Professional Documents
Culture Documents
Week 12 - Care of The Pediatric Client With Neurologic Disorder
Uploaded by
Jaja Manez0 ratings0% found this document useful (0 votes)
6 views66 pagesOriginal Title
Week-12_Care-of-the-pediatric-client-with-Neurologic-Disorder-converted.pptx
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
6 views66 pagesWeek 12 - Care of The Pediatric Client With Neurologic Disorder
Uploaded by
Jaja ManezCopyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 66
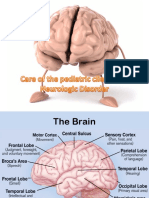
The Brain
• Complete assessment, evaluation
of mental & emotional status
– CN function, sensory function,
motor function, reflexes
• Know physical, psychomotor &
cognitive developmental milestones
• Mini assessment
– Bedside assessment: focus more on LOC,
pupillary response, motor function,
sensory function, reflexes, VS
• Assess eye opening, verbal &
motor responses
• Provides quick, standard account
of neuro status
• Pedia-version; pre-verbal child
• Each response receives numerical
value
• <7: comatose, severe neuro
damage
• 15: normal; 3: lowest possible score
(not always) – brain death
Eye opening (total 4
•points)
Spontaneous 4 points
• To voice 3
• To pain 2
• None 1
Verbal response (total points 5 points)
• Infants & young children Older
Children
• Fixes & follows
Appropriate words; smiles5 Oriented 5
• Consolable crying 4 Confused 4
• Persistently irritable 3 Inappropriate 3
• Restless, agitated 2 Incomprehensible 2
• None 1 None 1
Motor Response (total points 6
•points)
Obeys 6 points
• Localizes pain 5
• Withdraws 4
• Flexion 3
• Extension 2
• None 1
MOTOR FUNCTION MOTOR FUNCTION
• Good indicator of level • Mastery of gross &
fine motor skills
of consciousness related to myelination
• Can point to CNS & of NS
• Cephalo-caudal,
PNS damage proximodistal
development
• To evaluate muscle
strength
– Grip hand &
squeeze
– Push against palm
with foot
– Compare muscle
strngth on each side
PUPILLARY RESPONSE
• (+) Brain damage: lack
of changes in pupil size
in response to light
• Use flashlight/
penlight to assess
pupillary response at
bedside
• Minimize emotional trauma
– Tell child what to expect in simple, age appropriate term
(what he’ll see, hear & feel) & explain why
– Be honest about pain/ discomfort
• Tell child it’s ok to be afraid
– Reassure everyone involved to help him & keep him safe
• Allow child to see the equipment before test
• Encourage child to ask questions
• Allow parents to remain with child
• Give the child a “job” to do during the test (your job is to hold
very still) to give him sense of control
• After test, praise child for doing a good job
• Nurse should not expect cooperation from a young child
– May require sedation: IV pentobarbital/ oral chloral
hydrate (DOC for kids <2y/o)
Brain Scan Nursing consideration
• Measures gamma rays • Explain procedure to
produced by the radioisotope patient & family
material – Only discomfort is IV
• Identify focal brain lesions, puncture
pathologic conditions (tumor, – Contrast material is
infarction, mass, vascular
excreted within 6-24
lesions) involving cortex in
hours
patients with headache,
epilepsy, etc. • Encourage child to
• Test material accumulates in drink fluid after test to
areas where blood-brain aid in excretion of
barrier is defective isotope
• Distinguishes density of various
intracranial tissues &
structures
CT Scan Nursing consideration
• CNS disease suspected • Explain procedure:
cooperation is necessary ,
• 3-D image, identify tumor, must lie still during
infarcts, bleeding, hematoma, procedure
& provide information about • Show child picture of
ventricular system of brain machine
• May hear clicking noise as
scanner moves around his
head but machine won’t
touch him
• Child won’t be able to eat/
drink 4 hours before
scan: contrast dye may
cause nausea
• Assess for allergy to
iodinated dye/
shellfish
• Encourage to drink
fluids
Electroencephalogram
(EEG) Nursing consideration
• Graphic recording of electrical • Reassure he won’t feel
activity of brain anything
• Identify & evaluate patients • Child continues to eat/
with
drink
seizure
before test
• Identify tumor &
infarction, confirm brain • Child will not drink
death anything with caffeine on
morning of test because of
caffeine stimulating effect
• Patient needs to remain
still during test, movement
may cause interference
Lumbar Puncture
• Needle placed on
subarachnoid space of spinal
column
• Measure pressure of space
& obtain CSF for
examination & diagnosis
• L3-L4 or L4-L5
• Assist in diagnosis of brain
metastasis or spinal cord
neoplasm, meningitis,
cerebral hemorrhage,
encephalitis
Lumbar Puncture Nursing consideration
• Explain procedure
• Written informed consent
• Steps:
– Instruct child to empty his bladder & bowel before procedure
– Monitor VS during & after procedure (may sedate)
– Explain importance of remaining still throughout procedure:
side
lying knee chest position
– Gently hold child to prevent injury from unexpected/
involuntary movement
• LP positioning
– Lie on bedside at edge of bed, chin tucked to chest &
knees drawn up to abdomen
Lumbar Puncture Nursing consideration
• Make sure child’s spine curved & back
at edge of bed to widen space between
vertebra easing insertion of needle
• Place one hand behind his neck to
maintain position, place other hand
behind his knees & pull gently
• Hold child firmly to prevent
accidental needle displacement
• Monitor color & respiratory status –
infant’s
breathing may be interfered
Lumbar Puncture Nursing consideration
• Keep child on reclining position for 12 hours
to avoid discomfort of potential post
procedural spinal headache
• Encourage to drink lots of fluid with straw
to replace CSF removed
• Assess for numbnes, tingling, decrease
movement of extremities, pain at injection site,
drainage of blood/ CSF, inability to void
MRI Nursing considerations
• Non invasive • Explain procedure:
• Provides information no exposure to
about anatomy in radiation, may talk/
greater details than CT read to the child in
scan the imaging room
• No exposure to • Inform parents – child
ionizing radiation may be sedated, need
• For evaluation of to be motionless
headache or during procedure
neurologic signs of
CNS lesions • No food/
• Assess neck & back fluid
pain, lesions of bones & restriction
joints
• Occurs when the brain functions
abnormally, resulting in a change in
movement, attention, or level of
awareness
• 3% of all children have seizure <15 y/o,
half of which are febrile seizures .
• 1 in 100 children has epilepsy-recurring
seizures
• Disturbance in normal
brain function resulting
from abnormal electrical
discharge in the brain ,
which can cause
unconsciousness,
uncontrolled body
movement, changes in
behavior & sensation,
& changes in
autonomic system
• During a seizure, the
neurons in the brain
(nerve cells that produce
electrical discharges)
may
fire as many as 500 times
a second
• FEBRILE Seizure
– Occurs when a child contracts an illness
such as an ear infection, cold or chicken
pox accompanied by fever.
– Most common type seen in children
• PARTIAL Seizures
– Involve only a part of the brain and therefore only a part of
the body
– Major seizure happen on the first year of life
– Most affected: frontal, temporal, parietal lobes
1. Simple partial (Jacksonian) seizures
– Have a motor (movement) component that is located in
one portion of the body
– Average duration is 10-20 seconds
– Remains awake and alert; consciousness is not altered
(aura)
– May involve face, arms, extremities
– Movement abnormalities can “march” to other parts
of the
body as the seizure progresses
– Motor: change in position
– Sensory: hallucinations, autonomic (flushing,
tachycardia)
2. Complex partial seizure
– Similar, except that the child is not aware of
what is going on
– Repeat an activity, such as clapping
throughout the seizure
– With alteration of consciousness (no
memory of activity)
– Begins with aura (visual disturbances)
– Average 1-2 minutes
– After the seizure, child is disoriented known
as “postictal period”
– With EEG changes
• GENERALIZED Seizure
– Involve a much larger
portion of the brain
– Loss of consciousness:
initial clinical
manifestation
– No aura
– Occurs anytime day/
night
– Interval: minutes/
hours/ weeks/ years
– Grouped into 2
types:
• Convulsive (muscle
jerking)
• Nonconvulsive with
several subgroups
• Onset usually at 4 and 12 years of age
• More common in girls than in boys
• Usually cease at puberty
• Brief loss of consciousness
• Minimum or no alteration in muscle tone
• May go unrecognized because of little change in child’s
behavior
• Abrupt onset; suddenly develops 20 or more attacks daily
• Look like client is staring into space for a few seconds
• Doesn’t lead to physical injury
• Event often mistaken for inattentiveness, hypoglycemia,
stresses (emotional and physiologic), fatigue, or
sleeplessness
• Brief loss of consciousness
• Appear without warning or aura
• Usually last about 5 to 10 seconds
• Slight loss of muscle tone may cause
child to drop objects
• Ability to maintain postural control;
seldom falls
• Minor movements such as lip
smacking, twitching of eyelids or
face, slight hand movements
• Not accompanied by
incontinence
• Amnesia for episode
• May need to reorient self to previous
activity
• Brief shock-like jerks of a muscle
or group of muscles
• Awake and able to think clearly
• Don’t last more than a second or
two
• There can be just one, but
sometimes many will occur
within a short time
• Can be mistaken for tics,
tremors or clumsiness
• Usually involve the neck,
shoulders, upper arms and often
the face
• Most common and most dramatic
• Occur without warning
• Tonic phase
– Lasts approximately 10-20 seconds
• Clonic phase
– Lasts about 30 seconds but can vary from
only a few seconds to a half hour or
longer
– Violent jerking movements as the trunk and
extremities undergo rhythmic contraction
and relaxation
– May foam at the mouth
– May be incontinent of urine and feces
• Rhythmic jerking and
muscle spasm
• Difficulty breathing
and rolling eyes
• Sleepy and
confused
• Loss of awareness with
staring or blinking
• No convulsive
movements
• Sudden loss of
muscle tone in the
muscles that hold
the body and head
upright
• Occurs without
warning and usually
causes the person
to fall down
• Epilepsy
– Refers to a pattern of chronic seizures of any
type over a long period
– A condition characterized by recurrent 2 or >
unprovoked seizure in a day
– After a 5 to 10 years seizure free, without
medications, may considered to be resolved
– Derived from the greek word for “attack”
– Brain disorder in which clusters of nerve
cells, or
neurons, in the brain sometimes signal
abnormality
– Develop because of an abnormality in brain
wiring, an imbalance of nerve signaling chemicals
called neurotransmitters, or some combination of
these factors
Epilepsy
• Causes:
– Genetic factors
– Disorders (brain tumors, alcoholism, and
Alzheimer’s disease)
– Head injury
– Prenatal injury and Developmental
problem
– poisoning
Epilepsy Diagnostics
• First seizures, • EEG
febrile seizures, • Brain
nonepileptic scans
events, and
preeclampsia are
not associated with
epilepsy.
• V - Vascular (Stroke, embolic stroke)
• I - Infections (meningitis, encephalitis)
• T - Trauma (Head trauma)
• A - AV malformation
• M - Metabolic (hypoglycemia, hyponatremia,
hypoxia)
• I - Idiopathic
• N - Neoplasms (primary or secondaries)
• O - Others : sleep deprivation, drug overdose,
fever, eclampsia, hydrocephalus, Multiple
sclerosis
• Eyes roll upward
• Immediate loss of consciousness
• If standing, falls to floor or ground
• Stiffens in generalized, symmetric tonic
contraction of entire body
musculature
• Arms usually flexed
• Legs, head, and neck extended
• May utter a peculiar piercing cry
• Apneic, may become cyanotic
• Increased salivation and loss of swallowing
reflex
• Lumbar tap (spinal tap)
• CT scan
• MRI
• EEG
• Appropriate AED or combination of drugs
• Carbamazepines, phenytoin, valproic acids
(partial & / Generalized Sz)
• Ethosuximides/ valproic acids (absence
Sz)
• Single meds preferred to minimize adverse
effects
• (+) continuous Sz – multiple
anti- convulsants
• Other drugs: phenobarbital, diazepam,
lorazepam
• Assist client with KETOGENIC DIET (high fat, low
Carbohydrates, and low protein diet). Potential side
effects of the diet are constipation, weight loss, lethargy,
and kidney stones
• Observe the seizure episode and accurately document the
event
• Administer anti-epileptic drug
• Educate family and child, as appropriate, the purpose of
AEDs, expected response and action, potential side
effects, timing, dosage, route of administration, and how
to monitor effects
• Monitor side effects of AEDs and therapeutic levels
according to child’s growth, illness factors that affect
metabolism, and effects of drugs
• Stress importance of adherence to medication
regimen even if child has no evidence of seizure
activity
• Teach patient and family to identify and avoid
situations that are known to precipitate a seizure
(e.g. blinking lights, sleep deprivation, excess activity
or exercise, physical factor)
• Initiate seizure precautions in the hospital: pad side
rails of bed, crib, or wheelchair, keep bed relatively
free of objects
• Educate family to initiate seizure precautions at
home
SELF-CARE AT HOME
• Help the child to lie down
• Remove glasses or other harmful objects in the area
• Do not try to put anything in the child’s mouth. In
doing so, you may injure the child or yourself.
• After the seizure ends, place the child on one side
and stay with the child until fully awake. Observe the
child for breathing
• If the child has a fever, acetaminophen (such as
tylenol) may be given rectally
• Do not try to give food, liquid, or medications
by mouth to a child who has just had a seizure
PREVENTION
• Children who are known to have febrile
seizures should have their fevers well
controlled when sick
• To prevent further injury if a seizure does
occur
• A condition caused by an imbalance in the
production and absorption of CSF in the
ventricular system
• When production exceeds absorption, CSF
accumulates, usually under pressure, producing
dilation of the ventricles
• CSF volume: child = 60-100 ml
COMMUNICATING NONCOMMUNICATING
• Impaired absorption • Obstruction of CSF flow
within the subarachnoid within ventricular
space system
• Interference of CSF • Obstructive
within ventricular
system does not
occur
• Non-obstructive
• Congenital
hydrocephalus usually
results from defects
such as Chairi
malformation
s
• Acquired
hydrocephalus usually
results from space-
occupying lesions,
hemorrhage,
intracranial infections
or dormant
development defects
• Abnormal rate of head • Irritability and lethargy
growth with varying LOC
• Bulging fontanelle • Abnormal infantile
• Tense anterior fontanelle
reflexes
(often bulging and non-
• Possible cranial nerve
damage
pulsatile)
• Signs of increased
• Dilated scalp veins
ICP:
• Macewen’s sign (“cracked – Headache on
pot”) awakening with
improvement following
• Frontal bossing emesis
• Setting sun sign – Papilledema
• Sluggish and unequal – Strabismus
– Ataxia
pupils
– Irritability
• Level II ultrasonography of the fetus will
allow a prenatal diagnosis. (Transuterine
placement of ventriculoamniotic shunts
during late pregnancy is still being developed
as a treatment modality)
• CT scan (diagnose most cases postnatally)
• MRI (if complex lesion is suspected)
• Infections and malfunction (shunt)
• Subdural hematoma (too rapid reduction of
CSF)
• Peritonitis
• Abdominal abscess
• Perforation of organs
• Fistulas
• Hernias
• Ileus
Surgical Intervention
• VP shunt – remove CSF from
ventricles to peritoneal cavity
• VA shunt – to the right
atrium
• Ventriculopleural shunt – pleural
cavity
• Ventriculostomy (non-shunting
procedure)
• Surgical removal of obstruction
(if cause is removable such as
tumor/ hematoma
• DOC: Acetazolamide
• Preoperative care
– Assess head circumference, fontanelles, cranial
sutures, and LOC; check also for irritability, altered
feeding habits and a high-pitched cry
– Firmly support the head and neck when holding
the child
– Provide skin care for the head to prevent
breakdown
– Give small, frequent feedings to
decrease the risk
of vomiting
– Encourage parental-newborn bonding
• Postoperative care
– Assess for signs of increased ICP and check for the
ff: head circumference (daily), Anterior
fontanelle for size and fullness, and behavior
– Administer prescribed medications which may
include antibiotics to prevent infection and
analgesics for pain
– Provide shunt care
• Monitor for shunt infection and malfunction which may be
characterized by rapid onset of vomiting, severe headache,
irritability, lethargy, fever, redness along the shunt tract, and
fluid around the shunt valve
• Prevent infection (usually from staphylococcus epidermis or
aureus)
• Postoperative care
– Monitor for shunt overdrainage (headache,
dizziness and nausea)- may lead to slit ventricle
syndrome whereby the ventricle become
accustomed to a very small or slitlike
configuration, limiting the buffering ability to
increased ICP variations
• A group of disabilities caused by injury or insult
to the brain either before or during birth, or in
early infancy
• Most common permanent disability of
childhood
• Cerebral = refers to cerebrum; Palsy = refers to
disorder of movements
• Caused by damage to the motor control centers
of the developing brain and can occur during
pregnancy (75%), childbirth (5%) or after birth
(15%) up to age 3
• Prenatal brain abnormalities
• Brain anoxia
• Prematurity
• Twin births
• Other prenatal or perinatal risk factors: Aspyxia,
ischemia, perinatal trauma, congenital & perinatal
infections, perinatal metabolic problems such as
hyperbilirubenemia and hypoglycemia
• Infection, trauma and tumors can cause CP in early
infancy
• Unknown (24%)
Spastic Cerebral Palsy
• Affected area: cortex
• Tense, contracted muscles
• Walks on his toeswith scissor gait,
crossing one foot in front of the other
• Hypertonic, flexion, underdeveloped
upper limbs
• Most common type (70%)
and may involve one or both sides of
the body
– Hemiparesis
– Quadriparesis
– Diplegia
Dyskinetic/ Athetoid Cerebral Palsy
• Affected area: basal ganglia
• Constant, uncontrolled motion of
limbs, head, and eyes
• Involves abnormal involuntary
movements that disappear during
sleep and increase with stress
– Major manifestations are
athetosis (worm-like
movement), dyskinetic
movement of mouth, drooling
and dysarthria
ATAXIC Cerebral Palsy
• Poor sense of balance,
often causing falls and
stumbles
• Manifested by a wide-
based gait, rapid repetitive
movements performed
poorly, and disintegration
of movements of the
upper extremities when
the child reaches for
objects
The MIXED/ DYSTONIC
Cerebral Palsy
• Manifested by a
combination of the
characteristics of spastic
and athetoid CP
• Delayed gross motor
development – eating/
swallowing is difficult
• Disabilities usually result from injury to the
cerebellum, the basal ganglia or the motor
cortex
• Difficult to establish the precise location of
lesions
• Some cases, brain has gross malformations; in
others, vascular occlusion, atrophy, loss of
neurons and degeneration may be evident
• Non-progressive but become more apparent as
child grows older
• Delayed gross motor development
• Abnormal motor performance (eg. Early dominant
hand preference, abnormal & asymmetrical crawl,
poor sucking, feeding problems or persistent tongue
thrust)
• Alterations of muscle tone
• Abnormal postures (eg. Scissoring legs or
persistent infantile posturing)
• Reflex abnormalities (eg. Persistent primitive reflexes –
tonic neck of hyperreflexia)
• Mental retardation, seizures, attention deficit disorder
and sensory impairment
• Prenatal, birth and postnatal history
• Neurologic examination
• Assessment of muscle tone, behavior and
abilities
• Other disorders: metabolic disorders,
degenerative disorders and early slow-
growing tumors are ruled out
• Prevent physical injury by providing the child with
a safe environment, appropriate toys, and
protective gear (helmet, kneepads) if needed
• Prevent physical deformity by ensuring correct
use of prescribed braces and other devices and
by performing ROM exercises
• Promote mobility by encouraging the child to
perform age and condition-appropriate motor
activities
• Promote adequate fluid and nutritional
intake
• Foster relaxation and general health by
providing rest periods
• Administer prescribed medications which may
include sedatives, muscle relaxants and anti-
convulsants
• Encourage self-care by urging the child to
participate in activities of daily living (ADLs)
• Facilitated communication
– Talk to the child deliberately and slowly, using
pictures to reinforce speech when needed
– Encourage early speech therapy to prevent poor or
maladaptive communication habits
– Provide means of articulate speech such as sign
language or a picture board
– Technology such as computer use may help children
with severe articulation problems
• As necessary, seek referrals for corrective lenses and
hearing devices to decrease sensory deprivation related to
vision and hearing losses
• Help promote a positive self-image in the
child
– Praise his accomplishments
– Set realistic and attainable goals
– Encourage an appealing physical appearance
– Encourage his involvement with age and
condition-appropriate peer group activities
• Promote optimal family functioning
– Encourage family members to express anxieties,
frustrations and concerns and to explore support
networks
– Provide emotional support and help with
problem solving as necessary
– Refer the family to support organizations such as
the United Cerebral Palsy Association
You might also like
- Comprehensive Head To Toe AssessmentDocument22 pagesComprehensive Head To Toe Assessmentqueenzk80% (30)
- Comprehensive Head To Toe Assessment PDFDocument22 pagesComprehensive Head To Toe Assessment PDFVanessaMUellerNo ratings yet
- Week 12 - Care of The Pediatric Client With Neurologic DisorderDocument66 pagesWeek 12 - Care of The Pediatric Client With Neurologic DisorderLeyla GalyanoNo ratings yet
- Examination of Central Nervous SystemDocument85 pagesExamination of Central Nervous SystemdrbhawnavermaNo ratings yet
- Approach To Floppy Infant: LT Col (DR) Bindu T Nair Professor (Pediatrics)Document56 pagesApproach To Floppy Infant: LT Col (DR) Bindu T Nair Professor (Pediatrics)Dorjee SengeNo ratings yet
- Neurological ExaminationDocument71 pagesNeurological ExaminationAmbreen SabaNo ratings yet
- Neurological ExaminationDocument71 pagesNeurological ExaminationSiti Nursuhada binti Mohd AminNo ratings yet
- The Child With A Neurologic DisorderDocument42 pagesThe Child With A Neurologic DisorderLeilani FullerNo ratings yet
- Diah Mustika HW, SPS, Kic Intensive Care Unit of Emergency Department Naval Hospital DR Ramelan, SurabayaDocument33 pagesDiah Mustika HW, SPS, Kic Intensive Care Unit of Emergency Department Naval Hospital DR Ramelan, SurabayaNabilaNo ratings yet
- CPDocument86 pagesCPMahnoorNo ratings yet
- Peads AssessmentDocument63 pagesPeads AssessmentSrinivas MohanNo ratings yet
- Early Identification and Treatment Techniques in Babies WithDocument47 pagesEarly Identification and Treatment Techniques in Babies WithDr.GK. JeyakumarNo ratings yet
- Cerebral Palsy: PediatricsDocument50 pagesCerebral Palsy: PediatricsRANJIT GOGOINo ratings yet
- Health Promotion For Neonates and Infa NtsDocument55 pagesHealth Promotion For Neonates and Infa NtsawesomeNo ratings yet
- Neurological Examination of Infants: Herczegfalvi ÁgnesDocument17 pagesNeurological Examination of Infants: Herczegfalvi Ágnesaria tristayanthiNo ratings yet
- Cerebral Palsy MXDocument34 pagesCerebral Palsy MXNeeraj VermaNo ratings yet
- Check for facial droop, weakness, or paralysisDocument54 pagesCheck for facial droop, weakness, or paralysisابرار مساعدهNo ratings yet
- Neuro DisordersDocument159 pagesNeuro DisordersQuolette Constante100% (1)
- Neonatal Cns ExaminationDocument33 pagesNeonatal Cns ExaminationShishir KumarNo ratings yet
- Assessment of Neurologic System: Nursing Health Assessment NCM101 Paolo Christian Bautista, RN LecturerDocument58 pagesAssessment of Neurologic System: Nursing Health Assessment NCM101 Paolo Christian Bautista, RN LecturerShaira SariaNo ratings yet
- Assessing Neurological FunctionDocument59 pagesAssessing Neurological FunctionSherlyn PedidaNo ratings yet
- Coma Stimulation Therapy TechniquesDocument21 pagesComa Stimulation Therapy TechniquesPallavi Subbanna poojaryNo ratings yet
- A Fitting Child: By: Nur Fadhilah AhmadDocument23 pagesA Fitting Child: By: Nur Fadhilah AhmadazimahahmadNo ratings yet
- Neuro DiagDocument128 pagesNeuro DiagBars DenskieNo ratings yet
- Common nervous system disorders and age-related changes assessmentDocument82 pagesCommon nervous system disorders and age-related changes assessmentTaate MohammedNo ratings yet
- Elective - Neurologic Reporting 1Document23 pagesElective - Neurologic Reporting 1GenEsis CarandangNo ratings yet
- Assess Nervous System WeaknessDocument23 pagesAssess Nervous System Weaknessthe KLAWNo ratings yet
- Exploring Newborn DevelopmentDocument51 pagesExploring Newborn DevelopmentHsieh Yun JuNo ratings yet
- Nursing Care of A Family When A Child Has A Neurologic DisorderDocument8 pagesNursing Care of A Family When A Child Has A Neurologic DisorderBern NerquitNo ratings yet
- Case 5 SeizureDocument17 pagesCase 5 SeizureGrace Tanajura100% (2)
- Assessing The Neurologic System PDFDocument10 pagesAssessing The Neurologic System PDFYudi TrigunaNo ratings yet
- Pediatric AccidentsDocument91 pagesPediatric Accidentsokumu atanasNo ratings yet
- SeizuresDocument7 pagesSeizuresSaf Tanggo DiampuanNo ratings yet
- Neuro AssessmentDocument10 pagesNeuro AssessmentMonica RamboyongNo ratings yet
- 4-Lifespan-Ch 4 - Birth & Physical Dev 1st 3 YearsDocument15 pages4-Lifespan-Ch 4 - Birth & Physical Dev 1st 3 YearsJoseph Barnes100% (1)
- WA0044.encDocument40 pagesWA0044.encmalfed adrianoNo ratings yet
- Neurological Eval SensoryDocument25 pagesNeurological Eval SensoryAyen FornollesNo ratings yet
- A Case of Refractory EpilepsyDocument57 pagesA Case of Refractory EpilepsyAdela OkaforNo ratings yet
- Anamnesis Dan Diagnosis Topis (Dr. Hendro SP.S)Document27 pagesAnamnesis Dan Diagnosis Topis (Dr. Hendro SP.S)PatrickNicholsNo ratings yet
- Cerebral PalsyDocument96 pagesCerebral PalsyRahini PaniNo ratings yet
- New Born AssessmentDocument53 pagesNew Born AssessmentCelline Isabelle ReyesNo ratings yet
- Cerebral Palsy: A Guide to Diagnosis and ManagementDocument95 pagesCerebral Palsy: A Guide to Diagnosis and ManagementAgus WibowoNo ratings yet
- Week 7 - Neurological Disorders Fall 2020 - With NarrationsDocument30 pagesWeek 7 - Neurological Disorders Fall 2020 - With NarrationsM SHOAIB KHALIDNo ratings yet
- Responses To Altered PerceptionDocument74 pagesResponses To Altered PerceptionANDREA JUSTINE CARDEÑONo ratings yet
- Rest and Sleep 1Document36 pagesRest and Sleep 1Onyx ReyesNo ratings yet
- Pediatric Neurologic DisordersDocument97 pagesPediatric Neurologic DisordersMa Tosca Cybil TorresNo ratings yet
- Minor Head InjuryDocument2 pagesMinor Head InjurySamer FarhanNo ratings yet
- Neurologic Examination: Amanda Du, MD, Dpps Pediatrician-NeonatologistDocument91 pagesNeurologic Examination: Amanda Du, MD, Dpps Pediatrician-NeonatologistLyn LynNo ratings yet
- Pediatric Neurology History and Exam GuideDocument19 pagesPediatric Neurology History and Exam Guiderjh1895No ratings yet
- Neurological AssessmentDocument76 pagesNeurological Assessmentjcabatit3No ratings yet
- 1 Neuro AssessmentDocument10 pages1 Neuro Assessmentshuchi joshiNo ratings yet
- Exercicios para o CérebroDocument60 pagesExercicios para o CérebroMarco Aurélio de MeloNo ratings yet
- Gross Primitive Reflexes BW HandoutsDocument38 pagesGross Primitive Reflexes BW HandoutsristeacristiNo ratings yet
- Neurological AssessmentDocument127 pagesNeurological Assessmentstudent_019100% (1)
- SIGS Case 3.1b Sophia Watson Neural Tube DefectDocument37 pagesSIGS Case 3.1b Sophia Watson Neural Tube Defectbob thabuilderNo ratings yet
- Neurology - Part 2Document12 pagesNeurology - Part 2Fritz MirandaNo ratings yet
- Hana, ComaDocument45 pagesHana, ComaMeraol HusseinNo ratings yet
- Principles of Cns ExaminationDocument25 pagesPrinciples of Cns ExaminationBaraka SayoreNo ratings yet
- Narcolepsy, A Simple Guide to the Condition, Treatment and Related DiseasesFrom EverandNarcolepsy, A Simple Guide to the Condition, Treatment and Related DiseasesRating: 1 out of 5 stars1/5 (2)
- Critical Thinking Writing PromptsDocument2 pagesCritical Thinking Writing PromptsJaja ManezNo ratings yet
- Ncma Course Task 13 PDFDocument1 pageNcma Course Task 13 PDFJaja ManezNo ratings yet
- Bachelor of Science in Nursing: Care of Mother and Child and AdolescentDocument12 pagesBachelor of Science in Nursing: Care of Mother and Child and AdolescentJaja ManezNo ratings yet
- Week 16 - Musculoskeletal Disease in ChildrenDocument51 pagesWeek 16 - Musculoskeletal Disease in ChildrenJaja ManezNo ratings yet
- Critical Writing Skills for Workplace SuccessDocument5 pagesCritical Writing Skills for Workplace SuccessJaja ManezNo ratings yet
- 11 CRWT111 Barriers To Critical Thinking Week15 16Document51 pages11 CRWT111 Barriers To Critical Thinking Week15 16Jaja ManezNo ratings yet
- Hazmat EcolabDocument100 pagesHazmat EcolabJobanna Rpo FdezNo ratings yet
- PE 4thG QADocument4 pagesPE 4thG QALiah Mercado100% (1)
- Education &: DebateDocument5 pagesEducation &: DebateMac HusseyNo ratings yet
- Lesson Exemplar Health 4thDocument4 pagesLesson Exemplar Health 4thelmalynNo ratings yet
- JSA FOR Using The Hand and Power Tools - 2Document2 pagesJSA FOR Using The Hand and Power Tools - 2soubhagya100% (2)
- End of Surgery Clinical Placement Theory Test AnswersDocument16 pagesEnd of Surgery Clinical Placement Theory Test AnswersMustafaNo ratings yet
- Wheeless' Textbook of OrthopaedicsDocument6 pagesWheeless' Textbook of Orthopaedicsnurul auliaNo ratings yet
- Innervation and Vascularization of Head and NeckDocument36 pagesInnervation and Vascularization of Head and NeckDrgDondyNo ratings yet
- People v. Clarence Lee Scott, Court of Appeals of California, Fifth District. Opinion (3/3/11)Document8 pagesPeople v. Clarence Lee Scott, Court of Appeals of California, Fifth District. Opinion (3/3/11)Peter M. HeimlichNo ratings yet
- Rehabilitation Strategies After Spinal Cord InjuryDocument17 pagesRehabilitation Strategies After Spinal Cord Injuryhanna.oravecz1No ratings yet
- Hamstring Strains. Classification and ManagementDocument3 pagesHamstring Strains. Classification and ManagementJesusNavarrete97No ratings yet
- Biomechanics of Wrist ComplexDocument11 pagesBiomechanics of Wrist Complexakheel ahammed100% (2)
- Your Spine, Your Yoga: Developing Stability and Mobility For Your Spine - Bernie ClarkDocument5 pagesYour Spine, Your Yoga: Developing Stability and Mobility For Your Spine - Bernie ClarkbucabijoNo ratings yet
- Traumatic Brachial Plexus Injuries GuideDocument5 pagesTraumatic Brachial Plexus Injuries GuidedoruntineNo ratings yet
- List of anatomy mnemonicsDocument86 pagesList of anatomy mnemonicsKashar SaeedNo ratings yet
- ARNISDocument4 pagesARNISHiedelynLlanoNo ratings yet
- Exertional Leg Pain GuideDocument29 pagesExertional Leg Pain GuidejohanesNo ratings yet
- Hospital Incident ReportingDocument32 pagesHospital Incident Reportingakhtarulmunim2279No ratings yet
- Laser Therapy ProtocolsDocument89 pagesLaser Therapy ProtocolsSYED ALI HUSSAINNo ratings yet
- Basic Knee Arthroscopy Part 4Document2 pagesBasic Knee Arthroscopy Part 4Diego BellingNo ratings yet
- Clinical Notes of Cranial NervesDocument6 pagesClinical Notes of Cranial Nerveseducation HubNo ratings yet
- 01 Afialda vs. Hisole DigestDocument1 page01 Afialda vs. Hisole DigestNoreen AquinoNo ratings yet
- Anatomical Atlas, Illustrative of The Structure of The Human BodyDocument386 pagesAnatomical Atlas, Illustrative of The Structure of The Human BodyAmaterasuNo ratings yet
- Adult Brachial Plexus InjuryDocument13 pagesAdult Brachial Plexus Injurysunshine bloomNo ratings yet
- Ligamento Cruzado Doble FasciculoDocument16 pagesLigamento Cruzado Doble FasciculoAuusto CórdobaNo ratings yet
- Management of Head InjuriesDocument90 pagesManagement of Head InjuriesrobelNo ratings yet
- Plate Fixation For Letenneur Type I Hoffa Fracture - A Biomechanical StudyDocument7 pagesPlate Fixation For Letenneur Type I Hoffa Fracture - A Biomechanical StudyDiana Marcela Benítez HernándezNo ratings yet
- GV Series 4 Boiler ManualDocument96 pagesGV Series 4 Boiler ManualBruce GrantNo ratings yet
- Lecture F2F - Seriously Injured ChildDocument22 pagesLecture F2F - Seriously Injured ChildcolinjNo ratings yet
- Muscles of The BackDocument33 pagesMuscles of The Backtaha makhloufNo ratings yet