Professional Documents
Culture Documents
Cleft, Hirschsprung, Imperforate Anus
Uploaded by
Myraflor Caro0 ratings0% found this document useful (0 votes)
15 views3 pagesOriginal Title
Cleft, Hirschsprung, Imperforate anus
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
15 views3 pagesCleft, Hirschsprung, Imperforate Anus
Uploaded by
Myraflor CaroCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 3
Cleft Lip or Cleft Palate • In bilateral cleft lip, the midportion of the
upper lip is attached on both sides and may
➢ A commonly occurring congenital midline
be displaced forward.
fissure, or opening, in the lip or palate
• Dental anomalies (e.g., missing,
resulting from failure of the primary palate to
mispositioned, or deformed teeth) are
fuse
common.
➢ Results from failure of the maxillary and
premaxillary processes to fuse during the 5th Cleft Palate
to 8th week of intrauterine life
➢ Occurs when the primary and the secondary
Causes: palatine plates fail to fuse during the
embryonic development
1. Genetic and environmental factors
➢ May involve only the soft palate or may
2. Family history (strongest risk factor)
extend into the hard palate
3. Maternal smoking, consumption of large
➢ May occur only in the midline of the posterior
amounts of alcohol, medications taken during
palate or may extend to the nostril on one or
the first trimester, and maternal DM (not
both sides
gestational diabetes)
Complications:
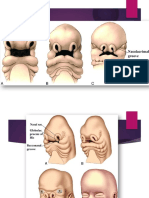
Development (intrauterine)
1. Difficulty feeding. While most babies with
1. During the 4th week of development, a series
cleft lip can breastfeed, a cleft palate may
of six paired (right and left) swellings form
make sucking difficult.
near the cranial end of the fetus. These are
2. Dental problems. If the cleft extends to the
called brachial arches.
upper gum, tooth development may be
2. The first brachial arche develop structures
affected.
called the maxillary and the mandibular
3. Speech difficulties. Because the palate is
prominences.
used in forming sounds, the development of
3. In the center of the upper face, there is a
normal speech can be affected by cleft palate.
structure called the frontonasal prominence.
Speech may sound too nasal.
Cleft Lip 4. Challenges of coping with a medical
condition. Children with clefts may face
➢ Results from embryonic fusion of the
social, emotional, and behavioral problems
embryonic structures surrounding the
due to differences in appearance and the
primitive oral cavity
stress of intensive medical care.
➢ May be unilateral or bilateral
➢ Associated with abnormal development of Nursing Interventions:
the external nose, nasal cartilages, nasal
1. Maintain adequate nutrition.
septum, and maxillary alveolar ridges
A soft nipple with a cross-cut made to
Note: promote easy flow of milk may work well.
Positioning
• The extent of the cleft varies, from an
The infant should be kept in an upright
indentation in the lip to a deep and wide
position during feeding.
fissure extending to the nostril
Tools for feeding.
• In severe clefts, the nostril on the affected Lamb’s nipples (extra long nipples) and
side is low and,the nose is deviated to that special cleft palate nipples molded to fit into
side the open palate area to close the gap may be
used.
One of the most effective methods may be the Absence/ delayed passage of meconium. During
use of an eyedropper or an asepto syringe the newborn period, infants affected with HD may
with a short piece of rubber tubing on the tip present failure of passage of meconium.
(Breck feeder).
Vomiting. Repeated vomiting is present due to
2. Promote family coping
intestinal obstruction.
3. Reduce family anxiety
4. Provide family teaching Malnourishment. Poor nutrition results from the
early satiety, abdominal discomfort, and distention
Hirschsprung’s Disease
associated with chronic constipation.
(Congenital Aganglionic Megacolon)
Fever and explosive diarrhea indicate enterocolitis,
• Characterized by persistent constipation a life-threatening condition.
resulting from partial or complete intestinal
Diagnostic Findings
obstruction of mechanical origin.
• Normally, when a stool enters the rectum, the 1. Laboratory studies (CBC). Order test if
internal sphincter relaxes and the stools are enterocolitis is suspected. Elevation of WBC
evacuated. In HD, the internal sphincter does count should raise concern for enterocolitis.
not relax. 2. Plain abdominal radiography. Perform this
test with any signs and symptoms of
Pathophysiology
abdominal obstruction.
• Results from the absence of enteric neurons 3. Unprepared single-contrast barium
within the mysenteric and submucosal plexus enema. If perforation and enterocolitis is not
of the rectum and/or colon. suspected, this may help to establish the
• Enteric neurons are derived from the neural diagnosis by identifying a transition zone
crest and migrate caudally with the vagal between a narrowed aganglionic segment and
nerve fibers along the intestine a dilated and normally innervated segment.
• These ganglion cells arrive in the proximal The study may also reveal a non-distensible
colon by 8 weeks gestation and in the rectum rectum, which is a classic sign of HD.
by 12 weeks gestation. 4. Rectal biopsy. Diagnosis is confirmed
• Arrest in migration leads to an aganglionic through rectal biopsy. It is a procedure used
segment. to extract a tissue sample from the rectum for
a laboratory analysis. The rectum is the
Clinical Manifestation lowest 6 inches of the large intestine located
just above the anal canal. The rectum’s
Abdominal distention. Infants with aganglionic
purpose is to store the body’s solid waste
megacolon show tympanic abdominal distention and
until it is released.
symptoms of intestinal obstruction.
Medical Management
Chronic constipation. Older infants and children
with HD usually present with chronic constipation. Initial therapy. If a child with Hirschsprung’s
disease has s/sx of a high grade intestinal obstruction,
Palpable intestinal loop. Upon abdominal
initial therapy should include intravenous hydration,
examination, these children may demonstrate
withholding of enteral intake, and intestinal and
marked abdominal distention with palpable dilated
gastric decompression.
loops of colon.
Decompression. Decompression can be
accomplished through placement of a nasogastric
tube and either digital rectal examination or normal hours, and immediately report any unusual drainage
saline rectal irrigations 3-4 times daily. such as bright-red bleeding.
Diet. A special diet is not required. However, Imperforate Anus
preoperative and in the early post-operative period,
Clinical Manifestations
infants of a non-constipated regimen, such as
breastmilk, are more easily managed. Absence of stools. There is no passage of stools
within a day or two after birth.
Surgical Management
Passing of stools in other opening. The infant may
1. Single stage pull-through procedure
pass stools through another opening like the urethra
May be performed with laparoscopic, open,
in boys or vagina in girls.
or transanal techniques. This procedure can
be performed at the time of diagnosis or after Swollen belly. The newborn could not pass stools,
the newborn has had rectal irrigation at home resulting in a swollen belly.
and has passed the physiologic nadir.
2. Leveling colostomy. Absence of anal opening. The opening of the anus
A colostomy at the level of normal bowel. A is missing or not in its usual place. In girls, this may
staged procedure with placement of a leveled be near the vagina.
colostomy followed by a pull-through Diagnostic Findings
procedure.
Sacral radiography. Two views of the sacrum,
Nursing Management posteroanterior and lateral, should be obtained to
Promote skin integrity. When performing routine measure sacral ratios and to look for sacral defects,
colostomy care, give careful attention to the area hemivertebrae, and presacral masses. This should be
around the colostomy. Record and report redness, performed before surgery.
irritation, and rashy appearancs of the skin around the Abdominal ultrasonography. This study is
stoma. Prepare the skin with skin-toughening specifically used to examine the GU tract and to look
preparations that strengthen it and provide better for any other masses.
adhesion of the appliance.
MRI. All children who have sacral defects on plain
Promote comfort. Observe for s/sx of pain, such as radiographs should undergo spine ultrasonography to
crying, pulse, and respiration rate increases, rule out associated malformations such as
restlessness, guarding of the abdomen, or drawing up meningococele, teratoma, or mixed lesions.
the legs.
CT scan. CT scanning presently plays no role in the
Administer analgesics as ordered. routine evaluation of children with anorectal
Additional nursing intervention include: changing malformations.
the child’s position, holding the child when possible, Medical Management
stroking, cuddling, and engaging in age-appropriate
activities. 1. Nothing per orem
2. Neonatal colostomy. A colostomy is
Maintain fluid balance. Accurate intake and output performed in children who are not responsive
determinations and reporting the character, amount, to primary pull-through either because of
and consistency of stools help determine when the malformation.
child may have oral feedings. To monitor fluid loss, 3. Primary neonatal pull-through without
record and report drainage from the NG tube every 8 colostomy.
You might also like
- Jigsaw 1 Group 8Document11 pagesJigsaw 1 Group 8Muhammad Jefri LukmanNo ratings yet
- Pediatric NursingDocument16 pagesPediatric NursingWendy Escalante100% (1)
- Cleft Lip and Cleft PalateDocument27 pagesCleft Lip and Cleft Palatenamah odatNo ratings yet
- Developmental Disturbances - Dr. Nermine El BaheyDocument11 pagesDevelopmental Disturbances - Dr. Nermine El BaheyMOHAMED AMINNo ratings yet
- Maternal First Quiz ReviewerDocument15 pagesMaternal First Quiz ReviewerRay Ann BorresNo ratings yet
- GASTROINTESTINAL DISORDERS Cleft Palate - Esophageal Atresia - Oral MoniliasisDocument7 pagesGASTROINTESTINAL DISORDERS Cleft Palate - Esophageal Atresia - Oral MoniliasisMikasa AckermanNo ratings yet
- Gastrointestinal SystemDocument14 pagesGastrointestinal SystemBrix ValdrizNo ratings yet
- Cleft Lip and Cleft PalateDocument16 pagesCleft Lip and Cleft Palatemacuka08100% (3)
- Cleft LipDocument5 pagesCleft LipGrazieNo ratings yet
- Nursing Care of The Child Born With PhysicalDocument55 pagesNursing Care of The Child Born With PhysicalJoy kimmNo ratings yet
- Cleft Lip & PalateDocument77 pagesCleft Lip & PalateRah Ma GhassanNo ratings yet
- Maulee Sheth Balraj ShuklaDocument45 pagesMaulee Sheth Balraj ShuklaJustforkiddslaserdental ChNo ratings yet
- The Child W/ Alterations in Nutrition/Metabolism: Report By: Anita P. Prieto & Sugar Lynn M. CafirmaDocument6 pagesThe Child W/ Alterations in Nutrition/Metabolism: Report By: Anita P. Prieto & Sugar Lynn M. CafirmaAnita PrietoNo ratings yet
- MCN Lec FinalsDocument51 pagesMCN Lec FinalsTrishaNo ratings yet
- HABITS SeminarDocument97 pagesHABITS SeminarsharunshankarnNo ratings yet
- Common Acquired and Congenital Anomalies (Infangy) Congenital Anomalies Signs and SymptomsDocument5 pagesCommon Acquired and Congenital Anomalies (Infangy) Congenital Anomalies Signs and SymptomsShermina JalaniNo ratings yet
- Cleft Lip and Cleft PalateDocument4 pagesCleft Lip and Cleft PalateJulliza Joy PandiNo ratings yet
- Feedingmanagementin Infantswithcraniofacial Anomalies: Jill M. MerrowDocument8 pagesFeedingmanagementin Infantswithcraniofacial Anomalies: Jill M. MerrowingridspulerNo ratings yet
- Tongue Tie: From Confusion To Clarity-A ReviewDocument4 pagesTongue Tie: From Confusion To Clarity-A Reviewrahmaputra100% (1)
- Tongue Thrusting PDFDocument5 pagesTongue Thrusting PDFRenieKumalaNo ratings yet
- Open Bite MalocclusionDocument71 pagesOpen Bite MalocclusionMohsen Saeed Ozaibi100% (1)
- Pedia Report 13Document10 pagesPedia Report 13laurie.charlynjaneNo ratings yet
- Cleft Lip and Palate - PPT - OrthodonticsDocument46 pagesCleft Lip and Palate - PPT - OrthodonticsDr.Neethu Salam100% (3)
- Teething: Krishna Chauhan 55 3 YearDocument29 pagesTeething: Krishna Chauhan 55 3 YearkrishnaNo ratings yet
- Tongue Thrusting Habit & Other Habits, Its Management 2Document20 pagesTongue Thrusting Habit & Other Habits, Its Management 2Madhu Sudan ReddyNo ratings yet
- LABIOPALATOSCHIZISDocument25 pagesLABIOPALATOSCHIZISEya Prepti SerraNo ratings yet
- Cleft Lip & Palate - KushDocument84 pagesCleft Lip & Palate - KushKush PathakNo ratings yet
- Tongue TieDocument12 pagesTongue TieLeTara DavisNo ratings yet
- A Feeding Appliance For A 2 Day Old Neonate With Cleft Lip and Palate - A Case ReportDocument4 pagesA Feeding Appliance For A 2 Day Old Neonate With Cleft Lip and Palate - A Case ReportPark Jimin100% (1)
- Pediatric Nursing CareDocument5 pagesPediatric Nursing CareValerie BeteNo ratings yet
- Habit Breaking Appliance For Tongue Thrusting - A ModificationDocument5 pagesHabit Breaking Appliance For Tongue Thrusting - A ModificationsrinandanNo ratings yet
- Development of PalateDocument41 pagesDevelopment of PalateNahid zafarNo ratings yet
- Obh 5 PDFDocument7 pagesObh 5 PDFFajrul AkmalNo ratings yet
- Self Correcting ANOMALIESDocument31 pagesSelf Correcting ANOMALIESDONA MARIAM SAMNo ratings yet
- Tongue TieDocument37 pagesTongue TieKamalakanta Das100% (2)
- Physical and Developmental Disorders of The Gastrointestinal SystemDocument10 pagesPhysical and Developmental Disorders of The Gastrointestinal SystemJo Marchianne PigarNo ratings yet
- Cleft Lip and Cleft Palate: College of Health Science Department of Midwifery Course Newborn Care For PostbasicDocument42 pagesCleft Lip and Cleft Palate: College of Health Science Department of Midwifery Course Newborn Care For PostbasicmichaelNo ratings yet
- Assessment Nursing Scientific Basis Objective of Care Implementation RationaleDocument3 pagesAssessment Nursing Scientific Basis Objective of Care Implementation RationaleCamille RamosNo ratings yet
- Cleft Lip and Cleft Palate: Sharada Pathak M.Sc. Nursing Department of Medical Surgical Nursing 2014 BatchDocument20 pagesCleft Lip and Cleft Palate: Sharada Pathak M.Sc. Nursing Department of Medical Surgical Nursing 2014 Batchurmila dewanNo ratings yet
- Oral Habits Part 2 Tongue ThrustingDocument45 pagesOral Habits Part 2 Tongue ThrustingSudeep M. Choudhary100% (1)
- CarsDocument6 pagesCarsVelado Alessandra Loraine B.No ratings yet
- Management of Feeding Problems in A Cleft Lip and Palate Patient With Feeding Appliance: A Case ReportDocument7 pagesManagement of Feeding Problems in A Cleft Lip and Palate Patient With Feeding Appliance: A Case ReportNadeemNo ratings yet
- Oral Habits 2021Document38 pagesOral Habits 2021afnanNo ratings yet
- Types of Cleft Palate Surgeries and Side EffectsDocument91 pagesTypes of Cleft Palate Surgeries and Side Effectsahmad shaddadNo ratings yet
- Cleft Lip and Cleft PalateDocument63 pagesCleft Lip and Cleft Palateياسر نعيم الربيعيNo ratings yet
- Functional Development of Arches - Factors InfluencingDocument21 pagesFunctional Development of Arches - Factors InfluencingAME DENTAL COLLEGE RAICHUR, KARNATAKANo ratings yet
- Pedia GiDocument10 pagesPedia GiCam IbardolasaNo ratings yet
- Lec.6 OrthoDocument3 pagesLec.6 OrthoHelpers 48No ratings yet
- Cleft Lip and Cleft PalateDocument6 pagesCleft Lip and Cleft PalatekrishnasreeNo ratings yet
- Ecc Rampant CariesDocument63 pagesEcc Rampant Carieselle70503No ratings yet
- ENT - Diseases of The Oral Cavity and PharynxDocument6 pagesENT - Diseases of The Oral Cavity and PharynxChristian LantanoNo ratings yet
- Cleft Lip and PalateDocument1 pageCleft Lip and PalatefdgrgNo ratings yet
- Cleft Lip and PalateDocument4 pagesCleft Lip and PalateAyah HyasatNo ratings yet
- Lesson 16Document20 pagesLesson 16Twinamasiko DanielNo ratings yet
- Prevention of Oral HabitsDocument20 pagesPrevention of Oral HabitsomarNo ratings yet
- Oral HabitsDocument78 pagesOral HabitsMrunali MaskeNo ratings yet
- Pedia PT3Document7 pagesPedia PT3Kun AndresNo ratings yet
- Cleft Lip PalateDocument4 pagesCleft Lip PalateMaricel DefiestaNo ratings yet
- Hernia, (Different Types) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHernia, (Different Types) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Trends and Constraints in ResearchDocument1 pageTrends and Constraints in ResearchMyraflor CaroNo ratings yet
- Reviewer For BioethicsDocument5 pagesReviewer For BioethicsMyraflor CaroNo ratings yet
- MCHN With Abnormalities ReviewerDocument8 pagesMCHN With Abnormalities ReviewerMyraflor CaroNo ratings yet
- Insulin AdministrationDocument45 pagesInsulin AdministrationMyraflor CaroNo ratings yet
- Covid19 - Pathophysiology and ManagementDocument51 pagesCovid19 - Pathophysiology and ManagementMyraflor CaroNo ratings yet
- Common Medical TermsDocument2 pagesCommon Medical TermsMyraflor CaroNo ratings yet
- Guia 6. Trastorno Motor y SensitivoDocument47 pagesGuia 6. Trastorno Motor y SensitivoLorna Varela ArquinNo ratings yet
- Muscle and Bone Strenthening ActivitiesDocument14 pagesMuscle and Bone Strenthening ActivitiesSussy BakaNo ratings yet
- Nitazoxanide, A New Thiazolide Antiparasitic AgentDocument8 pagesNitazoxanide, A New Thiazolide Antiparasitic AgentHenry CollazosNo ratings yet
- HANDOUTS Brain SurgeryDocument3 pagesHANDOUTS Brain SurgerynieltresNo ratings yet
- NRC - Skill Competency Checklist - PainAsessmentOlderAdults - SkillChecklistDocument2 pagesNRC - Skill Competency Checklist - PainAsessmentOlderAdults - SkillChecklist紅玉練No ratings yet
- UDID What Medical Doctors May Need To KnowDocument37 pagesUDID What Medical Doctors May Need To KnowdrhareeshNo ratings yet
- SciaticaDocument35 pagesSciaticaRahmadanii RahmadaniiNo ratings yet
- MAPEHDocument3 pagesMAPEHGermaine Guimbarda MiguelesNo ratings yet
- Gad Accomplishment Report: I Narrative Report II Program of WorksDocument5 pagesGad Accomplishment Report: I Narrative Report II Program of WorksSARAH JEAN CABUGNASONNo ratings yet
- Spinal Tumors Intra-Extra (Turgut Tali)Document92 pagesSpinal Tumors Intra-Extra (Turgut Tali)Drbaddireddy RayuduNo ratings yet
- Blood Safety and SURVEILLANCE PDFDocument629 pagesBlood Safety and SURVEILLANCE PDFsahrish100% (1)
- Risk Assessment Envirn Mad Cow Disease-2Document9 pagesRisk Assessment Envirn Mad Cow Disease-2api-436969344No ratings yet
- D-37/1, TTC MIDC, Turbhe, Navi Mumbai-400 703: Test Name ResultDocument3 pagesD-37/1, TTC MIDC, Turbhe, Navi Mumbai-400 703: Test Name ResultShaikh EsaNo ratings yet
- BE FAST ED FormDocument1 pageBE FAST ED FormTHARHATA I JUHASANNo ratings yet
- An Introduction To The Mckenzie Method: Treating Your Own BackDocument24 pagesAn Introduction To The Mckenzie Method: Treating Your Own BackR HariNo ratings yet
- Psychopathology Os SisaDocument7 pagesPsychopathology Os SisaJoannaNo ratings yet
- Is Vaginal Delivery or Caesarean Section The Safer Mode of Delivery in Patients With Adult Congenital Heart DiseaseDocument7 pagesIs Vaginal Delivery or Caesarean Section The Safer Mode of Delivery in Patients With Adult Congenital Heart DiseaseNathania TjuwatjaNo ratings yet
- Botany 4Document6 pagesBotany 4Upadhyay HarshitNo ratings yet
- Aslani 2023Document5 pagesAslani 2023Marcos DuarteNo ratings yet
- Campy Lo Bacterio SisDocument14 pagesCampy Lo Bacterio SisHarikrishnan NamNo ratings yet
- Multiple Organ Dysfunction Syndrome: HistoryDocument6 pagesMultiple Organ Dysfunction Syndrome: HistoryJasmine BaduaNo ratings yet
- Urethritis Guideline 2017 PDFDocument3 pagesUrethritis Guideline 2017 PDFPggil Puthree Tiga KaliyNo ratings yet
- How We Conquered SmallpoxDocument4 pagesHow We Conquered SmallpoxNadir BaghdadNo ratings yet
- Pathophysiology of Chronic Renal Failure PDFDocument4 pagesPathophysiology of Chronic Renal Failure PDFDewa Made Rendy SanjayaNo ratings yet
- Microbiology MB QuestionsDocument13 pagesMicrobiology MB QuestionsRashmi Ranjan100% (1)
- Chapter 3 SOAP NoteDocument2 pagesChapter 3 SOAP NoteKatrina Litzko50% (2)
- NBME 26 Question - AnswerDocument54 pagesNBME 26 Question - AnswerAsmaaNasserNo ratings yet
- HSE Bulletin - March 2024 - RamadanDocument2 pagesHSE Bulletin - March 2024 - RamadanraiavaniranjanNo ratings yet
- 54750174Document3 pages54750174Rouwi DesiatcoNo ratings yet
- 1.5A Copd: OutlineDocument12 pages1.5A Copd: OutlineCecille Ann CayetanoNo ratings yet