Professional Documents
Culture Documents
Basic Concepts in Transplant Immunology
Uploaded by
Muhammad Haikal Ahmed KhirOriginal Description:
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Basic Concepts in Transplant Immunology
Uploaded by
Muhammad Haikal Ahmed KhirCopyright:
Available Formats
CAQ CORNER
Basic Concepts in Transplant Immunology
Olivia M. Martinez1 and Hugo R. Rosen2
he liver is unique among transplanted organs with respect to its complex, and sometimes paradoxical, interaction with the host immune system. Early liver transplantation studies with outbred swine demonstrated that a signicant percentage of recipients maintained their graft in the absence of immunosuppression.1 Subsequently, spontaneous liver allograft acceptance was also observed in transplants done in several allogeneic rat strain combinations and most allogeneic mouse strain combinations. Moreover, other experimental studies in rodents demonstrated that allogeneic liver transplantation provides immune protection against subsequent cardiac, kidney, pancreas, islet, and skin grafts from the same donor.1-7 Finally, in clinical transplantation there is increasing evidence, both anecdotal and documented, that some liver transplant recipients who cease taking immunosuppressive drugs maintain allograft function, suggesting robust tolerance is in place. Hence, the liver shows features of immune privilege. Nevertheless, the liver can display destructive immunologic processes since acute liver allograft rejection does occur in approximately 50% to 75% of liver transplant recipients, although in the majority of cases it is readily reversed with immunosuppressive approaches tailored to treat cellular rejection (covered in a separate CAQ corner). Whereas immune responses within the liver can effectively eliminate hepatotropic pathogens including hepatitis A, other liver pathogens such as hepatitis C persist and manage to avoid elimination by the immune system. Finally, a variety of autoimmune diseases with unknown
Abbreviations: Th, T helper cell; IL, interleukin; DC, dendritic cell; APCs, antigen-presenting cells; MHC, major histocompatibility complex; LSEC, liver sinusoidal endothelial cell; NK, natural killer; TCR, T-cell receptor; IFN, interferon; CTLA4, cytotoxic T lymphocyte associated antigen 4; Ig, immunoglobulin; ICOS, inducible costimulator; PD, programmed death; PDL, programmed death ligand; CTLs, cytotoxic T lymphocytes; FasL, Fas ligand; HLA, human leukocyte antigen. From the 1Stanford University School of Medicine, Stanford, CA; and 2Oregon Health and Science University / Portland VAMC, Portland, OR. Address reprint requests to Olivia Martinez, PhD, Stanford University School of Medicine, 1201 Welch Road, MSLS P312, Stanford, CA 94305-5492. Telephone: 650-498-6247; FAX: 650-498-6250; E-mail: omm@stanford.edu Copyright 2005 by the American Association for the Study of Liver Diseases Published online in Wiley InterScience (www.interscience.wiley.com). DOI 10.1002/lt.20406
etiologies target the liver, including primary biliary cirrhosis, primary sclerosing cholangitis, autoimmune hepatitis, and biliary atresia. Together, these observations underscore the enigmatic relationship between the liver and host immunity. In this article, we discuss the hepatic immune system, basic principles governing the host T-cell response to alloantigen following liver transplantation, experimental studies elucidating the cellular and molecular mechanisms of liver allograft rejection and tolerance, and immunologic perspectives of recent developments in clinical liver transplantation.
Role of the Immune System: The Major Players
The primary role of the immune response is to protect the individual from invasion by infectious pathogens and to provide self-nonself discrimination. The coordination of an efcient immune response requires the recognition of pathogens and subsequent activation of immune cells and soluble mediators of immunity. The innate immune system, through its ability to rapidly limit the spread of infectious pathogens provides the speed component. In contrast, classical T cells provide the specicity, which requires days to weeks to develop. These discrete subsets function as part of a coordinated and complementary system, and their importance for host defense is seen in secondary responses in which speed and specicity are united in the form of immunological memory.8 Although graft rejection is mediated primarily by T cells, as indicated by the fact that skin grafted onto nude mice, which lack T cells, is not rejected, it is important to understand the division of labor by diverse cells comprising the immune system. Moreover, increasing evidence indicates that T cells also exert regulatory functions, favoring peripheral tolerance.9 Several subsets of CD4 T cells with suppressive properties have been described, including naturally occurring CD4 CD25 regulatory T cells, T regulatory type 1, and T helper (Th) type 3 cells.10 CD4 CD25 regulatory T cells suppress the response of conventional T cells via a cell contact-dependent mechanism, whereas Th3 and T regulatory type 1 cells produce immunosuppressive cytokines, e.g., transforming growth factor- and interleukin (IL)-10. Dendritic cells (DCs) are professional antigen-pre-
370
Liver Transplantation, Vol 11, No 4 (April), 2005: pp 370-381
CAQ Corner
371
senting cells (APCs) that are present in virtually all organs and provide a critical link between innate and adaptive immunity. The ability of DCs to process and present various types of antigens, including antigens derived from dead cells, is unmatched in the human body.11 Immature DCs express low levels of major histocompatibility complex (MHC) class II, adhesion, and costimulatory molecules, but their expression is dramatically upregulated during maturation in response to appropriate inammatory stimuli.12 There is expanding evidence that liver-derived DCs can downregulate immune responses, hence inducing and maintaining peripheral T-cell tolerance.13 Furthermore, it has been hypothesized that following liver transplantation, the existence of large numbers of DCs within the donor liver that circulate and repopulate the recipient contributes to microchimerism.14
The Liver as an Immune Organ
Because of its location and function, the liver is continuously exposed to diverse and large antigenic loads, including pathogens, toxins, and tumor cells, as well as dietary and commensal proteins.15 The liver must be actively immunocompetent and simultaneously control inappropriate inammatory responses to dietary and other harmless antigens encountered in the portal circulation, thus being able to selectively induce immunity or tolerance to antigens.16 Hepatic suppression of sensitization to antigen absorbed by the portal system was demonstrated as early as 1967.17 The context in which antigen is presented to T cells determines whether the responding T cell is activated or tolerized. This includes the nature of the APC, the presence or absence of costimulatory molecules and the cytokine microenvironment.17 In particular, hepatic APCs have a constitutive ability to activate and induce tolerogenic responses in T cells.18 Liver sinusoidal endothelial cells (LSECs) have a unique immune phenotype, expressing markers typical of cells of myeloid lineage (CD1, CD4, CD11c), even though recent data suggest that these cells differentiate from hepatocyte progenitors.17 LSECs resemble immature DCs more than typical microvascular endothelial cells from other organs and seem to be a new type of organ-specic APCs.17 CD4 T cells primed by antigen-presenting LSECs fail to differentiate toward effector Th1 cells but, instead, express high levels of immune suppressive IL-10. Moreover, antigen presentation to CD8 T cells by LSECs in vivo leads to their inability to respond to specic antigen upon restimulation.19 Taken together, these data implicate antigen presentation by LSECsthe only cells to
have direct contact with immune cells passing through the liveras a primary mechanism of systemic tolerance. Lymphocytes are broadly divided into B cells, T cells, and natural killer (NK) cells; whereas B and T cells possess clonotypic antigen receptors that confer specicity for diverse antigenic structures, NK cells possess multiple receptors that can detect conserved antigens or danger signals that mediate MHC-unrestricted cytolysis of susceptible tumor and virus-infected cells.15,20 Golden-Mason and colleagues have documented an unusually high percentage of unconventional lymphoid cells in the liver that are rarely present in the blood, including NK cells, NKT cells expressing the T-cell receptor (TCR) and the invariant V 24J Q TCR, and DCs.21,22 Although the precise nature of the antigens recognized by these putative regulatory cells is currently unknown, CD1d (expressed on the surface of APCs [Kupffer cells] and hepatocytes23) has been shown to be a natural ligand for NKT cells.24 Figure 1 shows the relative proportions of the major lymphocyte subsets present in the healthy adult human liver as compared with the lymphocyte repertoire found in the peripheral blood (used with permission, from Doherty and OFarrelly15). For example, NK (CD3 CD16 CD56 ) cells represent 5% to 15% of the peripheral mononuclear cell population, but in the liver can comprise 45% of the lymphocyte population.25,26 It has been suggested that these cells deliver a death signal to circulating recipient derived T cells that migrate through the liver after transplantation, contributing to tolerance.27 Thus, the adult human liver contains several populations of lymphocytes that exhibit rapid antigen-nonspecic cytotoxicity and regulatory cytokine secretion28; these cells play important roles in containment of tumor and viral infections, brosis development,29 and allograft rejection/tolerance.
Basic Aspects of T-Cell Recognition of Alloantigen and T-Cell Activation
Recipient T lymphocytes can recognize donor alloantigen through either of two pathways. In the direct pathway, host T lymphocytes recognize native MHC molecules expressed on graft-associated APCs. In the indirect pathway, host T lymphocytes recognize donor alloantigen-derived peptides in the context of self MHC molecules expressed on recipient APCs (Fig. 2). Evidence for both pathways exists in liver transplantation.30 It is likely that the direct pathway predominates early posttransplant and is a major factor in acute rejection since graft-derived APCs expressing donor alloan-
372
Martinez and Rosen
Figure 1. Distribution of lymphocyte subpopulations in healthy human blood and liver. (Adapted from Doherty and OFarrelly.15)
tigen rapidly egress from the graft and enter secondary lymphoid tissue, where they can encounter allospecic T cells.31 Host T cells primed through the direct pathway have the ability to engage the allograft directly and, thus, to efciently mediate effector functions. Further, the proportion of host T cells that can respond to native alloantigen is substantially greater than the proportion of host T cells that can respond through the indirect pathway to donor-derived peptides presented in the context of self MHC.32 The indirect pathway probably emanates from donor alloantigen that is shed from damaged graft tissue, or perhaps in the case of the liver, from soluble MHC class I molecules, that are picked up and presented by self APCs. Thus, while the direct pathway may be important in initiating the classical form of acute rejection, the indirect pathway may be important in sustaining an ongoing, persistent response that is fueled by epitope spreading as a variety of allopeptides are successively presented by self APCs. Indeed, T cells with specicity for allopeptides were readily detected in liver recipients undergoing chronic rejection.33 At the same time it is possible that the indirect pathway is involved in immune regulation since T cells with allopeptide specicity were shown to have regulatory function through inhibition of interferon (IFN)- production in kidney recipients.34 The relative importance of the direct and indirect pathways in liver allograft rejection and tolerance induction remains to be claried.
Costimulatory Pathways and Transplantation
T lymphocytes must receive two distinct but coordinated signals in order to achieve optimal activation. The rst signal is delivered by the TCR following recognition of peptide/MHC complexes on APCs and the second signal is provided by the interaction of costimulatory molecules on the T cells and their cognate ligand/s on APCs. Signal 1 in the absence of signal 2, as likely occurs in the liver, leads to a state of T-cell nonresponsiveness, or anergy, in which T cells can recognize cognate antigen through the TCR but fail to mount a functional response upon reencounter with the antigen. Thus, there has been signicant effort towards inhibiting or blocking costimulation as a means to prolong allograft survival. Two costimulatory molecule-ligand pairs that are important in the generation of a complete T-cell response are CD28/B735 and CD40/CD154.36 CD28 represents the prototypical T-cell costimulatory molecule. In humans, CD28 is expressed on 90% of CD4 T cells and 50% of CD8 T cells. In conjunction with TCR stimulation, ligation of CD28 leads to increased production of cytokines such as IL-2, cellular proliferation, and induction of antiapoptotic proteins. The ligands for CD28, B7-1 (CD80), and B7-2 (CD86), are found on a variety of APCs including DCs, B cells, and macrophages. The constitutive expression of CD86 is greater than for CD80 on APCs, although CD80 expression is enhanced during APC activation. The
CAQ Corner
373
Figure 2. Allorecognition pathways and graft rejection. (A) Pathways of allorecognition. In the direct pathway, T cells recognize intact major histocompatibility molecules on donor antigen-presenting cells (left). In the indirect pathway, T cells recognize processed alloantigen in the form of peptides presented by recipient antigen-presenting cells (right). (B) Interactions among endothelial cells, T cells, and recipient antigen-presenting cells in allograft rejection. Recipient monocytes are recruited by endothelial cells to the graft tissue. They are also transformed to become highly efcient antigen-presenting dendritic cells that may need to recirculate to peripheral lymphoid organs for maturation. The dendritic cells and intragraft macrophages present donor peptides via the indirect pathway to recruited CD4 T cells. CD8 T cells, on the other hand, are activated by donor endothelial cells and can either directly kill endothelial cells or traverse the endothelium and kill parenchymal graft cells. (From Briscoe and Sayegh30; used with permission from Nature Publishing Group, http://www.nature.com)
expression of CD80 and CD86 has been examined by immunohistochemistry and real-time polymerase chain reaction in human livers following transplantation.37 CD86 was found on the majority of Kupffer cells in all transplanted livers and in normal liver. CD80 was instead differentially expressed and was present only sporadically on normal liver but was present on at least 25% of the Kupffer cells in 45% of the transplanted livers. However, CD80 expression did not correlate with the occurrence of acute rejection. Cytotoxic T lymphocyte associated antigen 4
(CTLA4) is a CD28-related protein that is upregulated upon T-cell activation and, like CD28, binds to B7-1 and B7-2. Whereas CD28 delivers a positive costimulatory signal to T cells, CTLA4 delivers a negative signal that attenuates T-cell function. Because CTLA4 expression is enhanced following T-cell activation, and because it has a higher afnity for B7 than CD28 does, it has been proposed that the physiologic function of CTLA4 is to dampen or downregulate T-cell responses. Thus, specic activation of CTLA4 could potentially yield immunoinhibitory function and tolerance induction, but this approach has been hampered by the lack of suitable reagents to deliver the negative signal. The CD40/CD154 costimulation pathway is a second receptor/ligand pair that is critical in alloimmune responses. CD40 is constitutively expressed on APCs, including B cells, monocytes, macrophages, and DCs, but can also be expressed on nonimmune cells including endothelial cells, mast cells, platelets, and epithelial cells. In contrast, CD154 is expressed on CD4 T cells following activation, and to a lesser extent on NK cells, B cells, and CD8 T cells. Unlike the CD28/B7 costimulatory pathway that has primarily been dened in the context of effects on T-cell function, CD40/ CD154 ligation augments APC function as measured by upregulation of class II, CD80, and CD86 expression and production of cytokines, including IL-12. The sum effect of these changes to the APC is to signicantly enhance B- and T-cell responses to alloantigen. Molecular and immunohistochemical analysis of CD80, CD86, and CD154 expression in biopsies of liver recipients demonstrated an association between increased expression of CD86 and CD154, but not CD80, in the graft during severe acute cellular rejection.38 CD154 was also detected on Kupffer cells and sinusoidal macrophages in livers during chronic rejection but not in stable liver allografts or normal liver.39 Approaches to inhibit the CD28/B7 and CD40/ CD154 pathways have relied upon specic blocking antibodies or soluble fusion proteins such as CTLA4immunoglobulin (Ig). In the orthotopic rat liver transplantation model, repeated administration of CTLA4-Ig beginning at the time of transplantation, or delayed administration of CTLA4-Ig in combination with donor splenocytes, lead to extended graft survival of 100 days, whereas delayed administration of CTLA4-Ig alone or donor splenocytes alone did not.40 Gene therapy approaches to deliver CTLA4-Ig to liver allografts have been used with some success. Delivery of CTLA4-Ig by adeno-associated virus vectors or low dose FK506 alone failed to induce long-term graft survival. In contrast, the combination of adeno-associated
374
Martinez and Rosen
virus CTLA4-Ig transduction and low dose FK506 resulted in long-term graft survival, with most animals maintaining their graft over 180 days.41 Adenoviralmediated gene delivery of CTLA4-Ig through ex vivo perfusion of cold preserved livers lead to indenite survival of rat liver allografts and the generation of donorspecic unresponsiveness.42 Adenoviral-mediated delivery of CD40-Ig fusion proteins also resulted in indenite rat liver allograft survival and donor specic tolerance.43 The efcacy of anti-CD154 and CTLA4-Ig were compared in a rearterialized rat liver allograft model.44 Both treatments lead to prolonged allograft survival but treatment with anti-CD154 was associated with less biliary and endothelial cell injury compared with CTLA4-Ig. The CD40/CD154 pathway was also shown to play a role in ischemia/reperfusion injury.45 Mice decient in CD154 or wild-type animals treated with anti-CD154, had diminished hepatic injury and neutrophil inltration in a warm ischemia reperfusion model compared with control mice. While the CD28/B7 and CD40/CD154 costimulatory pathways have garnered the bulk of attention in transplantation, there is emerging evidence that other receptor/ligand pairs also play important roles in alloimmune responses.46,47 Recently, there has been considerable interest in two new members of the CD28/B7 family. Inducible costimulator (ICOS) is expressed following T-cell activation and augments cellular proliferation and cytokine production. The ligand for ICOS, B7h, is constitutively expressed on B cells, macrophages and dendritic cells as well as many nonlymphoid tissues, including the liver.48 The ICOS/B7h pathway was originally thought to provide a costimulatory signal for Th2 cytokine production, although it is now apparent that, under certain circumstances, ICOS can also trigger the production of the Th1 cytokine IFN- . Further, ICOS costimulation plays a central role in T-dependent B-cell activation and isotype switching. Intriguingly, ICOS may also participate in development of T regulatory cells.49 Programmed death-1 (PD-1) is induced upon activation of T cells, shares sequence homology with CTLA4, and contains an immunoreceptor tyrosinebased inhibitory motif in the cytoplasmic tail, characteristic of cellular receptors that deliver a negative signal. Indeed, mice decient in PD-1 develop autoimmune-like syndromes. PD-1 binds to two ligands, programmed death ligand (PDL)-1 and PDL-2, each differentially regulated by Th1 and Th2 cytokines, respectively. PDL-1 is constitutively expressed in the liver on Kupffer cells and sinusoidal
endothelium.50 Interestingly, PDL-1 decient mice display a spontaneous accumulation of CD8 T cells in the liver.51 Moreover, in the absence of PDL-1, T-cell activation lead to an accelerated form of experimental autoimmune hepatitis suggesting that PDL-1 plays a role in the deletion of CD8 T cells in the liver Several members of the tumor necrosis factor/tumor necrosis factor receptor families, of which CD40/ CD154 are members, can also provide alternate costimulatory signals to T lymphocytes. These receptor/ligand pairs include 4-1BB/4-1BBL (CD137), OX-40/OX-40L (CD134/CD134L), and CD30CD30L(CD153). The receptor 4-1BB is expressed on CD4 and CD8 T cells following activation, while its ligand, 4-1BBL, is expressed on activated B cells, macrophages, and DCs. The receptor 4-1BB appears to be particularly important in CD8 T-cell responses. In contrast, OX-40 / OX-40L primarily acts on CD4 T cells. CD30 is another T-cell costimulatory molecule that has been implicated in alloimmune responses. CD30 has been shown to mark the predominant proliferating Tcell population in response to alloantigen52 and CD30 T cells comprise the major population of IFN- and IL-5 producing cells following alloactivation.53 A soluble form of CD30 measured in the blood early posttransplantation was shown to be a highly sensitive and specic marker for acute rejection in kidney recipients.54 In general, these alternate costimulatory molecules are expressed on T cells relatively late following activation and their relationship to CD28 signaling is still to be determined. OX-40, 4-1BB, and CD30 may act to further modulate T-cell function in the context of CD28 signaling or to provide distinct, independent signaling. However, their role in liver transplantation remains to be studied.
Effector Pathways of Graft Injury
Once nave T cells have received signals through the TCR and the appropriate costimulatory molecules for complete activation, and any additional cues from cytokines or cell surface receptors required for differentiation, they transition to effector cells. Mature effector T cells, be they CD4 or CD8 , are capable of mediating graft injury. Recently, much work has focused on the phenotypic distinction of effector T cells from nave cells and memory T cells,55 and this line of investigation will likely expand our understanding of the immune status of graft recipients in the future. The long-standing triumvirate of effector pathways in graft rejection is (1) T-cellmediated cytotoxicity, (2) delayed type hypersensitivity, and (3) antibody-mediated damage.
CAQ Corner
375
The relative importance of each of these pathways in graft rejection is likely to depend on a variety of factors, including the organ transplanted, the sensitization status of the recipient, concomitant infections, and the immunosuppressive protocols that are utilized. Activated CD8 cytotoxic T lymphocytes (CTLs) specic for donor class I can interact with the graft directly and cause tissue injury through biochemical mechanisms that induce apoptosis. Indeed, apoptosis is a prominent component of cell death in liver allograft rejection.56 In the perforin/granzyme pathway, effector cell-derived perforin and the serine protease granzyme B collaborate to induce target cell death. Perforin is inserted into the target cell membrane in a Ca dependent process forming pores that permit the delivery and entry of granzyme B into the target cell cytosol from preformed cellular granules. This ultimately leads to target cell death through apoptosis. Elevations in granzyme B messenger ribonucleic acid are associated with acute liver allograft rejection, suggesting that this pathway is operative following human liver transplantation.57 The Fas/Fas ligand (FasL) pathway is another death-inducing pathway utilized by CTL. Whereas FasL is specically induced upon CTL activation, Fas is ubiquitously expressed on lymphoid and nonlymphoid tissue including the liver. Cross-linking of Fas with trimerized FasL or agonist antibodies leads to formation of the death inducing signaling complex in target cells, activation of caspase 8, and propagation of a death signal that culminates in apoptosis. The Fas/FasL pathway is thought to play an important role in a variety of hepatic pathologies and there is evidence that this pathway is also active during liver allograft rejection.58,59 A more recently characterized molecule, granulysin, is expressed by CD8 T cells as well as by CD4 T cells and NK cells and can also induce target cell apoptosis.60 However, there have been no reports on the involvement of granulysin in liver allograft rejection. Delayed type hypersensitivity is initiated by alloantigen-primed CD4 T cells specic for donor class II. Upon reexposure to specic alloantigen, CD4 T cells release IFN- , a proinammatory cytokine that can cause activation of macrophages and the subsequent release of a variety of soluble mediators. These inammatory mediators can augment the cellular antigraft response or can cause direct tissue damage. The presence of donor-sensitized T cells in graft recipients can be revealed in the trans-vivo delayed type hypersensitivity response in which peripheral blood mononuclear cells from graft recipients are injected into the ear or footpad of immunodecient severe combined immunodeciency mice.61 The degree of swelling following
challenge with specic alloantigen provides an index of prior sensitization. Further, the use of the trans-vivo assay revealed the presence of active regulatory pathways in 3 patients, including 1 liver transplant recipient, who had suspended immunosuppression but maintained stable graft function.62 In this study, peripheral blood mononuclear cells from the 3 patients showed diminished response to donor antigen, but good recall responses to unrelated antigens such as Epstein-Barr virus in the trans-vivo assay. Suppression of antidonor responses could be broken with antibodies to IL-10 or transforming growth factor- , indicating that these cytokines were essential to maintaining active regulation. Antibodies specic for graft antigens can mediate graft injury through activation of the complement cascade or through binding to Fc receptors on effector cells and triggering antibody-dependent cell-mediated cytotoxicity. Unlike humoral rejection caused by ABO blood group incompatibilities, alloantibodies directed at MHC class I or class II disparities are not considered to play a prominent role in liver allograft rejection. However, a novel mechanism was recently proposed in which antibodies against LSECs indirectly promote acute rejection.63 In this study, it was determined that antibodies against LSECs were more frequently observed in patients undergoing rejection than in patients without rejection. Furthermore, the antibodies induced expression of CD86 on LSECs and increased T-cell proliferation while decreasing transforming growth factor- production in mixed LSEC/T-cell cultures. Interestingly, a signicant fraction of the anti-LSEC reactivity was not directed against human leukocyte antigen (HLA) antigens, suggesting that other cellular components are the target of these antibodies. It has been a challenging process to try to unravel the participation of specic effector pathways, and their interrelationships, in liver allograft rejection. It is possible to denitively state that CD4 T cells, CD8 T cells, macrophages, and plasma cells can be found in the liver during rejection. However, it is much more difcult to demonstrate that any of these cell types are actively involved in a destructive immune response. The multitude of studies using gene-decient mice in experimental transplantation models has taught us that it is difcult to denitively identify any single mediator or cell type that is absolutely required for graft rejection. Rather, it appears that several redundant and compensatory mechanisms are in place that can contribute to graft rejection. Moreover, the participation of alternate pathways of graft
376
Martinez and Rosen
rejection by other cell types found within the inammatory inltrate, such as eosinophils, has been proposed and should be considered as well.64
Experimental Studies on Tolerance in the Liver and Associated Mechanisms
A series of experimental and clinical observations indicating that the liver is less immunogenic than other vascularized organs, and that liver allografts can even provide tolerogenic properties for other organ grants, have led to a search for mechanisms that account for these ndings. It is clear from rat and mouse transplantation models of spontaneous liver tolerance that an active immune process of some type is initiated in nonrejecting mouse70 and rat strain combinations,71 since an inammatory inltrate and early liver injury, which ultimately resolves, can be observed. It has been considered that the large mass of the liver and its regenerative potential could overcome the early injury, but this is unlikely to account for the robust protection that the liver affords to subsequent allografts. Thus, it is reasonable to consider that some active immunoregulatory process is associated with the liver effect. Multiple mechanisms have been proposed to explain how the liver could inuence or modulate the host immune system. These mechanisms can be divided into 3 categories: soluble factors, cellular components, and structural features of the liver. Almost 20 years ago, it was noted that the liver produced and secreted large amounts of soluble MHC class I that could readily be measured in the circulation of healthy individuals and liver recipients.72,73 Thus, it has been proposed that soluble donor class I could have immunomodulatory properties through passive blockade of alloantibodies and donor-specic effectors or through induction of activation-induced cell death of allospecic CTL.74 Direct tests of the effects of soluble class I on graft survival, however, have been difcult to reconcile. In some studies, direct in vivo administration of rat liver derived soluble class I prolonged cardiac allograft survival, particularly when class I proteins were complexed with anti-class I monoclonal antibodies.75 However, in other studies soluble MHC class I failed to modulate kidney or cardiac allograft survival or inhibit generation of CTL in vivo.76 The nding that serum from rats that spontaneously accept their liver allograft could transfer the protective effect led to a search to identify the suppressive activity. Liver suppressor factor 1 is a 40-kD protein isolated from the serum of spontaneously tolerant recipients (dark Agouti3 Piebald-Viral-Glaxo [PVG]). Administration of liver suppressor factor 1 can prolong rat cardiac allograft survival,77 but elucidation of the mechanism of liver suppressor factor 1 and the broad applicability of these ndings remain to be determined.
Experimental Studies on Mechanisms of Liver Allograft Rejection
The rat orthotopic liver transplant model has been particularly useful in gaining insight into the immunologic mechanisms that are active following liver transplantation. In the rat, the outcome of liver transplantation is highly dependent upon the particular strain combination used, as some combinations lead to classic acute cellular rejection, whereas others lead to spontaneous tolerance. The strain combinations that result in acute rejection fairly closely recapitulate the features of human liver allograft rejection. Thus, in the dark Agouti3 Lewis combination, a slight mixed and mononuclear cell inltrate in the portal region and venous endothelialitis are seen by day 2 posttransplantation.65 One day later mononuclear cell inltration, venous endothelialitis, and parenchymal changes are apparent. By day 7, severe acute rejection is underway, with marked inammatory inltrates, bridging necrosis, and endothelialitis. Elevations in liver enzymes are measurable in allografts on days 3 to 4, with progressive increases through at least day 7. Within the graft, transcripts for IL-2, IFN- , IL-4, tumor necrosis factor- , and IL-10 are noted,65 indicating that rejection is not associated with a polarized Th1 or Th2 cytokine response. Apoptosis of graft cells is a noted feature of liver allograft rejection,59,66 and it is accompanied by specic increases in messenger ribonucleic acid for perforin, granzyme B, and FasL in allografts, but not isografts, suggesting that these mediators participate in the induction of cell death in the graft.59,67 Interestingly, apoptosis and graft rejection can occur in the absence of CD8 T cells.59 One candidate cell population that could account for the increase in FasL, perforin, and granzyme B in rejecting liver allograft are NK cells. As described above, NK cells were originally identied on the basis of their ability to kill tumor targets without prior activation or sensitization. Recent studies indicate that large numbers of host NK cells inltrate liver allografts early posttransplantation68 and express high levels of FasL and granzyme B. Moreover, a novel NK cell activation receptor, rNKp30, was cloned from a rejecting liver allograft, suggesting that NK cells within the liver have the potential to mediate cytotoxicity.69
CAQ Corner
377
Finally, normal human hepatocytes can produce a soluble form of Fas that is derived from a variant transcript lacking the terminal 5 amino acids of the extracellular region and 16 of 17 amino acids of the transmembrane region.78 Hepatocyte lysates containing soluble Fas could inhibit anti-Fas induced apoptosis of Jurkat cells in vitro. Moreover, the levels of soluble Fas decreased in patients undergoing graft rejection as compared to patients with a stable course. These data suggest that soluble Fas could modulate the Fas/FasL pathway in liver recipients. In the case of each of these soluble mediators, it has been shown that they can inhibit CTL function in vitro; however, their participation in the liver effect in vivo is unclear. While it is unlikely that any one of these factors is solely responsible for the tolerogenic properties of liver allografts, it is possible that they act in concert with other hepatic components to promote tolerance. Along these lines, it has been denitively shown that depletion of resident leukocytes from liver allografts by irradiation markedly diminishes the tolerogenic effect, suggesting that some cellular component of the graft is responsible.79 Similar conclusions can be drawn from studies by Sriwatanawaongsa et al.80 In this model, recovery and retransplantation of a tolerant allograft into a second recipient of the same strain as the rst leads to graft rejection rather than tolerance. This can be explained by the fact that temporarily parking the allogeneic donor liver in the rst recipient results in the replacement of the passenger leukocytes with host leukocytes, thereby creating a chimeric liver. When the chimeric liver is retransplanted into the second recipient, spontaneous tolerance does not occur and the graft is rejected, because donor leukocytes are required for induction of tolerance. This concept, of course, is in marked contrast to the traditional paradigm of the role of passenger leukocytes in organ allografts in which bone marrow derived leukocytes associated with the graft are thought to be the critical cell type involved in priming nave recipient T cells to donor antigens in secondary lymphoid organs, and thereby precipitating destructive alloimmune responses.81 This disparity between the liver and other organ grafts could be due to multiple factors, not the least of which are differences in the number and type of passenger leukocytes in the various organ grafts and their intrinsic potential for modulating alloimmune responses. As such, a prominent model proposed by Starzl et al.14 attributes the tolerogenic properties of the liver to the ability of graft-derived stem cells to migrate out of the graft following transplantation, to persist, and to interact in some fashion with host elements to establish
a state of microchimerism that can lead to clonal exhaustion or deletion of host alloreactive T cells. Support for this model comes from the observation that patients with long-term surviving allografts have evidence of donor cell microchimerism in peripheral tissue. However, because it has not been feasible to establish whether donor microchimerism in clinical allograft recipients is a cause or an effect of long-term graft survival, and because the correlation of microchimerism and graft survival is not absolute, validation of this model has not been achieved. While a multitude of studies have implicated liverassociated cells with migratory potential in spontaneous liver tolerance, the identity of the cell or cells involved has not been solved. One such candidate cell type is the immature DCs found in the liver, as discussed previously. Mature DCs, rich in MHC class II and costimulatory molecule expression, are exquisitely efcient antigen-presenting cells and are potent inducers of alloreactivity. Immature DCs, by contrast, do not express signicant levels of the costimulatory molecules CD80 and CD86 and as such are poor inducers of Tcell activation, and may in fact inhibit T-cell responses through incomplete activation. Indeed, administration of immature DCs to mice did lead to prolonged cardiac allograft survival in the absence of immunosuppression, although the effect was relatively modest.82 Furthermore, progenitor DCs isolated from the liver and propagated in GM-CSF failed to stimulate allogeneic T cells in MLR, and transfer of the immature DCs to islet allograft recipients prolonged graft survival.83 Other resident APCs in the liver have also been implicated in liver tolerance. As already discussed, LSECs are a unique nonmyeloid APCs found in the liver that can efciently cross present soluble antigen to CD8 T cells but, through this process, induces tolerance rather than immunity.84 Finally, Kupffer cells, macrophage-like APCs found in the hepatic sinusoids, were shown many years ago to be required for tolerance induction by the liver. In these studies, inactivation of Kupffer cells with gadolinium chloride inhibited tolerance induced via the portal vein route.85 Possible mechanisms for the effect of Kupffer cells in liver tolerance come from recent studies by Sun et al.,86 demonstrating that Kupffer cells express functional FasL that can induce apoptosis of T cells and that transfer of Kupffer cells derived from accepted grafts can prolong graft survival in an acute rejection model. Finally, unique aspects of the livers architecture that allow T cells to come in close contact with tissue cells, including the LSECs and perhaps hepatocytes, could promote T-cell nonresponsiveness or deletion.87 Clearly, examples of functional immune
378
Martinez and Rosen
activation and tolerance induction can be readily demonstrated in the liver. The factors that determine either outcome remain to be determined, but unifying paradigms to explain these observations have been proposed.88
Immune Aspects of Clinical Liver Transplantation: Rejection, Recurrence of Autoimmune Liver Disease, and Hepatitis C Virus Recurrence
Acute cellular rejection occurs in 50% to 75% of liver allograft recipients and the majority of episodes occur within 90 days of transplant surgery.89 The targets of activated lymphocytes are donor-derived bile duct epithelial cells and vascular endothelium, whereas direct involvement of hepatocytes is uncommon. Chronic rejection, often termed ductopenic rejection, is characterized by ischemic injury to and paucity of bile ducts; the frequency of chronic rejection has decreased in the past decade and currently occurs in less than 5% of patients. The pharmacologic agents used to prevent and treat acute and chronic rejection are covered in great detail in a separate CAQ Corner by Douglas and colleagues from the Mayo Clinic. The induction of transplantation tolerance, dened as the survival of a functioning allograft in the absence of continuing immunosuppressive therapy, would obviously represent a major advance. Experimental and emerging clinical data have suggested that transplantation tolerance could be induced by pretransplantation myeloconditioning and infusion of donor hematopoietic cells,90 but further experience is required. A number of diseases treated by liver transplantation are believed to be autoimmune in origin and, theoretically, any transplanted organ is as susceptible to the autoimmune process as the organ being replaced.91 In particular, evidence for recurrence of autoimmune hepatitis is supported by most studies, whereas data for recurrence of primary sclerosing cholangitis and primary biliary cirrhosis (which can be histopathologically indistinguishable from rejection) are controversial. The immunosuppression used to prevent graft rejection is in most cases sufcient to prevent signicant autoimmune damage to the allograft, but a proportion of patients may develop graft failure from disease recurrence. Liver transplantation is performed with no regard to specic matching of donor-recipient HLA alleles, and this may serve as a barrier to the development of protective (i.e., antiviral) cell-mediated immunity directed against infected cells within the allograft. CD8 T cells are the primary effector lymphocytes for provision of
protective immunity against intracellular pathogen infection of parenchymal cells and are effective because of their ability to recognize infected cells as the combination of pathogen-derived peptides in the peptidebinding grooves of HLA class I molecules on the surface of infected cells. While incompletely understood, the immune recognition of the hepatitis C virus infected allograft may be essential in the containment of infection. Recognition of the allograft could occur either via recipient-derived T cells or via those derived from the donor. For the recipient-derived T cells, recognition could occur either through use of shared HLA molecules, or could occur through the expansion of recipient-derived T cells that are uniquely restricted by the HLA molecules of the donor liver. Because prior research has focused on CD8 T cells restricted by recipient MHC molecules, little is known about the relative contribution of those cells uniquely restricted by the donor liver. A recent report demonstrated the generation of hepatitis C virus specic T cells that are restricted by donor HLA alleles,92 underscoring the plasticity of the TCR, as well as the need to assess both recipient and allograft restricted CTL in order to develop a comprehensive understanding of protective immunity to hepatitis C virus after liver transplantation.
References
1. Calne RY, Sells RA, Pena JR, Davis DR, Millard PR, Herbertson BM, et al. Induction of immunological tolerance by porcine liver allografts. Nature 1969;223:472-476. 2. Kamada N, Davies HS, Roser B. Reversal of transplantation immunity by liver grafting. Nature 1981;92:840-842. 3. Kamada N, Wight DGD. Antigen-specic immunosuppression induced by liver transplantation in the rat. Transplantation 1984;38:217-221. 4. Zhong R, He G, Sakai Y, Li XY, Garciai B, Wall W, et al. Combined small bowel and liver transplantation in the rat: possible role of the liver in preventing intestinal allograft rejection. Transplantation 1991;52:550-552. 5. Wang C, Sun J, Wang L, Li L, Horvat M, Sheil R. Combined liver and pancreas transplantation induces pancreas allograft tolerance. Transplant Proc 1997;29:1145-1146. 6. Sarnacki S, Revillon Y, Cerf-Bensussan N, Calise D, Goulet O, Brousse N. Long-term small-bowel graft survival induced by a spontaneously tolerated liver allograft in inbred rat strains. Transplantation 1992;54:383-385. 7. Wang XY, Sun J, Wang C, France M, Sheil AG. Effect of liver transplantation on islet allografts: up-regulation of Fas ligand and apoptosis of T lymphocytes are associated with islet graft tolerance. Transplantation 2001;71:102-111. 8. Valiante N. Natural killer cells and other variations on the theme of a cytotoxic lymphocyte. Hepatic Inammation and Immunity Meeting, Galveston, TX, March 24, 2002. 9. Shevach EM. Regulatory T cells in autoimmunity. Annu Rev Immunol 2000;18:423-449.
CAQ Corner
379
NKT cells characterizes cirrhosis progression in chronic viral hepatitis. J Immunology 2004;173:1417-1425. Briscoe DM, Sayegh MH. A rendezvous before rejection: where do T cells meet transplant antigens? Nat Med 2002;8:220-222. Demetris AJ, Qian S, Sun H, Fung JJ, Yagihashi A, Murase N, et al. Early events in liver allograft rejection. Delineation of sites of simultaneous intragraft and recipient lymphoid tissue sensitization. Am J Pathol 1991;138:609-619. Illigens BM, Yamada A, Fedoseyeva EV, Anosova N, Boisgerault F, Valujskikh A, et al. The relative contribution of direct and indirect antigen recognition pathways to the alloresponse and graft rejection depends upon the nature of the transplant. Hum Immunol 63:912-925. Renna-Molajoni E, Cinti P, Evangelista B, Orlandini AM, Molajoni J, Cocciolo PL, et al. Role of the indirect recognition pathway in the development of chronic liver allograft rejection. Transplant Proc 1998;30:2140-2141. Salama AD, Najaan N, Clarkson MR, Harmon WE, Sayegh MH. Regulatory CD25 T cells in human kidney transplant recipients. J Am Soc Nephrol 2003;14:1643-1651. Carreno BM, Collins M. The B7 family of ligands and its receptors: new pathways for costimulation and inhibition of immune responses. Ann Rev Immunol 2002;20:29-53. Quezada SA, Jarvinen LZ, Lind EF, Noelle RJ. CD40 / CD154 interactions at the interface of tolerance and immunity. Annu Rev Immunol 2004;22:307-328. Kwekkeboom J, Kuijpers MA, Bruyneel B, Mancham S, De Baar-Heesakkers E, Ijzermans JN, et al. Expression of CD80 on Kupffer cells is enhanced in cadaveric liver transplants. Clin Exp Immunol 2003;132:345-351. Bartlett AS, McCall JL, Ameratunga R, Yeong ML, Gane E, Munn SR. Analysis of intragraft gene and protein expression of the costimulatory molecules, CD80, CD86 and CD154, in orthotopic liver transplant recipients. Am J Transplant 2003;3: 1363-1368. Gaweco AS, Wiesner RH, Yong S, Krom R, Porayko M, Chejfec G, et al. CD40L (CD154) expression in human liver allografts during chronic ductopenic rejection. Liver Transpl Surg 1999;5:1-7. Neumann UP, Fischer U, Schmitz V, Lang M, Langrehr JM, Neuhaus P. Long-term graft acceptance after rat liver allograft transplantation induced by application of CTLA4-Ig and donor specic spleen cell administration. Transplant Proc 2002;34: 1400-1401. Yang Z, Wu X, Tsui T-Y, Hou Y, Luk J, Fan S-T. Long term liver allograft survival induced by combined treatment with rAAV-hCTLA4Ig gene transfer and low dose FK506. Transplantation 2003;75:303-308. Olthoff K, Judge TA, Gelman AE, Xhen XD, Hancock WW, Turka LA, Shaked A. Adenovirus-mediated gene transfer into cold-preserved liver allografts: survival pattern and unresponsiveness following transduction with CTLA4Ig. Nat Med 1998;4: 194-200. Nomura M, Yamashita K, Murakami M, Takehara M, Echizenya H, Sunahara M, et al. Induction of donor-specic tolerance by adenovirus-mediated CD40Ig gene therapy in rat liver transplantation. Transplantation 2002;73:1403-1410. Bartlett AS, McCall, Ameratunga R, Howden B, Yeong M-L, Benjamin CD, et al. Costimulatory blockade prevents early rejection, promotes lymphocyte apoptosis and inhibits the upregulation of intergraft interleukin 6 in an orthotopic liver transplant model in the rat. Liver Transpl 2002;8:458-468. Shen X-D, Ke B, Amersi F, Gao FM, Anselmo DM, Busittil R,
10. Stassen M, Schmitt E, Jonuleit H. Human CD4 CD25 regulatory T cells and infectious tolerance. Transplantation 2004; 77(Suppl):S23-S25. 11. Jonuleit H, Schmitt E, Steinbrink K, Enk AH. Dendritic cells as a tool to induce anergic and regulatory T cells. Trends Immunol 2001;22:394-400. 12. Banchereau J, Steinman RM. Dendritic cells and the control of immunity. Nature 1998;392:245-252. 13. Lau AH, Thomson AW. Dendritic cells and immune regulation in the liver. Gut 2003;52:307-314. 14. Starzl TE, Demetris AJ, Murase N, Ildstad S, Ricordi C, Trucco M. Cell migration, chimerism and graft acceptance. Lancet 1992;339:1579-1582. 15. Doherty DG, OFarrelly C. Lymphoid repertoires in healthy liver. In: Gershwin ME, Vierling JM, Manns MP, eds. Liver immunology. Philadelphia: Hanley & Belfus, 2003:31-46. 16. Calne RY. Immunological tolerancethe liver effect. Immunol Rev 2000;174:280-282. 17. OFarrelly C. Immunoregulation in the liver and its extrahepatic relevance. J Pediatr Gastroenterol Nutr 2004;39(Suppl 3):S727S728. 18. Knolle PA, Limmer A. Role and function of liver sinusoidal endothelial cells. In: Gershwin ME, Vierling JM, Manns MP, eds. Liver immunology. Philadelphia: Hanley & Belfus, 2003: 59-73. 19. Katz SC, Pillarisetty VG, Bleier JI, Shah AB, DeMatteo RP. Liver sinusoidal endothelial cells are insufcient to activate T cells. J Immunol 2004;173:230-235. 20. Lanier LL. Natural killer cell receptor signaling. Curr Opin Immunol 2003;15:308-314. 21. Golden-Mason L, OFarrelly C. Having it all? Stem cells, haematopoiesis and lymphopoiesis in adult human liver. Immunol Cell Biol 2002;80:45-51. 22. Wertheimer AW, Bakke A, Rosen HR. Direct enumeration and functional assessment of circulating dendritic cells in patients with liver disease. Hepatology 2004;40:335-345. 23. Bendelac A, Rivera MN, Park SH, Roark JH. Mouse CD1specic NK1 T cells: development, specicity and function. Annu Rev Immunol 1997;15:535-562. 24. Ishigami M, Nishimura H, Naiki Y, Yoshioka K, Kawano T, Tonaka Y, et al. The roles of intrahepatic V 14 NK1 T cells for liver injury induced by Salmonella infection in mice. Hepatology 1999;29:1799. 25. Norris S, Collins C, Doherty DG, Smith F, McEntee G, Traynor O, et al. Resident human hepatic lymphocytes are phenotypically different from circulating lymphocytes. J Hepatol 1998;28:84 90. 26. Whiteside TL, Herberman RB. Role of human natural killer cells in health and disease. Clin Diagn Lab Immunol 1994;1:125 133. 27. Lilly LB, Ding J, Levy GA. The immunology of hepatic allograft rejection. In: Maddrey WC, Schiff ER, Sorrell M, eds. Transplantation of the liver. Philadelphia: Lippincott Williams & Wilkins, 2001:211-228. 28. Doherty DG, Norris S, Madrigal-Estebas L, McEntee G, Traynor O, Hegarty JE, et al. The human liver contains multiple populations of NK cells, T cells, and CD3 CD56 natural T cells with distinct cytotoxic activities and Th1, Th2, and Th0 cytokine secretion patterns. J Immunol 1999;163:2314-2321. 29. De Lalla C, Galli G, Aldrighetti L, Romeo R, Mariani M, Monno A, et al. Production of probrotic cytokines by invariant
30. 31.
32.
33.
34.
35.
36.
37.
38.
39.
40.
41.
42.
43.
44.
45.
380
Martinez and Rosen
46.
47. 48.
49.
50.
51.
52.
53.
54.
55.
56.
57.
58.
59.
60.
61.
62.
63.
Kupiec-Weglinski JW. CD154-CD40 T-cell costimulation pathway is required in the mechanism of hepatic ischemia/reperfusion injury, and its blockade facilitates and depends on heme oxygenase-1 mediated cytoprotection. Transplantation 2002;74: 315-319. Salama AD, Sayegh MH. Alternative T-cell costimulatory pathways in transplant rejection and tolerance induction: hierarchy or redundancy? Am J Transplant 2003;3:509-511. Martinez OM. Immunobiology of CD30 T lymphocytes. Graft 2001;3:180-187. Swallow MM, Wallin JJ, Sha WC. B7h, a novel costimulatory homolog of B7.1 and B7.2, is induced by TNFalpha. Immunity 1999;11:423-432. Akbari O, Freeman GJ, Meyer EH, Greeneld EA, Chang TT, Sharpe AH, et al. Antigen-specic regulatory T cells develop via the ICOS-ICOS-ligand pathway and inhibit allergen-induced airway hyperreactivity. Nat Med 2002;8:1024-1032. Iwai Y, Terawaki S, Ikegawa M, Okazaki T, Honjo T. PD-1 inhibits antiviral immunity at the effector phase in the liver. J Exp Med 2003;198:39-50. Dong H, Zhu G, Tamada K, Flies DB, van Deursen JM, Chen L. B7-H1 determines accumulation and deletion of intrahepatic CD8( ) T lymphocytes. Immunity 2004;20:327-336. Chan KW, Hopke CD, Krams SM, Martinez OM. CD30 expression identies the predominant proliferating T lymphocyte population in human alloimmune responses. J Immunol 2002;169:1784-1791. Martinez OM, Villanueva J, Abtahi S, Beatty PR, Esquivel CO, Krams SM. CD30 expression identies a functional alloreactive human T-lymphocyte subset. Transplantation 1998;65:1240 1247. Pelzl S, Opelz G, Daniel V, Wiesel M, Susal C. Evaluation of posttransplantation soluble CD30 for diagnosis of acute renal allograft rejection. Transplantation 2003;75:421-423. Sallusto F, Geginat J, Lanzavecchia A. Central memory and effector memory T cell subsets: function, generation, and maintenance. Ann Rev Immunol 2004;22:745-763. Krams SM, Egawa H, Quinn MB, Villanueva JC, GarciaKennedy R, Martinez OM. Apoptosis is a mechanism of cell death in liver allograft rejection. Transplantation 1995;59:621625. Krams SM, Villanueva JC, Quinn MB, Martinez OM. Expression of the cytotoxic T cell mediator granzyme B during liver allograft rejection. Transpl Immunol 1995;3:162-166. Tannapel A, Kohlhaw K, Ebelt J, Hauss J, Liebert U, Berr F, Wittekind C. Apoptosis and the expression of Fas and Fas ligand (FasL) antigen in rejection and reinfection in liver allograft specimens. Transplantation 1999;15:1079-1083. Ogura Y, Martinez OM, Villanueva JC, Tait JF, Strauss HW, Higgins JPT, et al. Apoptosis and allograft rejection in the absence of CD8 T cells. Transplantation 2001;71:18271834. Pena SV, Krensky AM. Granulysin, a new human cytolytic granule-associated protein with possible involvement in cell mediated cytotoxicity. Semin Immunol 1997;9:117-125. Carrodeguas L, Orosz CG, Waldman WJ, Sedmak DD, Adams PW, VanBuskirk AM. Trans vivo analysis of human delayed-type hypersensitivity reactivity. Hum Immunol 1999;60:640-651. VanBuskirk AM, Burlingham WJ, Jankowska-Gan E, Chin T, Kusaka S, Geissler F, et al. Human allograft acceptance is associated with immune regulation. J Clin Invest 2000;106:145-155. Sumitran-Holgersson S, Ge X, Karra Z, Xu B, Nava S, Broome
64.
65.
66.
67.
68. 69.
70.
71.
72.
73.
74.
75.
76.
77.
78.
79.
80.
U, et al. A novel mechanism of liver allograft rejection facilitated by antibodies to liver sinusoidal endothelial cells. Hepatology 2004;40:1211-1221. Martinez OM, Ascher NL, Ferrell L, Villanueva J, Lake J, Roberts JP, Krams SM. Evidence for a non-classical pathway of graft rejection involving interleukin 5 and eosinophils. Transplantation 1993;55:909-918. Egawa H, Martinez OM, Quinn MB, Villanueva JC, So S, Esquivel CO, Krams SM. Acute liver allograft rejection in the rat. An analysis of the immune response. Transplantation 1995; 59:97-102. Li X-K, Kita Y, Tamura A, Enosawa S, Amemiya H, S. Suzuki. Activation of Fas and perforin pathways in rat liver allograft rejection. Transplant Proc 1998;30:19-21. Hiroyasu S, Shiraishi M, Koji T, Mamadi T, Sugawa H, Muto Y. Analysis of the Fas system and Bcl-2 in rat liver allograft rejection. J Surg Res 1999;84:204-211. Hsieh CL, Obara H, Ogura Y, Martinez OM, Krams SM. NK cells and transplantation. Transpl Immunol 2002;9:111-114. Hsieh CL, Ogura Y, Obara H, Ali UA, Rodriquez GM, Nepomuceno RR, et al. Identication, cloning and characterization of a novel rat natural killer receptor, rNKp30: a molecule expressed in liver allografts. Transplantation 2004;77:121-128. Qian S, Lu L, Li Y, Fu F, Li W, Starzl TE, et al. Apoptosis within spontaneously accepted mouse liver allografts: evidence for deletion of cytotoxic T cells and implications for tolerance induction. J Immunol 1997;158:4654-4661. Farges O, Morris PJ, Dallman MJ. Spontaneous acceptance of liver allografts in the rat. Analysis of the immune response. Transplantation 1994;57:171-177. Spencer SC, Fabre JW. Bulk purication of a naturally occurring soluble form of RT1-A class I major histocompatibility complex antigens from DA rat liver, and studies of specic immunosuppression. Transplantation 1987;44:141-148. Davies H, Pollard S, Calne R. Soluble HLA antigens in the circulation of liver graft recipients. Transplantation 1989;47: 524-537. Zavazava N, Kronke M. Soluble HLA class I molecules induce apoptosis in alloreactive cytotoxic T lymphocytes. Nat Med 1996;2:1005-1010. Sumimoto R, Kamada N. Specic suppression of allograft rejection by soluble class I antigen and complexes with monoclonal antibody. Transplantation 1990;50:678-682. Priestley CA, Dalchau R, Sawyer GF, Fabre JW. A detailed analysis of the potential of water-soluble classical clas I MHC molecules for the suppression of kidney allograft rejection and in vitro cytotoxic T cell responses. Transplantation 1989;48:10311038. Edwards-Smith C, Goto S, Lord R, Shimizu Y, Vari F, Kamada N. Allograft acceptance and rejection, mediated by a liver suppressor factor, LSF-1, puried form serum of liver transplanted rats. Transpl Immunol 1996;4:287-292. Krams SM, Fox CK, Beatty F, Cao S, Villanueva JC, Esquivel CO, Martinez OM. Human hepatocytes produce an isoform of Fas that inhibits apoptosis. Transplantation 1998;65:713721. Sun J, McCaughan GW, Gallagher ND, Sheil AG, Bishop GA. Deletion of spontaneous rat liver allograft acceptance by donor irradiation. Transplantation 1995;60:233. Sriwatanawaongsa V, Davies HFF, Calne RY. The essential role of parenchymal tissues and passenger leukocytes in the tolerance induced by liver grafting. Nat Med 1995;1:431.
CAQ Corner
381
AM, Klein AS. Hepatic allograft-derived Kupffer cells regulate T cell response in rats. Liver Transpl 2003;9:489-497. Crispe IN. Hepatic T cells and liver tolerance. Nat Rev Immunol 2003;3:51-62. Reding R, Davies HFS. Revisiting liver transplant immunology: from the concept of immune engagement to the dualistic pathway paradigm. Liver Transpl 2004;10:1081-1086. Wiesner RH, Ludwig J, Krom RA, Hay JE, van Hoek B. Hepatic allograft rejection: new developments in terminology, diagnosis, prevention, and treatment. Mayo Clin Proc 1993;68:69-79. Donckier V, Troisi R, Toungouz M, Colle I, Van Vlierberghe H, Jacquy C, et al. Donor stem cell infusion after non-myeloablative conditioning for tolerance induction to HLA mismatched adult living-donor liver graft. Transpl Immunol 2004;13:139-146. Rosen HR. Disease recurrence following liver transplantation. Clin Liver Dis 2000;4:675-689. Rosen HR, Hinrichs DJ, Leistikow RL, Calendar G, Nishimura M, Lewinsohn DM. Cutting edge: identication of hepatitis C virus-specic CD8 T cells by donor HLA alleles following liver transplantation. J Immunol 2004;173:5355-5359.
81. Talmedge DW, Dart G, Radovich J, Lafferty KJ. Activation of transplant immunity: effect of donor leukocytes on thyroid allograft rejection. Science 1976;191;385-388. 82. Fu F, Li Y, Qian S, Lu L, Chambers F, Starzl TE, et al. Costimulatory molecule-0decient dendritic cell progenitors (MHC class II , CD80dim, CD86-) prolong cardiac allograft survival in nonimmunosuppressed recipients. Transplantation 1996;62: 659-665. 83. Rastellini C, Lu L, Ricordi C, Starzl TE, Rao AS, Thomson AW. Granulocyte/macrophage colony-stimulating factor stimulated hepatic dendritic cell progenitors prolong pancreatic islet allograft survival. Transplantation 1995;15:1366-1370. 84. Limmer A, Ohl J, Kurts C, Ljunggren HG, Reiss Y, Groettrup M, et al. Efcient presentation of exogenous antigen by liver endothelial cells to CD8 T cells results in antigen-specic T cell tolerance. Nat Med 2000;6:1348-1354. 85. Callery MP, Kamei T, Flye MW. Kupffer cell blockade inhibits induction of tolerance by the portal venous route. Transplantation 1989;47:1092-1094. 86. Sun Z, Wada T, Maemura K, Uchikura K, Hoshino S, Diehl
87. 88.
89.
90.
91. 92.
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (895)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Lymphatic SystemDocument37 pagesLymphatic SystemDam Lakbao100% (1)
- Procedures Required Prior To Restoration MCQDocument7 pagesProcedures Required Prior To Restoration MCQSR Shots100% (1)
- Triangles of The NeckDocument204 pagesTriangles of The Necknevmerka100% (3)
- Cardiovascular System PPT FeDocument26 pagesCardiovascular System PPT FeAngel Grace GaliasNo ratings yet
- 20) Dr. Dr. Himawan Sanusi, Sp. PD, KEMD - Cushing+conn+addsosnianDocument27 pages20) Dr. Dr. Himawan Sanusi, Sp. PD, KEMD - Cushing+conn+addsosnianAsridewi DewiNo ratings yet
- Blood DonationDocument16 pagesBlood DonationMarc Lloyd AlfonsoNo ratings yet
- SPEC I TASK 12 - Human Reproductive SystemDocument11 pagesSPEC I TASK 12 - Human Reproductive SystemJERIEL MARTIREZNo ratings yet
- Nephrolithotomy To Nephrectomy: A Rare Case in The Field of Philippine-Based SurgeriesDocument58 pagesNephrolithotomy To Nephrectomy: A Rare Case in The Field of Philippine-Based SurgeriesGiuseppe Carlo LaranangNo ratings yet
- Pathophysiology BPH Case StudyDocument3 pagesPathophysiology BPH Case Studyyhanne100% (24)
- Introduction of AnatomyDocument18 pagesIntroduction of Anatomyjames nginyangiNo ratings yet
- GIt HormonesDocument8 pagesGIt Hormonesriskyy1No ratings yet
- RBI Script 12Document4 pagesRBI Script 12Mary-Ann SanchezNo ratings yet
- Ana Lecture 1Document5 pagesAna Lecture 1Nureen Alizah OsbucanNo ratings yet
- Minnimally Invasive Surgical Management of Compound Odontoma at Floor Maxillary Sinus Associated With Impacted Caninus: A Case ReportDocument5 pagesMinnimally Invasive Surgical Management of Compound Odontoma at Floor Maxillary Sinus Associated With Impacted Caninus: A Case ReportRussi AshariNo ratings yet
- Word Roots and Combining Forms For AnatomyDocument7 pagesWord Roots and Combining Forms For AnatomyDavid HosamNo ratings yet
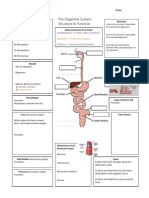
- The Digestive System Graphic OrganiserDocument1 pageThe Digestive System Graphic Organiserapi-350307578100% (1)
- ShockDocument29 pagesShockKoRnflakes100% (4)
- MY CLASS NOTES - BIOLOGY Circulatory SystemDocument3 pagesMY CLASS NOTES - BIOLOGY Circulatory SystemJjongNo ratings yet
- Chapter 8 - Transport in MammalsDocument119 pagesChapter 8 - Transport in Mammalsapi-3728508100% (1)
- 1st Year Histology, Id Points by DR RoomiDocument5 pages1st Year Histology, Id Points by DR RoomiMudassar Roomi100% (1)
- Human Biology Study GuideDocument12 pagesHuman Biology Study GuideDawn RobinNo ratings yet
- Histology of Digestive SystemDocument39 pagesHistology of Digestive Systemirakozehugue14No ratings yet
- Kuiz AnatomiDocument11 pagesKuiz AnatomiJackson JastariNo ratings yet
- Class II Deep BiteDocument12 pagesClass II Deep BitehabeebNo ratings yet
- Edgewise AppDocument27 pagesEdgewise AppReshamIrshadNo ratings yet
- Brain 1998 Perani 1841 52Document0 pagesBrain 1998 Perani 1841 52Alejandro Rodríguez NúñezNo ratings yet
- Buccal ObjectDocument46 pagesBuccal ObjectHeba DarwishNo ratings yet
- Dev of Hard & Soft PalateDocument94 pagesDev of Hard & Soft PalatepriyaNo ratings yet
- Dementia: College of NursingDocument47 pagesDementia: College of NursingIrish Jane Bayle CubilloNo ratings yet
- Anatomy and Physiology of PregnancyDocument20 pagesAnatomy and Physiology of PregnancyFeny JunaidyNo ratings yet