Professional Documents
Culture Documents
US Renal Doppler Complete
Uploaded by
Pakde RiOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
US Renal Doppler Complete
Uploaded by
Pakde RiCopyright:
Available Formats
UT Southwestern Department of Radiology
Ultrasound – Renal Doppler Complete (Renal Artery Stenosis)
PURPOSE:
To evaluate the vasculature associated with the native kidneys for arterial stenosis.
SCOPE:
Applies to all ultrasound abdominal studies performed in Imaging Services / Radiology
EPIC ORDERABLE:
• US Doppler Renal (perform this protocol only)
CHARGEABLES:
• US Doppler Renal (US DOPPLER COMPLETE CPT 93975)
• Add to US Renal if ordered together (US RENAL COMPLETE, CPT 76770)
o See specific US Renal protocol for details regarding a complete renal examination.
INDICATIONS:
• Suspected renal artery stenosis (examples: hypertension resistive to treatment, hypertension in
young patients etc.);
• Suspected vasculitis or fibromuscular dysplasia (FMD);
• Abnormal findings on other imaging studies;
• If renal vessel patency is the clinical concern, refer to protocol “US Renal Doppler Patency”;
• If nutcracker Syndrome (renal vein entrapment) is the clinical concern, refer to protocol “US
Renal Doppler Nutcracker).
CONTRAINDICATIONS:
• No absolute contraindications
• For unstable, hospitalized, and ventilated patients, ordering providers should consider
alternative modalities for ruling out RAS. Doppler is frequently nondiagnostic in these situations.
A diagnostic Doppler exam for RAS should be reserved for stable outpatients who are able to
comply with breathing instructions.
EQUIPMENT:
• Curvilinear transducer with a frequency range of 1-9 MHz that allows for appropriate
penetration and resolution depending on patient’s body habitus
PATIENT PREPARATION:
• Patient must be NPO for 4-6 hours prior to study
• Patients should be medically stable, able to following breathing instructions, and be transported
to the Radiology Department Ultrasound Lab
EXAMINATION:
GENERAL GUIDELINES:
A complete examination includes evaluation of:
• Both main renal arteries from origin to hilum and intrarenal branches, including
interlobar arteries
• Both main renal veins
US Renal Doppler RAS 08-12-2022 1|Page Revision date: 08-12-2022
• Abdominal aorta proximal to the origins of the main renal arteries.
• Additional image acquisition protocols based on orderable (above)
• NOTE: This examination is reserved for NPO patients able to be transported to
Radiology for scanning. For renal vessel patency (e.g. for ICU patients), refer to “US
Renal Doppler Limited” protocol
EXAM INITIATION:
• Introduce yourself to the patient and explain test
• Verify patient identity using patient name and DOB
• Obtain patient history including symptoms. Enter and store data page
• Place patient in supine position. Right or left lateral decubitus (RLD, LLD) positioning may be
required
TECHNICAL CONSIDERATIONS:
• Review any prior imaging, making note of abnormalities or other findings requiring further
evaluation-follow up.
• Optimize gain and display setting with respect to depth, dynamic range, and focal zone on
greyscale imaging first.
• Obtain renal length measurement.
ᴑ For the right kidney include adjacent liver for echogenicity comparison.
• Optimize color Doppler setting to show optimal flow
o Adjust scale and gain to maximally fill the vessel of interest without artifact
Light color in the middle of the vessel lumen
o Use Power Doppler if flow is not seen with color Doppler
o Look for color aliasing and/or post-stenotic turbulence to identify stenosis
o In severe stenosis, a color soft tissue “bruit” may be present
• Optimizing spectral Doppler:
o Place time-gate centrally within the vessel of interest
o Adjust scale to extend spectral waveform (amplitude adequate for interpretation)
o Eliminate aliasing for high flow evaluation by increasing the velocity scale and/or
lowering the base line.
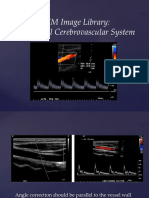
• As much as possible, utilize angle correction of < 60⁰ to measure velocities
o Angle correction should always be parallel to the vessel wall, in line with flow
direction
o For certain anatomy, may need to try from different approaches to optimize angle
• Aortic velocity (peak systole only) measurements should be obtained proximal to the main
renal arteries origins.
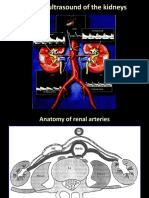
• Renal Arteries:
o Using color Doppler, survey the aorta for the multiple renal arteries. The arteries are
often best seen in the coronal view, with the patient in the decubitus position. This
view also gives the best Doppler angle for accurate velocity measurements.
o If able, obtain the “banana peel” view with both ostia of both main renal arteries,
including velocity measurements
o The majority of renal artery stenosis in adults occurs at the ostium.
If identified, measure the peak systolic velocity of the suspected stenotic
area (don’t forget to angle correct)
US Renal Doppler RAS 08-12-2022 2|Page Revision date: 08-12-2022
o Obtain the Acceleration Time (AT) and Acceleration Index (AI) of the interlobar
arteries in the upper pole, interpolar region, and lower pole. Several waveforms
may be needed to obtain an optimal waveform for accurate AT and AI
measurements. Be patient!
Choose the waveform that clearly shows an early systolic peak (ESP)
Beware of different variants of the ESP. If not clearly seen, look for the
“break point”. See Appendix).
IMAGE DOCUMENTATION:
Perform the blow measurements for LEFT and RIGHT kidneys.
If multiple arteries are present, obtain color and spectral images as above for each artery.
Anatomy Grey Color Waveform PSV RI eSAT eSAI
Scale Doppler
*
Longitudinal kidney: mid,
x
without and with measurements
Renal artery ostium x x X x
Renal artery: proximal x x X x
Renal artery: middle x x X x
Renal artery: distal x x X x
Interlobar artery: upper pole x x X x x x
Interlobar artery: mid segment x x X x x x
Interlobar artery: lower pole x x X x x x
Main renal vein x x X
Aorta: proximal to the renal
x x X x
arteries
Data page with measurements
*Include one grayscale image with length measurement and one without
PSV = peak systolic velocity
EDV =end diastolic velocity
RI = resistive index
eSAT = early systolic peak acceleration time
eSAI = early systolic peak acceleration index
PROCESSING:
• Review examination data
• Export all images to PACS
• Confirm data Imorgon (UTSW only)
• Note any study limitations (in Epic Study Note or paper communication, per Radiologist
preference)
US Renal Doppler RAS 08-12-2022 3|Page Revision date: 08-12-2022
REFERENCES:
• ACR-AIUM Practice Guideline (Revised 2007)
• ICAVL Guidelines (Updated 8/2012)
APPENDIX:
• Criteria for >60% stenosis of the renal artery:
o Indirect (interlobar artery) SAT > 0.1 sec SAT and AI < 300 cm/sec2
o Direct (main artery) PSV > 200cm/sec
RAR >3.5 (trumps a normal or abnormal PSV)
• Acceleration Time (AT) and Acceleration Index (AI) of the interlobar arteries are calculated by
identifying the point of systolic upstroke and the FIRST (early) systolic peak (ESP).
• Beware of different variants of the ESP. If not clearly seen, look for the “break point”.
Criteria s/p Renal Artery Stenting
• Change over time
• Intraluminal echoes on gray scale
• Narrowing and aliasing on color Doppler
• Tardus Parvus waveforms in the intraparenchymal vessels
• Renal artery velocity higher than 296 cm/sec (sensitive) to 395 cm/sec (specific)
• RAR ranging from 4.4 (sensitive) to 5.1 (specific)
References:
• Thornton SN, et al. Circulation 2007;116:II-745, New Doppler Ultrasound Criteria for Renal Artery In-
Stent Re-Stenosis
• Ultrasound velocity criteria for renal in-stent restenosis Yung-Wei Chi, DO, Christopher J. White, MD,
Stanley Thornton, MD, and Richard V. Milani, MD, New Orleans, La. Journal of Vascular Surgery, July
2009.
US Renal Doppler RAS 08-12-2022 4|Page Revision date: 08-12-2022
CHANGE HISTORY:
STATUS NAME & TITLE DATE BRIEF SUMMARY
Submission David Fetzer, MD, Director 1/31/2016 Submitted
Approval David Fetzer, MD, Director 1/31/2016 Approved
Review Anthony Setiawan, MD 11/14/2018 Reviewed
Revisions David Fetzer, MD 07/25/2016 Segmental renal artery
waveform descriptions
David Fetzer, MD 06-19-2017 Changes to list of relevant
orders to reflect
consolidation of EPIC
orderables.
David Fetzer, MD 01-14-2020 Renamed protocol to
specific RAS
David Fetzer, MD; Kanu 04-12-2021 Added criteria for RAS in
Vijay MD presence of stents
Skye Smola RDMS, RVT 8/12/2022 Removed all language
requiring Aorta images
and PSV “at and inf to
renal arteries”. Only prox
to renal artery Aorta
images and PSV need be
obtained.
US Renal Doppler RAS 08-12-2022 5|Page Revision date: 08-12-2022
You might also like
- US Liver Doppler OnlyDocument8 pagesUS Liver Doppler OnlymicropocketfilmsNo ratings yet
- Renal Ultrasound ProtocolDocument4 pagesRenal Ultrasound Protocolfouad tabetNo ratings yet
- Guidelines of Arterial Duplex ScanDocument23 pagesGuidelines of Arterial Duplex ScanMohamed Omar Elfarok100% (1)
- Renal Doppler Study: DR Subash Pathak 2nd Year Resident Radiodiagnosis NamsDocument98 pagesRenal Doppler Study: DR Subash Pathak 2nd Year Resident Radiodiagnosis NamsNam Đàm PhươngNo ratings yet
- Doppler Ultrasound of The KidneysDocument23 pagesDoppler Ultrasound of The KidneysivoklarinNo ratings yet
- Carotid Doppler Study: Dr.I.Gurubharath MD PHD DR - Pooja MDDocument116 pagesCarotid Doppler Study: Dr.I.Gurubharath MD PHD DR - Pooja MDJing CruzNo ratings yet
- Doppler Ultrasound of The KidneysDocument23 pagesDoppler Ultrasound of The KidneysivoklarinNo ratings yet
- Renal Artery StenosisDocument80 pagesRenal Artery StenosisAnn FloydNo ratings yet
- Sample Protocol For Performing Lower Extremity Arterial Duplex ExaminationsDocument2 pagesSample Protocol For Performing Lower Extremity Arterial Duplex ExaminationsMohamed Omar ElfarokNo ratings yet
- Renal Artery Doppler NsDocument15 pagesRenal Artery Doppler Nss0800841739No ratings yet
- Cardiac SurgeryDocument7 pagesCardiac Surgeryampogison08100% (1)
- Basic Cardiac ImagingDocument40 pagesBasic Cardiac ImagingSarah Sy-SantosNo ratings yet
- Renal Artery InterventionsDocument43 pagesRenal Artery InterventionsVivek JaganathanNo ratings yet
- Dr. Yash Kumar AchantaniDocument65 pagesDr. Yash Kumar AchantaniJenniffer FNo ratings yet
- The Role of Color Doppler Ultrasound in Living Donor Liver Transplantation 2008 Journal of Medical UltrasoundDocument11 pagesThe Role of Color Doppler Ultrasound in Living Donor Liver Transplantation 2008 Journal of Medical UltrasoundIman Ru-ancaNo ratings yet
- ANGIOGRAPHYDocument8 pagesANGIOGRAPHYAkazukin AineNo ratings yet
- Echocardiography DeepakDocument71 pagesEchocardiography DeepakDeepak Ghimire88% (8)
- ABG and Oximetry StudentDocument86 pagesABG and Oximetry StudentAlexander Santiago ParelNo ratings yet
- Extended Focused Assessment With Sonography in Trauma (eFAST)Document45 pagesExtended Focused Assessment With Sonography in Trauma (eFAST)vimal rajNo ratings yet
- Image ResourcesDocument31 pagesImage Resourcesralphmx11No ratings yet
- Cardiovascular InvestigationDocument51 pagesCardiovascular InvestigationSarahafattahNo ratings yet
- Renal Doppler Protocol 14 PDFDocument3 pagesRenal Doppler Protocol 14 PDFapi-390240132No ratings yet
- Echo With KosmosDocument57 pagesEcho With Kosmossamirmohamed900No ratings yet
- Policies and Statements: Peripheral Arterial UltrasoundDocument5 pagesPolicies and Statements: Peripheral Arterial UltrasoundJing CruzNo ratings yet
- Appendix A: Doppler Ultrasound and Ankle-Brachial Pressure IndexDocument26 pagesAppendix A: Doppler Ultrasound and Ankle-Brachial Pressure IndexabigailNo ratings yet
- Aug15 955 ChandraDocument78 pagesAug15 955 ChandraPedro BragatoNo ratings yet
- Introduction To Doppler ImagingDocument24 pagesIntroduction To Doppler Imagingdivyanshu kumarNo ratings yet
- JURNALDocument8 pagesJURNALICHWANUDDINBUCHORINo ratings yet
- Acute Aortic SyndromeDocument62 pagesAcute Aortic Syndromedr_antonio81No ratings yet
- 2 POCUS in Emergency FAST IVC LUNGresidents December 2022Document92 pages2 POCUS in Emergency FAST IVC LUNGresidents December 2022dr mohd abdul basithNo ratings yet
- Abdomen Complete ProtocolDocument7 pagesAbdomen Complete Protocolrdfj.muganhu1No ratings yet
- UltrasoundDocument47 pagesUltrasoundDavid KimunyanNo ratings yet
- Life Saving Pocket - GuideDocument10 pagesLife Saving Pocket - GuideNur FarhanaNo ratings yet
- Flowdynamics GovindDocument74 pagesFlowdynamics Govindgovind rajNo ratings yet
- VASCULAR - Abdominal Aorta Duplex ScanDocument24 pagesVASCULAR - Abdominal Aorta Duplex ScanSophia Elinor MenesesNo ratings yet
- Venous Congestion ChapterDocument8 pagesVenous Congestion ChapterpcarrascoeNo ratings yet
- 4-Cortical Thickness An Early Morphological Marker ofDocument8 pages4-Cortical Thickness An Early Morphological Marker ofjeb faqNo ratings yet
- Introduction To EchocardiographyDocument57 pagesIntroduction To EchocardiographyKEN KIZITONo ratings yet
- Renal Doppler Protocol 14 1Document4 pagesRenal Doppler Protocol 14 1api-349402240100% (1)
- 5 Upper Extremity Arterial Duplex Evaluation Updated 2018 PDFDocument8 pages5 Upper Extremity Arterial Duplex Evaluation Updated 2018 PDFHasan Mohammad NayeemNo ratings yet
- CMR Guide CHD 2014 PDFDocument105 pagesCMR Guide CHD 2014 PDFBasemAlharbiNo ratings yet
- Liver ImagingDocument7 pagesLiver ImagingBenn BerriganNo ratings yet
- Doppler Ultrasonography of The Lower Extremity ArteriesDocument34 pagesDoppler Ultrasonography of The Lower Extremity ArteriesNidaa MubarakNo ratings yet
- Basics of CathlabDocument39 pagesBasics of CathlabMemon RazakNo ratings yet
- 10 Upper Extremity Mapping For Creation of Dialysis Access or Bypass Graft Updated 2019Document7 pages10 Upper Extremity Mapping For Creation of Dialysis Access or Bypass Graft Updated 2019Marisol MorenoNo ratings yet
- CMR GuidecongenitasD 2014Document105 pagesCMR GuidecongenitasD 2014karen mendoza rodriguezNo ratings yet
- Basic EchocardiographyDocument63 pagesBasic EchocardiographyStella CooKeyNo ratings yet
- Ringelstein Et Al. - 1990 - Transcranial Doppler Sonography Anatomical LandmaDocument17 pagesRingelstein Et Al. - 1990 - Transcranial Doppler Sonography Anatomical LandmaMaya JacksonNo ratings yet
- Anatomía y Fisiología CardiovascularDocument15 pagesAnatomía y Fisiología Cardiovascularebriceno2211No ratings yet
- Uroradiology For Medical Students: Lesson 5 Nuclear Renography - 1 American Urological AssociationDocument49 pagesUroradiology For Medical Students: Lesson 5 Nuclear Renography - 1 American Urological AssociationlisarahmaasrilNo ratings yet
- Intracardiac Echo DR SrikanthDocument107 pagesIntracardiac Echo DR SrikanthNakka SrikanthNo ratings yet
- Dental ReportDocument9 pagesDental ReportJeshil ShahNo ratings yet
- Vexus ScoreDocument28 pagesVexus Scorerev nashrulezNo ratings yet
- 1 s2.0 S0085253815471595 MainDocument9 pages1 s2.0 S0085253815471595 Mainraihanul khairiNo ratings yet
- CH 0060Document7 pagesCH 0060Shreya SinhaNo ratings yet
- Cardiovascular Pathology: Professor Mircea BuruianDocument174 pagesCardiovascular Pathology: Professor Mircea BuruianDiana PopoviciNo ratings yet
- Topic: Recent Advances - Cardiac CT: Journal ClubDocument130 pagesTopic: Recent Advances - Cardiac CT: Journal Clubjai256No ratings yet
- Renal Doppler To Assess Renal Perfusion in The Critically Ill: A ReappraisalDocument10 pagesRenal Doppler To Assess Renal Perfusion in The Critically Ill: A ReappraisalFlávio AlvesNo ratings yet
- Renal Ultrasound Made Easy - Step-By-Step Guide - POCUS 101Document45 pagesRenal Ultrasound Made Easy - Step-By-Step Guide - POCUS 101skype72214100% (2)