Professional Documents
Culture Documents
Acute Pancreatitis
Uploaded by
sembakarani thevagumaran0 ratings0% found this document useful (0 votes)
5 views76 pagesOriginal Title
Acute pancreatitis(1)
Copyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
5 views76 pagesAcute Pancreatitis
Uploaded by
sembakarani thevagumaranCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 76
1.
relate clinical manifestation of the following conditions to
its
pathophysiology:
1.1 acute pancreatitis
1.2 acute hepatic failure
2. assess the severity of acute pancreatitis and the related
risk of mortality
3. state the “range of clinical syndromes” in acute hepatic
failure:
3.1 hyper-acute
3.2 acute
3.3 subacute
4. explain the complications associated with acute
hepatic failure:
4.1 encephalopathy
4.2 coagulopathy
4.3 metabolic derangement
4.4 cardiovascular derangement
4.5 acute kidney injury (hepatorenal syndrome)
formulate individualized patient care using the
nursing process as a
framework for the following conditions:
5.1 acute pancreatitis
5.2 acute hepatic failure
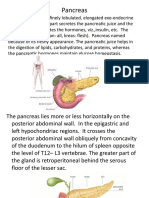
It is part of the digestive system and
produces important enzymes and hormones
that help break down foods.
The pancreas has an
endocrine function because it releases
juices directly into the bloodstream, and it
has an exocrine function because it
releases juices into ducts
Etiology
Commonest causes:
1) Biliary stone disease
2) Alcohol consumption
3) Drugs
4) Trauma
3) Idiopathic
4) Unknown
The pathogenesis of Acute
Pancreatitis is thought to be due to
premature activation of digestive
enzymes within the acinar cells.
Ordinarily, pancreatic proenzymes
become activated on release within
the duodenum.
Pancreatitis results from early
activation of pancreatic enzymes,
producing autodigestion of the
pancreas and surrounding tissues.
Digestive enzyme release is amplified
as acinar cells lyse, leading to a
vicious cycle of inflammation and
necrosis.
Acute pancreatitis manifests with the
sudden onset of epigastric pain radiating
to the back.
Eating food worsens pain;
bending forward ameliorates pain.
Abdominal pain lasts for days
and is associated with anorexia, nausea,
and vomiting
make (something bad or unsatisfactory) better."the
reform did much to ameliorate living
standards”synonyms:improve, make
better, better, make improvements
to, enhance, help,benefit, boost, amend;
fever,
tachycardia,
and hypotension.
Abdominal examination reveals epigastric
tenderness, with localized guarding and
rebound. Sluggish or absent bowel
sounds indicate coexisting ileus.
Less frequent findings signal complications,
including Grey Turner's (flank ecchymosis)
or Cullen's (umbilical ecchymosis)
signs suggestive of retroperitoneal hemorrhage,
a palpable mass suggestive of a pseudocyst,
and dullness to percussion of lung fields suggestive
of pleural effusion.
Grey Turner's sign refers to bruising of
the flanks, the part of the body between the last
rib and the top of the hip. The bruising appears as
a blue discoloration, and is a sign of
retroperitoneal hemorrhage, or bleeding behind
the peritoneum, which is a lining of the abdominal
cavity. Grey Turner's sign takes 24–48 hours to
develop, and can predict a severe attack of acute
pancreatitis.
Grey Turner's sign may be accompanied
by Cullen's sign. Both signs may be indicative of
pancreatic necrosis with retroperitoneal or
intraabdominal bleeding. Grey Turner's sign is
named after British surgeon George Grey Turner.
Scoring of patient with acute pancreatitis:
1) alerted to the presence of potentially
severe diseases
2) comparisons of severity between
patients
3) potential new treatments and
interventions
Serum Amylase and Lipase
- The diagnosis of Acute Pancreatitis is supported
by an elevation of the
serum amylase and lipase levels in excess of
three times the upper limit of
normal. The amylase level becomes elevated
within hours of the development of pain and may
remain elevated for 3 to 5 days.
Liver function tests (LFT)
- Mild elevations of LFT results
Full blood count
- Leukocytosis
Serum electrolytes, BUN, creatinine,
glucose, cholesterol, and triglycerides
CRP
ABG
Radiography (abdominal X-Ray,
abdominal ultrasound, abdominal CT,
ERCP)
is a blood test marker for inflammation in the
body. CRP is produced in the liver and its level is
measured by testingthe blood. CRP is classified
as an acute phase reactant, which means that its
levels will rise in response to inflammation.
This algorithm is based on the practice guidelines
from the American College of
Gastroenterology
Dynamic contrast-enhanced
computed tomography (CT) provides
the best
means of accurately visualizing the
pancreas and diagnosing pancreatitis
and its local complications. It may
also be used for guiding
percutaneous catheter drainage.
Following the initial CT scan, additional scanning is only
indicated if the patient’s clinical condition deteriorates,
usually through the development of
pancreatic necrosis,
abscess or
pancreatic pseudocyst,
haemorrhage, or
colonic ischemia
or perforation.
Ultrasonography in acute pancreatitis is less useful
since visualisation of the gland may be obscured by ‘gas
filled’ bowel.
Morphine infusion (2-4 mg/h) is still widely used
despite it may cause spasm
of the sphincter of Oddi and worsen the pain.
IV Fentanyl 1-2 ug/h may be used as an
alternative.
3. Endoscopic
ERCP represents an alternative
approach to surgery, particularly
for patients
with severe biliary pancreatitis.
The role of surgery remains a
controversial area in the management of
severe acute pancreatitis. Current
approach is the concept of a conservative,
non-surgical approach.
The presence of infected pancreatic
necrosis seems to be an undisputed
indication for urgent surgery.
Indications for surgery in severe acut
pancreatitis:
Stable but persistent necrosis
Deterioration in clinical course
Abdominal Compartment Syndrome
Deterioration in clinical course
‘resting the pancreas’, might improve outcome.
pancreatic secretions by ‘protease inhibitors’, and
somatostatin &
octreotide,are in widespread use in the hope of
improving the outcome.
Somatostatin and Octreotide:
potent inhibitors of pancreatic
secretion
• Protease Inhibitors: Aprotinin
and gabexate mesilate are
proteolytic
enzyme inhibitors
Total parenteral nutrition (TPN) in favour of enteral
nutrition (EN) in supporting the
critically ill.
Studies suggest that early EN started within 24
hours of admission to ICU, compared with TPN, is
associated with reduced infective
complications and hospital length of stay.
protocol ensuring strict glycaemic control is
recommended.
Problem 1: Fluid Volume deficit related to fluid
sequestration within the
peritoneum
Clinical Assessment Findings
Tachycardia
MAP < 70 mmHg
CVP < 7 mmHg
Capillary refill > 2 secs
Urine output < 0.5 ml/kg/hour
Intervention
1. Monitor hemodynamic status and oxygenation
(blood pressure, heart rate,
ECG)
Keep MAP > 70 mmHg
Observe ECG for myocardial ischemia
2. Estimate ongoing fluid losses
Measure all drainage from tubes, catheters and drains
Evaluate character of all fluid loss
Colour, odour, presence of particulate matter, fibrin
and clots
3. Replace volume with prescribed fluids
(crystalloids/colloids)
Keep MAP > 70 mmHg
CVP > 7 mmHg
Capillary refill < 2 secs
4. Measure urine output continuously
Keep Urine output > 0.5 ml/kg/hr
Problem 2 : Pain related to injury
to pancreatic tissue and
surrounding tissue
Clinical Assessment Findings
Patient discomfort evidenced by
pain score
Tachycardia
Irregular respiration
Intervention
1. Position patient to optimize comfort
2. Reduce anxiety that may contribute to pain relief
Provide reassurance
3. Administer IV analgo-sedation
Provide Midazolam/Morphine infusion 1-2mg/hour
4. Monitor hemodynamic and respiration
5. Assess level of pain by using Pain Score
Report if patient is persistently in pain. Dose of
analgesia need to be
adjusted accordingly
Clinical Assessment Findings
Weight loss
Intervention
1. Assess nutritional status
Body weight
2. Nutritional management
Collaborate with dietitian and pharmacist to estimate
patients’ nutritional needs.
Administer enteral feeding if tolerated.
Administer Total Parenteral Nutrition if enteral
feeding cannot be established.
In the majority of AHF, there is widespread
hepatocellular necrosis beginning in
the centrizonal distribution and progressing
towards portal tracts. The degree of
parenchymal inflammation is variable and is
proportional to duration of disease.
Acute hepatic failure (AHF) is a complex multi
systemic illness that evolves after
significant liver insult. It is a heterogeneous
condition incorporating a range of
clinical syndromes.
“Range of Clinical Syndromes” In Acute
Hepatic Failure
Acute hepatic failure (AHF) is a complex
multi-systemic illness that evolves after
significant liver insult. It is a
heterogeneous condition incorporating a
range of
clinical syndromes. Definitions according
to O’ Grady:-
1. Hyper-acute
- the onset of encephalopathy is within 7
days of the development of jaundice
2. Acute
- encephalopathy develops 8-28 days
after the onset of jaundice
3. Sub-acute
- encephalopathy develops 4-26 weeks
after the onset of jaundice
1. Encephalopathy
The spectrum extends from mild
confusion progressing to deep
coma,cerebral edema and raised
intracranial hypertension.
Coagulopathy is another cardinal feature of AHF. The
liver has the central role in synthesis of almost all
coagulation factors and some inhibitors of coagulation
and fibrinolysis. Hepatocellular necrosis leads to
impaired synthesis of many coagulation factors and
their inhibitors. The former produces a prolongation in
prothrombin time which is widely used to monitor
severity of hepatic injury. There is significant platelet
dysfunction (with both
quantitative and qualitative platelet defects).
Progressive thrombocytopenia with loss of larger and
more active platelet is almost universal.
Thrombocytopenia with or without DIC increases the
risk of intracerebral
bleeding.
Hypernatremia is an almost universal finding due
to water retention and a shift in intracellular
sodium transport from inhibition of Na/K ATPase.
Hypoglycemia (due to depleted hepatic glycogen
store and yperinsulinaemia), hypokalemia,
hypophosphatemia and metabolic alkalosis are
often present, independent of renal function.
Lactic acidosis occurs predominantly in
paracetamol overdose.
Patient with AHF develop hyper-dynamic circulation, with
peripheral vasodilatation and central volume depletion.
This will leads to hypotension
and may initially respond to volume replacement. There is
a compensatory increase in cardiac output. Hypotension
that does not respond to volume will
require some form of invasive hemodynamic monitoring
and frequently institution of vasopressor agents. The
requirement for vasopressor agents
should raise the possibility of adrenal dysfunction.
Hydrocortisone replacement therapy should be considered.
Renal failure is common, present in more than 50% of
AHF patients, either due to original insult such as
paracetamol resulting in acute tubular necrosis or from
hyperdynamic circulation leading to ‘hepatorenal
syndrome’ or functional renal failure. Because of
impaired production of urea, blood urea does not
represent degree of renal impairment. Established
renal failure requires the institution of renal
replacement therapy (RRT). The hemodynamic
instability and associated cerebral complications have
resulted in the application of continuous modes of
RRT rather than intermittent hemodialysis.
Management of ALF patients in ICU requires an
experienced multidisciplinary team.
Patients with stage I HE experience changes in
behavior, with minimal changes in their level of
consciousness, and may be initially managed in a step
-down or ward setting. On the other hand, patients
with drowsiness, asterixis, and any
degree of disorientation (stage II HE) are at a high risk
of decompensation and warrant ICU admission.
Patients with more severe neurologic impairment
(stages III – IV HE) require intubation and mechanical
ventilation.
a) Ammonia-lowering therapy with lactulose has
been the mainstay of treatment
for HE. A nasogastric tube may be used to
administer the frequent doses of
this medication. With lactulose therapy, the
potential side effect of colonic
distention should be taken into consideration.
b) Cerebral edema and ICH can lead to death from cerebral
herniation.
Recommended management includes intubation, sedation, head-of-
bed
elevation to at least 30 degrees, and efforts to minimize
interventions and
stimuli that result in increased ICP. Prophylactic dosing of
antiepileptic
medications has not been shown to improve outcomes. Intravenous
mannitol
at a dose of 1 g/kg body weight (dose range 0.25–2 g/kg) is a first-
line
therapy that may be used. Hyperventilation to reduce PaCO2 to
25–30 mmHg has been used as a short term solution to decrease
cerebral blood flow and lower ICP.
c) Infection has consistently remained the number
one cause of death in ALF
patients. Frequent surveillance of blood, urine,
and sputum cultures has been
shown to be useful and can direct therapy.
Prophylactic antibiotics have been
shown to reduce infection rates, though their use
has not been directly linked
to improved outcomes.
d) The circulatory disturbance in ALF is
characterized by decreased systemic
vascular resistance and elevated cardiac output.
Management consists of
intravenous fluid resuscitation and vasopressors
guided by invasive
hemodynamic monitoring.
e) Adrenal insufficiency is commonly
seen in ALF. The presence of
persistent
hypotension despite volume
resuscitation and vasopressors will
require
empiric treatment with intravenous
steroids.
f) Acute kidney injury (AKI) is common in ALF. Renal
failure often coexists with
a variety of metabolic derangements, including lactic
acidosis, hyponatremia,
hypophosphatemia, and, often profound hypoglycemia
requiring continuous
glucose infusion. The decision of when to begin renal
replacement therapy
(RRT) has been a subject of debate. There is
agreement that when an acute
indication for RRT exists, continuous RRT, rather than
intermittent
hemodialysis, is preferred to minimize cardiovascular
disturbances and
increased ICPs.
g) The risk of bleeding in ALF patient is increased in the
setting of AKI and ICH.
They often have markedly elevated prothrombin times or
INRs, as well as
thrombocytopenia, though these measures do not always
correlate to
increased rates of bleeding. Correction of coagulopathy
with fresh frozen
plasma or thrombocytopenia with platelet transfusion is not
indicated unless
an invasive procedure is planned. Vitamin K should be
administered to
facilitate synthesis of prothrombin and coagulation factor if
liver is functional.
h) Nutrition is another consideration in ALF
patients, with electrolyte and vitamin
replacement being important, as well as early
initiation of enteral nutrition.
Protein restriction is not indicated, and 1g/kg per
day of protein is
recommended. Parenteral nutrition may be
needed if enteral nutrition is
contraindicated.
Nursing Care of Patients with Acute Hepatic
Failure
Problem 1: Ineffective cerebral tissue perfusion
related to hepatic
encephalopathy
Clinical assessment findings
- Worsening level of consciousness
Interventions
1. Administer oxygen to improve cerebral
oxygenation
2. Intubate and ventilate if GCS < 8 or inability to
maintain adequate airway
3. Hyperventilation and intermittent Mannitol
boluses as temporary measures to
reduce ICP and increase cerebral perfusion
pressure
4. Monitor vital signs and hemodynamic
parameters
5. Monitor neurological status for changes in
mentation or level of consciousness
6. Monitor peripheral pulses
7. Monitor laboratory data: electrolytes,
coagulation profile, renal profile, liver
function, glycemia control
8. Administer lactulose to reduce ammonia levels
9. Use sedation to reduce stimuli for increasing
ICP or reduce cerebral
metabolism such as benzodiapines, propofol and
opioids.
Problem 2: Risk of bleeding related to coagulopathy
Clinical assessment findings
- Presence of petechiae, hematoma or bruising
Interventions
1. Monitor the presence of blood in body secretions eg
stool, urine and NG aspirate
2. Observe for bleeding from puncture sites
3. Monitor vital sign and hemodynamic parameters that
could indicate loss of circulating blood volume
4. Insert NG tube gently to prevent from bleeding
5. Administer Vitamin K that facilitates synthesis of
coagulation factor
You might also like
- Nephrotic Syndrome PathophysiologyDocument1 pageNephrotic Syndrome PathophysiologyKrisianne Mae Lorenzo FranciscoNo ratings yet
- Maxwell's Manual of Malicious MaladiesDocument35 pagesMaxwell's Manual of Malicious MaladiesJean Ariehn100% (1)
- Acute Pancreatitis: Presented By: DAHAL SHIRISHADocument25 pagesAcute Pancreatitis: Presented By: DAHAL SHIRISHASiruNo ratings yet
- Okell MedicineDocument300 pagesOkell MedicinePeprah Ondiba100% (2)
- Presentation 1Document50 pagesPresentation 1Isaac MwangiNo ratings yet
- Case 1Document4 pagesCase 1Irsanti SasmitaNo ratings yet
- Chauke NJ 201908564 NUTRITIONAL SCREENINGDocument7 pagesChauke NJ 201908564 NUTRITIONAL SCREENINGRulani PrinceNo ratings yet
- Cirrhosis AndrewDocument33 pagesCirrhosis Andrewlionel andreaNo ratings yet
- Chronic PancreatitisDocument42 pagesChronic PancreatitismmurugeshrajNo ratings yet
- Acute Pancreatitis by DR DilmoDocument50 pagesAcute Pancreatitis by DR Dilmosinan kNo ratings yet
- Surg 02 Manifestations of Gastrointestinal Diseases 2016 PDFDocument85 pagesSurg 02 Manifestations of Gastrointestinal Diseases 2016 PDFMarian Dane PunzalanNo ratings yet
- PancreatitisDocument59 pagesPancreatitisAarif RanaNo ratings yet
- PancreatitisDocument7 pagesPancreatitisavigenNo ratings yet
- Department of Faculty SurgeryDocument40 pagesDepartment of Faculty SurgeryMandar GokhaleNo ratings yet
- Exocrine Pancreatic and Biliary Disorders and ManagementDocument77 pagesExocrine Pancreatic and Biliary Disorders and ManagementAnthon Kyle TropezadoNo ratings yet
- PANCREASDocument74 pagesPANCREASzaiba0786No ratings yet
- Pancreatitis Group 5Document25 pagesPancreatitis Group 5Mark Jefferson LunaNo ratings yet
- Git 3 PDFDocument9 pagesGit 3 PDFAnonymous biAu5PONo ratings yet
- Hepatic Encephalopathy and ComaDocument4 pagesHepatic Encephalopathy and ComaAriana ValenciaNo ratings yet
- Welcome To The Morning Session: Dr. Sadia AfrinDocument37 pagesWelcome To The Morning Session: Dr. Sadia AfrinGENERAL sharpNo ratings yet
- Nu'man AS DaudDocument23 pagesNu'man AS DaudHidayat BazeherNo ratings yet
- Acute PancreatitisDocument79 pagesAcute Pancreatitiszaiba0786No ratings yet
- CPC PancreatitisDocument67 pagesCPC PancreatitisM. Baidar SaeedNo ratings yet
- Acute PancreatitisDocument10 pagesAcute PancreatitisHarbin NicholsonNo ratings yet
- Case Presentation: Family Medicine Team C Gerry Martin, MD Christie Prendergast, MS3 Annie Lim, MS3Document24 pagesCase Presentation: Family Medicine Team C Gerry Martin, MD Christie Prendergast, MS3 Annie Lim, MS3Aditya Sonal Mahajan100% (1)
- Guideline PancreatitisDocument39 pagesGuideline Pancreatitisanda_No ratings yet
- Acute Pancreatitis SymptomsDocument12 pagesAcute Pancreatitis SymptomsUthraa SalvatoreNo ratings yet
- What Are The Common Clinical Manifestation and Causes of Acute Pancreatitis?Document2 pagesWhat Are The Common Clinical Manifestation and Causes of Acute Pancreatitis?Nyein Nu WinnNo ratings yet
- Dr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyDocument33 pagesDr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyAjung SatriadiNo ratings yet
- Accesory OrganDocument12 pagesAccesory OrganTrisha SuazoNo ratings yet
- Acute AbdomenDocument60 pagesAcute AbdomenAnish DhamiNo ratings yet
- Acute PancreatitisDocument25 pagesAcute PancreatitisSunil YadavNo ratings yet
- Acute Pancreatitis With Normal Serum Lipase: A Case SeriesDocument4 pagesAcute Pancreatitis With Normal Serum Lipase: A Case SeriesSilvina VernaNo ratings yet
- Hepatobiliary DisorderDocument49 pagesHepatobiliary DisorderAhmed KanemazeNo ratings yet
- Pancreatitispptnitinm1st 181229090413Document58 pagesPancreatitispptnitinm1st 181229090413enam professorNo ratings yet
- Hematemesis Melena Due To Helicobacter Pylori Infection in Duodenal Ulcer: A Case Report and Literature ReviewDocument6 pagesHematemesis Melena Due To Helicobacter Pylori Infection in Duodenal Ulcer: A Case Report and Literature ReviewodiNo ratings yet
- TOGADO - SEVERE PERITONITIS (Disorder Analysis and NCP)Document10 pagesTOGADO - SEVERE PERITONITIS (Disorder Analysis and NCP)John Paul TogadoNo ratings yet
- პანკრეასიDocument24 pagesპანკრეასიSASIDHARNo ratings yet
- Acute Kidney Injury Case Study FinalDocument46 pagesAcute Kidney Injury Case Study FinalSalwa KaramanNo ratings yet
- Acute PancreatitisDocument19 pagesAcute PancreatitisFloida Rose KatterNo ratings yet
- Cirrhosis Hours: 5. Working Place: Classroom, Hospital Wards. QuestionsDocument5 pagesCirrhosis Hours: 5. Working Place: Classroom, Hospital Wards. QuestionsNahanNo ratings yet
- Update On The Management of PancreatitisDocument92 pagesUpdate On The Management of Pancreatitisadamu mohammadNo ratings yet
- Acute Renal FailureDocument15 pagesAcute Renal FailureFilip DadićNo ratings yet
- Towards Evidence-Based and Personalised Care of Acute PancreatitisDocument7 pagesTowards Evidence-Based and Personalised Care of Acute PancreatitisFavio Alvarez De BejarNo ratings yet
- Renal Nursing - HandoutDocument16 pagesRenal Nursing - HandoutJoms Kim Mina100% (3)
- Sas S8Document10 pagesSas S8Ralph Louie ManagoNo ratings yet
- Biliary System and Pancreatic DisorderDocument59 pagesBiliary System and Pancreatic DisorderAlda AdeliaNo ratings yet
- Peptic Ulsers CompicationesDocument40 pagesPeptic Ulsers CompicationesMr FuckNo ratings yet
- Pancreatitis: 1 Signs and SymptomsDocument6 pagesPancreatitis: 1 Signs and SymptomsZiedTrikiNo ratings yet
- Seminar On Acute PancreatitisDocument20 pagesSeminar On Acute PancreatitisJoice DasNo ratings yet
- Pancreatite AgudaDocument8 pagesPancreatite AgudaGabriel MouraNo ratings yet
- Liver, Pancreas and Biliary Tract Problems: Case StudyDocument62 pagesLiver, Pancreas and Biliary Tract Problems: Case StudyElaine Frances IlloNo ratings yet
- Pathophysiology of Pyelonephritis: How It HappensDocument6 pagesPathophysiology of Pyelonephritis: How It HappensReno Jun NagasanNo ratings yet
- Our Lady of Fatima University - Valenzuela Campus College of NursingDocument29 pagesOur Lady of Fatima University - Valenzuela Campus College of NursingMary Shine GonidaNo ratings yet
- 1 Problemas de Motilidad GIDocument13 pages1 Problemas de Motilidad GIFlor De LotoNo ratings yet
- Acute Pancreatitis: Mycobacterium Avium Complex), Peritoneal Dialysis, Cardiopulmonary Bypass, ERCPDocument8 pagesAcute Pancreatitis: Mycobacterium Avium Complex), Peritoneal Dialysis, Cardiopulmonary Bypass, ERCPRizka KartikasariNo ratings yet
- A Rare Complication of Acute Appendicitis: Superior Mesenteric Vein ThrombosisDocument4 pagesA Rare Complication of Acute Appendicitis: Superior Mesenteric Vein ThrombosisEsha Putriningtyas SetiawanNo ratings yet
- Acute Pancreatitis Case PresDocument29 pagesAcute Pancreatitis Case Preskristine keen buanNo ratings yet
- Case Alcohol Abuse and Unusual Abdominal Pain in A 49-Year-OldDocument7 pagesCase Alcohol Abuse and Unusual Abdominal Pain in A 49-Year-OldPutri AmeliaNo ratings yet
- A Rare Case Report: Subcapsular Hepatic Hematoma As A Complication of PreeclampsiaDocument3 pagesA Rare Case Report: Subcapsular Hepatic Hematoma As A Complication of PreeclampsiaasclepiuspdfsNo ratings yet
- Case Concept Acute PrancreatitisDocument8 pagesCase Concept Acute PrancreatitisGio GallegoNo ratings yet
- Drug Overdose and PoisoningDocument64 pagesDrug Overdose and Poisoningsembakarani thevagumaranNo ratings yet
- Obstetric EmergenciesDocument96 pagesObstetric Emergenciessembakarani thevagumaranNo ratings yet
- Near DrowningDocument19 pagesNear Drowningsembakarani thevagumaranNo ratings yet
- Severe Sepsis and Septic ShockDocument47 pagesSevere Sepsis and Septic Shocksembakarani thevagumaranNo ratings yet
- Git BleedingDocument28 pagesGit Bleedingsembakarani thevagumaranNo ratings yet
- MR K DemoDocument2 pagesMR K Demosembakarani thevagumaranNo ratings yet
- Return LabelDocument1 pageReturn Labelsembakarani thevagumaranNo ratings yet
- Peperiksaan Percubaan: (MCQ-T/F) ADIC 510302Document7 pagesPeperiksaan Percubaan: (MCQ-T/F) ADIC 510302sembakarani thevagumaranNo ratings yet
- Feature PhoneDocument5 pagesFeature Phonesembakarani thevagumaranNo ratings yet
- Jadual - Kelas 3BDocument2 pagesJadual - Kelas 3Bsembakarani thevagumaranNo ratings yet
- Maths Without Use of Pen Pencil (Sscstudy - Com)Document288 pagesMaths Without Use of Pen Pencil (Sscstudy - Com)sembakarani thevagumaranNo ratings yet
- SkinDocument20 pagesSkinsembakarani thevagumaranNo ratings yet
- DocumentDocument10 pagesDocumentsembakarani thevagumaranNo ratings yet
- How Do You Become A Mathematics Genius?Document4 pagesHow Do You Become A Mathematics Genius?sembakarani thevagumaranNo ratings yet
- Komplikasi Ginjal Dan HipertensiDocument8 pagesKomplikasi Ginjal Dan HipertensiEna ElisaNo ratings yet
- Teaching PlanDocument3 pagesTeaching PlanGiann AcuzarNo ratings yet
- Pharmacology of AntimycobacterialDocument7 pagesPharmacology of Antimycobacterialselflessdoctor100% (1)
- UremiaDocument10 pagesUremiaRye CalderonNo ratings yet
- Challenging Neurological Manifestations in Large Cell Neuroendocrine Carcinoma Lcnec A Case Study of Extensive Intracranial and Intradural MetastasesDocument3 pagesChallenging Neurological Manifestations in Large Cell Neuroendocrine Carcinoma Lcnec A Case Study of Extensive Intracranial and Intradural MetastasesHerald Scholarly Open AccessNo ratings yet
- Pelvic Inflammatory Disease-SCIENCEDocument7 pagesPelvic Inflammatory Disease-SCIENCELeanne Marie Paredes TanNo ratings yet
- Spirometry: How To Do The TestDocument4 pagesSpirometry: How To Do The TestMarc AbellaNo ratings yet
- Jurding DR Oyo PDFDocument12 pagesJurding DR Oyo PDFAlfred hartoyoNo ratings yet
- 2016 OITE Study Guide For ResidentsDocument273 pages2016 OITE Study Guide For Residentschu_chiang_3100% (1)
- Baloon Tamponade of Gastroesophageal VaricesDocument8 pagesBaloon Tamponade of Gastroesophageal VaricesCecilio MartínNo ratings yet
- G.R. No. 72964 January 7, 1988 FILOMENO URBANO, Petitioner, Hon. Intermediate Appellate Court and People of The Philippines, RespondentsDocument8 pagesG.R. No. 72964 January 7, 1988 FILOMENO URBANO, Petitioner, Hon. Intermediate Appellate Court and People of The Philippines, RespondentsVeah CaabayNo ratings yet
- Animal HusbandryDocument21 pagesAnimal HusbandryKshiteeja DushingNo ratings yet
- Smoke Inhalation: Smoke Inhalation Is The Breathing in of Harmful FumesDocument4 pagesSmoke Inhalation: Smoke Inhalation Is The Breathing in of Harmful FumesalanNo ratings yet
- Scientific Research Journal of India SRJI Vol-3 Issue-3 Year 2014Document209 pagesScientific Research Journal of India SRJI Vol-3 Issue-3 Year 2014Dr. Krishna N. SharmaNo ratings yet
- BMI CalculatorDocument1 pageBMI CalculatorchandrimaNo ratings yet
- Diabetes Mellitus: Hyperglycemia (304 MG/DL, 13.2 MG/DL)Document3 pagesDiabetes Mellitus: Hyperglycemia (304 MG/DL, 13.2 MG/DL)John Henry ValenciaNo ratings yet
- Pe103-Course-Guide-And-Module-Sem. 2022-2023Document55 pagesPe103-Course-Guide-And-Module-Sem. 2022-2023Thomas Danjo ManulatNo ratings yet
- Diuretic Drugs For Nursing PharmacologyDocument1 pageDiuretic Drugs For Nursing Pharmacologylhayes1234100% (7)
- School Form 8 SF8 Learner Basic Health and Nutrition ReportDocument10 pagesSchool Form 8 SF8 Learner Basic Health and Nutrition ReportRey Moca100% (1)
- GsisDocument3 pagesGsisPecu MT ProvinceNo ratings yet
- Menstrual Disorders - SDYV TTC-2Document86 pagesMenstrual Disorders - SDYV TTC-2Joanna EvansNo ratings yet
- Myelomeningocele: A New Functional Classification: PerspectiveDocument5 pagesMyelomeningocele: A New Functional Classification: PerspectiveLema Ulloa ZoraidaNo ratings yet
- UG 1st 2nd 3rd Yr Syllabus BUMS Unani PDFDocument90 pagesUG 1st 2nd 3rd Yr Syllabus BUMS Unani PDFSameer Sam100% (1)
- HLTENN004 Assignment - NursingDocument4 pagesHLTENN004 Assignment - NursingJulianneTintNo ratings yet
- Care of A Bedridden Patient: Prepared by Jannet Reena PuraniDocument25 pagesCare of A Bedridden Patient: Prepared by Jannet Reena PuraniAnn Merlin Jobin100% (1)
- Case 76Document3 pagesCase 76Yelrebmik OdranrebNo ratings yet
- 1-History-of-MedTech 2Document47 pages1-History-of-MedTech 2Sarah NiñoNo ratings yet
- dotAIO V2 LiteDocument1 pagedotAIO V2 LiteStevanusNo ratings yet