Professional Documents
Culture Documents
I&I
Uploaded by
Jdee X0 ratings0% found this document useful (0 votes)
30 views7 pagesCholecystitis is inflammation of the gallbladder that can be acute or chronic. It is usually caused by gallstones blocking the cystic duct. There are two main types of gallstones - cholesterol stones made of hardened cholesterol and pigment stones made of calcium and bilirubin. Ultrasound is often the first diagnostic test used to detect gallstones and inflammation in the gallbladder. Other tests like CT scans, HIDA scans, and cholangiograms may also be used to diagnose cholecystitis and evaluate any bile duct obstruction.
Original Description:
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCholecystitis is inflammation of the gallbladder that can be acute or chronic. It is usually caused by gallstones blocking the cystic duct. There are two main types of gallstones - cholesterol stones made of hardened cholesterol and pigment stones made of calcium and bilirubin. Ultrasound is often the first diagnostic test used to detect gallstones and inflammation in the gallbladder. Other tests like CT scans, HIDA scans, and cholangiograms may also be used to diagnose cholecystitis and evaluate any bile duct obstruction.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
30 views7 pagesI&I
Uploaded by
Jdee XCholecystitis is inflammation of the gallbladder that can be acute or chronic. It is usually caused by gallstones blocking the cystic duct. There are two main types of gallstones - cholesterol stones made of hardened cholesterol and pigment stones made of calcium and bilirubin. Ultrasound is often the first diagnostic test used to detect gallstones and inflammation in the gallbladder. Other tests like CT scans, HIDA scans, and cholangiograms may also be used to diagnose cholecystitis and evaluate any bile duct obstruction.
Copyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 7
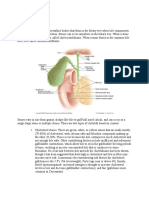
Cholecystitis 25% to 30% in women older than 50 years.
Cholelithiasis affects approximately 50% of
Inflammation of the gallbladder that may occur
women by the age of 70 years (Littlefield &
as an acute or chronic process
Lenahan, 2019).
Caused by gallstones results of hard particles
2. Chronic cholecystitis results when inefficient
that develop in the gallbladder.
bile emptying and gallbladder muscle wall
Gallstones develop because of an imbalance in disease cause a fibrotic and contracted
the chemical make-up of bile inside the gallbladder.
gallbladder.
Types 3. Acalculous cholecystitis occurs in the absence
of gallstones and is caused by bacterial invasion
1. Acute inflammation is associated with via the lymphatic or vascular system. Bacteria
gallstones (cholelithiasis). responsible are salmonella, Escherichia coli,
Cholethiasis is the presence of one or more Klebsiella species, and Streptococcus. It can
calculi or gallstones in the gallbladder, they also occur after major surgical procedures,
form from the solid constituent of bile and they orthopedic procedures, severe trauma, or
vary greatly in size, shape and composition. burns. Other factors associated with this type of
cholecystitis include torsion (twisting or
wrenching of the body by the exertion of
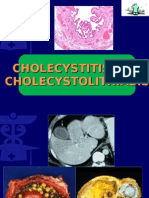
Examples of cholesterol gallstones (left) made forces), cystic duct obstruction, primary
up of a coalescence of multiple small stones and bacterial infections of the gallbladder, and
pigment gallstones (right) composed of calcium multiple blood transfusions. The usual finding of
bilirubinate. imaging studies is a distended acalculous
Level of cholesterol in bile becomes to high and gallbladder with thickened walls about 3-4mm
excess form into stones. Too much cholesterol, with or without pericholecystic fluid.
bilirubin, not enough bile salts. Bile salt hep Signs and Symptoms
with the digestion of fats.
1. Nausea and vomiting
Pigment stone associated with bacterial 2. Indigestion
infection or parasitic infestation of the biliary 3. Belching
system. Deconjugation of bilirubin. Consist of 4. Flatulence
calcium salts of bilirubin, phosphate carbonate 5. Epigastric pain that radiates to the scapula 2
(cholesterol stones are yellow-green and made to 4 hours after eating fatty foods and may
of hardened cholesterol while pigment stone persist for 4 to 6 hours
are dark in color and are made of bilirubin. 6. pain, tenderness, and rigidity of the upper
They are uncommon in children and young right abdomen that may radiate to the
adults but become more prevalent with midsternal area or right shoulder. pain of acute
increasing age. Women get gallstones more cholecystitis may be so severe that analgesic
often than men and more commonly after age medications are required. The use of morphine
40. It is estimated that the prevalence of has traditionally been avoided because of
gallstones ranges from 5% to 20% in women concern that it could cause spasm of the
between the ages of 20 and 55 years and from sphincter of Oddi. This is controversial,
because morphine is the preferred analgesic
agent for management of acute pain. Chemical reaction. Bile remaining in the
Furthermore, all opioids stimulate the gallbladder initiates a chemical reaction;
sphincter of Oddi to some degree. autolysis and edema occur.
7. Guarding – muscle spasm
Compression. Blood vessels in the gallbladder
8. Mass palpated in the right upper quadrant,
compressed, compromising its vascular supply
9. Murphy’s sign (cannot take a deep breath
when the examiner’s fingers are passed below Causes
the hepatic margin because of pain) Gallbladder stone. Cholecystitis is usually
10. Elevated temperature associated with gallstone impacted in the cystic
11. Tachycardia duct. There are two major types of gallstones:
12. Signs of dehydration those composed predominantly of pigment and
those composed primarily of cholesterol.
For Biliary obstruction Pigment stones probably form when
1. Jaundice, occurs in a few patients with unconjugated pigments in the bile precipitate to
gallbladder disease, usually with obstruction of form stones. Cholesterol, which is a normal
the common bile duct. The bile, which is no constituent of bile, is insoluble in water. Its
longer carried to the duodenum, is absorbed by solubility depends on bile acids and lecithin
the blood and gives the skin and mucous (phospholipids) in bile. In gallstone prone
membranes a yellow color. This is frequently patients, there is decreased bile acid synthesis
accompanied by marked pruritus (itching) of the and increased cholesterol synthesis in the liver,
skin. resulting in bile supersaturated with
2. Dark orange and foamy urine, The excretion cholesterol, which recipitates out of the bile to
of the bile pigments by the kidneys gives the form stones.
urine a very dark color. Bacteria. Bacteria plays a minor role in
3. Steatorrhea and clay-colored feces, as it is no cholecystitis; however, secondary infection of
longer colored with bile pigment. bile occurs in approximately 50% of cases. The
4. Pruritus, due to jaundice organisms involved are generally enteric
PATHOPHYSIOLOGY (normally live in the GI tract) and include
Escherichia coli, Klebsiella species, and
Calculous and acalculous cholecystitis have Streptococcus. Bacterial contamination is not
different origins. believed to stimulate the actual onset of acute
cholecystitis
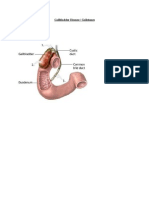
Calculous – develop when the main opening to
the gallbladder called the cystic duct gets Alterations in fluids and electrolytes.
blocked by a gallstone Acalculous cholecystitis is speculated to be
caused by alterations in fluids and electrolytes.
Acalculous – severe trauma, surgery, anorexia
that causes the bile to become stagnant Bile stasis. Bile stasis or the lack of gallbladder
contraction also play a role in the
Obstruction. Calculous cholecystitis occurs
development of cholecystitis.
when a gallbladder stone obstructs the bile
outflow.
Diagnostic procedures cholecystitis because patient is too ill to take
the dye by mouth.
Biliary ultrasound: Reveals calculi, with
gallbladder and/or bile duct distension Nonnuclear CT scan: May reveal gallbladder
(frequently the initial diagnostic procedure). cysts, dilation of bile ducts, and distinguish
between obstructive/nonobstructive jaundice.
Oral cholecystography (OCG): Preferred
method of visualizing general appearance and Hepatobiliary (HIDA, PIPIDA) scan: May be
function of gallbladder, including presence of done to confirm diagnosis of cholecystitis,
filling defects, structural defects, and/or stone especially when barium studies are
in ducts/biliary tree. Can be done IV (IVC) when contraindicated. Scan may be combined with
nausea/vomiting prevent oral intake, when the cholecystokinin injection to demonstrate
gallbladder cannot be visualized during OCG, or abnormal gallbladder ejection.
when symptoms persist following
Abdominal x-ray films (multipositional):
cholecystectomy. IVC may also be done
Radiopaque (calcified) gallstones present in
perioperatively to assess structure and function
10%–15% of cases; calcification of the wall or
of ducts, detect remaining stones after
enlargement of the gallbladder.
lithotripsy or
cholecystectomy, and/or to detect surgical Ultrasonography. Ultrasound is the preferred
complications. Dye can also be injected via T- initial imaging test for the diagnosis of acute
tube drain postoperatively. cholecystitis; scintigraphy is the preferred
alternative.
Percutaneous transhepatic cholangiography
(PTC): Fluoroscopic imaging distinguishes CT scan. CT scan is a secondary imaging test
between gallbladder disease and cancer of the that can identify extra-biliary disorders and
pancreas (when jaundice is present); supports acute complications of cholecystitis.
the diagnosis of obstructive jaundice and
reveals calculi in ducts. MRI. Magnetic resonance imaging is also a
possible secondary choice for confirming a
Nursing Implications diagnosis of acute cholecystitis.
Although the complication rate after this
procedure is low, the nurse must closely Ultrasonography-Ultrasonography is the
observe the patient for symptoms of bleeding, diagnostic procedure of choice because it is
peritonitis, and sepsis. The nurse assesses the rapid and accurate and can be used in patients
patient for pain and indications of these with liver dysfunction and jaundice. The
complications and reports them promptly to procedure is most accurate if the patient fasts
the primary provider, takes measures to overnight so that the gallbladder is distended.
reassure the patient, and ensures patient Ultrasonography can detect calculi in the
comfort. Antibiotic agents are often prescribed gallbladder or a dilated CBD with 90%
to minimize the risk of sepsis and septic shock. accuracy.
Radionuclide Imaging or Cholescintigraphy
Cholescintigraphy is used successfully in the
Cholecystograms (for chronic cholecystitis): diagnosis of acute cholecystitisor blockage of a
Reveals stones in the biliary bile duct. During this procedure, a radioactive
system. Note:Contraindicated in acute agent is administered intravenously (IV), which
is taken up by the hepatocytes and excreted
rapidly through the biliary tract. The biliary monitors the patient for side effects of any
tract is then scanned, and images of the medications received during the procedure.
gallbladder and biliary tract are obtained. This
Chest x-ray: Rule out respiratory causes of
test is more expensive than ultrasonography,
referred pain.
takes longer to perform, and exposes the
patient to radiation. It is often used when CBC: Moderate leukocytosis (acute).
ultrasonography is not conclusive, such as in
acalculous cholecystitis. Serum bilirubin and amylase: Elevated.
Endoscopic retrograde Serum liver enzymes—AST; ALT; ALP; LDH:
cholangiopancreatography. A fiberoptic Slight elevation; alkaline phosphatase and 5-
duodenoscope, with side-viewing apparatus, is nucleotidase are markedly elevated in biliary
inserted into the duodenum. The ampulla of obstruction
Vater is catheterized, and the biliary tree is Prothrombin levels: Reduced when obstruction
injected with contrast agent. The pancreatic to the flow of bile into the intestine
ductal system is also assessed, if indicated. This decreases absorption of vitamin K.
procedure is of special value in visualizing
neoplasms of the ampulla area and extracting a
biopsy specimen.
Management
NURSING IMPLICATION. Before ERCP, the Medical Management
patient is educated about the procedure and
Fasting. The patient may not be allowed to
their role in it. This preparation can allay anxiety
drink or eat at first in order to take the stress off
and facilitate the insertion of the endoscope
the inflamed gallbladder; IV fluids are
without damage to the GI tract structures,
prescribed to provide temporary food for the
including the biliary tree. The patient takes
cells. The diet immediately after an episode is
nothing by mouth for several hours before the
usually low-fat liquids. These can include
procedure. The procedure requires intravenous
powdered supplements high in protein and
(IV) sedation and monitored anesthesia care. In
carbohydrate stirred into skim milk. Cooked
some cases general anesthesia is required, and
fruits, rice or tapioca, lean meats, mashed
the sedated patient is monitored closely during
potatoes, non–gas-forming vegetables, bread,
and after the procedure (Brunicardi, 2019). It
coffee, or tea may be added as tolerated. The
may be necessary to administer medications,
patient should avoid eggs, cream, pork, fried
such as glucagon or anticholinergic agents, to
foods, cheese, rich dressings, gas forming
make cannulation easier by decreasing
vegetables, and alcohol. It is important to
duodenal peristalsis. The nurse observes closely
remind the patient that fatty foods may induce
for signs of respiratory and CNS depression,
an episode of cholecystitis. Dietary
hypotension, oversedation, and vomiting (if
management may be the major mode of
glucagon is given). During ERCP, the nurse
therapy in patients who have had only dietary
monitors IV fluids, administers medications, and
intolerance to fatty foods and vague GI
positions the patient. After the procedure, the
symptoms.
nurse monitors the patient’s condition,
observing vital signs and assessing for signs of Supportive medical care. This may include
perforation or infection. The nurse also restoration pf hemodynamic stability and
antibiotic coverage for gram-negative enteric
flora.
Gallbladder stimulation. Daily stimulation of
gallbladder contraction with IV cholecystokinin
may help prevent the formation of gallbladder
sludge in patients receiving TPN.
Antibiotic therapy. Levofloxacin and
Metronidazole for prophylactic antibiotic
coverage against the most common organisms.
Promethazine or Prochlorperazine may control
In laparoscopic cholecystectomy (A), the
nausea and prevent fluid and electrolyte
surgeon makes four small incisions (less than
disorders.
one half inch each) in the abdomen and inserts
Oxycodone or Acetaminophen may control a laparoscope with a miniature camera through
inflammatory signs and symptoms and reduce the umbilical incision (B). The camera apparatus
pain. displays the gallbladder and adjacent tissues on
a screen, allowing the surgeon to visualize the
Surgery
sections of the organ for removal.
Cholecystectomy. Removal of the gallbladder.
Small-Incision Cholecystectomy
Cholecystectomy is most commonly performed
Small-incision cholecystectomy is a surgical
by using a laparoscope and removing the
procedure in which the gallbladder is removed
gallbladder. In cholecystectomy, the gallbladder
through a small abdominal incision, as the name
is removed through an abdominal incision
implies. If needed, the surgical incision is
(usually right subcostal) after the cystic duct and
extended to remove larger gallbladder stones.
artery are ligated. The procedure is performed
Drains may or may not be used. The short
for acute and chronic cholecystitis.
length hospital stay has been identified as a
Laparoscopic Cholecystectomy major advantage of this type of procedure
Laparoscopic cholecystectomy is the standard
of therapy for symptomatic gallstones.
Laparoscopic cholecystectomy is performed Choledochostomy
through a small incision or puncture made Choledochostomy is reserved for the patient
through the abdominal wall at the umbilicus. with acute cholecystitis who may be too ill to
undergo a surgical procedure. This procedure
involves making an incision in the common
duct, usually for removal of stones. After the
stones have been evacuated, a tube is usually
inserted into the duct for drainage of bile until
edema subsides. This tube is connected to
gravity drainage tubing; the patient is
monitored closely, and a laparoscopic
cholecystectomy is planned for a future date
after acute inflammation has resolved.
Cholecystostomy is performed when the spontaneously into the duodenum. Another
patient’s condition precludes more extensive instrument with a small basket or balloon at its
surgery or when an acute inflammatory reaction tip may be inserted through the endoscope to
is severe. The gallbladder is surgically opened, retrieve the stones (see Fig. D–F). The patient is
stones and the bile or the purulent drainage are observed closely for bleeding, perforation, and
removed, and a drainage tube is secured with a the development of pancreatitis (see later
purse-string suture. The drainage tube is discussion) or sepsis. The ERCP procedure is
connected to a drainage system to prevent bile particularly useful in diagnosis and treatment of
from leaking around the tube or escaping into patients who have symptoms after biliary tract
the peritoneal cavity surgery, patients with intact gallbladders, and
patients for whom surgery is particularly
Nonsurgical Removal of Gallstones
hazardous.
Dissolving Gallstones
Intracorporeal Lithotripsy
Several methods have been used to dissolve
Stones in the gallbladder or CBD may be
gallstones by infusion of a solvent (mono-
fragmented by means of laser pulse technology.
octanoin or methyl tertiary butyl ether [MTBE])
A laser pulse is directed under fluoroscopic
into the gallbladder. The solvent can be infused
guidance with the use of devices that can
through the following routes: through a tube or
distinguish between stones and tissue. The laser
catheter inserted percutaneously directly into
pulse produces rapid expansion and
the gallbladder;
disintegration of plasma on the stone surface,
through a tube or drain inserted through a T-
resulting in a mechanical shock wave.
tube tract to dissolve stones not removed at the
Electrohydraulic lithotripsy uses a probe with
time of surgery, endoscopically with ERCP; or
two electrodes that deliver electric sparks in
via a transnasal biliary catheter, a rarely used
rapid pulses, creating expansion of the liquid
procedure due to its lack of success, potential
environment surrounding the gallstones. This
side effects, and recurrence rates of up to 50%
results in pressure waves that cause stones to
Stone Removal by Instrumentation fragment. This technique can be used
percutaneously with a basket or balloon
Several methods are used to remove stones catheter system or by direct visualization
that were not removed at the time of through an endoscope. Repeated procedures
cholecystectomy or have become lodged in the may be necessary because of stone size, local
CBD (see Fig. A,B). A catheter and instrument anatomy, bleeding, or technical difficulty. A
with a basket attached are threaded through nasobiliary tube can be inserted to allow for
the T-tube tract or fistula formed at the time of biliary decompression and to prevent stone
T-tube insertion; the basket is used to retrieve impaction in the common bile duct. This
and remove the stones lodged in the common approach allows time for improvement in the
bile duct. A second procedure involves the use patient’s clinical condition until gallstones are
of the ERCP endoscope (see Fig. C). After the cleared endoscopically, percutaneously, or
endoscope is inserted, a cutting instrument is surgically.
passed through the endoscope into the ampulla
of Vater of the common bile duct. It may be
used to cut the submucosal fibers, or papilla, of Extracorporeal Shock Wave Lithotripsy
the sphincter of Oddi, enlarging the opening, Extracorporeal shock wave lithotripsy (ESWL)
which may allow the lodged stones to pass has been used for nonsurgical fragmentation of
gallstones. ESWL is a noninvasive procedure Preoperative
that uses repeated shock waves directed at the
1. Maintain NPO status during nausea and
gallstones in the gallbladder or CBD to fragment
vomiting episodes.
the stones. The waves are transmitted to the
2. Maintain nasogastric decompression as
body through a fluidfilled bag or by immersing
prescribed for severe vomiting.
the patient in a water bath. After the stones are
3. Administer antiemetics as prescribed for
gradually broken up, the stone fragments can
nausea and vomiting.
be spontaneously passed from the gallbladder
4. Administer analgesics as prescribed to relieve
or common bile duct, removed by endoscopy,
pain and reduce spasm.
or dissolved with oral bile acid or solvents.
5. Administer antispasmodics (anticholinergics)
Because the procedure requires no incision and
as prescribed to relax smooth muscle.
no hospitalization, patients are usually treated
6. Instruct the client with chronic cholecystitis
as outpatients, but usually several sessions are
to eat small, low-fat meals.
necessary. This procedure has largely been
7. Instruct the client to avoid gas-forming foods.
replaced by laparoscopic cholecystectomy.
ESWL is used in some centers for a small
8. Prepare the client for nonsurgical and surgical
percentage of suitable patients (those with CBD
procedures as prescribed.
stones who may not be surgical candidates),
sometimes in combination with dissolution
therapy Postoperative interventions
(Feldman et al., 2016; Kellerman & Rakel, 2018). a. Monitor for respiratory complications caused
by pain at the incisional site.
Complications
b. Encourage coughing and deep breathing.
Empyema. An empyema of the bladder
c. Encourage early ambulation.
develops if the gallbladder becomes filled with
d. Instruct the client about splinting the
purulent fluid.
abdomen to prevent discomfort during
Gangrene. Gangrene develops because the coughing.
tissues do not receive enough oxygen and e.Administer antiemetics as prescribed for
nourishment at all. nausea and vomiting.
f. Administer analgesics as prescribed for pain
Cholangitis. The infection progresses as it relief.
reaches the bile duct g. Maintain NPO status and nasogastric tube
Surgical Management suction as prescribed.
Surgical treatment of gallbladder disease and h. Advance diet from clear liquids to solids
gallstones is carried out to relieve persistent when prescribed and as tolerated by the client.
symptoms, to remove the cause of biliary colic, I. Maintain and monitor drainage from the T-
and to treat acute cholecystitis. Surgery may tube, if present
be delayed until the patient’s symptoms have Goal: relief of pain, adequate ventilation, intact
subsided, or it may be performed as an skin and improved biliary drainage, optimal
emergency procedure, if necessitated by the nutritional intake, absence of complications,
patient’s condition. and understanding of self-care routines.
Nursing Management
You might also like
- Progesterone Has Been Shown To Decrease Gall-Bladder Motility, WhichDocument9 pagesProgesterone Has Been Shown To Decrease Gall-Bladder Motility, WhichFerreze AnnNo ratings yet
- Progesterone Has Been Shown To Decrease Gall-Bladder Motility, WhichDocument9 pagesProgesterone Has Been Shown To Decrease Gall-Bladder Motility, WhichFerreze AnnNo ratings yet
- Etiology, Pathophysiology, and Clinical Manifestations of CholecystitisDocument3 pagesEtiology, Pathophysiology, and Clinical Manifestations of CholecystitisGerriNo ratings yet
- CholelithiasisDocument6 pagesCholelithiasisLara GatbontonNo ratings yet
- CHOLECYSTITIS With CHOLECYSTOLITHIASISDocument33 pagesCHOLECYSTITIS With CHOLECYSTOLITHIASISSherry100% (3)
- Ntroduction: (1) (2) (3) Go ToDocument6 pagesNtroduction: (1) (2) (3) Go ToretnaNo ratings yet
- Extrahepatic Biliary Tract Pathology - Cholidolithiasis, Cholidocholithiasis, Cholecystitis and CholangitisDocument60 pagesExtrahepatic Biliary Tract Pathology - Cholidolithiasis, Cholidocholithiasis, Cholecystitis and CholangitisDarien LiewNo ratings yet
- Biliary Tract DiseasesDocument35 pagesBiliary Tract DiseasesSoumya Ranjan PandaNo ratings yet
- Hepatobiliary Tract and Pancreatic Pathology Assignment - PAYSONDocument22 pagesHepatobiliary Tract and Pancreatic Pathology Assignment - PAYSONRodrigo Joseph PaysonNo ratings yet
- CHOLELITIASISDocument31 pagesCHOLELITIASISRara ChanNo ratings yet
- Approach To Right Hypochondrium PainDocument34 pagesApproach To Right Hypochondrium PainkhansamrNo ratings yet
- Discussion of Disease (CholecystitisDocument3 pagesDiscussion of Disease (Cholecystitisjean paola nolascoNo ratings yet
- Cholecystitis Litiasis EctomyDocument23 pagesCholecystitis Litiasis EctomyTimothy WilliamsNo ratings yet
- Case Stydy On CholithiasisDocument29 pagesCase Stydy On CholithiasisDaniel TalleyNo ratings yet
- Disorders of The GallbladderDocument67 pagesDisorders of The GallbladderGeofry OdhiamboNo ratings yet
- Gallbladder 2Document8 pagesGallbladder 2hussain AltaherNo ratings yet
- CholedocholithiasisDocument3 pagesCholedocholithiasisPao AcelajadoNo ratings yet
- Acute and Chronic CholecystitisDocument10 pagesAcute and Chronic Cholecystitisissam_1994No ratings yet
- CHolelitiasis, CholesistitisDocument44 pagesCHolelitiasis, CholesistitistrianaamaliaNo ratings yet
- Cholecystolithiasis: Characteristics and CompositionDocument7 pagesCholecystolithiasis: Characteristics and Compositionjesabel_caraigNo ratings yet
- Dave Jay S. Manriquez RN. Acute CholecystitisDocument11 pagesDave Jay S. Manriquez RN. Acute CholecystitisChilleMaeNo ratings yet
- GallstoneDocument6 pagesGallstoneMushfique HussainNo ratings yet
- E. Coli Bacteroides: Cholelithiasis Gallstones Cystic Duct Inspissation Bile Stasis Murphy's SignDocument3 pagesE. Coli Bacteroides: Cholelithiasis Gallstones Cystic Duct Inspissation Bile Stasis Murphy's Sign121327No ratings yet
- The Diseases of GallbladderDocument27 pagesThe Diseases of GallbladderAroosha IbrahimNo ratings yet
- Cholelithiasis and Cholecystitis Nursing Care Plan ManagementDocument5 pagesCholelithiasis and Cholecystitis Nursing Care Plan ManagementCamille Joy BaliliNo ratings yet
- Chole Lithia SisDocument35 pagesChole Lithia SisKrismadhaNo ratings yet
- CholecystitisDocument15 pagesCholecystitisHala LeeNo ratings yet
- Cholecystitis Full With EditDocument43 pagesCholecystitis Full With Editmustafalotfy01No ratings yet
- Background: Biliary Colic Acute Cholecystitis Acute PancreatitisDocument14 pagesBackground: Biliary Colic Acute Cholecystitis Acute PancreatitisrhopmaeNo ratings yet
- Case StudyDocument24 pagesCase StudyPatricia Marie BuenafeNo ratings yet
- Case Study CholecystitisDocument27 pagesCase Study Cholecystitisyhanne98% (225)
- Cholelithiasis & CholecystitisDocument2 pagesCholelithiasis & CholecystitisKate DNo ratings yet
- Gallbladder DiseaseDocument67 pagesGallbladder DiseaseKhadira MohammedNo ratings yet
- Acute Cholecystitis From Biliary LithiasisDocument17 pagesAcute Cholecystitis From Biliary Lithiasisdhimas satriaNo ratings yet
- Gallstone DiseaseDocument104 pagesGallstone DiseaseTan DanNo ratings yet
- Cholelithiasis: Author: Douglas M Heuman, MD, FACP, FACG, AGAF, Chief of HepatologyDocument22 pagesCholelithiasis: Author: Douglas M Heuman, MD, FACP, FACG, AGAF, Chief of HepatologyYossy DelwitaNo ratings yet
- CholelithiasisDocument69 pagesCholelithiasisRashmita DahalNo ratings yet
- Gallstone DiseaseDocument104 pagesGallstone DiseaseEma RadulescuNo ratings yet
- Management Pancreas and GallbladderDocument21 pagesManagement Pancreas and Gallbladderapi-19790126No ratings yet
- Acute and Chronic PancreatitisDocument5 pagesAcute and Chronic Pancreatitisabdallah ANo ratings yet
- 13 CholecystitisDocument11 pages13 CholecystitisdorajuangaterNo ratings yet
- Topic: Cholecystitis: IntroductionDocument11 pagesTopic: Cholecystitis: IntroductionSyarafina AzmanNo ratings yet
- Cholelithiasis GallstoneDocument22 pagesCholelithiasis GallstoneBheru LalNo ratings yet
- SGD On Gallstones and Acute Cholecystitis 2-1Document9 pagesSGD On Gallstones and Acute Cholecystitis 2-1Rabbya Nasir 5No ratings yet
- Cholelithiasis RLDocument29 pagesCholelithiasis RLPrincess Joanna Marie B DelfinoNo ratings yet
- Gallstones Develop InsidiouslyDocument1 pageGallstones Develop InsidiouslyetengNo ratings yet
- Liver Cirrhosis, A Simple Guide To The Condition, Treatment And Related DiseasesFrom EverandLiver Cirrhosis, A Simple Guide To The Condition, Treatment And Related DiseasesNo ratings yet
- Diverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesFrom EverandDiverticulosis, A Simple Guide to the Condition, Treatment and Related DiseasesRating: 1 out of 5 stars1/5 (1)
- A Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisFrom EverandA Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisRating: 3 out of 5 stars3/5 (1)
- A Simple Guide to Cholangitis, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Cholangitis, Diagnosis, Treatment and Related ConditionsNo ratings yet
- Cholecystitis And Gallstones, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandCholecystitis And Gallstones, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsRating: 5 out of 5 stars5/5 (1)
- Diverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookFrom EverandDiverticulitis Cure: The Ultimate Diverticulitis Diet: Diverticulitis Recipes: Your Ultimate Diverticulitis CookbookNo ratings yet
- A Simple Guide to Cholecystitis, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Cholecystitis, Diagnosis, Treatment and Related ConditionsNo ratings yet
- The Liver and Gallbladder Miracle Cleanse: An All-Natural, At-Home Flush to Purify & Rejuvenate Your BodyFrom EverandThe Liver and Gallbladder Miracle Cleanse: An All-Natural, At-Home Flush to Purify & Rejuvenate Your BodyNo ratings yet
- Ulcerative Colitis, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandUlcerative Colitis, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- A Simple Guide to Acalculous Cholecystopathy, Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Acalculous Cholecystopathy, Diagnosis, Treatment and Related ConditionsNo ratings yet
- CHNDocument1 pageCHNJdee XNo ratings yet
- Guidelines For Trashion ShowDocument1 pageGuidelines For Trashion ShowJdee XNo ratings yet
- CHNDocument7 pagesCHNJdee XNo ratings yet
- Activity in ModuleDocument2 pagesActivity in ModuleJdee XNo ratings yet
- Pathology of The Bile Duct 2017 - Yasuni Nakanuma PDFDocument215 pagesPathology of The Bile Duct 2017 - Yasuni Nakanuma PDFHîrjoabă IoanNo ratings yet
- Acute Cholecystitis SeminarDocument42 pagesAcute Cholecystitis SeminarNatnaelNo ratings yet
- Case Presentation - CholelithiasisDocument35 pagesCase Presentation - Cholelithiasisarief2704900% (1)
- Assessment and Management of Patients With Biliary DisorderDocument50 pagesAssessment and Management of Patients With Biliary DisorderZanida ZainonNo ratings yet
- Pathophysiology: Cholecystitis Non Modifiable Factors Modifiable FactorsDocument4 pagesPathophysiology: Cholecystitis Non Modifiable Factors Modifiable FactorsLovely DaroleNo ratings yet
- CholedocholithiasisDocument44 pagesCholedocholithiasisGerli Bismonte100% (6)
- Vagus Nerve 101 Stimulation ExercisesDocument93 pagesVagus Nerve 101 Stimulation Exercisestrent bone100% (5)
- Batu EmpeduDocument140 pagesBatu Empeduyanuar h wijayaNo ratings yet
- Multiple Choice Questions of Radiology and ImagingDocument18 pagesMultiple Choice Questions of Radiology and ImagingVishakha Wahule90% (10)
- PACES 3 - AbdomenDocument14 pagesPACES 3 - AbdomenDrShamshad KhanNo ratings yet
- Cholelithiasis Case 1Document21 pagesCholelithiasis Case 1Arvin F. LansangNo ratings yet
- Gallbladder, Liver, Pancrea DisordersDocument82 pagesGallbladder, Liver, Pancrea Disordersm1k0e100% (2)
- Cholecystectomy With Intraoperative CholangiogramDocument8 pagesCholecystectomy With Intraoperative CholangiogramLourd Andrew VillegasNo ratings yet
- Abdominal DistentionDocument6 pagesAbdominal DistentionDumapis RichardNo ratings yet
- Symptoms of Celiac and Gluten Sensitivity - Gluten Free Girl and The ChefDocument255 pagesSymptoms of Celiac and Gluten Sensitivity - Gluten Free Girl and The Chefmusatii0% (1)
- 2cc2743-8f6c-31d0-D6d-Dd53e8140 Top 5 Gallbladder Support Supplements 2Document11 pages2cc2743-8f6c-31d0-D6d-Dd53e8140 Top 5 Gallbladder Support Supplements 2Rabisha AshrafNo ratings yet
- Bile Salts & It's FunctionsDocument10 pagesBile Salts & It's FunctionsJorge De Vera100% (1)
- Retrohepatic Gallbladder Masquerading As Hydatid Cyst in ADocument18 pagesRetrohepatic Gallbladder Masquerading As Hydatid Cyst in AMadalina BlagaNo ratings yet
- Azizah Clayton - BUDAPEST2 Conference 08Document21 pagesAzizah Clayton - BUDAPEST2 Conference 08namkay_tenzynNo ratings yet
- Gall Bladder - : Anatomy, Physiology and Benign Disease For Medical UndergraduatesDocument119 pagesGall Bladder - : Anatomy, Physiology and Benign Disease For Medical UndergraduatesMayadevi100% (1)
- Nbme Cbse Actual Test Questions and AnswersDocument175 pagesNbme Cbse Actual Test Questions and Answersgithijidennis99No ratings yet
- Open CholecystectomyDocument15 pagesOpen CholecystectomyjimdioNo ratings yet
- Gallbladder DiseaseDocument4 pagesGallbladder DiseaseNoreisZhaoTangNo ratings yet
- Miss.G.Nisha AS - TEN - US - 5726 19 - 005726 - 212267 13Y / Female DR - Self 4-Mar-2021Document2 pagesMiss.G.Nisha AS - TEN - US - 5726 19 - 005726 - 212267 13Y / Female DR - Self 4-Mar-2021jeyaraman jcbNo ratings yet
- Clinical Embriology and Anatomy of Gi Tract Part1Document44 pagesClinical Embriology and Anatomy of Gi Tract Part1trianaamalia100% (1)
- Calculous CholecystitisDocument137 pagesCalculous Cholecystitisrremonde100% (5)
- Sabiston Biliary System NotesDocument5 pagesSabiston Biliary System NotessvidrillionNo ratings yet
- DAFTAR PUSTAKA (Kasus Mendalam 2)Document4 pagesDAFTAR PUSTAKA (Kasus Mendalam 2)mkpnurdinNo ratings yet
- Surgical Notes A Pocket Survival GuideDocument197 pagesSurgical Notes A Pocket Survival Guidevin100% (12)
- Dr-Gerson Suppressed Congressional TestimonyDocument10 pagesDr-Gerson Suppressed Congressional TestimonyJacek Rafał Tatko100% (1)