Professional Documents
Culture Documents
Welcome: By-Bhavesh Kumar B.SC (N) 2 Year
Uploaded by
MV Production0 ratings0% found this document useful (0 votes)
5 views28 pagesThis document provides information about leprosy (Hansen's disease), including its causes, signs and symptoms, classifications, global prevalence, treatment, nursing management, and prevention. Leprosy is caused by the bacterium Mycobacterium leprae and affects the skin and nerves. It is classified based on clinical presentation and bacterial load. Globally, leprosy prevalence has decreased but it remains a problem in some countries. Treatment involves multidrug therapy administered over 6 months to 1 year. Nursing focuses on managing symptoms, educating patients, and supporting rehabilitation. Prevention emphasizes avoiding contact with infectious cases and early detection and treatment to control spread.
Original Description:
Leprosy 2
Original Title
leprosy 2
Copyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document provides information about leprosy (Hansen's disease), including its causes, signs and symptoms, classifications, global prevalence, treatment, nursing management, and prevention. Leprosy is caused by the bacterium Mycobacterium leprae and affects the skin and nerves. It is classified based on clinical presentation and bacterial load. Globally, leprosy prevalence has decreased but it remains a problem in some countries. Treatment involves multidrug therapy administered over 6 months to 1 year. Nursing focuses on managing symptoms, educating patients, and supporting rehabilitation. Prevention emphasizes avoiding contact with infectious cases and early detection and treatment to control spread.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
5 views28 pagesWelcome: By-Bhavesh Kumar B.SC (N) 2 Year
Uploaded by
MV ProductionThis document provides information about leprosy (Hansen's disease), including its causes, signs and symptoms, classifications, global prevalence, treatment, nursing management, and prevention. Leprosy is caused by the bacterium Mycobacterium leprae and affects the skin and nerves. It is classified based on clinical presentation and bacterial load. Globally, leprosy prevalence has decreased but it remains a problem in some countries. Treatment involves multidrug therapy administered over 6 months to 1 year. Nursing focuses on managing symptoms, educating patients, and supporting rehabilitation. Prevention emphasizes avoiding contact with infectious cases and early detection and treatment to control spread.
Copyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 28
WELCOME
By- Bhavesh kumar
B.Sc (N) 2nd year
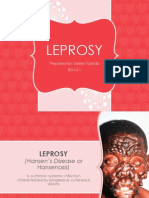
LEPROSY
INTRODUCTION
• Leprosy also known as HANSEN’s disease.
Leprosy is an infectious disease caused by
the acid- fast, rod-shaped bacteria
mycobacterium leprae, which was
discovered in 1873 by G.A. Hansen. It is
clinically characterised by hypopigmented
patches,partial or total loss of sensation
presence of thickened nerves and the
presence of acid-fast bacilli in skin
smears.
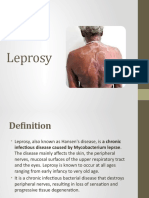
DEFINITION
• Leprosy is a chronic disabling disease
caused by mycobacterium leprae. The
disease affects mainly the peripheral
nerves. It also affects the
skin,muscles, eye, bones, testes and
internal organ.
CLASSIFICATION
• The indian classification which is the
official classification of the Hind Kusht
Nivaran Sangh is as below:
(a) Indeterminate type
(b) Tuberculoid type
(c) Lepromatus type
(d) Pure neuritic type
Cont…
• Cases have been further classified as:
(a) Multibacillary leprosy- this covers the
lepromatous leprosy and the borderline
cases, that is all infectious cases.
(b) Paucibacillary leprosy – This covers the
categories described as indeterminate,
tuberculoid and the pure neuritic types
of leprosy.
MAGNITUDE OF THE
PROBLEM
• WORLD-Leprosy is a major health and
socioeconomic problem because of long duration
of the disease.
• It has been estimated that there were about 0.2
million cases of leprosy in the world during the
year 2005 and global prevalence rate of leprosy
was below 1 case per 10,000 population. At the
end of 2006, leprosy was a public health problem
only in 6 countries most of the cases occur in
Asia, Africa and latin america.
Cont…..
• INDIA- leprosy is widely prevalent in India. The goal of
elimination of leprosy at the national level (i.e. prevalence
rate of less than 1 case per 10,000 population) has been
achieved in the month of December 2005 when prevalence
rate was 0.95 per 10,000 population.
• In the month of march 2006 it has further dropped down to
0.84 per 10,000 population with 0.95 Lack cases on record.
• In the march 2006, 26 states have achieved the status of
leprosy elimination and 9 states are with Prevalence rate of
1-2 case per 10,000 population. These states are Bihar,
Chhattisgarh, Jarkhand, Orrisa, UP, West Bengal,
Chandigarh, and Delhi.
leprosy control programme
• The government of India launched the national
leprosy control program in the year 1955 in close
collaboration with state government to control the
spread of the disease and modern treatment
facilities to leprosy patient. The program is
implemented through the establishment of leprosy
control units, survey education and treatment
centers, Urban leprosy centers, temporary
Hospitalization wards and reconstructive surgery
units, by the state governments.
Cont….
• At the central level the leprosy cell of the Director general
of health services is responsible for planning, supervision
and monitoring of the programe. The cell is under the
control of an assistant director general, who advice the
government on all anti –leprosy activities in the country. He
is under the overall supervision of the director general of
health services and ministry of health and family welfare.
• At the state level, the state leprosy officers are
responsible for organisation, supervision, guidance and
monitoring of all anti-leprosy activities. At the district
level, the district leprosy officer is responsible for the
implementation and supervision of the program.
LEPROSY ERADICTION
PROGRAME
In 1983, the national leprosy control
program was enhanced to national leprosy
eradication program on the
recommendation of working group on
leprosy. This was done because of
availability of highly effective treatment
for leprosy. The objective of eradication
program was to eliminate leprosy from the
country by the end of 20th century.
EPIDEMIOLOGICAL
FACTOR
1. AGENT- The causative agent is
Mycobacterium Leprae. The organism is
now grown in the foot pads of Mice and
in the Armadillo.
2. HOST –(a) AGE- Infection can take
place at any age. In endemic areas, the
disease is usually acquired in childhood.
Cont….
• (b) SEX- More commonly seen in male than in
female.
• (c) RACE- All human races are susceptible.
• 3. ENVIROMENT- (Climate) - More
common in warm and humid climate.
• SOCIAL FACTOR- poverty, poor
environmental surroundings,
overcrowding, low personal hygiene, use
of common clothing and linen.
MODE OF
TRANSMISSION
1. Contact transmission- Direct or indirect
contact between an infectious and
healthy person.
2. Droplet infection is very common
airborne disease play any part.
3. Other route –labra bacilli have been
found in human milk.
INCUBATION PERIOD- It is not exactly
known. Commonly between 2 to 5 year.
PATHOPHYSIOLOGY
CLINICAL FEATURE
• EARLY SIGNS – 1. hypopigmented patches on
the skin
• 2. diffuse thickening of the skin with a shiny
appearance.
• 3. loss of sweating or loss of hair over the skin
lesion.
• 4. loss of sentation to pain, touch and
temperature in the hands and feet.
Cont….
• 5. Nodules in the skin especially of the nose, chin and ears.
• 6. Thikening of earlobes.
• LATER DEFORMITIES-(a) Depression of the
bridge of nose
• (b) wrinkling of the facial skin.
• (c) Loss of eye brows.
• (d) Stiffness of joint of fingers.
• (e) SHORTENING AND LOSS OF FINGER &TOE
• (f) Blindness
DIAGNOSTIC TEST
1. Case history
2. Physical examination
3. Histamine test
4. Skin biopsy
5. Nasal smear
Cont….
• Histamine test- Intradermal Injection of 0.1ml of
histamine phosphate is injected intradermally
into hypopigmental patches or in areas of
anesthesia. in leprosy, flare response is lost.
• Nasal smears -These can be prepared from
early morning mucus material or an alternative is
to use an nasal mucosal scrapper. The smear is
immediately fixed by passing over a spirit lamp
and stained with ziehl-neelsen method, 5 percent
HCL is used for decolurisation.
TREATMENT
• Patient with paucibacillary leprosy are
given Rifampicin 600 mg once a month and
dapson 100 mg daily for six months.
• For multibacillary leprosy, rifampicin 600
mg once a month, dapsone 100 mg daily,
clofazimine 300 mg once a month, and 50
mg clofazimine daily are given for one
year.
NURSING
MANAGEMENT
NURSING DIAGNOSIS:
• Activity intolerance related to pain
• Self care deficit related to impaired vision.
• Disturbed body image related to change in
appearance.
• Acute pain related to injury to biological agents.
• Disturbed sleep pattern related to pain.
NURSING
MANAGEMENT
• Nurse will support the patient to cope with
disease condition.
• Nurse provide education related to disease
condition and its prevention.
• Take care of localized wound.
• Nurse should provide psychological support to the
patient because appearance of the skin may
affect the patient self –esteem.
• As a nurse co-operate to doctor plans to
elimination the disease condition and rehabilited
to the patient daily activity.
MEDICAL
MANAGEMENT
• 1981 – WHO proposes multidrug
therapy – combination of dapsone,
rifampicin and clofazimine.
COMPLICATION
• Permanent damage to the nerves in the fingers,
toes, hands and feet.
• This may affect a person ability to feel pain and
temperature in these areas of the body.
• Muscle weakness.
• Deformities and even the loss of fingers and toes.
• Untreated leprosy can also cause swelling and skin
sores and lesion that are more severe.
• Leprosy can also damage the kidney, which can
lead to kidney failure.
PREVENTION &
CONTROL
• The best way to prevent is to avoid contact with body fluids
and the rashes of people who have leprosy.
• CONTROL- (1) survey
• (2) early detection of cases
• (3) chemotherapy
• (4) selective isolation
• (5) prevention of contact
• (6) chemoprophylaxis
• (7) health education
HEALTH EDUCATION
• The community health nurse should teach the family about the
nature of the disease the need for strict home isolation of the
patient and the need for the regular treatment of the patient.
• Instruction should be given about keeping the eating and drinking,
utensil of the patient separeted, so also the clothes towels and
other linen used by the patient keep seprated.
• Follow up of patient during and after completion of chemotherapy.
• Educate the client about her medicine to take regular medicine as
per doctor order.
• Ulcer or tissue damage can result, leading to skin infection and
disability.
• Proper footwear and injury prevention should be encouraged.
SUMMARY
THANK YOU
You might also like
- Handout CompilationDocument199 pagesHandout CompilationG Fab100% (2)
- Wonderlic Sample Test (50 Questions)Document28 pagesWonderlic Sample Test (50 Questions)Heather Chavez0% (2)
- Pangmalakasan NP1Document134 pagesPangmalakasan NP1MikEeAyanEsterasNo ratings yet
- Geetanjali Medical College and Hospital, Udaipur: Department of CommunitymedicineDocument44 pagesGeetanjali Medical College and Hospital, Udaipur: Department of CommunitymedicineKamlesh SharmaNo ratings yet
- Leprosy Prevention ProgramDocument48 pagesLeprosy Prevention Programlunaghilvin2026No ratings yet
- LeprosyDocument16 pagesLeprosyNipul MondolNo ratings yet
- Document From BenjaminfjodDocument21 pagesDocument From BenjaminfjodBenjamin VanlaltlansangaNo ratings yet
- LEPROSYDocument27 pagesLEPROSYMohan SrinivasNo ratings yet
- NLEP-Bsc NSG pt-IVDocument6 pagesNLEP-Bsc NSG pt-IVSree LathaNo ratings yet
- Communicable Diseases Kala Azar May 07Document4 pagesCommunicable Diseases Kala Azar May 07Niraj KumarNo ratings yet
- Leprosy 2023Document55 pagesLeprosy 2023Obatoye SeyiNo ratings yet
- Filariasis Control ProgramDocument3 pagesFilariasis Control ProgramCate LagradaNo ratings yet
- LeprosyDocument68 pagesLeprosyMamata Manandhar100% (2)
- Group 17-1Document80 pagesGroup 17-1Jake MillerNo ratings yet
- Lymphatic FilariasisDocument36 pagesLymphatic FilariasisSan MohapatraNo ratings yet
- Epidemiology of Lymphatic FilariasisDocument26 pagesEpidemiology of Lymphatic FilariasisvaishnaviNo ratings yet
- Neglected Tropical DiseasesDocument84 pagesNeglected Tropical DiseasesAbhinesh Kr JhaNo ratings yet
- Filariasis: By: Barrantes, Patrick and Garcia, Charina JaneDocument17 pagesFilariasis: By: Barrantes, Patrick and Garcia, Charina Janerhimineecat71No ratings yet
- Leprosy HansenÔÇÖs DiseaseDocument50 pagesLeprosy HansenÔÇÖs DiseaseRovaidKhanNo ratings yet
- LeprosyDocument32 pagesLeprosySiselle FajardoNo ratings yet
- LEPROSYDocument55 pagesLEPROSYGeraldine Marie SalvoNo ratings yet
- Communicable Diseases GR.8 HealthDocument40 pagesCommunicable Diseases GR.8 HealthAiza May RosasNo ratings yet
- LeprosyDocument45 pagesLeprosyrouhanbinrashidNo ratings yet
- Leprosy - Mumal BakliwalDocument13 pagesLeprosy - Mumal BakliwalAni SharmaNo ratings yet
- Common Communicable Diseases GR.8 Lesson 3RD QDocument54 pagesCommon Communicable Diseases GR.8 Lesson 3RD QAiza May RosasNo ratings yet
- Visceral Leishmaniasis in IndiaDocument27 pagesVisceral Leishmaniasis in IndiaNishant SrivastavaNo ratings yet
- PEMPHIGUSDocument20 pagesPEMPHIGUSAshish SNo ratings yet
- 03 Leprosy and BrucillosisDocument5 pages03 Leprosy and BrucillosisMaeen Gamal AlhadhramiNo ratings yet
- Epidemiology of TrachomaDocument46 pagesEpidemiology of TrachomaaanandhiNo ratings yet
- PediculosisDocument28 pagesPediculosisLucy PalmaNo ratings yet
- PCM 1Document9 pagesPCM 1alzysamNo ratings yet
- 2019TOPNOTCHERDocument27 pages2019TOPNOTCHERjimboyNo ratings yet
- DiseasesDocument36 pagesDiseasesKayla WeirNo ratings yet
- Soil Transmitted Helminthiasis IHCPDocument50 pagesSoil Transmitted Helminthiasis IHCPARACELI RAITNo ratings yet
- TB and Scabies Ni NikkaDocument5 pagesTB and Scabies Ni NikkaLouise OpinaNo ratings yet
- National Vector Borne Disease Control ProgrammeDocument100 pagesNational Vector Borne Disease Control ProgrammeThe ThemerNo ratings yet
- Leprosy: Communicable Diseases FactsheetDocument2 pagesLeprosy: Communicable Diseases FactsheetelisabethNo ratings yet
- Infectious Diseases and Rural Health Module Microbiology and ParasitologyDocument65 pagesInfectious Diseases and Rural Health Module Microbiology and ParasitologyDagnachew kasayeNo ratings yet
- MF3 - LeprosyDocument25 pagesMF3 - LeprosyAnnbe BarteNo ratings yet
- Soil Transmitted Helminthiasis CompressedDocument73 pagesSoil Transmitted Helminthiasis CompressedBbNo ratings yet
- Leptospirosis PresentationDocument7 pagesLeptospirosis PresentationCharmagne Joci EpantoNo ratings yet
- Leishmania SisDocument27 pagesLeishmania SisAdnanhaider 03049907445No ratings yet
- Communicable Diseases 2Document7 pagesCommunicable Diseases 2jeromejamora7No ratings yet
- Microbial ResearchDocument12 pagesMicrobial Researchharshit kumarNo ratings yet
- Guideline For Management of Scabies in Adults and ChildrenDocument20 pagesGuideline For Management of Scabies in Adults and ChildrenDharmaMaya ChandrahasNo ratings yet
- Acute Necrotizing Ulcerative Gingivitis: (ANUG)Document36 pagesAcute Necrotizing Ulcerative Gingivitis: (ANUG)Louis HutahaeanNo ratings yet
- Cholera: Alyssa P. BagaporoDocument39 pagesCholera: Alyssa P. BagaporoDimple BagaporoNo ratings yet
- MonkeypoxDocument8 pagesMonkeypoxTabarak BhuiyanNo ratings yet
- Communicable Diseases 1Document41 pagesCommunicable Diseases 1Dinah MwakapilaNo ratings yet
- Management of Scabies PDFDocument5 pagesManagement of Scabies PDFAfnindyas AtikaNo ratings yet
- Orofacial Complications of Non Surgical Cancer TherapyDocument59 pagesOrofacial Complications of Non Surgical Cancer TherapyKassim OboghenaNo ratings yet
- RabiesDocument50 pagesRabiesMichael John TahadlangitNo ratings yet
- FilariaDocument65 pagesFilarialunaghilvin2026No ratings yet
- Intro Neuroschistosomiasis 2Document4 pagesIntro Neuroschistosomiasis 2Haidee GervacioNo ratings yet
- Tuberculosis Synonyms: Mycobacterium Organisms Are Facultative Intracellular Pathogens, Gram PositiveDocument4 pagesTuberculosis Synonyms: Mycobacterium Organisms Are Facultative Intracellular Pathogens, Gram PositiveVenkatapradeepNo ratings yet
- Com App Leprosy Abortion E. Pregnancy 1Document91 pagesCom App Leprosy Abortion E. Pregnancy 1Leogalvez BedanoNo ratings yet
- Seminar On MumpsDocument40 pagesSeminar On Mumpssushmitabiswas052No ratings yet
- Theme: Human Health: Project Title: Infectious & Non Infectious DiseaseDocument15 pagesTheme: Human Health: Project Title: Infectious & Non Infectious DiseasemitrashinyNo ratings yet
- Leprosy Control Program: Vision: Mission: ObjectivesDocument5 pagesLeprosy Control Program: Vision: Mission: ObjectivesAngelica VillalonNo ratings yet
- LeprosyDocument49 pagesLeprosysumita85No ratings yet
- LEPROSYDocument7 pagesLEPROSYEzra Manalansan-Beltran BaulNo ratings yet
- Folliculitis, A Simple Guide To the Condition, Treatment And Related DiseasesFrom EverandFolliculitis, A Simple Guide To the Condition, Treatment And Related DiseasesNo ratings yet
- Fite - FaracoDocument8 pagesFite - Faracoirwan junNo ratings yet
- NCP - LeprosyDocument3 pagesNCP - LeprosyKevin DareNo ratings yet
- Leprosy: BY:-Sweta Upadhyay BPT 4 YearDocument29 pagesLeprosy: BY:-Sweta Upadhyay BPT 4 YearSweta upadhyayNo ratings yet
- Another ReflectionDocument2 pagesAnother ReflectionMaeve AguerroNo ratings yet
- Orthopedic Case Proformas-1Document19 pagesOrthopedic Case Proformas-1md maaz100% (1)
- Tropical DiseasesDocument44 pagesTropical DiseasesOsmanNo ratings yet
- Communicable DiseasesDocument176 pagesCommunicable DiseasesKimsha ConcepcionNo ratings yet
- John Bunyan (1628-1688) : The Captain of All These Men of Death'Document56 pagesJohn Bunyan (1628-1688) : The Captain of All These Men of Death'Johir ChowdhuryNo ratings yet
- Identification and Classification According To Bergy's Manual of Systemic Bacteriology 2Document46 pagesIdentification and Classification According To Bergy's Manual of Systemic Bacteriology 2Cezar Alexander GuevaraNo ratings yet
- National Leprosy Eradication ProgrammeDocument11 pagesNational Leprosy Eradication ProgrammeNikhil SinghalNo ratings yet
- Agape Counseling For A Cured Leprosy Patient Facing Discrimination in OfficeDocument11 pagesAgape Counseling For A Cured Leprosy Patient Facing Discrimination in OfficeVivek Ray100% (1)
- Solution Manual For Macroeconomics 3rd Edition David Miles Andrew Scott Francis BreedonDocument24 pagesSolution Manual For Macroeconomics 3rd Edition David Miles Andrew Scott Francis BreedonBonnieGoodmanxajb100% (42)
- Bacillary DysenteryDocument8 pagesBacillary DysenteryRijane Tabonoc OmlangNo ratings yet
- MycobacteriumDocument11 pagesMycobacteriumskNo ratings yet
- Foundations in Microbiology: TalaroDocument65 pagesFoundations in Microbiology: Talaromertx013No ratings yet
- Botany AssignmentDocument21 pagesBotany Assignmentabdul hadiNo ratings yet
- Integ CD TipsDocument2 pagesInteg CD TipsNia KayeNo ratings yet
- MICRO Classification of LeprosyDocument1 pageMICRO Classification of LeprosyherrerachaimNo ratings yet
- Draft OperationalGuidelines LCDCDocument84 pagesDraft OperationalGuidelines LCDCDian Muspitaloka HikmayatiNo ratings yet
- IAL Textbook of Leprosy - Hemanta Kumar Kar and Bhushan KumarDocument3 pagesIAL Textbook of Leprosy - Hemanta Kumar Kar and Bhushan KumarindraNo ratings yet
- Case Report: Supevisor: Dr. Irma Tarida Listiawati, SP - KK By: Alif Ramadhan, S.KedDocument22 pagesCase Report: Supevisor: Dr. Irma Tarida Listiawati, SP - KK By: Alif Ramadhan, S.Kedpang_paangNo ratings yet
- Beepedia Daily Current Affairs (Beepedia) 27th January 2024Document8 pagesBeepedia Daily Current Affairs (Beepedia) 27th January 2024pr354038No ratings yet
- Lorenzo v. Director of HealthDocument1 pageLorenzo v. Director of HealthYeyen M. EvoraNo ratings yet
- National Leprosy Eradication ProgrammeDocument9 pagesNational Leprosy Eradication ProgrammeRekha ChaudharyNo ratings yet
- Locally Endemic Diseases ControlhandoutDocument3 pagesLocally Endemic Diseases ControlhandoutEshiebel OrganistaNo ratings yet
- 7.29th April - AF and Endospore StainingDocument20 pages7.29th April - AF and Endospore StainingUmme RubabNo ratings yet