Professional Documents
Culture Documents
Mitral Stenosis
Uploaded by
sruthimeena68910 ratings0% found this document useful (0 votes)
66 views50 pagesEcho in Mitral stenosis by Sruthi Meenaxshi S R
Original Title
mitral stenosis
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentEcho in Mitral stenosis by Sruthi Meenaxshi S R
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
66 views50 pagesMitral Stenosis
Uploaded by
sruthimeena6891Echo in Mitral stenosis by Sruthi Meenaxshi S R
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 50
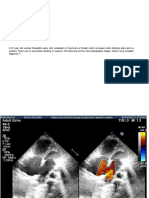
15 year old boy Rahul came with symptoms
dyspnea ,migratory joint pains, fever. His
echocardiogram showed the following features,
What is your probable diagnosis ?
Echocardiographic evaluation of
mitral stenosis
Dr.Sruthi Meenaxshi MBBS,MD ,PDF
• Mitral stenosis (MS) is a mechanical
obstruction in blood flow from the left atrium
to the left ventricle.
• The normal area of the mitral valve orifice is
about 4–6 cm2
• Impediment to the flow of blood into left
ventricle creating pressure gradient occurs
when the mitral valve area goes below 2 cm2
Etiology
• Mitral stenosis consists of 12% of all valvular heart disease in Euro
Heart Survey.
• Rheumatic heart disease (90 %)
• Infective endocarditis, ball valve thrombosis , atrial myoxma
• Mitral annular calcification
• Congenital malformation ( parachute mitral valve)
• Systemic lupus erythematosis
• Carcinoid heart disease
• Endomyocardial fibrosis
• Radiation-associated valve disease, including MS, is increasingly
recognized as late manifestation in survivors of Hodgkin’s lymphoma
• M-mode echocardiogram — The M-mode
examination is performed from the precordium
and guided from the 2D long and short axis views.
• Normally, the anterior mitral leaflet exhibits a
motion pattern that reflects the phasic nature of
ventricular filling and produces a familiar M-
shaped pattern
• The posterior leaflet moves in a nearly mirror
image "W" pattern with a smaller excursion
M mode mitral valve
2D of mitral stenosis
• The following parameters need to be assessed
about the valve morphology:
• Thickening
• Mobility
• Subvalvular fusion
• Commissural fusion
• Calcification.
Valvular thickening
• Normal mitral valve thickness is 2-4 mm
• Mitral leaflet thickness can be compared to
posterior aortic wall thickness, and the ratio gives
an objective assessment.
• Normally, the ratio of valve thickness/posterior
aortic wall thickness is < 1.4.
• 1.4 to2.0 mild Thickening
• 2 to 5 moderate thickening
• >5 severe thicknening
Mobility of valve
• (PLAX) and apical four‑chamber views
• Assessed by reid index by a line drawn from
posterior aortic root wall to the anterior mitral
leaflet tip
• H/L ratio (ab/xy ratio)
• <0.25 mild
• 0.25-0.44 moderate
• >0.45 severe
Reid index
Subvalvular apparatus
• Measuring chordal shortening
• Mild stenosis is if chordal length > 10 mm
• Severe disease chordal length < 10 mm
Calcification
• Bright echogenicity of the leaflets –
calcification
• Commisural calcification is absolute
contraindication for BMV
• Two-dimensional echocardiogram — The 2D
appearance of the normal mitral valve on TTE
depends somewhat upon the imaging plane
from which it is viewed.
• In the parasternal short axis plane, the valve
presents itself as an ovoid (fish mouth) orifice
• parasternal long axis and apical views, it
resembles clapping hands
• anterior hand longer and more mobile than
the posterior
• mitral valve leaflets are thin and translucent;
the rough attachment points of its chordae to
their free margins are thicker than their
smooth bellies. The chordae from each leaflet
connect to both papillary muscles.
• the valve appears homogeneous and thin, <4
mm in thickness.
What happens in mitral stenosis ?
• Anatomically, the commissural separation
between the anterior and posterior or mural
leaflets is
• subvalvular apparatus is altered by chordal
foreshortening
• Immobility of the posterior leaflet is a
common early finding with a "hockey
stick/knee bend" appearance to the anterior
mitral leaflet due to leaflet tethering.
• Doming of the anterior leaflet corresponds
temporally to the opening snap on
auscultation.
M Mode diagnosis for mitral stenosis
• early diastolic closure slope, the E-F slope,
produces an easily recognized pattern
• severity of obstruction, a slope of less than 10
mm/sec (normal is >60 mm/sec) during suspended
respiration means severe mitral stenosis
• Reversal of diastolic motion from the normal
pattern makes the M-mode of the posterior leaflet
one of the most valuable means of identifying
mitral stenosis
2 D evaluation of mitral stenosis
• dome or bulge into the ventricle throughout
diastole
• "knee bend" appearance on the precordial
long axis view
Doming of AML
2D Planimetry
• In the parasternal short axis plane, the opening
of the valve can be imaged just above the tips
of the papillary muscles.
• From this orientation, its maximum diastolic
opening area can be measured by direct
planimetry of the 2D image.
• A mitral valve area (MVA) of less than 1.5 cm2 is
considered severe, regardless of the method
used to calculate its size.
Doppler methods
• Doppler methods can measure the velocity of mitral inflow.
• In mitral stenosis, this velocity increases at rest from a normal value of less
than 1 m/sec to greater than 1.5 m/sec.
• The algorithm to convert Doppler velocity into pressure gradient is the
modified Bernoulli equation.
Peak gradient, in mmHg = 4 x peak velocity
• Thus, a peak velocity of 1 m/sec indicates a peak gradient of 4 mmHg; a
peak velocity of 2 m/sec indicates a peak gradient of 16 mmHg; 3 m/sec
indicates a peak gradient of 36 mmHg.[
• The mean transmitral gradient can be
measured by tracing the area-under-the-curve
of the mitral E and A waves obtained by
continuous wave Doppler.
• With severe mitral stenosis, the mean
transmitral gradient is >10 mmHg in sinus
rhythm at heart rates between 60 and 80 bpm
continous wave doppler in mitral valve tips ( apical 4 chamber view )
Calculate the pressure gradient
value > 10 is severe mitral stenosis
Calculation of mitral valve area
• Pressure half time method
• convert Doppler velocity into a pressure
gradient, the initial flow velocity is divided by
1.41 (square root of 2), because velocity bears
a second order relationship to pressure.
Empirically, a pressure half-time of 220 msec is
equivalent to a valve area of 1.0 cm2; therefore:
• MVA = 220 ÷ pressure half-time
Severity grading of mitral stenosis
Indirect methods to identify severity of mitral
stenosis
• degree of foreshortening of the chordae
tendineae
• leaflet calcification
• left atrial enlargement
• right ventricular and atrial dilatation
• measuring degree of tricuspid regurgitation
and pulmonary hypertension, as determined
by Doppler of tricuspid regurgitant jet.
• 2014 AHA/ACC guideline for valvular heart
disease defined severe mitral stenosis as
• MVA ≤1.5 cm2 (MVA ≤1.0 cm2 with very severe
MS) and diastolic pressure half-time ≥150 ms
• diastolic pressure half-time ≥220 ms with very
severe MS, along with severe left atrial
enlargement and pulmonary artery systolic
pressure >30 mmHg
Wilkins score
Mitral stenosis
• Assess valve doming / restriction / calcification
• 2D planimetry – Mitral valve area
• Assess Pressure gradient and TR jet velocity
associated Pulmonary artery hypertension
• Coexisting MR /LA thrombus
• Left ventricular and Right ventricular function
Assessment of mitral stenosis
THANKYOU
You might also like
- TheTruth About Food Grade Hydrogen Peroxide H2O2 by James Paul RoguskiDocument86 pagesTheTruth About Food Grade Hydrogen Peroxide H2O2 by James Paul RoguskiTheRazorsEdge80% (5)
- The Concise Human Body Book An Illustrated Guide To Its Structure, Function, and Disorders PDFDocument322 pagesThe Concise Human Body Book An Illustrated Guide To Its Structure, Function, and Disorders PDFBriyith Triana Rondon100% (4)
- Ventricular Tachycardia in The Ischemic HeartDocument57 pagesVentricular Tachycardia in The Ischemic Heartusfcards100% (3)
- Study of Pediatric Congenital Cardiac Malformations by EchocardiographyDocument23 pagesStudy of Pediatric Congenital Cardiac Malformations by EchocardiographyRana Abd AlmugeethNo ratings yet
- Echocardiography Board Review: 400 Multiple Choice Questions With DiscussionFrom EverandEchocardiography Board Review: 400 Multiple Choice Questions With DiscussionNo ratings yet
- HEARTDocument14 pagesHEARTNag Mallesh RaoNo ratings yet
- MapseDocument6 pagesMapseRaul GascueñaNo ratings yet
- Hepatic Vein FlowDocument14 pagesHepatic Vein FlowJORGENo ratings yet
- Aortic Root & Ascending Aortic Aneurysm Surgery OptionsTITLEDocument82 pagesAortic Root & Ascending Aortic Aneurysm Surgery OptionsTITLEMustafa KamalNo ratings yet
- Cardiomyopathy: Leonard Shaju Joisy AloorDocument34 pagesCardiomyopathy: Leonard Shaju Joisy AloorJoisy AloorNo ratings yet
- BradyarrthmiaDocument73 pagesBradyarrthmiaKuba ArebaNo ratings yet
- Left and Right Heart Cath Procedure OverviewDocument43 pagesLeft and Right Heart Cath Procedure OverviewIr Soebagoes100% (2)
- Mitral Valve Prolapse, A Simple Guide to The Condition, Treatment And Related ConditionsFrom EverandMitral Valve Prolapse, A Simple Guide to The Condition, Treatment And Related ConditionsNo ratings yet
- Aortic StenosisDocument3 pagesAortic StenosisMaxine BaraquiaNo ratings yet
- EXERCISE Stress Testing FOR HEARTDocument52 pagesEXERCISE Stress Testing FOR HEARTBenjamin GonzalezNo ratings yet
- Pericardial Diseases 3rd Yr BMTDocument38 pagesPericardial Diseases 3rd Yr BMT211941103014100% (1)
- 04 - Elements of EchocardiographyDocument56 pages04 - Elements of EchocardiographyMariana CabralNo ratings yet
- Atrial Septial DefectDocument22 pagesAtrial Septial DefectJulie MckinneyNo ratings yet
- Avnrt AvrtDocument21 pagesAvnrt AvrtRima Rovanne Wenas100% (1)
- Aortic RegurgitationDocument41 pagesAortic RegurgitationMedi PutraNo ratings yet
- M-Mode Echocardiography: John N. Hamaty D.O. SJHGDocument37 pagesM-Mode Echocardiography: John N. Hamaty D.O. SJHGhirsi200518No ratings yet
- Doppler Echocardiography: Dr.S.R.Sruthi Meenaxshi MBBS, MD, PDFDocument38 pagesDoppler Echocardiography: Dr.S.R.Sruthi Meenaxshi MBBS, MD, PDFsruthimeena6891No ratings yet
- 4th Quarter Exam P.EDocument3 pages4th Quarter Exam P.EKim Reyes Balen100% (3)
- Cardiac Output and Hemodynamic MeasurementDocument29 pagesCardiac Output and Hemodynamic Measurementdeepa100% (1)
- Dr. Alurkur's Book On Cardiology - 2Document85 pagesDr. Alurkur's Book On Cardiology - 2Bhattarai ShrinkhalaNo ratings yet
- Diseases of The AortaDocument48 pagesDiseases of The AortaYibeltal AssefaNo ratings yet
- Noakes 2000Document23 pagesNoakes 2000Nicolás Ayelef ParraguezNo ratings yet
- Dr. Firman Leksmono SP - JP Basic ECG Interpretation For StudentDocument54 pagesDr. Firman Leksmono SP - JP Basic ECG Interpretation For Studentadela_97line100% (2)
- ECG Master Class-3Document97 pagesECG Master Class-3Shohag ID CenterNo ratings yet
- Ngaji Arrythmia Cordis 3Document122 pagesNgaji Arrythmia Cordis 3Dhita Dwi NandaNo ratings yet
- Diastolic Dysfunction AssessmentDocument42 pagesDiastolic Dysfunction AssessmentMustajab MujtabaNo ratings yet
- MVR CabgDocument57 pagesMVR CabgRoshani sharmaNo ratings yet
- Left Ventricular Hypertrophy: Detection, Significance and TreatmentDocument27 pagesLeft Ventricular Hypertrophy: Detection, Significance and TreatmentKudor Szabadi ZoltánNo ratings yet
- ElectrocardiogramDocument52 pagesElectrocardiogramTuong HoangManhNo ratings yet
- Systolic Murmurs: DR Muhammed Aslam Junior Resident Pulmonary Medicine ACME PariyaramDocument39 pagesSystolic Murmurs: DR Muhammed Aslam Junior Resident Pulmonary Medicine ACME PariyaramPriyanshiSharmaNo ratings yet
- Diastolic DysfunctionDocument6 pagesDiastolic DysfunctionMarina SecureanuNo ratings yet
- Blood Gas HandbookDocument112 pagesBlood Gas HandbookNuno Silva100% (1)
- CARDIAC CYCLE New For StudentDocument54 pagesCARDIAC CYCLE New For StudentDavi DzikirianNo ratings yet
- DELNIDODocument32 pagesDELNIDOsarwansyahNo ratings yet
- Coronary Artery DiseaseDocument33 pagesCoronary Artery DiseaseAlma Rifa'Ana LiskaNo ratings yet
- Mitral RegurgitationDocument11 pagesMitral RegurgitationAbdur RaqibNo ratings yet
- Right Heart Catheterization, NicvdDocument17 pagesRight Heart Catheterization, NicvdNavojit ChowdhuryNo ratings yet
- Pacing Week PresentationsDocument54 pagesPacing Week PresentationsjoejenningsNo ratings yet
- Aortic Stenosis:: Updates in Diagnosis & ManagementDocument48 pagesAortic Stenosis:: Updates in Diagnosis & ManagementCuca PcelaNo ratings yet
- Perioperative Cardiovascular Evaluation For Noncardiac SurgeryDocument46 pagesPerioperative Cardiovascular Evaluation For Noncardiac SurgeryErinne DefrianiNo ratings yet
- Focal Atrial Tachycardia I: Clinical Features, DiagnosisDocument10 pagesFocal Atrial Tachycardia I: Clinical Features, Diagnosisapi-26166949No ratings yet
- American Heart Association Guide to Auscultating the HeartDocument42 pagesAmerican Heart Association Guide to Auscultating the HeartHananya ManroeNo ratings yet
- Pharmacotherapy of ShockDocument23 pagesPharmacotherapy of ShockIgor Stefanet100% (2)
- Ecg Pathology 02Document95 pagesEcg Pathology 02Andi MP Manurung100% (1)
- RV (Dys)function assessment by echocardiographyDocument52 pagesRV (Dys)function assessment by echocardiographyNag Mallesh RaoNo ratings yet
- 2021 ESC Preporuke Za Srčani Pejsing I Srčanu Resinhronizacionu TerapijuDocument68 pages2021 ESC Preporuke Za Srčani Pejsing I Srčanu Resinhronizacionu TerapijuDaria Lily MićanovićNo ratings yet
- Dyslipidemia MXDocument72 pagesDyslipidemia MXsruthimeena6891No ratings yet
- DR Thite DigestionDocument120 pagesDR Thite DigestionAnonymous wu6RXuNo ratings yet
- Tissue Doppler ImagingDocument37 pagesTissue Doppler ImagingSruthiNo ratings yet
- Echocardiographic Evaluation of Mitral RegurgitationDocument48 pagesEchocardiographic Evaluation of Mitral RegurgitationSruthiNo ratings yet
- Mitral StenosisDocument17 pagesMitral Stenosispriyanka bhowmikNo ratings yet
- L-R ShuntDocument88 pagesL-R ShuntnanohaniwiekoNo ratings yet
- Captopril Renography - Detect Renal Artery StenosisDocument3 pagesCaptopril Renography - Detect Renal Artery StenosisSri HariNo ratings yet
- Contrast EchocardiographyDocument54 pagesContrast EchocardiographySruthiNo ratings yet
- A Handbook On Clinical Echo CardiographyDocument71 pagesA Handbook On Clinical Echo Cardiographysri RamalakshmiNo ratings yet
- Management of Perioperative ArrhythmiasDocument51 pagesManagement of Perioperative ArrhythmiasAbhishek LonikarNo ratings yet
- Aortic Regurgitation CaseDocument38 pagesAortic Regurgitation CaseIka MagfirahNo ratings yet
- Vascular Acess Number 1Document45 pagesVascular Acess Number 1Paulo GalangNo ratings yet
- Procedure For Patent Ductus Arteriosus (PDA) Device ClosureDocument13 pagesProcedure For Patent Ductus Arteriosus (PDA) Device ClosurejaganjaggiNo ratings yet
- HUTTDocument25 pagesHUTTdrdj14100% (1)
- DR Sandeep - EISENMENGER SYNDROMEDocument81 pagesDR Sandeep - EISENMENGER SYNDROMEAlexandrescuNo ratings yet
- CCTGA Diagnosis, Treatment & OutcomesDocument94 pagesCCTGA Diagnosis, Treatment & OutcomesVik SharNo ratings yet
- Austin Journal of Clinical CardiologyDocument15 pagesAustin Journal of Clinical CardiologyAustin Publishing GroupNo ratings yet
- Left Ventricular Non-CompactionDocument20 pagesLeft Ventricular Non-CompactionlawlietNo ratings yet
- Atrial Septal DefectDocument77 pagesAtrial Septal Defectsruthimeena6891No ratings yet
- ASD Device ClosureDocument46 pagesASD Device Closuresruthimeena6891No ratings yet
- ASD Device ClosureDocument46 pagesASD Device Closuresruthimeena6891No ratings yet
- LV Systolic FunctionDocument36 pagesLV Systolic Functionsruthimeena6891No ratings yet
- Environmental Cleaning PDFDocument18 pagesEnvironmental Cleaning PDFsruthimeena6891No ratings yet
- Myocardial Infarction (Autosaved)Document46 pagesMyocardial Infarction (Autosaved)sruthimeena6891No ratings yet
- Conduction System of Heart: DR - Sruthi Meenaxshi PDF in VMCRHDocument27 pagesConduction System of Heart: DR - Sruthi Meenaxshi PDF in VMCRHsruthimeena6891No ratings yet
- 2.neurology History Part 2Document28 pages2.neurology History Part 2sruthimeena6891No ratings yet
- Whats New in GINA 2018 - V1.2Document17 pagesWhats New in GINA 2018 - V1.2sruthimeena6891No ratings yet
- Cauda-Conus SyndromesDocument28 pagesCauda-Conus Syndromessruthimeena6891No ratings yet
- Duplimuab Efficacy in AsthmaDocument37 pagesDuplimuab Efficacy in Asthmasruthimeena6891No ratings yet
- GINA 2017 Teaching Slide Set FullDocument181 pagesGINA 2017 Teaching Slide Set FullhaeranyNo ratings yet
- MerckDocument48 pagesMercksruthimeena6891No ratings yet
- Chapter 11 (11-23-04)Document61 pagesChapter 11 (11-23-04)sruthimeena6891No ratings yet
- Trace EvidenceDocument5 pagesTrace Evidencesruthimeena6891No ratings yet
- Forensic Medicine Toxicology Last Minute ReviewDocument102 pagesForensic Medicine Toxicology Last Minute Reviewsruthimeena6891No ratings yet
- Trace EvidenceDocument5 pagesTrace Evidencesruthimeena6891No ratings yet
- Anto PsychoticsDocument3 pagesAnto Psychoticssruthimeena6891No ratings yet
- Daftar Pustaka ImaDocument2 pagesDaftar Pustaka ImaDesrina PungkyNo ratings yet
- Handbook Language Course Teaching Methods For SenDocument49 pagesHandbook Language Course Teaching Methods For SensagagossardNo ratings yet
- ZabuDocument8 pagesZabuZabu CastilloNo ratings yet
- Pulse Rates and Target Heart Rates of Students and OthersDocument8 pagesPulse Rates and Target Heart Rates of Students and OthersMuhd MuqriNo ratings yet
- UNIT 3 (What Do You Feel)Document33 pagesUNIT 3 (What Do You Feel)oktika100% (1)
- Mitral Valve Disease: A Comprehensive ReviewDocument8 pagesMitral Valve Disease: A Comprehensive ReviewArthurNo ratings yet
- Rat ExperimentDocument7 pagesRat ExperimentKavithaa Sengalrayan0% (1)
- Blood pressure checklistDocument1 pageBlood pressure checklistbethuelNo ratings yet
- 2607 FullDocument94 pages2607 FullanindiawNo ratings yet
- Teorias de La ContraccionDocument24 pagesTeorias de La ContraccionCarlos Navarro alonsoNo ratings yet
- Case 3: Aortic StenosisDocument11 pagesCase 3: Aortic StenosisfmNo ratings yet
- Vii Science Student Study Material - Final New 1Document101 pagesVii Science Student Study Material - Final New 1YASHVI MODINo ratings yet
- Systemic Circulation NotesDocument4 pagesSystemic Circulation NotesMHAREY C. ARELLANONo ratings yet
- IV. Dizoxia PDFDocument11 pagesIV. Dizoxia PDFIvanes IgorNo ratings yet
- Case Based Panel DiscussionDocument49 pagesCase Based Panel DiscussiondrmohangNo ratings yet
- PericardiumDocument2 pagesPericardiumUDIT MANCHANDANo ratings yet
- Biology: Higher TierDocument32 pagesBiology: Higher TierT SolomonNo ratings yet
- June 2014 Question Paper 21 - 0 PDFDocument24 pagesJune 2014 Question Paper 21 - 0 PDFLast MadanhireNo ratings yet
- Grade 11 BiologyDocument50 pagesGrade 11 BiologyLax ReignNo ratings yet