Professional Documents
Culture Documents
Introduction To Anemia
Uploaded by
genobisacn000 ratings0% found this document useful (0 votes)
3 views6 pagesAnemia is associated with decreased red blood cell mass and oxygen-carrying capacity of blood. It can be classified based on red blood cell morphology and underlying pathophysiological causes. Megaloblastic anemia is a macrocytic anemia where red blood cells have an MCV over 100 fL due to impaired DNA synthesis causing asynchronous nuclear and cytoplasmic development. Normocytic anemia has a normal MCV of 80-100 fL and requires examining red blood cell morphology to determine the cause of anemia. Laboratory diagnosis of anemia involves a complete blood count and red blood cell indices like MCV, MCH, and MCHC.
Original Description:
Original Title
INTRODUCTION-TO-ANEMIA
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentAnemia is associated with decreased red blood cell mass and oxygen-carrying capacity of blood. It can be classified based on red blood cell morphology and underlying pathophysiological causes. Megaloblastic anemia is a macrocytic anemia where red blood cells have an MCV over 100 fL due to impaired DNA synthesis causing asynchronous nuclear and cytoplasmic development. Normocytic anemia has a normal MCV of 80-100 fL and requires examining red blood cell morphology to determine the cause of anemia. Laboratory diagnosis of anemia involves a complete blood count and red blood cell indices like MCV, MCH, and MCHC.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
3 views6 pagesIntroduction To Anemia
Uploaded by
genobisacn00Anemia is associated with decreased red blood cell mass and oxygen-carrying capacity of blood. It can be classified based on red blood cell morphology and underlying pathophysiological causes. Megaloblastic anemia is a macrocytic anemia where red blood cells have an MCV over 100 fL due to impaired DNA synthesis causing asynchronous nuclear and cytoplasmic development. Normocytic anemia has a normal MCV of 80-100 fL and requires examining red blood cell morphology to determine the cause of anemia. Laboratory diagnosis of anemia involves a complete blood count and red blood cell indices like MCV, MCH, and MCHC.
Copyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 6
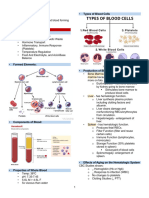
INTRODUCTION TO ANEMIA
ANEMIA (a Quantitative hematologic Physiologic Response to Anemia
disorder)
• Chemical and physical response
• Associated with decreased Red Cell o Compensations:
Mass (RCM) ▪ Shift to the right (↓ O2
o RCM: synonymous to affinity, ↑ 2,3- DPG)
circulating RBCs in the body ▪ Selective redistribution of
o Increased RCM: Polycythemia blood flow in areas with
and Erythrocytosis highest oxygen demand
• From Greek word “anaimia” meaning ▪ Increased cardiac output
“without blood” and RR
• Functional definition: Decreased in
oxygen carrying capacity of the blood Physiologic Response to Anemia
because of decrease RCM • Hematologic response
• Used to denote conditions association o Slower but more effective
with decreased RBCs and decreased o Kidney will Increased EPO (6-
Hb concentration which leads to 8x) takes 1 week
hypoxia ▪ Presence of "shift
• Classic symptoms of anemia: Fatigue reticulocytes" or Stress
and shortness of breath reticulocytes
o ↓ RCM • Larger (release
o ↓ Hb from bone
• Other symptoms marrow)
o Increased heart rate, RR • Immature retic
o Headache • 2-3 days before
o Chest pain it becomes
• In reference to hemoglobin levels mature – they
o Polycythemia and help because
erythrocytosis: in relation to these cells
hematocrit levels though they ae
o Suffix cytosis: Increase in the not yet fully
number of a specified type of mature they
cells have hemoglobin
o Suffix Polycythemia: Increase already where
new cell in the blood esp. RBC; oxygen can
Hypervolemia & hyper viscosity already bind for
▪ Absolute: True ↑ in the delivery of
RCM oxygen
▪ Relative: 2nd to • Increased RPI
change in plasma; it
(Retic Production
might be due to
Index) – useful
increase in the
tool in assessing
plasma volume of
if the bone
the blood
marrow is
responding
o Categories
adequately to
▪ Hypo-proliferative
anemia
anemia
▪ Maturation disorders
• Ineffective erythropoiesis
▪ Hemolytic disorders
o Refers to the production of
▪ Blood loss
erythroid precursor cells that
are defective
INTRODUCTION TO ANEMIA
o Defective RBC precursors
undergo apoptosis (natural
Two widely used classification schemes:
cell death)
Morphology of red blood cells and
o RBC production is high (↓ cells
pathophysiological conditions responsible for
in the circulation)
patients’ anemia
o Ex. Megaloblastic anemia
• Insufficient erythropoiesis CLASSIFICATION
o Refers to a decrease in the
number of erythroid Morphologic classification
precursors in the bone
marrow o Established using RBC
o Decreased RBC production indices and direct
examination of
LABORATORY DIAGNOSIS morphology using
peripheral blood smear
• Complete blood count with RBC o Anemia is classified
indices according to RBC size and
o CBC hemoglobin content
▪ Hematocrit • The MCV is the average
▪ Hemoglobin volume(size) of the RBC,
▪ RBC count expressed in femtoliters (fL), or
o RBC indices 10-15:
▪ MCV o MCV= Hct(%) x 10/RBC
▪ MCH count (x 1012/L)
▪ MCHC o Normal: 80-100 fL
• Reticulocyte count – whether the o Microcytic: < 80
bone marrow is responding to o Macrocytic >100
anemia
• Peripheral blood film
examination
o Color
o RBC inclusions; shape
o Anisocytosis - red blood
cells of varying sizes on
your blood smear
o Poikilocytosis - red blood • MCH is the average weight of
cells of varying shapes on hemoglobin in an RBC,
your blood smear expressed in picograms (pg), or
o Bone marrow 10-12 g:
examination- if hindi nila o MCH= Hb (g/dL) x 10/ RBC
ma pinpoint ang mismong count (x 1012/L)
cause ng anemia o Normal range: 26-32 pg
OTHER TESTS
• Urinalysis
• Occult blood test
• Serum haptoglobin
(intravascular hemolysis)
• Lactate dehydrogenase
• Bilirubin
• Renal and hepatic function test
INTRODUCTION TO ANEMIA
• MCHC is the average ▪ MCV up to 150 fL
concentration of hemoglobin in ▪ Caused by
each individual erythrocyte. The asynchrony between
units used are grams per nuclear and
deciliter (formerly given as cytoplasmic
percentage): development as a
o MCHC= Hb (g/dL) x 100/ result of impaired
Hct (%) DNA synthesis
o Normal range: 32-36 g/dL; o Macrocytic anemia (non-
Normochromic → pallor of megaloblastic)
1/3 ▪ MCV <115 fL
o Hypochromic: <32; pallor ▪ Related to
>1/3 membrane changes
Note: Hyperchromic – misnomer; no owing to disruption
such thing as that except spherocytes of the cholesterol-
to- phospholipid
ratio
o Normocytic Anemia
▪ MCV 80-100 fL
▪ RBC morphology
must be examined to
rule out dimorphic
(big and small cell)
population
▪ May be due to
premature
CLASSIFICATION destruction and
shortened survival of
• Morphologic classification: MCV RBCs
o Microcytic anemia + • Characterized
hypochromic by elevated
▪ MCV <80 fL (<6 um reticulocyte
in diameter) count
▪ MCHC<32 g/dL ▪ May be due to
(increased central decrease production
pallor) or RBCs
▪ Caused by • Characterized
conditions that result by decreased
in reduced reticulocyte
hemoglobin count
synthesis
o Macrocytic anemia
▪ MCV >100 fL (>8 um
in diameter)
▪ Caused by
conditions that result
in megaloblastic and
non-megaloblastic
red cell development
in the bone marrow
o Macrocytic anemia
(Megaloblastic)
INTRODUCTION TO ANEMIA
SITC: Sideroblastic anemia; Iron erythropoietic
deficiency anemia; Thalassemia; activity of the bone
Chronic inflammation marrow
o Reticulocyte
• MCV: represents the mean size ▪ Any nonnucleated
of the given heterogeneous RBC RBC that
population contains two or
☺ Does not reflect size variation more particles
with the population of blue—
stained
granulofilamentous
Red cell Distribution Width or RDW:
material after
index of variation of red cell volume
supravital staining:
☺ Size distribution measurement
Anisocytosis – if the red • In a slide drop
blood cell is malalki or blood (whole
maliliit blood; EDTA)
+ New
methylene
• RDW: coefficient of variation of blue (2-3
RBC volume expressed in drops w/o
percentage smearing) →
o Indicated the variation in incubate @RT
RBC volume for 3-10 mins
o Used in conjunction with = then smear
MCV ▪ Normallly: 0.5-
• RDW + MCV 2.0% in the
o Subclassification: circulation
o Normal RDW: ▪ Number of
homogeneous reticulocyte/1000
o Increased RDW: (RBCs observed) x
heterogeneous 100 = percentage
reticulocytes
• Example:
reticulocyte
(%) =
15/1000 x 100
= 1.5%
• Or the number
of reticulocyte
counted can
PHYSIOLOGIC CLASSIFICATION be multiplied
by 0.1
(100/1000) to
o Based on the ability of the bone
marrow to respond anemia with
increased erythropoiesis
o Assesses reticulocyte count and
RPI
o Reticulocyte count
▪ Serve as an
important tool to
assess
INTRODUCTION TO ANEMIA
obtain the
result.
• Adjustment in the reticulocyte count
due to the presence of shift
reticulocytes
• Reference range: An adequate
bone marrow response usually is
indicated by an RPI that is greater
than 3. An inadequate
erythropoietic response is seen
when RPI is less than 2.
• < 2.0
o Hypo proliferative
a. Normocytic,
Normochromic
b. Bone marrow
examination ex.
Aplastic anemia
o Maturation Disorder
a. Microcytic: low MCV;
nucleus mature, and
cytoplasm may
problema
• SIT-C: iron
deficiency,
heme problem,
or globin or
hemoglobin
problem→
Require iron
studies and Hb
electrophoresis
b. Macrocytic: depends
on the type of
megaloblastic or non;
delay of nuclear
Reticulocyte production index maturation compared
with cytoplasmic
o Useful when there is maturation
polychromasia→ pertains to • Megaloblastic:
150 fL –vitamin
RBC that has a bluish inch?
Under the microscope using B12/ folate def.
wright stain
• Non
megaloblastic <
115 fL—liver
disorder
INTRODUCTION TO ANEMIA
c. RPI >3.0
• Normo, Normo
(slightly increased
in MCV)
o Hemolytic
anemia—
caused by
hereditary or
acquired
either intrinsic
or extrinsic
defect →
Blood film for
detection of
Poikilocytoses
o Blood loss
ETIOLOGIC CLASSIFICATION
• Focuses on the principal underlying
pathophysiologic mechanisms
• Not reliable
Useful approach: taking patient
history and performing physical
examination
You might also like
- Notes On Blood BankingDocument99 pagesNotes On Blood Bankingapi-30646820490% (20)
- Heamatology Dr. Osama PDFDocument94 pagesHeamatology Dr. Osama PDFAnmar ZawahraNo ratings yet
- MicrobiologyDocument103 pagesMicrobiologyBhanu RajawatNo ratings yet
- Ninja Nerd AnemiaDocument13 pagesNinja Nerd AnemiaAndra Bauer100% (3)
- Hema Lec CompiledDocument68 pagesHema Lec Compiledchris andrieNo ratings yet
- Hematology Trans 10Document6 pagesHematology Trans 10Claire GonoNo ratings yet
- (PATHO) LEC 013 RBC-and-Bleeding-DisordersDocument20 pages(PATHO) LEC 013 RBC-and-Bleeding-DisordersEzhilNo ratings yet
- Anemia and Red Blood Cell Disorder Lecture by Dr. Rosales (Nov 6, 2017)Document7 pagesAnemia and Red Blood Cell Disorder Lecture by Dr. Rosales (Nov 6, 2017)Ian Gabrielle Mercado CuynoNo ratings yet
- Selective MediaDocument10 pagesSelective Mediaprincess_likemist4No ratings yet
- RBC DISORDERS StudentsDocument84 pagesRBC DISORDERS Studentskimberly abianNo ratings yet
- Sample MCQs of VirologyDocument4 pagesSample MCQs of VirologyTemesgen Endalew100% (2)
- 8C Summary SheetDocument2 pages8C Summary Sheet박찬우100% (2)
- (Trans) Chapter 16: Anemias - Red Blood Cell Morphology and Approach To DiagnosisDocument4 pages(Trans) Chapter 16: Anemias - Red Blood Cell Morphology and Approach To Diagnosisgotvelvet world dominationNo ratings yet
- RBC MorphologyDocument9 pagesRBC MorphologybiancsNo ratings yet
- Blood Pharmacology PDFDocument13 pagesBlood Pharmacology PDFManikanta GupthaNo ratings yet
- Chapter 1 - Introduction To HematologyDocument9 pagesChapter 1 - Introduction To HematologyMonica DomingoNo ratings yet
- Chapter Five To Seven ReviewDocument12 pagesChapter Five To Seven ReviewToshNikolNo ratings yet
- HEMATOLOGY (Week 2) LABDocument8 pagesHEMATOLOGY (Week 2) LABJessica PontanaresNo ratings yet
- (MT 56) HISTO - Blood and HemopoeisisDocument9 pages(MT 56) HISTO - Blood and HemopoeisisLiana JeonNo ratings yet
- Hema 11-ReviewerDocument59 pagesHema 11-ReviewerMJ ArboledaNo ratings yet
- Physiotherapy Blood Investigations JPDocument51 pagesPhysiotherapy Blood Investigations JPJesusNavarrete97No ratings yet
- Hematology Pathology - 002) CBC - Approach To Polycythemia (Notes)Document4 pagesHematology Pathology - 002) CBC - Approach To Polycythemia (Notes)Aro DanaNo ratings yet
- Anemia & Sickle Cell AnemiaDocument5 pagesAnemia & Sickle Cell AnemiaDIANA CAMILLE CARITATIVONo ratings yet
- Hematology CHapter 1Document3 pagesHematology CHapter 1Rheila DuyaNo ratings yet
- Anatomy and Physiology With PhatophysiologyDocument6 pagesAnatomy and Physiology With PhatophysiologyJustine Mae OyongNo ratings yet
- Hematology Week 4 PDFDocument9 pagesHematology Week 4 PDFKenj Yolleth IbañezNo ratings yet
- Anemias: RBC Morphology & Approach To Diagnosis: Physiologic AdaptationsDocument5 pagesAnemias: RBC Morphology & Approach To Diagnosis: Physiologic AdaptationsASHLEY ALEXIS GUEVARRANo ratings yet
- CP RBC DisorderDocument15 pagesCP RBC DisorderDETECTIVE CONANNo ratings yet
- Hereditary Red Blood Cell Membrane AbnormalitiesDocument29 pagesHereditary Red Blood Cell Membrane AbnormalitiesKristine Mae D. GregorioNo ratings yet
- 1.07 - The BloodDocument5 pages1.07 - The Blood13PLAN, SENTH RUEN, ANo ratings yet
- vt59.2708-21242375124 394146998891967 4683953301704066077 n.pdfHEMA-HANDOUTS-1.pdf NC Cat 106&ccb 1-7&Document15 pagesvt59.2708-21242375124 394146998891967 4683953301704066077 n.pdfHEMA-HANDOUTS-1.pdf NC Cat 106&ccb 1-7&jasminemuammilNo ratings yet
- HEMA 2 - Midterm Topic 1 - ADDITIONAL NOTESDocument6 pagesHEMA 2 - Midterm Topic 1 - ADDITIONAL NOTESLowenstein JenzenNo ratings yet
- Physiology Lecture 2: RBC S Characteristics, Function and FormationDocument20 pagesPhysiology Lecture 2: RBC S Characteristics, Function and FormationdarkboiNo ratings yet
- 2 Red Blood CellsDocument14 pages2 Red Blood CellsJezreelyan VillanuevaNo ratings yet
- 112 Lecture MidtermsDocument18 pages112 Lecture MidtermsRose Ann CammagayNo ratings yet
- 112 Lecture MidtermsDocument8 pages112 Lecture MidtermsRose Ann CammagayNo ratings yet
- Mtap 2 HematologyDocument15 pagesMtap 2 HematologyNaomi NicoleNo ratings yet
- Cardiovascular System - BloodDocument8 pagesCardiovascular System - BloodVernice LopezNo ratings yet
- Clinpath - : Red Blood CellsDocument14 pagesClinpath - : Red Blood CellsYolanda Primrosa NurhanNo ratings yet
- RBC PathologyDocument7 pagesRBC PathologyKent CruzNo ratings yet
- Midterm Topics Hema 1 LecDocument37 pagesMidterm Topics Hema 1 Lec4jzbxz64kqNo ratings yet
- Blood 2Document4 pagesBlood 2Jhes D.No ratings yet
- LEC 5 RBC METABOLISM AND Membrane StructureDocument30 pagesLEC 5 RBC METABOLISM AND Membrane StructureFrancis ValdezNo ratings yet
- Blood and LymphaticDocument4 pagesBlood and LymphaticCKNo ratings yet
- HEMA311LECWEEK2Document3 pagesHEMA311LECWEEK2Daphlene Kayt A. MapoyNo ratings yet
- Blood Lectures 2 2017Document41 pagesBlood Lectures 2 2017Philip Abayomi VincentNo ratings yet
- Lee EllenCLPC Spring 2017 - CBC ColorDocument13 pagesLee EllenCLPC Spring 2017 - CBC ColorChristine Joy MolinaNo ratings yet
- Chapter 10 BloodDocument3 pagesChapter 10 BloodinitaygracileshayneNo ratings yet
- AnemiaDocument29 pagesAnemiaShahid F.S.D.No ratings yet
- 219 D2 - Blood TransfusionDocument5 pages219 D2 - Blood TransfusionAngelina Mei BenitezNo ratings yet
- Hema FinalsDocument12 pagesHema FinalsHANA LUNARIANo ratings yet
- Lecture Lesson 9. Red Blood Cell DisordersDocument7 pagesLecture Lesson 9. Red Blood Cell DisordersHANA LUNARIANo ratings yet
- Hemolytic Anemia IntrinsicDocument14 pagesHemolytic Anemia IntrinsicSophia Gail ChingNo ratings yet
- Approach To Anemia: - Reticulocyte Count Is Most Important TestDocument15 pagesApproach To Anemia: - Reticulocyte Count Is Most Important TestJanella SuerteNo ratings yet
- U. 6 Blood FunctionsDocument41 pagesU. 6 Blood FunctionsRania HamamNo ratings yet
- RBC Anomalies: I. Variation in Hemoglobin ContentDocument6 pagesRBC Anomalies: I. Variation in Hemoglobin ContentMARIE NELLIE MOSTRADONo ratings yet
- Introduction To HematologyDocument2 pagesIntroduction To HematologyMary Joy HersaliaNo ratings yet
- FR2 PDFDocument4 pagesFR2 PDFRaphael Joshua De GuzmanNo ratings yet
- Hematology: AbbreviationsDocument5 pagesHematology: AbbreviationsReyven Niña DyNo ratings yet
- CBC (Complete Blood Count)Document38 pagesCBC (Complete Blood Count)yeshitla amsaluNo ratings yet
- Anemia, Polycythemia and Jaundice PDFDocument5 pagesAnemia, Polycythemia and Jaundice PDFAnshumaan PatraNo ratings yet
- Anemia OsamaDocument57 pagesAnemia Osamaosamafoud7710No ratings yet
- Feline Nonregenerative Anemia Pathophysiology and ErilologiesDocument7 pagesFeline Nonregenerative Anemia Pathophysiology and ErilologiesTORRES GUTIERREZ JOYNY RAQUEL catedraticoNo ratings yet
- Body Fluids and Circulation - Mind Maps - Arjuna NEET 2024Document5 pagesBody Fluids and Circulation - Mind Maps - Arjuna NEET 2024aashish.tskauthNo ratings yet
- Sheetal GaonkarogDocument2 pagesSheetal Gaonkarognadar.rajNo ratings yet
- Laboratory Results and Interpretations of AGEDocument2 pagesLaboratory Results and Interpretations of AGEYnah Sayoc100% (3)
- LP 4-ImmunoprophylaxisDocument15 pagesLP 4-ImmunoprophylaxismlinaballerinaNo ratings yet
- EnterobacteriaceaeDocument35 pagesEnterobacteriaceaeFaisal AbbasNo ratings yet
- STD Pre TestDocument2 pagesSTD Pre TestCrystal Ann Monsale TadiamonNo ratings yet
- Micro Notes 1Document3 pagesMicro Notes 1roldanNo ratings yet
- Lecture 16 Escherichia ColiDocument18 pagesLecture 16 Escherichia ColiKhawla AliNo ratings yet
- Sop For Thalassemia Screening Wwith NbsDocument11 pagesSop For Thalassemia Screening Wwith NbsUMMID WashimNo ratings yet
- Quiz 2Document5 pagesQuiz 2Ramesh KumarNo ratings yet
- Blood Products. Preparation of Blood ComponentsDocument32 pagesBlood Products. Preparation of Blood ComponentsSanthiya MadhavanNo ratings yet
- Lectura InglesDocument1 pageLectura InglesliaguerreroNo ratings yet
- SVLT Lab Report DetailsDocument2 pagesSVLT Lab Report DetailsKirtivaan MishraNo ratings yet
- Antimicrobial Activity of Leaf Extracts of Asparagus Racemosus Willd-A Medicinal PlantDocument3 pagesAntimicrobial Activity of Leaf Extracts of Asparagus Racemosus Willd-A Medicinal PlantIJSTANo ratings yet
- Chicken Embryo Inoculation As A Diagnostic ToolDocument29 pagesChicken Embryo Inoculation As A Diagnostic ToolAdarshBijapur100% (1)
- VMD-422 Questions - (II)Document8 pagesVMD-422 Questions - (II)ਰੋਹਿਤ ਬਾਵਾNo ratings yet
- Management of HemorrhageDocument11 pagesManagement of HemorrhageClara VerlinaNo ratings yet
- Bacterial Detection Live Dead PDFDocument6 pagesBacterial Detection Live Dead PDFMuhamad ZakyNo ratings yet
- Texas Children's Hospital 5 Annual Advanced Practice Provider ConferenceDocument64 pagesTexas Children's Hospital 5 Annual Advanced Practice Provider ConferenceEngSabbaghNo ratings yet
- Blood Bank ProposalDocument31 pagesBlood Bank Proposalzfnef608No ratings yet
- Human Virus Families and Their DiseasesDocument1 pageHuman Virus Families and Their DiseasesKate EvangelistaNo ratings yet
- Klebsiella Sp. Epidemiology Taxonomy and PatogenicityDocument15 pagesKlebsiella Sp. Epidemiology Taxonomy and PatogenicityDulce MariaNo ratings yet
- Hema I Chapter 12 - ESRDocument30 pagesHema I Chapter 12 - ESRTesfaNo ratings yet
- AnaisDocument272 pagesAnaisJean Gabriel V. Coutinho100% (2)
- Hematology 1 (Laboratory) - Week 10-11 ModuleDocument8 pagesHematology 1 (Laboratory) - Week 10-11 ModuleJam RamosNo ratings yet