Professional Documents
Culture Documents
Hemorrhoid Externa Treatment Options
Uploaded by
Qara Syifa F0 ratings0% found this document useful (0 votes)
9 views25 pagesHemorrhoids are dilated veins in the hemorrhoidal plexus. External hemorrhoids occur outside the anal verge. Causes include chronic constipation, straining during bowel movements, pregnancy, obesity, low fiber diet, and venous reflux. Symptoms include painful masses, bleeding, and skin tags. Diagnosis involves history, exam, and sometimes anoscopy. Initial treatment is lifestyle changes like increased fiber and fluids. Topical treatments provide temporary relief. Surgeries like hemorrhoidectomy or stapled hemorrhoidopexy are considered for severe cases. Recurrence rates are 10-50% with conservative care versus 26% with surgery.
Original Description:
Original Title
HEMORRHOID EXTERNAL
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentHemorrhoids are dilated veins in the hemorrhoidal plexus. External hemorrhoids occur outside the anal verge. Causes include chronic constipation, straining during bowel movements, pregnancy, obesity, low fiber diet, and venous reflux. Symptoms include painful masses, bleeding, and skin tags. Diagnosis involves history, exam, and sometimes anoscopy. Initial treatment is lifestyle changes like increased fiber and fluids. Topical treatments provide temporary relief. Surgeries like hemorrhoidectomy or stapled hemorrhoidopexy are considered for severe cases. Recurrence rates are 10-50% with conservative care versus 26% with surgery.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
9 views25 pagesHemorrhoid Externa Treatment Options
Uploaded by
Qara Syifa FHemorrhoids are dilated veins in the hemorrhoidal plexus. External hemorrhoids occur outside the anal verge. Causes include chronic constipation, straining during bowel movements, pregnancy, obesity, low fiber diet, and venous reflux. Symptoms include painful masses, bleeding, and skin tags. Diagnosis involves history, exam, and sometimes anoscopy. Initial treatment is lifestyle changes like increased fiber and fluids. Topical treatments provide temporary relief. Surgeries like hemorrhoidectomy or stapled hemorrhoidopexy are considered for severe cases. Recurrence rates are 10-50% with conservative care versus 26% with surgery.
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 25
HEMORRHOID EXTERNA
Qara Syifa Fachrani
1610211039
DEFINISI
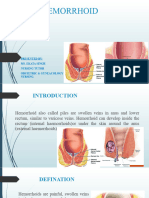
• Hemoroid adalah pelebaran vena di dalam
pleksus hemoroidalis yang tidak merupakan
keadaan patologik, hanya apabila hemoroid ini
menyebabkan keluhan atau peenyulit, maka
diperlukan tindakan.
• Hemoroid eksterna merupakan pelebaraan
dan penonjolan pleksus hemoroidalis inferior,
terdapat di sebelah distal garis mukokutan di
dalam jaringan di bawah epitel anus.
ETIOLOGI
• Penyebab hemoroid tidak diketahui, konstipasi kronis
dan mengejan saat defekasi mungkin penting.
• Mengejan menyebabkan pembesaran dan prolapsus
sekunder bantalan pembuluh darah hemoroidalis. Jika
mengejan terus menerus, pembuluh darah menjadi
berdilatasi secara progresif dan jaringan sub mukosa
kehilangan perlekatan normalnya dengan sfingter
internal di bawahnya, yang menyebabkan prolapsus
hemoroid yang klasik dan berdarah.
ETIOLOGI
• Faktor penyebab hemoroid yang lain yaitu :
– Kehamilan
– Obesitas
– Diet rendah serat
– Aliran balik venosa.
EPIDEMIOLOGI
• Hemorrhoid disease is the fourth leading outpatient
gastrointestinal diagnosis, accounting for~3.3 million
ambulatory care visits in the United States.
• Self-reported incidence of hemorrhoids in the United States is
10 million per year, corresponding to 4.4% of the population.
• Both genders report peak incidence from age 45 to 65 years.
• Notably, Caucasians are affected more frequently than African
Americans,
• Higher socioeconomic status is associated with increased
prevalence.
FAKTOR RISIKO
• Contributing factors for increased incidence of
symptomatic hemorrhoids include conditions
that elevate intra-abdominal pressure such as:
– Pregnancy
– Straining,
– Or those that weaken supporting tissue.
KLASIFIKASI
• Bentuk hemoroid biasa tapi letaknya distal
linea pectinea.
• Bentuk trombosis atau benjolan hemoroid
yang terjepit.
• Bentuk skin tags.
P
A
T
O
F
I
S
I
O
L
O
G
I
GEJALA KLINIS
• A total of 40% of individuals with hemorrhoids are
asymptomatic.
• For symptomatic hemorrhoids, there is great variance in the
constellation of symptoms. In addition, many other anorectal
pathologies such as:
• Anal fissure,
• Fistula,
• Pruritus,
• Condyloma,
• And even anal cancer are often labeled as “hemorrhoids” by
the layperson.
GEJALA KLINIS
• External hemorrhoids are more likely to be associated with
pain, due to activation of perianal innervations associated with
thrombosis.
• Patients typically describe a painful perianal mass that is tender
to palpation. This painful mass may be initially increasing in size
and severity over time.
• Bleeding can also occur if ulceration develops from necrosis of
the thrombosed hemorrhoid, and this blood tends to be darker
and more clotted than the bleeding from internal disease.
• Painless external skin tags often result from previous
edematous or thrombosed external hemorrhoids.
DIAGNOSIS
• A thorough history and physical examination is required to
help identify any possible alternative diagnosis,
• And the possibility of a more insidious cause of rectal
bleeding should always be considered.
• Patients may be examined in a prone-jackknife or left lateral
position.
• External inspection will reveal any thrombosed external
hemorrhoid, which often appears as a firm, purplish nodule
that is tender to palpation.
• Thrombosed hemorrhoids may also have ulcerations with
bloody drainage.
DIAGNOSIS
• Skin tags maybe signs not only of prior hemorrhoids but also
of fissure disease.
• Digital examination will exclude distal rectal mass and
anorectal abscess or fistula. Evaluation of sphincter integrity
during the digital examination is important to establish
baseline function, and is especially important in patients
who report incontinence as any future surgical intervention
may further worsen function.
• Lastly, anoscopy and rigid or flexible proctosigmoidoscopy
should be performed routinely to identify internal
hemorrhoids or fissures, and to rule out distal rectal masses.
DIAGNOSIS
• On histopathological examination, changes seen in the
anal cushions include :
– Abnormal venous dilatation,
– Vascular thrombosis,
– Degenerative process in the collagen fibers
– Fibroelastic tissues,
– Distortion and rupture of the anal subepithelial muscle.
• In severe cases, a prominent inflammatory reaction
involving the vascular wall and surrounding connective
tissue has been associated with mucosal ulceration,
ischemia, and thrombosis.
TATALAKSANA
• Lifestyle modifications should include:
– Increasing oral fluid intake,
– Reducing fat consumptions,
– Avoiding straining,
– Regular exercise.
• Diet recommendations should include:
– Increasing fiber intake, which decreases the shearing action of
passing hard stool.
– Fiber supplementation (7–20 g/d) reduced risk of persisting
symptoms and bleeding by 50%. However, fiber intake did not
improve symptoms of prolapse, pain, and itching.
TATALAKSANA
• For symptomatic control:
– Topical treatments containing various local anesthetics,
– Corticosteroids,
– Anti-inflammatory drugs are available.
• Notable topical drugs include 0.2% glyceryl trinitrate, which has been
studied to relieve grade I or II hemorrhoids with high resting anal canal
pressures, but is associated with headaches in 43% of patients.
• Patients also commonly self-medicate with Preparation-H (Pfizer
Incorporated, Kings Mountain, NC), a formulation of phenylephrine,
petroleum, mineral oil, and shark liver oil (vasoconstrictor and protectants),
which provides temporary relief in acute symptoms of hemorrhoids such as
bleeding and pain on defecation.
• Topic corticosteroids in cream or ointment formulations are commonly
prescribed, but their efficacy remains unproven.
TATALAKSANA
• Except in the case of thrombosis, both internal
and external hemorrhoids respond readily to
conservative medical therapy.
• However, when medical interventions fail to
resolve symptoms or if the extent of
hemorrhoid disease is severe, there are
various options for invasive procedures
available to the colorectal surgeon.
TATALAKSANA
• For patients who present with thrombosed external
hemorrhoids, surgical evaluation and intervention within 72
hours of thrombosis may result in significant relief, as pain and
edema peak at 48 hours.
• However, after 48 to 72 hours, organization of the thrombus
and amelioration of symptoms generally obviates the need for
surgical evacuation, which is consistent with the natural
history of hemorrhoidal thrombosis.
• After the initial 72-hour window, the pain typically plateaus
and slowly improves, at which point the pain from hemorrhoid
excision would exceed the pain from the thrombosis itself.
TATALAKSANA
• Hemorrhoidectomy
There are two major types of hemorrhoidectomy:
– Ferguson, or closed hemorrhoidectomy
– The Milligan–Morgan, or openhemorrhoidectomy.
The open hemorrhoidectomy is often the
preferred approach to surgically treat severe
acute gangrenous hemorrhoids where tissue
edema and necrosis preclude closure of the
mucosa.
TATALAKSANA
• Stapled Hemorrhoidopexy
An alternative to operative hemorrhoidectomy is
stapled hemorrhoidopexy, in which a stapling device is
used to resect and fixatethe internalhemorrhoid
tissuestothe rectalwall.
• Doppler-guided Hemorrhoidal Artery Ligation
This technique involves use of Doppler ultrasound to
identify and ligate the hemorrhoidal arteries. This is
also referred to as transanal hemorrhoidal
dearterialization (THD).
TATALAKSANA
PROGNOSIS
• Pada umumnya, kasus hemoroid dapat
sembuh dengan spontan ataupun dengan
pengobatan konservatif. Namun, tingkat
rekurensi pengobatan konservatif lebih tinggi
dari pada tindakan pembedahan, yaitu 10-50%
dalam 5 tahun, sedangkan pada tindakan
pembedahan diperkirakan 26%.
You might also like
- A Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisFrom EverandA Simple Guide to Blood in Stools, Related Diseases and Use in Disease DiagnosisRating: 3 out of 5 stars3/5 (1)
- 3Document5 pages3snrarasatiNo ratings yet
- HemorrhoidsDocument25 pagesHemorrhoidsAdoma SportsNo ratings yet
- RicoDocument62 pagesRicoCunCunAlAndraNo ratings yet
- Hemorrhoids Treatment GuideDocument35 pagesHemorrhoids Treatment GuiderizqinadiaNo ratings yet
- Presentation HemorroidDocument35 pagesPresentation HemorroidNuneng RinensaNo ratings yet
- Hemoroid JurnalDocument7 pagesHemoroid JurnalAsti HaryaniNo ratings yet
- HemerroidDocument24 pagesHemerroidVina WineNo ratings yet
- HEMOROIDDocument29 pagesHEMOROIDDanang Aryo PinujiNo ratings yet
- Hemorrhoids and Anal Fissures: Causes, Symptoms and TreatmentsDocument4 pagesHemorrhoids and Anal Fissures: Causes, Symptoms and TreatmentsSanthu SuNo ratings yet
- HemorrhoidDocument37 pagesHemorrhoidAbay WehNo ratings yet
- Hemorrhoid Treatment OptionsDocument30 pagesHemorrhoid Treatment OptionsRosa NurkholidNo ratings yet
- SeminarDocument32 pagesSeminarsachin84mittalNo ratings yet
- Gastro Week 4Document39 pagesGastro Week 4Reynaldi FernandesNo ratings yet
- Rectal Bleeding Causes GuideDocument35 pagesRectal Bleeding Causes GuidetharakaNo ratings yet
- Deep Venous Thrombosis: Farouq Muhammad 6-10-11Document59 pagesDeep Venous Thrombosis: Farouq Muhammad 6-10-11farouqmuhdNo ratings yet
- Manage Hemorrhoid ComplicationsDocument28 pagesManage Hemorrhoid ComplicationsWilliam GiovanniNo ratings yet
- Laporan Kasus - HemorrhoidsDocument41 pagesLaporan Kasus - HemorrhoidsMetyana CahyaningtyasNo ratings yet
- Pemicu 5 GIT DevinDocument131 pagesPemicu 5 GIT DevinDevin AlexanderNo ratings yet
- Polyp DKKDocument45 pagesPolyp DKKNadya Beatrix Yohanna NapitupuluNo ratings yet
- Hemorrhoids and Anal ProblemsDocument64 pagesHemorrhoids and Anal ProblemsAhmed Noureldin Ahmed100% (3)
- Lower Gastrointestinal Bleeding: Clinical Science SessionDocument48 pagesLower Gastrointestinal Bleeding: Clinical Science SessionNissaa IslamiatiNo ratings yet
- HemorrhoidDocument12 pagesHemorrhoidAdelia Maharani DNo ratings yet
- Anorectal Disorders Guide: Hemorrhoids, Fissures, Fistulas & MoreDocument41 pagesAnorectal Disorders Guide: Hemorrhoids, Fissures, Fistulas & MoreMuhammadNo ratings yet
- HemorrhoidsDocument9 pagesHemorrhoidsaix_santosNo ratings yet
- NO Particular Pages 1. 2 2. Problem Statement 3 3. Literature Review 4-6 4. Discussion 7-13 5. Conclusion 14 6. Reference List 15 7. Attachment 16-17Document17 pagesNO Particular Pages 1. 2 2. Problem Statement 3 3. Literature Review 4-6 4. Discussion 7-13 5. Conclusion 14 6. Reference List 15 7. Attachment 16-17Fardzli MatjakirNo ratings yet
- GI Bleeding 20-21Document38 pagesGI Bleeding 20-212859bathinaNo ratings yet
- Hemorrhoids: Dr. Muhammad Khadafi SPBDocument35 pagesHemorrhoids: Dr. Muhammad Khadafi SPBEka Retning Oktavanny0% (1)
- Male Genitalia Disorders LectureDocument37 pagesMale Genitalia Disorders LectureSisay FentaNo ratings yet
- Diagnosing and Treating Common Salivary Gland IssuesDocument45 pagesDiagnosing and Treating Common Salivary Gland Issuesmulle0608No ratings yet
- Hemorrhoids: Causes, Symptoms, TreatmentsDocument10 pagesHemorrhoids: Causes, Symptoms, Treatmentsshelly_shellyNo ratings yet
- Hemorrhoid Treatment and SymptomsDocument12 pagesHemorrhoid Treatment and SymptomsSasqia Trizolla0% (1)
- Deep Vein ThrombosisDocument42 pagesDeep Vein ThrombosisNsklm100% (7)
- Atul Sharma Uppergi Fcccm23Document47 pagesAtul Sharma Uppergi Fcccm23Atul SharmaNo ratings yet
- Hemorrhoid SurgeryDocument20 pagesHemorrhoid SurgerydiyahseptitiwulanNo ratings yet
- HEMORRHOIDDocument24 pagesHEMORRHOIDShriram SinghNo ratings yet
- Manage Upper GI Bleed in 33yo Hotel ReceptionistDocument42 pagesManage Upper GI Bleed in 33yo Hotel ReceptionistMuhammad Naveed AslamNo ratings yet
- Ugib &lgibDocument41 pagesUgib &lgibDawex IsraelNo ratings yet
- D231: Medical & Surgical Nursing Lecture On GASTROINTESTINAL (GI) BLEEDINGDocument37 pagesD231: Medical & Surgical Nursing Lecture On GASTROINTESTINAL (GI) BLEEDINGAnamul MasumNo ratings yet
- Hernia and Perianal ConditionsDocument58 pagesHernia and Perianal ConditionsSocial Media workingNo ratings yet
- Seminar on Hemorrhage and ShockDocument239 pagesSeminar on Hemorrhage and Shockparmeshori100% (1)
- Hemorhhoids CssDocument31 pagesHemorhhoids CssNaren RenNo ratings yet
- MSc Nursing Guide to HaemorrhageDocument39 pagesMSc Nursing Guide to HaemorrhageEsha KuttiNo ratings yet
- Anal FissureDocument45 pagesAnal FissureMinale MenberuNo ratings yet
- The Stomach and Duodenum: Dr. Elian EliasDocument48 pagesThe Stomach and Duodenum: Dr. Elian EliasmodarNo ratings yet
- Hemorrhoids, ParaproctitisDocument56 pagesHemorrhoids, ParaproctitisСандагсүрэн СандагдоржNo ratings yet
- Hemorrhoids: What Are Hemorrhoids? What Are The Symptoms of Hemorrhoids?Document6 pagesHemorrhoids: What Are Hemorrhoids? What Are The Symptoms of Hemorrhoids?Devina NugrohoNo ratings yet
- Anorectal Disorders, Haemorrhoids, Fissure, FistulaDocument74 pagesAnorectal Disorders, Haemorrhoids, Fissure, FistulaAbdulsalam DostNo ratings yet
- Gastrointestinal Bleeding: Prepared By: DR Gloria Lyimo Facilitated By: DR MbeleDocument43 pagesGastrointestinal Bleeding: Prepared By: DR Gloria Lyimo Facilitated By: DR MbeleSamar AhmadNo ratings yet
- Hemorrhoidectomy Case StudyDocument19 pagesHemorrhoidectomy Case StudyJoyJoy Tabada CalunsagNo ratings yet
- Internal HemmorhoidsDocument5 pagesInternal Hemmorhoids2netvelasquezNo ratings yet
- Clinical Clerk Seminar Series: Approach To Gi BleedsDocument11 pagesClinical Clerk Seminar Series: Approach To Gi BleedsAngel_Liboon_388No ratings yet
- Upper GI Bleeding Causes, Signs, Risk Factors & ManagementDocument46 pagesUpper GI Bleeding Causes, Signs, Risk Factors & ManagementRashed ShatnawiNo ratings yet
- Hemorrhoids 1Document19 pagesHemorrhoids 1susulemani3No ratings yet
- Meckels DiveritulumDocument30 pagesMeckels DiveritulumFrancis Adrian O. LadoresNo ratings yet
- Other No Trauma Urological Emergencies GinaDocument53 pagesOther No Trauma Urological Emergencies GinaRwabugili ChrisNo ratings yet
- DAFTAR PUSTAKA Seminar BHP VII Tutor C2Document1 pageDAFTAR PUSTAKA Seminar BHP VII Tutor C2Qara Syifa FNo ratings yet
- Plurals of NounsDocument3 pagesPlurals of NounsQara Syifa FNo ratings yet
- Black Memphis - PPTMONDocument26 pagesBlack Memphis - PPTMONJack Wanto SagendengNo ratings yet
- Nouns and QuantifiersDocument1 pageNouns and QuantifiersQara Syifa FNo ratings yet
- Presentation SubtitleDocument26 pagesPresentation SubtitleQara Syifa FNo ratings yet
- Black Memphis - PPTMONDocument26 pagesBlack Memphis - PPTMONJack Wanto SagendengNo ratings yet
- Abstract Purple - PPTMONDocument26 pagesAbstract Purple - PPTMONJack Wanto SagendengNo ratings yet
- Abstract MemphisDocument26 pagesAbstract MemphisJnafisahNo ratings yet
- Qara Syifa Fachrani - 2010221030 - Case Report Exercise-Induced Supraventricular Tachycardia in A 16-Year-Old Boy With Tricuspid RegurgitationDocument7 pagesQara Syifa Fachrani - 2010221030 - Case Report Exercise-Induced Supraventricular Tachycardia in A 16-Year-Old Boy With Tricuspid RegurgitationQara Syifa FNo ratings yet
- Abstract Background - PPTMONDocument26 pagesAbstract Background - PPTMONsquidawarkdNo ratings yet
- Qara Syifa Fachrani - 2010221030 - Description of Ventricular Arrhythmia After Taking Herbal Medicines in Middle-Aged CouplesDocument4 pagesQara Syifa Fachrani - 2010221030 - Description of Ventricular Arrhythmia After Taking Herbal Medicines in Middle-Aged CouplesQara Syifa FNo ratings yet
- Abstract Frame - PPTMONDocument26 pagesAbstract Frame - PPTMONJack Wanto SagendengNo ratings yet
- Abstract Business Corporate Free Powerpoint Presentation Templates - PPTMONDocument26 pagesAbstract Business Corporate Free Powerpoint Presentation Templates - PPTMONJack Wanto SagendengNo ratings yet
- Esophagitis Types, Causes, Symptoms, Diagnosis and TreatmentDocument32 pagesEsophagitis Types, Causes, Symptoms, Diagnosis and TreatmentQara Syifa FNo ratings yet
- Altitude Decompression Sickness & Trapped GasDocument16 pagesAltitude Decompression Sickness & Trapped GasQara Syifa FNo ratings yet
- Systemic Inflamatory Response Syndrome PathophysiologyDocument5 pagesSystemic Inflamatory Response Syndrome PathophysiologyQara Syifa FNo ratings yet
- Anxiety: Maudhira Anindita 16-036Document7 pagesAnxiety: Maudhira Anindita 16-036Qara Syifa FNo ratings yet
- Faktor Neurobiologi: Qara Syifa Fachrani 1610211039Document22 pagesFaktor Neurobiologi: Qara Syifa Fachrani 1610211039Qara Syifa FNo ratings yet
- Altitude Decompression Sickness & Trapped GasDocument16 pagesAltitude Decompression Sickness & Trapped GasQara Syifa FNo ratings yet
- Altitude Decompression Sickness & Trapped GasDocument16 pagesAltitude Decompression Sickness & Trapped GasQara Syifa FNo ratings yet
- Systemic Inflamatory Response Syndrome PathophysiologyDocument5 pagesSystemic Inflamatory Response Syndrome PathophysiologyQara Syifa FNo ratings yet
- Update On Congenital Nasolacrimal Duct ObstructionDocument7 pagesUpdate On Congenital Nasolacrimal Duct ObstructionLovely PoppyNo ratings yet
- Assessing The Relationship Between Anxiety Levels and Panic Attacks Among The Youth in ShimlaDocument52 pagesAssessing The Relationship Between Anxiety Levels and Panic Attacks Among The Youth in ShimlaAni RudhNo ratings yet
- ACLS (Notes) (Printable)Document2 pagesACLS (Notes) (Printable)mike_germain1172No ratings yet
- Ambulatory Blood Pressure JournalDocument7 pagesAmbulatory Blood Pressure JournalApt RiskaNo ratings yet
- Angiogenesis in CancerDocument4 pagesAngiogenesis in CanceranonymousNo ratings yet
- HAI Surveillance ChallengesDocument78 pagesHAI Surveillance ChallengesMichael EdmondNo ratings yet
- EndometriosisDocument45 pagesEndometriosisIngrid MiñanoNo ratings yet
- How Pets Can Improve Health and Well-BeingDocument3 pagesHow Pets Can Improve Health and Well-BeingThenaNo ratings yet
- IGCSE Excretion in Humans (Edited)Document59 pagesIGCSE Excretion in Humans (Edited)elizabethNo ratings yet
- Pathophysiology of Congestive Heart Failure NarrativeDocument4 pagesPathophysiology of Congestive Heart Failure NarrativeAlfred BucabucaNo ratings yet
- NAMA BARANG LIST AND PRICESDocument51 pagesNAMA BARANG LIST AND PRICESlevely rizkiNo ratings yet
- LAB RESULT RANGESDocument4 pagesLAB RESULT RANGESSila DarmanaNo ratings yet
- Effect of Intraoperative Dexmedetomidine On Post-Craniotomy PainDocument9 pagesEffect of Intraoperative Dexmedetomidine On Post-Craniotomy PainIva SantikaNo ratings yet
- Clinical Examinations Crib Sheet v7Document36 pagesClinical Examinations Crib Sheet v7aparish10100% (1)
- Herbal Concoctions Used in The Management of Some Women-Related Health Disorders in Ibadan, Southwestern NigeriaDocument9 pagesHerbal Concoctions Used in The Management of Some Women-Related Health Disorders in Ibadan, Southwestern NigeriaAbubakar MuhammadNo ratings yet
- First Generation Anti-Depressants: TCAs and MAOIsDocument54 pagesFirst Generation Anti-Depressants: TCAs and MAOIssangha_mitra_2No ratings yet
- The 10 Most Addictive Pain MedicationsDocument17 pagesThe 10 Most Addictive Pain MedicationslabendetNo ratings yet
- DiethylcarbamazineDocument8 pagesDiethylcarbamazinePrakob GikokNo ratings yet
- ZumbaDocument13 pagesZumbaamitsingh_singh041No ratings yet
- ME210 Gastrointestinal TimetableDocument6 pagesME210 Gastrointestinal TimetableEka Irina Akma KamaruddinNo ratings yet
- Bulbena CAbretalCNPS2016 PDFDocument11 pagesBulbena CAbretalCNPS2016 PDFLucero Corrales HuamánNo ratings yet
- Pengaruh Cognitive Behavioral Therapy (CBT) Terhadap Perubahan Kecemasan, Mekanisme Koping, Harga Diri Pada Pasien Gangguan Jiwa Dengan SkizofreniaDocument23 pagesPengaruh Cognitive Behavioral Therapy (CBT) Terhadap Perubahan Kecemasan, Mekanisme Koping, Harga Diri Pada Pasien Gangguan Jiwa Dengan Skizofreniaharyati soyNo ratings yet
- OBA Medical QuestionsDocument9 pagesOBA Medical QuestionsishafaraNo ratings yet
- Fight Against Corona: Know Where and How Much Beds Left in Ahmedabad Private HospitalDocument4 pagesFight Against Corona: Know Where and How Much Beds Left in Ahmedabad Private HospitalThe Voice Of GujaratNo ratings yet
- 3E - Agustin, Anne Julia - Group 1 - Case 7,8Document5 pages3E - Agustin, Anne Julia - Group 1 - Case 7,8Anne Julia AgustinNo ratings yet
- Hiv AidsDocument472 pagesHiv AidsDevendrapratapdpNo ratings yet
- Daftar PustakaDocument4 pagesDaftar PustakaDeasy Arindi PutriNo ratings yet
- CidoyDocument2 pagesCidoyElaine Fiona VillafuerteNo ratings yet
- Book Eyelid Tumor)Document288 pagesBook Eyelid Tumor)evelyn100% (1)
- Journal Heptojugular RefluxDocument5 pagesJournal Heptojugular RefluxFarhan RezaNo ratings yet