Professional Documents
Culture Documents
Fecal Elimination
Uploaded by
Crazy Stranger0 ratings0% found this document useful (0 votes)
2 views13 pagesOriginal Title
FECAL ELIMINATION
Copyright
© © All Rights Reserved
Available Formats
DOCX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
2 views13 pagesFecal Elimination
Uploaded by
Crazy StrangerCopyright:
© All Rights Reserved
Available Formats
Download as DOCX, PDF, TXT or read online from Scribd
You are on page 1of 13
FECAL ELIMINATION o 100 ml is reabsorbed and 100 ml of
fluid is excreted in the feces
PHYSIOLOGY OF DEFACATION o Colon serves as a protective
o Elimination of waste products of function in that it secretes mucous
digestion from the body is essential o Mucous secretion is stimulated by
o Feces or stool – excreted waste excitation of parasympathetic nerves
products o During extreme stimulation large
amounts of mucous secreted,
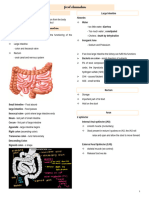
LARGE INTESTINES resulting in the passage of stringy
mucous with little or no feces
o Extend from the iloecal valve to the o Mucous serves to protect the wall of
anus the large intestine from trauma
o Has 7 parts: o It serves and adherent for holding
Cecum the fecal material together
Ascending colon - Mucous also protects the
Transverse colon intestinal wall from bacterial
Descending colon activity
Sigmoid colon o Colon acts as transport along its
Rectum
lumen the product of digestion –
Anus
flatus and feces
o A muscular tube lined with mucous
Flatus
membrane
- Largely air and the by-
o The muscle fibers are both circular
products of the digestion of
and longitudinal carbohydrates
o Longitudinal muscle are shorter than
Haustra churning
the colon and cause the large - Involves movement of the
intestine to form pouches or haustra chyme back and forth within
o Main function: the haustra
Absorption of water and - This action aids in the
nutrients absorption of water and
Mucoid protection of the moves the contents to the
intestinal wall next haustra
Fecal elimination Peristalsis
Ingestion – act of taking in food - Wave-like movement
Chyme produced the circular and
- Waste products leaving the longitudinal muscle fibers
stomach through the small - It propels the intestinal
intestine and then passing contents forward
through the ileocal value - Colon peristalsis is very
Ileocal valve sluggish and is thought to
- Regulates the flow of chime move the chyme very little
into the large intestine and along large intestine
prevents backflow into the Mass peristalsis
ileum
- Involves a wave of powerful o When internal anal sphincter
muscular contraction that relaxes, feces move into the anal
moves over large areas of canal
colon o Expulsion of the feces is assisted by
- Occurs after eating contraction of the abdominal muscle
and diaphragm
RECTUM AND ANAL CANAL
o Normal defecation is assisted:
Rectum Thigh flexion, increases the
- Has folds that extend pressure within the abdomen
vertically Sitting position, increases the
- Each of the vertical folds downward pressure on the
contains a vein and an artery rectum
- These folds help retain feces o If defecation reflex is ignored, the
within rectum urge to detach normally disappears
Hemorrhoids
FECES
- When veins become
distended, as can occur with o Made of 75% water and 25% solid
repeated pressure material
Anal canal o If quickly propelled = not time for
- Bounded by an internal and most of the water in the chyme to be
external sphincter reabsorbed
- Internal sphincter is under o Normal feces require a normal fluid
involuntary control and intake
innervated by the autonomic o Feces that contain less water may
nervous system be difficult to expel
- External sphincter is under o Feces are normally brown, due to
voluntary control and the presence of stercobilin and
innervated by the somatic urobilin
nervous system o Another factor that affects fecal color
DEFECATION is the actionof bacteria
o Action of microorganism on the
o Expulsion of the feces from the anus chyme is responsible for the odor of
and rectum the feces
o Also called bowel movement o Gases:
o Frequency of defecation is highly Carbon dioxide
individual Methane
o Amount defecated also varies from Hydrogen
person to person Oxygen
o Peristaltic waves move the feces Nitrogen
into the sigmoid colon and the
FACTORS
rectum, sensory nerves in the
rectum are stimulated and becomes DEVELOPMENT
aware of the need to defecate
NEWBORN AND INFANTS OLDER ADULT
Meconiun o Up to half of all older adults suffer
- First fecal material passed by from constipation
the newborn o Due to:
- Black, tarry, odourless, and Reduced activity levels
sticky Inadequate fluid and fiber
- Transitional stools are intake
greenish yellow; they contain Muscle weakness
mucous and are loose o Older adults should be advised that
o Infants pass stool frequently often normal patterns of bowel movement
after each feeding vary considerably
o Intestine is immature, water is not o Constipation can be relieved by
well absorbed and stool is soft, increasing the fiber intake to 20-35
liquid, and frequent grams per day, unless
o When matures, bacterial flora contraindicated
increase o Preventive measures:
o Infants who are breast-fed have light Adequate roughage in the
yellow to golden feces diet
o Infants taking formula will have a Adequate exercise
dark yellow or tan stool 6-8 glass of fluid daily
Cup of hot water or tea at
TODDLERS regular time
Gastrocolic reflex
o Nervous and muscular system are
- Increased peristalsis of the
sufficiently well developed to permit
colon after food has entered
bowel control
the stomach
o Desire to control day time movement
o Consistent use laxatives inhibits
use the toilet when:
natural defecation reflex
Discomfort caused by a
o Laxatives may interfere with
soiled diaper
Sensation that indicates the electrolyte balance and decrease the
need for bowel movement absorption of certain vitamins
o Day time control is attained by age 2 o Nurse should evaluate any
½ after process of toilet training complaints of constipation
o Change in bowel habits over several
SCHOOL-AGE AND ADOLESCENTS weeks with or without weight loss,
pain, or fever should referred to
o Have bowel habits similar to those of primary care provider
adults
o Patterns of defecation vary in ACTIVITY
frequency, quantity, and consistency
o Activity stimulates peristalsis
o Some school age may delay
defecation because of an activity
such as play
o Weak abdominal and pelvic muscle through the digestive
are ineffective in increasing the intra- system
abdominal persn Increase stool bulk
o Weak muscle can result from: Sources: whole
Lack of exercise wheat, wheat bran,
Immobility nuts, and vegetables
Neurologic functioning Soluble fibers
o Clients confined to bed are often Dissolves in water to
constipated form gel-like material
Help lower blood
FLUID INTAKE AND OUTPUT cholesterol and
glucose level
o Even when fluid intake is inadequate
Sources: oats, peas,
or output is excessive, the body beans, apples, citrus
continuous to reabsorb fluid from the fruits, carrots, barley,
chyme as it passes along the colon psyllium
o Chyme becomes drier resulting in o Daily amount of fibers:
hard feces Men ages 50 and younger =
o Reduced fluid intake slows the 38 grams
chymes passage along the Men ages 51 and older = 30
intestines, increasing reabsorption of grams
fluid Women ages 50 and
o Healthy fecal elimination requires younger = 25 grams
daily fluid intake of 2,000 to 3,000 ml Women ages 51 and older =
o If chyme moves abnormally quickly, 21 grams
less time for fluid to be absorbed into o Important to drink plenty of water
the blood; the feces are soft or even because fiber works best when it
watery absorbs water
o Bland diets and low-fiber diets are
DIET
lacking in bulk and creates
o Sufficient bulk (cellulose, fiber) in the insufficient residue of waste
diet is necessary provide fecal products to stimulate reflex for
volume defecation
o Inadequate intake of dietary fiber o Low residue foods move more
contributed to the risk of developing: slowly through the intestinal tract
Obesity thus increase fluid intake
Type 2 diabetes o Irregular eating can also impair
Coronary artery disease regular defecation
Colon cancer o Spicy foods can produce diarrhea
o 2 types of fiber: and flatus
Insoluble fibers o Excessive sugar can also cause
Promotes the diarrhea
movement of material o Foods that influence bowel
movement:
Gas-producing o Early bowel training may establish
Laxative-producing the habit of defecating at a regular
Constipation-producing time
o Many people defecate after
PSYCHOLOGICAL FACTOR
breakfast, when gastrocolic reflex
o Anxiety and anger increase cause mass peristaltic waves in the
peristaltic activity and subsequent large intestine
nausea or diarrhea o Normal defecation reflex is ignored,
o People who are depressed may reflexes tend to progressively
experience slowed intestinal motility weakened
= constipation o Habitually ignored, urge to defecate
o Responses to these emotional is ultimately lost
states is the result of individual o Adult may ignore these reflexes
differences in the response of the because of the pressure of time or
enteric nervous system to vagal work
stimulation from the brain o Hospitalized client may suppress the
urge because of embarrassment
MEDICATION about using a bedpan, lack of
privacy, or defecation us too
o Repeated administration of
uncomfortable
morphine and codeine, cause
constipation because they decrease DIAGNOSTIC PROCEDURE
gastrointestinal activity through their
action on the CNS o Before certain diagnostic procedure,
o Iron supplements act more locally on the client is restricted from ingesting
the bowel mucosa and can cause food or fluid
constipation or diarrhea o Client may also be given a cleansing
laxatives – stimulate bowel activity enema prior to the examination
and so assist fecal elimination o In these instances normal defecation
o drug that causes gastrointestinal usually will not occur until eating
bleeding can cause the stool to be resumes
red or black
PATHOLOGIC CONDITION
o iron salts lead to black stool because
of oxidation of the iron o Spinal cord injuries and head injuries
o antibiotics cause gray-green can decrease the sensory
discoloration stimulation for defecation
o antacids can cause whitish o Impaired mobility may limit client’s
discoloration or white specks ability to respond to the urge to
Pepto-Bismol – causes stools to be defecate and the client may
black experience constipation
o Client may experience fecal
DEFACATION HABIT
incontinence because of poorly
functioning anal sphincters
ANESTHESIA AND SURGERY o Careful assessment of the person’s
habits is necessary before a
o Cause the normal colonic diagnosis of constipation is made
movements to cease or slow by o Causes and factors:
blocking parasympathetic stimulation
Insufficient fiber intake
to the muscles of the colon
Insufficient fluid intake
o Regional or spinal anesthesia are
Insufficient activity or mobility
less likely to experience this problem Irregular defecation habits
o Surgery that involves direct handling Change in daily routine
of the intestines can cause Lack of privacy
temporary cessation of intestinal Chronic use of laxatives or
movement last 24-48 hrs – ileus enemas
o Listening for bowel sounds that Irritable bowel syndrome
reflect intestinal motility is an Pelvic floor dysfunction
important nursing assessment Poor motility
following surgery Neurologic condition
Emotional disturbance
PAIN
Medication
o Discomfort when defecating often Habitual denial and ignoring
suppress the urge to defecate to urge
avoid the pain o In children, constipation is often
o Clients taking narcotic analgesics for associated with changes in activity,
pain may also experience diet, and toileting habits
constipation as a side effect of the o Valsalva maneuver can present
medication serious problem to people with heart
disease, brain injuries, or respiratory
FECAL ELIMINATION PROBLEMS disease
o Holding the breath while bearing
CONSTIPATION
down increases intrathoracic
o Fewer than three bowel movement pressure and vagal tone, slowing
per week pulse rate
o Infers the passage of dry, hard stool,
FECAL IMPACTION
or the passage of no stool
o Occur when movement of feces o Mass or collection of hardened feces
through the large intestine is slow in the folds of the rectum
o Associated with constipation: o Results from prolonged retention
Difficult evacuation of stool and accumulation of fecal material
Increased effort or straining o Severe impactions, the feces
of the voluntary muscles of accumulate and extend up into the
defecation sigmoid colon and beyond
Feeling of incomplete stool o Client will experience the passage of
evacuation liquid fecal seepage (diarrhea) and
no normal stool
o Assessed by digital examination of o Spasmodic cramps are associated
the rectum with diarrhea
o Symptoms: o Bowel sounds are increased
Frequent but non-productive Persistent diarrhea – irritation of
desire to defecate the anal region extending to the
Rectal pain perineum and buttocks
o Generalized feelings of illness: Prolonged diarrhe – fatigue,
Anorexic weakness, malaise, and emaciation
Abdomen becomes are results
distended o Cause is irritants:
Nausea and vomiting Is thought to be a protective
o Causes of fecal impaction: flushing mechanism
Poor defecation habit Can create serious fluid and
Constipation electrolyte losses
Medication (anticholinergic Clostridium Difficile
and antihistamines) - Produces mucoid and foul-
Barium – used in radiologic smelling diarrhea
examination - Highest risk:
o Client is often given: Immunosuppressed
Oil retention enema individual
Cleansing enema Client on
Daily additional cleansing chemotherapy
enema Used antimicrobial
Suppositories agent
Stool softness - Older adult are at great risk
o If these measures fails, manual - Infection control:
removal is often necessary Hand hygiene (soap
and water)
DIARRHEA Contact precautions
Cleaning with bleach
o Passage of liquid feces and an
solution
increased frequency of defecation
o Irritating effects of diarrhea stool
o Results from rapid movement of
increases the risk of skin breakdown
fecal contents through the large
o Area around the anal region should
intestines
be kept clean and dry and protected
o Reduces the time available for the
with zinc oxide or other ointment
large intestines to reabsorb
o Fecal collector can be used
electrolyte and water
o Diarrhea is not present unless the BOWEL INCONTINENCE
stool is relatively unformed and
excessively liquid o Also called fecal incontinence
o Finds it difficult or impossible to o Loss of voluntary ability to control
control the urge to defecate fecal and gaseous discharges
through anal sphincter
o Two types of bowel incontinence: BOWEL DIVERSION OSTOMIES
Partial incontinence
- Inability to control Ostomy – opening for the GI,
flatus or to prevent urinary, respiratory tract on the skin
minor soiling Gastrostomy – opening through
Major incontinence abdominal wall into the stomach
- Inability to control Jejunostomy – abdominal wall into
feces of normal jejunum
consistency Ileostomy – opens into the ileum
o Associated with impaired function of Colostomy – opens into the colon
the anal sphincter or its nerve supply o Provide alternate route for food
o Prevalence of bowel incontinence o Purpose: divert and drain fecal
increase with age material
o Bowel incontinence is emotionally o Classification:
distressing problem that can lead to Permanent or temporary
social isolation Anatomic location
o Several surgical procedures are Construction of stoma
used for the treatment: Stoma
Repair of the sphincter Opening creased the
Colostomy (bowel diversion) abdominal all by ostomy
Red in color and moist
FLATULENCE No nerve endings
o 3 primary sources: PERMANENCE
Action of bacteria on the
chyme in the colon o Temporary colostomies are
Swallowed air generally performed for traumatic
Gas that diffuses between injuries or inflammatory conditions of
the bloodstream and the bowel
intestine Allow the distal diseased
Most gases that are portion of the bowel to rest
swallowed are expelled and heal
through the mouth by o Permanent colostomies are
eructation (belching) performed to provide means of
Presence of excessive flatus elimination hen the rectum or anus is
in the intestines and leads to nonfunctional
stretching and inflation of the
intestines ANATOMICAL LOCATION
Can occur in the colon from
Ileostomy – empties from the distal
variety of causes
end of the small intestine
If gas is propelled by
Cecostomy – empties from the
increase colon activity, it may
cecum
be expelled through the anus
Ascending colostomy – empties
If not, insert rectal tube to
from the ascending colon
remove it
o Location of the ostomy influences Loop of bowel is brought out
the character and management of onto the abdominal wall and
the fecal drainage supported by a plastic bridge
o The farther along the bowel, the or by a piece of rubbing tube
more formed the stool and more Usually performed in
control over the frequency of stomal emergency procedure and
discharge can be establish often situated on the right
Ileostomy transverse colon
Produces liquid fecal Bulky stoma is more difficult
drainage to manage than a single
Constant and cannot be stoma
regulated Loop stoma has two
Contains digestive enzyme openings:
Odor is minimal Proximal / Afferent –
Ascending colostomy active
Drainage is liquid and cannot Distal / Efferent -
be regulated inactive
Odor is a problem requiring Divided colostomy
control Consist of two edges of
Transverse colostomy bowel brought out onto the
Malodorous, mushy drainage abdomen but separated from
Usually no control each other
Descending colostomy Opening from the digestive
Solid fecal drainage or proximal end is the
Formed consistency, and colostomy
frequency of discharge can Distal end is called/referred
be regulated as mucous fistula
o Length of time also helps to Often used in situation where
spillage feces into the distal
determine the consistency of the
end of the bowel needs to be
stool
avoided
SURGICAL CONSTRUCTION OF STOMA Double-barrelled colostomy
Resembles a double-
o Described as single, loop, divided, or barrelled shotgun
double-barrelled colostomies Proximal and distal loops of
o Single stoma is created when one bowels are sutured together
end of bowel is brought out through and both ends are brought
an opening onto the anterior up unto the abdominal wall
abdominal wall
Referred to as an end or NURSING MANAGEMENT
terminal colostomy; stoma is
ASSESSING
permanent
Loop colostomy NURSING HISTORY
o Helps the nurse ascertain the client’s DIAGNOSING
normal pattern
o Diagnostic labels for fecal
o Elicits a description of usual feces
and any recent changes and collects elimination:
information about any past or current Bowel incontinence
problems about elimination, the Constipation
presence of anostomy, and factors Risk for constipation
influencing elimination pattern Perceived constipation
o Nurse needs to understand that the Diarrhea
Dysfunctional GI motility
time of defecation and the amount of
o Etiology:
feces expelled are as individual as
the frequency of defecation Risk for Deficient Fluid
o Patterns individual follow depend Volume and/or Risk for
Electrolyte Imbalance
largely on early training and on
Prolonged diarrhea
convenience
Abnormal fluid loss
PHYSICAL EXAMINATION through ostomy
Risk for Impaired Skin
o Physical examination includes Integrity
inspection, auscultation, percussion, Prolonged diarrhea
and palpation Bowel incontinence
o Auscultation precedes palpation Bowel diversion
because palpation can alter ostomy
peristalsis Situational Low Self-Esteem
o Examination of rectum and anus Ostomy
includes inspection and palpation Fecal incontinence
Need for assistance
INSPECTING FECES with toileting
Disturbed Body Image
o Observe:
Ostomy
Color
Bowel incontinence
Consistency
Deficient Knowledge
Shape
Anxiety
Amount
Lack of control of
Odor
fecal elimination
Presence of abnormal
Response of others to
constituents
ostomy
DIAGNOSTIC STUDIES
PLANNING
o Diagnostic studies of GI tact:
o Major goals:
Direct visualization technique
Maintain or restore normal
Indirect visualization
bowel elimination pattern
technique
Maintain or regain normal
Laboratory tests for abnormal
stool consistency
constituents
Prevent associated risk Types of foods to assist
o Appropriate preventive and client with normal defecation
corrective nursing interventions that For constipation
relate to these must be identified Increase daily fluid intake
o Specific nursing intervention can be Drink hot liquids
selected to meet the client’s Warm water with squirt of
individual needs fresh water
Include fiber in diet
PLANNING FOR HOMECARE For diarrhea
o In preparation for discharge, the Encourage oral intake of
fluids and bland food
nurse needs to assess the clients
Eating small amounts can be
and family’s ability to met specific
helpful
care needs
Excessively hot or cold
o The nurse designs a teaching plan
should be avoided
for the client and family
Highly spiced food and high
IMPLEMENTING fiber can aggravate diarrhea
For flatulence
PROMOTING REGULAR DEFACATION Limit carbonated beverages
Use of drinking straw
PRIVACY
Chewing gum
o Nurse should provide as much Gas forming foods should be
privacy as possible but may need to avoided
stay with those who are too weak
EXERCISE
o Some clients prefer to wipe, wash,
and dry themselves after defecating o Helps clients develop a regular
o Nurse may need to provide water, defecation pattern
washcloth, and towel o Client with weak abdominal and
pelvic muscles may be strengthen
TIMING
through isometric contraction
o Client should be encouraged to
POSITIONING
defecate when urge is recognize
o To establish regular elimination, the o Squatting position best facilitates
client and nurse can discuss when defecating
mass peristalsis usually occur and o For clients who have difficult sitting
provide time for defecation down and getting up, an elevated
seat can be attached to a regular
NUTRITION AND FLUIDS
toilet
o The diet a client needs for regular Bedside commode
normal elimination Portable chair with a toilet
o Depending: seat and a receptacle
Kind of feces beneath that can be emptied
Frequency of defecation Bedpan
Receptacle for urine and Establish regular
feces defecation habits
Two main types: o Suppositories
High-back pan Softening the feces by:
Slipper pan – used for Releasing gas to
clients unable to raise distend the rectum
their buttocks Stimulate the nerve
endings in the rectal
TEACHING MEDICATIONS
mucosa
CATHARTICS AND LAXATIVES
ANTIDIARRHEAL MEDICATION
Cathartics o Show the motility of the insertion or
Drugs that induce defecation
absorb excess fluid in the intestine
Can have strong, purgative
effect ANTIFLATULENT MEDICATIONS
Examples:
Castor oil o They also coalesce the gas bubbles
Cascara and facilitate their passage by
Phenolphthalein belching through the mouth or
bisacodyl expulsion to the arms
Laxatives o Combination of simithicone and
Is mild and produces soft or loperamide is effective in relieving
liquid stools that are abdominal bloating and gas
sometimes accompanied by associated with acute diarrhea
abdominal cramps Carminatives
Contraindicated in the client Herbal oils known to act as
who has nausea, cramps, agents that help expel gas
colic, vomiting, or from the stomach and
undiagnosed abdominal pain intestines
Clients need to be informed o Suppositories can also be given to
about danger of laxative use relieve flatus by increasing intestinal
Continual use of laxative motility
weakens the bowel’s natural
responses to fecal distention, DECREASING FLATULENCE
resultingto chronic o Ways to reduce or expel flatus:
constipation
Exercise
To eliminate chronic laxative
Moving in bed
use:
Ambulation
Teach about dietary
Avoiding gas-producing
fiber
foods
Regular exercise
o Movement stimulates peristalsis and
Taking sufficient
the escape of flatus and
fluids
reabsorption of gases in the
intestinal capillaries
Probiotics Remove feces
Helpful in the management of in the
flatulence and bloating instances of
Helpful for various GI constipation or
disorders impaction
Bismuth Subsalicylate Carminative enema
Can be effective but should - Given primarily to
not be used as a continuous expel flatus
treatment because it contains - Solution instilled into
aspirine and could cause the rectum release
salicylate toxicity gas, which distend
Alpha-galactosidase the rectum and colon,
Effective for reducing stimulating peristalsis
flatulence caused by eating Retention enema
fermentable carbohydrates - Introduces oil or
medication into the
ADMINISTERING ENEMAS rectum and sigmoid
colon
Enema - Acts to soften the
Solution introduced into the feces and to lubricate
rectum and large intestine the rectum and anal
Distend the intestine and canala
irritate the intestinal mucosa, - Antibiotic enemas –
increasing the peristalsis and treat infection
the excretion of feces and - Anthelmintic – kill
flatus hemlinths
Enema solution should be at - Nutritive –administer
37.7°C because a solution fluids and nutrients
that is too hot or too cold is into the rectum
uncomfortable and cause Return-flow enema
cramping - Called a Harris Flush
o 4 groups: - Used to expel flatus
Cleansing enema - Repeated for 5-6
- Intended to remove times until flatus is
feces expelledand
- Given chiefly to: abdominal distention
Prevent is relieved
escape of
feces during
surgery
Prepare the
intestine for
certain
diagnostic test
You might also like
- Enema - HANDOUTSDocument4 pagesEnema - HANDOUTSYalc LapidNo ratings yet
- Reviewer Chap 49 Fecal EliminationDocument3 pagesReviewer Chap 49 Fecal EliminationKeren GaciasNo ratings yet
- Bowel and Urine EliminationDocument25 pagesBowel and Urine Elimination3amabelle arevalo100% (1)
- 01 EnemaDocument4 pages01 Enemabunso padillaNo ratings yet
- Gross Anatomy of The Digestive System Lecture Notes Lecture 2Document5 pagesGross Anatomy of The Digestive System Lecture Notes Lecture 2Lorelie AsisNo ratings yet
- Large Intestine 2021Document18 pagesLarge Intestine 2021ABDUL AZIZ ASYHARI 1No ratings yet
- CatheterizationDocument11 pagesCatheterizationSJ MNo ratings yet
- Patho - Digestive SystemDocument17 pagesPatho - Digestive SystemLinda XueNo ratings yet
- Gross Finals LabKaBa 1Document56 pagesGross Finals LabKaBa 1Nadith BalansayNo ratings yet
- GI Review BulletsDocument19 pagesGI Review Bulletsjanet_alexisNo ratings yet
- Bowel EliminationDocument4 pagesBowel Eliminationdlneisha61100% (3)
- Chapter 46 Fecal Elimination EnemaDocument2 pagesChapter 46 Fecal Elimination EnemaPerry BearNo ratings yet
- Catheterization HANDOUTSDocument9 pagesCatheterization HANDOUTSYalc LapidNo ratings yet
- Reviewer Anaphy Lec Digestive System 2nd PartDocument6 pagesReviewer Anaphy Lec Digestive System 2nd PartAubrey Gale MendozaNo ratings yet
- Problem 3 GI Tract Group 13Document159 pagesProblem 3 GI Tract Group 13Alicia TjinNo ratings yet
- Bowel EliminationDocument6 pagesBowel Elimination2022105340No ratings yet
- Digestive System Lecture NotesdocxDocument11 pagesDigestive System Lecture NotesdocxAdaNo ratings yet
- 6 - Body Human SystemDocument19 pages6 - Body Human SystemANDREA PAOLA DIAZ ANDRADENo ratings yet
- Problem 5 Git Aldi FDocument158 pagesProblem 5 Git Aldi Faldi firdausNo ratings yet
- Lower GI System Infants: Caoili, Maria EstrelaDocument21 pagesLower GI System Infants: Caoili, Maria EstrelaanreilegardeNo ratings yet
- Anatomy and Physiology of The GIT NotesDocument20 pagesAnatomy and Physiology of The GIT NotesAndreNo ratings yet
- Gastro NotesDocument11 pagesGastro NotesMonica JubaneNo ratings yet
- Digestive System 1Document11 pagesDigestive System 1Louise Mica LeeNo ratings yet
- Small Intestine 1Document4 pagesSmall Intestine 1Ha Jae kyeongNo ratings yet
- Function Differences Between Small and Large IntestineDocument2 pagesFunction Differences Between Small and Large IntestineKayal KumarNo ratings yet
- L8 - Digestion and Absorption - 6th AugDocument45 pagesL8 - Digestion and Absorption - 6th AugSupritam KunduNo ratings yet
- Clinical Micrsocopy 1.2Document5 pagesClinical Micrsocopy 1.2monzon.mika1801No ratings yet
- Fecal Elimination, Hayam?Document5 pagesFecal Elimination, Hayam?Aryam SNo ratings yet
- GI - HUGE Table No Hilight PDFDocument52 pagesGI - HUGE Table No Hilight PDFAabraNo ratings yet
- Exam 2 NotesDocument36 pagesExam 2 NotesClara PianaltoNo ratings yet
- Stomach: Anatomy, Functions and SecretionsDocument29 pagesStomach: Anatomy, Functions and SecretionsSaad Zafar AwanNo ratings yet
- Problem 5 Git: Ivan MichaelDocument68 pagesProblem 5 Git: Ivan MichaelCunCunAlAndraNo ratings yet
- Can Hold 4l of Food (Maximum)Document4 pagesCan Hold 4l of Food (Maximum)Sofronio OmboyNo ratings yet
- Pemicu 1 Blok GiDocument35 pagesPemicu 1 Blok GiMudita DewiNo ratings yet
- Ncmb316 Prelim (Bai)Document41 pagesNcmb316 Prelim (Bai)kpbalay5921pamNo ratings yet
- Plenary 5B Group 13Document163 pagesPlenary 5B Group 13Obet Agung 天No ratings yet
- PINK Cream and Green Illustrative Science Project PresentationDocument31 pagesPINK Cream and Green Illustrative Science Project Presentationereneovalerozo22No ratings yet
- Animal Physiology: Human NutritionDocument30 pagesAnimal Physiology: Human NutritionHtet Htet NaingNo ratings yet
- Jawaban Tugas Biology Digestive SystemDocument3 pagesJawaban Tugas Biology Digestive Systemaulia nurfadillahNo ratings yet
- (L4) - Digestion and Absorption - 25th MayDocument75 pages(L4) - Digestion and Absorption - 25th MayHarshil PatelNo ratings yet
- 3.4 Process of Absorption and Transportation of Digested Food and DefecationDocument9 pages3.4 Process of Absorption and Transportation of Digested Food and DefecationYu Xuan ChongNo ratings yet
- Anatomi Sistem Digesti.1Document71 pagesAnatomi Sistem Digesti.1Izaz Fishal ShafaNo ratings yet
- THE Disgestive System: by Second GroupDocument17 pagesTHE Disgestive System: by Second GroupAuliya AlfaNo ratings yet
- 6.1 Concepts of UrinaryDocument10 pages6.1 Concepts of UrinaryIvy VillalobosNo ratings yet
- Digestive SystemDocument78 pagesDigestive SystemBerrak AydınNo ratings yet
- Glomerular FiltrationDocument3 pagesGlomerular FiltrationVincent Paul SantosNo ratings yet
- ZOOlogyDocument23 pagesZOOlogyBASI, HEINDRICH LLOYD M.No ratings yet
- III - Digestive SystemDocument3 pagesIII - Digestive SystemGael QuingNo ratings yet
- NCM107 PediatricsDocument11 pagesNCM107 PediatricsKM PanganibanNo ratings yet
- Urogenital System: By:Mariska Fitri Silvia (1710422003) Salsabila Luqyana (1710422023)Document26 pagesUrogenital System: By:Mariska Fitri Silvia (1710422003) Salsabila Luqyana (1710422023)Salsabila LuqyanaNo ratings yet
- Urinary SystemDocument8 pagesUrinary SystemTana OquendoNo ratings yet
- UntitledDocument9 pagesUntitledLeyluhgheylNo ratings yet
- 3.4 Process of Absorption and Transportation of Digested Food and DefecationDocument9 pages3.4 Process of Absorption and Transportation of Digested Food and DefecationFrank ZachNo ratings yet
- Fecal Elimination EnemaDocument5 pagesFecal Elimination EnemaVia Kristel ZapantaNo ratings yet
- 10 L 11, The Large Intestine.Document21 pages10 L 11, The Large Intestine.classicalphantom31No ratings yet
- Lab Act DigestiveDocument8 pagesLab Act DigestiveJhia TorreonNo ratings yet
- Medical School Notes On Physiology of The Colon and Bowel CancerDocument43 pagesMedical School Notes On Physiology of The Colon and Bowel CancerDeji KajiNo ratings yet
- Fecal EliminationDocument4 pagesFecal EliminationEzra MaeNo ratings yet
- Urinary SystemDocument9 pagesUrinary SystemMa Ellen LumauagNo ratings yet
- PLANNINGDocument3 pagesPLANNINGCrazy StrangerNo ratings yet
- ASSESSINGDocument3 pagesASSESSINGCrazy StrangerNo ratings yet
- Margaret Newman and Rosemarie Rizzo-ParseDocument2 pagesMargaret Newman and Rosemarie Rizzo-ParseCrazy StrangerNo ratings yet
- Lydia HallDocument1 pageLydia HallCrazy StrangerNo ratings yet
- Imogen KingDocument1 pageImogen KingCrazy StrangerNo ratings yet
- Dorothy JohnsonDocument2 pagesDorothy JohnsonCrazy StrangerNo ratings yet
- 2) Megaloblastic AnemiaDocument17 pages2) Megaloblastic AnemiaAndrea Aprilia100% (1)
- Fre Orto 3Document4 pagesFre Orto 3PutriNo ratings yet
- Icmr Specimen Referral Form For Covid-19 (Sars-Cov2) : Nic - (Https://Covid19Cc - Nic.In) Page 1/18 27-04-2021 13:49:04Document18 pagesIcmr Specimen Referral Form For Covid-19 (Sars-Cov2) : Nic - (Https://Covid19Cc - Nic.In) Page 1/18 27-04-2021 13:49:04Sumit PatelNo ratings yet
- Clinical Manual - Part 2 - Drug Infusion Guidelines Revised - July 2015 - V7.11Document58 pagesClinical Manual - Part 2 - Drug Infusion Guidelines Revised - July 2015 - V7.11Jayaprakash KuppusamyNo ratings yet
- 1-29-20 Diabetes Protocol Draft With Pandya and Alvarez EditsDocument12 pages1-29-20 Diabetes Protocol Draft With Pandya and Alvarez Editsapi-552486649No ratings yet
- Icd 10Document3 pagesIcd 10ghinaNo ratings yet
- Therapeutic Management of Clinical Mastitis in Goat: A Case StudyDocument5 pagesTherapeutic Management of Clinical Mastitis in Goat: A Case StudyIJAR JOURNALNo ratings yet
- I Jos 201129Document9 pagesI Jos 201129jklhjNo ratings yet
- Filosofi Kesehatan MasyarakatDocument4 pagesFilosofi Kesehatan MasyarakatJennilynn YusameNo ratings yet
- Ace The OSCE2 BookDocument126 pagesAce The OSCE2 BookVijay Mg100% (5)
- Legal Aspects of MedicationDocument17 pagesLegal Aspects of MedicationRitaNo ratings yet
- C-Reactive Protein: TurbilatexDocument1 pageC-Reactive Protein: TurbilatexAssane Senghor100% (1)
- Akapulko: Herbal Medicines Approved by DOHDocument4 pagesAkapulko: Herbal Medicines Approved by DOHYohan NahoNo ratings yet
- Interstitial Lung Diseases Radiology 22222Document26 pagesInterstitial Lung Diseases Radiology 22222Daniel AshooriNo ratings yet
- Diagnostic Challenges and Uncertainties of Embolic Strokes of UndeterminedDocument4 pagesDiagnostic Challenges and Uncertainties of Embolic Strokes of UndeterminedDarliana Ospina DuarteNo ratings yet
- Ptj/pzaa 200Document39 pagesPtj/pzaa 200Yenie YenNo ratings yet
- NRSG1025 Fundamental Healing Arts Lab Manual Learner Prep Workbook - FALL 2023 WINTER 2024Document88 pagesNRSG1025 Fundamental Healing Arts Lab Manual Learner Prep Workbook - FALL 2023 WINTER 2024pham vanNo ratings yet
- Ternian HCIS InteractiveDocument10 pagesTernian HCIS InteractivetrninsgrpNo ratings yet
- Strickland PresentationDocument1 pageStrickland Presentationmariopi2495No ratings yet
- Narrative Report ContentsDocument15 pagesNarrative Report ContentsGladie Ann Dela RosaNo ratings yet
- Shock RosenDocument10 pagesShock RosenJuan GallegoNo ratings yet
- 1000 Multiple Response Questions in Paediatric Dentistry: January 2013Document3 pages1000 Multiple Response Questions in Paediatric Dentistry: January 2013Kiran KumarNo ratings yet
- Abilify Dosing GuideDocument2 pagesAbilify Dosing GuidemtassyNo ratings yet
- Ch-8 Excretion in Animals & PlantsDocument4 pagesCh-8 Excretion in Animals & PlantsRonnith NandyNo ratings yet
- For Health & Wellness: Magnetic Therapy 101Document3 pagesFor Health & Wellness: Magnetic Therapy 101rodonetNo ratings yet
- Paper 1 Bio Skills Practise 2023Document18 pagesPaper 1 Bio Skills Practise 2023nairamathrawala3000No ratings yet
- DM & DI ExamsDocument11 pagesDM & DI ExamsTomzki CornelioNo ratings yet
- Presidential Theme: 66 (LXVI) Annual Conference of Indian Orthopaedic AssociationDocument17 pagesPresidential Theme: 66 (LXVI) Annual Conference of Indian Orthopaedic AssociationnipundaveNo ratings yet
- A Leading Surgical Gastroenterologist in Hyderabad Dr. Dinesh ReddyDocument4 pagesA Leading Surgical Gastroenterologist in Hyderabad Dr. Dinesh Reddydrdineshreddy02No ratings yet
- User Manual Buble Cpap PDFDocument7 pagesUser Manual Buble Cpap PDFmamahosieleNo ratings yet
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (24)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 5 out of 5 stars5/5 (80)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeNo ratings yet
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (5)
- Why We Die: The New Science of Aging and the Quest for ImmortalityFrom EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityRating: 4 out of 5 stars4/5 (3)
- Sleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningFrom EverandSleep Stories for Adults: Overcome Insomnia and Find a Peaceful AwakeningRating: 4 out of 5 stars4/5 (3)
- Gut: the new and revised Sunday Times bestsellerFrom EverandGut: the new and revised Sunday Times bestsellerRating: 4 out of 5 stars4/5 (392)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 3.5 out of 5 stars3.5/5 (3)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (1)
- When the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisFrom EverandWhen the Body Says No by Gabor Maté: Key Takeaways, Summary & AnalysisRating: 3.5 out of 5 stars3.5/5 (2)
- An Autobiography of Trauma: A Healing JourneyFrom EverandAn Autobiography of Trauma: A Healing JourneyRating: 5 out of 5 stars5/5 (2)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (169)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessFrom EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessRating: 4.5 out of 5 stars4.5/5 (328)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisFrom EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (1)
- Summary: The Myth of Normal: Trauma, Illness, and Healing in a Toxic Culture By Gabor Maté MD & Daniel Maté: Key Takeaways, Summary & AnalysisFrom EverandSummary: The Myth of Normal: Trauma, Illness, and Healing in a Toxic Culture By Gabor Maté MD & Daniel Maté: Key Takeaways, Summary & AnalysisRating: 4 out of 5 stars4/5 (9)
- 12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosFrom Everand12 Rules for Life by Jordan B. Peterson - Book Summary: An Antidote to ChaosRating: 4.5 out of 5 stars4.5/5 (207)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (44)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (253)