Professional Documents
Culture Documents
Ulcerative Colitis (Uc)
Uploaded by
zulaikhaa.bbOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Ulcerative Colitis (Uc)
Uploaded by
zulaikhaa.bbCopyright:
Available Formats
ULCERATIVE COLITIS (UC)
What is UC
Chronic, relapsing-remitting, inflammatory disease of the GI tract - rectum
and colon
Non-infectious - not causes by pathogens so does not spread
Continuous - will affect a part of the colon continously (not one part, then
miss and then another part)
Has a range of extra-intestinal manifestations
NEVER spreads into small intestines or anus
What is the epidemiology of UC
Most common form of IBD
Bimodal distribution - highest incidence is in 15-25 and 55-65 age groups
What is the aetiology of UC
Polygenic predisposition (more than one gene causes it)
Environmental factors
Immune dysfunction
Inflammation extends from rectum proximally to affect a variable length of
continuous colon
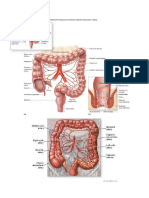
What part of the anatomy does UC affect
Affects the large bowel - mainly colon and rectum
Large bowel - caecum, colon, rectum and anal canal
Colon - ascending colon, transverse colon, descending colon, sigmoid colon
Ileocaecal valve - between the ilium and the colon
Below the ileocaecal valve is the caecum
Above the ileocaecal valve is the colon
In UC, the inflammation starts at the rectum and never spreads beyond the
ileocaecal valce
ULCERATIVE COLITIS (UC) 1
Can affect just the rectum (ulcerative proctitis), the left-side of the colon (left-
sided colitis) or the whole colon (pancolitis)
Ulcerative proctitis is more common - only within rectum
Left-sided colitis - inflammation involves rectum and doesnt extend beyond
splenic flexure
Pancolitis - inflammation extends from rectum to ileocaecal valve
What is the pathophysiology of UC
Microscopically
Acute and chronic inflammatory cells invade lamina propria
Affects just the inner layer of mucosa
Crypt branching
Villous atrophy
Neutrophils migrate through walls of glands to form crypt abscesses
No granulomas present
Depletion of goblet cells and mucin from gland epithelium
No inflammation beyond submucosa
Widerspread ulceration with perservation of adjacent mucosa - appearance
of polyps (pseudopolyps)
What are pseudopolyps
Masses of scar tissue - develop from granulation tissue during the healing
phase in repeated cycle of ulceration
Project out of wall
Marker of episodes of severe infection
What are the risk factors of UC
Family history - 1 degree relatives of someone with UC have a higher
chance of developing UC compared to those without a UC relative
Oral contraceptives - association between use of oral contraceptives and
development of IBD
Not smoking - risk of UC is less in smokers
ULCERATIVE COLITIS (UC) 2
What are the intestinal symptoms of UC
Diarrhoea - can contain mucus and blood
Left iliac fossa/ LUQ pain
Pale - anaemia due to blood in stool
Urgency
Tenesmus - feeling that you need to pass stools even though bowels are
empty, can involve straining, pain, cramping
Systemic symptoms - malaise, fever, weight loss
What are the extra-intestinal symptoms of UC (that are related to disease
activity)
Dermatological manifestations - erythema nodosum
Occular manifestations - episcleritis
MSK manifestations - osteoporosis, arthritis (that is pauciarticular (affects
only a few joints), non-deforming, assymetrical)
Aphthous ulcers
What are the extra-intestinal symptoms of UC (that are not related to disease
activity)
Dermatological manifestations - pyoderma gangrenosum
Occular manifestations - anterior uveitis, conjuctivitis
MSK manifestations - clubbing, sacroilitis
Hepatobiliary manifestations - primary sclerosing cholangitis (PSC - more
common in UC compared to CD and more common in males)
Ankylosing spondylitis
AA amyloidosis - secondary to chronic inflammation, rare and serious
What are the clinical signs of UC
Distension of adbomen on palpitation
Tenderness of adbomen on palpitation
PR exam - tenderness, blood, mucus
How is the severity of UC assessed
ULCERATIVE COLITIS (UC) 3
Truelove and Witts’ Severity Index
FAB CHEF - what the severity index focuses on (acronym has no order, just
to remember the different components of the severity index)
Frequency of stools in a day
Anaemia
Blood in stool - how much
CRP
HR
ESR
Fever
Mild - under 4 stools a day, small amounts of blood stool, no anaemia or
fever, HR below 90, normal ESR/CRP
Moderate - 4-6 stools a day, blood in stool (more than in mild), no anaemia
or fever, HR below 90, normal ESR/CRP
Severe - over 6 stools a day, visible blood in stool/alot of blood, one feature
of systemic involvement (fever, HR above 90, ESR above 30, CRP can be
raised sometimes)
What investigations are done for UC
Bloods
Stools
Imaging such as AXR, erect CXR
Barium enema - loss of haustrations, superficial ulceration, pseudopolyps,
lead pipe/ drain pipe colon (colon is narrow and short)
Rigid/flexible sigmoidoscopy - with biopsy, can check for toxic megacolon
Colonoscopy with multiple biopsies - first line to diagnose colitis
Which bloods are done for UC
FBC - leukocytosis in flare up
ESR/CRP - can increase in active disease
U&E’s
ULCERATIVE COLITIS (UC) 4
LFT’s - check 6-12 months to screen for PSC
Which stool tests are done for UC
Culture and microscopy
Faecal calprotein
A small calcium binding protein
Raised in IBD
Concentration of calprotein in faeces can correlate with severity of
disease
Helps to differentiate from IBS
Which imaging is done for UC
AXR - can assess extent of colonic involvement in acute severe colitis, can
show lack of faecal shadows, mucosal thickening or toxic megacolon
Erect CXR - rule out perforation in acute severe colitis
What can be found on a colonscopy with biopsy
Red and raw mucosa
No inflammation beyond submucosa
Pseudopolyps may be seen
Crypt abscesses (occur due to neutrophil migration)
What is the general rules for managing UC
Management will depend on severity and location of UC
If UC is mild to moderate - oral steroids
If UC is acute and severe - first line is IV steroids, second line is IV
Cyclosporin
What is the management for UC when inducing remission
Topical rectal aminosalicylayes or rectal steroids
For distal colitis - rectal Mesalazine works better than rectal steroids and oral
aminosalicylates
Oral aminosalicylates
ULCERATIVE COLITIS (UC) 5
Second line for those who don’t reespond to aminosalicylates - oral
Prednisolone
Severe colitis - IV steroids
Infliximab - moderate to severe UC, when disease is resistant to
conventional treatment that uses corticosteroids and immunosuppressive
agents
What is the management for UC to maintain remission
Oral aminosalicylates such as Mesalazine
Azathioprine and Mercaptopurine
Probiotics may help to prevent relapse in those with mild-moderate disease
What surgical treatment is available for UC
Surgery is curative of UC
Colectomy
Indications for surgical intervention - patients who fail to respond/intolerant of
treatment, if complications occur such as colorectal cancer
What are the complications of UC
Psychological effects
Toxic megacolon
Colorectal cancer such as colonic adenocarcinoma
VTE - venous thromboembolism (VTE includes both DVT and PE)
Perforation
Strictures and obstructions - bowel loops can develop strictures following
chronic inflammation, strictures can lead to obstruction
Some forms of extra-intestinal manifestations such as AA amyloidosis,
osteoporosis (due to steroid use)
What is toxic megacolon
Acute form of colonic distension
Can become septic and perforate
Requires supportive care, bowel rest, NG decompression and antibiotics
ULCERATIVE COLITIS (UC) 6
Needs colectomy if no improvement within 24-48 hours
ULCERATIVE COLITIS (UC) 7
You might also like
- Acute Abdominal Pain 2Document72 pagesAcute Abdominal Pain 2ngockhanh1971No ratings yet
- Ulcerative ColitisDocument21 pagesUlcerative ColitisShofiyyah SaniNo ratings yet
- Set 3 COMP-2Document71 pagesSet 3 COMP-2Appu ayyalaNo ratings yet
- Ulcerative ColitisDocument21 pagesUlcerative Colitismel_chakNo ratings yet
- Ashley Esdaile MSIII Byron Baptist MSIII Mike Pothen MS IIIDocument77 pagesAshley Esdaile MSIII Byron Baptist MSIII Mike Pothen MS IIISutapa PawarNo ratings yet
- 01 14 2021 GERD Inflammatory Bowel Disease Irritable Bowel Syndrome ALLENDocument66 pages01 14 2021 GERD Inflammatory Bowel Disease Irritable Bowel Syndrome ALLENMikey ZhitnitskyNo ratings yet
- DDocument56 pagesDDarren Balbas100% (1)
- Emergencies in Pediatric SurgeryDocument61 pagesEmergencies in Pediatric Surgeryapi-198361160% (1)
- NCM 103 Metab N EndocrineDocument148 pagesNCM 103 Metab N EndocrinernrmmanphdNo ratings yet
- Colon, Rectum and AnusDocument30 pagesColon, Rectum and AnusKiara GovenderNo ratings yet
- DDX of RIF Mass (Syazwani)Document44 pagesDDX of RIF Mass (Syazwani)Nurul Syazwani RamliNo ratings yet
- Exams MedsurgDocument29 pagesExams MedsurgUy Jezrielle MicahNo ratings yet
- 14 - Barium Studies For GIT With NotesDocument50 pages14 - Barium Studies For GIT With NotesSunil ThomasNo ratings yet
- By Col - Abrar Hussain ZaidiDocument47 pagesBy Col - Abrar Hussain ZaidiSilvanaPutriNo ratings yet
- General Surgery A Revision Session For FinalsDocument69 pagesGeneral Surgery A Revision Session For Finalsimperiallight100% (2)
- Inflammatory Bowel DiseaseDocument59 pagesInflammatory Bowel DiseaseLala Rahma Qodriyan SofiakmiNo ratings yet
- Nbme 16Document31 pagesNbme 16apple seedNo ratings yet
- Acute Abdominal PainDocument72 pagesAcute Abdominal PainJoseph Stans Kasirye100% (1)
- Neonatal Acute Abdomen. 7th YrDocument54 pagesNeonatal Acute Abdomen. 7th YrFreeburn SimunchembuNo ratings yet
- M Digestion" Absorption" EliminationDocument104 pagesM Digestion" Absorption" EliminationChristine Carol FilipinasNo ratings yet
- Crohns DiseaseDocument32 pagesCrohns DiseaseMin Chi PakNo ratings yet
- Dr. Kessler'S Homeopathy Book: Polycrests and Other Remedies Index of DiseasesDocument375 pagesDr. Kessler'S Homeopathy Book: Polycrests and Other Remedies Index of DiseasesVishalNo ratings yet
- Inflammatory Bowel Disease FinalDocument60 pagesInflammatory Bowel Disease FinalRawabi rawabi1997No ratings yet
- Gi Long CaseDocument8 pagesGi Long CaseNadia SalwaniNo ratings yet
- UlcerativecolitisDocument27 pagesUlcerativecolitisMohamed Abdulrazaq100% (1)
- Fast Facts: Enfermedad inflamatoria intestinal Para Pacientes y las Personas que los Apoyan: Colitis ulcerativa y enfermedad de Crohn Información + Tomar el control = El mejor resultadoFrom EverandFast Facts: Enfermedad inflamatoria intestinal Para Pacientes y las Personas que los Apoyan: Colitis ulcerativa y enfermedad de Crohn Información + Tomar el control = El mejor resultadoNo ratings yet
- Ibd AnushaDocument32 pagesIbd AnushaRupesh R100% (1)
- Inflammatory Bowel Disease (Ibd)Document28 pagesInflammatory Bowel Disease (Ibd)suhaNo ratings yet
- Ulcerativecolitis 170323180448 PDFDocument88 pagesUlcerativecolitis 170323180448 PDFBasudewo Agung100% (1)
- Lecture 2-Part 1Document90 pagesLecture 2-Part 1mashe1No ratings yet
- Crohn ' S Disease (Regional EnteritisDocument26 pagesCrohn ' S Disease (Regional EnteritisRasti AmediNo ratings yet
- IBD - Shane Ryan ApperleyDocument63 pagesIBD - Shane Ryan Apperleyvivi avisaNo ratings yet
- Ulcerative Colitis: DR Syed Ubaid Associate Professor of SurgeryDocument71 pagesUlcerative Colitis: DR Syed Ubaid Associate Professor of SurgeryFachry Al RafiqiNo ratings yet
- Ulcerative ColitisDocument88 pagesUlcerative ColitisYulia DjatiwardaniNo ratings yet
- Askep IbdDocument43 pagesAskep IbdYou100% (1)
- Acute Appendicitis Pathophysiology: MycobacteriaDocument10 pagesAcute Appendicitis Pathophysiology: MycobacteriaUzma KhanNo ratings yet
- Eric Ji-Yuan Mao, MD Samir A. Shah, MD, Facg, Fasge, AgafDocument18 pagesEric Ji-Yuan Mao, MD Samir A. Shah, MD, Facg, Fasge, AgafMuhammad GassanNo ratings yet
- CD8 2021 InflammatoryDocument191 pagesCD8 2021 InflammatoryNhelia Santos BañagaNo ratings yet
- Appendicitis 5.9Document50 pagesAppendicitis 5.9Smart SaravanaNo ratings yet
- 28 - IbdDocument57 pages28 - IbdsitiNo ratings yet
- Ulcerative Colitis: PseudopolypsDocument26 pagesUlcerative Colitis: PseudopolypsSocorro S. Gantalao-CorbedaNo ratings yet
- Clinical Feature and Diagnosis of IbdDocument56 pagesClinical Feature and Diagnosis of IbdVicks Vikash KumarNo ratings yet
- Exemplar - Inflammatory Bowel DiseaseDocument1 pageExemplar - Inflammatory Bowel DiseaseMary GiuntiniNo ratings yet
- IBD Obat Ganguan Saluran CernaDocument13 pagesIBD Obat Ganguan Saluran CernaKhumairah mohtarNo ratings yet
- Git TutorialDocument7 pagesGit Tutorialmiss latteNo ratings yet
- Inflammatoray Bowel DiseaseDocument14 pagesInflammatoray Bowel DiseaseSadr AkrmNo ratings yet
- 03 150427073915 Conversion Gate01Document52 pages03 150427073915 Conversion Gate01maithamNo ratings yet
- Gastro NotesDocument18 pagesGastro NoteslukeNo ratings yet
- Leukemia Cells & ColorectalDocument40 pagesLeukemia Cells & ColorectalYum CNo ratings yet
- Powerpoint: Chronic Inflammatory DisordesDocument55 pagesPowerpoint: Chronic Inflammatory Disordesj.doe.hex_87No ratings yet
- AppendicitiesDocument58 pagesAppendicitiesGAURAV50% (2)
- Appendicitis: San Roque Extension, Roxas City, Capiz 5800Document10 pagesAppendicitis: San Roque Extension, Roxas City, Capiz 5800GUEZIL JOY DELFINNo ratings yet
- DefinitionDocument12 pagesDefinitionAylol 23No ratings yet
- GIS-K-25 Acute Appendicitis Appendiceal Mass / AbscessDocument24 pagesGIS-K-25 Acute Appendicitis Appendiceal Mass / AbscessYasmine Fitrina SiregarNo ratings yet
- Yosephine Case 5aDocument31 pagesYosephine Case 5aRanto B. TampubolonNo ratings yet
- NCM-Ulcerative Colitis ReportDocument22 pagesNCM-Ulcerative Colitis ReportJocelyn RiveraNo ratings yet
- Inflammatory Bowel DiseaseDocument19 pagesInflammatory Bowel Diseasenathan asfahaNo ratings yet
- Inflammatory Bowel DiseaseDocument52 pagesInflammatory Bowel DiseaseWilliams Emmanuel AdeyeyeNo ratings yet
- Ulcerative ColitisDocument9 pagesUlcerative ColitisMike GNo ratings yet
- Inflammatory Bowel Disease: By: Yilak G. Augst 2015Document44 pagesInflammatory Bowel Disease: By: Yilak G. Augst 2015TESFAYE YIRSAWNo ratings yet
- Abdominal Pain MARS 2.0 - Dr. Siswidiyati, SP - RadDocument34 pagesAbdominal Pain MARS 2.0 - Dr. Siswidiyati, SP - RadarifdeathsciethNo ratings yet
- I. Understanding The Disease and PathophysiologyDocument14 pagesI. Understanding The Disease and PathophysiologyKipchirchir AbednegoNo ratings yet
- Ulcerative Colitis SeminarDocument15 pagesUlcerative Colitis Seminar23mby004No ratings yet
- Inflammatory Bowel Disease (IBD)Document41 pagesInflammatory Bowel Disease (IBD)ririNo ratings yet
- Pancreaticobiliary Lesions: DR Rofanda BakeerDocument29 pagesPancreaticobiliary Lesions: DR Rofanda BakeerKareem DawoodNo ratings yet
- IBD Final11Document41 pagesIBD Final11abraham debebeNo ratings yet
- Acute Appendicitis by DR.S.HDocument24 pagesAcute Appendicitis by DR.S.Hkevinharahap26No ratings yet
- Disease Rectum. - Inflammatory Disease Colon Intestine (Nonspecific Ulcerative Colitis, Crohn's Disease) - Colon Cancer IntestineDocument22 pagesDisease Rectum. - Inflammatory Disease Colon Intestine (Nonspecific Ulcerative Colitis, Crohn's Disease) - Colon Cancer IntestineTojan Faisal AlzoubiNo ratings yet
- Presented by Dr. Ayalew ZDocument35 pagesPresented by Dr. Ayalew Zyared getachewNo ratings yet
- Curcumin Alleviates Experimental Colitis Via A Potential Mechanism Involving Memory B Cells and Bcl-6-Syk-BLNK SignalingDocument20 pagesCurcumin Alleviates Experimental Colitis Via A Potential Mechanism Involving Memory B Cells and Bcl-6-Syk-BLNK SignalingRohaniNo ratings yet
- IBDDocument31 pagesIBDEdwardArielTadeaNo ratings yet
- Bhagatwala Et Al 2015, Indications and ContraindicationsDocument27 pagesBhagatwala Et Al 2015, Indications and Contraindicationsedo adimastaNo ratings yet
- NCM Digestive 2 PDFDocument11 pagesNCM Digestive 2 PDFsamantha lumapasNo ratings yet
- Case Study 1 - Ulcerative ColitisDocument17 pagesCase Study 1 - Ulcerative ColitisJossua RyanNo ratings yet
- IBD - Shane Ryan ApperleyDocument63 pagesIBD - Shane Ryan Apperleyvivi avisaNo ratings yet
- Ulcerative ColitisDocument7 pagesUlcerative ColitisShaira Anne Fuentes BaroniaNo ratings yet
- Crohn's Disease: ClassificationDocument15 pagesCrohn's Disease: ClassificationAlleson John A. BayganNo ratings yet
- Gi Disorders in PregnancyDocument43 pagesGi Disorders in PregnancyDiana MurguiaNo ratings yet
- HEMATOCHEZIADocument26 pagesHEMATOCHEZIAAlvin HartantoNo ratings yet
- Consenso Brasileiro Doença Inflamatória IntestinalDocument32 pagesConsenso Brasileiro Doença Inflamatória IntestinalCarla MartinsNo ratings yet
- Coloi Eeml Disease: Original ArticlesDocument67 pagesColoi Eeml Disease: Original ArticlesLuisAngelPonceTorresNo ratings yet
- Colorectal Cancer - Epidemiology, Risk Factors, and Protective Factors - UpToDateDocument38 pagesColorectal Cancer - Epidemiology, Risk Factors, and Protective Factors - UpToDateYdeli DetanNo ratings yet
- Surgery Surgical Nursing Objs With AnsDocument136 pagesSurgery Surgical Nursing Objs With AnsmintahmeshackbenjaminNo ratings yet
- Overview of Colon Polyps - UpToDateDocument44 pagesOverview of Colon Polyps - UpToDateHartemes RosarioNo ratings yet
- Infliximab: Drug Treatment InformationDocument7 pagesInfliximab: Drug Treatment InformationAlin-Ionuț SălcianuNo ratings yet
- Case Study2Document11 pagesCase Study2Jainet Aira S. AmanteNo ratings yet
- Colostomy Care: A Guide For Home Care CliniciansDocument11 pagesColostomy Care: A Guide For Home Care Cliniciansdika franNo ratings yet
- ThesisDocument75 pagesThesisleartaNo ratings yet
- EMRAP 2022 07 July Vol.22Document18 pagesEMRAP 2022 07 July Vol.22suNo ratings yet
- Probiotics in GI DisordersDocument35 pagesProbiotics in GI Disordersmango91286No ratings yet