Professional Documents
Culture Documents
Alex - Direct Pulp Capping 2018
Uploaded by
rodrigo guiboneCopyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Alex - Direct Pulp Capping 2018
Uploaded by
rodrigo guiboneCopyright:
Available Formats
CLINICAL TECHNIQUE REVIEW
Pulp Capping
Direct and Indirect Pulp Capping: A Brief History,
Material Innovations, and Clinical Case Report
Gary Alex, DMD
Abstract: Among the goals of pulp capping are to manage bacteria, arrest caries progression, stimulate pulp
cells to form new dentin, and produce a durable seal that protects the pulp complex. This article will provide
a general discussion of direct and indirect pulp capping procedures, offering practitioners a pragmatic and
science-based clinical protocol for treatment of vital pulp exposures. A clinical case will be presented in
which a novel light-cured resin-modified mineral trioxide aggregate hybrid material was used to manage a
mechanical vital pulp exposure that occurred during deep caries excavation.
D
irect and indirect pulp capping, employing various hybrid material to manage a mechanical vital pulp exposure that
materials and clinical protocols, has been used for occurred during deep caries excavation. The article aims to provide
many years to preserve the health and vitality of the a pragmatic, practical, and science-based clinical protocol for deal-
pulp complex and induce pulp cells to form hard tis- ing with vital pulp exposures.
sue (reparative/tertiary dentin). Direct pulp capping
is used when the pulp is visibly exposed (vital pulp exposure) due Indirect Pulp Capping: Two-Stage Approach
to caries, trauma, or iatrogenic insult such as accidental exposure When used appropriately, both direct and indirect pulp capping pro-
during tooth preparation or caries removal. Indirect pulp capping cedures have the potential to preserve pulp health, function, and
is generally used in deep cavity preparations, with or without caries vitality.1 In the case of indirect pulp capping, where the cavity prepa-
remaining, that are in close proximity to the pulp but with no visible ration is in close proximity to the pulp but with no visible exposure,
exposure. The ultimate objectives of any pulp capping procedure various one- and two-stage protocols have been advocated.2 With
should be to manage bacteria, arrest any residual caries progression, two-stage or stepwise caries removal techniques all carious dentin
stimulate pulp cells to form new dentin, and provide a biocompat- typically is removed from the walls and dentino-enamel junction of
ible and durable seal that protects the pulp complex from bacteria the cavity preparation. A layer of deep carious dentin, which is usu-
and noxious agents. ally discolored but firm, may be left on the floor of the preparation
The success of both direct and indirect pulp capping procedures is, if its removal might cause a pulp exposure.3 Typically, a liner such as
of course, contingent on the health and vitality of the pulp complex to calcium hydroxide [Ca(OH)2] is then placed and overlaid by a provi-
begin with. Teeth that have a history of unprovoked spontaneous pain, sional restoration such as zinc oxide and eugenol or glass ionomer.
necrotic or partially necrotic pulps, radiographic pathology, or exces- Of vital importance with this technique is the placement of a
sive hyperemia on direct pulp exposure due to irreversible pulpitis well-sealing provisional restoration for several months that isolates
have a poor prognosis and often require endodontic intervention or any remaining caries and bacteria from the oral environment. In
extraction at some point. Conversely, pulps that are vital and healthy fact, in terms of caries arrestment and dentin remineralization/
are viable candidates for pulp capping procedures. Indeed, the pulp reorganization, several studies suggest the provision of a seal and
may be a far more resilient tissue then many believe, provided it is entombment of residual bacteria to arrest caries progression is
healthy to begin with, bacteria is managed, and an environment and more important than any specific base or liner placed initially.4-6
durable seal can be created using materials conducive to the pulp’s As an example, a recent clinical study restoring deep carious le-
continued health. sions using a two-stage indirect pulp capping protocol that used a
This article will provide a general discussion of direct and indi- resin-modified glass ionomer (RMGI) provisional with and without
rect pulp capping procedures and highlight a clinical case using a first placing a calcium hydroxide liner found no clinical benefit to
novel light-cured resin-modified mineral trioxide aggregate (MTA) using said liner.7 Although this was a short-term study (3 months)
2 compendium March 2018 Volume 39, Number 3
it supports the view held by some that the provision of a seal (in differentiate between infected and affected dentin. Caries detect-
this case by the RMGI provisional) is more important than any ing solutions (typically propylene glycol mixed with various dyes)
specific indirect pulp capping liner or base that is placed initially. that in principle stain only the denatured collagen of the infected
After several months, and assuming all goes well during the provi- dentin (Figure 1 and Figure 2) may be useful adjuncts in this regard,
sional trial period (ie, no signs or symptoms of pain or pathology), the but their accuracy is questionable and it is doubtful they indicate
patient returns for the second step of the two-stage indirect pulp cap- with certainty that all active caries has or has not been removed.16,17
ping procedure. While there are variations in materials and technique, The technique the author prefers is the judicious use of caries
the provisional is typically removed, remaining caries is removed to detecting solutions in conjunction with careful and thorough use
hard tissue, and a final restoration is placed. The hope is that some of tactile and visual criteria to assess the caries status of the dentin
degree of dentin remineralization, along with formation of reparative during cavity excavation and preparation. Also, dentists must be
dentin and dentin bridging, occurred during the time interval between aware that it is more difficult to predictably bond directly to deep
the first and second appointments allowing for residual caries removal caries-affected dentin than normal dentin, because caries-affected
during the second appointment without exposing the pulp. dentin is different in morphological, chemical, and physical char-
While a number of studies and case reports support or advo- acteristics.18,19 Many dentists prefer to place some type of base or
cate for various two-stage indirect pulp capping procedures,8-12 liner in deep cavity preparations prior to the use of an adhesive sys-
many dentists are not comfortable leaving residual caries in their tem and placement of the final restoration. One technique that has
cavity preparations and prefer to remove all caries at the initial worked well for the author when dealing with deep caries-affected
appointment even at the risk of pulp exposure.13 Indeed, a PEARL dentin is to first disinfect the substrate with a 2% aqueous solu-
(Practitioners Engaged in Applied Research and Learning) study tion of chlorhexidine digluconate (eg, Cavity Cleanser™, BISCO,
conducted in 2007 indicated that most dentists prefer to remove all bisco.com; Concepsis®, Ultradent Products, ultradent.com) followed
decay initially, while only 20% favored by the placement of a RMGI liner (eg,
partial caries removal.14 These findings Vitrebond™, 3M, 3m.com; Fuji Lining™
are corroborated in a more recent study LC, GC America, gcamerica.com) (Figure
that also found the vast majority of sur- 3 through Figure 6). The RMGI liner is
veyed dentists, when restoring deep cari- placed in a thin layer (≤1 mm) before plac-
ous lesions, preferred complete carious ing a dentin bonding agent and composite
removal to hard dentin at the initial restorative. In vivo clinical studies sup-
appointment even at the risk of pulp port this general protocol.20,21
exposure.15 RMGI liners have several positive at-
tributes, including good adhesive and
Indirect Pulp Capping: sealing properties via micromechanical
One-Step Approach and chemical interaction with dentin.22
With one-stage indirect pulp capping They are simple to mix and place, re-
techniques typically all or most of the lease high sustained levels of fluoride,23
caries is removed at the initial appoint- Fig 1. have significant antimicrobial proper-
ment, some type of indirect pulp capping ties24,25 and low solubility,26,27 and exhibit
material is placed in close approximation a favorable modulus of elasticity and co-
to but not in direct contact with the pulp, efficient of thermal expansion and con-
and the final restoration is placed, all in traction (similar to that of dentin).28,29 In
the same appointment. One common addition, RMGI liners have been shown
technique is to remove only the “infect- in many studies to help reduce gap for-
ed dentin” (dentin that is demineralized mation and microleakage.30-34 While
with denatured collagen, infiltrated with there is scientific and anecdotal 35,36
bacteria, and irreparably damaged) while evidence supporting the use of RMGI
leaving the “affected dentin” in place liners in close proximity to (but not in
(dentin that is also demineralized but direct contact with) pulp, their use as
with the collagen structure still largely direct pulp capping agents is generally
intact, is bacteria free, and still has the contraindicated in the literature.1,29,37,38
potential for remineralization). Typically, Clearly, the remaining dentin thickness,
the affected dentin is then covered with Fig 2. which is very difficult to access clinically,
a base and/or liner in the hope that over has an effect on the pulpal response to
time it will remineralize, forming hard Fig 1. Caries detecting solution placed and any indirect pulp capping material.38
bacteria-free dentin. While this seems allowed to dwell for at least 10 seconds. The author has previously discussed in
Fig 2. Tooth shown in Fig 1 after thorough
reasonable in theory, the clinical real- rinsing and drying. Theoretically, only the detail the use of RMGI liners as indirect
ity is that it can be extremely difficult to caries-infected dentin picks up the stain. pulp capping agents.39,40
www.compendiumlive.com March 2018 compendium 3
Clinical TECHNIQUE REVIEW | pulp capping
Direct Pulp Capping school. By and large, dentists use what they know, are comfortable
Direct pulp capping is used when the pulp is visibly exposed (vital with, and have had a reasonable degree of success with. Even when
pulp exposure) due to caries, trauma, or iatrogenic insult such as newer and potentially superior techniques and materials emerge,
accidental exposure during tooth preparation or caries removal. change can be slow to come. “Science and technology revolutionize
The procedure typically involves arresting any pulpal hemorrhage our lives, but memory, tradition, and myth frame our response.”46
followed by covering and sealing exposed pulp tissue in some fash- Although successful outcomes are sometimes achieved with cal-
ion to preserve its health, function, and viability. Calcium hydroxide cium hydroxide direct pulp caps, calcium hydroxide does have sig-
has traditionally been considered the “gold standard” and is the nificant disadvantages, including lack of innate adhesive and sealing
most commonly used material in this regard.41 This is partly be- abilities, poor physical properties, and dissolution over time.47 In
cause of its ability to dissociate into calcium and hydroxyl ions, its addition, some studies show that the dentin bridge formed under
high pH, antibacterial properties, and apparent ability to stimulate calcium hydroxide pulp caps contains multiple “tunnel” defects
odontoblasts and other pulp cells in various ways to form reparative and porosities.48-50
dentin.1,41-43 Studies have also shown that the high pH of calcium Although it has long been accepted that calcium hydroxide has
hydroxide causes superficial coagulation necrosis where it contacts significant antimicrobial properties (most studies support this),
the pulp. This provides a degree of hemostasis and stimulates min- at least one study questions this assumption.51 Long-term clini-
eralized tissue and dentin bridge formation.44,45 cal studies show success rates with calcium hydroxide pulp caps
Most likely, another reason for the widespread use of calcium on carious exposures to be highly variable, generally unpredict-
hydroxide as a direct pulp capping agent on vital exposures is be- able, and often unsuccessful.52 It makes sense to develop and test
cause this is the technique most dentists were taught in dental medicaments for direct pulp capping that overcome some of the
Fig 3. Fig 4.
Fig 5. Fig 6.
Fig 3. Deep cavity preparation showing what is most likely caries-affected dentin remaining. The preparation is cleaned and disinfected with a
pumice/2% chlorhexidine mixture, rinsed, and briefly air-dried. Fig 4. A thin (<1 mm) layer of a RMGI liner is placed on the floor and run up the
walls of the preparation with a Dycal applicator (enamel margins are not covered). Fig 5. RMGI liner is light-polymerized for at least 20 seconds.
Fig 6. Finished indirect pulp cap with RMGI liner.
4 compendium March 2018 Volume 39, Number 3
deficiencies of calcium hydroxide and have the potential to provide Although MTA was originally developed primarily for endodontic
more consistent and predictable clinical outcomes. purposes, such as a root end sealant and for sealing inadvertent fur-
In 1824 Joseph Aspdin, a British stone mason, obtained a patent for cation and root canal perforations, its use as a potential direct pulp
a cement he formulated in his kitchen. The inventor heated a mixture capping agent was quickly recognized.61 Indeed, there is a growing
of finely ground limestone and clay and ground the mixture into a pow- body of scientific evidence, including controlled clinical studies, that
der creating a hydraulic cement (one that hardens with the addition has found MTA typically has better clinical outcomes and histologic
of water). Aspdin named the product Portland cement because the responses than calcium hydroxide when both are compared head to
set cement resembled a stone quarried on the Isle of Portland off the head in direct pulp capping studies.65-70 While studies indicate MTA is
British coast.53 Today, various versions and formulations of Aspdin’s a viable, and perhaps better, option than calcium hydroxide for direct
Portland cement are used to create everything from concrete blocks, pulp capping procedures, traditional powder/liquid formulations
support beams, grout, mortar, and foundation slabs for roadways, of MTA have significant drawbacks and are not used in most dental
buildings, and backyard patios. Aspdin had no way of knowing that offices.36 For example, they are not especially user friendly, require
roughly 170 years after his discovery this same product would form very precise mixing, can cause tooth discoloration, and manipula-
the backbone of a new class of calcium and tion and placement can be challenging. In
alumina silicate based so-called “bioactive” addition, traditional MTA formulations
dental materials, one of which was mineral require long setting times (typically 2 to 4
trioxide aggregate (MTA). hours), with one study that simulated in-
traoral conditions finding that the MTA
Emergence of MTA and MTA/ formulation tested (ProRoot® MTA) was
Hybrid Materials still not set after 6 hours.71 Hydration
In the early 1990s Torabinejad and col- accelerators, such as citric acid, lactic
leagues began testing and experimenting acid, calcium chloride, and calcium
with an MTA compound they developed lactate gluconate, have been added to
at Loma Linda University that was essen- some modified MTA formulations (eg,
tially a modified Portland cement.54 They Biodentine®, Septodont, septodontusa.
found it had significantly better sealing com; MTA Angelus®, Angelus Soluções
abilities than conventional endodontic Odontológicas, angelus.ind.br). This,
materials when used as a root end sealer along with incorporation of the powder
and in the repair of furcation and lateral and liquid components into capsules that
root perforations.55-58 This was due, in part, can be triturated (ie, Biodentine) and the
to the fact that MTA sets and functions manipulation of particle sizes and pow-
well in the inherently moist environment der/liquid ratios, as well as other modi-
in and around a tooth in an in vivo situa- fications, has significantly decreased the
tion. In fact, just as water is an essential setting time of some MTA formulations
component in the setting of Portland ce- Fig 7. to a much more clinically manageable,
ment, it is also required in and enhances though still long, 10 to 15 minutes.
the setting of MTA. Fig 7. Radiograph of tooth No. 4 taken at Biodentine is designed as a dentin re-
While the chemical reactions that oc- presentation showing extensive decay. placement (base) and, according to the
cur when MTA is mixed with water are manufacturer, has physical properties
actually quite complex and beyond the similar to dentin. It can be used as a den-
scope of this article, the main reactants of MTA (tricalcium and tin substitute under composites for direct and indirect pulp capping,
dicalcium silicate and tricalcium aluminate) break down into a or as an endodontic repair material. One study showed Biodentine
number of reaction products, including calcium silicate and the induced odontoblast differentiation from pulp progenitor cells.72
familiar calcium hydroxide.59 The calcium hydroxide dissociates Another in vivo study showed complete dentinal bridge formation,
into hydroxyl ions (-OH) resulting in a high pH local environment. as well as an absence of an inflammatory pulp response, in the major-
Unlike regular calcium hydroxide, which has solubility issues over ity of teeth whose pulps were purposely exposed, pulp capped with
time, this conglomeration of reaction products has very low solubil- Biodentine, and subsequently extracted after 6 weeks for histologic
ity and maintains its physical integrity long after placement. examination.73 Positive clinical outcomes have been reported using
In addition to its low solubility, MTA has several other positive Biodentine as a direct pulp capping material.74 While the setting
attributes, including high biocompatibility, bioactivity, hydrophi- time of some MTA-based materials such as Biodentine has been sig-
licity, radiopacity, less toxicity than calcium hydroxide, and good nificantly improved, the still relatively long setting times of 10 to 15
sealing ability.60-62 MTA has been shown to promote regeneration of minutes can be problematic. MTA-based resin-modified materials
the periodontal ligament, dental pulp, and peri-radicular tissues.61,63 that set on demand via light polymerization may offer an attractive
As with calcium hydroxide, there is equivocation in the literature alternative, as having the ability to cure quickly offers a significant
regarding the antibacterial abilities of MTA.64 clinical advantage. One important consideration regarding such a
www.compendiumlive.com March 2018 compendium 5
Clinical TECHNIQUE REVIEW | pulp capping
hybrid product is whether or not the incorporation of light-curable this water source assists in the initial setting reaction of the MTA.
resin components and chemistry into an MTA matrix would in any In addition, due to the hydrophilic nature of polymerized TheraCal
way compromise the bioactive capabilities and desirable proper- LC, it is postulated that water/fluids that are inherent in intertubu-
ties of the MTA. While there are promising studies and anecdotal lar dentin, dentin tubules, and (in the case of direct pulp capping)
evidence (discussed below) that support such a product, further the pulp itself diffuse into the polymer matrix over time, reacting
research is warranted to fully address this important issue. with the MTA-releasing calcium and hydroxide ions in the process.
A study by Gandolfi and colleagues found TheraCal LC had
Development of a Light-Curable Resin-Modified higher calcium releasing ability and lower solubility than either
MTA-Based Material ProRoot MTA or Dycal® (Dentsply Sirona) throughout the testing
In the early 2000s, chemists Dr. Byoung Suh, Dr. Rui Yin, and David period of 28 days when the samples were stored in water.75 Another
Martin, along with dentist and researcher Dr. Mark Cannon, began study found that samples of TheraCal LC and Dycal (again stored
developing and experimenting with a single-component hydrophilic in water) tested for calcium-ion concentration at different time
resin-modified light-curable MTA-based material. In November intervals (7, 14, and 21 days) showed TheraCal LC had greater ion
2011, after nearly 10 years of research, the finished product (Thera- release at all time intervals.76 However, there is equivocation in
Cal LC®, BISCO) was introduced into the marketplace (according the literature as another comprehensive study, in which a highly
to a personal communication the author had with Dr. Liang Chen, sensitive ion detecting technique (ion chromatography) was used,
head chemist at BISCO, in July 2017). The company markets this reported significantly higher calcium-ion levels leached from
product as a “light-cured resin-modified calcium silicate” (RMCS) Biodentine compared to that of TheraCal LC (samples stored in
formulated to be used as a liner for both direct and indirect pulp both water and physiologic saline solution).77
capping procedures. The chemistry of the product includes, but is not It is important to note that measurement of ion release from
limited to, approximately 45% by weight MTA (type III Portland ce- MTA and MTA/hybrid materials such as TheraCal LC typi-
ment), calcium oxide, barium zirconate (for radiopacity), fumed silica cally occurs with samples submerged in water and/or simulated
Fig 8. Fig 9. Fig 10. Fig 11. Fig 12.
Fig 8. A vital pulp exposure that occurred during caries excavation. Fig 9. Bleeding was stopped with direct pressure from a cotton pellet soaked
in 2% chlorhexidine. Fig 10. The preparation was left visibly moist and a MTA hybrid material (TheraCal LC) was applied in a thin layer and light-
polymerized. Fig 11. The TheraCal LC was covered with a RMGI liner (Vitrebond). Fig 12. The tooth was then built up for an eventual crown using
a total-etch bonding system and self-cure core build-up material.
(thicken agent), strontium glass, bisphenol A-glycidyl methacrylate physiologic solutions. While this technique enables comparative
(bis-GMA), photoinitiators, and polyethylene glycol dimethacrylate ion values for different materials to be ascertained under those
(PEGDMA, hydrophilic monomer). conditions, such an abundant water source is not the clinical reality
The material is designed to be placed in a thin layer (1-mm incre- for pulp capping materials that are typically sealed deep inside a
ment) and light-polymerized for 20 seconds. Once the resin compo- cavity preparation and cut off from an external water supply. Other
nents of TheraCal LC are light-polymerized the MTA is essentially authors and researchers have also raised this critical issue and
trapped in the polymer matrix. It is logical to assume that the pres- found ion release for some products to be significantly less than
ence of the resin matrix modifies both the setting mechanism and reported when tested under more realistic clinical conditions.78
ion leaching abilities and characteristics of the MTA in TheraCal LC. The ultimate test for any restorative material, of course, is clini-
It is important to remember water is needed for the hydraulic setting cal performance—ie, does it work? TheraCal LC has demonstrated
reactions and ion releasing abilities of MTA. Because there is no the ability to form apatite similar to that of ProRoot MTA when
water inherent in TheraCal LC’s formulation this water must come immersed in simulated phosphate-containing body fluid,79 and
from another source. Instructions for the application of TheraCal has also been shown to induce odontoblastic differentiation and
LC state it should be placed on “visibly moist” dentin. It is possible mineralization.80 Two in vivo studies have shown that TheraCal
6 compendium March 2018 Volume 39, Number 3
LC has the potential to induce reparative dentin and dentin bridge
formation when used as a direct and indirect pulp capping agent.81,82
However, one study found TheraCal LC did not have as favorable
a pulpal response as ProRoot MTA when used to cap pulpotomies
in dogs’ teeth.83 It should be pointed out that the company does not
advocate the use of Theracal LC for this procedure. One research-
er reported an impressive 20 out of 20 teeth with exposed pulps
capped with TheraCal LC remained vital after 2 years.84 That same
researcher reported 19 out of 20 of those same teeth remained vital
after 4 years (according to a personal communication the author
had with that researcher, Dr. Scotti Nicola, in January 2016). While
Fig 13. Fig 14.
positive studies and anecdotal reports of clinical success using
MTA/resin hybrid products such as TheraCal LC exist, caution is
urged before they can be unequivocally endorsed.
Case Report
In September 2015 the patient, a 40-year-old man, presented to
the office with the chief complaint of cold sensitivity in the upper
right quadrant. A radiograph revealed extensive decay on the distal
of tooth No. 4 (Figure 7). The tooth was not percussive sensitive
but was sensitive when stimulated with cold. After discussion with
the patient, the area was anesthetized with articaine, the tooth
opened, and the decay visualized. Extensive soft decay was evident
and removed with the aid of caries detecting solution, slow-speed
round burs, and spoon excavators, until the clinician reached solid
dentin that appeared to be caries-free. Fig 15.
A bleeding pulp exposure was evident (Figure 8). The bleeding
was stopped with direct pressure for approximately 60 seconds us-
Fig 13. Radiograph taken immediately after direct pulp cap and crown
ing a cotton pellet soaked in a 2% chlorhexidine solution (Figure 9). build-up. Fig 14. Radiograph taken 14 months later showing apparent
The chlorhexidine-soaked cotton pellet was removed but the dentin formation of reparative dentin. The tooth was asymptomatic and pulp-
not dried. A thin layer of TheraCal LC was placed directly over the tested vital. Fig 15. Finished restoration tooth No. 4 (lithium-disilicate
crown) placed approximately 22 months after the direct pulp capping
exposed pulp and onto the still-moist (with chlorhexidine) dentin
surrounding the pulp. The TheraCal LC was then light-polymerized
for 20 seconds using a light-curing unit with a power density of ap- strength of adhesive systems, and may have a synergistic effect
proximately 1,000 mW/cm2 (Figure 10). The preparation was then with calcium hydroxide (one of the reaction products of MTA).39,85
briefly air-dried and a thin layer of Vitrebond was placed over and Overlaying TheraCal LC with the RMGI liner and extending the
beyond the borders of the set TheraCal LC and light-polymerized RMGI liner onto dentin beyond the borders of the TheraCal LC
(Figure 11). The tooth was then built up for a future crown using a offers several potential benefits, including preventing the Thera-
total-etch adhesive system and self-curing core build-up material Cal LC from accidently dislodging at some point in the restorative
(Figure 12). protocol (as some have reported).
Comparative radiographs taken approximately 14 months apart In addition, Vitrebond may provide additional antimicrobial ac-
showed what appeared to be the formation of tertiary (reparative) tivity24,25 and improve the overall seal of the pulp and restoration in
dentin (Figure 13 and Figure 14). The tooth remained asymptom- general.30-34 This RMGI liner also has a significant amount of water
atic throughout this time period and pulp-tested vital 14 and 22 in its formulation. It is possible, though speculative, that some of
months after the direct pulp cap was performed. After approxi- this water could be absorbed by TheraCal LC (which is hydrophilic)
mately 22 months the tooth was restored with a full-coverage and assist in the setting and ion exchange of the MTA in the material.
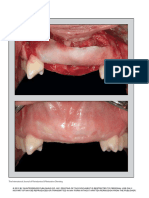
lithium-disilicate restoration (Figure 15).
Conclusion
Discussion While the case presented appears to show dentin bridging and a
The author has experienced good clinical success using a com- positive clinical outcome after 22 months, it is premature to draw
bination of products for direct pulp capping procedures that in- definitive conclusions as to the exact reason for this short-term
cludes chlorhexidine, TheraCal LC, and Vitrebond RMGI liner. success. It may be the combination of products used, and not any
Chlorhexidine is a potent antimicrobial, has been shown to inhibit specific product, that led to success in this case. Moreover, it may
matrix metalloproteinases that may contribute to the breakdown of also be that bacteria was managed and the pulp, which likely was
the adhesive interface over time, does not interfere with the bond reasonably healthy to begin with and still had the capacity for
www.compendiumlive.com March 2018 compendium 7
Clinical TECHNIQUE REVIEW | pulp capping
self-repair, was then well sealed allowing normal physiologic re-
sponses and healing to occur. Clearly, additional research, including
controlled clinical studies, is required to better assess the long-term
clinical ramifications of this exciting though relatively new class
of dental materials.
ABOUT THE AUTHOR
Gary Alex, DMD
Private Practice, Huntington, New York
REFERENCES
1. Hilton TJ. Keys to clinical success with pulp capping: a review of the
literature. Oper Dent. 2009;34(5):615-625.
2. Thompson V, Craig RG, Curro FA, et al. Treatment of deep carious
lesions by complete excavation or partial removal. J Am Dent Assoc.
2008;139(6):705-712.
3. Carrotte PV, Waterhouse PJ. A clinical guide to endodontics—up-
date part 2. Br Dent J. 2009;206(3):133-139.
4. Kuhn E, Reis A, Chibinski AC, Wambier DS. The influence of the lin-
ing material on the repair of the infected dentin in young permanent
molars after restoration: a randomized clinical trial. J Conserv Dent.
2016;19(6):516-521.
5. Dalplan DM, Casagrande L, Franzom R, et al. Dentin microhardness
of primary teeth undergoing partial carious removal. J Clin Pediatr
Dent. 2012;36(4):363-367.
6. Chibinski AC, Reis A, Kreich EM, et al. Evaluation of primary carious
dentin after cavity sealing in deep lesions: a 10-13 month follow-up.
Pediatr Dent. 2013;35(3):e107-e112.
7. Pereira MA, Santos-Junior RBD, Tavares JA, et al. No additional ben-
efit of using a calcium hydroxide liner during stepwise caries removal.
J Am Dent Assoc. 2017;148(6):369-376.
8. Pinto AS, de Araujo FB, Franzon R, et al. Clinical and microbiologi-
cal effect of calcium hydroxide protection in indirect pulp capping in
primary teeth. Am J Dent. 2006;19(6):382-386.
9. Marchi JJ, de Araujo FB, Froner AM, et al. Indirect pulp capping in
the primary dentition: a four year follow-up study. J Clin Pediatr Dent.
2006;31(2):68-71.
10. Evidenced-based review of clinical studies on indirect pulp cap-
ping. J Endod. 2009;35(8):1147-1151.
11. Biorndal L, Reit C, Markvart M, et al. Treatment of deep caries le-
sions in adults: randomized clinical trials comparing stepwise vs. direct
complete excavation, and direct pulp capping vs. partial pulpotomy.
Eur J Oral Sci. 2010;118(3):290-297.
12. Fagundes TC, Barata TJ, Prakki A, et al. Indirect pulp treatment in
a permanent molar: case report of a 4-year follow-up. J Appl Oral Sci.
2009;17(1):70-74.
13. Weber CM, Alves LS, Maltz M. Treatment decisions for deep carious
lesions in the Public Health Service in Southern Brazil. J Public Health
Dent. 2011;71(4):265-270.
14. Oen KT, Thompson VP, Vena D, et al. Attitudes and expecta-
tions of treating deep caries: a PEARL Network survey. Gen Dent.
2007;55(3):197-203.
15. Koopaeei MM, Inglehart MR, McDonald N, Fontana M. General den-
tists’, pediatric dentists’, and endodontists’ diagnostic assessment and
treatment strategies for deep carious lesions: a comparative analysis. J
Am Dent Assoc. 2017;148(2):64-74.
16. MaComb D. Caries-detector dyes—how accurate and useful are
they? J Can Dent Assoc. 2000;66(4):195-198.
17. Javaheri M, Maleki-kambakhsh S, Etemad-Moghadam S. Efficacy
of two caries detector dyes in the diagnosis of dental caries. J Dent
(Tehran). 2010;7(2):71-76.
> For the full reference list, visit dentalaegis.com/go/ccedxxx.
8 compendium March 2018 Volume 39, Number 3
You might also like
- Inlays Onlays 1Document18 pagesInlays Onlays 1Alireza NaderiNo ratings yet
- Astropalmistry From The Cradle of AstropalmistryDocument3 pagesAstropalmistry From The Cradle of AstropalmistryANTHONY WRITERNo ratings yet
- Frequently Asked Questions in Composite Restorative Dentistry and RestorationsDocument6 pagesFrequently Asked Questions in Composite Restorative Dentistry and RestorationsRose Sky100% (1)
- Mycobacteria Protocol BookDocument413 pagesMycobacteria Protocol Book신정이100% (1)
- Homestay Business AgreementDocument17 pagesHomestay Business AgreementRasyidahNo ratings yet
- Project Proposal For Parish Youth Congress 2021Document5 pagesProject Proposal For Parish Youth Congress 2021Denry BaracenaNo ratings yet
- The Road Cormac McCarthy PDFDocument3 pagesThe Road Cormac McCarthy PDFAvilioNo ratings yet
- Desert EcosystemDocument36 pagesDesert EcosystemmadhumithavaniNo ratings yet
- Approximating The Measures of Quantities Particularly Length, Weight or Mass, Volume, Time, Angle, Temperature and RateDocument27 pagesApproximating The Measures of Quantities Particularly Length, Weight or Mass, Volume, Time, Angle, Temperature and RateSharmane Flores SanorjoNo ratings yet
- (2019) Cervical Margin Relocation - Case Series and New Classification Systems. CHECKDocument13 pages(2019) Cervical Margin Relocation - Case Series and New Classification Systems. CHECKBárbara Meza Lewis100% (1)
- Ra 11642Document43 pagesRa 11642pureroseroNo ratings yet
- Indirect and Direct Pulp Capping: Reactionary vs. Reparative DentinsDocument6 pagesIndirect and Direct Pulp Capping: Reactionary vs. Reparative Dentinshafizhuddin muhammadNo ratings yet
- The Protocols of Biomimetic Restorative DentistryDocument13 pagesThe Protocols of Biomimetic Restorative DentistryPedroFelipeRojasMonárdezNo ratings yet
- The Protocols of Biomimetic Restorative Dentistry - 2002 To 2017 - Inside DentistryDocument8 pagesThe Protocols of Biomimetic Restorative Dentistry - 2002 To 2017 - Inside DentistryjaverdayNo ratings yet
- Injectabletechniquefordirectprovisionalrestoration PDFDocument5 pagesInjectabletechniquefordirectprovisionalrestoration PDFCSilva16No ratings yet
- IJEDe 15 01 Part-IDocument18 pagesIJEDe 15 01 Part-IDanny Eduardo Romero100% (1)
- Deep Margin ElevationDocument19 pagesDeep Margin ElevationAlejandra Estrada RengelNo ratings yet
- New Adhesives and Bonding Techniques. Why and When?: Nicola ScottiDocument12 pagesNew Adhesives and Bonding Techniques. Why and When?: Nicola ScottiDr. Naji ArandiNo ratings yet
- The Current State of Adhesive DentistryDocument9 pagesThe Current State of Adhesive DentistrymishNo ratings yet
- 3D - Printed Crowns - Cost EffectiveDocument4 pages3D - Printed Crowns - Cost EffectiveLuis Felipe SchneiderNo ratings yet
- Conservative Restoration of The Worn Dentition - The Anatomically DrivenDocument34 pagesConservative Restoration of The Worn Dentition - The Anatomically DrivenFrancisco Javier Sánchez Hernández100% (1)
- Direct and Indirect Pulp Capping: A Brief History, Material Innovations, and Clinical Case ReportDocument9 pagesDirect and Indirect Pulp Capping: A Brief History, Material Innovations, and Clinical Case ReportNaeimaNo ratings yet
- Jurnal Direct and Indirect Pulp CappingDocument9 pagesJurnal Direct and Indirect Pulp Cappingninis anisaNo ratings yet
- Vital Pulp Therapy 1Document6 pagesVital Pulp Therapy 1Mostafa Afifi Ali100% (1)
- Conventional and Adhesive Luting Cements PDFDocument8 pagesConventional and Adhesive Luting Cements PDFZahraa HamedNo ratings yet
- Sealers, Liners, and Bases: Contemporary IssuesDocument3 pagesSealers, Liners, and Bases: Contemporary IssuesD-F-093/Associate Professor/Dental Materials Dr. Shahreen ZahidNo ratings yet
- Ledermix Pulp Treatment in A Permanent Molar A CasDocument8 pagesLedermix Pulp Treatment in A Permanent Molar A Casqiao fenNo ratings yet
- Vital Pulp Capping: A Worthwhile Procedure: Lawrence W. Stockton, DMDDocument4 pagesVital Pulp Capping: A Worthwhile Procedure: Lawrence W. Stockton, DMDShofia MoehNo ratings yet
- Clinical Evaluation of Stress-Reducing Direct Composite Restorations in Structurally Compromised Molars: A 2-Year ReportDocument8 pagesClinical Evaluation of Stress-Reducing Direct Composite Restorations in Structurally Compromised Molars: A 2-Year ReportLucianoNo ratings yet
- Semidirect Vital Tooth Onlay Restoration: A Case ReportDocument5 pagesSemidirect Vital Tooth Onlay Restoration: A Case ReportResa YudhistiNo ratings yet
- Interest of Biodentine As Pulp-Capping Materiel Under CAD/CAM Ceramic InlayDocument4 pagesInterest of Biodentine As Pulp-Capping Materiel Under CAD/CAM Ceramic InlayMaya RahayuNo ratings yet
- Biodentine PulpotomyDocument3 pagesBiodentine PulpotomyDANIELA TOLOZANo ratings yet
- [British Dental Journal 2014-may 23 vol. 216 iss. 10] Ngo, H._ Opsahl-Vital, S. - Minimal intervention dentistry II_ part 7. Minimal intervention in cariology_ the role of glass-ionomer cements in the preservat (201Document5 pages[British Dental Journal 2014-may 23 vol. 216 iss. 10] Ngo, H._ Opsahl-Vital, S. - Minimal intervention dentistry II_ part 7. Minimal intervention in cariology_ the role of glass-ionomer cements in the preservat (201كرم الباريNo ratings yet
- Vital Pulp Theray in Permenant Tooth Kursus Resto FinalDocument55 pagesVital Pulp Theray in Permenant Tooth Kursus Resto FinalAmni AzmiNo ratings yet
- Case ReportDocument5 pagesCase Reportadrianafrcv26No ratings yet
- Cureus 0015 00000039374Document7 pagesCureus 0015 00000039374AlexaNo ratings yet
- DZZ International 04 2022 The Two-Step Direct CompositeDocument9 pagesDZZ International 04 2022 The Two-Step Direct CompositeDiego A. SequeraNo ratings yet
- Review Article: Gingival Retraction Made EasierDocument5 pagesReview Article: Gingival Retraction Made EasierKrupali JainNo ratings yet
- Nicholson 1992Document6 pagesNicholson 1992abcder1234No ratings yet
- Facial Slot Class II Restorations: A Conservative Technique RevisitedDocument5 pagesFacial Slot Class II Restorations: A Conservative Technique RevisitedAlyaa NabiilaNo ratings yet
- 64d09f3bd01 InglesDocument7 pages64d09f3bd01 InglesPedro Maria Crizul BarretoNo ratings yet
- 44.the Utilization of Snap-On Provisionals For Dental Veneers - From An Analog To A Digital Approach. Esquivel - 2020. J Esthet Restor DentDocument10 pages44.the Utilization of Snap-On Provisionals For Dental Veneers - From An Analog To A Digital Approach. Esquivel - 2020. J Esthet Restor DentValeria CrespoNo ratings yet
- Minimally Invasive Caries Management ProtocolDocument8 pagesMinimally Invasive Caries Management ProtocolKarReséndizNo ratings yet
- Case Report Ledermix Pulp Treatment in A Permanent Molar: A Case ReportDocument7 pagesCase Report Ledermix Pulp Treatment in A Permanent Molar: A Case ReportNaji Z. ArandiNo ratings yet
- Atraumatic Restorative Treatment: A Review: ShefallyDocument7 pagesAtraumatic Restorative Treatment: A Review: ShefallykholisNo ratings yet
- Hall Technique, Stepwise Excavation, Partial Caries Removal TechniqueDocument4 pagesHall Technique, Stepwise Excavation, Partial Caries Removal TechniqueImbador LiesiesNo ratings yet
- Mohamad Jalloul Endo Assign 2023Document13 pagesMohamad Jalloul Endo Assign 2023AliciaNo ratings yet
- Improvement of Aesthetics in A Patient With Tetracycline Stains Using The Injectable Composite ResinDocument5 pagesImprovement of Aesthetics in A Patient With Tetracycline Stains Using The Injectable Composite ResinJoshua ValdezNo ratings yet
- Sellantes A Base de IonomeroDocument4 pagesSellantes A Base de IonomeroNatalia Iglesias RoaNo ratings yet
- Effect of Glass-Ionomer Cement Lining On Postoperative Sensitivity in Occlusal Cavities Restored With Resin Composite - A Randomized Clinical TrialDocument8 pagesEffect of Glass-Ionomer Cement Lining On Postoperative Sensitivity in Occlusal Cavities Restored With Resin Composite - A Randomized Clinical TrialNaji Z. ArandiNo ratings yet
- Porosity Formation and Microleakage of Composite Resins Using The Snowplow TechniqueDocument5 pagesPorosity Formation and Microleakage of Composite Resins Using The Snowplow TechniqueUnlikely QuestionsNo ratings yet
- ROA Scopin 2014 4Document24 pagesROA Scopin 2014 4Patrick Castillo SalazarNo ratings yet
- Simion 2012)Document13 pagesSimion 2012)SergioNo ratings yet
- Adhesive Performance of A Multi-Mode Adhesive System - 1-Year in Vitro Study Lorenzo Breschi DDocument10 pagesAdhesive Performance of A Multi-Mode Adhesive System - 1-Year in Vitro Study Lorenzo Breschi DEliseu LucenaNo ratings yet
- Atraumatic Restorative Treatment (ART)Document4 pagesAtraumatic Restorative Treatment (ART)solodont1No ratings yet
- s40563 019 0118 7 PDFDocument13 pagess40563 019 0118 7 PDFXray PolyclinicNo ratings yet
- Total Etch Vs Self Etch Adhesives PDFDocument3 pagesTotal Etch Vs Self Etch Adhesives PDFAfia IzzaNo ratings yet
- Posterior Composites: A Practical Guide Revisited: Dental Update April 2012Document5 pagesPosterior Composites: A Practical Guide Revisited: Dental Update April 2012tsukiyaNo ratings yet
- Taniguchi G, Et Al. 2009. Improving The Effect of NaOCl Pretreatment On Bonding To Caries Affected Dentin Using Self Etch Adhesives.Document7 pagesTaniguchi G, Et Al. 2009. Improving The Effect of NaOCl Pretreatment On Bonding To Caries Affected Dentin Using Self Etch Adhesives.Ranulfo Castillo PeñaNo ratings yet
- HUSNI ADAM - Jurnal Utama No.3Document3 pagesHUSNI ADAM - Jurnal Utama No.3Adam HusniNo ratings yet
- Semidirect Composite Onlay With Cavity Sealing: A Review of Clinical ProceduresDocument11 pagesSemidirect Composite Onlay With Cavity Sealing: A Review of Clinical ProceduresMihaela VasiliuNo ratings yet
- 2013 Direct Anterior Composites A Practical GuideDocument16 pages2013 Direct Anterior Composites A Practical Guidemaroun ghalebNo ratings yet
- J Esthet Restor Dent - 2023 - FicheraDocument12 pagesJ Esthet Restor Dent - 2023 - FicheraFedex Du moralexNo ratings yet
- 62 - The Open PDFDocument9 pages62 - The Open PDFSandeep Lal CherukaraNo ratings yet
- 10-Year Clinical Evaluation of A Self-Etching Adhesive SystemDocument8 pages10-Year Clinical Evaluation of A Self-Etching Adhesive SystemRamy AmirNo ratings yet
- Sandwich TechniqueDocument14 pagesSandwich TechniqueHarish KhundrakpamNo ratings yet
- Zygomatic Implants: Optimization and InnovationFrom EverandZygomatic Implants: Optimization and InnovationJames ChowNo ratings yet
- Peri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentFrom EverandPeri-Implant Complications: A Clinical Guide to Diagnosis and TreatmentNo ratings yet
- MD Sabbir SarkerDocument7 pagesMD Sabbir SarkerMd. Sabbir Sarker 1611386630No ratings yet
- C. SGH-wall 3Document61 pagesC. SGH-wall 3MoustafaNo ratings yet
- Solved Pablo Is Studying Financial Statements To Decide Which CompaniesDocument1 pageSolved Pablo Is Studying Financial Statements To Decide Which CompaniesAnbu jaromiaNo ratings yet
- Justin LaNasa OrderDocument1 pageJustin LaNasa Orderbcm924No ratings yet
- Resume Jasmine Ervin1Document2 pagesResume Jasmine Ervin1api-241347777No ratings yet
- FIDIC ImpDocument60 pagesFIDIC ImpSajad WaniNo ratings yet
- Post Graduate Diploma in Management (2019-21) (Retail Management)Document1 pagePost Graduate Diploma in Management (2019-21) (Retail Management)Amitava DeNo ratings yet
- 1 Overview of Statistics Basic Concepts and TermsDocument15 pages1 Overview of Statistics Basic Concepts and Termsjohny BraveNo ratings yet
- Minglanilla BarangaysDocument4 pagesMinglanilla BarangaysBED DublinNo ratings yet
- Difference Between Literature Review and Background of StudyDocument4 pagesDifference Between Literature Review and Background of StudyafdtnybjpNo ratings yet
- Advisory Re CELEBRATING THE 33RD LIBRARY AND INFORMATION SERVICES MONTH (LISM) IN NOVEMBER 2023Document2 pagesAdvisory Re CELEBRATING THE 33RD LIBRARY AND INFORMATION SERVICES MONTH (LISM) IN NOVEMBER 2023Bienvenido TamondongNo ratings yet
- LG L246WP Blanking AdjustmentDocument14 pagesLG L246WP Blanking AdjustmentErnie De LeonNo ratings yet
- Rights of A ChildDocument2 pagesRights of A ChildAytona Villanueva PearlNo ratings yet
- Indemnity Bond For Lost Document by Borrower To HDFCDocument1 pageIndemnity Bond For Lost Document by Borrower To HDFCAdarsh PandeyNo ratings yet
- EEE 462 Switch Gear and ProtectionDocument18 pagesEEE 462 Switch Gear and ProtectionEmdadul Hoq RakibNo ratings yet
- Jquery - Introduction: Welcome To The Odyssey With Jquery!Document17 pagesJquery - Introduction: Welcome To The Odyssey With Jquery!Shubham Mittal100% (1)
- Rotvel - An Effective Strain Concept For Crack Propagation and Fatigue Life With Specific Applications To Biaxial Stress FatigueDocument19 pagesRotvel - An Effective Strain Concept For Crack Propagation and Fatigue Life With Specific Applications To Biaxial Stress FatigueDavid C HouserNo ratings yet
- Financial Health RatiosDocument29 pagesFinancial Health Ratiosmushiechan888No ratings yet
- CTCMA Bylaws Without Schedules April-2011Document49 pagesCTCMA Bylaws Without Schedules April-2011Jason TuttNo ratings yet
- CHEM1 Q2 M2-Lewis-StructuresDocument32 pagesCHEM1 Q2 M2-Lewis-StructuresMark TerradoNo ratings yet
- Fuel CellDocument44 pagesFuel CellPrernaNo ratings yet
- BCP Week 9 Upper SecondaryDocument9 pagesBCP Week 9 Upper SecondaryGjieBaxNo ratings yet




























![[British Dental Journal 2014-may 23 vol. 216 iss. 10] Ngo, H._ Opsahl-Vital, S. - Minimal intervention dentistry II_ part 7. Minimal intervention in cariology_ the role of glass-ionomer cements in the preservat (201](https://imgv2-2-f.scribdassets.com/img/document/649305346/149x198/7311994bf1/1710571811?v=1)