Professional Documents
Culture Documents
AEDguidelines
Uploaded by
Mezga Mzperx0 ratings0% found this document useful (0 votes)
6 views3 pagesCopyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
6 views3 pagesAEDguidelines
Uploaded by
Mezga MzperxCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 3
Resuscitation 48 (2001) 207– 209
www.elsevier.com/locate/resuscitation
European Resuscitation Council Guidelines 2000 for
Automated External Defibrillation
A statement from the Basic Life Support and Automated External Defibrillation Working
Group1 and approved by the Executive Committee of the European Resuscitation Council
Koenraad G. Monsieurs *,1, Anthony J. Handley, Leo L. Bossaert
Ghent Uni6ersity Hospital, Intensi6e Care Unit 1K12IC, De Pintelaan 185, 9000 Ghent, Belgium
1. Introduction changes have been made to achieve international
uniformity.
The European Resuscitation Council (ERC) is- The major changes in technique are as follows:
sued guidelines for the use of Automated External (a) Delivery of basic life support has been
Defibrillators (AEDs) in 1998 [1]. The American revised to accord with the new ERC BLS guide-
Heart Association (AHA), together with represen- lines. There are two important changes.
tatives of the International Liaison Committee on (i) Immediately after identifying absence of
Resuscitation (ILCOR) then undertook a series of normal breathing two initial rescue breaths are
evidence based evaluations of the science of resus- delivered. In the 1998 guidelines it was stated that
citation [2] which culminated in the publication of the initial breaths could be omitted when a defi-
Guidelines 2000 for Cardiopulmonary Resuscita- brillator was immediately available. This has been
tion and Emergency Cardiovascular Care in changed to achieve uniformity between the BLS
August 2000 [3,4]. The Basic Life Support and and the AED protocols which should aid skill
Automated External Defibrillation Working retention. Moreover, the delivery of the two initial
Group (BLS and AED Working Group of the breaths is an essential part of the assessment of
ERC) has considered this document and the sup- signs of a circulation (see below).
(ii) The carotid pulse check is no longer in-
porting scientific literature and has recommended
cluded in the protocol for lay rescuers. The reason
changes to the ERC AED guidelines. These are
for this change is that several studies have shown
presented in this paper.
that well in excess of 10 s is required for the
diagnosis of the presence or absence of a carotid
pulse [5–9] and even with prolonged palpation
2. Guidelines changes
significant errors in diagnosis occur [10]. Lay res-
cuers will now ‘look for signs of a circulation’
Some of the changes reflect changes in BLS
meaning look, listen and feel for normal breath-
procedure during the AED protocol. Other
ing, coughing or movement for no more than 10 s.
For the initial assessment, this is performed after
* Corresponding author.
E-mail address: koen.monsieurs@rug.ac.be (K.G. Monsieurs). delivery of two rescue breaths. If the rescuer is not
1
ERC BLS and AED Working Group: Arntz H-R, Bahr J, Baubin confident that one or more of these signs of a
M, Bossaert L, Brucan A, Carneiro A, Cassan P, Chamberlain D, circulation are present he or she should begin
Davies S, De Vos R, Ekstrom L, Evans T, Gwinnutt C, Handley A,
Lexow K, Marsden A, Monsieurs K, Petit P, Sofianos E, Van Dreuth chest compressions immediately and continue with
A, Van Rillaer L, Wik L, Wolcke B. the AED protocol.
0300-9572/01/$ - see front matter © 2001 European Resuscitation Council. Published by Elsevier Science Ireland Ltd. All rights reserved.
PII: S 0 3 0 0 - 9 5 7 2 ( 0 0 ) 0 0 3 7 8 - 6
208 K.G. Monsieurs et al. / Resuscitation 48 (2001) 207–209
Healthcare providers should continue to perform
a carotid pulse check in addition to checking the
other signs of a circulation; they should take no
more than 10 s to do this.
A potential problem with omission of the pulse
check is that return of a spontaneous circulation
may go undetected if the victim does not make any
movement or start breathing. In these circum-
stances, the lay rescuer will continue to deliver
chest compressions. Undesirable as this may be, the
evidence that lay rescuers are unable to determine
the presence or absence of a carotid pulse reliably
suggests that this would happen even if a pulse
check was included. When healthcare providers
arrive they will feel for a pulse and confirm the
presence of a circulation.
(b) When no shock is indicated, or immedi-
ately after a series of three shocks, CPR should be
given for 1 min. In the 1998 ERC guidelines the
duration of CPR was 3 min after ‘no shock indi-
cated’, except when the message followed a success-
ful defibrillation, when it was 1 min [1]. Although
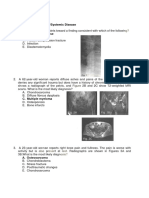
the 1998 guidelines were developed for optimal Fig. 1. Automated external defibrillation.
delivery of CPR in case of non-shockable rhythms, availability of an AED have priority. In the text,
the new guidelines achieve uniformity between use of the masculine includes the feminine (Fig. 1).
AED protocols. It is hoped that this simplification
will result in better acquisition and retention of 1. Assess 7ictim
skills. Check response: gently shake his shoulders
The international guidelines AED algorithm rec- and ask loudly ‘Are you all right?’
ommends a circulation check after the completion Open airway; tilt head and lift chin. Check for
of each minute of CPR, followed by manual activa- breathing
tion of the analysis sequence [3,4]. Many AEDs do Assuming he is not breathing, activate EMS
not have an analysis button and will initiate each and if not already obtain AED
analysis automatically. Therefore this additional Give two effective breaths
check for signs of a circulation is omitted from the Check for signs of a circulation:
current ERC guidelines. – for lay rescuers this means look, listen and
(c) If the AED protocol is to be used by feel for normal breathing, coughing, or move-
advanced life support (ALS) providers, adrenaline/ ment by the victim. Take no more than 10 s to
epinephrine should be administered every 2–3 min, do this.
not during each cycle of CPR, which lasts only 1 – for health care providers this will also include
min. checking the carotid pulse.
2A. If signs of a circulation are present
3. Sequence of actions If breathing present put victim into recovery
position
The following is the agreed sequence of actions If no breathing, start rescue breathing and
that constitute the ERC Guidelines 2000 for AED. re-check for signs of a circulation every minute
The algorithm is intended for the resuscitation of
persons aged 8 years or over. The algorithm as- 2B. If no signs of a circulation
sumes that only one rescuer is present. If more than Switch on AED
one rescuer is present, tasks should be assigned. Attach electrodes
Activation of the EMS system and immediate Follow spoken/visual instructions
K.G. Monsieurs et al. / Resuscitation 48 (2001) 207–209 209
Ensure that nobody touches the victim whilst References
the AED is analysing the rhythm.
[1] Early Defibrillation Task Force of the European Re-
3A. If a shock is indicated suscitation Council. The 1998 European Resuscitation
Ensure that everybody is clear of the victim Council guidelines for the use of automated external
Push shock button as directed defibrillators by EMS providers and first responders.
Resuscitation 1998;37:91– 4
Repeat ‘analyse’ or ‘shock’ as directed
[2] American Heart Association in collaboration with
If at any time a ‘no shock indicated’ condition is the International Liaison Committee on Resuscitation
present: see 3B (ILCOR). Introduction to the International Guidelines
Do not check for signs of a circulation between 2000 for CPR and ECC. Guidelines 2000 for car-
the first three shocks diopulmonary resuscitation and emergency cardiovas-
After three shocks check for signs of a cular care— An international consensus on science.
Resuscitation 2000;46:3– 15.
circulation
[3] American Heart Association in collaboration with the
If no signs of a circulation present International Liaison Committee on Resuscitation
Perform CPR for 1 min
(ILCOR). Guidelines 2000 for cardiopulmonary resus-
There should be no voice prompts during this citation and emergency cardiovascular care. An inter-
time. CPR will be timed by the AED timer. national consensus on science. Circulation
After 1 min stop CPR to allow rhythm 2000;102(Suppl. I):I-1– I-384.
analysis [4] American Heart Association in collaboration with
Continue the AED algorithm as directed by the International Liaison Committee on Resuscitation
(ILCOR). Guidelines 2000 for cardiopulmonary resus-
voice and visual prompts
citation and emergency cardiovascular care— An inter-
If signs of a circulation ARE present national consensus on science. Resuscitation
If breathing is present, put victim into recov-
2000;46:1– 447.
ery position [5] Flesche CW, Breuer S, Mandel LP, Brevik H, Tarnow
If no breathing, start rescue breathing and J. The ability of health professionals to check the
re-check for signs of a circulation every minute carotid pulse. Circulation 1994;90(Suppl. 1):288.
[6] Mather C, O’Kelly S. The palpitation of pulses.
3B. If no shock indicated Anaesthesia 1996;51:189– 91.
Look for signs of a circulation [7] Monsieurs KG, De Cauwer HG, Bossaert LL. Feeling
for the carotid pulse: is five seconds enough? Resusci-
If no signs of a circulation present, perform
tation 1996;31:S3.
CPR for 1 min [8] Bahr J, Klingler H, Panzer W, Rode H, Kettler D.
There should be no voice prompts during this Skills of lay people in checking the carotid pulse. Re-
time. CPR will be timed by the AED timer. suscitation 1997;35:23– 6.
After 1 min stop CPR to allow rhythm [9] Ochoa FJ, Ramalle-Gomara E, Carpintero JM,
analysis Garcia A, Saralegui I. Competence of health profes-
Continue the AED algorithm as directed by sionals to check the carotid pulse. Resuscitation
1998;37:173– 5.
voice and visual prompts [10] Eberle B, Dick WF, Schneider T, Wisser G, Doetsch
S, Tzanova I. Checking the carotid pulse: Diagnostic
4. Continue to follow AED instructions until ALS is accuracy of first responders in patients with and with-
a7ailable out a pulse. Resuscitation 1996;33:107– 16.
You might also like
- BLS With MCQDocument37 pagesBLS With MCQKIMS quality100% (1)
- Hi-Yield Notes in SurgeryDocument18 pagesHi-Yield Notes in SurgeryJohn Christopher Luces50% (2)
- Guidelines - In-Hospital ResuscitationDocument18 pagesGuidelines - In-Hospital ResuscitationparuNo ratings yet
- BLS MCQ For Final Exam PDFDocument33 pagesBLS MCQ For Final Exam PDFMoaz Albaba86% (14)
- Neuropsychology of Bipolar DisorderDocument9 pagesNeuropsychology of Bipolar DisorderwulanfarichahNo ratings yet
- Anesthesiology Resident Manual of Procedures: A Step-by-Step GuideFrom EverandAnesthesiology Resident Manual of Procedures: A Step-by-Step GuideNo ratings yet
- Basic Life Support and Advanced Cardiovascular Life SupportDocument90 pagesBasic Life Support and Advanced Cardiovascular Life SupportRakhshanda khan100% (1)
- CPR GuidelinesDocument30 pagesCPR GuidelineswvhvetNo ratings yet
- First Aid Handbook: With Clear Explanations & 100+ Instructive ImagesFrom EverandFirst Aid Handbook: With Clear Explanations & 100+ Instructive ImagesNo ratings yet
- Dopesick - Opioid Epidemic On Healthcare and SocietyDocument11 pagesDopesick - Opioid Epidemic On Healthcare and Societyapi-482726932No ratings yet
- Adult Advanced Life SupportDocument14 pagesAdult Advanced Life SupportAnonymous TT7aEIjhuhNo ratings yet
- Emergency Guidelines for Medical EmergenciesDocument72 pagesEmergency Guidelines for Medical EmergenciesRumana Ali100% (2)
- Abrupta Placenta - 4 Pt presents with vaginal bleeding, ABDOMINAL PAIN, and uterine tendernessDocument211 pagesAbrupta Placenta - 4 Pt presents with vaginal bleeding, ABDOMINAL PAIN, and uterine tendernessroad2successNo ratings yet
- Insulin AdministrationDocument9 pagesInsulin AdministrationMonika JosephNo ratings yet
- Core ACLS ConceptsDocument60 pagesCore ACLS ConceptsLex CatNo ratings yet
- Guidelines Adult Advanced Life SupportDocument35 pagesGuidelines Adult Advanced Life SupportindahNo ratings yet
- ALS Manual PDFDocument74 pagesALS Manual PDFBlack Owell100% (1)
- Color Atlas of Small Animal Necropsy 1Document81 pagesColor Atlas of Small Animal Necropsy 1Sai KrupaNo ratings yet
- ESA2013 Abstract BookDocument300 pagesESA2013 Abstract BookAyyaz HussainNo ratings yet
- Orthopaedic Oncology Study QuestionsDocument18 pagesOrthopaedic Oncology Study QuestionsFasa RoshadaNo ratings yet
- Trauma and Emergency NursingDocument9 pagesTrauma and Emergency Nursingchinthaka18389021No ratings yet
- Bls - Acls Update American Heart Association 2020: Ns. Anastasia Hardyati., Mkep., Sp. KMBDocument26 pagesBls - Acls Update American Heart Association 2020: Ns. Anastasia Hardyati., Mkep., Sp. KMBcelvin sohilait100% (1)
- Ghiduriresuscitare2010V2 UnlockedDocument938 pagesGhiduriresuscitare2010V2 UnlockedMadalina Blaga100% (1)
- Advanced Life Support-RESSU CouncilDocument30 pagesAdvanced Life Support-RESSU CouncilGigel DumitruNo ratings yet
- ALS Guidelines 2000Document11 pagesALS Guidelines 2000xandra_lNo ratings yet
- Recommendations)Document10 pagesRecommendations)Niko NeznanovicNo ratings yet
- ERC Guidelines 2015 FULL PDFDocument311 pagesERC Guidelines 2015 FULL PDFISRAEL33JAGS0% (1)
- Tony Handley - New CPR Guidelines ExplainedDocument8 pagesTony Handley - New CPR Guidelines ExplainedJeaudeen JaleelNo ratings yet
- Guidelines Adult Advanced Life SupportDocument34 pagesGuidelines Adult Advanced Life SupportParvathy R NairNo ratings yet
- ANZCOR Guideline 11.2 - Protocols For Adult Advanced Life SupportDocument8 pagesANZCOR Guideline 11.2 - Protocols For Adult Advanced Life SupportMario Colville SolarNo ratings yet
- Word ERC Section 3. S0300-9572 (15) 00328-7 - MainDocument48 pagesWord ERC Section 3. S0300-9572 (15) 00328-7 - MainImam Hakim SuryonoNo ratings yet
- Concord CPR ManualDocument54 pagesConcord CPR ManualtntranNo ratings yet
- Resusitasi AnastesiDocument15 pagesResusitasi AnastesiFannia ReynathaNo ratings yet
- Practice: Adult and Paediatric Basic Life Support: An Update For The Dental TeamDocument4 pagesPractice: Adult and Paediatric Basic Life Support: An Update For The Dental TeamsmilekkmNo ratings yet
- CPR Guideline PDFDocument157 pagesCPR Guideline PDFPandu AnggoroNo ratings yet
- 44 CPR PDFDocument14 pages44 CPR PDFBramantyo NugrosNo ratings yet
- Weaning From Mechanical Ventilation in Neurocritical CareDocument10 pagesWeaning From Mechanical Ventilation in Neurocritical CareAngela Moreira ArteagaNo ratings yet
- European Resuscitation Council and European Society of Intensive Care Medicine Guidelines 2021: Post-Resuscitation CareDocument53 pagesEuropean Resuscitation Council and European Society of Intensive Care Medicine Guidelines 2021: Post-Resuscitation CareDaniel FajardoNo ratings yet
- Resusgl 2010Document157 pagesResusgl 2010Salman IslamNo ratings yet
- Executive Summary VF20101018Document24 pagesExecutive Summary VF20101018Dana SoimuNo ratings yet
- Anzcor Guideline 9 1 5 Harness Suspension Trauma April 2021 2Document3 pagesAnzcor Guideline 9 1 5 Harness Suspension Trauma April 2021 2mychaelNo ratings yet
- Of The Main Changes in The Resuscitation GuidelinesDocument24 pagesOf The Main Changes in The Resuscitation GuidelinesYapa YapaNo ratings yet
- Improve Circulation and Oxygenation During CPR with CPVDocument8 pagesImprove Circulation and Oxygenation During CPR with CPVCode ValmirNo ratings yet
- Referensi 7Document8 pagesReferensi 7Nophy NapitupuluNo ratings yet
- Adult Advanced Life Support: Resuscitation Council (UK)Document23 pagesAdult Advanced Life Support: Resuscitation Council (UK)Masuma SarkerNo ratings yet
- AAOS Paperchapter With Jupiter and AmadioDocument11 pagesAAOS Paperchapter With Jupiter and AmadioreyNo ratings yet
- Management of Respiratory Motion in PET/computed Tomography: Nuclear Medicine Communications February 2014Document11 pagesManagement of Respiratory Motion in PET/computed Tomography: Nuclear Medicine Communications February 2014Andreas RonaldNo ratings yet
- Freynet2016 PDFDocument2 pagesFreynet2016 PDFdesthalia cyatraningtyasNo ratings yet
- Basic Life Support (BLS) and Advanced Cardiac Life Support (ACLS)Document7 pagesBasic Life Support (BLS) and Advanced Cardiac Life Support (ACLS)Rizki YuliantoNo ratings yet
- BLS MCQSDocument6 pagesBLS MCQSNur IbrahimNo ratings yet
- Resuscitation Council (UK) In-Hospital Cardiac Arrest GuidelinesDocument10 pagesResuscitation Council (UK) In-Hospital Cardiac Arrest GuidelinesCzarian Estillore HigoyNo ratings yet
- ERC 2015 Basic Life SupportDocument19 pagesERC 2015 Basic Life SupportfentaNo ratings yet
- Bls Guideline For ResusDocument17 pagesBls Guideline For ResusirfanzukriNo ratings yet
- Basic Life Suppor T: Monalyn B. La-Ao, RN Glenn Ryan Palao-Ay, RNDocument37 pagesBasic Life Suppor T: Monalyn B. La-Ao, RN Glenn Ryan Palao-Ay, RNMarlon Pilis B CanggatNo ratings yet
- ERC Guidelines 2005Document186 pagesERC Guidelines 2005api-3743776No ratings yet
- ALS AlgorithmDocument22 pagesALS AlgorithmBookwormNo ratings yet
- ¡BLS Adults 2021! EuropeDocument13 pages¡BLS Adults 2021! EuropeSofía ACNo ratings yet
- CPR First? or Defibrillation First?: Re-AffirmedDocument4 pagesCPR First? or Defibrillation First?: Re-AffirmedangelNo ratings yet
- Cardio Pulmonary Resuscitation (CPR) : Tracey Gibson, Elaine Cole & Anne McleodDocument6 pagesCardio Pulmonary Resuscitation (CPR) : Tracey Gibson, Elaine Cole & Anne McleodRETINA CREATIONSNo ratings yet
- ACLS Practice QuizDocument29 pagesACLS Practice Quizezzat salemNo ratings yet
- Resuscitation Council AED GuidelinesDocument7 pagesResuscitation Council AED GuidelinesMon SoeNo ratings yet
- Cardiac Life Support Manual-Thiru 2016 -Revised (Repaired)_Aug 2017Document92 pagesCardiac Life Support Manual-Thiru 2016 -Revised (Repaired)_Aug 2017Petracharles AkashiNo ratings yet
- Transport: Administering Oxygen by Manual Resuscitation BAG Nursing Action RationaleDocument3 pagesTransport: Administering Oxygen by Manual Resuscitation BAG Nursing Action RationaleIan TuNo ratings yet
- Keys to Successful Orthotopic Bladder SubstitutionFrom EverandKeys to Successful Orthotopic Bladder SubstitutionUrs E. StuderNo ratings yet
- Current Techniques in Canine and Feline NeurosurgeryFrom EverandCurrent Techniques in Canine and Feline NeurosurgeryAndy ShoresNo ratings yet
- Preeklampsia Update - Layanan Primer - BPJSDocument50 pagesPreeklampsia Update - Layanan Primer - BPJSansyNo ratings yet
- Drug AddictionDocument7 pagesDrug AddictionZechariah NicholasNo ratings yet
- Treatment Options For Hyperemesis GravidarumDocument11 pagesTreatment Options For Hyperemesis GravidarumJC QuinNo ratings yet
- Guidelines of The American Thyroid Association PREGNANCY PDFDocument47 pagesGuidelines of The American Thyroid Association PREGNANCY PDFIqra AnugerahNo ratings yet
- Writing Hooks For EssaysDocument4 pagesWriting Hooks For Essaysb72hvt2d100% (2)
- Goto 2019Document6 pagesGoto 2019Marmox Lab.No ratings yet
- MCQ Ped EndocvsDocument2 pagesMCQ Ped EndocvsManveerNo ratings yet
- Ivf StudyDocument1 pageIvf StudyjeliinNo ratings yet
- The 1 ASMIHA Digital Conference: Indonesian Journal of CardiologyDocument256 pagesThe 1 ASMIHA Digital Conference: Indonesian Journal of CardiologysuprisuryadiNo ratings yet
- Ebola Virus: Sorveto, Dayle Daniel GDocument10 pagesEbola Virus: Sorveto, Dayle Daniel GDayledaniel SorvetoNo ratings yet
- Procedure (Blood Transfusion)Document4 pagesProcedure (Blood Transfusion)Richard PattersonNo ratings yet
- DHIS Monthly Reporting Form (PHC Facilities)Document4 pagesDHIS Monthly Reporting Form (PHC Facilities)Usman88% (8)
- NCM 112 (11F)Document15 pagesNCM 112 (11F)Justine April YbanezNo ratings yet
- Subjective Cues: Ineffective Tissue PerfusionDocument3 pagesSubjective Cues: Ineffective Tissue PerfusionFlorence Lacea Rotsap-DeguitNo ratings yet
- Policy For Patients Under Restraints: Nursing Excellence UnitDocument22 pagesPolicy For Patients Under Restraints: Nursing Excellence UnitjinoNo ratings yet
- Procedure:: Pada HastasanaDocument11 pagesProcedure:: Pada HastasanaSidharth TaylorNo ratings yet
- Drug Name Dosage Mechanism of Action Specific Interactions Contraindications and Cautions Adverse Reaction Nursing ConsiderationsDocument4 pagesDrug Name Dosage Mechanism of Action Specific Interactions Contraindications and Cautions Adverse Reaction Nursing ConsiderationsCeelin RoblesNo ratings yet
- Maternal NSG ProceduresDocument18 pagesMaternal NSG ProceduresGARCIA, KYLA MAE A.No ratings yet
- Basic Information On Pharmaceutical Dosage Forms and Drug Delivery SystemsDocument30 pagesBasic Information On Pharmaceutical Dosage Forms and Drug Delivery SystemsSyed Hussain AsafNo ratings yet
- NCM 107 5M Case Analysis PDFDocument9 pagesNCM 107 5M Case Analysis PDFKisha BethelNo ratings yet
- Copy 1 of Treatment Profile For Intern Docto 2Document57 pagesCopy 1 of Treatment Profile For Intern Docto 2AminulNo ratings yet
- Daily Learning Activity Sheet Peh1 All Strand Week 4Document4 pagesDaily Learning Activity Sheet Peh1 All Strand Week 4Joyce Dela Rama JulianoNo ratings yet