Professional Documents
Culture Documents
Eat 22242
Uploaded by
Ma José EstébanezOriginal Description:
Original Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Eat 22242
Uploaded by
Ma José EstébanezCopyright:
Available Formats
BRIEF REPORT
A Randomized Controlled Trial of Motivational
Interviewing 1 Self-Help Versus Psychoeducation 1
Self-Help for Binge Eating
Rachel A. Vella-Zarb, MA1* ABSTRACT
Objective: Motivational Interviewing
completed pre- and postsession, and at 1
and 4 months postsession.
Jennifer S. Mills, PhD1 (MI) is a collaborative therapy that focuses
Results: MI significantly increased
Henny A. Westra, PhD1 on strengthening a person’s internal
readiness to change and confidence in
Jacqueline C. Carter, PhD2 motivation to change. Research suggests
that MI may be helpful for treating binge ability to control binge eating, whereas
Leah Keating, MA1 eating; however, findings are limited and
psychoeducation did not. No group
little is known about how MI for binge differences were found when changes
in eating disorder attitudes and behav-
eating compares to active therapy con-
iors were examined.
trols. The present study aimed to build
on current research by comparing MI as Discussion: MI offers benefits for
a prelude to self-help treatment for binge increasing motivation and self-efficacy.
eating with psychoeducation as a prelude However, it may not be a uniquely
to self-help treatment for binge eating. effective treatment approach for reduc-
ing binge eating. V
C 2014 Wiley Periodi-
Method: Participants with full or sub-
threshold DSM-IV Binge Eating Disorder cals, Inc.
or nonpurging Bulimia Nervosa were ran-
Keywords: binge eating disorder;
domly assigned to receive either 60
minutes of MI followed by a self-help motivation; randomized controlled trial;
binge eating; self-help; psychoeducation
manual (n 5 24) or 60 minutes of psy-
choeducation followed by a self-help
manual (n 5 21). Questionnaires were (Int J Eat Disord 2015;48:328–332)
Introduction study,7 90 adults with full or subthreshold Bulimia
Nervosa (BN) or BED were randomly assigned to
Motivational Interviewing (MI) is a client-centered receive either one session of an adaptation of MI,
psychotherapy that aims to enhance motivation to called Motivational Enhancement Therapy
change through the use of empathy and directive (MET), followed by a self-help manual or self-
techniques.1,2 There has been interest in using MI help alone. MET resulted in increased readiness
for treating eating disorders (EDs) because of high to change binge eating and a significantly greater
rates of ambivalence about treatment in this popu- proportion of participants were abstinent from
lation3; however, findings are limited.4,5 Support to binge eating in the MET (24.4%) versus self-help
date is strongest for using MI as treatment for only condition (8.9%). In the second study,6 108
binge eating.4 women with BED were randomly assigned to
Two studies have examined the efficacy of MI receive either one session of MI followed by a
for Binge Eating Disorder (BED).6,7 In the first self-help manual or self-help alone. MI partici-
pants reported significantly greater self-efficacy
and greater improvements in binge eating, mood,
Accepted 22 December 2013 self-esteem, and quality of life. Although findings
Partial support for this research was provided by the Social Sci- are promising, implications are limited given that
ences and Humanities Research Council of Canada (SSHRC) Joseph
Armand-Bombardier Canada Graduate Scholarship, awarded to
both studies compared MI 1 self-help to self-help
Rachel Vella-Zarb. There are no known conflicts of interest. alone. It is unclear whether there is something
*Correspondence to: Rachel Vella-Zarb; York University, Faculty specific about MI that makes it an effective prel-
of Health, 4700 Keele Street, Toronto, Ontario M3J 1P3, Canada.
E-mail: rachelvz@yorku.ca
ude to treatment or whether there are other non-
1
York University, Toronto, Ontario, Canada specific factors that lead to benefits (e.g.,
2
Memorial University, St. John’s, Newfoundland, Canada therapist contact). Therefore, it is important to
Published online 13 January 2014 in Wiley Online Library
(wileyonlinelibrary.com). DOI: 10.1002/eat.22242
examine how MI for BED compares to an active
VC 2014 Wiley Periodicals, Inc. therapy control.
328 International Journal of Eating Disorders 48:3 328–332 2015
A RANDOMIZED CONTROLLED TRIAL FOR BINGE EATING
FIGURE 1 Summary of participant flow. MI, motivational interviewing. *Excluded as an outlier due to session length.
The present study built on previous research Method
by comparing one session of MI followed by a
self-help manual to one session of psychoeduca- Participants and Procedure
tion followed by a self-help manual for individu- The York University Psychology Research Ethics Board
als with clinically significant binge eating approved this study. Data collection occurred between
problems. Psychoeducation was chosen for com- September 2011 and August 2012. Participation involved
parison because it has been shown to be an informed consent. Participants were recruited from York
effective psychotherapeutic approach for treating University and the community. A priori power calcula-
binge eating and is often used as the first step in tions indicated a minimum overall sample of 38 partici-
stepped care treatment.8 The primary aim was to pants was necessary for an 80% chance of detecting
test the hypothesis that MI 1 self-help would significant effects on primary outcomes (p 5 .05).
lead to greater improvements in ED behaviors, Participants were required to meet full or subthreshold
attitudes, and abstinence from binge eating. The DSM-IV criteria for BED or Bulimia Nervosa, Non-
secondary aim was to examine whether MI Purging Subtype (BN-NP)a. “Subthreshold” was defined
would lead to greater improvements in readiness
to change and self-efficacy than would
psychoeducation.
a
It should be noted that DSM-5 no longer requires the identification
of Bulimia Nervosa subtypes.
International Journal of Eating Disorders 48:3 328–332 2015 329
VELLA-ZARB ET AL.
as one binge eating episode per week for 3 months. Par- years), and mean BMI was 27.06 (SD 5 6.54). Four partic-
ticipants were excluded if they were under 18, met crite- ipants (8.9%) were participating in psychotherapy for
ria for substance abuse, had diabetes, were pregnant, mood-related problems at prescreening (MI: n 5 3, psy-
were not proficient in English, expressed active suicidal choeducation: n 5 1). Approximately 73% of participants
ideation, had been using psychiatric medication for (n 5 33) met full (n 5 16) or subthreshold (n 5 17) criteria
under 3 months or dosage had varied over the previous 3 for BED; 27% (n 5 12) met full (n 5 8) or subthreshold
months. Eligibility was determined by an online ques- (n 5 4) criteria for BN-NP.
tionnaire and Structured Clinical Interview for DSM-IV
Disorders (SCID) ED section completed via telephone,
with binge eating frequency modified to study criteria. Results
Forty-seven participants were eligible to participate
Missing Data and Attrition
and were randomly assigned to condition, stratifying for
current involvement in psychotherapy. Randomization The majority of missing data were because of
was performed by an arms-length researcher using SPSS. inability to reach participants at follow-up.
Enrollment and assignment were performed by the first Attrition rate was 22.22% (n 5 10). There were no
author. Allocation was 1:1 in a parallel groups design. significant group differences in attrition. Compari-
Participants were blind to treatment assignment until son of completers and noncompleters on all meas-
after completing baseline measures. Following study ured variables revealed no significant differences.
completion, one participant from each group was Multiple imputation was used to estimate missing
removed as an outlier based on session length (psycho- datad.
education 5 27.03 minutes, MI 5 83.07 minutes), leaving Primary Outcomes. Eating disorder behaviors and atti-
a total of 45 participants (psychoeducation n 5 21; MI tudese. A repeated measures ANOVA showed a sig-
n 5 24) (see Fig. 1). nificant main effect of time on EDE-Q global
Following assignment, participants completed ques- scores, F(1.95, 83.67) 5 13.47, p < .001, gp2 5 0.24,
tionnaires assessing ED symptoms (Eating Disorder indicating an overall decrease in ED symptoms
Examination Questionnaire – EDE-Q), readiness to across groups. Significant changes occurred
change (University of Rhode Island Stages of Change between baseline and 1 month, F(1, 32) 5 19.87,
Assessment – URICA), and eating self-efficacy (Weight p < .001, gp2 5 0.31, and baseline and 4 months,
Efficacy Lifestyle Questionnaire – WEL). They then par- F(1, 43) 5 18.87, p < .001, gp2 5 0.30 only. No signifi-
ticipated in the intervention session to which they were cant Group 3 Time interaction was found (see
assignedb. The first author conducted all therapy ses- Table 1).
sions to control for potential discrepancies as a redult of Binge Eating Abstinence. Abstinence from binge
therapist characteristicsc. Mean MI session length was eating did not differ between groups at 1 month
55.76 minutes (SD 5 7.03) and mean psychoeducation (Fisher’s Exact Test: p 5 .71; 14% of psychoeduca-
session length was 49.73 minutes (SD 5 7.03); they were tion participants reported no binges in the previous
not statistically significantly different. month versus 21% of MI participants). At 4 months,
Following session completion, participants were given group differences were still not statistically signifi-
the self-help manual, Overcoming Binge Eating9 and cant, v2 (N545) 5 2.55, p 5 .15; 19% psychoeduca-
completed measures examining readiness to change tion versus 46% MI).
(URICA) and self-efficacy (WEL). One and 4 months Secondary Outcomes. Readiness to Change. A
later, participants were contacted via email to complete repeated measures ANOVA revealed a main effect
online follow-up questionnaires assessing ED symptoms of time on the URICA readiness composite,
(EDE-Q). F(1, 43) 5 16.31, p < .001, gp2 5 0.28. This finding
The majority of participants were Caucasian (77.8%)
and female (95.6%), mean age was 24.88 years (SD 5 6.91
d
Multiple imputation is highly recommended for dealing with missing
data because it eliminates problems associated with case-wise deletion,
such as reductions in power and loss of potentially predictive informa-
b
Complete protocol for both interventions is available by request from tion, and is not subject to many of the same biases as other imputation
the first author. There was no overlap in material between the two inter- methods. Although research indicates that multiple imputation is an
vention sessions. acceptable approach for minimizing bias because of missing data in lon-
c
In preparation, the first author (a senior-level PhD Clinical Psychol- gitudinal studies, all hypotheses were additionally tested using complete
ogy student) participated in a multiday MI training led by William Miller case analysis and results were compared. Findings indicated that results
and attended additional MI workshops. To ensure treatment protocols were comparable.
e
were followed in both conditions, two registered clinical psychologists Sphericity was violated for repeated measures ANOVAs examining
(Drs. Jennifer Mills and Henny Westra) reviewed a random selection of changes on the EDE-Q total. To account for this, Greenhouse-Geisser cor-
audiotaped sessions and provided clinical supervision. rections were used.
330 International Journal of Eating Disorders 48:3 328–332 2015
A RANDOMIZED CONTROLLED TRIAL FOR BINGE EATING
TABLE 1. Means and standard deviation by treatment group at all time points
PED baseline MI baseline PED post-session MI post-session PED 1-month MI 1-month PED 4-months MI 4-months
(N 5 21) (N 5 24) (N 5 21) (N 5 24) (N 5 21) (N 5 24) (N 5 21) (i5 24)
Variables M (SD) M (SD) M (SD) M (SD) M (SD) M (SD) M (SD) M (SD)
URICA Readiness 10.27 9.25 10.52 10.24 ___ ___ ___ ___
Compositea,b
(1.69) (1.85) (1.28) (1.35)
WEL Totala,b 71.62 72.83 73.04 92.39 ___ ___ ___ ___
(28.18) (25.80) (27.12) (26.07)
b
EDE-Q Global 3.48 3.46 ___ ___ 2.70 2.81 2.59 2.70
(0.90) (1.35) (1.00) (1.12) (1.19) (1.21)
a
p < .05 significant group 3 time interaction.
b
p < .01 significant main effect of time.
PED 5 Psychoeducation, MI 5 Motivational Interviewing, URICA 5 University of Rhode Island Stages of Change Assessment Scale, WEL 5 Weight Efficacy
Lifestyle Questionnaire, EDE-Q 5 Eating Disorder Examination Questionnaire.
was qualified by a significant Group 3 Time improved efficacy, although MI is intended to be
interaction, F(1, 43) 5 5.59, p 5 .02, gp2 5 0.12. MI brief, typically one or two sessions.1 Third, out-
participants showed a significant increase in readi- comes were measured by self-report question-
ness from pre- to postsession, t(23) 5 24.11, naires, which can be subject to bias; using a
p < .001, d 5 0.61, whereas psychoeducation partic- clinical interview to assess changes may have
ipants did not, t(20) 5 21.41, p 5 .17, d 5 0.17 (see been preferable. However, self-report measures
Table 1). reduce participant burden, which is important
Eating Self-Efficacy. A repeated measures ANOVA when measurements are frequent as in this study.
showed a main effect of time on self-efficacy meas- Fourth, all therapy sessions were conducted by a
ured by the WEL, F(1, 43) 5 9.19, p 5 .004, single therapist who was not blind to study
gp2 5 0.18. A significant Group 3 Time interaction hypotheses. Although she worked to ensure equiv-
was also found, F(1, 43) 5 6.87, p 5 .01, gp2 5 0.14. alent treatment across conditions, allegiance
MI participants displayed a significant increase effects remain a possibility. Fifth, this study did
in self-efficacy from pre- to postsession, t(20) 5 not include a “no treatment” control; findings
24.03, p 5 .001, d 5 0.75, whereas psychoeducation cannot rule out the possibility of regression to the
participants did not, t(20) 5 20.29, p 5 .78, d 5 0.05 mean.
(see Table 1). Findings indicate that MI is more effective than
psychoeducation at increasing readiness to
change and self-efficacy in individuals who binge
Discussion eat. However, MI 1 self-help does not appear to
offer any unique benefit for reducing binge
The purpose of this study was to compare MI as a eating.
prelude to self-help for binge eating to psycho-
education as a prelude to self-help for binge
eating. Participants in both groups showed signifi- References
cant and equivalent improvements in ED symp-
toms. MI led to significant increases in readiness 1. Miller WR, Rollnick S, Motivational interviewing: Preparing people for
to change and self-efficacy, whereas psychoeduca- change (2nd ed.). Motivational interviewing: Preparing people for change,
tion did not. Second ed. New York, NY: Guilford Press, 2002.
2. Miller WR, Rollnick S, Motivational interviewing: Helping people change.
This study has numerous strengths: an RCT Applications of motivational interviewing, Third ed. New York, NY: Guilford
design was employed, an active therapy compari- Press, 2012.
son group was used, and the interventions utilized 3. Geller J, Dunn EC. Integrating motivational interviewing and cognitive
were brief, inexpensive, and could be easily put behavioral therapy in the treatment of eating disorders: Tailoring interven-
into practice. This study also has its limitations. tions to patient readiness for change. Cogn Behav Pract 2011;18:5–15.
4. Knowles L, Anohkina S, Serpell L. Motivational interventions in the eating
First, sample size was small, but comparable to
disorders: What is the evidence? Int J Eat Disord 2013;46:97–107.
other studies examining MI for EDs.10–12 Second, 5. Macdonald P, Hibbs R, Corfield F, Treasure J. The use of motivational inter-
treatment involved only one 60-minute interven- viewing in eating disorders: A systematic review. Psychiatr Res 2012;200:
tion session. Adding multiple sessions may have 1–11.
International Journal of Eating Disorders 48:3 328–332 2015 331
VELLA-ZARB ET AL.
6. Cassin SE, von Ranson KM, Heng K, Brar J, Wojtowicz AE. Adapted motiva- 10. Dean HY, Touyz SW, Rieger E, Thornton CE. Group motivational enhance-
tional interviewing for women with binge eating disorder: A randomized ment therapy as an adjunct to inpatient treatment for eating disorders: A
controlled trial. Psychol Addict Behav 2008;22:417–425. preliminary study. Eur Eat Disord Rev 2008;16:256–267.
7. Dunn EC, Neighbors C, Larimer ME. Motivational enhancement therapy and 11. Feld R, Woodside DB, Kaplan AS, Olmsted MP, Carter JC. Pretreatment moti-
self-help treatment for binge eaters. Psychol Addict Behav 2006;20:44–52. vational enhancement therapy for eating disorders: A pilot study. Int J Eat
8. Wilson GT, Vitousek KM, Loeb KL. Stepped care treatment for eating disor- Dis 2001;29:393–400.
ders. J Consult Clin Psychol 2000;68:564–572. 12. Wade TD, Frayne A, Edwards S-A, Robertson T, Gilchrist P. Motivational
9. Fairburn CG, Overcoming Binge Eating. New York, NY: The Guilford Press, change in an inpatient anorexia nervosa population and implications for
1995. treatment. Aust N Z J Psychiatry 2009;43:235–243.
332 International Journal of Eating Disorders 48:3 328–332 2015
Copyright of International Journal of Eating Disorders is the property of John Wiley & Sons,
Inc. and its content may not be copied or emailed to multiple sites or posted to a listserv
without the copyright holder's express written permission. However, users may print,
download, or email articles for individual use.
You might also like
- Blueprints PsychiatryDocument432 pagesBlueprints PsychiatryFiona Fleming86% (14)
- Binge Killer The Use of Cognitive Behavioral Therapy to Address Shame in Binge Eating DisorderFrom EverandBinge Killer The Use of Cognitive Behavioral Therapy to Address Shame in Binge Eating DisorderRating: 2 out of 5 stars2/5 (1)
- Indian Company ListDocument1,230 pagesIndian Company ListSanjukta Nandi74% (70)
- Oxford Offer LetterDocument10 pagesOxford Offer LetterAlexánder Muñoz Ferrer100% (3)
- Armodafinil in Binge Eating Disorder A RandomizedDocument7 pagesArmodafinil in Binge Eating Disorder A RandomizedQuel PaivaNo ratings yet
- The Non-Diet Approach Guidebook for Dietitians (2013): A how-to guide for applying the Non-Diet Approach to Individualised Dietetic CounsellingFrom EverandThe Non-Diet Approach Guidebook for Dietitians (2013): A how-to guide for applying the Non-Diet Approach to Individualised Dietetic CounsellingNo ratings yet
- Full Download Test Bank For Tietz Fundamentals of Clinical Chemistry and Molecular Diagnostics 7th Edition by Burtis PDF Full ChapterDocument35 pagesFull Download Test Bank For Tietz Fundamentals of Clinical Chemistry and Molecular Diagnostics 7th Edition by Burtis PDF Full Chapterseesaw.insearchd8k4100% (23)
- Presentation On Hospital Management PolicyDocument11 pagesPresentation On Hospital Management PolicyMiriam ChristopherNo ratings yet
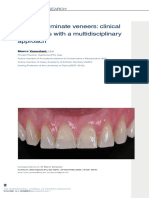
- Ceramic Laminate Veneers: Clinical Procedures With A Multidisciplinary ApproachDocument23 pagesCeramic Laminate Veneers: Clinical Procedures With A Multidisciplinary ApproachBenjiNo ratings yet
- Warren 2017Document12 pagesWarren 2017pimpamtomalacasitosNo ratings yet
- Schmidt2007 PDFDocument8 pagesSchmidt2007 PDFzogzzzzzNo ratings yet
- Kristeller. Mindfulness-Based Eating Awareness Training For Treating Binge Eating Disorder - The Conceptual Foundation - AlberxixoDocument14 pagesKristeller. Mindfulness-Based Eating Awareness Training For Treating Binge Eating Disorder - The Conceptual Foundation - AlberxixopaulabagnaroliNo ratings yet
- Mindfulness-Based Interventions For Binge Eating: A Systematic Review and Meta-AnalysisDocument15 pagesMindfulness-Based Interventions For Binge Eating: A Systematic Review and Meta-AnalysisAntonia LarisaNo ratings yet
- Handbook of Assessment and Treatment of Eating Dis... - (PART II Evaluation and Diagnosis of Eating Problems)Document114 pagesHandbook of Assessment and Treatment of Eating Dis... - (PART II Evaluation and Diagnosis of Eating Problems)Manny RosengallegosNo ratings yet
- A Systematic Review of Evidence For PsychologicalDocument8 pagesA Systematic Review of Evidence For PsychologicalLautaro FerreiraNo ratings yet
- Smitham Intuitive Eating Efficacy Bed 02 16 09Document43 pagesSmitham Intuitive Eating Efficacy Bed 02 16 09Evelyn Tribole, MS, RDNo ratings yet
- Mindfulness-Based Interventions For Obesity-Related Eating Behaviors: A Literature ReviewDocument20 pagesMindfulness-Based Interventions For Obesity-Related Eating Behaviors: A Literature ReviewEliseia CarvalhoNo ratings yet
- Dialectical Behavior Therapy For Binge-Eating DisorderDocument14 pagesDialectical Behavior Therapy For Binge-Eating DisorderelioraNo ratings yet
- Perplexities of Treatment Resistence in Eating Disorders: Review Open AccessDocument6 pagesPerplexities of Treatment Resistence in Eating Disorders: Review Open AccessStrejaru TeodoraNo ratings yet
- Kelly2013 PDFDocument11 pagesKelly2013 PDFditeABCNo ratings yet
- Recent Research On BulimiaDocument12 pagesRecent Research On BulimialoloasbNo ratings yet
- Cover Kel Ii, Effects of Routine Education On People Newly Diagnosed With Type 2 DiabetesDocument9 pagesCover Kel Ii, Effects of Routine Education On People Newly Diagnosed With Type 2 Diabetesalfin pratamaNo ratings yet
- Self-Efficacy: Strategy Enhancing: For DiabetesDocument5 pagesSelf-Efficacy: Strategy Enhancing: For DiabetesMery AgunNo ratings yet
- CBT For Bulimia NervosaDocument26 pagesCBT For Bulimia NervosaIsaacNo ratings yet
- CDocument144 pagesCHoang AnhNo ratings yet
- WHS PR Symposium - Obesity: The Power of Your EmotionsDocument16 pagesWHS PR Symposium - Obesity: The Power of Your EmotionsWomen's Health SocietyNo ratings yet
- The Effect of Motivational Interviewing On TheDocument8 pagesThe Effect of Motivational Interviewing On TheQQ1977No ratings yet
- PKFrun2 TIeha7p9v yHQA Mindfulness-and-EatingDocument11 pagesPKFrun2 TIeha7p9v yHQA Mindfulness-and-EatingGabriel Mario Rafael BursztynNo ratings yet
- The Relationship Between Emotional Regulation and Eating Behaviour: A Multidimensional Analysis of Obesity PsychopathologyDocument11 pagesThe Relationship Between Emotional Regulation and Eating Behaviour: A Multidimensional Analysis of Obesity PsychopathologyJosé RodríguezNo ratings yet
- Murphy Et Al 2012 IPT EDDocument9 pagesMurphy Et Al 2012 IPT EDCésar BlancoNo ratings yet
- Understanding and Recognizing Binge Eating Disorder Brochure For NPM 569Document2 pagesUnderstanding and Recognizing Binge Eating Disorder Brochure For NPM 569Ruqayyah Rivera ColinNo ratings yet
- Physiotherapy Improves Eating Disorders and Quality of Life in Bulimia and Anorexia NervosaDocument3 pagesPhysiotherapy Improves Eating Disorders and Quality of Life in Bulimia and Anorexia NervosaAzul MarinoNo ratings yet
- More Than Resisting TemptationDocument18 pagesMore Than Resisting TemptationGuille monsterNo ratings yet
- Integración de La Psicología y NutriciónDocument1 pageIntegración de La Psicología y NutriciónMiguel Angel Alemany NaveirasNo ratings yet
- Childhood ObesityDocument18 pagesChildhood Obesityapi-742948527No ratings yet
- Self Help For Bulimia NervosaDocument6 pagesSelf Help For Bulimia NervosaAnonymous lNDP8O6TNo ratings yet
- Nutrition in Pancreatic Cancer 1711036796Document20 pagesNutrition in Pancreatic Cancer 1711036796Azakari1993No ratings yet
- B A P F I O: Ehavioral ND Sychological Actors N BesityDocument4 pagesB A P F I O: Ehavioral ND Sychological Actors N BesityUjian LancarNo ratings yet
- New Insights Into BED HandoutDocument6 pagesNew Insights Into BED HandoutjuanNo ratings yet
- Medical Nutrition Therapy in Management of EatingDocument6 pagesMedical Nutrition Therapy in Management of Eatingwaraney palitNo ratings yet
- Pike Et Al 2003 PDFDocument5 pagesPike Et Al 2003 PDFAlexa AbendanoNo ratings yet
- GRP 4 CLO 2 Concept Map PT 1 PDFDocument14 pagesGRP 4 CLO 2 Concept Map PT 1 PDFMaria Lyn Ocariza ArandiaNo ratings yet
- Meta Analysis On The Efficacy of Psychological Treatments For Anorexia NervosaDocument21 pagesMeta Analysis On The Efficacy of Psychological Treatments For Anorexia NervosaGanellNo ratings yet
- 10 11648 J Ajpn 20170504 11 PDFDocument5 pages10 11648 J Ajpn 20170504 11 PDFAsti DwiningsihNo ratings yet
- Role of Anxiety, Depression and Anger in Eating Disorders-Structural ModelDocument5 pagesRole of Anxiety, Depression and Anger in Eating Disorders-Structural ModelAsti DwiningsihNo ratings yet
- Research ProposalDocument22 pagesResearch Proposalapi-662212007No ratings yet
- Cognitive Behavior Therapy in The Posthospitalization Treatment of Anorexia NervosaDocument4 pagesCognitive Behavior Therapy in The Posthospitalization Treatment of Anorexia NervosaD 13 Risna KhoirunnisaNo ratings yet
- Acceptance and Commitment Therapy For Women Diagnosed With Binge EatingDocument12 pagesAcceptance and Commitment Therapy For Women Diagnosed With Binge EatingPamela MaercovichNo ratings yet
- Assignment 2Document4 pagesAssignment 2Amina IftikharNo ratings yet
- Vanderlinden (2008)Document5 pagesVanderlinden (2008)Valerie Walker LagosNo ratings yet
- Impact of Wholeofdiet Interventions On Depression and Anxiety A Systematic Review of Randomised Controlled TrialsDocument20 pagesImpact of Wholeofdiet Interventions On Depression and Anxiety A Systematic Review of Randomised Controlled Trialsgiulia.santinNo ratings yet
- Delaney2014Document11 pagesDelaney2014ryselNo ratings yet
- Ed 2020 1Document25 pagesEd 2020 1Alejandra Loyo MonsalveNo ratings yet
- Efficacy of Combined Cognitive Behavior Therapy and Hypnotherapy in Anorexia Nervosa A Case StudyDocument8 pagesEfficacy of Combined Cognitive Behavior Therapy and Hypnotherapy in Anorexia Nervosa A Case StudyCarol Rio AguirreNo ratings yet
- Positive Psychology Interventions in In-Patients With DepressionDocument9 pagesPositive Psychology Interventions in In-Patients With DepressionRute LuzNo ratings yet
- BB-NEDIC - Nutrition Care For Individuals With Eating Disorders - WEBDocument4 pagesBB-NEDIC - Nutrition Care For Individuals With Eating Disorders - WEBangela cabrejosNo ratings yet
- Sweet Lies: Neural, Visual, and Behavioral Measures Reveal A Lack of Self-Control Conflict During Food Choice in Weight-Concerned WomenDocument11 pagesSweet Lies: Neural, Visual, and Behavioral Measures Reveal A Lack of Self-Control Conflict During Food Choice in Weight-Concerned WomenTetsuo MatsunagaNo ratings yet
- Palsson and Whitehead 2013 Psychological TreatmentsDocument9 pagesPalsson and Whitehead 2013 Psychological TreatmentsAgata AgniNo ratings yet
- Leslie Et Al-2018-European Eating Disorders ReviewDocument10 pagesLeslie Et Al-2018-European Eating Disorders ReviewGNo ratings yet
- Barriers To Diabetes Management: Patient and Provider FactorsDocument3 pagesBarriers To Diabetes Management: Patient and Provider FactorsSofyan IndrayanaNo ratings yet
- Journal of Clinical Child & Adolescent Psychology: Click For UpdatesDocument18 pagesJournal of Clinical Child & Adolescent Psychology: Click For UpdatesNaila Zahra MadinaNo ratings yet
- Gerontologic NCPDocument8 pagesGerontologic NCPLouren Grace Quinto AnceroNo ratings yet
- Trastorno Límite ChenDocument10 pagesTrastorno Límite ChenGabyMaría DelValle Cordero Gómez ⃝⃤No ratings yet
- Take Charge Personality As Predictor of Recovery From Eating DisorderDocument6 pagesTake Charge Personality As Predictor of Recovery From Eating DisorderRokas JonasNo ratings yet
- Promoting Mealtime Function in People With Dementia: A Systematic Review of Studies Undertaken in Residential Aged CareDocument20 pagesPromoting Mealtime Function in People With Dementia: A Systematic Review of Studies Undertaken in Residential Aged CaremalnatsNo ratings yet
- The Effect of Mindfulness Meditation Techniques During Yoga and CyclingDocument11 pagesThe Effect of Mindfulness Meditation Techniques During Yoga and CyclingPatriciaNo ratings yet
- Ultrasound System: Acoustic Output TablesDocument108 pagesUltrasound System: Acoustic Output TablesFoued MbarkiNo ratings yet
- Psychoanalytic TherapyDocument13 pagesPsychoanalytic TherapyNada Al AyoubiNo ratings yet
- Chapter 1Document12 pagesChapter 1Lenz Meret CataquisNo ratings yet
- PLS8003 Cultivating Resilience Seminar 1 - AY2122 Sem 1Document45 pagesPLS8003 Cultivating Resilience Seminar 1 - AY2122 Sem 1barry allenNo ratings yet
- A Systematic Review and Meta-Analysis of The Prevalence and Predictors of Anemia Among Children in EthiopiaDocument15 pagesA Systematic Review and Meta-Analysis of The Prevalence and Predictors of Anemia Among Children in EthiopiaAura NirwanaNo ratings yet
- Bioderma FinalDocument17 pagesBioderma FinalHậu PhúcNo ratings yet
- Notes For IvsDocument11 pagesNotes For IvsLujain Al OmariNo ratings yet
- Action Plan SBFP S.Y 2021-2022Document3 pagesAction Plan SBFP S.Y 2021-2022Claudine Moises GaciloNo ratings yet
- 000 00 Qa FRM 0108Document2 pages000 00 Qa FRM 0108vijay rajNo ratings yet
- Ordinance Number Title Category Date Published PenaltyDocument18 pagesOrdinance Number Title Category Date Published PenaltyRvbrRubaNo ratings yet
- Final Session Plan - Tam-An (TM1) Marwin NavarreteDocument163 pagesFinal Session Plan - Tam-An (TM1) Marwin NavarreteMarwin NavarreteNo ratings yet
- Hardware - SoftwareDocument12 pagesHardware - SoftwareMarie Kelsey Acena MacaraigNo ratings yet
- Key Slides: Individualizing Treatment Recommendations For Patients With Hepatitis B Based On EASL GuidanceDocument17 pagesKey Slides: Individualizing Treatment Recommendations For Patients With Hepatitis B Based On EASL GuidanceluamsmarinsNo ratings yet
- Academic Calendar 2012-2013 MITDocument6 pagesAcademic Calendar 2012-2013 MITnhartono_1No ratings yet
- 6.2. Human Movement & GrowthDocument20 pages6.2. Human Movement & GrowthOppp JinuNo ratings yet
- The Effect of Implant Abutment Junction Position On Crestal Bone Loss A Systematic Review and Meta AnalysisDocument17 pagesThe Effect of Implant Abutment Junction Position On Crestal Bone Loss A Systematic Review and Meta AnalysisBagis Emre GulNo ratings yet
- THE Quality OF Life AND Caregiving Burden Among Caregivers OF People With Dementia IN Hanoi, BAC Ninh AND HAI Phong, VietnamDocument310 pagesTHE Quality OF Life AND Caregiving Burden Among Caregivers OF People With Dementia IN Hanoi, BAC Ninh AND HAI Phong, VietnamCHEE KOK SENGNo ratings yet
- ReviewerDocument6 pagesReviewerSophia Gella FredilesNo ratings yet
- Ocp HukmDocument2 pagesOcp Hukmcac kepongNo ratings yet
- Check Sheet: Ellis Ratcliffe Plan Number 2Document3 pagesCheck Sheet: Ellis Ratcliffe Plan Number 2EllisNo ratings yet
- Safety Data Sheet According To Regulation (EC) 'No. 2015/830Document15 pagesSafety Data Sheet According To Regulation (EC) 'No. 2015/830Carlos Ortega MartinezNo ratings yet
- Revised Chapter 1 Group 2 CHECKEDDocument8 pagesRevised Chapter 1 Group 2 CHECKEDeeynaNo ratings yet
- I-Byte Healthcare July 2021Document89 pagesI-Byte Healthcare July 2021IT ShadesNo ratings yet
- Wk1 Theoretical Model in CHN PPT FormatDocument38 pagesWk1 Theoretical Model in CHN PPT FormatPucha MorinNo ratings yet