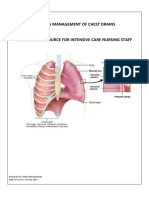
Professional Documents
Culture Documents
Chest Drain Management JAMA
Uploaded by
صقر قريشCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Chest Drain Management JAMA
Uploaded by
صقر قريشCopyright:
Available Formats
Clinical Review & Education
JAMA Surgery | Review
Comprehensive Review of Chest Tube Management
A Review
Devon Anderson, MD; Sarah A. Chen, MD, MA; Luis A. Godoy, MD; Lisa M. Brown, MD, MAS; David T. Cooke, MD
IMPORTANCE Thoracostomy, or chest tube placement, is used in a variety of clinical
indications and can be lifesaving in certain circumstances. There have been developments
and modifications to thoracostomy tubes, or chest tubes, over time, but they continue
to be a staple in the thoracic surgeon’s toolbox as well as adjacent specialties in medicine.
This review will provide the nonexpert clinician a comprehensive understanding of the types
of chest tubes, indications for their effective use, and key management details for ideal
patient outcomes.
OBSERVATIONS This review describes the types of chest tubes, indications for use, techniques
for placement, common anatomical landmarks that are encountered with placement and
management, and an overview of complications that may arise with tube thoracostomy. In
addition, the future direction of chest tubes is explored, as well as the management of chest
tubes during the COVID-19 pandemic. Author Affiliations: Division of
General Thoracic Surgery,
CONCLUSIONS AND RELEVANCE Chest tube management is subjective, but the compilation Department of Surgery, University of
of data can inform best practices and safe application to successfully manage the pleural California, Davis Health, Sacramento.
space and ameliorate acquired pleural space disease. Corresponding Author: David T.
Cooke, MD, University of California,
Davis Health, 2335 Stockton Blvd,
JAMA Surg. 2022;157(3):269-274. doi:10.1001/jamasurg.2021.7050 North Addition Office Building,
Published online January 26, 2022. Ste 6121, Sacramento, CA 95817-2214
(dtcooke@ucdavis.edu).
T
horacostomy tube, otherwise known as chest tube, trathoracic pressure, allowing the lung to reexpand and restore physi-
insertion can be traced back to the fifth century BCE when ologic ventilation and cardiac function.6-9 A tension pneumotho-
Hippocrates described using a hollow tin tube to drain rax develops when air enters on inspiration and is unable to escape
what was likely an empyema.1 In 1889, valved tubes with air-tight on expiration. This leads to effective mass effect on intrathoracic
seals were first reported to prevent outside atmospheric pressure structures, such as the lung itself; mediastinal structures, such as the
from collapsing the lung on inspiration.2 In 1922, chest tubes were venae cavae; and cardiac chambers, resulting in hemodynamic com-
first documented in the postoperative care of patients undergoing promise from restricted venous return and cardiac output. This is
modern thoracic surgery.3 They were used throughout World War II a medical emergency and should initially be managed with imme-
to restore lung function after traumatic thoracotomies, were used diate needle thoracentesis to decompress trapped and expanding
during the Korean War, and later became the standard of care for pleural air before the placement of a formal chest tube.
drainage of the pleural space for trauma during the Vietnam War.4 Chest tubes are also used to evacuate excessive fluid from the
Chest tubes and their management continue to evolve and are modi- pleural cavity, which is known as a pleural effusion. When there is
fied to fit modern needs, including clinical conditions associated pus in the pleural cavity, then it is considered an empyema. There
with the COVID-19 pandemic. are several ways to evacuate fluid from the pleural cavity and chest
tubes are only one of the many options. A Cochrane review from
201710 compared the surgical option of video-assisted thoracic sur-
gery (VATS) with chest tube drainage of pleural empyema and found
Indications
no difference in mortality or complications between the groups, but
The potential space between the visceral pleura that envelops the early VATS reduced the hospital length of stay. VATS has been con-
lungs and the parietal pleura covering the chest wall, diaphragm, and sidered the first-line treatment for retained hemothorax and em-
mediastinum is the pleural cavity, which contains lubricating pleu- pyemas with other modalities, such as intrapleural lytic therapy, re-
ral fluid secreted by the parietal pleural capillaries. Air and abnor- served for poor operative candidates or as a second line treatment.11
mal fluid can accumulate in this space, causing mass effect and dis- However, a meta-analysis by Hendriksen et al11 found that treating
ruptions in the normal negative intrathoracic pressure. retained hemothorax with lytic therapy rather than VATS allowed
When air fills the pleural cavity, it is called a pneumothorax, which for an overall operative avoidance rate of 87% (95% CI, 81%-92%),
is further categorized according to its etiology as primary sponta- with no heterogeneity in the pooled studies (Q = 10.2; df = 9; P = .33;
neous, secondary spontaneous, or traumatic.5-7 Chest tubes are used I2 = 15.07%). The type of intrapleural lytic treatment is also impor-
to evacuate air in the pleural cavity and reestablish the negative in- tant as Hendriksen et al11 found that using tissue plasminogen acti-
jamasurgery.com (Reprinted) JAMA Surgery March 2022 Volume 157, Number 3 269
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Jawaid Khan on 03/10/2022
Clinical Review & Education Review Chest Tube Management
Figure 1. Parapneumonic Effusions: University of California, Davis, Pulmonary
and General Thoracic Surgery Management Pathway
Parapneumonic effusion suspected; inpatient or being admitted from the ED; patient not in ICU
IP medicine consultationa
IP performs ultrasonography-guided thoracentesis; antibiotics Empiric chest
tube indicated
Intervention not indicated pH >7.20, No pus, culture pH ≤7.20, Pus, culture or
and Gram stain negative Gram stain positive
Antibiotics management
by primary team No chest tube
IP
Places chest tube (small-bore
pigtail recommended) within 24 h
Clinically responding after 48 h? Administers PA/DNAse twice a day, a
Pleural sepsis or Interventional pulmononologist (IP)
unsatisfactory radio- 3 times a day as indicated recommends thoracic surgery
graphic improvement
evaluation for late presentation
Yes No
(>7 d from index symptoms) plus
thick pleural rind or for very
Consult thoracic surgery after 72 h for: complex effusion. ED, emergency
Ongoing pleural sepsis department; ICU, intensive care
Management by primary team No Yes Unsatisfactory radiographic improvement
unit; PA, tissue plasminogen
activator.
vator (t-PA) as the lytic agent allowed for a favorable number of pa- Small-bore chest tubes are used as the first-line treatment for
tients to avoid surgical intervention compared with other lytic agents. pneumothorax, transudative pleural effusions, and simple empy-
The combination of t-PA and dornase (DNase) was associated with emas, whereas large-bore chest tubes are often necessary for more
a 60% reduction in pleural fluid collection as seen on imaging and viscous disease processes, such as a hemothorax and complex exu-
with a significant reduction in pleural opacity, compared with pla- dative effusions and empyemas.13,15 A meta-analysis by Chang et al5
cebo in the randomized clinical trial by Rahman et al.12 When t-PA demonstrated that small-bore chest tubes are associated with lower
and DNase were used on their own as opposed to in combination, complications rates and shorter drainage duration and hospital
this study did not find a significant reduction in the pleural fluid col- stay compared with large-bore chest tubes. A randomized clinical
lection compared with placebo.12 The evidence supports combin- trial by Hussain et al16 identified similar findings of a reduction in
ing t-PA and DNase for intrapleural lytic therapy. Given the effec- drainage duration and hospital stay with small-bore pigtail cath-
tiveness of treating early-phase empyema with a chest tube and eters compared with large-bore chest tubes in patients with sec-
intrapleural use of t-PA and DNase, as well as the use of VATS to re- ondary spontaneous pneumothorax. The most prominent advan-
duce length of hospital stay, the authors developed a multidisci- tage of a small-bore chest tube is its size, which allows for a smaller
plinary protocol with general thoracic surgery and interventional incision and decreased pain experienced by the patient.16,17 The
pulmonary medicine for the algorithmic care of patients present- randomized clinical trial by Kulvatunyou et al17 demonstrated a
ing with empyema, starting with a small-bore chest tube place- lower pain score in individuals with a pigtail catheter compared with
ment followed by intrapleural use of t-PA and DNase. If this initial a large-bore chest tube for traumatic pneumothorax. However, the
step is unsuccessful, the next stage of the pathway is thoracic small diameter of small-bore chest tubes may come at the cost of
surgical consultation for VATS decortication (Figure 1). inefficient flow, as per Poiseuille’s law (ΔP = 8μLQ/πR4, where Δp
is change in pressure, μ is viscosity, Q is flow and R is radius) the
decreasing radius of small-bore chest tubes can lend to a lower flow
rate, which is the reason large-bore chest tubes are necessary in con-
Types of Chest Tubes
ditions that would otherwise clog a smaller tube, such as high-
Chest tubes come in a variety of sizes and materials to best suit the viscosity (μ) fluid.5,13,15
clinical needs of the patient. In the US, they are generally measured
by the internal diameter of the tube in units of French. One incre-
ment of the French scale is equal to a one-third–millimeter diameter,
Insertion
(eg, 24F is equal to an 8-mm caliber). By most prevalent convention,
a tube of 20F or larger is considered a large-bore chest tube and a tube The placement of a chest tube is important and is performed by many
less than 20F tube is considered a small-bore chest tube, although different specialties in various settings. The ideal point of insertion
there are some studies that define a large-bore chest tube as larger is through an external landmark space known as the triangle of safety
than 14F.5,13,14 A common type of small-bore chest tube is a pigtail (Figure 2), which is bordered by the edge of the latissimus dorsi
catheter, named because the tip coils at the end like a pig’s tail to pre- muscle, pectoralis major muscle, the base of the axilla, and trans-
vent dislodgement.13 verse to the nipple line or inframammary fold, at or above the fifth
270 JAMA Surgery March 2022 Volume 157, Number 3 (Reprinted) jamasurgery.com
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Jawaid Khan on 03/10/2022
Chest Tube Management Review Clinical Review & Education
Figure 2. Triangle of Safety for Chest Tube Placement Figure 3. Representative Sonographic Image Demonstrating
the Target Abnormal Collection of Pleural Fluid
Diaphragm
Edge of pectoralis major muscle
Base of axilla
Collapsed lung
Edge of latissimus dorsi muscle
Fifth intercostal space
Liver
30°-60° Angle Pleural
fluid
intercostal space.13,14,18-20 However, placement of chest tubes is also
influenced by the indication. For an apical pneumothorax, a chest
tube can be placed in the second intercostal space in the midcla-
vicular line, although less comfortable for the patient, and ad-
equate drainage of an unloculated pneumothorax can be per-
formed via lateral insertion at the fifth intercostal space.14,18 If the
tube is placed in the triangle of safety, it is important to place it in a lead to small vessel disruption and subsequently hemothorax.13,14
line anterior to the anterior superior iliac spine. Placing in the tube The Seldinger technique uses guidewires and tract dilators to as-
in a line behind this surface landmark may cause the patient to lie sist the tube into the pleural cavity, all under ultrasonography
on the tube when in the supine position and mechanically occlude guidance.19,21 Lastly, the trocar method may be used; however, it is
the tube. For a pleural effusion, a lower intercostal space may be used associated with more complications owing to the rigid tip of the tro-
for insertion but special care must be taken to avoid penetrating the car causing intrathoracic injuries and has subsequently fallen out of
diaphragm, and subsequently the liver on the right and spleen and favor for chest tube insertion.19,20,22 Regardless of the insertion tech-
bowel on the left.13 nique, the chest tube needs to be advanced on the superior edge
The 3 ways to insert a chest tube are dissective, Seldinger of the rib to avoid the neurovascular bundle bordering the rib
(often ultrasonography guided), and the trocar technique, again above.13,14 It should also be positioned posteriorly and advanced un-
often ultrasonography guided.13,14,19,20 Ultrasonography can be an til the tip is in a posteroapical location. The tube should also be fully
invaluable tool to safely identify internal landmarks for chest tube inserted to ensure that the most proximal (sentinel) hole is within
placement. Figure 3 presents a representative sonographic image the pleural space to allow the chest tube to function properly.14 Lastly,
demonstrating the target abnormal collection of pleural fluid, in the it is important to secure the chest tube with a suture to prevent it
right chest, for chest tube drainage, and adjacent structures of at- from falling out. Most tubes can be removed without suture skin
electatic lung, diaphragm and liver. Figure 4A highlights an impor- closure, but in children and adults with very low body mass index
tant step for chest tube placement, which is using a finder needle (calculated as weight in kilograms divided by height in meters
(often a syringe with local anesthetic) just above the target rib to squared), placement of an untied adjunctive chest tube suture at the
avoid the intercostal neurovascular bundle and aspirating the pleu- time of insertion allows for closure of skin defects at the time of tube
ral space to confirm the location of the pleural pathology. For dis- removal, especially large-bore tubes, to prevent entraining atmo-
sective insertion, a 1- to 2-cm incision is made overlying the rib of spheric air with tube removal.
choice (the authors do not tunnel to a rib above), a Schnidt tonsil
clamp is used to bluntly dissect through the subcutaneous tissue,
the 3 muscular layers of the intercostal space (ie, the external inter-
costal muscle, the internal intercostal muscle, and innermost inter-
Management
costal muscle), transthoracic fascia, and the parietal pleural until the Once a chest tube is placed, it is connected to a drainage device,
clamp enters the pleural cavity. When attempting to enter the fifth which, like the chest tube itself, has evolved over the years. The first
intercostal space, it is important to dissect not perpendicular to the rendition was a 1-compartment system reported by Playfair23 in 1875,
chest wall, but generally posterior and apical, the direction that most which used a 1-way valve to allow air to egress from the pleural cav-
tubes should be placed (Figure 4B). Dissecting perpendicular to the ity during expiration without returning on inspiration. In 1926,
chest wall and into the fifth intercostal space can lead to the tube Lilienthal24 developed a 2-compartment system, which allowed the
heading directly into the oblique fissure, and then be entrapped by accumulation of fluid in the first collection bottle without compro-
the subsequent expanded lung, rendering the tube ineffective af- mising the efficiency of the system and its ability to drain, as would
ter lung expansion. After successful spreading into the pleura space, have been observed in the first model. Then, the 3-compartment
a finger is used to confirm entry into the pleural space and the pres- system emerged in 1952 with Howe, which allowed collection, wa-
ence of adhesions. Adhesions are not bluntly broken with the fin- ter sealing, and suction and manometer capabilities that are com-
ger, as pleural adhesions are often vascular and blunt dissection can bined into a single pleural drainage unit (PDU).19,25 This forms the
jamasurgery.com (Reprinted) JAMA Surgery March 2022 Volume 157, Number 3 271
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Jawaid Khan on 03/10/2022
Clinical Review & Education Review Chest Tube Management
Figure 4. Insertion Technique
A Tube placement over target rib B Posterior and apical tube placement
foundation of the modern PDU devices today, some of which are ing suction over water seal for both postthoracic surgery patients
digitally operated. and traumatic chest injury patients, until resolution of air leak.
Once placed, chest tubes may be attached to a PDU and set to
active suction or to water seal, which is simple dependent drain-
age. The phrase “place a chest tube on water seal” is a misnomer, as
Removal
modern PDUs have a constitutive water seal chamber that serves
as a 1-way valve, preventing air from returning into the pleural space; There are many factors that come into play when determining the
placing a chest tube on water seal simply means taking the tube correct time to remove a chest tube. The quality of the fluid should
off active suction. The randomized clinical trial by Cerfolio et al26 be free of chyle, or blood suggestive of active bleeding, and be
found that water sealing the chest tube on postoperative day 2 af- nonpurulent.31,32 However, the quantity of fluid that is acceptable
ter thoracic surgery resulted in a significant resolution of small air before the removal of a chest tube is without consensus, with vary-
leak the following day, with the authors noting that large air leaks ing recommended volume thresholds ranging from 200 mL per day
do not benefit from water sealing. Another randomized clinical trial27 to 500 mL per day.31-33 Cerfolio et al32 performed a retrospective
demonstrated similar results of a shorter duration of air leak with cohort analysis that demonstrated that chest tube removal up to
early water sealing for postthoracic surgery chest tubes, which 450 mL per day was acceptable in patients who underwent elec-
subsequently decreased the duration the chest tube was needed. tive pulmonary resection. They reported that 364 of 1988 patients
Both of these studies, albeit randomized clinical trials, are limited (18%) were able to go home sooner owing to surgeons changing to
by their small sample sizes. Brunelli et al28 performed a random- the higher threshold (450 mL per day) and only 11 patients (0.55%)
ized clinical trial with a larger sample size, did not find an advan- were readmitted as a result of a recurrent symptomatic effusion.
tage with water seal over suction for postthoracic surgery patients Grodzki et al34 tested this conclusion a year later and removed chest
and the authors favor a hybrid approach of moderate suction over- tubes at the higher threshold of 450 mL per day and found that 6
night and water sealing during the day to allow for mobilization of of 40 patients (15%) were readmitted with pleural effusions, thus
the patient. The systematic review and meta-analysis by Coughlin leading the authors to revert to their original practice of following a
et al29 determined that there was no advantage of suction over wa- threshold of 200 mL per day for chest tube removal. The limitation
ter seal after thoracic surgery, with the exception of suction being in the former study is the lack of reliable follow-up, which could ac-
superior to water seal in preventing a radiographic identification of count for the low readmission rate, and the limitation in the latter
pneumothoraces. study is the small sample size. Larger randomized clinical trials would
For patients with a traumatic chest injury, the systemic review be helpful in clarifying this gap in our understanding.
and meta-analysis by Feenstra et al9 demonstrated evidence that Whether to remove the chest tube at the end of expiration or
favors low-pressure suction over water seal. This meta-analysis is inspiration is another question that has been widely debated. No-
limited in the number of studies, and therefore patient sample voa et al31 recommended removing the chest tube at the end of ex-
size, included. In addition, there are few patients with chest tubes piration during a Valsalva maneuver, which corresponds to the time
in the setting of mechanical ventilation included in this study, which when the difference between the atmospheric pressure and pleu-
is an important subset of trauma patients. Patients who have an ral pressure is at its lowest.31 Other studies, such as French et al,35
occult pneumothorax and are receiving positive pressure mechani- emphasized the importance of a Valsalva maneuver during chest tube
cal ventilation are at risk of developing a tension pneumothorax, removal regardless of the respiratory phase in which it is removed.
therefore it may be necessary for a chest tube to be placed on suc- The chest tube should be removed swiftly and the defect in the chest
tion in this subset of patients.30 Overall, the management of a chest wall should be closed with either a suture that was placed at the time
tube depends on the indication for insertion with evidence favor- of chest tube placement or with a properly occlusive dressing.
272 JAMA Surgery March 2022 Volume 157, Number 3 (Reprinted) jamasurgery.com
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Jawaid Khan on 03/10/2022
Chest Tube Management Review Clinical Review & Education
Complications Future Directions
The retrospective review by Platnick et al36 found that certain risk More recent studies are leaning toward conservative management in
factors, such as chest tube placement in the emergency depart- some specific pleural disease processes. The randomized clinical trial
ment, placement by emergency medicine clinicians, and place- by Hallifax et al41 demonstrated that the use of ambulatory devices
ment in patients with a body mass index greater than 30 were all for the treatment of primary spontaneous pneumothorax compared
associated with chest tube complications. However, the exact com- with usual care, which included aspiration or chest tube insertion, was
plication rate associated with chest tubes is variable and has been associated with a significantly shorter hospital length of stay. These
quoted as high as 40%.36-38 The variability in the reported compli- findings suggest that this subset of patients can be treated in an out-
cation rate can be attributed to a lack of a universally accepted way patient setting and that ambulatory devices should be considered as
to categorize the many different complications. Aho et al20 pro- an effective treatment strategy for this disease process. However,
posed a way to standardize the reporting of complications surround- there was an increase in the number of adverse events associated with
ing chest tubes to allow for easier recording and collection of data. the treatment with ambulatory devices, including enlarging pneu-
The 5 complication categories proposed were insertional, posi- mothorax and problems associated with the device, such as kinking
tional, removal, infectious, and malfunction. Insertional complica- or dislodgement, which will require more research if this approach is
tions include injury to intrathoracic or extrathoracic organs within going to replace the current standard of care.
24 hours of insertion, which is a complication most common with In a study by Brown et al,42 conservative treatments, such as ob-
chest tubes being inserted via the trocar technique.19,20 Positional servation of moderate- to large-sized primary spontaneous pneumo-
complications are defined as occurring 24 hours after insertion, in- thorax, were found to be noninferior to the placement of a small-bore
cluding erosions into adjacent organs or any tube kinking, obstruc- chest tube regarding resolution of the pneumothorax within 8 weeks.
tion, or being entrapped in the fissure after lung expansion.19,20 The study reports that 118 of 125 patients (94%) of patients undergo-
Removal complications encompass failure to seal the chest defect ing conservative management did not require an invasive procedure,
after the chest tube is removed, resulting in entraining atmo- thus challenging the paradigm that all patients with a hemodynamic
spheric air, or the retention of any foreign objects after removal.20 andrespiratorystableprimarypneumothoraxshouldroutinelyundergo
Infectious complications involve any infection, either external from decompression with a chest tube as the first treatment option.
improper sterilizing techniques or internal with the development The routine placement of a chest tube after thoracic surgery is an-
of an empyema.20 Malfunction complications include problems other area with emerging research. The randomized clinical trial by
that may arise from the health care clinician managing the chest tube Zhang et al43 showed that the placement of a novel air-extraction
or equipment issues.20 Defining complications in these distinct double-lumencatheterwasnoninferiortotheplacementofatraditional
categories allows clinicians to create a foundation to compare data chest tube in the incidence of a pneumothorax on postoperative day
collected in future studies and protocols to reduce the risk of com- 1. The use of this air-extraction catheter was also associated with a sig-
plication associated with chest tubes. nificantly lower patient-reported pain score, which supports the argu-
ment that more conservative techniques can be used to optimize
patient comfort without compromising clinical outcomes.
COVID-19
Chest tube management during the COVID-19 pandemic, or any
Conclusions
future coronavirus or H1N1 pandemic, is challenging owing to the
risk of aerosolizing dangerous virions. Proper personal protective With the advancement of technology and the push toward less in-
equipment, minimizing water seal, and using filters to decrease vasive approaches, the treatment of pleural conditions that were
the number of aerosolized particles escaping into the air are modi- once managed solely by chest tubes continues to evolve. However,
fications that have been implemented in many intensive care units chest tubes are likely to continue to be a vital part of a clinician’s rep-
around the world.37,39 A small observational cohort study40 found ertoire as they are still considered the standard of care for certain
that connecting 2 closed underwater drainage systems in series pleural disease processes and life-saving devices in others. It is im-
with an air filter attached to the second system was associated with perative that trainees have a solid foundation on the management
a decrease in the dissemination of coronavirus particles, as evi- of chest tubes, as their use is a dynamic process that will continue
denced by a lack of COVID-19 infection reported in their health care to change as time progresses. This review highlights the studies that
workers during the study. However, this study was limited with its have shaped the way chest tubes are managed today and allows the
small power. reader to develop and cultivate their understanding.
ARTICLE INFORMATION during the conduct of the study. No other 2. Williams W. Treatment of empyema by a valvular
Accepted for Publication: October 22, 2021. disclosures were reported. tube hermetically sealed to the chest. Br Med J.
1889;1(1481):1107-1108. doi:10.1136/bmj.1.1481.1107
Published Online: January 26, 2022. REFERENCES
doi:10.1001/jamasurg.2021.7050 3. Lilienthal H. Resection of the lung for
1. Hippocrates. The Genuine Works of Hippocrates. suppurative infections with a report based on
Conflict of Interest Disclosures: Dr Brown Adams F, trans-ed. Sydenham Society; 1849. 31 operative cases in which resection was done or
reported grants from National Institutes of Health
jamasurgery.com (Reprinted) JAMA Surgery March 2022 Volume 157, Number 3 273
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Jawaid Khan on 03/10/2022
Clinical Review & Education Review Chest Tube Management
intended. Ann Surg. 1922;75(3):257-320. 17. Kulvatunyou N, Erickson L, Vijayasekaran A, resection with high output. J Thorac Cardiovasc Surg.
doi:10.1097/00000658-192203000-00001 et al. Randomized clinical trial of pigtail catheter 2008;135(2):269-273. doi:10.1016/j.jtcvs.2007.
4. Monaghan SF, Swan KG. Tube thoracostomy: the versus chest tube in injured patients with 08.066
struggle to the “standard of care”. Ann Thorac Surg. uncomplicated traumatic pneumothorax. Br J Surg. 33. Younes RN, Gross JL, Aguiar S, Haddad FJ,
2008;86(6):2019-2022. doi:10.1016/j.athoracsur. 2014;101(2):17-22. doi:10.1002/bjs.9377 Deheinzelin D. When to remove a chest tube?
2008.08.006 18. Venuta F, Diso D, Anile M, Rendina EA, a randomized study with subsequent prospective
5. Chang S-H, Kang Y-N, Chiu H-Y, Chiu Y-H. Onorati I. Chest tubes: generalities. Thorac Surg Clin. consecutive validation. J Am Coll Surg. 2002;195(5):
A systematic review and meta-analysis comparing 2017;27(1):1-5. doi:10.1016/j.thorsurg.2016.08.001 658-662. doi:10.1016/S1072-7515(02)01332-7
pigtail catheter and chest tube as the initial 19. Munnell ER. Thoracic drainage. Ann Thorac Surg. 34. Grodzki T. Prospective algorithm to remove
treatment for pneumothorax. Chest. 2018;153(5): 1997;63(5):1497-1502. doi:10.1016/S0003-4975(97) chest tubes after pulmonary resection with high
1201-1212. doi:10.1016/j.chest.2018.01.048 00082-9 output—is it valid everywhere? J Thorac Cardiovasc
6. Graham EA, Bell RD. Open pneumothorax: its 20. Aho JM, Ruparel RK, Rowse PG, Surg. 2008;136(2):536. doi:10.1016/j.jtcvs.2008.
relation to the treatment of empyema. Am J Med Sci. Brahmbhatt RD, Jenkins D, Rivera M. Tube 04.017
1918; 156 (6): 839-871. doi:10.1097/00000441- thoracostomy: a structured review of case 35. French DG, Dilena M, LaPlante S, et al.
191812000-00007 reports and a standardized format for reporting Optimizing postoperative care protocols in thoracic
7. MacDuff A, Arnold A, Harvey J; BTS Pleural complications. World J Surg. 2015;39(11): surgery: best evidence and new technology.
Disease Guideline Group. Management of 2691-2706. doi:10.1007/s00268-015-3158-6 J Thorac Dis. 2016;8(suppl 1):S3-S11.
spontaneous pneumothorax: British Thoracic 21. Seldinger SI. Catheter replacement of the 36. Platnick C, Witt CE, Pieracci FM, et al.
Society pleural disease guideline 2010. Thorax. needle in percutaneous arteriography; a new Beyond the tube: can we reduce chest tube
2010;65(suppl 2):ii18-ii31. doi:10.1136/thx.2010. technique. Acta radiol. 1953;39(5):368-376. complications in trauma patients? Am J Surg. Am J
136986 doi:10.3109/00016925309136722 Surg. 2021;222(5):1023-1028. doi:10.1016/j.
8. Wolcott MW, Shaver WA, Jennings WD. 22. John M, Razi S, Sainathan S, Stavropoulos C. amjsurg.2021.04.008
Spontaneous pneumothorax. Management by tube Is the trocar technique for tube thoracostomy safe 37. Pieracci FM, Burlew CC, Spain D, et al. Tube
thoracostomy and suction. Dis Chest. 1963;43(1): in the current era? Interact Cardiovasc Thorac Surg. thoracostomy during the COVID-19 pandemic:
78-81. doi:10.1378/chest.43.1.78 2014;19(1):125-128. doi:10.1093/icvts/ivu071 guidance and recommendations from the AAST
9. Feenstra TM, Dickhoff C, Deunk J. Systematic 23. Playfair WS. Thoracentesis in empyema. Br Med Acute Care Surgery and Critical Care Committees.
review and meta-analysis of tube thoracostomy J. 1872;1(593):498-498. doi:10.1136/bmj.1.593. Trauma Surg Acute Care Open. 2020;5(1):e000498.
following traumatic chest injury; suction versus 498-a doi:10.1136/tsaco-2020-000498
water seal. Eur J Trauma Emerg Surg. 2018;44(6): 24. Lilienthal H. Thoracic Surgery. Saunders; 1926. 38. Hernandez MC, El Khatib M, Prokop L,
819-827. doi:10.1007/s00068-018-0942-7 Zielinski MD, Aho JM. Complications in tube
25. Toth JW, Reed MF, Ventola LK. Chest tube thoracostomy: systematic review and
10. Redden MD, Chin TY, van Driel ML. Surgical drainage devices. Semin Respir Crit Care Med. 2019;
versus non-surgical management for pleural meta-analysis. J Trauma Acute Care Surg. 2018;85
40(3):386-393. doi:10.1055/s-0039-1694769 (2):410-416. doi:10.1097/TA.0000000000001840
empyema. Cochrane Database Syst Rev.2017;3(3):
CD010651. doi:10.1002/14651858.CD010651.pub2 26. Cerfolio RJ, Bass C, Katholi CR. Prospective 39. Dhanasopon AP, Zurich H, Preda A. Chest tube
randomized trial compares suction versus water drainage in the age of COVID-19. Physician Assist Clin.
11. Hendriksen BS, Kuroki MT, Armen SB, Reed MF, seal for air leaks. Ann Thorac Surg. 2001;71(5):
Taylor MD, Hollenbeak CS. Lytic therapy for 2021;6(2):261-265. doi:10.1016/j.cpha.2020.11.011
1613-1617. doi:10.1016/S0003-4975(01)02474-2
retained traumatic hemothorax: a systematic 40. Gedik İE, Alar T. Protective measures
review and meta-analysis. Chest. 2019;155(4): 27. Marshall MB, Deeb ME, Bleier JIS, et al. undertaken during chest tube thoracostomy in
805-815. doi:10.1016/j.chest.2019.01.007 Suction vs water seal after pulmonary resection: COVID-19 outbreak. Indian J Thorac Cardiovasc Surg.
a randomized prospective study. Chest. 2002;121 2020;37(2):1-4.
12. Rahman NM, Maskell NA, West A, et al. (3):831-835. doi:10.1378/chest.121.3.831
Intrapleural use of tissue plasminogen activator and 41. Hallifax RJ, McKeown E, Sivakumar P, et al.
DNase in pleural infection. N Engl J Med. 2011;365 28. Brunelli A, Monteverde M, Borri A, et al. Ambulatory management of primary spontaneous
(6):518-526. doi:10.1056/NEJMoa1012740 Comparison of water seal and suction after pneumothorax: an open-label, randomised
pulmonary lobectomy: a prospective, randomized controlled trial. Lancet. 2020;396(10243):
13. Cooke DT, David EA. Large-bore and small-bore trial. Ann Thorac Surg. 2004;77(6):1932-1937.
chest tubes: types, function, and placement. Thorac 39-49. doi:10.1016/S0140-6736(20)31043-6
doi:10.1016/j.athoracsur.2003.12.022
Surg Clin. 2013;23(1):17-24, v. doi:10.1016/j. 42. Brown SGA, Ball EL, Perrin K, et al; PSP
thorsurg.2012.10.006 29. Coughlin SM, Emmerton-Coughlin HM, Investigators. Conservative versus interventional
Malthaner R. Management of chest tubes after treatment for spontaneous pneumothorax. N Engl J
14. Filosso PL, Guerrera F, Sandri A, et al. Errors and pulmonary resection: a systematic review and
complications in chest tube placement. Thorac Surg Med. 2020;382(5):405-415. doi:10.1056/
meta-analysis. Can J Surg. 2012;55(4):264-270. NEJMoa1910775
Clin. 2017;27(1):57-67. doi:10.1016/j.thorsurg.2016. doi:10.1503/cjs.001411
08.009 43. Zhang J-T, Dong S, Chu X-P, et al. Randomized
30. Enderson BL, Abdalla R, Frame SB, Casey MT, trial of an improved drainage strategy versus
15. Liu Y-H, Lin Y-C, Liang S-J, et al. Gould H, Maull KI. Tube thoracostomy for occult
Ultrasound-guided pigtail catheters for drainage of routine chest tube after lung wedge resection. Ann
pneumothorax: a prospective randomized study Thorac Surg. 2020;109(4):1040-1046. doi:10.1016/
various pleural diseases. Am J Emerg Med. 2010;28 of its use. J Trauma. 1993;35(5):726-729.
(8):915-921. doi:10.1016/j.ajem.2009.04.041 j.athoracsur.2019.11.029
doi:10.1097/00005373-199311000-00013
16. Hussein RMM, Elshahat HM, Shaker A, 31. Novoa NM, Jiménez MF, Varela G. When to
Hashem AZA. Study of pigtail catheter and chest remove a chest tube. Thorac Surg Clin. 2017;27(1):
tube in management of secondary spontaneous 41-46. doi:10.1016/j.thorsurg.2016.08.007
pneumothorax. Egypt J Chest Dis Tuberc. 2017;66
(1):107-114. doi:10.1016/j.ejcdt.2016.08.011 32. Cerfolio RJ, Bryant AS. Results of a prospective
algorithm to remove chest tubes after pulmonary
274 JAMA Surgery March 2022 Volume 157, Number 3 (Reprinted) jamasurgery.com
© 2022 American Medical Association. All rights reserved.
Downloaded From: https://jamanetwork.com/ by Jawaid Khan on 03/10/2022
You might also like
- Anesthetic Management in Pediatric General Surgery: Evolving and Current ConceptsFrom EverandAnesthetic Management in Pediatric General Surgery: Evolving and Current ConceptsSusan T. VergheseNo ratings yet
- Are Chest Radiographs Routinely Indicated After Chest Tubes Placed For Non-Surgical Reasons Are Removed?Document9 pagesAre Chest Radiographs Routinely Indicated After Chest Tubes Placed For Non-Surgical Reasons Are Removed?jeremy joshuaNo ratings yet
- Principles and Practice of Lacrimal SurgeryFrom EverandPrinciples and Practice of Lacrimal SurgeryMohammad Javed AliNo ratings yet
- Academic Emergency Medicine - 2008 - Givens - Needle Thoracostomy Implications of Computed Tomography Chest Wall ThicknessDocument5 pagesAcademic Emergency Medicine - 2008 - Givens - Needle Thoracostomy Implications of Computed Tomography Chest Wall Thicknessdr.gergely.halaszNo ratings yet
- Normal and Pathological Bronchial Semiology: A Visual ApproachFrom EverandNormal and Pathological Bronchial Semiology: A Visual ApproachPierre Philippe BaldeyrouNo ratings yet
- Tracheostomy in Palliative CaraDocument9 pagesTracheostomy in Palliative CarameritaNo ratings yet
- Chest Drain Size Does It MatterDocument6 pagesChest Drain Size Does It MatterQamarAhmadNo ratings yet
- Chest Tube Insertion: Colleen Fitzpatrick, MD, and Karen J. Brasel, MD, MPH, FACSDocument5 pagesChest Tube Insertion: Colleen Fitzpatrick, MD, and Karen J. Brasel, MD, MPH, FACSenviNo ratings yet
- Postoperative Chest Tube Management For Patients Undergoing Lobectomy: Evidence-Based PracticeDocument3 pagesPostoperative Chest Tube Management For Patients Undergoing Lobectomy: Evidence-Based PracticeAEGEL DARO TORRALBANo ratings yet
- Autologous Blood Patch Pleurodesis: A Large Retrospective Multicenter Cohort StudyDocument7 pagesAutologous Blood Patch Pleurodesis: A Large Retrospective Multicenter Cohort StudySabri AbyNo ratings yet
- Pediatric Anesthesia - 2022 - Weatherall - Developing An Extubation Strategy For The Difficult Pediatric Airway Who WhenDocument8 pagesPediatric Anesthesia - 2022 - Weatherall - Developing An Extubation Strategy For The Difficult Pediatric Airway Who WhenPamela Mamani FloresNo ratings yet
- Minimally Invasive Thoracic Surgery ArticleDocument9 pagesMinimally Invasive Thoracic Surgery ArticleLEONEL ALFREDO GUILLEN MARINNo ratings yet
- Research Paper On PneumothoraxDocument7 pagesResearch Paper On Pneumothoraxgz8xbnex100% (1)
- Occult Pneumothorax in Patients Presenting With Blunt Chest Trauma: An Observational AnalysisDocument10 pagesOccult Pneumothorax in Patients Presenting With Blunt Chest Trauma: An Observational AnalysisAnangova PradiptaNo ratings yet
- Primary Thoracoscopic Treatment of Empyema in Children: General Thoracic SurgeryDocument6 pagesPrimary Thoracoscopic Treatment of Empyema in Children: General Thoracic SurgeryDr Nilesh NagdeveNo ratings yet
- The Management of Subcutaneous Emphysema in Pneumothorax: A Literature ReviewDocument6 pagesThe Management of Subcutaneous Emphysema in Pneumothorax: A Literature ReviewVivian FatharaniNo ratings yet
- Early and Persistent Hemothorax and PneumothoraxDocument7 pagesEarly and Persistent Hemothorax and Pneumothoraxtri_budi_20No ratings yet
- 05 N156 31823Document26 pages05 N156 31823tanmai nooluNo ratings yet
- 1 s2.0 S1836955319301262 Main PDFDocument8 pages1 s2.0 S1836955319301262 Main PDFAdilson Skalski ZabielaNo ratings yet
- Clamping Trials Prior To Thoracostomy Tube Removal and The Need For Subsequent Invasive Pleural DrainageDocument6 pagesClamping Trials Prior To Thoracostomy Tube Removal and The Need For Subsequent Invasive Pleural Drainagelutfor rahmanNo ratings yet
- JournalDocument5 pagesJournalKhumaira SantaNo ratings yet
- 1 s2.0 S002571251830172XDocument11 pages1 s2.0 S002571251830172XAndiie ResminNo ratings yet
- The Management of Subcutaneous Emphysema in PneumoDocument7 pagesThe Management of Subcutaneous Emphysema in PneumoRobert ChristevenNo ratings yet
- H2A019109 - Annisa R.A Putri - Last StepDocument8 pagesH2A019109 - Annisa R.A Putri - Last Step109 -Annisa RANo ratings yet
- OLV Protectora No Sirve?Document15 pagesOLV Protectora No Sirve?CristianMedranoVargasNo ratings yet
- Edwardus T. Adar 1308012050: Consultant Dr. Stef D. Soka, SP.BDocument21 pagesEdwardus T. Adar 1308012050: Consultant Dr. Stef D. Soka, SP.BAlbert RanggaNo ratings yet
- Literature Review Tension PneumothoraxDocument7 pagesLiterature Review Tension Pneumothoraxc5kgkdd4100% (1)
- The Changing Role For Tracheostomy in Patients Requiring Mechanical VentilationDocument11 pagesThe Changing Role For Tracheostomy in Patients Requiring Mechanical VentilationGhost11mNo ratings yet
- 1k0g01aDocument6 pages1k0g01aCarlos Manuel Cadena PuertasNo ratings yet
- Wa0139 PDFDocument12 pagesWa0139 PDFPaula SouzaNo ratings yet
- s44215 023 00094 7Document5 pagess44215 023 00094 7charlaayasyafefiNo ratings yet
- Chest Drains Learning ResourceDocument22 pagesChest Drains Learning ResourceSiriporn TalodkaewNo ratings yet
- Journal Reading Marsya Y. Loppies (201283003)Document9 pagesJournal Reading Marsya Y. Loppies (201283003)joions gilberth oppiesNo ratings yet
- Evaluation and Management of The Physiologically.16Document11 pagesEvaluation and Management of The Physiologically.16alveteNo ratings yet
- Rib Fixation Who What WhenDocument5 pagesRib Fixation Who What Whenfatimah putriNo ratings yet
- Assessment of Pulmonary Edema: Principles and PracticeDocument14 pagesAssessment of Pulmonary Edema: Principles and PracticeJeanPandieNo ratings yet
- Congenital Diaphragmatic HerniaDocument4 pagesCongenital Diaphragmatic HerniaJulio AltamiranoNo ratings yet
- Tracheostomy Management During The COVID-19 PandemicDocument3 pagesTracheostomy Management During The COVID-19 Pandemicika lestariNo ratings yet
- Wiring CostaDocument4 pagesWiring CostaKulo YitnoNo ratings yet
- CDH Modern MX PDFDocument12 pagesCDH Modern MX PDFThia SanjayaNo ratings yet
- Close, OpenDocument7 pagesClose, OpenNoeRhul M-lhati OelfhaNo ratings yet
- Classification System Improves Management of Open Abdomen PatientsDocument4 pagesClassification System Improves Management of Open Abdomen PatientsFlipNo ratings yet
- A Diff Erent Approach To Chest Tube Drainage After Cardiac Surgery: A Study On The Usage of A Single Versus Separate Drain VialsDocument4 pagesA Diff Erent Approach To Chest Tube Drainage After Cardiac Surgery: A Study On The Usage of A Single Versus Separate Drain VialsAldo AtjehNo ratings yet
- Surgical Management of Parapharyngeal AbscessDocument3 pagesSurgical Management of Parapharyngeal AbscessmeyNo ratings yet
- Damage Control Laparotomy and Management of The Open AbdomenDocument12 pagesDamage Control Laparotomy and Management of The Open AbdomenpipeudeaNo ratings yet
- International Journal of Surgery Case ReportsDocument5 pagesInternational Journal of Surgery Case ReportschrisantyNo ratings yet
- Intraoperative Protective Mechanical Ventilation Fact or FictionDocument3 pagesIntraoperative Protective Mechanical Ventilation Fact or Fictionema moralesNo ratings yet
- Thoracotomy and Decortication OutcomeDocument6 pagesThoracotomy and Decortication OutcomecemNo ratings yet
- Giant Pulmonary Bullae in Children: Journal of Pediatric Surgery Case Reports July 2020Document7 pagesGiant Pulmonary Bullae in Children: Journal of Pediatric Surgery Case Reports July 2020SOPHIASTIA KUSBIANTI MHS 2017No ratings yet
- Thoracoscopic Pulmonary Wedge Resection Without Post-OperativeDocument6 pagesThoracoscopic Pulmonary Wedge Resection Without Post-Operativelutfor rahmanNo ratings yet
- Bmri2016 3741426Document7 pagesBmri2016 3741426MandaNo ratings yet
- Salvaging The Unavoidable: A Review of Complications in Pediatric Tissue ExpansionDocument10 pagesSalvaging The Unavoidable: A Review of Complications in Pediatric Tissue Expansionsmansa123No ratings yet
- Achalasia With Megaesophagus and Tracheal Compr - 2015 - International Journal oDocument3 pagesAchalasia With Megaesophagus and Tracheal Compr - 2015 - International Journal ooomculunNo ratings yet
- 1999-Clinical Anatomy-Several Invasive ProceduresDocument12 pages1999-Clinical Anatomy-Several Invasive ProceduresmohamedadnanNo ratings yet
- Chest TubesDocument5 pagesChest TubesCristian Odany Lopez GregorioNo ratings yet
- Extracorporeal Oxygenation Prolonged Cardiopulmonary Bypass: (ECMO)Document11 pagesExtracorporeal Oxygenation Prolonged Cardiopulmonary Bypass: (ECMO)Almira IsmaryadiNo ratings yet
- 10 - (Rahman) The Relationship Between Chest Tube Size and Clinical Outcome in Pleural InfectionDocument8 pages10 - (Rahman) The Relationship Between Chest Tube Size and Clinical Outcome in Pleural InfectionfaisaldanyaniNo ratings yet
- Airway Clearance Techniques and Hyperinflation Therapy Walsh Chapter 12Document25 pagesAirway Clearance Techniques and Hyperinflation Therapy Walsh Chapter 12Dennis Páez Torres100% (2)
- Embolización Angiografica ArtDocument5 pagesEmbolización Angiografica ArtIsamar AlvarezNo ratings yet
- Nursing Practices: Troubleshooting Thoracostomy Tube ManagementDocument6 pagesNursing Practices: Troubleshooting Thoracostomy Tube ManagementDeo RizkyandriNo ratings yet
- Journal Theqnique of CircumcisionDocument8 pagesJournal Theqnique of CircumcisionAndi Muhamad RizqiNo ratings yet
- Cryosurgery For Common Skin Conditions - American Family PhysicianDocument8 pagesCryosurgery For Common Skin Conditions - American Family Physicianصقر قريشNo ratings yet
- MergedDocument12 pagesMergedصقر قريشNo ratings yet
- MergedDocument11 pagesMergedصقر قريشNo ratings yet
- MergedDocument8 pagesMergedصقر قريشNo ratings yet
- Abg Radial ArteryDocument22 pagesAbg Radial Arteryصقر قريشNo ratings yet
- Hemoroid 1Document8 pagesHemoroid 1Kanesti KamajayaNo ratings yet
- Primer: Hepatocellular CarcinomaDocument28 pagesPrimer: Hepatocellular CarcinomaAinun Aii NoorNo ratings yet
- Laparoscopy Instruments 64501087Document61 pagesLaparoscopy Instruments 64501087صقر قريشNo ratings yet
- My PostDocument1 pageMy Postصقر قريشNo ratings yet
- Hemoroid 1Document8 pagesHemoroid 1Kanesti KamajayaNo ratings yet
- My PostDocument1 pageMy Postصقر قريشNo ratings yet
- Respirator LangmanDocument10 pagesRespirator LangmanSavu MalinaNo ratings yet
- Anatomy and Cardiovascular AssessmentDocument52 pagesAnatomy and Cardiovascular AssessmentNaomi Anne AsuntoNo ratings yet
- Reversetotalshoulder Arthroplasty: Early Results of Forty-One Cases and A Review of The LiteratureDocument11 pagesReversetotalshoulder Arthroplasty: Early Results of Forty-One Cases and A Review of The LiteratureBruno FellipeNo ratings yet
- Landmark Papers in OtolaryngologyDocument433 pagesLandmark Papers in Otolaryngologyboilsfetcher0pNo ratings yet
- Gallbladder Mucocele A ReviewDocument6 pagesGallbladder Mucocele A ReviewThaís ChouinNo ratings yet
- HEARTDocument11 pagesHEART1NC21IS038 POLATHALA MOUNIKANo ratings yet
- Maximize Sinus Implant Procedures with the All-In-One SinusAll KitDocument22 pagesMaximize Sinus Implant Procedures with the All-In-One SinusAll KitsalehalsadiNo ratings yet
- By DR.: Haitham Mokhtar Mohamed Abd AllahDocument101 pagesBy DR.: Haitham Mokhtar Mohamed Abd AllahMohamed ElkadyNo ratings yet
- Jurnalul de Chirurgie IașiDocument96 pagesJurnalul de Chirurgie IașiFlaviu Ionuț FaurNo ratings yet
- Pathologic Obstetrics 100 Item Post TestDocument16 pagesPathologic Obstetrics 100 Item Post TestMomshie Felaih Binasoy Dela CruzNo ratings yet
- Normal Occlusion KeysDocument30 pagesNormal Occlusion KeysMuzna AftabNo ratings yet
- MCA - LAB - Sterile Technique Procedures - NotesDocument7 pagesMCA - LAB - Sterile Technique Procedures - NotesRaynelah AnnNo ratings yet
- Ultrasound, CT, MRI, Mammogram MCQsDocument9 pagesUltrasound, CT, MRI, Mammogram MCQsخلدون سليمNo ratings yet
- Investigation On Gastrointestinal Tract A ReviewDocument6 pagesInvestigation On Gastrointestinal Tract A ReviewHafidz Ma'rufNo ratings yet
- F1000research 7 16443Document8 pagesF1000research 7 16443Muhammad AzamNo ratings yet
- Sample Operative ReportsDocument24 pagesSample Operative ReportsIta Farica100% (1)
- Combinepdf 3Document95 pagesCombinepdf 3paruNo ratings yet
- 2021 ESC Guidelines On Cardiac Pacing andDocument94 pages2021 ESC Guidelines On Cardiac Pacing andLeo Purba100% (1)
- Msotransparent - Nic.in Writereaddata Cghsdata Mainlinkfile File287 PDFDocument25 pagesMsotransparent - Nic.in Writereaddata Cghsdata Mainlinkfile File287 PDFNeeraj Sharma100% (1)
- OB Notes: Theories of Labor, Stages, Powers and PassageDocument16 pagesOB Notes: Theories of Labor, Stages, Powers and Passagelily machan100% (3)
- Spondilolisthesis VAGDocument45 pagesSpondilolisthesis VAGvidro alifNo ratings yet
- Flyer PITO ORLIACDocument2 pagesFlyer PITO ORLIACCrumbolo LalaNo ratings yet
- 2016 Maxicare MaxiPlus Healthcare Program For 5-99 HeadsDocument30 pages2016 Maxicare MaxiPlus Healthcare Program For 5-99 HeadsOMG Solutions100% (2)
- A&P - 2. Blood Vessels of The Brain (9p)Document9 pagesA&P - 2. Blood Vessels of The Brain (9p)Gabriel StratulatNo ratings yet
- Operative ReportDocument3 pagesOperative ReportReshma Francis100% (1)
- Pacemaker Invasive Cardiac PacingDocument57 pagesPacemaker Invasive Cardiac PacingAhmad Khalil Ahmad Al-SadiNo ratings yet
- Article 2 - Bearing Surfaces in Hip ReplacementDocument6 pagesArticle 2 - Bearing Surfaces in Hip ReplacementAbishkar ShresthaNo ratings yet
- Single Use Cannula V-System: Efficient ERCP Cannulation & ExchangeDocument18 pagesSingle Use Cannula V-System: Efficient ERCP Cannulation & ExchangeEny Sri RyNo ratings yet
- Staff nurse coaching memory based questionsDocument8 pagesStaff nurse coaching memory based questionsVrindha VijayanNo ratings yet
- BSA-Group 3 - Natural Law Case StudyDocument2 pagesBSA-Group 3 - Natural Law Case Studynericuevas1030No ratings yet
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (402)
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (17)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (78)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 5 out of 5 stars5/5 (4)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- The Ultimate Guide To Memory Improvement TechniquesFrom EverandThe Ultimate Guide To Memory Improvement TechniquesRating: 5 out of 5 stars5/5 (34)
- Techniques Exercises And Tricks For Memory ImprovementFrom EverandTechniques Exercises And Tricks For Memory ImprovementRating: 4.5 out of 5 stars4.5/5 (40)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- Summary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: How to Be an Adult in Relationships: The Five Keys to Mindful Loving by David Richo: Key Takeaways, Summary & Analysis IncludedRating: 4 out of 5 stars4/5 (11)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisFrom EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisRating: 5 out of 5 stars5/5 (8)
- 12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosFrom Everand12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosRating: 4.5 out of 5 stars4.5/5 (207)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- The Happiness Trap: How to Stop Struggling and Start LivingFrom EverandThe Happiness Trap: How to Stop Struggling and Start LivingRating: 4 out of 5 stars4/5 (1)