Professional Documents
Culture Documents
Allergy: B Cells (B Lymphocytes)
Uploaded by
Xarius Fidel0 ratings0% found this document useful (0 votes)
9 views4 pagesOriginal Title
Allergy
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
9 views4 pagesAllergy: B Cells (B Lymphocytes)
Uploaded by
Xarius FidelCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 4
ALLERGY
An allergic reaction is a manifestation of tissue injury B cells (B lymphocytes)
resulting from interaction between an antigen and an
• are programmed to produce one specific
antibody. Allergy is an inappropriate and often
antibody.
harmful response of the immune system to normally
• on encountering a specific antigen, B cells
harmless substances, called allergens.
stimulate production of plasma cells, the site
Ex. of allergens: of antibody production. The result is the
outpouring of antibodies for the purpose of
a. Dust destroying and removing the antigens.
b. Pollen
• part of adaptive immunity.
c. Weeds
d. Dander
In the process of an allergic reaction, there will be a T cells (T lymphocytes)
release of chemical mediators that will produce a
range of symptoms ranging from mild to life • assist the B cells.
threatening. • secrete substances that direct the flow of
cell activity, destroy target cells, and
In allergic reactions, the body encounters allergens stimulate the macrophages.
that are types of antigens, usually proteins that the • digest antigens and assist in removing
body’s defenses recognize as foreign, and a series of cells and other debris.
events occur in an attempt to render the invaders • does not bind to free antigens.
harmless, destroy them, and remove them from the
body. Antigens
• acts as the trigger of immune response
• divided into 2 groups:
Role of Immunoglobulins
1. Complete Protein Antigens
Immunoglobulins - antibodies that are formed by
➢ Refers to animal dander, pollen,
lymphocytes and plasma cells in response to an
and horse serum.
immunogenic stimulus constitute a group of serum
➢ Stimulate a complete humoral
proteins.
response.
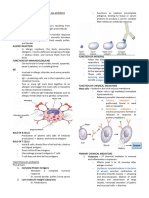
Immunoglobulins of the IgE class
• involved in allergic disorders and some 2. Low Molecular Weight Substances
parasitic infections. IgE-producing cells are ➢ such as medications, function as
located in the respiratory and intestinal haptens (incomplete antigens),
mucosa. binding to tissue or serum
• two or more IgE molecules bind together to proteins to produce a carrier
an allergen and trigger mass cells (basophil). complex that initiates an antibody
When they trigger basophil, it then releases response.
chemical mediators such as histamine, ➢ Haptens – molecules that are
serotonin, kinins, slow reacting substances of incapable alone of causing the
anaphylaxis and neutrophil factor thereby production of antibodies, but it
producing an allergic reaction. can do so when it is fastened to a
larger antigenic molecule called a
Atopy – refers to IgE mediated diseases, such as carrier.
allergic rhinitis, that have a genetic component.
Mast Cell Primary Mediators
• responsible for producing chemical mediators. 1. Histamine
➢ Vasodilation, smooth muscle
• Located in the skin and mucous membranes,
contraction, increased vascular
play a major role in IgE-mediated immediate
permeability, increased secretions.
hypersensitivity.
• When mast cells are stimulated by antigens,
2. Platelet-Activating Factor
powerful chemical mediators are release,
➢ Initiates platelet aggregation and
causing a sequence of physiologic events that
leukocyte infiltration at sites of
result in symptoms of immediate
immediate hypersensitivity reactions.
hypersensitivity.
➢ Causes vasodilation,
bronchoconstriction, and increased
vascular permeability.
Chemical Mediators produced by mast cell
3. Eosinophil Chemotactic Factor of Anaphylaxis
Histamine
➢ Attracts eosinophils
• Histamine action results from stimulation of
histamine-1 (H1) and histamine-2 (H2)
4. Prostaglandins
receptors.
➢ Produce smooth muscle contraction
➢ H1 receptors – found predominantly
as well as vasodilation and increased
on bronchiolar and vascular smooth
capability permeability. They sensitize
muscle cells.
pain receptors and increase the pain
➢ H2 receptors – found on gastric
associated with inflammation.
parietal cells.
➢ Methanolic acid – a drug that act on
• Histamine’s effects peak 5-10 minutes after
the prostaglandins and for the pain.
antigen contact and include the following:
➢ Erythema and itchyness
➢ Localized edema in the form of
Secondary Mediators
wheals
1. Leukotrienes
➢ Pruritis
➢ Initiate the inflammatory response.
➢ Contraction of bronchial smooth
➢ Responsible for smooth muscle
muscle, resulting in wheezing and
contraction, bronchial constriction,
bronchospasm
mucus secretion in the airways, and
➢ Dilation of small venules and
the typical wheal-and-flare reactions
constriction of larger vessels
of the skin.
➢ Increased secretion of gastric and
➢ 100-1,000 times more potent in
mucosal cells resulting in diarrhea.
causing bronchospasm compare to
histamine.
Diphenhydramine
• Antihistamine drug that targets histamine 2. Bradykinin
receptors. ➢ cause increased permeability,
• Medication that displays an affinity for H1 vasodilation, hypotension, and
receptors. contraction of many types of smooth
muscle, such as the bronchi.
Cimetidine and Ranitidine ➢ Increased permeability of the
• Target H2 receptor to inhibit gastric secretion capillaries results in edema.
in peptic ulcer disease.
➢ Stimulates nerve cell fibers and d. The second time that person has a
produces pain. brush with ragweed, the allergen
crosslinks the surface bound IgE and
3. Heparin – anticoagulant activated signal from the cytoplasmic
portion of Ige
4. Serotonin – acts as a potent vasoconstrictor e. The IgE primed mast cells then release
and causes contraction of bronchial smooth granules and powerful chemical
muscle. mediators, such as histamine and
cytokines, into the environment.
f. These chemical mediators cause the
HYPERSENSITIVITY characteristics symptoms of allergy.
➢ An excessive aberrant immune response to
any type of stimulus (Abbas et al., 2014). It
usually does not occur with the first exposure
to an allergen. Rather, the reaction follows a Clinical Manifestations of Anaphylaxis
re-exposure after sensitization, or buildup of ➢ Swelling of the conjunctiva
antibodies, in a predisposed person. ➢ Runny rose
Types of Hypersensitivity Reactions ➢ Swelling of lips, tongue and/or throat
➢ CNS: lightheadedness, loss of consciousness,
1. Anaphylactic (Type 1) Hypersensitivity confusion, headache, anxiety
➢ IgE-mediated ➢ Respi: shortness of breath, wheezes or
➢ Onset is within 1 hour stridor, hoarseness, pain with swallowing,
➢ The most severe hypersensitivity reaction cough
is anaphylaxis ➢ GI: crampy abdominal pain, diarrhea,
➢ Standard treatment for anaphylaxis is vomiting, loss of bladder control, pelvic pain
epinephrine ➢ Heart and vasculature: fast or slow heart rate
➢ Unanticipated severe allergic reaction and low blood pressure
that is rapid in onset. ➢ Skin: hives, itchiness, flushing
➢ Anaphylaxis is characterized by edema in
many tissues, including the larynx, and
often accompanied by hypotension, 2.Cytotoxic (Type 2) Hypersensitivity
bronchospasm, and cardiovascular ➢ IgM or IgG cytotoxic
collapse in severe cases. ➢ Onset: hours to days
➢ An immediate reaction beginning within ➢ Ex. hemolytic anemia
minutes of exposure to an antigen. ➢ Occurs when the system mistakenly identifies
➢ Primary chemical mediators are a normal constituent of the body as foreign.
responsible for the symptoms of type 1 This reaction may be the result of a cross
hypersensitivity because of their effects reacting antibody, possibly leading to cell and
on the skin, lungs, and gastrointestinal tissue damage.
tract. ➢ Example is blood transfusion reaction:
➢ Happens during the second time. a. Donate type A blood with type A
➢ Pathophysiology: antigens enters bloodstream of type B
a. First time an allergy prone person recipient
runs across an allergen such as b. Anti-A antibodies in plasma if type B
ragweed recipient bind to donated type AA red
b. He/she makes large amounts of blood cells
ragweed IgE antibody c. Bound anti-A antibodies activate
c. Then, the IgE molecules attach complement cascade, causing
themselves to mast cells hemolysis and release of hemoglobin.
3. Immune Complex (Type 3) Hypersensitivity ➢ This type of reaction to the subcutaneous
➢ Immune complex-mediated injection of antigen is often used as an assay
➢ Onset: 1-3 weeks for cell-mediated immunity (e.g., the purified
➢ Involves immune complexes that are formed protein derivative skin test or immunity to
when antigens bind to antibodies. Mycobacterium tuberculosis)
➢ Cleared from the circulation by phagocytic ➢ Ex. kidney transplant
action.
➢ If these type 3 complexes are deposited in
Diagnostic Findings
tissues or vascular endothelium, two factors
contribute to injury: 1. Complete Blood Count with differential
a. The increased amount of circulating • Eosinophil level greater than 5% to
complexes 10% is considered abnormal and may
b. The presence of vasoactive amines be found in patients with allergic
➢ As a result, there is an increase in vascular disorders.
permeability and tissue injury.
➢ Happens in patient with systemic lupus 2. Eosinophil Count
erythematosus (SLE)
• Smears obtained from nasal
➢ Pathophysiology:
secretions and sputum of patients
a. Antigen and B cell activated
with allergic usually reveal an increase
b. Stimulates plasma cell and produce
in eosinophils, indicating an active
antibodies
allergic response.
c. Antibodies bind with antigen forming
immune complex
3. Total Serum Immunoglobulin E levels
d. Excess immune complex
• High total serum IgE levels support
e. Complexes get deposited in certain target
the diagnosis of allergic disease.
tissues on which circulation is low or
filtration of blood occurs like kidney and
4. Skin Tests
synovial membrane of joints
• Considered to be the most accurate
f. Activate a complement cascade which
confirmation of an allergy.
results in the formation of vaso-active
amines.
5. Provocative Test
g. Complement cascade generates
• Involves the direct administration of
fragments which are chemotactic to
the suspected allergen to the
neutrophils (neutrophil activation)]
sensitive tissue such as conjunctive,
h. Process of phagocytosis, there is a release
nasal, bronchial mucosa or GI tract
of degradative enzymes (lysosmal)
• Helpful in identifying clinically
i. Amines altered the permeability of the
significant allergens in patients who
affected tissue thereby causing tissue
have a large number of positive tests
damage
6. Serum-specific IgE Test
• Automated test performed on blood
4. Delayed-Type (Type 4) Hypersensitivity sample
➢ T cell-mediated • Detects free-antigen-specific IgE in
➢ Onset: days to weeks serum as opposed to antigen-specific
➢ Ex. Rash Stevens-Johnson syndrome (SJS) IgE bound to mast cells in the skin
➢ Immune reaction in which T-cell dependent • Includes decreased risk of systemic
macrophage activation and inflammation reaction, stability of antigen, and lack
cause tissue injury. of dependence and skin reactivity
modified by medications
You might also like
- Pervez Akbar - Basis of PediatricsDocument649 pagesPervez Akbar - Basis of PediatricsIshfaq Samtia100% (4)
- CPNRE Studying Checklist (2hr)Document35 pagesCPNRE Studying Checklist (2hr)B89% (9)
- Appy DictationDocument2 pagesAppy Dictationsgod34100% (1)
- Management of Patients On Systemic Steroids - An Oral Surgery PerspectiveDocument7 pagesManagement of Patients On Systemic Steroids - An Oral Surgery PerspectiveMohammad Abdulmon’emNo ratings yet
- Allergic DisordersDocument20 pagesAllergic DisorderskiyoorexenNo ratings yet
- Topic 11 - Hypersensitivity and Autoimmuninty ProblemsDocument7 pagesTopic 11 - Hypersensitivity and Autoimmuninty ProblemsMatt Andrei P. SongcuanNo ratings yet
- Hypersensitivity ReactionsDocument12 pagesHypersensitivity Reactionsella Sy100% (1)
- Allergen Sensitization: Primary MediatorsDocument14 pagesAllergen Sensitization: Primary Mediatorsjelly bean100% (1)
- Assessment and Management of Pt's W/ Allergic Disorders: Physiologic OverviewDocument11 pagesAssessment and Management of Pt's W/ Allergic Disorders: Physiologic OverviewChristina RichardsNo ratings yet
- 13-Hypersensitivities Type I With Audio 2021Document24 pages13-Hypersensitivities Type I With Audio 2021Rami AlhilliNo ratings yet
- MODULE 3 PharmaDocument13 pagesMODULE 3 Pharmadelie joy dacdacNo ratings yet
- Complete Protein Antigens and Low - Molecular-Weight Substances - Complete Protein Antigens, Such As AnimalDocument1 pageComplete Protein Antigens and Low - Molecular-Weight Substances - Complete Protein Antigens, Such As AnimalApple BananaNo ratings yet
- Hypersensitivity-1 Very ImportantDocument114 pagesHypersensitivity-1 Very ImportantNusrat JahanNo ratings yet
- 1.11 Hypersensitivity (Dr. Dacula)Document5 pages1.11 Hypersensitivity (Dr. Dacula)John Benedict BondocNo ratings yet
- Imunați-Mă ChanismeDocument3 pagesImunați-Mă ChanismeAurelia AlexandraNo ratings yet
- PharmaDocument13 pagesPharmaMARIEMIL FOLLOSONo ratings yet
- TaxolDocument83 pagesTaxolCrazy Chase and CamNo ratings yet
- AnaphylaxisDocument4 pagesAnaphylaxisyaminduhairNo ratings yet
- STUDY GUIDE 2 (Operaña, Ellayza)Document4 pagesSTUDY GUIDE 2 (Operaña, Ellayza)OPERAñA ELLAYZA RB DECANONo ratings yet
- NOTES DAY 59 Human Health & Disease L15 2022Document5 pagesNOTES DAY 59 Human Health & Disease L15 2022Neha SharmaNo ratings yet
- Unit 3Document46 pagesUnit 3tanmai nooluNo ratings yet
- Pharma Reviewer MidtermDocument21 pagesPharma Reviewer Midtermjana whiteNo ratings yet
- Week 4 - Drugs Acting On The Immune SystemDocument16 pagesWeek 4 - Drugs Acting On The Immune SystemDino MicaNo ratings yet
- Hypersensitivity Reactions PDFDocument3 pagesHypersensitivity Reactions PDFRonald BeasleyNo ratings yet
- Immunopharmacology: Yung Nagfoformulate NG Antibodies)Document5 pagesImmunopharmacology: Yung Nagfoformulate NG Antibodies)Lloyd LinNo ratings yet
- Lymphatic SysDocument19 pagesLymphatic SyschennielafleurNo ratings yet
- The Allergic Response: Kathleen Nicole B. Bidua First Year ResidentDocument44 pagesThe Allergic Response: Kathleen Nicole B. Bidua First Year ResidentNicole BiduaNo ratings yet
- 1 Hypersensitivity Reaction - Juli 2021Document39 pages1 Hypersensitivity Reaction - Juli 2021Arianti Miranti Lestari FajrinNo ratings yet
- Lecture - Week 3 (Natural Immunity & Complement System)Document5 pagesLecture - Week 3 (Natural Immunity & Complement System)rennel ybarolaNo ratings yet
- FinaDocument19 pagesFinaZabdiel Ann SavellanoNo ratings yet
- Chapter 11 Undisarable and Alterd ImmunotyDocument81 pagesChapter 11 Undisarable and Alterd ImmunotyTofikNo ratings yet
- Immunology & Serology Section Chapter 1: Immunology: Initial Immune ResponseDocument43 pagesImmunology & Serology Section Chapter 1: Immunology: Initial Immune ResponseCharmaine Dela CruzNo ratings yet
- Medical Veterinary Programe UB: Dr. Sri Murwani, DRH, MPDocument46 pagesMedical Veterinary Programe UB: Dr. Sri Murwani, DRH, MPrifqi rahmanNo ratings yet
- Inflammation 2Document21 pagesInflammation 2Umar'Farouq OniNo ratings yet
- Hypersensitivity 150525050534 Lva1 App6892 PDFDocument117 pagesHypersensitivity 150525050534 Lva1 App6892 PDFPriya Dharshini PalanimuthuNo ratings yet
- Hypersensitivity: Mark Christian D. Duatin, RMTDocument43 pagesHypersensitivity: Mark Christian D. Duatin, RMTJoyce Anne Faith Estrella100% (1)
- Immune SystemDocument24 pagesImmune SystemSteffanie TalaueNo ratings yet
- Nursing Care of A Child With Immune DisordersDocument4 pagesNursing Care of A Child With Immune DisordersChin T. OndongNo ratings yet
- HISTOLOGY-NOTES-by-Red ImmuneDocument4 pagesHISTOLOGY-NOTES-by-Red ImmuneEdzeal Bruan JrNo ratings yet
- Concept of Inflammatory and Immune SystemDocument15 pagesConcept of Inflammatory and Immune SystemUchiha Dominic100% (1)
- Immunology in Health and DiseasesDocument7 pagesImmunology in Health and DiseasesLianneRaoNo ratings yet
- Nursing Care of Clients With Allergic DisordersDocument12 pagesNursing Care of Clients With Allergic Disordersbwee bweeNo ratings yet
- 12.hypersensitivity 2013Document58 pages12.hypersensitivity 2013lookmoo100% (1)
- Inflmmation and ImmunityDocument19 pagesInflmmation and ImmunityShawn TejanoNo ratings yet
- HypersensitivityDocument9 pagesHypersensitivityJirah RuedasNo ratings yet
- Mechanism of Type I Hypersensitivity: Important MediatorDocument4 pagesMechanism of Type I Hypersensitivity: Important MediatorSifat DewanNo ratings yet
- ImmunologyDocument9 pagesImmunologyRamadhan Dwi AnggoroNo ratings yet
- 6.3 Innate ImmunityDocument1 page6.3 Innate ImmunityjanNo ratings yet
- Mediators of Inflammation and The Inflammatory Process: Martha White, MD Washington, D.CDocument4 pagesMediators of Inflammation and The Inflammatory Process: Martha White, MD Washington, D.CBlackHAT GAMINGNo ratings yet
- The Role of Inflammation in The Healing Process - ABUTTDocument10 pagesThe Role of Inflammation in The Healing Process - ABUTTMayra GarciaNo ratings yet
- HypersensitivityDocument43 pagesHypersensitivityMazhar RehmanNo ratings yet
- Physiology Presentation Ch. 6, 7 & 14 Aleta Anderton University of Phoenix Online HCA 220 Medical Language Instructor: Rebecca Hopwood May 15, 2011Document14 pagesPhysiology Presentation Ch. 6, 7 & 14 Aleta Anderton University of Phoenix Online HCA 220 Medical Language Instructor: Rebecca Hopwood May 15, 2011aleta-nicholsonNo ratings yet
- BLOOD LECTURE 4 2017 Immunity 1Document38 pagesBLOOD LECTURE 4 2017 Immunity 1Philip Abayomi VincentNo ratings yet
- Micro20 Chapter 19 (Notes)Document10 pagesMicro20 Chapter 19 (Notes)Princess BalanonNo ratings yet
- Function of LeukicytesDocument9 pagesFunction of Leukicytesdeput_rprNo ratings yet
- Lecture 21 - HypersensitivityDocument25 pagesLecture 21 - Hypersensitivityapi-3703352100% (2)
- Immune System My NotesDocument12 pagesImmune System My NotesSelin AtalayNo ratings yet
- Finals Lesson 3Document6 pagesFinals Lesson 3Kevin Vincent AquinoNo ratings yet
- University of Santo Tomas: Faculty of Pharmacy - Department of Medical TechnologyDocument7 pagesUniversity of Santo Tomas: Faculty of Pharmacy - Department of Medical TechnologyWynlor AbarcaNo ratings yet
- Concepts in Immunologic Function: Chapter 35: Assessment of Immune FunctionDocument9 pagesConcepts in Immunologic Function: Chapter 35: Assessment of Immune FunctionKristine KimNo ratings yet
- Anti Allergic Drugs: Abdullaev Dzhumadil, PharmdDocument21 pagesAnti Allergic Drugs: Abdullaev Dzhumadil, PharmdRtxGaming Zone 73No ratings yet
- 2 Allergic DiseasesDocument27 pages2 Allergic DiseasesMuhammad AgussalimNo ratings yet
- Immunology AND Inflammatory: Mr. Bernie Pedrigal Malabanan, RN Lecture SeriesDocument64 pagesImmunology AND Inflammatory: Mr. Bernie Pedrigal Malabanan, RN Lecture SeriesPrincess Naome Calma CantilloNo ratings yet
- Untitled ARCHDocument4 pagesUntitled ARCHJessray RepunteNo ratings yet
- GEO195 Practice 3Document4 pagesGEO195 Practice 3Jhervin GutierrezNo ratings yet
- 66Document1 page66Xarius FidelNo ratings yet
- BIO191 Diagram 5Document4 pagesBIO191 Diagram 5Xarius FidelNo ratings yet
- BIO191 Lec Notes 1Document4 pagesBIO191 Lec Notes 1Xarius FidelNo ratings yet
- FASH257 Topic 2Document4 pagesFASH257 Topic 2Cj DatoyNo ratings yet
- FIN303 Research 10Document4 pagesFIN303 Research 10Ksks KsksNo ratings yet
- ACC197 Presentation 9Document4 pagesACC197 Presentation 9Dini Aulia PutryNo ratings yet
- 11Document3 pages11Xarius FidelNo ratings yet
- 61Document1 page61Xarius FidelNo ratings yet
- 65Document1 page65Xarius FidelNo ratings yet
- 70Document1 page70Xarius FidelNo ratings yet
- 62Document1 page62Xarius FidelNo ratings yet
- 1Document1 page1Xarius FidelNo ratings yet
- New Essay!Document1 pageNew Essay!Xarius FidelNo ratings yet
- 68Document1 page68Xarius FidelNo ratings yet
- 11Document1 page11Xarius FidelNo ratings yet
- 13Document2 pages13Xarius FidelNo ratings yet
- 3Document2 pages3Xarius FidelNo ratings yet
- 12Document2 pages12Xarius FidelNo ratings yet
- New Essay!Document1 pageNew Essay!Xarius FidelNo ratings yet
- 14Document1 page14Xarius FidelNo ratings yet
- New Essay!Document2 pagesNew Essay!Xarius FidelNo ratings yet
- 4Document2 pages4Xarius FidelNo ratings yet
- 7Document2 pages7Xarius FidelNo ratings yet
- 1Document2 pages1Xarius FidelNo ratings yet
- 8Document2 pages8Xarius FidelNo ratings yet
- 2Document2 pages2Xarius FidelNo ratings yet
- New Essay!Document2 pagesNew Essay!Xarius FidelNo ratings yet
- 9Document2 pages9Xarius FidelNo ratings yet
- The Stages of Prevention - Primer On Public Health PopulationDocument2 pagesThe Stages of Prevention - Primer On Public Health PopulationBSN 201450% (2)
- Acute Renal FailureDocument13 pagesAcute Renal FailureGlorianne Palor100% (2)
- Nle FC Manila 2023 May - EDITEDDocument12 pagesNle FC Manila 2023 May - EDITEDAngela NeriNo ratings yet
- ImmunizationDocument2 pagesImmunizationannamcconkeyNo ratings yet
- Metabolic and Endocrine 2010 2 With AnswersDocument13 pagesMetabolic and Endocrine 2010 2 With AnswersWenzy Razzie cruzNo ratings yet
- Anatomy Endocrine Q and ADocument16 pagesAnatomy Endocrine Q and ASamantha Frey LopezNo ratings yet
- Psychiatric Aspects of Liver DiseaseDocument8 pagesPsychiatric Aspects of Liver DiseaseBrian AsayasNo ratings yet
- Conversion Disorder: Etiology/ Causal FactorsDocument4 pagesConversion Disorder: Etiology/ Causal FactorsSrishti GaurNo ratings yet
- Cirrhosis in Adults - Etiologies, Clinical Manifestations, and Diagnosis - UpToDate PDFDocument33 pagesCirrhosis in Adults - Etiologies, Clinical Manifestations, and Diagnosis - UpToDate PDFDonto KonoNo ratings yet
- Physiotherapy in Parkinsons DiseaseDocument21 pagesPhysiotherapy in Parkinsons DiseaseeimearNo ratings yet
- The Science of NutritionalDocument738 pagesThe Science of NutritionalMonching Adecer100% (1)
- Liver PathologyDocument16 pagesLiver PathologyMuhammad Salman100% (1)
- KG Cystic Fibrosis Case Study Alvarez 1Document7 pagesKG Cystic Fibrosis Case Study Alvarez 1api-309995064No ratings yet
- Minor Disorders in PregnancyDocument35 pagesMinor Disorders in PregnancyRaniNo ratings yet
- Rehab Medik - Dr. Joudy Gessal, SPRM - Modul Penurunan KesadaranDocument17 pagesRehab Medik - Dr. Joudy Gessal, SPRM - Modul Penurunan KesadaranRian Candra IbrahimNo ratings yet
- Chronic Diarrhea in ChildrenDocument4 pagesChronic Diarrhea in ChildrenDaffa Ahmad NaufalNo ratings yet
- Goldenhar Syndrome An Unusual Case ReportDocument4 pagesGoldenhar Syndrome An Unusual Case ReportInternational Journal of Innovative Science and Research TechnologyNo ratings yet
- Anger Management JournalDocument1 pageAnger Management JournalRidwan SyafiudinNo ratings yet
- Nmm2017 Infographic BookDocument36 pagesNmm2017 Infographic BooksandhiyaNo ratings yet
- Abnoramal ECGDocument20 pagesAbnoramal ECGImmanuelNo ratings yet
- Glossary of TermesDocument4 pagesGlossary of TermesLa Vie JesusGodNo ratings yet
- Food Standards Agency Guidance On The Safety and Shelf-Life of Vacuum and Modified Atmosphere Packed Chilled Foods With Respect To Non-ProteolyticDocument22 pagesFood Standards Agency Guidance On The Safety and Shelf-Life of Vacuum and Modified Atmosphere Packed Chilled Foods With Respect To Non-ProteolyticAsiwome Charcha Kodjo TsamenyiNo ratings yet
- USMLE High YieldDocument13 pagesUSMLE High YieldShirkeIncNo ratings yet
- Pelvic Trauma Final 210409Document8 pagesPelvic Trauma Final 210409Dwi ApriliziaNo ratings yet
- Research Menopause DepressionDocument5 pagesResearch Menopause DepressionVinitha JobyNo ratings yet
- UntitledDocument340 pagesUntitledAlistair KohNo ratings yet