Professional Documents
Culture Documents
Ada Therapeutic Inertia Infographic Final 2
Uploaded by
Jia-PeiWuOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ada Therapeutic Inertia Infographic Final 2
Uploaded by
Jia-PeiWuCopyright:
Available Formats
Make a Difference:
Achieve Glycemic Goals Early in
Patients with Type 2 Diabetes
With These Best Practice Strategies
Intensify Treatment of Newly Diagnosed Patients and Patients with A1C Above Target
Early and appropriate therapy improves patients’
chances of reaching A1C goals.
The Legacy Effect: Landmark clinical trials and
research studies show that reaching A1C targets in
the first year of treatment results in sustained,
long-term health improvements even when control
waned over time1-7.
Achieve glycemic goals in < 6—12 months
Create Personalized Diabetes Care Plans
Assess patient's: Have ongoing conversations about Use shared decision making to
Health literacy and numeracy the progressive nature of type 2 determine individual glycemic
Attitudes and beliefs regarding diabetes and management options. targets and how to achieve glyce-
medication therapy Diabetes changes over time and mic targets within 3—6 months.
Social determinants of health therefore their treatment plan will
change too
Implement a Team-Based Approach
Empower the appropriate team Refer to:
members to independently initiate Diabetes self-management Trained community
and adjust medications. education and support health worker
Use medication algorithms and specialist Other diabetes care
protocols for therapeutic changes Registered dietitian team members
Effective team communication Pharmacist
Behavioral health specialist
Improve A1C by leveraging Reductions in A1C compared to usual care8:
the multidisciplinary team -0.40% to -1.62% -0.30% to -1.20% -0.60% to -0.90% -0.26% to -0.40%
A recent systematic review and
meta-analysis8 found that, compared
to usual care, interventions where
non-physician providers initiate and
intensify treatment, with support
from guidelines, had greater
reductions in A1C.
Nurse- or Certified Care management & Pharmacist-based Physician-based
Diabetes Care & Education patient education interventions interventions
Specialist-led medication interventions
management
Results may be less dependent on who intensifies therapy but rather how they intensify. Frequency of contact and delivery methods matter. Nearly all care
management and patient education interventions resulting in statistically and clinically significant reduction in A1C used technology to communicate with patients.8
Leverage Tools and Technology
My Glucose
GLUCOSE IN RANGE 1m ago
125 mg/dL
350
250
150
125 mg
dL
50 350
250
2pm 6pm 10pm 150
50
2pm 6pm 10pm
Use technology for glycemic assessments to adjust Communicate frequently with patients.
therapy before/between 3-month A1C checks. Patient-provider portals
Blood glucose monitoring data HIPAA-compliant texting modalities
Continuous glucose monitoring data Telehealth visits where appropriate
Patient self-tracking tools and support apps Schedule diabetes-only visits
Use electronic health records to identify high risk Use team members to increase touchpoints
patients and implement guidelines Utilize patient registries and chronic care coordinators
Take Action to Bust Therapeutic Inertia! Learn more and access tools to implement these
strategies from the Overcoming Therapeutic Inertia
Therapeutic inertia is the inaction of the clinician initiative from the American Diabetes Association
to intensify or de-intensify treatment when A1C
goals are not met. at therapeuticinertia.diabetes.org
References: 1. Holman RR, et al. N Engl J Med. 2008; 359: 1577–1589 2. Laiteerapong N, Ham S, Goo Y, et al. Diabetes Care 2019;42:416-0426 3. Mehta R, et al. Journal of
Clinical & Translational Endocrinology. 19(2020) 100215 4.ADA Standards of Care 2022 5.Khunti K, et al. Diab Care 2013;36:3411–7;6. Del Prato S, et al. Int J Clin Pract
2005;59:1345–1355 7. UKPDS 33. Lancet. 1998; 352: 837–853 8. Powell RE, et al. Diabetes Obes Metab. 2021;23:2137–2154.
You might also like
- Assessment 2Document12 pagesAssessment 2ODIPLEXNo ratings yet
- Comprehensive Approaches To Diabetes Care & Collaborative ManagementDocument17 pagesComprehensive Approaches To Diabetes Care & Collaborative ManagementCharisse TaylanNo ratings yet
- DiabetesDocument46 pagesDiabetesanamikapokhariaNo ratings yet
- Comprehensive Approaches To DM & Collaborative MGTDocument17 pagesComprehensive Approaches To DM & Collaborative MGTCharisse TaylanNo ratings yet
- Adult Guideline - Update Thru 10-23-14 2Document20 pagesAdult Guideline - Update Thru 10-23-14 2Indira VenegasNo ratings yet
- Case Study - A Patient With Type 1 Diabetes WhoDocument4 pagesCase Study - A Patient With Type 1 Diabetes WhoWulan AnggrahiniNo ratings yet
- 2011 FullDocument7 pages2011 FullDiana PutriNo ratings yet
- Diabetes T 2Document16 pagesDiabetes T 2Huma Hameed DogarNo ratings yet
- NU 608 guideline statement paperDocument4 pagesNU 608 guideline statement paperkaylabarnes74No ratings yet
- Diab MGMTDocument7 pagesDiab MGMTPrabJot SinGhNo ratings yet
- Family Physicians & Hypertension: Moving ForwardDocument4 pagesFamily Physicians & Hypertension: Moving ForwardSusi DesmaryaniNo ratings yet
- Adult Guidelines - Edit 7-2-10Document13 pagesAdult Guidelines - Edit 7-2-10Sivakumar NadellaNo ratings yet
- Standards of Medical Care in Diabetes - 2021: Abridged For Primary Care ProvidersDocument30 pagesStandards of Medical Care in Diabetes - 2021: Abridged For Primary Care Providersmỹ duyên đoànNo ratings yet
- Modified Brief Counseling-5a, Motivational SMS On Medication Taking Behavior and Compliance Among Diabetic PatiDocument9 pagesModified Brief Counseling-5a, Motivational SMS On Medication Taking Behavior and Compliance Among Diabetic PatiIJPHSNo ratings yet
- Care Plan 1Document5 pagesCare Plan 1gyanendraNo ratings yet
- Diabetes Spectrum-The Meal Time Challenge Nutrition & Glycemic Control in The HospitalDocument6 pagesDiabetes Spectrum-The Meal Time Challenge Nutrition & Glycemic Control in The HospitalYuanita PurnamiNo ratings yet
- Diaclincd 21 As 01Document30 pagesDiaclincd 21 As 01renzo cardenasNo ratings yet
- Impact of Pharmacist Insulin Management On Hemoglobin A1c in Outpatient Hospital Clinic SettingDocument7 pagesImpact of Pharmacist Insulin Management On Hemoglobin A1c in Outpatient Hospital Clinic SettingSabrina JonesNo ratings yet
- Required: Body System: Session Topic: Educational Format Faculty Expertise RequiredDocument16 pagesRequired: Body System: Session Topic: Educational Format Faculty Expertise RequiredThaysa LimaNo ratings yet
- Chatbots For Diabetes Self-Management: Diabetes Coaching at ScaleDocument12 pagesChatbots For Diabetes Self-Management: Diabetes Coaching at ScaleDaniel T. DinkaNo ratings yet
- Quality Improvement Project.Document7 pagesQuality Improvement Project.rhinoNo ratings yet
- Sugar - Fit: A Personalized Evidence Based Path To Type 2 and Prediabetes ReversalDocument4 pagesSugar - Fit: A Personalized Evidence Based Path To Type 2 and Prediabetes ReversalRamesh EmandiNo ratings yet
- Foundations of Care: Education, Nutrition, Physical Activity, Smoking Cessation, Psychosocial Care, and ImmunizationDocument11 pagesFoundations of Care: Education, Nutrition, Physical Activity, Smoking Cessation, Psychosocial Care, and ImmunizationrakolovaNo ratings yet
- NCP 1Document2 pagesNCP 1Jerreca DasasNo ratings yet
- Diabetes Abridged 2017Document19 pagesDiabetes Abridged 2017SerGoR12No ratings yet
- Role of knowledge and self-care in diabetes managementDocument5 pagesRole of knowledge and self-care in diabetes managementpraveena thanavelNo ratings yet
- Pharmacologic Therapy For Type 2 Diabetes: Synopsis of The 2017 American Diabetes Association Standards of Medical Care in DiabetesDocument8 pagesPharmacologic Therapy For Type 2 Diabetes: Synopsis of The 2017 American Diabetes Association Standards of Medical Care in DiabetesSharan KaurNo ratings yet
- Health Care Team in Health AssessmentDocument43 pagesHealth Care Team in Health AssessmenthectorNo ratings yet
- Comprehensive Medical Evaluation and Assessment of Comorbidities: Standards of Medical Care in Diabetesd2018Document10 pagesComprehensive Medical Evaluation and Assessment of Comorbidities: Standards of Medical Care in Diabetesd2018Vartika SinghalNo ratings yet
- Clinical Nutrition Quality IndicatorsDocument7 pagesClinical Nutrition Quality Indicatorsmaricarmen IbarraNo ratings yet
- Diabetes PassportDocument1 pageDiabetes PassportJessica MooreNo ratings yet
- IPE Program in My InstitutionDocument11 pagesIPE Program in My InstitutionLOGESWARRY K.VESUPATHYNo ratings yet
- Self-Management Enhancement Programme PDFDocument18 pagesSelf-Management Enhancement Programme PDFSriMathi Kasi Malini ArmugamNo ratings yet
- S38 Full PDFDocument13 pagesS38 Full PDFAntika CahyatiNo ratings yet
- Effect of An Intensive Lifestyle Intervention On Glycemic Control in Patients With Type 2 Diabetes A Randomized Clinical TrialDocument10 pagesEffect of An Intensive Lifestyle Intervention On Glycemic Control in Patients With Type 2 Diabetes A Randomized Clinical TrialTanzo GremoryNo ratings yet
- Impact of Health Education On Knowledge Attitude PDocument8 pagesImpact of Health Education On Knowledge Attitude Palfrida100% (1)
- Guideline Recommendations For Obesity ManagementDocument15 pagesGuideline Recommendations For Obesity ManagementFranciele AnjosNo ratings yet
- Diabetes GuidelinesDocument29 pagesDiabetes GuidelinesFabiola NogaNo ratings yet
- Teaching Diabetes ManagementDocument5 pagesTeaching Diabetes ManagementWebster Claveria100% (5)
- Case Study: A Patient With Uncontrolled Type 2 Diabetes and Complex Comorbidities Whose Diabetes Care Is Managed by An Advanced Practice NurseDocument4 pagesCase Study: A Patient With Uncontrolled Type 2 Diabetes and Complex Comorbidities Whose Diabetes Care Is Managed by An Advanced Practice NurseSulaiman AlqatfNo ratings yet
- MSN - Capstone - Proposal - Poster - NSG6999 South UniversityDocument1 pageMSN - Capstone - Proposal - Poster - NSG6999 South UniversityMelinda PowellNo ratings yet
- (1998) Chronic Disease Management What Will It Take To Improve Care For Chronic IllnessDocument3 pages(1998) Chronic Disease Management What Will It Take To Improve Care For Chronic IllnessDaniel MeloNo ratings yet
- Nutrition Therapy For Diabetes Effectiveness Carbohydrates and AlcoholDocument12 pagesNutrition Therapy For Diabetes Effectiveness Carbohydrates and Alcoholscience lulNo ratings yet
- Ada 2022 Standards of Care For Primary Care ProvidersDocument29 pagesAda 2022 Standards of Care For Primary Care ProvidersAngela Zapata Garrido100% (1)
- The Abcs: of MeasurementDocument20 pagesThe Abcs: of MeasurementScribdMeUpNo ratings yet
- Type 2 Diabetes: Quick Reference GuideDocument20 pagesType 2 Diabetes: Quick Reference GuideAnny AunNo ratings yet
- 06 Insulin InitiationDocument6 pages06 Insulin InitiationamalNo ratings yet
- DC 21 SintDocument2 pagesDC 21 SintMahmoud FathyNo ratings yet
- Standards of Medical Care in Diabetes-2022Document2 pagesStandards of Medical Care in Diabetes-2022IRIS SARAHI IBARRA AGUILARNo ratings yet
- Diaclincd 23 As 01Document28 pagesDiaclincd 23 As 01Michelle WongNo ratings yet
- 688 FullDocument6 pages688 FullKhaulla KarimaNo ratings yet
- Standards of Medical Care in Diabetes-2022Document2 pagesStandards of Medical Care in Diabetes-2022Carlos MatuteNo ratings yet
- Policy Implementation Training SessionDocument9 pagesPolicy Implementation Training SessionabuumaiyoNo ratings yet
- Diabetes 2022 ReviewDocument29 pagesDiabetes 2022 ReviewIngrid MiñanoNo ratings yet
- DM GuidelinesDocument29 pagesDM GuidelinesfirdiantyNo ratings yet
- Standards of Medical Care in Diabetes - 2022Document9 pagesStandards of Medical Care in Diabetes - 2022Flórian JeffersonNo ratings yet
- Appropriate Titration of Basal Insulin in Type 2 Diabetes and The Potential Role of The PharmacistDocument21 pagesAppropriate Titration of Basal Insulin in Type 2 Diabetes and The Potential Role of The PharmacistOlesiaNo ratings yet
- Diaclincd 22 As 01Document29 pagesDiaclincd 22 As 01RyuNo ratings yet
- NCPPartIII2019 PDFDocument28 pagesNCPPartIII2019 PDFjothiNo ratings yet
- DC 23 SrevDocument5 pagesDC 23 SrevLiz NaagNo ratings yet
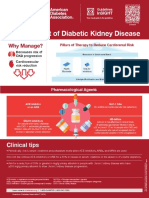
- Management of Diabetic Kidney Disease Updated 0Document1 pageManagement of Diabetic Kidney Disease Updated 0Jia-PeiWuNo ratings yet
- Treating Hypertension in People With DiabetesDocument1 pageTreating Hypertension in People With DiabetesJia-PeiWuNo ratings yet
- Standard CGM Report 0Document1 pageStandard CGM Report 0Jia-PeiWuNo ratings yet
- Blood Glucose Monitoring-CompletedDocument1 pageBlood Glucose Monitoring-CompletedJia-PeiWuNo ratings yet
- Community Acquired PneumoniaDocument6 pagesCommunity Acquired PneumoniaJia-PeiWuNo ratings yet
- Hemodynamic Management Pocket Card PDFDocument8 pagesHemodynamic Management Pocket Card PDFjenn1722No ratings yet
- By Dr. Nouran Abou Khedr: Xeroderma PigmentosumDocument6 pagesBy Dr. Nouran Abou Khedr: Xeroderma PigmentosumBahaa ShaabanNo ratings yet
- Chapter22 PregnancyDocument38 pagesChapter22 PregnancyAnnie Grace VillanuevaNo ratings yet
- Dust Work QuestionnaireDocument2 pagesDust Work QuestionnaireHykidNo ratings yet
- IVT Completion Case Form EditedDocument1 pageIVT Completion Case Form EditedNURSETOPNOTCHERNo ratings yet
- Benha University Hospital, Egypt E-Mail: Elnashar53@Document58 pagesBenha University Hospital, Egypt E-Mail: Elnashar53@khadzx100% (3)
- Hiv AidsDocument472 pagesHiv AidsDevendrapratapdpNo ratings yet
- Case Study On Prostate CancerDocument16 pagesCase Study On Prostate Cancerferdz02100% (5)
- NAMA BARANG LIST AND PRICESDocument51 pagesNAMA BARANG LIST AND PRICESlevely rizkiNo ratings yet
- ZumbaDocument13 pagesZumbaamitsingh_singh041No ratings yet
- Fogsi ChecklistDocument131 pagesFogsi ChecklistParimi VinodNo ratings yet
- 29 - Toronto Notes 2011 - Urology PDFDocument44 pages29 - Toronto Notes 2011 - Urology PDFDewa Gede Reza Sanjaya0% (1)
- Osteoartritis: Dr. Dewi Nur Fiana.,Sp - KFRDocument28 pagesOsteoartritis: Dr. Dewi Nur Fiana.,Sp - KFRgita cahayaNo ratings yet
- MCQ Pract Pharma 1Document9 pagesMCQ Pract Pharma 1Syamil AzharNo ratings yet
- Common Diseases and Epidemics: PolioDocument7 pagesCommon Diseases and Epidemics: PolioTheAwein ChannelNo ratings yet
- Komplikasi Pada Pasien Infark Miokard Akut ST-Elevasi (STEMI) Yang Mendapat Maupun Tidak Mendapat Terapi Reperfu..Document13 pagesKomplikasi Pada Pasien Infark Miokard Akut ST-Elevasi (STEMI) Yang Mendapat Maupun Tidak Mendapat Terapi Reperfu..aris hidayatul mNo ratings yet
- N220 W9 Nursing Care PlanDocument3 pagesN220 W9 Nursing Care PlanVivian PhamNo ratings yet
- Samantha Bradley: Work ExperienceDocument3 pagesSamantha Bradley: Work Experienceapi-399988983No ratings yet
- Public Health Surveillance TrainingDocument51 pagesPublic Health Surveillance TrainingSalihu MustaphaNo ratings yet
- MalariaDocument44 pagesMalariasantosh goitNo ratings yet
- The Child With A Fluid and Electrolyte Alteration: Body Water Is Located in Two Major CompartmentsDocument19 pagesThe Child With A Fluid and Electrolyte Alteration: Body Water Is Located in Two Major CompartmentsAyeza DuaNo ratings yet
- SorbitolDocument2 pagesSorbitolfara_1691100% (1)
- What Are The Signs of Autism in GirlsDocument8 pagesWhat Are The Signs of Autism in GirlsAna Sofia Nunes JorgeNo ratings yet
- PharmNotesDocument210 pagesPharmNoteschiragvetsNo ratings yet
- JUNE 2008 NP1 BOARD EXAM QUESTIONSDocument70 pagesJUNE 2008 NP1 BOARD EXAM QUESTIONSPrecious Nidua100% (1)
- Shigella SPP, Vibrio SPPDocument6 pagesShigella SPP, Vibrio SPPtomal7811islamNo ratings yet
- Pengaruh Cognitive Behavioral Therapy (CBT) Terhadap Perubahan Kecemasan, Mekanisme Koping, Harga Diri Pada Pasien Gangguan Jiwa Dengan SkizofreniaDocument23 pagesPengaruh Cognitive Behavioral Therapy (CBT) Terhadap Perubahan Kecemasan, Mekanisme Koping, Harga Diri Pada Pasien Gangguan Jiwa Dengan Skizofreniaharyati soyNo ratings yet
- Definisi & PICO 3, 4Document5 pagesDefinisi & PICO 3, 4Dionisius KevinNo ratings yet
- NURS 6521N Final Exam Question and Answers Feb 2020 (100/100)Document19 pagesNURS 6521N Final Exam Question and Answers Feb 2020 (100/100)Judy Durkin0% (1)
- Lecturenote - 344164470lecture 3 - QuantificationDocument74 pagesLecturenote - 344164470lecture 3 - Quantificationbkamurendo100% (1)