Professional Documents
Culture Documents
7pelvic Cavity
Uploaded by
Dan Mupenzi0 ratings0% found this document useful (0 votes)
11 views71 pagesanatomy on pelvis
Original Title
7Pelvic cavity
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentanatomy on pelvis
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
11 views71 pages7pelvic Cavity
Uploaded by
Dan Mupenzianatomy on pelvis
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 71
Pelvic Cavity
Prof. Julien GASHEGU
The Pelvis
The pelvis is divided into two regions:
The false pelvis (greater pelvis)→ part of the abdomen .
The true pelvis (lesser pelvis) → has an inlet and an
outlet.
The pelvic cavity enclosed by the true pelvis consists of
the pelvic inlet, walls, and floor.
1/8/2023
Bones of the pelvis
The bony pelvis is composed by:
1. 2 hip bones: described in detail in Gross
Anatomy I module.
- Students are advised to recall that gained
knowledge
2. sacrum and coccyx : same as above
1/8/2023
Joints and ligaments of the pelvis
Joints of pelvis include:
a. symphysis pubis between the 2 pubic bones
b. sacro-iliac joints: between the auricular surfaces of
sacrum and ilium + syndesmose between sacral
tuberosity and iliac tuberosity
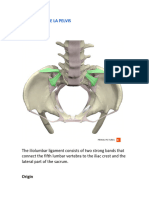
Main ligaments of the pelvis are:
a. sacrotuberous ligaments
b. sacrospinous ligaments
c. inguinal ligament
* The 2 ligaments define with the posterior border of hip
bone
- greater sciatic foramen and lesser sciatic foramen
* The inguinal ligament define with the anterior border of hip
bone the subinguinal space
1/8/2023
1/8/2023
Functions of the pelvis girdle
◼ Protect pelvic viscera
◼ Support weight of body and transmit it to lower
limbs
◼ Facilitate the walking movement by swinging
side to side during walk
◼ Provide attachment to muscles
◼ In female, provide bony support of birth canal
◼ Anchors the roots of the external genitalia
The pelvic inlet
◼ Heart shaped and completely ringed by bone.
◼ Posteriorly bordered by the sacral promontory
and the alae (wings) of the sacrum
◼ Laterally, a prominent rim on the pelvic bone
continues the boundary of the inlet forward to
the pubic symphysis.
1/8/2023
The Pelvic outlet
◼ The diamond-shaped
◼ Formed by both bone and ligaments.
◼ Limited anteriorly by the pubic symphysis.
◼ On each side, the pubic arch (the ischiopubic ramus)
and ischial tuberosity → margin of the anterior
half
◼ The sacrotuberous ligament continues this margin
posteriorly from the ischial tuberosity to the coccyx and
sacrum.
The pelvic diameters
The pelvic walls and floor
◼ Bones,
◼ sacrum,
◼ coccyx,
◼ inferior half of the pelvic bones
◼ Muscles
◼ obturator internus
◼ piriformis muscles
◼ Ligaments converting the greater and lesser
sciatic notches into foraminae.
◼ sacrospinous ligament
◼ sacrotuberous ligament.
Antero-inferior pelvic wall
The antero-inferior pelvic wall is formed by
bones only:
- bodies of pubic bones
- rami of pubic bones
- pubic symphysis
It support the urinary bladder
Lateral pelvic walls
* the lateral pelvic walls are formed by the
right and left hip bones
* each hip bone includes the obturator
foramen that is closed by the obturator
membrane
* the obturator internus muscle is the muscle
of lateral wall and is covered by the
obturator fascia
* the obturator fascia is thickened centrally
to form the tendinous arch that provides
attachment to pelvic diaphragm
Posterio-lateral wall and Roof
* the posterio-superior wall is formed by:
- sacrum and coccyx
- sacroiliac, sacrotuberous and sacrospinous
ligaments
- piriformis muscles
The pelvic floor
◼ Formed by the pelvic diaphragm
◼ The attachment of the pelvic diaphragm to the
tendinous arch divides the obturator internus muscles
into a superior or pelvic part and an inferior or
perineal part
◼ The pelvic diaphragm consists of the coccygeus and
levator ani muscles and fasciae
◼ Coccygeus muscles arise on lateral side of the
inferior sacrum and coccyx and attach on the
sacrospinous ligaments
1/8/2023
The pelvic floor
◼ Levator ani muscles is larger and most important
part of the pelvic floor. It stretches between anterior,
lateral and posterior walls of pelvis.
◼ Levator ani muscles limit an anterior gap: the urogenital
hiatus for passage of the urethra and in female the
vagina
◼ Levator ani muscle consists of 3 parts:
1. puborectalis: thicker, narrower, medial part of
levator ani. It forms a U-shaped muscular ring that
pass posterior to the anorectal junction, bounding the
urogenital hiatus. It plays a role in fecal continence
The pelvic floor
◼ Levator ani muscle consists of 3 parts:
2. pubococcygeus: wider and thinner intermediate part
of the levator ani. It arises for the body of pubis and
tendinous arch and attaches on the coccyx;
◼ Shorter muscular slips of the pubococcgeus extend middle to
attach on midline stuctures forming pubovaginalis,
puboprostaticus, puboperinealis, puboanalis muscles
◼ 3. iliococcygeus: posterolateral part on the levator ani. It
arises from the tendinous arch and ischial tuberosity to attach
on the coccyx
◼ The pelvic diaphragm supports abdominopelvic viscera and
plays a role in urinary and fecal continence
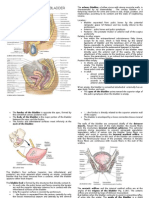
Pelvic cavity
◼ The peritoneum drapes over the superior aspects of
the pelvic viscera.
◼ The pelvic viscera located in the midline of the pelvic
cavity.
◼ The bladder is anterior and the rectum is posterior. In
women, the uterus between the bladder and rectum.
◼ The reflexion of peritoneum of pelvic viscera
explain the pelvic fossa or pouches: supra-vesical
fossa, recto-vesical pouch, vesico-uterine pouch,
rectouterine pouch = cul-de-sac of Douglas
◼ Vessels and nerves, lie deep to the peritoneum in
association with the pelvic walls
Pelvic fasciae
◼ The pelvic fascia is connective tissue that occupies space
between the peritoneum and muscular pelvic walls and floor.
◼ Pelvic fascia consists of membranous pelvic fascia and
endopelvic fascia.
◼ Membranous pelvic fascia consists of visceral pelvic fascia that
covers pelvic viscera (adventitia) and parietal pelvic fascia
covering muscles of pelvic walls and floor. The parietal fascia
is thicker where pelvic viscera enter the floor to form
tendinous arch of pelvis
◼ Endopelvic fascia is the term given to the loose connective tissue
between parietal and visceral pelvic fascia.
◼ The loose tissue is site of potential space: retro-pubic and
retro-rectal spaces
Pelvic fasciae: hypogastric sheath
The endopelvic fascia is condensed into hypogastric sheath for
passage of vessels and nerve and fascial ligaments which act as
supports for pelvic viscera.
These ligaments include the:
◼Cardinal (Mackenrodt’s) ligaments: pass laterally from the
cervix and upper vagina to the pelvic side walls.
◼Utero-sacral ligaments: pass backwards from the cervix and
vaginal fornices to the fascia overlying the sacro-iliac joints.
◼Pubocervical ligaments: extend anteriorly from the cardinal
ligaments to the pubis (puboprostatic in the male).
◼Pubovesical ligaments: from the back of the symphysis
pubis to the bladder neck
PELVIC NERVES
◼ Somatic nerves from sacral and coccygeal plexuses:
see Gross Anatomy I module
◼ Pelvic autonomous nerves have 4 routes:
◼ 1. sacral sympathetic ganglia and trunks: each has 4
sacral ganglia and the 2 end by ganglion impar. They
send branches to the inferior pelvic plexus
◼ 2. peri-arterial plexuses: sympathetic fibers around
arteries in the pelvis
◼ 3. hypogastric plexuses: superior and inferior pelvic
plexuses
PELVIC NERVES
◼ 3. hypogastric plexuses: superior and inferior pelvic plexuses
- the superior hypogastric plexus (sympathetic) gives the right
and left hypogastric nerves that contribute to form the inferior
hypogastric plexus
- the inferior hypogastric plexuses (sympathetic and
parasympathetic)
◼ 4. pelvic splanchnic nerves: arise from the anterior rami of S2-
S4 and contain parasympathetic fibers that contribute to form
the inferior hypogastric plexuses
◼ Around viscera there are pelvic plexuses from the inferior
hypogastric plexuses
Pelvic Blood vessels
Arterial blood supply
◼Internal Iliac artery has 2 divisions
•I. posterior division that gives rise to 3 branches:
- iliolumbar artery ascends to give an iliac branch and a
lumbar branch
- lateral sacral artery supplies sacral meninges and
anterior sacral rami
- superior gluteal artery, the largest branch of the
posterior division that passes in the greater sciatic
foreman to supply the gluteal region
•2. anterior division:
Pelvic Blood vessels
◼Internal Iliac artery has 2 divisions:
•II. anterior division gives branches that are mainly visceral:
1. umbilical artery: its distal part is occluded and become the medial
inguinal ligament, its proximal part is the superior vesical artery
2. obturator artery
3. Inferior vesical artery in male is replaced by Vaginal artery in female
4. Uterine artery in female
5. Middle rectal artery
6. Internal pudendal artery
7. inferior gluteal artery
◼Median sacral artery from abdominal aorta
◼Ovarian or testicular arteries from abdominal aorta
1/8/2023
The Pelvic veins
◼ Pelvic veins follow the course of all branches of
the internal iliac artery except for the umbilical
artery, its branch the superior vesical artery and
the iliolumbar artery.
◼ On each side, the veins drain into internal iliac
veins, which leave the pelvic cavity to join
common iliac veins.
Lymphatics
◼ Lymph nodes distributed along the internal iliac
and external iliac arteries and their associated
branches →nodes associated with the common
iliac arteries → nodes associated with the lateral
surfaces of the abdominal aorta → the lumbar
trunks →the thoracic duct
You might also like
- GRDA Intro Bony PelvisDocument5 pagesGRDA Intro Bony PelvisKingNo ratings yet
- Gluteal RegionDocument66 pagesGluteal Regionashley nicholeNo ratings yet
- Anat 5.2 Pelvis and Perineum - ElevazoDocument14 pagesAnat 5.2 Pelvis and Perineum - Elevazolovelots1234No ratings yet
- Elte SGD b8 GenitalDocument4 pagesElte SGD b8 GenitalGWKNANDANo ratings yet
- PelvisDocument35 pagesPelvisAdan ImanNo ratings yet
- Bony Pelvis, Pelvic Walls, and Pelvic Measurements Text - PDocument0 pagesBony Pelvis, Pelvic Walls, and Pelvic Measurements Text - PShouq Khair AllaNo ratings yet
- Joints of The Lower LimbDocument63 pagesJoints of The Lower LimbEliud MbuteNo ratings yet
- Review of Anatomy and Physiology of Human ReproductiveDocument68 pagesReview of Anatomy and Physiology of Human Reproductivesavita hanamsagarNo ratings yet
- 1 Introduction To The Pelvis and The Pelvic Peritoneum DIYADocument38 pages1 Introduction To The Pelvis and The Pelvic Peritoneum DIYAOmotosho DavidNo ratings yet
- Abdominal Wall and HerniaDocument35 pagesAbdominal Wall and HerniaMohammad BanisalmanNo ratings yet
- Anatomia TrabajoDocument60 pagesAnatomia TrabajoFelipe Domínguez FigueroaNo ratings yet
- Pelvic WallDocument56 pagesPelvic WallYousef El bannaNo ratings yet
- Pelvic Diaphragm & Pelvic FasciaDocument22 pagesPelvic Diaphragm & Pelvic Fasciafarwafurqan1No ratings yet
- Worku Antomy and Physiology of Reproductive OrganDocument206 pagesWorku Antomy and Physiology of Reproductive OrganMignot AnileyNo ratings yet
- Maternal Anatomy WilliamsDocument60 pagesMaternal Anatomy WilliamsZari Novela100% (2)
- Pelvic FractureDocument22 pagesPelvic FractureAgeng BudianantiNo ratings yet
- CBL 2Document20 pagesCBL 2Hammad AkramNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument36 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreabctutorNo ratings yet
- Bony Pelvis and Pelvic FloorDocument73 pagesBony Pelvis and Pelvic Floormamai elijahNo ratings yet
- Pelvic Wall-Cont.: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistDocument39 pagesPelvic Wall-Cont.: Dr:Ahmed Ibrahim Abdi (Nawawi) AnatomistSAKARIYE MAXAMEDNo ratings yet
- Abdomen#2: DR - Bushra Haseeb BDS, Rds Demonstrator in The Dental Section, Azra Naheed Medical CollegeDocument15 pagesAbdomen#2: DR - Bushra Haseeb BDS, Rds Demonstrator in The Dental Section, Azra Naheed Medical CollegeTanveer AhmadNo ratings yet
- Last's Anatomy - Pelvis Annotated Question BankDocument90 pagesLast's Anatomy - Pelvis Annotated Question BankHarriott MaixnerNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument36 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreabctutorNo ratings yet
- Online Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreDocument36 pagesOnline Practice Tests, Live Classes, Tutoring, Study Guides Q&A, Premium Content and MoreYoAmoNYCNo ratings yet
- Anatomy 1Document17 pagesAnatomy 1Uljana NasonovaNo ratings yet
- Lower LimbpostgDocument79 pagesLower LimbpostgBuya kasahunNo ratings yet
- Pelvic and PerineumDocument20 pagesPelvic and PerineumRahaf MajadlyNo ratings yet
- Gross Anatomy of The Pelvis & Perineum DR Ogedengbe O.ODocument162 pagesGross Anatomy of The Pelvis & Perineum DR Ogedengbe O.OKolawole Adesina KehindeNo ratings yet
- ÇÇÇÇÇÇÇÇÇÇDocument18 pagesÇÇÇÇÇÇÇÇÇÇsostegnawNo ratings yet
- Anatomy of The Female Reproductive SystemDocument62 pagesAnatomy of The Female Reproductive SystemBibek GajmerNo ratings yet
- Anterior Abdominal WallDocument108 pagesAnterior Abdominal WallMunikrishna Salavakam100% (1)
- Maternal Anatomy WilliamsDocument52 pagesMaternal Anatomy WilliamsMariane Tejano100% (1)
- PELVIS AND PERINEUM Session 4 - 2022Document53 pagesPELVIS AND PERINEUM Session 4 - 2022zealotwisdom0No ratings yet
- Pelvic Cavity PDFDocument10 pagesPelvic Cavity PDFRigor MortisNo ratings yet
- 4 - Anatomy of PelvisDocument10 pages4 - Anatomy of PelvisJISHNU TKNo ratings yet
- Anatomy of The Female PelvisDocument60 pagesAnatomy of The Female PelvisMignot AnileyNo ratings yet
- Anatomy Research Paper PelvisDocument4 pagesAnatomy Research Paper PelvisBasil AdeelNo ratings yet
- Gross Anatomy: Abdomen 4 Kidneys, Ureter and Urinary BladderDocument74 pagesGross Anatomy: Abdomen 4 Kidneys, Ureter and Urinary BladderBibek GajmerNo ratings yet
- Maternal Pelvis Fetal Skull PDFDocument13 pagesMaternal Pelvis Fetal Skull PDFAnuradha Maurya100% (2)
- Urinary BladderDocument35 pagesUrinary Bladderfabunmiopeyemiv23No ratings yet
- Anterior Posterior: o Posterior Renal Fascia Is Also Known As Zuckerkandl's Fascia)Document4 pagesAnterior Posterior: o Posterior Renal Fascia Is Also Known As Zuckerkandl's Fascia)Lester AldridgeNo ratings yet
- AnatomyDocument74 pagesAnatomyhafeez khanNo ratings yet
- Introduction To Lower Limb, Adaptation and Function 3 PDFDocument18 pagesIntroduction To Lower Limb, Adaptation and Function 3 PDFosunmuyiwaaNo ratings yet
- Anatomy of Urinary BladderDocument5 pagesAnatomy of Urinary BladderyolandadwiooNo ratings yet
- The Kidneys (Nephros) : FunctionsDocument6 pagesThe Kidneys (Nephros) : FunctionsOjambo FlaviaNo ratings yet
- Anatomy of The Female Pelvis FinalDocument209 pagesAnatomy of The Female Pelvis FinalMignot Aniley86% (14)
- Anterolateral Abdominal Wall and Reg2Document70 pagesAnterolateral Abdominal Wall and Reg2saint thuggerNo ratings yet
- Anterior Abdominal WallDocument47 pagesAnterior Abdominal WallJohn NgumbiNo ratings yet
- The PerineumDocument3 pagesThe PerineumSanjay KishoreNo ratings yet
- Skeletal System Notes 2023Document16 pagesSkeletal System Notes 2023shinamaejNo ratings yet
- Knee JointDocument49 pagesKnee JointRiaz SialNo ratings yet
- 2-Pelvic Walls, Joints, Vessels & NervesDocument32 pages2-Pelvic Walls, Joints, Vessels & NervesAbdul Rafay ShaikhNo ratings yet
- 6 Lower LimbDocument19 pages6 Lower LimbMOHAMMED BIN BAREKNo ratings yet
- Anterior Abdominal WallDocument10 pagesAnterior Abdominal WallZhy CatliNo ratings yet
- Perineum AnatomyDocument23 pagesPerineum Anatomyrohitrohillapalwal999No ratings yet
- Final Obstetrics and GynacologyDocument88 pagesFinal Obstetrics and Gynacologysis8100% (2)
- Subjects: - Introduction - Pelvic Girdle - Pelvic CavityDocument39 pagesSubjects: - Introduction - Pelvic Girdle - Pelvic CavityAshraf SidrahNo ratings yet
- A Simple Guide to the Voice Box and Its Disorders, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to the Voice Box and Its Disorders, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Anatomy QBank Volume Two ThoraxDocument57 pagesAnatomy QBank Volume Two ThoraxDan Mupenzi100% (1)
- 9 PerineumDocument67 pages9 PerineumDan MupenziNo ratings yet
- Ucalgary 2012 Adams CourtenayDocument153 pagesUcalgary 2012 Adams CourtenayDan MupenziNo ratings yet
- Handbook 2008Document48 pagesHandbook 2008Dan MupenziNo ratings yet
- Fbla Scavenger Hunt 1Document3 pagesFbla Scavenger Hunt 1api-472648158No ratings yet
- Applied Computational AerodynamicsDocument15 pagesApplied Computational AerodynamicsjoereisNo ratings yet
- Autodesk Design Review: About DWF and DWFXDocument7 pagesAutodesk Design Review: About DWF and DWFXNesreNo ratings yet
- Construction of Perimeter Fence of BFP NHQ PDFDocument133 pagesConstruction of Perimeter Fence of BFP NHQ PDFYalla ChaitanyaNo ratings yet
- Review of Related Literature and Related StudiesDocument23 pagesReview of Related Literature and Related StudiesReynhard Dale100% (3)
- Grade 7 First Quarter ExamDocument3 pagesGrade 7 First Quarter ExamBILLY JOE ARELLANONo ratings yet
- EHR StandardsIndia - August 2013-32630521Document54 pagesEHR StandardsIndia - August 2013-32630521kartiksinhNo ratings yet
- Components of Vectors Prepared By: Victor Rea OribeDocument17 pagesComponents of Vectors Prepared By: Victor Rea OribeGerone Tolentino AtienzaNo ratings yet
- HBS - Zara Fast Fashion Case Write UpDocument4 pagesHBS - Zara Fast Fashion Case Write Upaaronhwalton100% (1)
- Epidemiological Triad of HIV/AIDS: AgentDocument8 pagesEpidemiological Triad of HIV/AIDS: AgentRakib HossainNo ratings yet
- TEFL Entrance ExamDocument3 pagesTEFL Entrance ExammerekNo ratings yet
- 1evolution of O and M TheoryDocument27 pages1evolution of O and M TheoryTracy AdraNo ratings yet
- H I Ôn Thi Aptis & Vstep - Tài Liệu - Anna MaiDocument4 pagesH I Ôn Thi Aptis & Vstep - Tài Liệu - Anna Maihanh.mt2022No ratings yet
- Review Problems On Gas TurbineDocument9 pagesReview Problems On Gas TurbinejehadyamNo ratings yet
- Cambridge IGCSE Physics 0625 Complete Notes PDocument5 pagesCambridge IGCSE Physics 0625 Complete Notes PYamikani ManthandoNo ratings yet
- Bill - AKIJDocument3 pagesBill - AKIJm.tanjil2005No ratings yet
- Quizlet Table 7Document1 pageQuizlet Table 7JosielynNo ratings yet
- Content Analysis of Tea BrandsDocument49 pagesContent Analysis of Tea BrandsHumaRiaz100% (1)
- Writing Short StoriesDocument10 pagesWriting Short StoriesRodiatun YooNo ratings yet
- Federal Government Employees Housing FoundationDocument2 pagesFederal Government Employees Housing FoundationMuhammad Shakil JanNo ratings yet
- MELASMA (Ardy, Kintan, Fransisca)Document20 pagesMELASMA (Ardy, Kintan, Fransisca)Andi Firman MubarakNo ratings yet
- Electric Valve Actuator Type Car: For 2 & 3-Way Valves Type G/L/M/S 2Fm-T & G/L/M/S 3Fm-T Page 1 of 4 0-4.11.08-HDocument4 pagesElectric Valve Actuator Type Car: For 2 & 3-Way Valves Type G/L/M/S 2Fm-T & G/L/M/S 3Fm-T Page 1 of 4 0-4.11.08-HMuhd Khir RazaniNo ratings yet
- CA-idms Ads Alive User Guide 15.0Document142 pagesCA-idms Ads Alive User Guide 15.0svdonthaNo ratings yet
- Piezoelectric-Material Based Energy Harvesting Device.Document29 pagesPiezoelectric-Material Based Energy Harvesting Device.jobert100% (1)
- GCG Damri SurabayaDocument11 pagesGCG Damri SurabayaEndang SusilawatiNo ratings yet
- Job Sheet 1Document5 pagesJob Sheet 1Sue AzizNo ratings yet
- Misc Ar2019Document207 pagesMisc Ar2019Sharon12 ArulsamyNo ratings yet
- Maven MCQDocument55 pagesMaven MCQANNAPUREDDY ANIL KUMAR REDDY CSENo ratings yet
- Calculate Breakeven Point in Units and Revenue Dollars: Intermediate Cost Analysis and ManagementDocument52 pagesCalculate Breakeven Point in Units and Revenue Dollars: Intermediate Cost Analysis and ManagementNavice Kie100% (1)
- Al Multaqaa Presentation v2Document22 pagesAl Multaqaa Presentation v2Hasaan WaheedNo ratings yet