Professional Documents
Culture Documents
Special Organs-Eye, Ear, Nose
Uploaded by
عبدالسلام الأسمرOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Special Organs-Eye, Ear, Nose
Uploaded by
عبدالسلام الأسمرCopyright:
Available Formats
H I G H - YI E L D FAC TS I N
Special Organs—Eye, Ear, Nose
Eye 428 Recurrent Acute Otitis Media 435
Amblyopia 428 Otitis Media with Effusion 435
Strabismus 428 Otitis Externa 436
Optic Neuritis 429 Mastoiditis 437
Conjunctivitis 429 Tinnitus 437
Episcleritis/Scleritis 430 Vertigo 437
Blepharitis 430 Ototoxic Drugs 438
Dacryostenosis 431 Nose 438
Chalazion 431 Sinusitis 438
Hordeolum 432 Epistaxis 439
Periorbital Cellulitis 432 Allergic Rhinitis 440
Orbital Cellulitis 432 Choanal Atresia 440
Corneal Ulcer 433
Retinoblastoma 434
Ear 434
Otitis Media 434
Acute Otitis Media 435
427
ch18.indd 427 26-08-2017 10:11:34
428 HIGH-YIELD FACTS IN SPECIAL ORGANS—EYE, EAR, NOSE
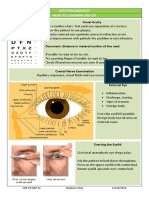
WARD TIP Eye
Amblyopia has been called “lazy eye.”
A m b ly o p i a
Definition
EX AM TIP A ↓ in visual acuity in one or both eyes caused by blurred retinal images lead-
ing to failure of the visual cortex to develop properly.
Strabismus is the most common cause of
amblyopia. Etiology
■ Strabismus.
■ Refractive errors.
■ Opacity in the visual path (e.g., cataract, ptosis, eyelid hemangioma).
EX AM TIP
Diagnosis
Amblyopia is usually asymptomatic Diagnosis is made by visual acuity testing.
and can be detected only by screening
examination. Treatment
■ Treatment of the pathology, such as removal of a cataract.
■ Prescription glasses to correct refractive errors.
■ Patching the good eye until the ambylopic eye has improved its vision.
EX AM TIP
Strabismus
Younger children are more susceptible to
the development of amblyopia.
Definition
■ Deviation or misalignment of the eye (see Figure 18-1).
■ “To squint or to look obliquely.”
■ Strabismus can lead to vision loss which often results in permanent
EX AM TIP amblyopia.
For the best results, amblyopia should be Diagnosis
treated by age 4. The earlier the better.
■ Corneal light reflex: The child looks directly into a light source and the
doctor observes where the reflex lies in both eyes; if the light is off center
in one pupil or asymmetric, then strabismus exists.
■ Alternative cover test: The child stares at an object in the distance and
the doctor covers one of the child’s eyes; if there is movement of the
EX AM TIP uncovered eye once the other eye is covered, then strabismus exists.
Amblyopia can be reversed more rapidly Treatment
in younger children. ■ Prescription glasses may help if the strabismus is secondary to refraction error.
■ Extraocular muscle surgery may be necessary.
FIGURE 18-1. Child with strabismus.
ch18.indd 428 26-08-2017 10:11:35
SPECIAL ORGANS—EYE, EAR, NOSE HIGH-YIELD FACTS IN 429
Optic Neuritis
Definition EX AM TIP
■ Inflammation of the optic nerve.
■ Retrobulbar optic neuritis: Without ophthalmoscopically visible signs of A deviated eye is described as being
disc inflammation. turned “eso” (inward), “exo” (outward),
■ Papillitis or intraocular optic neuritis: Ophthalmoscopically visible “hypo” (downward), or “hyper”
evidence of inflammation of the nerve head. (upward) -tropic.
■ Neuroretinitis: Inflammation of both the retina and papilla.
Etiology
■ Idiopathic.
■ Secondary to underlying disease—multiple sclerosis, lupus.
■ Recent immunization or viral infection (measles, chickenpox, influenza).
■ Extension from an infection involving the teeth, sinuses, or meninges.
■ Side effect of treatment with vincristine or chloramphenicol.
■ Secondary to a toxin such as lead.
Signs and Symptoms
■ Loss of visio or central scotoma.
■ Pain with extraocular motion.
■ Pain to palpation of the globe.
■ Afferent papillary defect.
■ Bilateral in children (unilateral in adults).
Complications
■ Color deficits.
■ Motion perception deficits.
■ Brightness sense deficits.
EX AM TIP
Treatment
A trial of intravenous (IV) steroids may ↓ the length of time for symptoms but In children, optic neuritis is rarely
has no effect on the outcome. Methylprednisolone also prolongs the onset to associated with multiple sclerosis.
develop MS in those who are predisposed.
Conjunc tivitis
Definition
Inflammation of the conjunctiva.
Types
Allergic
■ Immunoglobulin E (IgE)–mediated reaction caused by triggers such as
pollen or dust.
■ Signs and symptoms: Watery, itchy, red eyes with edema to the conjunctiva WARD TIP
and lids. Typically bilateral.
■ Pruritus and chemosis are common. Adenovirus is the most common viral
■ Treatment: Includes removal of the trigger, cold compresses, and cause of conjunctivitis.
antihistamines.
ch18.indd 429 26-08-2017 10:11:35
430 HIGH-YIELD FACTS IN SPECIAL ORGANS—EYE, EAR, NOSE
Viral
■ Adenovirus and coxsackievirus are typical causes.
■ Adenovirus: Pharyngoconjunctival fever—triad: Pharyngitis, fever, and
conjunctivitis.
WARD TIP ■ Epidemic keratoconjunctivitis: Fulminant vision-threatening condition
with the involvement of cornea.
Conjunctivitis with lymph nodes. Think: ■ Signs and symptoms: Watery, red eyes with preauricular lymph nodes.
Viral etiology. ■ Treatment: Includes supportive treatment with constant hand washing to
prevent transmission.
Bacterial
■ Three organisms: Nontypeable Haemophilus influenzae, Streptococcus
pneumoniae, and Staphylococcus aureus.
■ Highly contagious, outbreaks can occur.
■ Signs and symptoms: Mucopurulent discharge, red eyes, and edema of
the conjunctiva. More often unilateral; can be bilateral.
■ Treatment: Topical antibiotics (drops or ointment).
Episcleritis/Scleritis
Definition
Inflammation of the episclera or sclera.
E tiology
High association with autoimmune diseases.
Signs and Symptoms
■ Eye pain.
WARD TIP ■ Photophobia.
■ Erythema.
Episcleritis/scleritis is usually unilateral. ■ ↓ visual acuity.
■ Perforation is associated only with scleritis.
Treatment
■ Topical steroids.
■ Nonsteroidal anti-inflammatory drugs (NSAIDs).
■ Immunosuppressive drugs in cases of steroid failure.
■ Surgery for thinning or perforated sclera.
Blepharitis
Definition
Inflammation of the eyelid margins.
E tiology
■ Staphylococcus aureus.
■ Staphylococcus epidermidis.
■ Seborrheic.
■ A combination of the above.
Signs and Symptoms
■ Burning.
■ Itching.
■ Erythema.
ch18.indd 430 26-08-2017 10:11:35
SPECIAL ORGANS—EYE, EAR, NOSE HIGH-YIELD FACTS IN 431
■ Scaling.
■ Ulceration of the lid margin.
Treatment
■ Daily eyelid cleansing to remove scales.
■ Topical antibiotics.
D a c r y o s t en o s i s
A 4-month-old child presents with an exudative eye discharge and a painful, red
lacrimal sac. Think: Dacrocystitis.
Dacrocystitis is the most common infection of the lacrimal system. It is often a
complication of dacryocystocele. Excessive tearing, purulent eye discharge, and fever
are the common symptoms. S. aureus and streptococci are the common organisms.
Most patients require admission for intravenous antibiotics. An incision and drainage
may be needed in the presence of a lacrimal sac abscess.
Definition EX AM TIP
A congenital nasolacrimal duct obstruction.
Dacryostenosis is the most common
Epidemiology disorder of the lacrimal system.
Occurs in 5% of infants; appears a few weeks after birth.
Etiology
Failure of the epithelial cells of tear duct to come apart.
Signs and Symptoms
■ Chronic tearing.
■ Crusty discharge noted especially in AM. Typically without conjunctival
injection.
Complications
Dacrocystitis—inflammation of the nasolacrimal sac; this must be treated
with topical or systemic antibiotic and warm compresses.
Treatment
■ Digital massage of the lacrimal sac and warm compresses are recommended,
though it is unclear if they change the outcome from the natural course. WARD TIP
■ Eyelid cleansing.
■ Vast majority resolve before 1 year of age. Most dacryostenosis will resolve by
■ Probing/instrumentation if still present after 1 year of age to rupture the 8 months of age.
membrane.
Chalazion
Definition
Inflammation of a meibomian (tarsal) gland leading to the formation of a
granuloma.
Signs and Symptoms
■ Firm nodule on the eyelid.
■ Nontender.
ch18.indd 431 26-08-2017 10:11:35
432 HIGH-YIELD FACTS IN SPECIAL ORGANS—EYE, EAR, NOSE
Treatment
■ Warm compresses.
■ Excision if necessary.
■ Most subside spontaneously over months.
H o r de o l u m
Types
■ External hordeolum, or stye, is an infection of the glands of Zeis or Moll.
■ Internal hordeolum is infection of the meibomian gland.
E tiology
S. aureus.
Signs and Symptoms
■ Localized swelling.
■ Tenderness.
■ Erythema.
Treatment
■ Warm compresses.
■ Topical antibiotics general ineffective.
WARD TIP ■ Incision and drainage if there is no spontaneous rupture.
Orbital cellulitis is postseptal.
Pe r i o r b i ta l Ce l l u l i t i s
Definition
Inflammation of the eyelids and periorbital tissue anterior to the septum.
WARD TIP
Etiology
Periorbital cellulitis is much more Extension of local infections including upper respiratory infection (URI),
common than orbital cellulitis.
sinusitis, dental infection, facial cellulitis, trauma, or eyelid infection.
S igns and Symptoms
■ Erythema.
WARD TIP ■ Edema.
■ Induration and tenderness.
The most common organisms causing ■ No pain with extraocular movements.
both preorbital and orbital cellulitis—
SHIP Complications
S. aureus Development of orbital cellulitis.
H. influenzae
S. Pneumoniae Treatment
Oral or IV antibiotics (e.g., ceftriaxone).
O r b i ta l Ce l l u l i t i s
Definition
Inflammation of the orbital tissues behind the septum.
E tiology
■ Extension of a local infection including paranasal sinusitis, facial cellulitis,
or dental abscess.
■ Trauma.
ch18.indd 432 26-08-2017 10:11:35
SPECIAL ORGANS—EYE, EAR, NOSE HIGH-YIELD FACTS IN 433
■ The most common organisms are H. influenza, S. aureus, and S. pneumoniae.
■ Most common site: Medial orbital wall.
■ ↑ incidence secondary to ↑ in methicillin-resistant S. aureus (MRSA).
■ Orbital cellulitis is caused most commonly by ethmoid sinusitis.
Signs and Symptoms
■ Proptosis, ophthalmoplegia, and ↓ vision differentiate it from preseptal
cellulitis.
■ Painful extraocular motion is often the first sign.
■ Proptosis is classic, but late, sign.
■ Decreased visual acuity.
■ Erythema in conjunctiva.
■ Edema.
Diagnosis
Orbital computed tomography (CT) scan with IV contrast.
Treatment
■ Ophthalmology consultation.
■ Intravenous antibiotics, possible surgical drainage.
Complications WARD TIP
■ Loss of vision.
■ Meningitis. Periorbital cellulitis is preseptal.
■ Central nervous system (epidural) abscess.
C o r nea l U l c e r
Etiology
■ Trauma (sand, contact lens, etc.) with secondary infection. Often preceded
by a traumatic corneal abrasion.
■ Bacterial: Pseudomonas aeruginosa, Neisseria gonorrhoeae.
■ Fungal: Especially in contact lens users.
Signs and Symptoms
■ Corneal haze.
■ Painful.
■ Photophobia.
■ Tearing.
EX AM TIP
Complications
■ Perforation. Retinoblastoma gene: Mutation in the
■ Scarring. long arm of chromosome 13.
■ Blindness.
Diagnosis
■ Slit-lamp exam: Fluorescein staining reveals an epithelial defect. WARD TIP
■ Scraping of the cornea to identify infectious etiology.
Must evaluate for the presence of
Treatment retinoblastoma in a child presenting with
■ Local antibiotics. strabismus.
■ In some cases, systemic treatment may be required.
ch18.indd 433 26-08-2017 10:11:35
434 HIGH-YIELD FACTS IN SPECIAL ORGANS—EYE, EAR, NOSE
Re t i n o b l as t o m a
■ The most common primary ocular malignancy in children.
■ Average age: 18 months (90% <5 years).
EX AM TIP Signs and Symptoms
■ Leukocoria: White pupillary reflex is the most common presentation.
Retinoblastoma is the most common ■ Strabismus is the second most common presentation.
primary malignant intraocular tumor in ■ Orbital inflammation.
children. ■ Hyphema: Blood layering anterior to the iris.
■ May be bilateral (40%).
Diagnosis
■ Direct visualization during eye exam.
■ Computed tomography (CT) or ultrasound (US) can help confirm and
evaluate spread.
WARD TIP Treatment
■ Chemotherapy.
Family members of a patient with ■ Laser photocoagulation.
retinoblastoma should be checked ■ Cryotherapy.
because it may be hereditary. ■ Enucleation for unresponsive tumors.
■ Referral for genetic counseling for families with a history of retinoblastoma.
Ear
O t i t i s Med i a
Definition
Inflammation of the middle ear.
Epidemiology
■ The incidence of otitis media is higher in:
■ Boys.
■ Children in day care.
■ Children exposed to secondhand smoke.
■ Non-breast-fed infants.
■ Immunocompromised children,
■ Children with craniofacial defects like cleft palate,
■ Children with a strong family history for otitis media,
■ The incidence of infection is higher in children because of their eusta-
chian tube anatomy:
■ Horizontal.
■ Short in length.
■ ↓ tone.
EX AM TIP
Etiology
The most common overall complication ■ S. pneumoniae.
of otitis media is hearing loss. ■ H. influenzae.
■ Moraxella catarrhalis.
Complications
■ Hearing loss due to persistent middle-ear effusion.
■ Perforation.
ch18.indd 434 26-08-2017 10:11:35
SPECIAL ORGANS—EYE, EAR, NOSE HIGH-YIELD FACTS IN 435
■ Mastoiditis.
■ Cholesteatoma: Saclike epithelial structures.
■ Facial nerve paralysis: The facial nerve may not be completely covered
with bone in the middle ear; therefore, infection can spread to the nerve. EX AM TIP
■ Labyrinthitis.
■ Abscess formation. The most common intracranial
■ Tympanosclerosis: Scarring of the tympanic membrane. complication of otitis media is meningitis.
■ Meningitis.
A c u t e O t i t i s Med i a
Eustachian tube dysfunction is the most important factor.
Signs and Symptoms WARD TIP
■ Ear tugging.
■ Ear pain. Remember that younger children who
■ Fever. are unable to communicate may have
■ Malaise. only nonspecific signs like nausea and
■ Irritability. vomiting with an acute illness such as
■ Hearing loss. acute otitis media.
■ Nausea and vomiting.
Diagnosis
■ Diagnosis is made with a pneumatic otoscope—the tympanic membrane WARD TIP
will have ↓ mobility and will appear hyperemic and bulging with loss of
landmarks. A red eardrum in a crying child is normal;
■ Tympanocentesis should be used as an adjunct in patients who are <8 the most specific sign of acute otitis
weeks old, are immunocompromised, have a complication, or were treated media is ↓ mobility of the tympanic
with multiple courses of antibiotics without improvement; the fluid is sent membrane.
for culture and sensitivity.
Treatment
■ Typically, the first-line antibiotic is amoxicillin. High dose can be used
for cases most likely to be resistant (antibiotics within 3 months, less than
2 years of age, in day care or with sibling in school or day care).
■ Antipyretics: Ibuprofen and/or acetaminophen.
■ Topical anesthetic eardrops (e.g., benzocaine).
■ For healthy children >2 years old with milder case, watchful waiting for
24–48 hours is an option.
■ Pneumococcal vaccine has reduced the incidence of acute otitis media.
Re c u r r en t A c u t e O t i t i s Med i a
Definition
Three to four episodes of acute otitis media in 6 months or 6 episodes in a year.
Treatment
■ Prophylactic antibiotics.
■ Myringotomy and ventilating tubes should be considered.
O t i t i s Med i a w i t h E f f u s i o n
Signs and Symptoms
■ Hearing loss.
■ Dizziness.
ch18.indd 435 26-08-2017 10:11:35
436 HIGH-YIELD FACTS IN SPECIAL ORGANS—EYE, EAR, NOSE
■ No fever.
■ No ear pain.
Diagnosis
Pneumatic otoscope shows a retracted eardrum with loss of landmarks and
air-fluid levels or bubbles.
Treatment
■ If asymptomatic, a child is observed for 3 months to see if effusion resolves.
■ If symptomatic after 3 months of observation, treatment includes antibiot-
ics and possibly myringotomy and insertion of tympanostomy tubes.
O t i t i s E x t e r na
A 4-year-old boy presents with what looks like herpetic vesicles in the ear canal
and tympanic membrane. Think: Ramsay Hunt syndrome (facial paralysis + herpes
zoster oticus). CN VIII involved = sensorineural hearing loss or vertigo.
It is due to herpetic involvement of the facial (geniculate), vestibulocochlear, or
trigeminal ganglia which results in pain and vesicular eruptions about the auricle and
external ear canal.
WARD TIP Definition
■ Inflammation of the external auditory canal.
Otitis externa is known as “swimmer’s ear.” ■ Occurs when trauma introduces bacteria into an area that is excessively
wet or dry.
Etiology
■ Bacterial: P. aeruginosa, S. aureus, Proteus mirabilis, Klebsiella pneumoniae.
■ Viral: HSV/Zoster.
■ Fungal: Candida.
Signs and Symptoms
■ Ear pain with movement of the tragus or pinna.
■ Pruritus of the ear canal.
■ Edema of the ear canal.
■ Otorrhea: Usually white in color.
■ Palpable lymph nodes: Peri- and preauricular.
■ Normal tympanic membrane.
Complications
■ Malignant otitis externa leads to hearing loss, vertigo, and facial nerve
paralysis.
■ Temporary hearing loss secondary to swelling.
■ Necrotizing otitis externa:
■ Pseudomonas osteomyelitis in the temporal bone.
■ Risk factors: Diabetes, immunocompromised (Aspergillus fumigatus).
EX AM TIP
Diagnosis
Malignant otitis externa is caused by Diagnosis is made by otoscopic examination.
P. aeruginosa and must be treated
systemically (i.e., oral or IV antibiotics; Treatment
NOT drops alone). Topical antibiotics and steroids to reduce edema (e.g., Cortisporin suspension
[hydrocortisone-polymyxin-neomycin-bacitracin]).
ch18.indd 436 26-08-2017 10:11:35
SPECIAL ORGANS—EYE, EAR, NOSE HIGH-YIELD FACTS IN 437
Mas t o i d i t i s
Definition
■ Inflammation of the mastoid air cells in the temporal bone.
■ Most common pathogen: S. pneumoniae.
Acute Mastoiditis
■ Mostly seen in children after/with an acute otitis media.
■ If resolution does not occur, may lead to acute mastoiditis with periosteitis,
acute mastoid osteitis, or chronic mastoiditis.
■ Fever.
■ Pain and induration behind the ear overlying mastoid air cells and tempo-
ral bone.
■ Erythema and tenderness over the mastoid area.
Acute Mastoiditis with Periosteitis
■ Includes the involvement of the periosteum.
■ Treatment: Includes myringotomy with ventilation tube placement and
IV antibiotics.
Acute Mastoid Osteitis
■ Occurs when there is an empyema and destruction of the mastoid cells.
■ The child will have a tender, swollen, red mastoid process with the ear dis-
placed down and out.
■ Treatment: Includes IV antibiotics, and mastoidectomy may be necessary.
Chronic Mastoiditis
Involves treatment with antibiotics and possibly a mastoidectomy if osteitis is
present.
Complications
■ Hearing loss.
■ Facial nerve palsy.
■ Subperiosteal abscess.
■ Cranial osteomyelitis.
■ Labyrinthitis.
■ Intracranial spread (meningitis, epidural or cerebellar abscess, subdural
empyema).
■ Dural sinus thrombosis.
T i nn i t u s
Definition
■ Ringing in the ear.
■ Commonly found in children who have middle-ear disease or hearing loss.
Also associated with salicylate use.
Ve r t i g o
Definition
Dizziness with the feeling that one’s body is in motion.
ch18.indd 437 26-08-2017 10:11:35
438 HIGH-YIELD FACTS IN SPECIAL ORGANS—EYE, EAR, NOSE
T A B L E 1 8 - 1 . Ototoxic Drugs
Diuretics Furosemide
Ethacrynic acid
Antibiotics Aminoglycosides
Minocycline
Quinolones
Chemotherapeutics Cisplatin
Vinblastine
Antimalarials Quinine
Chloroquine
Mefloquine
Antiarrhythmics Quinidine
Salicylates Aspirin
Signs and Symptoms
WARD TIP
■ Difficulty walking straight, or stumbling.
Benign positional vertigo (BPV) will
■ Spinning sensation.
■ Vomiting.
present with ataxia and horizontal
nystagmus.
E tiology
May occur secondary to the following conditions:
■ Otitis media.
■ Labyrinthitis.
EX AM TIP ■ Trauma.
■ Cholesteatoma.
Ménière triad includes vertigo, tinnitus, ■ BPV.
and hearing loss. ■ Ménière disease.
■ CNS disease.
Treatment
Address the underlying cause.
Ototoxic Drugs
See Table 18-1.
Nose
Sinusitis
Definition
Inflammation of the membranes covering the sinuses. Clinical definition also
includes minimum duration of 10 days of symptoms that are worsening.
ch18.indd 438 26-08-2017 10:11:35
SPECIAL ORGANS—EYE, EAR, NOSE HIGH-YIELD FACTS IN 439
Sinus Development
■ Ethmoid sinus at birth.
■ Maxillary sinus at birth.
■ Sphenoid sinus 5 years.
■ Frontal sinus 7 years.
Etiology
■ A child may be at risk for sinusitis if there is an obstruction or cilia impairment.
■ S. pneumoniae.
■ H. influenzae.
■ M. catarrhalis.
■ Rhinovirus is the most common viral pathogen.
■ Bacterial sinusitis is usually preceded by a viral upper respiratory infection.
Predispositions
■ Occlusion of the sinus ostium.
■ Cystic fibrosis.
■ Allergy/asthma.
■ Cyanotic congenital heart disease.
■ Dental infections.
Signs and Symptoms
■ Headache—worse when bending foward.
■ Sinus tenderness to palpation. EX AM TIP
■ Persistent nasal discharge (purulent) >10 days’ duration.
■ Halitosis. At birth, only the maxillary and ethmoid
■ Cough secondary to postnasal drip. sinuses are present.
■ Early AM nausea or emesis.
Complications
■ Cellulitis. WARD TIP
■ Abscess formation.
■ Osteomyelitis.
The most common location for epistaxis
■ Meningitis may occur through spread of the ethmoid, sphenoid, or frontal
in children is from the anterior nasal
sinuses. septum because Kiesselbach’s plexus is
located there.
Diagnosis
■ Diagnosis is made clinically.
■ If imaging is required, a CT scan is preferred over plain films, which are
not as sensitive.
WARD TIP
Treatment
■ First line is amoxicillin for 14–21 days. Blood in vomit may be present if a child
■ If no improvement, a macrolide or amoxicillin-clavulanate may be used. has swallowed blood from epistaxis;
■ Decongestants. always ask about epistaxis if a patient
■ Nasal saline drops/mist. presents with hematemesis.
■ Nasal irrigation.
E p i s tax i s
Definition
■ Nosebleed.
■ Common age: 2–10 years.
■ Unusual during infancy; must consider coagulopathy or nasal organic causes
(e.g., choanal atresia).
ch18.indd 439 26-08-2017 10:11:35
440 HIGH-YIELD FACTS IN SPECIAL ORGANS—EYE, EAR, NOSE
Etiology
■ The most common location for a nosebleed in children is the anterior
EX AM TIP
septum.
■ The most common cause is trauma secondary to a fingernail.
Isolated nosebleeds are rarely a sign of a ■ Other causes may include foreign bodies, inflammation, or dry air.
bleeding disorder. ■ If a child has recurrent, severe epistaxis, more serious causes should be looked
into such as thrombocytopenia, clotting deficiencies, and angiofibromas.
Signs and Symptoms
EX AM TIP Bleeding may occur from one or both nostrils.
Allergic rhinitis is the most common Treatment
atopic disease. ■ Compression for 10 minutes with head tilted forward.
■ Cold compresses to the nose.
■ Topical vasoconstrictors may allow visualization and identification of the
bleeding site.
■ Cauterization using silver nitrite.
WARD TIP ■ Packing the nose.
The “allergic salute,” seen in allergic
rhinitis—horizontal crease on the nose Allergic Rhinitis
that occurs from constant rubbing.
Definition
An IgE-mediated response to an allergen causing an inflammation of the
nasal mucous membranes.
Signs and Symptoms
WARD TIP
■ Generally does not develop until 2–3 years of age.
■ Sneezing.
Children with allergic rhinitis may exhibit
■ Watery nasal discharge.
rabbit-like nose wrinkling because of
■ Red, watery eyes.
pruritus.
■ Itchy ears, eyes, nose, and throat.
■ Nasal obstruction secondary to edema.
Diagnosis
Characteristic findings on physical exam:
WARD TIP ■ Boggy, bluish mucous membranes of the nose.
■ Dark circles under the lower eyelids (“allergic shiners”).
Allergic rhinitis in children may be a ■ Allergic salute (transverse nasal crease from rubbing and pushing the nose
precursor for the development of asthma.
up with your hand).
■ A smear of nasal secretions will show a high number of eosinophils.
Treatment
WARD TIP
■ Avoid triggers.
Fifty percent of children with choanal
■ Antihistamines.
■ Decongestants.
atresia have other associated congenital
■ Cromolyn nasal solution.
anomalies—
■ Topical steroids.
CHARGE syndrome:
Coloboma
Heart disease C h o ana l At r es i a
Atresia choanae
Retarded growth Definition
Genital anomalies ■ A separation of the nose and pharynx by a membrane or bone (90%); may
Ear involvement be unilateral or bilateral.
■ The most common congenital anomaly of the nose.
ch18.indd 440 26-08-2017 10:11:36
SPECIAL ORGANS—EYE, EAR, NOSE HIGH-YIELD FACTS IN 441
Signs and Symptoms
■ Each child’s presentation will differ depending on his or her ability to
mouth breathe.
■ Respiratory distress that improves as the child cries because the mouth is
open.
■ Cyanosis, especially when the child is feeding or sucking. Crying relieves the
cyanosis.
Diagnosis
■ Inability to pass a catheter through one or both nostrils.
■ CT will show the extent of the atresia.
Treatment
■ Prompt placement of an oral airway, maintaining the mouth in an open WARD TIP
position or intubation.
■ Maintaining an open airway by an orogastric tube or large nipple. Restenosis of corrected choanal atresia is
■ Tracheostomy or intubation may be required depending on the severity. common.
■ The ultimate treatment is surgical correction.
ch18.indd 441 26-08-2017 10:11:36
You might also like
- NCLEX SimpleNursing PediatricsDocument120 pagesNCLEX SimpleNursing PediatricsOlrac Agairdam100% (4)
- Survival - MCRP 3-02f FM 21-76Document571 pagesSurvival - MCRP 3-02f FM 21-76markdcoco690100% (4)
- Assignment Topic: Under The Supervision of Mam SehrishDocument18 pagesAssignment Topic: Under The Supervision of Mam SehrishAttarehman QureshiNo ratings yet
- Large ExotropiaDocument67 pagesLarge ExotropiaTri Kartika UtomoNo ratings yet
- The Authentic I Ching The Three Classic Methods of PredictionDocument4 pagesThe Authentic I Ching The Three Classic Methods of Predictionmaximo0% (1)
- Vision and Hearing Disorders FinalsDocument7 pagesVision and Hearing Disorders FinalsMary Reigns BuhatNo ratings yet
- Interactive Workbook - Design Habits That Last PDFDocument10 pagesInteractive Workbook - Design Habits That Last PDFjoseNo ratings yet
- Hernia QuestionsDocument6 pagesHernia QuestionsNica Lopez FernandezNo ratings yet
- Strategic Planning, Sales Strategy, Sales Forecasting, and BudgetingDocument18 pagesStrategic Planning, Sales Strategy, Sales Forecasting, and BudgetingMona AgarwalNo ratings yet
- Blurred Vision Headache: Hyperopia Myopia AstigmatismDocument4 pagesBlurred Vision Headache: Hyperopia Myopia Astigmatismraquel maniego100% (1)
- Dermatologic DiseaseDocument31 pagesDermatologic Diseaseعبدالسلام الأسمرNo ratings yet
- Days of Prayer and FastingDocument40 pagesDays of Prayer and FastingVictor saintNo ratings yet
- QHSE DashboardDocument5 pagesQHSE DashboardParure DoréeNo ratings yet
- Performing Physical Assessment of The EyeDocument14 pagesPerforming Physical Assessment of The Eyezyrine jhen100% (1)
- U10d2 CultureDocument4 pagesU10d2 Culturearhodes7770% (1)
- DARE's Eye PDFDocument33 pagesDARE's Eye PDFvirag.patilNo ratings yet
- F.A.T. Kee Computer Systems V Online Networks InternationalDocument2 pagesF.A.T. Kee Computer Systems V Online Networks InternationalJodi Anne AmoyoNo ratings yet
- Strabismus: Dr. Digin Mariam OphthalmologyDocument94 pagesStrabismus: Dr. Digin Mariam OphthalmologyVishnu SaiNo ratings yet
- Activity 1: Making A Simple Rapid Curriculum EvaluationDocument9 pagesActivity 1: Making A Simple Rapid Curriculum EvaluationShainnah Cawa75% (4)
- NCM 116 Ee Module 4Document18 pagesNCM 116 Ee Module 4Meryville JacildoNo ratings yet
- Refractive Errors Amblyopia SquintsDocument27 pagesRefractive Errors Amblyopia SquintssamxtraNo ratings yet
- Strabismus, Amblyopia & LeukocoriaDocument14 pagesStrabismus, Amblyopia & LeukocoriaMuhammad Naufal WidyatmakaNo ratings yet
- Eye ExaminationDocument34 pagesEye ExaminationSashwini DheviNo ratings yet
- L9 PediaDocument47 pagesL9 PediaNawaf AleanziNo ratings yet
- FIXXXXXXDocument35 pagesFIXXXXXXRani Dwi HapsariNo ratings yet
- EktropionDocument31 pagesEktropionapriliaNo ratings yet
- Ophthalmology - Optics and RefractionDocument10 pagesOphthalmology - Optics and RefractionjbtcmdtjjvNo ratings yet
- Geraitric Examination of EyeDocument37 pagesGeraitric Examination of Eyetanishqa eye careNo ratings yet
- Amblyopia, Astigmatism & HyperopiaDocument1 pageAmblyopia, Astigmatism & HyperopiaBaebee LouNo ratings yet
- NYSTAGMUSDocument13 pagesNYSTAGMUSwillemlrouxNo ratings yet
- Hyperopia & PresbyopiaDocument30 pagesHyperopia & PresbyopiaTalha UR RehmanNo ratings yet
- 07 Crossed Eyes Nystagmus and AmblyopiaDocument7 pages07 Crossed Eyes Nystagmus and AmblyopiaMwanja MosesNo ratings yet
- Ragay - Notes of EentDocument15 pagesRagay - Notes of Eentaynin39No ratings yet
- Neuro-Ophthalmology: Bethlehem Girma (M.D) Assistant Professor of OphthalmologyDocument117 pagesNeuro-Ophthalmology: Bethlehem Girma (M.D) Assistant Professor of Ophthalmologyhenok birukNo ratings yet
- 8 SquintDocument46 pages8 Squintwanderer_1010No ratings yet
- Assessment of The EyesDocument68 pagesAssessment of The EyesGemmalene PaclebNo ratings yet
- C 5Document9 pagesC 5Joy LayNo ratings yet
- StrabismusDocument19 pagesStrabismusSoumya Ranjan PandaNo ratings yet
- Congenital Optic Nerve Anomalies: Nandini Singh S.NO: 63 Roll No:68Document54 pagesCongenital Optic Nerve Anomalies: Nandini Singh S.NO: 63 Roll No:68nandini singhNo ratings yet
- Tatalaksana Awal Kegawatdaruratan Pada Mata - Dr. Nuke Erlina Mayasari, SPMDocument23 pagesTatalaksana Awal Kegawatdaruratan Pada Mata - Dr. Nuke Erlina Mayasari, SPMwahyu ardiNo ratings yet
- Childhood Eye DiseasesDocument5 pagesChildhood Eye DiseasesKeyien RadonesNo ratings yet
- Strabismus For Med VDocument102 pagesStrabismus For Med Vhenok birukNo ratings yet
- Day 9 STRABISMUS SquintDocument24 pagesDay 9 STRABISMUS Squint'Ema Surya PertiwiNo ratings yet
- DT StrabismusDocument42 pagesDT StrabismushamzahNo ratings yet
- Lecture 11 Special Senses Part 6-VisionDocument48 pagesLecture 11 Special Senses Part 6-VisionMoses Jr KazevuNo ratings yet
- Ankit Verma PHYSICSDocument11 pagesAnkit Verma PHYSICSANKIT VERMANo ratings yet
- Visual Faults and Their Correction: by Dhujana NsDocument20 pagesVisual Faults and Their Correction: by Dhujana NsRiniya NajeebNo ratings yet
- Lesson 1: Assessment of The EyesDocument3 pagesLesson 1: Assessment of The Eyesmeena jeerhNo ratings yet
- лекц 4Document39 pagesлекц 4A A D H INo ratings yet
- CN Name Type Function Testing Lesions/ResultsDocument5 pagesCN Name Type Function Testing Lesions/ResultsBen SarNo ratings yet
- Ophthalmology How To Examine An Eye: Visual AcuityDocument2 pagesOphthalmology How To Examine An Eye: Visual AcuityOlalekan OgundareNo ratings yet
- Gradual Loss of Vision-Nurses - 065937Document73 pagesGradual Loss of Vision-Nurses - 065937CosbyNo ratings yet
- 07 斜弱視Document72 pages07 斜弱視kenny631653No ratings yet
- P.E. - Eyes 2020 PDFDocument45 pagesP.E. - Eyes 2020 PDFAira Mae PenaredondoNo ratings yet
- InggrisDocument32 pagesInggrisRani Dwi HapsariNo ratings yet
- L3 - Strabismus, Amblyopia - LeukocoriaDocument20 pagesL3 - Strabismus, Amblyopia - LeukocoriaConger CongerNo ratings yet
- LangesDocument3 pagesLangesjeff.aufderheide2634No ratings yet
- Notes50 - PEDIATRIC VISION OR HEARING DISORDERSDocument9 pagesNotes50 - PEDIATRIC VISION OR HEARING DISORDERSTJ ZamarroNo ratings yet
- MEDSURG II (2nd Sem - ENDTERM NOTES)Document39 pagesMEDSURG II (2nd Sem - ENDTERM NOTES)Meryville JacildoNo ratings yet
- S3-03 Ophthalmology Acute Visual Loss PDFDocument10 pagesS3-03 Ophthalmology Acute Visual Loss PDFAl SyNo ratings yet
- Eyecare Review - : For Primary Care PractitionersDocument108 pagesEyecare Review - : For Primary Care PractitionersprilaviaramadhaniNo ratings yet
- E-Book Ophthalmology Referral Guide For GPsDocument11 pagesE-Book Ophthalmology Referral Guide For GPsnaravichandran3662No ratings yet
- Basic Neuro-Ophthalmology: Common Problems SeenDocument6 pagesBasic Neuro-Ophthalmology: Common Problems SeenMiguel C. DolotNo ratings yet
- Eyes Lecture 2Document4 pagesEyes Lecture 2Rue Cheng MaNo ratings yet
- Week 3 or 4 Eye Assessment Health AssessmentDocument34 pagesWeek 3 or 4 Eye Assessment Health Assessmentaabbccss1.z71No ratings yet
- Management of DiplopiaDocument5 pagesManagement of Diplopiacahyati syhrilNo ratings yet
- Health Assessment - Midterm - Assessing The EyesDocument4 pagesHealth Assessment - Midterm - Assessing The Eyesaina marie templonuevoNo ratings yet
- (OPT) 1.01 Eye Symptoms and Eye Examination Aclan v2Document14 pages(OPT) 1.01 Eye Symptoms and Eye Examination Aclan v2gprint1122No ratings yet
- Unit IV B. Physical AssessmentDocument116 pagesUnit IV B. Physical AssessmentJules Lorenz AbasoloNo ratings yet
- 3 - Refractive ErrorsDocument17 pages3 - Refractive ErrorsF ParikhNo ratings yet
- Salcedo Ha Cu 7 Adult Assessment Eyes 24Document69 pagesSalcedo Ha Cu 7 Adult Assessment Eyes 24shaimonteverdeNo ratings yet
- Endocrine DiseaseDocument38 pagesEndocrine Diseaseعبدالسلام الأسمرNo ratings yet
- Gastrointestinal DiseaseDocument36 pagesGastrointestinal Diseaseعبدالسلام الأسمرNo ratings yet
- Cardiovascular DiseaseDocument37 pagesCardiovascular Diseaseعبدالسلام الأسمرNo ratings yet
- Respiratory DiseaseDocument27 pagesRespiratory Diseaseعبدالسلام الأسمرNo ratings yet
- NutritionDocument14 pagesNutritionعبدالسلام الأسمرNo ratings yet
- Neurologic DiseaseDocument45 pagesNeurologic Diseaseعبدالسلام الأسمرNo ratings yet
- ToxicologyDocument78 pagesToxicologyعبدالسلام الأسمرNo ratings yet
- Ebook4Expert Ebook CollectionDocument157 pagesEbook4Expert Ebook CollectionandreaknsrNo ratings yet
- JudiciaryDocument21 pagesJudiciaryAdityaNo ratings yet
- Thinking ErrorDocument33 pagesThinking Errormohammad alaniziNo ratings yet
- Tenses MergedDocument76 pagesTenses MergedMihály Bence SzabóNo ratings yet
- Is Understanding Factive - Catherine Z. Elgin PDFDocument16 pagesIs Understanding Factive - Catherine Z. Elgin PDFonlineyykNo ratings yet
- ADL Audit of Anti-Semitic Incidents 2021Document38 pagesADL Audit of Anti-Semitic Incidents 2021Michael_Roberts2019No ratings yet
- Ielts Cracker: LeapscholarDocument10 pagesIelts Cracker: LeapscholarmobileNo ratings yet
- NP9 VISVAS 9am 3avarthies 24th NovDocument1 pageNP9 VISVAS 9am 3avarthies 24th Novkomala2447_157422965No ratings yet
- 7a - Alfa R CBT Training Certificate of CompletionDocument1 page7a - Alfa R CBT Training Certificate of Completionapi-355974373No ratings yet
- Field Strength MeterDocument9 pagesField Strength MeterVinod JagdaleNo ratings yet
- 3 Angels NepalDocument46 pages3 Angels Nepalविवेक शर्माNo ratings yet
- 08 08 The Picture of Dorian Gray 3and4ESO ENG TEACHER Telf2Document15 pages08 08 The Picture of Dorian Gray 3and4ESO ENG TEACHER Telf2Laura BabiciNo ratings yet
- Literature of Cagayan ValleyDocument30 pagesLiterature of Cagayan ValleyCara DonafrioNo ratings yet
- Designing Organizational Structure: Authority and ControlDocument48 pagesDesigning Organizational Structure: Authority and ControlArvind DawarNo ratings yet
- Cheiloscopy in Gender Determination: A Study On 2112 IndividualsDocument5 pagesCheiloscopy in Gender Determination: A Study On 2112 Individualsknr crsNo ratings yet
- 12th Bio Botany EM Important Questions English Medium PDF DownloadDocument7 pages12th Bio Botany EM Important Questions English Medium PDF DownloadPrase 1815No ratings yet
- Case Study ICM Solution For MindTreeDocument3 pagesCase Study ICM Solution For MindTreevinodNo ratings yet
- FileContent 9Document103 pagesFileContent 9Samadashvili ZukaNo ratings yet
- 09Document69 pages09Sakshi VermaNo ratings yet