Professional Documents
Culture Documents
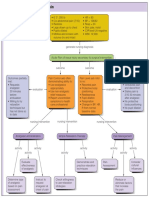
Nursing care plan for patient with acute pancreatic pain
Uploaded by
Kate Aenyle AgsoyOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Nursing care plan for patient with acute pancreatic pain
Uploaded by
Kate Aenyle AgsoyCopyright:
Available Formats
CU-QMS-NURSING-0017
CAPITOL UNIVERSITY
COLLEGE OF NURSING
Name of Student: _________________________________________________ Date of Assignment: ________________________________
Name of Patient: _________________________________________________ Ward: ____________________ Bed No. ________________
NURSING CARE PLAN
ASSESSMENT DATA NURSING DIAGNOSIS GOALS AND NURSING INTERVENTIONS AND EVALUATION
(Subjective & Objective Cues) (Problem and Etiology) OBJECTIVES RATIONALE
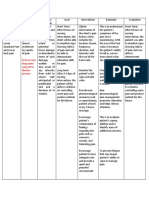
Subjective: Acute Pain related to inflammatory Within 6 hr of intervention, Assess for and document the degree and The patient will:
The patient states “I can feel process of the pancreas the patient’s subjective character of the patient’s Report pain is
abdominal pain that radiates to my perception of discomfort discomfort. Devise a pain scale with the controlled.
back and I loss my appetite” decreases, and it is controlled patient, rating discomfort on Follow prescribed
within 24 hr, as documented a scale of 0 (no pain) to 10 (worst pain). therapeutic
Objective: by pain scale. Nonverbal Rationale: Pain characteristics may signal regimen.
Yellowing of skin and the indicators, such as grimacing varying problems. Baseline and subsequent Demonstrate use of
whites of the eyes (jaundice) and splinting of abdominal use of a pain scale helps methods that
Itchy skin muscles, are absent or determine effectiveness of pain relief. provide relief.
unintended weight loss diminished.
Assess the patient’s previous responses to
Lab results: pain and previously effective
Light-colored stools pain relief measures.
Dark-colored urine Rationale: The patient’s previous history of
pain and how well it was managed
influence perceptions and trust in present
pain relief measures.
Maintain bedrest during acute attack.
Provide quiet, restful environment.
Rationale: Decreases metabolic rate and GI
stimulation and secretions, thereby reducing
pancreatic activity.
Provide alternative comfort measures (back
rub), encourage relaxation techniques
(guided imagery, visualization), quiet
diversional activities (TV, radio).
Rationale: Promotes relaxation and enables
patient to refocus attention; may enhance
coping.
Administer analgesics in timely manner
(smaller, more frequent doses).
Rationale: Severe and prolonged pain can
aggravate shock and is more difficult to
relieve, requiring larger doses of
medication, which can mask underlying
problems and complications and may
contribute to respiratory depression.
Issue: 05 April 2006 Revision Code : 003
CU-QMS-NURSING-0018
You might also like
- Nursing Care Plan For Labor Pain FinaloutputDocument2 pagesNursing Care Plan For Labor Pain FinaloutputVic Intia Paa100% (5)
- Pain Management Guidelines 15-11-2012Document62 pagesPain Management Guidelines 15-11-2012Galuh NurfadillahNo ratings yet
- NCP-Acute PainDocument2 pagesNCP-Acute PainMatt Reyes Del CastilloNo ratings yet
- Nursing Care Plan: Chronic PancreatitisDocument8 pagesNursing Care Plan: Chronic PancreatitisAnne B. Buenvenida100% (2)
- Subjective: Long Term: Independent:: Iloilo Doctors' College College of NursingDocument5 pagesSubjective: Long Term: Independent:: Iloilo Doctors' College College of NursingAbie Jean Balbontin100% (1)
- Nursing Care Plan For CholecystitisDocument4 pagesNursing Care Plan For CholecystitisEemyaj Jaymee88% (8)
- Patient NCPDocument8 pagesPatient NCPlouie john abilaNo ratings yet
- Nursing Care Plan for Postpartum PainDocument2 pagesNursing Care Plan for Postpartum PainJoseph Nawen Sindiong100% (1)
- NCP - Acute Abdominal PainDocument3 pagesNCP - Acute Abdominal PainJet Bautista100% (2)
- Demonstrate: Pain Coping TechniquesDocument4 pagesDemonstrate: Pain Coping TechniquesMae Therese B. MAGNO100% (1)
- Physical Education and Health 2: IN Grade 11 Quarter 4, Module 5Document9 pagesPhysical Education and Health 2: IN Grade 11 Quarter 4, Module 5triicciaa faithNo ratings yet
- Action Plan Health Week 2021-2022Document2 pagesAction Plan Health Week 2021-2022Laarni Kiamco Ortiz Epan100% (2)
- Nursing Assessment and Interventions for Acute Chest PainDocument3 pagesNursing Assessment and Interventions for Acute Chest PainAjay SupanNo ratings yet
- NCP NephrolithiasisDocument3 pagesNCP NephrolithiasisMANUEL EMERSONNo ratings yet
- Pain - Post Partum MotherDocument2 pagesPain - Post Partum Motherulrikov91% (11)
- Nursing Care Plan-Epigastric PainDocument2 pagesNursing Care Plan-Epigastric PainK-anne Cherubic100% (3)
- Acute Gastritis NCPDocument6 pagesAcute Gastritis NCPCharlene Grace ReginoNo ratings yet
- NCP-Acute Postpartum Perineal PainDocument2 pagesNCP-Acute Postpartum Perineal PainFrenzylane Diane CoralNo ratings yet
- NCP Charm EditedDocument6 pagesNCP Charm EditedampogeNo ratings yet
- Arthritis NCPDocument2 pagesArthritis NCPTri Sha100% (3)
- NCP LymphomaDocument3 pagesNCP Lymphomamahmoud fuqahaNo ratings yet
- Assessment Diagnosis Planning Intervention Rationale EvaluationDocument5 pagesAssessment Diagnosis Planning Intervention Rationale EvaluationArian May MarcosNo ratings yet
- NURSING CARE PLAN of Hodgkin's Lymphoma: Assessment Nursing Diagnosis Planning Nursing Interventions Rationale EvaluationDocument5 pagesNURSING CARE PLAN of Hodgkin's Lymphoma: Assessment Nursing Diagnosis Planning Nursing Interventions Rationale Evaluationjoyrena ochondraNo ratings yet
- Flank Pain, Anxiety...Document7 pagesFlank Pain, Anxiety...reneighdNo ratings yet
- Nursing Care Plan: Assessment Planning Interventions Rationale EvaluationDocument2 pagesNursing Care Plan: Assessment Planning Interventions Rationale EvaluationVanessa Belmonte AzurinNo ratings yet
- Nursing Care Plan for Acute PainDocument2 pagesNursing Care Plan for Acute Painunnamed person100% (1)
- Heart Clinic: Alternative Learning System Related Learning ExperienceDocument8 pagesHeart Clinic: Alternative Learning System Related Learning ExperienceEdson John DemayoNo ratings yet
- Iloilo Doctors' College College of Nursing West Avenue, Molo, Iloilo City NURSING CARE PLAN - Acute PancreatitisDocument2 pagesIloilo Doctors' College College of Nursing West Avenue, Molo, Iloilo City NURSING CARE PLAN - Acute PancreatitisKiara Denise TamayoNo ratings yet
- Assessment Nursing Diagnosis Scientific Explanation Planning Intervention Rationale Evaluation IndeoendentDocument3 pagesAssessment Nursing Diagnosis Scientific Explanation Planning Intervention Rationale Evaluation IndeoendentDiane Sarino CabonceNo ratings yet
- NCP 1Document2 pagesNCP 1oguitekim1No ratings yet
- Managing Pain and Constipation Through Targeted Nursing InterventionsDocument4 pagesManaging Pain and Constipation Through Targeted Nursing InterventionsCiara ManguiatNo ratings yet
- Nursing Care Plan: Assessment Diagnosis Planning Intervention Rationale EvaluationDocument1 pageNursing Care Plan: Assessment Diagnosis Planning Intervention Rationale EvaluationJoselyn M. LachicaNo ratings yet
- Nursing Diagnosis, Goals, and Interventions for Acute Pain, Nutrition Imbalance, and Fluid Volume DeficitDocument5 pagesNursing Diagnosis, Goals, and Interventions for Acute Pain, Nutrition Imbalance, and Fluid Volume DeficitAngelica ValeraNo ratings yet
- Assessment Nursing Diagnosis Analysis Planning Implementation Rationale EvaluationDocument1 pageAssessment Nursing Diagnosis Analysis Planning Implementation Rationale EvaluationAnne Beatriz SantiagoNo ratings yet
- NCP Activity NavidasDocument2 pagesNCP Activity NavidasFran LanNo ratings yet
- NCP Acute Pain RT CancerDocument3 pagesNCP Acute Pain RT CancerCharissa Magistrado De LeonNo ratings yet
- Mga NCP For Preterm Birth Case 2Document9 pagesMga NCP For Preterm Birth Case 2John Rendel LopezNo ratings yet
- Nursing Care Plan: Clinical Portrait Pertinent DataDocument4 pagesNursing Care Plan: Clinical Portrait Pertinent DataChristine GallegoNo ratings yet
- No Diagnose Liver Cancer NOC NIC Nutrition Imbalance Less Body Requirements Nutrition ManagementDocument2 pagesNo Diagnose Liver Cancer NOC NIC Nutrition Imbalance Less Body Requirements Nutrition ManagementBobbye MardaNo ratings yet
- Nursing interventions for pain and nutrition managementDocument8 pagesNursing interventions for pain and nutrition managementNyeam NyeamNo ratings yet
- Nursing Care Plan: Acute Pain Related To Inflammatory Response Secondary To InfectionDocument2 pagesNursing Care Plan: Acute Pain Related To Inflammatory Response Secondary To InfectionTammy De GuzmanNo ratings yet
- Subjective Cues: Short Term Goal: Short Term GoalDocument4 pagesSubjective Cues: Short Term Goal: Short Term GoalLarr SumalpongNo ratings yet
- NCP NewDocument16 pagesNCP Newmsfts.No ratings yet
- ASSESSMENT DIAGNOSIS PLANNING INTERVENTIONDocument2 pagesASSESSMENT DIAGNOSIS PLANNING INTERVENTIONArianne BalodNo ratings yet
- Nursing Care Plans for Pain & Pressure Ulcer ManagementDocument25 pagesNursing Care Plans for Pain & Pressure Ulcer ManagementZhyraine CaluzaNo ratings yet
- Acute Pain - Marcos NCPDocument4 pagesAcute Pain - Marcos NCPArian May MarcosNo ratings yet
- Potts Disease NCP .. JustificationDocument8 pagesPotts Disease NCP .. JustificationMicah SalesNo ratings yet
- Gastric Ulcer Nursing CareDocument6 pagesGastric Ulcer Nursing CareAesthea BondadNo ratings yet
- Acute PainDocument1 pageAcute Painnursing concept mapsNo ratings yet
- Care PlanDocument2 pagesCare PlanAnonymous 9QBCcNNo ratings yet
- Nursing Analysis, Goals, Interventions, and Evaluations for Acute Pain and Risks of Imbalanced Nutrition and Fluid Volume DeficitDocument5 pagesNursing Analysis, Goals, Interventions, and Evaluations for Acute Pain and Risks of Imbalanced Nutrition and Fluid Volume DeficitAngelica ValeraNo ratings yet
- Nursing Care Plan for Acute Gastritis, Adrenal Crisis and COPDDocument6 pagesNursing Care Plan for Acute Gastritis, Adrenal Crisis and COPDCharlene Grace ReginoNo ratings yet
- NCP & Drug Study for Post-Op PainDocument22 pagesNCP & Drug Study for Post-Op PainTheo Roi MusniNo ratings yet
- Nursing Care Plan: Assessment Nursing Diagnosis Planning Nursing Interventi ON Rationale EvaluationDocument2 pagesNursing Care Plan: Assessment Nursing Diagnosis Planning Nursing Interventi ON Rationale EvaluationRaidis PangilinanNo ratings yet
- NCP Acute Pain CholeDocument2 pagesNCP Acute Pain CholeMary Kaye SilvestreNo ratings yet
- Managing Labor Pain Through Non-Pharmacological MethodsDocument4 pagesManaging Labor Pain Through Non-Pharmacological MethodsFran LanNo ratings yet
- NCP - Baby Final PDFDocument11 pagesNCP - Baby Final PDFCindy MariscotesNo ratings yet
- Assessment Nursing Diagnosis Goals and Objective Nursing Interventions Rationale Evaluation SubjectiveDocument2 pagesAssessment Nursing Diagnosis Goals and Objective Nursing Interventions Rationale Evaluation SubjectiveDanica Kate GalleonNo ratings yet
- UntitledDocument5 pagesUntitledJayelles Dixien JuguilonNo ratings yet
- 'Urdaneta City University College of Health Sciences: Bachelor of Science in NursingDocument4 pages'Urdaneta City University College of Health Sciences: Bachelor of Science in NursingDan Dan ManaoisNo ratings yet
- Holistic Approach to Relieve Neck Pain, Back, and Shoulder Pain: An Effective Method for Pain ReductionFrom EverandHolistic Approach to Relieve Neck Pain, Back, and Shoulder Pain: An Effective Method for Pain ReductionRating: 3 out of 5 stars3/5 (1)
- Holistic Home Remedies for Acute Low Back Pain: Incorporating Stretching and the McKenzie MethodFrom EverandHolistic Home Remedies for Acute Low Back Pain: Incorporating Stretching and the McKenzie MethodNo ratings yet
- A.) 62 Yo Male, S/P (Status Post) Exploratory Laparotomy Secondary Intestinal ObstructionDocument4 pagesA.) 62 Yo Male, S/P (Status Post) Exploratory Laparotomy Secondary Intestinal ObstructionKate Aenyle AgsoyNo ratings yet
- Journal & ReflectionDocument4 pagesJournal & ReflectionKate Aenyle AgsoyNo ratings yet
- Nursing care plan for patient with acute pancreatic painDocument2 pagesNursing care plan for patient with acute pancreatic painKate Aenyle AgsoyNo ratings yet
- Nursing care plan for acute confusionDocument2 pagesNursing care plan for acute confusionKate Aenyle AgsoyNo ratings yet
- Nursing care plan for patient with acute pancreatic painDocument2 pagesNursing care plan for patient with acute pancreatic painKate Aenyle AgsoyNo ratings yet
- Nursing care plan for acute confusionDocument2 pagesNursing care plan for acute confusionKate Aenyle AgsoyNo ratings yet
- Triamcinolone acetonide injectable suspension for intramuscular or intra-articular useDocument7 pagesTriamcinolone acetonide injectable suspension for intramuscular or intra-articular useziddin_ahmadNo ratings yet
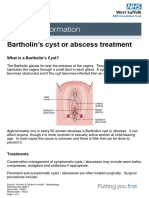
- Bartholin's Cyst or Abscess TreatmentDocument4 pagesBartholin's Cyst or Abscess TreatmentRezaFArthaNo ratings yet
- COVID-19 Current State Analysis and Forecasting For The DFW RegionDocument14 pagesCOVID-19 Current State Analysis and Forecasting For The DFW RegionSourav SutradharNo ratings yet
- Allocation of Health Care ResourceDocument2 pagesAllocation of Health Care ResourceSha Btsta100% (1)
- Psoriatic Arthritis Nature ReviewDocument17 pagesPsoriatic Arthritis Nature ReviewJose Shaid Delgado OlveraNo ratings yet
- Brain AbscessDocument2 pagesBrain AbscessIan RomanNo ratings yet
- Quiz (4 Mei - 7 Mei)Document3 pagesQuiz (4 Mei - 7 Mei)NdyNo ratings yet
- European Journal of Obstetrics & Gynecology and Reproductive BiologyDocument5 pagesEuropean Journal of Obstetrics & Gynecology and Reproductive BiologyMariana González DíazNo ratings yet
- Chronic and Acute GoutDocument20 pagesChronic and Acute GoutDan TranNo ratings yet
- Research PaperDocument8 pagesResearch Paperapi-449021066No ratings yet
- Mental HealthDocument5 pagesMental HealthSofia Cinderella QuimoNo ratings yet
- Infection Control and Related Health and Safety in The Dental OfficeDocument48 pagesInfection Control and Related Health and Safety in The Dental OfficeKim Lien TrinhNo ratings yet
- Beyond Wet To DryDocument45 pagesBeyond Wet To DryGabriel Urrea BoteroNo ratings yet
- Organizational-Skills PIDENDocument6 pagesOrganizational-Skills PIDENczarinaNo ratings yet
- Open Letter To Mayor-Elect Wu - Mass and CassDocument2 pagesOpen Letter To Mayor-Elect Wu - Mass and Cassdialynn dwyerNo ratings yet
- Polymyalgia Rheumatica Diagnosis and TreatmentDocument7 pagesPolymyalgia Rheumatica Diagnosis and Treatmenttika tikaNo ratings yet
- DownloadfilesDocument26 pagesDownloadfilesDowntoearthNo ratings yet
- Dental NotationDocument4 pagesDental NotationHemanth KumarNo ratings yet
- Portfolio Cover LetterDocument1 pagePortfolio Cover Letterapi-322795813No ratings yet
- Food Deterioration and Its CausesDocument10 pagesFood Deterioration and Its CausesM ZAHID SADIQNo ratings yet
- Manufacturer of Medical Devices and Medical Instrument.Document1 pageManufacturer of Medical Devices and Medical Instrument.Angiplast Private LimitedNo ratings yet
- CE Childhood-ObesityDocument3 pagesCE Childhood-ObesityPaola BertelloNo ratings yet
- Infectious Diseases Lecture on Fever PathophysiologyDocument2 pagesInfectious Diseases Lecture on Fever PathophysiologyNonoy JoyaNo ratings yet
- Data Ruangan Intensive (071020)Document31 pagesData Ruangan Intensive (071020)Andrew WarankiranNo ratings yet
- NursDocument4 pagesNursapi-323159742No ratings yet
- COPD Significantly Increases Cerebral and Cardiovascular Events in HypertensivesDocument8 pagesCOPD Significantly Increases Cerebral and Cardiovascular Events in HypertensivesAndreea MoalesNo ratings yet
- Speech Recognition in Noise Test (Sprint) For H-3 ProfileDocument8 pagesSpeech Recognition in Noise Test (Sprint) For H-3 ProfileshivfifaNo ratings yet