Professional Documents
Culture Documents
Hypertensive Emergencies Guidelines and Best Practice Recommendations
Hypertensive Emergencies Guidelines and Best Practice Recommendations
Uploaded by
Frida HinojosCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Hypertensive Emergencies Guidelines and Best Practice Recommendations
Hypertensive Emergencies Guidelines and Best Practice Recommendations
Uploaded by
Frida HinojosCopyright:
Available Formats
JUNE 2023 | VOLUME 25 | ISSUE 6
Emergency Medicine Practice Evidence-Based Education • Practical Application
CLINICAL CHALLENGES:
• What defines hypertensive
emergency?
• What are the most common and
dangerous end-organ dysfunctions
to watch for?
• How do the different society
guidelines define and treat
hypertensive emergencies?
Authors
Ari B. Davis, DO
Department of Emergency Medicine, Einstein
Medical Center, Philadelphia, PA
Kyle Hughes, MD
Department of Emergency Medicine, Einstein
Medical Center, Philadelphia, PA
Jonathan Pun, MD
Department of Emergency Medicine, Einstein
Medical Center, Philadelphia, PA
Scott Goldstein, DO, FACEP,
Hypertensive Emergencies:
FAEMS, EMT-PHP
Director, Division of EMS/Disaster Medicine,
Guidelines and Best-Practice
Einstein Healthcare Network, Philadelphia, PA Recommendations
Peer Reviewers n Abstract
Due to a variety of demographic and public health factors, the
Aman Pandey, MD
Assistant Professor, Emergency Medicine, number of emergency department visits related to hypertensive
University of Florida Health Jacksonville, emergencies has increased dramatically in recent decades,
Jacksonville, FL making it imperative that clinicians clearly understand the
Christopher R. Tainter, MD, RDMS, current treatment guidelines and definitions for the spectrum
FACEP, FCCM of hypertensive disease. This issue reviews current evidence on
Clinical Professor, Department of identifying and managing hypertensive emergencies and the
Anesthesiology, Division of Critical Care, differences between expert opinions on diagnosing and managing
University of California San Diego, San Diego, these emergencies. Clear protocols differentiating patients with
CA
hypertension from patients with hypertensive emergencies are
needed to appropriately manage this patient population.
Prior to beginning this activity, see “CME
Information” on page 2.
For online For mobile
access: app access:
This issue is eligible for CME credit. See page 2. EBMEDICINE.NET
CME Information
Date of Original Release: June 1, 2023. Date of most recent review: May 10, 2023. Termination date: June 1, 2026.
Accreditation: EB Medicine is accredited by the Accreditation Council for Continuing Medical Education (ACCME) to provide
continuing medical education for physicians.
Credit Designation: EB Medicine designates this enduring material for a maximum of 4 AMA PRA Category 1 CreditsTM. Physi-
cians should claim only the credit commensurate with the extent of their participation in the activity.
Specialty CME: Included as part of the 4 credits, this CME activity is eligible for 2 Pharmacology CME credits, subject to your state and institu-
tional approval. For more information, contact Customer Service at 678-366-7933.
ACEP Accreditation: Emergency Medicine Practice is approved by the American College of Emergency Physicians for 48 hours of ACEP Cat-
egory I credit per annual subscription.
AAFP Accreditation: The AAFP has reviewed Emergency Medicine Practice, and deemed it acceptable for AAFP credit. Term of approval is from
07/01/2022 to 06/30/2023. Physicians should claim only the credit commensurate with the extent of their participation in the activity. This session,
Hypertensive Emergencies: Guidelines and Best-Practice Recommendations, is approved for 4.0 enduring material AAFP Prescribed credits.
AOA Accreditation: Emergency Medicine Practice is eligible for 4 Category 2-A or 2-B credit hours per issue by the American Osteopathic Association.
Needs Assessment: The need for this educational activity was determined by a practice gap analysis; a survey of medical staff, including the
editorial board of this publication; review of morbidity and mortality data from the CDC, AHA, NCHS, and ACEP; and evaluation responses from
prior educational activities for emergency physicians.
Target Audience: This enduring material is designed for emergency medicine physicians, physician assistants, nurse practitioners, and residents.
Goals: Upon completion of this activity, you should be able to: (1) identify areas in practice that require modification to be consistent with current
evidence in order to improve competence and performance; (2) develop strategies to accurately diagnose and treat both common and critical ED
presentations; and (3) demonstrate informed medical decision-making based on the strongest clinical evidence.
CME Objectives: Upon completion of this activity, you should be able to: (1) define hypertensive emergency, including its clinical presentations,
diagnostic criteria, and potential complications; (2) explain the epidemiology and pathophysiology of hypertensive emergency, including risk
factors and underlying mechanisms; (3) discuss the current evidence-based approaches to the management of hypertensive emergency; and (4)
describe the different multidisciplinary society guidelines and how to use them.
Discussion of Investigational Information: As part of the activity, faculty may be presenting investigational information about pharmaceutical
products that is outside Food and Drug Administration approved labeling. Information presented as part of this activity is intended solely as
continuing medical education and is not intended to promote off-label use of any pharmaceutical product.
Disclosure: It is the policy of EB Medicine to ensure objectivity, balance, independence, transparency, and scientific rigor in all CME activities.
All individuals in a position to control content have disclosed all financial relationships with ACCME-defined ineligible companies. EB Medicine
has assessed all relationships with ineligible companies disclosed, identified those financial relationships deemed relevant, and appropriately
mitigated all relevant financial relationships based on each individual’s role(s). Please find disclosure information for this activity below:
Planners Faculty
• Daniel J. Egan, MD (Course Director): Nothing to Disclose • Ari B. Davis, DO (Author): Nothing to Disclose
• Andy Jagoda, MD (Editor-in-Chief): • Kyle Hughes, MD (Author): Nothing to Disclose
l Pfizer (Consultant/Advisor) • Jonathan Pun, MD (Author): Nothing to Disclose
l Janssen (Consultant/Advisor) • Scott Goldstein, DO (Author): Nothing to Disclose
l Abbott Laboratories (Consultant/Advisor) • Aman Pandey, MD (Peer Reviewer): Nothing to Disclose
• Kaushal Shah, MD (Associate Editor-in-Chief): Nothing to Disclose • Christopher R. Tainter, MD (Peer Reviewer): Nothing to Disclose
• Aimee Mishler, PharmD (Pharmacology Editor): Nothing to Disclose
• Joseph D. Toscano, MD (Research Editor): Nothing to Disclose
• Dorothy Whisenhunt, MS (Content Editor): Nothing to Disclose
• Cheryl Belton, PhD (Content Editor): Nothing to Disclose
Commercial Support: This issue of Emergency Medicine Practice did not receive any commercial support.
Earning CME Credit: Go online to https://www.ebmedicine.net/CME and click on the title of the test you wish to take. When completed, a CME
certificate will be emailed to you.
Additional Policies: For additional policies, including our statement of conflict of interest, source of funding, statement of informed consent, and
statement of human and animal rights, visit https://www.ebmedicine.net/policies
CEO: Stephanie Williford
Director of Finance & Analytics: Robin Wilkinson
Publisher: Suzanne Verity
Director of Editorial Quality: Dorothy Whisenhunt, MS
Content Editor: Cheryl Belton, PhD, ELS
Direct all inquiries to: Managing Editor: Angie Wallace
Phone: 678-366-7933 CME Coordinator: Kristen Raynor, MEd
Fax: 770-500-1316 Education Coordinator: Kandis Slater
5600 Spalding Drive, Unit 921697 Customer Service Representative: Katie Resumovic
Norcross, GA 30010-1697 Account Executive: Dana Stenzel
Director of Marketing: Anna Motuz, MBA
E-mail: ebm@ebmedicine.net Email Marketing Specialist: Joshua Devou, MBA
Website: www.ebmedicine.net Marketing Specialist: Valerie Yuhouse
Database Administrator: Jose Porras
ISSN info and disclaimer:
Emergency Medicine Practice (ISSN Print: 1524-1971, ISSN Online: 1559-3908, ACID-FREE) is published monthly (12 times per year) by EB Medicine
(5600 Spalding Drive, Unit 921697, Norcross, GA 30010-1697). Opinions expressed are not necessarily those of this publication. Mention of products
or services does not constitute endorsement. This publication is intended as a general guide and is intended to supplement, rather than substitute,
professional judgment. It covers a highly technical and complex subject and should not be used for making specific medical decisions. The materials
contained herein are not intended to establish policy, procedure, or standard of care. Copyright © 2023 EB Medicine. All rights reserved. No part of
this publication may be reproduced in any format without written consent of EB Medicine. This publication is intended for the use of the individual
subscriber only and may not be copied in whole or part or redistributed in any way without the publisher’s prior written permission.
JUNE 2023 • www.ebmedicine.net 2 ©2023 EB MEDICINE
Case Presentations
A 62-year-old man presents via EMS with swelling of his legs that makes it hard for him to walk...
• EMS states he wasn’t able to walk because of his lower extremity swelling. Vital signs en route are:
temperature, 37°C; heart rate, 90 beats/min; blood pressure, 193/118 mm Hg; respiratory rate, 20
breaths/min; and oxygen saturation, 94% on room air.
• The patient reports his medication was across the room, and he wasn’t able to reach it due to his inabil-
ity to walk from his leg swelling. He states he has a history of congestive heart failure with a left ventric-
CASE 1
ular ejection fraction of 25%. He pulls out from his jacket a copy of his latest echocardiogram report.
• On physical examination, you notice he has bilateral lower extremity pitting edema and that he is
becoming increasingly more tachypneic. On pulmonary examination, you hear fine crackles bilaterally
and diffusely. You notice his oxygen saturation is dropping on the monitor, despite just having put him
on 2 L of oxygen via nasal cannula. As you continue to talk to him, his oxygen requirements increase to
non-rebreather mask.
• You wonder what type of hypertensive emergency this is, and what treatment must be implemented
immediately?
A 76-year-old man presents to the ED with his family, who are concerned he might have dementia…
• The family informs you that he is normally a sweet old man, but recently he has been having episodes
of confusion and agitation. Yesterday, the police found him walking along the highway in his bathrobe.
• His family tells you he has a history of diabetes and hypertension. They don’t know if he has been
CASE 2
taking his medications regularly or what his medications are.
• His temperature is 37°C; blood pressure, 236/113 mm Hg; heart rate, 62 beats/min; respiratory rate, 14
breaths/min; and oxygen saturation, 96% on room air. His blood glucose level is 185 mg/dL.
• On examination, he is alert and oriented to name only. He complains of a “headache all over,” seeing
strange flashing lights, and is annoyed by your continued questioning. As you continue, he no longer
participates in the physical examination and begins to have jerking movements.
• Which medication(s) should you use to treat him?
A 59-year-old woman presents to the ED after being seen at her primary care physician’s office…
• Her doctor was concerned because her blood pressure was 206/120 mm Hg. Her blood pressure
normally runs high, but they had never seen it this high.
CASE 3
• The patient states that she feels fine. She denies any vision changes, headache, chest pain, or shortness
of breath. Her past medical history is relevant for hypertension and pre-diabetes. She states that she
did not take her blood pressure medications this morning, since her primary care doctor‘s office told
her to not eat or drink anything prior to getting her laboratory work today.
• You wonder whether anything needs to be done in the ED about her blood pressure…
n Introduction Several definitions have been used to classify
Hypertensive emergency is a clinical syndrome of severe hypertension and hypertensive emergencies.
significantly elevated blood pressure (BP) associated The terms hypertensive urgency, hypertensive crisis,
with rapidly progressive end-organ damage. While and malignant hypertension are historically defined as
survival from hypertensive emergency has improved severely elevated BP without evidence of end-organ
considerably in recent years, it is still associated with damage. With some variability from study to study,
significant morbidity and mortality, as case-controlled severe hypertension is usually defined as systolic
studies have reported an all-cause mortality of 10% at BP (SBP) ≥180 mm Hg or a diastolic BP (DBP) ≥110
5 years, with 20% of patients requiring kidney trans- mm Hg. The key distinction of severe hypertension
plantation.1 To identify patients who need intensive from a hypertensive emergency is the lack of rapidly
treatment and to avoid harm in those who do not, evolving end-organ damage in severe hypertension.
a thorough history, physical examination, and clini- Differentiating this collection of terms is the first step
cal assessment are required. Unfortunately, unclear in the safe management of hypertensive patients. For
terminology for describing these patients clinically is this review, a BP of ≥180/110 mm Hg and a mean
often a source of confusion and can present a barrier arterial pressure (MAP) of ≥135 mm Hg will be used
to appropriate recognition and management. to define severe hypertension. The designation of
JUNE 2023 • www.ebmedicine.net 3 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
severe hypertension may be helpful to alert clinicians clinical trials to direct optimal BP management, and
to assess for the presence of end-organ damage, but therefore recommendations can differ widely between
it will not constitute a hypertensive emergency. This guidelines. For example, the AHA/American College
issue of Emergency Medicine Practice will discuss the of Cardiology (ACC) non-ST-elevation myocardial
best available evidence for identification and man- infarction (NSTEMI) guidelines recommend intrave-
agement of hypertensive emergencies. nous (IV) nitroglycerin for patients who are hyperten-
sive, with a B level of evidence,7 while the European
Society of Cardiology (ESC) guidelines specifically
n Critical Appraisal of the Literature state that there is no indication for nitrate treatment
A literature review was conducted in the Cochrane in patients with an NSTEMI, beyond symptomatic
Database of Systematic Reviews, the Cochrane Central treatment.8 Similarly, the AHA/ACC published guide-
Register of Controlled Trials, and PubMed for articles lines for hypertension management in ACS with a
published between 2000 and 2023 using the terms recommended target BP <140/90 mm Hg (class of
hypertensive crisis, hypertensive emergency, malignant recommendation 2a, level of evidence C),9 while ESC
hypertension, and hypertensive emergencies. Specific guidelines mention no specific target for BP manage-
hypertensive emergency terms acute ischemic stroke, ment, stating that nitrates, angiotensin-converting en-
aortic dissection, and acute heart failure were also zyme (ACE) inhibitors, angiotensin II receptor block-
searched. 5180 articles were screened, and of those, ers (ARBs), and beta blockers can be used during the
122 articles were included for discussion and evaluation. acute phase of BP management.10
Of the articles included, there were few well- With limited well-designed prospective studies
designed randomized controlled trials (RCTs) evalu- and conflicting recommendations between guide-
ating optimal BP management during hypertensive lines, the ESC and AHA/ACC both published broad
emergencies. Among all hypertensive emergencies, guidelines on how to manage all hypertensive emer-
the strongest evidence to guide optimal BP manage- gencies. Table 1 lists the ESC-recommended MAP or
ment is from patients with intracranial hemorrhage SBP reductions for each hypertensive emergency.12
(ICH). The American Heart Association (AHA)/Ameri- The AHA/ACC simplify hypertensive emergency
can Stroke Association (ASA)2 and European Stroke management to reducing BP by a maximum of 25%
Organisation (ESO)3 guidelines reference the ATACH4 in the first hour and then to 160/100-110 mm Hg over
and INTERACT trials5,6 as high-quality randomized the next 2 to 6 hours for all hypertensive emergencies
trials that give clinicians strong evidence for a specific except aortic dissections, pre-eclampsia/eclampsia,
BP target, making treatment recommendations similar and pheochromocytoma crisis.11
across multiple guidelines. Guidance on which antihypertensive agent to use
Other hypertensive emergencies, such as in acute for managing hypertensive emergencies is even more
coronary syndromes (ACS), have no well-designed sparse than BP targets, with no blinded prospective
Table 1. Hypertensive Emergencies Requiring Immediate Blood Pressure Lowering12
Clinical Presentation Timeline and Target BP First-line Treatments Alternative Treatments
Malignant hypertension with or without throm- Several hours; Labetalol, nicardipine Nitroprusside, urapidil
botic microangiopathy or acute renal failure MAP −20% to −25%
Hypertensive encephalopathy Immediate; MAP −20% to −25% Labetalol, nicardipine Nitroprusside
Acute ischemic stroke and SBP >220 mm Hg or 1 hour; MAP −15% Labetalol, nicardipine Nitroprusside
DBP >120 mm Hg
Acute ischemic stroke with indication for 1 hour; MAP −15% Labetalol, nicardipine Nitroprusside
thrombolytic therapy and SBP >185 mm Hg or
DBP >110 mm Hg
Acute hemorrhagic stroke and SBP >180 mm Hg Immediate; SBP 130-180 mm Hg Labetalol, nicardipine Urapidil
Acute coronary event Immediate; SBP <140 mm Hg Nitroglycerine, labetalol Urapidil
Acute cardiogenic pulmonary edema Immediate, SBP <140 mm Hg Nitroprusside or nitroglycerine Urapidil (with loop diuretic)
+ loop diuretic
Acute aortic disease Immediate; SBP <120 mm Hg and Esmolol + nitroprusside or Labetalol or metoprolol
heart rate <60 beats/min nitroglycerine or nicardipine
Eclampsia and severe pre-eclampsia/HELLP Immediate; SBP <160 mm Hg and Labetalol or nicardipine + Not applicable
DBP <105 mm Hg magnesium sulfate
Abbreviations: BP, blood pressure; DBP, diastolic blood pressure; HELLP, hemolysis, elevated liver enzymes and low platelets; MAP, mean arterial
pressure; SBP, systolic blood pressure.
Bert-Jan van den Born, Gregory Y H Lip. ESC Council on Hypertension position document on the management of hypertensive emergencies. European
Heart Journal – Cardiovascular Pharmacotherapy. Volume 5, Issue 1. By permission of European Society of Cardiology.
JUNE 2023 • www.ebmedicine.net 4 ©2023 EB MEDICINE
trials comparing one antihypertensive agent to an- to play a significant role. In persons with normal BP
other. There are some prospective and retrospective regulation, there is an appropriate balance between
studies comparing labetalol to nicardipine for manag- normal vital organ perfusion, hypoperfusion, and
ing acute ischemic strokes and ICH; however, none hyperperfusion. The balance between cardiac out-
found a difference in patient-centered outcomes.13-17 put and peripheral vascular resistance depends on
Although there are no strong data to recommend a complex set of integrated actions between the
a class of antihypertensive for each hypertensive cardiovascular, neural, renal, and endocrine sys-
emergency, some guidelines do make specific rec- tems that is not fully understood. (See Figure 1.) A
ommendations (eg, beta blockers for acute aortic multisystem approach to BP regulation allows the
dissection) based on retrospective studies and expert body to respond to internal and external demands
opinion.18,19 The American College of Obstetricians such as hypervolemia or hypovolemia, thirst, infec-
and Gynecologists (ACOG) acknowledge there is no tion, trauma, and rapid changes in position.22,23 The
single agent that is superior to another in manag- sympathetic nervous system also plays a major role,
ing severe hypertension in pregnancy.20 More well- particularly during times of physical stress, by in-
designed trials comparing antihypertensive agents for creasing cardiac output and arterial vasoconstriction.
each specific hypertensive emergency are needed. Endothelial function is also important in modulating
BP regulation. The endothelium of the vascular wall
acts as a regulator of BP by secreting vasodilators and
n Etiology And Pathophysiology vasoconstrictors in response to various stimuli.22,23
Hypertensive emergencies are more likely in per- While the underlying mechanisms of primary hy-
sons aged >60 years, and those who are Black, pertension and hypertensive emergency are not fully
male, underinsured or uninsured, and those who live understood, there seems to be several overlapping
in lower-socioeconomic areas.21 While the precise causes. The initial event appears to be an abrupt rise
pathophysiology of hypertensive emergency re- in BP from a known or unknown stimulus followed by
mains unclear, dysfunctional autoregulation appears compensatory mechanisms arising from the vascular
Figure 1. Pathophysiology of Hypertensive Emergencies
Eric Adua. Decoding the mechanism of hypertension through multiomics profiling. Journal of Human Hypertension. Volume 37, Issue 4. Pages 253-264.
2023. Available at: https://www.nature.com/articles/s41371-022-00769-8/figures/1 Used, without changes, according to Creative Commons Attribution
4.0 International Licence
JUNE 2023 • www.ebmedicine.net 5 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
endothelium. Initially, the endothelium releases the hypertensive emergencies, a secondary cause can be
vasodilator, nitric oxide, to compensate for the in- found in 20% to 40%.27 Secondary causes of hyper-
crease in intravascular pressure. The arterioles sense a tensive emergency refers to cases where the sudden
rise in BP and, in turn, arterial smooth muscle relaxes, increase in BP is a result of an underlying medical con-
causing vasodilation to reduce the rise in BP. A vicious dition. It is important to differentiate between primary
cycle occurs, with prolonged arterial smooth muscle and secondary causes of hypertensive emergency,
relaxation leading to prolonged endothelial dysfunc- because the management of each condition differs. In
tion and an inability to release additional nitric oxide, cases of primary hypertensive emergency, the goal of
resulting in a further increase in BP. 24 treatment is to lower the BP gradually to avoid further
Inflammation is also a major factor in endothelial end-organ damage. In cases of secondary hyperten-
dysfunction. The mechanical shear forces on the vas- sive emergency, the underlying condition must be
cular wall result in endothelial damage and dysfunc- identified and treated, which can help control the BP.
tion. Endothelial dysfunction results in the expres-
sion of inflammatory markers such as endothelin-1,
endothelial adhesion molecules, and cytokines. The n Prehospital Care
inflammatory component of hypertension is be- Prehospital providers can be critical to early iden-
lieved to promote coagulation, platelet aggregation, tification of hypertensive emergencies. In the
endothelial layer permeability, and vasoconstriction. prehospital setting, hypertensive emergencies are
Thus, there appears to be a complex interaction of typically not treated directly in the field. This is consis-
the renin-angiotensin-aldosterone system, sympa- tent with ESO3 and European Academy of Neurology
thetic nervous system, and endothelial dysfunction, (EAN) guidelines.28 The AHA and ASA do not make
regardless of the initial stimulus. There is also evi- any recommendations regarding this topic.11
dence that angiotensin II activates the expression of Nitroglycerin is often given for chest pain sus-
genes for proinflammatory cytokines and activation pected to be cardiac in nature and occasionally due
of transcription factor NF-kB, causing a direct toxic to acute heart failure, consistent with the 2017 ACC/
effect to the vessel wall. An increased level of von AHA guidelines.11 Of note, pain relief following ad-
Willebrand factor, von Willebrand factor prepeptide, ministration of nitroglycerin is not diagnostically help-
plasmin-antiplasmin complexes, and reduced levels ful to differentiate ACS.29 Important questions to ask
of ADAMTS (a disintegrin and metalloproteinase with prior to administration of nitroglycerin include wheth-
thrombospondin motifs)13 are seen in patients with er the patient has used nitrates or phosphodiesterase
hypertensive emergency, suggesting that thrombotic inhibitors (eg, sildenafil or tadalafil), since concomitant
microangiopathy may also play a role.23,25 administration can result in precipitous hypotension.
It is the rate of change of BP that increases the A full set of vital signs should always be obtained
likelihood of end-organ damage, as the degree of BP by emergency medical services, if possible, and re-
elevation does not always correlate with the severity ported on arrival to the ED. IV access should also be
of end-organ damage.26 Individuals with long-stand- obtained in the prehospital setting to expedite medi-
ing hypertension may have adaptive autoregulatory cation administration in the hospital, whether to con-
changes that protect organs from sudden increases trol BP or to administer time-sensitive medications for
in BP. In previously normotensive patients who have underlying etiologies. In patients with symptoms of
acute hypertension (eg, pregnant women with pre- an acute ischemic stroke (which may be seen with se-
eclampsia), hypertensive emergency can occur at vere hypertension), the patient’s last-known-well time
lower MAPs. Alternatively, patients with chronic hy- is also helpful to guide care, as it has been shown
pertension may have extremely elevated BP without that decreased time from ischemic stroke onset to
hypertensive emergency. administration of thrombolytics improves outcomes.
Reducing BP for thrombolytic candidacy prehospital
may improve door-to-needle time; however, no trials
n Differential Diagnosis have established this. The INTERACT4 trial is cur-
As the term implies, hypertensive emergency carries rently recruiting patients to study this question.
a significant mortality rate, and clinical manifesta-
tions are considered life-threatening. A differential
diagnosis for hypertensive emergencies can be found n Emergency Department Evaluation
in Table 2, page 7. Primary causes of hypertensive History
emergency refers to cases where no underlying cause A hypertensive emergency can be identified based
for the sudden increase in BP can be identified. In on the patient’s past and present history and results
these cases, the increase in BP is due to a combina- of the physical examination, laboratory analysis,
tion of genetic, environmental, and lifestyle factors, and imaging. There is no specific BP threshold that
including obesity, lack of exercise, and a diet high in defines hypertensive emergency; however, guidelines
sodium. In patients presenting to the ED with primary recommend that patients with BP readings ≥180/110
JUNE 2023 • www.ebmedicine.net 6 ©2023 EB MEDICINE
Table 2. Differential Diagnosis of Hypertensive Emergencies
System Differential Diagnosis Clinical Findings and Features Workup
Brain Hypertensive encephalopathy Headache, nausea, vomiting, confusion, seizures, Diagnosis of exclusion, MRI brain to
Posterior reversible encephalopathy coma evaluate for edema
syndrome
Reversible posterior
leukoencephalopathy syndrome
Acute ischemic stroke Focal neurological deficits Diagnosis of exclusion, MRI brain to
evaluate for ischemia
Subarachnoid hemorrhage Thunderclap headache, meningismus CT/CTA/MRI brain, lumbar puncture
Intracranial hemorrhage Stroke-like symptoms, Cushing triad (bradycardia, CT brain
respiratory depression/irregularity, widened pulse
pressure), fixed dilated pupil
Hypertensive retinopathy Visual acuity changes Fundoscopy
Arteries Aortic dissection Acute heart failure, acute coronary syndromes, CTA chest, abdominal/thoracic
cardiac tamponade, ischemic limb, stroke, ultrasound, angiography
mesenteric ischemia, renal failure
Pre-eclampsia/eclampsia/HELLP Severe headache, visual disturbances, altered Urinalysis, serum creatinine, platelet
mental status, seizure count, liver function tests
Hypertensive retinopathy Vision changes, often asymptomatic Fundoscopy
Thrombotic thrombocytopenic purpura Fever, anemia, thrombocytopenia, altered mental CBC, CMP, PT, PTT, fibrinogen,
status, renal failure LDH
Hemolytic-uremic syndrome Renal failure, anemia, thrombocytopenia
Disseminated intravascular coagulation Coagulopathy, thrombosis
Polyarteritis nodosa Cutaneous lesions, fatigue, weight CRP, ESR, CTA, angiography
loss, fever, arthralgia
Takayasu arteritis Aortic regurgitation, claudication, bruits CTA/MRI chest, angiography,
ESR/CRP
Kidney Acute renal failure Oliguria, confusion, pericarditis Urinalysis, BMP, renal ultrasound
Scleroderma renal crisis Oliguria, anemia
Acute glomerulonephritis Recent upper respiratory infection or skin infection Urinalysis, BMP, C3/C4, CBC
Renal artery stenosis Young-onset hypertension, abdominal bruit Duplex renal ultrasound, CTA/MRA
Heart Myocardial infarction Chest pain, shortness of breath Electrocardiogram, troponin
Congestive heart failure Shortness of breath, lower extremity edema, Chest x-ray, +/- brain natriuretic
jugular vein distension, S3/S4 peptide, electrocardiogram
Substance/ Tyramine reaction Monoamine oxidase inhibitor use, tyramine-rich Medication reconciliation
medication diet, sympathomimetic syndrome (diaphoresis,
induced mydriasis, tachycardia, hyperthermia)
Abrupt withdrawal of clonidine, Reflex tachycardia, headache
ACE inhibitors, or beta blockers
Serotonin syndrome Altered mental status, hyperthermia, tachycardia,
clonus, hyperreflexia
Sympathomimetic exposure Diaphoresis, mydriasis, tachycardia, hyperthermia +/- urine drug screen
Withdrawal (alcohol, benzodiazepines) Autonomic hyperactivity, seizures, delirium tremens Diagnosis of exclusion
Endocrine Cushing syndrome Hyperpigmentation, hirsutism, amenorrhea 24-hour urinary free cortisol or
dexamethasone suppression test
Pheochromocytoma Episodic hypertension, tachycardia, flushed skin Plasma/urine metanephrines, CT
adrenal
Hyperthyroidism Exophthalmos, goiter, hyperreflexia TSH, free T3/T4
Other Burns Blisters, eschar, electrical injury Clinical diagnosis
Pain Tachycardia
Abbreviations: ACE, angiotensin-converting enzyme; BMP, basic metabolic panel; CBC, complete blood cell count; CMP, comprehensive metabolic panel;
CRP, C-reactive protein; CT, computed tomography; CTA, CT angiography; ESR, erythrocyte sedimentation rate; HELLP, hemolysis, elevated liver
enzymes, and low platelets; LDH, lactate dehydrogenase; MRA, magnetic resonance angiography; MRI, magnetic resonance imaging; PT, prothrombin;
PTT, partial thromboplastin time; TSH, thyroid-stimulating hormone.
www.ebmedicine.net
JUNE 2023 • www.ebmedicine.net 7 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
mm Hg be evaluated promptly because they are der should encircle 80% or more of the patient’s arm.
at increased risk for adverse cardiovascular out- An undersized cuff will typically overestimate the BP
comes.11,30 It is important to remember that during and an oversized cuff will underestimate the BP. Initial
the clinical evaluation, regardless of the BP measure- pressure measurement in the ED is often transiently
ment, the emphasis remains on determining whether elevated. Simply allowing the patient to rest quietly
end-organ damage is present or imminent. and repeating the test will often lead to a more ac-
A thorough evaluation must include the curate reading.33
patient’s prior hypertensive history, including current MAP is often the preferred measurement of BP
antihypertensive medications as well as compliance. for several reasons: (1) automated oscillometric BP
Any recent medication changes must also be noted. cuffs measure MAP directly, effectively making it more
Special attention must be paid to a patient’s history accurate than systolic or diastolic readings, which are
of over-the-counter medications such as cough calculated based on the MAP reading; (2) systemic
and cold medications (particularly those containing autoregulation adapts to changes in MAP, and the risk
pseudoephedrine or phenylephrine), as well as for hypertensive emergency therefore appears to be
substances such as cocaine, methamphetamines, or more closely related to MAP rather than SBP;34,35 and
other sympathomimetics. A complete medication (3) titration of antihypertensive medications is usually
history should be conducted to identify other based on a single variable, and by using MAP, there
medications that are not used for treatment of is a less variability compared to systolic or diastolic
hypertension that may lead to a presentation of readings. Unfortunately, most of the society recom-
hypertension (eg, monoamine oxidase [MAO] mendations described do not use MAP.
inhibitors, serotonergic medications). The comprehensiveness of each part of the physi-
When asking about past medical history, it is cal examination should be dictated by the patient’s
important to inquire about any pre-existing organ chief complaint. There are key findings the clinician
dysfunction to distinguish it from an acute process. should be aware of, as they may indicate underlying
Data from a 2021 meta-analysis demonstrate that end-organ damage. Table 3 lists the most common
the risk for hypertensive emergency is higher in presenting symptoms of hypertensive emergency and
patients with a history of comorbid cardiovascular the most common sequelae of end-organ damage.
conditions, such as chronic kidney disease (odds Lung and heart auscultation should be performed for
ratio [OR], 2.9), coronary artery disease (OR, signs of congestive heart failure or pulmonary edema
1.65), or stroke (OR, 1.77).31 In a large multicenter (third heart sound, elevated jugular venous pres-
study of patients hospitalized with acute severe sure, and crackles on lung examination). A new-onset
hypertension, the presence of either chronic kidney cardiac murmur may signify papillary muscle rupture
disease or acute kidney injury was associated with during an acute myocardial infarction or type A aortic
worse outcomes, including increased length of dissection. Evaluation of the abdomen should include
hospitalization. Even after accounting for baseline assessment for a bruit/mass that can suggest renal
renal dysfunction, the presence of acute kidney injury artery stenosis and aortic aneurysm.
or an acute deterioration in kidney function during The neurologic examination should note mental
hospitalization was associated with morbidity and status changes such as delirium and depressed
predicted mortality.32 Women should be asked about level of consciousness, which are found in patients
pregnancy and postpartum status as well as previous with hypertensive encephalopathy. Lateralizing
peripartum diseases such as gestational diabetes, signs, however, are uncommon in hypertensive
hypertension, and pre-eclampsia or eclampsia.
A social history should include a rough estimate
of sodium intake, general diet intake (eg, tyramine- Table 3. Common Symptoms and Sequelae
rich foods) as well as the consumption of alcohol or of Hypertensive Emergencies11,36
other gamma-aminobutyric acid (GABA)-agonists, Most common presenting symptoms of hypertensive emergency:
including their abrupt cessation, all of which can • Shortness of breath (29%)
increase the likelihood of hypertensive emergencies. • Chest pain (26%)
• Headache (23%)
• Altered mental status (20%)
Physical Examination • Focal neurologic deficit (11%)
The physical examination should include serial BP
measurements with an appropriate-sized cuff on both Most common sequelae of hypertension-induced end-organ
arms while the patient is in a resting position. Patients damage:
should be seated comfortably, with back supported, • Pulmonary edema/heart failure (32%)
• Ischemic stroke (29%)
legs uncrossed, and all clothing covering the cuff
• Acute coronary syndromes (18%)
removed. The patient’s arm should be supported at • Hemorrhagic stroke (11%)
heart level, as measurements above and below this • Acute aortic syndrome (aortic dissection) (2%)
level may give misleading readings. The cuff blad- • Hypertensive encephalopathy (2%)
JUNE 2023 • www.ebmedicine.net 8 ©2023 EB MEDICINE
encephalopathy not complicated by ischemic brain Figure 2. Malignant Hypertension on
injury and suggest a vascular event. Fundoscopic Imaging
Traditionally, patients with suspected hypertensive
emergency warrant fundoscopic examination, since the
presence of grade III or IV hypertensive retinopathy is a
sign of microvascular dysfunction and impaired cere-
bral autoregulation, and can be the only sign of end-
organ damage.23,37 Retinopathy grade III or IV is pres-
ent when bilateral cotton wool spots, flame-shaped
hemorrhages, and/or papilledema are found by means
of retinal examination. An image of these findings can
be seen in Figure 2. There are currently no guidelines
or significant evidence to suggest whether all patients
being evaluated for hypertensive emergency require
fundoscopic examination. Therefore, the decision to
perform fundoscopy is ultimately provider-dependent.
Recently, the BARKH-based algorithm was
proposed by the Department of Medicine Emergen-
cies and Hypertension Unit, in Padova, Italy for quick
identification of hypertensive emergencies and their
associated acute organ damage. Figure 3 outlines
Image shows flame-shaped hemorrhages, cotton wool spots, and
the BARKH algorithm. The acronym stands for Brain, papilledema consistent with grade III/IV retinopathy.
Arteries, Retina, Kidney, and Heart, and offers a sim- Reprinted with permission of https://EyeRounds.org, the University of
plified, streamlined approach to assessing the patho- Iowa. https://eyerounds.org/atlas/photos/malignant-HTN.jpg
logical changes associated with hypertensive emer-
gency. Although the list is not exhaustive, it offers
emergency clinicians a quick bedside tool to help aid n Diagnostic Studies
decision-making. For more detailed treatment recom- Patients who present with a BP ≥180/110 mm Hg-
mendations, see the “Treatment” section, beginning without signs or symptoms of a possible underlying
on page 11. hypertensive emergency should not be subjected to
routine diagnostic studies in the
10 G. P. ROSSI ET AL. emergency department (ED) on
Figure 3. The BARKH Algorithm the basis of their hypertension
alone. It is well-documented that
Grade III arterial HT evaluating for end-organ dam-
age in asymptomatic patients
Evidence of BARKH
does not change ED manage-
(HT-Mediated Organ Damage) ment, nor does it improve
outcomes. It does, however,
increase the likelihood for un-
necessary hospitalizations.38,39
Brain Arteries Re�na Kidney Heart Patients who present with
(Stroke (Acute aor�c (Grade III-IV (Acute renal (Acute Heart asymptomatic hypertension are
or syndromes Keith-Wagener- insufficiency failure,
hypertensive or Barker or pulmonary
at no increased risk for major
encephalopathy) (Pre)eclampsia re�nopathy) thrombo�c edema) adverse cardiovascular events,
or HELLP) microangiopathy) acutely. Any subsequent major
adverse cardiovascular event in
patients who are discharged with
asymptomatic hypertension is
Hypertensive Emergency likely secondary to other risk fac-
tors such as age, sex, diabetes,
Rapid BP reduc�on with i.v. drugs chosen according to BARKH atrial fibrillation or prior cardio-
vascular disease, or consequenc-
igure 2. Simplified brain, arteries, retina, kidney and/or heart (BARKH)-based algorithm for a quick identification of the es hyperten-
of chronic hypertension that
ve emergenciesAbbreviation:
(HEs) and the associated
BARKH, acute organ
brain, arteries, retina,damage. If BARKH
kidney, heart; involvement
BP, blood pressure; is detected,
HELLP, the reduction would
hemolysis, of BP values
not immediately benefit
hould be undertaken withliver
elevated i.v. enzymes,
treatment;andin low
any platelets;
other case,
HT, an oral treatment is recommended. BP: blood pressure; HT: hyperten-
hypertension.
on; HELLP: haemolysis elevated
Management liver enzymes
of hypertensive low platelets.
emergencies: a practical approach. Gian Paolo Rossi, Giacomo Rossitto,
from aggressive antihyperten-
Chiarastella Maifredini, et al. Blood Pressure. 2021. Volume 30, Issue 4. Reprinted by permission of sive therapy or further inpatient
Taylor & Francis Ltd, http://www.tandfonline.com evaluation.38,40
etermining prognosis. Accordingly, to save the Pathophysiological considerations and implication
atient’s life, an immediate
JUNE decrease of BP values to
2023 • www.ebmedicine.net for management9 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
mit the extension of organ damage, is mandatory
The speed and severity of BP elevation are the main
12]. Consensus exists (Class of Recommendation I,
If a patient does present with symptoms sug- indicated on a case-by-case basis, although routine
gestive of an underlying hypertensive emergency, pregnancy testing is generally relevant in the appro-
diagnostic studies should focus on areas that may priate population.
reveal end-organ damage.
Electrocardiogram
Basic Laboratory Analysis If there is concern for myocardial ischemia or
The laboratory workup for patients suspected of dysrhythmia (eg, chest pain, palpitations, shortness
having hypertensive emergency may include testing of breath), an electrocardiogram (ECG) should be
to assess renal function, electrolyte balance, and obtained, although ECG is not particularly sensitive in
red blood cell parameters. Suspicion may come detecting left ventricular hypertrophy, and its sensitiv-
from reports of fatigue, generalized weakness, ity varies according to body habitus. The presence
excessive fluid loss from vomiting/diarrhea, and of left ventricular hypertrophy is associated with
dehydration, or other elements obtained from long-standing hypertension, increased incidence of
the history and physical examination. If there is cardiovascular disease, and early death.42 In addi-
suspicion for renal injury, testing may include a tion to left ventricular hypertrophy, the presence of
basic chemistry panel (including creatinine) and a left heart strain pattern on ECG has been shown
urinalysis with microscopy to assess for significant to identify patients with greater left ventricle mass, a
changes in glomerular filtration rate, proteinuria, higher prevalence of echocardiographic left ventricu-
red blood cells, and cellular casts that may indicate lar hypertrophy that is more likely to be concentric,
renal parenchymal disease. A complete blood cell and lower myocardial contractility and higher estimat-
count can be helpful to assess for the presence ed myocardial oxygen demand.43 The classic strain
of anemia and thrombocytopenia, which can be pattern is typically described as ST depression with a
indicative of a microangiopathic hemolytic process. down-sloping convex ST segment and discordant T-
A lactate dehydrogenase level and haptoglobin wave inversions in the lateral precordial leads. Figure
level can also be obtained to help determine the 4 shows the characteristic ECG findings seen in left
degree of hemolysis. ventricular hypertrophy with strain pattern.
For patients presenting with altered mental status
or neurologic deficits, a point-of-care glucose level Imaging Studies
should be obtained to exclude acute hypoglyce- Imaging studies should be tailored to clinical con-
mia. If there is concern for myocardial injury, cardiac cerns. A chest radiograph may be useful to evaluate
troponin-I (cTnI), a cardiac-specific protein with a very for interstitial pulmonary edema or cardiomegaly, or it
high sensitivity and specificity for myocardial injury, may show a widened mediastinum in the setting of a
should be obtained. Patients with elevated cTnI have thoracic aortic dissection. A point-of-care ultrasound
a higher risk for mortality, independent of other clini- by an experienced clinician may help identify aortic
cally relevant variables, including baseline character- dissection, evidence of left ventricular hypertrophy, di-
istics and comorbidities.41 Additional studies may be minished ejection fraction, pulmonary edema, or other
causes of elevated blood
pressure, such as bladder
Figure 4. Left Ventricular Hypertrophy outlet obstruction.
CT imaging of the
head is useful when
assessing for acute
intracranial hemorrhage
(ICH), and is often indi-
cated if there is concern
for cerebrovascular
ischemia or hypertensive
encephalopathy. See
Figure 5, page 11, for
common locations of
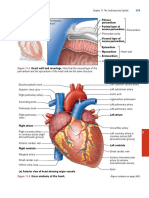
ICH seen on CT imaging.
CT imaging can suggest
hypertensive encepha-
lopathy in certain clini-
cal contexts; however,
Left: Image shows thickening of the myocardium of the left ventricle.
Right: Electrocardiogram (ECG) shows evidence of left ventricular hypertrophy with increased R-wave amplitude
an MRI of the brain is
in the left-sided ECG leads (I, aVL, V4-6) and increased S-wave depth in the right-sided leads (III, aVR, V1-3). needed to confirm the
Additionally, there are discordant T-wave inversions in leads V5 and V6 that are consistent with left heart strain. diagnosis (T2-weighted
JUNE 2023 • www.ebmedicine.net 10 ©2023 EB MEDICINE
FLAIR MRI).44 While CT may not be as sen- Figure Access
5. Common Locations of Intracranial
sitive as MRI in identifying regions of brain
Open
Hemorrhage Secondary to Hypertension
edema, it is usually more readily available,
takes less time to perform, and is essential and
for ruling out other intracranial lesions. mass
When conducted within 6 hours of Ha
symptom onset, noncontrast head CT
remains the gold standard for diagnosing
using
subarachnoid hemorrhage (SAH), with a toma
negative predictive value of 99.9%.46 CT area,
sensitivity for intracranial blood decreases to A
substantially over time, particularly in the
subarachnoid space. To confirm the di-
mult
agnosis, a lumbar puncture is required. of h
If a CT is nondiagnostic for exclusion of slice)
ICH, xanthochromia or red blood cells tion,
in the cerebrospinal fluid from a lumbar
puncture are highly suggestive of SAH. CT
to be
angiography of the brain is often used to MR
look for intracranial aneurysms that often ence
cause SAH.47 matio
Figure 6 shows the classic findings with
posterior reversible encephalopathy syn-
requ
drome (PRES) seen on MRI. Papilledema, of de
a surrogate marker for cerebral edema, is be
can also be evaluated using ultrasound to ation
measure the optic nerve sheath diameter.
Figure
Reproduced1 from
Typical locations
Stroke and of hypertensive
Vascular Neurology. Cyrus K. Dastur, ICH
WenguiareYu.putamen
Volume 2, caver
Optic nerve sheath diameter >5 mm
has been shown to be 95% sensitive for (A), thalamus (B), subcortical white matter (C), pons (D) Ltd.
Issue 1. Pages 21-29. Copyright 2017, with permission from BMJ Publishing Group and CT
papilledema and is therefore a feasible tool cerebellum (E). Thalamic and subcortical haemorrhages often vascu
to assess for increased intracranial pres- extend into ventricles (B and C). CAA, drug abuse or vascular sign’.
sure.45 (See Figure 7, page 12.) Figure 6.
anomaly High
often Signal-Intensity
causes lobar haemorrhage Vasogenic
Posterior (F).
reversible ICH,Edema
encephalopathy on
syndrome Liman et al.
ciated
Magnetic Resonance
intracerebral haemorrhage; Imaging of the amyloid
CAA, cerebral Brain angiopathy.
risk
n Treatment HTN
Acute Decompensated Heart Failure newe
Treatment of hypertensive acute
Lobar ICH is commonly the result of cerebral amyloid
angiopathy (CAA).14 Amyloid deposition in small-sized to the ‘
decompensated heart failure (ADHF)
should focus both on lowering the pa- medium-sized cortical perforators may lead to the haem
tient’s SBP as well as improving respiratory rupture of these vessels, resulting in asymptomatic micro- signifi
distress. Three interventions that are often requi
employed to manage hypertensive ADHF
haemorrhages or symptomatic lobar haemorrhages.14
Non-lobar ICH is most often the result of long-standing ation
are noninvasive positive-pressure ventila-
tion (NIPPV), diuretics, and vasodilators. All high blood pressure resulting in lipohyalinosis of small Re
of these interventions have varying degrees perforating arteries of the basal ganglia, thalamus, pons ation
of evidence in improving patient outcomes. exam
and cerebellum, leading to deep haemorrhages, often
Because this review is focused on BP man- vascu
agement during hypertensive emergencies, with extension into the ventricles.12 15 The most common
NIPPV for ADHF will not be discussed. locations of hypertensive ICH are the putamen, thal-
amus, subcortical white matter, pons and cerebellum
Diuretics
(figure 1). EMER
There is conflicting evidence about the ICH
utility of early IV diuretic use in ADHF. One Secondary ICH is associated with a number of con-
study showed early administration of IV genital
High and acquired
signal-intensity
shine through on DWI ADC values.conditions
vasogenic edema
and elevated such as
on magnetic resonance
(b) Cytotoxic edema, characterized vascular
signal elevation,malfor-
FIGURE 4. Diffusivity in PRES. (a) Vasogenic edema, characterized by increased signal in T2, normal signal or variable T2
imaging
by T2
of the brain,
DWI hypersignal
given
diuretics reduces in-hospital mortality in consistentADC
mations,
and corresponding withreduction
posterior
tumours,
reversible
(circle). encephalopathy
coagulation
Vasogenic syndrome.
edema is virtually always
disorders,
co-present (arrows).
use of or m
Thomas G. Liman, Eberhard Siebert, Matthias Endres. Posterior reversible
ADHF. A post hoc analysis of a large multi- PROGNOSIS their
anticoagulants
encephalopathy
AND OUTCOME and
syndrome. thrombolytic
Current Opinion inof 0.2 agents,
Neurology.
(95% Volume
CI, cerebral vascu-the
32,
0.15-04)[33 Issue
].
&&
1. Pages
However, 25-
given
center prospective registry enrolling ADHF Even though PRES has gained
35. By permission increased
of Wolters attention
Kluwer Health Inc.heterogeneity of studies with differences in outcome
https://journals.lww.com/co-neurology/ 3 16 17 (EMS
patients in the ED (REALITY-AHF registry) data litis,
since drug
its first abuse
description more than and cerebral
two decades ago, venous
variables (e.g. thrombosis.
Abstract/2019/02000/Posterior_reversible_encephalopathy_syndrome.6.aspx
in-hospital death, functional outcome
on outcome from prospective studies are
still lacking.
with modified Rankin scale, Glasgow outcome scale),
study populations and case numbers, results have to toma
In most cases, PRES has a good short-term and be interpreted with caution. Furthermore, mortality
long-term prognosis if treated fast and adequately and morbidity in PRES are also dependent on the sever
JUNE 2023 • www.ebmedicine.net 11 clinical symptoms are revers-
© 2023underlying
EB MEDICINE. ALL RIGHTS RESERVED.
EARLY DIAGNOSIS
and MRI findings and disease, that is women with PRES in
ible after several hours or days [31]. However, cerebral eclampsia have a better prognosis than patient with Sta
hemorrhage or ischemia and irreversible neurologi- chemotherapy-associated PRES in incurable
ICH should be suspected in any patient with severe
cal deficits or death occur. Studies reported complete cancer patients. (ABC
resolution of edema and clinical recovery in 70-90% In all available studies, death occurred in 8-17%
demonstrated that patients who received any dosage mon, with close monitoring of urine output. If little or
of IV furosemide within 60 minutes of arrival had a no diuretic response is seen, the diuretic dose can be
3-fold lower in-hospital mortality than those who re- doubled.
ceived IV furosemide later during their stay. However,
it should be noted there were significant baseline dif- Vasodilators
ferences between the early treatment and non-early Multiple large systematic reviews and RCTs have
treatment groups. The early groups were (1) more demonstrated that vasodilators are safe and effective
likely to present via ambulance; (2) presented with in lowering SBP in ADHF, but fail to show any consis-
more acute symptom onset; (3) had higher BPs and tent improvement in short- or long-term survival.53-56
heart rates; and (4) had significantly more patients This may be due to different phenotypes observed in
with symptoms suggestive of being volume over- patients with ADHF. Some patients’ symptoms may
loaded (peripheral edema, pulmonary edema, rales, be secondary to an acute increase in left ventricular
jugular vein distension, and orthopnea). There was afterload, leading to rapid fluid redistribution into the
also no standardized dosage of IV furosemide ob- lungs, while others may experience a gradual increase
served. Each of these confounders, alone, could lead of cardiac filling pressures related to pre-existing
to earlier recognition and treatment.48 Two other post structural heart disease. ESC guidelines state that
hoc analyses from different multicenter prospective patients of the former phenotype may benefit from
registries enrolling ADHF patients in the ED showed nitrates or nitroprusside to decrease afterload,51 while
no in-hospital mortality difference between early AHA guidelines state that the role of nitroglycerin and
versus late loop diuretic administration; however, nitroprusside is uncertain and recommend their use
one study was limited by similar baseline differences only as an adjuvant, to decrease preload, for relief of
between early and non-early treatment groups (eg, dyspnea in hypertensive patients.52
pulmonary edema, elevated jugular vein distension, Administering a high-dose nitroglycerin IV bolus 1.2 a 8 mL
and dyspnea),49 and the other did not report the tim- (600 mcg to 4 mg administered over several minutes), (preparación
: 2 amp de
ing or quantity of diuretics given.50 The 2021 ESC51 followed by a nitroglycerin infusion (started at 50-
25 mg/100
and 2022 AHA guidelines52 recommend using loop 100 mcg/min and titrated down based on symptom mL)
diuretics for those with signs of volume overload, as improvement and SBP) has been shown to be safe57,58
they provide the most rapid and effective diuresis for and may help reduce intensive care unit (ICU) admis-
patients with ADHF. The general recommendation sions.59 A systematic review found, with a moderate
LETTERSof
TOan IV EDITOR
THE dose 1 to 2 times the patient’s equivalent quality of evidence, that high-dose nitrates may lower
maintenance dose of their oral loop diuretic is com- rates of mechanical ventilation, improve BP, shorten
length of stay, and lower
Figure 7. Optic Nerve Sheath Evaluation Using Ocular Ultrasound rates of ICU admission;
however, the authors not-
ed that these conclusions
are limited due to the
heterogeneity and varying
quality of studies in-
cluded.58 A well-designed
RCT is needed to clarify
the utility of high-dose
nitroglycerin for patients
with acute increases in
volume overload.
Clevidipine has also
shown to be effective in
quickly reducing SBP in
patients with hypertensive
ADHF, possibly making it
an alternative if nitrates
are contraindicated,
FIGURE. A, Essential structures of the eye visualized with ocular point-of-care ultrasound. Ocular point-of-care ultrasound (POCUS)
Ocular point-of-care ultrasound (POCUS) can be performed using a high-frequency linear array transducer
although nicardipine may
can be used to visualize the dimensions of critical ocular structures (A) at the bedside. This representative image (B) shows an ocular
through a closed eyelid on a supine patient. View A: Diagram of the structures visualized using POCUS. View be a more available and
POCUS image taken at the bedside using a 7.5-mHz linear probe through a closed eyelid on a supine patient. The diameter of the
B: The
optic nerve diameter
should of the optic
be measured nerve3 is
at a point mmmeasured
posterior3 to
mm theposterior to the retina.
retina. Increased heightIncreased height
of the optic disc of
andthe diametercost-effective
optic disc
expanded of option.60,61
and expanded diameter of the optic nerve sheath (>5 mm) are indicative of papilledema,
the optic nerve are indicative of papilledema, which may be indicative of elevated intracranial pressure. a sign of elevated Patients may develop
intracranial pressure.
tolerance to nitroglycerin,
Reprinted from Mayo Clinic Proceedings. Volume 95, Issue 9. Gregory W. Heinicke, Justin M. Chen, Emily J.
Cox, et al. A case of elevated intracranial pressure diagnosed with point-of-care ocular ultrasound. Pages 2046-
requiring higher doses or
A 5.8 mm2048.
cutoff for ONSD
Copyright 2020, aswith
a diag- thisfrom
permission case, by the patient’s photo-
Elsevier. transition
Data Previously Presented at: 2019 Society of to a different
nostic criteria for IIH previously phobia). Additionally, use of POCUS General Internal Medicine Annual Meeting,
Washington, DC, May 8 e May 11, 2019. Con-
yielded a sensitivity of 90% and can facilitate compliance with the ference proceedings available at: Abstracts from
JUNE
specificity of 2023
84%7•; www.ebmedicine.net
however, this reduced imaging recommendations 12 ©2023 EB MEDICINE
the 2019 Annual Meeting of the Society of Gen-
criterion may need to be refined as from the Choose Wisely Campaign, eral Internal Medicine. J Gen Intern Med.
elevated ONSD and optic disc height while also soothing some concerns 2019;34(Suppl 2): 99-867 (Abstract ID
vasodilator.62 Authors of a small retrospective study analysis found a statistically significant increase in
comparing nicardipine to nitroglycerin for ADHF in the 90-day mortality.6,69 For patients receiving mechani-
ICU found a significant number of patients who were cal thrombectomy, there are no RCTs that assess
given nitroglycerin required nicardipine for BP control, optimal BP management prior to intervention. AHA/
and they theorized that this may reflect patients devel- ASA and ESO recommendations to lower BP to
oping a tolerance to nitroglycerin.63 <185/110 mm Hg prior to intervention stem primarily
Urapidil, which is not available in the United States from inclusion criteria of prior clinical trials in which
but is available in Europe, is a sympatholytic vasodila- patients received thrombolytic medications, and then
tor that might improve short-term cardiac function additional prospective data demonstrated a statisti-
when given in the ED, although further studies are cally significant increased mortality and functional
necessary to determine its efficacy.64 disability in those with elevated BP before and after
receiving thrombolytic medications or mechanical
Other Treatments thrombectomy.70-74 ESO guidelines do not mention
Additional treatments used historically for ADHF any specific antihypertensive medication to use; the
include morphine and nesiritide. Morphine should not AHA/ASA recommend using nicardipine, clevidipine,
be used in the management of patients with ADHF, as or labetalol, though there are no data or recommen-
multiple studies have shown that patients who receive dations regarding one medication over another.75,76
morphine have an increased mortality risk, estimated For patients who are not receiving antithrombotic
to be 5-fold higher than those who do not receive agents or a mechanical thrombectomy, there is no
morphine.65,66 Nesiritide should also not be used to strong evidence to identify an optimal BP in the
manage ADHF. The ASCEND-HF trial, a large double- first few hours after onset of symptoms. If patients
blinded RCT, demonstrated that nesiritide provided are hypertensive >220/120 mm Hg, both AHA/ASA
no clinical benefit and was significantly more likely to and ESO guidelines state that lowering BP no more
cause hypotension.67 than 15% is reasonable and likely to be safe, with
no evidence to suggest that doing so improves or
Blood Pressure Targets worsens outcomes.2,3 Recommendations to treat
There are no RCTs or large studies to demonstrate excessive hypertension are supported by data from
a specific target SBP that is best for patients with multiple large retrospective and prospective studies
hypertensive ADHF. The ESC and AHA guidelines do demonstrating a U-curve pattern in the relationship
not mention any specific target for SBP.51,52 A post between admission SBP and mortality.77-79 That being
hoc analysis of the REALITY-AHF study reported that said, one should be extremely careful when lowering
patients in the ED whose SBP was reduced by >25% SBP, as reducing admission SBP >15% is significantly
may have had a higher mortality rate; however, this associated with worse outcomes, especially for those
study did not report any baseline characteristics of aged >70 years.80 Additional RCTs evaluating BP
the BP groups that could explain the difference in management within the first few hours of symptom
mortality and had several limitations to consider.68 onset are needed to clarify whether there is any ben-
Therefore, it is reasonable to target lowering SBP by efit or harm to reducing BP in patients not receiving
10% to 25% for patients with hypertension and ADHF. antithrombotic agents or mechanical thrombectomy.
Acute Ischemic Stroke Acute Coronary Syndromes
Once noncontrast CT excludes ICH as a cause ACS includes STEMI, NSTEMI, and unstable angina.
for a patient’s stroke-like symptoms, treatment Although unstable angina is considered its own entity
should be guided by whether the patient will re- within ACS, new high-sensitivity troponin testing has
ceive a thrombolytic medication or a mechanical made the diagnosis of unstable angina quite rare, and
thrombectomy. The decision to perform one or its management will not be discussed here.
both of these interventions should be made by an
interventionalist or neurologist. For patients receiving Blood Pressure Targets
thrombolytics or mechanical thrombectomy, AHA/ During the acute stage of ACS (ie, within the first
ASA and ESO guidelines both recommend lowering 24 hours, or prior to definitive treatment with
BP to <185/110 mm Hg prior to the intervention and thrombolysis or percutaneous coronary intervention),
maintaining BP <180/105 mm Hg for 24 hours post there are no good data to suggest an optimal BP
intervention.2,3 Only one RCT has assessed outcomes target. ESC guidelines specify a normotensive target
in patients managed at different BP ranges prior to for NSTEMI patients, while AHA guidelines do not
thrombolysis. The ENCHANTED trial randomized comment on any target BP. There are, however, corre-
patients to SBP 130 to 140 mm Hg or SBP <180 lations between admission BP and patient outcomes.
mm Hg prior to receiving IV alteplase. The authors It is well documented that an SBP <100 mm Hg on
found a statistically significant reduction in ICH in admission is a strong predictor of increased mortality
the intensive BP control group; however, post hoc within 6 months, reflected in clinical decision-making
JUNE 2023 • www.ebmedicine.net 13 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
tools such as GRACE and TIMI.81-83 Multiple large patients with ACS. Although a mortality benefit was
prospective studies have shown lower in-hospital seen in this systematic review, there are no RCTs with-
mortality rates and reduced major adverse cardio- in the last 20 years to clarify whether nitrate therapy
vascular events in patients who are hypertensive on improves mortality.
presentation.83-85 Acute hypertension in patients with
ACS may signify good cardiac function in response Intracerebral Hemorrhage
to significant stress, and is associated with improved Blood Pressure Targets
outcomes. AHA and ESC STEMI management guide- Relative to other hypertensive emergencies, ICH has
lines state that SBP >180 mm Hg and DBP >110 the most data to support recommendations for a
mm Hg are relative contraindications to fibrinolytic specific BP target. There is debate about how much
therapy, but caution that BP frequently fluctuates in BP should be lowered to optimize outcomes.91 Both
the early stages of ACS, and management should be the AHA/ASA and ESO guidelines recommend im-
focused first on pain control and clinical stabilization.9 mediately lowering SBP to <140 mm Hg when ICH
is recognized, and maintaining SBP between 130
Beta Blockers and 150 mm Hg, but not <130 mm Hg, to prevent
The AHA and ESC guidelines recommend admin- hematoma expansion.3,92 The largest RCTs to assess
istering beta blockers with high beta-1 affinity (eg, mortality and degree of disability for patients with
metoprolol) to hypertensive patients with STEMI.10,88 ICH are the INTERACT-2 and ATACH-2 trials, where
(Class I, level of evidence A, for oral administration; patients’ SBPs were lowered to either <140 mm Hg or
class IIA, level of evidence B for IV administration.) <180 mm Hg.5,93 The AHA/ASA guideline specifically
Multiple RCTs have demonstrated that beta block- states their recommendations are based on these 2
ers can reduce recurrent myocardial infarctions trials and the subsequent post hoc analyses of these
and ventricular fibrillation, and decrease infarction trials. A pooled analysis of both studies found that for
size.86,87 However, patients with SBP <120 mm Hg, every 10-mm Hg reduction from 170 mm Hg, there
age >70 years, or a heart rate >110 beats/min who was a trend toward lower mortality rates, smaller
were given IV beta blockers were found to have a hematoma expansion, and better functional recovery,
statistically significant higher risk for developing with a statistically significant reduced rate of neurolog-
cardiogenic shock. AHA guidelines cite these findings ical deterioration in patients with an SBP maintained
as contraindications to giving beta blockers to STEMI between 120 and 130 mm Hg.94 A post hoc analysis
patients in the first 24 hours, while ESC guidelines of ATACH-2 showed statistically significant higher
cite only ADHF, hemodynamic instability, or high- rates of neurologic deterioration and cardiac-related
degree atrioventricular block as contraindications.88 adverse events in patients maintained between 100
A recent Cochrane review that included these studies and 140 mm Hg, which is in contrast to what a post
stated that beta blockers probably reduce the long- hoc analysis of ATACH-2 trial alone found.4,74
term risk for all-cause and cardiovascular mortality.89 Lowering SBP when ≥180 mm Hg clearly im-
Although AHA/ESC guidelines state that beta block- proves patient outcomes, potentially reaching a peak
ers can be used to treat hypertension in patients benefit when lowered <140 mm Hg; however, other
with ACS, it is recommended to lower the BP slowly variables such as SBP variability and relative SBP
and avoid DBP <60 mm Hg, to maintain coronary reduction are important to be cognizant of when con-
perfusion. Well-designed RCTs directed at BP control sidering BP goals. The pooled analysis of ATACH-2
prior to definitive treatment in patients with ACS are and INTERACT-2 showed statistically significant
needed to clarify the relationship between BP and improved functional recovery when SBP was reduced
patient outcomes.89 40 to 59 mm Hg below the baseline SBP; however,
reduction ≥60 mm Hg worsened outcomes.94 The
Nitrates analysis also found a greater variability in SBP had
Both the AHA and ESC guidelines state that the a statistically significant greater number of adverse
use of IV nitrates for patients with STEMI who are events and neurologic deterioration, and a post hoc
hypertensive may be useful in the acute phase; analysis of INTERACT-2 identified variability in SBP as
however, neither cite evidence for this or a specific one of the strongest predictors of worse outcomes in
BP target.10,88 Both the AHA and ESC guidelines the first few hours of treatment.95
recommend IV nitrates for hypertensive patients Clinicians should be cognizant of iatrogenic
with NSTEMI. For the use of nitrates in ACS, both hypotension, as a large prospective study found it to
guidelines reference studies conducted more than be the highest risk factor for mortality, with its great-
20 years ago.7,8 A recent systematic review evaluated est risk in the first 6 hours.96 One might hypothesize
these studies and found a mortality benefit at day 2 that invasive (ie, arterial line) measurement of SBP
from nitrate therapy within 24 hours.90 No mortality reduces SBP variability, making it superior to nonin-
benefit was found at day 10 or >30 days. The authors vasive devices; however, there are no data to support
concluded that nitrates should be routinely given to this hypothesis.
JUNE 2023 • www.ebmedicine.net 14 ©2023 EB MEDICINE
Antihypertensive Medications is more efficacious than another.11,18,30 It is reason-
The AHA/ASA and ESO do not mention a specific anti- able to use a fast-acting, easily titratable beta blocker
hypertensive to use, and recommend using medication (such as esmolol) as a first-line agent to immediately
that has a fast time of onset and short half-life, to pre- control the patient’s heart rate. The ESC guidelines
vent excessive BP lowering and allow for easy titration, also recommend using an IV beta blocker to simul-
reducing the potential for variability.3,92 One retrospec- taneously lower a patient’s heart rate and SBP. ESC
tive study did not show a difference in hospital mor- guidelines cite a SBP goal of <120 mm Hg, with no
tality or functional recovery, and there are conflicting specific heart rate.18 If a patient has a contraindication
results from studies comparing time to BP goal, time at to beta blockers, nondihydropyridine calcium chan-
BP goal, and variability of BP between nicardipine and nel blockers (such as diltiazem or verapamil) could
labetalol.13-17 Therefore, either nicardipine or labetalol be an alternative for heart rate control. Vasodilators
are reasonable first-line medications. recommended by the ACC/AHA guideline include
To summarize, both nicardipine and labetalol ef- nicardipine, clevidipine, and nitroprusside.19
fectively and safely reduce SBP in patients with ICH,
with no clear evidence to suggest one works better Hypertensive Encephalopathy
than the other. A small pilot study demonstrated the Hypertensive encephalopathy is most commonly seen
efficacy of clevidipine to reduce SBP in patients with with BP > 220/120 mm Hg.105 There are no RCTs to
ICH,97 while another retrospective study found no dif- suggest a specific goal in BP reduction or which anti-
ference in time to SBP goal, length of stay, mortality, hypertensive agent to use.44,105 The International So-
or disposition between nicardipine and clevidipine.98 ciety of Hypertension guidelines recommend immedi-
When choosing an antihypertensive agent, clinicians ately reducing MAP by 20% to 25% using nicardipine
should consider practicability, variability, pharmaco- or labetalol as first-line agents.30 PRES is a form of
logical profile, and potential side effects of the agent. encephalopathy diagnosed on CT or MRI and can be
seen in hypertensive encephalopathy; however, one
Subarachnoid Hemorrhage should be careful not to attribute the presence of
There are little to no data to guide treatment in PRES to the patient’s hypertension. PRES can be pres-
patients with non–aneurysmal SAH. When caring ent in normotensive and even hypotensive patients.
for patients with an aneurysmal SAH, the focus is Retrospective studies have also shown no difference
primarily on prevention of rebleeding within the first in BP in those diagnosed with PRES compared to con-
12 hours, as this has been shown to worsen patient trols.44,106 Additional steps should be taken to identify
outcomes.47,99,100 Elevated BP is a known risk factor other causes of the patient’s PRES, such as immuno-
for rebleeding; however, there are no good data suppressive/cytotoxic drugs, a flare of the patient’s
to support the benefit of lowering BP in the acute autoimmune disorder, or renal failure.44,105
phase of SAH.101 A 2021 Cochrane review found a
single RCT from the 1980s evaluating the effect of Severe Pre-Eclampsia and Eclampsia
BP reduction, ultimately finding no significant benefit Blood Pressure Targets
to lowering BP.102 AHA/ASA guidelines recommend This review will discuss only the management of
lowering SBP to <160 mm Hg; ESO guidelines hypertension in patients with pre-eclampsia with
recommend lowering SBP <180 mm Hg; and the severe features and eclampsia. BP targets differ
Neurocritical Care Society guidelines recommend widely among guidelines. ESC guidelines recom-
treating only extreme hypertension (MAP >110 mm mend hospital admission when patients have a single
Hg).47,99,100 No specific antihypertensive agent is BP reading ≥170/110 mm Hg; however, they do not
mentioned in any of these guidelines. specify the timing of when the high BP reading should
be confirmed, nor do they specify which weeks of
Aortic Dissection gestation this applies to.107 ACOG is more specific in
To date, there have been no RCTs evaluating specific their guidelines, recommending hospital admission
BP targets during the acute management of aortic for women after 20 weeks’ gestation who have pre-
dissection, although there are several retrospective eclampsia with severe features. ACOG defines this as
evaluations.103 There are also no randomized studies SBP >160 mm Hg or DBP >110 mm Hg, confirmed by
that have evaluated the efficacy of different medical a repeat BP 15 minutes later; or 2 BP readings ≥140/90
treatments for aortic dissections. The 2022 ACC/AHA mm Hg (and ≤160/110 mm Hg) 4 hours apart, with
guidelines recommend reducing the patient’s heart thrombocytopenia, impaired liver function, renal
rate to 60 to 80 beats/min and then lowering SBP to insufficiency, pulmonary edema, new-onset headache
<120 mm Hg, citing one small retrospective study unresponsive to medication, or visual disturbances.20
and expert opinion.104 It also recommends using an IV ACOG recommends treating hypertensive patients
beta blocker before lowering the patient’s BP to pre- quickly, as they are at an increased risk for cerebro-
vent any possible reflex tachycardia.19 There are no vascular accidents, and patients with BP <140/90 mm
data to suggest a specific beta blocker or vasodilator Hg have lower rates of pre-eclampsia, eclampsia,
JUNE 2023 • www.ebmedicine.net 15 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
and preterm delivery.20 Whether strict BP control to maternal oliguria, stillbirth, and low Apgar score at 1
<140/90 mm Hg reduces cardiac- and neurovascular- minute. The authors concluded that the results warrant
associated morbidity and mortality remains unclear. advising against using hydralazine as first-line treat-
ment; however, they were not robust enough to guide
Antihypertensive Medications clinical practice.109,110 Efficacy and risk of side effects
For pregnant patients, ACOG guidelines specifi- from these antihypertensive medications should be
cally recommend IV labetalol, IV hydralazine, or oral further evaluated with larger head-to-head RCTs. There
immediate-release nifedipine as first-line therapies to is evidence that IV nicardipine can adequately treat
manage acute severe hypertension (SBP ≥160 mm Hg hypertension in antepartum and postpartum patients
or DBP ≥110 mm Hg that is persistent for 15 minutes and should be considered for treatment-resistant hy-
or more).20 See Table 4 for dosage and timing recom- pertension after using hydralazine, labetalol, or imme-
mendations. One Cochrane review found no evidence diate-release nifedipine.111-113 Whether nicardipine
that one medication is more effective or provides im- can be considered a first-line agent requires additional
proved outcomes for the fetus and mother; however, a studies, but its use as a continuous infusion may limit
meta-analysis of 21 trials comparing hydralazine to oth- its practicality.
er antihypertensive medications found that hydralazine For pregnant patients with pre-eclampsia with
was associated with more adverse outcomes, which severe features or those with eclampsia, the ACOG
included maternal hypotension, placental abruption, guidelines recommend magnesium sulfate at a
adverse effects on fetal heart rate, caesarean delivery, loading dose of 4 to 6 g IV over 20 to 30 minutes,
Table 4. Selected Medications Commonly Used in Hypertensive Emergencies108
Drug Name Dosage Max Dose Onset of Duration Adverse Mechanism of Action
Action of Action Effects
Clevidipine Initial: 1-2 mg/hr IV 32 mg/hr 2-4 min 5-15 min Hypotension, Nondihydropyridine calcium
Titrate: 2 mg/hr q90 sec reflex channel blocker
Max: 32 mg/hr tachycardia
Enalaprilat 1.25 mg-5 mg IV q6 hr 5 mg/24 hrs 15 min 12-24 hr Hypotension, Angiotensin-converting
hyperkalemia, enzyme inhibitor
cough
Esmolol Loading dose: 0.5-1mg/kg IV over No max dose, 1-2 min 10-30 min Hypotension, Selective beta-1 receptor
1 min but titrated to bradycardia antagonist
Maintenance: 50-300 mcg/kg/min IV effect
Titrate: 5-50 mcg/kg/min q5min
Hydralazine 10-20 mg IV every 6 hr 40 mg/24 hr 5-20 min 12-24 hr Hypotension, Direct-acting smooth
tachycardia, muscle relaxant
headache
Labetalol 20 mg IV; may repeat q10 min 300 mg/24h 2-5 min 2-18 hr Hypotension, Non-selective beta receptor
Max cumulative dose: 300 mg/24hr bradycardia antagonist and alpha
receptor antagonist
Magnesium 4-6g IV over 15-30 min No max dose, Immediate 30 min to Hypotension, Smooth muscle relaxant
sulfate Maintenance: 1-3 g/hr but titrated to 2 hr flushing, (vasodilator), calcium
effect weakness, channel blocker, anti-
respiratory arrhythmic
depression
Nicardipine Initial: 5 mg/hr IV 15 mg/hr Immediate 5-15 min Hypotension, Nondihydropyridine calcium
Titrate: 2.5 mg/hr every 5-15 min reflex channel blocker
Max: 15 mg/hr tachycardia
Nitroglycerin 5 mcg/min IV 200 mcg/min Immediate 3-5 min Hypotension, Vasodilator
Titrate: 5 mcg/min q3-5 min up to headache,
20 mcg/min; can increase by flushing
10-20 mcg/min every 3-5 min up to
200 mcg/min
Sodium Initial: 0.25-0.5 mcg/kg/min IV 2 mcg/kg/min Immediate 1-10 min Hypotension, Vasodilator, releases nitric
nitroprusside Titrate: 0.5 mcg/kg/min q5-10 min for more than cyanide toxic- oxide
Max: 2 mcg/kg/min 10 min ity, thiocyanate
toxicity, avoid
if possible
Abbreviations: IV, intravenous; q, every.
JUNE 2023 • www.ebmedicine.net 16 ©2023 EB MEDICINE
followed by a maintenance dose of 1 to 2 g/hr as a that acutely reducing BP in ED patients who present
seizure prophylaxis or treatment.20 The efficacy of with severe hypertension has any benefits in short-term
magnesium has been well-demonstrated by mul- risk reduction. In its 2013 clinical policy, the American
tiple large RCTs, and it can more than halve the risk College of Emergency Physicians (ACEP) discouraged
of developing eclampsia.114,115 ACOG guidelines initiation of BP medication in the ED for asymptomatic
acknowledge that a therapeutic range of 4.8 to 9.6 patients with hypertension. However, clinicians can
mg/dL to prevent eclampsia is questionable.20,116 consider initiating BP medications for those who are
When administering magnesium sulfate, the patient’s at high risk, such as patients who are Black, elderly,
deep tendon reflexes and respiratory status should be uninsured, or likely to be lost to follow-up.118
reassessed frequently, in addition to urine output, as There are no studies comparing oral to IV medi-
it may cause respiratory depression and is excreted cation in the management of hypertensive emer-
almost exclusively in the urine.20 gencies. Therefore, if the clinician decides to treat a
A checklist ACOG developed specifically for patient’s hypertensive emergency to improve their
hypertensive emergency treatment is available here: symptoms and prevent further end-organ damage, it
https://www.acog.org/-/media/project/acog/acogorg/ is recommended to use fast-acting, easily titratable,
files/forms/districts/smi-hypertension-bundle- and reliable IV antihypertensives.
emergency-checklist.pdf
Acute Renal Failure n Controversies and Cutting Edge
There is no consensus as to what degree of acute kid- Arterial Monitoring
ney injury constitutes acute renal failure, nor whether Due to advancements in ED capabilities, the use of
there is benefit to rapid BP management. The Inter- invasive BP monitoring (ie, arterial lines) has increased
national Society of Hypertension guidelines recom- in recent years. Invasive BP monitoring allows for
mend using either nicardipine or labetalol as first-line more accurate, real-time BP measurements, which
therapy for acute renal failure associated with severe subsequently allows for more rapid therapeutic ad-
hypertension, while ACC/AHA guidelines recommend justment, and presumably higher-quality care. How-
using nicardipine, clevidipine, or fenoldopam.11,30 ever, there is currently substantial variation in practice
The ACC/AHA guidelines directly contradict the as to who receives arterial lines.119 Unfortunately,
Kidney Disease Improving Global Outcomes (KDIGO) there are no good data to help guide this decision,
guidelines, which state that there is no utility for and there is no consensus as to what the standard of
fenoldopam to manage acute kidney injury, as it has care should be. Current indications for an arterial line
not shown efficacy in improving outcomes.117 There might include labile BPs, concern for inadequate or
are no RCTs to suggest one medication is preferable inaccurate automated oscillometric BP cuff readings,
over another, nor a specific BP target. Reducing SBP or clinical deterioration despite noninvasive manage-
or MAP by a maximum of 25% might be a reasonable ment. Realistically, an arterial line is probably unnec-
option, if hypertensive emergency is the suspected essary in most cases of hypertensive emergency for a
cause of the acute renal failure.11,30 few reasons: (1) the pain of arterial line insertion can
exacerbate hypertension, (2) there is no prospective
Oral Versus Intravenous Antihypertensives evidence to show this procedure is beneficial or nec-
As previously stated, there is no utility in emergently essary, and (3) current BP targets are mostly arbitrary
treating a patient’s hypertension if the clinician does and poorly defined with the exception of ICH and
not believe the BP is directly related to the patient’s acute ischemic stroke. Until more conclusive evidence
symptoms. Many patients will likely have evidence of exists, this will remain a topic of debate.
underlying end-organ damage (such as proteinuria)
on diagnostic evaluation, especially if their chronic Beta Blockers in Cocaine-Induced Hypertension
hypertension is poorly controlled. IV antihyperten- The use of beta blockers in patients with cocaine-
sives should be given only if the clinician believes the induced severe hypertension is controversial. Medi-
patient’s symptoms and end-organ damage is second- cal folklore has taught that there is a theoretical risk
ary to an acute rise in the patient’s BP and needs to be for unopposed alpha adrenergic stimulation when
rapidly corrected. For example, if a patient presents using beta blockade in conjunction with cocaine use,
hypertensive and short of breath, but is found on leading to unopposed vasoconstriction. This belief
diagnostic workup to have pneumonia with no signs of is founded on a small number of studies and case
end-organ damage that could explain their shortness reports that have not been replicated and were based
of breath, the patient’s high BP should not be treated mostly on adverse patient-reported events, with few
with IV antihypertensives. Optimal treatment of severe statistically relevant data.120-122 To date, the only
hypertension in this population is close outpatient fol- statement that can be made is that unopposed alpha
low-up, with a gradual move toward oral antihyperten- stimulation after beta blockade in cocaine toxicity is
sive medications.11 No validated studies have shown inconsistent, unpredictable, and a rare phenomenon
JUNE 2023 • www.ebmedicine.net 17 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
that can be addressed with the use of vasodilating of antihypertensives, guided by the type of end-organ
medications titrated to counteract vasoconstriction. damage, and frequently reassessed. Patients with no
evidence of hypertensive emergency do not need
n Disposition BP management and can be discharged with primary
All patients diagnosed with hypertensive emergency care follow-up. There is limited strength to the recom-
require hospital admission. The ACC/AHA Task Force mendations and guidance on treatment, as the major-
recommends admitting adults with hypertensive emer- ity of data are retrospective in nature. Many subjects
gencies to an ICU for continuous monitoring of BP discussed within this issue lack quality prospective
and for parenteral administration of antihypertensive blinded control trials.
agents. An intermediate care unit may also be consid-
ered, depending on hospital resources.
Patients presenting to the ED who do not meet n Time- and Cost-Effective Strategies
criteria for hypertensive emergency can be safely dis- • Patients with no evidence of hypertensive emer-
charged with close outpatient follow-up for repeat BP gency do not need BP management and can be
monitoring and consideration of hypertensive medi- discharged with primary care follow-up.
cation management. Additionally, initiation of oral an- Risk Management Caveat: Make sure the patient
tihypertensive medications in the ED does not appear has adequate access to primary care prior to con-
to be necessary. In 2 recent studies, one involving sidering discharge. Patients with severe hyperten-
2839 patients seen in an ED5 and another involving sion often need medication adjuncts or adjust-
58,535 outpatients38 who presented with significantly ments, and lack of follow-up can lead to repeat
elevated BP levels but no end-organ damage, were visits and detrimental long-term effects.
either observed for a few hours after treatment with • Epistaxis, proteinuria, chronic renal failure, and
oral antihypertensive agents and follow-up versus headaches do not qualify as signs of target end-
follow-up without initiation of oral antihypertensive organ damage.
treatment. These studies demonstrated very low rates Risk Management Caveat: While these findings
of morbidity/mortality, and no significant difference in themselves are not signs of end-organ dam-
in prognosis for those treated acutely, compared with age, they can be ominous signs of other etiolo-
those who were discharged with rapid follow-up. gies and should be addressed accordingly.
• Troponin-I elevation is not associated with in-
creased mortality in hypertensive emergency and
n Summary does not need to be routinely obtained if there is
Hypertensive emergency is associated with substantial no concern for ACS.
morbidity and in-hospital mortality, thus requiring im- Risk Management Caveat: Atypical presenta-
mediate treatment. Patients with severely elevated BP tions of ACS as seen in elderly, female, and
(≥180/110 mm Hg or MAP ≥135 mm Hg) should be diabetic populations should be considered. Other
rapidly assessed for evidence of hypertensive emer- diagnostics such as ECG and bedside ultrasound,
gency to prevent further end-organ damage. Assess- in addition to cardiac risk factors, should be con-
ment should focus on a thorough history and physical sidered when considering the diagnosis of ACS.
examination, with additional testing, as needed, based Troponin-I elevation due to decreased kidney
on clinical features present on evaluation. Hypertensive function, demand ischemia, or chronic heart fail-
emergencies should be managed with careful titration ure should also be considered.
Class of Evidence Definitions
Each action in the clinical pathways section of Emergency Medicine Practice receives a score based on the following definitions.
Class I Class II
• Always acceptable, safe • Safe, acceptable Class III Indeterminate
• Definitely useful • Probably useful • May be acceptable • Continuing area of research
• Proven in both efficacy and effectiveness • Possibly useful • No recommendations until further
Level of Evidence: • Considered optional or alternative research
Level of Evidence: • Generally higher levels of evidence treatments
• One or more large prospective studies • Nonrandomized or retrospective stud- Level of Evidence:
are present (with rare exceptions) ies: historic, cohort, or case control Level of Evidence: • Evidence not available
• High-quality meta-analyses studies • Generally lower or intermediate levels • Higher studies in progress
• Study results consistently positive and • Less robust randomized controlled trials of evidence • Results inconsistent, contradictory
compelling • Results consistently positive • Case series, animal studies, • Results not compelling
consensus panels
• Occasionally positive results
This clinical pathway is intended to supplement, rather than substitute for, professional judgment and may be changed depending upon a patient’s individual
needs. Failure to comply with this pathway does not represent a breach of the standard of care.
Copyright © 2023 EB Medicine. www.ebmedicine.net. No part of this publication may be reproduced in any format without written consent of EB Medicine.
JUNE 2023 • www.ebmedicine.net 18 ©2023 EB MEDICINE
Clinical Pathway for Managing Hypertensive Emergencies
in the Emergency Department
Severe hypertension (MAP ≥135 mm Hg or
SBP ≥180 mm Hg, or DBP ≥110 mm Hg)
Is there evidence of end-organ damage? • No indication for blood pressure
(See Figure 3, BARKH algorithm for NO reduction
list of end-organ damage) • Consider discharge with primary
care follow-up
YES
Is there a potential secondary cause Treat the underlying cause
YES (eg, alcohol withdrawal,
of the hypertension?
uncontrolled pain)
NO
• This is a hypertensive emergency
• Treat the underlying condition
Heart Kidney Arteries Brain/Retina
Acute coronary Aortic dissection: Hypertensive
Acute renal failure:
syndromes: • Esmolol for a goal HR encephalopathy/
• Reduce MAP by a
• IV/SL/topical nitroglycerin <60 beats/min and SBP retinopathy:
maximum of 25% in the
or IV metoprolol (if no risk <120 mm Hg (consider • Reduce MAP by 20%-25%
first hour (Class II)
factors present: age >70, addition of nicardipine if using IV nicardipine or
• Appropriate first-line
HR >110 beats/min, SBP unable to reach BP goal) labetalol as first-line agent
agents include nicardipine,
<120 mm Hg) to achieve (Class II) (Class II)
clevidipine, or labetalol
no more than 25% MAP Severe pre-eclampsia, Intracerebral hemorrhage:
(Class II)
reduction within 1st hour eclampsia, or HELLP: • Lower BP to SBP
(Class II) • Magnesium sulfate at a <140 mm Hg using IV
Acute heart failure: loading dose of 4-6 g IV nicardipine or labetalol
• NIPPV over 20-30 min, followed (Class I)
• Short-term high-dose by a maintenance infusion Acute ischemic stroke:
nitroglycerin titrated down of 1-2 g/hr (Class I) • If receiving thrombolytics
after symptoms relief • BP should be decreased or mechanical
(Class II) to <160/110 mm Hg thrombectomy, lower to
• BP reduction no greater with IV labetalol (or IV goal BP <185/110 mm Hg
than 25% within 1st hour hydralazine if unable to prior to intervention and
(Class II) tolerate labetalol) (Class maintain a BP <180/105
• IV diuretics (2-3 × PO II) mm Hg (Class II)
dose) (Class II) • If no intervention and
BP is ≥220/120 mm Hg,
consider lowering BP by
no more than 15%
(Class II)
Abbreviations: BP, blood pressure; DBP, diastolic blood pressure; HELLP, hemolysis, elevated liver enzymes, low platelets; HR, heart rate; IV, intravenous;
MAP, mean arterial pressure; NIPPV, noninvasive positive-pressure ventilation; PO, orally; SBP, systolic blood pressure; SL, sublingual.
For Class of Evidence definitions, see page 18.
JUNE 2023 • www.ebmedicine.net 19 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
Risk Management Pitfalls for Hypertensive Emergencies
in the Emergency Department
1. “The labs and imaging I ordered should have 6. “At first I treated the systolic pressure,
been enough to tell if there was end-organ but then I realized the diastolic pressure
damage.” Physical examination findings should was way too high.” Not using MAP can
guide the clinician’s decision to obtain advanced cause inconsistencies in treatment and lead to
imaging and laboratory analysis. There are nu- treatment errors. Automated oscillometric BP
merous presenting complaints for patients with cuffs measure the MAP directly. This also allows
severe hypertension, and historical features can for dosing of antihypertensive medications to
be subtle. The more time spent asking the appro- be titrated against a single variable. Attempting
priate questions, such as medication compliance, to titrate antihypertensive infusions with systolic
as well as subtle examination findings as simple and diastolic BPs simultaneously can lead to
as a murmur can help confirm the diagnosis. overshooting your target pressure.
2. “The patient‘s BP was really high; I thought 7. “Metoprolol is a beta blocker just like
it must have been hypertensive emergency.” labetalol.” While metoprolol is a beta blocker,
Severe hypertension is a frequent presenting its beta-1 receptor selectivity acts almost
complaint and referral to the ED. Unfortunately, exclusively as a rate control agent, and it has
overdiagnosis of hypertensive emergency among little vasodilatory effect, unlike labetalol, which is
patients with severe hypertension is common and a nonselective beta blocker that also has alpha
often inaccurate. This can lead to inappropriate antagonist effects. Metoprolol has very little role
admissions as well as harm to patients who do in the treatment of hypertensive emergency.
not have end-organ damage and are started on
parenteral antihypertensive medication. 8. “She was having a hypertensive emergency;
fluids will only make it worse.” Not considering
3. “The patient should be normotensive.” volume depletion as a cause of hypertension
Treating hypertensive emergency too (intravascularly volume-depleted due to renin-
aggressively is just as dangerous as failure to angiotensin system activation and sodium
treat. It is important to remember each patient’s excretion) is a frequent mistake. Using bedside
autoregulatory mechanisms adapt over time ultrasound in conjunction with other examination
and are unique to the individual, thus a normal features and diagnostics (eg, urine output, skin
BP may lead to hypoperfusion in a patient with turgor) to evaluate intravascular volume status
chronically elevated blood pressure. Try to avoid can help to mitigate this issue.
treating a numerical value.
9. “The BP was better after an hour, so I gave
4. “We had difficulty getting IV access, so we him oral medications.” Trying to transition from
started with oral medications.” Using oral, an antihypertensive infusion to an oral agent
intramuscular, or intranasal medications to treat can be dangerous. Treatment of hypertensive
hypertensive emergency is inadvisable, as they emergency should be a gradual and frequently
are not easily titratable. Treatment should consist monitored process over the course of days.
of short-acting, titratable parenteral medications
to avoid treatment errors, dose stacking, and 10. “Why didn’t my middle-aged White female
poor patient outcomes. patient respond like my chronic hypertensive
elderly Black male patient?” Not considering
5. “We needed a second agent to control the age, sex, race, and concomitant conditions when
BP.” There is often more than one compounding deciding on a treatment approach can cause
variable contributing to the patient’s unexpected results. There is substantial evidence
hypertension. Failing to treat pain, agitation, that ethnicity, sex, and age all play a large role in
substance withdrawal, or urinary retention an individual’s response to different medications.
as causes of hypertension will often lead to Consider these factors when choosing an agent
treatment failure. and make dosing adjustments accordingly.
JUNE 2023 • www.ebmedicine.net 20 ©2023 EB MEDICINE
Case Conclusions
For the 62-year-old man who presented by EMS with swelling of his legs and worsening shortness of
breath…
CASE 1
Based on the patient‘s history of congestive heart failure and physical examination, you believed that he
was having acute “flash” pulmonary edema. Point-of-care ultrasound showed bilateral B-lines, and chest
x-ray showed cardiomegaly with pulmonary congestion. He was immediately started on CPAP and given
a high-dose nitroglycerin infusion, with relief of symptoms. The patient was given furosemide IV and was
admitted for further management of his flash pulmonary edema.
For the 76-year-old man with history of diabetes and hypertension who presented with altered
mental status and then started seizing...
CASE 2
He was given IV lorazepam for his seizure, and you ordered a stat CT head, which appeared to be normal.
You performed a bedside ocular ultrasound, which showed evidence of papilledema, raising concern for
cerebral edema. An MRI was obtained, which showed posterior cerebral edema, confirming the diagnosis,
He was treated for PRES with a nicardipine infusion.
For the 59-year-old woman with elevated BP who presented to the ED from her primary care
physician’s office…
You obtained extensive past medical, social, and family history, and found no increased risk factors for
CASE 3
hypertensive emergency. Her review of systems and physical examination, including visual acuity, was
unremarkable. Based on your clinical evaluation, you had very low concern for end-organ damage. Given
her lack of5 significant risk factors and your low level of concern for poor follow-up, you discussed strict
Recommendations
return precautions with
To Apply theinpatient and advised her to follow up with her primary care doctor in the next few
Practice
days for a repeat evaluation.
5 Recommendations
To Apply in Practice
n References
Evidence-based medicine requires a critical appraisal
5 Things
5 That Will Change
Recommendations of the literature based upon study methodology and
Your Practice
To Apply in Practice number of subjects. Not all references are equally
1. Consider using the MAP instead of only the robust. The findings of a large, prospective, random
SBP or DBP when assessing BP. ized, and blinded trial should carry more weight than
a case report.
2. Any patient diagnosed with hypertensive To help the reader judge the strength of each
emergency needs to be started on short- reference, pertinent information about the study will
acting IV antihypertensive medication that be included in bold type following the reference,
allows for titration. where available. In addition, the most informative
references cited in this paper, as determined by the
3. The use of oral antihypertensive medications
authors, will be noted by an asterisk (*) next to the
in the ED to decrease a patient’s BP is a prac-
number of the reference.
tice that may be unnecessary.
4. Patients who do not meet the criteria for 1. Amraoui F, Van Der Hoeven NV, Van Valkengoed IG, et al.
Mortality and cardiovascular risk in patients with a history of
hypertensive emergency may be discharged malignant hypertension: a case-control study. J Clin Hypertens
with outpatient follow-up. Evaluating for (Greenwich). 2014;16(2):122-126. (Comparative study; 240
end-organ damage in asymptomatic patients patients)
does not change ED management or improve 2. Powers WJ, Rabinstein AA, Ackerson T, et al. Guidelines for the
outcomes.38,39 early management of patients with acute ischemic stroke: 2019
update to the 2018 guidelines for the early management of
5. The degree of BP elevation does not always acute ischemic stroke: a guideline for healthcare professionals
correlate with the severity of end-organ dam- from the American Heart Association/American Stroke Associa-
tion. Stroke. 2019;50(12):e344-e418. (Guideline)
age, and may indicate a better prognosis for
3. Sandset EC, Anderson CS, Bath PM, et al. European Stroke
the patient, such as in ACS.83-85
Organisation (ESO) guidelines on blood pressure management
JUNE 2023 • www.ebmedicine.net 21 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
in acute ischaemic stroke and intracerebral haemorrhage. Eur 18. Erbel R, Aboyans V, Boileau C, et al. 2014 ESC guidelines on the
Stroke J. 2021;6(2). (Guideline) diagnosis and treatment of aortic diseases: document covering
4. Qureshi AI, Palesch YY, Foster LD, et al. Blood pressure-at- acute and chronic aortic diseases of the thoracic and abdominal
tained analysis of ATACH 2 trial. Stroke. 2018;49(6):1412-1418. aorta of the adult. The Task Force for the Diagnosis and Treat-
(Prospective study; 1000 patients) ment of Aortic Diseases of the European Society of Cardiology
(ESC). Eur Heart J. 2014;35(41):2873-2926. (Guideline)
5. Anderson CS, Heeley E, Huang Y, et al. Rapid blood-pressure
lowering in patients with acute intracerebral hemorrhage. N 19. Isselbacher EM, Preventza O, Hamilton Black J 3rd, et al. 2022
Engl J Med. 2013;368(25):2355-2365. (Prospective study; ACC/AHA guideline for the diagnosis and management of aor-
2839 patients) tic disease: a report of the American Heart Association/Ameri-
can College of Cardiology Joint Committee on Clinical Practice
6. Anderson CS, Huang Y, Lindley RI, et al. Intensive blood
Guidelines. Circulation. 2022;146(24):e334-e482. (Guideline)
pressure reduction with intravenous thrombolysis therapy for
acute ischaemic stroke (ENCHANTED): an international, ran- 20. No authors listed. Gestational hypertension and preeclampsia:
domised, open-label, blinded-endpoint, phase 3 trial. Lancet. ACOG Practice Bulletin, Number 222. Obstet Gynecol.
2019;393(10174):877-888. (Prospective study; 2196 patients) 2020;135(6):e237-e260. (Guideline)
7. Amsterdam EA, Wenger NK, Brindis RG, et al. 2014 AHA/ 21. Katz JN, Gore JM, Amin A, et al. Practice patterns, outcomes,
ACC guideline for the management of patients with non-ST- and end-organ dysfunction for patients with acute severe hy-
elevation acute coronary syndromes: executive summary: a pertension: the Studying the Treatment of Acute hyperTension
report of the American College of Cardiology/American Heart (STAT) registry. Am Heart J. 2009;158(4):599-606. (Retrospec-
Association Task Force on Practice Guidelines. Circulation. tive study; 1588 patients)
2014;130(25):2354-2394. (Guideline) 22. Aggarwal M, Khan IA. Hypertensive crisis: hypertensive
8. Collet JP, Thiele H, Barbato E, et al. 2020 ESC Guidelines for emergencies and urgencies. Cardiol Clin. 2006;24(1):135-146.
the management of acute coronary syndromes in patients (Review)
presenting without persistent ST-segment elevation. Eur Heart 23. Vaughan CJ, Delanty N. Hypertensive emergencies. Lancet.
J. 2021;42(14):1289-1367. (Guideline) 2000;356(9227):411-417. (Review)
9. Rosendorff C, Lackland DT, Allison M, et al. Treatment of hy- 24. Derhaschnig U, Testori C, Riedmueller E, et al. Hypertensive
pertension in patients with coronary artery disease: a scientific emergencies are associated with elevated markers of inflamma-
statement from the American Heart Association, American tion, coagulation, platelet activation and fibrinolysis. J Hum Hy-
College of Cardiology, and American Society of Hypertension. pertens. 2013;27(6):368-373. (Prospective study; 60 patients)
J Am Soc Hypertens. 2015;9(6):453-498. (Guideline) 25. Marik PE, Rivera R. Hypertensive emergencies: an update. Curr
10. Ibanez B, James S, Agewall S, et al. 2017 ESC guidelines for Opin Crit Care. 2011;17(6):569-580. (Review)
the management of acute myocardial infarction in patients 26. Williams B, Mancia G, Spiering W, et al. 2018 ESC/ESH guide-
presenting with ST-segment elevation: the Task Force for the lines for the management of arterial hypertension. Eur Heart J.
Management of Acute Myocardial Infarction in Patients Pre- 2018;39(33):3021-3104. (Guidelines)
senting with ST-segment Elevation of the European Society of
27. van den Born BJ, Koopmans RP, Groeneveld JO, et al. Ethnic
Cardiology (ESC). Eur Heart J. 2018;39(2):119-177. (Guideline)
disparities in the incidence, presentation and complications of
11. Whelton PK, Carey RM, Aronow WS, et al. 2017 ACC/AHA/ malignant hypertension. J Hypertens. 2006;24(11):2299-2304.
AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guide- (Retrospective cohort study; 122 patients)
line for the prevention, detection, evaluation, and management
28. Kobayashi A, Czlonkowska A, Ford GA, et al. European Acade-
of high blood pressure in adults: executive summary: a report of
my of Neurology and European Stroke Organization consensus
the American College of Cardiology/American Heart Associa-
statement and practical guidance for pre-hospital management
tion Task Force on Clinical Practice Guidelines. Hypertension.
of stroke. Eur J Neurol. 2018;25(3):425-433. (Guideline)
2018;71(6):1269-1324. (Guideline)
29. Henrikson CA, Howell EE, Bush DE, et al. Chest pain relief by
12. van den Born BH, Lip GYH, Brguljan-Hitij J, et al. ESC Council
nitroglycerin does not predict active coronary artery disease.
on Hypertension position document on the management of hy-
Ann Intern Med. 2003;139(12):979-986. (Prospective study;
pertensive emergencies. Eur Heart J Cardiovasc Pharmacother.
459 patients)
2019;5(1):37-46. (Guideline)
30. Unger T, Borghi C, Charchar F, et al. 2020 International Society
13. Starr JB, Tirschwell DL, Becker KJ. Labetalol use is associated
of Hypertension global hypertension practice guidelines. Hy-
with increased in-hospital infection compared with nicardipine
pertension. 2020;75(6):1334-1357. (Guideline)
use in intracerebral hemorrhage. Stroke. 2017;48(10):2693-
2698. (Prospective; 525 patients) 31. Benenson I, Waldron FA, Jadotte YT, et al. Risk factors for hy-
pertensive crisis in adult patients: a systematic review. JBI Evid
14. Hecht JP, Richards PG. Continuous-infusion labetalol vs
Synth. 2021;19(6):1292-1327. (Systematic review; 19 studies)
nicardipine for hypertension management in stroke patients. J
Stroke Cerebrovasc Dis. 2018;27(2):460-465. (Retrospective; 32. Szczech LA, Granger CB, Dasta JF, et al. Acute kidney injury
99 patients) and cardiovascular outcomes in acute severe hypertension.
Circulation. 2010;121(20):2183-2191. (Retrospective cohort
15. El-Ghoroury H, Sudekum DM, Hecht JP. Blood pressure control
study; 1982 patients)
in acute stroke: labetalol or nicardipine? J Stroke Cerebrovasc
Dis. 2021;30(9):105959. (Retrospective; 3093 patients) 33. Jolly H, Freel EM, Isles C. Management of hypertensive
emergencies and urgencies: narrative review. Postgrad Med J.
16. Liu-DeRyke X, Levy PD, Parker D Jr, et al. A prospective
2021;Oct 20;postgradmedj-2021-140899. (Review)
evaluation of labetalol versus nicardipine for blood pressure
management in patients with acute stroke. Neurocrit Care. 34. Stevens SL, Wood S, Koshiaris C, et al. Blood pressure variability
2013;19(1):41-47. (Prospective study; 54 patients) and cardiovascular disease: systematic review and meta-analysis.
BMJ. 2016;354:i4098. (Meta-analysis; 41 studies)
17. Ortega-Gutierrez S, Thomas J, Reccius A, et al. Effectiveness
and safety of nicardipine and labetalol infusion for blood 35. Melgarejo JD, Yang WY, Thijs L, et al. Association of fatal and
pressure management in patients with intracerebral and nonfatal cardiovascular outcomes with 24-hour mean arterial
subarachnoid hemorrhage. Neurocrit Care. 2013;18(1):13-19. pressure. Hypertension. 2021;77(1):39-48. (Prospective cohort;
(Retrospective; 81 patients) 11,596 patients)
36. Astarita A, Covella M, Vallelonga F, et al. Hypertensive emer-
JUNE 2023 • www.ebmedicine.net 22 ©2023 EB MEDICINE
gencies and urgencies in emergency departments: a systematic for the diagnosis and treatment of acute and chronic heart
review and meta-analysis. J Hypertens. 2020;38(7):1203-1210. failure. Eur Heart J. 2021;42(36):3599-3726. (Guideline)
(Systematic review; 8 studies, 1970 hypertensive emergen- 52.* Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/
cies, 4983 hypertensive urgencies) HFSA guideline for the management of heart failure: a report of
37. Immink RV, van den Born BJ, van Montfrans GA, et al. Impaired the American College of Cardiology/American Heart Associa-
cerebral autoregulation in patients with malignant hyperten- tion Joint Committee on Clinical Practice Guidelines. Circula-
sion. Circulation. 2004;110(15):2241-2245. (Prospective; 8 tion. 2022;145(18):e1033. (Guideline)
patients) DOI: 10.1161/CIR.0000000000001062
38. Patel KK, Young L, Howell EH, et al. Characteristics and 53. Wakai A, McCabe A, Kidney R, et al. Nitrates for acute
outcomes of patients presenting with hypertensive urgency heart failure syndromes. Cochrane Database Syst Rev.
in the office setting. JAMA Intern Med. 2016;176(7):981-988. 2013;2013(8):CD005151. (Review)
(Retrospective cohort study; 58,535 patients) 54. Alexander P, Alkhawam L, Curry J, et al. Lack of evidence for
39. Karras DJ, Kruus LK, Cienki JJ, et al. Utility of routine testing for intravenous vasodilators in ED patients with acute heart failure:
patients with asymptomatic severe blood pressure elevation in a systematic review. Am J Emerg Med. 2015;33(2):133-141.
the emergency department. Ann Emerg Med. 2008;51(3):231- (Review)
239. (Prospective observational study; 109 patients) 55. Ho EC, Parker JD, Austin PC, et al. Impact of nitrate use on sur-
40. McAlister FA, Youngson E, Rowe BH. Elevated blood pres- vival in acute heart failure: a propensity-matched analysis. J Am
sures are common in the emergency department but are they Heart Assoc. 2016;5(2). (Retrospective study; 11,078 patients)
important? A retrospective cohort study of 30,278 adults. Ann 56. Kozhuharov N, Goudev A, Flores D, et al. Effect of a strategy
Emerg Med. 2021;77(4):425-432. (Retrospective cohort study; of comprehensive vasodilation vs usual care on mortality
30,278 patients) and heart failure rehospitalization among patients with acute
41. Kim W, Kim BS, Kim HJ, et al. Clinical implications of cardiac heart failure: the GALACTIC randomized clinical trial. JAMA.
troponin-I in patients with hypertensive crisis visiting the emer- 2019;322(23):2292-2302. (Prospective study; 788 patients)
gency department. Ann Med. 2022;54(1):507-515. (Observa- 57. Mathew R, Kumar A, Sahu A, et al. High-dose nitroglycerin
tional study; 3938 patients) bolus for sympathetic crashing acute pulmonary edema:
42. Bacharova L, Schocken D, Estes EH, et al. The role of ECG in a prospective observational pilot study. J Emerg Med.
the diagnosis of left ventricular hypertrophy. Curr Cardiol Rev. 2021;61(3):271-277. (Prospective study; 25 patients)
2014;10(3):257-261. (Review) 58. Wang K, Samai K. Role of high-dose intravenous nitrates
43. Okin PM, Devereux RB, Nieminen MS, et al. Relationship of the in hypertensive acute heart failure. Am J Emerg Med.
electrocardiographic strain pattern to left ventricular structure 2020;38(1):132-137. (Review)
and function in hypertensive patients: the LIFE study. Losartan 59. Wilson SS, Kwiatkowski GM, Millis SR, et al. Use of nitroglycerin
Intervention For End point. J Am Coll Cardiol. 2001;38(2):514- by bolus prevents intensive care unit admission in patients
520. (Retrospective cohort study; 886 participants) with acute hypertensive heart failure. Am J Emerg Med.
44. Fugate JE, Rabinstein AA. Posterior reversible encepha- 2017;35(1):126-131. (Retrospective; 395 patients)
lopathy syndrome: clinical and radiological manifestations, 60. Peacock WF, Chandra A, Char D, et al. Clevidipine in acute
pathophysiology, and outstanding questions. Lancet Neurol. heart failure: results of the a study of blood pressure control
2015;14(9):914-925. (Review) in acute heart failure-a pilot study (PRONTO). Am Heart J.
45. Ohle R, McIsaac SM, Woo MY, et al. Sonography of the optic 2014;167(4):529-536. (Prospective study; 104 patients)
nerve sheath diameter for detection of raised intracranial pres- 61. Peacock FW 4th, Varon J, Ebrahimi R, et al. Clevidipine for
sure compared to computed tomography: a systematic review severe hypertension in acute heart failure: a VELOCITY trial
and meta-analysis. J Ultrasound Med. 2015;34(7):1285-1294. analysis. Congest Heart Fail. 2010;16(2):55-59. (Prospective
(Literature review; 45 studies) study; 126 patients)
46. Perry JJ, Stiell IG, Sivilotti ML, et al. Sensitivity of computed 62. Kaesemeyer W, Suvorava T. Nitric oxide is the cause of
tomography performed within six hours of onset of headache nitroglycerin tolerance: providing an old dog new tricks
for diagnosis of subarachnoid haemorrhage: prospective cohort for acute heart failure. J Cardiovasc Pharmacol Ther.
study. BMJ. 2011;343:d4277. (Prospective cohort study; 3132 2022;27:10742484221086091. (Review)
patients in 11 tertiary care EDs)
63. Koroki T, Abe T, Ochiai H. Nicardipine versus nitroglycerin for
47. Connolly ES Jr, Rabinstein AA, Carhuapoma JR, et al. Guide- hypertensive acute heart failure syndrome: a single-center ob-
lines for the management of aneurysmal subarachnoid servational study. J Rural Med. 2022;17(1):33-39. (Retrospec-
hemorrhage: a guideline for healthcare professionals from tive, observational study; 58 patients)
the American Heart Association/American Stroke Association.
64. Shi J, Li Y, Xing C, et al. Urapidil, compared to nitroglycerin, has
Stroke. 2012;43(6):1711-1737. (Guideline)
better clinical safety in the treatment of hypertensive patients
48. Matsue Y, Damman K, Voors AA, et al. Time-to-furosemide with acute heart failure: a meta-analysis. Drug Des Devel Ther.
treatment and mortality in patients hospitalized with acute heart 2019;13:161-172. (Literature review; 7 studies)
failure. J Am Coll Cardiol. 2017;69(25):3042-3051. (Prospective
65.* Peacock WF, Hollander JE, Diercks DB, et al. Morphine and
study; 1291 patients)
outcomes in acute decompensated heart failure: an ADHERE
49. Ouwerkerk W, Tromp J, Cleland JGF, et al. Association of time- analysis. Emerg Med J. 2008;25(4):205-209. (Retrospective
to-intravenous furosemide with mortality in acute heart failure: study; 147,362 patients) DOI: 10.1136/emj.2007.050419
data from REPORT-HF. Eur J Heart Fail. 2023;25(1):43-51.
66. Miró Ò, Gil V, Martín-Sánchez FJ, et al. Morphine use in the ED
(Prospective study; 15,078 patients)
and outcomes of patients with acute heart failure: a propensity
50. Miró Ò, Harjola P, Rossello X, et al. The FAST-FURO study: effect score-matching analysis based on the EAHFE registry. Chest.
of very early administration of intravenous furosemide in the 2017;152(4):821-832. (Prospective study; 6516 patients)
prehospital setting to patients with acute heart failure attending
67. O’Connor CM, Starling RC, Hernandez AF, et al. Effect of
the emergency department. Eur Heart J Acute Cardiovasc Care.
nesiritide in patients with acute decompensated heart failure.
2021;10(5):487-496. (Prospective study; 12,595 patients)
N Engl J Med. 2011;365(1):32-43. (Randomized double-blind,
51. McDonagh TA, Metra M, Adamo M, et al. 2021 ESC guidelines placebo-controlled trial; 7007 patients)
JUNE 2023 • www.ebmedicine.net 23 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
68. Kitai T, Tang WHW, Xanthopoulos A, et al. Impact of early presenting blood pressure in non-ST-segment elevation acute
treatment with intravenous vasodilators and blood pressure re- coronary syndrome in relation to prior history of hyperten-
duction in acute heart failure. Open Heart. 2018;5(2):e000845. sion. Am Heart J. 2013;166(4):716-722. (Retrospective study;
(Prospective study; 1670 patients) 10,337 patients)
69. Minhas JS, Wang X, Lindley RI, et al. Comparative effects of 84. Pei J, Wang X, Xing Z, et al. Association between admission
intensive-blood pressure versus standard-blood pressure-low- systolic blood pressure and major adverse cardiovascular
ering treatment in patients with severe ischemic stroke in the events in patients with acute myocardial infarction. PLoS One.
ENCHANTED trial. J Hypertens. 2021;39(2):280-285. (Prospec- 2020;15(6):e0234935. (Prospective study; 21,364 patients)
tive study; 1311 patients) 85. Park JS, Cha KS, Shin D, et al. Prognostic significance of pre-
70. Malhotra K, Goyal N, Katsanos AH, et al. Association of blood senting blood pressure in patients with ST-elevation myocardial
pressure with outcomes in acute stroke thrombectomy. Hyper- infarction undergoing percutaneous coronary intervention.
tension. 2020;75(3):730-739. (Literature review; 25 studies) Am J Hypertens. 2015;28(6):797-805. (Retrospective study;
71. Mistry EA, Sucharew H, Mistry AM, et al. Blood pressure after 11,292 patients)
endovascular therapy for ischemic stroke (BEST): a multicenter 86. Roolvink V, Ibáñez B, Ottervanger JP, et al. Early intravenous
prospective cohort study. Stroke. 2019;50(12):3449-3455. (Pro- beta-blockers in patients with ST-segment elevation myocardial
spective study; 385 patients) infarction before primary percutaneous coronary intervention.
72. Ahmed N, Wahlgren N, Brainin M, et al. Relationship of blood J Am Coll Cardiol. 2016;67(23):2705-2715. (Prospective; 683
pressure, antihypertensive therapy, and outcome in ischemic patients)
stroke treated with intravenous thrombolysis: retrospective 87. Chen ZM, Pan HC, Chen YP, et al. Early intravenous then oral
analysis from Safe Implementation of Thrombolysis in Stroke- metoprolol in 45,852 patients with acute myocardial infarction:
International Stroke Thrombolysis Register (SITS-ISTR). Stroke. randomised placebo-controlled trial. Lancet. 2005;366(9497):1622-
2009;40(7):2442-2449. (Retrospective study) 1632. (Prospective study; 45,852 patients)
73. Tsivgoulis G, Katsanos AH, Mandava P, et al. Blood pres- 88. O’Gara PT, Kushner FG, Ascheim DD, et al. 2013 ACCF/AHA
sure excursions in acute ischemic stroke patients treated with guideline for the management of ST-elevation myocardial
intravenous thrombolysis. J Hypertens. 2021;39(2):266-272. infarction: a report of the American College of Cardiology
(Retrospective study) Foundation/American Heart Association Task Force on Practice
74. Berge E, Cohen G, Lindley RI, et al. Effects of blood pressure Guidelines. Circulation. 2013;127(4):e362-e425. (Guideline)
and blood pressure-lowering treatment during the first 24 89. Safi S, Sethi NJ, Nielsen EE, et al. Beta-blockers for suspected
hours among patients in the Third International Stroke Trial or diagnosed acute myocardial infarction. Cochrane Database
of Thrombolytic Treatment for Acute Ischemic Stroke. Stroke. Syst Rev. 2019;12(12):CD012484. (Cochrane review; 63 trials)
2015;46(12):3362-3369. (Prospective study; 3035 patients) 90.* Perez MI, Musini VM, Wright JM. Effect of early treatment with
75. Lees KR, Emberson J, Blackwell L, et al. Effects of alteplase anti-hypertensive drugs on short and long-term mortality in pa-
for acute stroke on the distribution of functional outcomes: a tients with an acute cardiovascular event. Cochrane Database
pooled analysis of 9 trials. Stroke. 2016;47(9):2373-2379. (Lit- Syst Rev. 2009(4):CD006743. (Cochrane review; 65 RCTs)
erature review; 9 studies) DOI: 10.1002/14651858.CD006743.pub2
76. Saver JL, Goyal M, van der Lugt A, et al. Time to treatment 91. Sakamoto Y, Koga M, Yamagami H, et al. Systolic blood pres-
with endovascular thrombectomy and outcomes from ischemic sure after intravenous antihypertensive treatment and clini-
stroke: a meta-analysis. JAMA. 2016;316(12):1279-1288. (Lit- cal outcomes in hyperacute intracerebral hemorrhage: the
erature review; 28 studies) stroke acute management with urgent risk-factor assessment
77. Bangalore S, Schwamm L, Smith EE, et al. Blood pressure and and improvement-intracerebral hemorrhage study. Stroke.
in-hospital outcomes in patients presenting with ischaemic 2013;44(7):1846-1851. (Prospective study; 211 patients)
stroke. Eur Heart J. 2017;38(37):2827-2835. (Retrospective 92. Greenberg SM, Ziai WC, Cordonnier C, et al. 2022 guideline
study; 309,611 patients) for the management of patients with spontaneous intracerebral
78. Leonardi-Bee J, Bath PM, Phillips SJ, et al. Blood pressure hemorrhage: a guideline from the American Heart Association/
and clinical outcomes in the International Stroke Trial. Stroke. American Stroke Association. Stroke. 2022;53(7):e282-e361.
2002;33(5):1315-1320. (Retrospective study; 17,398 patients) (Guideline)
79. Vemmos KN, Tsivgoulis G, Spengos K, et al. U-shaped rela- 93.* Qureshi AI, Palesch YY, Barsan WG, et al. Intensive blood-
tionship between mortality and admission blood pressure in pressure lowering in patients with acute cerebral hemorrhage.
patients with acute stroke. J Intern Med. 2004;255(2):257-265. N Engl J Med. 2016;375(11):1033-1043. (Prospective study;
(Retrospective study; 1121 patients) 1000 patients) DOI: 10.1056/NEJMoa1603460
80. Leira R, Millán M, Díez-Tejedor E, et al. Age determines the 94. Moullaali TJ, Wang X, Martin RH, et al. Blood pressure control
effects of blood pressure lowering during the acute phase of and clinical outcomes in acute intracerebral haemorrhage:
ischemic stroke: the TICA study. Hypertension. 2009;54(4):769- a preplanned pooled analysis of individual participant data.
774. (Retrospective study; 1092 patients) Lancet Neurol. 2019;18(9):857-864. (Prospective study; 3829
patients)
81. Morrow DA, Antman EM, Charlesworth A, et al. TIMI risk score
for ST-elevation myocardial infarction: a convenient, bedside, 95. Manning L, Hirakawa Y, Arima H, et al. Blood pressure variability
clinical score for risk assessment at presentation: an intrave- and outcome after acute intracerebral haemorrhage: a post-hoc
nous nPA for treatment of infarcting myocardium early II trial analysis of INTERACT2, a randomised controlled trial. Lancet
substudy. Circulation. 2000;102(17):2031-2037. (Prospective Neurol. 2014;13(4):364-373. (Retrospective study)
study; 14,114 patients) 96. Mayer SA, Kurtz P, Wyman A, et al. Clinical practices, complica-
82. Fox KA, Dabbous OH, Goldberg RJ, et al. Prediction of risk of tions, and mortality in neurological patients with acute severe
death and myocardial infarction in the six months after presen- hypertension: the studying the treatment of acute hypertension
tation with acute coronary syndrome: prospective multinational registry. Crit Care Med. 2011;39(10):2330-2336. (Multicenter
observational study (GRACE). BMJ. 2006;333(7578):1091. prospective study; 432 patients)
(Prospective study; 43,810 patients) 97. Allison TA, Bowman S, Gulbis B, et al. Comparison of
83. Lee D, Goodman SG, Fox KA, et al. Prognostic significance of clevidipine and nicardipine for acute blood pressure reduction
in patients with stroke. J Intensive Care Med. 2019;34(11-
JUNE 2023 • www.ebmedicine.net 24 ©2023 EB MEDICINE
12):990-995. (Retrospective cohort; 210 patients) al. Magnesium sulphate and other anticonvulsants for
98. Graffagnino C, Bergese S, Love J, et al. Clevidipine rapidly and women with pre-eclampsia. Cochrane Database Syst Rev.
safely reduces blood pressure in acute intracerebral hemor- 2010;2010(11):CD000025. (Cochrane review; 15 trials)
rhage: the ACCELERATE trial. Cerebrovasc Dis. 2013;36(3):173- 116. Okusanya BO, Oladapo OT, Long Q, et al. Clinical
180. (Prospective cohort; 35 patients) pharmacokinetic properties of magnesium sulphate in women
99. Steiner T, Juvela S, Unterberg A, et al. European Stroke with pre-eclampsia and eclampsia. BJOG. 2016;123(3):356-366.
Organization guidelines for the management of intracranial (Literature review; 28 studies)
aneurysms and subarachnoid haemorrhage. Cerebrovasc Dis. 117. Khwaja A. KDIGO clinical practice guidelines for acute kidney
2013;35(2):93-112. (Guideline) injury. Nephron Clin Pract. 2012;120(4):c179-c184. (Guideline)
100. Diringer MN, Bleck TP, Claude Hemphill J 3rd, et al. Criti- 118. Wolf SJ, Lo B, Shih RD, et al. Clinical policy: critical issues in the
cal care management of patients following aneurysmal evaluation and management of adult patients in the emergency
subarachnoid hemorrhage: recommendations from the department with asymptomatic elevated blood pressure. Ann
Neurocritical Care Society’s Multidisciplinary Consensus Confer- Emerg Med. 2013;62(1):59-68. (Clinical policy)
ence. Neurocrit Care. 2011;15(2):211-240. (Guideline) 119. McCord J, Jneid H, Hollander JE, et al. Management of
101. Tang C, Zhang TS, Zhou LF. Risk factors for rebleeding of aneu- cocaine-associated chest pain and myocardial infarction: a
rysmal subarachnoid hemorrhage: a meta-analysis. PLoS One. scientific statement from the American Heart Association Acute
2014;9(6):e99536. (Literature review; 14 studies) Cardiac Care Committee of the Council on Clinical Cardiology.
102. Maagaard M, Karlsson WK, Ovesen C, et al. Interventions for al- Circulation. 2008;117(14):1897-1907. (Review)
tering blood pressure in people with acute subarachnoid haem- 120. Anderson JL, Adams CD, Antman EM, et al. ACC/AHA 2007
orrhage. Cochrane Database Syst Rev. 2021;11(11):CD013096. guidelines for the management of patients with unstable
(Cochrane review; 3 studies) angina/non ST-elevation myocardial infarction: a report of the
103. Mussa FF, Horton JD, Moridzadeh R, et al. Acute aortic dis- American College of Cardiology/American Heart Association
section and intramural hematoma: a systematic review. JAMA. Task Force on Practice Guidelines (Writing Committee to Revise
2016;316(7):754-763. (Review) the 2002 Guidelines for the Management of Patients With Un-
stable Angina/Non ST-Elevation Myocardial Infarction): devel-
104. Kumar KU, Zhao Q, Bai X, et al. Controlled heart rate and blood
oped in collaboration with the American College of Emergency
pressure reduce the life threatening aortic events and increase
Physicians, the Society for Cardiovascular Angiography and
survival in patients with type B aortic dissection: a single center
Interventions, and the Society of Thoracic Surgeons: endorsed
experience. Int J Cardiol Heart Vasc. 2015;8:73-74. (Retrospec-
by the American Association of Cardiovascular and Pulmonary
tive cohort study; 193 patients)
Rehabilitation and the Society for Academic Emergency Medi-
105. Miller JB, Suchdev K, Jayaprakash N, et al. New develop- cine. Circulation. 2007;116(7):e148-e304. (Guideline)
ments in hypertensive encephalopathy. Curr Hypertens Rep.
121. Richards JR, Garber D, Laurin EG, et al. Treatment of cocaine
2018;20(2):13. (Review)
cardiovascular toxicity: a systematic review. Clin Toxicol (Phila).
106. Rabinstein AA, Mandrekar J, Merrell R, et al. Blood pressure 2016;54(5):345-364. (Review)
fluctuations in posterior reversible encephalopathy syndrome.
122. Fanari Z, Kennedy KK, Lim MJ, et al. Comparison of in-hospital
J Stroke Cerebrovasc Dis. 2012;21(4):254-258. (Retrospective
outcomes for beta-blocker use versus non-beta blocker use in
study; 50 patients)
patients presenting with cocaine-associated chest pain. Am J
107. Regitz-Zagrosek V, Roos-Hesselink JW, Bauersachs J, et al. 2018 Cardiol. 2014;113(11):1802-1806. (Retrospective study; 376
ESC guidelines for the management of cardiovascular diseases dur- patients)
ing pregnancy. Eur Heart J. 2018;39(34):3165-3241. (Guideline)
108. Elliott WJ, Varon J. Drugs used for the treatment of hyperten-
sive emergencies. UpToDate. Accessed May 10, 2023. https:// n CME Questions
tinyurl.com/3trkhv663 (Online medical reference)
Current subscribers receive CME credit
109. Duley L, Meher S, Jones L. Drugs for treatment of very high
absolutely free by completing the
blood pressure during pregnancy. Cochrane Database Syst Rev.
2013;2013(7):CD001449. (Cochrane review; 35 trials, 3573 following test. Each issue includes 4 AMA
patients) PRA Category 1 CreditsTM, 4 ACEP
110. Magee LA, Cham C, Waterman EJ, et al. Hydralazine for treat- Category I credits, 4 AAFP Prescribed
ment of severe hypertension in pregnancy: meta-analysis. BMJ. credits, or 4 AOA Category 2-A or 2-B credits.
2003;327(7421):955-960. (Meta-analysis; 21 trials) Online testing is available for current and archived
111. Nij Bijvank SW, Duvekot JJ. Nicardipine for the treatment of issues. To receive your free CME credits for this
severe hypertension in pregnancy: a review of the literature. issue, scan the QR code below with your
Obstet Gynecol Surv. 2010;65(5):341-347. (Review)
smartphone or visit www.ebmedicine.net/0623
112. Qi H, Qin J, Ren L, et al. Efficacy of low-dose nicardipine for
emergent treatment of severe postpartum hypertension in
maternal intensive care units: an observational study. Pregnancy
Hypertens. 2020;21:43-49. (Observational study)
113. Committee on Obstetric Practice. Committee Opinion No.
692: Emergent therapy for acute-onset, severe hypertension
during pregnancy and the postpartum period. Obstet Gynecol.
2017;129(4):e90-e95. (Review)
114. Altman D, Carroli G, Duley L, et al. Do women with pre-eclamp-
sia, and their babies, benefit from magnesium sulphate? The
Magpie Trial: a randomised placebo-controlled trial. Lancet.
2002;359(9321):1877-1890. (Retrospective study; 10,110
patients)
115. Duley L, Gülmezoglu AM, Henderson-Smart DJ, et
JUNE 2023 • www.ebmedicine.net 25 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
1. When administering nitroglycerin, which of the 6. A 47-year-old man presents with a severe,
following medications would cause concern if sudden, and unrelenting headache for 3 hours.
it had been taken earlier that day? He denies a previous history of headaches. His
a. Amlodipine BP is 210/110 mm Hg. What is the best next
b. Lisinopril step to diagnose the patient’s condition?
c. Tamsulosin a. Lumbar puncture
d. Sildenafil b. Noncontrast head CT
c. Cerebral angiography
2. A 70-year-old man with a history of diabetes d. Brain MRI
and coronary artery disease presents from his
primary care provider for high blood pressure 7. A patient presents with an acute ischemic
(BP). On examination, he is noted to have a stroke and qualifies for thrombolysis. Prior
BP of 180/110 mm Hg. Which of the following to administering thrombolytics, which of the
symptoms would be least likely to contribute following should be done?
to a diagnosis of hypertensive emergency? a. Maintain BP >200 mm Hg
a. Vision changes b. Initiate a heparin infusion
b. Chest pain c. Reduce BP to <185/110 mm Hg and maintain
c. Headache BP <180/105 mm Hg
d. Oliguria d. Perform mechanical thrombectomy
3. A 56-year-old man with no previous seizure 8. A patient with acute ischemic stroke and
history presents after sustaining a tonic-clonic BP of 226/125 mm Hg is not a candidate
seizure. He is post ictal but protecting his air- for antithrombotic agents or mechanical
way. His past medical history is significant for thrombectomy. What do the AHA/ASA and
a new diagnosis of colon cancer for which he ESO guidelines say is a reasonable BP recom-
just started immunotherapy. His BP is 200/115 mendation?
mm Hg. Which diagnostic study confirms pos- a. Reduce the BP by no more than 15%
terior reversible encephalopathy syndrome? b. Reduce the SBP to <140 mm Hg
a. Ocular ultrasound c. Reduce the SBP to <130 mm Hg
b. Fundoscopy d. There is no reason to reduce the BP if he is
c. Magnetic resonance imaging (MRI) not receiving any intervention
d. Electroencephalogram
9. A patient presents with hypertensive
4. A 58-year-old man with no past medical history emergency and acute coronary syndrome.
presents to the ED with poison ivy rash. His Which of the following may be a risk factor for
BP is 185/110 mm Hg. Review of systems increased development of cardiogenic shock
is negative, and his workup is negative for when administering IV beta blockers?
evidence of end-organ damage. Which of the a. Heart rate <110 beats/min
following is the most appropriate disposition? b. Age <70 years
a. Obtain a head CT c. SBP >120 mm Hg
b. Admit to the progressive care unit on a d. Acute pulmonary edema
nicardipine infusion
c. Initiate 2 antihypertensives and admit to the 10. A 25-year-old woman is 35 weeks‘ pregnant
general medical floor and presents with a BP of 175/99 mm Hg
d. Discharge home with close primary care and pre-eclampsia with severe symptoms.
follow-up According to the American College of
Obstetricians and Gynecologists guidelines,
5. Which of the following medications has which of the following medications should be
been shown to be significantly more likely initiated immediately?
to cause hypotension in patients with acute a. Oral captopril
decompensated heart failure? b. Oral metoprolol
a. Clevidipine c. IV labetalol
b. Nitroglycerine d. IV esmolol
c. Nesiritide
d. Nicardipine
JUNE 2023 • www.ebmedicine.net 26 ©2023 EB MEDICINE
The Emergency Medicine Practice Editorial Board
EDITOR-IN-CHIEF
Andy Jagoda, MD, FACEP Daniel J. Egan, MD Charles V. Pollack Jr., MA, MD, CRITICAL CARE EDITORS
Professor and Chair Emeritus, Harvard Affiliated Emergency FACEP, FAAEM, FAHA, FACC, William A. Knight IV, MD,
Department of Emergency Medicine Residency, FESC FACEP, FNCS
Medicine; Director, Center for Massachusetts General Hospital/ Clinician-Scientist, Department Associate Professor of
Emergency Medicine Education Brigham and Women's Hospital, of Emergency Medicine, Emergency Medicine and
and Research, Icahn School of Boston, MA University of Mississippi School Neurosurgery, Medical Director,
Medicine at Mount Sinai, New of Medicine, Jackson MS
Marie-Carmelle Elie, MD EM Advanced Practice Provider
York, NY
Professor and Chair, Department Ali S. Raja, MD, MBA, MPH Program; Associate Medical
ASSOCIATE EDITOR-IN-CHIEF of Emergency Medicine Executive Vice Chair, Emergency Director, Neuroscience ICU,
Kaushal Shah, MD, FACEP University of Alabama at Medicine, Massachusetts General University of Cincinnati,
Assistant Dean of Academic Birmingham, Birmingham, AL Hospital; Professor of Emergency Cincinnati, OH
Advising, Vice Chair of Medicine and Radiology, Harvard Scott D. Weingart, MD, FCCM
Nicholas Genes, MD, PhD
Education, Professor of Medical School, Boston, MA Editor-in-Chief, emCrit.org
Clinical Assistant Professor,
Clinical Emergency Medicine, Ronald O. Perelman Department Robert L. Rogers, MD, FACEP, PHARMACOLOGY EDITOR
Department of Emergency of Emergency Medicine, NYU FAAEM, FACP
Medicine, Weill Cornell School of Grossman School of Medicine, Assistant Professor of Emergency Aimee Mishler, PharmD, BCPS
Medicine, New York, NY New York, NY Medicine, The University of Emergency Medicine Pharmacist,
Maryland School of Medicine, St. Luke's Health System,
EDITORIAL BOARD Michael A. Gibbs, MD, FACEP
Baltimore, MD Boise, ID
Saadia Akhtar, MD, FACEP Professor and Chair, Department
RESEARCH EDITOR
Associate Professor, Department of Emergency Medicine, Alfred Sacchetti, MD, FACEP
of Emergency Medicine, Carolinas Medical Center, Assistant Clinical Professor, Joseph D. Toscano, MD
Associate Dean for Graduate University of North Carolina Department of Emergency Chief, Department of Emergency
Medical Education, Program School of Medicine, Medicine, Thomas Jefferson Medicine, San Ramon Regional
Director, Emergency Medicine Chapel Hill, NC University, Philadelphia, PA Medical Center, San Ramon, CA
Residency, Mount Sinai Beth Steven A. Godwin, MD, FACEP Robert Schiller, MD INTERNATIONAL EDITORS
Israel, New York, NY Professor and Chair, Department Chair, Department of Family Peter Cameron, MD
William J. Brady, MD of Emergency Medicine, Medicine, Beth Israel Medical Academic Director, The Alfred
Professor of Emergency Assistant Dean, Simulation Center; Senior Faculty, Family Emergency and Trauma Centre,
Medicine and Medicine; Education, University of Medicine and Community Monash University, Melbourne,
Medical Director, Emergency Florida COM-Jacksonville, Health, Icahn School of Medicine Australia
Management, UVA Medical Jacksonville, FL at Mount Sinai, New York, NY
Center; Operational Medical Andrea Duca, MD
Joseph Habboushe, MD MBA Scott Silvers, MD, FACEP
Director, Albemarle County Fire Attending Emergency Physician,
Assistant Professor of Clinical Associate Professor of
Rescue, Charlottesville, VA Ospedale Papa Giovanni XXIII,
Emergency Medicine, Emergency Medicine, Chair of Bergamo, Italy
Calvin A. Brown III, MD Department of Emergency Facilities and Planning, Mayo
Director of Physician Medicine, Weill Cornell School Clinic, Jacksonville, FL Suzanne Y.G. Peeters, MD
Compliance, Credentialing of Medicine, New York, NY; Co- Attending Emergency Physician,
Corey M. Slovis, MD, FACP,
and Urgent Care Services, founder and CEO, MDCalc Flevo Teaching Hospital, Almere,
FACEP
Department of Emergency The Netherlands
Eric Legome, MD Professor and Chair Emeritus,
Medicine, Brigham and Women's Chair, Emergency Medicine, Department of Emergency Edgardo Menendez, MD,
Hospital, Boston, MA Mount Sinai West & Mount Sinai Medicine, Vanderbilt University FIFEM
Peter DeBlieux, MD St. Luke's; Vice Chair, Academic Medical Center, Nashville, TN Professor in Medicine and
Professor of Clinical Medicine, Affairs for Emergency Medicine, Emergency Medicine; Director of
Stephen H. Thomas, MD, MPH
Louisiana State University School Mount Sinai Health System, Icahn EM, Churruca Hospital of Buenos
Department of Emergency
of Medicine; Chief Experience School of Medicine at Mount Aires University, Buenos Aires,
Medicine, Beth Israel Deaconess
Officer, University Medical Sinai, New York, NY Argentina
Medical Center and Harvard
Center, New Orleans, LA Keith A. Marill, MD, MS Medical School, Boston, MA Dhanadol Rojanasarntikul, MD
Deborah Diercks, MD, MS, Associate Professor, Department Attending Physician, Emergency
Ron M. Walls, MD
FACEP, FACC of Emergency Medicine, Harvard Medicine, King Chulalongkorn
Professor and COO, Department
Professor and Chair, Department Medical School, Massachusetts Memorial Hospital; Faculty
of Emergency Medicine, Brigham
of Emergency Medicine, General Hospital, Boston, MA of Medicine, Chulalongkorn
and Women's Hospital, Harvard
University of Texas Southwestern University, Thailand
Angela M. Mills, MD, FACEP Medical School, Boston, MA
Medical Center, Dallas, TX Professor and Chair, Department Edin Zelihic, MD
of Emergency Medicine, Head, Department of Emergency
Columbia University Vagelos Medicine, Leopoldina Hospital,
College of Physicians & Schweinfurt, Germany
Surgeons, New York, NY
JUNE 2023 • www.ebmedicine.net 27 © 2023 EB MEDICINE. ALL RIGHTS RESERVED.
Points & Pearls
QUICK READ
Hypertensive Emergencies:
Guidelines and Best-Practice
Recommendations
JUNE 2023 | VOLUME 25 | ISSUE 6
Points
• Hypertensive urgency, hypertensive crisis, and
Pearls
malignant hypertension are terms that have his- • Severe hypertension is usually defined: systolic
torically been used to describe severely elevated BP (SBP ≥180 mm Hg, diastolic BP (DBP) ≥110
blood pressure (BP) with no evidence of end- mm Hg, or mean arterial pressure (MAP) ≥135.
organ damage. • The degree of BP elevation does not always
• Hypertensive emergency is a clinical syndrome of correlate with severity of end-organ damage;
significantly elevated BP that is associated with it is the rate of change of BP that increases the
end-organ damage. damage.26
• Hypertensive emergencies are more likely • In patients presenting to the ED with primary
among patients aged >60 years, male, Black, hypertensive emergencies, a secondary cause
underinsured or uninsured, and/or living in lower can be found in 20%-40% of cases.27 It is im-
socioeconomic areas.21 These factors should be portant to investigate the causes, as manage-
considered in disposition. ment will differ.
• The patient history should include any pre-exist- • The comprehensiveness of the physical ex-
ing end-organ dysfunction, so it can be differenti- amination is dictated by the chief complaint,
ated from an acute process. as this may indicate underlying end-organ
• The mnemonic, BARKH (brain, arteries, retina, damage. See Table 3 for the most common
kidney, heart), summarizes the most likely loca- symptoms and etiologies.
tions of end-organ damage. (See Figure 4.) • Diagnostic studies will be directed by clinical
• Choose fast-acting, easily titratable, and reliable findings. See Table 2 for an extensive differen-
IV antihypertensive drugs. (See Table 1.) tial diagnosis summary, by system, including
Acute Decompensated Heart Failure recommended workups.
• The 3 primary interventions: noninvasive positive- • Patients who do not meet criteria for hyperten-
pressure ventilation, diuretics, and vasodilators. sive emergency can be safely discharged with
Acute Ischemic Stroke close outpatient follow-up for monitoring and
• When noncontrast CT excludes intracerebral medication management.
hemorrhage (ICH) as a cause, BP manage-
ment will depend on the treatment plan chosen
(thrombolytics or mechanical thrombectomy). Aortic Dissection
Acute Coronary Syndromes • 2022 ACC/AHA guidelines recommend reducing
• There are no definitive data on BP targets, but heart rate to 60-80 beats/min and then lowering
there is evidence that patients with ACS who SBP to <120 mm Hg,19,104 with a beta blocker, be-
present with elevated BP have better out- fore lowering BP to prevent reflex tachycardia.19
comes.83-85 Management should focus on pain Hypertensive Encephalopathy
control and clinical stabilization.9 • Most commonly seen with BP >220/120 mm Hg
Intracerebral Hemorrhage • Posterior reversible encephalopathy syndrome
• ICH has the most evidence regarding BP targets (PRES), if seen, may not be attributable to BP.44,106
and timelines, but guidelines disagree on recom- Severe Pre-Eclampsia and Eclampsia
mendations. • ACOG recommends hospital admission for pa-
• In ICH, iatrogenic hypotension presents the high- tients >20 weeks‘ gestation who have pre-eclamp-
est risk for mortality.96 sia with severe features.20
Subarachnoid Hemorrhage Acute Renal Failure
• There are few to no data on BP targets for SAH, • If hypertensive emergency is the suspected cause,
and guidelines disagree, with no specific antihy- reducing SBP or MAP 25% is a reasonable op-
pertensive drug recommendations.47,99-102 tion.11,30
JUNE 2023 • www.ebmedicine.net 28 ©2023 EB MEDICINE
You might also like
- CPR ScriptDocument13 pagesCPR ScriptMary Benjie BandelariaNo ratings yet
- Case-Based Pace, ICDs, and CRT Volume 1Document234 pagesCase-Based Pace, ICDs, and CRT Volume 1oxequlalisNo ratings yet
- Algorithm-PALS Ped Systematic Approach 200615Document1 pageAlgorithm-PALS Ped Systematic Approach 200615Erica Yamamoto100% (2)
- Cardiovascular MCQs For Pharmacology ReviewDocument14 pagesCardiovascular MCQs For Pharmacology ReviewBhopesh Kadian38% (8)
- Jaundice An Emergency Department Approach To Diagnosis and ManagementDocument24 pagesJaundice An Emergency Department Approach To Diagnosis and ManagementAmali FikriahNo ratings yet
- Stemi PDFDocument60 pagesStemi PDFPraveen100% (1)
- 2019 Acute Appendicitis in Pediatric Patients: An Evidence-Based Review PDFDocument26 pages2019 Acute Appendicitis in Pediatric Patients: An Evidence-Based Review PDFVladimir BasurtoNo ratings yet
- AngioedemaDocument24 pagesAngioedemaMed. TrackNo ratings yet
- Pulmonary EmbolismDocument28 pagesPulmonary EmbolismMaNiaaa LoxONo ratings yet
- Surgical AirwaysDocument24 pagesSurgical AirwaysMed. TrackNo ratings yet
- Toxic Ingestions Pediatric EmergencyDocument24 pagesToxic Ingestions Pediatric EmergencyXimenaEspinaNo ratings yet
- Advances in Cardiac Resuscitation in The Emergency Department 1Document24 pagesAdvances in Cardiac Resuscitation in The Emergency Department 1Jhon Bayron Muñoz QuinteroNo ratings yet
- Diabetic EmergenciesDocument24 pagesDiabetic EmergencieshabibfmNo ratings yet
- 0822 Cardiac Valve EmergenciesDocument23 pages0822 Cardiac Valve EmergenciessarahmacielNo ratings yet
- Management of Allergic Reactions and Anaphylaxis in The EmergencyDocument23 pagesManagement of Allergic Reactions and Anaphylaxis in The EmergencyAna Belén Viteri luzuriagaNo ratings yet
- Headache Emergency MedicineDocument24 pagesHeadache Emergency MedicineMohamed OsmanNo ratings yet
- HFNC Noninvasive VentilationDocument24 pagesHFNC Noninvasive VentilationAbody MenaNo ratings yet
- Management of Deep Vein Thrombosis in The Emergency DepartmentDocument24 pagesManagement of Deep Vein Thrombosis in The Emergency Departmentmundode paisajes100% (1)
- Community Acquired Pneumonia 2Document22 pagesCommunity Acquired Pneumonia 2carosegurallNo ratings yet
- Emp Chest PainDocument32 pagesEmp Chest PainWilmer JimenezNo ratings yet
- Infective EndocarditisDocument24 pagesInfective EndocarditisNicolás HonoresNo ratings yet
- 0712 StrokeDocument28 pages0712 Strokejkim2097No ratings yet
- Emergency Room: Case Scenario (Group 1)Document40 pagesEmergency Room: Case Scenario (Group 1)Victoria Castillo TamayoNo ratings yet
- Procedural Sedation AnalgesiaDocument24 pagesProcedural Sedation Analgesiabenitez1228No ratings yet
- Intensive Care Fundamentals: František Duška Mo Al-Haddad Maurizio Cecconi EditorsDocument278 pagesIntensive Care Fundamentals: František Duška Mo Al-Haddad Maurizio Cecconi EditorsthegridfanNo ratings yet
- Avinash B Kumar MD Assistant Professor Anesthesiology and Critical Care Dec 2006Document29 pagesAvinash B Kumar MD Assistant Professor Anesthesiology and Critical Care Dec 2006sgod34No ratings yet
- Abg PrimerDocument22 pagesAbg PrimerAraceli Ecot CalunodNo ratings yet
- ATSP (Asked To See Patient) BookletDocument24 pagesATSP (Asked To See Patient) BookletCindy WongNo ratings yet
- 0221 Community-Acquired-PneumoniaDocument29 pages0221 Community-Acquired-PneumoniaDiego YanezNo ratings yet
- Antrim ED Handbook 2019Document238 pagesAntrim ED Handbook 2019Chris Jardine LiNo ratings yet
- Preguntas de Cardiology 2016Document168 pagesPreguntas de Cardiology 2016lemaotoyaNo ratings yet
- Identifying Emergency Department Patients With Chest Pain Who Are at Low Risk For Acute Coronary SyndromesDocument24 pagesIdentifying Emergency Department Patients With Chest Pain Who Are at Low Risk For Acute Coronary SyndromesCarlos Alejandro Rojas CastellanosNo ratings yet
- 0115 Seizures and SEDocument28 pages0115 Seizures and SEGavin TexeirraNo ratings yet
- Supraglottic Airway DevicesDocument20 pagesSupraglottic Airway Devicesvaletg27No ratings yet
- Drug Treatment For Hypertensive Emergencies: New Concepts and Emerging Technologies For Emergency PhysiciansDocument0 pagesDrug Treatment For Hypertensive Emergencies: New Concepts and Emerging Technologies For Emergency PhysiciansRajihah JihahNo ratings yet
- Emp SyncopeDocument20 pagesEmp SyncopeWilmer JimenezNo ratings yet
- Sepsis, Severe Sepsis, and Septic Shock: Current Evidence For Emergency Department ManagementDocument24 pagesSepsis, Severe Sepsis, and Septic Shock: Current Evidence For Emergency Department ManagementAdrianita0716No ratings yet
- Pain Management in The Emergency DepartmentDocument28 pagesPain Management in The Emergency DepartmentJuan Carlos CostaNo ratings yet
- AsfixiabuenoDocument24 pagesAsfixiabuenoAdrianaGallardoTapiaNo ratings yet
- Approach To TruamaDocument29 pagesApproach To TruamaIbsa ShumaNo ratings yet
- 2020 Acls Megacode Testing Scenarios - 2Document13 pages2020 Acls Megacode Testing Scenarios - 2Dr. Saqib RazaNo ratings yet
- Emergency Department Management of Cellulitis and Other Skin andDocument24 pagesEmergency Department Management of Cellulitis and Other Skin andJesus CedeñoNo ratings yet
- Hemodialysis Emergencies: Core Curriculum 2021.Document14 pagesHemodialysis Emergencies: Core Curriculum 2021.Tariq ZayanNo ratings yet
- Emergency Department Management of Acute Asthma ExacerbationsDocument32 pagesEmergency Department Management of Acute Asthma ExacerbationsFercho MedNo ratings yet
- Emergency Medicine Practice MTBI Article With CMEDocument35 pagesEmergency Medicine Practice MTBI Article With CMEAnonymous 2ur6PyFNo ratings yet
- Heart Failure 2022-2023 First Semester - FinalDocument69 pagesHeart Failure 2022-2023 First Semester - FinalAlaa zayadnehNo ratings yet
- AAP Emergencies Ped Drug Doses PDFDocument20 pagesAAP Emergencies Ped Drug Doses PDFUlvionaNo ratings yet
- Symptomatic Hypotension ED Stabilization and The Emerging Role of Sonography Emergency Medicine PracticeDocument28 pagesSymptomatic Hypotension ED Stabilization and The Emerging Role of Sonography Emergency Medicine Practiceme4milaNo ratings yet
- Wide QRS Complex TachyarrhythmiaDocument36 pagesWide QRS Complex TachyarrhythmiaMaruliNo ratings yet
- (James T. Willerson MD, Jay N. Cohn MD, James T. WDocument2,877 pages(James T. Willerson MD, Jay N. Cohn MD, James T. WHoàng LongNo ratings yet
- 0218 Acute Gastroenteritis EvidenceDocument25 pages0218 Acute Gastroenteritis EvidenceCristian C Becerra100% (1)
- ACCA Toolkit Abridged VersionDocument124 pagesACCA Toolkit Abridged VersionWillian Eduardo Camacho RojasNo ratings yet
- Evidence Based Emergency Care PDFDocument2 pagesEvidence Based Emergency Care PDFMelissa0% (1)
- Post Op Cardiac Care ReviewDocument11 pagesPost Op Cardiac Care ReviewNuha AL-YousfiNo ratings yet
- Fever in ChildrenDocument179 pagesFever in ChildrenhebaNo ratings yet
- Role of Observational Medicine in EmergencyDocument13 pagesRole of Observational Medicine in EmergencyazhaabazNo ratings yet
- Assessment of bleeding Shock in a Politraumatized PatientFrom EverandAssessment of bleeding Shock in a Politraumatized PatientNo ratings yet
- 2015 Chest - Blue & Falls ProtocolsDocument12 pages2015 Chest - Blue & Falls ProtocolsWilmer Yanquen VillarrealNo ratings yet
- 0413 Massive Upper GI BleedingDocument12 pages0413 Massive Upper GI BleedingIsaura MendezNo ratings yet
- CCSAP 2017book3 Sample ChapterDocument20 pagesCCSAP 2017book3 Sample ChapterMohanBabuNo ratings yet
- Cardiac Catheterization and MonitoringDocument40 pagesCardiac Catheterization and MonitoringMarissa Asim100% (1)
- Post OP STROK Management ASMA AlshehriDocument12 pagesPost OP STROK Management ASMA AlshehriasmashNo ratings yet
- American Society of ExtraCorporeal Technology Standards and GuidelinesDocument22 pagesAmerican Society of ExtraCorporeal Technology Standards and GuidelinesErkanNo ratings yet
- LARIO Score For LVO - 2019Document5 pagesLARIO Score For LVO - 2019Aik NoeraNo ratings yet
- 4 5931499803149076504 PDFDocument126 pages4 5931499803149076504 PDFCristianAltunaSotomayorNo ratings yet
- LercanidipineDocument8 pagesLercanidipineddandan_2No ratings yet
- Cardiac Risk Assessemnt FlowchartDocument1 pageCardiac Risk Assessemnt FlowchartjamesomooreNo ratings yet
- Nursing Exam PowerpointDocument100 pagesNursing Exam PowerpointAngelica Fontanilla Bajo RNNo ratings yet
- Pharmaceutical Care Plan: Pharmacy 302Document5 pagesPharmaceutical Care Plan: Pharmacy 302Louisa WongNo ratings yet
- Cardiovascular System - Printable Pages - MariebDocument6 pagesCardiovascular System - Printable Pages - MariebChristal Rae Tac-anNo ratings yet
- Basic Electrocardiography NewDocument25 pagesBasic Electrocardiography NewMoh Arif KurniawanNo ratings yet
- AHA (2018) - Blood CholesterolDocument36 pagesAHA (2018) - Blood CholesterolTia MahniarNo ratings yet
- Omron M6 Instruction ManualDocument24 pagesOmron M6 Instruction ManualsvigosNo ratings yet
- Kelompok 16 PBL CVSDocument11 pagesKelompok 16 PBL CVSTutde SedanaNo ratings yet
- Hypertensive EmergencyDocument25 pagesHypertensive Emergencyzainab.mohammed.2307No ratings yet
- Deep Vein Thrombosis - Wikipedia, The Free EncyclopediaDocument13 pagesDeep Vein Thrombosis - Wikipedia, The Free Encyclopediamypinklagoon8411No ratings yet
- Stroke Types and Management PDFDocument5 pagesStroke Types and Management PDFwandymargoNo ratings yet
- MORAES-SILVA Et Al 2017Document20 pagesMORAES-SILVA Et Al 2017Luiza MartinsNo ratings yet
- 87EOLT49DDocument6 pages87EOLT49DGlecy AdrianoNo ratings yet
- Heart Failure in ChildrenDocument36 pagesHeart Failure in ChildrenCristinaGheorgheNo ratings yet
- Prolonged QTC Interval in Rat After Long 2e7a2682Document6 pagesProlonged QTC Interval in Rat After Long 2e7a2682arisNo ratings yet
- Hearts and Minds -Сърца и умове-25 обобщава връзката между влошеното психично здраве и сърдечните заболяванияDocument137 pagesHearts and Minds -Сърца и умове-25 обобщава връзката между влошеното психично здраве и сърдечните заболяванияGeorgi IlievNo ratings yet
- 3 Vs Apical PulseDocument2 pages3 Vs Apical Pulse잔잔No ratings yet
- Use of Lung Ultrasound For The Assessment of Volume Status in CKDDocument11 pagesUse of Lung Ultrasound For The Assessment of Volume Status in CKDAnnisa RabbaniNo ratings yet
- Heart - Anatomy and FunctionDocument13 pagesHeart - Anatomy and FunctionAlok KumarNo ratings yet
- Next Step Advanced Medical Coding and Auditing 2017 2018 Edition 1St Edition Buck Solutions Manual Full Chapter PDFDocument36 pagesNext Step Advanced Medical Coding and Auditing 2017 2018 Edition 1St Edition Buck Solutions Manual Full Chapter PDFmichaelkrause22011998gdj100% (8)
- Chd. AmiDocument4 pagesChd. AmiDead shotNo ratings yet