Professional Documents
Culture Documents
Jamapediatrics Fraiman 2022 Oi 210085 1648672932.43603
Uploaded by
Luke EishenhowerOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Jamapediatrics Fraiman 2022 Oi 210085 1648672932.43603
Uploaded by
Luke EishenhowerCopyright:
Available Formats
Research
JAMA Pediatrics | Original Investigation
Effect of a Novel Mindfulness Curriculum on Burnout
During Pediatric Internship
A Cluster Randomized Clinical Trial
Yarden S. Fraiman, MD, MPH; Christine C. Cheston, MD; Howard J. Cabral, PhD, MPH; Celeste Allen, MD;
Andrea G. Asnes, MD, MSW; Jefferson T. Barrett, MD, MPH; Maneesh Batra, MD, MPH; William Bernstein, MD;
Tammy Bleeker, MEd; Pam M. Dietz, MD; Joanna Lewis, MD; Su-Ting T. Li, MD, MPH; T. Marsha Ma, MD;
John D. Mahan, MD; Catherine D. Michelson, MD, MMSc; Sue E. Poynter, MD, MEd; Mark A. Vining, MD;
Katherine Watson, DO; Colin M. Sox, MD, MS
Visual Abstract
IMPORTANCE Mindfulness curricula can improve physician burnout, but implementation Supplemental content
during residency presents challenges.
OBJECTIVE To examine whether a novel mindfulness curriculum implemented in the first 6
months of internship reduces burnout.
DESIGN, SETTING, AND PARTICIPANTS This pragmatic, multicenter, stratified cluster
randomized clinical trial of a mindfulness curriculum randomized 340 pediatric interns to the
intervention or control arm within program pairs generated based on program size and
region. Fifteen US pediatric training programs participated from June 14, 2017, to February
28, 2019.
INTERVENTIONS The intervention included 7 hour-long sessions of a monthly mindfulness
curriculum (Mindfulness Intervention for New Interns) and a monthly mindfulness refresher
implemented during internship. The active control arm included monthly 1-hour social
lunches.
MAIN OUTCOMES AND MEASURES The primary outcome was emotional exhaustion (EE) as
measured by the Maslach Burnout Inventory 9-question EE subscale (range, 7-63; higher
scores correspond to greater perceived burnout). Secondary outcomes were
depersonalization, personal accomplishment, and burnout. The study assessed mindfulness
with the Five Facet Mindfulness Questionnaire and empathy with the Interpersonal Reactivity
Index subscales of perspective taking and empathetic concern. Surveys were implemented at
baseline, month 6, and month 15.
RESULTS Of the 365 interns invited to participate, 340 (93.2%; 255 [75.0%] female; 51
[15.0%] 30 years or older) completed surveys at baseline; 273 (74.8%) also participated at
month 6 and 195 (53.4%) at month 15. Participants included 194 (57.1%) in the Mindfulness
Intervention for New Interns and 146 (42.9%) in the control arm. Analyses were adjusted for
baseline outcome measures. Both arms’ EE scores were higher at 6 and 15 months than at
baseline, but EE did not significantly differ by arm in multivariable analyses (6 months: 35.4 vs
32.4; adjusted difference, 3.03; 95% CI, −0.14 to 6.21; 15 months: 33.8 vs 32.9; adjusted
difference, 1.42; 95% CI, −2.42 to 5.27). None of the 6 secondary outcomes significantly
differed by arm at month 6 or month 15.
CONCLUSIONS AND RELEVANCE A novel mindfulness curriculum did not significantly affect EE,
burnout, empathy, or mindfulness immediately or 9 months after curriculum
implementation. These findings diverge from prior nonrandomized studies of mindfulness
interventions, emphasizing the importance of rigorous study design and suggesting that
additional study is needed to develop evidence-based methods to reduce trainee burnout.
TRIAL REGISTRATION ClinicalTrials.gov Identifier: NCT03148626 Author Affiliations: Author
affiliations are listed at the end of this
article.
Corresponding Author: Yarden S.
Fraiman, MD, Department of
Neonatology, Beth Israel Deaconess
Medical Center, 330 Brookline Ave,
JAMA Pediatr. 2022;176(4):365-372. doi:10.1001/jamapediatrics.2021.5740 Rose 3, Boston, MA 02215 (yfraiman
Published online January 24, 2022. @bidmc.harvard.edu).
(Reprinted) 365
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Zwingly Christian Porajow on 04/05/2022
Research Original Investigation Effect of a Novel Mindfulness Curriculum on Burnout During Pediatric Internship
B
urnout is a triad of emotional exhaustion (EE), deper-
sonalization, and feelings of inefficacy.1 Between 39% Key Points
and 75% of pediatric trainees experience burnout, with
Question Can a novel mindfulness curriculum designed for
a worsening trend in prevalence during the past few decades.2-5 implementation in residency that does not require facilitator
Burnout affects physicians’ well-being, performance during training reduce burnout among pediatric interns?
training, risk of suicide, and patient care. Physicians with burn-
Findings This cluster randomized clinical trial found that the levels
out are more likely to make medical errors and be less empa-
of emotional exhaustion, depersonalization, burnout, empathy,
thetic, and the patients of physicians with burnout are less and mindfulness among pediatric interns who completed the
likely to adhere to medical plans.6-11 Physician burnout costs 6-month mindfulness curriculum did not significantly differ from
the US health care system approximately $4.6 billion per year those assigned to social lunches both immediately after
related to physician turnover and reduced productivity.12 completing the training experience and 9 months later.
Mindfulness, a state of nonjudgmental awareness in the Meaning A novel mindfulness curriculum did not affect pediatric
present moment, can prevent burnout. Mindfulness curri- interns’ levels of burnout, empathy, and mindfulness compared
cula can reduce burnout among physicians and other with social time only, suggesting that additional study is needed to
professionals.13-18 Mindfulness is the only evidence-based ap- develop evidence-based methods to reduce trainee burnout.
proach to reduce burnout included in an Accreditation Coun-
cil for Graduate Medical Education and American Academy of
Pediatrics call for systems-level change to address trainee Intervention Arm
burnout.19 Although mindfulness curricula are effective, po- A 6-step approach to curricular design informed the devel-
tential barriers to implementing mindfulness curricula in- opment of MINdI.22,23 The MINdI curriculum easily inte-
clude time required by the trainees and availability of facili- grates into existing 1-hour didactic time ubiquitous among
tators with content expertise. Small single-center trials17,18,20,21 training programs and requires no additional facilitator
of mindfulness have found variable effects. We know of no pub- training.22 Intervention programs received the MINdI facili-
lished multicenter randomized clinical trials of mindfulness tator manual and all necessary curriculum implementation
curricula that target trainee burnout. To assess the effective- supplies. The intervention was delivered monthly, starting
ness of a novel mindfulness curriculum that does not require during the first quarter of the intern year and continuing for
prior facilitator training, Mindfulness Intervention for New In- 6 months, for a total of 7 sessions; programs were encour-
terns (MINdI),22 on burnout among pediatric interns, we con- aged to facilitate interns’ attendance at MINdI sessions,
ducted a multicenter cluster randomized clinical trial. We hy- although attendance was not required.
pothesized that interns training in programs randomized to the The MINdI curriculum was developed by a multidisciplinary
mindfulness curriculum would have less burnout than in- team of medical education experts, residency program leader-
terns randomized to the control arm. ship, a chief resident, mindfulness practitioners, and trainees.
Briefly, each session begins with a social lunch, followed by a min-
ute of silence, introductory remarks regarding the mindfulness
exercise, a mindfulness exercise, and a debriefing period. The cur-
Methods riculum is designed to provide mindfulness exercises that can eas-
Study Sample and Randomization ily be integrated into a medical trainee’s day or highlight a unique
We conducted a pragmatic, multicenter, stratified cluster ran- aspect of mindfulness that can be beneficial to medical trainees.
domized clinical trial of a mindfulness curriculum during pe- In addition to the monthly curriculum, intervention programs
diatric internship. See Supplement 1 for full trial protocol. We were encouraged to invite participants to conduct a short mind-
recruited 15 US pediatric residency programs to participate in fulness refresher, a 10-minute prerecorded body scan exercise,
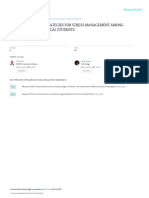
this study and sent surveys to 365 eligible interns (Figure 1). 2 weeks after each MINdI session.
All sites’ institutional review boards approved the study. To
be eligible for inclusion, each participating pediatric resi- Control Arm
dency program agreed to be randomized to have their interns In the active control arm, participants were scheduled to at-
experience the MINdI curriculum or social lunches. From June tend 6 interns-only, 1-hour social lunches that involved no
14 to September 29, 2017, pediatric and medicine-pediatric in- mindfulness activities, as other mindfulness curricula ran-
terns training in study programs gave implied written con- domized clinical trials have done.18
sent by returning the baseline survey. All data were deidenti-
fied. This study followed the Consolidated Standards of Outcomes
Reporting Trials (CONSORT) reporting guideline. Outcomes were measured through surveys at baseline,
After pairing programs by location and size, we used a month 6, and month 15. The Maslach Burnout Inventory
random-number generator to assign, within a pair, each program’s Human Services Survey was used under license with Mind
cluster of interns to experience a novel 7-session MINdI curricu- Garden Inc. The primary outcome (EE) was measured using
lum or an active control experience of nondidactic social lunch. the Maslach Burnout Inventory 9-question EE subscale
Because an odd number of programs participated, we created 1 (range, 7-63; higher scores correspond to higher degrees of
dummy variable for paired randomization. Each program’s interns perceived burnout). 1 Prespecified secondary outcomes
had the same arm-specific unblinded training experience. included dichotomized burnout and the Maslach Burnout
366 JAMA Pediatrics April 2022 Volume 176, Number 4 (Reprinted) jamapediatrics.com
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Zwingly Christian Porajow on 04/05/2022
Effect of a Novel Mindfulness Curriculum on Burnout During Pediatric Internship Original Investigation Research
Inventory 5-item depersonalization subscale (range, 7-35;
Figure 1. CONSORT Study Flow Diagram
higher scores correspond to higher degrees of perceived
burnout) and 8-item personal accomplishment subscale
365 Assessed for eligibility
(range, 7-56; higher scores correspond to lower degrees of
perceived burnout), as well as mindfulness and empathy. 6 Excluded for declining
We defined burnout as having an EE score of 27 or higher participation
and/or a depersonalization score of 10 or higher. 1,24 We
measured mindfulness using the 39-item Five Facet Mind- 359 Randomized
fulness Questionnaire, on which higher scores on a scale of
39 to 195 are interpreted as increased mindfulness. 25,26
We assessed empathy using the Interpersonal Reactivity 204 Allocated to MINdI intervention 155 Allocated to control arm
Index’s Perspective Taking and Empathic Concern sub-
scales, on which higher scores are interpreted as increased 194 Baseline questionnaire returned 146 Baseline questionnaire returned
empathy.27,28
The baseline survey also collected demographic informa-
148 6-mo Questionnaire returned 125 6-mo Questionnaire returned
tion and report of prior mindfulness behaviors; surveys at
months 6 and 15 also collected self-report of mindfulness-
related knowledge, attitudes, and behaviors. Surveys at base- 106 15-mo Questionnaire returned 89 15-mo Questionnaire returned
line were implemented before participants completed the first
study session, and those at month 6 were implemented after 194 Analyzed 146 Analyzed
completing the final study session. Participants were offered
a $5 coffee gift card after completing each survey. MINdI indicates Mindfulness Intervention for New Interns.
Statistical Analysis
To examine whether subject characteristics varied by study arm
while addressing hierarchical effects of cluster randomiza- were performed in PROC MI via a multiple imputation with
tion, we conducted bivariate linear generalized estimating chained equations approach with fully conditional specifi-
equations and logistic regressions clustered on center. To es- cation. Data were imputed when missing at baseline given
timate the between-group difference in outcome between the variables with fully observed values. Then the baseline data
randomized groups while addressing hierarchical effects of and fully observed variables at 6 months were used to
cluster randomization, we used multivariate generalized es- impute values for variables with missing data at 6 months.
timating equations and logistic regressions clustered on cen- This process continued in a similar fashion, with prior data
ter. All regressions included study arm, independent mea- and variables fully observed at 15 months used to impute
sures that significantly differed by study arm, or measures that missing values at 15 months. We report effect sizes as linear
were of a priori clinical interest, including self-identified gen- regression coefficients quantifying differences in means or
der and age. Race and ethnicity data were not collected be- in logistic model odds ratios (ORs) with 95% CIs, as well as
cause we did not consider race or ethnicity to be significantly 2-sided P values for primary outcome analyses. A 2-sided
associated with burnout during the study design. To address P < .05 was considered statistically significant.
the concern of including independent variables possibly in the Setting 1 − β = 0.8 and 2-sided α = .05, our a priori
causal pathway, we performed additional sensitivity analy- power calculations determined that at least 139 participants
ses without these variables and that included only baseline per group were needed to determine a 0.29 difference in
variables. mean EE to be statistically significant, a threshold selected
In addition, analyses of data at month 6 and/or month 15 because a meta-analysis 30 found that burnout reduction
controlled for the outcome at baseline, baseline survey month, interventions significantly lowered EE scores by 0.28. These
prior weekend off at month 6, inpatient or intensive care ro- c alculations, however, did not account for possible
tation at month 15, and an arm × survey period interaction term clustering by site. Had this been done, applying a reason-
based on prior data.29 If the arm × survey month interaction able intraclass correlation of 0.01 would have yielded a
term was statistically significant, we conducted stratified analy- required enrollment sample with an additional 256 partici-
ses of the month 6 and month 15 data. If the interaction term pants to achieve 80% power with a 2-sided α = .05. This
was not significant, then we removed the interaction term and addition of participants to the sample would not have been
conducted longitudinal analyses comparing the pooled out- feasible, however, given the planned study period. We note
comes at month 6 and month 15 while controlling for that our sample as implemented was larger than other ran-
baseline. domized clinical trials of mindfulness curricula that have
Because 29.8% of data was missing, we conducted all intended to address burnout. We have provided 95% CIs
multivariable analyses on 20 imputed data sets created with all estimates of group differences so that readers can
using individual-level data following standard imputation judge the precision, or lack thereof, of our findings in this
procedures using PROC MI and PROC MI ANALYZE in SAS sample, in particular with respect to prior research14-17 with
software, version 9.4 (SAS Institute Inc). These imputations smaller samples.
jamapediatrics.com (Reprinted) JAMA Pediatrics April 2022 Volume 176, Number 4 367
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Zwingly Christian Porajow on 04/05/2022
Research Original Investigation Effect of a Novel Mindfulness Curriculum on Burnout During Pediatric Internship
Table 1. Study Sample Characteristics and Outcome at Baselinea
All MINdI arm Control arm
Characteristic or outcome (N = 340) (n = 194) (n = 146)
Personal characteristics
Gender
Female 255 (75.0) 153 (78.9) 102 (69.9)
Abbreviation: MINdI, Mindfulness
Male 85 (25.0) 41 (21.1) 44 (30.1) Intervention for New Interns.
Age ≥30 y 51 (15.0) 32 (16.6) 19 (13.0) a
Data are presented as number
No prior mindfulness training 103 (30.5) 61 (31.6) 42 (29.0) (percentage) of interns unless
No prior mindfulness practice 56 (16.5) 30 (15.5) 26 (17.8) otherwise indicated.
Program characteristics b
On the basis of analyses of
Program with <20 interns 93 (27.4) 48 (24.7) 45 (30.8) nonimputed responses from study
US region participants measured at baseline.
c
Eastern 159 (44.3) 66 (34.0) 91 (62.3) Total scores on the 9-item
Central 118 (32.9) 59 (30.4) 42 (27.8) emotional exhaustion subscale
(range, 7-63; higher scores
Western 82 (22.8) 69 (35.6) 13 (8.9)
correspond to higher degrees of
Medicine-pediatrics residents 16 (4.7) 11 (5.7) 5 (3.5)
perceived burnout).
Survey implementation d
Total scores on the 5-item
Baseline (survey during intern orientation) 213 (62.7) 118 (60.8) 95 (65.1) depersonalization subscale (range,
Month 6 7-35; higher scores correspond to
Vacation in prior month 77 (30.4) 43 (31.4) 34 (29.3) higher degrees of perceived
Prior weekend off 108 (42.7) 54 (39.4) 54 (46.6) burnout).
e
Rotating on inpatient or intensive care service 184 (73.0) 104 (76.5) 80 (69.0) Total scores on the 8-item personal
Month 15 accomplishment subscale (range,
Vacation in prior month 61 (32.8) 29 (28.2) 32 (38.6) 7-56; higher scores correspond to
lower degrees of perceived
Prior weekend off 98 (52.7) 58 (56.3) 40 (48.2)
burnout).
Rotating on inpatient or intensive care service 92 (50.0) 44 (43.1) 48 (58.5) f
Total scores on the 7-item
Outcomes at baselineb
perspective taking subscale (range,
Burnout 233 (68.5) 145 (74.7) 88 (60.3) 7-35; higher scores correspond to
Emotional exhaustion, mean (SD)c 27.2 (9.7) 28.2 (10.1) 25.9 (8.9) higher degrees of perceived
Depersonalization, mean (SD)d 11.5 (5.1) 11.9 (5.0) 11.0 (4.8) empathy).
Personal accomplishment, mean (SD)e 39.3 (8.2) 41.5 (4.1) 36.3 (10.9) g
Total scores on the 39-item Five
Empathetic concerns, mean (SD)f 17.9 (2.2) 18.0 (2.0) 17.9 (2.2) Facet Mindfulness scale (range,
Perspective taking, mean (SD)f 19.3 (2.9) 19.4 (3.0) 19.2 (2.8) 39-195; higher scores correspond to
higher degrees of perceived
Mindfulness, mean (SD)g 127.7 (16.3) 126.7 (16.5) 126.7 (16.1)
mindfulness).
[10.9]; P = .003). Although burnout and mean EE and deper-
Results sonalization scores did not differ at baseline by arm, these mea-
sures significantly increased during the 78-day enrollment pe-
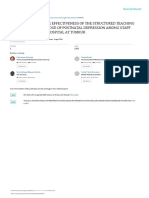
Study Participants riod for 4 months in both groups (Figure 2). At month 6, MINdI
Of the 359 consenting interns, 340 (94.7%; 255 [75.0%] fe- participants were significantly less likely to have had the prior
male; 51 [15.0%] 30 years or older) completed surveys at base- weekend off than controls (54 [39.4%] vs 54 [46.6%]; P = .04).
line, 273 at month 6 (76.0%), and 195 at month 15 (54.3%); the At month 15, MINdI participants were significantly less likely
19 interns who did not complete the baseline survey were ex- to be rotating on an inpatient or intensive care service than con-
cluded. Analyses included 194 intervention participants (57.1%) trols (44 [43.1%] vs 48 [58.5%]; P = .02). Table 2 and Table 3
and 146 control participants (42.9%). The dropout rate was present results of multivariable analyses of 20 imputed data
19.7% at 6 months and 42.6% at 15 months. Characteristics be- sets conducted to determine the effect of arm on continuous
tween those who were lost to follow-up and those who com- and dichotomous outcomes, respectively.
pleted the study were not markedly different (eTable in
Supplement 2). Primary Outcomes
Table 1 presents the study population characteristics. Gen- In multivariable analyses of imputed data, EE at baseline did not
der was the only personal or program characteristic that sig- significantly differ between the MINdI and control arms (adjusted
nificantly differed by arm, with more female interns in the difference, −0.37; 95% CI, −3.03 to 3.77) (Table 2). The MINdI and
MINdI arm than in the control arm (female vs male: 255 [75.0%] control arms’ mean (SD) EE scores were higher at month 6 (35.4
vs 85 [25.0%] for all interns; 153 [78.9%] vs 41 [21.1%] for MINdI vs 32.4) than baseline (28.3 vs 25.6); however, multivariable analy-
arm; and 102 [69.9%] vs 44 [30.1%] for the control arm; ses controlling for baseline EE revealed that EE at month 6 did not
P = .002). The only outcome that significantly differed at base- significantly differ by study arm (adjusted difference, 3.03; 95%
line in bivariate analyses was personal accomplishment, with CI, −0.14 to 6.21). Both arms’ mean EE scores remained higher
the MINdI arm’s mean (SD) personal accomplishment score than baseline at month 15 (33.8 vs 32.9). In multivariable longi-
being higher than that in the control group (41.5 [4.1] vs 36.3 tudinal analyses, the arm-period interaction term was statistically
368 JAMA Pediatrics April 2022 Volume 176, Number 4 (Reprinted) jamapediatrics.com
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Zwingly Christian Porajow on 04/05/2022
Effect of a Novel Mindfulness Curriculum on Burnout During Pediatric Internship Original Investigation Research
significant (P = .02); in stratified multivariable analyses, EE did
Figure 2. Burnout at Baseline Measurement
not significantly differ by arm at month 15 (adjusted difference,
1.42; 95% CI, −2.42 to 5.27).
Emotional exhaustion (MINdI) Emotional exhaustion (control)
Depersonalization (MINdI) Depersonalization (control)
Secondary Outcomes Personal accomplishment (MINdI) Personal accomplishment (control)
Most respondents had burnout at baseline (74.7% in the
50 100
MINdI arm and 60.3% in the control arm, month 6 (92.0%
in the MINdI arm and 80.5% in the control arm), and month
40 80
15 (83.7% in the MINdI arm and 88.3% in the control arm)
Mean subscale score
(Table 3). At baseline, no differences by arm were found in
Burnout, %
30 60
burnout, depersonalization (mean [SD] scores, 11.9 [5.0] for
the MINdI arm and 11.0 [4.8] for the control arm), mindful-
20 40
ness (mean [SD] scores, 126.6 [16.4] for the MINdI arm and
126.5 [16.1] for the control arm), empathetic concerns (mean
10 20
[SD] scores, 18.0 [2.0] for the MINdI arm and 17.9 [2.2] for
the control arm), or perspective taking (mean [SD] scores
0 0
19.4 [3.0] for the MINdI arm and 19.2 [2.8] for the control June July-September
arm). Month of baseline survey
No significant differences by arm were found in prior mind-
MINdI indicates Mindfulness Intervention for New Interns.
fulness training (31.6% in the MINdI arm and 29.0% in the con-
trol arm) or practice (15.5% in the MINdI arm and 17.8% in the
control arm) at baseline. Multivariable longitudinal analyses
revealed that levels of mindfulness (adjusted difference, −1.07;
95% CI, −5.27 to 3.13), empathetic concerns (adjusted differ- Discussion
ence, 0.27; 95% CI, −0.54 to 1.08), perspective taking (ad-
justed difference, 0.74; 95% CI, −0.53 to 2.02), and personal Our multicenter cluster randomized clinical trial of a novel mind-
accomplishment (adjusted difference, 0.14; 95% CI, −1.70 to fulness curriculum implemented early in pediatric internship
1.98) did not significantly differ by arm between month 6 and found that the intervention did not significantly affect interns’
month 15. The arm × period interaction term was statistically EE, depersonalization, burnout, personal accomplishment, mind-
significant in multivariable longitudinal analyses conducted fulness, or empathy immediately after curriculum implementa-
to the effect of arm on depersonalization (P < .001) and burn- tion and 15 months later. After the 6-month curriculum was com-
out (P = .004); subsequent multivariable analyses stratified by pleted, MINdI participants were significantly more likely than con-
period revealed that these outcomes did not significantly dif- trols to report knowing how to apply mindfulness techniques and
fer by arm at month 15. their evidence, as well as having a positive attitude about mind-
At month 6, multivariable analyses identified significant fulness and believing it benefited their life. Fifteen months after
increases in report of knowing the evidence to support mind- curriculum implementation, the only measure with a statistically
fulness (adjusted OR, 3.23; 95% CI, 1.63-6.39), how to apply significant between-arm difference was in knowledge of the evi-
mindfulness (adjusted OR, 3.99; 95% CI, 3.25-4.90), the be- dence supporting the use of mindfulness.
lief that mindfulness benefited their life (adjusted OR, 2.51; 95% In contrast to prior studies14,15,17,18 of mindfulness curricu-
CI, 1.03-6.11), and having a positive attitude toward mindful- lum, our study found no changes in burnout rates or levels of EE,
ness (adjusted OR, 2.60; 95% CI, 1.67-4.07). Most of these depersonalization, mindfulness, or empathy between interven-
changes were not persistent over time. Self-reported fre- tion and control participants. Our study intervention differs from
quency of mindfulness practice at baseline and month 6 did prior studies14,15 in a number of important ways. First, our cur-
not significantly differ by arm (adjusted OR, 1.48; 95% CI, 0.72- riculum was not facilitated by an experienced mindfulness prac-
3.02). The odds of using these techniques more after the cur- titioner. Recognizing the limitation of facilitation by a local con-
riculum did not significantly differ by arm between month 6 tentexpertonthefeasibilityofwidespreaddisseminationofmind-
and month 15 (adjusted OR, 1.02; 95% CI, 0.57-1.82). The fulness curricula, our curriculum relied on a scripted curriculum
arm × period interaction term was statistically significant that did not require a content expert to facilitate education. How-
(P < .001) in multivariable longitudinal analyses conducted to ever, our results prompt us to question the potential effect of
test the effect of arm on reporting to know how to apply, be- greater facilitator experience in mindfulness training on curricu-
lief in the benefit of, and having a positive attitude toward lum effectiveness.
mindfulness; subsequent multivariable analyses stratified by Second, prior curricula have been more robust compared
period revealed that none of these outcomes significantly dif- with MINdI.13-15,21,30,31 For example, the mindfulness-based
fered by arm at month 15. stress reduction curriculum published by Krasner et al14 was
In the sensitivity analyses in which time-dependent vari- composed of an 8-week intensive phase that included 2.5 hours
ables were removed, the results relating to intervention ef- per week and a 7-hour retreat followed by a 2.5-hour per month
fects were similar to those described above and in the tables maintenance period for 10 months. In contrast, our 7-session
of our regression models. monthly curriculum was specifically designed to integrate into
jamapediatrics.com (Reprinted) JAMA Pediatrics April 2022 Volume 176, Number 4 369
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Zwingly Christian Porajow on 04/05/2022
Research Original Investigation Effect of a Novel Mindfulness Curriculum on Burnout During Pediatric Internship
Table 2. Impact of the MINdI Curriculum on Continuous Measures of Burnout, Mindfulness, and Empathy at Baseline, Month 6, and Month 15a
Baseline, Month 6 Month 15 Pooled MINdI vs control
unadjusted Unadjusted Adjusted difference Unadjusted Adjusted difference Unadjusted Adjusted difference
Outcomes mean mean (95% CI)b mean (95% CI)c mean (95% CI)d
Emotional exhaustion
MINdI arm 28.3 35.4 33.8 NA NA
3.03 (−0.14 to 6.21) 1.42 (−2.42 to 5.27)
Control arm 25.6 32.4 32.9 NA NA
Depersonalization
MINdI arm 11.9 16.0 15.0 NA NA
1.2 (−0.56 to 2.96) −0.27 (−2.37 to 1.83)
Control arm 11.0 14.8 15.5 NA NA
Personal accomplishment
MINdI arm 41.5 41.6 NA NA 40.5
0.06 (−1.80 to 7.91) 0.14 (−1.70 to 1.98)
Control arm 36.3 41.6 NA NA 39.5
Mindfulness
MINdI arm 126.6 125.5 NA NA 128.6
−0.91 (−5.67 to 3.85) −1.07 (−5.27 to 3.13)
Control arm 126.5 126.4 NA NA 127.1
Empathetic concerns
MINdI arm 18.0 17.2 NA NA 16.7
0.24 (−0.71 to 1.18) 0.27 (−0.54 to 1.08)
Control arm 17.9 17.0 NA NA 17.0
Perspective taking
MINdI arm 19.4 21.5 NA NA 20.7
1.02 (−0.36 to 2.41) 0.74 (−0.53 to 2.02)
Control arm 19.2 20.4 NA NA 20.8
Abbreviations: MINdI, Mindfulness Intervention for New Interns; NA, not 15 clustered on site while controlling for gender, age, month at baseline,
applicable (pooled analyses were not completed based on the interaction baseline personal accomplishment, current inpatient rotation, and the level of
term). the outcome at month 6. The longitudinal data were stratified by assessment
a
Mean results are from multivariable analyses of 20 imputed data sets. period (month 6 and month 15) because preliminary models that included a
b
MINdI arm × period interaction term were statistically significant.
Results of multivariable generalized estimating equation regressions at month
d
6 clustered on site while controlling for gender, age, month at baseline, Results of multivariable longitudinal generalized estimating equation
baseline personal accomplishment, prior weekend off, and the outcome of regressions comparing pooled month 6 and month 15 while controlling for
interest at baseline. gender, age, month at baseline, baseline personal accomplishment, current
c
inpatient rotation, and the outcome at baseline.
Results of multivariable generalized estimating equation regressions at month
preexisting residency didactic time. It is possible our curricu- Finally, selection bias may have influenced prior
lum may not have been robust enough to induce a change in cohort studies13-16 conducted among physicians who chose
behavior and objective metrics of burnout, mindfulness, or em- to participate in the mindfulness training that found
pathy, although changes in mindfulness-related knowledge and mindfulness to be associated with decreased burnout.
attitudes were apparent. Although programs were encour- Small studies and those among medical trainees have often
aged to take attendance, it was not required. Thus, we have failed to show large or statistically significant effects of
no consistent data on how many training sessions each intern mindfulness on objective measures of burnout, empathy, or
experienced. We wonder whether there could be a dose mindfulness.13,16,17,20,21,30
response in the mindfulness training that we are not able to
assess in which more participation may have led to better out- Limitations
comes among trainees. This study has several limitations. First, cluster randomiza-
In our study population, most participants in both arms tion resulted in an imbalance in gender and baseline personal
had scores indicating burnout at baseline, and burnout wors- accomplishment between study arms. Second, our study is lim-
ened during the study period. Because most participants com- ited by missing data, a common limitation that may intro-
pleted the baseline survey before internship began, efforts to duce bias into the results; to address this, we estimated miss-
reduce burnout among trainees should be integrated into un- ing values by multiple imputation, which may have resulted
dergraduate medical education. Despite reporting increased in underestimation of SEs. Third, our sample size was based
mindfulness-related knowledge and positive attitudes to- on power calculations that did not account for possible clus-
ward mindfulness after completing the curriculum, partici- tering by site. Thus, findings of clinical importance that were
pants did not report corresponding increases in mindfulness not statistically significant should be cautiously interpreted
practice or objective measures of mindfulness. Perhaps com- and their precision judged by the widths of their 95% CIs.
peting demands and priorities early in medical training, in- Fourth, our pragmatic trial design allowed variation in month
cluding a primary focus on increasing clinical competence, per- of the intervention and control experiences and survey imple-
sistently outweighed prioritization of new self-care techniques mentation, so temporal trends in burnout during training may
to prevent burnout. have influenced intervention efficacy and our findings.
370 JAMA Pediatrics April 2022 Volume 176, Number 4 (Reprinted) jamapediatrics.com
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Zwingly Christian Porajow on 04/05/2022
Effect of a Novel Mindfulness Curriculum on Burnout During Pediatric Internship Original Investigation Research
Table 3. Impact of the MINdI Curriculum on Dichotomous Measure of Burnout and Mindfulness-Related Knowledge,
Behavior, and Attitudes at Baseline, Month 6, and Month 15a
Baseline, Month 6 Month 15 Pooled MINdI vs control
unadjusted Unadjusted Unadjusted Unadjusted
b c
Outcomes rate rate, % AOR (95% CI) rate, % AOR (95% CI) rate, % AOR (95% CI)d
Burnoute
MINdI arm 74.7 92.0 83.7 NA NA
2.28 (0.77-6.71) 0.60 (0.17-2.20)
Control arm 60.3 80.5 88.3 NA NA
Knows evidence supporting mindfulness
MINdI arm NA 69.4 NA NA 68.3
3.23 (1.63-6.39) 2.56 (1.46-4.47)
Control arm NA 40.4 NA NA 58.1
Knows how to apply mindfulness in own life
MINdI arm NA 76.9 80.4 NA NA
3.99 (3.25-4.90) 1.64 (0.66-4.10)
Control arm NA 42.5 71.0 NA NA
Believes mindfulness benefited their life
MINdI arm NA 60.1 73.0 NA NA
2.51 (1.03-6.11) 1.24 (0.44-3.49)
Control arm NA 27.0 63.2 NA NA
Holds positive attitude toward mindfulness
MINdI arm NA 72.2 64.1 NA NA
2.60 (1.67-4.07) 0.64 (0.24-1.74)
Control arm NA 56.5 67.8 NA NA
Uses mindfulness techniques more often
MINdI arm NA 38.9 NA NA 64.7
1.48 (0.72-3.02) 1.02 (0.57-1.82)
Control arm NA 25.9 NA NA 61.9
Abbreviations: AOR, adjusted odds ratio; MINdI, Mindfulness Intervention for the outcome at month 6. The longitudinal data were stratified by assessment
New Interns; NA, not applicable (pooled analyses were not completed based on period (month 6 and month 15) because preliminary models that included a
the interaction term). MINdI arm × period interaction term were statistically significant.
a d
Mean results are from multivariable analyses of 20 imputed data sets. Results of multivariable longitudinal logistic regressions comparing month 6 to
b
Results of multivariable logistic regressions at month 6 clustered on site while month 15 while controlling for gender, age, month at baseline, baseline
controlling for gender, age, month at baseline, baseline personal personal accomplishment, prior weekend off, current inpatient rotation, the
accomplishment, prior weekend off, current inpatient rotation, and the outcome at baseline, assessment period, and a MINdI arm × period interaction
outcome of interest at baseline. term.
e
c
Results of multivariable logistic regressions at month 15 clustered on site while Because initial logistic regressions models analyzing burnout at month 6 that
controlling for gender, age, month at baseline, baseline personal clustered on site did not converge, the final regression model for burnout at
accomplishment, prior weekend off, current inpatient rotation, and the level of month 6 did not cluster on site.
The mixed results of our methodologically rigorous driven more at a systems level than a personal one, and in
cluster randomized clinical trial of MINdI may indicate that the context of pediatric internship, efforts to reduce burn-
trainees face unique challenges in integrating mindfulness out should focus more on system reform than personal
knowledge into behavior change. The study demonstrated training.21,30,32
that improvements in mindfulness-related knowledge and
attitudes failed to translate into effects on burnout, empa-
thy, and mindfulness. Although we cannot be sure why the
intervention did not have its intended effect, we hypoth-
Conclusions
esize 2 explanations. First, although MINdI was robust This multicenter cluster randomized clinical trial of a novel
enough to affect knowledge and attitudes, it was not strong mindfulness curriculum demonstrated that the intervention
enough to affect distal outcomes. Second, our study identi- did not significantly affect measures of burnout, mindful-
fied higher rates of burnout than previously reported in the ness, or empathy among pediatric interns training across the
literature of pediatric trainees. It is possible that the high US. However, intervention participants reported improved
levels of burnout we detected represent a meaningful tem- mindfulness-related knowledge, behaviors, and attitudes. The
poral shift and the diminished efficacy of individual-level mixed results of this large, multicenter randomized clinical trial
interventions, such as mindfulness, to address epidemic suggest that there is a need for further study, mechanism elu-
levels of burnout. Burnout in medical training may be cidation for behavior change, and curriculum optimization.
ARTICLE INFORMATION Children’s Hospital, Boston, Massachusetts Benioff Children’s Hospital Oakland, Oakland
Accepted for Publication: October 4, 2021. (Fraiman); Department of Pediatrics, Harvard (Allen); Yale-New Haven Hospital, New Haven,
Published Online: January 24, 2022. Medical School, Boston, Massachusetts (Fraiman); Connecticut (Asnes); Floating Hospital for Children–
doi:10.1001/jamapediatrics.2021.5740 Boston Medical Center, Department of Pediatrics, Tufts Medical Center, Boston, Massachusetts
Author Affiliations: Department of Neonatology, Boston University School of Medicine, Boston, (Barrett); Division of Emergency Medicine,
Beth Israel Deaconess Medical Center, Boston, Massachusetts (Cheston, Michelson, Sox); Department of Pediatrics, Boston Children’s
Massachusetts (Fraiman); Division of Newborn Deparment of Biostatistics, Boston University Hospital, Boston, Massachusetts (Barrett);
Medicine, Department of Pediatrics, Boston School of Public Health, Boston, Massachusetts Department of Pediatrics, The Children’s Hospital at
(Cabral); University of California, San Francisco Montefiore, Bronx, New York (Barrett); Division of
jamapediatrics.com (Reprinted) JAMA Pediatrics April 2022 Volume 176, Number 4 371
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Zwingly Christian Porajow on 04/05/2022
Research Original Investigation Effect of a Novel Mindfulness Curriculum on Burnout During Pediatric Internship
Neonatology, Department of Pediatrics, Seattle REFERENCES 16. Goldhagen BE, Kingsolver K, Stinnett SS,
Children’s Hospital, University of Washington, 1. Maslach C, Jackson SE, Leiter MP. Maslach Rosdahl JA. Stress and burnout in residents: impact
Seattle (Batra); Department of Pediatrics, Saint Burnout Inventory: third edition. In: Evaluating of mindfulness-based resilience training. Adv Med
Peter’s University Hospital, New Brunswick, New Stress: A Book of Resources. Scarecrow Education; Educ Pract. 2015;6:525-532. doi:10.2147/AMEP.
Jersey (Bernstein); Department of Pediatrics, 1997:191-218. Accessed March 9, 2019. https:// S88580
University of Florida, Gainesville (Bleeker); psycnet.apa.org/record/1997-09146-011 17. Verweij H, van Ravesteijn H, van Hooff MLM,
Department of Pediatrics, Maine Medical Center, Lagro-Janssen ALM, Speckens AEM.
2. Shanafelt TD, Hasan O, Dyrbye LN, et al.
Portland, Maine (Dietz); Department of Pediatrics, Mindfulness-based stress reduction for residents:
Changes in burnout and satisfaction with work-life
a randomized controlled trial. J Gen Intern Med.
Advocate Children’s Hospital, Park Ridge, Illinois balance in physicians and the general US working
2018;33(4):429-436. doi:10.1007/s11606-017-
(Lewis); Department of Pediatrics, University of population between 2011 and 2014. Mayo Clin Proc.
4249-x
California, Davis, Sacramento (Li); Pediatric 2015;90(12):1600-1613. doi:10.1016/j.mayocp.2015.
18. Ireland MJ, Clough B, Gill K, Langan F, O’Connor
Cardiology, Loyola Medicine, Maywood, Illinois 08.023
A, Spencer L. A randomized controlled trial of
(Ma); Division of Nephrology and Hypertension, 3. Ishak WW, Lederer S, Mandili C, et al. Burnout
mindfulness to reduce stress and burnout among
Department of Pediatrics, Nationwide Children’s, during residency training: a literature review. J Grad
intern medical practitioners. Med Teach. 2017;39
Columbus, Ohio (Mahan); Division of Critical Care, Med Educ. 2009;1(2):236-242. doi:10.4300/JGME-
(4):409-414. doi:10.1080/0142159X.2017.1294749
Department of Pediatrics, Cincinnati Children’s D-09-00054.1
19. McClafferty H, Brown OW; Section on
Hospital, University of Cincinnati, Cincinnati, Ohio 4. Baer TE, Feraco AM, Tuysuzoglu Sagalowsky S, Integrative Medicine; Committee on Practice And
(Poynter); Department of Pediatrics, University of Williams D, Litman HJ, Vinci RJ. Pediatric resident Ambulatory Medicine; Section on Integrative
Massachusetts Medical School, Worcester (Vining); burnout and attitudes toward patients. Pediatrics. Medicine. Physician health and wellness. Pediatrics.
2017;139(3):e20162163. doi:10.1542/peds.2016-2163 2014;134(4):830-835. doi:10.1542/peds.2014-2278
Division of General Academic Pediatrics, Children’s
Hospital of Pittsburgh, Pittsburgh, Pennsylvania 5. Zhou AY, Panagioti M, Esmail A, Agius R, 20. Lebares CC, Guvva EV, Olaru M, et al. Efficacy
Van Tongeren M, Bower P. Factors associated with of mindfulness-based cognitive training in surgery:
(Watson).
burnout and stress in trainee physicians: additional analysis of the mindful surgeon pilot
Author Contributions: Drs Cabral and Sox had full a systematic review and meta-analysis. JAMA Netw randomized clinical trial. JAMA Netw Open. 2019;2
access to all the data in the study and take Open. 2020;3(8):e2013761. doi:10.1001/ (5):e194108. doi:10.1001/jamanetworkopen.2019.
responsibility for the integrity of the data and the jamanetworkopen.2020.13761 4108
accuracy of the data analysis. 6. West CP, Huschka MM, Novotny PJ, et al. 21. West CP, Dyrbye LN, Erwin PJ, Shanafelt TD.
Concept and design: Fraiman, Cheston, Ma, Mahan, Association of perceived medical errors with Interventions to prevent and reduce physician
Michelson, Poynter, Watson, Sox. resident distress and empathy: a prospective burnout: a systematic review and meta-analysis.
Acquisition, analysis, or interpretation of data: longitudinal study. JAMA. 2006;296(9):1071-1078. Lancet. 2016;388(10057):2272-2281. doi:10.1016/
Fraiman, Cheston, Cabral, Allen, Asnes, Barrett, doi:10.1001/jama.296.9.1071 S0140-6736(16)31279-X
Batra, Bernstein, Bleeker, Dietz, Lewis, Li, Mahan, 7. Shanafelt TD, Balch CM, Bechamps G, et al. 22. Cheston CC, Sox CM, Michelson CD, Fraiman
Michelson, Poynter, Vining, Sox. Burnout and medical errors among American YS. MINdI: Mindfulness Instruction for New Interns.
Drafting of the manuscript: Fraiman, Cheston, surgeons. Ann Surg. 2010;251(6):995-1000. doi:10. MedEdPORTAL. 2020;16:10933. doi:10.15766/mep_
Cabral, Bleeker, Poynter, Sox. 1097/SLA.0b013e3181bfdab3 2374-8265.10933
Critical revision of the manuscript for important 8. Shanafelt TD, Noseworthy JH. Executive 23. Kern DE, Thomas PA, Howard DM, Bass EB.
intellectual content: Cheston, Cabral, Allen, Asnes, leadership and physician well-being: nine Curriculum Development for Medical Education:
Barrett, Batra, Bernstein, Dietz, Lewis, Li, Ma, organizational strategies to promote engagement A Six-Step Approach. Johns Hopkins University
Mahan, Michelson, Poynter, Vining, Watson, Sox. and reduce burnout. Mayo Clin Proc. 2017;92(1): Press; 1998.
Statistical analysis: Fraiman, Cabral, Sox. 129-146. doi:10.1016/j.mayocp.2016.10.004 24. Eckleberry-Hunt J, Kirkpatrick H, Barbera T.
Obtained funding: Fraiman, Sox. 9. Shanafelt TD, Balch CM, Dyrbye L, et al. Special The problems with burnout research. Acad Med.
report: suicidal ideation among American surgeons. 2018;93(3):367-370. doi:10.1097/ACM.
Administrative, technical, or material support:
Arch Surg. 2011;146(1):54-62. doi:10.1001/archsurg. 0000000000001890
Fraiman, Cheston, Allen, Asnes, Bernstein, Bleeker,
2010.292 25. Baer RA, Smith GT, Lykins E, et al. Construct
Ma, Mahan, Michelson, Poynter, Vining,
10. Dyrbye LN, Thomas MR, Massie FS, et al. validity of the five facet mindfulness questionnaire
Watson, Sox. in meditating and nonmeditating samples.
Supervision: Cheston, Allen, Bernstein, Burnout and suicidal ideation among U.S. medical
students. Ann Intern Med. 2008;149(5):334-341. Assessment. 2008;15(3):329-342. doi:10.1177/
Watson, Sox. 1073191107313003
Other - implementation of the mindfulness course at doi:10.7326/0003-4819-149-5-200809020-
00008 26. Baer RA, Smith GT, Hopkins J, Krietemeyer J,
1 institution: Dietz. Toney L. Using self-report assessment methods to
Other - coordination and implementation of 11. Staples BB, Burke AE, Batra M, et al; Pediatric
explore facets of mindfulness. Assessment. 2006;13
Resident Burnout-Resilience Study Consortium.
curriculum at 1 site: Barrett. (1):27-45. doi:10.1177/1073191105283504
Burnout and association with resident performance
Conflict of Interest Disclosures: None reported. 27. Davis MH. Measuring individual differences in
as assessed by pediatric milestones: an exploratory
Funding/Support: This study was supported in empathy: evidence for a multidimensional
study. Acad Pediatr. 2021;21(2):358-365. doi:10.
part by the Association of Pediatric Program approach. J Pers Soc Psychol. 1983;44(1):113-126.
1016/j.acap.2020.08.006
doi:10.1037/0022-3514.44.1.113
Directors’ Special Projects Program (Drs Fraiman 12. Han S, Shanafelt TD, Sinsky CA, et al. Estimating
and Sox) and the Fred Lovejoy House-staff 28. Davis MH. A multidimensional approach to
the attributable cost of physician burnout in the
individual differences in empathy. J Pers Soc Psychol.
Research and Education Fund at Boston Children’s United States. Ann Intern Med. 2019;170(11):784-790.
1980;10:85.
Hospital (Dr Fraiman). Dr Fraiman was supported by doi:10.7326/M18-1422
29. Kemper KJ, Schwartz A, Wilson PM, et al;
grant T32HS000063 from the Agency for 13. Lamothe M, Rondeau É, Malboeuf-Hurtubise C,
Pediatric Resident Burnout-Resilience Study
Healthcare Research and Quality as part of the Duval M, Sultan S. Outcomes of MBSR or
Consortium. Burnout in pediatric residents: three
Harvard-wide Pediatric Health Services Research MBSR-based interventions in health care providers:
years of national survey data. Pediatrics. 2020;145
Fellowship Program. a systematic review with a focus on empathy and
(1):e20191030. doi:10.1542/peds.2019-1030
Role of the Funder/Sponsor: The funding sources emotional competencies. Complement Ther Med.
2016;24:19-28. doi:10.1016/j.ctim.2015.11.001 30. Panagioti M, Panagopoulou E, Bower P, et al.
had no role in the design and conduct of the study; Controlled interventions to reduce burnout in
collection, management, analysis, and 14. Krasner MS, Epstein RM, Beckman H, et al.
physicians: a systematic review and meta-analysis.
interpretation of the data; preparation, review, or Association of an educational program in mindful
JAMA Intern Med. 2017;177(2):195-205. doi:10.1001/
approval of the manuscript; and decision to submit communication with burnout, empathy, and
jamainternmed.2016.7674
attitudes among primary care physicians. JAMA.
the manuscript for publication. 31. Beckman HB, Wendland M, Mooney C, et al.
2009;302(12):1284-1293. doi:10.1001/jama.2009.
Data Sharing Statement: See Supplement 3. The impact of a program in mindful communication
1384
Additional Contributions: We acknowledge the on primary care physicians. Acad Med. 2012;87(6):
15. Goodman MJ, Schorling JB. A mindfulness 815-819. doi:10.1097/ACM.0b013e318253d3b2
voluntary contributions made by faculty and course decreases burnout and improves well-being
administrators at each site who facilitated 32. Shanafelt TD, Dyrbye LN, West CP. Addressing
among healthcare providers. Int J Psychiatry Med.
implementing the study activities. physician burnout: the way forward. JAMA. 2017;
2012;43(2):119-128. doi:10.2190/PM.43.2.b
317(9):901-902. doi:10.1001/jama.2017.0076
372 JAMA Pediatrics April 2022 Volume 176, Number 4 (Reprinted) jamapediatrics.com
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Zwingly Christian Porajow on 04/05/2022
You might also like
- Therapist's Guide to Pediatric Affect and Behavior RegulationFrom EverandTherapist's Guide to Pediatric Affect and Behavior RegulationNo ratings yet
- Easy Reeding!-August 2009Document8 pagesEasy Reeding!-August 2009yara20No ratings yet
- SQL Queries Interview Questions and Answers - Query ExamplesDocument25 pagesSQL Queries Interview Questions and Answers - Query Examplesiveraj67% (9)
- Ralph Alan Dale 1972 Hypnotism and EducationDocument21 pagesRalph Alan Dale 1972 Hypnotism and EducationFrancis Gladstone-Quintuplet100% (2)
- Interpersonal Psychotherapy For Depressed Adolescents (IPT-A)Document8 pagesInterpersonal Psychotherapy For Depressed Adolescents (IPT-A)Wiwin Apsari WahyuniNo ratings yet
- Radhu's Recipes - 230310 - 180152 PDFDocument123 pagesRadhu's Recipes - 230310 - 180152 PDFl1a2v3 C4No ratings yet
- Jewelry 7000 Years An International History and Illustrated Survey From The Collections of The - Hugh Tait - May 1991 - Abradale Books - 9780810981034 - Anna's ArchiveDocument264 pagesJewelry 7000 Years An International History and Illustrated Survey From The Collections of The - Hugh Tait - May 1991 - Abradale Books - 9780810981034 - Anna's Archiveeve100% (2)
- The Entheogen Review׃ Vol. 16, No. 1 (2008)Document44 pagesThe Entheogen Review׃ Vol. 16, No. 1 (2008)HoorayFrisbeeHead100% (2)
- Synopsis MSNDocument23 pagesSynopsis MSNSaurabh MNo ratings yet
- Logix 5000 Controllers Tasks, Programs, and RoutinesDocument73 pagesLogix 5000 Controllers Tasks, Programs, and Routinesobi SalamNo ratings yet
- Teaching Listening and Speaking in Second and Foreign Language Contexts (Kathleen M. Bailey)Document226 pagesTeaching Listening and Speaking in Second and Foreign Language Contexts (Kathleen M. Bailey)iamhsuv100% (1)
- Mind Magic: Building a Foundation for Emotional Well-BeingFrom EverandMind Magic: Building a Foundation for Emotional Well-BeingNo ratings yet
- Effectiveness of Mindfulness Intervention in Reducing Stress and Burnout For Mental Health Professionals in SingaporeDocument26 pagesEffectiveness of Mindfulness Intervention in Reducing Stress and Burnout For Mental Health Professionals in SingaporeMuqaddas GhoriNo ratings yet
- Addicted1 - The Inquietude of YouthDocument867 pagesAddicted1 - The Inquietude of YouthIlsa Krisdwiyani100% (1)
- Stress Management in Medical Education A Review.23Document12 pagesStress Management in Medical Education A Review.23Kaycee100% (1)
- Rod and Pump DataDocument11 pagesRod and Pump DataYoandri Stefania Guerrero CamargoNo ratings yet
- Integrative ReviewDocument20 pagesIntegrative Reviewapi-485309887No ratings yet
- University of Tennessee Religious ExemptionDocument3 pagesUniversity of Tennessee Religious ExemptionDonnaNo ratings yet
- OVERVIEWDocument16 pagesOVERVIEWjae eNo ratings yet
- 2022-Ayub Med ExploringcopingstrspdfDocument6 pages2022-Ayub Med ExploringcopingstrspdfDr. Sajida NaseemNo ratings yet
- NguyenaDocument12 pagesNguyenaapi-699842071No ratings yet
- Effect of A Brief Mindfulness-Based Program On Stress in Health Care ProfessionalsDocument12 pagesEffect of A Brief Mindfulness-Based Program On Stress in Health Care ProfessionalsrajeshskNo ratings yet
- A Systematic Review of Prevention Programs Targeting Depression, Anxiety, and Stress in University StudentsDocument17 pagesA Systematic Review of Prevention Programs Targeting Depression, Anxiety, and Stress in University StudentsMacarena PalauNo ratings yet
- A Mindfulness Workshop For Health Science Graduate StudentsDocument8 pagesA Mindfulness Workshop For Health Science Graduate StudentsAnnette WillgensNo ratings yet
- Running Head: Nurse BurnoutDocument11 pagesRunning Head: Nurse BurnoutPaul MumoNo ratings yet
- Burnout in Pediatric ResidentsDocument5 pagesBurnout in Pediatric Residentslina7soteroNo ratings yet
- Video-Delivered Relaxation Intervention Reduces Late-Life Anxiety: A Pilot Randomized Controlled TrialDocument12 pagesVideo-Delivered Relaxation Intervention Reduces Late-Life Anxiety: A Pilot Randomized Controlled TrialMega Agustin CahyandariNo ratings yet
- Reducing Stress and Burnout in Junior Doctors: The Impact of Debriefing SessionsDocument22 pagesReducing Stress and Burnout in Junior Doctors: The Impact of Debriefing SessionsMinodora MilenaNo ratings yet
- The Effects On The Level of Mental Stability of Nurses at Camp Crame General HospitalDocument11 pagesThe Effects On The Level of Mental Stability of Nurses at Camp Crame General HospitalGaea Atheena Dela CruzNo ratings yet
- Jama 2009 1384Document10 pagesJama 2009 1384Katherine ChicasNo ratings yet
- Nurs702 Critique Final2Document9 pagesNurs702 Critique Final2natalie nodayNo ratings yet
- The Relationship Between Spirituality and Burnout Among Medical StudentsDocument16 pagesThe Relationship Between Spirituality and Burnout Among Medical StudentsChristiana TomescuNo ratings yet
- NURS702 Critique 2Document9 pagesNURS702 Critique 2natalie nodayNo ratings yet
- File 1Document4 pagesFile 1fitri dewi maharaniNo ratings yet
- Bluth Journal of Adolescence - 2023 - Bluth - Feasibility Acceptability and Depression Outcomes of A Randomized ControlledDocument15 pagesBluth Journal of Adolescence - 2023 - Bluth - Feasibility Acceptability and Depression Outcomes of A Randomized ControlledĐan TâmNo ratings yet
- Literature Review On Nurse BurnoutDocument5 pagesLiterature Review On Nurse Burnouteyewhyvkg100% (1)
- 1 s2.0 S1550830716301616 MainDocument20 pages1 s2.0 S1550830716301616 MainnataliaNo ratings yet
- Am J Crit Care-2015-Rushton-412-20 PDFDocument11 pagesAm J Crit Care-2015-Rushton-412-20 PDFOwais ZiaNo ratings yet
- Annotated Bibliography and ReflectionDocument5 pagesAnnotated Bibliography and ReflectionwacraellaNo ratings yet
- Jurnal 1Document7 pagesJurnal 1enunzNo ratings yet
- Cultivating Mindfulness in Health Care Professionals - A Review of Empirical Studies of Mindfulness-Based Stress Reduction (MBSR)Document6 pagesCultivating Mindfulness in Health Care Professionals - A Review of Empirical Studies of Mindfulness-Based Stress Reduction (MBSR)rahul gajbhiyeNo ratings yet
- Yoga Intervention - Mccall2017Document2 pagesYoga Intervention - Mccall2017DavidNo ratings yet
- MBSR Training For AdolescentsDocument17 pagesMBSR Training For AdolescentsEmmanuel Raphael SanturayNo ratings yet
- Final Ebp Holistic Approached and Nursing Burnout v1Document14 pagesFinal Ebp Holistic Approached and Nursing Burnout v1api-620262107No ratings yet
- Jamapsychiatry Buckman 2022 Oi 220004 1651602243.58743Document11 pagesJamapsychiatry Buckman 2022 Oi 220004 1651602243.58743vedavathiNo ratings yet
- Efectiveness of SFBC Full ArticlesDocument21 pagesEfectiveness of SFBC Full Articlesgopi krishna ranjanNo ratings yet
- Running Head: Nurse BurnoutDocument10 pagesRunning Head: Nurse BurnoutPaul MumoNo ratings yet
- 2019 Article 2503Document8 pages2019 Article 2503Frida RasyidNo ratings yet
- 30 EffectivenessofthestructuredteachingprogramonknowledgeofpostnataldepressionDocument6 pages30 EffectivenessofthestructuredteachingprogramonknowledgeofpostnataldepressionDrPreeti Thakur ChouhanNo ratings yet
- Evans Et Al-2017-Journal of Advanced NursingDocument41 pagesEvans Et Al-2017-Journal of Advanced NursingBides RebornNo ratings yet
- Journal ClubDocument20 pagesJournal Clubapi-379570200No ratings yet
- Running Head: Compassion Fatigue in Nursing 1Document11 pagesRunning Head: Compassion Fatigue in Nursing 1api-489685873No ratings yet
- Mindfulness-Based Stress Reduction and Health Benefits A Meta-AnalysisDocument9 pagesMindfulness-Based Stress Reduction and Health Benefits A Meta-AnalysisVladNo ratings yet
- Ijerph 19 00649 v2Document18 pagesIjerph 19 00649 v2Odessa Fernandez DysangcoNo ratings yet
- Designing A Resilience Program For Critical Care NursesDocument8 pagesDesigning A Resilience Program For Critical Care NursesgabbbbbyNo ratings yet
- Hojat 2004Document8 pagesHojat 2004Jair Benavente AsinNo ratings yet
- Jessica Article Critique NotesDocument6 pagesJessica Article Critique NotesJessicaNo ratings yet
- BATARA Assignment Related Assignment From Activity 1 2Document5 pagesBATARA Assignment Related Assignment From Activity 1 2Trisha Anne BataraNo ratings yet
- Problem-Based ResearchDocument8 pagesProblem-Based Researchapi-480618512No ratings yet
- 9 - Efficacy of Psychosocial InterventionsDocument18 pages9 - Efficacy of Psychosocial Interventionskhan.larissaNo ratings yet
- Effectiveness of Aerobic Exercises On StressDocument20 pagesEffectiveness of Aerobic Exercises On StressRegina EstherNo ratings yet
- Prevalence and Predictors of Anxiety in Healthcare Professions StudentsDocument10 pagesPrevalence and Predictors of Anxiety in Healthcare Professions StudentsMihaela PanaitNo ratings yet
- The Impact of Burnout On Medical StudentsDocument3 pagesThe Impact of Burnout On Medical StudentsJulie Ann BagamaspadNo ratings yet
- Emotional Intelligence and Fieldwork SuccessDocument27 pagesEmotional Intelligence and Fieldwork Successilove linuxNo ratings yet
- Implementation of Perinatal Collaborative Care A Health Services Approach To Perinatal Depression CareDocument9 pagesImplementation of Perinatal Collaborative Care A Health Services Approach To Perinatal Depression CaresalamahNo ratings yet
- Jamapsychiatry Buckman 2022 Oi 220004 1646792725.75755Document11 pagesJamapsychiatry Buckman 2022 Oi 220004 1646792725.75755SabrinaNo ratings yet
- Effectiveness of Psychoeducation For Relapse, Symptoms, Knowledge, Adherence and Functioning in Psychotic Disorders: A Meta-AnalysisDocument14 pagesEffectiveness of Psychoeducation For Relapse, Symptoms, Knowledge, Adherence and Functioning in Psychotic Disorders: A Meta-AnalysisPatty IzquierdoNo ratings yet
- Annotated BibliographyDocument8 pagesAnnotated BibliographyEunice AppiahNo ratings yet
- Aet2 10354Document8 pagesAet2 10354Edris ZamroniNo ratings yet
- Your Examination for Stress & Trauma Questions You Should Ask Your 32nd Psychiatric Consultation William R. Yee M.D., J.D., Copyright Applied for May 31st, 2022From EverandYour Examination for Stress & Trauma Questions You Should Ask Your 32nd Psychiatric Consultation William R. Yee M.D., J.D., Copyright Applied for May 31st, 2022No ratings yet
- Children of Divorced Parents: Assertiveness Training and Cognitive Restructuring Techniques in Increasing Self-Esteem of Female Adolescents from Divorced HomesFrom EverandChildren of Divorced Parents: Assertiveness Training and Cognitive Restructuring Techniques in Increasing Self-Esteem of Female Adolescents from Divorced HomesNo ratings yet
- Practical Treatment Options for Chronic Pain in Children and Adolescents: An Interdisciplinary Therapy ManualFrom EverandPractical Treatment Options for Chronic Pain in Children and Adolescents: An Interdisciplinary Therapy ManualNo ratings yet
- [1479683X - European Journal of Endocrinology] How important is obesity as a risk factor for respiratory failure, intensive care admission and death in hospitalised COVID-19 patients_ Results from a single Italian cDocument9 pages[1479683X - European Journal of Endocrinology] How important is obesity as a risk factor for respiratory failure, intensive care admission and death in hospitalised COVID-19 patients_ Results from a single Italian cLuke EishenhowerNo ratings yet
- Systems Science For Developing Policy To Improve Physical Activity, The CaribbeanDocument8 pagesSystems Science For Developing Policy To Improve Physical Activity, The CaribbeanLuke EishenhowerNo ratings yet
- BLT 19 247874Document8 pagesBLT 19 247874Luke EishenhowerNo ratings yet
- Improvements To A Framework For Gender and Emerging InfectiousDocument3 pagesImprovements To A Framework For Gender and Emerging InfectiousLuke EishenhowerNo ratings yet
- Geologic Report Arches NationalDocument9 pagesGeologic Report Arches NationalJacob AndersonNo ratings yet
- Pps Overview BrochureDocument15 pagesPps Overview BrochureizzybjNo ratings yet
- Children With Cochlear Implants The Communication JourneeyDocument22 pagesChildren With Cochlear Implants The Communication Journeeyismail39No ratings yet
- Analogy - 10 Page - 01 PDFDocument10 pagesAnalogy - 10 Page - 01 PDFrifathasan13No ratings yet
- Penjelasan IMRAD StructureDocument2 pagesPenjelasan IMRAD Structureaji bondesNo ratings yet
- Have To, Has To, Had To - Exercise 1 - Worksheet English GrammarDocument1 pageHave To, Has To, Had To - Exercise 1 - Worksheet English Grammarjonni jonsonNo ratings yet
- Usability Test Report MemoDocument2 pagesUsability Test Report MemoTiffany PetersonNo ratings yet
- Pyneng Readthedocs Io en LatestDocument702 pagesPyneng Readthedocs Io en LatestNgọc Duy VõNo ratings yet
- Tpa6404 q1Document12 pagesTpa6404 q1siogNo ratings yet
- 1.1.DeFacto Academy enDocument7 pages1.1.DeFacto Academy enYahya AçafNo ratings yet
- Pms 500 - International Mechanics KitDocument0 pagesPms 500 - International Mechanics KitArsul RNo ratings yet
- PGCC 2022 HandbookDocument17 pagesPGCC 2022 HandbookhasnainNo ratings yet
- Heat Transfer Fluid O&MDocument14 pagesHeat Transfer Fluid O&MOcto Adhi W PryhantoNo ratings yet
- Chapter 3 - Instructional PlanningDocument30 pagesChapter 3 - Instructional PlanningMadelyne BenitezNo ratings yet
- IPS e El 110Document105 pagesIPS e El 110alinaghibNo ratings yet
- HET Neoclassical School, MarshallDocument26 pagesHET Neoclassical School, MarshallDogusNo ratings yet
- Bourbon Explorer 500 Series Commercial LeafletDocument6 pagesBourbon Explorer 500 Series Commercial LeafletDaniel ZhangNo ratings yet
- Math Achievement Gr11GenMathDocument3 pagesMath Achievement Gr11GenMathMsloudy VilloNo ratings yet






































































![[1479683X - European Journal of Endocrinology] How important is obesity as a risk factor for respiratory failure, intensive care admission and death in hospitalised COVID-19 patients_ Results from a single Italian c](https://imgv2-1-f.scribdassets.com/img/document/611186342/149x198/c6f04b8508/1710559969?v=1)




















