Professional Documents
Culture Documents
Trigger Point Therapy
Uploaded by
Dina Umarella Pihang0 ratings0% found this document useful (0 votes)
73 views45 pagesTrigger Point Therapi and prevention
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentTrigger Point Therapi and prevention
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
73 views45 pagesTrigger Point Therapy
Uploaded by
Dina Umarella PihangTrigger Point Therapi and prevention
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 45
Trigger Point Therapy
Pembimbing: dr.Semuel A.Wagiu, Sp.S
By: Hapsah Faradina Umarella
2012-83-023
Introductions
1. How many here know what myofascial pain is?
2. How many know what a trigger point is ?
3. How many have experienced a tightness in your muscles causing you
to lose ROM and cause pain ?
Objectives
1. Provide facts and understand of myofascial pain syndrome (MPS)
and trigger points (TrPs)
2. Provide you with techniques to self treat MPS and TrPs
3. Provide guidelines for the prevention of MPS and TrPs
Facts
1. Currently reported to affect approximately 85% of the population at
some point during their lives
2. The mean prevalence of this condition among middle-aged adults
(30-60 years) is reported to be 37% in men and 65% in women
3. In the elderly (>65 years), in the prevalence reaches 85%
What is Myofascial
Combination of two Latin words:
“Myo” meaning muscle
“Fascia” meaning connective tissue surrounding the muscle
What is Fascia ?
1. Tough connective tissue that
lies just under the skin
2. It surrounds every organ,
muscle, bone, nerve and blood
vessel
3. Extends uninterrupted from
head to toe
What is a Trigger Point (TrP)
1. Hypersensitive areas
2. Palpated as a nodule within a tight band of muscle
3. Can cause pain, tingling, burning, weakness and loss of range of
motion (ROM)
Brief History
1. 1930s- Dr. Hans Langue used sclerometer to prove that tender areas in muscles are
50% harder than surrounding areas
2. 1940s- Janet Travell developed trigger point injection therapy and termed the
“tender areas” described by Dr.Hans “Trigger Points”
3. Travell’s therapy called for the injection of saline (a salt solution) and procaine
(also known as Novocaine, an anesthetic) into the trigger point
4. Travell maped what she termed the body’s trigger points and the manner in which
pain radiates to the rest of the body
5. Travell’s work came to national attention when she treated President John
F.Kennedy for his bak pain
Correlation Between TrP and MFP
1. MFP is an umbrella term that is given to TrPs and referred pain
2. TrPs are the TRUE source of soft tissue pain
3. MPS is more of a medical “garbage” term expressing the fact that the
person is experiencing broad soft tissue pain unrelated to any
possibly the results of multiple TrPs with referred pain
4. Tight MF and or tight, fatigue, strained muscles can develop active
TrPs therefore creating pain
Myofascial Pain Syndrome
a. Chronic or acute pain disorder
b. Initiated trough TrP’s, inducing referred pain into a specific body
region depending on the muscle involved
c. Typically occurs after a muscle has been contracted repetitively
d. Untreated it can cause tightness, tenderness, stiffness, popping and
clicking, loss of ROM
The Trigger Point Complex
How are they formed ?
Increased neural input to muscles, macrotrauma, or repeated microtrauma Ca
release prolong muscle contraction depress circulation lack of O2 intake
ATP decreases muscles are unable to relax.
The Trigger Point Complex
Different Types of Trigger Points
The main types of trigger point are:
a. Active trigger points
b. Latent trigger points
Latent Trigger Point
Latent MTrPs are usually asymptomatic, do not cause pain during daily
activities, but are painful when given external stimulation, such as
palpation, and can be activated if muscles are tense, tired, or injured.
Active Trigger Point
Active myofascial trigger points
will cause pain, thereby preventing
maximal muscle lengthening,
muscle weakness, mediating local
twitch response when stimulated,
and causing referred pain in the
area of pain concerned.
Symptoms of Trigger Points
Active trigger point referral symptoms:
1. Pressing Pain
2. Stabbing
3. Burning
4. Referred Pain
5. Common reports of the headaches, dizziness
Referred Pain
“Pain that arises in a trigger point, but is felt at a distance, often entirely
remote from the source”
Referred Pain Patterns
Prevalent in the head, neck, shoulders, hips and low back
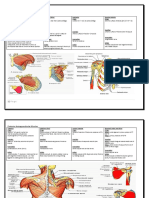
Referred Pain Guide
Sternocleidomastoid and Masseter
Referred Pain Guide
Trapezius
Referred Pain Guide
Pectorals
Referred Pain Guide
Quadratus lumborum
Referred Pain Guide
Piriformis
Referred Pain Guide
Glute maximus, medius and minimus
Referred Pain Guide
Tensor Fasciae Latae
Referred Pain Guide
Vastus Lateralis
Referred Pain Guide
Hamstrings
Sign and Symptoms
a. Tight muscle
b. Tender points in muscle
c. Palpable nodules
d. Decreased range of motion
e. Weakness without atrophy
f. As dull, achy, or deep pain the radiates and is non specific
g. Local spasm in affected muscle
Other Symptoms
A sensation of: A loss of:
a. Numbness a. Flexibility
b. Fatigue b. Range of movement (ROM)
c. Weakness c. Muscular power and strength
Diagnose
The typical findings complained of by myofascial pain patients include:
•The range of motion (ROM) of the servical spine is often limited and
painful
•The patient may describe as a lump or painful lump in the trapezius or
cervical paraspinal muscles.
•Massages can often help, as can provide a burning sensation to the
surface of the skin
•The patient's sleep may be disturbed by pain
Diagnose
•Turning the neck while driving is difficult
•The patient may describe pain radiating to the upper limb, accompanied
by numbness and tingling, making it difficult to distinguish from
radiculopai or peripheral nerve displacement.
•It is possible for the patient to feel dizzy or nauseous
•The patient experiences pain radiating in a characteristic pattern that
switches from trigger points.
Diagnose
Common findings on physical examination include:
1. Bad posture
2. Trigger points are often seen on m. trapezius, m. supraspinatus,
m.infraspinatus, m. rhomboids, and m. levator scapula
3. Tight muscle protrusions are palpable on the skeletal muscles
4. ROM in the cervical spine can be limited
Differential Diagnose
1. Sciatica
2. Migraine headaches
3. Fibromyalgia
4. Plantar fasciitis
5. Thoracic outlet syndrome
Predisposes
Treatment
1. Self treatmens: Strecthing, massage, heat or ice, foam roller, trigger
ball, strengthening
2. Medical treatments: Trigger point injection, acupuncture
3. Rehabilitation: Ultrasound, stretch and spray, therapeutic massage,
electrical stimulation
Myofascial Release
1. Technique used to help lengthen the muscle and fascial layers and
enable them to remain in the lengthened state
2. Goal is to decrease the amount of tension to the trigger points and
decrease their hypersensitivity
Pharmacologic Management of
Myofascial Pain/Trigger Points
a. NSAIDS (ibuprofen)
b. Muscle Relaxants (Cyclobenzaprine, Methocarbamol,
Baclofen,Tizanidine)
c. Injections: Saline, corticosteroids, lidocaine/bupivicaine
d. Topical Therapies: NSAIDS, capcasin, analgesics, methyl
salicylate/menthol cream
Trigger Point Injection
Set Up:
1. Lidocaine 1 % & Bupivicaine
2. Sterile gloves
3. Alcohol swab
4. 1.5 inch needle
5. Tape/plester
6. Have assistant to help you draw up
lidocaine/bupivacaine
Trigger Point Injection
Mark your patient
Trigger Point Injection
One technique
Post Procedure Care
1. Stretch
2. Heat
3. Will be sore for 2-3 days but effects can last several days to weeks
4. May have some bruising
Prevention
a. Ergonomics
b. Posture training
c. Exercise
d. Stress management
Prognosis
If patients with myofascial pain receive appropriate treatment (eg,
physical therapy, massage therapy, stretching techniques, injection at
trigger points), the prognosis is generally good. However, relapses can
be common
Take Home Points
1. Myofascial pain and TrPs are cause from a contraction of the muscle
fibers, such as repetative motions or injury
2. Self techniques that help enchance the treatment of MPS and TrPs
include stretching, strengthening, foam rolling and massage
3. Techniques involved in the prevention include ergonomic, postural
training, exercise and stress management
You might also like
- Gross B 2.17. FaceDocument5 pagesGross B 2.17. FaceShaira Aquino VerzosaNo ratings yet
- Spinal Stenosis And Pinched Nerve A Simple Guide to These conditionsFrom EverandSpinal Stenosis And Pinched Nerve A Simple Guide to These conditionsRating: 5 out of 5 stars5/5 (1)
- Managing LymphedemaDocument8 pagesManaging Lymphedemaوحش الصاعقهNo ratings yet
- What Is Shock Wave Therap 2Document7 pagesWhat Is Shock Wave Therap 2api-457017927No ratings yet
- Myofascial Release/ Therapeutic Massage TechniquesDocument21 pagesMyofascial Release/ Therapeutic Massage TechniquesadeshNo ratings yet
- ISMST GuidelinesDocument112 pagesISMST GuidelinesDhrubo TaraNo ratings yet
- Trigger Points Massage Therapy GuideDocument24 pagesTrigger Points Massage Therapy GuideTaina Avramescu100% (2)
- Medback MPSDocument8 pagesMedback MPSDavid TiongsonNo ratings yet
- Fibromyalgia and Myofascial PainDocument33 pagesFibromyalgia and Myofascial Painlichugojavier100% (1)
- TMD - نسخةDocument36 pagesTMD - نسخةZakria Al-HadadNo ratings yet
- Fibromyalgia Syndrome: Understanding Widespread Muscle PainDocument10 pagesFibromyalgia Syndrome: Understanding Widespread Muscle Painbujor2000ajaNo ratings yet
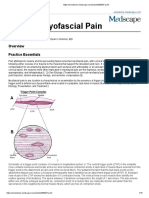
- Myofascial Pain SyndromeDocument4 pagesMyofascial Pain SyndromeHifnaDavesal'AyeshaNo ratings yet
- Sindrome MiofacialDocument13 pagesSindrome MiofacialAngie Paola RodriguezNo ratings yet
- 4 Common Musculoskeletal ProblemDocument54 pages4 Common Musculoskeletal ProblemMaria Lynne ParambitaNo ratings yet
- Myofascial Pain Syndrome inDocument17 pagesMyofascial Pain Syndrome inEdogawa RakhmanNo ratings yet
- Myofascial Release for Piriformis MyalgiaDocument14 pagesMyofascial Release for Piriformis MyalgiaApoorvNo ratings yet
- Fisiopatologia Do Ponto GatilhoDocument3 pagesFisiopatologia Do Ponto GatilhoAndréLuisVargasNo ratings yet
- Trigger Points Release Through Scalp AcupunctureDocument112 pagesTrigger Points Release Through Scalp AcupunctureTri Dewi Larasati80% (5)
- Self Myofascial ReleaseDocument22 pagesSelf Myofascial ReleaseMuhammad Fahmy100% (1)
- Trigger Point Homp. TehranDocument46 pagesTrigger Point Homp. TehranKasra Chehrazy100% (1)
- Pain Management GuideDocument85 pagesPain Management Guidemannsaab19No ratings yet
- MFS)Document47 pagesMFS)SanthiyaNo ratings yet
- Trigger Points - PhysiopediaDocument8 pagesTrigger Points - PhysiopediaJéssica ByronNo ratings yet
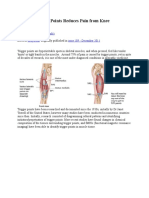
- Treating Trigger Points Reduces Pain From Knee OsteoarthritisDocument8 pagesTreating Trigger Points Reduces Pain From Knee OsteoarthritisAdi SuryawanNo ratings yet
- Myofascial Pain Syndrome ALICEDocument14 pagesMyofascial Pain Syndrome ALICEAlice dakshNo ratings yet
- Myofascial Pain SyndromeDocument4 pagesMyofascial Pain SyndromeDusan OrescaninNo ratings yet
- Promoting Comfort, Rest and SleepDocument59 pagesPromoting Comfort, Rest and Sleepkarendelarosa0627775% (4)
- MPDS-Multifactorial Etiology and Varied Pathophysiology: A ReviewDocument7 pagesMPDS-Multifactorial Etiology and Varied Pathophysiology: A Reviewsnehal jaiswalNo ratings yet
- Intrp PT4Document3 pagesIntrp PT4Floriza de LeonNo ratings yet
- Pain ManagementDocument49 pagesPain ManagementQasim ChacharNo ratings yet
- Exam 3 Study Guide: Pain and Peripheral Vascular DiseaseDocument5 pagesExam 3 Study Guide: Pain and Peripheral Vascular DiseaseFarzanaAziziNo ratings yet
- NM20110200002 13838543Document7 pagesNM20110200002 13838543Roy AriadyNo ratings yet
- Pain and SurgeryDocument15 pagesPain and SurgeryXinn Xinn Vanzandt100% (1)
- Trigger Point TheoryDocument3 pagesTrigger Point Theoryarun_chhedaNo ratings yet
- Cyriax HandoutDocument43 pagesCyriax HandoutMeenakshiputraeashwarprasad MacherlaNo ratings yet
- Stephens Painful AwarenessDocument4 pagesStephens Painful Awarenessmax00haNo ratings yet
- Myofascial Pain Syndrome in The Pelvic FloorDocument31 pagesMyofascial Pain Syndrome in The Pelvic FlooralgomohsinNo ratings yet
- Pain Management BasicsDocument39 pagesPain Management Basicsjamilicius100% (1)
- Trigger PointsDocument4 pagesTrigger PointsMarlene CarstensNo ratings yet
- Understanding Nociceptors and Phantom Limb PainDocument4 pagesUnderstanding Nociceptors and Phantom Limb PainluisaNo ratings yet
- Manual Trigger Point Therapy and Dry Needling Top 30 MusclesDocument84 pagesManual Trigger Point Therapy and Dry Needling Top 30 MusclesManuela CormioNo ratings yet
- UntitledDocument43 pagesUntitledmsah820No ratings yet
- Herniated Nucleus PulposusDocument29 pagesHerniated Nucleus PulposusRussel JanoloNo ratings yet
- HandsOn Muscle TherapyDocument38 pagesHandsOn Muscle TherapyPhoenixRising61100% (2)
- MUSCULOSKELETAL PAINDocument20 pagesMUSCULOSKELETAL PAINFatima JamalNo ratings yet
- Positional Release HandoutDocument38 pagesPositional Release Handoutaishwarya desaiNo ratings yet
- Name: Adeleke kemiDocument15 pagesName: Adeleke kemiKemi AdelekeNo ratings yet
- Intervertebral Disc ProlapseDocument46 pagesIntervertebral Disc Prolapsehellosir8273No ratings yet
- TMJ Disorders - Part IIDocument49 pagesTMJ Disorders - Part IIJu JuNo ratings yet
- 305937-Print 111Document15 pages305937-Print 111Nurul PutriNo ratings yet
- Pain Management: Kim L. Paxton MSN, ANP, APRN-BC Bro. Jim O'Brien, OFM, Conv. R.N., M.S.N., O.C.NDocument69 pagesPain Management: Kim L. Paxton MSN, ANP, APRN-BC Bro. Jim O'Brien, OFM, Conv. R.N., M.S.N., O.C.NsmusquizNo ratings yet
- Pressure Pointer ManualDocument17 pagesPressure Pointer ManuallucymayNo ratings yet
- Management: Education Department KKCHDocument76 pagesManagement: Education Department KKCHJuliet PuaNo ratings yet
- HNPDocument7 pagesHNPLyka Mae Imbat - Pacnis100% (1)
- Concept of PainDocument98 pagesConcept of PainEnrico Carlo EstacioNo ratings yet
- Trigger Point Therapy First, What Is A Trigger Point?Document2 pagesTrigger Point Therapy First, What Is A Trigger Point?Stephanie HuntNo ratings yet
- The Therapeutics of Acupuncture and Moxibustion (Myofascial, Bi Syndrome, Lower Back, Waist Sprain, Sciatica) (1) - 1Document44 pagesThe Therapeutics of Acupuncture and Moxibustion (Myofascial, Bi Syndrome, Lower Back, Waist Sprain, Sciatica) (1) - 1clerise3No ratings yet
- Complex Regional Pain SyndromeDocument10 pagesComplex Regional Pain SyndromegeejeiNo ratings yet
- Histology of Cardiac MuscleDocument13 pagesHistology of Cardiac MuscleAslinNo ratings yet
- Facial AnatomyDocument4 pagesFacial AnatomyPaul926870% (10)
- Sample Muscular System WorksheetsDocument8 pagesSample Muscular System WorksheetsAbigailBarrionGutierrezNo ratings yet
- REGIO CAPITIS LATERAL RevDocument53 pagesREGIO CAPITIS LATERAL RevHana AdivaNo ratings yet
- Muscular SystemDocument88 pagesMuscular SystemLewis RamosNo ratings yet
- The Muscular System Anaphy LabDocument12 pagesThe Muscular System Anaphy LabHannah Grace CorveraNo ratings yet
- Diagnostic Criteria Examination Form PDFDocument2 pagesDiagnostic Criteria Examination Form PDFNor Nadia Zakaria50% (2)
- MuscleDocument23 pagesMuscleLaw Ngo LengNo ratings yet
- Multiple Choice QuestionsDocument4 pagesMultiple Choice Questionsapi-19916399No ratings yet
- Skeletal MuscleDocument98 pagesSkeletal MuscleMoon Moon100% (1)
- Meal Plan Based On Individual'S Job ShiftDocument4 pagesMeal Plan Based On Individual'S Job ShiftNikhil ManjrekarNo ratings yet
- Anatomi RegioDocument38 pagesAnatomi RegioSuryo SuwandithoNo ratings yet
- Bulking Up WorkoutDocument7 pagesBulking Up WorkoutP_leeNo ratings yet
- Elbow Approaches and AnatomyDocument5 pagesElbow Approaches and Anatomyhaitham alkhamaisehNo ratings yet
- True Muscle CalendarDocument3 pagesTrue Muscle CalendarasdfNo ratings yet
- Anatomy II LabDocument48 pagesAnatomy II LabAddicted Outaku اوتاكوNo ratings yet
- The Sliding Filament TheoryDocument4 pagesThe Sliding Filament TheoryJinno VeldadNo ratings yet
- Fascias of H&NDocument71 pagesFascias of H&NAditi RapriyaNo ratings yet
- Analec B3 Brachial PlexusDocument2 pagesAnalec B3 Brachial PlexusCaesar Anthony Dequito SamsonNo ratings yet
- Physiology05 Muscle CellDocument37 pagesPhysiology05 Muscle CellsmpoojasubashNo ratings yet
- Biophysics of Muscle ContractionDocument53 pagesBiophysics of Muscle ContractionMaitree UpadhayayNo ratings yet
- CPT7 Static Dynamic Posture Assessment TemplateDocument2 pagesCPT7 Static Dynamic Posture Assessment TemplateNazmul Islam100% (1)
- Muscle Innervation Chart IIDocument7 pagesMuscle Innervation Chart IIkimsue9448No ratings yet
- GaitDocument8 pagesGaitruch_pt75% (4)
- Muscle Origins and InsertionsDocument9 pagesMuscle Origins and Insertionsnoisytaost92% (12)
- Head and Neck Muscle IdentificationDocument3 pagesHead and Neck Muscle IdentificationPrincess Faniega SugatonNo ratings yet
- Analysis of MovementDocument18 pagesAnalysis of MovementEfren Jonicel Daguio Domingo50% (2)
- Pert 10 - Core Stability ExerciseDocument30 pagesPert 10 - Core Stability ExerciseAlfiya HasnaNo ratings yet
- The Anatomy of the Vertical Jump in BasketballDocument3 pagesThe Anatomy of the Vertical Jump in Basketballewer27No ratings yet
- Bedah 2 Dr. UswaDocument36 pagesBedah 2 Dr. UswaSiq Febri SmnjtkNo ratings yet