Professional Documents
Culture Documents
EOVSAB
Uploaded by
Robert KerwickOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
EOVSAB
Uploaded by
Robert KerwickCopyright:
Available Formats
1
Evaluation of Oxygenation, Ventilatory Status, and Acid-
Base Balance
REVIEW OF ARTERIAL BLOOD GASES
The analysis of arterial blood gases (ABGs) provides valuable information about a patients
oxygenation and ventilatory and acid-base status. Table 1 presents the normal values for arterial
and mixed venous blood measurements. Blood gas results are often a vital part of the assessment
and management of a mechanically ventilated patient, but they should be used with caution.
A detailed explanation of the interpretation of oxygenation status and acid-base balance is
beyond the scope of this text; the reader is assumed to have a basic understanding of ABG
interpretation. Several of the references listed at the end of this chapter provide sources for
review of the subject.
1-14
Methods for noninvasive evaluation of oxygenation and ventilation are
reviewed in Chapter 10 and also are available in other references.
15
This review provides tables, figures, and boxes that can be used as resources as the reader
progresses through the each tab or section. In addition, various approaches to the interpretation
of ABG results in the clinical setting are provided.
The American Association for Respiratory Care (AARC) has established a clinical practice
guideline (CPG) for blood gas analysis and hemoximetry.
16
The CPG provides information about
indications, contraindications, hazards and complications, limitations of the procedure, validation
of results, assessment of need, assessment of test quality, resources, and infection control in
ABG sampling and analysis. AARC also has created a CPG for capillary blood gas sampling for
neonatal and pediatric patients.
17
An exercise at the end of this review allows readers to test their ability to interpret ABG results.
2
Table 1: Normal Arterial and Venous Blood Gas Values
*
Parameter Arterial Value Venous Value
Dissolved CO2 (mL/dL) 1.2 1.5
Combined CO2 (mL/dL) 24.0 27.1
Total CO2 (mL/dL) 25.2 28.6
PCO2 (mm Hg) 40 46
pH 7.40 7.37
3
HCO
(mEq/L)
24 21
Base excess (mEq/L) 2 2
PO2 (mm Hg) 90 40
SO2 (%) 97 75
Dissolved O2 (vol%) 0.3 0.12
Combined O2 (vol%) 19.5 14.7
Total O2 (vol%) 19.8 14.82
*
Sea level, ambient air conditions, average value for a young adult. Ranges not included.
EVALUATING OXYGENATION
Evaluating blood levels of oxygen is essential for the assessment of critically ill patients. A
variety of parameters are used to assess oxygen status. Table 2 provides a list of these
components and their normal values, including the PaO
2
, SaO
2
, and CaO
2
. Box 1 presents the
equations for calculating parameters not directly measured, such as the CaO
2
.
As shown in Table 2, the normal PaO
2
is 80 to 100 mm Hg. This value can be affected by other
factors, such as age. A normal PaO
2
based on age is described by the following equation
18
:
PaO
2
= 104.2 (0.27 Age)
In the clinical setting, the following equation can be used as a simple estimate of the PaO
2
:
PaO
2
= 105
4
1
Age in years (see Case Study 1)
Altitude affects the PaO
2
by altering the inspired oxygen pressure.
(NOTE: The F
I
O
2
does not change with altitude. The barometric pressure changes, thus reducing
the P
I
O
2
as a person travels from sea level to higher altitudes. Table 4 provides estimated values
for the P
A
O
2
and PaO
2
based on altitude.
19,20
For practitioners working at higher elevations, this
is valuable information when interpreting a patients oxygenation status.)
3
Box 1: Equations Used to Calculate Oxygenation Status
Alveolar air equation (calculation of alveolar PO
2
, P
A
O
2
):
where P
A
O
2
= alveolar partial pressure of oxygen (mm Hg)
F
I
O
2
= inspired oxygen fraction
P
B
= barometric pressure (mm Hg)
PH
2
O = water vapor pressure (at 37C = 47 mm Hg)
R = respiratory quotient (
.
V
CO
2
/
.
V
O
2
; R of 0.8 is commonly used)
With an F
I
O
2
0.6 (low value), the effect of R on the P
A
O
2
is small.
To estimate the P
A
O
2
for F
I
O
2
values <0.6: P
A
O
2
= F
I
O
2
(P
B PH
2
O) (1.25 PaCO
2
)
Partial pressure of inspired oxygen: P
I
O
2
= F
I
O
2
(P
B
PH
2
O)
Oxygen content (CaO
2
): CaO
2
= [%Sat Hb 1.34] + (PO
2
0.003 mL/dL)
Oxygen consumption (
.
V O
2
):
.
V O
2
= Cardiac output (CO) (CaO
2
C
v O
2
)
Oxygen delivery (DO
2
): DO
2
= CO CaO
2
Pulmonary shunt
,
_
T
.
S
.
Q Q :
T
.
S
.
Q Q
=
) vO C CcO (
) CaO CcO (
2 2
2 2
where
S
.
Q
is the shunted portion of the cardiac output,
T
.
Q
is total cardiac output, CcO
2
is the
content of oxygen of the pulmonary end-capillary, CaO
2
is the arterial O
2
content, and C
v O
2
is the mixed venous oxygen content. CcO
2
is calculated on the assumption that the pulmonary
end-capillary PO
2
is the same as the P
A
O
2
. Mixed venous blood can be obtained from a
pulmonary artery catheter.
4
Table 2: Measures and Values Used in the Evaluation of Oxygenation Status
Term Abbreviation Average Normal Value
Partial pressure of arterial oxygen PaO
2
80-100 mm Hg
Partial pressure of mixed venous oxygen
P
v O
2
40 mm Hg
Alveolar partial pressure of oxygen P
A
O
2
100-673 mm Hg
F
I
O
2
range: 0.21-1.0
Alveolar-arterial oxygen tension gradient P(A-a)O
2
5-10 mm Hg (F
I
O
2
=
0.21)
30-60 mm Hg (F
I
O
2
=
1.0)
Ratio of PaO
2
to fractional inspired oxygen
(PaO
2
range = 80-100 mm Hg; F
I
O
2
= 0.21)
PaO
2
/F
I
O
2
380-475
Ratio of PaO
2
to partial pressure of alveolar
oxygen (PaO
2
range = 80-100 mm Hg; F
I
O
2
=
0.21)
PaO
2
/P
A
O
2
0.8-1.0
Saturation of arterial oxygen SaO
2
97%
Saturation of mixed venous oxygen
S
v O
2
75%
Oxygen content of arterial blood CaO
2
20 vol%
Oxygen content of mixed venous blood
C
v O
2
15 vol%
Arterial-to-mixed venous oxygen content
difference
[C(a
v )O
2
]
3.5- 5 mL/dL
Oxygen delivery DO
2
1000 mL/min
Oxygen consumption
.
V
O
2
250 mL/min
Two terms frequently used to describe low oxygen levels are hypoxia and hypoxemia. Hypoxia
refers to lower than normal oxygen pressure in the tissues or alveoli. Hypoxemia describes a low
arterial blood oxygen pressure (<80 mm Hg).
13
Table 3 lists the criteria used to establish the
degree of hypoxia and hypoxemia.
Table 3: Levels of Hypoxemia
Level* PaO
2
Value PaO
2
Range Saturation (SaO
2
)
Mild hypoxemia <80 mm Hg 60 to 79 mm Hg 90% to 94%
Moderate hypoxemia <60 mm Hg 40 to 59 mm Hg 75% to 89%
Severe hypoxemia <40 mm Hg <40 mm Hg <75%
*
Values given are for a young adult and room air. (NOTE: The levels of hypoxemia may be
defined differently, depending on the author or institution.)
Types of hypoxia and their causes include the following
13
:
Hypoxemic hypoxia (lower than normal PaO
2
) (See Table 3.)
5
Anemic hypoxia (lower than normal red blood cell count [anemia], abnormal hemoglobin,
carboxyhemoglobin)
Circulatory hypoxia (reduced cardiac output, decreased tissue perfusion)
Histotoxic hypoxia (cyanide poisoning)
Affinity hypoxia (reduced release of O
2
from hemoglobin to the tissues [e.g., fetal
hemoglobin])
Causes of hypoxemia include the following:
Hypoventilation (increased CO
2
resulting from neuromuscular disorders, chronic increased
work of breathing, depression of the respiratory centers)
Reduced inspired oxygen (high altitudes, low F
I
O
2
)
Shunt (atelectasis, pulmonary edema, pneumonia, acute respiratory distress syndrome
[ARDS])
Diffusion defects (pulmonary resection, emphysema, pulmonary fibrosis)
Poor distribution of ventilation (obstructed airways, bronchospasm)
Table 4: Calculated Changes in Alveolar and Arterial PO
2
with Altitude, with and without
Changes in Alveolar Ventilation
Altitude (feet) P
B
* (mm Hg) P
A
O
2
(mm Hg) PaO
2
(mm Hg) P
A
O
2
(mm
Hg)
(PaCO
2
variable)
PaO
2
(mm
Hg)
(PaCO
2
= 40 mm Hg)
Sea level 760 101.7 91.7 101.7 (PaCO
2
= 40
mm Hg)
91.7
5000 650 78.6 68.6 84.6 (PaCO
2
= 35
mm Hg)
74.6
10,000 540 55.5 45.5 67.5 (PaCO
2
= 30
mm Hg)
57.5
15,000 430 32.4 22.4 50.4 (PaCO
2
= 25
mm Hg)
40.4
20,000 360 17.7 7.7 41.7 (PaCO
2
= 20
mm Hg)
31.7
25,000 280 0.9 0 36.9 (PaCO
2
= 10
mm Hg)
26.9
Modified from Kacmarek RM, Hess D, Stoller JK: Monitoring in respiratory care, Chicago,
1993, Mosby.
P
B
, Barometric pressure; P
A
O
2
, alveolar PO
2
, calculated from the alveolar air equation; PaO
2
,
arterial PO
2
, assuming P
A
O
2
PaO
2
= 10 mm Hg.
*
P
B
is an approximate relative to altitude, because it varies with climatic conditions.
6
EVALUATING THE TRANSFER AND UPTAKE OF OXYGENP(A-a)O
2
, PaO
2
/P
A
O
2
,
AND PaO
2
/F
I
O
2
P(A-a)O
2
The ability of the lungs to bring in and transfer oxygen to the alveolar capillaries is described by
the alveolar-arterial oxygen tension gradient (P[A-a]O
2
) (see Table 2 and Box 1). The normal
P(A-a)O
2
is about 5 mm Hg at the age of 20 and increases with age.
12
As shown in the equation
in Box 1, the P
A
O
2
changes with the F
I
O
2
. Because calculating the P
A
O
2
is cumbersome, Table 5
lists P
A
O
2
values for commonly used F
I
O
2
values.
Table 5: Changes in P
A
O
2
with Changes in F
I
O
2
*
F
I
O
2
P
A
O
2
0.21 100
0.35 200
0.40 235
0.50 307
0.60 388
0.70 459
0.80 530
0.90 602
1.00 673
*
Using the equations P
A
O
2
= F
I
O
2
(P
B
PH
2
O) (1.25 PaCO
2
) and P
A
O
2
= F
I
O
2
(760 47 mm
Hg) (1.25 40 mm Hg). With an F
I
O
2
0.6, the factor 1.25 is not used.
Changes in the lung that reduce its ability to transfer oxygen from the alveolus to the pulmonary
capillary (e.g., aging, lung disease) cause the PaO
2
to drop in relation to the available oxygen
(P
A
O
2
), just as the P(A-a)O
2
is increased under abnormal conditions, such as entilation/perfusion
abnormalities (
. .
Q V
), shunt, and diffusion defects. (See Appendix B in text for a review of
these concepts.)
PaO
2
/P
A
O
2
Some clinicians use the ratio of arterial-to-alveolar oxygen tension (PaO
2
/P
A
O
2
) to evaluate the
transfer of oxygen from the lungs to the pulmonary circulation. The PaO
2
/P
A
O
2
ratio should
remain stable with changes in the F
I
O
2
. The ratio basically is a statement of the question, What
fraction of the oxygen is getting to the artery (PaO
2
) compared with the amount available in the
alveolus (P
A
O
2
)? A normal ratio for a PaO
2
of 90 mm Hg and a P
A
O
2
of 100 mm Hg (F
I
O
2
=
0.21) is 0.9 (PaO
2
/P
A
O
2
= 90/100 = 0.9). This value shows that 90% of the O
2
available in the
alveolus is moving into the capillary. A ratio less than 0.75 indicates a pulmonary problem, such
as a shunt, ventilation/perfusion abnormality, or diffusion defect. For example, the ratio of a
PaO
2
of 50 mm Hg and a P
A
O
2
of 673 mm Hg (100% O
2
) is 0.07. This suggests that only 7% of
the oxygen (100 0.07) is moving from the alveolus into the blood.
7
PaO
2
/F
I
O
2
A simpler clinical parameter is the PaO
2
/F
I
O
2
ratio, sometimes called the P-to-F ratio. This ratio
does not require the calculation of the P
A
O
2
but still describes the amount of oxygen moving into
the blood in relation to the amount inspired (F
I
O
2
). The PaO
2
/F
I
O
2
ratio often is used to describe
the degree of lung injury. A PaO
2
/F
I
O
2
ratio of 200 or lower indicates ARDS. A PaO
2
/F
I
O
2
ratio
of 200 to 300 indicates acute lung injury (ALI). (The normal range for the PaO
2
/F
I
O
2
ratio is 380
to 476 [80 mm Hg/0.21 = 380; 100 mm Hg/0.21 = 476]). A severely low PaO
2
/F
I
O
2
is any value
below 100. Example: 50 mm Hg/1.0 = 50 mm Hg.)
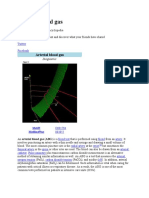
Oxyhemoglobin Dissociation Curve
The oxyhemoglobin dissociation curve (OHDC) describes the relationship of the oxygen tension
to the percent saturation of hemoglobin with oxygen. Table 6 shows the relation of specific O
2
saturation values to specific PO
2
values. Figure 1 shows the OHDC and the ways various factors
can affect hemoglobins ability to pick up oxygen as the PO
2
changes.
Fig. 1 The oxyhemoglobin dissociation curve with normal values and showing the effects of changes in pH
(hydrogen ion concentration), PCO2, temperature, 2,3-diphosphoglycerate, and various hemoglobin types on the
curve. (Redrawn from Lane EE, Walker JF: Clinical arterial blood gas analysis, St Louis, 1987, Mosby.)
8
The following factors cause a right shift in the curve:
Hyperthermia (increased temperature)
Hypercapnia (increased PCO
2
)
Acidosis (increased hydrogen ion concentration)
Increased 2,3-diphosphoglycerate (2,3 DPG)
Certain abnormal hemoglobins
Factors that cause a left shift in the curve include the following:
Hypothermia (decreased temperature)
Hypocarbia (decreased PCO
2
)
Alkalosis (decreased hydrogen ion concentration)
Decreased 2,3 DPG
Carbon monoxide poisoning
Fetal hemoglobin
Right shifting of the curve decreases the attraction of hemoglobin and oxygen and promotes
unloading of oxygen. Left shifting of the curve increases the attraction of hemoglobin and
oxygen and promotes the binding of oxygen.
Shifting of the curve to the right or left of normal affects the partial pressure of oxygen required
to produce 50% saturation of hemoglobin. In other words, the P
50
(PaO
2
at 50% saturation)
changes as the curve shifts. The P
50
at a normal pH is 27 mm Hg. In Figure 1 the P
50
is 20 mm
Hg when the curve is left shifted and about 32 mm Hg when the curve is right shifted.
Although the y, or vertical axis, of the OHDC usually is represented as percent saturation of
hemoglobin, it also can be represented as arterial oxygen content (CaO
2
).
Table 6: Hemoglobin Saturation and Its Approximate PO
2
Value at Normal pH
Saturation PO
2
(mm Hg)
50% 27 (P
50
at normal pH)
75%
40 (mixed venous saturation and P
v O
2
)
90% 60
97% 80-100 (normal arterial values)
Oxygen Content
Clinicians often place too much importance on PaO
2
and SaO
2
values without looking at the
patients hemoglobin level. The CaO
2
and the amount of oxygen delivered to the tissues
determine the amount of oxygen available for utilization at the tissue level. O
2
delivery (DO
2
) is
the product of both cardiac output and arterial oxygen content (see Box 1). Figure 2 shows how
the CaO
2
decreases as the level of hemoglobin decreases. Patients with severe anemia are at great
risk of inadequate oxygen delivery, and patients with a low cardiac output are at similar risk.
Even when the CaO
2
is adequate, if it is not delivered to the tissues, the tissues will not receive
adequate amounts of oxygen
9
Figure 2
Fig. 2 The relationship between the CaO2 and PaO2 as a function of blood hemoglobin (Hb) concentrations.
Progressive decreases in Hb cause large drops in the CaO2. (From Wilkins RL, Kacmarek B, Stoller JK: Egans
fundamentals of respiratory care, ed 9, St Louis, 2009, Mosby.)
Pulmonary Shunt
A shunt exists when perfusion in the lungs occurs without gas exchange. A pulmonary shunt is
the part of the blood that leaves the right side of the heart and passes through the lungs to the left
side of the heart without participating in any gas exchange (Box 1 shows the shunt equation).
The calculation of shunt provides a value that represents the percentage of cardiac output that is
not exposed to ventilated alveoli. Normal anatomical shunt is about 2% to 3% of the cardiac
output and is present in all individuals. As the percentage of shunt increases, the PaO
2
decreases
and hypoxemia results. Shunts exceeding 30% are associated with a high mortality rate. Shunt
effects can be caused by such disorders as atelectasis, pulmonary edema, pneumonia,
pneumothorax, and complete airway obstruction (see Appendix B of text).
10
VENTILATION
EVALUATING VENTILATORY STATUS
CHANGES IN ALVEOLAR VENTILATION ASSOCIATED WITH CHANGES IN P
A
O
2
AND P
A
CO
2
Under normal circumstances, alveolar ventilation provides air to the alveoli at a rate of about 4 to
5 L/min (Box 2). At this level, enough gas exchange can occur in the lung to keep ABG values
within a normal range. The relationship of alveolar ventilation to alveolar partial pressures of
oxygen and carbon dioxide is illustrated by the graph in Figure 3. Note that the P
A
O
2
and P
A
CO
2
values are normal with an alveolar ventilation of about 4.5 L/min.
Figure 3
Fig. 3 The effect of changes in alveolar ventilation on the alveolar gases PAO2 and PACO2. (See the text for further
explanation.)
11
As alveolar ventilation increases, the alveolar carbon dioxide tension (P
A
CO
2
) decreases until it
plateaus at about 15 to 20 mm Hg. Hyperventilation also increases the alveolar partial pressure of
oxygen (P
A
O
2
) above normal. The P
A
O
2
plateaus at approximately 120 mm Hg when a person
breathes room air. With hypoventilation a reduction in alveolar ventilation occurs, resulting in a
rise in the P
A
CO
2
and a fall in the P
A
O
2
.
Under normal circumstances, the P
A
CO
2
is approximately equal to the PaCO
2
(40 mm Hg), with
the P v CO
2
slightly higher at 45 mm Hg. When ventilation is inadequate, CO
2
rises above its
normal value in the alveoli (see Figure 3). As carbon dioxide increases, the carbon dioxide
molecules displace oxygen molecules in the alveoli. Thus the P
A
O
2
decreases, and less oxygen is
available to diffuse across the alveolar-capillary membrane. Therefore, changes in the P
A
CO
2
affect the PaO
2
. This relationship is illustrated by Figure 3 and is best described by the alveolar
air equation (see Box 1). The equation assumes that the PaCO
2
is equal to the P
A
CO
2
. A
simplified form of the alveolar air equation is: P
A
O
2
= P
I
O
2
(PaCO
2
1.25), where P
I
O
2
is the
partial pressure of inspired oxygen (see Box 1). This is an easy formula to use when quick
clinical evaluation of ABGs is needed and a calculator is not readily available. It is more
accurate if the patient is receiving a low F
I
O
2
(<0.6).
At sea level (760 mm Hg) and at a normal F
I
O
2
of 0.21 with a water vapor pressure of 47 mm Hg
(saturated at 37C), the P
I
O
2
is 149 mm Hg, based on the equation P
I
O
2
= F
I
O
2
(P
B
47) = 0.21
(760 47), where P
B
is the barometric pressure. Using the simplified version of the alveolar air
equation, P
A
O
2
= P
I
O
2
(1.25 PaCO
2
), when the PaCO
2
is 40 mm Hg, the alveolar PO
2
(P
A
O
2
)
is 99 mm Hg [149 (1.25 40)].
As the PaCO
2
rises due to hypoventilation, the P
A
O
2
falls. For example, if the PaCO
2
is 80 mm
Hg, the P
A
O
2
is 149 (80 1.25), or 49 mm Hg. When this occurs, less oxygen is present in the
alveoli. As a result, less oxygen is available to the blood and tissues.
During hyperventilation the P
A
O
2
increases because of the drop in the PaCO
2
. For example, if the
PaCO
2
is 20 mm Hg and the P
I
O
2
is 149 mm Hg, the P
A
O
2
is 149 (1.25 20), or 124 mm Hg.
Because more oxygen is now available in the alveoli, more oxygen can be delivered to the
Box 2: Calculation of Alveolar Ventilation
Per breath: Alveolar ventilation in one breath (V
A
) equals tidal volume (V
T
) minus dead space
(V
D
), which normally is considered to equal anatomical dead space: V
A
= V
T V
D
.
Per minute: Alveolar ventilation per minute (
.
A
V
) equals tidal volume minus dead space
multiplied by the respiratory rate: (V
T
V
D
) f =
.
A
V
, where f is the respiratory rate.
Also: Minute ventilation minus dead space ventilation in 1 minute equals alveolar ventilation in 1
minute:
E
.
V
D
.
V
=
A
.
V
, where
E
.
V
is the minute ventilation (V
T
respiratory rate [f]) and
D
.
V
is the dead space ventilation per minute (V
D
f).
12
arterial blood. (This assumes that the level of shunting and diffusion is normal and that no other
pathological conditions are present that would cause hypoxemia.)
In general, as the PaCO
2
increases by 1 mm Hg, the PaO
2
decreases by 1.25 mm Hg.
21
For
example, if the PaCO
2
increases from 40 to 50 mm Hg, a PaO
2
of 100 mm Hg decreases to about
88 mm Hg (Table 7).
Table 7: Effect of PaCO
2
on PaO
2
*
PaCO
2
(mm Hg) P
A
O
2
(mm Hg) PaO
2
(mm Hg)
40 97 87
64 67 57
80 47 37
*
Patient with a normal P(A-a)O
2
of 10 mm Hg breathing room air.
ALVEOLAR VENTILATION, PaCO
2
, AND
.
V CO
2
A relationship exists among the arterial pressure of carbon dioxide (PaCO
2
), the amount of
carbon dioxide produced (
.
V
CO
2
), and the alveolar ventilation (
.
A
V
). Cellular metabolism
produces CO
2
, and the lungs are the primary organs for removing it. The following formula
describes the amount produced and how well CO
2
is removed by the lungs to achieve a given
PaCO
2
:
<equation>
.
A
2
.
2
2
) V ( n ventilatio Alveolar
) CO V ( production CO
PaCO
Using
.
V
CO
2
in milliliters per minute and
.
A
V
in liters per minute, this equation can be
rewritten as
.
A
2
.
2
V
) CO V ( 0.863
PaCO
where 0.863 is a correction factor for
.
A
V
reported in liters per minute, body temperature and
pressure, saturated (BTPS) and the
.
V
CO
2
reported in milliliters per minute, standard
temperature and pressure, dry (STPD).
For example, if the
.
A
V
is 4.5 L/min and the
.
V
CO
2
is normal (200 mL/min), the PaCO
2
is 38 mm
Hg. If the alveolar ventilation is half of normal (2.25 L/min) and the
.
V
CO
2
is normal, the
PaCO
2
would be calculated as follows:
13
Hg mm 7 . 76
min / L 25 . 2
mL/min 200 0.863
PaCO
2
Therefore, when alveolar ventilation is halved, the PaCO
2
approximately doubles. Minute
ventilation and alveolar ventilation are similar in their effects on the PaCO
2
, as long as dead
space volume remains constant. Table 8 presents additional examples of expected PaCO
2
values
as
E
.
V
changes in a normal, resting individual.
13
Table 8: Expected PaCO
2
Based on Minute Ventilation
*
in Normal Individuals
Minute Ventilation P
A
CO
2
(mm Hg) PaCO
2
(mm Hg)
4 times normal 20 15-25
2 times normal 30 25-35
Normal 40 35-45
*
Note that this is minute ventilation, not alveolar ventilation.
14
ACID-BASE BALANCE
CHANGES IN pH, PaCO
2
, AND SODIUM BICARBONATE
As the arterial partial pressure of CO
2
increases, the level of acid in the blood also increases. The
pH becomes more acidotic and has a lower numerical value. The advantage of knowing the pH
and PaCO
2
values is that this information allows evaluation of a patients condition and
determination of the cause of the instability in these variables. The relationship of the pH, the
PaCO
2
(mm Hg), and the bicarbonate level (mEq/L) can be described by the Henderson-
Hasselbalch equation:
pH = pK + log[(
3
HCO )/(H
2
CO
3
)]
The equation can be simplified into the following form
13
:
) L / mEq ( HCO
) Hg mm ( PaCO 24
] H [
3
2
where [H
+
] is the hydrogen ion concentration in nanomoles per liter (nmol/L) and 24 is
derived from the dissociation constant for carbonic acid. Table 9 provides values for the
hydrogen ion concentration for a given pH. Once the [H
+
] has been calculated, the pH can be
determined from Table 9 For example, if the PaCO
2
is 50 mm Hg and the
3
HCO is 24
mEq/L, the pH is calculated as follows:
L / nM 50
24
50 24
] H [
+
If the hydrogen ion concentration is 50 nM/L, the pH is close to 7.30.
Bicarbonate can also be calculated by rearranging the equation:
3
2
HCO
PaCO 24
] H [
] H [
PaCO 24
] HCO [
2
3
+
If the pH is 7.40 and the PaCO
2
is 50 mm Hg, the bicarbonate is 30 mEq/L (see Table 9for
the nanomole concentration for [H
+
] when the pH is 7.40):
] H [
PaCO 24
] HCO [
2
3
+
L / mEq 30
40
Hg mm 50 24
] HCO [
3
Remember that these determinations are estimations of the actual value. They can be useful
in clinical situations for a quick determination of a patients bicarbonate, pH, and PaCO
2
15
values when two of the factors are known. Table 10 lists examples of common ABG
abnormalities. Figure 4 presents a blood gas flow chart (algorithm) that reviews the mental
process required to interpret a set of ABG results.
The following is another common method of applying the Henderson-Hasselbalch equation:
pH = pK
a
+ log[(
3
HCO )/(H
2
CO
3
)]
where pK is 6.1, the dissolved CO
2
is calculated (PCO
2
0.03), and the values are substituted
into the equation. For example, using normal values:
1
]
1
+
) 03 . 0 40 (
) L / mEq 24 (
log 1 . 6 pH
= 6.1 + log (20/1)
= 6.1 + 1.3
= 7.40 (normal pH)
Table 9: Relationship Between pH and Hydrogen Ion [H
+
] Concentration
pH Approximate [H
+
] (nmol/L)
8.0 10
7.8 16
Alkalosis 7.7 20
7.6 26
7.5 32
Normal 7.4 40
7.3 50
Acidosis 7.2 63
7.1 80
7.0 100
6.9 125
16
Table 10: Examples of Common Arterial Blood Gas Abnormalities
Conditions pH PaCO
2
(mm Hg)
3
HCO
(mEq/L)
PaO
2
*
(mm
Hg)
Possible Causes
Normal 7.35-7.45 35-45 24-28 80-100 Normal ventilation without
pulmonary pathology
RESPIRATORY
Acute acidosis 7.0-7.34 >45 24-28 80 Hypoventilation, sedation, drug
overdose, cardiopulmonary arrest,
chest trauma, pneumothorax,
central nervous system (CNS)
trauma, restrictive pulmonary
disease
Chronic acidosis
(compensated)
7.35-7.40 >45 30-48 <80 Hypoventilation, chronic
obstructive pulmonary disease
(COPD), chronic neuromuscular
disease, muscle wasting, late CNS
injury
Acute alkalosis 7.42-7.70 <35 24-28 >80 Increased alveolar ventilation,
hypoxemia (if PaO
2
is low), pain,
anxiety, mechanical ventilation,
encephalitis, cirrhosis of the liver,
pulmonary emboli (if PaO
2
is low),
severe infection, fever, salicylate
intoxication
Chronic alkalosis
(compensated)
7.41-7.45 <35 12-24 80-100 Long-term mechanical ventilatory
support with increased alveolar
ventilation
METABOLIC
Acute acidosis 7.0-7.34 35-46 12-22 80-100 Ketoacidosis (alcoholic, starvation,
diabetic), uremic acidosis (failure of
renal acid excretion), loss of
3
HCO
(diarrhea), renal loss of
base (carbonic anhydrase inhibitors
[Diamox], renal tubular acidosis),
overproduction of acid (lactic
acidosis), conversion of toxins to
acids (methanol, ethylene glycol,
salicylate)
Compensated 7.35-7.40 <35 12-22 >80 Respiratory compensation for
17
acidosis metabolic acidosis as with diabetic
acidosis and lactic acidosis
Acute alkalosis 7.42-7.70 35-46 30-48 80-100
3
HCO
ingestion or administration
of bicarbonate, vomiting (acid loss),
gastrointestinal (GI) suction (acid
loss), diuretic-induced K
+
or Cl
loss, steroids, licorice ingestion
Compensated
alkalosis
7.41-7.45 >45 30-48 <80 Primary hypokalemic metabolic
alkalosis with dehydration/azotemia
(rare)
*
Assuming no pulmonary pathology other than respiratory hypoventilation and no therapeutic
oxygen
CHANGES IN pH CAUSED BY CHANGES IN PaCO
2
Table 11 provides another method that can help clinicians evaluate the relationship between the
PaCO
2
level and the pH.
13
This method can be used to determine whether changes in pH are
reflections of changes in the PaCO
2
or are due to metabolic changes. For example, a PaCO
2
of 80
mm Hg is 40 mm Hg above the normal of 40 mm Hg. The pH would decrease by about 0.2 and
would be equal to about 7.20 if the change were due to hypoventilation. During hyperventilation,
if the PaCO
2
is 20 mm Hg, or 20 mm Hg less than normal, then the expected pH would be 7.60.
If the actual pH is 7.50, not 7.60, the pH is not entirely due to ventilatory changes. This situation
suggests respiratory alkalosis with metabolic acidosis. Again, this relationship is an estimate
intended to aid rapid clinical assessment of the patient. (NOTE: Buffers make it more difficult for
the blood to become acidotic; therefore, the CO
2
must increase more to change the pH compared
with how much it must drop to raise the pH.)
Table 11: Relationship Between Changes in PaCO
2
and the pH
13
Given a starting PaCO
2
of 40 mm Hg, every 20 mm Hg increase in PaCO
2
decreases pH by 0.10
unit. For example:
PaCO
2
pH
3
HCO
40 mm Hg 7.40 24 mEq/L
60 mm Hg 7.30 26 mEq/L
80 mm Hg 7.20 28 mEq/L
This is true in individuals with normal blood buffers.
(NOTE: Remember that this is an approximation.)
When the PaCO
2
decreases 10 mm Hg, the pH increases by 0.10 unit.
PaCO
2
pH
3
HCO
30 mm Hg 7.50 22 mEq/L
20 mm Hg 7.60 20 mEq/L
As the PaCO
2
increases, the PaO
2
decreases.
18
CHANGES IN PLASMA BICARBONATE CAUSED BY CHANGES IN PaCO
2
7,13,22,23
The amount of change in the PaCO
2
and the
3
HCO
for an acid-base disorder can be calculated.
The following section reviews the determination of these values.
Acute Alveolar Hypoventilation
During hypoventilation, carbon dioxide is not eliminated at a normal rate through the lungs, and
CO
2
is increased. For each 10 mm Hg increase in the PaCO
2
, bicarbonate increases about 1
mEq/L. In acute changes, such as acute respiratory acidosis, the following equation can be used:
3
HCO = 0.10 PaCO
2
Where represents change. As an example, the PaCO
2
is 40 mm Hg and the
3
HCO
is 24
mEq/L. If the PaCO
2
increases to 50 mm Hg (PaCO
2
= 10), the
3
HCO
increases as
follows:
3
HCO = 0.10 PaCO
2
3
HCO = 0.10 10 = 1.0
The
3
HCO
increases from 24 to 25 mEq/L.
Acute Alveolar Hyperventilation
As the PaCO
2
decreases by 10 mm Hg with hyperventilation, bicarbonate decreases about 2
mEq/L.
13,22,23
The following equation can be used for acute respiratory alkalosis:
3
HCO = 0.2 PaCO
2
As an example of respiratory alkalosis, the PaCO
2
is 40 mm Hg and the
3
HCO
is 24 mEq/L
at the start. If the PaCO
2
decreases to 20 mm Hg (PaCO
2
= 20 mm Hg), the
3
HCO
decreases as follows:
3
HCO = 0.2 PaCO
2
3
HCO = 0.20 20 = 4.0
The
3
HCO decreases from 24 to 20 mEq/L.
Chronic Changes
If hypoventilation or hyperventilation continues for 2 to 3 days, normal kidney function helps
correct the pH and compensates by retaining or excreting bicarbonate.
Because hypoventilation produces a chronic respiratory acidosis, the kidneys compensation can
be estimated using the following equation:
3
HCO = 0.35 PaCO
2
19
In the example for acute respiratory acidosis, the PaCO
2
is 50 mm Hg and the
3
HCO is 25
mEq/L. In this example, the PaCO
2
is 10 mm Hg; therefore the equation is:
3
HCO = 0.35 10 = 3.5 mEq/L
The bicarbonate increases from 25 to about 28.5 mEq/L as the kidneys compensate and the
pH moves toward normal.
On the other hand, during chronic hyperventilation, compensation by the kidneys results in the
excretion of bicarbonate. The following equation can be used to calculate bicarbonate in chronic
respiratory alkalosis:
3
HCO = 0.5 PaCO
2
For example, if the PaCO
2
is 20 mm Hg (20 mm Hg less than normal) and the
3
HCO is 21
mEq/L, the equation becomes:
3
HCO = 0.5 20 = 10
As the kidneys compensate, the bicarbonate falls to about 11 mEq/L after a few days.
METABOLIC CHANGES IN BICARBONATE AND pH
7,22,23
Another rule of thumb can help describe the relationship between the pH and bicarbonate. When
changes in the pH are caused by metabolic rather than respiratory changes, a pH change of 0.15
is approximately equal to a change in base of 10 mEq/L.
For example, if the pH rises from 7.40 to 7.55 (an increase of 0.15) as a result of metabolic
causes, the base increases by 10 mEq/L (e.g., from a normal of 24 to 34 mEq/L). If the pH drops
from 7.40 to 7.25 (a decrease of 0.15), the expected decrease in bicarbonate would be 10 mEq/L,
to 14 mEq/L. This is true as long as the change in pH results from purely metabolic causes and
the PaCO
2
does not change.
20
REVIEW Exercises
Case Study 1
Evaluate the P(A-a)O2
A 40-year-old patient has a P(A-a)O2 of 15 mm Hg. Is this in the normal range for this patient?
Case Study 2
Oxygenation Status
A patient has a measured PaO
2
of 80 mm Hg and an SaO
2
of 97%. The hemoglobin is 10 g %.
Does this patient have a normal oxygenation status?
Case Study 3
ABG Analysis
A patient has a PaO
2
of 50 mm Hg and a PaCO
2
of 80 mm Hg. If the PaCO
2
were to decrease to a
normal of 40 mm Hg, what would you expect the PaO
2
to be after the change (assuming the PaO
2
changes were due to the PaCO
2
changes alone and not to lung pathology)?
Case Study 4
Calculate Bicarbonate
A patient has a PaCO
2
of 78 mm Hg and a pH of 7.20. Estimate the patients bicarbonate level.
Exercise 5. Interpret the Following Blood Gases
1. pH PaCO
2
PaO
2
3
HCO
7.39 44 mm Hg 89 mm Hg 25 mEq/L
2. pH PaCO
2
PaO
2
3
HCO
7.12 42 mm Hg 155 mm Hg 13 mEq/L
3. pH PaCO
2
PaO
2
3
HCO
7.25 65 mm Hg 55 mm Hg 28 mEq/L
4. pH PaCO
2
PaO
2
3
HCO
7.52 32 mm Hg 105 mm Hg 26 mEq/L
5. pH PaCO
2
PaO
2
3
HCO
7.42 33 mm Hg 102 mm Hg 21 mEq/L
6. pH PaCO
2
PaO
2
3
HCO
7.55 38 mm Hg 98 mm Hg 32 mEq/L
7. pH PaCO
2
PaO
2
3
HCO
7.37 66 mm Hg 68 mm Hg 36 mEq/L
21
8. pH PaCO
2
PaO
2
3
HCO
7.29 73 mm Hg 69 mm Hg 34 mEq/L
9. pH PaCO
2
PaO
2
3
HCO
7.33 65 mm Hg 78 mm Hg 33 mEq/L
10. pH PaCO
2
PaO
2
3
HCO
7.52 25 mm Hg 99 mm Hg 20 mEq/L
11. pH PaCO
2
PaO
2
3
HCO
7.10 99 mm Hg 22 mm Hg 30 mEq/L
12. pH PaCO2 PaO
2
3
HCO
7.32 60 mm Hg 78 mm Hg 29 mEq/L
13. pH PaCO2 PaO
2
3
HCO
7.25 24 mm Hg 110 mm Hg 9 mEq/L
14. pH PaCO
2
PaO
2
3
HCO
7.55 50 mm Hg 83 mm Hg 41 mEq/L
15. pH PaCO
2
PaO
2
3
HCO
7.51 20 mm Hg 112 mm Hg 15 mEq/L
16. pH PaCO
2
PaO
2
3
HCO
7.21 90 mmHg 45 mm Hg 35 m Eq/L
17. pH PaCO
2
PaO
2
3
HCO
7.35 46 mm Hg 44 mm Hg 25 mEq/L
18. pH PaCO
2
PaO
2
3
HCO
7.49 21 mm Hg 98 mm Hg 16 mEq/L
19. pH PaCO
2
PaO
2
3
HCO
7.38 60 mm Hg 61 mm Hg 36 mEq/L
20. pH PaCO
2
PaO
2
3
HCO
7.20 60 mm Hg 55 mm Hg 23 mEq/L
21. pH PaCO
2
PaO
2
3
HCO
7.49 43 mm Hg 98 mm Hg 33 mEq/L
22. pH PaCO
2
PaO
2
3
HCO
7.10 13 mm Hg 75 mm Hg 4 mEq/L
23. pH PaCO
2
PaO
2
3
HCO
7.58 59 mm Hg 77 mm Hg 55 mEq/L
24. pH PaCO
2
PaO
2
3
HCO
7.54 29 mm Hg 56 mm Hg 23 mEq/L
25. pH PaCO
2
PaO
2
3
HCO
7.31 60 mm Hg 75 mm Hg 30 mEq/L
26. pH PaCO
2
PaO
2
3
HCO
7.43 24 mm Hg 119 mm Hg 15 mEq/L
27. pH PaCO
2
PaO
2
3
HCO BE* SaO
2
*
22
7.43 41 mm Hg 94 mm Hg 26 mEq/L + 2 95
28. pH PaCO
2
PaO
2
3
HCO BE SaO
2
7.52 30 mm Hg 45 mm Hg 24 mEq/L + 2 86
29. pH PaCO
2
PaO
2
3
HCO BE SaO
2
7.15 80 mm Hg 80 mm Hg 27 mEq/L 0 92
30. pH PaCO
2
PaO
2
3
HCO BE SaO
2
7.20 55 mm Hg 55 mm Hg 21 mEq/L -8 79
31. pH PaCO
2
PaO
2
3
HCO BE SaO
2
7.60 40 mm Hg 85 mm Hg 39 mEq/L +10 97
32. pH PaCO
2
PaO
2
3
HCO BE SaO
2
7.54 25 mm Hg 52 mm Hg 21 mEq/L +8 90
33. pH PaCO
2
PaO
2
3
HCO BE SaO
2
7.25 65 mm Hg 39 mm Hg 28 mEq/L +15 65
34. pH PaCO
2
PaO
2
3
HCO BE SaO
2
7.39 38 mm Hg 65 mm Hg 24 mEq/L 0 92
*BE, Base excess; SaO
2
, oxygen saturation.
Exercise 6. Answer the Following Questions
1. List the normal arterial values for the following: pH, total CO
2
, PaCO
2
, CaO
2
, PaO
2
, SaO
2
.
2. Give the normal mixed venous values for the following: pH, total CO
2
,
,
,
.
3. A 95-year-old patient has a PaO
2
of 78 mm Hg on room air. How would you interpret this
result?
4. An 18-year-old patient breathing room air is evaluated in the emergency department of a
hospital in Vail, Colorado (elevation = 10,000 feet). The PaCO
2
is 30 mm Hg, and the PaO
2
is 58 mm Hg. How would you interpret the arterial oxygenation level?
5. What would be a normal value for P(A-a)O
2
in a 70-year-old patient?
6. A patient has a PaO
2
/P
A
O
2
of 0.5. How would you interpret this value?
7. A PaO
2
/F
I
O
2
ratio < 200 indicates which of the following?
a. Acute respiratory distress syndrome
b. Hypoventilation
c. F
I
O
2
>0.6
d. Acute lung injury
8. A P
50
of 20 indicates that the oxyhemoglobin dissociation curve has done which of the
following?
a. Shifted left
b. Shifted right
c. Remained in the normal position
9. A patients hemoglobin is 8 g, the SaO
2
is 97%, and the PaO
2
is 100 mm Hg. Given these
measurements, which of the following is(are) correct?
1. Normal oxygenation
2. Reduced CaO
2
23
3. Anemia
4. Low oxygen delivery to the tissues
a. 1 only
b. 2 and 3 only
c. 3 and 4 only
d. 2, 3, and 4 only
10. An excitable patient is admitted to the outpatient clinic after an emotionally traumatic event.
ABGs on room air are as follows: PaCO
2
= 20 mm Hg, PaO
2
= 110 mm Hg, SaO
2
= 99%.
What would you expect the pH to be if the blood gas changes were due to respiratory
changes? How would you interpret these ABG values? What treatment do you think might be
appropriate for the patient?
11. A patient in the emergency department is being treated for severe congestive heart failure.
ABGs on room air are as follows: PaCO
2
= 78 mm Hg, PaO
2
= 65 mm Hg, SaO
2
= 90%.
What would the pH be if these results were due to hypoventilation alone? How would you
interpret the acid-base status? What respiratory care might this patient need?
12. An ABG sample has a pH of 7.30 and a PaCO
2
of 25 mm Hg. What is the estimated
3
HCO
based on these two values?
13. An ABG sample has a pH of 7.39 and a PaCO
2
of 61 mm Hg. What is the estimated
3
HCO
based on these two values?
14. How much effect would an increase in the PaCO
2
from 40 to 50 mm Hg have on a
3
HCO
of
25 mEq/L?
15. A patient has a constant CO
2
production. The patients alveolar ventilation drops from 5 to 2
L/min. If the patients PaCO
2
was 50 mm Hg at the start, what would you expect the PaCO
2
to be after the change in
.
A
V
?
16. A patient hyperventilates from a PaCO
2
of 40 to 30 mm Hg. The
3
HCO is 24 mEq/L
initially. What will the
3
HCO be after the change in the PaCO
2
?
17. A stable patient with chronic obstructive pulmonary disease (COPD) routinely has the
following blood gas values: PaCO
2
= 52 mm Hg, pH = 7.39, HCO
3
= 33 mEq/L. The patient
begins to vomit, and the pH rises to 7.53. In what way might the change in pH affect the
HCO
3
?
18. A patient has the following ABG values: PaCO
2
= 38 mm Hg, pH = 7.30, HCO
3
= 18
mEq/L. The patients HCO
3
increases to 28 mEq/L after intravenous administration of
HCO
3
. You would expect the pH to change to what value?
19. A blood gas slip shows the following values: pH = 7.33, PaCO
2
= 68 mm Hg, HCO
3
= 35
mEq/L. How would you interpret these results? (See Figure 4.)
20. If the pH is 7.10 and the PaCO
2
is 21 mm Hg, what is the HCO
3
? How would you interpret
these results?
24
Fig. 4 Blood gas flow chart showing the process for interpreting a set of blood gas values.
25
References
1. Adrogue HE, Adrogue HJ: Acid-base physiology, Respir Care 46:328, 2001.
2. Beachey W: Acid-base balance. In Wilkins RL, Stoller JK, Scanlan CL, editors: Egans
fundamentals of respiratory care, ed 8, St Louis, 2003, Mosby.
3. Davenport HW: The ABCs of acid-base chemistry, ed 5, Chicago, 1969, University of
Chicago Press.
4. Des Jardins T: Cardiopulmonary anatomy and physiology: essentials for respiratory care, ed
4, Albany, NY, 2002, Delmar.
5. Epstein SK, Singh N: Respiratory acidosis, Respir Care 46:366, 2001.
6. Foster GT, Vaziri ND, Sassoon CSH: Respiratory alkalosis, Respir Care 46:384, 2001.
7. Huang YCT: Arterial blood gases. In Hess RH, MacIntyre NR, Mishoe SC, et al, editors:
Respiratory care principles and practices, Philadelphia, 2002, WB Saunders.
8. Khanna A, Kurtzman NA: Metabolic alkalosis, Respir Care 46:354, 2001.
9. Kraut JA, Madias NE: Approach to patients with acid-base disorders, Respir Care 46:392,
2001.
10. Malley W: Clinical blood gases: assessment and intervention, Philadelphia, 2005, WB
Saunders.
11. Mathews P, Conway L: Arterial blood gases and noninvasive monitoring of oxygen and
carbon dioxide. In Wyka KA, Mathews PJ, Clark WF, editors: Foundations of respiratory
care, Albany, NY, 2002, Delmar.
12. Scanlan CL, Wilkins RL: Gas exchange and transport. In Wilkins RL, Stoller JK, Scanlan
CL, editors: Egans fundamentals of respiratory care, ed 8, St Louis, 2003, Mosby.
13. Shapiro BA, Peruzzi WT, Kozelowski-Templin R: Clinical application of blood gases, ed 5,
St Louis, 1994, Mosby.
14. Swenson ER: Metabolic acidosis, Respir Care 46:342, 2001.
15. Cairo JM, Pilbeam SP: Mosbys respiratory care equipment, ed 7, St Louis, 2004, Mosby.
16. American Association for Respiratory Care: Clinical practice guideline: blood gas analysis
and hemoximetry: 2001 revision and update, Respir Care 46:498, 2001.
17. American Association for Respiratory Care: Clinical practice guideline: capillary blood gas
sampling for neonatal and pediatric patients, Respir Care 39:1180, 1994.
18. Sorbini CA, Grassi V, Solinas E, et al: Arterial oxygen tension in relation to age in healthy
subjects, Respiration 25:3, 1968.
19. Schoene RB: Adaptation and maladaptation to high altitude. In Pierson DJ, Kacmarek RM,
editors: Foundations of respiratory care, New York, 1992, Churchill Livingstone.
20. Kacmarek RM, Hess D, Stoller JK: Monitoring in respiratory care, Chicago, 1993, Mosby.
21. Light RW: Conservative treatment of hypercapneic acute respiratory failure, Respir Care
28:561, 1983.
22. Otis AB: Quantitative relationships in steady-state gas exchange. In Fenn WO, Rahn H,
section editors: Handbook of physiology, Section 3: Respiration, Washington, DC, 1964, The
American Physiological Society.
23. Murray JF: Pathophysiology of acute respiratory failure, Respir Care 28:531, 1983.
Case Study/Exercise Answers
26
Answer: Case Study 1
At age 20, the normal P(A-a)O2 is about 5 mm Hg; it increases 4 mm Hg per decade. At age 4,0
this would represent an increase of 8 mm Hg, or a value of 13 mm Hg. The value of 15 mm Hg is
reasonably close to normal.
Answer Case Study 2
Although the PaO
2
and SaO
2
are normal, the low hemoglobin will cause a reduction in this
patients CaO
2
. Therefore, this patient does not have a normal oxygenation status.
Answer Case Study 3
A change in the PaCO
2
from 80 to 40 mm Hg is a 40 mm Hg difference; 40 mm Hg 1.25 = 50
mm Hg. The PaO
2
would be expected to increase by about 50 mm Hg to approximately 100 mm
Hg.
Answer Case Study 4
Use this equation:
L / mEq 29 or 8 . 28
65
78 24
HCO
3
Answer Exercise 5:
1. Normal
2. Uncompensated metabolic acidosis with hyperoxemia
3. Uncompensated respiratory acidosis with moderate hypoxemia
4. Uncompensated respiratory alkalosis with hyperoxemia
5. Compensated respiratory alkalosis with hyperoxemia
6. Uncompensated metabolic alkalosis
7. Compensated respiratory acidosis with mild hypoxemia
8. Partially compensated respiratory acidosis with mild hypoxemia
9. Partially compensated respiratory acidosis with mild hypoxemia
10. Partially compensated respiratory alkalosis
11. Partially compensated respiratory acidosis with severe hypoxemia
12. Partially compensated respiratory acidosis with mild hypoxemia
13. Partially compensated metabolic acidosis with hyperoxemia
14. Partially compensated metabolic alkalosis
15. Partially compensated respiratory alkalosis with hyperoxemia
16. Partially compensated respiratory acidosis with moderate hypoxemia
17. Possible venous sample
18. Partially compensated respiratory alkalosis
19. Compensated respiratory acidosis with mild hypoxemia
20. Uncompensated respiratory acidosis with moderate hypoxemia
21. Uncompensated metabolic alkalosis
22. Partially compensated metabolic acidosis with mild hypoxemia
23. Partially compensated metabolic alkalosis with mild hypoxemia
27
24. Uncompensated respiratory alkalosis with moderate hypoxemia
25. Partially compensated respiratory acidosis with mild hypoxemia
26. Compensated respiratory alkalosis with hyperoxemia
27. Normal ABGs
28. Uncompensated respiratory alkalosis with moderate hypoxemia
29. Uncompensated respiratory acidosis
30. Combined acidosis with moderate hypoxemia
31. Uncompensated metabolic alkalosis
32. Partially compensated respiratory alkalosis with moderate hypoxemia
33. Uncompensated respiratory acidosis with severe hypoxemia
34. Normal acid-base balance with mild hypoxemia
Answers Exercise 6
1. pH = 7.4; total CO
2
= 25.2 (mmol/L); PaCO
2
= 40 mm Hg; CaO
2
= 19.8 vol%; PaO
2
= 80 to
100 mm Hg; SaO
2
= 97%.
2. pH = 7.37; P
v
CO
2
= 46 mm Hg; C
v
O
2
= 14.8 vol%; P
v
O
2
= 40 mm Hg; S
v
O
2
= 75%.
3. Remember that PaO
2
= 104.2 (0.27 Age). For a 95-year-old patient, this is a normal value
for PaO
2
.
4. This is a normal PaO
2
for this elevation.
5. A normal P(A-a)O
2
for a 70-year-old person would be about 25 mm Hg. Recall that it is
about 5 mm Hg at age 20 and increases about 4 mm Hg per decade over 20.
6. A PaO
2
/P
A
O
2
of 0.5 is much lower than the normal value of approximately 0.9 to 1. This
suggests that only about 50% of the oxygen available in the alveolus is getting into the
arteries.
7. a
8. a
9. d
10. With a decrease in PaCO
2
of 20 mm Hg, the pH should increase by 0.2, so that the pH value
would be about 7.6. This is an example of respiratory alkalosis. The patient needs to
rebreathe CO
2
, perhaps by breathing into a bag, and should be calmed down.
11. The increased PaCO
2
of 78 mm Hg is about 40 mm Hg above the normal PaCO
2
. The pH
would be about 7.2, a decrease of 0.2 from normal. This is respiratory acidosis; the patient
needs increased ventilation to reduce the PaCO
2
.
12. HCO
3
= (24 PaCO
2
)/(H+); HCO
3
= (24 25)/50; HCO
3
= 12 mEq/L
13. HCO
3
= (24 PaCO
2
)/(H+); HCO
3
= (24 61)/40; HCO
3
= 36.6 mEq/L
14. An increase in the PaCO
2
from 40 to 50 mm Hg (10 mm Hg) increases the HCO
3
from 25 to
about 26 mEq/L.
15. Recall that PaCO
2
= [0.863 (
.
V
CO
2
)]/
A
.
V
; the first step is to determine the patients V.
Rearranging the equation:
.
V
CO
2
= [
A
.
V
PaCO
2
]/0.863;
.
V
CO
2
= (5 50)/0.863 = 287
mL/min. With the decrease in
A
.
V
, the PaCO
2
increases: PaCO
2
= (0.863 287)/2 = 124 mm
Hg.
16. The PaCO
2
drops by 10 mm Hg; the HCO
3
will decrease by about 2 to 22 mEq/L.
28
17. An increase in pH of 0.15 increases the HCO
3
by 10 mEq/L. The expected HCO
3
is about
43 mEq/L.
18. The pH will increase to 7.45.
19. Partially compensated respiratory acidosis
20. 6.3 mEq/L; partially compensated metabolic acidosis
You might also like
- Review of Respiratory PhysiologyDocument46 pagesReview of Respiratory Physiologylovelyc95No ratings yet
- Interpret The Abgs in A Stepwise Manner:: Reference ReferenceDocument6 pagesInterpret The Abgs in A Stepwise Manner:: Reference ReferenceYogeshRavalNo ratings yet
- Interpretation of Arterial Blood Gases and Acid-Base DisordersDocument44 pagesInterpretation of Arterial Blood Gases and Acid-Base DisordersSuren VishvanathNo ratings yet
- Med Lecture - Causes of HypoxemiaDocument6 pagesMed Lecture - Causes of HypoxemiaZoherNBezantiNo ratings yet
- ABG Made EasyDocument9 pagesABG Made EasyDrShruthi PradeepNo ratings yet
- Translateturn Off Instant TranslationDocument38 pagesTranslateturn Off Instant TranslationListaNo ratings yet
- ABG InterpretationDocument38 pagesABG Interpretationmahmod omerNo ratings yet
- AbgDocument66 pagesAbgindyaphdNo ratings yet
- Arterial Blood Gas AnalysisDocument23 pagesArterial Blood Gas AnalysisVartika SainiNo ratings yet
- Gas ExchangeDocument15 pagesGas ExchangeOsolemio Mer100% (1)
- Interpretation of Blood Gas Reports - Made Easy: Dr. A K Sethi's EORCAPS-2010, DelhiDocument0 pagesInterpretation of Blood Gas Reports - Made Easy: Dr. A K Sethi's EORCAPS-2010, DelhiPrabhakar KumarNo ratings yet
- Common Causes of HypoxemiaDocument6 pagesCommon Causes of HypoxemiaSamantha LuiNo ratings yet
- Measures of Oxygenation and Mechanisms of Hypoxemia - UpToDateDocument11 pagesMeasures of Oxygenation and Mechanisms of Hypoxemia - UpToDateraniakusmantoNo ratings yet
- Interpreting Arterial Blood Gas Results: Nicholas J Cowley, Andrew Owen, Julian F BionDocument4 pagesInterpreting Arterial Blood Gas Results: Nicholas J Cowley, Andrew Owen, Julian F BionNayem Hossain HemuNo ratings yet
- Oxygen TransportDocument40 pagesOxygen TransportMike MayerNo ratings yet
- ABGDocument16 pagesABGKesavanVeeraNo ratings yet
- Metabolic Rate and Alveolar VentilationDocument9 pagesMetabolic Rate and Alveolar VentilationSimran SukhijaNo ratings yet
- Interpretasi Agd Juni 2020Document34 pagesInterpretasi Agd Juni 2020Christiana TrijayantiNo ratings yet
- 9 - Respiratory FailureDocument7 pages9 - Respiratory Failureعبدالحكيم حثولNo ratings yet
- Blood Gas AnalysisDocument31 pagesBlood Gas AnalysisBagas Dyakso DarmojoNo ratings yet
- Respiratory Monitoring in Mechanical Ventilation: Techniques and ApplicationsFrom EverandRespiratory Monitoring in Mechanical Ventilation: Techniques and ApplicationsJian-Xin ZhouNo ratings yet
- Arterial Blood Gas: Interpretation and Clinical ImplicationsDocument112 pagesArterial Blood Gas: Interpretation and Clinical ImplicationsmatrixtrinityNo ratings yet
- Rs4-Gas Exchange and TransportDocument5 pagesRs4-Gas Exchange and TransportGabriella ChafrinaNo ratings yet
- Arterial Blood GasDocument6 pagesArterial Blood GasnsfanfoinNo ratings yet
- Arterial Blood GasDocument33 pagesArterial Blood GaskartikaparamitaNo ratings yet
- Oxygen Solubility in Experimental Media: Oxygraph-2kDocument6 pagesOxygen Solubility in Experimental Media: Oxygraph-2kRamachandran VenkateshNo ratings yet
- Arterial Blood Gases, Ox..., Lawrence Martin, M.D.Document9 pagesArterial Blood Gases, Ox..., Lawrence Martin, M.D.mrezasyahliNo ratings yet
- Arterial Blood Gases: Laboratory InsightsDocument9 pagesArterial Blood Gases: Laboratory InsightsYusuf NugrohoNo ratings yet
- Respiratory Acid-Base DisordersDocument13 pagesRespiratory Acid-Base DisordersAlfredo PreciadoNo ratings yet
- Arterial Blood GasDocument255 pagesArterial Blood GasMark Joshua S CruzNo ratings yet
- Acido Base Critical CareDocument18 pagesAcido Base Critical CareJulia Uchoa UchoaNo ratings yet
- PCO2 Cartridge Test Information SheetDocument6 pagesPCO2 Cartridge Test Information SheetMa Louise PetateNo ratings yet
- Abg AnalysisDocument65 pagesAbg AnalysisSyed Farooque AliNo ratings yet
- Arterial Blood Gas AnalysisDocument28 pagesArterial Blood Gas Analysishendra_darmawan_4No ratings yet
- Blood Gas MachineDocument33 pagesBlood Gas MachinenofearnofearNo ratings yet
- D MystifiedDocument10 pagesD MystifiedWalaa YousefNo ratings yet
- Why Measure Blood Gases A Threepart Introduction For The Novice Part 3Document9 pagesWhy Measure Blood Gases A Threepart Introduction For The Novice Part 3Tibi TibiNo ratings yet
- Arterial Blood Gase1Document5 pagesArterial Blood Gase1meku mekuNo ratings yet
- Arterial Blood Gas Analysis - Hand OutsDocument3 pagesArterial Blood Gas Analysis - Hand OutsRANo ratings yet
- Blood Gas AnalysisDocument5 pagesBlood Gas Analysissraji64No ratings yet
- V/Q and Oxygen: Anuja Abayadeera Part 1B AnaesthsiologyDocument42 pagesV/Q and Oxygen: Anuja Abayadeera Part 1B Anaesthsiologyv_vijayakanth7656No ratings yet
- Arterial Blood GasesDocument10 pagesArterial Blood GasesSoumya BhattacharyaNo ratings yet
- Capnography in DogsDocument14 pagesCapnography in DogswalczakcNo ratings yet
- Oxygen Allows Less VentilationDocument1 pageOxygen Allows Less VentilationSyed Shahrul Naz SyedNo ratings yet
- Arterial Blood Gas.Document4 pagesArterial Blood Gas.Sathish KumarNo ratings yet
- ABG GeekymedicsDocument13 pagesABG Geekymedicscharlyn206No ratings yet
- Analisis Gas DarahDocument2 pagesAnalisis Gas DarahTri GunawanNo ratings yet
- Hydrogen Ion Concentration and PH: Basic ConceptsDocument16 pagesHydrogen Ion Concentration and PH: Basic Conceptsvanessa armeliaNo ratings yet
- BSAVA - Interpretation of Arterial Blood Gas - VINDocument5 pagesBSAVA - Interpretation of Arterial Blood Gas - VINvetthamilNo ratings yet
- Blood Gas and Acid Base AnalysisDocument1 pageBlood Gas and Acid Base AnalysisErdi TuwenoNo ratings yet
- Analisis Gas DarahDocument2 pagesAnalisis Gas DarahTri GunawanNo ratings yet
- Blood Gas Questions With Answers - 1998Document11 pagesBlood Gas Questions With Answers - 1998somarajakNo ratings yet
- Arterial Blood Gas Analysis: BY-Shivam Sachan (JR Ii) Moderator - Dr. R.K YADAV (M.D)Document52 pagesArterial Blood Gas Analysis: BY-Shivam Sachan (JR Ii) Moderator - Dr. R.K YADAV (M.D)imranqazi11No ratings yet
- Arterial Blood Gas InterpretationDocument65 pagesArterial Blood Gas InterpretationDaniel AryanNo ratings yet
- How To Interpret Arterial Blood Gas ResultsDocument9 pagesHow To Interpret Arterial Blood Gas ResultsteleasadgramNo ratings yet
- Abg Analysis ReviewerDocument21 pagesAbg Analysis ReviewerAyiessa_AJNo ratings yet
- ABGDocument45 pagesABGHasan SudirgoNo ratings yet
- Essential Respiratory Calculation: Lung Volumes, Dead Space, and Alveolar VentilationDocument6 pagesEssential Respiratory Calculation: Lung Volumes, Dead Space, and Alveolar VentilationHéctor GarcíaNo ratings yet
- Arterial Blood Gas Analysis - making it easyFrom EverandArterial Blood Gas Analysis - making it easyRating: 4.5 out of 5 stars4.5/5 (4)
- Chapter 02Document3 pagesChapter 02Robert Kerwick100% (2)
- Chapter 01Document7 pagesChapter 01Robert Kerwick100% (5)
- EquationsDocument24 pagesEquationsRobert Kerwick100% (2)
- Chapter 01Document7 pagesChapter 01Robert Kerwick100% (5)
- Assessment Nursing Diagnosis Inference Objectives Nursing Intervention Rationale EvaluationDocument10 pagesAssessment Nursing Diagnosis Inference Objectives Nursing Intervention Rationale EvaluationJobelle AcenaNo ratings yet
- Pa Essentials of Clinical Pathology 2010 PDF UnitedvrgDocument382 pagesPa Essentials of Clinical Pathology 2010 PDF UnitedvrgSafdar Ali67% (3)
- Introduction To ElectrolytesDocument13 pagesIntroduction To ElectrolytesMaam ShaNo ratings yet
- Hypovolemic Shock Pathophysiology, Symptoms, Signs, Treatment - EHealthStarDocument15 pagesHypovolemic Shock Pathophysiology, Symptoms, Signs, Treatment - EHealthStarKaloy KamaoNo ratings yet
- ABG - Simplified: Dr.S.Arun CheguevaraDocument29 pagesABG - Simplified: Dr.S.Arun CheguevaraSmilewith RakshiNo ratings yet
- Diagnosis and Management of Fetal DIstress - A Review Based On Modern Concept and Ancient Ayurvedic GranthasDocument3 pagesDiagnosis and Management of Fetal DIstress - A Review Based On Modern Concept and Ancient Ayurvedic GranthasaginaNo ratings yet
- Acid Base Balance in Critical Care Medicine-NELIGAN PDFDocument0 pagesAcid Base Balance in Critical Care Medicine-NELIGAN PDFAdistya SariNo ratings yet
- ABG ExamplesDocument31 pagesABG ExamplesKEROLOS MAHROUSNo ratings yet
- Chapter 39: Fluid, Electrolytes, and Acid-Base Balance Yoost & Crawford: Fundamentals of Nursing: Active Learning For Collaborative Practice, 2nd EditionDocument12 pagesChapter 39: Fluid, Electrolytes, and Acid-Base Balance Yoost & Crawford: Fundamentals of Nursing: Active Learning For Collaborative Practice, 2nd Editionbafraley7No ratings yet
- CCRN Synergy and Exam StartegiesDocument12 pagesCCRN Synergy and Exam StartegiesMarcus, RN100% (2)
- Arawali Veterinary College Bajor, SikarDocument8 pagesArawali Veterinary College Bajor, Sikarashish kumarNo ratings yet
- Examples of Mixed Acid-Base DisordersDocument2 pagesExamples of Mixed Acid-Base DisordersAfifa Noori SiddiquiNo ratings yet
- Acidosis and Alkalosis: Common Causes of Acid-Base DisordersDocument1 pageAcidosis and Alkalosis: Common Causes of Acid-Base DisordersErand TopalliNo ratings yet
- Case Study - NephroticDocument23 pagesCase Study - NephroticLorelyn Delfin0% (1)
- BSAVA - Interpretation of Arterial Blood Gas - VINDocument5 pagesBSAVA - Interpretation of Arterial Blood Gas - VINvetthamilNo ratings yet
- Acid Base BalanceDocument56 pagesAcid Base BalanceVirendra Joshi100% (1)
- Acid-Base Homeostasis: Clin J Am Soc Nephrol. 10.2215/CJN.07400715 26597304Document18 pagesAcid-Base Homeostasis: Clin J Am Soc Nephrol. 10.2215/CJN.07400715 26597304Christine SiraitNo ratings yet
- Acidosis and AlkalosisDocument10 pagesAcidosis and AlkalosisNealeth NanquilNo ratings yet
- UntitledDocument8 pagesUntitledYou TuberNo ratings yet
- MGR University SyllabusDocument33 pagesMGR University SyllabussanjviewsNo ratings yet
- Acute Renal Failure: John FeehallyDocument107 pagesAcute Renal Failure: John Feehallygede wira mahaditaNo ratings yet
- Nursing Practice III Care of Clients Part BDocument29 pagesNursing Practice III Care of Clients Part BAnnica Lozano100% (1)
- Inborn Errors of Metabolism in Infancy: A Guide To DiagnosisDocument11 pagesInborn Errors of Metabolism in Infancy: A Guide To DiagnosisEdu Diaperlover São PauloNo ratings yet
- Surgical ICU Exam Content OutlineDocument6 pagesSurgical ICU Exam Content OutlineDarren DawkinsNo ratings yet
- Acid Base Disorders JAPIDocument5 pagesAcid Base Disorders JAPIVitrag_Shah_1067No ratings yet
- Lab Dept: Chemistry Test Name: Lactate: General InformationDocument2 pagesLab Dept: Chemistry Test Name: Lactate: General InformationŽeljkoNo ratings yet
- IADVL Color Atlas of Dermatopathology - BookDocument41 pagesIADVL Color Atlas of Dermatopathology - Book65gkenNo ratings yet
- Causes and Evaluation of Hyperkalemia in Adults - UpToDateDocument25 pagesCauses and Evaluation of Hyperkalemia in Adults - UpToDateDaniely FreitasNo ratings yet
- The Toxicology Handbook For CliniciansDocument359 pagesThe Toxicology Handbook For Cliniciansmariposa_061280% (5)
- Lecture NotesDocument56 pagesLecture NotesLalaine April E. Ortiola100% (13)