Professional Documents
Culture Documents
Lecture 3 Thyroid, Parathyroid and Adrenal Gland
Uploaded by
Muhammad Shayan0 ratings0% found this document useful (0 votes)
3 views74 pagesCopyright
© © All Rights Reserved
Available Formats
PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
3 views74 pagesLecture 3 Thyroid, Parathyroid and Adrenal Gland
Uploaded by
Muhammad ShayanCopyright:
© All Rights Reserved
Available Formats
Download as PDF, TXT or read online from Scribd
You are on page 1of 74
Thyroid Gland And Parathyroid
Gland And Disorders
By
Saleet Abdullah
Lecturer KMU-IHS Swabi
Objectives
• Review the anatomy and physiology of thyroid
gland and parathyroid gland
• Discuss the mechanism of hypothalamic
pituitary thyroid feedback system
• Discuss Hypothyroidism [Goiter (Non-Toxic),
Cretinism, Myxedema] as thyroid gland
disorders
• Discuss the Hyperthyroidism [Grave's Disease
and Goiter (Toxic)] as thyroid gland disorders
Objectives
• Explain the mechanism of action of
parathyroid hormone (Parathormone and
Calcitonin
• Analyze effects of hypo and hyper-
parathyroidism on body systems (Renal and
musculoskeletal)
• Review the Anatomy and Physiology of the
Adrenal gland
Objectives
• Describe the functions of adrenal cortex
hormones (corticosteroid)
• Discuss Cushing’s syndrome and Addison’s
disease
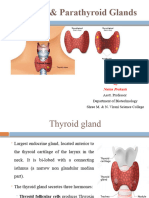
Thyroid Gland
• The thyroid gland—the largest endocrine
gland—is a butterfly-shaped organ located in
the lower neck, anterior to the trachea .
• It consists of two lateral lobes connected by
an isthmus. The gland is about 5 cm long and
3 cm wide and weighs about 30 g.
Thyroid Gland Cont..
• The blood flow to the thyroid is very high
(about 5 mL/min per gram of thyroid tissue),
approximately five times the blood flow to the
liver. The thyroid gland produces three
hormones: thyroxine (T4 ), triiodothyronine
(T3 ), and calcitonin.
Thyroid Gland Cont..
Physiology Of Thyroid Gland
• Thyroid hormone is comprised of T4 and T3 ,
two separate hormones produced by the
thyroid gland.
• Both are amino acids that contain iodine
molecules bound to the amino acid structure;
T4 contains four iodine atoms in each
molecule, and T3 contains three.
Physiology of thyroid Gland
• Thyroid hormone increases the metabolism
and protein synthesis in nearly all of the
tissues of the body.
• It also is necessary for brain development and
growth in infants and small children.
• The thyroid hormones influence cell
replication and are important in brain
development.
Hypothalamic-Pituitary-
Thyroid Feedback System.
Hypothyroidism
• Hypothyroidism can occur as a congenital or
an acquired defect.
• Congenital Hypothyroidism affects
approximately 1 of 5000 infants.
Hypothyroidism in the infant may result from
a congenital lack of the thyroid gland or from
abnormal biosynthesis of thyroid hormone or
deficient TSH secretion.
Hypothyroidism Cont..
• Acquired Hypothyroidism occurs in older
children and adults causes a general slowing
down of metabolic processes.
Causes of Hypothyroidism
• Autoimmune disease (Hashimoto thyroiditis)
• Atrophy of thyroid gland with aging
• Therapy for hyperthyroidism
• Thyroidectomy
• Medications
S/S Hypothyroidism
Pathophysiology
Hypothyroidism
• TSH, which is created and secreted in the anterior
pituitary under activation of thyrotropin-releasing
hormone produced in the hypothalamus, directly
stimulates thyroid gland hormone synthesis.
• The thyroid glands metabolism is regulated by a
negative feedback regulatory system in people with
a healthy hypothalamic-pituitary-thyroid axis.
• TSH levels are controlled by the pituitary gland in
response to feedback from T4 and T3 levels, which
act as biosensors of thyroid hormone levels.
Pathophysiology
Hypothyroidism
• TSH secretion is increased when thyroid
hormone synthesis declines.
• TSH stimulates hypertrophy and hyperplasia of
the thyroid gland.
Goiter (Non-Toxic)
• A nontoxic goiter is a diffuse or nodular
enlargement of the thyroid gland that does not
result from an inflammatory or neoplastic
process.
Causes
1. Iodine deficiency
2. Childhood head and neck radiation - Radiation
exposure during childhood results in benign and
malignant nodules.
Cretinism
• The manifestations of untreated congenital
hypothyroidism (stunted growth and mental
retardation) are referred to as Cretinism.
• Thyroid hormone is essential for normal growth
and brain development, almost half of which
occurs during the first 6 months of life. If
untreated, congenital hypothyroidism causes
Mental Retardation and Impairs Physical
Growth.
• Congenital primary hypothyroidism, occurring in
approximately 1:2000 to 1:4000 newborns
Cretinism Causes
• Lack of thyroid gland and failure of the thyroid gland to
produce thyroid hormones.
• Iodine deficiency in the diet.
• A missing, poorly formed, or abnormally small thyroid
gland
• A genetic defect that affects thyroid hormone
production
• Too little iodine in the mother’s diet during pregnancy
• Anti-thyroid treatment for thyroid cancer during
pregnancy
• Use of medicines that disrupt thyroid hormone
production — such as anti-thyroid drugs, sulfonamides,
or lithium — during pregnancy
Clinical Manifestations
• Generally characterized by stunted growth
and mental retardation.
• Short stature (dwarfism)
• The sparseness(thinly dispersed or scattered.)
of hair and nails.
• Retardation of sexual attributes.
• Hearing and speech defects.
• Constipation
Myxedema
• Myxedema is another term for severely
advanced hypothyroidism. It’s a condition that
occurs when your body doesn’t produce
enough thyroid hormone.
• It is a medical emergency with a high mortality
rate.
• More severe symptoms, such as hypothermia
or shock, could indicate a myxedema crisis
requiring immediate medical attention.
Myxedema Causes
Hypothyroidism occurs when the thyroid stops
functioning correctly. This may be caused by:
• An autoimmune condition,
including Hashimoto’s thyroiditis
• Surgical removal of your thyroid
• Radiation therapy for cancer
• Certain medications, like lithium
or amiodarone (pacerone)
Clinical Manifestation
Myxedema
• Weight gain
• Weakness
• Cold intolerance
• Constipation
• Depressed mood
• Low systolic and high diastolic blood pressure
• Low heart rate
• Sparse or brittle hair
Hyperthyroidism
• Hyperthyroidism happens when the thyroid
gland makes too much thyroid hormone. This
condition also is called overactive thyroid.
• Hyperthyroidism, a common endocrine
disorder, is a form of Thyrotoxicosis resulting
from an excessive synthesis and secretion of
endogenous or exogenous thyroid hormones
by the thyroid.
Hyperthyroidism Causes
• Graves disease: the most common cause of
hyperthyroidism.
• Thyroid nodules: A thyroid nodule is a lump or growth of
cells in your thyroid gland. They can produce more
hormones than your body needs. Thyroid nodules are
rarely cancerous.
• Thyroiditis: Thyroiditis is inflammation of your thyroid
gland.
• Consuming excess iodine.
• Amiodarone: a medication that contains a high amount of
iodine, may also cause hyperthyroidism.
Hyperthyroidism Pathophysiology
• The production and release of thyroid hormones is regulated by a
sensitive negative feedback loop involving the hypothalamus,
pituitary gland, and thyroid gland.
• The increased production of thyroid hormone normally causes
inhibition of TRH and TSH release by the hypothalamus and pituitary
respectively.
• Disruption of this delicate system leads to additional production and
release of thyroid hormone and subsequent hyperthyroidism.
• TSH-secreting pituitary tumors release biologically active hormone
that is unresponsive to normal feedback control.
• The tumors may co-secrete prolactin or growth hormone; therefore,
patients may present with amenorrhea, galactorrhea, or signs of
acromegaly.
S/S Hyperthyroidism
Graves Disease
• The condition gets its name from Robert Graves, an
Irish Doctor who first described the condition in the
1800s.
• Graves’ disease affects nearly 1 in 100
Americans. About 4 out of 5 cases of
hyperthyroidism in the United States are caused by
Graves’ disease.
• Graves’ disease affects more people assigned
Female at Birth than people assigned male at birth.
It typically occurs in people between the ages of 30
and 50, but it can affect children and older adults.
Causes Graves Disease
• Researchers don’t know what causes autoimmune
diseases like Graves’ disease. Something triggers
your immune system to overproduce an antibody
called thyroid-stimulating immunoglobulin (TSI). TSI
attaches to healthy thyroid cells, causing your thyroid
to overproduce thyroid hormones.
• Virus/infection.
S/S Graves Disease
Patients with hyperthyroidism exhibit a characteristic group of
signs and symptoms.
• Palpitations
• Tachycardia or dysrhythmias, increased pulse pressure
• Myocardial hypertrophy
• Exophthalmos (abnormal protrusion of one or both
eyeballs)
• Increased appetite and dietary intake
• Weight loss, fatigability and weakness (difficulty in climbing
stairs and rising from a chair)
• Amenorrhea
• Changes in bowel function.
Goiter (Toxic)
• Goiter is a condition where the thyroid
gland grows larger. The entire thyroid can
grow larger or it can develop one or more
small lumps called Thyroid nodules.
• A goiter may be associated with no change in
thyroid function or with an increase or
decrease in thyroid hormones.
Diffuse Goiter Nodular Goiter
Causes Goiter(Toxic)
• Iodine deficiency
• Graves' disease
• Hashimoto's disease
• Thyroid cancer
• Pregnancy
• Thyroiditis
S/S Goiter(Toxic)
• A lump in the front of your neck, just below
your Adam's apple.
• A feeling of tightness in your throat area.
• Hoarseness (scratchy voice).
• Neck vein swelling.
Parathyroid Gland
• The parathyroid glands (normally four) are
situated in the neck and embedded in the
posterior aspect of the thyroid gland .
• Each gland is usually oval in shape and about
the size of a pea.
Parathyroid Gland
Physiology Parathyroid Gland
• Parathormones (parathyroid hormone)—the
protein hormone produced by the parathyroid
glands—regulates calcium and phosphorus
metabolism. Increased secretion of
Parathormones results in increased calcium
absorption from the kidney, intestine, and
bones, which raises the serum calcium level.
Physiology Parathyroid
Gland
Parathyroid glands produce parathyroid hormone, which plays a
key role in the regulation of calcium levels in the blood.
Precise calcium levels are important in the human body, since
small changes can cause muscle and nerve problems.
• The parathyroid hormone stimulates the following functions:
• Release of calcium by bones into the bloodstream
• Absorption of calcium from food by the intestines
• Conservation of calcium by the kidneys
• Stimulates cells in the kidney to transforms weaker forms of
vitamin D into the form that is strongest at absorbing calcium
from the intestines
Mechanism Of Action Of
Parathyroid Hormone
• Parathyroid hormone is an essential regulator
of extracellular calcium and phosphate.
• PTH enhances calcium re-absorption while
inhibiting phosphate re-absorption in the
kidneys, increases the synthesis of vitamin D,
which then increases gastrointestinal
absorption of calcium, and increases bone
resorption to increase calcium and phosphate.
Mechanism Of Action Of
Parathyroid Hormone
Calcitonin
• Calcitonin is a hormone that your thyroid
gland makes and releases to help regulate
calcium levels in your blood by decreasing it.
Calcitonin opposes the actions of the
parathyroid hormone, which is a hormone
that increases your blood calcium levels.
Mechanism Of Action Of
Calcitonin
Calcitonin’s main job is to lower calcium levels in your
blood (not your bones). It does this in two main ways:
• Calcitonin inhibits (blocks) the activity of osteoclasts,
which are cells that break down bone. When osteoclasts
break down your bone, the calcium from your bone is
released into your bloodstream. Therefore, the
temporary blocking of osteoclasts by calcitonin reduces
the amount of calcium that enters your blood.
• Calcitonin can decrease the amount of calcium that
your kidneys reabsorb and release back into your
bloodstream, thus causing lower blood calcium levels.
Mechanism Of Action Of
Calcitonin
Hyperparathyroidism
• Hyperparathyroidism is a condition in which
one or more of your parathyroid glands
become overactive and release (secrete) too
much parathyroid hormone (PTH). This causes
the levels of calcium in your blood to rise, a
condition known as hypercalcemia.
Hyperparathyroidism
There are two types of hyperparathyroidism, primary and
secondary:
• In primary hyperparathyroidism, your parathyroid
glands make too much PTH, which causes the level of
calcium in your blood to rise.
• In secondary hyperparathyroidism, the over activity of
the parathyroid glands occurs in response to another
condition that’s causing calcium loss. Parathyroid over
activity is an attempt on your body’s part to keep the
calcium levels normal. Examples of conditions that
lower calcium levels include kidney failure,
severe vitamin D deficiency and severe calcium
deficiency.
HPT Effects on Kidneys
• The formation of stones in one or both kidneys
(nephrolithiasis), related to the increased urinary
excretion of calcium and phosphorus, is one of
the major complications of hyperparathyroidism.
• The small intestine may absorb more calcium
from food, adding to high levels of calcium in
your blood. Extra calcium that isn’t used by your
bones and muscles goes to your kidneys and is
flushed out in urine. Too much calcium in your
urine can cause kidney stones.
HPT Effects on Kidneys
Increased Calcium Reabsorption:
Hyperparathyroidism stimulates the renal tubules
to reabsorb more calcium from the urine. This
contributes to hypercalcemia and can lead to the
formation of kidney stones.
Nephrolithiasis (Kidney Stones):Elevated levels of
calcium in the urine due to hyperparathyroidism
increase the risk of kidney stone formation.
Calcium oxalate and calcium phosphate stones
are common in hyperparathyroid patients.
HPT Effects on
Musculoskeletal
• The patient may develop skeletal pain and
tenderness, especially of the back and joints;
pain on weight bearing; pathologic fractures;
deformities; and shortening of body stature.
Bone loss attributable to hyperparathyroidism
increases the risk of fracture
HPT Effects on
Musculoskeletal
Bone Resorption
• Effect: Hyperparathyroidism stimulates
osteoclasts, the cells responsible for breaking
down bone tissue. This process, known as bone
resorption, releases calcium from bones into the
bloodstream.
Osteoporosis and Increased Fracture Risk:
• Effect: Chronic elevation of PTH and subsequent
bone resorption can lead to a decrease in bone
mineral density, resulting in osteoporosis. This
makes the bones more prone to fractures.
HPT Effects on
Musculoskeletal
Muscle Weakness and Fatigue
• Effect: Hyperparathyroidism can lead to
muscle weakness and fatigue, although the
mechanisms are not fully understood. It may
be related to the direct effects of elevated PTH
on muscle cells.
Adrenal Gland
Anatomy:
Adrenal glands, also known as suprarenal
glands, are small, triangular-shaped glands
located on top of both kidneys.
Each person has two adrenal glands, one
attached to the upper portion of each kidney
(Porth, 2015).
Adrenal Gland
An adrenal gland is made of two main parts:
The adrenal cortex is the outer region and also
the largest part of an adrenal gland. It is
divided into three separate zones: zona
glomerulosa, zona fasciculata and zona
reticularis. Each zone is responsible for
producing specific hormones.
Adrenal Gland
• The adrenal medulla is located inside the
adrenal cortex in the center of an adrenal
gland. It produces “stress hormones,”
including adrenaline.
• The adrenal cortex and adrenal medulla are
enveloped in an adipose capsule that forms a
protective layer around an adrenal gland.
Adrenal Gland
Adrenal Gland
Physiology:
The role of the adrenal glands in your body is to
release certain hormones directly into the
bloodstream. Many of these hormones have
to do with how the body responds to stress,
and some are vital to existence. Both parts of
the adrenal glands — the adrenal cortex and
the adrenal medulla — perform distinct and
separate functions.
Adrenal Gland
• Each zone of the adrenal cortex secretes a
specific hormone. The key hormones produced
by the adrenal cortex include:
• Cortisol
• Cortisol is a glucocorticoid hormone produced by
the zona fasciculata that plays several important
roles in the body. It helps control the body’s use
of fats, proteins and carbohydrates; suppresses
inflammation; regulates blood pressure;
increases blood sugar; and can also decrease
bone formation.
Adrenal Gland
• This hormone also controls the sleep/wake
cycle. It is released during times of stress to
help your body get an energy boost and better
handle an emergency situation.
Adrenal Gland
• Aldosterone
• This mineralocorticoid hormone produced by the
zona glomerulosa plays a central role in
regulating blood pressure and certain electrolytes
(sodium and potassium). Aldosterone sends
signals to the kidneys, resulting in the kidneys
absorbing more sodium into the bloodstream and
releasing potassium into the urine. This means
that aldosterone also helps regulate the blood pH
by controlling the levels of electrolytes in the
blood.
Adrenal Gland
Androgenic Steroids:
These hormones produced by the zona
reticularis are weak male hormones. They are
precursor hormones that are converted in the
ovaries into female hormones (estrogens) and
in the testes into male hormones (androgens).
Adrenal Gland
Epinephrine (Adrenaline) and Norepinephrine
(Noradrenaline):
• The adrenal medulla, the inner part of an
adrenal gland, controls hormones that initiate
the flight or fight response. The main
hormones secreted by the adrenal medulla
include epinephrine (adrenaline) and
norepinephrine (noradrenaline), which have
similar functions.
Adrenal Gland
Cushing Syndrome:
Cushing syndrome is an uncommon condition
that happens when your body has too much
of a hormone called cortisol.
Another word for Cushing syndrome is
hypercortisolism.
A syndrome is a medical term that refers to a
group of signs and symptoms that happen
together.
Adrenal Gland
Pathophysiology:
• When stimulated by ACTH, the adrenal gland
secretes cortisol and other steroid hormones.
• The switch that controls the feedback
mechanism is cortisol
• When the levels are low the system turns on
and when high the system turns off.
• Excessive use of steroids leads to excess free
circulation of cortisol in the body.
Adrenal Gland
• Excess cortisol in the body will cause the liver
to release more sugar, increased breakdown
of muscle and fat for energy and also lowers
the amount of energy used by the cells of the
body.
• It will also increase the inflammatory effects
and lowers the body's ability to protect itself.
Adrenal Gland
Causes:
• Use of glucocorticoid medications.
Glucocorticoid medications (for example,
prednisone) are used to treat many
autoimmune diseases, such as chronic
asthma, rheumatoid arthritis.
• Pituitary tumors. Pituitary tumors that make
too much ACTH (the hormone that tells the
adrenal glands to make cortisol)
Adrenal Gland
• Adrenal cortical tumors. A tumor on the
adrenal gland itself can make too much
cortisol.
• Lung, pancreas, thyroid and thymus tumors.
Ectopic ACTH syndrome happens when
tumors that develop outside of the pituitary
gland produce ACTH. These types of tumors
are typically malignant. The most common
type is small cell lung cancer.
Adrenal Gland
Sign & Symptoms:
• Rapid weight gain in the face (sometimes
called “moon face”), abdomen, back of the
neck (sometimes called “buffalo hump”) and
chest.
• A red, round face.
• Wounds that heal poorly.
• High blood pressure (hypertension).
Adrenal Gland
• Excessive hair growth on the face, neck, chest,
abdomen, breasts and thighs, or balding.
• Diabetes.
• Other signs and symptoms of Cushing
syndrome include:
• Purple stretch marks over the abdomen.
• Easy bruising on the arms and legs
Adrenal Gland
Addison Disease:
Addison’s disease is also called primary adrenal
insufficiency.
Addison’s disease is a chronic condition in which
your adrenal glands don’t produce enough of
the hormones cortisol and aldosterone.
Adrenal Gland
Causes:
• Approximately 75% of cases of Addison’s
disease are due to an autoimmune attack.
• Repeated infections, including HIV/AIDS-
related infections and fungal infections.
• When cancer cells from another part of your
body invade your adrenal glands.
• Bleeding (hemorrhaging) into your adrenal
glands.
• Surgical removal of your adrenal glands.
Adrenal Gland
Adrenal Gland
Sign & Symptoms:
• Extreme fatigue
• Weight loss and loss of appetite
• Areas of darkened skin
• Low blood pressure, even fainting
• Salt craving
• Low blood sugar, also called hypoglycemia
• Nausea, diarrhea or vomiting
• Abdominal pain
• Muscle and joint pain
• Irritability
• Depression
• Body hair loss or sexual issues in some people
References
• Pathophysiology concepts of altered health states(eighth
edition)
• Brunner Suddarth's Textbook of Medical-surgical Nursing,(14th
edition)
• emedicine.medscape.com/article/120392
• www.healthline.com/health/congenital-
hypothyroidism#causes
• https://my.clevelandclinic.org/health/diseases/14129-
hyperthyroidism
• https://www.austinpublishinggroup.com/endocrinology-
diabetes/fulltext/ajed-v9-id1091.pdf
• my.clevelandclinic.org/health/diseases/12625-goiter
References
• www.sciencedirect.com/topics/biochemistry-
genetics-and-molecular-biology/parathyroid-
hormone
• Hyperparathyroidism: Treatment, Symptoms,
Causes & Diagnosis (clevelandclinic.org)
• Silverberg, S. J., & Bilezikian, J. P. (2003).
"Asymptomatic primary hyperparathyroidism."
The Journal of Clinical Endocrinology &
Metabolism, 88(12), 5651-5656.
References
• Bilezikian, J. P., Marcus, R., & Levine, M. A. (Eds.). (2001). The
Parathyroids: Basic and Clinical Concepts. Academic Press.
• Coe, F. L., Parks, J. H., & Asplin, J. R. (1992). The pathogenesis and
treatment of kidney stones. New England Journal of Medicine,
327(16), 1141-1152.
• Bilezikian, J. P., et al. (2014). "Guidelines for the management of
asymptomatic primary hyperparathyroidism: summary statement
from the third international workshop." The Journal of Clinical
Endocrinology & Metabolism, 99(10), 3561-3569.
• Vestergaard, P. (2007). "Muscular weakness and functional stability
in the elderly: an overview." Journal of Musculoskeletal Neuronal
Interactions, 7(3), 277-283.
You might also like
- EI Laying OFC 310107Document21 pagesEI Laying OFC 310107agmtechnical100% (1)
- Overview:: Book Title:-Strategic Management Author:-Michael A. Hitt - R. Duane Ireland - Robert E. HoskissonDocument2 pagesOverview:: Book Title:-Strategic Management Author:-Michael A. Hitt - R. Duane Ireland - Robert E. HoskissonSuvid Sharma0% (1)
- Program Book ICHVEPS 2019 1 PDFDocument41 pagesProgram Book ICHVEPS 2019 1 PDFkuncoroNo ratings yet
- Magnetic Memory Method 1029Document17 pagesMagnetic Memory Method 1029asoooomi_11No ratings yet
- Thyroid Gland Dont Erase Ate KatDocument24 pagesThyroid Gland Dont Erase Ate KatThess Tecla Zerauc AzodnemNo ratings yet
- Thyroid and Adrenal MedullaDocument32 pagesThyroid and Adrenal MedullaDipika RawatNo ratings yet
- Thyroid Gland EnlargementDocument51 pagesThyroid Gland EnlargementKhodijah SalahudinNo ratings yet
- Thyrotoxicosi S: Dr.P.Viswakumar M.S Assistant Professor, Dept of General Surgery, PsgimsrDocument57 pagesThyrotoxicosi S: Dr.P.Viswakumar M.S Assistant Professor, Dept of General Surgery, PsgimsrpurnaNo ratings yet
- Hypo Thyroids MDocument26 pagesHypo Thyroids MBridget NjambiNo ratings yet
- Disorders of The Thyroid1Document22 pagesDisorders of The Thyroid1Saddamix AL OmariNo ratings yet
- Autoimmune Disease - Hashimoto's ThyroiditisDocument17 pagesAutoimmune Disease - Hashimoto's Thyroiditisitsme.chandlermbingNo ratings yet
- Thyroid Gland An Diseases of Thyroid D Gland: Omc LectureDocument59 pagesThyroid Gland An Diseases of Thyroid D Gland: Omc LectureEdward MakemboNo ratings yet
- Thyroid and ParathyroidDocument29 pagesThyroid and Parathyroidpranutan739No ratings yet
- Thyroid DiseaseDocument30 pagesThyroid Diseasemy Lord JesusNo ratings yet
- Endo Lect 7-THDocument30 pagesEndo Lect 7-THdoctorrfarrukhNo ratings yet
- Prac Theme 2.5Document182 pagesPrac Theme 2.5alkalicharanNo ratings yet
- Hyperthyroidism and HypothyroidismDocument59 pagesHyperthyroidism and HypothyroidismJun AmaroNo ratings yet
- Thyrotoxicosis Seb 4Document35 pagesThyrotoxicosis Seb 4Bersisa chalchisaNo ratings yet
- Thyroid and Antithyroid DrugsDocument59 pagesThyroid and Antithyroid DrugsKhairunnisa LoqmanNo ratings yet
- Hormones of Thyroid and Parathyroid GlandDocument16 pagesHormones of Thyroid and Parathyroid Glandapi-25908492100% (1)
- Assessment and Management of Patients With Endocrine DisordersDocument55 pagesAssessment and Management of Patients With Endocrine Disorderseliza marie luisNo ratings yet
- ENDOCRINE SYSTEM DISORDERS Unit 1Document8 pagesENDOCRINE SYSTEM DISORDERS Unit 1Rizza Mae MaglacionNo ratings yet
- Week 16 EndocrineDocument55 pagesWeek 16 EndocrineEditha LucasNo ratings yet
- Thyroid DrugsDocument22 pagesThyroid Drugsanon_569360085No ratings yet
- ThyroidDocument20 pagesThyroidako798918No ratings yet
- CVD & ThyroidDocument12 pagesCVD & ThyroidShang AllertseNo ratings yet
- ThyroidDocument44 pagesThyroidHossen AliNo ratings yet
- ThyroidDocument96 pagesThyroidNimer Abdelhadi AliNo ratings yet
- Endocrine Physiology Lecture by Mrs M MUTSANGU POLY ND1Document56 pagesEndocrine Physiology Lecture by Mrs M MUTSANGU POLY ND1letwinemwale02No ratings yet
- Hypothyroidism and Pregnancy What Should I Know FactsheetDocument1 pageHypothyroidism and Pregnancy What Should I Know FactsheetNicole KrishnaNo ratings yet
- HypothyroidismDocument4 pagesHypothyroidismDennis RosinNo ratings yet
- HPERTHYROIDISMDocument4 pagesHPERTHYROIDISMSalwa KaramanNo ratings yet
- Thyroid Hormones: K.Ramachandran M.Sc. Medical Biochemistry SRM Medical CollegeDocument31 pagesThyroid Hormones: K.Ramachandran M.Sc. Medical Biochemistry SRM Medical CollegeKuzhandai VeluNo ratings yet
- 35thyroid DisordersDocument21 pages35thyroid DisordersDurga VoraNo ratings yet
- Thyroid Function: Clinical Chemistry IiiDocument20 pagesThyroid Function: Clinical Chemistry IiiJannica Dominique ClarosNo ratings yet
- Hyperthyroidism: What Is The Thyroid Gland?Document8 pagesHyperthyroidism: What Is The Thyroid Gland?scremo_xtremeNo ratings yet
- Pathophysiology of Endocrine SystemDocument64 pagesPathophysiology of Endocrine SystemTess MohamedNo ratings yet
- Hyperthyroid Is MDocument22 pagesHyperthyroid Is MCsiangel NopuetoNo ratings yet
- Thyroid Gland Diseases in ChildrenDocument29 pagesThyroid Gland Diseases in ChildrenadinayNo ratings yet
- Archivo en Ingles-Patologias TiroideasDocument4 pagesArchivo en Ingles-Patologias Tiroideasesther avilaNo ratings yet
- Thyroid PresentationDocument38 pagesThyroid Presentation천사자No ratings yet
- Thyroid Hormones: Sherwin B. Toriano, RMT, MSMTDocument33 pagesThyroid Hormones: Sherwin B. Toriano, RMT, MSMTBenedikt WeinholdNo ratings yet
- Thyroid Diet: How to improve and cure thyroid disorders, lose weight, and improve metabolism with the help of food!From EverandThyroid Diet: How to improve and cure thyroid disorders, lose weight, and improve metabolism with the help of food!No ratings yet
- Patofisiologis Hipertiroid Dan HipotiroidDocument21 pagesPatofisiologis Hipertiroid Dan HipotiroidaidillahNo ratings yet
- Endocrine System 5Document15 pagesEndocrine System 5Ace Vincent LunaNo ratings yet
- Thyroid FinalDocument25 pagesThyroid Finalgowrie sangkarNo ratings yet
- Thiroid DisordersDocument11 pagesThiroid Disordersرعد النميريNo ratings yet
- PATIENT WITH ENDOCRINE DYSFUNCTION THYROID .pptx1Document52 pagesPATIENT WITH ENDOCRINE DYSFUNCTION THYROID .pptx1sembakarani thevagumaranNo ratings yet
- THYROID GLAND Final (Autosaved)Document81 pagesTHYROID GLAND Final (Autosaved)ABUBEKER BESHIRNo ratings yet
- Thyroid DisordersDocument32 pagesThyroid DisordersHarshilPatelNo ratings yet
- Pituitary DisorderDocument34 pagesPituitary DisorderSoniya ShivanshNo ratings yet
- Endocrine Diseases 1Document66 pagesEndocrine Diseases 1Nathaniel BudayNo ratings yet
- THYROID Disorders For PB BSCDocument81 pagesTHYROID Disorders For PB BSCchetankumarbhumireddy67% (3)
- Bio ProjectDocument7 pagesBio ProjectSakshi MakkarNo ratings yet
- Thyroid DisordersDocument55 pagesThyroid DisordersNsubuga Ivan100% (1)
- Thyroid and Parathyroid AgentsDocument28 pagesThyroid and Parathyroid AgentsMary Faith Kiat-ongNo ratings yet
- Goiter: Prepared By: Felix Kevin M. Villa Iv, RNDocument47 pagesGoiter: Prepared By: Felix Kevin M. Villa Iv, RNFelix Kevin VillaNo ratings yet
- Endocrine System 13 معدلDocument11 pagesEndocrine System 13 معدلhanaalhadidi567No ratings yet
- THYROIDDocument17 pagesTHYROIDvinolashrimmishma.sNo ratings yet
- Щитоподібна залоза ангDocument24 pagesЩитоподібна залоза ангdenysvorobchak-12No ratings yet
- Hypothyroidism (Underactive)Document3 pagesHypothyroidism (Underactive)jhNo ratings yet
- ThyrotoxicosisDocument105 pagesThyrotoxicosisAli Murtaza Abbas100% (1)
- Case Study of Hypothroidism SAHIL GUNJALDocument27 pagesCase Study of Hypothroidism SAHIL GUNJALDarling DadaNo ratings yet
- Mardinthyroid 141212101640 Conversion Gate02Document42 pagesMardinthyroid 141212101640 Conversion Gate02NiyaNo ratings yet
- C Programming Functions HomeworkDocument2 pagesC Programming Functions HomeworkAnonymous PDGLsjN1Q5No ratings yet
- Flir m100 m200 Series User ManualDocument112 pagesFlir m100 m200 Series User ManualAditi DasNo ratings yet
- University of Okara: 4th Merit List Department:School of Law Admissions:FALL 2020Document2 pagesUniversity of Okara: 4th Merit List Department:School of Law Admissions:FALL 2020Saghar Asi AwanNo ratings yet
- 2CDC446001D0201 Busbar SystemsDocument36 pages2CDC446001D0201 Busbar SystemsBorislav ChavdarovNo ratings yet
- Matrix-Vector Multiplication: Annika BiermannDocument34 pagesMatrix-Vector Multiplication: Annika BiermannSur3nNo ratings yet
- Prometric Test For Nurses Sample QuestionsDocument4 pagesPrometric Test For Nurses Sample QuestionsТанюша Галкина100% (1)
- PL Bardi LH RSDocument3 pagesPL Bardi LH RSwaskitowwNo ratings yet
- ABSU Post-UTME Past Questions and Answers For Science Students (Sciences, Medicine, Engineering and Agriculture)Document45 pagesABSU Post-UTME Past Questions and Answers For Science Students (Sciences, Medicine, Engineering and Agriculture)Kelvin Rex100% (1)
- WWWWMDocument36 pagesWWWWMRude Gal SheenaNo ratings yet
- Scribble and Jot Brand Style GuideDocument34 pagesScribble and Jot Brand Style GuideJoanna MalcomNo ratings yet
- OTA External Alarm Solution V1 18 - FinalDocument32 pagesOTA External Alarm Solution V1 18 - FinalKhaled NoNo ratings yet
- Exercise 1Document47 pagesExercise 1asthaNo ratings yet
- Explosive RegDocument26 pagesExplosive RegvictorNo ratings yet
- As7263 DS000476 1-00Document45 pagesAs7263 DS000476 1-00Faby ReveloNo ratings yet
- Untitled DocumentDocument4 pagesUntitled Documentallyssa abrogenaNo ratings yet
- Brain Activity During Second Language Processing (ERP)Document7 pagesBrain Activity During Second Language Processing (ERP)Su AjaNo ratings yet
- Knee Examination: DR Ghayur Abbas MBBS, Fcps (Pak), Frcs A (Eng)Document19 pagesKnee Examination: DR Ghayur Abbas MBBS, Fcps (Pak), Frcs A (Eng)awais ahmedNo ratings yet
- Self-Study Worksheet III Isomerism ANSWERSDocument2 pagesSelf-Study Worksheet III Isomerism ANSWERSkjjkimkmkNo ratings yet
- Sgaw Karen StoryDocument22 pagesSgaw Karen StoryMoodawNo ratings yet
- Environmental StudiesDocument2 pagesEnvironmental StudiesBlessy BlessyNo ratings yet
- Skin Diseases: 100 Million Three MillionDocument2 pagesSkin Diseases: 100 Million Three MillionAria DomingoNo ratings yet
- Assignment Christianity Chapter 2Document5 pagesAssignment Christianity Chapter 2MohichehraNo ratings yet
- Advanced Hair Transplant 5Document18 pagesAdvanced Hair Transplant 5Naveed KhanNo ratings yet
- RC Detailers ManualDocument133 pagesRC Detailers Manualrealchic100% (2)
- Anesthesia For Laparoscopy in The Pediatric PatientDocument20 pagesAnesthesia For Laparoscopy in The Pediatric PatientfathiahusainNo ratings yet
- Toyota Avalon XL V6-3.0L (1MZ-FE) 2001: Timing Belt: Service and RepairDocument15 pagesToyota Avalon XL V6-3.0L (1MZ-FE) 2001: Timing Belt: Service and RepairFrancisco Guillen-DorantesNo ratings yet