Professional Documents
Culture Documents
RAD001
RAD001
Uploaded by
api-26302710Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
RAD001
RAD001
Uploaded by
api-26302710Copyright:
Available Formats
Articles
Efficacy of everolimus in advanced renal cell carcinoma:
a double-blind, randomised, placebo-controlled phase III trial
Robert J Motzer, Bernard Escudier, Stéphane Oudard, Thomas E Hutson, Camillo Porta, Sergio Bracarda, Viktor Grünwald, John A Thompson,
Robert A Figlin, Norbert Hollaender, Gladys Urbanowitz, William J Berg, Andrea Kay, David Lebwohl, Alain Ravaud, for the RECORD-1 Study Group*
Summary
Background Everolimus (RAD001) is an orally administered inhibitor of the mammalian target of rapamycin (mTOR), Lancet 2008; 372: 449–56
a therapeutic target for metastatic renal cell carcinoma. We did a phase III, randomised, double-blind, placebo-controlled Published Online
trial of everolimus in patients with metastatic renal cell carcinoma whose disease had progressed on vascular July 23, 2008
DOI:10.1016/S0140-
endothelial growth factor-targeted therapy.
6736(08)61039-9
See Comment page 427
Methods Patients with metastatic renal cell carcinoma which had progressed on sunitinib, sorafenib, or both, were
*Members listed at end of paper
randomly assigned in a two to one ratio to receive everolimus 10 mg once daily (n=272) or placebo (n=138), in
Memorial Sloan-Kettering
conjunction with best supportive care. Randomisation was done centrally via an interactive voice response system Cancer Center, New York, NY,
using a validated computer system, and was stratified by Memorial Sloan-Kettering Cancer Center prognostic score USA (Prof R J Motzer MD);
and previous anticancer therapy, with a permuted block size of six. The primary endpoint was progression-free Institut Gustave Roussy,
survival, assessed via a blinded, independent central review. The study was designed to be terminated after 290 events Villejuif, France (B Escudier MD);
Hôpital Européen Georges
of progression. Analysis was by intention to treat. This study is registered with ClinicalTrials.gov, number Pompidou, Paris, France
NCT00410124. (Prof S Oudard MD); US
Oncology/Baylor-Sammons
Findings All randomised patients were included in efficacy analyses. The results of the second interim analysis Cancer Center, Dallas, TX, USA
(Prof T E Hutson DO); IRCCS
indicated a significant difference in efficacy between arms and the trial was thus halted early after 191 progression San Matteo University Hospital
events had been observed (101 [37%] events in the everolimus group, 90 [65%] in the placebo group; hazard ratio 0·30, Foundation, Pavia, Italy
95% CI 0·22–0·40, p<0·0001; median progression-free survival 4·0 [95% CI 3·7–5·5] vs 1·9 [1·8–1·9] months). (C Porta MD); Azienda
Stomatitis (107 [40%] patients in the everolimus group vs 11 [8%] in the placebo group), rash (66 [25%] vs six [4%]), and Ospedaliera, Perugia, Italy
(S Bracarda MD); Medical School
fatigue (53 [20%] vs 22 [16%]) were the most commonly reported adverse events, but were mostly mild or moderate in Hannover, Hannover, Germany
severity. Pneumonitis (any grade) was detected in 22 (8%) patients in the everolimus group, of whom eight had (Prof V Grünwald MD); Cancer
pneumonitis of grade 3 severity. Care Alliance, Seattle, WA, USA
(Prof J A Thompson MD); City of
Hope National Medical Center,
Interpretation Treatment with everolimus prolongs progression-free survival relative to placebo in patients with Duarte, CA, USA
metastatic renal cell carcinoma that had progressed on other targeted therapies. (Prof R A Figlin MD); Novartis
Oncology, Florham Park, NJ,
USA (N Hollaender PhD,
Funding Novartis Oncology.
G Urbanowitz BS, W J Berg MD,
A Kay MD, D Lebwohl MD); and
Introduction implicate mTOR as a valid target for treatment of renal Hôpital Saint André CHU,
Everolimus (RAD001) is an orally administered inhibitor cell carcinoma.3,4 Bordeaux, France
(Prof A Ravaud MD)
of the mammalian target of rapamycin (mTOR), a Until recently, metastatic renal cell carcinoma was
component of an intracellular signalling pathway that considered a cancer with a poor outlook, with treatment Correspondence to:
Dr Robert J Motzer, Memorial
regulates cellular metabolism, growth, proliferation, and options limited to cytokines (interferon, interleukin 2).5 Sloan-Kettering Cancer Center,
angiogenesis. Everolimus, a derivative of rapamycin, Median survival averaged 13 months.6 Two small 1275 York Ave, New York,
binds to an intracellular protein, FKBP-12, forming a molecules, sunitinib and sorafenib, which target the NY 10021, USA
complex that inhibits the mTOR serine-threonine kinase. VEGF receptor (VEGF receptor tyrosine kinase motzerr@mskcc.org
Abnormal functioning of signalling pathways is inhibitors), temsirolimus, another mTOR inhibitor, and
believed to contribute to the pathogenesis of many bevacizumab, a monoclonal antibody to VEGF, have
malignancies, and is particularly relevant to renal cancers. shown clinical benefit for patients with treatment-naive
The pathogenesis of clear-cell renal cell carcinoma is or cytokine-pretreated renal cell carcinoma by prolonging
linked to loss of the von Hippel-Lindau tumour progression-free or overall survival.7–10 A systematic
suppressor gene, leading to accumulation of review of studies assessing targeted therapies for
hypoxia-inducible factor 1 (HIF-1) and overexpression of advanced renal cell carcinoma has recently been
HIF-1 target gene products, such as vascular endothelial published.11
growth factor (VEGF). VEGF and other factors induced Drugs targeting these pathways have produced robust
by HIF-1 are thought to be the key drivers of tumour clinical effects in patients with advanced renal cell
angiogenesis, permitting the growth and progression of carcinoma. However, there now exists a high unmet
renal cancers.1 Activation of mTOR also leads to increased medical need for patients who have failed therapy with
expression of HIF-1,2 and several lines of evidence VEGF receptor tyrosine kinase inhibitors. At present, no
www.thelancet.com Vol 372 August 9, 2008 449
Articles
approved therapeutic option exists for this recently Criteria in Solid Tumours [RECIST]16), a Karnofsky
established, pretreated population. An uncontrolled performance status score of 70% or more (on a scale
phase II trial of everolimus in pretreated patients showed of 0 to 100, with higher scores indicating better
a high proportion of durable disease stabilisation or performance), and adequate bone marrow, hepatic, and
tumour shrinkage in patients with metastatic renal cell renal function. Patients were ineligible if they had
carcinoma and progression of disease on cytokines.12 previously received mTOR inhibitor therapy
Earlier studies had established a daily oral dosing (temsirolimus), had untreated CNS metastases, or
schedule and the safety of everolimus in patients with uncontrolled medical conditions (eg, unstable angina
various solid tumour malignancies.13–15 pectoris, symptomatic congestive heart failure, recent
In this international, multicentre, double-blind, myocardial infarction, or diabetes).
randomised phase III trial, everolimus was compared The protocol was approved by the institutional review
with placebo for the treatment of metastatic renal cell boards of the participating institutions and the study was
carcinoma in patients whose disease had progressed on done in accordance with international standards of good
treatment with VEGF receptor tyrosine kinase inhibitors. clinical practice. All patients provided written informed
consent.
Methods
Patients Procedures
This trial was done in 86 centres in Australia, Canada, Patients were stratified according to a Memorial
Europe, Japan, and the USA. The study population Sloan-Kettering Cancer Center (MSKCC) prognostic
consisted of adults (aged 18 years and above) with score (favourable vs intermediate vs poor risk) and
metastatic renal cell carcinoma that showed a clear-cell previous anticancer therapy (one vs two previous VEGF
component, which had progressed on or within receptor tyrosine kinase inhibitors).17 Patients were
6 months of stopping treatment with sunitinib or randomly assigned in a two to one ratio to everolimus or
sorafenib, or both drugs. Previous therapy with placebo with the use of permuted blocks of six (four to
bevacizumab, interleukin 2, or interferon alfa was also everolimus, two to placebo) within each stratum.
permitted. Key eligibility criteria included the presence Patients received either continuous treatment with oral
of measurable disease (as per the Response Evaluation everolimus 10 mg once daily or placebo, both in
conjunction with best supportive care. Study drugs
(identical tablets of everolimus or placebo) were provided
554 patients screened
by the study sponsor, and were self-administered orally
(two 5 mg tablets) daily in a fasting state or with a light
fat-free meal. Each cycle was considered as 28 days of
410 patients randomly
allocated to treatment treatment; safety was assessed every 14 days for the first
December, 2006, three cycles and every 4 weeks thereafter.
to October, 2007
Doses were delayed or reduced if patients had clinically
significant haematological or other adverse events that
were deemed to be related to everolimus, according to a
272 patients assigned 138 patients assigned nomogram described in the protocol. In such cases,
to everolimus to placebo
10 mg/day doses were reduced to 5 mg once daily.
Treatment in both groups was continued until disease
3 did not receive 2 did not receive
progression, unacceptable toxicity, death, or discontinu-
treatment treatment ation for any other reason. Investigators were unaware of
1 had no post-baseline the study group assignments, but disclosure was
safety assessment
permitted after documented progression on the basis of
investigator assessment. Patients who were initially
269 patients received 135 patients received randomised to placebo were then able to crossover to
treatment treatment
receive open-label everolimus. This element of the study
design was incorporated to address both ethical and
recruitment considerations.
140 patients continue 129 patients discontinued 30 patients continue 105 patients discontinued
in ongoing study from study in ongoing study from study
Progression-free survival, documented with RECIST
85 had disease 100 had disease and assessed via a blinded, independent central review,
progression progression was the primary endpoint, defined as the time from
26 had adverse events 3 died
9 withdrew consent 2 had adverse randomisation to the first documentation of disease
7 died events progression or death (from any cause). Secondary
2 lost to follow-up
endpoints included safety, objective tumour response
rate, overall survival, disease-related symptoms, and
Figure 1: Trial profile quality-of-life.
450 www.thelancet.com Vol 372 August 9, 2008
Articles
All randomly assigned patients were assessable for
Everolimus group Placebo group
efficacy (intention-to-treat analysis). Tumour measure- (N=272) (N=138)
ments (assessed by CT or MRI scans) were done at
Age (years) 61 (27–85) 60 (29–79)
screening and were subsequently repeated every 8 weeks
Sex
for the remainder of the study, as well as on
Male 212 (78%) 105 (76%)
discontinuation of study drug. Additional scans were
Female 60 (22%) 33 (24%)
done as warranted to confirm response (no sooner than
Karnofsky performance status
4 weeks and no later than 6 weeks after its initial
100 75 (28%) 40 (29%)
observation), or whenever disease progression was
90 98 (36%) 53 (38%)
suspected. Selection of target lesions and tumour
80 70 (26%) 30 (22%)
assessments by the blinded central review were done
70 28 (10%) 15 (11%)
independently of investigator evaluations.
All patients who received at least one dose of study Missing 1 (<1%) 0
drug and had follow-up were assessed for safety. Safety MSKCC risk factors for second-line therapy*
assessments consisted of monitoring and recording of all Favourable 79 (29%) 39 (28%)
adverse events, regular monitoring of haematology and Intermediate 153 (56%) 78 (57%)
clinical chemistry measurements (laboratory evaluations), Poor 40 (15%) 21 (15%)
regular measurement of vital signs, performance of Previous treatment with VEGF receptor tyrosine kinase inhibitors
physical examinations, and recording of all concomitant Sunitinib only 124 (46%) 60 (43%)
medications and therapies. Adverse events and laboratory Sorafenib only 77 (28%) 42 (30%)
abnormalities were graded according to the National Both sunitinib and sorafenib 71 (26%) 36 (26%)
Cancer Institute’s Common Terminology Criteria for Other previous systemic therapy
Adverse Events, version 3.0. Interferon 138 (51%) 72 (52%)
Health-related quality-of-life was assessed with the Interleukin 2 60 (22%) 33 (24%)
European Organization for the Research and Treatment Chemotherapy 36 (13%) 22 (16%)
of Cancer (EORTC) QLQ-3018 and Functional Assess- Bevacizumab 24 (9%) 14 (10%)
ment of Cancer Therapy Kidney Symptom Previous surgery (nephrectomy) 262 (96%) 131 (95%)
Index—Disease-Related Symptoms (FKSI-DRS) question- Previous radiotherapy 83 (31%) 38 (28%)
naires.19 These questionnaires were administered before Common sites of metastases
randomisation, on day one of each cycle, and on discon- Lymph nodes 203 (75%) 98 (71%)
tinuation from the study. Lung 199 (73%) 112 (81%)
Bone 100 (37%) 43 (31%)
Statistical analysis Liver 94 (35%) 49 (36%)
The sample size was calculated on the basis of the Number of disease sites†
primary endpoint. A clinically meaningful improvement 1 26 (10%) 14 (10%)
was defined as a 33% risk reduction (hazard ratio 0·67), 2 67 (25%) 35 (25%)
corresponding to a 50% prolongation in median 3 87 (32%) 41 (30%)
progression-free survival, from 3·0 months for the ≥4 88 (32%) 45 (33%)
placebo arm to 4·5 months for patients receiving
everolimus. With the two to one randomisation and Data are median (range) or n (%). *Risk factors associated with shorter survival in
second-line therapy were low serum haemoglobin, raised corrected serum calcium,
assuming a one-sided cumulative α of 0·025, we and poor performance status; favourable=no risk factors, intermediate=one risk
calculated that a total of 290 events as per central radiology factor, poor=two or more risk factors.14 †As per baseline assessment for
review were required to achieve 90% power for the independent central radiology review; seven patients did not have centrally
reviewed tumour assessments.
three-look group sequential plan. With a scheduled
recruitment period of 16 months and additional follow-up Table 1: Patient demographics and disease characteristics
of 5 months, we estimated that we would need to enrol
about 362 patients (assuming that around 10% of patients After the second interim analysis, the study steering
would be lost to follow-up) to observe the required committee, on the recommendation of the independent
number of events. data monitoring committee, decided to terminate the
The first and second interim analyses were planned trial early because the pre-specified efficacy stopping
after observing about 30% and 60%, respectively, of the boundary (p≤0·0057, determined according to the
targeted 290 events required for the final statistical method of Lan and DeMets with O’Brien-Fleming-type
analysis. These interim analyses allowed the study to be stopping rules20,21) was crossed, the null hypothesis
stopped on the basis of safety, or futility or efficacy rejected, and the criteria for a positive study met. This
(second analysis only). The final analysis was to be done second interim analysis was designed to have
when 290 progression events had been observed, if the 45% probability of detecting an effective treatment under
stopping rule had not been met at an interim analysis. protocol assumptions on the treatment effect. As per
www.thelancet.com Vol 372 August 9, 2008 451
Articles
Everolimus group Placebo group
adjusting for strata defined by MSKCC prognostic score
(N=272) (N=138) and the hazard ratio estimated by use of a stratified Cox
Progression-free survival proportional hazards model.
Number of progression events 101 (37%) 90 (65%) East version 3.1 was used to calculate the sample size
(independent central review) and stopping boundaries; all other statistical analyses
Progression 85 (31%) 82 (59%) were done with SAS version 8.2. This trial is registered
Death 16 (6%) 8 (6%) with ClinicalTrials.gov with the identifier NCT00410124.
Censored 171 (63%) 48 (35%)
Best objective response (independent central review) Role of the funding source
Partial response rate 3 (1%) 0 The study sponsor contributed to the design, conduct,
Disease stabilisation* 171 (63%) 44 (32%) data collection, and data analysis. The corresponding
Progressive disease 53 (19%) 63 (46%) author had access to all data and takes responsibility for
Disease could not be assessed 45 (17%) 31 (22%) the accuracy and completeness of the data reported. The
Overall survival corresponding author had final responsibility for the
Number of deaths 42 (15%) 26 (19%) decision to submit for publication.
*Stable disease was defined as disease that remained unchanged for at least 56 days. Results
Table 2: Summary of efficacy measures The trial profile is shown in figure 1. Baseline demographic
and disease characteristics were much the same in the two
protocol, this second interim analysis was planned after groups (table 1). Details of previous treatment for renal cell
observing about 60% of the targeted 290 progression-free carcinoma are shown in table 1. 193 (71%) patients in the
survival events (per central radiology); however, because everolimus group and 109 (79%) in the placebo group had
this central assessment was not done in real time and progressed while receiving previous therapy.
the number of events needed was unknown, the cutoff The median duration of treatment was 95 (range 12–315)
date (Oct 15, 2007) was determined using a statistical days in the everolimus group and 57 (21–237) days in the
prediction model based on events per the investigator. placebo group. Treatment was ongoing for 140 (51%)
The actual number of centrally assessed progression-free patients in the everolimus group and 30 (22%) patients
survival events observed as of the cutoff date and in the placebo group at the time of data cutoff for this
included in the analysis was 191 (or 66% of the targeted analysis. The main reasons for treatment discontinuation
290 events). included disease progression, adverse events, death, and
Patients without tumour progression or death at the withdrawal of consent (figure 1).
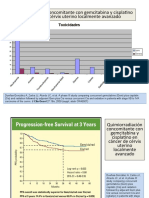
time of the data cutoff for the analysis or at the time of At the time of data cutoff, progression-free survival, as
receiving an additional anticancer therapy were censored assessed by independent central review, was significantly
at their last date of adequate tumour evaluation. prolonged in the everolimus group compared with the
Progression-free and overall survival curves were placebo group (hazard ratio 0·30, 95% CI 0·22–0·40;
estimated with Kaplan-Meier methodology; treatment p<0·0001; table 2 and figure 2). Median progression-free
arms were compared with a stratified log-rank test survival was 4·0 (95% CI 3·7–5·5) months in the
everolimus group and 1·9 (1·8–1·9) months for placebo.
100 | |
| |||
The probability of being progression-free at 6 months was
| |
|
||
| ||
||
| 26% (95% CI 14–37) for patients receiving everolimus
| ||
|| ||
|| compared with 2% (0–6) for patients in the placebo
80 | |||
||
| |||| | group.
|| || |
|
| || |
|||
Analyses of progression-free survival using investigator
Probability (%)
|
60 |||||
|
assessments of disease status, rather than central review,
|||
| |
|||||||| || | were consistent with those of the primary efficacy analysis
| | |
40
|
|||
(median progression-free survival 4·6 months, 95% CI
| |
| |
|| 3·9–5·5 in the everolimus group vs 1·8 months, 1·8–1·9;
|
| |
| | |
hazard ratio 0·31, 95% CI 0·24–0·41; p<0·0001).
20 |
| | Sensitivity analyses of potential confounding factors
|
Everolimus
| (including stratification factors at baseline and missing
0 Placebo data or loss to follow-up) confirmed the robustness of the
0 2 4 6 8 10 12
results for the primary efficacy analysis. Predefined
Time (months)
subset analyses (MSKCC risk classification) plus a series
Number at risk of exploratory analyses designed to investigate the
Everolimus 272 132 47 8 2 0 0
Placebo 138 32 4 1 0 0 0 homogeneity of the treatment effect across relevant
patient subgroups (number of previous VEGF receptor
Figure 2: Kaplan-Meier estimates of progression-free survival tyrosine kinase inhibitors, age, sex, and geographic
452 www.thelancet.com Vol 372 August 9, 2008
Articles
region) indicated that benefit was maintained across
HR p value N
subgroups (figure 3).
Central review 0·30 <0·0001 410
Confirmed objective tumour responses (all partial Investigator review 0·31 <0·0001 410
responses) assessed by independent central review were MSKCC risk
Favourable 0·35 <0·0001 118
seen in three (1%) patients receiving everolimus and Intermediate 0·25 <0·0001 231
none in the placebo group. The effect of everolimus on Poor 0·39 0·009 61
Previous treatment
progression-free survival is thus probably the result of Sorafenib only 0·29 <0·0001 119
disease stabilisation (table 2). Sunitib only 0·30 <0·0001 184
At the time of the analysis, median overall survival had Both 0·28 <0·0001 107
Age
not been reached for the everolimus group and <65 years 0·32 <0·0001 259
was 8·8 (95% CI 7·9–not available) months for the ≥65 years 0·29 <0·0001 151
Sex
placebo group. There was no significant difference Male 0·29 <0·0001 317
between groups in terms of overall survival (hazard Female 0·36 0·002 93
ratio 0·83, 95% CI 0·50–1·37; p=0·23; figure 4), probably Region
USA and Canada 0·24 <0·0001 130
due to confounding by crossover: of the 98 patients in the Europe 0·37 <0·0001 251
placebo group who progressed as per investigator Japan and Australia 0·10 0·001 29
assessment, 79 crossed over to open-label everolimus 0 0·2 0·4 0·6 0·8 1 1·2 1·4
after disease progression. 60 of these 79 patients had In favour of everolimus In favour of placebo
progressed within 8 weeks of enrolment.
No significant differences were evident between the Figure 3: Progression-free survival in sensitivity analyses and predefined subgroups (independent
central review)
two treatment groups in the time to definitive p values for subgroup analyses based on unstratified log-rank test. HR=hazard ratio.
deterioration of patient-reported outcomes, as determined
by pre-established criteria for clinically meaningful group and 20 (15%) in the placebo group required a dose
changes (EORTC QLQ-C30: physical functioning scale interruption, whereas 14 (5%) in the everolimus group
hazard ratio 0·94, 95% CI 0·64–1·39; global health and one (<1%) in the placebo group had a dose reduction
status/quality-of-life score 1·02, 0·70–1·50; FKSI-DRS with no previous interruption.
risk score: 0·82, 0·57–1·18). Longitudinal mean scores 14 (5%) patients receiving everolimus therapy and
for the FKSI-DRS and the physical functioning, global six (4%) in the placebo group died within 28 days of their
health status/quality-of-life, role functioning, emotional last dose (all causes). One patient in the everolimus
functioning, cognitive functioning, social functioning, group died from overwhelming candidal sepsis,
and symptoms scales of the EORTC QLQ-C30 complicated by acute respiratory failure, and which might
questionnaire indicated that quality of life was sustained have been attributable to study drug, and one patient
during treatment with everolimus relative to placebo, receiving placebo died from myocardial infarction; all of
irrespective of the adverse effects that might be expected the remaining deaths were attributed to the underlying
from the toxicities associated with an active treatment malignancy.
(data not shown).
As anticipated, adverse events were more frequently
reported within the everolimus treatment group than in
100
the placebo group (table 3); these events were mostly || ||
| | |||||| |||
|||||||||||||||||||
| | || ||||||
|||||||||||||
||||||| | |||
||||||| ||||||||| |||
|||
|||||||||||||| |||||
|||||| |||
|| ||||| |||
grade 1 or 2. The most common events were stomatitis, | |||
| |||
|| |||||
||| ||||
| | ||||
|| ||| |||
|| || ||| | |||| | |||
||| || ||
rash, fatigue or asthenia, and diarrhoea. The proportion of 80
| || | || | |||
| |||
| |||||||| ||||||||
|| ||||| |
grade 3 or 4 events was low for both groups. Patients || | ||||
|| |||
| |||||
||
||
|| |
||
|| | | |||
||||| |||| |
receiving everolimus had higher rates of grade 3 or 4 ||
||||||
||
Probability (%)
60 | |||
||||||| | | || |||| ||||| | | ||||
|||| |
stomatitis, infections, and non-infectious pneumonitis
than did those in the placebo group (table 3). Of the eight
patients with grade 3 pneumonitis, six discontinued 40
everolimus therapy. Four showed complete clinical
resolution, and three improvement to grade 2 or less. 20 |
Grade 3 or 4 lymphopenia, grade 3 hyperglycaemia, grade 3
hypophosphataemia, and grade 3 hypercholesterolaemia Everolimus
Placebo
occurred more often in patients receiving everolimus than 0
in those administered placebo (table 3). 0 2 4 6 8 10 12
Study drug toxicity led to treatment discontinuation Time (months)
Number at risk
for 28 (10%) patients receiving everolimus (with Everolimus 272 229 126 61 9 1 0
pneumonitis, dyspnoea, lung disorder, and fatigue the Placebo 138 111 62 25 9 1 0
most common reasons) and for five (4%) patients in the
placebo group. 92 (34%) patients in the everolimus Figure 4: Kaplan-Meier estimates of overall survival
www.thelancet.com Vol 372 August 9, 2008 453
Articles
Assessment of the primary endpoint of progression-free
Everolimus group (N=269) Placebo group (N=135)
survival was determined by independent review under
All grades Grade 3 Grade 4 All grades Grade 3 Grade 4 blinded conditions. The prolongation in progression-free
Adverse event survival seen here was greater than the expected
Stomatitis*† 107 (40%) 9 (3%) 0 11 (8%) 0 0 improvement that was used to calculate the sample size
Rash 66 (25%) 2 (<1%) 0 6 (4%) 0 0 for the study; the trial was thus halted at the second
Fatigue 53 (20%) 8 (3%) 0 22 (16%) 1 (<1%) 0 interim analysis. Progression-free survival is a recognised,
Asthenia 48 (18%) 4 (1%) 0 11 (8%) 1 (<1%) 0 credible endpoint for oncology trials,22 and prolongation
Diarrhoea 46 (17%) 4 (1%) 0 4 (3%) 0 0 of progression-free survival has been shown to correlate
Anorexia 44 (16%) 1 (<1%) 0 8 (6%) 0 0 with improved overall survival in renal cell carcinoma.8
Nausea 41 (15%) 0 0 11 (8%) 0 0 While designing our trial, we had advised the study
Mucosal inflammation 39 (14%) 3 (1%) 0 3 (2%) 0 0 sponsor that all patients experiencing disease progression
Vomiting 32 (12%) 0 0 5 (4%) 0 0 on placebo should be offered the option of receiving
Cough 32 (12%) 0 0 5 (4%) 0 0 open-label everolimus because there were no agents with
Dry skin 29 (11%) 1 (<1%) 0 5 (4%) 0 0 demonstrated efficacy available in this setting. This ethical
Infections*‡ 27 (10%) 6 (2%) 3 (1%) 3 (2%) 0 0 requirement to switch patients receiving placebo at the
Pneumonitis§ 22 (8%) 8 (3%) 0 0 0 0 time of disease progression to what was considered to be
Dyspnoea 22 (8%) 4 (1%) 0 3 (2%) 0 0 an active treatment23 meant that we were unable to
Laboratory abnormality
adequately address the effect of everolimus on overall
Anaemia 244 (91%) 24 (9%) 1 (<1%) 103 (76%) 7 (5%) 0
survival, since crossover would probably confound the
Hypercholesterolaemia* 205 (76%) 9 (3%) 0 43 (32%) 0 0
detection of any treatment-related benefit. We believe that
the improvement in progression-free survival seen in this
Hypertriglyceridaemia 191 (71%) 2 (<1%) 0 41 (30%) 0 0
trial is an appropriate indicator of everolimus’ anti-tumour
Hyperglycaemia* 135 (50%) 31 (12%) 0 31 (23%) 2 (1%) 0
effect in metastatic renal cell carcinoma. Our rationale
Raised creatinine 125 (46%) 1 (<1%) 0 44 (33%) 0 0
was to rely mainly on unbiased progression-free survival
Lymphopenia* 114 (42%) 38 (14%) 4 (1%) 39 (29%) 7 (5%) 0
data as opposed to confounded overall survival results. In
Raised alkaline phosphatase 101 (37%) 2 (<1%) 0 40 (30%) 2 (1%) 0
general, with the advent of ever more effective second and
Hypophosphataemia* 87 (32%) 12 (4%) 0 9 (7%) 0 0
third-line therapies as cancer treatments, and the growing
Leukopenia 70 (26%) 0 0 11 (8%) 0 1 (<1%)
use of crossover designs, it is becoming increasingly
Raised aspartate 56 (21%) 1 (<1%) 0 9 (7%) 0 0
aminotransferase
difficult to detect improvements in overall survival in
Thrombocytopenia 55 (20%) 2 (<1%) 0 3 (2%) 0 1 (<1%)
confirmatory phase III studies.
The administration of everolimus in conjunction with
Raised alanine 48 (18%) 1 (<1%) 0 5 (4%) 0 0
aminotransferase best supportive care in this trial was associated with more
Hypocalcaemia 46 (17%) 0 0 8 (6%) 0 0 toxic effects than was placebo plus best supportive care.
Neutropenia 29 (11%) 0 0 4 (3%) 0 0 Stomatitis, rash, and diarrhoea occurred with a higher
frequency among patients receiving everolimus, but were
*Sum of grade 3 and 4 events significantly different between everolimus group and placebo group (two-sided Fisher’s deemed to be severe in nine (3%) patients or fewer.
exact test): stomatitis, p=0·03; infections, p=0·03; hypercholesterolaemia, p=0·03; hyperglycaemia, p<0·0001;
lymphopenia, p=0·002; hypophosphataemia, p=0·01. No adaption for multiple testing was done. †Includes aphthous Hyperglycaemia, hypercholesterolaemia, and hyper-
stomatitis, mouth ulceration, and stomatitis. ‡Includes all infections. §Includes interstitial lung disease, lung lipidaemia were more common in the everolimus group
infiltration, pneumonitis, pulmonary alveolar haemorrhage, and pulmonary toxicity. than in the placebo group, probably as a result of inhibition
Table 3: Treatment-related adverse events of interest and those that occurred in at least 10% of patients of mTOR-regulated glucose and lipid metabolism.
in the everolimus group and laboratory abnormalities Non-infectious pneumonitis, a potentially serious
adverse event associated with rapamycin and rapamycin
Discussion derivative treatment,24 is also seen with everolimus. It
In this randomised, phase III study, everolimus was comprises one of a number of typical radiographic
associated with a reduction in the risk of progression or appearances with or without signs and symptoms (pleural
death compared with placebo in patients with metastatic effusion, hypoxia, cough, dyspnoea, malaise) in the
renal cell carcinoma whose disease had progressed after absence of a non-drug cause. Clinical evidence of grade 3
treatment with VEGF-targeted therapies. mTOR pneumonitis was reported for eight (3%) patients
inhibitors such as everolimus have a distinct mechanism receiving everolimus in the current trial. A detailed
of action from the recently established standard-of-care analysis is planned of the radiological and clinical findings
VEGF pathway inhibitors such as VEGF receptor tyrosine associated with lung symptoms and pneumonitis. This
kinase inhibitors (sunitinib and sorafenib) and VEGF will provide guidance for improved diagnosis,
ligand antibodies (bevacizumab).4 The results of our trial management and, if possible, prevention of this toxicity.
suggest that clinical resistance to VEGF inhibitors does The overall rate of severe events was low, and the
not imply clinical resistance to mTOR inhibitor treatment benefit-risk ratio was acceptable in the context of an
with everolimus. apparent clinical benefit in patients with a life-threatening
454 www.thelancet.com Vol 372 August 9, 2008
Articles
disease. Moreover, no detrimental effect on health-related E Calvo, P Maroto; USA—N Gabrail, L Appleman, D George, J Hamm,
quality-of-life was evident for everolimus compared with A Hussain, J Hajdenberg, N Vogelzang, T Logan, J Beck, K Rathmell,
P Lara, A Dudek, U Vaishampayan, M Gordon, T Anderson, M Danso,
placebo when assessed with the EORTC QLQ-C30 and W Berry, R Gersh, G Guzley, D Loesch, D Schlossman, D Smith.
FKSI-DRS questionnaires.
Conflict of interest statement
Everolimus is structurally and functionally similar to RAF has received research grants from Amgen, Argos, Keryx, Novartis,
temsirolimus, another mTOR inhibitor. Whereas Pfizer, and Wyeth. VG has received research grants from Bayer.
temsirolimus requires weekly intravenous administration,9 RJM has received research grants from Genentech, Novartis, Pfizer,
everolimus is administered orally; this could be viewed as and Wyeth. SB has acted as an adviser to Bayer, Novartis, Roche, and
Wyeth. AR has acted as an adviser to Bayer, GlaxoSmithKline, Novartis,
a distinct advantage by patients. This phase III trial with Pfizer, Roche, and Wyeth. TEH has acted as an adviser to Novartis.
everolimus and one other with temsirolimus9 establish SO has acted as an adviser to Pfizer, Roche, and Wyeth. BE received
mTOR inhibition as a valid therapeutic approach to consulting and/or lecture fees from Antigenics, Bayer, Innate,
Novartis, Pfizer, Roche, and Wyeth. RJM has received consulting
cancer therapy; in both instances the tumour type is renal
and/or lecture fees from Bayer. CP has received consulting and/or
cell carcinoma. In the temsirolimus phase III trial, lecture fees from Bayer, Novartis, Pfizer, Roche, and Wyeth. RAF has
patients with advanced renal cell carcinoma treated with received consulting and/or lecture fees from Bayer, Onyx, Pfizer, and
temsirolimus had improved progression-free and overall Wyeth. AR has received consulting and/or lecture fees from Bayer,
Novartis, Pfizer, and Wyeth. VG has received consulting and/or lecture
survival compared with those treated with interferon.9
fees from Novartis and Pfizer. JAT has received consulting and/or
However, there are several distinctions between this trial lecture fees from Pfizer. NH, GU, WJB, AK, and DL are full-time
and ours in terms of the clinical setting. Although most employees of, and own equity in, Novartis.
patients had clear-cell tumours, patients with less Acknowledgments
common renal cell histologies were also included in the The study and medical writing support were funded by Novartis
temsirolimus trial.9 The patient population for the Oncology. We thank all the patients and their families for their
participation in the study; Robert Amato (Methodist Hospital,
temsirolimus study was comprised of previously Houston) and Howard Burris (Sarah Cannon Cancer Center), for their
untreated, poor-prognosis renal cell carcinoma. Poor work with everolimus which led to the development of this trial; and
prognosis was assigned by number of adverse Peter Berry (Novartis Oncology) for assistance in the preparation of
pre-treatment clinical features.9 By contrast, the clinical this manuscript.
setting for our trial was in previously treated patients with References
demonstrated resistance to sunitinib or sorafenib, both 1 Kaelin WG. The von Hippel-Lindau tumor suppressor gene and
kidney cancer. Clin Cancer Res 2004; 10: 6290–95S.
inhibitors of receptors to VEGF and platelet-derived 2 Brugarolas J. Renal cell carcinoma—molecular pathways and
growth factors.7,8 Thus, this study extends the role for therapies. N Engl J Med 2007; 356: 185–87.
mTOR inhibitors beyond the first-line, poor-prognosis 3 Brugarolas JB, Vazquez F, Reddy A, Sellers WR, Kaelin WG. TSC2
regulates VEGF through mTOR-dependent and -independent
group setting. pathways. Cancer Cell 2003; 4: 147–58.
Treatment with VEGF receptor tyrosine kinase 4 Thomas GV, Tran C, Mellinghoff IK, et al. Hypoxia-inducible factor
inhibitors has provided a significant benefit to patients determines sensitivity to inhibitors of mTOR in kidney cancer.
Nat Med 2006; 12: 122–27.
with metastatic renal cell carcinoma;7,8 however, the
5 Motzer RJ, Bander NH, Nanus DM. Renal cell carcinoma.
therapy is not curative and a therapeutic option was N Engl J Med 1996; 335: 865–75.
lacking after progression on these agents. On the basis of 6 Coppin C, Porzsolt F, Autenrieth M, Kumpf J, Coldman A, Wilt T.
the results of this trial, we believe that everolimus should Immunotherapy for advanced renal cell cancer.
Cochrane Database Syst Rev 2004; 3: CD001425.
now be considered as the standard-of-care in patients with 7 Motzer RJ, Hutson TE, Tomczak P, et al. Sunitinib versus interferon
metastatic renal cell carcinoma whose disease has alfa in metastatic renal cell carcinoma. N Engl J Med 2007;
progressed after treatment with VEGF-targeted therapies. 356: 115–24.
8 Escudier B, Eisen T, Stadler WM, et al, for the TARGET Study
Contributors Group. Sorafenib in advanced clear-cell renal cell carcinoma.
RJM, BE, SO, TEH, CP, SB, VG, JAT, RAF, and AR contributed to the N Engl J Med 2007; 356: 125–34.
recruitment and treatment of patients in the trial. RJM, TEH, WJB, AK, DL, 9 Hudes G, Carducci M, Tomczak P, et al. Temsirolimus, interferon
and AR contributed to the design of the trial. All authors contributed to the alfa, or both for advanced renal cell carcinoma. N Engl J Med 2007;
interpretation of the data. NH contributed to the statistical design and 356: 2271–81.
analysis. All authors saw and approved the final version of the manuscript. 10 Escudier B, Pluzanska A, Korlewski P, et al. Bevacizumab plus
RECORD-1 Study Group interferon alfa-2a for treatment of metastatic renal cell carcinoma:
a randomised, double-blind phase III trial. Lancet 2007; 370: 2103–11.
Independent data monitoring committee—R Bukowski, W M Stadler,
D White, C Schmoor. 11 Coppin C, Le L, Porzsolt F, Wilt T. Targeted therapy for advanced
renal cell carcinoma. Cochrane Database Syst Rev 2008; 2: CD006017.
The following investigators recruited patients to this trial: Australia—
12 Jac J, Giessinger S, Khan M, Willis J, Chiang S, Amato R. A phase II
I Davis, H Gurney, K Pittman, D Goldstein, P Mainwaring; Canada—
trial of RAD001 in patients (pts) with metastatic renal cell
J Knox, S Ades, T Cheng, S Hotte, Y-J Ko, M MacKenzie, S North;
carcinoma (MRCC). J Clin Oncol 2007; 25 (18 suppl): 261S.
France—A Caty, F Rolland, C Chevreau, B Duclos, S Negrier;
13 O’Donnell A, Faivre S, Burris HA, et al. Phase I pharmacokinetic
Germany—J Gschwend, P Albers, L Bergmann, J Beck; Italy—E Bajetta,
and pharmacodynamic study of the oral mammalian target of
R Passalacqua, C Sternberg, F Boccardo, G Carteni, P F Conte; Japan— rapamycin inhibitor everolimus in patients with advanced solid
N Shinohara, N Tsuchiya, H Akaza, H Fujimoto, M Niwakawa, H Uemura, tumors. J Clin Oncol 2008; 26: 1588–95.
H Kanayama, M Eto, Y Sumiyoshi, T Tsukamoto, M Usami, A Terai, 14 Tabernero J, Rojo F, Calvo E, et al. Dose- and schedule-dependent
Y Hamamoto, M Maruoka; Netherlands—S Osanto, C Van Herpen, inhibition of the mammalian target of rapamycin pathway with
F Van Den Eertwegh, G Groenewegen; Poland—C Szczylik, J Pikiel, everolimus: a phase I tumor pharmacodynamic study in patients
A Pluzanska, R Zdrojowy; Spain—F del Muro, M Climent, D Castellano, with advanced solid tumors. J Clin Oncol 2008; 26: 1603–10.
www.thelancet.com Vol 372 August 9, 2008 455
Articles
15 Tanaka C, O’Reilly T, Kovarik JM, et al. Identifying optimal biologic 20 Lan KKG, DeMets DL. Discrete sequential boundaries for clinical
doses of everolimus (RAD001) in patients with cancer based on the trials. Biometrika 1983; 70: 659–63.
modeling of preclinical and clinical pharmacokinetic and 21 O’Brien PC, Fleming RT. A multiple testing procedure for clinical
pharmacodynamic data. J Clin Oncol 2008; 26: 1596–602. trials. Biometrics 1979; 35: 549–56.
16 Therasse P, Arbuck SG, Eisenhauer EA, et al. New guidelines to 22 Johnson JR, Williams G, Pazdur R. End points and United States
evaluate the response to treatment in solid tumors. Food and Drug Administration approval of oncology drugs.
J Natl Cancer Inst 2000; 92: 205–16. J Clin Oncol 2003; 21: 1404–11.
17 Motzer RJ, Bacik J, Schwartz LH, et al. Prognostic factors for 23 Amato RJ, Misellati A, Khan M, Chiang S. A phase II trial of
survival in previously treated patients with metastatic renal cell RAD001 in patients (pts) with metastatic renal cell carcinoma
carcinoma. J Clin Oncol 2004; 22: 454–63. (MRCC). J Clin Oncol 2006; 24 (18 suppl): abstract 4530.
18 Aaronson NK, Ahmedzai A, Bergman B, et al. The European 24 Atkins MB, Hidalgo M, Stadler WM, et al. Randomized phase II
Organization for Research and Treatment of Cancer QLQ-C30: study of multiple dose levels of CCI-779, a novel mammalian target
a quality-of-life instrument for use in international clinical trials in of rapamycin kinase inhibitor, in patients with advanced refractory
oncology. J Natl Cancer Inst 1993; 85: 365–76. renal cell carcinoma. J Clin Oncol 2004; 22: 909–18.
19 Cella D, Yount S, Brucker PS, et al. Development and validation of a
scale to measure disease-related symptoms of kidney cancer.
Value Health 2007; 10: 285–93.
456 www.thelancet.com Vol 372 August 9, 2008
You might also like
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeFrom EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeRating: 4 out of 5 stars4/5 (5811)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreFrom EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreRating: 4 out of 5 stars4/5 (1092)
- Never Split the Difference: Negotiating As If Your Life Depended On ItFrom EverandNever Split the Difference: Negotiating As If Your Life Depended On ItRating: 4.5 out of 5 stars4.5/5 (844)
- Grit: The Power of Passion and PerseveranceFrom EverandGrit: The Power of Passion and PerseveranceRating: 4 out of 5 stars4/5 (590)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceFrom EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceRating: 4 out of 5 stars4/5 (897)
- Shoe Dog: A Memoir by the Creator of NikeFrom EverandShoe Dog: A Memoir by the Creator of NikeRating: 4.5 out of 5 stars4.5/5 (540)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersFrom EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersRating: 4.5 out of 5 stars4.5/5 (348)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureFrom EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureRating: 4.5 out of 5 stars4.5/5 (474)
- Her Body and Other Parties: StoriesFrom EverandHer Body and Other Parties: StoriesRating: 4 out of 5 stars4/5 (822)
- The Emperor of All Maladies: A Biography of CancerFrom EverandThe Emperor of All Maladies: A Biography of CancerRating: 4.5 out of 5 stars4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)From EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Rating: 4.5 out of 5 stars4.5/5 (122)
- The Little Book of Hygge: Danish Secrets to Happy LivingFrom EverandThe Little Book of Hygge: Danish Secrets to Happy LivingRating: 3.5 out of 5 stars3.5/5 (401)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyFrom EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyRating: 3.5 out of 5 stars3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)From EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Rating: 4 out of 5 stars4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaFrom EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaRating: 4.5 out of 5 stars4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryFrom EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryRating: 3.5 out of 5 stars3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnFrom EverandTeam of Rivals: The Political Genius of Abraham LincolnRating: 4.5 out of 5 stars4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealFrom EverandOn Fire: The (Burning) Case for a Green New DealRating: 4 out of 5 stars4/5 (74)
- The Unwinding: An Inner History of the New AmericaFrom EverandThe Unwinding: An Inner History of the New AmericaRating: 4 out of 5 stars4/5 (45)
- Chapter 3 - Drug Information ResourcesDocument31 pagesChapter 3 - Drug Information Resourcesreham O100% (1)
- The Futility of PsychotherapyDocument16 pagesThe Futility of Psychotherapywturner65100% (1)
- Beethoven Piano Sonata Op. 57 N. 23Document29 pagesBeethoven Piano Sonata Op. 57 N. 23GiancarloNo ratings yet
- Mycosis Fungoides and Sézary Syndrome: SeminarDocument13 pagesMycosis Fungoides and Sézary Syndrome: Seminarapi-26302710No ratings yet
- Terapia Sistémica en Carcinoma Metastásico de Colon Y Recto: Mauricio Lema Medina MDDocument14 pagesTerapia Sistémica en Carcinoma Metastásico de Colon Y Recto: Mauricio Lema Medina MDapi-26302710No ratings yet
- Letters: Epigenetic Silencing of Tumour Suppressor Gene p15 by Its Antisense RNADocument6 pagesLetters: Epigenetic Silencing of Tumour Suppressor Gene p15 by Its Antisense RNAapi-26302710No ratings yet
- Nature 07385Document8 pagesNature 07385api-26302710No ratings yet
- For Refractory Cutaneous T-Cell Lymphoma (CTCL) Phase 2 Trial of Oral Vorinostat (Suberoylanilide Hydroxamic Acid, SAHA)Document10 pagesFor Refractory Cutaneous T-Cell Lymphoma (CTCL) Phase 2 Trial of Oral Vorinostat (Suberoylanilide Hydroxamic Acid, SAHA)api-26302710No ratings yet
- Ncologist: R I FDADocument7 pagesNcologist: R I FDAapi-26302710No ratings yet
- Sutent GistDocument10 pagesSutent Gistapi-26302710No ratings yet
- CaScreening2009 01Document16 pagesCaScreening2009 01api-26302710No ratings yet
- Guias para Administrar en Forma Segura Altas Dosis de Interleukina 2007Document2 pagesGuias para Administrar en Forma Segura Altas Dosis de Interleukina 2007api-26302710No ratings yet
- Aldesleukin For Injection RX Only: DescriptionDocument16 pagesAldesleukin For Injection RX Only: Descriptionapi-26302710No ratings yet
- Controversiesinthemanagementof Relapsedandprimaryrefractory Hodgkin'SlymphomaDocument8 pagesControversiesinthemanagementof Relapsedandprimaryrefractory Hodgkin'Slymphomaapi-26302710No ratings yet
- Ca Screening 2008Document20 pagesCa Screening 2008api-26302710No ratings yet
- Lysosomal Storage Disease 2: SeriesDocument12 pagesLysosomal Storage Disease 2: Seriesapi-26302710No ratings yet
- Gem Cis RTin Ca CervixDocument3 pagesGem Cis RTin Ca Cervixapi-26302710No ratings yet
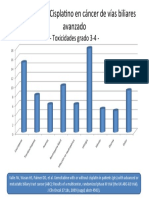
- Gem Cis ABC02Document1 pageGem Cis ABC02api-26302710No ratings yet
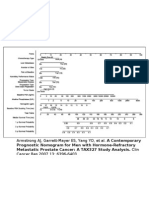
- HRPC Nomogram97Document1 pageHRPC Nomogram97api-26302710No ratings yet
- Molecular Targeted Therapy of Cancer: Brain TumorsDocument33 pagesMolecular Targeted Therapy of Cancer: Brain Tumorsapi-26302710No ratings yet
- Post-Operative Discharge ChecklistDocument1 pagePost-Operative Discharge ChecklistJunizar fzNo ratings yet
- Healing MagicDocument96 pagesHealing MagicDrAjey Bhat100% (20)
- Verification of Feeding Tube PlacementDocument4 pagesVerification of Feeding Tube Placementbilliam123No ratings yet
- Bakri: Tamponade Technique For Postpartum HemorrhageDocument2 pagesBakri: Tamponade Technique For Postpartum HemorrhageNoamen Graa100% (1)
- Decreased Cardiac OutputDocument3 pagesDecreased Cardiac OutputCristina L. JaysonNo ratings yet
- PATHOPHYSIOLOGY LAB - Hanbook of Pathophysiology SevastreDocument192 pagesPATHOPHYSIOLOGY LAB - Hanbook of Pathophysiology Sevastredorina0101No ratings yet
- Infographic Anaemia PDFDocument1 pageInfographic Anaemia PDFBarikahidayah barikahidayahNo ratings yet
- Blood Circulation and TransportDocument3 pagesBlood Circulation and TransportSselvi SubramoniamNo ratings yet
- Module 3 - Emergency Action PrinciplesDocument7 pagesModule 3 - Emergency Action PrinciplesRonald Michael QuijanoNo ratings yet
- Linx UpdatedDocument4 pagesLinx UpdatedDr.Ramkaran SainiNo ratings yet
- AsiaPCR2014 Programme FinalDocument56 pagesAsiaPCR2014 Programme Finalmohitmakkar.mmNo ratings yet
- Osteogenesis ImperfectaDocument6 pagesOsteogenesis Imperfectamiss RN100% (2)
- Acute Liver Failure EASL CPGDocument57 pagesAcute Liver Failure EASL CPGRicky Cornelius Tarigan0% (1)
- Meeting Briefing DocumentDocument53 pagesMeeting Briefing DocumentErin O'BrienNo ratings yet
- Reading Materials in Thoracic SurgeryDocument5 pagesReading Materials in Thoracic SurgeryPradeepNo ratings yet
- TRACHEOSTOMY and Wound CareDocument9 pagesTRACHEOSTOMY and Wound CareSUREEN MAY ANG REGULARNo ratings yet
- SSPEDocument8 pagesSSPEJanellah batuaan100% (1)
- Lumbar StenosisDocument104 pagesLumbar StenosismohamedwhateverNo ratings yet
- SpironolaktoneDocument2 pagesSpironolaktoneReza Ervanda ZilmiNo ratings yet
- Trauma: Dr. Hasanain Abdulammer JasimDocument41 pagesTrauma: Dr. Hasanain Abdulammer Jasimميمونه عبد الرحيم مصطفىNo ratings yet
- Robbart Van LinschotenDocument234 pagesRobbart Van LinschotenAtiKa YuLiantiNo ratings yet
- Sporotrichosis Outbreak Due ToDocument13 pagesSporotrichosis Outbreak Due ToChristian ValdésNo ratings yet
- B2B Proposal DeckDocument23 pagesB2B Proposal Deckdhika asahimasNo ratings yet
- BPH PDFDocument7 pagesBPH PDFJody FelizioNo ratings yet
- Thorax InjuryDocument55 pagesThorax Injuryrinadi_aNo ratings yet
- Osteopathic Manipulative Treatment For Low Back Pain. A Systematic Review and Meta-Analysis of Randomized Controlled TrialsDocument12 pagesOsteopathic Manipulative Treatment For Low Back Pain. A Systematic Review and Meta-Analysis of Randomized Controlled TrialsPaola GuerraNo ratings yet
- 2021 FIRST SEM BR - CebuDocument17 pages2021 FIRST SEM BR - CebuPatdeo CaacbayNo ratings yet
- Home Remedies For Ringworm - 11 Natural TreatmentsDocument11 pagesHome Remedies For Ringworm - 11 Natural TreatmentsHenz FreemanNo ratings yet