Professional Documents
Culture Documents
Nondestructive Measurements of Implant-Bone Interface Shear Modulus and Effects of Implant Geometry in Pull-Out Tests
Uploaded by
Lata DeshmukhOriginal Title
Copyright
Available Formats
Share this document
Did you find this document useful?
Is this content inappropriate?
Report this DocumentCopyright:
Available Formats
Nondestructive Measurements of Implant-Bone Interface Shear Modulus and Effects of Implant Geometry in Pull-Out Tests
Uploaded by
Lata DeshmukhCopyright:
Available Formats
Nondestructive measurements of implantbone interface
shear modulus and effects of implant geometry in
pull-out tests
A. Berzins,1,* B. Shah,1 H. Weinans,1,2 and D. R. Sumner1
1
Section of Orthopedic Research, Department of Orthopedic Surgery, Rush Arthritis and Orthopedics Institute,
RushPresbyterianSt. Lukes Medical Center, Chicago, Illinois 60612; 2Biomechanics Section, University of Nijmegen,
Institute of Orthopedics, Nijmegen, The Netherlands
Push-out and pull-out tests are used for destructive evaluation of implantbone interface strength. Because nondestructive mechanical tests would allow maintenance of an
intact interface for subsequent morphological study, we developed such a test to determine the shear modulus of the
interface by measuring the shear deformation of a thin layer
adjacent to the implant. A polyurethane foam model was
used to test the experimental setup on a group of nine cylindrical implants with three different lengths (1548 mm)
and three different diameters (59.7 mm). The shear modulus of the interface, as calculated from the pull-out test, was
validated against the shear modulus of the foam derived
from tensile tests. The two values of shear modulus were
well correlated (R2 = 0.8, p < 0.001), thus encouraging further
application of the setup for tests of implantbone interface
mechanics. In addition, we also examined the effects of implant length and diameter. The length of the implants had a
significant influence on the interface shear modulus (p <
0.05), indicating that comparisons of this variable should
only be made of implants with the same length. The length
and diameter of the implants were not critical parameters for
the ultimate fixation strength. 1997 John Wiley & Sons, Inc.
INTRODUCTION
tive about the type of tissues at the interface than the
strength obtained from destructive tests. Measurement of elastic properties is much more difficult than
measurement of the strength of fixation because the
interface zone constitutes only a thin layer (usually
less than 3 mm in most experiments).
It has been shown in push-out tests that certain test
conditions, such as the modulus of the implant and
the clearance of the hole in the supporting plate, can
affect the calculated strength.1 In pull-out tests, cylindrical implants varying from 5 to 9.7 mm in diameter
and from 15 to 48 mm in length have been used by
various laboratories.27 Because the stress distribution
along the interface is usually not uniform, particularly
for short implants, the actual strength values calculated from these tests may not be comparable.1,8 Similar limitations may apply to the interpretation of nondestructive interface modulus tests.
The purposes of the present study were to develop
a nondestructive mechanical test of the implanthost
bone interface shear modulus and to test the effects of
varying diameter and length of the implants on the
interface shear modulus and strength in trabecular
bone.
The mechanical competence of biological fixation of
orthopedic implants is most often characterized by the
strength of the implanthost interface. Usually, cylindrical plugs are tested after having been implanted in
vivo. The strength of fixation is determined by dividing the maximum force measured in a push-out or
pull-out test by the nominal surface area of the implant in contact with the host bone. Because these tests
are destructive, the ability to examine the intact interface after the test is lost, although it is still possible to
examine the implant itself or the host bed.
It would be helpful to have a nondestructive test to
characterize the mechanical behavior of the interface
so that mechanical and morphological assays of the
intact interface could be performed in the same specimen. Obviously, the strength of fixation cannot be determined nondestructively, but it should be possible to
determine the shear modulus of the interface zone. In
addition, the modulus may prove to be more sugges*To whom correspondence should be addressed.
Journal of Biomedical Materials Research, Vol. 34, 337340 (1997)
1997 John Wiley & Sons, Inc.
CCC 0021-9304/97/030337-04
338
BERZINS ET AL.
MATERIALS AND METHODS
A cylindrical steel implant with a diameter of 7 mm
and a length of 48 mm was machined. Fine threads
([40, U.S. standard) were used as a surface finish.
Polyurethane foam (RF-100, Daro Products, Butler,
WI) was used to simulate the surrounding bone. Foam
components underwent manual mixing for 1 min. Ten
foam bone models with 7 48 mm implants were
tested. Five of these foam bone models were made
using the manufacturers recommended ratio of 1.0
resin/0.9 isocyanate by weight. The other five models
were formed using an altered mixing ratio of 1.0
resin/1.5 isocyanate. The increased fraction of isocyanate reportedly raises the modulus of the foam product.9 Implants were coaxially held inside a 35-mm diameter aluminum split mold (Fig. 1) while premixed
foam was poured in the space between the implant
and the mold. Coarse threads ([8, U.S. standard) had
been machined on the inside of the mold to assure
interdigitation between the mold and the foam model
of the bone to assure a uniform stress transfer from the
mold to the bone model. Models were left to harden
for 24 h before the foam cylinder was retrieved from
the mold. Excess foam extending beyond the distal
portion of the implant was cut off. The model was refit
into the mold (1, Fig. 2), which was then used as a
holder for each model during the pull-out test. Tensile
force (F, Fig. 2) was applied to the implant (2, Fig. 2)
through a device consisting of an extended yoke (4,
Fig. 2) surrounded by a 20-mm diameter sliding sleeve
(5, Fig. 2), which was ground against the surface of the
foam model (3, Fig. 2) surrounding the implant. An
extensometer (6, Fig. 2) with a gauge length of 10 mm
and range of 1 (model 2620-830, Instron) sensed longitudinal displacements between the yoke and the
sleeve. Thus, in fact, the shear deformation in the thin
Figure 2. Experimental setup for a pull-out test (longitudinal cross section); 1, aluminum mold; 2, cylindrical implant;
3, foam model; 4, extended yoke; 5, sliding sleeve held
against the foam surface by springs; 6, extensometer; 7, foam
layer in which the interface shear modulus was measured;
and F, tensile force applied to the setup.
foam layer (7, Fig. 2) adjacent to the implant was
tested. Mechanical pull-out tests were performed on a
servohydraulic materials testing machine (model
1321, Instron) at a loading speed of 0.25 mm/min.
Loaddisplacement curves were recorded during each
test. The initial linear portion of the curve was used to
calculate the interface shear modules. Because the
measured displacement d can be expressed as
d=
R2
R1
gdr,
where g is the deformation due to shear, R1 is the
radius of the implant, and R2 is the radius of the
sleeve. When the shear stress is expressed as the axial
force over the area of the interface, the shear modulus
of the interface, Gif, can be expressed as
Gif = F
Figure 1. Split aluminum mold used to form foam models
and to hold them during pull-out tests. Shown inside the
mold are a foam model (sectioned longitudinally) with a
cylindrical implant.
ln R2 ln R1
,
2pdL
where F is the tensile force and L is the length of the
implant.
Because the foam was the only material present at
the implantbone interface in our model (7, Fig. 2), we
expected that the shear modulus of the interface foam
layer would be the same as the shear modulus of the
foam itself. Thus, for the purpose of validation, one
specimen was prepared from each foam model tested
to determine the tensile modulus. The tensile tests
were performed on cylindrical specimens machined to
ASTM standard E8 (gauge length of 25 mm and diameter of the waist portion of 6.25 mm) at 0.25 mm/
min and calculations were based on the linear part of
the load-deformation curve. The shear modulus of the
NONDESTRUCTIVE TESTS OF IMPLANTBONE INTERFACE STRENGTH
339
foam, Gfoam, was calculated according to normal isotropic material conditions using data from the tensile
test:
Gfoam =
E
2(1 + n)
where E is the axial modulus of the material and n is
Poissons ratio.
Poissons ratio of the foam was determined by compression loading of four cubic-shaped foam specimens
with two separate extensometers for simultaneous
measurements of the axial and transverse deformation. The average (SD) Poissons ratio of the foam
was 0.36 0.01. A linear regression was performed to
evaluate the relationship between the interface shear
modulus (Gif) and the shear modulus (Gfoam).
An additional eight cylindrical implants were machined to complete a set consisting of combinations of
three different diameters (5, 7, and 9.7 mm) and three
different lengths (15, 30, and 48 mm) for a total of nine
implant sizes. Foam models with the standard ratio
for components of 1.0 resin/0.9 isocyanate by
weight were used. In addition to the test for the interface shear modulus as described above, specimens
were tested to failure and the ultimate pull-out force
was recorded. The ultimate shear stress sult of the interface was calculated as
sult =
Fult
,
A
where Fult is the ultimate force and A is the nominal
surface area of the implant.
Each implant size was tested in five replicates for a
total of 45 foam bone models. Two-way analyses of
variance (ANOVA) were used to test for the effects of
the implant diameter and for the effect of implant
length. Separate analyses were applied to interface
shear modulus and to fixation strength. A significance
level of 0.05 was used.
Figure 3. Regression analysis between the shear modulus
of the foam (Gfoam) and shear modulus of the interface (Gif).
The solid line and R2 value represents the regular linear
regression. The dashed line and the regression equation represents a no-intercept model.
nificant influence on the ultimate shear stress of the
interface (Fig. 5). All failures in the pull-out tests occurred in the foam immediately adjacent to the implant; the threads on the implants always had attached
foam after the test.
DISCUSSION
The present study describes the development of a
nondestructive test to measure the shear modulus of
the interface zone of an implant placed in trabecular
bone. We chose this site, rather than cortical bone,
because most cementless joint replacement components are implanted in a trabecular bone bed. The elastic properties of the foam used in our study resemble
those of human cancellous bone.9 In addition, the average diameter of bubbles in the foam (between 200
and 300 mm)9 was similar to trabecular separation of
newly formed trabecular bone (between 300 and 400
RESULTS
The shear modulus as estimated from the tensile test
(Gfoam) was well correlated with the experimental
shear modulus of the interface based on the pull-out
tests (Gif) with R2 = 0.80 and p < 0.001. If we assume
that a no-intercept regression model can be applied
(Fig. 3), then the regression equation is
Gfoam = 1.01Gif.
The average (SD) tensile modulus of the foam models were 103 12 MPa (range 90121 MPa) for the
standard mixing ratio and 126 20 MPa (range 109
160 MPa) for the altered mixing ratio.
The shear modulus of the interface, as calculated
from the pull-out tests (Gif), was significantly affected
by the length of the implant (p < 0.05) (Fig. 4). Neither
the diameter nor the length of the implant had a sig-
Figure 4. Interface shear modulus as a function of implant
geometry.
340
BERZINS ET AL.
implants are in the range of lengths and diameters
tested in the present study.
The shear modulus of the interface zone is essentially uncharacterized. This information would be of
particular use as input into finite element models
where the nature of the connection between the implant and host can now only be roughly approximated. It can be argued that the shear modulus may
be more indicative of the tissue type at the interface
than the strength of fixation because dense fibrous
tissue can give a fixation strength at times approaching that given by bone ingrowth.4
This work was supported by NIH Grant RO1AR42862.
Figure 5.
etry.
Fixation strength as a function of implant geom-
References
mm) in a canine model. The site of failure during the
destructive portion of the tests (immediately adjacent
to the implant) was similar to that reported for pullout tests from a bone bed. The fixation strength in the
present study was comparable to the strength of biological fixation of similar cylindrical implants. Thus,
the present model is a good simulation of the biomechanical environment encountered during pull-out
tests from trabecular bone.
The shear modulus values obtained from the interface and values calculated from the tensile tests of
foam specimens were well correlated, thus encouraging further application of the setup for tests of implantbone interface mechanics. Based on the results
of the linear regression, one could extrapolate the results to bone tissue with an elastic modulus beyond
the range tested in this study (from 90 to 160 MPa).
It has been reported from theoretical models1,8,10
that interface stress around cylindrical implants is not
just a function of load and interface area, but depends
on the specific geometry (length and diameter). The
local effects at the ends of the implant substantially
affect the stress distribution, and a uniform distribution can only be expected along the middle portion of
the implant. However, experimental data from pushout and pull-out tests are often processed as if there
were a uniform stress distribution along the whole
length of the implant. If short cylinders are used,
stress distribution effects at the ends may overlap,
thus eliminating the middle portion, where the uniform interface stress calculations would have been applicable.
The length of the implants had a significant influence on the interface shear modulus, indicating that
comparisons should only be made of implants with
the same length. The length and diameter of the implants were not critical parameters for the ultimate
fixation strength. Thus, similar to results reported for
push-out tests,8 one can compare strength values from
pull-out tests of implants of different dimensions if the
7
1. W. J. A. Dhert, C. C. P. M. Verheyen, L. H. Braak, J. R.
de Wijn, C. P. A. T. Klein, K. de Groot, and P. M. Rozing, A finite element analysis of the push-out test:
Influence of test conditions, J. Biomed. Mater. Res., 26,
119130 (1992).
2. R. E. McLaughlin, S. I. Reger, M. Bolander, and H. C.
Eschenroeder, Enhancement of bone ingrowth by the
use of bone matrix as a biologic cement, Clin. Orthop.,
183, 255261 (1984).
3. C. L. Tisdel, V. M. Goldberg, J. A. Parr, J. S. Bensusan,
L. S. Staikoffs, and S. Stevenson, The influence of hydroxyapatite and tricalcium-phosphate coating on bone
growth in titanium fiber-metal implants, J. Bone Joint
Surg., 76A, 159171 (1994).
4. H. Kienapfel, D. R. Sumner, T. M. Turner, R. M. Urban,
and J. O. Galante, Efficacy of autograft and freezedried allograft to enhance fixation of porous coated implants in the presence of interface gaps, J. Orthop. Res.,
10, 423433 (1992).
5. D. R. Sumner, T. M. Turner, R. H. Pierson, H. Kienapfel, R. M. Urban, E. J. Liebner, and J. O. Galante,
Effects of radiation on fixation of non-cemented porous-coated implants in a canine model, J. Bone Joint
Surg., 72A, 15271533 (1990).
6. B. C. Callahan, E. J. Lisecki, R. E. Banks, J. E. Dalton,
S. D. Cook, and J. D. Wolff, The effect of warfarin on
the attachment of bone to hydroxyapatite-coated and
uncoated porous implants, J. Bone Joint Surg., 77A,
225230 (1995).
7. D. R. Sumner, T. M. Turner, A. F. Purchio, W. R. Gombotz, R. M. Urban, and J. O. Galante, Enhancement of
bone ingrowth by transforming growth factor beta, J.
Bone Joint Surg., 77A, 11351147 (1995).
8. T. P. Harrigan, J. Kareh, and W. H. Harris, The influence of support conditions in the loading fixture of
failure mechanisms in the push-out test: a finite element study, J. Orthop. Res., 8, 678684 (1990).
9. J. A. Szivek, M. Thomas, and J. B. Benjamin, Characterization of a synthetic foam as a model for human
cancellous bone, J. Appl. Biomater., 4, 269272 (1993).
10. T. E. Orr, S. L. Trillingand, and M. Spector, The testing
configuration for the most accurate determination of
shear strength at the implant/bone interface: the effect
of ingrowth, Trans SFB, XVIII, 373 (1995).
Received October 5, 1995
Accepted March 8, 1996
You might also like
- Implant Stability - Measuring DevicesDocument19 pagesImplant Stability - Measuring DevicesÁgnes Kocsis100% (1)
- Study Materials On Needles PDFDocument24 pagesStudy Materials On Needles PDFzilangamba_s4535No ratings yet
- ASTM Test Methods For GeotextilesDocument7 pagesASTM Test Methods For GeotextilesAaron HernandezNo ratings yet
- Basic Color TheoryDocument12 pagesBasic Color TheorysasankaNo ratings yet
- Shear Behavior of Thick Slabs-ACIDocument12 pagesShear Behavior of Thick Slabs-ACIJoão Paulo MendesNo ratings yet
- Overview of Gas Conditioning and ProcessingDocument14 pagesOverview of Gas Conditioning and ProcessingJOSE GONZALEZ VALERONo ratings yet
- Effects of Opening On The Behavior of Reinforced Concrete Beam I011275261Document10 pagesEffects of Opening On The Behavior of Reinforced Concrete Beam I01127526101010No ratings yet
- MODULE-11 Human Person As Oriented Towards Their Impending DeathDocument18 pagesMODULE-11 Human Person As Oriented Towards Their Impending DeathRoyceNo ratings yet
- 21st Bomber Command Tactical Mission Report 64, 65, OcrDocument57 pages21st Bomber Command Tactical Mission Report 64, 65, OcrJapanAirRaidsNo ratings yet
- Medical Development PowerPoint TemplateDocument16 pagesMedical Development PowerPoint TemplatesugamNo ratings yet
- Analysis of TMJ Replacement Using A Finite Element Model: Article InformationDocument5 pagesAnalysis of TMJ Replacement Using A Finite Element Model: Article Information100623No ratings yet
- Evaluation of The Tensile Strength of SFRC As Derived From Inverse Analysis of Notched Bending TestsDocument9 pagesEvaluation of The Tensile Strength of SFRC As Derived From Inverse Analysis of Notched Bending TestsJakob FiskerNo ratings yet
- Increase of Pullout Strength of Spinal Pedicle Screws With Conical Core: Biomechanical Tests and Finite Element AnalysesDocument7 pagesIncrease of Pullout Strength of Spinal Pedicle Screws With Conical Core: Biomechanical Tests and Finite Element AnalysesJavier Antonio Cardenas OliverosNo ratings yet
- (2004 Himmlova ) Influence of Implant Length and Diameter On Stress Distribution - A Finite Element AnalysisDocument6 pages(2004 Himmlova ) Influence of Implant Length and Diameter On Stress Distribution - A Finite Element Analysisyena1010No ratings yet
- Size Effects in Ductile Cellular Solid 2Document13 pagesSize Effects in Ductile Cellular Solid 2ulsanbada9343No ratings yet
- Shear Behaviour of Ferrocement Plates: Ms. Madhuri N. Savale, Prof. P. M. AlandkarDocument5 pagesShear Behaviour of Ferrocement Plates: Ms. Madhuri N. Savale, Prof. P. M. Alandkarluvjoshi1989No ratings yet
- Of Of: Evaluation Strain Terminal Abutmentsite Fixed Mandibular Prosthesis During Cantilever LoadingDocument10 pagesOf Of: Evaluation Strain Terminal Abutmentsite Fixed Mandibular Prosthesis During Cantilever Loadingjinny1_0No ratings yet
- Platform SwitchingDocument7 pagesPlatform SwitchingFernando CursachNo ratings yet
- Bond Strength of Dental Bracket The Finite Element Method: A Tool To Evaluate ShearDocument7 pagesBond Strength of Dental Bracket The Finite Element Method: A Tool To Evaluate ShearSundaraPandiyanNo ratings yet
- Stress Distribution in The Abutment and Retention Screw of A Single Implant Supporting A Prosthesis With Platform SwitchingDocument10 pagesStress Distribution in The Abutment and Retention Screw of A Single Implant Supporting A Prosthesis With Platform SwitchingMarlene Kasumi Gantier TakanoNo ratings yet
- In Vitro Degradation of Polyurethane Orthodontic Elastomeric Modules. BJO, 1999Document6 pagesIn Vitro Degradation of Polyurethane Orthodontic Elastomeric Modules. BJO, 1999Eryson Thiago PradoNo ratings yet
- EffectDocument8 pagesEffectelouis2No ratings yet
- Stress Distribution On The Prosthetic Screws in The All-On-4 Concept: A Three-Dimensional Finite Element AnalysisDocument10 pagesStress Distribution On The Prosthetic Screws in The All-On-4 Concept: A Three-Dimensional Finite Element AnalysisMario Troncoso AndersennNo ratings yet
- The Effect of Working Length, Fracture, and Screw Con Figuration On Plate Strain in A 3.5-mm LCP Bone Model of Comminuted FracturesDocument14 pagesThe Effect of Working Length, Fracture, and Screw Con Figuration On Plate Strain in A 3.5-mm LCP Bone Model of Comminuted FracturesEric RothNo ratings yet
- Parametric Studies of Steel Cold-Formed Section Beam To Column Moment Connections With Self-Drilling ScrewsDocument11 pagesParametric Studies of Steel Cold-Formed Section Beam To Column Moment Connections With Self-Drilling ScrewsAhmed SalehNo ratings yet
- Li 2011Document11 pagesLi 2011Hurāirāh ĐāřNo ratings yet
- J Korean Acad Conserv DentDocument22 pagesJ Korean Acad Conserv Dentsweet_apple921587No ratings yet
- Symmetry 11 01349 PDFDocument10 pagesSymmetry 11 01349 PDFEstebanNo ratings yet
- Stress Distribution in Roots Restored With Different Types of Post Systems With Composite ResinDocument7 pagesStress Distribution in Roots Restored With Different Types of Post Systems With Composite ResindmasuokaNo ratings yet
- 3153-Blinded Manuscript-23383-1-10-20200923Document8 pages3153-Blinded Manuscript-23383-1-10-20200923EstebanNo ratings yet
- Biomechanical Effects of Offset Placement of Dental Implants in The Edentulous Posterior MandibleDocument13 pagesBiomechanical Effects of Offset Placement of Dental Implants in The Edentulous Posterior MandibleDiamanta Yalomit CirsteaNo ratings yet
- Thread Pitch Variant in Orthodontic Mini-Screws: A 3-D Finite Element AnalysisDocument10 pagesThread Pitch Variant in Orthodontic Mini-Screws: A 3-D Finite Element AnalysisRebin AliNo ratings yet
- Influência Do Tipo de Rosca No Torque de Remoção Dos Mini-Implantes - HongDocument8 pagesInfluência Do Tipo de Rosca No Torque de Remoção Dos Mini-Implantes - HongUrsula Pantigozo MoránNo ratings yet
- Evaluation of Stresses Developed in Different Bracket-Cement-Enamel Systems Using Finite Element Analysis With in Vitro Bond Strength TestsDocument8 pagesEvaluation of Stresses Developed in Different Bracket-Cement-Enamel Systems Using Finite Element Analysis With in Vitro Bond Strength TestsMuhammad AdnanNo ratings yet
- Module 5 - Testing of Composites - IIDocument22 pagesModule 5 - Testing of Composites - IIP20MF010MANGESH SHARMANo ratings yet
- Bone Stress When Miniplates Are Used For OrthodontDocument7 pagesBone Stress When Miniplates Are Used For OrthodontNicolasFernandezNo ratings yet
- TMP 5387Document7 pagesTMP 5387FrontiersNo ratings yet
- E EignungsprufungDocument8 pagesE EignungsprufungMehdi BakhshiNo ratings yet
- Experimental Measurement of Gear Mesh Stiffness of Cracked Spur Gear by Strain Gauge TechniqueDocument10 pagesExperimental Measurement of Gear Mesh Stiffness of Cracked Spur Gear by Strain Gauge TechniqueRudolph ScheepersNo ratings yet
- OgBayrak - Response Prediction by Plastic Hinge AnalysisDocument6 pagesOgBayrak - Response Prediction by Plastic Hinge AnalysisRui CbNo ratings yet
- Effect of Various Bone Thickness On Stress Distribution at The Bone-Implant Interface Using Numerical Simulation TechniqueDocument8 pagesEffect of Various Bone Thickness On Stress Distribution at The Bone-Implant Interface Using Numerical Simulation TechniqueaDITYA GUJARENo ratings yet
- Finite Element Analysis of Miniscrew Implants Used For Orthodontic AnchorageDocument9 pagesFinite Element Analysis of Miniscrew Implants Used For Orthodontic Anchoragemanju deviNo ratings yet
- Vol 2 Bep 5Document10 pagesVol 2 Bep 5namasse.medamineNo ratings yet
- Resistencia Mecanica de La Fibra de VidrioDocument8 pagesResistencia Mecanica de La Fibra de VidriozayraNo ratings yet
- Short Fiber Reinforced Composite The Effect of Fiber Length and Volume FractionDocument10 pagesShort Fiber Reinforced Composite The Effect of Fiber Length and Volume FractionMiranti AuliaNo ratings yet
- Experimental Investigation On Possible Dependence of Plastic Zone Size On Specimen GeometryDocument8 pagesExperimental Investigation On Possible Dependence of Plastic Zone Size On Specimen Geometryanon_154169983No ratings yet
- Study of A Uniaxial Tension Test MethodologyDocument28 pagesStudy of A Uniaxial Tension Test MethodologyJuan Diego Vargas MendozaNo ratings yet
- Dynamic Frictional Behaviour of Orthodontic Archwires and BracketsDocument9 pagesDynamic Frictional Behaviour of Orthodontic Archwires and BracketsAstrid Carolina HerreraNo ratings yet
- Bearing Strength of Carbon Fibre - Epoxy Laminates - Effects of Bolt-Hole Clearance - ScienceDirectDocument10 pagesBearing Strength of Carbon Fibre - Epoxy Laminates - Effects of Bolt-Hole Clearance - ScienceDirectnitheeshgmenon5No ratings yet
- Tsumita 2013Document5 pagesTsumita 2013JesusCordobaNo ratings yet
- 27-Effect of Voids On Tensile StrengthDocument5 pages27-Effect of Voids On Tensile StrengthMuhammad TouheedNo ratings yet
- 36 Ijmperddec201836Document8 pages36 Ijmperddec201836TJPRC PublicationsNo ratings yet
- Mini Impantes Elementos FinitosDocument11 pagesMini Impantes Elementos FinitosDaniela Rizo AlvarezNo ratings yet
- Wesep Weml Reu PosterDocument1 pageWesep Weml Reu Posterapi-260130592No ratings yet
- Mechanical Properties of Nitinol Stents and Stent-Grafts: Comparison of 6 MM Diameter DevicesDocument16 pagesMechanical Properties of Nitinol Stents and Stent-Grafts: Comparison of 6 MM Diameter DevicesDeva RajNo ratings yet
- Joddd 13 85Document10 pagesJoddd 13 85Panaite TinelaNo ratings yet
- International Journal of Adhesion & Adhesives: Xiaocong HeDocument8 pagesInternational Journal of Adhesion & Adhesives: Xiaocong HeSatish KumarNo ratings yet
- Evaluation of Different in Vitro Testing Methods For Mechanical Properties of Veneer CeramicsDocument8 pagesEvaluation of Different in Vitro Testing Methods For Mechanical Properties of Veneer CeramicsDrg Sri Pandu UtamiNo ratings yet
- Evaluation of Design Parameters of Eight Dental Implant Designs: A Two-Dimensional Finite Element AnalysisDocument6 pagesEvaluation of Design Parameters of Eight Dental Implant Designs: A Two-Dimensional Finite Element AnalysisRadu PopescuNo ratings yet
- The Effect of Different Bone Level and Prosthetic Connection On The Biomechanical Response of Unitary Implants: Strain Gauge and Finite Element AnalysesDocument7 pagesThe Effect of Different Bone Level and Prosthetic Connection On The Biomechanical Response of Unitary Implants: Strain Gauge and Finite Element AnalysesIJAERS JOURNALNo ratings yet
- Wang 2014Document7 pagesWang 2014Dedy SetiawanNo ratings yet
- Factors Affecting On Springback in Sheet Metal Bending: A ReviewDocument5 pagesFactors Affecting On Springback in Sheet Metal Bending: A Reviewkhudhayer1970No ratings yet
- Short ImplantsFrom EverandShort ImplantsBoyd J. TomasettiNo ratings yet
- The Fatigue Strength of Transverse Fillet Welded Joints: A Study of the Influence of Joint GeometryFrom EverandThe Fatigue Strength of Transverse Fillet Welded Joints: A Study of the Influence of Joint GeometryNo ratings yet
- The Mechanical Properties of Wood: Including a Discussion of the Factors Affecting the Mechanical Properties, and Methods of Timber TestingFrom EverandThe Mechanical Properties of Wood: Including a Discussion of the Factors Affecting the Mechanical Properties, and Methods of Timber TestingNo ratings yet
- Gepi 1370100621Document5 pagesGepi 1370100621Lata DeshmukhNo ratings yet
- BF 01456737Document8 pagesBF 01456737Lata DeshmukhNo ratings yet
- A Homogenous Assay of FAD Using A Binding Between Apo-Glucose Oxidase and FAD Labeled Withan Electroactive CompoundDocument6 pagesA Homogenous Assay of FAD Using A Binding Between Apo-Glucose Oxidase and FAD Labeled Withan Electroactive CompoundLata DeshmukhNo ratings yet
- Electrochemical and Catalytic Properties of The Adenine Coenzymes FAD and Coenzyme A On Pyrolytic Graphite ElectrodesDocument7 pagesElectrochemical and Catalytic Properties of The Adenine Coenzymes FAD and Coenzyme A On Pyrolytic Graphite ElectrodesLata DeshmukhNo ratings yet
- (Micro) Fads Asset Evidence: FuturesDocument23 pages(Micro) Fads Asset Evidence: FuturesLata DeshmukhNo ratings yet
- BF 00314252Document2 pagesBF 00314252Lata DeshmukhNo ratings yet
- Infrared Spectroscopic Study of Thermally Treated LigninDocument4 pagesInfrared Spectroscopic Study of Thermally Treated LigninLata DeshmukhNo ratings yet
- Factor Analysis of Spectroelectrochemical Reduction of FAD Reveals The P K of The Reduced State and The Reduction PathwayDocument9 pagesFactor Analysis of Spectroelectrochemical Reduction of FAD Reveals The P K of The Reduced State and The Reduction PathwayLata DeshmukhNo ratings yet
- Covalent Immobilization of and Glucose Oxidase On Carbon ElectrodesDocument5 pagesCovalent Immobilization of and Glucose Oxidase On Carbon ElectrodesLata DeshmukhNo ratings yet
- Fid, Fads: If Cordorate Governance Is A We Need MoreDocument1 pageFid, Fads: If Cordorate Governance Is A We Need MoreLata DeshmukhNo ratings yet
- Spectroscopic Study of The Molecular Structure of A Lignin-Polymer SystemDocument5 pagesSpectroscopic Study of The Molecular Structure of A Lignin-Polymer SystemLata DeshmukhNo ratings yet
- Spectroscopic Study of Intermolecular Complexes Between FAD and Some Fl-Carboline DerivativesDocument5 pagesSpectroscopic Study of Intermolecular Complexes Between FAD and Some Fl-Carboline DerivativesLata DeshmukhNo ratings yet
- Apj 526Document7 pagesApj 526Lata DeshmukhNo ratings yet
- Task Group Osition Paper On Unbiased Assessment of CulturallyDocument5 pagesTask Group Osition Paper On Unbiased Assessment of CulturallyLata DeshmukhNo ratings yet
- Spectroscopic Study of Molecular Associations Between Flavins FAD and RFN and Some Indole DerivativesDocument6 pagesSpectroscopic Study of Molecular Associations Between Flavins FAD and RFN and Some Indole DerivativesLata DeshmukhNo ratings yet
- Editorial: Etiology Nutritional Fads: WilliamDocument4 pagesEditorial: Etiology Nutritional Fads: WilliamLata DeshmukhNo ratings yet
- Production of Recombinant Cholesterol Oxidase Containing Covalently Bound FAD in Escherichia ColiDocument10 pagesProduction of Recombinant Cholesterol Oxidase Containing Covalently Bound FAD in Escherichia ColiLata DeshmukhNo ratings yet
- Amperometric Assay Based On An Apoenzyme Signal Amplified Using NADH For The Detection of FADDocument4 pagesAmperometric Assay Based On An Apoenzyme Signal Amplified Using NADH For The Detection of FADLata DeshmukhNo ratings yet
- Integrated Project Development Teams: Another F A D - ., or A Permanent ChangeDocument6 pagesIntegrated Project Development Teams: Another F A D - ., or A Permanent ChangeLata DeshmukhNo ratings yet
- FAD Used As A Mediator in The Electron Transfer Between Platinum and Several BiomoleculesDocument11 pagesFAD Used As A Mediator in The Electron Transfer Between Platinum and Several BiomoleculesLata DeshmukhNo ratings yet
- Raman Scattering in Tellurium-Metal Oxyde Glasses: Journal of Molecular Structure 349 (1995) 413-416Document4 pagesRaman Scattering in Tellurium-Metal Oxyde Glasses: Journal of Molecular Structure 349 (1995) 413-416Lata DeshmukhNo ratings yet
- A Rapid Micromethod For Determination of FMN and FAD in MixturesDocument5 pagesA Rapid Micromethod For Determination of FMN and FAD in MixturesLata DeshmukhNo ratings yet
- A Defense of Popular Culture: Brustein, Munson, Rothstein, Simon, Nichols, Kimball, and Pinsker 73Document6 pagesA Defense of Popular Culture: Brustein, Munson, Rothstein, Simon, Nichols, Kimball, and Pinsker 73Lata DeshmukhNo ratings yet
- Sce 20287Document3 pagesSce 20287Lata DeshmukhNo ratings yet
- J Religion 2003 11 003Document2 pagesJ Religion 2003 11 003Lata DeshmukhNo ratings yet
- DOI 10.1007/s12138-009-0064-z: © Springer Science+Business Media B.V. 2008Document5 pagesDOI 10.1007/s12138-009-0064-z: © Springer Science+Business Media B.V. 2008Lata DeshmukhNo ratings yet
- Contrasting Zones of Comfortable Competence: Popular Culture in A Phonics LessonDocument15 pagesContrasting Zones of Comfortable Competence: Popular Culture in A Phonics LessonLata DeshmukhNo ratings yet
- PERDEV Week3Document26 pagesPERDEV Week3Coulline DamoNo ratings yet
- 839-4816 (Office) or (770) 301-8648 (Cell) : Corporate Finance: A Focused Approach, by Michael C. Ehrhardt / Eugene FDocument1 page839-4816 (Office) or (770) 301-8648 (Cell) : Corporate Finance: A Focused Approach, by Michael C. Ehrhardt / Eugene FlilbouyinNo ratings yet
- Nora Alexander: ProfileDocument1 pageNora Alexander: ProfilenorajuliaalexanderNo ratings yet
- Psycopathy Case StudyDocument8 pagesPsycopathy Case StudyNayab NoorNo ratings yet
- E Katalog 2019Document15 pagesE Katalog 2019Dwi Putri BastiyantiNo ratings yet
- Improved Mini-Silo For Studying Fermentation of Silage in Laboratory ConditionsDocument8 pagesImproved Mini-Silo For Studying Fermentation of Silage in Laboratory ConditionsCk_psihNo ratings yet
- Tanuj CVDocument2 pagesTanuj CVVikram Pratap SinghNo ratings yet
- Lambeth College: School of Science & Dental Technology Assignment Front SheetDocument5 pagesLambeth College: School of Science & Dental Technology Assignment Front SheetWillson DjohnNo ratings yet
- A Report: Smt. Shantaben Haribhai Gajera Engineering CollegeDocument5 pagesA Report: Smt. Shantaben Haribhai Gajera Engineering CollegePranav. ThubeNo ratings yet
- Module 2.1 Cultural Relativism-1Document20 pagesModule 2.1 Cultural Relativism-1Blad AnneNo ratings yet
- Bushman 2005Document8 pagesBushman 2005SOULAIMANE EZZOUINENo ratings yet
- Dynasylan BSM 40%Document3 pagesDynasylan BSM 40%Francois-No ratings yet
- Curl (Mathematics) - Wikipedia, The Free EncyclopediaDocument13 pagesCurl (Mathematics) - Wikipedia, The Free EncyclopediasoumyanitcNo ratings yet
- Incubator GinevriDocument24 pagesIncubator GinevriDivino Elisanto SitinjakNo ratings yet
- 1.draw The Circuit Diagram of A Mod-16 Asynchronous Counter and Explain Its Working WithDocument4 pages1.draw The Circuit Diagram of A Mod-16 Asynchronous Counter and Explain Its Working WithRajeshwari SNo ratings yet
- Practices Venn DiagramDocument2 pagesPractices Venn DiagramNathanNo ratings yet
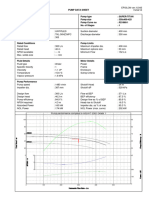
- TKL Pump - Data - SheetDocument1 pageTKL Pump - Data - Sheetธนาชัย เต็งจิรธนาภาNo ratings yet
- French 75-MM. GUN: NotesDocument12 pagesFrench 75-MM. GUN: NotesFabrizio De PetrilloNo ratings yet
- Program in Less Than 24 MonthsDocument2 pagesProgram in Less Than 24 MonthsHermi BurquesNo ratings yet
- Q4 TLE AFA Horticulture 9 Week3Document4 pagesQ4 TLE AFA Horticulture 9 Week3Dash Bello100% (1)
- LR Chapter 5 - Input and OutputDocument6 pagesLR Chapter 5 - Input and OutputAakash KumarNo ratings yet
- SY2021 2022 2ndsemesterDocument2 pagesSY2021 2022 2ndsemesterWilfredo III DayagdagNo ratings yet
- Asus X550JF x550jxDocument7 pagesAsus X550JF x550jxCiprian BalalauNo ratings yet
- Be11 enDocument12 pagesBe11 enSaqlain Mir100% (1)
- ENaresh BossBabu GRahul 33Document6 pagesENaresh BossBabu GRahul 33anthonyNo ratings yet