Professional Documents
Culture Documents
Navarrete 2021
Uploaded by
mariatul fithriasariOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Navarrete 2021
Uploaded by
mariatul fithriasariCopyright:
Available Formats
Patient-Oriented, Translational Research: Research Article
Am J Nephrol 2021;52:190–198 Received: October 25, 2020
Accepted: January 25, 2021
DOI: 10.1159/000514752 Published online: April 7, 2021
Epidemiology of COVID-19 Infection in
Hospitalized End-Stage Kidney Disease Patients
in a Predominantly African-American Population
José E. Navarrete a David C. Tong b Jason Cobb a Frederic F. Rahbari-Oskoui a
Darya Hosein c Sheryl C. Caberto a, d Janice P. Lea a Harold A. Franch a, d
aDivision
of Renal Medicine, Emory University School of Medicine, Atlanta, GA, USA; bDivision of Hospital Medicine,
Emory University School of Medicine, Atlanta, GA, USA; cClinical Research Coordinator I, Emory University School of
Medicine, Atlanta, GA, USA; dMedical Subspecialties Service Line, Atlanta Department of Veterans Affairs Medical
Center, Decatur, GA, USA
Keywords mission to intensive care unit, and 23% required mechanical
COVID-19 · Dialysis · Outcomes ventilation. The median length of stay was 10 days, while 11
patients (17%) died during hospitalization and 17% were dis-
charged to a temporary rehabilitation facility. Age >65 years
Abstract (RR 13.7, CI: 1.9–100.7), C-reactive protein >100 mg/dL (RR
Background: End-stage kidney disease patients on dialysis 8.3, CI: 1.1–60.4), peak D-dimer >3,000 ng/mL (RR 4.3, CI:
are particularly susceptible to COVID-19 infection due to co- 1.03–18.2), bilirubin >1 mg/dL (RR 3.9, CI: 1.5–10.4), and his-
morbidities, age, and logistic constraints of dialysis making tory of peripheral vascular disease (RR 3.2, CI: 1.2–9.1) were
social distancing difficult. We describe our experience with associated with mortality. Dialysis COVID-19-infected pa-
hospitalized dialysis patients with COVID-19 and factors as- tients were more likely to develop thromboembolic compli-
sociated with mortality. Methods: From March 1, 2020, to cations than those without COVID-19 (RR 3.7, CI: 1.3–10.1).
May 31, 2020, all dialysis patients admitted to 4 Emory Hos- Conclusion: In a predominantly African-American popula-
pitals and tested for COVID-19 were identified. Sociodemo- tion, the mortality of end-stage kidney disease patients ad-
graphic information and clinical and laboratory data were mitted with COVID-19 infection was 17%. Age, C-reactive
obtained from the medical record. Death was defined as an protein, D-dimer, bilirubin, and history of peripheral vascular
in-hospital death or transfer to hospice for end-of-life care. disease were associated with worse survival.
Patients were followed until discharge or death. Results: Six- © 2021 S. Karger AG, Basel
ty-four dialysis patients with COVID-19 were identified.
Eighty-four percent were African-American. The median age
was 64 years, and 59% were males. Four patients were on Introduction
peritoneal dialysis, and 60 were on hemodialysis for a me-
dian time of 3.8 years, while 31% were obese. Fever (72%), Dialysis patients carry a higher risk of infectious com-
cough (61%), and diarrhea (22%) were the most common plications, and from early reports, this risk includes com-
symptoms at presentation. Thirty-three percent required ad- plications from the severe acute respiratory syndrome
karger@karger.com © 2021 S. Karger AG, Basel Correspondence to:
www.karger.com/ajn Jason Cobb, jcobb2@emory.edu
coronavirus 2 (SARS-CoV-2) which causes COVID-19. Materials and Methods
In fact, the first US reported death from COVID-19 oc-
Data Selection and Extraction
curred in a hemodialysis patient [1]. Since then, there This study was approved by the Emory University Institution-
have been several reports describing the effect of CO al Review Board. The Emory nephrology consult database and Em-
VID-19 in the dialysis population [2–9]. ory Clinical Data Warehouse (CDW) containing electronical med-
A report of hospitalized COVID-19 patients from Wu- ical records from Emory University Hospital, Emory University
han, China, showed that hemodialysis patients had worse Hospital Midtown, Emory Saint Joseph’s Hospital, and Emory
Johns Creek Hospital were searched to identify all ESKD patients
outcomes compared to controls without kidney failure who were admitted between March 1, 2020, and May 31, 2020. Pa-
[5]. In addition, the hemodialysis COVID-19 patients de- tients undergoing emergency room visits or <24-h observation vis-
veloped serious complications such as shock, acute respi- its were excluded. ESKD was defined as patients receiving mainte-
ratory distress syndrome (ARDS), arrhythmias, and acute nance dialysis prior to admission. ICD10 codes, hemodialysis, and
cardiac injury at a higher rate. The authors concluded that peritoneal dialysis orders were identified. Patients tested for CO-
VID-19 by a polymerase chain reaction (PCR) were selected, and
patients on hemodialysis with COVID-19 were at higher those with positive results were identified. Our institutions used
risk of death (14 vs. 4%) [5]. In a population of hospital- nasopharyngeal samples for COVID-19 testing. Patients were fol-
ized dialysis patients in New York City, there was a 31% lowed until discharge from the hospital or death.
mortality rate and 75% of those who required mechanical Patient data, including sociodemographic information, clinical
ventilation died [2]. This dialysis patient population had data, medication use at time of admission, and laboratory data,
were obtained from the Emory CDW. Manual chart review was
similar mortality outcomes to those reported from Eu- performed on the COVID-19-positive patients. Symptoms on ad-
rope [7–9]. mission, comorbid conditions, and radiographic findings were ex-
Dialysis patients are a high-risk population for trans- tracted manually from the chart. Charlson Comorbidity Index [25]
mission of COVID-19 due to some of their underlying was calculated to determine the burden of comorbidities. Death
comorbidities and logistical difficulties of keeping ad- was defined as an in-hospital death or transfer to hospice for end-
of-life care.
equate social distancing as recommended by CDC
guidelines [6, 10–12]. However, it is unclear whether Statistical Methods
their outcomes are different than the nondialysis popu- Continuous variables were described as median (interquartile
lation. Additionally, new information suggests that the range [IQR]), and categorical variables as frequency rates or per-
rate of asymptomatic COVID-19 infection in dialysis centages. The Mann-Whitney-Wilcoxon test or Student’s t test
was used for comparison of continuous variables, whereas the χ2
patients is substantial [13]. In the USA, African Ameri- test or Fisher’s exact test was used for comparison of categorical
cans progress to end-stage kidney disease (ESKD) at variables. The Shapiro-Wilk test was used to determine distribu-
higher rates [14, 15] and make up nearly 30% of the tion normality of continuous variables. Relative risk of death was
ESKD population [16]. Furthermore, African Ameri- calculated to explore the association of relevant clinical and labora-
cans have been disproportionally affected by the CO- tory findings with mortality. Data processing, analysis, and graph-
ics were performed with R software (R Core Team [2019], R foun-
VID-19 pandemic due to a higher prevalence of comor- dation for Statistical Computing, Vienna, Austria).
bid conditions such as obesity, diabetes, and hyperten-
sion [17–20] and potentially socioeconomic disparities
such as institutional racism, poor housing, front-line
jobs that limit social distancing, and unemployment Results
and loss of health insurance exacerbated by the pan-
demic [21–24]. Patients and Clinical Characteristics
Given the vulnerability of the ESKD and African- From March 1, 2020, to May 31, 2020, 807 ESKD pa-
American populations to COVID-19 exposure and its tients were admitted. 554 of these patients (69%) were
complications, we sought to examine the risk factors, tested for COVID-19 infection. 490 patients tested nega-
clinical characteristics, and outcomes in hospitals serving tive, and 64 patients receiving renal replacement therapy
this patient population. Here we present our early experi- prior to admission had a positive test (12%) and represent
ence with COVID-19 in a predominantly African-Amer- the study population in this report.
ican ESKD population admitted to our large academic These 64 ESKD patients represent 9% of COVID-
health system with special emphasis on factors associated 19-related admissions during the study period. Sixty
with mortality. (94%) patients received in-center hemodialysis, and 4
were on peritoneal dialysis prior to admission. The ma-
jority of patients were African Americans (84%) with a
COVID-19 in Hospitalized ESKD Am J Nephrol 2021;52:190–198 191
DOI: 10.1159/000514752
Table 1. Baseline demographics and comorbidities
Total1 Survivors1 Deceased1 p value2
(N = 64) (n = 53) (n = 11)
Age, years 64 (53–75) 62 (52–69) 75 (69–76) 0.02
Gender, n (%)
Female 26 (41) 23 (43) 3 (27) 0.5
Male 38 (59) 30 (57) 8 (73)
Race, n (%)
African American or black* 54 (84) 43 (81) 11 (100) 0.6
Non-Hispanic Caucasian or white 6 (10) 6 (11) 0 (0)
Hispanic white 4 (6) 4 (7.5) 0 (0)
Vintage 3.8 (2.0–7.0) 3.5 (2.0–6.2) 6.0 (2.4–9.6) 0.4
Charlson Comorbidity Index (age adjusted) 7 (5–9) 6 (5–9) 8 (7–11) 0.06
History of hypertension, n (%) 60 (94) 49 (92) 11 (100) >0.9
History of diabetes, n (%) 31 (58) 9 (82) 0.26
History of CV disease**, n (%) 23 (36) 18 (34) 5 (45) 0.06
Congestive heart failure, n (%) 20 (31) 17 (32) 3 (27) >0.9
Peripheral vascular disease, n (%) 12 (19) 7 (13) 5 (45) 0.03
Chronic lung disease, n (%) 13 (20) 11 (21) 2 (18) >0.9
Arrhythmias, n (%) 11 (17) 9 (17) 2 (18) >0.9
Obesity (body mass index >30), n (%) 20 (31) 17 (32) 3 (27) 0.4
Body mass index 27 (23–33) 27 (23–33) 27 (22–30) >0.8
Dementia, n (%) 8 (12) 7 (13) 1 (9.1) >0.9
History of DVT/PE***, n (%) 6 (9.4) 5 (9.4) 1 (9.1) >0.9
Tobacco abuse, n (%) 24 (38) 17 (32) 7 (64) 0.08
Valvular disease, n (%) 5 (7.8) 4 (7.5) 1 (9.1) >0.9
* All African Americans were non-Hispanic. ** CV disease, coronary artery disease, cerebrovascular accident,
and/or valvular disease. *** DVT/PE, deep venous thrombosis or pulmonary embolism. 1 Statistics presented:
median (IQR); n (%). 2 Comparing survivors with deceased. Statistical tests performed: Wilcoxon rank-sum test,
Fisher’s exact test, and Student’s t test.
median age of 64 years. Fifty-nine percent were males, the Charlson Comorbidity Index. Medications prescribed
and 62% had diabetes. The median time on dialysis was in the outpatient setting and relevant inpatient medica-
3.8 years. These basic demographics are presented in Ta- tions are presented in online suppl. Table A; see www.
ble 1. Gender (59 vs. 53% males), race distribution (84 vs. karger.com/doi/10.1159/000514752 for all online suppl.
75% African Americans), median age (64 vs. 61 years), material. Patients who expired were more likely to have
and BMI (27 vs. 27 kg/m2) were similar in COVID- used renin-angiotensin system blockers (ACEi or ARBs)
19-positive and COVID-19-negative patients. than survivors (64 vs. 30%, p < 0.04).
The most common comorbidities recorded at the time
of admission were hypertension, diabetes, congestive Symptoms and Chest-X-Ray Findings
heart failure, coronary artery disease, peripheral vascular The most common symptoms at presentation were fe-
disease, chronic lung disease, and arrhythmias. There ver (72%), cough (61%), and diarrhea (22%). Dyspnea
were 2 HIV-positive patients. Thirty-one percent of pa- was also reported frequently. Not a single patient report-
tients had a body mass index of >30 kg/m2. A detailed ed anosmia as a symptom. The most common radio-
prevalence of comorbidities is presented in Table 1. Sur- graphic findings were bilateral patchy infiltrates (56%),
vivors were younger (median age 62 vs. 75 years, p = 0.01) pulmonary edema (11%), pleural effusions (6%), and at-
and had a lower prevalence of peripheral vascular disease electasis (5%). Twenty-two percent of chest radiographs
(13 vs. 45%, p = 0.025) compared to nonsurvivors. The were reported as normal or unremarkable at the time of
medical burden of comorbidities was similar as judged by admission.
192 Am J Nephrol 2021;52:190–198 Navarrete/Tong/Cobb/Rahbari-Oskoui/
DOI: 10.1159/000514752 Hosein/Caberto/Lea/Franch
Table 2. Baseline laboratory data
Total1 Survivors1 Deceased1 p value2
(N = 64) (n = 53) (n = 11)
Hemoglobin, g/dL 10.7 (9.2–11.8) 10.7 (9.1–11.7) 10.8 (9.8–11.9) 0.7
WBC, ×103/mL 7.0 (5.2–11.1) 6.0 (4.2–9.3) 8.1 (5.1–14.2) 0.3
Platelets, ×103/mL 210 (142–283) 210 (152–281) 209 (138, 295) 0.8
Lymphocyte count 0.82 (0.56–1.14) 0.84 (0.60–1.29) 0.74 (0.38–0.97) 0.14
Albumin, g/dL 3.8 (3.2–4.0) 3.8 (3.3–4.0) 3.6 (3.2–3.9) 0.5
Calcium, mg/dL 8.9 (8.5–9.4) 8.8 (8.4–9.3) 9.2 (8.9–10.0) 0.06
AST, units/L 28 (19–48) 24 (19–39) 41 (28–148) 0.02
ALT, units/L 14 (10–26) 15 (10–21) 14 (11–60) 0.2
Bilirubin, mg/dL 0.5 (0.4–0.7) 0.5 (0.4–0.7) 0.8 (0.5, 1.3) 0.03
Ferritin, ng/mL 1,800 (1,081–3,633) 1,788 (1,008–2,674) 3,664 (1,760–11,984) 0.2
CRP (admission), mg/dL 106 (51–182) 81 (45–124) 174 (138–267) <0.01
CRP (maximal), mg/mL 162 (65–198) 116 (49–191) 245 (177–333) 0.01
BNP, pg/mL 576 (291–2,046) 575 (268–1,650) 1,545 (205–2,115) 0.4
Troponin I, ng/mL 0.07 (0.04–0.23) 0.07 (0.04–0.11) 0.25 (0.06–0.87) 0.06
D-dimer (admission), ng/mL 1,736 (1,168–3,502) 1,682 (1,155–2,630) 1,844 (1,411–7,355) 0.4
D-dimer (peak), ng/mL 3,114 (1,474–7,728) 2,199 (1,342–4,851) 24,145 (4,172–60,000) <0.001
Lactic acid, mmol/L 1.10 (0.75–1.80) 0.80 (0.70–1.40) 1.90 (1.28–2.70 0.4
LDH, unit/L 371 (268–534) 371 (268–524) 424 (290–3,135) 0.4
WBC, white blood cell count; AST, aspartate aminotransferase; ALT, alanine aminotransferase; CRP,
C-reactive protein; BNP, brain natriuretic peptide; LDH, lactate dehydrogenase. 1 Statistics presented: median
(IQR). 2 Comparing survivors with deceased. Statistical tests performed: Wilcoxon rank-sum test; Fisher’s exact
test.
Laboratory Findings cantly higher AST, CRP, ferritin, hemoglobin, and tropo-
Laboratory data are presented in Table 2. Sixty-nine nin; meanwhile, BNP, lymphocyte count, and overall
percent of COVID-19-positive ESKD patients had lym- WBC count were lower (online suppl. Table B).
phopenia (defined as a lymphocyte count of <1,000 cells/
mL) on admission. All but 3 patients had C-reactive pro- Thromboembolic Complications
tein (CRP) above the normal range for our laboratory. As part of our institution treatment protocol, patients
When tested in 33 patients, ferritin was above 800 ng/dL were categorized based on D-dimer levels and assigned to
in 79% of patients. Troponin I was above the normal different levels of prophylactic anticoagulation or treat-
range (0.04 ng/mL) in 74% of tested patients (n = 47). ment if a thromboembolic event was documented. In
Brain natriuretic peptide (BNP) level was elevated in 89% ESKD COVID-19-positive patients, the median peak D-
of patients. Aspartate aminotransferase (AST), bilirubin, dimer was 3,114 ng/mL (normal upper limit 574 ng/mL)
CRP, and peak D-dimer were statistically higher in pa- with 42% of patients with D-dimer >3,000 ng/mL. Non-
tients who expired during hospitalization. D-dimer survivors had median peak D-dimer levels higher than
reached their peak level after a median of 5 days (IQR survivors (24,145 vs. 2,199 ng/mL, p = 0.004) (Table 2;
1–19). Troponin I on admission was also higher in non- Fig. 1). Interestingly, ESKD COVID-19-negative patients
survivors, but the difference did not reach statistical sig- admitted during the same period also had elevated D-di-
nificance (Table 2). Interleukin-6 (IL-6) was measured in mer, with a median of 3,124 ng/mL.
only 17 patients with 9 having levels above 5 pg/mL (con- Five patients (8%) developed thromboembolic com-
sidered the upper limit of normal in our reference labora- plications (2 pulmonary embolisms [PE] and 3 leg deep
tory), while 4 of those required ICU admission. None of venous thromboses [DVT]). As a reference, during the
the 8 patients with normal IL-6 levels required ICU ad- same period, only 2% of ESKD COVID-19-negative pa-
mission. In comparison to our COVID-19-negative pa- tients developed thromboembolic complications, 4 PE
tients, ESKD COVID-19-positive patients had signifi- and 8 DVT (relative risk [RR] 3.7, CI: 1.3–10.1). The me-
COVID-19 in Hospitalized ESKD Am J Nephrol 2021;52:190–198 193
DOI: 10.1159/000514752
Color version available online
60,000 10
400
30,000
300
Bilirubin, mg/dL. admission
D-dimer ng/mL. peak level
CRP mg/dL. admission
10,000 3
200
3,000
1
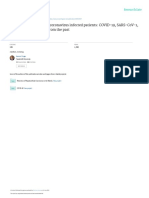
Fig. 1 Comparative serum concentration 100 1,000
levels of admission CRP, peak D-dimer,
and admission bilirubin in COVID-
19-positive (blue circles) and COVID- 300 0.3
0
19-negative (white circles) ESKD patients.
CRP, C-reactive protein.
dian D-dimer in patients with thromboembolic compli- Table 3. Outcomes
cations was 11,533 ng/mL (IQR: 4,406–28,382). We did
not include vascular access thrombosis as a thrombotic Total Survivors1 Deceased1 p value2
(N = 64) (n = 53) (n = 11)
complication.
ICU admission, n (%) 21 (33) 12 (23) 9 (82) <0.001
Outcomes and Factors Associated with Mortality Ventilator, n (%) 15 (23) 6 (11) 9 (82) <0.001
Table 3 describes the most relevant outcomes recorded CRRT use, n (%) 8 (38) 2 (4) 6 (55) <0.001
during hospitalization. Ten patients died, and 1 addition- Hospital days 10 (5–14) 10 (5–13) 11 (6–22) 0.4
al patient was discharged to hospice for end-of-life care CRRT, continuous renal replacement therapy. 1 Statistics
and was counted as a death. Twenty-one patients (33%) presented: n (%); median (IQR). 2 Statistical tests performed:
required admission to ICU. Fifteen patients required me- Fisher’s exact test; Wilcoxon rank-sum test.
chanical ventilation (23%). Sixty-six percent of ESKD
COVID-19-positive patients were discharged home, and
17% required temporary admission to a physical reha-
bilitation facility. Discussion
The mortality rate of ESKD patients with COVID-19
infection was 17%. As a reference, during the same time Dialysis patients are particularly vulnerable to poor
period, there were 490 ESKD patients admitted without outcomes related to COVID-19 due to their underlying
COVID-19. Thirty-eight of them died during their hos- comorbid illnesses and immunosuppression. Also, dialy-
pitalization (8%), and 13 were discharged to terminal sis patients are a high-risk population for transmission of
hospice care (3%) for a mortality rate of 11%. The mortal- COVID-19 due to difficulties to maintain adequate social
ity RR for ESKD patients with COVID-19 was 2.0 (CI: distancing due to attending dialysis sessions thrice week-
1.1–3.8) compared to ESKD patients without COVID-19 ly. We report our outcomes of ESKD patients admitted to
admitted during the same period. our academic health system with COVID-19-positive
Age >65 years (RR 13.7, CI: 1.9–100.7), CRP >100 mg/ tests in a predominantly African-American population.
dL (RR 8.3, CI: 1.1–60.4), peak D-dimer >3,000 ng/mL Our study highlighted specific risk factors for CO
(RR 4.3, CI: 1.03–18.2), bilirubin >1 mg/dL (RR 3.9, CI: VID-19 complications and death that have not been pre-
1.5–10.4), and history of peripheral vascular disease (RR viously reported in the ESKD population. Older age, his-
3.2, CI: 1.2–9.1) were associated with mortality. Figure 1 tory of peripheral vascular disease, and liver function ab-
displays values of D-dimer, CRP, and bilirubin on admis- normalities as well as elevated D-dimer and CRP levels
sion and their relationship with hospital mortality. were independent risk factors for death.
194 Am J Nephrol 2021;52:190–198 Navarrete/Tong/Cobb/Rahbari-Oskoui/
DOI: 10.1159/000514752 Hosein/Caberto/Lea/Franch
The hospital mortality rate seen in our cohort (17%) is VID-19 infection had a RR of death of 2.01 (CI: 1.06–
similar to that seen in a predominantly ethnic Chinese 3.84) compared to hospitalized ESKD patients that tested
ESKD cohort in Wuhan (14%) [5]. The Wuhan cohort negative for COVID-19.
had a similar age, ICU admission rate, and ventilator us- Activation of the coagulation cascade as measured by
age to ours, but their patients had significantly less diabe- D-dimer has emerged as a poor prognostic indicator in
tes and fewer cardiovascular comorbidities. Our cohort’s patients with COVID-19 [32–34]. We are the first to re-
mortality rate was lower than the 31% seen in a predom- port this finding in an ESKD cohort with 10-fold higher
inantly Hispanic cohort from New York. Average age and peak D-dimer in COVID-19-positive patients who died
comorbidities were similar between the 2 cohorts, but the compared to those who survived. The smaller French
New York cohort had higher ICU and ventilator use. Pre- and Spanish cohorts [7, 8] showed a trend for higher D-
dominantly White, European cohorts from Italy, France, dimer in ESKD patients who died compared to survivors,
and Spain had either similar or older ages (61–72 years), but the difference did not reach statistical significance.
similar comorbidities, and higher mortalities (27–31%) We also found elevated D-dimer levels in both ESKD
than our cohort [7–9]. COVID-19-positive and ESKD COVID-19-negative pa-
There are several explanations for our mortality being tients (online suppl. Table B), consistent with the obser-
lower than the European cohorts and similar to a cohort vation that ESKD itself is associated with higher D-dimer
with fewer comorbidities in China. First, our average age levels [35, 36]. Despite not observing any differences in
was lower than the European cohorts, even though co- D-dimer, we report a higher risk of thromboembolic
morbidities were similar. Second, our institutions’ ICU, complications in COVID-19-positive patients compared
ventilator, and dialysis capacity were not overwhelmed to ESKD COVID-19-negative patients. The elevated D-
at any time during the study period. In support of this dimer levels documented in ESKD patients [36, 37] have
explanation, our ICU survival was also significantly not previously been associated with increased mortality.
higher than other institutions [26]. A third explanation However, elevated D-dimer levels correlate with the se-
is that our population is predominantly African Ameri- verity of atherosclerotic burden and history of periph-
can as historically African-American ESKD patients eral vascular disease [38–42]. Studies related to uncover-
have had lower overall mortality rates than whites [27, ing mechanisms for COVID-19 thrombotic complica-
28]. tions are of extreme interest and ongoing [29, 30].
One reason often given for improved survival of Afri- Intensified anticoagulation strategies based exclusively
can Americans on dialysis is greater obesity which has on elevation of D-dimer have not been thoroughly tested
shown a paradoxical relationship with mortality in the in dialysis patients with COVID-19 infection, and con-
dialysis population [27–29]. Consistent with this para- cerns about the risk of bleeding have also been raised
dox, our current report is in contradiction to the general [43]. It is worth mentioning that the highest D-dimer
population affected by COVID-19 by not implicating levels occurred after a median of 5 days of hospitaliza-
obesity as a risk factor for worse outcomes in COVID-19 tion. Given the finding of significantly elevated D-dimer
[20, 30]. However, the New York, Spanish, and French levels in our ESKD COVID-19-negative cohort, dedicat-
ESKD COVID-19 cohorts had similar BMI to our pa- ed studies are needed to answer the issue of appropriate
tients and also showed no significant relationship of BMI and safe anticoagulation beyond standard care in this
with mortality [2, 7–9]. All of these results are consistent population.
with the observation that in dialysis patients, racial back- Data from French and Spanish cohorts agree with
ground does not modify the relationship of BMI with our finding that higher CRP is a powerful marker of
mortality [31]. Thus, obesity does not explain the better mortality. The French cohort found that CRP signifi-
survival seen in our cohort. cantly correlated with death in multivariate analysis
We experienced a lower prevalence of COVID-19 in- along with lactic dehydrogenase and thrombocytopenia
fection among ESKD patients admitted to the hospital [9]. In the Spanish cohort with 36 patients, laboratory
(12%) compared to the Wuhan and Italian cohorts [5, 8]. values were similar to ours with CRP and bilirubin be-
We had time to implement rigorous infection protocols ing significant in both univariate analyses. Age was the
in most of our dialysis centers early on in the pandemic dominant effect on mortality in the limited multivariate
and may have identified patients earlier in the course of analysis [7].
the disease resulting in a reduced risk of more severe In the respiratory tract and vascular endothelium,
complications. Nevertheless, ESKD patients with CO ACEIs and ARBs upregulate cell surface expression of an-
COVID-19 in Hospitalized ESKD Am J Nephrol 2021;52:190–198 195
DOI: 10.1159/000514752
giotensin-converting enzyme 2 (ACE2), the entry point Conclusion
for SARS-CoV-2 [44, 45]. However, higher ACE2 expres-
sion is associated with better outcomes in most viral We report our experience caring for predominantly
pneumonia. Our data provide a signal for potentially African-American ESKD patients hospitalized with CO-
worse outcomes in dialysis patients who were on ACEIs VID-19. Mortality rates are lower than other cohorts, and
and ARBs, but this could be confounding by indication as older age, history of peripheral vascular disease, and ele-
patients on ACEIs and ARBs likely have a higher burden vated CRP, bilirubin, and D-dimer emerged as important
of cardiovascular disease. risk factors for death. Better understanding of risk strati-
Lower lymphocyte counts are a hallmark of CO- fication could potentially lead to more precise targeting
VID-19 disease and are associated with poor outcomes, of therapies for COVID-19 in ESKD. The finding of in-
although it is unclear if the low counts are pathogenic creased D-dimer and lymphopenia in the COVID-
[46]. One study found worse survival in dialysis patients 19-negative dialysis patients raises questions about the
affected by COVID-19 [7]. Similarly, a lower lymphocyte role of these abnormalities in the general ESKD popula-
count has been reported to occur in 50% of the ESKD tion. In summary, our findings provide guidance on risk
population [47]. In our study, the absolute lymphocyte stratification for the vulnerable African-American ESKD
count was indeed lower in the ESKD COVID-19 cohort population and reinforce the need for dialysis centers to
compared to non-COVID-19 patients (online suppl. Ta- remain vigilant in following appropriate infection control
ble B); however, we did not find an association between measures to prevent the spread of the coronavirus.
lymphopenia and increased risk of mortality in the CO-
VID-19 cohort, perhaps due to our low number of patient
deaths. Statement of Ethics
We report that there were no differences in treatment
This study was approved by our institutional review board.
either in regard to anticoagulation or in steroid use
among survivors and nonsurvivors. Anticoagulation
was given to patients with higher D-dimer per hospital
Conflict of Interest Statement
protocol which could influence this finding. Steroids are
recognized now as a potential beneficial therapeutic The authors have no conflicts of interest to declare and have no
agent [48] but were not used during the time period of financial disclosures.
our report. No dialysis patient was offered remdesivir,
and only 6 patients received hydroxychloroquine while
hospitalized. Funding Sources
The low number of deaths likely limited our ability
to detect more statistically significant differences in No funding was received for this work.
other factors typically associated with worse clinical
outcomes in dialysis patients. The lack of racial diver-
sity in this cohort also limits the determination of racial Author Contributions
differences in risk factors and outcomes. However, our Jose E. Navarrete: conception, design, data collection, analysis,
predominantly African-American population is a interpretation of data, manuscript drafting, manuscript revision,
strength because it is compatible with the overrepresen- and lead author. David C. Tong: conception, design, data collec-
tation of African Americans in the non-ESKD popula- tion, analysis, interpretation of data, and manuscript drafting. Ja-
tion affected by COVID-19 and allows identification of son Cobb: conception, design, data collection, interpretation of
data, manuscript drafting, manuscript revision, and correspond-
potential risk factors that may be particularly informa- ing author. Frederic F. Rahbari-Oskoui: conception, design, inter-
tive for future mitigation strategies in this high-risk mi- pretation of data, manuscript drafting, and manuscript revision.
nority population. Our patient population was a 94% Darya Hosein: design, analysis, data collection, interpretation of
hemodialysis modality patient population which was data, and manuscript drafting. Sheryl C. Caberto: data collection,
similar to the ESRD Network 6 with a prevalence of 89% interpretation of data, and manuscript drafting. Janice P. Lea: con-
ception, design, interpretation of data, and manuscript drafting.
[49]. Lastly, the availability of detailed demographic Harold A. Franch: conception, design, analysis, interpretation of
and clinical variables allowed us to provide a more com- data, manuscript drafting, and manuscript revision.
prehensive assessment of putative risk factors for mor-
tality not previously reported.
196 Am J Nephrol 2021;52:190–198 Navarrete/Tong/Cobb/Rahbari-Oskoui/
DOI: 10.1159/000514752 Hosein/Caberto/Lea/Franch
References
1 Watnick S, McNamara E. On the frontline of 14 Norris KC, Williams SF, Rhee CM, Nicholas 28 Abbott KC, Glanton CW, Trespalacios FC,
the COVID-19 outbreak: keeping patients on SB, Kovesdy CP, Kalantar-Zadeh K, et al. He- Oliver DK, Ortiz MI, Agodoa LY, et al. Body
long-term dialysis safe. Clin J Am Soc modialysis disparities in African Americans: mass index, dialysis modality, and survival:
Nephrol. 2020;15(5):710–3. the deeply integrated concept of race in the analysis of the United States renal data system
2 Valeri AM, Robbins-Juarez SY, Stevens JS, social fabric of our society. Semin Dial. 2017; dialysis morbidity and mortality Wave II
Ahn W, Rao MK, Radhakrishnan J, et al. Pre- 30(3):213–23. Study. Kidney Int. 2004;65(2):597–605.
sentation and outcomes of patients with 15 Umeukeje EM, Young BA. Genetics and 29 Kalantar-Zadeh K, Abbott KC, Salahudeen
ESKD and COVID-19. J Am Soc Nephrol. ESKD disparities in African Americans. Am J AK, Kilpatrick RD, Horwich TB. Survival ad-
2020;31(7):1409–15. Kidney Dis. 2019;74(6):811–21. vantages of obesity in dialysis patients. Am J
3 Ma Y, Diao B, Lv X, Zhu J, Chen C, Liu L, et 16 Saran R, Robinson B, Abbott KC, Agodoa Clin Nutr. 2005;81(3):543–54.
al. Epidemiological, clinical, and immunolog- LYC, Bragg-Gresham J, Balkrishnan R, et al. 30 Price-Haywood EG, Burton J, Fort D, Seoane
ical features of a cluster of COVID-19-con- United States renal data system. 2019 USRDS L. Hospitalization and Mortality among black
tracted hemodialysis patients. Kidney Int annual data report: epidemiology of kidney patients and white patients with Covid-19. N
Rep. 2020;5(8):1333–41. disease in the United States. Am J Kidney Dis. Engl J Med. 2020;382(26):2534–43.
4 Wang R, Liao C, He H, Hu C, Wei Z, Hong Z, 2019;73(Suppl 1):A7–A8. 31 Park J, Jin DC, Molnar MZ, Dukkipati R, Kim
et al. COVID-19 in hemodialysis patients: a 17 Gold JAW, Wong KK, Szablewski CM, Patel YL, Jing J, et al. Mortality predictability of
report of 5 cases. Am J Kidney Dis. 2020; PR, Rossow J, da Silva J, et al. Characteristics body size and muscle mass surrogates in
76(1):141–3. and clinical outcomes of adult patients hospi- Asian vs. white and African American hemo-
5 Wu J, Li J, Zhu G, Zhang Y, Bi Z, Yu Y, et al. talized with COVID-19: Georgia, March dialysis patients. Mayo Clin Proc. 2013;88(5):
Clinical features of maintenance hemodialy- 2020. MMWR Morb Mortal Wkly Rep. 2020; 479–86.
sis patients with 2019 novel coronavirus-in- 69(18):545–50. 32 BikdeliBikdeli B, Madhavan MV, Jimenez D,
fected pneumonia in Wuhan, China. Clin J 18 Mohamed MMB, Lukitsch I, Torres-Ortiz Chuich T, Dreyfus I, Driggin E, et al. CO
Am Soc Nephrol. 2020;15(8):1139–45. AE, Walker JB, Varghese V, Hernandez-Ar- VID-19 and thrombotic or thromboembolic
6 Rombolà G, Heidempergher M, Pedrini L, Fa- royo CF, et al. Acute kidney injury associated disease: implications for prevention, anti-
rina M, Aucella F, Messa P, et al. Practical in- with coronavirus disease 2019 in Urban New thrombotic therapy, and follow-up: JACC
dications for the prevention and management Orleans. Kidney360. 2020;1(7):614–22. State-of-the-Art review. J Am Coll Cardiol.
of SARS-CoV-2 in ambulatory dialysis pa- 19 Suleyman G, Fadel RA, Malette KM, Ham- 2020;75:2950–73.
tients: lessons from the first phase of the epi- mond C, Abdulla H, Entz A, et al. Clinical 33 Levi M, Thachil J, Iba T, Levy JH. Coagulation
demics in Lombardy. J Nephrol. 2020; 33(2): characteristics and morbidity associated with abnormalities and thrombosis in patients
193–6. coronavirus disease 2019 in a series of patients with COVID-19. Lancet Haematol. 2020;7(6):
7 Goicoechea M, Sánchez Cámara LA, Macías in metropolitan detroit. JAMA Netw Open. e438–40.
N, Muñoz de Morales A, Rojas ÁG, Bascu- 2020;3(6):e2012270. 34 Guan WJ, Ni ZY, Hu Y, Guan WJ, Ni ZY, Hu
ñana A, et al. COVID-19: clinical course and 20 Stefan N, BirkenfeldBirkenfeld ALAL, Schul- Y, et al. China medical treatment expert group
outcomes of 36 hemodialysis patients in ze MB, Ludwig DS. Obesity and impaired for Covid-19: clinical characteristics of coro-
Spain. Kidney Int. 2020;98(1):27–34. metabolic health in patients with COVID-19. navirus disease 2019 in China. N Engl J Med.
8 Alberici F, Delbarba E, Manenti C, Econimo Nat Rev Endocrinol. 2020;16(7):341–2. 2020;382:1708–20.
L, Valerio F, Pola A, et al. A report from the 21 Crews DC, Purnell TS. COVID-19, racism, 35 Miozzari M, Wahl C. D-dimers in hemodialy-
Brescia renal COVID task force on the clinical and racial disparities in kidney disease: galva- sis patients. Nephron. 2001;88(3):278–9.
characteristics and short-term outcome of he- nizing the kidney community response. J Am 36 Gordge MP, Faint RW, Rylance PB, Ireland
modialysis patients with SARS-CoV-2 infec- Soc Nephrol. 2020;31(8):1–3. H, Lane DA, Neild GH. Plasma D dimer: a
tion. Kidney Int. 2020;98(1):20–6. 22 Kullar R, Marcellin JR, Swartz TH, Piggott useful marker of fibrin breakdown in renal
9 Tortonese S, Scriabine I, Anjou L, Loens C, DA, Macias Gil R, Mathew TA, et al. Racial failure. Thromb Haemost. 1989;61(3):522–5.
Michon A, Benabdelhak M, et al. COVID-19 disparity of coronavirus disease 2019 in Afri- 37 Spring JL, Winkler A, Levy JH. The influence
in patients on maintenance dialysis in the Par- can American Communities. J Infect Dis. of various patient characteristics on D-dimer
is region. Kidney Int Rep. 2020 Sep; 5(9): 2020;222:890–3. concentration in critically ill patients and its
1535–44. 23 Centor RM, Essien UR. Disparities and CO- role as a prognostic indicator in the intensive
10 Xiong F, Tang H, Liu L, Tu C, Tian JB, Lei CT, VID-19. Ann Intern Med. 2020;16:172. care unit setting. Clin Lab Med. 2014; 34(3):
et al. Clinical characteristics of and medical 24 Johnson-Mann C, Hassan M, Johnson S. CO- 675–86.
interventions for COVID-19 in hemodialysis VID-19 pandemic highlights racial health in- 38 Gubensek J, Lolic M, Ponikvar R, Buturovic-
patients in Wuhan, China. J Am Soc Nephrol. equities. Lancet Diabetes Endocrinol. 2020; Ponikvar J. D-dimer levels in maintenance
2020;31(7):1387–97. 8(8):663–4. hemodialysis patients: high prevalence of
11 Ikizler TA, Kliger AS. Minimizing the risk of 25 Charlson ME, Pompei P, Ales KL, MacKenzie positive values also in the group without pre-
COVID-19 among patients on dialysis. Nat CR. A new method of classifying prognostic disposing diseases. Hemodial Int. 2016;20(2):
Rev Nephrol. 2020;16(6):311–3. comorbidity in longitudinal studies: develop- 198–203.
12 Corbett RW, Blakey S, Nitsch D, Loucaidou ment and validation. J Chronic Dis. 1987; 39 Dubin R, Cushman M, Folsom AR, Fried LF,
M, McLean A, Duncan N, et al. Epidemiology 40(5):373–83. Palmas W, Peralta CA, et al. Kidney function
of COVID-19 in an Urban dialysis center. J 26 Auld SC, Caridi-Scheible M, Blum M, Robi- and multiple hemostatic markers: cross sec-
Am Soc Nephrol. 2020;31(8):1815–23. chaux C, Kraft C, Jacob JT, et al. ICU and ven- tional associations in the multi-ethnic study
13 Clarke C, Prendecki M, Dhutia A, Ali MA, Sa- tilator mortality among critically ill adults of atherosclerosis. BMC Nephrol. 2011;12(3):
jjad H, Shivakumar O, et al. High prevalence with coronavirus disease 2019. Crit Care Med. 3.
of asymptomatic COVID-19 infection in he- 2020;48:e799–e804.
modialysis patients detected using serological 27 Held PJ, Pauly MV, Diamond L. Survival
screening. J Am Soc Nephrol. 2020 Sep;31(9): analysis of patients undergoing dialysis.
1969–75. JAMA. 1987;257(5):645–50.
COVID-19 in Hospitalized ESKD Am J Nephrol 2021;52:190–198 197
DOI: 10.1159/000514752
40 Lassila R, Peltonen S, Lepäntalo M, Saarinen 43 Al-Samkari H, Karp Leaf RS, Dzik WH, Carl- tematic review and meta-analysis. J Intensive
O, Kauhanen P, Manninen V. Severity of pe- son JCT, Fogerty AE, Waheed A, et al. COV- Care. 2020;8:36.
ripheral atherosclerosis is associated with fi- ID-19 and coagulation: bleeding and throm- 47 Agarwal R, Light RP. Patterns and prognostic
brinogen and degradation of cross-linked fi- botic manifestations of SARS-CoV-2 infec- value of total and differential leukocyte count
brin. Arterioscler Thromb. 1993; 13(12): tion. Blood. 2020;136(4):489–500. in chronic kidney disease. Clin J Am Soc
1738–42. 44 Messerli FH, Siontis GCM, Rexhaj E. COV- Nephrol. 2011;6(6):1393–9.
41 Lee AJ, Fowkes FG, Lowe GD, Rumley A. Fi- ID-19 and renin angiotensin blockers: cur- 48 Horby P, Lim WS, Emberson JR, Mafham M,
brin D-dimer, haemostatic factors and pe- rent evidence and recommendations. Circu- Bell JL, Linsell L, et al. Dexamethasone in hos-
ripheral arterial disease. Thromb Haemost. lation. 2020;141(25):2042–4. pitalized patients with covid, preliminary re-
1995;74(3):828–32. 45 Fosbøl EL, Butt JH, Østergaard L, Andersson port. N Engl J Med. 2021 Feb 25;384(8):693–
42 Milburn JA, Ford I, Cassar K, Fluck N, C, Selmer C, Kragholm K, et al. Association of 704.
Brittenden J. Platelet activation, coagula- angiotensin-converting enzyme inhibitor or 49 United States Renal Data System. 2018
tion activation and C-reactive protein in angiotensin receptor blocker use with COV- USRDS annual data report: epidemiology of
simultaneous samples from the vascular ID-19 diagnosis and mortality. JAMA. 2020; kidney disease in the United States. Bethesda,
access and peripheral veins of haemodialy- 324:168–77. MD: National Institutes of Health, National
sis patients. Int J Lab Hematol. 2012; 34(1): 46 Huang I, Pranata R. Lymphopenia and severe Institute of Diabetes and Digestive and Kid-
52–8. coronavirus disease-2019 (COVID-19): sys- ney Diseases; 2018.
198 Am J Nephrol 2021;52:190–198 Navarrete/Tong/Cobb/Rahbari-Oskoui/
DOI: 10.1159/000514752 Hosein/Caberto/Lea/Franch
You might also like
- 10.5811@westjem.2020.6.47919 (2) 81105Document7 pages10.5811@westjem.2020.6.47919 (2) 81105Giovan GaulNo ratings yet
- Covid and CancerDocument11 pagesCovid and Cancerriska silviaNo ratings yet
- Pone 0239443Document8 pagesPone 0239443silviaNo ratings yet
- Covid 19 InfectionDocument2 pagesCovid 19 InfectionGheavita Chandra DewiNo ratings yet
- COVID-19 Severity and COVID-19-Associated Deaths Among Hospitalized Patients With HIV Infection - Zambia, March-December 2020Document4 pagesCOVID-19 Severity and COVID-19-Associated Deaths Among Hospitalized Patients With HIV Infection - Zambia, March-December 2020Kelven Estolloso EndricoNo ratings yet
- Circulating Markers of Angiogenesis and Endotheliopathy in COVID-19Document4 pagesCirculating Markers of Angiogenesis and Endotheliopathy in COVID-19Gonçalo MadureiraNo ratings yet
- Jurnal 7Document4 pagesJurnal 7Ariqa AzzhraNo ratings yet
- Underlying Medical Conditions and Immunosuppresive Medication COVID-19Document7 pagesUnderlying Medical Conditions and Immunosuppresive Medication COVID-19BhaviniNo ratings yet
- 4) Komorbid Dan Usia (Rebecca) 10.1002@art.41456Document25 pages4) Komorbid Dan Usia (Rebecca) 10.1002@art.41456Mastifa HanasitaNo ratings yet
- Covid Er ArticleDocument6 pagesCovid Er ArticleReeb BukhariNo ratings yet
- 2845-Article Text-24370-1-10-20210427Document10 pages2845-Article Text-24370-1-10-20210427DamNo ratings yet
- Acute Kidney Injury in Patients Hospitalized With COVID-19: ClinicalinvestigationDocument10 pagesAcute Kidney Injury in Patients Hospitalized With COVID-19: ClinicalinvestigationYunita AmiliaNo ratings yet
- AKI in Hospitalized Patients With and Without COVID-19 - A Comparison Study (JASN 20)Document13 pagesAKI in Hospitalized Patients With and Without COVID-19 - A Comparison Study (JASN 20)agboxNo ratings yet
- COVID-19 in Kidney Transplant Recipients: Original ArticleDocument7 pagesCOVID-19 in Kidney Transplant Recipients: Original ArticleGeysel SuarezNo ratings yet
- Meta 7Document11 pagesMeta 7Jonathan AiresNo ratings yet
- InternacionalDocument9 pagesInternacionalbryan ronaldNo ratings yet
- MyelomaDocument2 pagesMyelomaCookies CreamNo ratings yet
- Prevalence and Risk Factors of Mortality Among Hospitalized Patients PDFDocument26 pagesPrevalence and Risk Factors of Mortality Among Hospitalized Patients PDFMohamat MutajirNo ratings yet
- Acknowledgement & DedicationDocument20 pagesAcknowledgement & DedicationIceMaster MinatoNo ratings yet
- Acute Kidney Injury in COVID-19: A Single-Center Experience in NigeriaDocument8 pagesAcute Kidney Injury in COVID-19: A Single-Center Experience in NigeriaYUSUF MUSANo ratings yet
- Acute Kidney Injury in Patients Hospitalized With COVID-19Document11 pagesAcute Kidney Injury in Patients Hospitalized With COVID-19fannyNo ratings yet
- COVID 19 in Kidney Transplant RecipientsDocument11 pagesCOVID 19 in Kidney Transplant RecipientsDouglas SantosNo ratings yet
- Epidemiology of Covvid19 2021Document29 pagesEpidemiology of Covvid19 2021Chainsaw ManNo ratings yet
- Rüthrich2021 Article COVID-19InCancerPatientsClinicDocument11 pagesRüthrich2021 Article COVID-19InCancerPatientsClinicdianaNo ratings yet
- AKI in Hospitalized Patients With COVID19Document32 pagesAKI in Hospitalized Patients With COVID19Hue JacksonNo ratings yet
- Journal Pre-Proof: Prevalence and Predictors of In-Hospital Mortality of Patients Hospitalized With COVID-19 InfectionDocument29 pagesJournal Pre-Proof: Prevalence and Predictors of In-Hospital Mortality of Patients Hospitalized With COVID-19 InfectionMohammed Shuaib AhmedNo ratings yet
- Articulo OriginalDocument9 pagesArticulo Originalale zunigaNo ratings yet
- SMJ 2000 - Covid Research (Re-Write) .EditedDocument21 pagesSMJ 2000 - Covid Research (Re-Write) .EditedFarheen AhmedNo ratings yet
- News & Views: CKD Is A Key Risk Factor For COVID-19 MortalityDocument2 pagesNews & Views: CKD Is A Key Risk Factor For COVID-19 Mortalityrini trismiatiNo ratings yet
- 1.clinical Characteristics of 28 PatientsDocument7 pages1.clinical Characteristics of 28 PatientsTeguh WibowoNo ratings yet
- A Novel Severity Score To Predict Inpatient Mortality in COVID 19 PatientsDocument8 pagesA Novel Severity Score To Predict Inpatient Mortality in COVID 19 PatientsanscstNo ratings yet
- Artikel Covid-19Document9 pagesArtikel Covid-19nhshivani532000No ratings yet
- Henry2020Document8 pagesHenry2020TisaNo ratings yet
- Estudo DiabetesDocument9 pagesEstudo DiabetesFulano de TalNo ratings yet
- Clinical Microbiology and InfectionDocument6 pagesClinical Microbiology and InfectionMiguel AngelNo ratings yet
- 1 s2.0 S1936523323000955 MainDocument12 pages1 s2.0 S1936523323000955 MainDiana AyuNo ratings yet
- IJC 9999 NaDocument29 pagesIJC 9999 NaSimona VisanNo ratings yet
- Journal of Clinical Virology: SciencedirectDocument5 pagesJournal of Clinical Virology: Sciencedirectsameer sahaanNo ratings yet
- Chakra - Factors Associated With Complications of C DiffDocument8 pagesChakra - Factors Associated With Complications of C DiffCherry SmileNo ratings yet
- Clinical Characteristics of 116 Hospitalized Patients With COVID-19 in Wuhan, China: A Single-Centered, Retrospective, Observational StudyDocument11 pagesClinical Characteristics of 116 Hospitalized Patients With COVID-19 in Wuhan, China: A Single-Centered, Retrospective, Observational Studykristina dewiNo ratings yet
- Clinical Characteristics and Risk Factors of Cardiac Involvement in COVID-19Document11 pagesClinical Characteristics and Risk Factors of Cardiac Involvement in COVID-19Yerlis OspinoNo ratings yet
- COVID-19 in HIV: A Review of Published Case ReportsDocument11 pagesCOVID-19 in HIV: A Review of Published Case Reports6ixSideCreate MNo ratings yet
- 01 CCM 0000119424 31648 1eDocument6 pages01 CCM 0000119424 31648 1eumi far ainNo ratings yet
- Covid-19 and Coagulation: Bleeding and Thrombotic Manifestations of Sars-Cov-2 InfectionDocument12 pagesCovid-19 and Coagulation: Bleeding and Thrombotic Manifestations of Sars-Cov-2 InfectionDavid Mamani CardenasNo ratings yet
- Safety Update: COVID-19 Convalescent Plasma in 20,000 Hospitalized PatientsDocument10 pagesSafety Update: COVID-19 Convalescent Plasma in 20,000 Hospitalized PatientsVeloz RedNo ratings yet
- Fonc 12 857076Document10 pagesFonc 12 857076meenakshi.r.agrawalNo ratings yet
- Hematologic Complications in Patients Hospitalized With COVID 19 InfectionDocument7 pagesHematologic Complications in Patients Hospitalized With COVID 19 Infectionedson floresNo ratings yet
- Managing Patients With Hematological Malignancies During COVID 19 PandemicDocument8 pagesManaging Patients With Hematological Malignancies During COVID 19 PandemicSONIA MARLENE HUARACHE HERRERANo ratings yet
- Association of Procalcitonin Levels With The Progression and Prognosis of Hospitalized Patients With COVID-19Document9 pagesAssociation of Procalcitonin Levels With The Progression and Prognosis of Hospitalized Patients With COVID-19Dian Putri NingsihNo ratings yet
- Articulo 6 - OkDocument10 pagesArticulo 6 - OkLinda Elisa Gutierrez FloresNo ratings yet
- Usefulness of Elevated Troponin To Predict Death in Patients With COVID-19 and Myocardial InjuryDocument7 pagesUsefulness of Elevated Troponin To Predict Death in Patients With COVID-19 and Myocardial InjurySilvhy yujraNo ratings yet
- 34409900: Evaluating Red Blood Cell Distribution Width From Community Blood Tests As A Predictor of Hospitalization and Mortality in Adults With SARS-CoV-2 A Cohort StudyDocument10 pages34409900: Evaluating Red Blood Cell Distribution Width From Community Blood Tests As A Predictor of Hospitalization and Mortality in Adults With SARS-CoV-2 A Cohort StudyNico Angelo CopoNo ratings yet
- RISK of Thromboembolism in Patient With Covid 19 MétaanalysisDocument14 pagesRISK of Thromboembolism in Patient With Covid 19 MétaanalysisDelgado OnthemixNo ratings yet
- Renal Resistive Index As A Predictor of Acute Kidney Injury and Mortality in COVID-19 Critically Ill PatientsDocument8 pagesRenal Resistive Index As A Predictor of Acute Kidney Injury and Mortality in COVID-19 Critically Ill PatientsEko NoviantiNo ratings yet
- Acute Kidney Injury in COVIDDocument16 pagesAcute Kidney Injury in COVIDYUSUF MUSANo ratings yet
- The Effects of Alzheimer's and Parkinson's Disease FATHIDocument9 pagesThe Effects of Alzheimer's and Parkinson's Disease FATHICamila BarbosaNo ratings yet
- Coagulation Disorders in Coronavirus Infected PatientsDocument6 pagesCoagulation Disorders in Coronavirus Infected PatientsQuang TrầnNo ratings yet
- Journal Pre-Proof: Journal of Clinical VirologyDocument18 pagesJournal Pre-Proof: Journal of Clinical VirologyOkki Wahyu AtikasariNo ratings yet
- Epidemiology of Covid - 19 Hemodialysis Patients at The Military Hospital of RabatDocument7 pagesEpidemiology of Covid - 19 Hemodialysis Patients at The Military Hospital of RabatIJAR JOURNALNo ratings yet
- Summary of Brian Tyson, George Fareed & Mathew Crawford's Overcoming the COVID DarknessFrom EverandSummary of Brian Tyson, George Fareed & Mathew Crawford's Overcoming the COVID DarknessNo ratings yet
- COVID-19 and The Kidney: From Epidemiology To Clinical PracticeDocument29 pagesCOVID-19 and The Kidney: From Epidemiology To Clinical Practicemariatul fithriasariNo ratings yet
- Epidemiology and Outcomes of Acute Kidney Injury in COVID-19 Patients With Acute Respiratory Distress Syndrome: A Multicenter Retrospective StudyDocument7 pagesEpidemiology and Outcomes of Acute Kidney Injury in COVID-19 Patients With Acute Respiratory Distress Syndrome: A Multicenter Retrospective Studymariatul fithriasariNo ratings yet
- Hyperkalemia: Samir El AnsaryDocument45 pagesHyperkalemia: Samir El Ansarymariatul fithriasariNo ratings yet
- SCIENTIFIC SCHEDULE JNHC AND SH 2014 - Updated 15042014 - SenttomemberDocument4 pagesSCIENTIFIC SCHEDULE JNHC AND SH 2014 - Updated 15042014 - Senttomembermariatul fithriasariNo ratings yet
- ADVANCE-On EASD Study Rationale and DesignDocument26 pagesADVANCE-On EASD Study Rationale and Designmariatul fithriasariNo ratings yet
- ADVANCE-On EASD Glucose Arm ResultsDocument32 pagesADVANCE-On EASD Glucose Arm Resultsmariatul fithriasariNo ratings yet
- Adeera Levin Ckd-Cv-Lipid-Sharp Web HandoutsDocument12 pagesAdeera Levin Ckd-Cv-Lipid-Sharp Web Handoutsmariatul fithriasariNo ratings yet
- FCPS SurgeryDocument106 pagesFCPS Surgeryrehan hayderNo ratings yet
- Motor Neurone Disease: J GormallyDocument14 pagesMotor Neurone Disease: J GormallyBambang SutrisnoNo ratings yet
- Iron-Refractory Iron Deficiency Anemia May Not Lead To Neurocognitive Dysfunction: A Case ReportDocument6 pagesIron-Refractory Iron Deficiency Anemia May Not Lead To Neurocognitive Dysfunction: A Case ReportwitwiiwNo ratings yet
- Prostaglandins in Pregnancy: Scott W. Walsh, PHDDocument21 pagesProstaglandins in Pregnancy: Scott W. Walsh, PHDIrene AtimNo ratings yet
- Chronic Limb Ischaemia: MR Hanif Hussein Consultant Vascular Surgeon, HKLDocument35 pagesChronic Limb Ischaemia: MR Hanif Hussein Consultant Vascular Surgeon, HKLZulzaire ZulkefliNo ratings yet
- Types of Feeding-GastrostomyDocument8 pagesTypes of Feeding-GastrostomyElda KuizonNo ratings yet
- DrainsDocument19 pagesDrainspaulineNo ratings yet
- 2121-Article Text-9456-1-10-20230131Document8 pages2121-Article Text-9456-1-10-20230131Çağdaş BaytarNo ratings yet
- Principles of Emergency MedicineDocument2 pagesPrinciples of Emergency MedicinekavithaNo ratings yet
- Clinical Handbook of Insomnia (2017)Document292 pagesClinical Handbook of Insomnia (2017)jcholguin.conciencia4100100% (7)
- Walking: The 'Wonder Drug': VocabularyDocument3 pagesWalking: The 'Wonder Drug': VocabularyLiveLaugh LoveNo ratings yet
- Chapter 1: Introduction To Operative DentistryDocument11 pagesChapter 1: Introduction To Operative DentistryMariam AdnanNo ratings yet
- Punjab Public Service CommissionDocument2 pagesPunjab Public Service CommissionShehnila ShoukatNo ratings yet
- 13 - Digestive System - FullDocument29 pages13 - Digestive System - FullSamson Lee Yun ShenNo ratings yet
- Hemotology ReviewDocument61 pagesHemotology ReviewSukma EffendyNo ratings yet
- Diarrhoea Patient InformationDocument3 pagesDiarrhoea Patient InformationIgor DemićNo ratings yet
- Prev Med and Public Health Review ExamDocument6 pagesPrev Med and Public Health Review ExamRosel Ann BontiaNo ratings yet
- Urine Culture: D.M.M. LabDocument15 pagesUrine Culture: D.M.M. LabTomi RahmadaniNo ratings yet
- Sacra Men To Medical Transportation ServicesDocument2 pagesSacra Men To Medical Transportation ServicesSACPROS INC.No ratings yet
- HS Instructor ManualDocument122 pagesHS Instructor ManualJames Cojab SacalNo ratings yet
- Shock Comparison ChartDocument2 pagesShock Comparison Chartlinnaete88% (8)
- DR - Jetty - Executive Summary of Perioperative ManagementDocument28 pagesDR - Jetty - Executive Summary of Perioperative ManagementDilaNo ratings yet
- Nursing Care Plan - Activity IntoleranceDocument1 pageNursing Care Plan - Activity IntoleranceLei Ortega67% (9)
- Giardia Duodenalis Affect Farmers Child Growth and DevelopmentDocument2 pagesGiardia Duodenalis Affect Farmers Child Growth and DevelopmentAnitaNo ratings yet
- Restoration of The Worn Dentition. Part 2Document7 pagesRestoration of The Worn Dentition. Part 2Isharajini Prasadika Subhashni GamageNo ratings yet
- Fitzpatricks Dermatology in General Medicine 8ed 1Document10 pagesFitzpatricks Dermatology in General Medicine 8ed 1ANTINNo ratings yet
- Antimicrobial Effect of Aqueous Banana Peel Extract, IraqDocument4 pagesAntimicrobial Effect of Aqueous Banana Peel Extract, IraqLilis KhusnulNo ratings yet
- GTG 37bDocument32 pagesGTG 37bKadelsy BristolNo ratings yet
- Critical Hits Rolls by Josef Tham, v2.0 atDocument3 pagesCritical Hits Rolls by Josef Tham, v2.0 atghostvalleyNo ratings yet
- Tuesday 14 January 2020: BiologyDocument24 pagesTuesday 14 January 2020: Biologysham80% (5)