Professional Documents
Culture Documents
Calcium Physiology
Uploaded by
العياده التخصصيه للسكري0 ratings0% found this document useful (0 votes)
6 views17 pagesOriginal Title
CALCIUM PHYSIOLOGY
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
6 views17 pagesCalcium Physiology
Uploaded by
العياده التخصصيه للسكريCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 17
Determination of Serum
Calcium and Phosphorus
2nd Year Medical Students
Clinical Biochemistry Lab
02/03/2015
Introduction
Calcium is one of the most important divalent ions in our body
It is important for:
The transmission of nerve impulses
Maintaining normal muscle contractility
Certain enzymatic reactions as a cofactor
The coagulation of blood
Release of hormones (exocytosis)
Calcium Distribution
About 99% of calcium in our body is part of the bones
The remaining 1% is mostly in blood and other ECF and this found as
several forms:
45% as free or ionized calcium (physiologically active fraction)
40% as protein-bound calcium, mostly albumin
15% is bound to other anions as phosphate, citrate and bicarbonate
The serum total calcium concentration is tightly controlled at around
2.15-2.55 mmol/L
The serum ionized calcium is about 1.16-1.32 mmol/L
Calcium Homeostasis
Control of Plasma Calcium
Calcium homeostasis follow a general rule that EC
concentrations are controlled rather than the total body
content and the effectiveness of this depends on:
An adequate supply of calcium and vitamin D
Normal functioning of :
Intestine
Parathyroid gland
Kidneys
If any of these is impaired, calcium leaves bones by passive
diffusion and plasma concentration is maintained at the
expense of bone calcification
Regulation of Calcium level
Any change in serum protein concentration alter the concentration of
both protein bound and total calcium
Changes in pH also affects calcium-protein binding
Acidosis decreases calcium binding leading to an increase of free calcium (H+
compete with calcium for binding) and also increases calcium solubility
leading to increase in the release of calcium from bones
PTH , vitamin D and calcitonin are known to regulate calcium
homeostasis by altering their secretions in response to the changes of
ionized calcium level
Regulation of Calcium level
PTH
Secreted in response to a decrease in ionized calcium
In the bones, activates bone resorption releasing calcium and HPO4 into ECF
In the kidneys, PTH conserves Calcium by increasing its reabsorption (while
increasing HPO4 excretion) and also stimulates renal production of active
vitamin D
Vitamin D promotes intestinal absorption and renal reabsorption of
calcium and HPO4 and enhances PTH effect on bone resorption
Calcitonin, originating from thyroid gland, is secreted in response to
an increase in calcium and exerts its calcium lowering effect by
inhibiting the action of both PTH and vitamin D
Regulation of Calcium level
Hypocalcemia
• Hypocalcemia occur in the following cases:
• Primary hypoparathyroidism (glandular aplasia, destruction or surgical
removal)
• Pseudohypoparathyroidism (PTH target tissue response is decreased)
• Sever Hypomagnesaemia (inhibits PTH secretion or impair its action on the
bone , and possibly vit D resistance)
• Malabsorption states
• Drugs like loop diuretics
• Acute pancreatitis
• Chronic kidney disease
• Rhabdommyolysis (phosphate releases and complexes with calcium)
Hypercalcemia
• Due to the following reasons:
• Primary Hyperparathyroidism (adenoma or glandular hyperplasia)- this is the
leading cause
• Malignancy is the second leading cause , bony metastases like lung, breast
and kidney tumors
• Thyrotoxicosis (high bone turnover rate)
• Vitamin D toxicity
• Drugs like Thiazide diuretics (reduce renal calcium excretion)
Determination of Serum
phosphorous
Clinical Biochemistry Lab
2nd Year Medical Students
2/3/2015
Introduction
• Practically, all body phosphorus is present as phosphate
• Phosphate is the major intracellular anion
• Approximately 80% of which is found in the bony skeleton and 20% is
distributed in the soft tissues and muscles
• Blood phosphorous classified into:
• Organic phosphate (ATP)
• Inorganic phosphate as mono- and divalent anions
• Phosphate esters of lipids (phospholipids)
Physiological Importance of Phosphate
• Functions of phosphate:
• An important intracellular buffer
• As a component of phospholipids and nucleic acids
• Has a central role in metabolic pathways including glycolysis and oxidative
phosphorylation
• Also has a role in the optimal function of leucocytes like chemotaxis and
phagocytosis
• The most important energy reservoirs are ATP and creatine phosphate
Regulation
• The daily phosphate intake is about 30 mmol
• Protein-rich food is a major source of phosphate intake, as are nuts and
cereals
• The output is largely renal with more than 90% being excreted by this
route
• GI loss accounts for only 10% of the phosphate excretion
• It is regulated by:
• PTH which increases its renal excretion
• Vitamin D which increases both its absorption from GIT and renal
reabsorption
• Growth hormone which decreases renal excretion of phosphate
• Acid-base state (acidosis causes shifting of phosphate out of the cells)
Clinical Significance
Normal serum level in adults is 0.8-1.8 mmol/L
Although the concentration of all blood phosphate compounds is about 12 mg/dL
(3.9 mmol/L), only about 3-4 mg/dL is inorganic phosphate
Hyperphosphatemia
• Occur in the following cases:
• Artefact due to in vitro hemolysis or old blood sample
• Acute or chronic kidney disease
• Increased tissue breakdown
• Acidaemia (metabolic or respiratory acidosis)
• Diabetic ketoacidosis
• Hypoparathyroidism
• Excess vitamin D intake
• Sever infections, intensive exercise, and neoplastic disorders (increased
breakdown of cells)
Hypophosphatemia
• Can be seen in the following cases:
• Cellular redistribution ( intravenous glucose, alkalemia, insulin administration)
• Malabsorption states
• Long term parenteral nutrition without phosphate supplementation
• Liver disease
• Hyperparathyroidism (increased excretion)
• Vitamin D deficiency (decreased absorption)
You might also like
- Calcium, Phosphate, MagnesiumDocument55 pagesCalcium, Phosphate, MagnesiumUdochukwu EnebeNo ratings yet
- Calcium Metabolism and RegulationDocument39 pagesCalcium Metabolism and RegulationSanchita SahaNo ratings yet
- Parathyroid: Calcium and Vitamin DDocument135 pagesParathyroid: Calcium and Vitamin DPhysiology by Dr RaghuveerNo ratings yet
- Phosphorus ImbalanceDocument6 pagesPhosphorus ImbalanceJohnston AbaridoNo ratings yet
- Paratiroid Dan KalsiumDocument80 pagesParatiroid Dan KalsiumFebrina EvaNo ratings yet
- Hypo Phosphate MiaDocument15 pagesHypo Phosphate Miacute_maimaiNo ratings yet
- Ca, MG and PO4-1Document60 pagesCa, MG and PO4-1JoeyNo ratings yet
- Calcium and PhosporusDocument29 pagesCalcium and PhosporusJoe AjibadeNo ratings yet
- HypophosphatemiaDocument26 pagesHypophosphatemiaOxy GenNo ratings yet
- Phosphate ImbalanceDocument17 pagesPhosphate Imbalancemary ann corsanesNo ratings yet
- B50F712F-38CD-4A82-B61E-4E759B1D58EFDocument23 pagesB50F712F-38CD-4A82-B61E-4E759B1D58EFbf28215No ratings yet
- CA and Phosphate Metabolism - PDFXDocument25 pagesCA and Phosphate Metabolism - PDFXObsa AhmedNo ratings yet
- P ImbalancesDocument15 pagesP ImbalancesglamyposhNo ratings yet
- Calcium MetabolismDocument13 pagesCalcium MetabolismMaqbul AlamNo ratings yet
- Minerals FinalDocument103 pagesMinerals Finallovi bahunNo ratings yet
- HYPERCALCEMIADocument9 pagesHYPERCALCEMIAllonajoycesabadosn25No ratings yet
- Regulation of calcium, Parathyroid hormone, Vitamin D & CalcitoninDocument29 pagesRegulation of calcium, Parathyroid hormone, Vitamin D & CalcitoninJessica StewartNo ratings yet
- Lect 9 Parathyroid Gland-1Document30 pagesLect 9 Parathyroid Gland-1warda farooqNo ratings yet
- Calcium HomeostasisDocument38 pagesCalcium Homeostasiskelvinmaina9993No ratings yet
- 6.0 ElectrolytesDocument4 pages6.0 ElectrolytesHry WkNo ratings yet
- Substances Affecting Bone Mineral HomeostasisDocument33 pagesSubstances Affecting Bone Mineral Homeostasisanaya khan StudentNo ratings yet
- Diseases of The Parathyroid GlandDocument60 pagesDiseases of The Parathyroid GlandRuDy RaviNo ratings yet
- Calcium MetabolismDocument29 pagesCalcium MetabolismsnehaNo ratings yet
- Veterinary Clinics: Phosphorus: A Quick ReferenceDocument5 pagesVeterinary Clinics: Phosphorus: A Quick ReferenceDanilo JimenezNo ratings yet
- 27 - Hypo and Hypernatremia - and Hypo and Hyperkalieama PDFDocument48 pages27 - Hypo and Hypernatremia - and Hypo and Hyperkalieama PDFEITHAR OmarNo ratings yet
- Calcium and Phosphorus HomeostasisDocument3 pagesCalcium and Phosphorus Homeostasisshakila786No ratings yet
- Fluids and ElectrolytesDocument11 pagesFluids and Electrolytescarlo evardo100% (2)
- Calcium Homeostasis: Normal Plasma LevelsDocument5 pagesCalcium Homeostasis: Normal Plasma LevelsE MeerNo ratings yet
- Hyper para Thyroid Is MDocument27 pagesHyper para Thyroid Is MIbrahimWagesNo ratings yet
- MK Biokimia - Metabolisme MineralDocument84 pagesMK Biokimia - Metabolisme MineralmusimsemiNo ratings yet
- Calcium Salts Calcitonin and CA RegulatorsDocument40 pagesCalcium Salts Calcitonin and CA RegulatorsSudhakar LakavathNo ratings yet
- CALCIUM METABOLISM RaminDocument42 pagesCALCIUM METABOLISM RaminRamin MaharjanNo ratings yet
- Calcium HomeostasisDocument37 pagesCalcium Homeostasispolog.jm610No ratings yet
- Parathyroid Hormone and Calcium Regulation: By: Abebe TDocument29 pagesParathyroid Hormone and Calcium Regulation: By: Abebe TLidiya TeshomeNo ratings yet
- Parathyroid GlandsDocument4 pagesParathyroid GlandsMary Grace Buscargas PolancosNo ratings yet
- Calcium Regulation: 800-1200 Mg/dayDocument3 pagesCalcium Regulation: 800-1200 Mg/dayclarheenaNo ratings yet
- Calcium Homeostasis HormonesDocument31 pagesCalcium Homeostasis HormonesNoval FebriNo ratings yet
- Biochemical Markers of Bone Metabolism PPT LectureDocument89 pagesBiochemical Markers of Bone Metabolism PPT LectureNeil Vincent De AsisNo ratings yet
- Major IntracelularDocument67 pagesMajor Intracelularfarooq shah shabbirNo ratings yet
- Study Guide For Calcium and Phosphate MetabolismDocument74 pagesStudy Guide For Calcium and Phosphate MetabolismMohammad MamunuzzamanNo ratings yet
- Drugs Affecting Calcium Balance: Harsh Vinayak Roll No. 39 Mbbs 2 Yr Student BATCH 2019 Rdasmc, AyodhyaDocument24 pagesDrugs Affecting Calcium Balance: Harsh Vinayak Roll No. 39 Mbbs 2 Yr Student BATCH 2019 Rdasmc, AyodhyaA2Z GyanNo ratings yet
- Calcium Metabolism (PTH, Vitamin D, and Calcitonin)Document4 pagesCalcium Metabolism (PTH, Vitamin D, and Calcitonin)Saima SiddiqiNo ratings yet
- Hypo Phosphate MiaDocument7 pagesHypo Phosphate MiaChristian Manuel Chiara ChiletNo ratings yet
- Calcium, Phosphate and Vitamin D MetabolismDocument25 pagesCalcium, Phosphate and Vitamin D MetabolismRendy LectusNo ratings yet
- Major Intra and Extracellular IonsDocument29 pagesMajor Intra and Extracellular IonsRasel IslamNo ratings yet
- Hormonal Control of Calcium and Phosphate MetabolismDocument50 pagesHormonal Control of Calcium and Phosphate MetabolismhamidNo ratings yet
- PHYSIOLOGY OF CALCIUM AND VITAMIN D METABOLISM AND BONE MARKERS (39Document60 pagesPHYSIOLOGY OF CALCIUM AND VITAMIN D METABOLISM AND BONE MARKERS (39mohammad abdul naveedNo ratings yet
- A Simple Guide to Hyperparathyroidism, Treatment and Related DiseasesFrom EverandA Simple Guide to Hyperparathyroidism, Treatment and Related DiseasesNo ratings yet
- Hypokalemia Case StudyDocument10 pagesHypokalemia Case StudyJib SinsuatNo ratings yet
- Calcium Metabolism: Preparation byDocument18 pagesCalcium Metabolism: Preparation byAbhijeet KanjeNo ratings yet
- Group 1 HypokalemiaDocument6 pagesGroup 1 HypokalemiaAdegboye AdedayoNo ratings yet
- Calcium and Phosphate HomeosatsisDocument35 pagesCalcium and Phosphate HomeosatsisnirilibNo ratings yet
- Hypo and HyperalcemiaDocument3 pagesHypo and HyperalcemiaJulieNo ratings yet
- Hypokalemia - Practice Essentials, Pathophysiology, EtiologyDocument15 pagesHypokalemia - Practice Essentials, Pathophysiology, EtiologymirzeroNo ratings yet
- 3ES-4 CA Metabloism Final 1436Document47 pages3ES-4 CA Metabloism Final 1436Muath AlqarniNo ratings yet
- Clinical Pharmacokinetics in Liver Failure Patients SenddDocument30 pagesClinical Pharmacokinetics in Liver Failure Patients Senddthavia andrianiNo ratings yet
- Share Market Report 6Document13 pagesShare Market Report 6Nithish DevadigaNo ratings yet
- Mineral Homeostasis and Bone TurnoverDocument43 pagesMineral Homeostasis and Bone TurnoverDylan MansillaNo ratings yet
- Tyroid 10Document6 pagesTyroid 10Anonymous UTUWFODCEYNo ratings yet
- Hypocalcemia, (Low Blood Calcium) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandHypocalcemia, (Low Blood Calcium) A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- DIABETESDocument48 pagesDIABETESالعياده التخصصيه للسكريNo ratings yet
- 1 kumarMCQ "GIT"Document31 pages1 kumarMCQ "GIT"العياده التخصصيه للسكريNo ratings yet
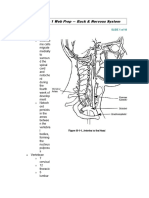
- 2 - Back & Nervous SystemDocument11 pages2 - Back & Nervous Systemالعياده التخصصيه للسكريNo ratings yet
- Clinical NotesDocument9 pagesClinical Notesالعياده التخصصيه للسكريNo ratings yet
- 6 An Indian American Woman in Space 2Document11 pages6 An Indian American Woman in Space 2Manju YadavNo ratings yet
- RIBA Outline Plan of Work ExplainedDocument20 pagesRIBA Outline Plan of Work ExplainedkenNo ratings yet
- Financial ManagementDocument2 pagesFinancial ManagementSanna KazmiNo ratings yet
- Altered Ventilatory Function Assessment at Pamantasan ng CabuyaoDocument27 pagesAltered Ventilatory Function Assessment at Pamantasan ng Cabuyaomirai desuNo ratings yet
- Parts of The Analog MultitesterDocument4 pagesParts of The Analog MultitesterDestiny Marasigan CanacanNo ratings yet
- Deviser TV Analyser S7000: Bagian 1: Fungsi AnalyzerDocument15 pagesDeviser TV Analyser S7000: Bagian 1: Fungsi AnalyzerAlexander WieseNo ratings yet
- Tax1 Course Syllabus BreakdownDocument15 pagesTax1 Course Syllabus BreakdownnayhrbNo ratings yet
- Atomic Structure QuestionsDocument1 pageAtomic Structure QuestionsJames MungallNo ratings yet
- Research on Comparisons between Sabah and Diesel CyclesDocument8 pagesResearch on Comparisons between Sabah and Diesel CyclesjorgeNo ratings yet
- Measurement of Mass and Weight by NPLDocument34 pagesMeasurement of Mass and Weight by NPLN.PalaniappanNo ratings yet
- Curriculam VitaeDocument3 pagesCurriculam Vitaeharsha ShendeNo ratings yet
- Summative Test For Quadratic Equations2Document2 pagesSummative Test For Quadratic Equations2AsmiraMangontra0% (1)
- Public OpinionDocument7 pagesPublic OpinionSona Grewal100% (1)
- Inventario de Autoestima de Coopersmith PDFDocument10 pagesInventario de Autoestima de Coopersmith PDFNancy BerduzcoNo ratings yet
- Engr2227 Apr03Document10 pagesEngr2227 Apr03Mohamed AlqaisiNo ratings yet
- Inspection and Test Plan Steel Sheet Pile DriDocument6 pagesInspection and Test Plan Steel Sheet Pile DriSofda Imela100% (1)
- 9284 - Technical Instruction Addenum 3 Corrigendum 2Document5 pages9284 - Technical Instruction Addenum 3 Corrigendum 2Bambang HerimantoNo ratings yet
- Optical Fiber Communication Case Study on Material DispersionDocument5 pagesOptical Fiber Communication Case Study on Material DispersionAyush SharmaNo ratings yet
- CS310 Sample PaperDocument10 pagesCS310 Sample PaperMohsanNo ratings yet
- FIL M 216 2nd Yer Panitikan NG PilipinasDocument10 pagesFIL M 216 2nd Yer Panitikan NG PilipinasJunas LopezNo ratings yet
- Chapter 6 Managing Quality (Sesi 3)Document68 pagesChapter 6 Managing Quality (Sesi 3)Nurmala SariNo ratings yet
- Power System Analysis and Design, SI EditionDocument5 pagesPower System Analysis and Design, SI EditionAkimeNo ratings yet
- Joe Ann MarcellanaDocument17 pagesJoe Ann MarcellanarudyNo ratings yet
- Bài tập tiếng Anh 12 (Reading)Document7 pagesBài tập tiếng Anh 12 (Reading)Minh AnhNo ratings yet
- Q3 Curriculum Map - Mathematics 10Document3 pagesQ3 Curriculum Map - Mathematics 10Manilyn BaltazarNo ratings yet
- The Manning EquationDocument10 pagesThe Manning EquationFederico LeonNo ratings yet
- Andromeda Council About The 4th DimensionDocument11 pagesAndromeda Council About The 4th DimensionWonderlust100% (1)
- Contemporary Issue in StrategyDocument13 pagesContemporary Issue in Strategypatrick wafulaNo ratings yet
- 2.2valves, Alarm - Ul Product IqDocument1 page2.2valves, Alarm - Ul Product Iqbhima irabattiNo ratings yet
- Fujitsu Lifebook p1120 ManualDocument91 pagesFujitsu Lifebook p1120 Manualمحمد يحىNo ratings yet