Professional Documents
Culture Documents
Benign Prostratic Hyperplasia
Uploaded by
preet kaur0 ratings0% found this document useful (0 votes)
38 views10 pagesThis document discusses benign prostatic hyperplasia (BPH), including its definition, causes, pathophysiology, clinical manifestations, diagnostic findings, management, and nursing care. BPH is the enlargement of the prostate gland due to increased epithelial cells and tissue. It is caused by factors like family history, age, diet, and hormone changes. Symptoms include problems with urinary flow and frequency. Diagnostic tests evaluate the prostate and urine. Management includes lifestyle changes, medications, and surgical procedures to relieve urinary obstruction. Nursing care focuses on urinary drainage and infection prevention after surgery.
Original Description:
Original Title
Benign prostratic Hyperplasia
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentThis document discusses benign prostatic hyperplasia (BPH), including its definition, causes, pathophysiology, clinical manifestations, diagnostic findings, management, and nursing care. BPH is the enlargement of the prostate gland due to increased epithelial cells and tissue. It is caused by factors like family history, age, diet, and hormone changes. Symptoms include problems with urinary flow and frequency. Diagnostic tests evaluate the prostate and urine. Management includes lifestyle changes, medications, and surgical procedures to relieve urinary obstruction. Nursing care focuses on urinary drainage and infection prevention after surgery.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
38 views10 pagesBenign Prostratic Hyperplasia
Uploaded by
preet kaurThis document discusses benign prostatic hyperplasia (BPH), including its definition, causes, pathophysiology, clinical manifestations, diagnostic findings, management, and nursing care. BPH is the enlargement of the prostate gland due to increased epithelial cells and tissue. It is caused by factors like family history, age, diet, and hormone changes. Symptoms include problems with urinary flow and frequency. Diagnostic tests evaluate the prostate and urine. Management includes lifestyle changes, medications, and surgical procedures to relieve urinary obstruction. Nursing care focuses on urinary drainage and infection prevention after surgery.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 10
By.
Ms Simranpreet kaur
M.Sc (N)
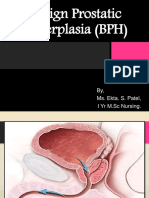
BENIGN PROSTRATIC HYPERPLASIA
DEFINITION
It is the enlargement of the prostate gland resulting
from an increase in the number of epithelial cells
and prostate tissue
CAUSES
Family history particularly involving first degree relatives,
environment history like exposure to environmental
allergens and diet history like consumption of increased
saturated fatty acids like butter, beef.
Age over 80 years associated with endocrine changes.
Increased alcohol intake
Obesity
Excessive accumulation of dihydroxytestosterone
hormone
PATHOPHYSIOLOGY
Due to endocrine changes in ageing
Stimulation of estrogen and local growth hormone
Increased production of 5-α reductase
Conversion of testosterone to dihydroxytestosterone
Excessive accumulation of dihydroxytestosterone
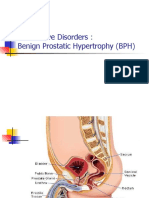
Enlargement of prostate tissue
Compression of the urethra
Obstruction of urinary outflow
Hydroureter & hydronephrosis
CLINICAL MANIFESTATIONS
Obstructive symptoms:
decrease in the force of urinary stream
difficulty in initiating voiding
intermittency (stopping and starting stream many times
while voiding)
dribbling at the end of urination
Irritative symptoms:
urinary frequency, urgency, dysuria
bladder pain, nocturia & incontinence.
DIAGNOSTIC FINDINGS
Digital rectal examination to evaluate the size, symmetry and
consistency of prostate gland.
Urine analysis to determine the presence of infection.
Prostate specific antigen test to rule out prostate cancer
Trans rectal ultrasound to detect the prostate size
Uroflowmetry to study the volume of urine expelled from the
bladder per second help in determining the extent of uretheral
blockage.
Post voidal residual urine volume to determine the degree of urine
outflow obstruction
Cystourethroscopy to allow visualisation of the urethra and bladder.
MANAGEMENT
Dietary modifications like decrease caeffine, artificial sweeteners, spicy
and alcoholic foods.
Avoid medications like decongesants and anticholinergics and restrict
evening fluid intake to reduce irritative symptoms.
Drug therapy :
5 α reductase inhibitors like finasteride & dutasteride to block the
conversion of testosterone to di-hydroxy testosterone.
α- adrenergic receptor blockers like alfuzosin, doxazosin, terazosin to
promote the smooth muscle relaxation in the prostate and facilitate
urinary outflow through the urethra.
herbal therapy like saw palmetto for management of urinary symptoms.
SURGICAL MANAGEMENT
Trans urethral resection of prostate(TURP):
This involves removal of prostate tissue using resectoscope inserted
through the urethra.
Trans urethral incision of prostate (TUIP): this involves making
transurethral slits or incisions in to the prostate tissue to relieve
obstruction.
Trans urethral microwave thermotherapy:
this involves a use of microwave radiating heat to produce
coagulative necrosis to the prostate.
Trans urethral needle ablation (TUNA): this uses a low wave
radiofrequency to heat the prostate causing necrosis.
CONTD…..
Open Prostatectomy: this is the surgery of choice
for men with large prostates which involves the
surgical excision of the prostate tissue.
Laser Prostatectomy: this procedure uses a laser
beam to cut or destroy the part of the prostate.
The destroyed prostate tissue gradually sloughs in
the urinary stream.
NURSING MANAGEMENT
Urinary drainage must be established with the catheter
before surgery
Bladder irrigation is done either intermittently or
continuously to remove clotted blood from the bladder.
Careful aseptic technique should be used when irrigating
the bladder to prevent possible infections
Activities that increase abdominal pressure like sitting or
standing for long periods and straining during defecation
should be avoided.
You might also like
- The Perfect Pancreatitis Diet Cookbook; The Complete Nutrition Guide To Managing And Healing Pancreatitis With Delectable And Nourishing Recipes;From EverandThe Perfect Pancreatitis Diet Cookbook; The Complete Nutrition Guide To Managing And Healing Pancreatitis With Delectable And Nourishing Recipes;No ratings yet
- The Ideal Pancreatitis Diet Cookbook; The Super Diet Guide To Suppres Inflammation, Control Pain And Manage Pancreatitis With Nutritious RecipesFrom EverandThe Ideal Pancreatitis Diet Cookbook; The Super Diet Guide To Suppres Inflammation, Control Pain And Manage Pancreatitis With Nutritious RecipesNo ratings yet
- benignprostatehyperplasia-190707164908 (1)Document50 pagesbenignprostatehyperplasia-190707164908 (1)jinsi georgeNo ratings yet
- Benign Prostate Hypertrophy Treatment OptionsDocument22 pagesBenign Prostate Hypertrophy Treatment Optionsjyoti kunduNo ratings yet
- Benign Prostatic HyperplasiaDocument9 pagesBenign Prostatic Hyperplasiaanju rachel joseNo ratings yet
- BPH DefinitionDocument5 pagesBPH DefinitionMadhu Sudhan PandeyaNo ratings yet
- Benign Prostate HyperthropyDocument3 pagesBenign Prostate Hyperthropyzmae23No ratings yet
- BPH 180828154943Document42 pagesBPH 180828154943Amandeep SinghNo ratings yet
- Benign Prostatic Hyperplasia (BPH)Document5 pagesBenign Prostatic Hyperplasia (BPH)Suneel Kumar PrajapatiNo ratings yet
- Wa0038.Document5 pagesWa0038.sham gowliNo ratings yet
- Benign Prostatic Hyperplasia (BPH) : Free Nursing LecturesDocument8 pagesBenign Prostatic Hyperplasia (BPH) : Free Nursing Lecturesmeshael_29No ratings yet
- Benign Prostatic HyperplasiaDocument4 pagesBenign Prostatic HyperplasiaAdelle Fortunato100% (2)
- Class Presentation ON BPH: Presented By: Ruchika Kaushal M.Sc. Nursing 1 YearDocument31 pagesClass Presentation ON BPH: Presented By: Ruchika Kaushal M.Sc. Nursing 1 YearRuchika KaushalNo ratings yet
- Benign Prostatic Hyperplasia (BPH) : By, Ms. Ekta. S. Patel, I Yr M.SC NursingDocument71 pagesBenign Prostatic Hyperplasia (BPH) : By, Ms. Ekta. S. Patel, I Yr M.SC NursingannisanabilaasNo ratings yet
- BPH & Urethral Stricture GuideDocument25 pagesBPH & Urethral Stricture Guidezaminazz100% (1)
- Benign Prostatic HyperplasiaDocument9 pagesBenign Prostatic Hyperplasiamardsz100% (1)
- Benign Prostatic Hypertrophy: Pathophysiology and EtiologyDocument4 pagesBenign Prostatic Hypertrophy: Pathophysiology and EtiologyErnestomalamionNo ratings yet
- BPH Symptoms, Risk Factors, and Treatment OptionsDocument60 pagesBPH Symptoms, Risk Factors, and Treatment OptionsMaddox EdeyajNo ratings yet
- Benign Prostatic HyperplasiaDocument19 pagesBenign Prostatic HyperplasiaEmmanuel MacheleleNo ratings yet
- Alpha Blockers & 5ARIs Relieve BPH SymptomsDocument73 pagesAlpha Blockers & 5ARIs Relieve BPH SymptomsSisay FentaNo ratings yet
- UtiDocument41 pagesUtiKetaks MooNo ratings yet
- Benign Prostate HyperplasiaDocument49 pagesBenign Prostate HyperplasiaRohani TaminNo ratings yet
- Trans Urethral Resection of The ProstateDocument8 pagesTrans Urethral Resection of The ProstateKath RecNo ratings yet
- Management of AROUDocument6 pagesManagement of AROUAung Ko HtetNo ratings yet
- Benigna Hiperplasia ProstatDocument23 pagesBenigna Hiperplasia ProstatShanti ArianiNo ratings yet
- Benign Prostatic HyperplasiaDocument6 pagesBenign Prostatic HyperplasiaHenny HansengNo ratings yet
- BphDocument23 pagesBphnobelaugustineNo ratings yet
- BPH and BOO Nursing CareDocument73 pagesBPH and BOO Nursing CareSwe Zin NaingNo ratings yet
- BENGIN PROSTATE HYPERPLASIA (BPH) GUIDEDocument31 pagesBENGIN PROSTATE HYPERPLASIA (BPH) GUIDENipul MondolNo ratings yet
- BPH Treatment and Surgical OptionsDocument25 pagesBPH Treatment and Surgical OptionsShreevidya GurunageshNo ratings yet
- Microsoft Office 2000Document3 pagesMicrosoft Office 2000Paillin EyeNo ratings yet
- Disorders of the Bladder and UrethraDocument48 pagesDisorders of the Bladder and Urethralytonia dampeerNo ratings yet
- BPHDocument20 pagesBPHHerly KakaNo ratings yet
- Obstructive Disorders: Benign Prostatic Hypertrophy (BPH)Document24 pagesObstructive Disorders: Benign Prostatic Hypertrophy (BPH)Pahlevie RezhaNo ratings yet
- Prostat: Dr. Delyuzar SP - PADocument66 pagesProstat: Dr. Delyuzar SP - PAJefry SNo ratings yet
- Benign Prostatic HyperplasiaDocument9 pagesBenign Prostatic HyperplasiaElizabeth Mapa100% (1)
- Benign Prostatic Hyperplasia CausesDocument4 pagesBenign Prostatic Hyperplasia CausesDae Young SeoNo ratings yet
- SL No Content NODocument12 pagesSL No Content NOPdianghunNo ratings yet
- Elderly Urinary Tract Disorders FixDocument36 pagesElderly Urinary Tract Disorders FixRyan Adi PutraNo ratings yet
- Unit-8: Benign Prostatic Hyperplasia (BPH)Document34 pagesUnit-8: Benign Prostatic Hyperplasia (BPH)urmila dewanNo ratings yet
- 1 BPHDocument27 pages1 BPHVikrant GholapNo ratings yet
- Cancer of The BladderDocument22 pagesCancer of The BladderKarl Kiw-isNo ratings yet
- BPH Case PresentationDocument15 pagesBPH Case PresentationxxandraNo ratings yet
- TURBT Procedure GuideDocument80 pagesTURBT Procedure GuideWindelyn GamaroNo ratings yet
- Urinary RetentionDocument24 pagesUrinary RetentionMuhammad Amri Kautsar100% (1)
- BPH PDFDocument13 pagesBPH PDFLorrine Mae ConcepcionNo ratings yet
- TURP Procedure Guide for Prostate RemovalDocument4 pagesTURP Procedure Guide for Prostate RemovalJylme Keziah Manzano DoronioNo ratings yet
- Transurethral Resection of The Prostate (TURP)Document4 pagesTransurethral Resection of The Prostate (TURP)Daniel Laurence Salazar ItableNo ratings yet
- Margaret Xaira R. Mercado RNDocument38 pagesMargaret Xaira R. Mercado RNxaira_rnNo ratings yet
- Joanalain C. Cortez, RN Clinical InstructorDocument179 pagesJoanalain C. Cortez, RN Clinical InstructorMark CadaNo ratings yet
- Interventions For Male Clients With Reproductive ProblemsDocument47 pagesInterventions For Male Clients With Reproductive Problemskimberlyrwarren8817No ratings yet
- Benign Prostatic HyperplasiaDocument3 pagesBenign Prostatic HyperplasiaRai HanahNo ratings yet
- Benign Prostatic HyperplasiaDocument28 pagesBenign Prostatic HyperplasiaFedrick MasatuNo ratings yet
- Fande Assignment: Saint Louis University School of NursingDocument6 pagesFande Assignment: Saint Louis University School of NursingMarion Liana DayritNo ratings yet
- BPH GuideDocument7 pagesBPH GuideSomesh GuptaNo ratings yet
- Urinary System DisordersDocument14 pagesUrinary System DisordersGideon P. CasasNo ratings yet
- Care for Urinary Problems & InfectionsDocument7 pagesCare for Urinary Problems & InfectionsJosephine NavarroNo ratings yet
- Pelvic Dysfunction in Men: Diagnosis and Treatment of Male Incontinence and Erectile DysfunctionFrom EverandPelvic Dysfunction in Men: Diagnosis and Treatment of Male Incontinence and Erectile DysfunctionNo ratings yet
- Hematuria, (Blood in Urine) A Simple Guide to The Condition, Related Diseases And Use in Diagnosis of DiseasesFrom EverandHematuria, (Blood in Urine) A Simple Guide to The Condition, Related Diseases And Use in Diagnosis of DiseasesRating: 5 out of 5 stars5/5 (2)
- The Ultimate Chronic Kidney Disease Diet Cookbook; The Complete Nutrition Guide To Restoring The Health Of Your Kidney With Meal Plan And Nourishing RecipesFrom EverandThe Ultimate Chronic Kidney Disease Diet Cookbook; The Complete Nutrition Guide To Restoring The Health Of Your Kidney With Meal Plan And Nourishing RecipesNo ratings yet
- Bone TumorsDocument12 pagesBone Tumorspreet kaurNo ratings yet
- Dermatitis: By. P. Dhilip KumarDocument8 pagesDermatitis: By. P. Dhilip Kumarpreet kaurNo ratings yet
- Alopecia: By. Mr. P. Dhilip KumarDocument9 pagesAlopecia: By. Mr. P. Dhilip Kumarpreet kaur100% (1)
- Bacterial Infections of SkinDocument13 pagesBacterial Infections of Skinpreet kaurNo ratings yet
- Alopecia: By. Mr. P. Dhilip KumarDocument9 pagesAlopecia: By. Mr. P. Dhilip Kumarpreet kaur100% (1)
- Amputation: by Mr. P. Dhilip KumarDocument16 pagesAmputation: by Mr. P. Dhilip Kumarpreet kaurNo ratings yet
- BURSITISDocument5 pagesBURSITISpreet kaurNo ratings yet
- Viral & Fungal Infections of SkinDocument15 pagesViral & Fungal Infections of Skinpreet kaurNo ratings yet
- Causes, Symptoms and Treatments of Anal Fissures and FistulasDocument12 pagesCauses, Symptoms and Treatments of Anal Fissures and Fistulaspreet kaurNo ratings yet
- Coronary Artery DiseaseDocument13 pagesCoronary Artery Diseasepreet kaurNo ratings yet
- Gi Tumors: By. P. Dhilip KumarDocument16 pagesGi Tumors: By. P. Dhilip Kumarpreet kaurNo ratings yet
- Congestive Heart FailureDocument13 pagesCongestive Heart Failurepreet kaurNo ratings yet
- DISASTER PREPAREDNESS: A GUIDE TO PLANNING AND RESPONSEDocument33 pagesDISASTER PREPAREDNESS: A GUIDE TO PLANNING AND RESPONSEpreet kaurNo ratings yet
- Chest Trauma and Thorocic InjuriesDocument17 pagesChest Trauma and Thorocic Injuriespreet kaurNo ratings yet
- Cardiomyopathy: By: P.Dhilip KumarDocument29 pagesCardiomyopathy: By: P.Dhilip Kumarpreet kaur100% (1)
- Congestive Heart FailureDocument13 pagesCongestive Heart Failurepreet kaurNo ratings yet
- Chest Trauma and Thorocic InjuriesDocument17 pagesChest Trauma and Thorocic Injuriespreet kaurNo ratings yet
- Coronary Artery DiseaseDocument13 pagesCoronary Artery Diseasepreet kaurNo ratings yet
- Shock: by Simranpreet KaurDocument10 pagesShock: by Simranpreet Kaurpreet kaurNo ratings yet
- Cardiomyopathy: By: P.Dhilip KumarDocument29 pagesCardiomyopathy: By: P.Dhilip Kumarpreet kaur100% (1)
- Angina By:P. Dhilip KumarDocument9 pagesAngina By:P. Dhilip Kumarpreet kaurNo ratings yet
- Angina By:P. Dhilip KumarDocument9 pagesAngina By:P. Dhilip Kumarpreet kaurNo ratings yet
- Causes and Management of VomitingDocument9 pagesCauses and Management of Vomitingpreet kaurNo ratings yet
- Syncope: By: P. Dhilip KumarDocument7 pagesSyncope: By: P. Dhilip Kumarpreet kaurNo ratings yet
- By Simranpreet KaurDocument10 pagesBy Simranpreet Kaurpreet kaurNo ratings yet
- Inflammation Definition and ResponsesDocument5 pagesInflammation Definition and Responsespreet kaurNo ratings yet
- Respiratory Obstruction: By: P. Dhilip KumarDocument6 pagesRespiratory Obstruction: By: P. Dhilip Kumarpreet kaurNo ratings yet
- Unconscious: By: Simranpreet KaurDocument12 pagesUnconscious: By: Simranpreet Kaurpreet kaurNo ratings yet
- Infections: by P. Dhilip KumarDocument10 pagesInfections: by P. Dhilip Kumarpreet kaurNo ratings yet
- MCQs on PharmacologyDocument101 pagesMCQs on PharmacologyMohammad Rashid88% (8)
- Ventilator Modes - WEANINGDocument3 pagesVentilator Modes - WEANINGAlaa OmarNo ratings yet
- Nelson Climate Change Plan UpdateDocument37 pagesNelson Climate Change Plan UpdateBillMetcalfeNo ratings yet
- Map Project Rubric 2018Document2 pagesMap Project Rubric 2018api-292774341No ratings yet
- Deutsche BankDocument4 pagesDeutsche BankMukesh KumarNo ratings yet
- Ch10 Stress in Simple WordsDocument7 pagesCh10 Stress in Simple Wordsmanaar munthirNo ratings yet
- USP FriabilityDocument2 pagesUSP Friabilityshdph100% (1)
- If Sentences Type 1 First Type Conditionals Grammar Drills - 119169Document2 pagesIf Sentences Type 1 First Type Conditionals Grammar Drills - 119169Ivanciu DanNo ratings yet
- TLM4ALL@1 Number System (EM)Document32 pagesTLM4ALL@1 Number System (EM)jkc collegeNo ratings yet
- Christos A. Ioannou & Dimitrios A. Ioannou, Greece: Victim of Excessive Austerity or of Severe "Dutch Disease"? June 2013Document26 pagesChristos A. Ioannou & Dimitrios A. Ioannou, Greece: Victim of Excessive Austerity or of Severe "Dutch Disease"? June 2013Christos A IoannouNo ratings yet
- 6 Construction of ShoeDocument33 pages6 Construction of ShoevedNo ratings yet
- Chapter 25 (10) Capital Investment Analysis: ObjectivesDocument40 pagesChapter 25 (10) Capital Investment Analysis: ObjectivesJames BarzoNo ratings yet
- Application of Gis in Electrical Distribution Network SystemDocument16 pagesApplication of Gis in Electrical Distribution Network SystemMelese Sefiw100% (1)
- Ed Brown CatalogDocument44 pagesEd Brown CatalogssnvetNo ratings yet
- Computer ViruesDocument19 pagesComputer ViruesMuhammad Adeel AnsariNo ratings yet
- Sand Compaction MethodDocument124 pagesSand Compaction Methodisaych33ze100% (1)
- Frequently Asked Questions About Ailunce HD1: Where Can Find HD1 Software & Firmware?Document5 pagesFrequently Asked Questions About Ailunce HD1: Where Can Find HD1 Software & Firmware?Eric Contra Color0% (1)
- Textbook of Heat Transfer Sukhatme S PDocument122 pagesTextbook of Heat Transfer Sukhatme S PSamer HouzaynNo ratings yet
- Community HelpersDocument3 pagesCommunity Helpersapi-252790280100% (1)
- Technical Information System Overview Prosafe-Com 3.00 Prosafe-ComDocument49 pagesTechnical Information System Overview Prosafe-Com 3.00 Prosafe-Comshekoofe danaNo ratings yet
- Measurement of Mass and Weight by NPLDocument34 pagesMeasurement of Mass and Weight by NPLN.PalaniappanNo ratings yet
- Dev OpsDocument28 pagesDev Opsdeb galangNo ratings yet
- Raiseyourvoice SFDocument26 pagesRaiseyourvoice SFAttila Engin100% (1)
- Science MELCsDocument42 pagesScience MELCsRanjell Allain TorresNo ratings yet
- Crashing Pert Networks: A Simulation ApproachDocument15 pagesCrashing Pert Networks: A Simulation ApproachRavindra BharathiNo ratings yet
- Plant Disease Detection Using Deep LearningDocument5 pagesPlant Disease Detection Using Deep LearningIJRASETPublicationsNo ratings yet
- Research on Comparisons between Sabah and Diesel CyclesDocument8 pagesResearch on Comparisons between Sabah and Diesel CyclesjorgeNo ratings yet
- 2.2valves, Alarm - Ul Product IqDocument1 page2.2valves, Alarm - Ul Product Iqbhima irabattiNo ratings yet
- Introduction To Drug DiscoveryDocument45 pagesIntroduction To Drug Discoveryachsanuddin100% (5)
- Twingo 3 & Clio 4Document10 pagesTwingo 3 & Clio 4Alexandre Le GrandNo ratings yet