Professional Documents
Culture Documents
Tinea
Uploaded by
Gail AidOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Tinea
Uploaded by
Gail AidCopyright:
Available Formats
400
Chapter 20
II. E
(6) Ultraviolet radiation (UV) has long been recognized as a safe and effective treatment
for managing psoriasis. Varying types of phototherapy are available to patients. All
phototherapy treatment regimens should be initiated and managed by a physician or
dermatologist.
III. FUNGAL INFECTIONS
A. Overview
1. Fungal skin infections, also known as tineas or ringworm (due to its characteristic circular
appearance), are some of the most commonly encountered dermatologic conditions. It is estimated that up to 20% of the American population may be infected with a tinea infection at any
given time.
2. Several factors may predispose people to becoming infected with a tinea. Fungi grow best in
warm, moist environments. Tight clothing or shoes that are worn on a repeated basis may facilitate fungal growth. Sharing public showers or pools can also promote the spread of tinea infections. Patients with diseases or conditions that suppress the bodys natural immune response
(such as diabetes, poor personal hygiene, malnutrition, or a compromised epithelium) are at
greater risk of contracting tinea infections.
3. Nonprescription therapies usually work quite well in resolving many types of tinea infections
completely.
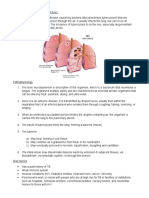
B. Pathophysiology
1. Tinea infections are typically superficial. The fungi that cause tineas thrive on dead skin cells
within the stratum corneum. Skin, hair, and nails may all be affected by a tinea infection.
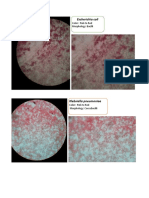
2. The three most prevalent fungi in the United States that cause tinea infections are Trichophyton,
Microsporum, and Epidermophyton.
3. Fungi may be transmitted to an unaffected individual either through direct contact with an infected person or animal or through contact with a fomite.
C. Clinical presentation. Tineas are categorized by the area of the body they affect.
1. Tinea capitis is also known as ringworm of the scalp. Tinea capitis occurs more frequently in children than adults. This may be due in part to a lack of social inhibition in sharing items like brushes
and combs. Epidermal gland secretions also increase at puberty and have a fungicidal effect.
2. Tinea corporis, or ringworm of the body, is not limited to a specific area of the body. Rather,
tinea corporis may take on several clinical appearances and can affect any area of the body. Often,
patients with tinea corporis are infected with one or more additional tineas.
3. Tinea cruris is more commonly referred to as jock itch. The intertriginous areas of the groin
make it an ideal environment for fungal infections. For anatomical reasons, males are more likely
to suffer from tinea cruris than females.
4. Tinea nigra is perhaps the least common of the tineas. It is mainly seen in people who live in humid coastal areas and may be transmitted through sand. Tinea nigra is primarily found on fingers
and feet.
5. Tinea pedis, or athletes foot, is by far the most common tinea infection. Sports players and
people who share pools or showers are at the greatest risk for contracting tinea pedis. Once
present, athletes foot is exacerbated in patients who continue to wear shoes and socks, fostering a
warm and moist environment for the fungus to survive.
6. Tinea unguium, or onychomycosis, is a fungal infection of the nails. Toenails are more frequently affected by tinea unguium than fingernails. Onychomycosis can ultimately lead to loss of
the affected nail if not treated appropriately.
7. Tinea versicolor is a chronic fungal infection of the skin. Tinea versicolor is caused by Pityrosporum (see II.B.2) and primarily affects people living in hot, humid climates.
D. Treatment
1. Nonpharmacological measures
a. To maintain proper hygiene and to minimize the likelihood of contracting a tinea or spreading a tinea to another person, patients should wash their body daily with soap and water.
b. Any contaminated towels and clothing must be washed in hot water.
c. Patients with tinea infections should be counseled to avoid sharing towels.
d. Allow shoes and clothing to dry completely before wearing them.
Shargel_8e_CH20.indd 400
07/08/12 1:32 AM
Over-the-Counter Dermatological Agents
401
e. As much as possible, noninfected patients should avoid direct contact with and avoid using
the same showers as people who have fungal infections.
f. If a shower must be shared, patients should be counseled to wear shower shoes/sandals while
in the shower.
2. Pharmacological therapies
a. Nonprescription topical medications
(1) Only three types of tinea infections respond to self-treatment with nonprescription therapies: tinea corporis, tinea cruris, and tinea pedis. All other tinea infections should be
referred to a physician for evaluation and treatment.
(2) Each of the antifungals listed in the following text is applied topically for 1 to 4 weeks.
These agents are generally well-tolerated, and systemic side effects are rare.
(a) Butenafine (Lotrimin Ultra) is available as a 1% cream. Butenafine should only be
used in patients 12 and older.
(b) Clotrimazole (Desenex AF Cream, Lotrimin AF Lotion) is also sold as a 1% cream,
lotion, or solution. Some patients will experience mild burning and stinging with use
of clotrimazole.
(c) Miconazole (Cruex Antifungal Spray Powder, Micatin Jock Itch Cream) is a 2%
powder, cream, or lotion and is closely related chemically to clotrimazole.
(d) Terbinafine (Lamisil AT) is available as a 1% cream, gel, or spray. Like butenafine,
terbinafine should only be recommended in patients age 12 and older.
(e) Tolnaftate (Tinactin) is a 1% cream, gel, or powder that has served as the OTC standard of care for fungal infections for decades (prior to many of these other products
being introduced). Tolnaftate is the only active ingredient that carries FDA approval
for both the treatment and prevention of athletes foot, when used on a daily basis.
(f) Undecylenic acid (Cruex Cream, Fungicure Liquid) is marketed in concentrations
of 10% to 25% and comes in multiple forms, including a cream, solution, powder,
and spray. Products containing undecylenic acid and its salts carry an unpleasant
odor, which may be unacceptable to some patients.
b. Prescription treatment options. Patients who do not respond to self-treatment with any of
the OTC therapies described previously within 1 week should be referred to their primary
care provider for evaluation. If the condition shows improvement within the first week, patients are free to continue with self-treatment.
(1) Topical antifungals are available for use in patients who do not experience resolution
of their tinea infection with OTC therapies or who have a tinea infection that cannot be
self-treated.
(a) Ciclopirox (Loprox) is available as a cream, gel, or lacquer for the treatment of tinea
corporis, cruris, pedis, versicolor, and unguium.
(b) Econazole (Spectazole) 1% cream is indicated for the treatment of tinea corporis,
cruris, pedis, and versicolor.
(2) More severe fungal infections require treatment with systemic therapies.
(a) The azole antifungals [fluconazole (Diflucan), itraconazole (Sporanox), ketoconazole (Nizoral), posaconazole (Noxafil), and voriconazole (Vfend)] are generally
well-tolerated. The azoles may cause varying degrees of hepatotoxicity, and the class
is notorious for its wide spectrum of drugdrug interactions.
(b) Griseofulvin (Grifulvin V) is available as both an oral tablet and suspension. Because
griseofulvin increases photosensitivity, patients taking this agent should avoid prolonged exposure to the sun.
(c) In addition to its status as an OTC topical agent, terbinafine (Lamisil) is also available
as a prescription oral antifungal. It is considered the first-line agent for onychomycosis.
IV. ACNE
A. Overview
1. Definition. Acne vulgaris is a disorder of the pilosebaceous units, mainly of the face, chest, and back.
The lesions usually start as open or closed comedones and evolve into inflammatory papules and pustules that either resolve as macules or become secondary pyoderma, which results in various sequelae.
Shargel_8e_CH20.indd 401
07/08/12 1:32 AM
You might also like
- A Simple Guide to Skin Fungal Infections, (Updated 2023) Diagnosis, Treatment and Related ConditionsFrom EverandA Simple Guide to Skin Fungal Infections, (Updated 2023) Diagnosis, Treatment and Related ConditionsRating: 5 out of 5 stars5/5 (2)
- Skin Infections, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsFrom EverandSkin Infections, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsNo ratings yet
- Treatment of Athlete's Foot: Topical vs Oral Antifungals (38 charactersDocument3 pagesTreatment of Athlete's Foot: Topical vs Oral Antifungals (38 charactersAbi ArellanoNo ratings yet
- AdrianDocument3 pagesAdrianJohn David ZabalaNo ratings yet
- Cutaneous Fungal InfectionsDocument8 pagesCutaneous Fungal InfectionsJudith GraalNo ratings yet
- Guidelines Therapy CLMDocument6 pagesGuidelines Therapy CLMAgaipNo ratings yet
- Topical Treatment of Common Superficial Tinea InfectionsDocument8 pagesTopical Treatment of Common Superficial Tinea InfectionsColate LocoNo ratings yet
- Skin Therapy Letter PDFDocument8 pagesSkin Therapy Letter PDFSherlocknovNo ratings yet
- RingwormDocument7 pagesRingwormSAMSON, MAXZENE ANICKANo ratings yet
- CANDIDIASISDocument20 pagesCANDIDIASISKylie GolindangNo ratings yet
- Ringworm Guide: Symptoms, Types, and TreatmentDocument5 pagesRingworm Guide: Symptoms, Types, and TreatmentAnnisa SyaflianiNo ratings yet
- Tinea pedis: More than just athlete's footDocument6 pagesTinea pedis: More than just athlete's footNyoman Arya Adi WangsaNo ratings yet
- Student Notes SCABIESDocument4 pagesStudent Notes SCABIEShannahbravo246No ratings yet
- Fungal Skin Infections: Education GapDocument17 pagesFungal Skin Infections: Education GapAncuta CalimentNo ratings yet
- Gupta Ak Et Al Fungal Skin Infections PDFDocument17 pagesGupta Ak Et Al Fungal Skin Infections PDFValeria BeltranNo ratings yet
- Athlete's Foot (Tinea Pedis)Document21 pagesAthlete's Foot (Tinea Pedis)farmasi_hm100% (1)
- Book May 14Document4 pagesBook May 14api-256332754No ratings yet
- Classification and Epidemiology of Communicable DiseasesDocument40 pagesClassification and Epidemiology of Communicable DiseasesRwapembe StephenNo ratings yet
- Chapter 42: Fungal Skin Infections: Handbook of Nonprescription Drugs: An Interactive Approach To Self-Care, 20th EditionDocument22 pagesChapter 42: Fungal Skin Infections: Handbook of Nonprescription Drugs: An Interactive Approach To Self-Care, 20th EditionOmnia El HossienyNo ratings yet
- Dengue InglésDocument2 pagesDengue InglésGohan MiguelNo ratings yet
- Trachoma; Tetanus; Leprosy (1)Document40 pagesTrachoma; Tetanus; Leprosy (1)Osama adel Mohamed SmadiNo ratings yet
- Therapy of Common Superficial Fungal Infections: D B. H, L O - Z, J J. W, K R. P & S K. TDocument7 pagesTherapy of Common Superficial Fungal Infections: D B. H, L O - Z, J J. W, K R. P & S K. TAji DwijayantoNo ratings yet
- Management of ScabiesDocument7 pagesManagement of ScabiesShinta Andi SarasatiNo ratings yet
- Diphtheria: Questions and Answers: Information About The Disease and VaccinesDocument3 pagesDiphtheria: Questions and Answers: Information About The Disease and Vaccinesbilalmd1701No ratings yet
- Vector and Pest Control in DisastersDocument10 pagesVector and Pest Control in DisastersTaufik RizkiandiNo ratings yet
- Microbial ResearchDocument12 pagesMicrobial Researchharshit kumarNo ratings yet
- Managing Athlete's FootDocument5 pagesManaging Athlete's FootCharlesMahonoNo ratings yet
- Ringworm Research PaperDocument4 pagesRingworm Research Papercarkdfp5100% (1)
- Viral Meningitis, Tetanus, Giardiasis and Westnile Fever Causes, Symptoms, TreatmentsDocument20 pagesViral Meningitis, Tetanus, Giardiasis and Westnile Fever Causes, Symptoms, TreatmentsFlorence ILoyd R. TorresNo ratings yet
- Chapter 18. Pinworm InfectionDocument12 pagesChapter 18. Pinworm InfectionMonica CiorneiNo ratings yet
- Activity 2 - Case StudyDocument5 pagesActivity 2 - Case StudyGrace MendozaNo ratings yet
- About Laser Toenail Fungus TreatmentsDocument10 pagesAbout Laser Toenail Fungus Treatmentsmohamed radwanNo ratings yet
- Tinea Corporis, Tinea Cruris, Tinea Nigra, and PiedraDocument6 pagesTinea Corporis, Tinea Cruris, Tinea Nigra, and PiedraIsni KhoirunisaNo ratings yet
- Midwifery Dipartment Impetigo TreatmentDocument13 pagesMidwifery Dipartment Impetigo TreatmentKubra ĖdrisNo ratings yet
- Animal and Insect Bites DiseasesDocument28 pagesAnimal and Insect Bites DiseasesAditya PrabawaNo ratings yet
- Fungal Skin Infections ملزمةDocument6 pagesFungal Skin Infections ملزمةعبدالرحمن طارق عبدالله صالحNo ratings yet
- Acral Manifestations of Fungal InfectionsDocument21 pagesAcral Manifestations of Fungal InfectionsanwarNo ratings yet
- Antifungal Therapy for Fungal InfectionsDocument186 pagesAntifungal Therapy for Fungal InfectionsRizweta DestinNo ratings yet
- Annular LesionsDocument8 pagesAnnular LesionshpmcentreNo ratings yet
- ScabiesDocument14 pagesScabiesRohini SelvarajahNo ratings yet
- Tinea CorporisDocument14 pagesTinea CorporisagungteukuNo ratings yet
- E Tra: Diagnosis and Management of Cutaneous Tinea InfectionsDocument8 pagesE Tra: Diagnosis and Management of Cutaneous Tinea InfectionsFuad hadyanNo ratings yet
- TB & Scabies Causes, Symptoms & TreatmentDocument5 pagesTB & Scabies Causes, Symptoms & TreatmentLouise OpinaNo ratings yet
- Clinical Review - FullDocument6 pagesClinical Review - Fullilham thohirNo ratings yet
- Tinea Corporis, Tinea Cruris, Tinea Nigra, and Piedra: Dermatologic Clinics August 2003Document7 pagesTinea Corporis, Tinea Cruris, Tinea Nigra, and Piedra: Dermatologic Clinics August 2003Dicky KurniawanNo ratings yet
- Fungal InfectionsDocument9 pagesFungal InfectionsCoral Srinivasa RamaluNo ratings yet
- Nursing Care of Upper Respiratory DisordersDocument3 pagesNursing Care of Upper Respiratory DisordersCamille SanguyoNo ratings yet
- Patofisiologi DifteriDocument11 pagesPatofisiologi DifteriicorrrNo ratings yet
- Pathogen Safety Data SheetsDocument9 pagesPathogen Safety Data Sheetsmike rezekiNo ratings yet
- Fungal InfectionsDocument21 pagesFungal InfectionsAyeshaNo ratings yet
- 2.-Schistosomiasis-Rabies-Pediculosis-Bubonic-Plague-Anthrax-HelminthesDocument92 pages2.-Schistosomiasis-Rabies-Pediculosis-Bubonic-Plague-Anthrax-Helminthesaltairejoshua.jalbayNo ratings yet
- DIPTHERIADocument3 pagesDIPTHERIARed Angela DinsonNo ratings yet
- New Antifungal Agents and New Formulations Against DermatophytesDocument15 pagesNew Antifungal Agents and New Formulations Against DermatophytesJanelle RocoNo ratings yet
- Bsn4a Group 4 Red Dog BitesDocument34 pagesBsn4a Group 4 Red Dog BitesNovie GarillosNo ratings yet
- Vitex negundo leaf extracts as an antimicrobial cream against Escherichia coliDocument51 pagesVitex negundo leaf extracts as an antimicrobial cream against Escherichia coliIanne Lorraine L. DANTENo ratings yet
- All Short Notes of ICDocument30 pagesAll Short Notes of ICaarti HingeNo ratings yet
- Tinea Pedis NewDocument6 pagesTinea Pedis NewRatih Oktaviana YahyaNo ratings yet
- Cutaneous Larva MigransDocument4 pagesCutaneous Larva MigransanissabilfaqihNo ratings yet
- Global epidemiology and etiology of common fungal infection tinea pedisDocument16 pagesGlobal epidemiology and etiology of common fungal infection tinea pedisasfwegereNo ratings yet
- Vectors of Disease and Vector ControlDocument18 pagesVectors of Disease and Vector ControlSanjoy RoyNo ratings yet
- June 2016 Board Exam QuestionsDocument24 pagesJune 2016 Board Exam QuestionsFanBayNo ratings yet
- Phytochem OnlyDocument4 pagesPhytochem OnlyGail AidNo ratings yet
- Sds Navigo 70 MCL enDocument10 pagesSds Navigo 70 MCL enGail AidNo ratings yet
- Adventist Medical Center College Andres Bonifacio Ave., San Miguel, Iligan City Department of PharmacyDocument5 pagesAdventist Medical Center College Andres Bonifacio Ave., San Miguel, Iligan City Department of PharmacyGail AidNo ratings yet
- Clint Ox Lab Anti MotilityDocument3 pagesClint Ox Lab Anti MotilityGail AidNo ratings yet
- qc2 ch1Document6 pagesqc2 ch1Gail AidNo ratings yet
- Plankton PPT For SurigaoDocument24 pagesPlankton PPT For SurigaoGail AidNo ratings yet
- Shig Ellos IsDocument15 pagesShig Ellos IsGail AidNo ratings yet
- Ionic Bonds ExplainedDocument35 pagesIonic Bonds ExplainedNear ChemNo ratings yet
- Escherichia Coli: Color: Pink To Red Morphology: BacilliDocument1 pageEscherichia Coli: Color: Pink To Red Morphology: BacilliGail AidNo ratings yet
- 2423L6Document11 pages2423L6Salman Dinani100% (1)
- Health EthicsDocument18 pagesHealth EthicsGail AidNo ratings yet
- ChapterDocument3 pagesChapterGail AidNo ratings yet
- Pharmaceutical Jurisprudence and EthicsDocument5 pagesPharmaceutical Jurisprudence and EthicsGail Aid100% (1)
- Who Trs 908-Annex9Document12 pagesWho Trs 908-Annex9Poorvi KumarNo ratings yet
- CEBUDocument6 pagesCEBUGail AidNo ratings yet
- Risk Factors For Common Chronic DiseasesDocument14 pagesRisk Factors For Common Chronic DiseasesGail AidNo ratings yet
- Org ChartDocument1 pageOrg ChartGail AidNo ratings yet
- 04 Drug Safety Final 08Document40 pages04 Drug Safety Final 08Gail AidNo ratings yet
- Lec 1Document5 pagesLec 1Gail AidNo ratings yet
- Adverse Drug ReactionDocument4 pagesAdverse Drug Reactionapi-246003035No ratings yet
- Crescentia Cujete Calabash-Tree: Fact Sheet ST-216Document3 pagesCrescentia Cujete Calabash-Tree: Fact Sheet ST-216Gail AidNo ratings yet
- Crescentia CujeteDocument40 pagesCrescentia CujeteGail AidNo ratings yet
- Miracle FruitDocument11 pagesMiracle FruitGail AidNo ratings yet
- Status of Macrobenthic Community and Its Relationships To Trace Metals and NaturalDocument8 pagesStatus of Macrobenthic Community and Its Relationships To Trace Metals and NaturalGail AidNo ratings yet
- Miracle FruitDocument9 pagesMiracle FruitGail AidNo ratings yet
- Crescentia Cujete Calabash-Tree: Fact Sheet ST-216Document3 pagesCrescentia Cujete Calabash-Tree: Fact Sheet ST-216Gail AidNo ratings yet
- PharmacodynamicsDocument62 pagesPharmacodynamicsGail AidNo ratings yet
- Radiopharmaceuticals Guide to Half-Lives & Medical UsesDocument31 pagesRadiopharmaceuticals Guide to Half-Lives & Medical UsesGail AidNo ratings yet
- 120 141 Anatomy and PhysiologyDocument3 pages120 141 Anatomy and PhysiologyTin BabistaNo ratings yet
- Reasons For Testing: Air LungsDocument12 pagesReasons For Testing: Air LungsNathyNo ratings yet
- Ace CPT Study Summary PDFDocument69 pagesAce CPT Study Summary PDFychauhanNo ratings yet
- Preparing The Dental O Ce For Medical Emergencies: Harry Dym, DDSDocument4 pagesPreparing The Dental O Ce For Medical Emergencies: Harry Dym, DDSVenkata Ramana Murthy VasupilliNo ratings yet
- Surgical Site InfectionsDocument52 pagesSurgical Site Infectionssahabatsalam07100% (5)
- Caring in NursingDocument60 pagesCaring in NursingChadrie SanchezNo ratings yet
- Gynecologic Emergencies: Farhad Takhti M.D. Senior Consultant Landesklinikum Neunkirchen AustriaDocument52 pagesGynecologic Emergencies: Farhad Takhti M.D. Senior Consultant Landesklinikum Neunkirchen Austriamadmax500No ratings yet
- AnnexIIRecommendationsbyHOTCCommittee06 11 18Document6 pagesAnnexIIRecommendationsbyHOTCCommittee06 11 18Bilal AbbasNo ratings yet
- Pediatric Blueprints NotesDocument96 pagesPediatric Blueprints NotesPisiform90100% (2)
- Classification and Definitions of Pain DisordersDocument4 pagesClassification and Definitions of Pain DisordersDian Istiqamah MardhatillahNo ratings yet
- LaserDocument43 pagesLaserTommy AgustinusNo ratings yet
- 30613167: Management of Osteitis Pubis in Athletes Rehabilitation and Return To Training - A Review of The Most Recent Literature PDFDocument10 pages30613167: Management of Osteitis Pubis in Athletes Rehabilitation and Return To Training - A Review of The Most Recent Literature PDFRicovially DavyaNo ratings yet
- Secrets of HappinessDocument110 pagesSecrets of HappinessEcaterina IrimiaNo ratings yet
- Ge Session TwoDocument4 pagesGe Session TwocrbrunelliNo ratings yet
- Whitford Et Al - 2012 - The Discovery of Insulin PDFDocument6 pagesWhitford Et Al - 2012 - The Discovery of Insulin PDFJessica ArciniegasNo ratings yet
- BPH Guide: Symptoms, Causes and Diagnostic TestsDocument57 pagesBPH Guide: Symptoms, Causes and Diagnostic TestsDiannetotz MoralesNo ratings yet
- Patient Assessment LimmerEdDocument2 pagesPatient Assessment LimmerEdepraetorian92% (13)
- James D Smrtic - Abnormal Psychoogy PDFDocument28 pagesJames D Smrtic - Abnormal Psychoogy PDFioan_nebunuNo ratings yet
- 2018 Glucocorticoid-Induced OsteoporosisDocument10 pages2018 Glucocorticoid-Induced OsteoporosisMiguel Angel Carrasco MedinaNo ratings yet
- LTO Application FormDocument7 pagesLTO Application Formemma alingasa67% (3)
- Microdacyn60 - FlyerDocument2 pagesMicrodacyn60 - Flyerdex99No ratings yet
- 29 Zvornicanin EtalDocument2 pages29 Zvornicanin EtaleditorijmrhsNo ratings yet
- Mentorship Assignment - Janedene GuevaraDocument3 pagesMentorship Assignment - Janedene Guevaraapi-485132528No ratings yet
- STROKE GUIDELINES FOR MANAGEMENTDocument1 pageSTROKE GUIDELINES FOR MANAGEMENTthapanNo ratings yet
- Case StudyDocument24 pagesCase StudyNurulIzzatiZainudinNo ratings yet
- Lucrări Ştiinţifice, Seria I, Vol. Xi (4) : Key WordsDocument10 pagesLucrări Ştiinţifice, Seria I, Vol. Xi (4) : Key WordsDana BudaiNo ratings yet
- DR Martine Faure Alderson - Cranio Sacral Reflexology Is BornDocument3 pagesDR Martine Faure Alderson - Cranio Sacral Reflexology Is BornCatherine Smith100% (1)
- The Jet Volume 5 Number 3Document44 pagesThe Jet Volume 5 Number 3THE JETNo ratings yet
- Acarbose: Prescriber HighlightsDocument4 pagesAcarbose: Prescriber HighlightsDr. Anil Virani AlliedNo ratings yet
- Case Presentation 2Document11 pagesCase Presentation 2Angel Jonele ManongsongNo ratings yet
- 1 s2.0 S0957417414001249 MainDocument14 pages1 s2.0 S0957417414001249 MainBegoña MartinezNo ratings yet