Professional Documents
Culture Documents
Hormonal Biochemistry
Uploaded by
Ruth0 ratings0% found this document useful (0 votes)
11 views82 pagesbiochemistry notes about endocrinology
Original Title
Hormonal Biochemistry copy
Copyright
© © All Rights Reserved
Available Formats
PPTX, PDF, TXT or read online from Scribd
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this Documentbiochemistry notes about endocrinology
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
0 ratings0% found this document useful (0 votes)
11 views82 pagesHormonal Biochemistry
Uploaded by
Ruthbiochemistry notes about endocrinology
Copyright:
© All Rights Reserved
Available Formats
Download as PPTX, PDF, TXT or read online from Scribd
You are on page 1of 82
Hormonal Biochemistry
Course content as outlined in the curriculum of
BMS KIU:
• General characteristics of Hormones
• Molecular mechanism of action of hormones
• Synthesis of hormones
• Methods of hormone Assay
What is a Hormone?
• Hormones are chemical messengers that coordinate
different functions in the body.
• They are produced by endocrine glands
General characteristics of hormones:
• They act as body catalysts resembling enzymes in
some aspect.
• They are required only in small quantities.
• They are not used up during the reaction.
General characteristics of hormones Contd
• They are produced in an organ other than that in which
they perform their action
• They are secreted in blood prior to use.
• Thus the circulating levels of hormones can give some
indication of endocrine gland activity and target organ
exposure
• some hormones are protein in nature.
• some are small peptides.
• Some hormones are derived from amino acids
• some are steroid in nature.
Classification of hormones based on their
chemical nature
1. Steroid hormones:
• These are steroid in nature such as adrenocorticosteroid
hormones, androgens, estrogens and progesterone.
2. Amino acid derivatives:
• These are derived from amino acid tyrosine, e.g.
epinephrine, norepinephrine and thyroid hormones.
3. Peptide/Protein hormones:
• These are either large proteins or small or medium size
peptides, e.g. Insulin, glucagon, parathormone,
calcitonin, pituitary hormones, etc.
Molecular mechanism of action of
hormones
• Steroid hormones are lipophilic in nature
• Hence,they can easily pass across the plasma membrane.
• They bind to the intracellular receptors in the cytosol or the
nucleus forming hormone –receptor complex.
• The hormone-receptor complex binds to specific regions on
the DNA called hormone responsive element (HRE) and
causes increased expression of specific genes.
• The interaction of hormone receptor complex with HRE
promotes transcription and Translation.
• The ultimate outcome is the production of specific proteins
in response to hormonal action.
Molecular mechanism of action of Steroid
hormones
Major endocrine glands
• Pituitary gland
• Thyroid gland-Thyroid hormones
• Parathyroid gland –Parathyroid hormone
• Adrenal gland –adrenocorticoids i.e glucocorticoids
and mineralocorticoids
• Pancreas –Insulin and Glucagon
• Ovaries –Progesterone and estrogen
• Testes-testosterone
Hypothalamus
• Hypothalamus is a specialized center in the brain that
functions as a master coordinator of hormonal action.
• In response to the stimuli of central nervous system,
hypothalamus liberates certain releasing factors or
hormones.
• These factors stimulate or inhibit the release of
corresponding tropic hormones from the anterior
pituitary.
• Tropic hormones stimulate the target endocrine tissues
to secrete the hormones they synthesize
Hypothalamic hormones
• Hypothalamus produces six releasing factors or
hormones.
1. Thyrotropin-releasing hormone (TRH
2. Corticotropin-releasing hormone (CRH)
3. Gonadotropin-releasing hormone (GnRH)
4. Growth hormone-releasing hormone (GRH)
5. Growth hormone release-inhibiting hormone
(GRIH)
6. Prolactin release-inhibiting hormone (PRIH)
Thyrotropin-releasing hormone
(TRH)
• TRH stimulates anterior pituitary to release thyroid
stimulating hormone (TSH )/Thyrotropin.
• TSH, stimulates the release of thyroid hormones (T3
and T4).
Corticotropin-releasing hormone (CRH)
• It stimulates the anterior pituitary to release Adreno-
cortocotropic hormone (ACTH).
• ACTH acts on adrenal cortex to liberate
adrenocorticosteroids.
Gonadotropin-releasing hormone
(GnRH) :
• GnRH stimulates anterior pituitary to release
gonadotropins, namely luteinizing hormone (LH) and
follicle stimulating hormone (FSH).
Growth hormone-releasing hormone (GRH)
• stimulates the release of growth hormone (GH or
somatotropin) which promotes growth.
Growth hormone release-inhibiting
hormone (GRIH):
• It is also known as somatostatin.
• GRIH inhibits the release of growth hormone from
the anterior pituitary
Prolactin release-inhibiting hormone (PRIH) :
• It inhibits the release of prolactin (PRL) from
anterior pituitary.
Pituitary gland
• It is located below the hypothalamus of the brain.
• lt has the anterior and the posterior pitutitary glands.
• Anterior pituitary is truly the master endocrine organ.
Hormones of anterior pituitary gland:
1.Growth hormone(GH)
2.Prolactin(PRL)
3.Thyroid stimulating hormone(TSH)
4. Adrenocorticotropic hormone (ACTH)
5.Gonadotropins i.e Follicle stimulating hormone(FSH),
Luteinizing hormone (LH).
Growth hormone
• It is also known as somatotropin
• The growth hormone releasing hormone (GRH)
stimulates the release of GH .
• The growth hormone release-inhibiting hormone
(GRlH) inhibits GH production.
• This, in turn, is regulated by a feedback mechanism
• Growth hormone production is influenced by sleep,
stress , exercise, food intake etc.
• The largest increase in the production of GH occurs
after the onset of sleep.
Biochemical functions of growth
hormone
• It promotes growth
• It enhances protein synthesis
• Growth hormone is anti-insulin and causes
hyperglycemia.
• GH increases lipolysis in adipose tissue.
• Growth hormone promotes bone mineralization
and its growth,as seen in growing children.
Abnormalities of GH production
Deficiency of GH :
• lmpairment in the secretion of growth hormone in the
growing age causes dwarfism.
Overproduction of GH:
• Excessive production of GH causes gigantism in children
and acromegaly in adults
• Gigantism is characterized by increased growth of long
bones.
• Acromegaly is characterized by increase in the size of
hands, facial changes (enlarged nose, protruding jaw),
excessive hair, thickening of skin etc
Prolactin (PRL)
• Prolactin is concerned with the initiation and
maintenance of lactation in mammals
• PRL promotes HMP shunt, increases lipid
biosynthesis and stimulates lactose production in
mammary glands.
• Prolactin promotes the growth of corpus luteum and
stimulates the production of progesterone.
Thyroid stimulating Hormone
(TSH)
• The release of TSH from anterior pituitary is
controlled by a feedback mechanism.
• This involves the hormones of thyroid gland (T3 and
T4) and thyrotropin releasing hormone (TRH) of
hypothalamus.
Gonadotropins:
• The release of FSH and LH from the anterior
pituitary is controlled by gonadotropin-releasing
hormone (GnRH) of hypothalamus
Gonadotropins
• The FSH, LH and human chorionic gonadotropin
(hcG) are commonly known as gonadotropins.
• These hormones are glycoproteins.
Biochemical functions of FSH :
• In females, FSH stimulates follicular growth,
increases the weight of the ovaries and enhances the
production of estrogens.
• ln males, FSH stimulates testosterone production,
required for spermatogenesis.
• FSH also promotes growth of seminiferous tubules
Biochemical functions of LH
• Luteinizing hormone stimulates the production of
progesterone in females and testosterone in males.
• LH and FSH are responsible for the development and
maintenance of secondary sexual characters in males.
Human chorionic gonadotropin (hCG) :
• Produced by cells of placenta
• The levels of hCG in plasma and urine increase
immediately after the implantation of fertilized ovum.
• The detection of hCG in urine is used for detection
of pregnacy .
Adrenocorticotropic hormone
(ACTH)
• The release of ACTH from the anterior pituitary is
under the regulation of hypothalamic hormone,
corticotropin releasing hormone (CRH).
Biochemical functions of ACTH:
• ACTH increases lipolysis by activating lipase of
adipose tissue.
• lt enhances RNA and protein synthesis and thus
promotes adrenocortical growth
• ACTH promotes the conversion of cholesterol to
pregnenolone in the adrenal cortex
Overproduction of ACTH
• Excessive production of ACTH causes Cushing's
syndrome .
• This may be due to a tumor.
Characteristics of cushing’s syndrome :
• Hyperpigmentation
• increased production of adrenocorticosteroids.
Associated symptoms:
• negative nitrogen balance, impaired glucose
tolerance, hypertension, edema, muscle atrophy
Posterior pituitary hormones
1.Oxytocin
2.Antidiuretic hormone/vasopressin
Effects of oxytocin:
• Stimulates uterine contractions in labor and child
birth
• Stimulates contractions of breast tissue to aid in
lactation after child birth
• Pitocin is the synthetic derivative of oxytocin
• Pitocin, is used to induce labor.
Antidiuretic hormone(ADH)
Biochemical functions
• ADH regulates water balance in the body.
• lt stimulates kidneys to retain water and, thus,
increases the blood pressure
Diabetes insipidus:
• lt is due to insufficient levels of ADH or a defect in
the receptors of target cells.
• This disorder is characterized by the excretion of
large volumes of dilute urine (polyuria).
Synthesis of Hormones
• Peptide and protein hormones are synthesized from
amino acids.
• Steroid hormones are derivatives of cholesterol.
• Amine hormones are derivatives of tyrosine.
• The primary amino acid sequence of the peptide is
dictated by a specific messenger ribonucleotide
(mRNA) which has been transcribed from the gene
for that hormone.
Synthesis of peptide hormones
1.In the nucleus ,the gene for the hormone is transcribed
into an mRNA.
• Generally ,a single gene is responsible for directing the
primary structure of each peptide hormone.
2.The mRNA is transferred to the cytoplasm and
translated on the ribosomes to the first protein products, a
preprohormone.
• Translation stops, and the signal peptide attaches
to receptors on the endoplasmic reticulum
Steps for synthesis of peptide hormones
contd.
3.The signal peptide is removed in the ER, converting
the preprohormone to a prohormone.
• The prohormone contains the complete hormone
sequence plus other peptide sequences, which will be
removed in the final step.
• Some of the other peptide sequences in the
prohormone are necessary for proper folding of the
hormone.
Synthesis of peptide hormones Contd..
4.The prohormone is transferred to Golgi
apparatus ,where it is packaged in secretory vesicles.
• In the secretory vesicles ,proteolytic enzymes cleave
peptide sequences from the prohormone to produce
the final hormone.
5.The hormone is stored in secretory vesicles untill the
endocrine cell is stimulated.
Steroid hormone synthesis
• Steroid hormones are synthesized and secreted by
the adrenal cortex and gonads.
• The steroid hormones are cortisol,
aldosterone,estradiol and estriol, progesterone and
testosterone
• All steroid hormones are derived from cholesterol
• Steroid hormones include sex hormones and
adrenocorticoids.
Adrenal glands
• The adrenal glands are two small organs located
above the kidneys.
Each adrenal consists of :
i.An outer Adrenal cortex (with 3 zones)
ii.An inner Adrenal medulla .
• The adrenal cortex consists of 3 zones namely
a.Zona glomerulosa
b.Zona fasciculata
c.Zona reticularis
Hormones of Adrenal Cortex
• Glucocorticoids, Mineralocorticoids,
• Androgens and estrogens
1.Glucocorticoids:
• These are produced by zona fasciculata.
• They affect glucose , amino acid and fat metabolism
in a manner that is opposite to the action of insulin
• Cortisol is the main glucocorticoid in humans.
Mineralocorticoids
• They are produced by zona glomerulosa
• They regulate water and electrolyte balance.
• Aldosterone is the most prominent mineralocorticoid
Androgens and Estrogens
• The innermost adrenal cortex zona reticularis produces
small quantities of androgens and estrogens .
• These hormones affecting sexual development and
functions are mostly produced by gonads.
• Dehydroepiandrosterone a precursor for androgens is
synthesized in adrenal cortex.
Steroid hormones
• Steroid hormones include Adrenal cortical hormones
and sex hormones
Adrenal cortical hormones
• The adrenal cortex has 3 different zones :
1.Zona glomerulosa -the outermost
• Produces mineralo-corticoids.
2.The zona fascicularis- The middle zone of the adrenal
cortex, produces the glucocorticoids .
3. The zona reticularis – is the innermost ,produces the
androgens and estrogens
Synthesis of Steroid hormones
1.Cholesterol is first acted upon by desmolase and a 6-
carbon unit is cleaved off, forming pregnenolone.
• It is a common precursor for all the steroid hormones.
• ACTH stimulates this step.
• This is the rate limiting step for synthesis of all steroid
hormones.
2.Prognenolone is converted to progesterone.
• Pregesterone is the first steroid hormone .
3.Progesterone is further converted into glucocorticoids ,
mineralocorticoids and sex steroids.
Synthesis of steroid hormones Contd
• These reactions are effected by hydroxylation
reactions which are catalysed by hydroxylases.
• The major adrenal glucocorticoids are cortisol,
cortisone and corticosterone in that order.
• The major mineralocorticoid is aldosterone, but 11-
deoxy-corticosterone and corticosterone also have
significant mineralocorticoid activity.
Synthesis of Steroid hormones
Abnormalities of Adrenocortical
function
• Addison's disease
• Cushing's syndrome
Addison’s disease
• lmpairment in adrenocortical function results in Addison's
disease
• This disorder is characterized by decreased blood glucose
level (hypoglycemia).
• Loss of weight, loss of appetite (anorexia), muscle
weakness, impaired cardiac function, low blood pressure,
decreased Na+ and increased K+ level in serum, increased
susceptibility to stress.
Cushing's syndrome
-It is due to hyperfunction of adrenal cortex.
Causes of Cushing’s syndrome :
• Long term pharmacological use of steroids
• Tumor of adrenal cortex
• Tumor of pituitary gland
Characteristics of Cushing's syndrome
• Hyperglycemia, Fatigue, muscle wasting,
• Edema, osteoporosis, negative nitrogen balance,
hypertension, moon-face etc.
Amine hormone synthesis
• The amine hormones are catecholamines and
Thyroid hormones.
Catecholamines:
• Epinephrine,
• Norepinephrine
• Dopamine
Hormones of Adrenal Medulla
• It produces dopamine ,epinephrine ( adrenaline) ,
norepinephrine (noradrenaline).
• These hormones are called catecholamine.
• Norepinephrine and dopamine are important
neurotransmitters in the brain and autonomic
nervous system.
• Catecholamines are produced in response to fight,flight
and fright.
• These include the emergencies like shock, cold, fatigue,
emotional conditions like anger etc.
Synthesis of Catecholamines
• The conversion of tyrosine to catecholamines occurs
in adrenal medulla and central nervous system.
• Tyrosine is hydroxylated to dihydroxyphenylalanine
(DOPA) by tyrosine hydroxylase.
• This enzyme catalyses the rate limiting reaction and
requires tetrahydrobiopterin as coenzyme .
• Tyrosinase present in melanocytes converts tyrosine
to DOPA.
Synthesis of Catecholamines contd
• DOPA undergoes PLP-dependent decarboxylation to
give dopamine which, in turn, is hydroxylated to
produce norepinephrine.
• Methylation of norepinephrine by S-
adenosylmethionine gives epinephrine.
• The difference between epinephrine and
norepinephrine is only a methyl group .
Abnormalities of Catecholamine
production
1.Pheochromocytomas
2.Parkinson’s disease
Pheochromocytomas:
• These are the tumors of adrenal medulla.
• It is characterized by an excessive production of
epinephrine and norepinephrine
• Overproduction of the two catecholamines causes severe
hypertension.
• The measurement of urinary Vanillyl mandelic acid
(VMA) is used in diagnosis of pheochromocytomas.
Parkinson's disease
• Parkinson's disease affects people above 60 years .
• Parkinson's disease is due to decreased production of
dopamine.
• The disease is due to degeneration of certain parts of
the brain leading to the impairment in the synthesis
of dopamine.
• characteristics of Parkinson’s disease:
• Muscular rigidity, tremors, expressionless face,
• Lethargy, involuntary movements etc.
Treatment of Parkinson’s disease
• DOPA (levodopa or L-dopa) is used in the treatment
of Parkinson's disease.
• In the brain, DOPA is decarboxylated to dopamine
which alleviates the symptoms of this disorder.
• Dopa analogs i.e Carbidopa and methyl-dopa are
administered along with dopa for the treatment of
Parkinson's disease.
Thyroid gland
• Produces thyroxine (T4) and triiodothyronine(T3).
• T4 and T3 regulate the metabolic rate of the body.
• Thyroid gland also secretes calcitonin, a hormone
concerned with calcium homeostasis .
Biosynthesis of thyroid hormones:
• lodine is essential for the synthesis of thyroid
hormones.
Uptake of Iodide
• The uptake of iodide by the thyroid gland
occurs against a concentration gradient .
• lt is an energy requiring process and is linked
to the ATPase dependent Na+-K+ pump.
• lodide uptake is primarily controlled by TSH
• Antithyroid agents such as thiocyanate and
perchlorate inhibit iodide transport.
Formation of active Iodine
• The conversion of iodide (l-) to active iodine (l+) is
an essential step for its incorporation into thyroid
hormones.
• Thyroid is the only tissue that can oxidize l- to a
higher valence state l+
• This reaction requires H2O2 and is catalysed by the
enzyme thyroperoxidase.
• TSH promotes the oxidation of iodide to active iodine
while the antithyroid drugs (thiourea, thiouracil,
methinazole) inhibit.
Thyroglobulin and synthesis of T3 and
T4
• Thyroglobulin is a glycoprotein and precursor for the
synthesis of T3 and T4.
• Thyroglobulin contains 140 tyrosine residues which serve
as substrates for iodine for the formation of thyroid
hormones.
• Tyrosine is first iodinated at position 3 to form
monoiodotyrosine (MlT) and then at position 5 to form
diiodotyrosine (DlT).
• Two molecules of DIT couple to form thyroxine (T4)
• One molecule of MlT, when coupled with one molecule of
DlT, triiodothyronine (T3) is produced.
Storage and Release of Thyroid hormones
• Thyroglobulin containing T4 and T3 can be stored for
several months in the thyroid gland.
• lt is estimated that the stored thyroid hormones can meet
the body requirement for 1-3 months.
• Thyroglobulin is digested by lysosomal proteolytic
enzymes in the thyroid gland
• The free hormones thyroxine and triiodothyronine are
released into the blood, a process stimulated by TSH.
• MIT and DIT produced in the thyroid gland undergo
deiodination by the enzyme deiodinase and the iodine thus
liberated can be reutilized.
Transport of T3 and T4
• Two specific binding proteins-thyroxine binding
globulin (TBG) and thyroxine binding prealbumin
(TBPA)-are responsible for the transport of thyroid
hormones.
• Both T4 and T3 are more predominantly bound to
TBG.
• A small fraction of free hormones are biologically
active.
• T4 has a half-life of 4-7 days while T3 has about one
day
Biochemical functions of Thyroid
hormones
1. Influence on the metabolic rate :
• Thyroid hormones stimulate the metabolic activities
and increases the oxygen consumption in most of the
tissues of the body except-brain, lungs, testes and
retina.
2. Effect on protein synthesis :
• Thyroid hormones promote protein synthesis .
• They function as anabolic hormones and cause
positive nitrogen balance and promote growth and
development.
Biochemical functions of thyroid
hormones contd
3. Influence on carbohydrate metabolism :
• Thyroid hormones promote intestinal absorption of
glucose and its utilization.
• These hormones increase gluconeogenesis and
glycogenolysis, with an overall effect of enhancing
blood glucose level .
4.Effect on lipid metabolism :
• Lipid turnover and utilization are stimulated by
thyroid hormones.
Abnormalities of Thyroid gland
Goitre:
• Goitre is an abnormal increase in the size of the
thyroid gland .
• Enlargement of thyroid gland is to compensate the
decreased synthesis of thyroid hormones
• It is associated with elevated TSH
• Goiter is due to lack of iodine.
Hyperthyroidism
• This is due to overproduction of thyroid hormones.
Characteristics of Hyperthyroidism :
• Increased metabolic rate (higher BMR)
• Nervousness, Irritability ,Anxiety
• Rapid heart rate
• Loss of weight despite increased appetite
• Weakness, Diarrhea, Sweating,
• Sensitivity to heat and often protrusion of eyeballs
(exopthalmos).
Hyperthyroidism
• Hyperthyroidism is caused by Grave's disease or due
to increased intake of thyroid hormones.
• T3 and T4 are elevated in blood.
• It is diagnosed by estimation of T3 and T4 .
Treatment :
• Administration of antithyroid drugs.
• In severe cases, thyroid gland is surgically removed.
Hypothyroidism
• This is due to an impairment in the function of thyroid
gland that causes decreased circulatory levels of T3
and T4.
• Disorders of pituitary or hypothalamus also contribute
to hypothyroidism.
• Women are more susceptible than men.
Characteristics of Hypothyroidism:
• Reduced BMR, slow heart rate, weight gain,
• sluggish behaviour, constipation, sensitivity to cold,
Dry skin
Hypothyroidism cont’d
• Hypothyroidism in children leads to cretinism.
• It is manifested by physical and mental retardation.
• Hypothyroidism in adults causes myxoedema.
Characteristics of Myxoedema
• Bagginess under the eyes, slow heart rate,weight gain
• Cold intolerance,slow in physical and mental activities.
Treatment of hypothyroidism:
• Administration of thyroid hormones.
Hormones of Gonads
• The gonads are testes in males and ovaries in
females.
Functions of Gonads:
1.Synthesize sex hormones
2.Produce germ cells
• The steroid sex hormones are responsible for growth,
development, maintenance and regulation of
reproductive system.
• Sex hormones are essentially required for the
development of germ cells
Sex hormones
1. Androgens or male sex hormones
2. Estrogens or female sex hormones
3. Progesterone is produced during the luteal phase of
menstrual cycle and also during pregnancy
Androgens:
• The male sex hormones or androgens are produced by
the Leydig cells of the testes and to a minor extent by
the adrenal glands in both the sexes.
• Ovaries also produce small amounts of androgens
Biosynthesis of androgens
• Cholesterol is the precursor for the synthesis of
androgens.
• lt is first converted to pregnenolone which then forms
androstenedione by two pathways--either through
progesterone or through 1 7-hydroxypregnenolone.
• Testosterone is produced from androstenedione.
• The production of androgens is under the control of
LH and FSH
Biosynthesis of androgens Contd
Active form of androgen
• The primary product of testes is testosterone.
• However, the active hormone in many tissues is not
testosterone but its metabolite dihydrotestosterone
(DHT).
• Testosterone, on reduction by the enzyrne 5 alpha-
reductase, forms DHT.
Physiological functions of Androgens
1.Sex-related physiological functions :
The androgens, primarily DHT and testosterone,
influence :
• Growth, development and maintenance of male
reproductive organs.
• Sexual differentiation and secondary sexual
characteristics.
• Spermatogenesis.
• Male pattern of aggressive behavior.
Biochemical functions of Androgens
1.Effects on protein metabolism :
• Androgens promote RNA synthesis (transcription) and
protein synthesis (translation).
• Androgens cause positive nitrogen balance and increase the
muscle mass.
2.Effects on carbohydrate and fat metabolism :
• Androgens increase glycolysis ,fatty acid synthesis and
citric acid cycle
3.Effects on mineral metabolism :
• Androgens promote mineral deposition and bone growth
before the closure of epiphyseal cartilage
Estrogens
• Estrogens are predominantly ovarian hormones,
systhesized by the follicles and corpus luteum of
ovary.
• These hormones are responsible for maintenance of
menstrual cycle and reproductive process in women.
Synthesis of Estrogens
• Estrogen synthesis occurs from the precursor
cholesterol.
• Estrogens are produced by aromatization (formation
of aromatic ring) of androgens.
Synthesis of Estrogens Cont’d
• The ovary produces estradiol (E2) and estrone (E1)
while the placenta synthesizes these two steroid
hormones and estriol (E3).
• The synthesis of estrogens is under the control of LH
and FSH.
Physiological functions of Estrogens
1.Sex-related physiological functions :
The estrogens are primarily concerned with .
• Growth, development and maintenance of female
reproductive organs.
physiological functions of Estrogens
Contd
• Maintenance of menstrual cycles.
• Development of female sexual characteristics
Biochemical functions of Estrogens:
1.Lipogenic effect :
• Estrogens increase lipogenesis in adipose tissue and, for this reason
women have more fat than men.
2.Hypocholesterolemic effect :
• Estrogens lower the plasma total cholesterol.
• The LDL fraction of lipoproteins is decreased while the HDL
fraction is increased.
• This explains the low incidence of atherosclerosis and coronary
heart diseases in the women during reproductive age.
Biochemical effects of estrogens Contd
Anabolic effect :
• Estrogens in general promote transcription and
translation. The synthesis of many proteins in liver is
elevated e.g. transferrin, ceruloplasmin
Effect on bone growth:
• Estrogens like androgens promote calcification and
bone growth.
• lt is believed that decalcification of bone in the
postmenopausal women leading to osteoporosis is
due to lack of estrogen
Biochemical effects of Estrogens Contd
Effect on transhydrogenase :
• Transhydrogenase is an enzyme activated by estrogen.
• lt is capable of transferring reducing equivalents from
NADPH to NAD+.
• The NADH so formed can be oxidized.
• lt is explained that in the women after menopause, due
to deficiency of estrogens, the transhydrogenase activity
is low.
• This results in the diversion of NADPH towards
Lipogenesis-causing obesity
Progesterone
• Progesterone is synthesized and secreted by corpus
luteum and placenta.
• Progesterone, as such, is an intermediate in the
formation of steroid hormones from cholesterol.
• LH controls the production of progesterone
Biochemical Functions of progesterone
1.Progesterone is essentially required for the
implantation of fertilized ovum and maintenance
of pregnancy
2. lt promotes the growth of glandular tissue in uterus
and mammary gland.
3. Progesterone increases the body temperature
• The measurement of temperature was used as an
indicator for ovulation
METHODS OF HORMONAL ASSAY
1. Enzyme Linked Immuno sorbent assay (ELISA)
2.Radioimmuno assay (RIA)
ELISA TEST
• ELISA is Enzyme Linked Immuno sorbent assay.
• It is used to detect antigens or antibodies present
in very small quantities in tissues or blood.
Principle :
• ELISA is based on the immunochemical
principles of antigen-antibody reaction.
Antibody detection by ELISA
• This is useful to detect small quantities of antibodies
in the blood.
• A good example is the test for detection of HIV
antibody.
• In patients with AIDS, the human immuno
deficiency virus (HIV) produces specific antibody.
• To detect the HIV antibody, the following method is
used.
Procedure for Antibody detection by
ELISA
• Antigen from HIV is coated in the wells of a
multiwell (microtiter) plate.
• Patient's serum is added, and incubated.
• If it contains the antibody, it is fixed.
• The wells are washed.
• This is to remove excess antibodies in serum.
• Next ,a second antibody (antibody against human
immunoglobulin)conjugated with Horse radish
peroxidase (HRP) is added.
Procedure for Antibody detection by
ELISA Contd
• Then color reagent, containing hydrogen peroxide
and diamino benzidine is poured over.
• If a brown color develops, it means that the antibody
was originally present in the patient's serum.
• The color developed is proportional to the antibody
concentration.
• Any antibody can be detected using the specific
antigen.
Antigen detection by ELISA method
• Antibody is fixed to the well of a microtiter plate.
• A good example is the assay of thyroid hormone, T4.
• The patient's serum is added in the well, and
incubated for 30 minutes at 37°C.
• Antigen i.e T4 present in the serum is fixed on the
antibody.
• Excess antigen and other unwanted proteins are
washed out.
Antigen Detection by ELISA Method
• Then, specific antibody (antibody against T4, tagged
with enzyme horse radish peroxidase (HRP) is added.
• If the antigen is already fixed, the antibody-HRP-
conjugate will be fixed in the well.
• Then a color reagent, containing hydrogen peroxide
(H2O2) and diamino benzidine (DAB) are added.
• This is known as “sandwich” ELISA
• Development of a brown color indicates that the
antigen is originally present in the patient's serum.
Antigen Detection by ELISA Method
• Color developed is proportional to the antigen in the
serum.
• Therefore intensity of the color may be measured,
from which the concentration of the antigen is
calculated.
Radio Immuno Assay (RIA)
• The technique of RIA was developed by Rosalyn
Yalow (Nobel prize, 1977).
• Insulin was the first substance quantitated by RIA.
• Hormones, growth factors, tumor markers, cytokines
and bacterial antigens can be quantitated by the RIA
method.
• The specificity of antibody and the sensitivity of
radioactivity are combined in this technique.
Radio immuno assay (RIA)
Principle:
• Radioimmunoassay combines the principles of
radioactivity of isotopes and immunological reactions of
antigen and antibody.
• It usually measures the concentration of antigens by use
of antibodies.
• Example of antigen that can be measured by RIA
is ,Hormone levels in blood.
• A known quantity of antigen is made radioactive by
labeling it with radioactive isotopes such as iodine ,125-I .
RIA Cont’d
• This radiolabeled antigen is then mixed with a known
amount of antibody , and as a result, the two
specifically bind to one another .
• Then, a sample of serum, from a patient containing an
unknown quantity of that same antigen is added.
• This causes the unlabeled antigen from the serum to
compete with the radiolabeled antigen for antibody
binding sites.
RIA Cont’d
• As the concentration of unlabelled antigen is
increased, more of it binds to the antibody.
• Hence, displacing the radiolabeled antigen, and
reducing the ratio of antibody-bound radiolabeled
antigen to unbound radiolabeled antigen.
• The bound antigens are then separated and radio
activity of the unbound antigens remaining is
measured using a gamma counter.
You might also like
- Balancing Hormones Naturally: A Woman's Guide to Hormonal Harmony: HealthFrom EverandBalancing Hormones Naturally: A Woman's Guide to Hormonal Harmony: HealthNo ratings yet
- Hormones 080623Document83 pagesHormones 080623Rao Asad MubeenNo ratings yet
- Hormone Balance: How To Reclaim Hormone Balance , Sex Drive, Sleep & Lose Weight Now: The Blokehead Success SeriesFrom EverandHormone Balance: How To Reclaim Hormone Balance , Sex Drive, Sleep & Lose Weight Now: The Blokehead Success SeriesNo ratings yet
- Endocrine PhysiologyDocument98 pagesEndocrine PhysiologyMohan GuptaNo ratings yet
- Endocrinology Endocrinology: H. KibichoDocument370 pagesEndocrinology Endocrinology: H. KibichoMursal RashidNo ratings yet
- Endocrine System: Endocrine: Which Have No Duct and ReleaseDocument36 pagesEndocrine System: Endocrine: Which Have No Duct and Releasedr_saleh77No ratings yet
- HORMONESDocument65 pagesHORMONESsoumya palavalasaNo ratings yet
- Hypothalamus & Pituitary GlandDocument39 pagesHypothalamus & Pituitary GlandVishal DodejaNo ratings yet
- Endocrine SystemDocument69 pagesEndocrine SystemDivya JaiswalNo ratings yet
- Anterior Pituitary (Autosaved)Document33 pagesAnterior Pituitary (Autosaved)BABLU GAMINGNo ratings yet
- ENDOCRINE SYSTEM DISORDERS PROPER best (1)Document370 pagesENDOCRINE SYSTEM DISORDERS PROPER best (1)ronaronixstheboyNo ratings yet
- Endocrine SystemDocument30 pagesEndocrine SystemAkshat RastogiNo ratings yet
- Hypothalamus and PituitaryDocument60 pagesHypothalamus and Pituitarydhruvdesai24No ratings yet
- The Endocrine System The Endocrine System: © 2018 Pearson Education, Ltd. 1Document12 pagesThe Endocrine System The Endocrine System: © 2018 Pearson Education, Ltd. 1lourd nabNo ratings yet
- Endocrine System: Glands & HormonesDocument78 pagesEndocrine System: Glands & HormonesJerilee SoCute WattsNo ratings yet
- Endocrine SystemDocument96 pagesEndocrine SystemSandhya Kakkar100% (3)
- Anterior Pituitary GlandDocument33 pagesAnterior Pituitary Glandmarianne.erdooNo ratings yet
- Endocrine System GuideDocument37 pagesEndocrine System GuideKochaMsangiNo ratings yet
- Endocrine GlandsDocument36 pagesEndocrine GlandsnasyitahnorzlanNo ratings yet
- Hypothalamus and Pituitary GlandDocument62 pagesHypothalamus and Pituitary GlandphyMedza AppNo ratings yet
- Endocrine SystemDocument15 pagesEndocrine SystemNyakie MotlalaneNo ratings yet
- EndocrinologyDocument74 pagesEndocrinologysyedahaleemajunaidsNo ratings yet
- Hypothalamic-Pituitary Axis: - Oleh: - I Dewa Made RuspawanDocument33 pagesHypothalamic-Pituitary Axis: - Oleh: - I Dewa Made RuspawanherlinaNo ratings yet
- BSC Anterior Pituitary HormonesDocument27 pagesBSC Anterior Pituitary HormonesThalapathy PrakashNo ratings yet
- EndocrineDocument94 pagesEndocrineHira NawazNo ratings yet
- LECTURE 1 Endocrine Diseases Lecture 1 January 10-020Document68 pagesLECTURE 1 Endocrine Diseases Lecture 1 January 10-020aleen qawareetNo ratings yet
- Hypothalamus and Pituitary Gland FunctionsDocument48 pagesHypothalamus and Pituitary Gland FunctionsMohsin AbbasNo ratings yet
- Pituitary and ThyroidDocument54 pagesPituitary and ThyroidSaif AliNo ratings yet
- Metabolic & Endocrine DiseasesDocument280 pagesMetabolic & Endocrine DiseasesHussenNo ratings yet
- Seminor On Hormons Slide2 by Prof - Dr.HariharDocument49 pagesSeminor On Hormons Slide2 by Prof - Dr.Hariharhariharb999_23960100No ratings yet
- Module 22 HormonesDocument23 pagesModule 22 HormonesCrystal ManguneNo ratings yet
- HormonesDocument29 pagesHormonesCandy Chieng67% (3)
- Regulasi Endokrin 22 IntensifDocument25 pagesRegulasi Endokrin 22 IntensifWignes WarenNo ratings yet
- Chemical Coordination and IntegrationDocument34 pagesChemical Coordination and IntegrationBiju Mylachal100% (9)
- Endocrine SystemDocument75 pagesEndocrine SystemReneilwe MoshidiNo ratings yet
- EndocrineDocument94 pagesEndocrineSuzana VoiculescuNo ratings yet
- Unit IV. Endocrine SystemDocument44 pagesUnit IV. Endocrine Systemtajuddin shaikNo ratings yet
- Pituitary GlandDocument25 pagesPituitary GlandIshaqNo ratings yet
- Endocrine and SecretionsDocument25 pagesEndocrine and SecretionsNelson Louie III RicerraNo ratings yet
- Presentation 1Document20 pagesPresentation 1Rajeev NaikNo ratings yet
- Ila College of Health: Endocrine PhysiologyDocument40 pagesIla College of Health: Endocrine PhysiologyDaniel DendaNo ratings yet
- 4 Pituitary HormonesDocument18 pages4 Pituitary HormonesRana AbdullahNo ratings yet
- Hormones SubtopicsDocument77 pagesHormones SubtopicsSulaiman UmraniNo ratings yet
- Endocrine System: Clarence L. Nuval, RMT, MDDocument66 pagesEndocrine System: Clarence L. Nuval, RMT, MDCla NuvalNo ratings yet
- Corticotropins and GonadotropinsDocument39 pagesCorticotropins and GonadotropinsSudhakar LakavathNo ratings yet
- Endocrinology: The Regulation and Function of HormonesDocument136 pagesEndocrinology: The Regulation and Function of HormonesShiela Torres100% (9)
- Endocrine System AnatomyDocument41 pagesEndocrine System Anatomypizzyray640No ratings yet
- Lec-4 The Anterior Pituitary Gland-IIDocument32 pagesLec-4 The Anterior Pituitary Gland-IIMowlidAbdirahman Ali madaaleNo ratings yet
- ENDOCRINOLOGYDocument8 pagesENDOCRINOLOGYshaairatogleNo ratings yet
- 09 Endocrine System PhysiologyDocument43 pages09 Endocrine System PhysiologyKaye Alyssa Enriquez100% (1)
- Pituitary Gland IntroDocument40 pagesPituitary Gland IntroSaif AliNo ratings yet
- ENDOCRINE SYSTEM OVERVIEWDocument86 pagesENDOCRINE SYSTEM OVERVIEWsheryl dungogNo ratings yet
- Endocrine System/socialDocument33 pagesEndocrine System/socialrpant3165No ratings yet
- A&PII Test 1Document14 pagesA&PII Test 1Alyssa BattcockNo ratings yet
- The Endocrine System: Endocrine Gland (Ductless Gland)Document50 pagesThe Endocrine System: Endocrine Gland (Ductless Gland)Mohammad AliNo ratings yet
- Chemical Coordination and Integration by - Dr. Sunita SaxenaDocument66 pagesChemical Coordination and Integration by - Dr. Sunita SaxenaDivya AgarawalNo ratings yet
- Hormones:: Signaling MoleculesDocument20 pagesHormones:: Signaling MoleculesSangeeta DwivediNo ratings yet
- Hypothalamus and HypophysisDocument32 pagesHypothalamus and HypophysisAlok KumarNo ratings yet
- System Glands Hormone: NeurotransmittersDocument6 pagesSystem Glands Hormone: NeurotransmittersShaheryar HasanNo ratings yet
- Endocrine System Student - S Copy1Document28 pagesEndocrine System Student - S Copy1Dayanara VillanuevaNo ratings yet
- Basis of Cancer 1Document62 pagesBasis of Cancer 1RuthNo ratings yet
- Immunochemistry 2Document50 pagesImmunochemistry 2RuthNo ratings yet
- Immunochemistry 1Document51 pagesImmunochemistry 1RuthNo ratings yet
- XenobioticsDocument30 pagesXenobioticsRuthNo ratings yet
- Infertility IDocument36 pagesInfertility Idr_asaleh100% (1)
- 0003-Pemberitahuan - Perubahan Harga Per 01 Feb 2022-Rev1Document4 pages0003-Pemberitahuan - Perubahan Harga Per 01 Feb 2022-Rev1Nora AyuNo ratings yet
- Journal of Endocrinology Androgens and Ovarian Function - Translation From Basic Discovery Research To Clinical ImpactDocument28 pagesJournal of Endocrinology Androgens and Ovarian Function - Translation From Basic Discovery Research To Clinical ImpactHong Ngoc PhamNo ratings yet
- Self-Monitoring of Blood Glucose in Type 2 Diabetes Recent StudiesDocument11 pagesSelf-Monitoring of Blood Glucose in Type 2 Diabetes Recent StudiesSelaNo ratings yet
- Endo Final 2Document3 pagesEndo Final 2joseph mouawadNo ratings yet
- Special Chemistry: Final ReportDocument1 pageSpecial Chemistry: Final ReportAMIRNo ratings yet
- Nodular Non Toxic GoiterDocument36 pagesNodular Non Toxic Goiterjean_arellanoNo ratings yet
- Biochemical Changes at MenopauseDocument14 pagesBiochemical Changes at MenopauseSyedSaqibHussainNo ratings yet
- Thyroid GlandDocument30 pagesThyroid GlandahmedkomranNo ratings yet
- Keyword Avg. Search Volume CPC PPC KDDocument13 pagesKeyword Avg. Search Volume CPC PPC KDAndreea Cruceanu-StoliNo ratings yet
- Pharmacology Test 3 ReviewDocument6 pagesPharmacology Test 3 ReviewNatalia BortellNo ratings yet
- The Complete Integumentary System Study GuideDocument72 pagesThe Complete Integumentary System Study GuideDeborahMcCloudNo ratings yet
- Blistering DiseasesDocument26 pagesBlistering DiseasesLia-Maria BufteaNo ratings yet
- REAL in Nursing Journal (RNJ) : Relaksasi Autogenik Menurunkan Kadar Gula Darah Pasien Diabetes Melitus Tipe 2Document9 pagesREAL in Nursing Journal (RNJ) : Relaksasi Autogenik Menurunkan Kadar Gula Darah Pasien Diabetes Melitus Tipe 2gherice serumenaNo ratings yet
- PHARMACOLOGY 2 FINAL EXAM REVIEWDocument16 pagesPHARMACOLOGY 2 FINAL EXAM REVIEWT'amo HanashNo ratings yet
- General Principles of Metabolism Regulation. HormonesDocument90 pagesGeneral Principles of Metabolism Regulation. HormonesМохіт Кумар ЯмпатіNo ratings yet
- Discuss Di Erence Between Diabetes Mellitus Type 1 and DM Type 2Document3 pagesDiscuss Di Erence Between Diabetes Mellitus Type 1 and DM Type 2DHANNILLIE JHAIRA NU�EZNo ratings yet
- Efektifitas Senam Diabetes Terhadap Kadar Gula Darah Pada Pasien Diabetes Mellitus Di LamonganDocument6 pagesEfektifitas Senam Diabetes Terhadap Kadar Gula Darah Pada Pasien Diabetes Mellitus Di Lamonganfitrianingsih d4 kepNo ratings yet
- Psychological & Physiological Changes of PregnancyDocument8 pagesPsychological & Physiological Changes of PregnancyGwyneth ManioNo ratings yet
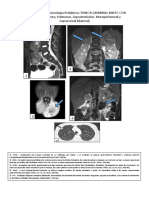
- Pediatric Endocrinology Images: MIXED GERM CELL TUMOR WITH METASTASISDocument4 pagesPediatric Endocrinology Images: MIXED GERM CELL TUMOR WITH METASTASISEnrique GonzalvusNo ratings yet
- The Endocrine System and Glands of The Human BodyDocument2 pagesThe Endocrine System and Glands of The Human BodyFungo JasmineNo ratings yet
- Gineco ENGLISHDocument198 pagesGineco ENGLISHVașadi Razvan CristianNo ratings yet
- Pathanatomy Lecture - 21 Acute & Chronic Renal FailureDocument52 pagesPathanatomy Lecture - 21 Acute & Chronic Renal FailureChris QueiklinNo ratings yet
- Pituitary DisorderDocument34 pagesPituitary DisorderSoniya ShivanshNo ratings yet
- Abnormalities Of The Testis And Scrotum: A Concise GuideDocument34 pagesAbnormalities Of The Testis And Scrotum: A Concise GuideIma MoriNo ratings yet
- Levothyroxine Nursing ResponsibilitiesDocument2 pagesLevothyroxine Nursing ResponsibilitiesKrisianne Mae Lorenzo FranciscoNo ratings yet
- Atlantis by Samael Aun WeorDocument4 pagesAtlantis by Samael Aun WeorBob MarinoNo ratings yet
- Hypoglycemia - Schermerhorn, ThomasDocument2 pagesHypoglycemia - Schermerhorn, ThomasJuanMartínezNo ratings yet
- Gyna Endocrinology DR Nadine 2021Document16 pagesGyna Endocrinology DR Nadine 2021Community Round3 G1No ratings yet
- INFERTILITY Obg SeminarDocument19 pagesINFERTILITY Obg SeminarDelphy Varghese100% (2)