Professional Documents
Culture Documents
How Stem Cells Could Fix Type 1 Diabetes
How Stem Cells Could Fix Type 1 Diabetes
Uploaded by
Ioannis Chaidos TransitusOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
How Stem Cells Could Fix Type 1 Diabetes
How Stem Cells Could Fix Type 1 Diabetes
Uploaded by
Ioannis Chaidos TransitusCopyright:
Available Formats
Autoimmune disease
outlook
At the turn of the 21st century, hard-won
breakthroughs showed that transplants of
β cells from deceased donors could suc-
cessfully treat people with T1D2. Several
complicating factors — not least a shortage
of donors — limit this approach. But today,
stem-cell biology allows the creation of
glucose-sensing, insulin-dispensing cells in
the laboratory — offering the possibility of an
almost limitless supply of replacement cells.
In June, at the virtual annual meeting of the
American Diabetes Association, regenera-
tive medicine company ViaCyte, based in San
Diego, California, reported that in a small clin-
ical trial, cells derived from embryonic stem
cells had helped people with T1D to gain better
control of their blood sugars. “Seeing clinically
relevant results that drastically change man-
agement for patients with T1D is incredibly
exciting,” says Manasi Sinha Jaiman, ViaCyte’s
vice-president of clinical development. “It is
the culmination of 20 years of research.”
ViaCyte’s success and other scientific
advances are drawing more companies into the
field. But although the idea of making β cells
and transferring them into people sounds
REF. 8
simple, fundamental questions remain.
Encapsulated stem cell-derived islets could shield β cells from the immune system. Researchers still need to resolve which cells are
best to use, where they should be implanted,
Beta testing
and — crucially — how to ensure that they are
protected from recipients’ immune systems.
Success from failure
T1D is considered one of the lowest-hanging
Trials to replace the pancreatic β cells that are fruits in regenerative medicine. It is a condition
in which autoimmunity selectively kills a single
destroyed by an errant immune system in type 1 cell type, so it is clear what needs replacing.
diabetes are raising hopes of a cure. By Liam Drew Additionally, only a small amount of tissue is
I
needed. In the pancreas, β cells are one of five
endocrine cell types that reside in small pock-
nsulin has been one of the most transform- This chronic hyperglycaemia damages blood ets of hormone-producing cells known as islets
ative discoveries in medicine. The isolation vessels and nerves, leading to an accumulation of Langerhans. Although there are around one
of this hormone in 1921 made type 1 of ill-health effects and, if untreated, death. million islets dotted throughout the organ,
diabetes (T1D) a treatable, rather than a Today, the effects of T1D can be mitigated they amount to only 1–2% of its overall mass.
terminal, illness. However, there is growing through a combination of careful blood glu- Equally importantly, although the pancreas
hope that 100 years later, insulin therapy for cose monitoring and insulin administration. is the natural home, β cells could be placed
T1D might be on the brink of obsolescence. However, despite advances in automated elsewhere. Unlike in Parkinson’s disease, where
Insulin is crucial to maintaining safe levels insulin delivery systems, for most people this implanted neurons would have to integrate
of glucose in the blood. It is produced in means a life dominated by the need to con- into existing brain networks to restore func-
the pancreas by β cells, which continuously scientiously manage their own physiology. And tion, experiments in rats with diabetes in the
detect circulating glucose concentrations even with people taking on this burden, the life early 1970s showed that the rats regained nor-
and secrete insulin accordingly — the higher expectancy for somebody with T1D is 12 years mal blood sugar control after isolated islets
sugar levels go, the more hormone is released below average1. Frederick Banting, who won a were infused into the portal veins of their
to counteract the increase. In T1D, however, share of the Nobel Prize in Physiology in 1923 livers2. All that β cells require to function, it
the β cells are destroyed by a person’s own for discovering insulin, knew his work offered seems, is good access to the bloodstream.
immune system. no panacea — he concluded his Nobel lecture Attempts to replicate this result in people
The cause of this autoimmunity, which by saying “insulin is not a cure for diabetes”. with T1D in the 1980s and 1990s — using islets
typically manifests in childhood, is incom- Now, though, a growing number of scientists taken from the pancreases of deceased donors
pletely understood, but the effect is clear: with and physicians are talking about curing T1D. — were rarely successful2. When surgeon James
neither β cells nor insulin, circulating sugar Their focus is not supplying the body with insu- Shapiro arrived at the University of Alberta in
levels remain constantly, toxically elevated. lin, but rather replacing the β cells that make it. Edmonton, Canada, in 1993, the university’s
S64 | Nature | Vol 595 | 15 July 2021
©
2
0
2
1
S
p
r
i
n
g
e
r
N
a
t
u
r
e
L
i
m
i
t
e
d
.
A
l
l
r
i
g
h
t
s
r
e
s
e
r
v
e
d
.
transplant programme had lapsed. “Nobody more generally) would therefore provide an
wanted to run this”, he says, “because it was essentially inexhaustible supply of implant-
such a failure.” able cells.
But reviewing the literature convinced This cell product is regenerative medicine’s
Shapiro that if the cells actually engrafted and equivalent of a drug. The field’s primary
survived, they helped. He increased the dose challenge is developing a good one.
of cells — using tissue from two to four donors Doug Melton, a stem-cell biologist at Harvard
per recipient — and cut the interval between University in Cambridge, Massachusetts, is
harvesting and implantation to improve cell something of a talisman for this field. He was
health. Crucially, he also realized that the a developmental neurobiologist until his six-
drugs previously used to stop the immune month-old son was diagnosed with T1D in the
VIACYTE, INC.
system from attacking the transplanted tissue early 1990s. He dropped everything to seek a
were probably also damaging the β cells. To cure for the condition, eventually entering the
avoid this, he designed a new drug regimen3. stem-cell field. He recalls telling his wife that he
All seven of Shapiro’s first patients were was going to work out a way to make β cells, and ViaCyte’s pancreatic cells in a pouch.
able to come off insulin for at least one year that it would take four or five years.
— one, remarkably, remains insulin free more His estimate was a little off. Creating a β cell islet cells and the immunosuppressed mice
than 20 years later. “We showed conceptually required coaxing stem cells through a series began to show controlled blood glucose levels7.
that islet cell transplantation can dramatically of intermediate stages, such as making cells Consequently, by the time Melton and
improve patients’ lives,” Shapiro says. that could become any cell of the pancreas. others had determined how to make β cells,
Shapiro’s method, now known as the Working out all those steps and how to nav- ViaCyte was commencing its first clinical trial
Edmonton protocol, is used today at a hand- igate them ultimately took Melton closer to implanting pancreas progenitor cells — and is
ful of centres to transplant β cells into people 15 years. Melton’s group — and, independently, now running its fourth and fifth trials.
whose T1D is poorly controlled by insulin. The that of Tim Kieffer at the University of British Distinguishing which cells make the best
downside of the procedure is that recipients Columbia in Vancouver, Canada, — published therapies will take time. Melton thinks that
must commit to a long-term regimen of their methods in 2014 (refs 4 & 5). implanting fully differentiated cells will provide
powerful immunosuppressive drugs, which With patents secured on β-cell production better control of the cell dosage that people
leave them vulnerable to infections and other protocols, in 2015 Melton co-founded a receive. Kieffer agrees that relying on progen-
complications. And even if large numbers of start-up company, which was acquired itors to mature inside recipients introduces
people with T1D were willing to make this trade, by Vertex Pharmaceuticals in Boston, extra layers of variability and uncertainty, as
too few donors exist to provide cells for more Massachusetts, for US$950 million in Septem- well as months of waiting for functional cells
than a small fraction of recipients. ber 2019. In March, Vertex announced that the to emerge. But he also notes that progenitor
US Food and Drug Administration had granted cells might be more resilient to implantation
Unlimited supply its proprietary mixture of insulin-making cells procedures, and that they’re easier and cheaper
The key characteristic of stem cells is that they and other endocrine cells, now called VX-880, to manufacture. Only clinical trials, he says, can
have the potential to differentiate into other fast track designation — and that the company determine which cell type is best.
cell types. Initial research involving human was commencing a 17-person phase I clinical
stem cells relied on cells taken from embryos trial that would be the first test in people of Immune protection
of terminated pregnancies; these cells can islet cells derived from stem cells. No matter which cells are implanted, however,
grow into almost any type. Later methods recipients’ bodies will not welcome them with
created stem cells from adult cells, known as “We showed conceptually open arms. Not only are these foreign cells,
induced pluripotent stem cells (iPSCs). Scien- and therefore prime targets for any immune
tists have worked to discover ways of direct-
that islet cell transplantation system, but they are also being administered
ing stem cells along particular developmental can dramatically improve to people whose bodies have a track record of
trajectories by applying signalling molecules patients’ lives.” specifically attacking β cells.
that switch the cells from one type to another. The simplest way to protect implanted cells
Although guided by knowledge of normal from immune destruction, which could make
development, uncovering the right signalling ViaCyte, meanwhile, has taken a slightly dif- the treatment pointless, is to administer them
molecules — and their correct concentrations ferent approach. “We and everyone else in the according to the Edmonton protocol, with a
and exposure times — is a largely empirical pro- field had the idea that we’re going to take stem full regimen of immunosuppressive drugs.
cess. Kevin D’Amour, who recently stepped cells, we’re going to make functional islets, This is what Vertex is doing in its first trial.
down as chief scientific officer at ViaCyte but then we’re going to transplant,” says D’Amour. “There aren’t a lot of cell therapies where you
remains an adviser to the company, recalls But an experiment he did in the mid-2000s have such a strong clinical precedent for the
“hundreds, if not thousands, of experiments” changed ViaCyte’s strategy. type of therapy,” says Vertex’s Felicia Pagliuca,
inching stem cells towards a β-cell phenotype. D’Amour’s group was leading the race to make who was involved in the creation of β cells
A huge appeal of this technology is that stem β cells, having pioneered methods for trans- in Melton’s laboratory. The trial will allow a
cells can be turned into continuously dividing forming human stem cells into pancreatic pro- comparison between VX-880 cells and islets
cell lines — cells from a single donor can give genitor cells6. But rather than trying to further transplanted from cadavers.
rise to trillions more. A self-renewing cell line transform these into islet cells, they injected the Ultimately, researchers want to spare recipi-
that can be straightforwardly transformed pancreatic progenitors straight into diabetic ents from lifelong immunosuppression. Current
into β cells (or hormone-making islet cells mice. Over 2–3 months, the cells matured into strategies focus on encapsulation, whereby
Nature | Vol 595 | 15 July 2021 | S65
©
2
0
2
1
S
p
r
i
n
g
e
r
N
a
t
u
r
e
L
i
m
i
t
e
d
.
A
l
l
r
i
g
h
t
s
r
e
s
e
r
v
e
d
.
Autoimmune disease
outlook
modify them to evade immune detection.
ViaCyte and Vertex are both exploring this,
but are tight-lipped about their strategies.
Melton sees several possible solutions.
One is to take cues from how cancer cells
evade immune destruction. Oncological
research has shown that expression of
certain cell-surface proteins inhibits immune
responses — a phenomenon that could be used
to protect β cells.
Another option is to engineer the cells’
antigen-presenting molecules. These could be
removed or, as Melton is doing, replaced. He’s
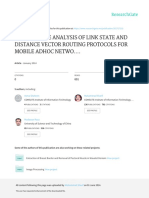
ALI ASADI (KIEFFER LABORATORY)
studying what happens if islet cells express the
fetal form of these molecules, which normally
prevent the mother’s immune system from
attacking fetuses.
And the possibilities offered by gene
editing do not end at cloaking the cells. The
technology could also be used “to enhance
In type 1 diabetes, immune cells (red) attack β cells (green) in the pancreatic islets. engraftment, survival and performance”,
Kieffer says. Cells could be adapted to better
implanted cells are shielded from the immune micro-encapsulation and has developed tolerate the mild hypoxia associated with
system by a physical barrier. This encapsula- a hydrogel-coating for cells that excludes encapsulation devices or poorly vascular-
tion can be macro, in which a credit card-sized immune cells while permitting β cell func- ized implantation sites, for instance, or even
device is filled with cells and implanted, or tion8. She is collaborating with Sernova, a to better tolerate being frozen for storage.
micro, where islets are individually coated in a regenerative-medicine company in London, “When we started on this, our goal was to
shielding polymer before delivery. Canada, on an approach where a cell pouch make a normal, natural β cell,” Melton says.
Encapsulation entails a delicate balance. is inserted below the skin two weeks before “Now I have a different goal. I don’t want to
Although the cells need to be isolated from micro-encapsulated islets are introduced. In make a normal cell — I want to make a super cell.”
the immune system, they must still have access this two-week period, new blood vessels enter The concern with all these approaches is
to nutrients and oxygen to survive. And in the the pouch and the initial inflammation subsides that the cells become too good at surviving.
case of β cells, to respond to circulating glu- — both of which should aid islet engraftment. In the absence of functional immune surveil-
cose they need excellent access to the blood- Sernova is currently assessing a basic cell pouch lance, if implanted cells become infected
stream, explains Alice Tomei, a biomedical in a phase I/II trial. with a virus or start to divide — potentially
engineer at the University of Miami in Florida. causing cancer or dangerously releasing
“If there is no vascularization, they can’t really “Now I have a different excess hormones — there needs to be a way
provide a good metabolic control,” she says. to eradicate them. Consequently, researchers
In 2014, ViaCyte’s first clinical trial of a
goal. I don’t want to make are studying ways of spiking β cells with sui-
macro-encapsulation device failed: recipi- a normal cell — I want to cide genes, which would produce a cell-killing
ents’ bodies recognized the device as foreign make a super cell.” protein upon cell division or when people are
and deposited a layer of immune cells on it, kill- given a specific drug.
ing the cells inside. The trial ViaCyte reported Melton thinks that incorporating suicide
in June, showing that its cells could mature in A further crucial aspect of continuing trials genes is a straightforward challenge compared
humans and provide a degree of clinical benefit, is determining where cells can be optimally with evading immune destruction. He dreams
used a stopgap encapsulation device punched placed. “I don’t think anybody knows where to of a future where cell therapy is routine and
with holes. The perforations allowed blood ves- put the devices,” says Melton. The field has so people can go years without thinking about
sels to grow into the device, sustaining the cells, far experimented with implanting them in vari- their diabetes. “I think it’s challenging,” he
but recipients required chronic immunosup- ous subcutaneous locations and is also, among says, “but I don’t think that’s crazy.”
pression because immune cells could also enter. other possibilities, considering the omentum —
ViaCyte and Vertex are now both develop- a large flap of fatty tissue that surrounds the Liam Drew is a freelance writer near London.
ing new macro-encapsulation devices that use intestines. Sites differ in their ability to gen-
innovative materials designed to not provoke erate vasculature in and around devices; their 1. Katsarou, A. et al. Nature Rev. Dis. Primers 3, 17016 (2017).
2. Gamble, A., Pepper, A. R., Bruni, A. & Shapiro, A. M. J.
a foreign body response. Vertex’s proprietary ability to hold devices and potentially tolerate
Islets 10, 80–94 (2018).
technology was developed in-house, whereas multiple implantations, if and when cells need 3. Shapiro, A. M. J. et al. N. Engl. J. Med. 343, 230–238
ViaCyte has partnered with materials company replacing; and also simply in how comfortable (2000).
W. L. Gore in Newark, Delaware, best known for it is to have a device implanted there. 4. Pagliuca, F. W. et al. Cell 159, 428–439 (2014).
5. Rezania, A. et al. Nature Biotechnol. 32, 1121–1133 (2014).
its Gore-Tex waterproof fabrics. The device
6. D’Amour, K. A. et al. Nature Biotechnol. 24, 1392–1401
they have worked on together is now entering Super cells
(2006).
phase II trials. An alternative to physically shielding islet 7. Kroon, E. et al. Nature Biotechnol. 26, 443–452 (2008).
Tomei, meanwhile, is focused on cells from the immune system is to genetically 8. Stock, A. A. et al. Stem Cell Rep. 14, 91–104 (2020).
S66 | Nature | Vol 595 | 15 July 2021
©
2
0
2
1
S
p
r
i
n
g
e
r
N
a
t
u
r
e
L
i
m
i
t
e
d
.
A
l
l
r
i
g
h
t
s
r
e
s
e
r
v
e
d
.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5811)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (844)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- Statement of Purpose (SOP) ExampleDocument2 pagesStatement of Purpose (SOP) ExampleMỹ Anh100% (1)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Mukul Bishwas - Internship ReportDocument51 pagesMukul Bishwas - Internship ReportAjayNo ratings yet
- The Client Brief - Full GuidelinesDocument131 pagesThe Client Brief - Full GuidelinesErhan İğdemir100% (1)
- High Frequency CommunicationDocument26 pagesHigh Frequency CommunicationpkNo ratings yet
- Report The History-Present and Future of CoachingDocument34 pagesReport The History-Present and Future of CoachingTeodoraNo ratings yet
- Hunter X Hunter Chapter 340 - English ScansDocument1 pageHunter X Hunter Chapter 340 - English ScansArya GhoshNo ratings yet
- Ravi Teja TalasilaDocument9 pagesRavi Teja TalasilaRafael AlacornNo ratings yet
- SOCIALSCIENCEDocument162 pagesSOCIALSCIENCES Lal100% (2)
- Trip The SafaryDocument3 pagesTrip The SafaryJorge InostrozaNo ratings yet
- Dark Blue Simple Modern ResumeDocument1 pageDark Blue Simple Modern ResumeHina UroojNo ratings yet
- WORKSHEET #8-Substitution of IngredientsDocument6 pagesWORKSHEET #8-Substitution of IngredientsJANICE RUBIALESNo ratings yet
- Do Small Businesses Get The Credit They Need?: Michaël Dewally, PH.DDocument4 pagesDo Small Businesses Get The Credit They Need?: Michaël Dewally, PH.DAnonymous Feglbx5No ratings yet
- The Collapse of Securitization: From Subprimes To Global Credit CrunchDocument14 pagesThe Collapse of Securitization: From Subprimes To Global Credit CrunchFernanda UltremareNo ratings yet
- ProjectReport PDFDocument86 pagesProjectReport PDFjerry tomNo ratings yet
- Haiti - Situation Report Nr. 6 - Insecurity - Access - Final - ENGDocument6 pagesHaiti - Situation Report Nr. 6 - Insecurity - Access - Final - ENGFuad AlawzariNo ratings yet
- CS1 HR 504Document2 pagesCS1 HR 504Alhad Posam100% (3)
- Standard Labour RateDocument10 pagesStandard Labour RateabasNo ratings yet
- Tutorial 2 EECF1624 2022 MemoDocument10 pagesTutorial 2 EECF1624 2022 MemoTshegofatso MatlalaNo ratings yet
- Giant ListDocument978 pagesGiant ListMark van EschNo ratings yet
- Week 8 - Q2 - Math 8Document11 pagesWeek 8 - Q2 - Math 8Jennilyn Salih AnogNo ratings yet
- Grade 9 Activity Sheets Quarter 1 Week 3Document8 pagesGrade 9 Activity Sheets Quarter 1 Week 3LadyAn DegamoNo ratings yet
- Ganpat University: Semester Grade ReportDocument1 pageGanpat University: Semester Grade ReportRishikesh KumarNo ratings yet
- Gato BarbieriDocument1 pageGato Barbierireihuno0% (1)
- Importance of Phonetics and Phonology in Language LearningDocument8 pagesImportance of Phonetics and Phonology in Language LearningoserobritonNo ratings yet
- Maxbridge Training and Cocsultancy A5Document9 pagesMaxbridge Training and Cocsultancy A5Awol AminNo ratings yet
- Guide To CGSTDocument12 pagesGuide To CGSTSunil RAYALASEEMA GRAPHICSNo ratings yet
- Hermann Herlinghaus Narcoepics A Global Aesthetics of SobrietyDocument273 pagesHermann Herlinghaus Narcoepics A Global Aesthetics of SobrietyAna Lucero Troncoso100% (1)
- Physics NLMDocument8 pagesPhysics NLMShrishNo ratings yet
- RismaAnisa-Tabel Pilihan Jurnal Timeline Final Progress Per MingguDocument22 pagesRismaAnisa-Tabel Pilihan Jurnal Timeline Final Progress Per MingguRisma AnisaNo ratings yet
- ComparativeSttate DVR LSRDocument7 pagesComparativeSttate DVR LSRAgrasen SinghNo ratings yet