Professional Documents
Culture Documents
Diuretics
Uploaded by
Chantal Carnes0 ratings0% found this document useful (0 votes)
8 views18 pagesCopyright
© © All Rights Reserved
Available Formats
PPT, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
8 views18 pagesDiuretics
Uploaded by
Chantal CarnesCopyright:
© All Rights Reserved
Available Formats
Download as PPT, PDF, TXT or read online from Scribd
You are on page 1of 18
Diuretics
Alison J. Montpetit, RN, PhD
NURS 366 Spring 2015
I. Overview
A. Kidney function
1. Maintain ECF volume and composition
2. Maintain acid - base balance
3. Excrete waste products and toxic substances
4. Nice review in Lehne r/t filtration, reabsorption,
secretion
B. Diuretic uses
1.Treatment of HTN
2.Mobilization of fluid
3.Prevent renal failure
C. Diuretic action
1. Most have same action
2. When solute reabsorption is blocked, tubular
osmotic pressure is increased and water is
therefore passively excreted also.
3. The amount of diuresis that occurs is directly
related to amount of Na and CL blockade.
4. The earlier the site of action in the nephron, the
greater the amount of Na and CL blockade.
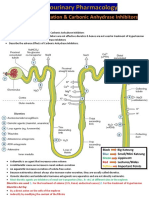
Osmotic diuretics Thiazide diuretics
Increases osmotic pressure so Similar to loops
H2O not filtered
Rule of thumb…the earlier in the K sparing
site of the nephron the greater Blocks
Loop diuretics aldosterone,
the diuretic effect Blocks NaCl
excretion of Na,
**dependent on renal function, etc. reabsorption
retention of K
II. Types of Diuretics
A. High ceiling (Loop) Diuretics
1. Action
a) Most effective diuretics
b) Blocks significant amounts of NaCL reabsorption
2. Pharmacology
a) Acts quickly (in 60 minutes for po, 5 minutes with
IV)
b) Lasts 2 (IV) to 5 hrs (po)
3. Uses
a) For conditions requiring significant fluid loss
b) Acute pulm edema with CHF
c) Edema of liver disease
d) Effective in renal disease since it can cause diuresis even
with low GFR and RBF
e) Used after other diuretics have failed
f) More IS better
4. ADRs
a) Dehydration
b) Hypotension
c) Electrolyte imbalances; ↓Na, ↓K, ↓Cl
d) Ototoxicity
e) Hyperuricemia - common side effect but may be
asymptomatic – can lead to gout, kidney stones
5. Drug Interactions
a) Digoxin
b) Lithium - with low Na levels lithium level will
increase
c) Ototoxic drugs
d) Potassium sparing diuretics
e) Antihypertensives
f) NSAIDs - decrease effect of diuretics
6. Drugs
a) Furosemide (Lasix)
b) Ethacrynic acid (Edecrin)
c) Bumetanide (Bumex)
B. Thiazide diuretics
1. Action
a) Similar to loops
b) Block absorption of Na, Cl in distal convoluted
tubule
c) Water moves osmotically with Na and Cl
d) Action dependent on adequate renal function
2. Pharmacology / Uses
a) Onset (po) 1-2 hrs, duration 6-12; some drugs are
slow release (24-48 hrs)
b) Used for HTN, mild to moderate CHF, mobilize
mild to moderate edema with liver impairment.
3. ADRs
a) Same as Loops
b) Hyperlipidemia - some evidence that these may increase total
cholesterol ( ↑LDL) - but over time may decrease it
c) Hypersensitivity
d) Not ototoxic
4. DI
a) Same as Loops
b) Not a problem with ototoxic drugs
c) Bile acid resins can bind the drug - decrease effect of diuretic
5. Drugs
a) 8 different types - all end in Athiazide: Hydrochlorothiazide
most common
b) All given only PO - except Chlorothiazide (IV also)
c) 4 related drugs – “thiazide – like” drugs
(1) Metolazone
(a) unlike other thiazides in that it does have
good activity in pts with renal failure (low
GFR, RBF)
(b) used with Lasix resistance
(c) give 30 minutes before Lasix to increase
effect of Lasix
(2) Chlorthalidone
(3) Indapamide
(4) Quinethazone
C. Potassium Sparing Diuretics
1. Spironolactone (Aldactone)
a) Action
(1) blocks actions of aldosterone in distal tubule and
collecting duct
(2) causes excretion of Na and retention of K
(3) only small amts of Na are reabsorbed here
(4) diuresis is minimal
(5) action is delayed -- up to 48 hrs
b) Uses
(1) HTN and edema
(2) Often used with thiazides or loops - to prevent
hypokalemia
(3) To block effects of aldosterone in pts with
hyperaldosteronism
(4) Secondary aldosteronism from CHF, hepatic
disease, nephrotic syndrome
(5) Spironolactone recently noted to have significant effect in
reducing morbidity and mortality in CHF due to aldosterone
blocking.
» Longer lasting aldosterone blocking than ACEI
» Aldosterone levels - 20 times greater in CHF due to
overproduction by the adrenal glands and reduced hepatic
aldosterone clearance.
» Drug is “cardioprotective” - aldosterone causes
myocardial and vascular fibrosis (remodeling) and direct
vascular damage – this drug reduces these adverse actions
» Should be used with ACEI and diurectics (and maybe
Digoxin) in CHF
c) ADRs
(1) Hyperkalemia
(2) Endocrine effects - menstrual irregularity,
impotence, deepening of voice, gynecomastia
2. Triamterene
a) Actions
(1) Direct inhibitor of exchange of Na and K in DCT
(2) Not through aldosterone mechanism
(3) Na excretion increased, K retained
(4) Acts more quickly
(5) Diuresis minimal
b) Uses
(1) Alone or with other diuretics to treat HTN
(2) Edema
(3) Augments other diuretics’ effect
c) ADRs
(1) Hyperkalemia
(2) N/V, leg cramps, dizziness - r/t hyperkalemia
3. Amiloride - similar to triamterene
D. Osmotic Diuretics
1. Drug
a) Mannitol (Osmitrol)
b) There are other osmotic diuretics, but only
mannitol is used for its diuretic action
c) It is used clinically
1. Action
a) Very different from other diuretics
b) Simple sugar that creates osmotic force in glomerulus
c) Is freely filtered at the glomerulus, has little
reabsorption, not metabolized, pharmacologically inert
d) Increases osmotic pressure of filtrate, water is not
reabsorbed and therefore excreted
e) Amount of diuresis r/t amount of drug
f) Little effect on excretion of electrolytes
G) Effective in reducing intracranial edema and therefore
ICP
3. Pharmacology
a) Does not cross GI endothelium
b) Given IV only
c) Does cross capillary endothelium, except in brain
4.ADRs
a) Edema
b) Fluid and electrolyte imbalances
5. Uses
a) Renal failure
b) Reduction of increased intracranial pressure
c) Reduction of intraocular pressure
Topics for Exam – Be sure you know
• Processes of filtration, reabsorption and secretion
• Identify changes in diagnostic tests associated with the diseases
covered; especially GFR, BUN, creatinine clearance
• Types of obstructions and renal stones
• Differentiate among type of infections (compare, contrast)
• All glomerulonephropathies, azotemia
• All the effects of uremia, on every system
• Causes of acute renal failure; examples of each and ATN;
nephrotic syndrome; definitions of pediatric terms/conditions
• All effects of chronic renal failure – on all systems
• Major disorders in children (causing acute and chronic disease);
differences in children
• Specifics of all diuretics – compare and contrast types
You might also like
- The Heart and Circulatory System and The Kidney 2Document28 pagesThe Heart and Circulatory System and The Kidney 2Izzuddin AhmadNo ratings yet
- Diuretic DrugsDocument62 pagesDiuretic DrugsAbdul WahabNo ratings yet
- Diuretics 1Document34 pagesDiuretics 1ياسمين مجديNo ratings yet
- Diuretics: BY-DR. Saurabh Kansal Dept. of Pharmacology Msy Medical College MeerutDocument33 pagesDiuretics: BY-DR. Saurabh Kansal Dept. of Pharmacology Msy Medical College MeerutPrakhar GoelNo ratings yet
- PDF DiureticsDocument20 pagesPDF DiureticsIhjas HabeebNo ratings yet
- Diuretics and Anti Diuretics: Year Iii Pharm.D Dr. V. ChitraDocument49 pagesDiuretics and Anti Diuretics: Year Iii Pharm.D Dr. V. ChitranikithaNo ratings yet
- Diuretics: By: Prof. A. AlhaiderDocument33 pagesDiuretics: By: Prof. A. AlhaiderNina KerafNo ratings yet
- Chapter 3 CVS & RenalDocument116 pagesChapter 3 CVS & RenalKIDUS YAREDNo ratings yet
- Diuretics: Sumolly Anak DavidDocument29 pagesDiuretics: Sumolly Anak Davidfarmasi_hmNo ratings yet
- The Renal SYSTEM: Supriya VeerallaDocument53 pagesThe Renal SYSTEM: Supriya VeerallaherbirdNo ratings yet
- DiureticsDocument27 pagesDiureticsAnonymous whcvnPBeQNo ratings yet
- Diuretics: Professor C. B. Choudhary Department of Pharmacology NMCTH, BiratnagarDocument52 pagesDiuretics: Professor C. B. Choudhary Department of Pharmacology NMCTH, BiratnagarKulgaurav RegmiNo ratings yet
- DiureticsDocument83 pagesDiureticsKarami BrutusNo ratings yet
- DrugsDocument116 pagesDrugsRyan FlahertyNo ratings yet
- Pharmacology of Diuretics: DR - Datten Bangun MSC, SPFKDocument46 pagesPharmacology of Diuretics: DR - Datten Bangun MSC, SPFKRizky Pramata Simamora 19000029No ratings yet
- 1 DiurethicsDocument8 pages1 DiurethicsMoataz TrabehNo ratings yet
- Renal Drugs Diuretics Agents: by Desalegn Chilo (B.Pharm, MSC)Document54 pagesRenal Drugs Diuretics Agents: by Desalegn Chilo (B.Pharm, MSC)Remedan TahaNo ratings yet
- Diuretics MergedDocument727 pagesDiuretics MergedRinkiNo ratings yet
- Diuretics: Diuretics Are Drugs That Increase The Volume of Urine FlowDocument35 pagesDiuretics: Diuretics Are Drugs That Increase The Volume of Urine FlowAmanuel Maru100% (1)
- Yuktiana Kharisma Bagian Farmakologi FK UNISBA 2017Document55 pagesYuktiana Kharisma Bagian Farmakologi FK UNISBA 2017Nurul PertiwiNo ratings yet
- Lecture 7 Cardiovascular System CvsDocument36 pagesLecture 7 Cardiovascular System CvsakramuddaulaNo ratings yet
- Classification of DiureticsDocument23 pagesClassification of DiureticsBeryl MarshallNo ratings yet
- Ph'cology of Diuretics (RZH)Document48 pagesPh'cology of Diuretics (RZH)beby febyola siagianNo ratings yet
- Genitourinary System PharmaDocument32 pagesGenitourinary System PharmaMD SHEMIM HUSSAINNo ratings yet
- Diuretics AaupDocument25 pagesDiuretics AaupSabrina ShalhoutNo ratings yet
- Diuretics: Basic Pharmacology Block Pdnt/Pmed - PMSC/PPHR - 213Document19 pagesDiuretics: Basic Pharmacology Block Pdnt/Pmed - PMSC/PPHR - 213JedoNo ratings yet
- c15 Diuretic AgentsDocument13 pagesc15 Diuretic AgentsmohammadNo ratings yet
- Diuretics: A. Overview of The Clinical Use of Diuretics B. Classification of DiureticsDocument22 pagesDiuretics: A. Overview of The Clinical Use of Diuretics B. Classification of DiureticsSteven GonzalesNo ratings yet
- Dr. Prajogo - PharmacologyDocument144 pagesDr. Prajogo - Pharmacologydelia rahmaNo ratings yet
- Lecture 9Document14 pagesLecture 9Aan KurniawanNo ratings yet
- Pharmacology Review Questions For QuizDocument14 pagesPharmacology Review Questions For QuizusedforfunplocNo ratings yet
- Beige Brown Vintage Group Project Presentation - 20230922 - 184226 - 0000Document25 pagesBeige Brown Vintage Group Project Presentation - 20230922 - 184226 - 0000Mercurio AysonNo ratings yet
- DiuréticosDocument58 pagesDiuréticosMajuOrellanaNo ratings yet
- Diuretics 140628134114 Phpapp02Document45 pagesDiuretics 140628134114 Phpapp02P merugu100% (1)
- Vidconf Diuretic Antidiuretic 2014Document51 pagesVidconf Diuretic Antidiuretic 2014naltrisilvianNo ratings yet
- Diuretic Drugs Dr. DarmawanDocument54 pagesDiuretic Drugs Dr. DarmawanEdi KurniadiNo ratings yet
- Renal Drugs (2014)Document22 pagesRenal Drugs (2014)Mohammad Hazamyn Hazrul HamzahNo ratings yet
- Diuretics NewDocument21 pagesDiuretics NewPawan RajNo ratings yet
- Genitourinary PharmacologyDocument11 pagesGenitourinary PharmacologySadia YousafNo ratings yet
- Farmakoterapi Sistem RenalDocument89 pagesFarmakoterapi Sistem RenalNhovieNhowaaNo ratings yet
- LECTURE Renal DisordersDocument21 pagesLECTURE Renal DisordersAnnie Rose Dorothy MamingNo ratings yet
- DiureticsDocument31 pagesDiureticsRameez ShamounNo ratings yet
- DiureticsDocument61 pagesDiureticsJoyce WacukaNo ratings yet
- DiureticsDocument29 pagesDiureticsdeepak askarNo ratings yet
- DIURETICSDocument55 pagesDIURETICSRAVISHNo ratings yet
- Diuretics: Pranjal Wagh Master of Pharmacy (2021-2023) Poona College of PharmacyDocument39 pagesDiuretics: Pranjal Wagh Master of Pharmacy (2021-2023) Poona College of PharmacyPranjalNo ratings yet
- DiureticsDocument58 pagesDiureticsabenezergebrekirstosNo ratings yet
- Drugs Affecting Renal SystemDocument58 pagesDrugs Affecting Renal SystemDaniel OkakaNo ratings yet
- DiureticsDocument12 pagesDiureticslandita683No ratings yet
- Pharmacology I, Diuretics NK-modified 2Document32 pagesPharmacology I, Diuretics NK-modified 289c8g7bvvvNo ratings yet
- Chapter 18 DIURETICSDocument14 pagesChapter 18 DIURETICSAlexandra AlexaNo ratings yet
- Anti Hypertensive Drugs - DiureticsDocument49 pagesAnti Hypertensive Drugs - DiureticsApurba Sarker Apu100% (1)
- Cardiovascular For PharmacologDocument134 pagesCardiovascular For Pharmacologephremtigabie7No ratings yet
- Renal Note On DiureticsDocument12 pagesRenal Note On DiureticsLilian EdeniNo ratings yet
- Diuretics: DR Sindwa KanyimbaDocument43 pagesDiuretics: DR Sindwa Kanyimbaedward kaumbaNo ratings yet
- Drugs Affecting The Renal SystemDocument8 pagesDrugs Affecting The Renal SystemAmandaNo ratings yet
- CVS - DiureticsDocument8 pagesCVS - Diureticshlouis8No ratings yet
- Drugs Affecting Renal SystemDocument44 pagesDrugs Affecting Renal SystemRwapembe StephenNo ratings yet
- "Natriuresis": Prepared by Dr. Hala Zaqout 1Document89 pages"Natriuresis": Prepared by Dr. Hala Zaqout 1Ahmed FouadNo ratings yet
- Ascites, A Simple Guide To The Condition, Treatment And Related ConditionsFrom EverandAscites, A Simple Guide To The Condition, Treatment And Related ConditionsNo ratings yet
- Case Presentation On Parkinson'S Disease: Presented By: T.Avinash Vith Pharm D Y13PHD0721Document21 pagesCase Presentation On Parkinson'S Disease: Presented By: T.Avinash Vith Pharm D Y13PHD0721AVINASH TALAPALA100% (1)
- Wa0012.Document19 pagesWa0012.sg carNo ratings yet
- Encyclopedia of Traditional Chinese Medicines - Molecular Structures, Pharmacological Activities, Natural Sources and Applications - Vol. 3 - Isolated Compounds H-MDocument702 pagesEncyclopedia of Traditional Chinese Medicines - Molecular Structures, Pharmacological Activities, Natural Sources and Applications - Vol. 3 - Isolated Compounds H-MThaís Hélène100% (1)
- Medical CannabisDocument14 pagesMedical CannabisEnzo TimbolNo ratings yet
- 2 - Cannabis Intoxication Case SeriesDocument8 pages2 - Cannabis Intoxication Case SeriesPhelipe PessanhaNo ratings yet
- Service Manual Harman Kardon AVR-1500Document74 pagesService Manual Harman Kardon AVR-1500aliarroNo ratings yet
- MICROEMULSIONDocument18 pagesMICROEMULSIONteasha chakraborty100% (1)
- Nepafenac An Ophthalmic Nonsteroidal Antiinflammatory DrugDocument6 pagesNepafenac An Ophthalmic Nonsteroidal Antiinflammatory DrugLalo ZaraloNo ratings yet
- Guaranteed To Pass: Exam Tidbits in Easy To Digest, Bite Sized MorselsDocument2 pagesGuaranteed To Pass: Exam Tidbits in Easy To Digest, Bite Sized MorselsCarl LeeNo ratings yet
- Pcol MidtermsDocument13 pagesPcol MidtermsJoyce VillanuevaNo ratings yet
- Analgesic Effects of Eucalyptus Essential Oil in M PDFDocument8 pagesAnalgesic Effects of Eucalyptus Essential Oil in M PDFChibani ZinebNo ratings yet
- Sagas of The SolanaceaeDocument7 pagesSagas of The SolanaceaeEvangelinaUrdialesNo ratings yet
- Don Honorio Ventura State University College of Education Bachelor of Physical EducationDocument3 pagesDon Honorio Ventura State University College of Education Bachelor of Physical EducationPrinces YumulNo ratings yet
- Module 5 and 6-Alzheimer's Disease, ACSDocument28 pagesModule 5 and 6-Alzheimer's Disease, ACSAngelica DapitoNo ratings yet
- Dissertation Topics of PG Degree Mdms Submitted For The Academic Year 2018-19-2019 20 and 2020 21Document227 pagesDissertation Topics of PG Degree Mdms Submitted For The Academic Year 2018-19-2019 20 and 2020 21Asra QuadriNo ratings yet
- 2021 LactateDocument8 pages2021 LactateMiky DinuNo ratings yet
- Case Study OF Hypokalemia Periodic ParalysisDocument34 pagesCase Study OF Hypokalemia Periodic ParalysisVivian Montesena BreganzaNo ratings yet
- Generic DrugsDocument3 pagesGeneric DrugsDarshan RNo ratings yet
- Review: Antimicrobial Resistance in Hospitals: How Concerned Should We Be?Document8 pagesReview: Antimicrobial Resistance in Hospitals: How Concerned Should We Be?Victor GodwinNo ratings yet
- Listes Des Medicaments Sur Sites 0Document2 pagesListes Des Medicaments Sur Sites 0Esperant RivoNo ratings yet
- Heparin Sodium Injection, USP: RX Only DescriptionDocument29 pagesHeparin Sodium Injection, USP: RX Only DescriptionArchie TobiasNo ratings yet
- After Hours StocksDocument4 pagesAfter Hours StocksbillNo ratings yet
- Latihan Diskusi KasusDocument3 pagesLatihan Diskusi Kasusrani nurindahNo ratings yet
- Managing Pulmonary EmbolismDocument9 pagesManaging Pulmonary EmbolismBolívar IseaNo ratings yet
- OBAT Life Saving FixDocument2 pagesOBAT Life Saving FixDevi0% (1)
- UoP Patient Care PlanDocument11 pagesUoP Patient Care PlanJessica WurtzelNo ratings yet
- Risk Assesment Approaches For Carcinogenic Food Contaminants PDFDocument19 pagesRisk Assesment Approaches For Carcinogenic Food Contaminants PDFJulio A. Pacheco CastilloNo ratings yet
- Xarelto Tablet Salut Selaput 20 MG - Rivaroksaban - DKI1251602517C1 - 2020Document26 pagesXarelto Tablet Salut Selaput 20 MG - Rivaroksaban - DKI1251602517C1 - 2020Dimas RfNo ratings yet
- Pedia Drug StudyDocument11 pagesPedia Drug StudyPeetah PanNo ratings yet
- GPAT - 2021: PharmacognosyDocument35 pagesGPAT - 2021: PharmacognosyBashar AhmedNo ratings yet