level of – 45 mv.
• is due to decrease potassium efflux and increase
sodium and calcium influx.
– Depolarization of action potential occurs by
calcium influx
– Repolarization occurs by potassium efflux.
Fast response
• It is the action potential recorded from
contractile cells.It is formed of the following
phases :
– Phase 4 : resting state -90 mv.
– Phase 0 : fast depolarization from -90 mv to + 30
mv it is due to sodium influx through fast volt-
sensitive sodium channels.
– Phase 1 : rapid small repolarization : It is due to
potassium efflux.
– Phase 2 : Plateau : It is a plateau phase and is due
to both calcium influx and potassium efflux.
– Phase 3 : rapid repolarization : It is due to
potassium efflux.
During which phase
of the ventricular
action potential is
the conductance to
Ca2+ highest?
(A) Phase 0
(B) Phase 1
(C) Phase 2
(D) Phase 3
(E) Phase 4
Contractility
It is the intrinsic ability of cardiac muscle
to generate force at a constant length.
Excitation contraction coupling
◦ depolarization of cardiac muscle cells will lead
to opening of volt sensitive calcium channels in
the sarcolemma causing calcium influx.
◦ The increased intracellular calcium will activate
another calcium sensitive calcium channels in
the cisternae of sarcoplasmic reticulum
◦ release of calcium from sarcoplasmic reticulum
to the cytoplasm
Contractility
Excitation contraction coupling
◦ increase intracellular calcium will bind troponin
c
◦ this will cause binding of actin to myosin with
sliding of actinover myosin.
◦ shortening of sarcomeres and so muscle
contraction
◦ Relaxation of cardiac muscle occurs by
decreasing cytosolic calcium
◦ pumping calcium to extracellular fluid or to
cisternae of sarcoplasmic reticulumby active
mechanism.
Ion movements during the contraction of cardiac muscle. ATPase = adenosine
triphosphatase
Factors affecting cardiac muscle
contractility
Intrinsic:
◦ Preload
◦ Afterload
◦ Heart Rate
Extrinsic
◦ Nervous
Sympathetic
Parasympathetic
◦ Humoral
Hormones
Chemixcals and drugs
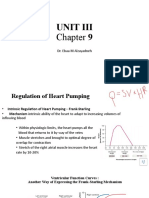
Intrinsic regulation of Contractility
Preload
◦ Its effect is determined by Starling law
◦ It is a direct relationship within limit . So
◦ Increase VR (venous return) will cause stretch
of the muscle of ventricle and this leads to
increase preload so force of contraction
increases.
◦ If the ventricle is overstretched, force of
contraction will decrease.
Intrinsic regulation of Contractility
Afterload
◦ it is defined as the load imposed on the muscle
during contraction or the force against which
the heart pumps blood
◦ The high arterial blood pressure and aortic
stenosis are examples of afterloads.
◦ Increase afterload is inversely proportional to
the velocity of shortening.
Effect of heart rate on contraction
◦ Increase HR increases force of contraction
Extrinsic regulation of Contractility
Nervous factors
◦ Sympathetic stimulation has a positive inotropic
effect by increasing availability of calcium
◦ Parasympathetic stimulation has negative inotropic
effect by decreasing calcium but this effect is
exerted only on the atria
Humoral factors
◦ Catecholamines have a positive inotropic
◦ Calcium may stop the heart in systole
◦ potassium stops the heart in diastole.
◦ Digitalis has a positive inotropic effect by
increasing calcium inside the cardiac cells.
◦ Calcium channel blockers (nefidipine) : has a
negative inotropic effect
You might also like
- CSCS Study GuideDocument50 pagesCSCS Study GuideMatt Siniscalchi100% (5)
- Tissue Structure and FunctionDocument3 pagesTissue Structure and FunctionAnna Margarett Mutia60% (5)
- Bio 137 Lab ManualDocument185 pagesBio 137 Lab ManualReedNo ratings yet
- Discromatie Test 38Document13 pagesDiscromatie Test 38nelutza_popNo ratings yet
- Prokaryotic Cell Eukaryotic Cell: Lab 3 (Virtual Lab and Worksheet)Document2 pagesProkaryotic Cell Eukaryotic Cell: Lab 3 (Virtual Lab and Worksheet)Enzo MendozaNo ratings yet
- Cvs 1Document37 pagesCvs 1atefmoussaNo ratings yet
- Characteristic of Cardiac Muscle Cells - CVSK4Document36 pagesCharacteristic of Cardiac Muscle Cells - CVSK4Lydia KosasihNo ratings yet
- Cardiac Conduction: Shoiab AlamDocument26 pagesCardiac Conduction: Shoiab AlamUzma KhanNo ratings yet
- KondukDocument33 pagesKondukaliusman laseNo ratings yet
- Cardiac Muscle2Document39 pagesCardiac Muscle2Darius GanNo ratings yet
- Conducting System of The HeartDocument27 pagesConducting System of The HeartMuhammadNo ratings yet
- Mechanical Function of The HeartDocument28 pagesMechanical Function of The HeartKarmilahNNo ratings yet
- Basic ElectrophysiologyDocument46 pagesBasic Electrophysiologyiin setiyanaNo ratings yet
- Cardiovasular SystemDocument26 pagesCardiovasular SystemPhai KoemhienNo ratings yet
- Cardiac L1CVSDocument19 pagesCardiac L1CVSQutaybah JahmanyNo ratings yet
- Cardio PhysioDocument11 pagesCardio Physioanonymousperson4696No ratings yet
- Cardiovascular Physiology 0 Anesthetic ImportanceDocument100 pagesCardiovascular Physiology 0 Anesthetic ImportanceSurya SuryaNo ratings yet
- 2-Cardiac Electical ActivityDocument26 pages2-Cardiac Electical ActivityhalayehiahNo ratings yet
- CVS DMDocument32 pagesCVS DMsuman palNo ratings yet
- Cardiac L3Document18 pagesCardiac L3Qutaybah JahmanyNo ratings yet
- 01-02. Ecg Course - The Conducting System and Cardiac Action PotentialDocument28 pages01-02. Ecg Course - The Conducting System and Cardiac Action PotentialFATHICHAHNo ratings yet
- Cardiac PhysiologDocument30 pagesCardiac PhysiologKannan GNo ratings yet
- CVS PhysiologyDocument43 pagesCVS Physiologyapi-3705050100% (1)
- Cardiovascular System TamreedDocument8 pagesCardiovascular System TamreedslmylwkaaNo ratings yet
- Physiology Lec: 2 Cardiovascular System دــيز .د يجقراطلاDocument7 pagesPhysiology Lec: 2 Cardiovascular System دــيز .د يجقراطلاArif NabeelNo ratings yet
- Cardiac Electrical ActivityDocument17 pagesCardiac Electrical ActivitySalah Salah 201-901-341No ratings yet
- 05 - Fisiologi - Jantung PDFDocument63 pages05 - Fisiologi - Jantung PDFfadhila dzatu rifqiNo ratings yet
- Physiology of The HeartDocument34 pagesPhysiology of The Heartalyssa_marie_keNo ratings yet
- Sifat Dan Kerja Otot Jantung - CVS-K10Document21 pagesSifat Dan Kerja Otot Jantung - CVS-K10Suci Intan FatrisiaNo ratings yet
- الوحدة الثانيهDocument7 pagesالوحدة الثانيهHUAWEI HUAWEINo ratings yet
- Electrical Properties of The HeartDocument25 pagesElectrical Properties of The HeartSherwan R Shal100% (3)
- Lecture - 3 Properties of Cardiac MuscleDocument35 pagesLecture - 3 Properties of Cardiac MuscleMRM7MDNo ratings yet
- Unit Iii: Dr. Ebaa M AlzayadnehDocument17 pagesUnit Iii: Dr. Ebaa M AlzayadnehEbaa Moh'd ZayadnehNo ratings yet
- Aktivitas Elektrik Jantung: Rahmatina B. Herman Bagian Fisiologi Fakultas Kedokteran - UnandDocument33 pagesAktivitas Elektrik Jantung: Rahmatina B. Herman Bagian Fisiologi Fakultas Kedokteran - UnandRUNNINo ratings yet
- Unit 8 PresentationDocument34 pagesUnit 8 Presentation03152788No ratings yet
- Or Cardiac Physiology, Pathophysiology, and Some PharmacologyDocument58 pagesOr Cardiac Physiology, Pathophysiology, and Some PharmacologyJacob StoneNo ratings yet
- Normal Heart Rhythm: Mutiara Budi AzharDocument27 pagesNormal Heart Rhythm: Mutiara Budi AzharAditya Fresno Dwi WardhanaNo ratings yet
- Contractility: The Strength of Contraction at Any Given End-Diastolic VolumeDocument4 pagesContractility: The Strength of Contraction at Any Given End-Diastolic VolumezaidNo ratings yet
- Lec13 Sem2 CVSWK2 20130706Document13 pagesLec13 Sem2 CVSWK2 20130706Uloko ChristopherNo ratings yet
- CardioDocument40 pagesCardioOctavio González InversonNo ratings yet
- Biochemistry of The Heart and Blood Vessels 2021 3 4Document44 pagesBiochemistry of The Heart and Blood Vessels 2021 3 4jakukNo ratings yet
- Phase 2 Cardiac Muscle - 1Document30 pagesPhase 2 Cardiac Muscle - 1erenyorulmaz143No ratings yet
- Rhythmicity and ExcitabilityDocument29 pagesRhythmicity and ExcitabilityKero amgedNo ratings yet
- C9Document15 pagesC9SLKNo ratings yet
- 11 Ant HEART MUSCLEDocument57 pages11 Ant HEART MUSCLEZuhaib AhmedNo ratings yet
- 05 Cardiovascular System PhysiologyDocument34 pages05 Cardiovascular System PhysiologyKaye Alyssa EnriquezNo ratings yet
- Cardiovascular Physiology Lecture 1Document95 pagesCardiovascular Physiology Lecture 1Freelance LeagueNo ratings yet
- Mechanisms of Cardiac Arrythmias: Conduction, or BothDocument5 pagesMechanisms of Cardiac Arrythmias: Conduction, or BothdeaNo ratings yet
- Heart As A PumpDocument41 pagesHeart As A PumpFirst LuckNo ratings yet
- Cardiac Arrhythmia: Prepared By: Charina Gail O. Baloy, RPH, Msc. (C.)Document44 pagesCardiac Arrhythmia: Prepared By: Charina Gail O. Baloy, RPH, Msc. (C.)Chinenye Akwue100% (1)
- 04b-Fungsi Mekaninik JantungDocument28 pages04b-Fungsi Mekaninik JantungCitra Wulandari SofyanNo ratings yet
- Physiology DES: Biruk A. (Balemaye@sgu - Edu) & Sami Ahmed. (Sahmed10@sgu - Edu)Document56 pagesPhysiology DES: Biruk A. (Balemaye@sgu - Edu) & Sami Ahmed. (Sahmed10@sgu - Edu)Joseph KimNo ratings yet
- Heart Muscles, Valves & Blood Vessels (I)Document31 pagesHeart Muscles, Valves & Blood Vessels (I)Hussain GauharNo ratings yet
- Electrical Activity of The HeartDocument28 pagesElectrical Activity of The Heartsultan khabeebNo ratings yet
- Physiology of Heart in DetailDocument101 pagesPhysiology of Heart in Detailakanksha sharmaNo ratings yet
- 4 1Document2 pages4 1Raj BulaNo ratings yet
- Physiology of HeartDocument74 pagesPhysiology of Heartmadeha goharNo ratings yet
- The Cardiovascular SystemDocument4 pagesThe Cardiovascular SystemSharie Mae MataumNo ratings yet
- Oxygenated and Deoxygenated Do Not Mix DueDocument5 pagesOxygenated and Deoxygenated Do Not Mix DueNathaly Kate BohulanoNo ratings yet
- Heart ActionDocument14 pagesHeart ActionNqaba SisoNo ratings yet
- CV RegulatnDocument28 pagesCV RegulatnShahin KhanNo ratings yet
- Cardiac Muscle PropertiesDocument4 pagesCardiac Muscle PropertiesSurpreet AroraNo ratings yet
- Physiology - Rhythmical Excitation of Heart by Dr. Mudassar Ali RoomiDocument18 pagesPhysiology - Rhythmical Excitation of Heart by Dr. Mudassar Ali RoomiMudassar Roomi100% (2)
- Second Session 1Document22 pagesSecond Session 1Aamir EjazNo ratings yet
- Physiology CNS: Sensory SystemDocument22 pagesPhysiology CNS: Sensory SystematefmoussaNo ratings yet
- L1 Development of The BrainDocument42 pagesL1 Development of The Brainatefmoussa100% (1)
- CVS 6, 7 and 8Document37 pagesCVS 6, 7 and 8atefmoussaNo ratings yet
- CVS 6, 7 and 8Document37 pagesCVS 6, 7 and 8atefmoussaNo ratings yet
- CNS Physiotherapy 2021Document88 pagesCNS Physiotherapy 2021atefmoussaNo ratings yet
- Practical MotorDocument7 pagesPractical MotoratefmoussaNo ratings yet
- Physiology of PainDocument65 pagesPhysiology of PainatefmoussaNo ratings yet
- How To Use The Ishihara TestDocument6 pagesHow To Use The Ishihara TestatefmoussaNo ratings yet
- Uworld SampleDocument47 pagesUworld SampleatefmoussaNo ratings yet
- L5 Surface Anatomy & DiaphragmDocument45 pagesL5 Surface Anatomy & DiaphragmatefmoussaNo ratings yet
- Anatomy and Healing Process of Paediatric Bone - Dato DR Zulkiflee OsmanDocument56 pagesAnatomy and Healing Process of Paediatric Bone - Dato DR Zulkiflee OsmanMuhammad Naqiuddin JalaluddinNo ratings yet
- Organization and Composition of Body FluidsDocument7 pagesOrganization and Composition of Body FluidsEVELYN ITZEL OCHOA VARGASNo ratings yet
- Blood CoagulationDocument10 pagesBlood CoagulationgauravkokraNo ratings yet
- Varsity Science Questions-BiologyDocument19 pagesVarsity Science Questions-BiologySlasher124No ratings yet
- Lec 3 &4 (Skeletal Appendicular Skeleton)Document123 pagesLec 3 &4 (Skeletal Appendicular Skeleton)Nengah VindiNo ratings yet
- Lesson 1: Muscle and Bone-Strengthening ActivitiesDocument25 pagesLesson 1: Muscle and Bone-Strengthening ActivitiesAshley Keith RamiloNo ratings yet
- Debusk College of Osteopathic Medicine: Oms-I Fall Class Schedule 2021 KeyDocument21 pagesDebusk College of Osteopathic Medicine: Oms-I Fall Class Schedule 2021 KeyIsmail IsmatNo ratings yet
- DLL Quarter 2 Week 1 (Melc - Idea - 5e's - Pivot - Adm-Pasay)Document64 pagesDLL Quarter 2 Week 1 (Melc - Idea - 5e's - Pivot - Adm-Pasay)Misha Madeleine GacadNo ratings yet
- Chapter 62 Musculoskeletal SystemDocument5 pagesChapter 62 Musculoskeletal SystemRichard MooreNo ratings yet
- A Critical Appraisal of Garbha Avkranti Vis-A-VisDocument10 pagesA Critical Appraisal of Garbha Avkranti Vis-A-VisAmitabh BachhanNo ratings yet
- Divine Word College of Laoag School of Arts, Sciences and Education Laoag CityDocument5 pagesDivine Word College of Laoag School of Arts, Sciences and Education Laoag Cityelfe deramaNo ratings yet
- FibrothecomaDocument94 pagesFibrothecomaMindy SantiagoNo ratings yet
- Ent History Taking and Examination-1Document16 pagesEnt History Taking and Examination-1Jyotirmayee100% (5)
- 3448 7726 1 SMDocument14 pages3448 7726 1 SMyg SuyantoroNo ratings yet
- ACFrOgAQi3DcTfwqz2AAs6VzlcO-ZrPS0VejMlcIYkk2ZRbVOHsk99RC35KLj5K5Oqju7VGTE1GX7R AReFHzI7kwkc0GfFoQP0hP08pK3pivZZYBxugMMQrNyoMeHU1GFiC1y1IPOBG5Y6cQM1f PDFDocument42 pagesACFrOgAQi3DcTfwqz2AAs6VzlcO-ZrPS0VejMlcIYkk2ZRbVOHsk99RC35KLj5K5Oqju7VGTE1GX7R AReFHzI7kwkc0GfFoQP0hP08pK3pivZZYBxugMMQrNyoMeHU1GFiC1y1IPOBG5Y6cQM1f PDFJewel-Jue Jue Kyaw MinNo ratings yet
- Plant Structures and Physiology NotesDocument97 pagesPlant Structures and Physiology Notesapi-292966101No ratings yet
- Lect 1 Host ModulationDocument22 pagesLect 1 Host ModulationrupaliNo ratings yet
- Anatomy of Oral Cavity, Pharynx and EsophagusDocument52 pagesAnatomy of Oral Cavity, Pharynx and EsophagusYashoda Amarasekera100% (1)
- Determination of Blood GroupDocument2 pagesDetermination of Blood GroupRoshan KashyapNo ratings yet
- Cow Dissection DayDocument16 pagesCow Dissection Dayapi-108435797No ratings yet
- 3 Minute German Die KörperteileDocument11 pages3 Minute German Die KörperteileBahar TukanovaNo ratings yet
- Ss Organ Systems WorksheetDocument2 pagesSs Organ Systems Worksheet땡뿍뿍No ratings yet
- Azzi1983bone ESCANEADODocument5 pagesAzzi1983bone ESCANEADOCristhian BurbanoNo ratings yet
- Benign Ovarian Tumors With Solid and Cystic Components That Mimic MalignancyDocument7 pagesBenign Ovarian Tumors With Solid and Cystic Components That Mimic Malignancynautilus81No ratings yet
- Physical Assessment CataractDocument12 pagesPhysical Assessment CataractEries Lacanlale LumbaNo ratings yet
- Activity 4Document10 pagesActivity 4Kalea Kassandra MatthewsNo ratings yet