Professional Documents
Culture Documents
Screenshot 2023-03-17 at 12.32.32 AM
Uploaded by
RenadCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Screenshot 2023-03-17 at 12.32.32 AM
Uploaded by
RenadCopyright:
Available Formats
Expand all sections REGISTER LOG IN
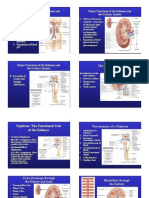
Physiology of the kidney Last updated: July 15, 2022
Summary
Urine production
Hormone synthesis
Physiology of the tubular system
Renal blood flow
Renal blood supply
Renal arteries (from the aorta) → segmental arteries → interlobar renal arteries → arcuate arteries →
intralobular renal arteries → afferent arterioles → glomeruli → efferent arterioles → vasa recta
(kidneys) and peritubular capillaries → renal veins (merge into the inferior vena cava)
Renal blood flow
Renal blood flow (RBF): the blood volume that flows through the kidney per unit of time
Normal: ∼ 20% of cardiac output, i.e., 1.2 L/min; kept at a constant rate by the renal autoregulatory
mechanism
RBF = RPF/(1 - Hct)
Renal plasma flow (RPF): the volume of plasma that flows through the kidney per unit of time
Para-aminohippuric acid (PAH): nearly 100% of PAH that enters the kidney is also excreted
(completely filtrated and secreted), thus clearance rate is used to estimate RPF
Effective renal plasma flow (eRPF)
eRPF = urine concentration of PAH × (urine flow rate/plasma concentration of PAH)
eRPF calculated with PAH slightly underestimates true RPF (see “Para-aminohippuric acid” below)
Regulation of renal blood flow [1]
The kidney has multiple mechanisms to regulate its own blood flow. This allows for changing the rate of
glomerular filtration if fluctuations in systemic blood pressure occur.
Myogenic autoregulation (Bayliss effect)
Mechanism
Blood flow in the renal arteries remains constant with varying arterial blood pressure (between 80–
180 mmHg).
Afferent arterioles contract if blood pressure increases; to maintain a normal pressure within the
glomeruli: ↑ arterial pressure → stretching of smooth muscle cells in the afferent arteriole wall →
contraction of vascular smooth muscles → vasoconstriction → ↓ RBF
If blood pressure drops, afferent arterioles dilate, to increase the pressure within the glomeruli
Prostaglandins
Mechanism: renal hypoperfusion (particularly renal medulla) → stimulation of prostaglandin synthesis
→ vasodilation of renal vessels → increased renal perfusion
Tubuloglomerular feedback
Description: feedback system between the tubules and glomeruli that adjusts the GFR according to the
resorption capacity of the tubules
Mechanism: macula densa (of the juxtaglomerular apparatus) senses alterations in the NaCl
concentration in the DCT
Hypotonic urine (↓ intraluminal Cl- concentration) → vasodilation of afferent arterioles → ↑ GFR
→ ↑ Cl- intraluminal concentration → ↑ RBF
Hypertonic urine (↑ intraluminal Cl- concentration) → adenosine secretion; → vasoconstriction
of afferent arterioles → ↓ capillary pressure → ↓ GFR → ↓ intraluminal Cl- concentration → ↓
RBF
Renin-angiotensin-aldosterone system (RAAS) [2]
Description: hormonal system that regulates arterial blood pressure and sodium concentration
Mechanism
Baroreceptors in the afferent arteriole detect the following
Renal hypoperfusion (e.g., caused by hypotension or hypovolemia)
Hyponatremia (registered by the macula densa when sodium concentration in the
distal convoluted tubule decreases)
Increased sympathetic tone (via activation of renal β1-receptors)
These changes cause a release of renin by juxtaglomerular cells → conversion of angiotensinogen
(produced in the liver) to angiotensin I → conversion of angiotensin I to angiotensin II via
angiotensin-converting enzyme (mostly produced in the lungs)
Angiotensin II
Acts as a strong vasoconstrictor
Desensitizes baroreceptors to hypertension preventing reflex bradycardia
Stimulates thirst in the hypothalamus
Increases ADH secretion from the posterior pituitary
Induces the secretion of aldosterone by the adrenal cortex
Aldosterone increases renal reabsorption of sodium and water; and augments the excretion of
potassium and protons → ↑ extracellular fluid, ↑ blood pressure, ↓ K+, ↑ pH
Effects
Systemic: ↑ arterial blood pressure and ↑ blood volume
Renal: maintenance of renal function and volume status in low volume states
↑ Vasoconstriction of the efferent arteriole causes ↑ effective filtration pressure and ↑
filtration fraction which helps maintain GFR (i.e., renal function) during renal hypoperfusion (i.e.,
decreased renal plasma flow)
Maintenance of GFR (i.e., renal function) during renal hypoperfusion (i.e., decreased
renal plasma flow) which is achieved by ↑ vasoconstriction of the efferent arteriole causing ↑
effective filtration pressure and ↑ filtration fraction
Compensatory increase in Na+ reabsorption in the proximal convoluted tubule (PCT) and
distal convoluted tubule (DCT) prevents net volume loss
ACE inhibitors inhibit the conversion of angiotensin I to angiotensin II. ARBs inhibit the
effect of angiotensin II. Both drug classes are used to treat arterial hypertension.
Besides their inhibitory effects on the heart (e.g., ↓ heart rate), β-blockers decrease blood
pressure by inhibiting β1-receptors of the juxtaglomerular apparatus (JGA), which leads to
decreased renin release.
Hormonal effects on the kidney
Natriuretic peptides
Atrial natriuretic peptide (ANP): volume overload → dilation of atria → secretion of ANP by
myocytes
Brain natriuretic peptide (BNP): volume overload → dilation of ventricles → secretion of BNP by
myocytes
Effects
Inhibit epithelial Na+ transporter in the collecting duct → increased Na+ and water secretion →
decrease in the central venous pressure
Dilates renal afferent arterioles (via ↑ cGMP in vascular smooth muscle) → ↑ GFR (without
compensatory Na+ reabsorption; ) and ↑ natriuresis
Inhibits secretion of aldosterone, renin, ADH, and ACTH
Antidiuretic hormone (ADH)
Increases contraction of smooth muscle in blood vessels via V1 receptor → increased blood pressure
→ increased kidney perfusion
Increases free water reabsorption in the collecting duct; (stimulation of adenylate cyclase → ↑
cAMP → incorporation of aquaporins in the luminal membrane of collecting ducts)
Increases urea resorption (↑ incorporation of urea transporters in the collecting duct) → increased
corticomedullary osmotic gradient → facilitated concentration of urine
Angiotensin II and aldosterone: see “Renin-angiotensin-aldosterone system“ section above
Parathyroid hormone (PTH)
Secretion is induced by ↓ Ca2+, ↓ 1,25-(OH)2 vitamin D3, and ↑ PO43- in the plasma
Effects on the proximal convoluted tubule (PCT): ↑ Ca2+ reabsorption, ↑ 1,25-(OH)2 vitamin D3
synthesis, and ↓ PO43- reabsorption
Autonomic regulation
Mechanism
Noradrenaline → binds to α1 receptors → vasoconstriction of arterioles → ↑ resistance → ↓
renal blood flow
Dopamine → binds to D1 receptors → vasodilatation of arterioles → ↓ resistance → ↑
renal blood flow
Hypovolemic shock with severe hypotension activates the sympathetic nervous system.
Subsequently, the hypovolemia and noradrenaline-induced vasoconstriction result in low
renal blood flow → low GFR → low urine production → acute renal injury
You have 2 free articles left for this month.
Extend your medical knowledge beyond Physiology of the kidney
Start your trial, and get 5 days unlimited access to over 1,100 medical articles and 5,000 USMLE
and NBME exam-style questions.
TRY FREE FOR 5 DAYS
Measurement of renal function
This section focuses on fluid compartments, the basics of glomerular filtration, and tubular secretion. For
more information on kidney function tests, see “Diagnostic evaluation of the kidney and urinary tract.”
Fluid compartments
60% of body mass is composed of water.
Two-thirds of the total body water (i.e., 40% of body mass) is intracellular fluid (ICF), which is mainly
composed of potassium, magnesium, and organic phosphates.
One-third of the total body water (i.e., 20% of body mass) is extracellular fluid (ECF), which is mainly
composed of sodium, chloride, bicarbonate, and albumin.
75% of ECF is interstitial fluid.
25% of ECF is plasma.
A small amount (∼ 500 mL) of ECF is transcellular fluid (e.g., gastrointestinal secretions, sweat,
pleural fluid, pericardial fluid, urine, synovial fluid, intraocular fluid, CSF).
ECF volume can be measured with crystalloid tracers such as inulin or mannitol, which distribute
throughout the ECF but do not enter cells.
ICF and ECF are separated by capillary walls and cellular membranes.
H2O can move between fluid compartments by osmosis or in response to pressure differences.
Total blood volume (TBV) is ∼ 6 L. Blood is composed of:
∼ 45% cellular components (99% of which are red blood cells), which is equivalent to hematocrit (Hct
)
∼ 55% plasma ∼ 55% plasma
Plasma volume can be calculated with VPlasma = TBV x (1 - Hct)
Serum osmolality (or plasma osmolality): 285–295 mOsm/kg H2O
The 60–40–20 rule refers to total body water (60% of body mass), ICF (40% of body mass),
and ECF (20% of body mass).
Think of HIKIN to help you remember the main intracellular ion: HIgh K+ INtracellularly.
Renal clearance
Description: : the volume of plasma that is cleared of a certain substance per unit of time
Mechanism
Cx = Ux x V/Px
Px = Plasma concentration of substance X (mg/mL)
V = Urine flow rate (mL/min)
Ux = Urine concentration of substance X (mg/mL)
Cx = Clearance of substance X (mL/min)
If the clearance of substance X is:
> GFR: net tubular secretion of substance X
< GFR: net tubular reabsorption or substance X is not freely filtered in the glomerulus
= GFR: no net tubular secretion of reabsorption
Glomerular filtration rate [3]
Description: : the rate at which fluid is filtered by the kidneys
Mechanism
Normal GFR
2
♂ 95–145 mL/min/1.73 m
2
♀ 75–125 mL/min/1.73 m
The GFR physiologically declines with age.
GFR depends on the effective filtration pressure and is driven by the difference between hydrostatic
and osmotic pressure
EFP = (PGC – PBS) – (πGC – πBS)]
GC = glomerular capillary
BS = Bowman space
P = hydrostatic pressure
π = osmotic pressure
πBS normally equals 0
Normal effective filtration pressure is 13 mm Hg.
GFR can be described by the Starling equation for the glomerulus: Jv = Kf × [(PGC - PBS) - σ(πGC -
πBS)]
Jv = net fluid flow
Kf = filtration constant
σ = Staverman reflection coefficient sigma
In clinical settings, the two most commonly used equations for calculation of estimated GFR are the
“Modification of Diet in Renal Disease (MDRD) Study equation” and the “Chronic Kidney Disease
Epidemiology Collaboration (CKD-EPI) equation” (see “Creatinine clearance“ below.
The GFR is used to estimate kidney function and to stage chronic kidney disease.
Relative solute concentrations along proximal convoluted tubules
Mechanism
Water is absorbed along the PCT along with other solutes (e.g., creatinine, electrolytes, glucose)
At the beginning of the PCT, the concentration of all solutes within the glomerularly filtered tubular
fluid (TF) is equivalent to the plasma concentration (P).
Compared to water, solutes can be reabsorbed along the PCT:
At the same rate →; no change in tubular fluid concentration compared to plasma concentration
(TF/P = 1)
At a lower rate →; increased tubular fluid concentration compared to plasma concentration (TF/P
> 1)
At a higher rate →; decreased tubular fluid concentration compared to plasma concentration (TF/P
< 1)
Specific solutes
Sodium (Na+): reabsorbed at the same rate as water throughout the PCT → (TF/P)Sodium = 1
Inulin
Not reabsorbed, nor secreted along the PCT → (TF/P)Inulin > 1
Inulin is unique in that its amount does not change along the PCT but its tubular concentration is
determined solely by water reabsorption.
PAH and creatinine: net tubular secretion along the PCT → (TF/P)PAH/Creat./Creat. > (TF/P)Inulin
>1
Chloride (Cl-): (TF/P)Chloride > 1 throughout the PCT
Initially reabsorbed at a slower rate than water and sodium → (TF/P)Chloride > 1 and rising
More distally in the PCT, reabsorbed at the same rate as water and sodium → still (TF/P)
Chloride > 1 but no longer increasing (plateaued)
Glucose: reabsorbed at a higher rate than water → (TF/P)Glucose < 1
The increase in inulin concentration along the PCT is the result of a constant amount of
inulin within the tubular fluid (no reabsorption or secretion) and the reabsorption of water.
The increase in inulin concentration along the PCT is the result of water reabsorption and
a constant amount of inulin within the tubular fluid (without tubular inulin secretion).
Water is reabsorbed along the PCT while the amount of inulin within the tubular fluid
stays the same (no reabsorption or secretion of inulin). This leads to an increasing
concentration of inulin along the PCT.
Inulin clearance
Description: used to assess the GFR
Mechanism
Inulin is freely filtered and neither reabsorbed nor secreted in the tubular system, i.e., the amount of
inulin in the urine reflects the amount that is filtered by the kidneys.
Inulin clearance can be used to calculate GFR: GFR = Uinulin x V/Pinulin = Cinulin
Uinulin = urine concentration of inulin
V = urine flow rate
Pinulin = plasma concentration of inulin
Cinulin = clearance of inulin
Creatinine clearance
Description: the rate of renal clearance of creatinine
Mechanism
Used in clinical settings to calculate GFR
Creatinine clearance = U x V / P
U = daily urine concentration of creatinine
V = rate of urine flow in mL/min
P = plasma concentration of creatinine
Direct calculation of creatinine clearance is time-consuming and becomes inaccurate if daily urine is
collected inappropriately.
Cockroft–Gault equation allows to estimate creatinine clearance
Creatinine clearance = ((140 - age) x weight (kg) x constant)/serum creatinine (mmol/L)
Constant = 1.23 for males and 1.04 for females
There are several prediction equations used in clinical practice to calculate estimated GFR (eGFR)
from serum creatinine concentration and demographic data:
Modification of Diet in Renal Disease (MDRD) Study equation
Chronic Kidney Disease Epidemiology Collaboration (CKD-EPI) equation
All of the equations typically overestimate actual GFR slightly because small amounts of creatinine
are secreted by the renal tubules; in clinical practice, this overestimation can be neglected.
Para-aminohippuric acid (PAH) [2]
Description: used to estimate effective renal plasma flow
Mechanism
PAH is freely filtered in the glomerulus; and secreted into the tubular lumen, but not reabsorbed.
Hence, almost 100% of the PAH that enters the kidney is excreted.
Effective renal plasma flow (eRPF)
See “Renal blood flow” section above
eRPF = UPAH x V/PPAH = CPAH
CPAH = clearance of PAH
PPAH = plasma concentration of PAH
V = urine flow rate
UPAH = urine concentration of PAH
Clearance depends on the plasma concentration of PAH (∼ 650 mL/min)
If the plasma concentration of PAH is low, it gets completely excreted from the plasma through
filtration and secretion.
Secretion is dependent on an organic anion transporter that is located on the basolateral
membrane of the proximal convoluted tubule.
If concentration of PAH surpasses the transport capacity of the anion transporters (or if there is
damage to the PCT ), secretion is impaired, which reduces the total excreted amount of PAH.
This leads to slight underestimation of renal plasma flow.
Glucose clearance
Description: used to assess for glucosuria
Mechanism
In normoglycemic states (blood glucose: 60–120 mg/dL), glucose is completely filtered and
completely reabsorbed in the proximal convoluted tubule (PCT) through
sodium-glucose cotransporters (SGLT2). Glucose is not secreted, therefore, its clearance is normally
0 mL/min.
Glucose threshold
Defined as the plasma glucose concentration at which glucose is no longer reabsorbed but instead
excreted in urine
It equals to 180 mg/dL
Splay phenomenon
When the glucose threshold is met, the tubular sodium-glucose cotransporters in some nephrons
are fully saturated, causing glucose to be excreted into the urine.
At the same time, the maximum glucose reabsorption rate in other nephrons is only reached with
higher glucose concentrations (heterogeneity of nephrons).
Therefore, after exceeding the glucose threshold, the overall glucose reabsorption rate initially
increases further with rising glucose concentrations until all glucose transporters in all nephrons
are saturated.
At a tubular glucose transport rate ; of 380 mg/min, all glucose transporters (SGLT2) are saturated
and glucose reabsorption cannot increase further.
Above the glucose filtration rate of 380 mg/min the glucose clearance is proportional to the plasma
concentration.
Pregnancy: ↑ GFR → ↑ filtration of all solutes (including glucose) → glucosuria with normal plasma
glucose levels
SGLT2 inhibitors: inhibition of sodium-glucose cotransporters → decrease of glucose threshold →
glucosuria with plasma glucose levels below 180 mg/dL
SGLT1 is located in the 1ntestine.
SGLT2 is located in the proximal 2bule.
Renal filtration
Filtration fraction (FF)
Description: the fraction of the renal plasma flow (RPF) that is filtered from the capillaries into the
Bowman space
Mechanism
FF = GFR/RPF (i.e., FF = CInulin/CPAH)
CInulin = inulin clearance
CPAH = PAH clearance
Normal: 20%
Regulated via:
Prostaglandins → dilation of afferent arterioles → ↑ GFR and ↑ RPF (FF unchanged)
Angiotensin II → constriction of efferent arterioles → ↑ GFR and ↓ RPF → ↑ FF
PDA - Prostaglandins Dilate Afferent arterioles
ACE - Angiotensin II Constricts Efferent arterioles
Filtered load
Description: the amount of a substance X that is filtered by the glomerulus per unit of time
Mechanism: filtered load (mg/min) = GFR (mL/min) x plasma concentration of substance X (mg/mL)
Changes in glomerular dynamics
Renal plasma Filtration Possible cause
flow fraction
↓ ↓ Unchanged Afferent arteriole constriction (e.g., due to ↓ prostaglandins from
NSAID use)
GFR
Renal artery stenosis
Unchanged ↓ Increased plasma protein concentration (e.g., due to
multiple myeloma)
Unchanged ↓ Obstructive nephropathy
↓ ↑ Severe dehydration (e.g., due to diarrhea, vomiting)
↓ Unchanged Glomerulonephritis
↑ ↓ ↑ Efferent arteriole constriction (e.g., due to ↑ angiotensin II due to
RAAS activation)
GFR
Unchanged ↑ Decreased plasma protein concentration (e.g., due to cirrhosis,
malnutrition)
Renal excretion
Excretion rate
Description: the amount of substance X that is excreted into the urine per unit of time
Mechanism: excretion rate (mg/min) = urine flow rate (mL/min) x urine concentration of substance X
(mg/mL)
Fractional excretion
Description: the proportion of the glomerular filtered substance X that is excreted in the urine
Mechanism
Fractional excretion = excreted load (urinary flow rate x urinary concentration of X)/filtered load (
GFR × plasma concentration of X)
FE < 1: a large proportion of the filtered substance is reabsorbed in the tubules (e.g., water,
glucose, amino acids, sodium chloride)
FE > 1: a small proportion of the filtered substance is reabsorbed or additional tubular secretion
occurs (e.g., PAH, atropine)
Fractional excretion of sodium (FeNa): percentage of the glomerular filtered sodium that is excreted
in the urine
Used to establish the cause of acute kidney injury
FeNa = (UNa x SCr/SNa x UCr) x 100
UNa = urine concentration of Na
SNa = serum concentration of Na
UCr = urine concentration of creatinine
SCr = serum concentration of creatinine
Reabsorption rate = filtered load (GFR × plasma concentration of X) - excreted load (urine flow rate x
urine concentration of X)
Secretion rate = excreted load - filtered load
Renal metabolism
The kidneys and heart are the organs with the highest resting metabolic rates and mitochondrial content.
Catabolism: The kidneys have a high demand for nutrients and oxygen for ATP production. The energy
is needed to excrete waste products, reabsorb nutrients, and regulate blood pressure, electrolytes,
serum osmolality, and acid-base balance.
Substrate utilization by individual nephron segments is determined by the following factors:
Availability of oxygen and pO2: decreases gradually from the renal cortex, which relies on
beta-oxidation and oxidative phosphorylation, to the renal medulla, which is more dependent on
anaerobic glycolysis to fulfill energy demands
Density of pumps and channels utilizing ATP (primarily Na+/K+-ATPase):
The more intensive the transtubular transport, the higher the energy demand and the more
intensive the substrate utilization.
The proximal tubules reabsorb 80% of filtrate, including ions, glucose, and nutrients, and
therefore require more ATP for active transport than other segments.
Main substrates
Proximal tubule: fatty acids
Thick ascending limb of the loop of Henle: glucose
Distal convoluted tubule and the collecting duct: glucose
[6]
Anabolism: Cortical renal cells are capable of gluconeogenesis in fasting states.
The limited oxygen supply to the medulla makes it highly susceptible to hypoxic injury
(especially the S3 segment of the proximal tubule and the medullary thick ascending limb
of the loop of Henle).
References
© 2020 AMBOSS Medical Knowledge Terms and Conditions Privacy Privacy Settings Legal Notice
Get Support & Contact Us
You might also like
- Anaesthesia in Renal Failure: Nadia Van Heerden Kimberley Hospital Complex 30 January 2015Document56 pagesAnaesthesia in Renal Failure: Nadia Van Heerden Kimberley Hospital Complex 30 January 2015Khaeril IrfanNo ratings yet
- RenalDocument8 pagesRenalLoislane RullNo ratings yet
- Perfusion for Congenital Heart Surgery: Notes on Cardiopulmonary Bypass for a Complex Patient PopulationFrom EverandPerfusion for Congenital Heart Surgery: Notes on Cardiopulmonary Bypass for a Complex Patient PopulationRating: 5 out of 5 stars5/5 (2)
- Renal Notes Unit 1Document66 pagesRenal Notes Unit 1Zha-Raa'iaam L SamoriNo ratings yet
- Renal Blood Flow SheetDocument16 pagesRenal Blood Flow SheetAmjad AmjadNo ratings yet
- EDEMA - 2023-2024 - 15 ModuleDocument7 pagesEDEMA - 2023-2024 - 15 Modulerislariyas13No ratings yet
- 3 - Regulation of RBF & GFRDocument12 pages3 - Regulation of RBF & GFRHamzehNo ratings yet
- 101 OHara PDFDocument11 pages101 OHara PDFAntonio Lopez HernandezNo ratings yet
- Functions of The Urinary System Anatomy of The Kidney Urine FormationDocument71 pagesFunctions of The Urinary System Anatomy of The Kidney Urine FormationmaninagaNo ratings yet
- Control of Extracellular Fluid Volume by The KidneyppDocument28 pagesControl of Extracellular Fluid Volume by The KidneyppLilian EdeniNo ratings yet
- Describe Long Term Regulation of Arterial Blood PressureDocument1 pageDescribe Long Term Regulation of Arterial Blood Pressurelinna chinNo ratings yet
- Urinary Sys@completeDocument48 pagesUrinary Sys@completeGhina MengalNo ratings yet
- Renal Blood FlowDocument17 pagesRenal Blood FlowAbu RidhuwanNo ratings yet
- ReninDocument3 pagesReninAli GalaNo ratings yet
- Renin-Angiotensin System: Navigation SearchDocument5 pagesRenin-Angiotensin System: Navigation SearchArchit PatelNo ratings yet
- Fluids and Electrolytes: Presented byDocument17 pagesFluids and Electrolytes: Presented byJohn Henry ValenciaNo ratings yet
- Renal PhysiologyDocument12 pagesRenal Physiologymina mounirNo ratings yet
- VSP-UG-7 (Kidney - Excretory System)Document50 pagesVSP-UG-7 (Kidney - Excretory System)6qhx62pr42No ratings yet
- Urinary Module NotesDocument22 pagesUrinary Module NotesAthira SureshNo ratings yet
- Urinary System: - Ridho IslamieDocument27 pagesUrinary System: - Ridho IslamieLaksmi DwiNo ratings yet
- Edema 231118 223936Document12 pagesEdema 231118 223936Sriram SriNo ratings yet
- JGLG TLA2 Refelective WritingDocument3 pagesJGLG TLA2 Refelective WritingJunnin Gay GarayNo ratings yet
- Kuliah Water Turnover 1Document25 pagesKuliah Water Turnover 1Sari JardiNo ratings yet
- Arterial Blood Pressure Regulation MechanismsDocument21 pagesArterial Blood Pressure Regulation Mechanismsnaresh sharmaNo ratings yet
- Nephron Structure and FunctionDocument7 pagesNephron Structure and FunctionAbdullah RajaNo ratings yet
- Renal Perfusion and Filtration: Alan Stephenson BBSG 503 - Systems BiologyDocument38 pagesRenal Perfusion and Filtration: Alan Stephenson BBSG 503 - Systems BiologyAfsaneh JavanmardNo ratings yet
- Renin-Angiotensin-Aldosterone System (RAAS) : Hyponatremia or Increased Sympathetic ToneDocument2 pagesRenin-Angiotensin-Aldosterone System (RAAS) : Hyponatremia or Increased Sympathetic ToneDrbee10No ratings yet
- 2long Term Regulation of Blood PressureDocument21 pages2long Term Regulation of Blood PressureamrendraNo ratings yet
- Renal Physiology: Functions of The KidneyDocument16 pagesRenal Physiology: Functions of The KidneyUsman Ali Akbar0% (1)
- Renin - Angiotensin System RAS Renin - Angiotensin-Aldosterone System RaasDocument3 pagesRenin - Angiotensin System RAS Renin - Angiotensin-Aldosterone System RaasReynaKatNo ratings yet
- Regulation of BPDocument48 pagesRegulation of BPSuiweng WongNo ratings yet
- Urine Formation-SGD 3Document9 pagesUrine Formation-SGD 3LA Yogore JermeoNo ratings yet
- Physio B 1.2 Renal Physiology Pt. 4 (Dr. Vila) : Because of Increase Water ReabsorptionDocument5 pagesPhysio B 1.2 Renal Physiology Pt. 4 (Dr. Vila) : Because of Increase Water ReabsorptionAnny AlvrzNo ratings yet
- Renal Lecture 1 PDFDocument29 pagesRenal Lecture 1 PDFSirajum MuneeraNo ratings yet
- Cvs 8Document45 pagesCvs 8Kim Sa-buNo ratings yet
- Renal Blood FlowDocument6 pagesRenal Blood FlowOsama MohamedNo ratings yet
- Urine FormationDocument49 pagesUrine FormationMajd HusseinNo ratings yet
- Questions From Exam 08.09.22Document12 pagesQuestions From Exam 08.09.22Ismo SNo ratings yet
- Blood Volume Systemic Vascular Resistance Cardiac Output Arterial PressureDocument2 pagesBlood Volume Systemic Vascular Resistance Cardiac Output Arterial PressureEdwin IndraNo ratings yet
- Renal Physiology: Glomerular Filtration Andrenal Blood Flow: Emmanuel A. Gutierrez, MDDocument73 pagesRenal Physiology: Glomerular Filtration Andrenal Blood Flow: Emmanuel A. Gutierrez, MDEmmanuel GutierrezNo ratings yet
- Leg Swelling Fluid Balance: Urine Insensible Fluid LossDocument9 pagesLeg Swelling Fluid Balance: Urine Insensible Fluid LossDarwithaNo ratings yet
- D - Renal PhysiologyDocument26 pagesD - Renal PhysiologyMohamad Zekry ZuhairyNo ratings yet
- Renal System: Powered by ATPDocument165 pagesRenal System: Powered by ATPNashir MahmudNo ratings yet
- Lo 1.2Document2 pagesLo 1.2robert leeNo ratings yet
- Kidney Anatomy & Physiology Modified. Anas ElianDocument11 pagesKidney Anatomy & Physiology Modified. Anas ElianAnas Abu ElianNo ratings yet
- Anatomi Dan Fisiologi GinjalDocument32 pagesAnatomi Dan Fisiologi GinjalScholastika PalayukanNo ratings yet
- Renin Angiotensin Aldosterone SystemDocument3 pagesRenin Angiotensin Aldosterone SystemDivya Ranasaria100% (1)
- Renal Physiology NotesDocument6 pagesRenal Physiology Notescipa920% (1)
- Practice Paper For MD1 2021 - AnswersDocument10 pagesPractice Paper For MD1 2021 - AnswersAlex TaylorNo ratings yet
- Fisiologi Pembentukan UrinDocument23 pagesFisiologi Pembentukan UrinKavin Maalan SadasseevanNo ratings yet
- Regulation of GFR Micturition ReflexDocument54 pagesRegulation of GFR Micturition ReflexadystiNo ratings yet
- Renin-Angiotensin SystemDocument5 pagesRenin-Angiotensin SystemZiedTrikiNo ratings yet
- Kidney_AG-1Document170 pagesKidney_AG-1aleenashibu993No ratings yet
- Renal PhysiologyDocument87 pagesRenal PhysiologyQusaiBadrNo ratings yet
- Kidneys BiochemistryDocument53 pagesKidneys BiochemistryMi PatelNo ratings yet
- Lung InflammationDocument44 pagesLung InflammationOnSolomonNo ratings yet
- Mechanism of Urine FormationDocument35 pagesMechanism of Urine FormationHemanth PrakashNo ratings yet
- Support of Renal Function: A Guide to Acute Renal Failure, Anatomy, Physiology and RegulationDocument86 pagesSupport of Renal Function: A Guide to Acute Renal Failure, Anatomy, Physiology and RegulationRo-Anne LozadaNo ratings yet
- Water Homeostasis: Benjamin/Cummings Publishing CoDocument11 pagesWater Homeostasis: Benjamin/Cummings Publishing CoDawlat SalamaNo ratings yet
- Nursing Drug CardsDocument32 pagesNursing Drug CardsJenna Rasmussen100% (3)
- Bazopril Is Legit (2023) Latest Updates!Document1 pageBazopril Is Legit (2023) Latest Updates!BazoprilBloodPressure SupportFormulaNo ratings yet
- Flash Pulmonary Oedema and Bilateral Renal Artery Stenosis: The Pickering SyndromeDocument8 pagesFlash Pulmonary Oedema and Bilateral Renal Artery Stenosis: The Pickering SyndromeMahmoud DiaaNo ratings yet
- Acute Glomerulonephritis Case StudyDocument12 pagesAcute Glomerulonephritis Case StudyPrincess Tindugan100% (1)
- Test Bank UrinaryDocument58 pagesTest Bank UrinaryDesiree ArquisolaNo ratings yet
- 10,11-Arterial Blood Pressure & Its Regulation Team441Document51 pages10,11-Arterial Blood Pressure & Its Regulation Team441saran kNo ratings yet
- Fluid Management An Update For Perioperative PractitionersDocument9 pagesFluid Management An Update For Perioperative PractitionersYuda PrawiraNo ratings yet
- Endocrine SystemDocument59 pagesEndocrine SystemCharm Angeles100% (3)
- Regulation of BPDocument48 pagesRegulation of BPSuiweng WongNo ratings yet
- Metheny - Fluid and Electrolyte Balance 4th EdDocument227 pagesMetheny - Fluid and Electrolyte Balance 4th Edfirst aid kit100% (1)
- Medications To Avoid in Retinitis PigmentosaDocument7 pagesMedications To Avoid in Retinitis PigmentosasosoNo ratings yet
- 10 - AutacoidsDocument67 pages10 - AutacoidscchatrumaNo ratings yet
- Renal Basic Good NotesDocument25 pagesRenal Basic Good Noteslovelyc95No ratings yet
- Insuficiencia Cardiaca Congestiva IzquierdaDocument10 pagesInsuficiencia Cardiaca Congestiva IzquierdaCindy Karina Carbajal MurilloNo ratings yet
- Neuroendocrinology and Behavior - T. Sumiyoshi (Intech, 2008) WWDocument172 pagesNeuroendocrinology and Behavior - T. Sumiyoshi (Intech, 2008) WWvladex77100% (2)
- AutacoidsDocument34 pagesAutacoidsBrîndușa PetruțescuNo ratings yet
- Acupuncture Application in Chronic Kidney Disease and Its Potential MechanismsDocument17 pagesAcupuncture Application in Chronic Kidney Disease and Its Potential MechanismsHenrique Martins FilhoNo ratings yet
- Pathophysiology and Etiology of Edema - IDocument9 pagesPathophysiology and Etiology of Edema - IBrandy MaddoxNo ratings yet
- Renal McqsDocument13 pagesRenal McqsShahabuddin Shaikh100% (1)
- HT Age Based PDFDocument8 pagesHT Age Based PDFDoni TrinandaNo ratings yet
- Endocrine EssentialsDocument226 pagesEndocrine EssentialsMxt Nút100% (3)
- Pediatric Nephrology, 7th EditionDocument65 pagesPediatric Nephrology, 7th EditionDavien Utoyo100% (1)
- Biochem Final Exam MCQs PDFDocument173 pagesBiochem Final Exam MCQs PDFzeeshan jaskaniNo ratings yet
- 2023 ESH Guidelines For The Management of Arterial HypertensionDocument199 pages2023 ESH Guidelines For The Management of Arterial HypertensionErika Jiménez De LaraNo ratings yet
- RAAS: (Renin Angiotensin Aldosterone System) : How Does This System Work?Document3 pagesRAAS: (Renin Angiotensin Aldosterone System) : How Does This System Work?Sameen FatimaNo ratings yet
- Adrenal Function: T. Creighton Mitchell, A. Wayne MeikleDocument19 pagesAdrenal Function: T. Creighton Mitchell, A. Wayne MeikleWho KnowsNo ratings yet
- Endocrinology of Genitourinary SystemDocument4 pagesEndocrinology of Genitourinary SystemGerardLumNo ratings yet
- Antagonis Reseptor Angiotensin 2, AIIRADocument31 pagesAntagonis Reseptor Angiotensin 2, AIIRAsuho exoNo ratings yet
- Presented by - Yogesh Dengale 1 M.SC NursingDocument56 pagesPresented by - Yogesh Dengale 1 M.SC NursingalexjohnvtNo ratings yet