Professional Documents
Culture Documents
Review: Wilmar M Wiersinga
Uploaded by
Zuni TriyantiOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Review: Wilmar M Wiersinga
Uploaded by
Zuni TriyantiCopyright:
Available Formats
Review
Advances in treatment of active, moderate-to-severe Graves’
ophthalmopathy
Wilmar M Wiersinga
Graves’ ophthalmopathy is defined as autoimmune inflammation of extraocular muscles and orbital fat or connective Lancet Diabetes Endocrinol 2016
tissue, usually in patients with Graves’ disease. About one in 20 patients with Graves’ hyperthyroidism has moderate- Published Online
to-severe Graves’ ophthalmopathy. Corticosteroids have been the mainstay of treatment, but new evidence about June 23, 2016
http://dx.doi.org/10.1016/
immune mechanisms has provided a basis to explore other drug classes. Intravenous methylprednisolone pulses are
S2213-8587(16)30046-8
more effective and better tolerated than oral prednisone in the treatment of active, moderate-to-severe Graves’
Department of Endocrinology
ophthalmopathy. Rituximab has also been suggested as a possible replacement for intravenous corticosteroids. and Metabolism, Academic
Two randomised controlled trials of rituximab reached seemingly contradictory conclusions—rituximab was not Medical Centre, University of
better with respect to the primary outcome (clinical activity score) than placebo in one trial (which, however, was Amsterdam, Netherlands
(Prof W M Wiersinga MD)
confounded by rather long Graves’ ophthalmopathy duration), but was slightly better than intravenous
methylprednisolone pulses in the other (disease flare-ups occurred only in the latter group). On the basis of evidence Correspondence to:
Prof Wilmar M Wiersinga,
published so far, rituximab cannot replace intravenous methylprednisolone pulses, but could have a role in Department of Endocrinology
corticosteroid-resistant cases. Open-label studies of tumour-necrosis-factor-α blockade had limited efficacy, but other and Metabolism, Academic
studies showed that interleukin-6 receptor antibodies were effective. Results of randomised controlled trials Medical Centre, University of
Amsterdam, Meibergdreef 9,
investigating the efficacy of the IGF-1 receptor antibody teprotumumab and the interleukin-6 receptor antibody
Amsterdam 1105AZ,
tocilizumab are expected shortly. Approaches that target the causal mechanism of Graves’ ophthalmopathy (antibodies Netherlands
or antagonists that block thyroid-stimulating-hormone receptors) also look promising. w.m.wiersinga@amc.uva.nl
Introduction in the autoimmune attack of orbital tissues, which has
Graves’ ophthalmopathy is one of the remaining led to several innovative therapies, including rituximab
enigmas in thyroidology. It is an autoimmune disease and drugs that target orbital fibroblast receptors or
that occurs predominantly in patients with Graves’ inflammatory cytokines.4
hyperthyroidism, which is caused by thyroid-stimulating- The precise pathogenesis of this thyroid-associated
hormone (TSH) receptor-stimulating antibodies ophthalmopathy remains incompletely understood,
produced initially by lymphocytes in the thyroid gland although autoimmune mechanisms clearly play a part
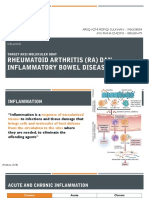
and neighbouring lymph nodes. Signs and symptoms of (figure). Immunocompetent cells such as T cells, B cells,
Graves’ ophthalmopathy involve swollen extraocular monocytes, fibrocytes, macrophages, and mast cells are
muscles and expansion of orbital fat and connective recruited into the orbit. Macrophages, but also B cells,
tissue, and include swelling and redness of eyelids and might present the responsible autoantigen—most likely
conjunctiva, exophthalmos, double vision, and, in severe the TSH receptor—to T cells, which are then stimulated
cases, corneal ulceration and decreased visual acuity. to recognise orbital fibroblasts, the target cells of the
The incidence of Graves’ hyperthyroidism was orbital autoimmune attack. Activated infiltrating T cells
210 per million per year in a population-based study secrete cytokines and chemokines; in the early stages of
in Sweden, 20·1% of whom had symptoms of the disease T-helper-1-derived cytokines (interferon γ,
Graves’ ophthalmopathy (non-infiltrative in 15·2% and tumour necrosis factor α, interleukins 1β and 2)
infiltrative in 4·9%).1 In a Danish study2 published in predominate, whereas later T-helper-2 responses
2012, the incidence of moderate-to-severe Graves’ (interleukins 4, 5, and 10) predominate. The release of
ophthalmopathy was 4·9% among patients with Graves’ cytokines induces synthesis and release of large amounts
hyperthyroidism. These figures are in good agreement of glycosaminoglycans like hyaluronan by orbital
with a single-centre study3 from Italy in patients with fibroblasts, which, as a result of their hydrophilic
newly diagnosed Graves’ hyperthyroidism, in whom nature, cause swelling of orbital tissues—especially of
the prevalence of mild, moderate-to-severe, and extraocular muscles. Some cytokines also cause
sight-threatening Graves’ ophthalmopathy was 20·0%, differentiation of a subset of orbital fibroblasts called
5·8%, and 0·3%, respectively. Thus, moderate-to-severe preadipocytes (present in orbital fat but not in muscles)
disease occurs in about one in every 20 patients with into mature adipocytes via adipogenesis. Orbital
Graves’ hyperthyroidism. fibroblasts express TSH receptors, which are upregulated
A therapy targeting the most likely cause of Graves’ in the active stages of the disease. TSH-receptor-
ophthalmopathy (ie, TSH receptor antibodies recognising stimulating antibodies increase hyaluronan production
TSH receptors expressed on orbital fibroblasts) has not and adipogenesis in cultured human fibroblasts.
yet been tested in human beings, and corticosteroids are IGF-1-receptor expression is also increased in orbital
still used. However, considerable progress has been fibroblasts during active disease, and ligation with
made in unravelling the molecular mechanisms involved IGF-1 also stimulates hyaluronan and adipogenesis.
www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8 1
Review
Antigen-presenting cell
Corticosteroids
Ever since the report of Lord Brain in The Lancet in 1955,5
corticosteroids have been the mainstay of treatment of
severe Graves’ ophthalmopathy. The mode of
TSH receptor
MHC molecule administration has changed, however: meta-analyses of
(presenting TSH receptor randomised clinical trials clearly demonstrate that
peptide)
intravenous methylprednisolone pulses (IVMP) have
IGF-1 receptor
greater efficacy than oral prednisone (response rate 74%
T-cell receptor B cell vs 51%) and fewer side-effects (56% vs 81%).6,7
Consequently, guidelines recommend IVMP for active,
T cell
moderate-to-severe Graves’ ophthalmopathy—preferably
Cytokines
500 mg weekly for 6 weeks followed by 250 mg weekly
for another 6 weeks (cumulative dose 4·5 g).8
An alternative schedule with the same cumulative dose
TSH receptor antibodies
of 4·5 g administered over 4 weeks had lower efficacy
(41% vs 77%) and more side-effects than did the 12 week
Macrophage
regimen.9
CD40 L TSH receptor
Cytokine IGF-1 receptor Cumulative doses of 7·47 g, 4·98 g, and 2·25 g given
CD40
receptor over 12 weeks were compared in a large randomised
controlled trial.10 Clinical activity score (panel) decreased
with all doses, but a composite ophthalmic score
Orbital fibroblast
improved greatest with the highest dose (response rates
52%, 35%, and 28%, respectively) at the expense of more
side-effects. Flare-ups of Graves’ ophthalmopathy after
corticosteroid discontinuation occurred in 12% overall
(13% in the high-dose group, 7% in the intermediate-
dose group, and 11% in the low-dose group).10 It is
Hyaluronan production Adipocytes
Muscle swelling Adipogenesis
hypothesised that these flare-ups can be counteracted by
administering low doses of oral prednisone in between
pulses12 or by combining IVMP with orbital irradiation.13
Notably, orbital irradiation plus oral prednisone is more
effective than oral prednisone alone.14 The most effective
approach to counteracting flare-ups has yet to be proven
in randomised controlled trials.
Corticosteroids usually improve soft-tissue changes
(swelling and redness of eyelids and conjunctiva) and
eye-muscle motility (diplopia), but are less effective at
reducing exophthalmos. IVMP have been associated
Figure: Immunopathogenesis of Graves’ ophthalmopathy. with acute and severe liver damage, sometimes resulting
Cytokines released from T cells (activated by immunocompetent cells infiltrating the orbit) and TSH receptor
antibodies stimulate orbital fibroblasts to produce hyaluronan and to differentiate into adipocytes, thereby causing in fatal liver failure.15,16 A questionnaire survey17 among
swelling of extraocular muscles and orbital fat. CD40 L=CD40 ligand. TSH=thyroid-stimulating hormone. members of the European Thyroid Association showed
seven deaths (four due to acute liver failure, two due to
cerebrovascular disease, and one due to pulmonary
TSH-receptor and IGF-1-receptor signalling pathways embolism) occurring between 4 and 120 days after
overlap downstream of their receptors, but there is starting IVMP. All but one of the patients who died had
insufficient evidence that the IGF-1 receptor is a major received a cumulative dose of more than 8 g.17 Identified
autoantigen in Graves’ ophthalmopathy.4 risk factors for adverse effects from IVMP are dose, age
Corticosteroids have been the mainstay of treatment older than 53 years, daily pulses, and pre-existing
for Graves’ ophthalmopathy since the 1950s, but hepatitis.18–20 A 2011 review of IVMP in 1045 patients
increasing evidence about pathological mechanisms has showed a morbidity of 6·5% and mortality of 0·57%.21
provided a basis to explore other drug classes for disease Contraindications for IVMP are recent hepatitis, liver
treatment. In this Review, I discuss studies from the dysfunction (five-times increased liver enzymes), cardio-
past 5 years about safety and optimum dosage of vascular morbidity, severe hypertension, uncontrolled
corticosteroids, and whether new treatment modalities diabetes, and glaucoma.21 When administering IVMP,
like rituximab and other biologicals could replace cumulative doses greater than 8 g and administration on
corticosteroids in active, moderate-to-severe Graves’ consecutive days should be avoided (except in dysthyroid
ophthalmopathy. optic neuropathy—defined as loss of visual functions
2 www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8
Review
caused by pressure of enlarged orbital tissues on the optic
nerve). Monthly monitoring of liver chemistry, glucose, and Panel: Assessment of Graves’ ophthalmopathy in terms of
blood pressure is warranted in all patients receiving IVMP.21 disease activity and severity
In a 2015 single-centre study22 following these Disease activity (based on the clinical activity score11
recommendations, acute liver damage (defined as an [maximum score 7])*
alanine aminotransferase increase exceeding four times • Spontaneous retrobulbar pain
the upper limit of normal) was reported in four of • Pain on attempted up, down, or side gaze
376 patients (1%); there were no deaths. The cumulative • Redness of the eyelids
dose of 4·5 g is preferred, because this dose does not result • Redness of the conjunctiva
in suppression of the hypothalamus–pituitary–adrenal • Swelling of the eyelids
axis.23 The 7·5 g schedule is an option in severe cases with • Swelling of the caruncle or plica, or both
troubling diplopia. Administration of alendronate could • Chemosis
suppress IVMP-induced bone resorption, which can occur
in any patient receiving IVMP.24 Disease severity (NO SPECS as a mnemonic)
• No signs or symptoms
Rituximab • Only signs, no symptoms
Early evidence • Lid aperture in midline in mm
Rituximab is a monoclonal antibody directed against • Soft-tissue involvement
CD20, which is expressed by B cells but not stem cells or • Swelling and redness of eyelids and conjunctiva
B-cell precursors. It causes B-cell depletion, but antibody • Proptosis
production can be maintained because CD20 is not • Hertel in mm
expressed by antibody-producing plasma cells in the • Extraocular muscle involvement
bone marrow.25 Thus any decreases in serum • Eye muscle ductions, diplopia†
concentrations of TSH-receptor antibodies after treat- • Corneal involvement
ment of Graves’ ophthalmopathy appear unrelated to • Punctate keratopathy, ulcer
B-cell depletion. The effect of rituximab in Graves’ • Sight loss (as a result of optic nerve involvement)
ophthalmopathy might result from the blockade of • Best-corrected visual acuity, colour vision, optic disc,
antigen presentation by B cells after anti-CD20-induced visual fields
lysis, resulting in decreased T-cell activation.25 *Clinical activity score is the sum of all items present, with a maximum score of 7;
In 2006, two case reports26,27 of spectacular improvement a score of 3 or higher suggests active Graves’ ophthalmopathy. †Score: 0=no diplopia,
1=intermittent diplopia (ie, when tired or upon waking), 2=inconstant diplopia
of corticosteroid-resistant Graves’ ophthalmopathy after (ie, at extremes of gaze), 3=constant diplopia (ie, in primary or reading position).
treatment with rituximab were published. As of 2013,
reports had been published of 43 patients with Graves’
ophthalmopathy who had been treated with rituximab The discrepant outcomes could be confusing because
(usually 1 g 2 weeks apart), mostly after previous the conclusions of both trials are mutually exclusive. If
corticosteroid failure.25 Graves’ ophthalmopathy activity rituximab is at least as effective as corticosteroids, as
and severity improved in 98% and 91% of patients, shown in the second trial, why wasn’t this efficacy
respectively. Clinical activity score decreased from detected in the first? If you accept that rituximab is not
4·9 (range 4·7–7·0) before therapy to 2·2 (0–7) after better than placebo, you have to conclude that the effect
16 weeks.25 Responses were observed in each of the of corticosteroids in the second trial is inferior to that of
disease severity categories (panel). Side-effects occurred placebo, and it is hard to believe that corticosteroids are
in 13 patients (30%); they were minor in ten patients and devoid of efficacy. A placebo-controlled double-blind
major in three patients. One patient developed dysthyroid randomised controlled trial31 showed that IVMP are
optic neuropathy.28 The overall favourable results in more efficacious than placebo in active, moderate-to-
these uncontrolled studies suggested the possibility that severe disease (response rate 83% vs 11%, p<0·005).
rituximab might replace corticosteroids as first-line So, how can the seemingly discrepant outcomes of
treatment of active, moderate-to-severe Graves’ these trials29,30 be explained? The parallel double-blind
ophthalmopathy. study designs of both trials were very similar: patients
with Graves’ ophthalmopathy of similar activity and
Efficacy severity were included and initially given the same
In February, 2015, the results of two randomised rituximab dosage schedule, and the same primary
controlled trials of rituximab in active, moderate-to- outcome measure at 24 weeks was used in both.
severe Graves’ ophthalmopathy were published. However, there were obvious baseline differences
Rituximab was not better than placebo in improving between the studies with regard to smoking, duration
clinical disease activity (the primary outcome) in the of disease, and previous corticosteroid use (table 1).
first trial, by Stan and colleagues,29 but was slightly Smoking is associated with less favourable responses to
better than IVMP in the second, by Salvi and colleagues.30 corticosteroids and retrobulbar irradiation in patients
www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8 3
Review
with Graves’ ophthalmopathy.32,33 A possible interaction allowed interval between discontinuation of cortico-
between smoking and the response to rituximab has steroids and enrolment was shorter in the placebo-
not been assessed in Graves’ ophthalmopathy, but in controlled trial29 (at least 4 weeks) than in the
rheumatoid arthritis the response rate to the drug was corticosteroid-controlled trial30 (at least 12 weeks). The
lower in current smokers than in previous and never planned rituximab dose was initially the same in both
smokers (20% vs 61% vs 98%).33 Smoking was more trials (two intravenous doses of 1 g), but in the
prevalent in Salvi and coworkers’ trial30 than in Stan corticosteroid-controlled trial, ten patients received a
and colleagues’ trial,29 and therefore lower rituximab lower single dose of 500 mg, which was as efficacious as
efficacy might have been expected in the corticosteroid- the full dose in depleting B cells and improving clinical
controlled trial; the opposite, however, was observed. activity scores. Therefore differences in rituximab
Smoking is thus an unlikely explanation for the dosages are unlikely to have affected observed efficacy.
discrepant outcomes. On the basis of existing data, in my view it is
However, perhaps the long duration of disease in premature to conclude that rituximab is devoid of any
patients in the placebo-controlled trial29 could have efficacy in the treatment of Graves’ ophthalmopathy.
contributed to rituximab’s observed lack of efficacy The much longer duration of disease in Stan and
(table 1). Six patients had Graves’ ophthalmopathy for colleagues’ trial29 than in Salvi and colleagues’ trial30
more than 2 years.29 The longer the duration, the greater (probably reflecting different referral patterns) can
the chance the disease has reached its inactive, fibrotic explain at least partly why rituximab was not efficacious
stage, and the smaller the chance that immuno- in the placebo-controlled trial.
suppression will be effective.4 The high baseline clinical
activity score of 5·1 in the placebo-controlled trial29 is Extent of efficacy: primary and secondary outcomes
taken as evidence of active disease, but some items of The rate of decline in the primary outcome measure,
this disease measure (eg, redness) could be due to clinical activity score, over a year was the same in both
congestion as a result of long-standing Graves’ randomisation groups in the placebo-controlled trial,29
ophthalmopathy—a weakness of the clinical activity suggesting that the fall in clinical activity score might
score for determination of disease activity. reflect the natural history of Graves’ ophthalmopathy. In
Patients who had previously been treated with Salvi and colleagues’ trial,30 the decline in clinical activity
corticosteroids were included in both trials, but the score was the same in both groups up to 12 weeks;
thereafter it did not decrease any further in the IVMP
group (coinciding with corticosteroid discontinuation at
Stan et al29 Salvi et al30 12 weeks), but continued to decrease up to 24 weeks in
Rituximab (n=13) Placebo (n=12) Rituximab (n=15) Intravenous the rituximab group. With regard to secondary outcomes,
corticosteroids rituximab was superior to IVMP at 24 weeks in terms of
(n=16) effects on lid aperture (improvement 13% vs 0%,
Female 9 (69%) 8 (67%) 14 (93%) 12 (75%) respectively) and eye-muscle motility (combined ductions
Age, years (SD) 58 (13) 62 (11) 52 (13) 50 (11) 197 degrees vs 178 degrees out of a maximum of
Smoking 2 (15%) 2 (17%) 10 (67%) 9 (56%) 210 degrees) but not proptosis (improvement in 0% vs
Disease duration 373 days (range 299 days (range 4·5 months 4·6 months 6%) or diplopia (improvement in 20% vs 19%). Thus, in
240–1080) 253–595) (SD 2·9) (SD 2·6) the first 24 weeks of treatment, the superiority of
Previous corticosteroids 4 (31%) 6 (50%) 6 (40%) 6 (38%) rituximab seems limited.
Corticosteroid-free period At least 4 weeks At least 4 weeks At least 12 weeks At least 12 weeks At 52 weeks rituximab was better than IVMP (in
before trial
clinical activity score, lid aperture, proptosis, and
TSHR antibodies, U/L 20 (range 9–60) 20 (range 2–29) 10·7 (SD 9·1) 18·2 (SD 21·7)
diplopia score). None of the 15 patients in the rituximab
Lid aperture, mm (SD) 11·1 (2·8) 9·8 (2·0) 11·9 (2·3) 11·5 (1·8) group had disease relapses compared with five (31%) of
Proptosis, mm (SD) 24·2 (3·3) 23·0 (2·4) 23·5 (3·5) 22·5 (3·7) 16 patients in the IVMP group.30 Additional surgical
Diplopia score (range) 2 (1–2·5) 2 (1–3·75) 1 (0–2·5) 1 (0–2) treatment was required more often in the IVMP group
Rituximab dosage 2 × 1000 mg .. 2 × 1000 mg .. (ten [62%] of 16 vs three [20%] of 15 in the rituximab
(n=5) or 1 × 500 mg
(n=10)
group). Improvement by 6 or more points on the
Baseline clinical activity 4·9 (1·0) 5·3 (1·0) 4·4 (0·7) 4·7 (0·7)
disease-specific quality-of-life questionnaire was more
score (SD) frequent in the rituximab than in the IVMP group at
Clinical activity score at 3·7 (1·9) 3·8 (1·4) 0·6 (0·3) 2·3 (0·5) 52 weeks, both in terms of appearance (eight [62%] of
24 weeks (SD) 13 vs six [46%] of 13) and in the visual functioning scale
(ten [77%] of 13 vs seven [54%] of 13) . Thus, the greater
Data are n (%) unless otherwise specified. In one trial, rituximab was compared with placebo,29 in the other it was
compared with intravenous corticosteroids.30 TSHR=thyroid-stimulating-hormone receptor. efficacy of rituximab compared with IVMP (given in a
high cumulative dose of 7·5 g) seems to become evident
Table 1: Baseline characteristics and primary outcomes (clinical activity score) of two randomised clinical
after 24 weeks, especially in terms of the frequency of
trials of rituximab in patients with active, moderate-to-severe Graves’ ophthalmopathy
relapse after discontinuation of corticosteroids.
4 www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8
Review
Tolerability lower doses of ritumimab might be equally effective
In Stan and colleagues’ trial,29 11 adverse events occurred and are probably better tolerated. This subject is actively
in eight (80%) of ten patients in the rituximab group under investigation.
group (six minor and five moderate-to-severe, including
two cases of dysthyroid optic neuropathy), and four Feasibility of other novel therapies
adverse events occurred in three (27%) of 11 patients in Targeting of orbital fibroblasts
the placebo group (three minor, one moderate-to-severe). Table 2 lists possible targets of future therapies.
In Salvi and coworkers’ investigation,30 13 adverse events The stimulating effects of TSH-receptor-stimulating
occurred in 13 (87%) of 15 patients in the rituximab group antibodies on hyaluronan production and adipogenesis
(11 minor, two moderate-to-severe—both dysthyroid in cultured human orbital fibroblasts can be blocked in
optic neuropathy), and ten adverse events occurred in vitro by TSH-receptor-blocking monoclonal antibodies34,35
ten (62%) of 16 patients in the IVMP group (seven minor, and by small molecule TSH-receptor antagonists
three moderate-to-severe). (In the secondary outcomes (low-molecular-weight compounds binding in the
section of the Salvi trial,30 a patient randomly assigned transmembrane domain of the TSH receptor).36–38
to IVMP who developed optic neuropathy and was Blockade of TSH-receptor-mediated signalling holds
unresponsive to additional corticosteroids was described; great promise for the future as it directly interferes with
this patient, however, is not mentioned in the table listing the action of thyroid-stimulating immunoglobulins, the
all adverse events.) immediate cause of Graves’ disease.
Overall, dysthyroid optic neuropathy developed in four Postreceptor signalling pathways of TSH receptors and
(16%) of 25 patients who received rituximab compared IGF-1 receptors overlap, and ligation of IGF-1 receptors
with none of the 27 patients receiving placebo or with IGF-1 also results in increased hyaluronan production
corticosteroids. The rather acute loss of visual function and adipogenesis.45–47 There is good evidence that these
during or shortly after rituximab infusion was attributed in-vitro effects can be blocked by IGF-1-receptor-blocking
to rapid and massive release of cytokines, known as antibodies (eg, teprotumumab).48 A randomised controlled
cytokine-release syndrome. Alternatively, this effect trial in which teprotumumab is compared with placebo
might reflect progression of pre-existing orbitopathy in in active, moderate-to-severe Graves’ ophthalmopathy
patients in whom immunosuppression is not effective. (NCT01868997) has completed recruitment.
Loss of visual function was fortunately transient in two Orbital fibroblasts express PDGF receptors. PDGF
of the four patients; in the other two, urgent surgical isoforms AA, AB, and BB are all increased in orbital
decompression of the orbit was done (the outcome in
these patients was not reported, although orbital surgical Drug Evidence of efficacy
decompression is usually very effective in restoring
Orbital fibroblast
visual acuity in Graves’ ophthalmopathy).
TSH receptor TSH-receptor-blocking antibodies, In-vitro inhibition of hyaluronan and
TSH-receptor antagonist adipogenesis34–38
Role in therapy IGF-1 receptor IGF-1-receptor-blocking antibodies Placebo-controlled randomised controlled
Rituximab appears slightly more efficacious than (teprotumumab) trial (to complete in 2017; NCT01868997)
intravenous steroids, but its safety profile is less good PDGF Tyrosine-kinase inhibitors (imatinib, In-vitro inhibition of hyaluronan
than that of IVMP. On the basis of existing data, nilotinib, dasatinib) production39,40
rituximab should not replace IVMP as the treatment of Somatostatin Somatostatin receptor analogues None
receptor (pasireotide)
choice in active, moderate-to-severe Graves’ ophthal-
B cells
mopathy. It can be tried in severe corticosteroid-resistant
cases, although chances of a favourable response appear CD20 CD20 monoclonal antibody (rituximab) Two conflicting randomised controlled
trials29,30
lower with longer disease duration.
T cells
A few cases of optic neuropathy that have been
CD3 CD3 monoclonal antibody (teplizumab) None
successfully treated with rituximab have been
CTLA4 CTLA4 analogue (abatacept) None
described,25 but rituximab should not be given if
Cytokines
dysthyroid optic neuropathy is suspected. It is
Tumour Anti-tumour necrosis factor α (etanercept, Limited efficacy in open-label case series41–43
hypothesised that the patients who developed necrosis factor α infliximab, adalimumab)
dysthyroid optic neuropathy when given rituximab had Interleukin 1 Soluble-interleukin-1 receptor (rilonacept) In-vitro inhibition of hyaluronan
subclinical dysthyroid optic neuropathy already, and Interleukin-1-receptor antagonist production44
that rituximab induced a massive release of cytokines (anakinra)
that caused further acute swelling of orbital tissues, Interleukin 6 Interleukin-6-receptor monoclonal Good efficacy in open-label case series,
thereby compressing the optic nerve.28 Perhaps the antibody (tocilizumab) randomised controlled trial in progress
(NCT01297699 )
most important implications of both Stan and
colleagues’ and Salvi and colleagues’ trials29,30 are that TSH=thyroid-stimulating hormone.
the earlier you treat, the greater the chance of
Table 2: Possible targets of future therapies for active, moderate-to-severe Graves’ ophthalmopathy
immunosuppression being successful, and that much
www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8 5
Review
tissues of patients with active and inactive Graves’ Targeting of cytokines
ophthalmopathy, and are produced by infiltrating Expression of cytokine mRNA in orbital fat and connective
monocytes, macrophages, and mast cells. PDGF induces tissue is much higher in active than in inactive disease for
proliferation and hyaluronan and cytokine production, several cytokines (eg, interleukins 1β, 2, 6, 8, 10), but
and increases expression of TSH receptors in cultured similar between both groups for others (eg, tumour
orbital fibroblasts.39 Tyrosine-kinase inhibitors like necrosis factor α, interferon γ, interleukin 1RA).59,60
imatinib and nilotinib inhibit PDGF-receptor signalling Tumour-necrosis-factor-α blockade in patients with
in orbital fibroblasts by preventing receptor auto- Graves’ ophthalmopathy has not been tested in
phosphorylation upon ligand binding, but have serious randomised controlled trials, and results in small case
side-effects such as periorbital oedema, peripheral series have not been very successful. Etanercept improved
arterial occlusive disease, and cerebrovascular events.49 Graves’ ophthalmopathy in six of ten patients, more so in
More promising is dasatinib, which has the lowest IC50 terms of activity (ie, clinical activity score) than severity of
of all tyrosine-kinase inhibitors for PDGF receptors.40 disease; after discontinuation of etanercept, a flare-up was
Orbital uptake on octreotide scintigraphy is increased reported in three patients.41 There is one case report42 of a
in active Graves’ ophthalmopathy but not in inactive patient with dysthyroid optic neuropathy, in whom clinical
disease, and has been proposed as a disease-activity activity score, colour vision, and visual acuity improved
parameter (it suggests involvement of somatostatin after an infusion of infliximab. A case series43 showed
receptors in disease).50 Compared with those from improvement in an inflammatory score in five of
controls with unrelated eye conditions (eg, trauma, ten patients given adalimumab (noted only in patients
osteoma, strabismus), there is an upregulation of SST1 with high baseline scores for inflammation); proptosis or
and SST5 in orbital fibroblasts from patients with motility were not improved.
Graves’ ophthalmopathy.51 However, several randomised There is fair evidence that glycosaminoglycan
controlled trials with the somatostatin analogues production in cultured human orbital fibroblasts is
octreotide and lanreotide showed no or marginal inhibited by interleukin-1-receptor antagonists or soluble
improvement of eye changes in Graves’ ophthalmopathy.52 interleukin-1 receptors,44 but such treatment has not been
This lack of efficacy might be explained by the low tested in patients.
binding affinities of octreotide and lanreotide for SST1 A non-randomised, open-label study61 showed remarkable
and SST5.53 The new analogue pasireotide has much success with tocilizumab (an interleukin-6-receptor
higher binding affinities for somatostatin receptors, monoclonal antibody) in 18 patients with active
especially for SST1 and SST5,54 and might thus be corticosteroid-resistant Graves’ ophthalmopathy. Mean
effective in Graves’ ophthalmopathy. However, the disease duration was 16 months. 8 mg/kg of tocilizumab
efficacy of pasireotide in Graves’ ophthalmopathy has was given per month (minimum 480 mg per session)
not been investigated. intravenously for a mean of five sessions (range 4–9), with
a follow-up of 15 (9–27) months. Improvement occurred in
Targeting of T and B cells all patients: clinical activity score decreased from
Given the pathological role of T cells in Graves’ 6·5 (SD 1·2) to 0·6 (0·8), proptosis decreased from
ophthalmopathy (figure), antibodies targeting these 22·3 mm (3·2) to 19·8 mm (2·6), eye muscle motility
cells could be investigated as a potential therapy. For improved in 15 patients, diplopia in primary gaze was
example, CD3 antibodies (eg, otelixizumab, teplizumab) present in 13 patients before treatment compared with
deplete T cells, and have shown some benefit in six afterwards, and visual acuity increased from
preservation of β-cell function in patients with type 1 0·75 (0·19) to 0·86 (0·14). TSH-receptor antibodies
diabetes when given in the early stages of the disease.55 decreased by about 40%. The safety profile of tocilizumab
Another approach could be treatment with abatacept (an appears rather good: side-effects occur in 66% but are
analogue of CTLA4 that limits further activation of mostly mild and transient in nature.62 The results are
T cells), which has been used in corticosteroid-resistant almost too good to believe. However, treatment success is
rheumatoid arthritis.56 Induction of T-cell tolerance to claimed more often in uncontrolled studies than in studies
target autoantigens with synthetic peptides has also in which controls have been used; claims for the success of
attracted much interest. Peptide immunotherapy is a treatment are closely associated with the absence of
highly effective at silencing autoimmune responses in the means whereby these claims can be scientifically
experimental autoimmune encephalomyelitis, an substantiated.63 A randomised controlled trial comparing
animal model of multiple sclerosis.57 However, none of tocilizumab with placebo has been completed
these T-cell-directed interventions have been applied in (NCT01297699) but the results have not yet been published.
autoimmune thyroid disease.58
As discussed earlier, CD20 antibodies (eg, rituximab) Need for randomised clinical trials
deplete B cells, but it will be another few years before the As noted previously, moderate-to-severe Graves’ ophthal-
right dose and indication for use in patients with Graves’ mopathy occurs in about one in every 20 patients with
ophthalmopathy are settled upon. Graves’ hyperthyroidism—a low incidence of around
6 www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8
Review
10–16 patients per million people per year. There is also a TSH receptor cDNA.67,68 An animal model is, however,
noteworthy trend towards less active and less severe unlikely to answer all remaining questions. Intriguing
Graves’ ophthalmopathy: patients referred to the clinical questions include why not all patients with
European Group On Graves’ Orbitopathy centres in 2012 Graves’ hyperthyroidism develop clinically overt For the European Group On
more often had inactive (63% vs 40%, p<0·01) or mild ophthalmopathy, and why Graves’ ophthalmopathy Graves’ Orbitopathy see http://
www.eugogo.eu/
(61% vs 41%, p<0·01) disease than did those referred in develops in about 13% of all cases in the absence of
2000.64 Possible explanations for the decline in incidence hyperthyroidism. The most promising drugs in the near
and severity are secular trends toward lower prevalence of future are presumably teprotumumab and tocilizumab.
smoking and earlier diagnosis and treatment of Graves’ Declaration of interests
hyperthyroidism. At the same time, the number of I am a consultant for Riverside Vision Development Corporation,
potential novel therapies for Graves’ ophthalmopathy is New York, NY, USA.
rising. The efficacy and tolerability of these new treatment References
modalities have to be investigated in randomised 1 Abraham-NordingM, Bystrom K, Torring O, et al. Incidence of
hyperthyroidism in Sweden. Eur J Endocrinol 2011; 165: 899–905.
controlled trials, which should have an adequate sample 2 Laurberg P, Berman DC, Bulow Pedersen I, Andersen S, Carle A.
size (eg, 53 participants in each randomisation arm were Incidence and clinical presentation of moderate to severe Graves’
required to detect differences in response rates of 80%, orbitopathy in a Danish population before and after iodine
fortification of salt. J Clin Endocrinol Metab 2012; 97: 2325–32.
65%, and 55% with 80% power and a significance level of 3 Tanda ML, Piantanida L, Liparulo G, et al. Prevalence and natural
p=0·05).10 There will probably be a shortage of patients history of Graves’ orbitopathy in a large series of patients with
suitable for inclusion in trials. Multicentre cooperation is newly diagnosed Graves’ hyperthyroidism seen at a single center.
J Clin Endocrinol Metab 2013; 98: 1443–49.
thus required, and, against this background, consortiums 4 Bahn R. Current insights into the pathogenesis of Graves’
like the European Group On Graves’ Orbitopathy provide ophthalmopathy. Horm Metab Res 2015; 47: 773–78.
the ideal environment for timely completion of 5 Cortisone in exophthalmos: report on a therapeutic trial of cortisone
and corticotrophin (ACTH) in exophthalmos and exophthalmic
randomised controlled trials. ophthalmoplegia by a panel appointed by the Medical Research
The most appropriate outcome measures of such trials Council. Lancet 1955; 268: 6–9.
in active, moderate-to-severe Graves’ ophthalmopathy 6 Stiebel-Kalish H, Robenshtok E, Hasanreisoglu M, Ezrachi D,
should also be considered— standardisation would allow Shimon I, Leibovici L. Treatment modalities for Graves’
ophthalmopathy: systematic review and meta-analysis.
better comparison between trials. In my opinion, there J Clin Endocrinol Metab 2009; 94: 2708–16.
should be two primary outcomes: one subjective measure 7 Gao G, Dai J, Qian Y, Ma F. Meta-analysis of methylprednisolone
reported by the (blinded) patient (like the Graves’ pulse therapy for Graves’ ophthalmopathy. Clin Exp Ophthalmol
2014; 42: 769–77.
ophthalmopathy quality-of-life questionnaire),65 and one 8 Bartalena L, Baldeschi L, Dickinson A, et al. Consensus statement
objective measure assessed by the (blinded) physician. of the European Group on Graves’ Orbitopathy (EUGOGO) on
Nowadays, the clinical activity score is used most frequently management of GO. Eur J Endocrinol 2008; 158: 273–85.
9 Zhu W, Ye L, Shen L, et al. A propsective, randomized trial of
as the primary (objective) outcome measure. However, it is intravenous glucocorticoids therapy with different protocols for
pertinent to remember that the score was introduced in patients with Graves’ ophthalmopathy. J Clin Endocrinol Metab 2014;
1997 as a predictor of response to corticosteroids to 99: 1999–2007.
10 Bartalena L, Krassas GE, Wiersinga W, et al. Efficacy and safety of
save non-responders from unnecessary exposure and three different cumulative doses of intravenous methylprednisolone
side-effects.11 Thus, a question arises about the goal of for moderate to severe and active Graves’ orbitopathy.
immunosuppressive treatment in active, moderate-to- J Clin Endocrinol Metab 2012; 97: 4454–63.
severe Graves’ ophthalmopathy.66 If the aim is to inactivate 11 Mourits MP, Prummel MF, Wiersinga WM, Koornneef L.
Clinical activity score as a guide in the management of patients
Graves’ ophthalmopathy to allow rehabilitative surgery with Graves’ ophthalmopathy. Clin Endocrinol 1997; 47: 9–14.
(eg, for diplopia) sooner, then the clinical activity score 12 Nedeljkovic Beleslin B, Ciric J, Zarkovic M, et al. Efficacy and safety
seems adequate as primary outcome. However, if it is to of combined parenteral and oral steroid therapy in Graves’
orbitopathy. Hormones (Athens) 2014; 13: 222–28.
reduce inflammation and symptoms (like diplopia), 13 Bartalena L, Marcocci C, Chiovato L, et al. Orbital cobalt irradiation
clinical activity score does not suffice as the primary combined with systemic corticosteroids for Graves’
outcome, and assessment of lid aperture, proptosis, eye ophthalmopathy: comparison with systemic corticosteroids alone.
J Clin Endocrinol Metab 1983; 56: 1139–44.
muscle motility, and diplopia should be incorporated. To 14 Marcocci C, Bartalena L, Bogazzi F, et al. Orbital radiotherapy
this end, the European Group On Graves’ Orbitopathy has combined with high dose systemic glucocorticoids is more effective
designed a composite ophthalmic score as an objective than radiotherapy alone. Results of a prospective randomised study.
J Endocrinol Invest 1991; 14: 853–60.
primary outcome measure,6 which takes into account 15 Weissel M, Hauff W. Fatal liver failure after high-dose
difficulties that can arise when improvement occurs in one glucocorticoid pulse therapy in a patient with severe thyroid eye
item but deterioration in another item or in the other eye.10 disease. Thyroid 2000; 10: 521.
A reliable animal model of Graves’ ophthalmopathy, in 16 Marino M, Morabito E, Brunetto MR, Bartalena L, Pinchera A,
Marcocci C. Acute and severe liver damage associated with
which the efficacy of novel therapies could be tested, intravenous glucocorticoid pulse therapy in patients with Graves’
would be very useful. Paul Banga’s group has made ophthalmopathy. Thyroid 2004; 14: 403–06.
substantial progress in this respect: a mouse model of 17 Marcocci C, Watt T, Altea MA, et al. Fatal and non-fatal adverse
events of glucocorticoid therapy for Graves’ orbitopathy:
Graves’ disease with some features mimicking Graves’ a questionnaire survey among members of the European Thyroid
ophthalmopathy was created by genetic immunisation of Association. Eur J Endocrinol 2012; 166: 247–53.
www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8 7
Review
18 Marino M, Morabito E, Altea MA, et al. Autoimmune hepatitis 40 Virakul S, Dalm VA, Paridaens D, et al. The tyrosine kinase
during intravenous glucocorticoid pulse therapy for Graves’ inhibitor dasatinib effectively blocks PDGF-induced orbital
ophthalmopathy treated successfully with glucocorticoids fibroblast activation. Graefes Arch Clin Exp Ophthalmol 2014;
themselves. J Endocrinol Invest 2005; 28: 280–84. 252: 1101–09.
19 Moli R, Baldeschi L, Saeed P, Regensburg N, Mourits MP, 41 Paridaens D, van den Bosch WA, van der Loos TL, Krenning EP,
Wiersinga WM. Determinants of liver damage associated with van Hagen PM. The effect of etanercept on Graves’
intravenous methylprednisolone pulse therapy in Graves’ ophthalmopathy: a pilot study. Eye 2005; 19: 1286–89.
ophthalmopathy. Thyroid 2007; 17: 357–62. 42 Durrani OM, Reuser TQ, Murray PI. Infliximab: a novel treatment
20 Sisti E, Coco B, Menconi F, et al. Age and dose are major risk for sight-threatening thyroid associated ophthalmopathy. Orbit
factors for liver damage associated with intravenous glucocorticoid 2005; 24: 117–19.
pulse therapy for Graves’ orbitopathy. Thyroid 2015; 25: 846–50. 43 Ayabe R, Rootman DB, Hwang CJ, Ben-Artzi A, Goldberg R.
21 Zang S, Ponto KA, Kahaly GJ. Clinical review: intravenous Adalimumab as steroid-sparing treatment of inflammatory-stage
glucocorticoids for Graves’ orbitopathy: efficacy and morbidity. thyroid eye disease. Ophthal Plast Reconstr Surg 2014; 30: 415–19.
J Clin Endocrinol Metab 2011; 96: 320–32. 44 Tan GH, Dutton CM, Bahn RS. Interleukin-1 (IL-1) receptor
22 Sisti E, Coco B, Menconi F, et al. Intravenous glucocorticoid therapy antagonist and soluble IL-1 receptor inhibit IL-1 induced
for Graves’ ophthalmopathy and acute liver damage: glycosaminoglycan production in cultured human fibroblasts from
an epidemiological study. Eur J Endocrinol 2015; 172: 269–76. patients with Graves’ ophthalmopathy. J Clin Endocrinol Metab 1996;
23 Giotaki Z, Fountas A, Tsirouki T, Bargiota A, Tigas S, Tsatsoulis A. 81: 449–52.
Adrenal reserve following treatment of Graves’ orbitopathy with 45 Smith TJ, Hegedus L, Douglas RS. Role of insulin-like growth
intravenous glucocorticoids. Thyroid 2015; 25: 462–63. factor-1 (IGF-1) pathway in the pathogenesis of Graves’ orbitopathy.
24 Gasinska T, Borowska A, Wichary H, Dec R. Effect of Best Pract Res Clin Endocrinol Metab 2012; 26: 291–302.
methylprednisolone pulse therapy with and without alendronate on 46 Kumar S, Nadeem S, Stan MN, Coenen M, Bahn RS. A stimulatory
biochemical markers of bone turnover in patients with Graves’ TSH receptor antibody enhances adipogenesis via phosphoinositide
ophthalmopathy. Pol Arch Med Wewn 2012; 122: 341–47. 3-kinase activation in orbital preadipocytes from patients with
25 Salvi M, Vannucchi G, Beck-Peccoz P. Potential utility of rituximab Graves’ ophthalmopathy. J Mol Endocrinol 2011; 46: 155–63.
for Graves’ orbitopathy. J Clin Endocrinol Metab 2013; 98: 4291–99. 47 Kumar S, Iver S, Bauer H, Coenen M, Bahn RS. A stimulatory
26 El Fassi D, Nielsen CH, Hasselbalch HC, Hegedus L. thyrotropin receptor antibody enhances hyaluronic acid synthesis in
Treatment-resistant severe, active Graves’ ophthalmopathy Graves’ orbital fibroblasts: inhibition by an IGF-1 receptor blocking
successfully treated with B lymphocyte depletion. Thyroid 2006; antibody. J Clin Endocrinol Metab 2012; 97: 1681–87.
16: 709–10. 48 Chen H, Mester T, Raychaudhuri N, et al. Teprotumumab, an
27 Salvi M, Vannuchi G, Campi I, et al. Efficacy of rituximab treatment IGF-1R blocking monoclonal antibody inhibits TSH and IGF-1
for thyroid-associated ophthalmopathy as a result of intraorbital action in fibrocytes. J Clin Endocrinol Metab 2014; 99: E1635–40.
B-cell depletion in one patient unresponsive to steroid 49 Kim TD, Rea D, Schwarz M, et al. Peripheral artery occlusive
immunosuppression. Eur J Endocrinol 2006; 154: 511–17. disease in chronic phase chronic myeloid leukemia patients treated
28 Krassas GE, Stafilidou A, Boboridis KG. Failure of rituximab with nilotinib or imatinib. Leukemia 2013; 27: 1316–21.
treatment in a case of severe thyroid ophthalmopathy unresponsive 50 Gerding MN, van der Zant FM, van Royen EA, et al.
to steroids. Clin Endocrinol 2010; 72: 853–55. Octreotide-scintigraphy is a disease-activity parameter in Graves’
29 Stan MN, Garrity JA, Carranza L, et al. Randomized controlled trial ophthalmopathy. Clin Endocrinol 1999; 50: 373–79.
of rituximab in patients with Graves’ orbitopathy. 51 Pasquali D, Vassallo P, Esposito D, Bonavolonta G, Bellastella A,
J Clin Endocrinol Metab 2015; 100: 432–41. Sinisi AA. Somatostatin receptor gene expression and inhibitory
30 Salvi M, Vannucchi G, Curro N, et al. Efficacy of B-cell targeted effects of octreotide on primary cultures of orbital fibroblasts from
therapy with rituximab in patients with active moderate-severe Graves’ ophthalmopathy. J Mol Endocrinol 2000; 25: 63–71.
Graves’ orbitopathy: a randomized controlled study. 52 Tanda ML, Bartalena L. Currently available somatostatin analogs are
J Clin Endocrinol Metab 2015; 100: 422–31. not good for Graves’ orbitopathy. J Endocrinol Invest 2006;
31 Van Geest RJ, Sasim IV, Koppeschaar HP, et al. Methylprednisolone 29: 389–390.
pulse therapy for patients with moderately severe Graves’ 53 Cozma I, Zhang L, Uddin J, Lane C, Rees A, Ludgate M.
orbitopathy: a prospective, randomized, placebo-controlled study. Modulation of expression of somatostatin receptor subtypes in
Eur J Endocrinol 2008; 158: 229–37. Graves’ ophthalmopathy orbits: relevance to novel analogs.
32 Wiersinga WM. Smoking and thyroid. Clin Endocrinol 2013; Am J Physiol Endocrinol Metab 2007; 293: E1630–35.
79: 145–51. 54 Bruns C, Lewis I, Briner U, Meno-Tetang G, Weckbecker G.
33 Khan A, Scott DL, Batley M. Smoking, rheumatoid factor status and SOM230: a novel somatostatin peptidomimetic with broad
responses to rituximab. Ann Rheum Dis 2012; 71: 1588–90. somatotropin release inhibiting factor (SRIF) receptor binding
34 Morshed SA, Davies TF. Graves’ disease mechanisms: the role of and a unique antisecretory profile. Eur J Endocrinol 2002;
stimulating, blocking, and cleavage region TSH receptor antibodies. 146: 707–16.
Horm Metab Res 2015; 47: 727–34. 55 Daifotis AG, Koenig S, Chatenoud L, et al. Anti-CD3 clinical trials
35 Furmaniak J, Sanders J, Nunez Miguel R, Rees Smith B. in type 1 diabetes mellitus. Clin Immunol 2013; 149: 268–78.
Mechanism of action of TSHR autoantibodies. Horm Metab Res 56 Herrero-Beaumont G, Martinez Calatrava MJ, Castaneda S.
2015; 47: 735–52. Abatacept mechanism of action: concordance with its clinical
36 Van Zeijl CJ, van Koppen CJ, Surovtseva OV, et al. profile. Reumatol Clin 2012; 8: 78–83.
Complete inhibition of rhTSH-, Graves’ disease IgG-, and 57 Anderton SM. Peptide immunotherapy in experimental
M22-induced cAMP production in differentiated orbital fibroblasts autoimmune encephalomyelitis. Biomed J 2015; 38: 206–214.
by a low-molecular-weight TSHR antagonist. 58 Bartalena L. Commentary: rituximab, adalimumab, etanercept,
J Clin Endocrinol Metab 2012; 97: E781–85. tocilizumab—are biologicals the future for Graves’ orbitopathy?
37 Turcu AF, Kumar S, Neumann S, et al. A small molecule antagonist Ophthal Plast Reconstr Surg 2014; 30: 420–23.
inhibits thyrotropin receptor antibody-induced orbital fibroblast 59 Wakelkamp IM, Gerding MN, van der Meer JW, Prummel MF,
functions involved in the pathogenesis of Graves’ ophthalmopathy. Wiersinga WM. Both Th1- and Th2-derived cytokines are elevated in
J Clin Endocrinol Metab 2013; 98: 2153–59. Grvaes’ ophthalmopathy. Clin Exp Immunol 2000; 121: 453–57.
38 Neumann S, Place RF, Krieger CC, Gershengorn MC. 60 Wakelkamp IM, Bakker O, Baldeschi L, Wiersinga WM,
Future prospects for the treatment of Graves’ hyperthyroidism and Prummel MF. TSH-R expression and cytokine profile in orbital
eye disease. Horm Metab Res 2015; 47: 789–96. tissue of active vs inactive Graves’ ophthalmopathy patients.
39 Virakul S, van Steensel L, Dalm VA, Paridaens D, van Hagen PM, Clin Endocrinol 2003; 58: 280–87.
Dik WA. Platelet-derived growth factor: a key factor in the 61 Perez-Moreiras JV, Alvarez-Lopez A, Gomez EC. Treatment of
pathogenesis of Graves’ ophthalmopathy and potential target for active corticosteroid-resistant Graves’ orbitopathy.
treatment. Eur Thyroid J 2014; 3: 217–26. Opthal Plast Reconstr Surg 2014; 30: 162–67.
8 www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8
Review
62 Yamamoto K, Goto H, Hirao K, et al. Longterm safety of 66 Yang M, Wiersinga WM, Soeters MR, Mourits MP. What is the aim
tocilizumab: results from 3 years of followup postmarketing of immunosuppressive treatment in patients with Graves’
surveillance of 5573 patients with rheumatoid arthritis in Japan. orbitopathy? Ophthal Plast Reconstr Surg 2014; 30: 157–61.
J Rheumatol 2015; 42: 1368–75. 67 Zhao SX, Tsui S, Cheung A, Douglas RS, Smith TJ, Banga JP.
63 Laurence DR. Clinical pharmacology, 3rd edn. London: Orbital fibrosis in a mouse model of Graves’ disease induced by
J & A Churchill, 1966. genetic immunization of thyrotropin receptor cDNA. J Endocrinol
64 Perros P, Zarkovic M, Azzolini C, et al. PREGO (presentation of 2011; 210: 369–77.
Graves’ orbitopathy) study: changes in referral patterns to European 68 Moshkelgosha S, So PW, Deasy N, Diaz-Cano S, Banga JP. Cutting
Group On Graves’ Orbitopathy (EUGOGO) centres over the period edge: retrobulbar inflammation, adipogenesis, and acute orbital
from 2000 to 2012. Br J Ophthalmol 2015; 99: 1531–35. congestion in a preclinical female mouse model of Graves’
65 Terwee CB, Dekker FW, Mourits MP, et al. Interpretation and orbitopathy induced by thyrotropin receptor plasmid-in vivo
validity of changes in scores on the Graves’ ophthalmopathy quality electroporation. Endocrinology 2013; 154: 3008–15.
of life questionnaire (GO-QoL) after different treatments.
Clin Endocrinol 2001; 54: 391–98.
www.thelancet.com/diabetes-endocrinology Published online June 23, 2016 http://dx.doi.org/10.1016/S2213-8587(16)30046-8 9
You might also like
- English - Basic Immunological Mechanism in Uveitis To Explain The Efficacy of Steroid and Immunosuppressive TreatmentDocument8 pagesEnglish - Basic Immunological Mechanism in Uveitis To Explain The Efficacy of Steroid and Immunosuppressive TreatmentardiansyahNo ratings yet
- Thyroid-Associated Ophthalmopathy: ReviewDocument12 pagesThyroid-Associated Ophthalmopathy: Reviewkevin_jawanNo ratings yet
- J, Kalita., Et Al. 2016Document6 pagesJ, Kalita., Et Al. 2016Ubaida AssalwaNo ratings yet
- Milta 2 - MarcadoDocument4 pagesMilta 2 - MarcadoVictor RoticivNo ratings yet
- New Drugs and Treatment Targets in Psoriasis: Review ArticleDocument7 pagesNew Drugs and Treatment Targets in Psoriasis: Review Article5netNo ratings yet
- Successful Management of Granulocytic Sarcoma With Co - 2016 - Pediatric HematolDocument2 pagesSuccessful Management of Granulocytic Sarcoma With Co - 2016 - Pediatric HematolHawin NurdianaNo ratings yet
- Jhe2021 6455659Document5 pagesJhe2021 6455659Septi MuninggarNo ratings yet
- 2016 Article 139Document10 pages2016 Article 139Naura Dhia FadylaNo ratings yet
- Nephrotic SyndromeDocument13 pagesNephrotic SyndromeImanuel Far-FarNo ratings yet
- Glutathione Peroxidase 1 Activity and Cardiovascular Events in Patients With Coronary Artery DiseaseDocument9 pagesGlutathione Peroxidase 1 Activity and Cardiovascular Events in Patients With Coronary Artery Diseaseapi-26034055No ratings yet
- Poster LESDocument6 pagesPoster LESAlejandra LuqueNo ratings yet
- An 1Document10 pagesAn 1Faqih SultonfaqNo ratings yet
- A Placebo-Controlled Trial of Oral Fingolimod in Relapsing Multiple SclerosisDocument15 pagesA Placebo-Controlled Trial of Oral Fingolimod in Relapsing Multiple SclerosisNidia BracamonteNo ratings yet
- Hormonal Therapies in Septic Shock: Review ArticleDocument8 pagesHormonal Therapies in Septic Shock: Review ArticleJhon3xNo ratings yet
- Cregan. 2016. KAT5 (Tip60) Is A Potential Therapeutic TargetDocument7 pagesCregan. 2016. KAT5 (Tip60) Is A Potential Therapeutic TargetAnonymous lXHxUzdc3No ratings yet
- Ref 12Document12 pagesRef 12Tiago BaraNo ratings yet
- DTSCH Arztebl Int-118 0680bDocument3 pagesDTSCH Arztebl Int-118 0680bkeisy MarquezNo ratings yet
- Olokizumab Versus Placebo or Adalimumab in Rheumatoid ArthritisDocument12 pagesOlokizumab Versus Placebo or Adalimumab in Rheumatoid ArthritisLee Foo WengNo ratings yet
- Lovastatin For The Treatment of Adult Patients With Dengue: A Randomized, Double-Blind, Placebo-Controlled TrialDocument9 pagesLovastatin For The Treatment of Adult Patients With Dengue: A Randomized, Double-Blind, Placebo-Controlled TrialBpmStfbNo ratings yet
- 10 5923 J Ijim 20150401 03 PDFDocument3 pages10 5923 J Ijim 20150401 03 PDFRiyan AdriyanNo ratings yet
- Overcoming Challenges in The Diagnosis and Treatment of Myasthenia GravisDocument13 pagesOvercoming Challenges in The Diagnosis and Treatment of Myasthenia GravisAndres MardonesNo ratings yet
- Medical Progress: Review ArticlesDocument12 pagesMedical Progress: Review ArticlesgibsonrajanNo ratings yet
- Ref 1Document7 pagesRef 1Tiago BaraNo ratings yet
- Rheumatology 05Document6 pagesRheumatology 05C Bala DiwakeshNo ratings yet
- Jem 20130084Document12 pagesJem 20130084Vivien WuNo ratings yet
- Fisetin Prevents Angiogenesis in Diabetic Retinopathy by Downregulating VEGFDocument7 pagesFisetin Prevents Angiogenesis in Diabetic Retinopathy by Downregulating VEGFvirginiaNo ratings yet
- European J of Heart Fail - 2019 - Markousis Mavrogenis - The Clinical Significance of Interleukin 6 in Heart FailureDocument9 pagesEuropean J of Heart Fail - 2019 - Markousis Mavrogenis - The Clinical Significance of Interleukin 6 in Heart FailureGenesis PerezNo ratings yet
- Lenalidomide Plus Prednisone Results in Durable Clinical, Histopathologic, and Molecular Responses in Patients With MyelofibrosisDocument7 pagesLenalidomide Plus Prednisone Results in Durable Clinical, Histopathologic, and Molecular Responses in Patients With MyelofibrosisRima RahmounNo ratings yet
- Systemic Immunomodulating Therapies For Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis A Systematic Review and Meta-AnalysisDocument9 pagesSystemic Immunomodulating Therapies For Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis A Systematic Review and Meta-AnalysisSri DarmayaniNo ratings yet
- Corticosteroid Adverse Effects - StatPearls - NCBI BookshelfDocument12 pagesCorticosteroid Adverse Effects - StatPearls - NCBI Bookshelfantonio.mastrangelo.999No ratings yet
- Antiphospholipid Syndrome A Review PDFDocument9 pagesAntiphospholipid Syndrome A Review PDFDiah Puspita RiniNo ratings yet
- Anti Thyroid AntibodyDocument16 pagesAnti Thyroid AntibodyFritz HaryadiNo ratings yet
- A Comprehensive Review of Current Treatments For Granulomatous Cheilitis (British Journal of Dermatology, Vol. 166, Issue 5) (2012)Document4 pagesA Comprehensive Review of Current Treatments For Granulomatous Cheilitis (British Journal of Dermatology, Vol. 166, Issue 5) (2012)Padmapriya SrinivasanNo ratings yet
- Polymer Drug Conjugates As Potent Against Cellular ApoptosisDocument8 pagesPolymer Drug Conjugates As Potent Against Cellular ApoptosisGourav DasNo ratings yet
- Radio-Contrast Agent-Induced Hyperthyroidism: Case Report and Review of The LiteratureDocument3 pagesRadio-Contrast Agent-Induced Hyperthyroidism: Case Report and Review of The LiteratureIwan SaputeraNo ratings yet
- Immunosuppressive Drug TherapyDocument25 pagesImmunosuppressive Drug Therapyapi-3741769100% (2)
- Notes To Remember: For Clinical Ophthalmology MCQ ExamsDocument89 pagesNotes To Remember: For Clinical Ophthalmology MCQ ExamsMohamed Gaber100% (1)
- Emerging Treatments For Crohn's Disease: Cells, Surgery, and Novel TherapeuticsDocument10 pagesEmerging Treatments For Crohn's Disease: Cells, Surgery, and Novel Therapeuticsellya theresiaNo ratings yet
- Terapia Inmunomoduladora 1Document9 pagesTerapia Inmunomoduladora 1Nathy Pasapera AlbanNo ratings yet
- 1 s2.0 S2095881118301379 MainDocument7 pages1 s2.0 S2095881118301379 MainAnita DewiNo ratings yet
- A Pragmatic Guide To Choosing Biologic Therapies in Severe AsthmaDocument15 pagesA Pragmatic Guide To Choosing Biologic Therapies in Severe Asthmahebert ramos100% (1)
- Avances en LESDocument8 pagesAvances en LESFranciscoJoseNo ratings yet
- Correspondence: Serotonin Syndrome Due To Co-Administration of Linezolid and VenlafaxineDocument2 pagesCorrespondence: Serotonin Syndrome Due To Co-Administration of Linezolid and Venlafaxineracm89No ratings yet
- Clinical Implication of Cyclophosphamide in Oncology, Hematology and Bone Marrow Transplantation (BMT)Document7 pagesClinical Implication of Cyclophosphamide in Oncology, Hematology and Bone Marrow Transplantation (BMT)International Journal of Innovative Science and Research TechnologyNo ratings yet
- He Ming 2018Document11 pagesHe Ming 2018Aulia RamadhaniNo ratings yet
- Nihms 690170Document10 pagesNihms 690170Dryuberth Alexander Pico MaciasNo ratings yet
- Wu 2016Document8 pagesWu 2016Anonymous n2DPWfNuNo ratings yet
- INSSafety BenningerDocument12 pagesINSSafety Benningerdr_ferryansofyanNo ratings yet
- Lee 2015Document9 pagesLee 2015BA OngNo ratings yet
- Scitranslmed Abb5817Document16 pagesScitranslmed Abb5817Andrew GrantNo ratings yet
- Research Article: SOCS1 Mimetic Peptide Suppresses Chronic Intraocular Inflammatory Disease (Uveitis)Document33 pagesResearch Article: SOCS1 Mimetic Peptide Suppresses Chronic Intraocular Inflammatory Disease (Uveitis)Paulus SidhartaNo ratings yet
- Clinical Characterization Cohort Systemic Lupus Erythematosus. PLoS One-2023Document14 pagesClinical Characterization Cohort Systemic Lupus Erythematosus. PLoS One-2023Jorge Ricardo Parra CamachoNo ratings yet
- Ferrara 2003Document8 pagesFerrara 2003Chaima DjabouNo ratings yet
- 1 Vol. 12 Issue 7 July 2021 IJPSR RA 15012Document16 pages1 Vol. 12 Issue 7 July 2021 IJPSR RA 15012VinayNo ratings yet
- Review On Pulse Therapy A Novel Approach in The Treatment of Pemphigus Vulgaris PDFDocument4 pagesReview On Pulse Therapy A Novel Approach in The Treatment of Pemphigus Vulgaris PDFtaniaNo ratings yet
- Jiw 632Document10 pagesJiw 632Robert StryjakNo ratings yet
- Hydroxychloroquine Effects On Mir-155-3P and Mir-219 Expression Changes in Animal Model of Multiple SclerosisDocument9 pagesHydroxychloroquine Effects On Mir-155-3P and Mir-219 Expression Changes in Animal Model of Multiple SclerosisAlvesnigelNo ratings yet
- Eritropoyesis Normal o Patologica en AdultosDocument11 pagesEritropoyesis Normal o Patologica en AdultosErikadelCorralNo ratings yet
- NIH Public Access: The Pathophysiology of Thyroid Eye Disease (TED) : Implications For ImmunotherapyDocument10 pagesNIH Public Access: The Pathophysiology of Thyroid Eye Disease (TED) : Implications For ImmunotherapySetiawan Arif WibowoNo ratings yet
- Creatinine Clearance: 58 Ml/min: Fasting Lipid ProfileDocument4 pagesCreatinine Clearance: 58 Ml/min: Fasting Lipid ProfileAnn DassNo ratings yet
- 5 Hospital CommunicationDocument11 pages5 Hospital CommunicationAtraoNo ratings yet
- Stock SekarangDocument26 pagesStock SekarangNita FitriNo ratings yet
- Immuno Multi Therapy and Prophylaxis Efficacy Against COVID 19Document9 pagesImmuno Multi Therapy and Prophylaxis Efficacy Against COVID 19Athenaeum Scientific PublishersNo ratings yet
- PCM PoisonDocument23 pagesPCM PoisonPrabhat KcNo ratings yet
- WFSA Craniopharyngioma Resection PDFDocument5 pagesWFSA Craniopharyngioma Resection PDFpitriaNo ratings yet
- JurnalDocument10 pagesJurnalZaoldyeck PutriNo ratings yet
- In Situ and Ex Vivo Nasal Models For Preclinical DDocument24 pagesIn Situ and Ex Vivo Nasal Models For Preclinical DEvelyn de OliveiraNo ratings yet
- TCCC-MP Test Answer Key 140602Document16 pagesTCCC-MP Test Answer Key 140602samfarmer333100% (2)
- BDS MBBS Concepts PharmacologyDocument117 pagesBDS MBBS Concepts PharmacologyKashmalaNo ratings yet
- Us 9241911Document63 pagesUs 9241911Scott DavisNo ratings yet
- Cardiology MnemonicDocument46 pagesCardiology MnemonicA.h.Murad100% (1)
- Meta Analysis DPP Plus SGPL2Document8 pagesMeta Analysis DPP Plus SGPL2Lokesh KhuranaNo ratings yet
- Choose The Correct Answer For Question (1 - 86)Document13 pagesChoose The Correct Answer For Question (1 - 86)Ahmed Fouad100% (2)
- PPT Farmakologi Molekuler Inflamasi - RA & IBDDocument40 pagesPPT Farmakologi Molekuler Inflamasi - RA & IBDVicko SuswidiantoroNo ratings yet
- Prescription 1680280210034Document3 pagesPrescription 1680280210034Vedant ChughNo ratings yet
- Renal TransplantationDocument33 pagesRenal TransplantationRohini Rai100% (1)
- Module 8 - Group 3Document16 pagesModule 8 - Group 3MEDECIELO MELONo ratings yet
- NainpreetDocument12 pagesNainpreetNainpreet KaurNo ratings yet
- Acute Rheumatic FeverDocument26 pagesAcute Rheumatic FeverAshvanee sharma100% (1)
- Obat Mendekati KadaluarsaDocument10 pagesObat Mendekati Kadaluarsadewi ayu kurniasariNo ratings yet
- Pharmacology and The Nursing Process Lilley 6th Edition Test BankDocument5 pagesPharmacology and The Nursing Process Lilley 6th Edition Test BankStephen Breedon100% (30)
- Pharmacy Study Plan2016eDocument41 pagesPharmacy Study Plan2016eأحمد العراقيNo ratings yet
- Acetylsalicylic AcidDocument5 pagesAcetylsalicylic Acidarfa shemnaNo ratings yet
- 353 Pharmacy Practice Lab IDocument4 pages353 Pharmacy Practice Lab IPharmacist Mohammed Abu SayeedNo ratings yet
- Cutaneous Reactions To Chemo and RadiotherapyDocument37 pagesCutaneous Reactions To Chemo and Radiotherapyimdad khanNo ratings yet
- Unit 5, Novel Drug Delivery Systems, B Pharmacy 7th Sem, Carewell PharmaDocument30 pagesUnit 5, Novel Drug Delivery Systems, B Pharmacy 7th Sem, Carewell Pharma47 DevendraNo ratings yet
- HPLC RifampicinDocument6 pagesHPLC RifampicinJatuna AyundaNo ratings yet
- ACTD Rev.1 Part IV Clinical DocumentDocument50 pagesACTD Rev.1 Part IV Clinical DocumentRaeanne SabadoNo ratings yet
- Gujarat Technological University: W.E.F. AY 2017-18Document3 pagesGujarat Technological University: W.E.F. AY 2017-18raj royelNo ratings yet
- The Age of Magical Overthinking: Notes on Modern IrrationalityFrom EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityRating: 4 out of 5 stars4/5 (32)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDFrom EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDRating: 5 out of 5 stars5/5 (3)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedFrom EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedRating: 4.5 out of 5 stars4.5/5 (82)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)From EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Rating: 3 out of 5 stars3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionFrom EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionRating: 4 out of 5 stars4/5 (404)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsFrom EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsNo ratings yet
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaFrom EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaRating: 4.5 out of 5 stars4.5/5 (266)
- To Explain the World: The Discovery of Modern ScienceFrom EverandTo Explain the World: The Discovery of Modern ScienceRating: 3.5 out of 5 stars3.5/5 (51)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeFrom EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeRating: 2 out of 5 stars2/5 (1)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsFrom EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsRating: 4 out of 5 stars4/5 (4)
- The Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeFrom EverandThe Twentysomething Treatment: A Revolutionary Remedy for an Uncertain AgeRating: 4.5 out of 5 stars4.5/5 (2)
- The Obesity Code: Unlocking the Secrets of Weight LossFrom EverandThe Obesity Code: Unlocking the Secrets of Weight LossRating: 4 out of 5 stars4/5 (6)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisFrom EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisRating: 4.5 out of 5 stars4.5/5 (42)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.From EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Rating: 4.5 out of 5 stars4.5/5 (110)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesFrom EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesRating: 4.5 out of 5 stars4.5/5 (1412)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsFrom EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsRating: 5 out of 5 stars5/5 (1)
- Critical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsFrom EverandCritical Thinking: How to Effectively Reason, Understand Irrationality, and Make Better DecisionsRating: 4.5 out of 5 stars4.5/5 (39)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeFrom EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeRating: 4.5 out of 5 stars4.5/5 (254)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsFrom EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsRating: 4.5 out of 5 stars4.5/5 (170)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryFrom EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryRating: 4 out of 5 stars4/5 (46)
- The Marshmallow Test: Mastering Self-ControlFrom EverandThe Marshmallow Test: Mastering Self-ControlRating: 4.5 out of 5 stars4.5/5 (60)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsFrom EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsNo ratings yet
- Hearts of Darkness: Serial Killers, The Behavioral Science Unit, and My Life as a Woman in the FBIFrom EverandHearts of Darkness: Serial Killers, The Behavioral Science Unit, and My Life as a Woman in the FBIRating: 4 out of 5 stars4/5 (20)